Comparative Efficacy of Active Group Music Intervention versus Group Music Listening in Alzheimer’s Disease
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Research Design, Procedure, and Interventions
- Welcome song. At the beginning of each session, residents had to greet and introduce themselves. This activity was selected to create an atmosphere of trust and facilitate residents’ interaction.
- Rhythmic exercises. For this activity, three well-known songs were used. The music facilitator and the residents had to keep the songs’ rhythm by clapping their hands each time they heard the chorus. For example, in the song “Quizás, quizás, quizás”, by Nat King Cole, residents had to clap their hands each time the singer says “quizás.”
- Dance exercises. In this activity, three songs were used. The facilitator encouraged residents to make free body movements in response to music and facilitated residents dancing by reflecting or amplifying their spontaneous movements. Besides, they tried to engage residents more reluctant to participate by talking to them or making eye contact.
- Music quiz. For this task, the residents were divided into two teams. A list of four songs was played. Each team should guess the songs’ names. Then, the facilitator encouraged residents to name the singer as well. Finally, the facilitator and the residents sang the chorus of the song. This activity aimed to facilitate interaction among residents as well as improve semantic and autobiographical memory.
- Goodbye song. At the end of each session, residents said goodbye to the group.
2.3. Outcome Measures
2.4. Statistical Analysis
3. Results
3.1. Baseline Assessment
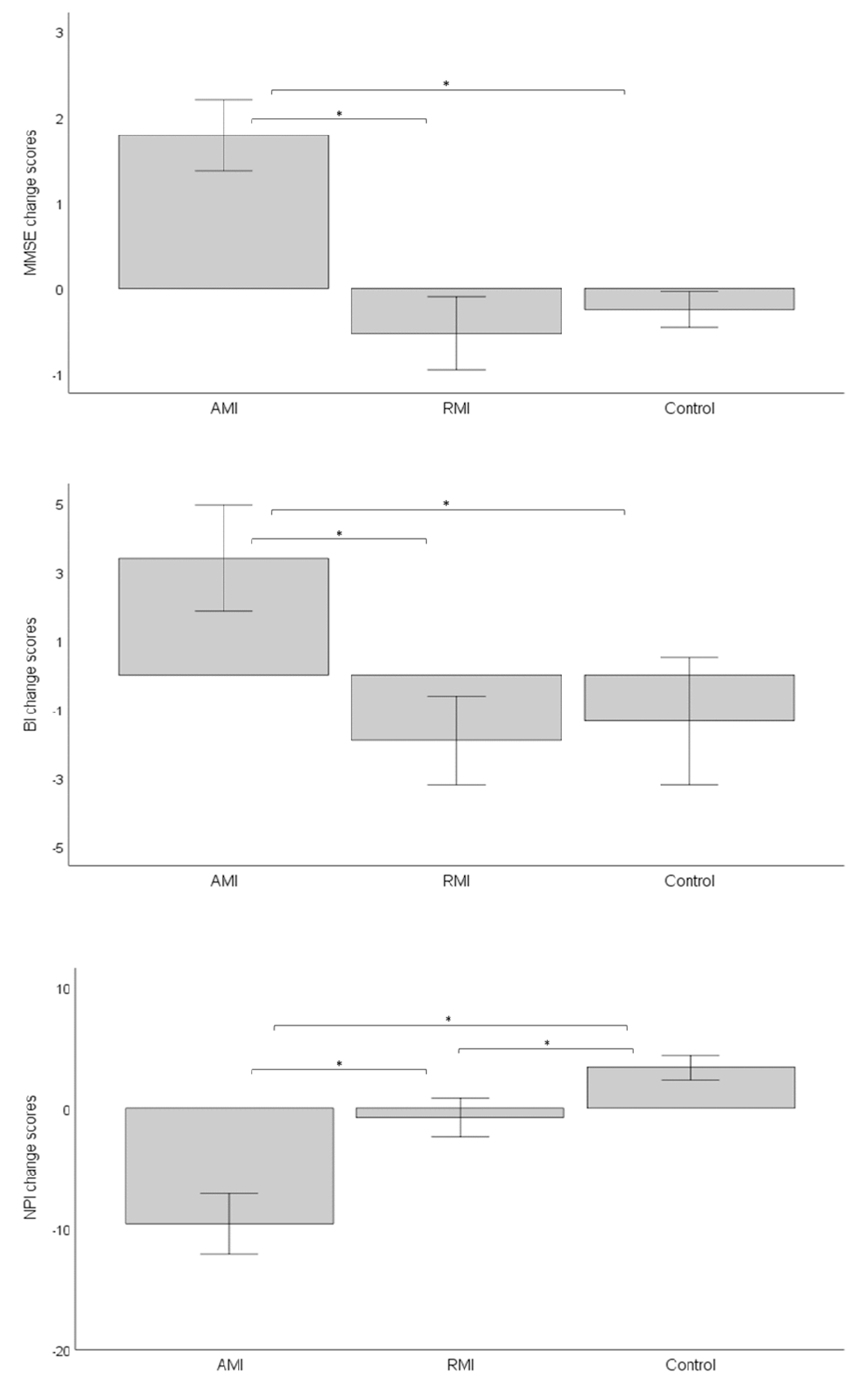
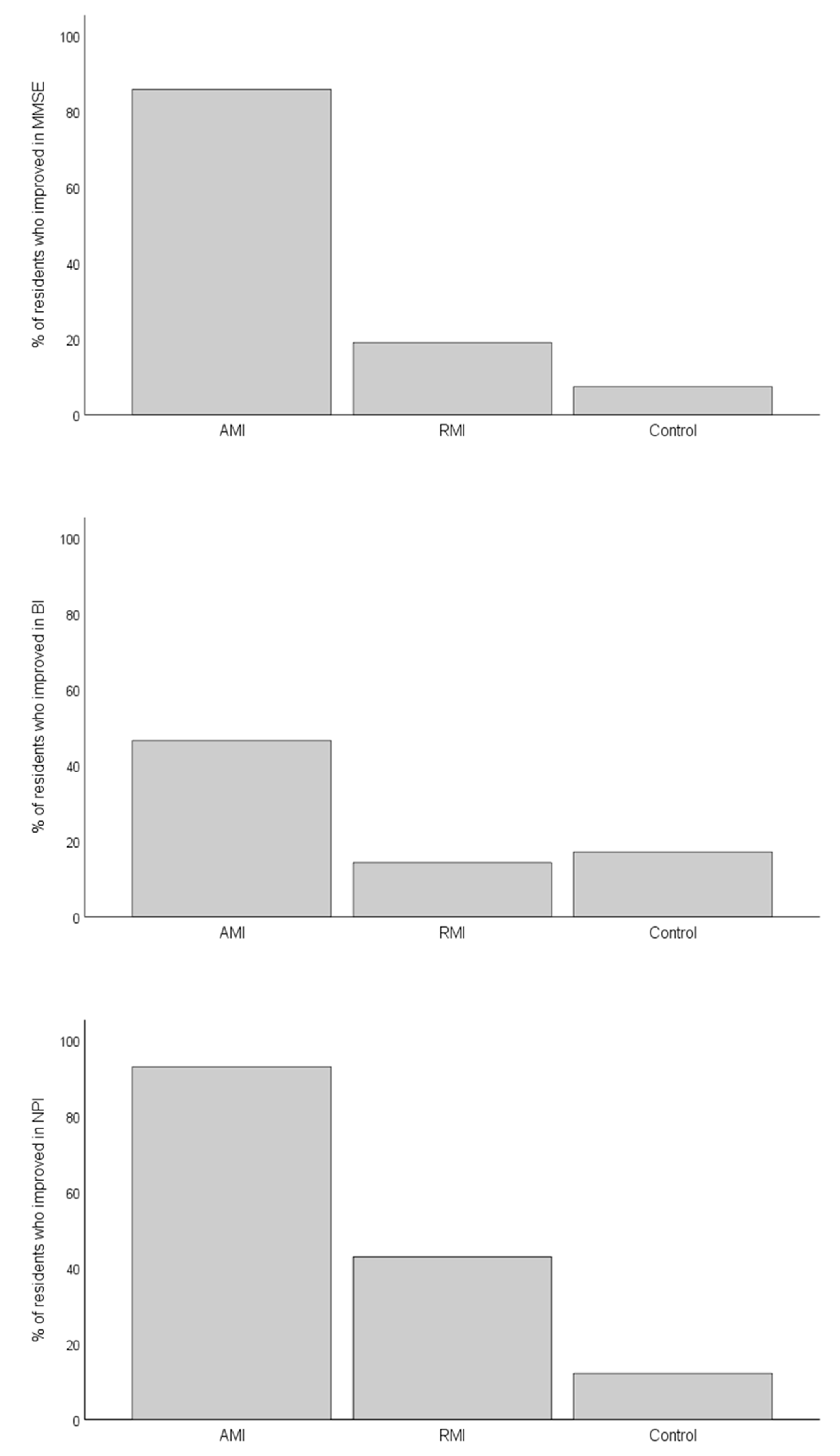
3.2. Efficacy of Music-Based Interventions
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Nichols, E. Global, regional, and national burden of Alzheimer’s disease and other dementias, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019, 18, 88–106. [Google Scholar] [CrossRef] [Green Version]
- Olazarán, J.; Agüera-Ortiz, L.; Argimón, J.M.; Reed, C.; Ciudad, A.; Andrade, P.; Dilla, T. Costs and quality of life in community-dwelling patients with Alzheimer’s disease in Spain: Results from the GERAS II observational study. Int. Psychogeriatr. 2017, 29, 2081–2093. [Google Scholar] [CrossRef] [PubMed]
- Dubois, B.; Padovani, A.; Scheltens, P.; Rossi, A.; Dell’Agnello, G. Timely Diagnosis for Alzheimer’s Disease: A Literature Review on Benefits and Challenges. J. Alzheimer’s Dis. 2015, 49, 617–631. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Choi, J.; Twamley, E.W. Cognitive Rehabilitation Therapies for Alzheimer’s Disease: A Review of Methods to Improve Treatment Engagement and Self-Efficacy. Neuropsychol. Rev. 2013, 23, 48–62. [Google Scholar] [CrossRef] [Green Version]
- Gonzalez-Hoelling, S.; Bertran-Noguer, C.; Reig-Garcia, G.; Suñer-Soler, R. Effects of a Music-Based Rhythmic Auditory Stimulation on Gait and Balance in Subacute Stroke. Int. J. Environ. Res. Public Health 2021, 18, 2032. [Google Scholar] [CrossRef]
- Schlaug, G. Part VI Introduction: Listening to and making music facilitates brain recovery processes. Ann. N. Y. Acad. Sci. 2009, 1169, 372–373. [Google Scholar] [CrossRef]
- Thoma, M.V.; La Marca, R.; Brönnimann, R.; Finkel, L.; Ehlert, U.; Nater, U.M. The Effect of Music on the Human Stress Response. PLoS ONE 2013, 8, e70156. [Google Scholar] [CrossRef] [Green Version]
- Thompson, W.; Schlaug, G. The Healing Power of Music. Sci. Am. Mind 2015, 26, 32–41. [Google Scholar] [CrossRef]
- Sixsmith, A.; Gibson, G. Music and the wellbeing of people with dementia. Ageing Soc. 2006, 27, 127–145. [Google Scholar] [CrossRef]
- Guétin, S.; Portet, F.; Picot, M.; Pommié, C.; Messaoudi, M.; Djabelkir, L.; Olsen, A.; Cano, M.; Lecourt, E.; Touchon, J. Effect of Music Therapy on Anxiety and Depression in Patients with Alzheimer’s Type Dementia: Randomised, Controlled Study. Dement. Geriatr. Cogn. Disord. 2009, 28, 36–46. [Google Scholar] [CrossRef]
- Sakamoto, M.; Ando, H.; Tsutou, A. Comparing the effects of different individualized music interventions for elderly individuals with severe dementia. Int. Psychogeriatr. 2013, 25, 775–784. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.M.; Tims, F.; Cruess, D.G.; Mintzer, M.J.; Ironson, G.; Loewenstein, D.; Cattan, R.; Fernandez, J.B.; Eisdorfer, C.; Kumar, M. Music therapy increases serum melatonin levels in patients with Alzheimer’s disease. Altern. Ther. Health Med. 1999, 5, 49–57. [Google Scholar]
- Vink, A.C.; Zuidersma, M.; Boersma, F.; De Jonge, P.; Zuidema, S.U.; Slaets, J.P.J. The effect of music therapy compared with general recreational activities in reducing agitation in people with dementia: A randomised controlled trial. Int. J. Geriatr. Psychiatry 2012, 28, 1031–1038. [Google Scholar] [CrossRef]
- Lyu, J.; Gao, T.; Li, M.; Xie, L.; Li, W.; Jin, W.; Hao, Z.; Mu, H. The effect of music therapy on memory, language, and psychological symptoms of patients with mild Alzheimer’s disease. Chin. J. Neurol. 2014, 47, 831–835. [Google Scholar]
- Arroyo-Anlló, E.M.; Díaz, J.P.; Gil, R. Familiar Music as an Enhancer of Self-Consciousness in Patients with Alzheimer’s Disease. BioMed Res. Int. 2013, 2013, 752965. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gallego, M.G.; García, J.G. Music therapy and Alzheimer’s disease: Cognitive, psychological, and behavioural effects. Neurología 2017, 32, 300–308. [Google Scholar] [CrossRef]
- Bruer, R.A.; Spitznagel, E.; Cloninger, C.R. The temporal limits of cognitive change from music therapy in elderly people with dementia or dementia-like cognitive impairment: A randomized controlled trial. J. Music Ther. 2007, 44, 308–328. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Morales, C.; Calero, R.; Moreno-Morales, P.; Pintado, C. Music Therapy in the Treatment of Dementia: A Systematic Review and Meta-Analysis. Front. Med. 2020, 7, 160. [Google Scholar] [CrossRef]
- American Music Therapy Association. What Is Music Therapy. 2020. Available online: https://www.musictherapy.org/about/musictherapy/ (accessed on 29 July 2021).
- Li, H.-C.; Wang, H.-H.; Lu, C.-Y.; Chen, T.-B.; Lin, Y.-H.; Lee, I. The effect of music therapy on reducing depression in people with dementia: A systematic review and meta-analysis. Geriatr. Nurs. 2019, 40, 510–516. [Google Scholar] [CrossRef] [PubMed]
- Silverman, M.J. Music Therapy in Mental Health for Illness Management and Recovery; Oxford University Press: Oxford, UK, 2015. [Google Scholar]
- Jacobsen, J.H.; Stelzer, J.; Fritz, T.H.; Chetelat, G.; La Joie, R.; Turner, R. Why musical memory can be preserved in advanced Alzheimer’s disease. Brain 2015, 138, 2438–2450. [Google Scholar] [CrossRef] [Green Version]
- Särkämö, T.; Laitinen, S.; Numminen, A.; Kurki, M.; Johnson, J.K.; Rantanen, P. Pattern of Emotional Benefits Induced by Regular Singing and Music Listening in Dementia. J. Am. Geriatr. Soc. 2016, 64, 439–440. [Google Scholar] [CrossRef]
- Särkämö, T.; Laitinen, S.; Numminen, A.; Kurki, M.; Johnson, J.K.; Rantanen, P. Clinical and Demographic Factors Associated with the Cognitive and Emotional Efficacy of Regular Musical Activities in Dementia. J. Alzheimer’s Dis. 2015, 49, 767–781. [Google Scholar] [CrossRef] [PubMed]
- Särkämö, T.; Tervaniemi, M.; Laitinen, L.S.; Numminen, A.; Kurki, M.; Johnson, J.K.; Rantanen, P. Cognitive, Emotional, and Social Benefits of Regular Musical Activities in Early Dementia: Randomized Controlled Study. Gerontologist 2013, 54, 634–650. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Raglio, A.; Bellandi, D.; Baiardi, P.; Ma, M.G.; Ubezio, M.C.; Zanacchi, E.; Granieri, E.; Imbriani, M.; Stramba-Badiale, M. Effect of Active Music Therapy and Individualized Listening to Music on Dementia: A Multicenter Randomized Controlled Trial. J. Am. Geriatr. Soc. 2015, 63, 1534–1539. [Google Scholar] [CrossRef]
- Raglio, A.; Bellandi, D.; Baiardi, P.; Gianotti, M.; Ubezio, M.C.; Granieri, E. Listening to Music and Active Music Therapy in Behavioral Disturbances in Dementia: A Crossover Study. J. Am. Geriatr. Soc. 2013, 61, 645–647. [Google Scholar] [CrossRef]
- Tsoi, K.K.; Chan, J.Y.; Ng, Y.-M.; Lee, M.M.; Kwok, T.C.; Wong, S.Y.-S. Receptive Music Therapy Is More Effective than Interactive Music Therapy to Relieve Behavioral and Psychological Symptoms of Dementia: A Systematic Review and Meta-Analysis. J. Am. Med. Dir. Assoc. 2018, 19, 568–576.e3. [Google Scholar] [CrossRef] [PubMed]
- Hughes, C.P.; Berg, L.; Danziger, W.L.; Coben, L.A.; Martin, R.L. A New Clinical Scale for the Staging of Dementia. Br. J. Psychiatry 1982, 140, 566–572. [Google Scholar] [CrossRef]
- Mercadal-Brotons, M.; Martí Augé, P. Manual de Musicoterapia en Geriatría y Demencias; Monsa-Prayma: La Coruña, Spain, 2008. [Google Scholar]
- Folstein, M.F.; Folstein, S.E.; McHugh, P.R. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 1975, 12, 189–198. [Google Scholar] [CrossRef]
- Blesa, R.; Pujol, M.; Aguila, M. Clinical validity of the “mini-Mental State” for Spanish-speaking communities. Tests Neuropsicol. 2004, 2, 31–35. [Google Scholar] [CrossRef]
- Cummings, J.L.; Mega, M.; Gray, K.; Rosenberg-Thompson, S.; Carusi, D.A.; Gornbein, J. The Neuropsychiatric Inventory: Comprehensive assessment of psychopathology in dementia. Neurology 1994, 44, 2308. [Google Scholar] [CrossRef] [Green Version]
- Yesavage, J.A. Geriatric Depression Scale. Psychopharmacol Bull. 1988, 24, 709–711. [Google Scholar]
- Lucas-Carrasco, R. Spanish version of the Geriatric Depression Scale: Reliability and validity in people with mild–moderate dementia. Int. Psychogeriatr. 2012, 24, 1284–1290. [Google Scholar] [CrossRef]
- Mahoney, F.I.; Barthel, D.W. Functional evaluation: The Barthel Index. Md. State Med. J. 1965, 14, 61–65. [Google Scholar]
- González, N.; Bilbao, A.; Forjaz, M.J.; Ayala, A.; Orive, M.; Garcia-Gutierrez, S.; Hayas, C.L.; Quintana, J.M.; OFF (Older Falls Fracture)-IRYSS Group. Psychometric characteristics of the Spanish version of the Barthel Index. Aging Clin. Exp. Res. 2018, 30, 489–497. [Google Scholar] [CrossRef]
- Tinetti, M.E.; Williams, T.F.; Mayewski, R. Fall risk index for elderly patients based on number of chronic disabilities. Am. J. Med. 1986, 80, 429–434. [Google Scholar] [CrossRef]
- Hair, J.F.; Anderson, R.E.; Babin, B.J.; Black, W.C. Multivariate Data Analysis: A Global Perspective, 7th ed.; Pearson: London, UK, 2010. [Google Scholar]
- Raglio, A.; Oasi, O. Music and health: What interventions for what results? Front. Psychol. 2015, 6, 230. [Google Scholar] [CrossRef] [Green Version]
- Janata, P. Effects of Widespread and Frequent Personalized Music Programming on Agitation and Depression in Assisted Living Facility Residents with Alzheimer-Type Dementia. Music Med. 2011, 4, 8–15. [Google Scholar] [CrossRef]
- García, J.J.M.; Iodic, R.; Carro, J.; Sánchez, J.A.; Palmero, F.; Mateo, A.M. Improvement of autobiographic memory recovery by means of sad music in alzheimer’s disease type dementia. Aging Clin. Exp. Res. 2012, 24, 227–232. [Google Scholar]
- Ceccato, E.; Vigato, G.; Bonetto, C.; Bevilacqua, A.; Pizziolo, P.; Ceccato, E.; Zanfretta, E.; Pollini, L.; Caneva, P.A.; Baldin, L.; et al. STAM protocol in dementia: A multicenter, single-blind, randomized, and controlled trial. Am. J. Alzheimer’s Dis. Dement. 2012, 27, 301–310. [Google Scholar] [CrossRef]
- Simmons-Stern, N.R.; Budson, A.E.; Ally, B.A. Music as a memory enhancer in patients with Alzheimer’s disease. Neuropsychologia 2010, 48, 3164–3167. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Raglio, A.; Galandra, C.; Sibilla, L.; Esposito, F.; Gaeta, F.; Di Salle, F.; Moro, L.; Carne, I.; Bastianello, S.; Baldi, M.; et al. Effects of active music therapy on the normal brain: fMRI based evidence. Brain Imaging Behav. 2015, 10, 182–186. [Google Scholar] [CrossRef] [PubMed]
- van Noorden, L. Auto-correlation and entrainment in the synchronous reproduction of musical pulse: Developments in childhood. Procedia Soc. Behav. Sci. 2014, 124, 117–118. [Google Scholar] [CrossRef] [Green Version]
- Rehfeld, K.; Lüders, A.; Hökelmann, A.; Lessmann, V.; Kaufmann, J.; Brigadski, T.; Müller, P.; Müller, N.G. Dance training is superior to repetitive physical exercise in inducing brain plasticity in the elderly. PLoS ONE 2018, 13, e0196636. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ruiz-Muelle, A.; López-Rodríguez, M.M. Dance for People with Alzheimer’s Disease: A Systematic Review. Curr. Alzheimer Res. 2019, 16, 919–933. [Google Scholar] [CrossRef] [PubMed]
| AMI (n = 28) | RMI (n = 21) | Control (n = 41) | p-Value | ||||
|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | Mean | SD | ||
| Age | 83.93 | 8.01 | 78.67 | 5.73 | 80.02 | 5.78 | 0.009 |
| ED | 7.28 | 1.04 | 7.04 | 1.74 | 7.48 | 1.93 | 0.081 |
| MMSE | 17.79 | 3.90 | 18.28 | 6.14 | 19.95 | 3.19 | 0.094 |
| NPI | 20.92 | 9.20 | 18.38 | 7.48 | 24.53 | 10.91 | 0.053 |
| BI | 70.89 | 13.88 | 70.71 | 17.34 | 77.93 | 12.39 | 0.065 |
| TS | 12.25 | 2.74 | 11.67 | 1.71 | 11.39 | 1.61 | 0.235 |
| GDS | 6.71 | 1.60 | 5.47 | 1.93 | 5.88 | 1.87 | 0.051 |
| Basal | Final | ||||||
|---|---|---|---|---|---|---|---|
| Group | Mean | SD | Mean | SD | t | p-Value | |
| MMSE | AMI | 17.79 | 3.90 | 19.57 | 3.80 | 8.548 | <0.001 |
| RMI | 18.28 | 6.14 | 17.57 | 6.14 | 3.873 | <0.001 | |
| Control | 19.95 | 3.19 | 19.83 | 3.31 | 1.954 | 0.058 | |
| NPI | AMI | 20.92 | 9.20 | 11.36 | 4.01 | 7.665 | <0.001 |
| RMI | 18.38 | 7.48 | 17.62 | 8.27 | 0.954 | 0.351 | |
| Control | 24.53 | 10.91 | 27.90 | 13.14 | 6.533 | <0.001 | |
| BI | AMI | 70.89 | 13.88 | 74.29 | 12.96 | −4.385 | <0.001 |
| RMI | 70.71 | 17.34 | 68.81 | 18.43 | 2.961 | 0.008 | |
| Control | 77.93 | 12.39 | 76.59 | 13.76 | 1.451 | 0.155 | |
| TS | AMI | 12.25 | 2.74 | 13.39 | 2.64 | −8.034 | <0.001 |
| RMI | 11.67 | 1.71 | 11.57 | 1.75 | 0.525 | 0.605 | |
| Control | 11.39 | 1.61 | 11.63 | 3.48 | 0.522 | 0.604 | |
| GDS | AMI | 6.71 | 1.60 | 6.46 | 1.55 | 1.491 | 0.148 |
| RMI | 5.47 | 1.93 | 4.95 | 1.28 | 1.714 | 0.102 | |
| Control | 5.88 | 1.87 | 5.85 | 1.84 | 0.255 | 0.800 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gómez-Gallego, M.; Gómez-Gallego, J.C.; Gallego-Mellado, M.; García-García, J. Comparative Efficacy of Active Group Music Intervention versus Group Music Listening in Alzheimer’s Disease. Int. J. Environ. Res. Public Health 2021, 18, 8067. https://doi.org/10.3390/ijerph18158067
Gómez-Gallego M, Gómez-Gallego JC, Gallego-Mellado M, García-García J. Comparative Efficacy of Active Group Music Intervention versus Group Music Listening in Alzheimer’s Disease. International Journal of Environmental Research and Public Health. 2021; 18(15):8067. https://doi.org/10.3390/ijerph18158067
Chicago/Turabian StyleGómez-Gallego, María, Juan Cándido Gómez-Gallego, María Gallego-Mellado, and Javier García-García. 2021. "Comparative Efficacy of Active Group Music Intervention versus Group Music Listening in Alzheimer’s Disease" International Journal of Environmental Research and Public Health 18, no. 15: 8067. https://doi.org/10.3390/ijerph18158067
APA StyleGómez-Gallego, M., Gómez-Gallego, J. C., Gallego-Mellado, M., & García-García, J. (2021). Comparative Efficacy of Active Group Music Intervention versus Group Music Listening in Alzheimer’s Disease. International Journal of Environmental Research and Public Health, 18(15), 8067. https://doi.org/10.3390/ijerph18158067





