“Healthcare Kamikazes” during the COVID-19 Pandemic: Purpose in Life and Moral Courage as Mediators of Psychopathology
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Sociodemographic Characteristics of the Sample
3.2. Exposure to SARS-CoV-2, Modulating Variables and Psychopathology
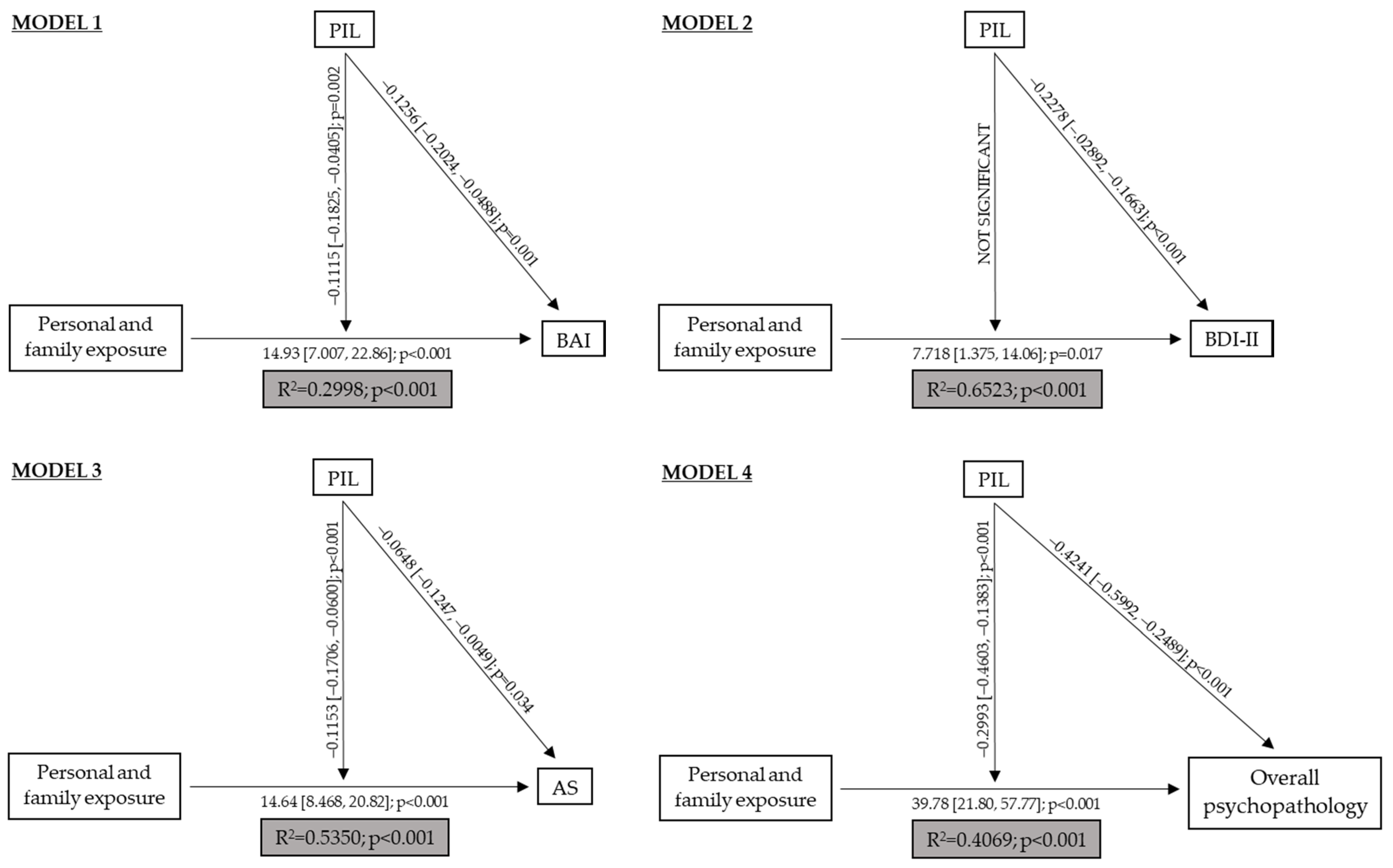
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- ECDC. Rapid Risk Assessment: Coronavirus Disease 2019 (COVID-19) Pandemic: Increased Transmission in the EU/EEA and the UK—Eighth Update. April 2020. Available online: https://www.ecdc.europa.eu/en/publications-data/rapid-risk-assessment-coronavirus-disease-2019-covid-19-pandemic-eighth-update (accessed on 30 April 2020).
- Tiefenthäler, A. ‘Health Care Kamikazes’: How Spain’s Workers Are Battling Coronavirus, Unprotected. The New York Times. (In Press). Available online: https://www.nytimes.com/video/world/europe/100000007051789/coronavirus-ppe-shortage-health-care-workers.html (accessed on 1 April 2020).
- Numminen, O.; Repo, H.; Leino-Kilpi, H. Moral courage in nursing: A concept analysis. Nurs. Ethics 2016, 24, 878–891. [Google Scholar] [CrossRef]
- Corley, M.C. Nurse Moral Distress: A proposed theory and research agenda. Nurs. Ethics 2002, 9, 636–650. [Google Scholar] [CrossRef]
- Glaw, X.; Kable, A.; Hazelton, M.; Inder, K. Meaning in Life and Meaning of Life in Mental Health Care: An Integrative Literature Review. Issues Ment. Health Nurs. 2016, 38, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Marco, J.H.; Alonso, S. Meaning in life buffers the association between clinical anxiety and global maladjustment in participants with common mental disorders on sick leave. Psychiatry Res. 2019, 271, 548–553. [Google Scholar] [CrossRef]
- Cheng, S.K.W.; Wong, C.W.; Tsang, J.; Wong, K.C. Psychological distress and negative appraisals in survivors of severe acute respiratory syndrome (SARS). Psychol. Med. 2004, 34, 1187–1195. [Google Scholar] [CrossRef] [PubMed]
- McAlonan, G.M.; Lee, A.M.; Cheung, V.; Cheung, C.; Tsang, K.W.; Sham, P.C.; Chua, S.E.; Wong, J.G. Immediate and Sustained Psychological Impact of an Emerging Infectious Disease Outbreak on Health Care Workers. Can. J. Psychiatry 2007, 52, 241–247. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.M.; Wong, J.G.; McAlonan, G.M.; Cheung, V.; Cheung, C.; Sham, P.C.; Chu, C.-M.; Wong, P.-C.; Tsang, K.W.; Chua, S.E. Stress and Psychological Distress among SARS Survivors 1 Year after the Outbreak. Can. J. Psychiatry 2007, 52, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Lai, J.; Ma, S.; Wang, Y.; Cai, Z.; Hu, J.; Wei, N.; Wu, J.; Du, H.; Chen, T.; Li, R.; et al. Factors Associated With Mental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease. JAMA Netw. Open 2020, 3, e203976. [Google Scholar] [CrossRef]
- Kang, L.; Ma, S.; Chen, M.; Yang, J.; Wang, Y.; Li, R.; Yao, L.; Bai, H.; Cai, Z.; Yang, B.X.; et al. Impact on mental health and perceptions of psychological care among medical and nursing staff in Wuhan during the 2019 novel coronavirus disease outbreak: A cross-sectional study. Brain Behav. Immun. 2020, 87, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Alonso, J.; Vilagut, G.; Mortier, P.; Ferrer, M.; Alayo, I.; Aragón-Peña, A.; Aragonès, E.; Campos, M.; Cura-González, I.D.; Emparanza, J.I.; et al. Mental health impact of the first wave of COVID-19 pandemic on Spanish healthcare workers: A large cross-sectional survey. Rev. Psiquiatr. Salud Ment. 2021, 14, 90–105. [Google Scholar] [CrossRef]
- Faul, F.; Erdfelder, E.; Lang, A.-G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Sanz, J.; García-Vera, M.P.; Fortún, M. El ‘Inventario de Ansiedad, de Beck’ (BAI): Propiedades Psicométricas de la Versión Española en Pacientes con Trastornos Psicológicos. Behav. Psychol. 2012, 20, 563–583. Available online: https://www.behavioralpsycho.com/wp-content/uploads/2019/08/05.Sanz_20-3oa.pdf (accessed on 5 April 2020).
- Sanz, J.; García-Vera, M.P.; Fortún, M. Spanish Adaptation of the Beck Depression Inventory-II (BDI-II): Psychometric Features in Patiens with Psychological Disorders. Clin. Salud. 2005, 16, 121–142. Available online: https://journals.copmadrid.org/clysa/art/37bc2f75bf1bcfe8450a1a41c200364c (accessed on 5 April 2020).
- Gálvez, B.P.; Fernández, L.G.; Manzanaro, M.P.D.V.; Valenzuela, M.A.O.; Lafuente, M.L. Spanish Validation of the Drug Abuse Screening Test (DAST-20 y DAST-10)/Validación española del Drug Abuse Screening Test (DAST-20 y DAST-10). Health Addict. Drog. 2010, 10, 35–50. [Google Scholar] [CrossRef][Green Version]
- Martínez Delgado, J.M. Validación de Los Cuestionarios Breves: Audit, Cage y Cba Para la Deteccion Precoz del Sindrome de Dependencia de Alcohol en Atencion Primaria. Available online: https://dialnet.unirioja.es/servlet/tesis?codigo=53557 (accessed on 5 April 2020).
- de la Flor, M.Á.N. Logoterapia: Fundamentos, Principios y Aplicación una Experiencia de Evaluación del Logro Interior de Sentido. Available online: https://eprints.ucm.es/id/eprint/3776/1/T19896.pdf (accessed on 5 April 2020).
- Martinez, W.; Bell, S.K.; Etchegaray, J.M.; Lehmann, L.S. Measuring Moral Courage for Interns and Residents: Scale Development and Initial Psychometrics. Acad. Med. 2016, 91, 1431–1438. [Google Scholar] [CrossRef]
- Sekerka, L.E.; Bagozzi, R.P.; Charnigo, R. Facing Ethical Challenges in the Workplace: Conceptualizing and Measuring Professional Moral Courage. J. Bus. Ethic 2009, 89, 565–579. [Google Scholar] [CrossRef]
- Mcgrath, R.E. The VIA Assessment Suite for Adults: Development and Initial Evaluation Revised Edition. Available online: https://www.viacharacter.org/pdf/Technical%20Report%20Revised%20Edition%202019_1.pdf (accessed on 5 April 2020).
- Hayes, A.F. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach; Guilford Publications: New York, NY, USA, 2017; pp. 120–141. [Google Scholar]
- Zhang, W.-R.; Wang, K.; Yin, L.; Zhao, W.-F.; Xue, Q.; Peng, M.; Min, B.-Q.; Tian, Q.; Leng, H.-X.; Du, J.-L.; et al. Mental Health and Psychosocial Problems of Medical Health Workers during the COVID-19 Epidemic in China. Psychother. Psychosom. 2020, 89, 242–250. [Google Scholar] [CrossRef]
- da Silva, F.C.T.; Neto, M.L.R. Psychiatric symptomatology associated with depression, anxiety, distress, and insomnia in health professionals working in patients affected by COVID-19: A systematic review with meta-analysis. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2021, 104, 110057. [Google Scholar] [CrossRef]
- Min, J.-A.; Jung, Y.-E.; Kim, D.-J.; Yim, H.-W.; Kim, J.-J.; Kim, T.-S.; Lee, C.-U.; Lee, C.; Chae, J.-H. Characteristics associated with low resilience in patients with depression and/or anxiety disorders. Qual. Life Res. 2013, 22, 231–241. [Google Scholar] [CrossRef]
- Schaefer, S.M.; Boylan, J.; Van Reekum, C.M.; Lapate, R.C.; Norris, C.J.; Ryff, C.D.; Davidson, R.J. Purpose in Life Predicts Better Emotional Recovery from Negative Stimuli. PLoS ONE 2013, 8, e80329. [Google Scholar] [CrossRef]
- Harlow, L.L.; Newcomb, M.D.; Bentler, P.M. Depression, self-derogation, substance use, and suicide ideation: Lack of purpose in life as a mediational factor. J. Clin. Psychol. 1986, 42, 5–21. [Google Scholar] [CrossRef]
- Windsor, T.D.; Curtis, R.G.; Luszcz, M.A. Sense of purpose as a psychological resource for aging well. Dev. Psychol. 2015, 51, 975–986. [Google Scholar] [CrossRef] [PubMed]
- Feder, A.; Ahmad, S.; Lee, E.J.; Morgan, J.E.; Singh, R.; Smith, B.W.; Southwick, S.M.; Charney, D.S. Coping and PTSD symptoms in Pakistani earthquake survivors: Purpose in life, religious coping and social support. J. Affect. Disord. 2013, 147, 156–163. [Google Scholar] [CrossRef] [PubMed]
- Schippers, M.C.; Ziegler, N. Life Crafting as a Way to Find Purpose and Meaning in Life. Front. Psychol. 2019, 10, 2778. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Wills, T.A. Stress, social support, and the buffering hypothesis. Psychol. Bull. 1985, 98, 310–357. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, R.P.; Garros, D.; Carnevale, F. Difficult decisions in pediatric practice and moral distress in the intensive care unit. Rev. Bras. Ter. Intensiv. 2018, 30, 226–232. [Google Scholar] [CrossRef]
- Roustaei, N.; Jafari, P.; Sadeghi, E.; Jamali, J. Evaluation of the Relationship between Social Desirability and Minor Psychiatric Disorders among Nurses in Southern Iran: A Robust Regression Approach. Int. J. Community Based Nurs. Midwifery 2015, 3, 301–308. [Google Scholar]
- Linde, P. El Colapso del Sistema Obliga a Sanidad a Contratar a Miles de Jubilados y Estudiantes. El País. (In Press). Available online: https://elpais.com/sociedad/2020-03-19/espana-suma-169-muertos-y-3431-nuevos-casos-de-coronavirus.html (accessed on 1 May 2020).
- Galván-Molina, J.F.; Jiménez-Capdeville, M.E.; Hernández-Mata, J.M.; Arellano-Cano, J.R. Psychopathology screening in medical school students. Gac. Med Mex. 2017, 153, 75–85. Available online: http://www.anmm.org.mx/GMM/2017/n1_english/3942AX171_153_2017_UK1_069-080.pdf (accessed on 5 May 2020).
- Atienza-Carbonell, B.; Balanzá-Martínez, V. Prevalence of depressive symptoms and suicidal ideation among spanish medical students. Actas Esp. Psiquiatr. 2020, 48, 154–164. Available online: https://www.actaspsiquiatria.es/repositorio/22/126/ESP/22-126-ESP-154-62-862241.pdf (accessed on 5 May 2020).
| Total n = 205 | Students n = 56 | Mexican Professionals n = 59 | Spanish Professionals n = 90 | ||
|---|---|---|---|---|---|
| n (%)/ M (SD) | n (%)/ M (SD) | n (%)/ M (SD) | n (%)/ M (SD) |
(p) Post-Hoc/CTR | |
| AGE | 37.4 (11.9) | 24.7 (3.8) | 40.7 (8.1) | 44.8 (10.7) | 97.807 (<0.001) 0.037 (Mx < Sp) <0.001 (St < Mx) <0.001 (St < Sp) |
| SEX | 6.762 (0.034) | ||||
| Female | 144 (70.2) | 44 (78.6) | 34 (57.6) | 66 (73.3) | 1.6/0.9/2.5 |
| Male | 61 (29.8) | 12 (21.4) | 25 (42.4) | 24 (26.7) | −1.6/−0.9/-2.5 |
| RELIGIOSITY Yes | 138 (67.3) | 33 (58.9) | 49 (83.1) | 56 (62.2) | 9.791 (0.009) −1.6/3.1/−1.4 |
| MARITAL STATUS | 80.230 (<0.001) | ||||
| Single | 92 (44.9) | 53 (94.6) | 16 (27.1) | 23 (25.6) | 8.8/−3.2/−4.9 |
| Married | 87 (42.4) | 2 (3.6) | 30 (50.8) | 55 (61.1) | −6.9/1.5/4.8 |
| Divorced | 22 (10.7) | 1 (1.8) | 11 (16.9) | 10 (11.1) | −2.5/2.3/0.2 |
| Widowed | 4 (2.0) | 0 | 2 (3.4) | 2 (2.2) | −1.2/0.9/0.2 |
| EDUCATION | 211.600 (<0.001) | ||||
| University education | 113 (55.4) | 0 | 45 (77.6) | 68 (75.6) | −9.8/4.0/5.1 |
| Pursuing university degree | 56 (27.5) | 56 (100) | 0 | 0 | 14.3/−5.5/−7.8 |
| Did not finish university education | 8 (3.9) | 0 | 1 (1.7) | 7 (7.8) | −1.8/−1.0/2.5 |
| Secondary education/vocational training/preparatory courses | 18 (8.8) | 0 | 5 (8.6) | 13 (14.4) | −2.7/−0.1/2.5 |
| Did not finish secondary education/vocational training/preparatory courses | 9 (4.4) | 0 | 7 (12.1) | 2 (2.2) | −1.9/3.4/−1.4 |
| EDUCATION CENTER | 91.975 (<0.001) | ||||
| Private | 80 (43.5) | 54 (96.4) | 13 (22) | 13 (18.8) | 9.6/−4.0/−5.2 |
| Public | 104 (56.5) | 2 (3.6) | 46 (78) | 56 (81.2) | −9.6/4.0/5.2 |
| PHYSICAL ILLNESS Yes | 55 (26.8) | 8 (14.3) | 20 (33.9) | 27 (30.3) | 6.526 (0.038) (−2.5/1.4/1.0) |
| SMOKER Yes | 39 (19.1) | 10 (17.9) | 7 (11.9) | 22 (24.7) | 3.871 (0.144) |
| CIGARETTES/DAY | 1.6 (4.5) | 1.4 (3.8) | 0.2 (.7) | 2.7 (5.9) | 5.591 (0.004) 0.001 (Mx < Sp) |
| PSYCHIATRIC HISTORY Yes | 43 (21.0) | 8 (14.3) | 15 (25.4) | 20 (22.2) | 2.301 (0.317) |
| PSYCHOLOGICAL OR PSYCHOPHARMACOLOGICAL TREATMENT DURING QUARANTINE Yes | 15 (7.4) | 2 (3.6) | 8 (13.6) | 5 (5.6) | 4.905 (0.086) |
| Total n = 205 | Students n = 56 | Professionals Mexican n = 59 | Professionals Spanish n = 90 | ||
|---|---|---|---|---|---|
| n (%)/ M (SD) | n (%)/ M (SD) | n (%)/ M (SD) | n (%)/ M (SD) |
(p) Post-Hoc/CTR | |
| PERSONAL AND FAMILY EXPOSURE | 0.65 (0.94) | 0.62 (0.90) | 0.45 (0.93) | 0.81 (0.96) | 2.507 (0.084) |
| WORK EXPOSURE | 5.08 (3.94) | 0 (0) | 5.10 (1.87) | 8.30 (2.57) | 303,490 (<0.001) <0.001 (St < Mx) <0.001 (St < Sp) <0.001 (Mx < Sp) |
| TOTAL EXPOSURE | 5.55 (4.09) | 0.62 (0.90) | 5.55 (2.35) | 9.03 (2.66) | 240,101 (<0.001) <0.001 (St < Mx) <0.001 (St < Sp) <0.001 (Mx < Sp) |
| MCSP | 7.99 (1.02) | 7.96 (1.00) | 8 (1.03) | 7.9 (1.03) | 0.082 (0.921) |
| PMCS | 10.77 (1.33) | 10.48 (1.53) | 11.1 (0.93) | 10.6 (1.36) | 4.241 (0.016) 0.036 (Sp < Mx) 0.014 (St < Mx) |
| PIL | 113.24 (15.4) | 109.30 (14.1) | 123.3 (12.6) | 109.0 (14.9) | 21.397 (<0.001) <0.001 (Sp < Mx) <0.001 (St < Mx) |
| PURPOSE IN LIFE Yes | 113 (55.4) | 27 (48.2) | 47 (79.7) | 39 (43.8) | 20.054 (<0.001) (−1.3/4.4/−2.9) |
| GACS-24 | 136.7 (17.4) | 133.2 (15.6) | 145.7 (16.9) | 132.9 (16.7) | 12.198 (<0.001) <0.001 (Sp < Mx) <0.001 (St < Mx) |
| BAI | 8.15 (8.14) | 8.85 (6.99) | 6.71 (7.95) | 8.67 (8.88) | 1319 (0.270) |
| ANXIETY Yes | 86 (42.6) | 30 (53.6) | 18 (30.5) | 38 (43.7) | 6.327 (0.042) (2.0/−2.2/0.3) |
| BDI-II | 7.50 (7.09) | 8.80 (5.82) | 4.45 (5.63) | 8.69 (8.07) | 8.177 (<0.001) <0.001 (Mx < St) 0.001 (Mx < Sp) |
| DEPRESSION Yes | 35 (17.2) | 9 (16.1) | 7 (11.9) | 19 (21.3) | 2.309 (0.315) |
| ACUTE STRESS | 7.06 (6.30) | 6.07 (3.61) | 5.71 (5.49) | 8.59 (7.70) | 4.852 (0.009) 0.024 (Mx < Sp) 0.024 (St < Sp) |
| ACUTE STRESS Yes | 45 (22.1) | 8 (14.3) | 8 (13.6) | 29 (32.6) | 10.182 (0.006) (−1.6/−1.9/3.2) |
| DAST-10 | 0.11 (0.45) | 0.17 (0.54) | .05 (.22) | 0.11 (0.50) | 1.123 (0.327) |
| DRUGS Yes | 15 (7.4) | 7 (12.5) | 3 (5.1) | 5 (5.6) | 3.017 (0.221) |
| AUDIT | 2.69 (2.58) | 3.51 (3.28) | 2.37 (2.53) | 2.37 (1.94) | 4.065 (0.019) Not significant |
| ALCOHOL Yes | 18 (8.9) | 7 (12.5) | 4 (6.8) | 7 (8.0) | 1.299 (0.522) |
| PSYCHOPATHOLOGY | 26.01 (19.82) | 28.42 (14.65) | 20.30 (17.89) | 28.43 (23.25) | 3.569 (0.030) 0.024 (Mx < St) |
| MENTAL DISORDER Yes | 114 (55.6) | 39 (69.6) | 23 (39.0) | 52 (57.8) | 11.256 (0.004) (2.5/−3.0/0.6) |
| RESPONSE | PREDICTORS | UOR 95% CI | p-Value | AOR 95% CI | p-Value |
|---|---|---|---|---|---|
| BAI | Personal and family exposure | 3.071 1.934, 4.207 | <0.001 | 1.959 0.719, 3.200 | 0.002 |
| Work exposure | 0.072 −0.220, 0.364 | 0.627 | 0.042 −0.233, 0.317 | 0.766 | |
| Total exposure | 0.249 −0.033, 0.532 | 0.084 | - | - | |
| MCSP | 0.589 −0.608, 1.785 | 0.333 | 1.060 −0.173, 2.293 | 0.092 | |
| PMCS | −0.047 −0.924, 0.831 | 0.917 | 0.508 −0.368, 1.384 | 0.256 | |
| PIL | −0.216 −0.283, −0.149 | <0.001 | −0.166 −0.274, −0.057 | 0.003 | |
| GACS-24 | −0.148 −0.211, −0.085 | <0.001 | −0.055 −0.148, 0.039 | 0.252 | |
| BDI-II | Personal and family exposure | 2.434 1.417, 3.451 | <0.001 | 1.308 0.351, 2.265 | 0.007 |
| Work exposure | 0.082 −0.169, 0.333 | 0.521 | 0.040 −0.170, 0.250 | 0.708 | |
| Total exposure | 0.198 −0.050, 0.447 | 0.116 | - | - | |
| MCSP | −0.106 −1.106, 0.894 | 0.834 | 0.941 −0.015, 1.896 | 0.054 | |
| PMCS | −0.406 −1.159, 0.347 | 0.289 | 0.125 −0.554, 0.804 | 0.718 | |
| PIL | −0.272 −0.324, −0.221 | <0.001 | −0.206 −0.289, −0.123 | <0.001 | |
| GACS-24 | −0.207 −0.256, −0.158 | <0.001 | −0.084 −0.156, −0.012 | 0.022 | |
| ACUTE STRESS | Personal and family exposure | 2.218 1.334, 3.103 | <0.001 | 1.181 0.247, 2.116 | 0.013 |
| Work exposure | 0.343 0.125, 0.561 | 0.002 | 0.320 0.115, 0.525 | 0.002 | |
| Total exposure | 0.424 0.215, 0.634 | <0.001 | - | - | |
| MCSP | 0.407 −0.491, 1.305 | 0.372 | 0.662 −0.271, 1.595 | 0.164 | |
| PMCS | 0.003 −0.659, 0.665 | 0.992 | 0.326 −0.336, 0.989 | 0.334 | |
| PIL | −0.149 −0.201, −0.097 | <0.001 | −0.147 −0.228, −0.066 | <0.001 | |
| GACS-24 | −0.101 −0.149, −0.053 | <0.001 | −0.003 −0.073, 0.067 | 0.929 | |
| DAST-10 | Personal and family exposure | −0.012 −0.081, 0.058 | 0.743 | −0.004 −0.083, 0.074 | 0.912 |
| Work exposure | −0.008 −0.025, 0.008 | 0.303 | −0.006 −0.023, 0.011 | 0.502 | |
| Total exposure | −0.008 −0.024, 0.009 | 0.356 | - | - | |
| MCSP | −0.005 −0.069, 0.059 | 0.880 | 0.002 −0.077, 0.080 | 0.968 | |
| PMCS | 0.006 −0.043, 0.056 | 0.796 | 0.002 −0.054, 0.058 | 0.952 | |
| PIL | −0.006 −0.010, −0.002 | 0.003 | −0.009 −0.016, −0.002 | 0.013 | |
| GACS-24 | −0.001 −0.004, 0.003 | 0.704 | 0.003 −0.003, 0.009 | 0.261 | |
| AUDIT | Personal and family exposure | 0.270 −0.121, 0.661 | 0.174 | 0.332 −0.105, 0.768 | 0.137 |
| Work exposure | −0.132 −0.222, −0.043 | 0.004 | −0.161 −0.257, −0.065 | 0.001 | |
| Total exposure | −0.119 −0.208, −0.029 | 0.009 | - | - | |
| MCSP | −0.276 −0.656, 0.105 | 0.155 | −0.103 −0.539, 0.333 | 0.643 | |
| PMCS | −0.160 −0.442, 0.123 | 0.267 | −0.012 −0.322, 0.298 | 0.940 | |
| PIL | −0.018 −0.041, 0.006 | 0.140 | 0.010 −0.028, 0.048 | 0.608 | |
| GACS-24 | −0.024 −0.045, −0.003 | 0.023 | −0.039 −0.071, −0.006 | 0.021 | |
| PSYCHOPATHOLOGY | Personal and family exposure | 8.144 5.386, 10.903 | <0.001 | 4.995 2.219, 7.771 | <0.001 |
| Work exposure | 0.267 −0.449, 0.983 | 0.463 | 0.168 −0.447, 0.783 | 0.592 | |
| Total exposure | 0.709 0.013, 1.405 | 0.046 | - | - | |
| MCSP | 0.742 −2.123, 3.608 | 0.610 | 2.534 −0.225, 5.293 | 0.072 | |
| PMCS | −0.282 −2,454, 1.891 | 0.798 | 0.902 −1.058, 2.862 | 0.367 | |
| PIL | −0.655 −0.813, −0.498 | <0.001 | −0.513 −0.756, −0.271 | <0.001 | |
| GACS-24 | −0.480 −0.626, −0.334 | <0.001 | −0.180 −0.389, 0.030 | 0.093 |
| RESPONSE | PREDICTORS | OR (95% CI) | p-Value |
|---|---|---|---|
| Anxiety disorder | Personal and family exposure | 1.662 (1.090, 2.533) | 0.018 |
| MCSP | 1.650 (1.102, 2.472) | 0.015 | |
| GACS-24 | −0.965 (−0.940, −0.989) | 0.005 | |
| Age | −0.958 (−0.927, −0.990) | 0.010 | |
| Male gender | −0.371 (−0.154, −0.895) | 0.027 | |
| Psychological/psychiatric treatment during the pandemic | −0.080 (−0.014, −0.468) | 0.005 | |
| Depressive disorder | Personal and family exposure | 1.968 (1.235, 3.136) | 0.004 |
| PIL | −0.931 (−0.900, −0.962) | <0.001 | |
| Acute stress disorder | Personal and family exposure | 1.911 (1.227, 2.977) | 0.004 |
| MCSP | 1.753 (1.097, 2.801) | 0.019 | |
| PIL | −0.949 (−0.919, −0.980) | 0.001 | |
| Religiosity | −0.229 (−0.082, −0.642) | 0.005 | |
| Psychological/psychiatric treatment during the pandemic | −0.080 (−0.015, −0.421) | 0.003 | |
| Psychiatric history | 4.190 (1.133, 15.498) | 0.032 | |
| Problematic drug use | Psychiatric history | −0.289 (−0.090, −0.928) | 0.037 |
| Problematic alcohol use | - | - | - |
| Any mental disorder | Personal and family exposure | 1.858 (1.203, 2.870) | 0.005 |
| MCSP | 1.682 (1.151, 2.458) | 0.007 | |
| GACS-24 | −0.968 (−0.946, −0.991) | 0.007 | |
| Age | −0.970 (−0.941, −0.999) | 0.044 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Echeverria, I.; Peraire, M.; Haro, G.; Mora, R.; Camacho, I.; Almodóvar, I.; Mañes, V.; Zaera, I.; Benito, A. “Healthcare Kamikazes” during the COVID-19 Pandemic: Purpose in Life and Moral Courage as Mediators of Psychopathology. Int. J. Environ. Res. Public Health 2021, 18, 7235. https://doi.org/10.3390/ijerph18147235
Echeverria I, Peraire M, Haro G, Mora R, Camacho I, Almodóvar I, Mañes V, Zaera I, Benito A. “Healthcare Kamikazes” during the COVID-19 Pandemic: Purpose in Life and Moral Courage as Mediators of Psychopathology. International Journal of Environmental Research and Public Health. 2021; 18(14):7235. https://doi.org/10.3390/ijerph18147235
Chicago/Turabian StyleEcheverria, Iván, Marc Peraire, Gonzalo Haro, Rafael Mora, Isabel Camacho, Isabel Almodóvar, Vicente Mañes, Ignacio Zaera, and Ana Benito. 2021. "“Healthcare Kamikazes” during the COVID-19 Pandemic: Purpose in Life and Moral Courage as Mediators of Psychopathology" International Journal of Environmental Research and Public Health 18, no. 14: 7235. https://doi.org/10.3390/ijerph18147235
APA StyleEcheverria, I., Peraire, M., Haro, G., Mora, R., Camacho, I., Almodóvar, I., Mañes, V., Zaera, I., & Benito, A. (2021). “Healthcare Kamikazes” during the COVID-19 Pandemic: Purpose in Life and Moral Courage as Mediators of Psychopathology. International Journal of Environmental Research and Public Health, 18(14), 7235. https://doi.org/10.3390/ijerph18147235







