Systematic Review on Healthcare and Societal Costs of Tinnitus
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Sources and Search Strategy
2.2. Eligibility Criteria
2.3. Study Selection
2.4. Data Extraction
3. Results
4. Discussion
4.1. Main Findings
4.2. Cost Categories
4.3. Country Differences
4.4. Impact of Patients’ and Tinnitus Characteristics (e.g., Severity) on Costs
4.5. Strengths and Limitations of the Review
4.6. Future Perspectives and UNITI Project
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Møller, A.R. Epidemiology of Tinnitus in Adults. In Textbook of Tinnitus; Møller, A.R., Langguth, B., De Ridder, D., Kleinjung, T., Eds.; Springer: New York, NY, USA, 2011. [Google Scholar] [CrossRef]
- McCormack, A.; Edmondson-Jones, M.; Somerset, S.; Hall, D. A systematic review of the reporting of tinnitus prevalence and severity. Hear. Res. 2016, 337, 70–79. [Google Scholar] [CrossRef] [PubMed]
- Gallus, S.; Lugo, A.; Garavello, W.; Bosetti, C.; Santoro, E.; Colombo, P.; Perin, P.; La Vecchia, C.; Langguth, B. Prevalence and Determinants of Tinnitus in the Italian Adult Population. Neuroepidemiology 2015, 45, 12–19. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baguley, D.; McFerran, D.; Hall, D. Tinnitus. Lancet 2013, 382, 1600–1607. [Google Scholar] [CrossRef] [Green Version]
- Langguth, B.; Kreuzer, P.M.; Kleinjung, T.; De Ridder, D. Tinnitus: Causes and clinical management. Lancet Neurol. 2013, 12, 920–930. [Google Scholar] [CrossRef]
- Langguth, B.; Salvi, R.; Elgoyhen, A.B. Emerging pharmacotherapy of tinnitus. Expert Opin. Emerg. Drugs 2009, 14, 687–702. [Google Scholar] [CrossRef] [Green Version]
- Maes, I.H.; Cima, R.F.; Vlaeyen, J.W.; Anteunis, L.J.; Joore, M.A. Tinnitus: A cost study. Ear Hear. 2013, 34, 508–514. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Trpchevska, N.; Bulla, J.; Prada Hellberg, M.; Edvall, N.K.; Lazar, A.; Mehraei, G.; Uhlen, I.; Schlee, W.; Canlon, B.; Gallus, S.; et al. Sex-Dependent Aggregation of Tinnitus in Swedish Families. J. Clin. Med. 2020, 9. [Google Scholar] [CrossRef] [PubMed]
- Cederroth, C.R.; PirouziFard, M.; Trpchevska, N.; Idrizbegovic, E.; Canlon, B.; Sundquist, J.; Sundquist, K.; Zoller, B. Association of Genetic vs. Environmental Factors in Swedish Adoptees With Clinically Significant Tinnitus. JAMA Otolaryngol. Head Neck Surg. 2019, 145, 222–229. [Google Scholar] [CrossRef]
- Hall, D.A.; Lainez, M.J.; Newman, C.W.; Sanchez, T.G.; Egler, M.; Tennigkeit, F.; Koch, M.; Langguth, B. Treatment options for subjective tinnitus: Self reports from a sample of general practitioners and ENT physicians within Europe and the USA. BMC Health Serv. Res. 2011, 11, 302. [Google Scholar] [CrossRef] [Green Version]
- Langguth, B.; Elgoyhen, A.B.; Cederroth, C.R. Therapeutic Approaches to the Treatment of Tinnitus. Annu. Rev. Pharmacol. Toxicol. 2019, 59, 291–313. [Google Scholar] [CrossRef]
- Simoes, J.; Neff, P.; Schoisswohl, S.; Bulla, J.; Schecklmann, M.; Harrison, S.; Vesala, M.; Langguth, B.; Schlee, W. Toward Personalized Tinnitus Treatment: An Exploratory Study Based on Internet Crowdsensing. Front. Public Health 2019, 7, 157. [Google Scholar] [CrossRef] [PubMed]
- Henry, J.A.; Dennis, K.C.; Schechter, M.A. General review of tinnitus: Prevalence, mechanisms, effects, and management. J. Speech Lang. Hear. Res. 2005, 48, 1204–1235. [Google Scholar] [CrossRef]
- Hoare, D.J.; Gander, P.E.; Collins, L.; Smith, S.; Hall, D.A. Management of tinnitus in English NHS audiology departments: An evaluation of current practice. J. Eval. Clin. Pract. 2012, 18, 326–334. [Google Scholar] [CrossRef] [Green Version]
- Cima, R.F.F.; Mazurek, B.; Haider, H.; Kikidis, D.; Lapira, A.; Norena, A.; Hoare, D.J. A multidisciplinary European guideline for tinnitus: Diagnostics, assessment, and treatment. HNO 2019, 67, 10–42. [Google Scholar] [CrossRef] [Green Version]
- McFerran, D.J.; Stockdale, D.; Holme, R.; Large, C.H.; Baguley, D.M. Why Is There No Cure for Tinnitus? Front. Neurosci. 2019, 13, 802. [Google Scholar] [CrossRef] [Green Version]
- Friberg, E.; Jansson, C.; Mittendorfer-Rutz, E.; Rosenhall, U.; Alexanderson, K. Sickness absence due to otoaudiological diagnoses and risk of disability pension: A nationwide Swedish prospective cohort study. PLoS ONE 2012, 7, e29966. [Google Scholar] [CrossRef] [PubMed]
- Friberg, E.; Rosenhall, U.; Alexanderson, K. Sickness absence due to otoaudiological diagnoses; a descriptive nationwide study. BMC Public Health 2013, 13, 635. [Google Scholar] [CrossRef] [Green Version]
- Maes, I.H.; Cima, R.F.; Anteunis, L.J.; Scheijen, D.J.; Baguley, D.M.; El Refaie, A.; Vlaeyen, J.W.; Joore, M.A. Cost-effectiveness of specialized treatment based on cognitive behavioral therapy versus usual care for tinnitus. Otol. Neurotol. 2014, 35, 787–795. [Google Scholar] [CrossRef]
- Stockdale, D.; McFerran, D.; Brazier, P.; Pritchard, C.; Kay, T.; Dowrick, C.; Hoare, D.J. An economic evaluation of the healthcare cost of tinnitus management in the UK. BMC Health Serv. Res. 2017, 17, 577. [Google Scholar] [CrossRef] [Green Version]
- Cederroth, C.R.; Canlon, B.; Langguth, B. Hearing loss and tinnitus—Are funders and industry listening? Nat. Biotechnol. 2013, 31, 972–974. [Google Scholar] [CrossRef]
- Goldstein, E.; Ho, C.X.; Hanna, R.; Elinger, C.; Yaremchuk, K.L.; Seidman, M.D.; Jesse, M.T. Cost of care for subjective tinnitus in relation to patient satisfaction. Otolaryngol. Head Neck Surg. 2015, 152, 518–523. [Google Scholar] [CrossRef] [PubMed]
- Newman, C.W.; Sandridge, S.A. A comparison of benefit and economic value between two sound therapy tinnitus management options. J. Am. Acad. Audiol. 2012, 23, 126–138. [Google Scholar] [CrossRef] [PubMed]
- Boccuzzi, S.J. Indirect Health Care Costs. In Cardiovascular Health Care Economics; Weintraub, W.S., Ed.; Humana Press: Totowa, NJ, USA, 2003; pp. 63–79. [Google Scholar]
- Schlee, W.; Schoisswohl, S.; Staudinger, S.; Schiller, A.; Lehner, A.; Langguth, B.; Schecklmann, M.; Simoes, J.; Neff, P.; Marcrum, S.C.; et al. Towards a unification of treatments and interventions for tinnitus patients: The EU research and innovation action UNITI. In Progress in Brain Research; Elsevier: Amsterdam, The Netherlands, 2021; pp. 441–451. [Google Scholar]
| First Author, Year [reference] | Study Design | Country (Study Period) | Tinnitus Cost Determination | Study Population | Outcome Measures | Estimates |
|---|---|---|---|---|---|---|
| Goldstein, 2015 [22] | Cross-sectional | USA (2011) | Costs were estimated through local hospital data stores | Sample of 692 patients with subjective tinnitus who visited the clinic in 2011 | Total annual clinical costs for tinnitus-related visits | Estimates are provided in annual mean per person (SD) Annual tinnitus-related cost for clinical visits only: USD 663 (USD 1395) (i.e., EUR 564 (EUR 1186)) |
| Newman, 2012 [23] | Cohort | USA (not specified) | Cost estimates were based on patient charges for each treatment option | 56 patients enrolled from a tinnitus clinic: 23 treated with SG, 33 with NTT | Healthcare costs for 1 year of two specific treatments | SGs total costs: USD 1633 (i.e., EUR 1388) NTT total costs: USD 4382 (i.e., EUR 3725) |
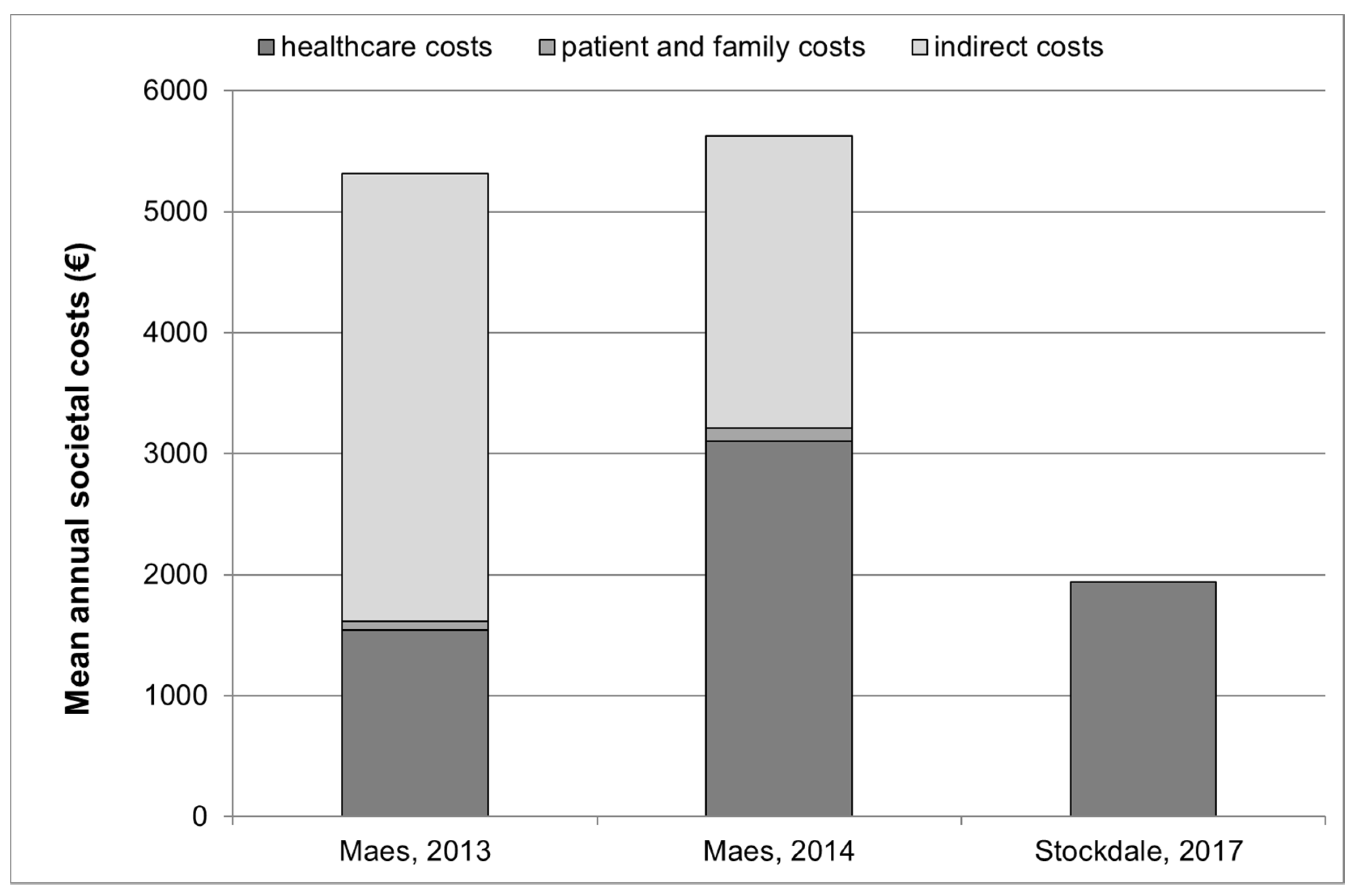
| Maes, 2013 [7] | Cross-sectional | Netherlands (not specified) | Costs were estimated using a self-administered questionnaire with a recall period of 3 months. The mean costs were then multiplied by 4 to obtain annual mean costs per patient. | Sample of 492 patients referring to an audiological secondary-care facility | Mean annual costs divided into three categories: healthcare costs, patient and family costs and indirect costs | Healthcare costs: EUR 1544 These costs include those for GP practice (EUR 225; visit, home visit, assistant visit, weekend and evening), medical specialists (EUR 771; ENT specialist visit, dental surgeon visit, neurologist visit, other medical specialists), other healthcare professionals (EUR 527; clinical physicist in audiology, physiotherapist, psychologist, psychiatrist, social worker, occupational therapist, company doctor, homeopath, acupuncturist, haptonomist, magnetizer), prescribed medication (EUR 21). Patient and family costs: EUR 69 These costs include over-the-counter medication, traveling expenses, sports, medication, ear candle, other costs. Productivity loss (loss of productivity at paid labor): EUR 3702 Total annual costs: EUR 5315 |
| Maes, 2014 [19] | RCT | Netherlands (2007–2011) | Costs were estimated from the exact amount of care consumed at the audiologic center by each patient, from the GIP databank 2009 and from the information of the Dutch Association of Hearing Aid Dispensers. | 492 tinnitus patients who referred to the audiologic center and were randomized to SC or UC | Mean annual costs divided into three categories: healthcare costs, patient and family costs and indirect costs | Healthcare costs: UC: USD 3882 (i.e., EUR 3300) and SC: USD 4034 (i.e., EUR 3429) These costs include first-level tinnitus care (UC: USD 1848 and SC: USD 2091; pure tone audiometry, speech audiometry, tympanometry, tinnitus analysis, uncomfortable loudness levels, individual consult by clinical physicist in audiology, hearing aid fitting, new hearing aid, hearing aid check and optimization, fitting tinnitus masker, new tinnitus masker, BERA, intake psychologist, tinnitus educational group session), second-level tinnitus care (UC: USD 365 and SC: USD 694; individual trajectory, treatment group A, treatment group B, social work trajectory), general practitioner practice (UC: USD 166 and SC: USD 97; GP visit, GP home visit, GP assistant visit, GP weekend and evening), hospital care (UC: USD 562 and SC: USD 479; ENT specialist visit, neurologist visit, dental surgeon visit, other medical specialist), other healthcare professionals (UC: USD 941 and SC: USD 674; physiotherapist, psychologist, psychiatrist, social worker, occupational therapist, company physician, homeopath, acupuncturist, haptonomist, magnetizer), prescribed medication. Patient and family costs: UC: USD 135 (i.e., EUR 115), SC: USD 106 (i.e., EUR 90) These are divided into: over-the-counter medication, traveling expenses, sports, medication or other costs. Productivity loss (loss of productivity at paid labor): UC: USD 3018 (i.e., EUR 2565), SC: USD 3252 (i.e., EUR 2764) Total annual costs: UC: USD 7035 (i.e., EUR 5980) SC: USD 7392 (i.e., EUR 6283) |
| Stockdale, 2017 [20] | Cohort | UK (not specified) | A cost model was constructed considering the most common treatment pathways and was applied to a cohort of patients | Cohort of patients referring to a GP for tinnitus for the first time | Annual healthcare treatment costs | Digital hearing aids: GBP 85 Hearing aids assessments: GBP 65 Hearing aid fitting: GBP 65 Hearing aid follow-up: GBP 108 Hearing aid batteries: GBP 12 Hearing aid repairs: GBP 52 CBT: GBP 471 Tinnitus therapy plus wearable sound generator: GBP 303 GP session: GBP 52 Pharmacotherapy—betahistine: GBP 25 Pharmacotherapy—amitriptyline: GBP 13 MRI: GBP 85 Associate medical specialist in ENT: GBP 121 Audiologist (1 h): GBP 19 Clinical psychologist (2 h): GBP 286 Total healthcare costs: GBP 1762 (i.e., EUR 1938) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Trochidis, I.; Lugo, A.; Borroni, E.; Cederroth, C.R.; Cima, R.; Kikidis, D.; Langguth, B.; Schlee, W.; Gallus, S. Systematic Review on Healthcare and Societal Costs of Tinnitus. Int. J. Environ. Res. Public Health 2021, 18, 6881. https://doi.org/10.3390/ijerph18136881
Trochidis I, Lugo A, Borroni E, Cederroth CR, Cima R, Kikidis D, Langguth B, Schlee W, Gallus S. Systematic Review on Healthcare and Societal Costs of Tinnitus. International Journal of Environmental Research and Public Health. 2021; 18(13):6881. https://doi.org/10.3390/ijerph18136881
Chicago/Turabian StyleTrochidis, Ilias, Alessandra Lugo, Elisa Borroni, Christopher R. Cederroth, Rilana Cima, Dimitris Kikidis, Berthold Langguth, Winfried Schlee, and Silvano Gallus. 2021. "Systematic Review on Healthcare and Societal Costs of Tinnitus" International Journal of Environmental Research and Public Health 18, no. 13: 6881. https://doi.org/10.3390/ijerph18136881
APA StyleTrochidis, I., Lugo, A., Borroni, E., Cederroth, C. R., Cima, R., Kikidis, D., Langguth, B., Schlee, W., & Gallus, S. (2021). Systematic Review on Healthcare and Societal Costs of Tinnitus. International Journal of Environmental Research and Public Health, 18(13), 6881. https://doi.org/10.3390/ijerph18136881









