Reproductive Health Risks Associated with Occupational and Environmental Exposure to Pesticides
Abstract
1. Introduction
2. Material and Methods
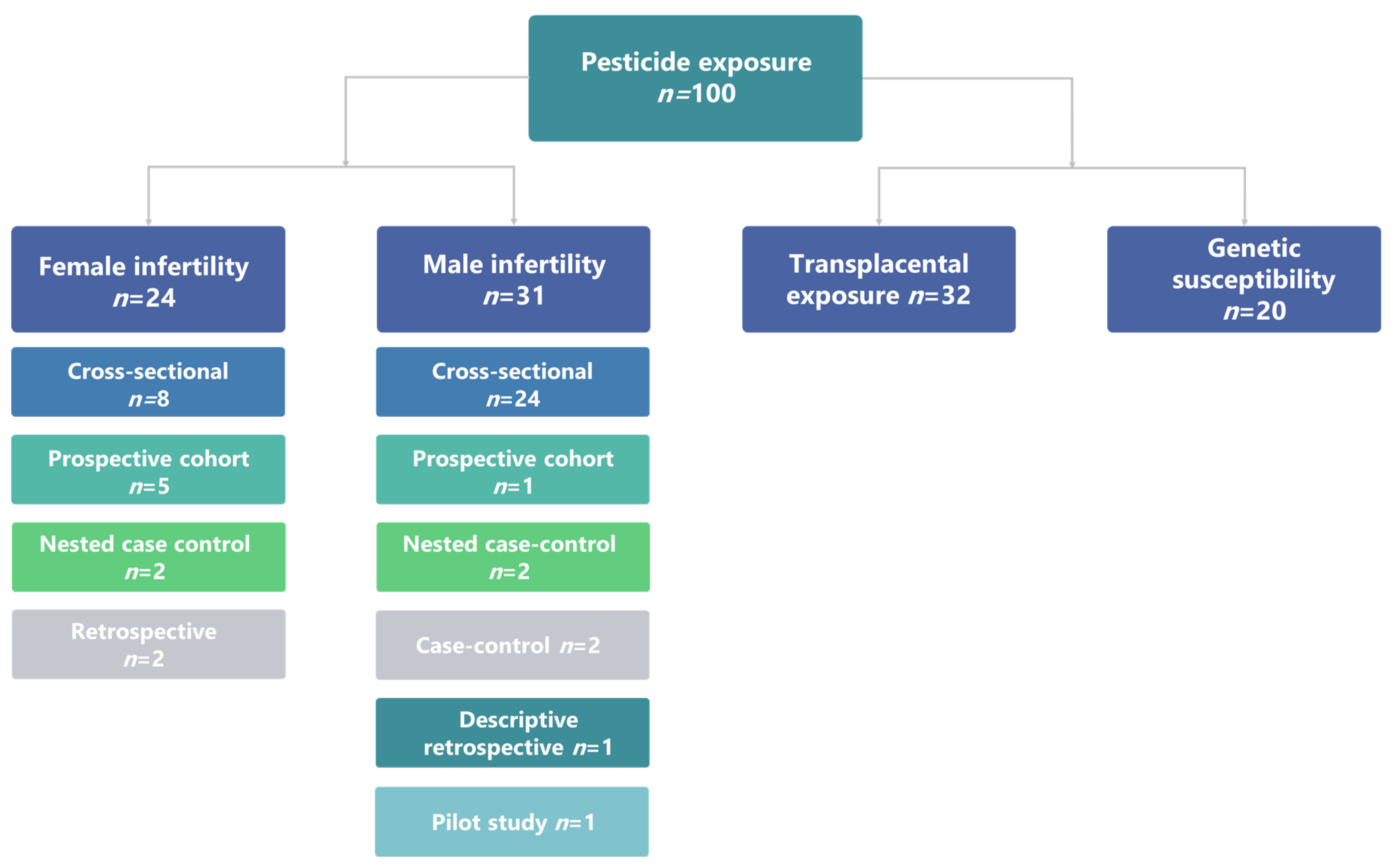
3. Results
3.1. Female Fertility
3.1.1. Time to Pregnancy and Infertility
3.1.2. Assisted Reproduction
3.1.3. Ovarian Reserve and Hormone Levels
3.1.4. Spontaneous Fetal Loss (Miscarriage)
3.1.5. Age at Menarche
3.1.6. Menstrual Cycle Length
| Study | Site | Design | Exposure | Duration of Exposure | Sample | Outcome | Results |
|---|---|---|---|---|---|---|---|
| Björvang et al., 2020 [24] | Sweden (environmental exposure) | Cross-sectional | Serum gestational POPs (9 OCPs, 10 PCBs and 3 PBDEs) | Long-term | n = 818 women with a pregnancy | TTP and clinical infertility | 3rd Q vs. 1st Q HCB associated with: (1) infertility (OR = 2.25, 95%CI: 1.06, 4.78); (2) longer TTP among women < 29 years of age who used COCs. DDE associated with longer TTP among women ≥ 29 years who used COCs. |
| Bloom et al., 2017 [32] | United States (environmental exposure) | Prospective cohort | Ovarian follicular fluid organochlorines (2 OCPs and 43 PCBs) | Long-term | n = 32 women undergoing IVF | Measures of ovarian reserve and IVF outcomes | DDE associated with oocyte maturity (RR = 0.72; 95% CI: 0.60, 0.86) and live birth (RR = 3.65; 95% CI: 1.08, 12.31). DDT associated with E2 (β = 1.45, 95%CI: 0.92, 1.97) |
| Chiu et al., 2018 [33] | United States (environmental exposure) | Prospective cohort | Self-reported consumption of fruit and vegetable pesticide residues | Short-term (past 3 months) | n = 325 women undergoing IVF (541 cycles) | Pregnancy and live birth | High pesticide residue fruits and vegetables associated with lower probabilities for pregnancy (p = 0.04) and live birth (p = 0.02). |
| Garry et al., 2002 [42] | United States (Occupational exposure) | Cross-sectional | Self-reported application of herbicides, insecticides, fungicides and fumigants | Current and historic | n = 522 women with singleton pregnancies fathered by a licensed pesticide applicator | Pregnancy loss and menstrual function | Herbicide/insecticide/fungicide use vs. herbicide only use associated with pregnancy loss (OR = 1.64, 95%CI: 1.01, 2.67). |
| Hu et al., 2018 [26] | China (environmental exposure) | Prospective cohort | Urinary organophosphate (6) and pyrethroid (3) metabolites | Short-term | n = 615 women planning a pregnancy | TTP and clinical infertility | 4th Q vs. 1st Q DETP associated with TTP (FOR = 0.68, 95%CI: 0.51, 0.92) and infertility (OR = 2.17, 95%CI: 1.19, 3.93); 4th Q vs. 1st Q 3-PBA associated with TTP (FOR = 0.72, 95%CI: 0.53, 0.98) and infertility (OR = 2.03, 95%CI: 1.10–3.74) in nulliparas. |
| Jurewicz et al., 2020 [34] | Poland (environmental exposure) | Cross-sectional | Urinary pyrethroid metabolites (4) | Short-term | n = 511 women undergoing infertility evaluation | Measures of ovarian reserve | 3-PBA associated with AFC (β = −0.02 follicles, 95%CI: −0.06, −0.01), AMH (β = −0.04 ng/mL, 95%CI: −0.12, −0.04), FSH (β = 0.01 IU/L, 95%CI: 0.01, 0.25) per ng/mL. |
| Louis et al., 2011 [49] | United States (environmental exposure) | Prospective cohort | Serum organochlorines (7 OCPs and 76 PCBs) | Long-term | n = 83 women planning a pregnancy (447 cycles) | Menstrual function | 3rd T vs. 1st T aromatic fungicides associated with days bleeding (β=−0.15 days, 95%CI: −0.29, −0.002). |
| Mahalingaiah, 2012 [30] | United States (environmental exposure) | Nested case control | Serum DDT, DDE and HCB | Long-term | n = 720 women undergoing IVF (827 cycles) | Failed implantation, pregnancy and pregnancy loss | 4th Q vs. 1st Q HCB associated with failed implantation (OR = 2.32, 95%CI: 1.38, 3.90). |
| Naidoo et al., 2011 [43] | South Africa (occupational exposure) | Cross-sectional | Self-reported pesticide spraying | Short-term (during early pregnancy) | n = 887 farm workers with a pregnancy | Pregnancy loss | Spraying pesticides associated with greater risk of spontaneous loss (OR = 2.6, 95%CI: 1.6, 6.4). |
| Namulanda et al., 2017 [48] | England (environmental exposure) | Nested case control | Gestational urinary atrazine metabolites (6) | Short-term | n = 369 girls (174 cases, 195 controls) | Menarche (<11.5 years) | Diaminochlorotriazine associated with non-significant odds of early menarche (OR = 1.13, 95% CI: 0.82, 1.55). |
| Ouyang et al., 2005 [47] | China (environmental exposure) | Cross-sectional | Serum DDT and DDE | Long-term | n = 466 nulliparous textile workers | Menarche and menstrual function | DDT associated with: (1) age at menarche (−0.20 years, 95%CI: −0.28, −0.13 per 10 ng/g); (2) short menstrual cycle (<21 days) 4th Q vs. 1st Q (OR = 2.78, 95%CI 1.07, 7.14). |
| Rahimi et al., 2020 [44] | Iran (occupational exposure) | Cross-sectional | Self-reported workplace pesticide exposure | Current and historic | n = 645 women (308 exposed greenhouse workers and 337 unexposed housewives) | Pregnancy loss and infertility | Greenhouse workers had significantly greater prevalence of spontaneous loss (p = 0.019) and infertility (p = 0.003) than housewives. |
| Sanin et al., 2009 [27] | Colombia (environmental exposure) | Retrospective cohort | Aerial glyphosate spraying programs in 4 regions | Up to 12 months (while trying to conceive) | n = 2592 women with a pregnancy in prior 5 years | TTP | TTP greater in regions with glyphosate spraying than without (p < 0,01). |
| Vasiliu et al., 2004 [45] | United States (environmental exposure) | Retrospective cohort | Back extrapolated pregnancy serum DDE and PCBs | Long-term | n = 151 daughters of Lake Michigan anglers | Menarche and menstrual cycle | Extrapolated gestational DDE associated with age at menarche (β = −0.07 years; p = 0.038 per µg/L). |
| Whitworth et al., 2015 [35] | South Africa (environmental exposure) | Prospective cohort | Plasma DDT and DDE and indoor pesticide spraying | Short-term (seasonal) | n = 420 women from rural villages | Plasma AMH | Indoor pyrethroid spraying vs. no indoor spraying associated with AMH (−25%, 95%CI: −39%, −8%). |
| Ye et al., 2017 [46] | China (environmental exposure) | Cross-sectional | Urinary 3-PBA (a pyrethroid metabolite) | Short-term | n = 305 girls (9−15 years of age) | Self-assessed (with mother) sexual development (Tanner stages) | 3-PBA associated with breast stage 3 (OR = 0.55, 95%CI: 0.31, 0.98), pubic hair stage 2 (OR = 0.56, 95%CI: 0.36, 0.98) and menarche (OR = 0.51, 95%CI: 0.28, 0.93). |
3.2. Male Infertility
| Study | Site | Design | Exposure | Duration of Exposure | Sample | Outcome | Results |
|---|---|---|---|---|---|---|---|
| Abell et al., 2000 [1] | Denmark | Cross-sectional | Self- and greenhouse owners reported workplace pesticide exposure | Short- and long-term | n = 122 healthy men from 30 ornamental flower greenhouses | Semen analysis and sex hormones | Median sperm concentration 40% lower in men with > 10 years vs. men with < 5 years’ experience. Age adjusted T/SHBG declined 1.9% (95%CI 0.4−3.4%) per year of work. |
| Aguilar-Garduno et al., 2012 [60] | Mexico | Longitudinal study | Urine DAP metabolites and serum p,p’-DDE | Long-term | n = 136 healthy industry workers | Semen analysis, sex hormones and PON1 activity | DEPT inversely assocaied with LH. Estradiol marginally significant positive trend with DEP and DEPT. |
| Bae et al., 2018 [73] | United States | Prospective cohort study | Serum OCPs (9), PBB (1), PBDEs (10) and PCBs (36) | Current | n = 235 men from couples undergoing fertility evaluation | Secondary sex ratio | Maternal PCB-128 and paternal HCB associated with female excess (RRs, 0.75 [95% CI, 0.60–0.94] and 0.81 [95% CI, 0.68–0.97]. Maternal mirex and paternal PCB 128 and p,p’-DDE associated with a male excess (RR range, 1.10–1.22). Only maternal mirex associated at p < 0.0009. |
| Celik-Ozenci et al., 2012 [59] | Turkey | Cross-sectional | Workplace abamectin exposure | Long-term | n = 20 exposed and 20 non-exposed men | Semen analysis, sperm maturity and sex hormones | Exposed group associated with decreased motility and increased sperm immaturity. |
| Cesaire Momo Tetsatsi et al., 2020 [50] | Cameroon | Descriptive retrospective study | Patient files | Historic | n = 379 men | Data on previous semen analysis | Farmers associated with the lowest quality spermogram. |
| Cremonese et al., 2017 [54] | Brazil | Cross-sectional | Self-reported application of pesticides | Long-term, maternal during pregnancy | n = 99 rural men and 36 urban men | Semen analysis, sex hormones and genital measurements | Rural men had poorer sperm morphology and count and lower LH. Maternal farming during pregnancy associated with larger AGD and TV. |
| Dhooge et al., 2007 [57] | Belgium | Cross-sectional | Reported consumption of self-grown vegetables | Long-term | n = 51 men | Semen analysis and sex hormones | Locally produced vegetables associated with lower free T, sperm concentration, morphology, LH and FSH decline (p = 0.04, p = 0.04, p = 0.002, p = 0.02, p = 0.08). |
| Dziewirska et al., 2019 [78] | Poland | Cross-sectional | Urinary 1N and TCPY | Current | n = 315 men with normal semen concentration, under 45 years of age | Semen analysis and DNA fragmentation | TCPY concentration associated with decreased motility, positive association with DFI. 1N negatively associated with normal morphology and positively with CASA parameters. |
| Giwercman et al., 2007 [74] | Europe | Cross-sectional | Serum cb-153 and p,p’-DDE | Long-term | n = 680 men from Greenland (188), Warsaw (167), Swedish fisherman (178), Kharkiv (147) | Semen analysis, sperm DNA fragmentation, CAG and GGN repeats in leukocytes | CB-153 group (p = 0.03) and CAG repeat category (p = 0.01) associated with sperm concentration and total count. p,p’-DDE associated with DFI (p = 0.01). Above vs. below median CB-153 associated with lower sperm concentration and total count for CAG < 20. DFI associated with p,p’-DDE for CAG ≤ 21 |
| Haugen et al., 2011 [71] | Norway | Cross-sectional | Serum CB-153 and p, p’-DDE | Long-term | n = 197 men from southern or northern Norway | Semen analysis and sex hormones | Levels of p, p’-DDE, total and free T higher in south, FSH lower. CB-153 and SHBG associated in total, south and north cohorts (B = 0.12, p < 0.01; B = 0.13, p = 0.01; B = 0.12, p < 0.01) |
| Hauser et al., 2003 [70] | United States | Cross-sectional | Serum PCBs and p, p’-DDE | Current | n = 212 men undergoing fertility evaluation | Semen analysis | Dose–response relationship between PCB-138, sperm motility (OR = 1.00, 1.68, 2.35, p-value = 0.03) and morphology (OR = 1.00, 1.36, 2.53, p = 0.04) |
| Hu et al., 2020 [61] | China | Cross-sectional | Urinary pyrethroid metabolites | Current | n = 346 men undergoing fertility evaluation | Semen analysis | Negative association of 3PBA and morphology (ß = −2.12, 95%CI: −4.02 to −0.22), TDCCA and log transformed total count (ß = −0.09, 95%CI: −0.16 to −0.01); 4thQ 3PBA associated with lower sperm parameters and morphology (OR = 2.40, 95%CI: 1.26−4.54; OR = 3.08, 95%CI: 1.10−8.60). |
| Imai et al., 2014 [64] | Japan | Cross-sectional | Urinary 3-PBA | Current | n = 323 male university students | Semen analysis | No association between 3-PBA and semen quality |
| Ji et al., 2011 [62] | China | Cross-sectional | Urinary pyrethroid metabolites | Current | n = 240 men undergoing fertility evaluation | Semen analysis and DNA fragmentation | Inverse correlation between 3-PBA and sperm concentration (ß=−0.27, 95%CI: −0.41 to −0.12, p < 0.001). Positive correlation between 3-PBA and DFI (ß = 0.27, 95%CI: 0.15–0.39, p < 0.001). |
| Lwin et al., 2018 [51] | Myanmar | Cross-sectional | Self-reported application of pesticides | Long-term | n = 400 | Semen analysis, sex hormones and plasma cholinesterase | Differences in seminal parameters and sex hormones (p < 0.05) between growing and nongrowing period. Cholinesterase levels significantly higher in growing periods (p < 0.05) |
| Luderer et al., 2013 [81] | United States | Nested case–control | Mothers of participants reported heptachlor epoxide exposure | Maternal, during pregnancy and lactation | n = 216 males and 183 females born in Oahu, Hawaii during 1981–1982 | Semen analysis, sex hormones and onset of puberty | No strong association, weak association in males with higher FSH and LH concentrations, no dose–response relationship. |
| Meeker et al., 2008 [67] | United States | Cross-sectional | Urinary pyrethroid metabolites | Current | n = 207 men undergoing fertility evaluation | Semen analysis and sperm DNA damage | 4thQ 3PBA associated with concentration reduction (95%CI: −37.1 to +2.6). 4thQ TDCCA associated with motility decline (95%CI: −26.2 to −4.8). 3- PBA and CDCCA associated with increased sperm DNA damage. |
| Miranda-Contresas et al., 2013 [55] | Venezuela | Cross-sectional | Self-reported workplace pesticide exposure | Long-term | n = 64 male farm workers and 35 healthy men, 18–52 years of age | Sperm analysis, DNA fragmentation, sex hormone analysis and cholinesterase activity | DFI negatively correlated with BuChE, sperm concentration, morphology and vitality in farm workers. No association with levels of Tt, PRL, FT4 and TSH. Tendency for increased LH and FSH in exposed workers. |
| Neghab et al., 2014 [53] | Iran | Cross-sectional | Self-reported application of pesticides | Long-term | n = 268 randomly selected married farm workers | Primary infertility | Primary infertility higher among farm workers (p < 0.05). Stillbirth and spontaneous abortion more common in wives of farm workers. |
| Pant et al., 2014 [69] | India | Case–control | Seminal levels of p, p’-DDE and lindane | Current | n = 278 men undergoing fertility evaluation (21–40 years of age) | Semen analysis, sperm mitochondrial status, ROS and SCSA | Correlation between seminal lindane, p, p’-DDE, concentration (r = −0.53, -0.48) and motility (r = −0.51, −0.37). Positive association between p, p’-DDE, lindane, ROS (r = 0.61, 0.53), lipid peroxidation (r = 0.58, 0.51) and MM dysfunction |
| Perry et al., 2016 [72] | United States | Cross-sectional | Adult serum (n = 90), cord blood and age-14 serum (n = 40) levels of p, p’-DDE and PCBs 118, 138, 153, 180. | Long-term | n = 90 men from Faroe Islands | X, Y, 18 chromosome disomy | 3rd T vs. 1st T p,p’-DDE associated with XX18 (IRR = 1.52; 95%CI: 1.35, 1.72), XY18 (IRR = 1.40; 95%CI: 1.30, 1.51) and total disomy (IRR = 1.32; 95%CI: 1.25, 1.35). 2nd T YY & Σ4PCBs increased (IRR = 1.16; 95%CI: 1.03, 1.32), 3rd T decreased (IRR = 0.85; 95%CI: 0.74, 0.96). Similar in adults and those aged14. |
| Radwan et al., 2014 [66] | Poland | Cross-sectional | Urinary pyrethroid metabolites | Current | n = 334 men undergoing fertility evaluation | Semen analysis and sex hormones | Urinary pyrethroids associated with abnormal morphology (CDCCA, TDCCA, sum of pyrethroids) and decreased concentration, T level (TDCCA) and CASA parameters (LIN to 3-PBA and DBCA; VSL to VCL and DBCA). |
| Stronati et al., 2006 [77] | Europe | Cross-sectional | Serum CB-153 and p, p’-DDE | Long-term | n = 798 men from Greenland (201), Warsaw (198), Swedish fisherman (191), Kharkiv (208) | Sperm DNA fragmentation and apoptosis | CB-153 associated with altered sperm DNA integrity and Bcl-xL levels-No association for p, p’-DDE. |
| Swan et al., 2003 [80] | United States | Case–control | Serum pesticide and herbicide metabolites | Long-term | n = 50 cases and 36 controls | Semen analysis | Cases had higher levels of alachlor or IMPY (ORs = 30.0 and 16.7) and atrazine levels higher than LOD (OR = 11.3). 2,4-D and metolachlor associated with poor semen quality. Acetochlor levels lower in cases vs. controls (p = 0.04). |
| Swan et al., 2006 [79] | United States | Nested case–control | Serum non-persistent pesticide (8) metabolites | Current | n = 25 cases and 25 controls | Semen analysis | High levels of alachlor or diazinon (OR = 30.0, 16.7) and men with atrazine (OR = 11.3) over LOD significantly more among cases. |
| Tiido et al., 2006 [76] | Europe | Cross-sectional | Serum PCB-153 and p, p’-DDE | Long-term | n = 547 men from Greenland (157), Warsaw (121), Swedish fisherman (149), Kharkov (120) | Y:X ratio | Y-sperm associated with higher PCB-153 in Greenlandic and Swedish vs. Warsaw and Kharkov men. Log-transformed PCB-153 (p = 0.04) and p, p’-DDE (p < 0.001) associated with Y-fraction. Negatively associated PCB-153 and Y-chromosome in Polish cohort (p = 0.008) |
| Toft et al., 2006 [75] | Europe | Cross-sectional | Serum CB-153 and p, p’-DDE | Long-term | n = 763 men from Greenland (194), Warsaw (189), Swedish fisherman (185), Kharkov (195) | Semen analysis | In all regions, sperm motility associated with CB-153 blood concentration (ß = −3.6% per log unit CB-153 (ng/g lipid); 95%CI = −5.6 to −1.7). p, p’-DDE negatively associated with motility in Greenlandic population. |
| Toshima et al., 2012 [65] | Japan | Pilot study | Urinary metabolites of 5 phthalate diesters, pyrethroids, soy isoflavones and cadmium | Current | n = 42 men from couples undergoing fertility evaluation | Semen analysis | Weak positive correlation between concentration and cadmium (r = −0.316, p = 0.044). Negative correlation between concentration and daidzein (r = −0.292, p = 0.064). Equol correlated to motility (48.2 ± 21.0% in equol non-detectable group vs. 32.5 ± 16.8% in equol detectable, p = 0.013). |
| Young et al., 2013 [68] | United States | Cross-sectional | Urinary pyrethroids: 3-PBA, CDCCA and TDCCA | Current | n = 75 men undergoing fertility evaluation | X, Y and 18 chromosomes disomy | Sex chromosome disomies increased 7–30% in men above LOD vs. below LOD. YY18 disomy 1.28 times higher in 3-PBA group above LOD (95%CI: 1.15; 1.42). Reduced rate for XY18 and total disomy for 3-PBA (IRR = 0.82, 95% CI: 0.77; 0.87; IRR = 0.93; 95% CI: 0.87–0,97). No association for XX18 and 1818. |
| Yoshinaga et al., 2014 [63] | Japan | Cross-sectional | Urinary 3-PBA | Current | n = 322 male university students | Sex hormones | No association between 3-PBA and hormone levels. |
| Yucra et al., 2006 [56] | Peru | Cross-sectional | Self-reported workplace pesticide exposure | Long-term | n = 31 pesticide applicators and 80 non-exposed | Semen analysis and sex hormones | Volume (p = 0.02), motility grade A (p = 0.003), grade A+B (p = 0.002), normal morphology (p = 0.000) and zinc concentration (p = 0.02) lower, while pH (p = 0.003), liquefaction (p = 0.000), immature sperm (p = 0.01) and leukocytes (p = 0.000) higher in exposed men. T and LH levels lower (p = 0.001 and p = 0.02), T/LH significantly higher (p = 0.001) in exposed men. |
| Yucra et al., 2008 [58] | Peru | Cross-sectional | Urinary OP metabolites (6) | Long-term | n = 31 exposed and 31 non-exposed men | Semen analysis | DEDTP (p = 0.04) and DETP (p = 0.02) reflected occupational exposure. OP metabolites associated with lower volume and higher pH. Workplace and exposure time more strongly related to lower semen quality than urine OP metabolites. |
3.3. Transplacental Exposure Impact on Fertility
3.4. Genetic Susceptibility to Pesticide Exposure
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Abell, A.; Ernst, E.; Bonde, J.P. Semen quality and sexual hormones in greenhouse workers. Scand. J. Work. Environ. Health 2000, 26, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Food and Agriculture Organization of the United Nations (FAO). Prevention and Disposal of Obsolete Pesticides. Available online: http://www.fao.org/agriculture/crops/obsolete-pesticides/why-problem/pesticide-bans/en/ (accessed on 15 March 2021).
- Pesticide Action Network International (PAN). PAN International Consolidated List of Banned Pesticides. Available online: http://pan-international.org/pan-international-consolidated-list-of-banned-pesticides/ (accessed on 19 March 2021).
- Donley, N. The USA lags behind other agricultural nations in banning harmful pesticides. Environ. Health 2019, 18, 1–12. [Google Scholar] [CrossRef] [PubMed]
- UTZ. List of Banned Pesticides and Pesticides Watchlist. Version. Available online: https://utz.org/wp-content/uploads/2015/12/EN_UTZ_List-of-Banned-PesticidesWatchlist_v1.0_2015.pdf (accessed on 23 March 2021).
- Di Renzo, G.C.; Conry, J.A.; Blake, J.; DeFrancesco, M.S.; DeNicola, N.; Martin, J.N., Jr.; McCue, K.A.; Richmond, D.; Shah, A.; Sutton, P.; et al. International Federation of Gynecology and Obstetrics opinion on reproductive health impacts of exposure to toxic environmental chemicals. Int. J. Gynecol. Obstet. 2015, 131, 219–225. [Google Scholar] [CrossRef] [PubMed]
- American College of Obstetricians and Gynecologists; American Society for Reproductive Medicine. Exposure to toxic environmental agents. Obstet. Gynecol. 2013, 122, 931–935. [Google Scholar] [CrossRef] [PubMed]
- Gore, A.C.; Chappell, V.A.; Fenton, S.E.; Flaws, J.; Nadal, A.; Prins, G.S.; Toppari, J.; Zoeller, R.T. EDC-2: The Endocrine Society’s Second Scientific Statement on Endocrine-Disrupting Chemicals. Endocr. Rev. 2015, 36, E1–E150. [Google Scholar] [CrossRef]
- La Merrill, M.A.; Vandenberg, L.N.; Smith, M.T.; Goodson, W.; Browne, P.; Patisaul, H.B.; Guyton, K.Z.; Kortenkamp, A.; Cogliano, V.J.; Woodruff, T.J.; et al. Consensus on the key characteristics of endocrine-disrupting chemicals as a basis for hazard identification. Nat. Rev. Endocrinol. 2020, 16, 45–57. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Aponte-Mellado, A.; Premkumar, B.J.; Shaman, A.; Gupta, S. The effects of oxidative stress on female reproduction: A review. Reprod. Biol. Endocrinol. 2012, 10, 49. [Google Scholar] [CrossRef]
- Al-Gubory, K.H. Environmental pollutants and lifestyle factors induce oxidative stress and poor prenatal development. Reprod. Biomed. Online 2014, 29, 17–31. [Google Scholar] [CrossRef]
- Giudice, L.C. Environmental toxicants: Hidden players on the reproductive stage. Fertil. Steril. 2016, 106, 791–794. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.-H.; Jacobs, D.R. Firm human evidence on harms of endocrine-disrupting chemicals was unlikely to be obtainable for methodological reasons. J. Clin. Epidemiol. 2019, 107, 107–115. [Google Scholar] [CrossRef]
- Porta, M.; Vandenberg, L.N. There are good clinical, scientific, and social reasons to strengthen links between biomedical and environmental research. J. Clin. Epidemiol. 2019, 111, 124–126. [Google Scholar] [CrossRef] [PubMed]
- Autrup, H.; Barile, F.A.; Berry, S.C.; Blaauboer, B.J.; Boobis, A.; Bolt, H.; Borgert, C.J.; Dekant, W.; Dietrich, D.; Domingo, J.L.; et al. Human exposure to synthetic endocrine disrupting chemicals (S-EDCs) is generally negligible as compared to natural compounds with higher or comparable endocrine activity: How to evaluate the risk of the S-EDCs? Arch. Toxicol. 2020, 94, 2549–2557. [Google Scholar] [CrossRef] [PubMed]
- Levine, H.; Jørgensen, N.; Martino-Andrade, A.; Mendiola, J.; Weksler-Derri, D.; Mindlis, I.; Pinotti, R.; Swan, S.H. Temporal trends in sperm count: A systematic review and meta-regression analysis. Hum. Reprod. Update 2017, 23, 646–659. [Google Scholar] [CrossRef] [PubMed]
- Skakkebaek, N.E.; Meyts, E.R.-D.; Louis, G.M.B.; Toppari, J.; Andersson, A.-M.; Eisenberg, M.L.; Jensen, T.K.; Jørgensen, N.; Swan, S.H.; Sapra, K.J.; et al. Male Reproductive Disorders and Fertility Trends: Influences of Environment and Genetic Susceptibility. Physiol. Rev. 2016, 96, 55–97. [Google Scholar] [CrossRef] [PubMed]
- Petraglia, F.; Serour, G.I.; Chapron, C. The changing prevalence of infertility. Int. J. Gynecol. Obstet. 2013, 123, S4–S8. [Google Scholar] [CrossRef]
- Mascarenhas, M.N.; Flaxman, S.R.; Boerma, T.; Vanderpoel, S.; Stevens, G.A. National, Regional, and Global Trends in Infertility Prevalence Since 1990: A Systematic Analysis of 277 Health Surveys. PLoS Med. 2012, 9, e1001356. [Google Scholar] [CrossRef]
- Zaccai, J.H. How to assess epidemiological studies. Postgrad. Med. J. 2004, 80, 140–147. [Google Scholar] [CrossRef]
- Baird, D.D.; Wilcox, A.; Weinberg, C.R. Use of time to pregnancy to study environmental exposures. Am. J. Epidemiol. 1986, 124, 470–480. [Google Scholar] [CrossRef]
- Gurunath, S.; Pandian, Z.; Anderson, R.A.; Bhattacharya, S. Defining infertility—A systematic review of prevalence studies. Hum. Reprod. Update 2011, 17, 575–588. [Google Scholar] [CrossRef] [PubMed]
- Practice Committee of the American Society for Reproductive Medicine. Definitions of infertility and recurrent pregnancy loss. Fertil. Steril. 2008, 89, 1603. [Google Scholar] [CrossRef] [PubMed]
- Björvang, R.D.; Gennings, C.; Lin, P.-I.; Hussein, G.; Kiviranta, H.; Rantakokko, P.; Ruokojärvi, P.; Lindh, C.H.; Damdimopoulou, P.; Bornehag, C.-G. Persistent organic pollutants, pre-pregnancy use of combined oral contraceptives, age, and time-to-pregnancy in the SELMA cohort. Environ. Health 2020, 19, 1–14. [Google Scholar] [CrossRef]
- Carrico, C.; Gennings, C.; Wheeler, D.C.; Factor-Litvak, P. Characterization of Weighted Quantile Sum Regression for Highly Correlated Data in a Risk Analysis Setting. J. Agric. Biol. Environ. Stat. 2015, 20, 100–120. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Ji, L.; Zhang, Y.; Shi, R.; Han, W.; Tse, L.A.; Pan, R.; Wang, Y.; Ding, G.; Xu, J.; et al. Organophosphate and Pyrethroid Pesticide Exposures Measured before Conception and Associations with Time to Pregnancy in Chinese Couples Enrolled in the Shanghai Birth Cohort. Environ. Health Perspect. 2018, 126, 077001. [Google Scholar] [CrossRef]
- Sanin, L.-H.; Carrasquilla, G.; Solomon, K.R.; Cole, D.C.; Marshall, E.J.P. Regional Differences in Time to Pregnancy Among Fertile Women from Five Colombian Regions with Different use of Glyphosate. J. Toxicol. Environ. Health Part. A 2009, 72, 949–960. [Google Scholar] [CrossRef] [PubMed]
- Olsen, J.; Bonde, J.; Hjøllund, N.; Basso, O.; Ernst, E. Using infertile patients in epidemiologic studies on subfecundity and embryonal loss. Hum. Reprod. Update 2005, 11, 607–611. [Google Scholar] [CrossRef]
- Cabry, R.; Merviel, P.; Madkour, A.; Lefranc, E.; Scheffler, F.; Desailloud, R.; Bach, V.; Benkhalifa, M. The impact of endocrine disruptor chemicals on oocyte/embryo and clinical outcomes in IVF. Endocr. Connect. 2020, 9, R134–R142. [Google Scholar] [CrossRef] [PubMed]
- Mahalingaiah, S.; Missmer, S.A.; Maity, A.; Williams, P.L.; Meeker, J.D.; Berry, K.; Ehrlich, S.; Perry, M.J.; Cramer, D.W.; Hauser, R. Association of Hexachlorobenzene (HCB), Dichlorodiphenyltrichloroethane (DDT), and Dichlorodiphenyldichloroethylene (DDE) with in Vitro Fertilization (IVF) Outcomes. Environ. Health Perspect. 2012, 120, 316–320. [Google Scholar] [CrossRef]
- Meeker, J.D.; Missmer, A.S.; Altshul, L.; Vitonis, A.F.; Ryan, L.; Cramer, D.W.; Hauser, R. Serum and follicular fluid organochlorine concentrations among women undergoing assisted reproduction technologies. Environ. Health 2009, 8, 10–32. [Google Scholar] [CrossRef] [PubMed]
- Bloom, M.S.; Fujimoto, V.Y.; Storm, R.; Zhang, L.; Butts, C.D.; Sollohub, D.; Jansing, R.L. Persistent organic pollutants (POPs) in human follicular fluid and in vitro fertilization outcomes, a pilot study. Reprod. Toxicol. 2017, 67, 165–173. [Google Scholar] [CrossRef] [PubMed]
- Chiu, Y.-H.; Williams, P.L.; Gillman, M.W.; Gaskins, A.J.; Mínguez-Alarcón, L.; Souter, I.; Toth, T.L.; Ford, J.B.; Hauser, R.; Chavarro, J.E.; et al. Association Between Pesticide Residue Intake from Consumption of Fruits and Vegetables and Pregnancy Outcomes Among Women Undergoing Infertility Treatment with Assisted Reproductive Technology. JAMA Intern. Med. 2018, 178, 17–26. [Google Scholar] [CrossRef]
- Jurewicz, J.; Radwan, M.; Wielgomas, B.; Karwacka, A.; Klimowska, A.; Kałużny, P.; Radwan, P.; Hanke, W. Parameters of ovarian reserve in relation to urinary concentrations of parabens. Environ. Health 2020, 19, 1–8. [Google Scholar] [CrossRef]
- Whitworth, K.W.; Baird, D.D.; Steiner, A.Z.; Bornman, R.M.S.; Travlos, G.S.; Wilson, R.E.; Longnecker, M.P. Anti-Müllerian Hormone and Lifestyle, Reproductive, and Environmental Factors Among Women in Rural South Africa. Epidemiology 2015, 26, 429–435. [Google Scholar] [CrossRef]
- Marettova, E.; Maretta, M.; Legáth, J. Effect of pyrethroids on female genital system. Review. Anim. Reprod. Sci. 2017, 184, 132–138. [Google Scholar] [CrossRef]
- Patel, S. Disruption of aromatase homeostasis as the cause of a multiplicity of ailments: A comprehensive review. J. Steroid Biochem. Mol. Biol. 2017, 168, 19–25. [Google Scholar] [CrossRef]
- Rattan, S.; Zhou, C.; Chiang, C.; Mahalingam, S.; Brehm, E.; Flaws, J.A. Exposure to endocrine disruptors during adulthood: Consequences for female fertility. J. Endocrinol. 2017, 233, R109–R129. [Google Scholar] [CrossRef] [PubMed]
- Sharma, R.K.; Singh, P.; Setia, A.; Sharma, A.K. Insecticides and ovarian functions. Environ. Mol. Mutagen. 2020, 61, 369–392. [Google Scholar] [CrossRef]
- Piazza, M.J.; Urbanetz, A.A. Environmental toxins and the impact of other endocrine disrupting chemicals in women’s reproductive health. JBRA Assist. Reprod. 2019, 23, 154–164. [Google Scholar] [CrossRef] [PubMed]
- Vabre, P.; Gatimel, N.; Moreau, J.; Gayrard, V.; Picard-Hagen, N.; Parinaud, J.; Léandri, R. Environmental pollutants, a possible etiology for premature ovarian insufficiency: A narrative review of animal and human data. Environ. Health 2017, 16, 1–18. [Google Scholar] [CrossRef]
- Garry, V.F.; Harkins, M.; Lyubimov, A.; Erickson, L.; Long, L. Reproductive outcomes in the women of the red river valley of the north. I. The spouses of pesticide applicators: Pregnancy loss, age at menarche, and exposures to pesticides. J. Toxicol. Environ. Health Part. A 2002, 65, 769–786. [Google Scholar] [CrossRef]
- Naidoo, S.; London, L.; Burdorf, A.; Naidoo, R.; Kromhout, H. Spontaneous miscarriages and infant deaths among female farmers in rural South Africa. Scand. J. Work. Environ. Health 2010, 37, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Rahimi, T.; Rafati, F.; Sharifi, H.; Seyedi, F. General and reproductive health outcomes among female greenhouse workers: A comparative study. BMC Women’s Health 2020, 20, 103. [Google Scholar] [CrossRef] [PubMed]
- Vasiliu, O.; Muttineni, J.; Karmaus, W. In utero exposure to organochlorines and age at menarche. Hum. Reprod. 2004, 19, 1506–1512. [Google Scholar] [CrossRef]
- Ye, X.; Pan, W.; Zhao, Y.; Zhao, S.; Zhu, Y.; Liu, W.; Liu, J. Association of pyrethroids exposure with onset of puberty in Chinese girls. Environ. Pollut. 2017, 227, 606–612. [Google Scholar] [CrossRef]
- Ouyang, F.; Perry, M.J.; Venners, A.S.; Chen, C.; Wang, B.; Yang, F.; Fang, Z.; Zang, T.; Wang, L.; Xu, X.; et al. Serum DDT, age at menarche, and abnormal menstrual cycle length. Occup. Environ. Med. 2005, 62, 878–884. [Google Scholar] [CrossRef]
- Namulanda, G.; Taylor, E.; Maisonet, M.; Barr, D.B.; Flanders, W.D.; Olson, D.; Qualters, J.R.; Vena, J.; Northstone, K.; Naeher, L. In utero exposure to atrazine analytes and early menarche in the Avon Longitudinal Study of Parents and Children Cohort. Environ. Res. 2017, 156, 420–425. [Google Scholar] [CrossRef] [PubMed]
- Louis, G.M.B.; Rios, L.I.; McLain, A.; Cooney, M.A.; Kostyniak, P.J.; Sundaram, R. Persistent organochlorine pollutants and menstrual cycle characteristics. Chemosphere 2011, 85, 1742–1748. [Google Scholar] [CrossRef]
- Tetsatsi, A.C.M.; Munyali, D.A.; Fozin, G.R.B.; Ngadjui, E.; Wankeu-Nya, M.; Watcho, P. Semen quality among men attending urology services in the Dschang Health District, west Cameroon: A retrospective study on 379 cases. Int. J. Reprod. Biomed. 2020, 18, 121–128. [Google Scholar] [CrossRef]
- Lwin, T.Z.; Than, A.A.; Min, A.Z.; Robson, M.G.; Siriwong, W. Effects of pesticide exposure on reproductivity of male groundnut farmers in Kyauk Kan village, Nyaung-U, Mandalay region, Myanmar. Risk Manag. Health. Policy 2018, 11, 235–241. [Google Scholar] [CrossRef]
- Sengupta, P.; Nwagha, U.; Dutta, S.; Krajewska-Kulak, E.; Izuka, E. Evidence for decreasing sperm count in African population from 1965 to 2015. Afr. Health Sci. 2017, 17, 418–427. [Google Scholar] [CrossRef]
- Neghab, M.; Momenbella-Fard, M.; Naziaghdam, R.; Salahshour, N.; Kazemi, M.; Alipour, H. The effects of exposure to pesticides on the fecundity status of farm workers resident in a rural region of Fars province, southern Iran. Asian Pac. J. Trop. Biomed. 2014, 4, 324–328. [Google Scholar] [CrossRef] [PubMed]
- Cremonese, C.; Piccoli, C.; Pasqualotto, F.; Clapauch, R.; Koifman, R.J.; Koifman, S.; Freire, C. Occupational exposure to pesticides, reproductive hormone levels and sperm quality in young Brazilian men. Reprod. Toxicol. 2017, 67, 174–185. [Google Scholar] [CrossRef]
- Miranda-Contreras, L.; Gómez-Pérez, R.; Rojas, G.; Cruz, I.; Berrueta, L.; Salmen, S.; Colmenares, M.; Barreto, S.; Balza, A.; Zavala, L.; et al. Occupational Exposure to Organophosphate and Carbamate Pesticides Affects Sperm Chromatin Integrity and Reproductive Hormone Levels among Venezuelan Farm Workers. J. Occup. Health 2013, 55, 195–203. [Google Scholar] [CrossRef]
- Yucra, S.; Rubio, J.; Gasco, M.; Gonzales, C.; Steenland, K.; Gonzales, G.F. Semen Quality and Reproductive Sex Hormone Levels in Peruvian Pesticide Sprayers. Int. J. Occup. Environ. Health 2006, 12, 355–361. [Google Scholar] [CrossRef]
- Dhooge, W.; Van Larebeke, N.; Comhaire, F.; Kaufman, J.-M. Reproductive Parameters of Community-Dwelling Men From 2 Regions in Flanders Are Associated With the Consumption of Self-Grown Vegetables. J. Androl. 2007, 28, 836–846. [Google Scholar] [CrossRef] [PubMed]
- Yucra, S.; Gasco, M.; Rubio, J.; Gonzales, G.F. Semen quality in Peruvian pesticide applicators: Association between urinary organophosphate metabolites and semen parameters. Environ. Health 2008, 7, 59. [Google Scholar] [CrossRef]
- Celik-Ozenci, C.; Tasatargil, A.; Tekcan, M.; Sati, L.; Gungor, E.; Isbir, M.; Usta, M.F.; Akar, M.E.; Erler, F. Effect of abamectin exposure on semen parameters indicative of reduced sperm maturity: A study on farmworkers in Antalya (Turkey). Andrologia 2012, 44, 388–395. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Garduño, C.; Lacasaña, M.; Blanco-Muñoz, J.; Rodríguez-Barranco, M.; Hernández, A.; Bassol, S.; González-Alzaga, B.; Cebrián, M. Changes in male hormone profile after occupational organophosphate exposure. A longitudinal study. Toxicology 2013, 307, 55–65. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Zhang, Y.; Vinturache, A.; Wang, Y.; Shi, R.; Chen, L.; Qin, K.; Tian, Y.; Gao, Y. Effects of environmental pyrethroids exposure on semen quality in reproductive-age men in Shanghai, China. Chemosphere 2020, 245, 125580. [Google Scholar] [CrossRef] [PubMed]
- Ji, G.; Xia, Y.; Gu, A.; Shi, X.; Long, Y.; Song, L.; Wang, S.; Wang, X. Effects of non-occupational environmental exposure to pyrethroids on semen quality and sperm DNA integrity in Chinese men. Reprod. Toxicol. 2011, 31, 171–176. [Google Scholar] [CrossRef] [PubMed]
- Yoshinaga, J.; Imai, K.; Shiraishi, H.; Nozawa, S.; Yoshiike, M.; Mieno, M.N.; Andersson, A.-M.; Iwamoto, T. Pyrethroid insecticide exposure and reproductive hormone levels in healthy Japanese male subjects. Andrology 2014, 2, 416–420. [Google Scholar] [CrossRef] [PubMed]
- Imai, K.; Yoshinaga, J.; Yoshikane, M.; Shiraishi, H.; Mieno, M.N.; Yoshiike, M.; Nozawa, S.; Iwamoto, T. Pyrethroid insecticide exposure and semen quality of young Japanese men. Reprod. Toxicol. 2014, 43, 38–44. [Google Scholar] [CrossRef] [PubMed]
- Toshima, H.; Suzuki, Y.; Imai, K.; Yoshinaga, J.; Shiraishi, H.; Mizumoto, Y.; Hatakeyama, S.; Onohara, C.; Tokuoka, S. Endocrine disrupting chemicals in urine of Japanese male partners of subfertile couples: A pilot study on exposure and semen quality. Int. J. Hyg. Environ. Health 2012, 215, 502–506. [Google Scholar] [CrossRef] [PubMed]
- Radwan, M.; Jurewicz, J.; Wielgomas, B.; Sobala, W.; Piskunowicz, M.; Radwan, P.; Hanke, W. Semen Quality and the Level of Reproductive Hormones After Environmental Exposure to Pyrethroids. J. Occup. Environ. Med. 2014, 56, 1113–1119. [Google Scholar] [CrossRef] [PubMed]
- Meeker, J.D.; Barr, D.B.; Hauser, R. Human semen quality and sperm DNA damage in relation to urinary metabolites of pyrethroid insecticides. Hum. Reprod. 2008, 23, 1932–1940. [Google Scholar] [CrossRef] [PubMed]
- Young, A.H.; Meeker, J.D.; Martenies, E.S.; Figueroa, I.Z.; Barr, D.B.; Perry, M.J. Environmental exposure to pyrethroids and sperm sex chromosome disomy: A cross-sectional study. Environ. Health 2013, 12, 111. [Google Scholar] [CrossRef]
- Pant, N.; Shukla, M.; Upadhyay, A.D.; Chaturvedi, P.K.; Saxena, D.K.; Gupta, Y.K. Association between environmental exposure to p, p’-DDE and lindane and semen quality. Environ. Sci. Pollut. Res. 2014, 21, 11009–11016. [Google Scholar] [CrossRef]
- Hauser, R.; Chen, Z.; Pothier, L.; Ryan, L.; Altshul, L. The relationship between human semen parameters and environmental exposure to polychlorinated biphenyls and p,p’-DDE. Environ. Health Perspect. 2003, 111, 1505–1511. [Google Scholar] [CrossRef] [PubMed]
- Haugen, T.B.; Tefre, T.; Malm, G.; Jönsson, B.A.; Rylander, L.; Hagmar, L.; Bjørsvik, C.; Henrichsen, T.; Sæther, T.; Figenschau, Y.; et al. Differences in serum levels of CB-153 and p,p’-DDE, and reproductive parameters between men living south and north in Norway. Reprod. Toxicol. 2011, 32, 261–267. [Google Scholar] [CrossRef]
- Perry, M.J.; Young, H.A.; Grandjean, P.; Halling, J.; Petersen, M.S.; Martenies, S.; Karimi, P.; Weihe, P. Sperm Aneuploidy in Faroese Men with Lifetime Exposure to Dichlorodiphenyldichloroethylene (p,p’-DDE) and Polychlorinated Biphenyl (PCB) Pollutants. Environ. Health Perspect. 2016, 124, 951–956. [Google Scholar] [CrossRef]
- Bae, J.; Kim, S.; Barr, D.B.; Louis, G.M.B. Maternal and paternal serum concentrations of persistent organic pollutants and the secondary sex ratio: A population-based preconception cohort study. Environ. Res. 2018, 161, 9–16. [Google Scholar] [CrossRef]
- Giwercman, A.; Rylander, L.; Rignell-Hydbom, A.; Jönsson, B.A.; Pedersen, H.S.; Ludwicki, J.K.; Lesovoy, V.; Zvyezday, V.; Spano, M.; Manicardi, G.C.; et al. Androgen receptor gene CAG repeat length as a modifier of the association between persistent organohalogen pollutant exposure markers and semen characteristics. Pharm. Genom. 2007, 17, 391–401. [Google Scholar] [CrossRef] [PubMed]
- Toft, G.; Rignell-Hydbom, A.; Tyrkiel, E.; Shvets, M.; Giwercman, A.; Lindh, C.H.; Pedersen, H.S.; Ludwicki, J.K.; Lesovoy, V.; Hagmar, L.; et al. Semen Quality and Exposure to Persistent Organochlorine Pollutants. Epidemiology 2006, 17, 450–458. [Google Scholar] [CrossRef]
- Tiido, T.; Rignell-Hydbom, A.; Jönsson, B.A.; Giwercman, Y.L.; Pedersen, H.S.; Wojtyniak, B.; Ludwicki, J.K.; Lesovoy, V.; Zvyezday, V.; Spano, M.; et al. Impact of PCB andp,p’-DDE Contaminants on Human Sperm Y:X Chromosome Ratio: Studies in Three European Populations and the Inuit Population in Greenland. Environ. Health Perspect. 2006, 114, 718–724. [Google Scholar] [CrossRef]
- Stronati, A.; Manicardi, G.C.; Cecati, M.; Bordicchia, M.; Ferrante, L.; Spanò, M.; Toft, G.; Bonde, J.P.; Jönsson, B.A.G.; Rignell-Hydbom, A.; et al. Relationships between sperm DNA fragmentation, sperm apoptotic markers and serum levels of CB-153 and p,p’-DDE in European and Inuit populations. Reproduction 2006, 132, 949–958. [Google Scholar] [CrossRef] [PubMed]
- Dziewirska, E.; Radwan, M.; Wielgomas, B.; Klimowska, A.; Radwan, P.; Kałużny, P.; Hanke, W.; Słodki, M.; Jurewicz, J. Human Semen Quality, Sperm DNA Damage, and the Level of Urinary Concentrations of 1N and TCPY, the Biomarkers of Nonpersistent Insecticides. Am. J. Men’s Health 2018, 13, 1557988318816598. [Google Scholar] [CrossRef] [PubMed]
- Swan, S.H. Semen quality in fertile US men in relation to geographical area and pesticide exposure. Int. J. Androl. 2006, 29, 62–68. [Google Scholar] [CrossRef]
- Swan, S.H.; Kruse, R.; Liu, F.; Barr, D.B.; Drobnis, E.Z.; Redmon, J.B.; Wang, C.; Brazil, C.; Overstreet, J.W. Study for Future Families Research Group Semen quality in relation to biomarkers of pesticide exposure. Environ. Health Perspect. 2003, 111, 1478–1484. [Google Scholar] [CrossRef]
- Luderer, U.; Kesner, J.S.; Fuller, J.M.; Krieg, E.F.; Meadows, J.W.; Tramma, S.L.; Yang, H.; Baker, D. Effects of gestational and lactational exposure to heptachlor epoxide on age at puberty and reproductive function in men and women. Environ. Res. 2013, 121, 84–94. [Google Scholar] [CrossRef]
- Mathiesen, L.; Mørck, T.A.; Poulsen, M.S.; Nielsen, J.K.S.; Mose, T.; Long, M.; Bonefeld-Jørgensen, E.; Bossi, R.; Knudsen, L.E. Placental transfer of pesticides studied in human placental perfusion. Basic Clin. Pharmacol. Toxicol. 2020, 127, 505–515. [Google Scholar] [CrossRef]
- Fukata, H.; Omori, M.; Osada, H.; Todaka, E.; Mori, C. Necessity to Measure PCBs and Organochlorine Pesticide Concentrations in Human Umbilical Cords for Fetal Exposure Assessment. Environ. Health Perspect. 2005, 113, 297–303. [Google Scholar] [CrossRef] [PubMed]
- Vizcaino, E.; Grimalt, J.O.; Somoano, A.F.; Tardon, A. Transport of persistent organic pollutants across the human placenta. Environ. Int. 2014, 65, 107–115. [Google Scholar] [CrossRef]
- Yin, S.; Zhang, J.; Guo, F.; Poma, G.; Covaci, A.; Liu, W. Transplacental transfer mechanism of organochlorine pesticides: An in vitro transcellular transport study. Environ. Int. 2020, 135, 105402. [Google Scholar] [CrossRef]
- Zhang, X.; Wu, X.; Lei, B.; Jing, Y.; Jiang, Z.; Zhang, X.; Fang, X.; Yu, Y. Transplacental transfer characteristics of organochlorine pesticides in paired maternal and cord sera, and placentas and possible influencing factors. Environ. Pollut. 2018, 233, 446–454. [Google Scholar] [CrossRef] [PubMed]
- Holland, N.; Furlong, C.; Bastaki, M.; Richter, R.; Bradman, A.; Huen, K.; Beckman, K.; Eskenazi, B. Paraoxonase Polymorphisms, Haplotypes, and Enzyme Activity in Latino Mothersand Newborns. Environ. Health Perspect. 2006, 114, 985–991. [Google Scholar] [CrossRef] [PubMed]
- Wohlfahrt-Veje, C.; Andersen, H.R.; Schmidt, I.M.; Aksglaede, L.; Sørensen, K.; Juul, A.; Jensen, T.K.; Grandjean, P.; Skakkebaek, N.E.; Main, K.M. Early breast development in girls after prenatal exposure to non-persistent pesticides. Int. J. Androl. 2012, 35, 273–282. [Google Scholar] [CrossRef] [PubMed]
- Wohlfahrt-Veje, C.; Andersen, H.R.; Jensen, T.K.; Grandjean, P.; Skakkebaek, N.E.; Main, K.M. Smaller genitals at school age in boys whose mothers were exposed to non-persistent pesticides in early pregnancy. Int. J. Androl. 2012, 35, 265–272. [Google Scholar] [CrossRef] [PubMed]
- Andersen, H.R.; Schmidt, I.M.; Grandjean, P.; Jensen, T.K.; Budtz-Jørgensen, E.; Kjærstad, M.B.; Bælum, J.; Nielsen, J.B.; Skakkebæk, N.E.; Main, K.M. Impaired Reproductive Development in Sons of Women Occupationally Exposed to Pesticides during Pregnancy. Environ. Health Perspect. 2008, 116, 566–572. [Google Scholar] [CrossRef]
- Gaspari, L.; Paris, F.; Jandel, C.; Kalfa, N.; Orsini, M.; Daurès, J.P.; Sultan, C. Prenatal environmental risk factors for genital malformations in a population of 1442 French male newborns: A nested case-control study. Hum. Reprod. 2011, 26, 3155–3162. [Google Scholar] [CrossRef]
- Dewan, P.; Jain, V.; Gupta, P.; Banerjee, B.D. Organochlorine pesticide residues in maternal blood, cord blood, placenta, and breastmilk and their relation to birth size. Chemosphere 2013, 90, 1704–1710. [Google Scholar] [CrossRef]
- Narduzzi, S.; Fantini, F.; Blasetti, F.; Rantakokko, P.; Kiviranta, H.; Forastiere, F.; Michelozzi, P.; Porta, D. Predictors of Beta-Hexachlorocyclohexane blood levels among people living close to a chemical plant and an illegal dumping site. Environ. Health 2020, 19, 1–9. [Google Scholar] [CrossRef]
- Yu, Y.; Wang, B.; Wang, X.; Wang, R.; Wang, W.; Shen, G.; Shen, H.; Li, W.; Wong, M.; Liu, W.; et al. Hexachlorocyclohexanes (HCHs) in placenta and umbilical cord blood and dietary intake for women in Beijing, China. Environ. Pollut. 2013, 179, 75–80. [Google Scholar] [CrossRef]
- Carlson, B.M.; Brudon, M.C. Human Embryology and Developmental Biology; Elsevier: St. Louis, MO, USA, 2019. [Google Scholar]
- Choi, S.; Kim, H.-J.; Kim, S.; Choi, G.; Kim, S.; Park, J.; Shim, S.-S.; Lee, I.; Kim, S.; Moon, H.-B.; et al. Current status of organochlorine pesticides (OCPs) and polychlorinated biphenyls (PCBs) exposure among mothers and their babies of Korea-CHECK cohort study. Sci. Total Environ. 2018, 618, 674–681. [Google Scholar] [CrossRef] [PubMed]
- Al-Saleh, I.; Al-Doush, I.; Alsabbaheen, A.; Mohamed, G.E.D.; Rabbah, A. Levels of DDT and its metabolites in placenta, maternal and cord blood and their potential influence on neonatal anthropometric measures. Sci. Total Environ. 2012, 416, 62–74. [Google Scholar] [CrossRef]
- Torres-Sanchez, L.; Zepeda, M.; Cebrian, M.E.; Belkind-Gerson, J.; Garcia-Hernandez, R.M.; Belkind-Valdovinos, U.; López-Carrillo, L. Dichlorodiphenyldichloroethylene exposure during the first trimester of pregnancy alters the anal position in male infants. Ann. New York Acad. Sci. 2008, 1140, 155–162. [Google Scholar] [CrossRef]
- Fernandez, M.F.; Olmos, B.; Granada, A.; López-Espinosa, M.J.; Molina-Molina, J.-M.; Fernandez, J.M.; Cruz, M.; Olea-Serrano, F.; Olea, N. Human Exposure to Endocrine-Disrupting Chemicals and Prenatal Risk Factors for Cryptorchidism and Hypospadias: A Nested Case–Control Study. Environ. Health Perspect. 2007, 115 (Suppl. 1), 8–14. [Google Scholar] [CrossRef]
- Eskenazi, B.; Rauch, S.A.; Tenerelli, R.; Huen, K.; Holland, N.T.; Lustig, R.H.; Kogut, K.; Bradman, A.; Sjödin, A.; Harley, K.G. In utero and childhood DDT, DDE, PBDE and PCBs exposure and sex hormones in adolescent boys: The CHAMACOS study. Int. J. Hyg. Environ. Health 2017, 220, 364–372. [Google Scholar] [CrossRef] [PubMed]
- Vested, A.; Ramlau-Hansen, C.H.; Olsen, S.F.; Bonde, J.P.; Støvring, H.; Kristensen, S.L.; Halldorsson, I.T.; Rantakokko, P.; Kiviranta, H.; Ernst, E.H.; et al. In utero exposure to persistent organochlorine pollutants and reproductive health in the human male. Reproduction 2014, 148, 635–646. [Google Scholar] [CrossRef] [PubMed]
- Cohn, A.B.; Cirillo, P.M.; Wolff, M.S.; Schwingl, P.J.; Cohen, R.D.; Sholtz, I.R.; Ferrara, A.; Christianson, E.R.; Berg, B.J.V.D.; Siiteri, P.K. DDT and DDE exposure in mothers and time to pregnancy in daughters. Lancet 2003, 361, 2205–2206. [Google Scholar] [CrossRef]
- You, L.; Sar, M.; Bartolucci, E.; Ploch, S.; Whitt, M. Induction of hepatic aromatase by p,p’-DDE in adult male rats. Mol. Cell. Endocrinol. 2001, 178, 207–214. [Google Scholar] [CrossRef]
- Massaad, C.; Entezami, F.; Massade, L.; Benahmed, M.; Olivennes, F.; Barouki, R.; Hamamah, S. How can chemical compounds alter human fertility? Eur. J. Obstet. Gynecol. Reprod. Biol. 2002, 100, 127–137. [Google Scholar] [CrossRef]
- Mohammed, A.M.; Karttunen, V.; Huuskonen, P.; Huovinen, M.; Auriola, S.; Vähäkangas, K. Transplacental transfer and metabolism of diuron in human placenta. Toxicol. Lett. 2018, 295, 307–313. [Google Scholar] [CrossRef] [PubMed]
- Qin, K.; Zhang, Y.; Wang, Y.; Shi, R.; Pan, R.; Yao, Q.; Tian, Y.; Gao, Y. Prenatal organophosphate pesticide exposure and reproductive hormones in cord blood in Shandong, China. Int. J. Hyg. Environ. Health 2020, 225, 113479. [Google Scholar] [CrossRef] [PubMed]
- Usmani, K.A.; Hodgson, E.; Rose, R.L. In vitro metabolism of carbofuran by human, mouse, and rat cytochrome P450 and interactions with chlorpyrifos, testosterone, and estradiol. Chem. Interact. 2004, 150, 221–232. [Google Scholar] [CrossRef]
- Araki, A.; Miyashita, C.; Mitsui, T.; Goudarzi, H.; Mizutani, F.; Chisaki, Y.; Itoh, S.; Sasaki, S.; Cho, K.; Moriya, K.; et al. Prenatal organochlorine pesticide exposure and the disruption of steroids and reproductive hormones in cord blood: The Hokkaido study. Environ. Int. 2018, 110, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Warembourg, C.; Debost-Legrand, A.; Bonvallot, N.; Massart, C.; Garlantézec, R.; Monfort, C.; Gaudreau, E.; Chevrier, C.; Cordier, S. Exposure of pregnant women to persistent organic pollutants and cord sex hormone levels. Hum. Reprod. 2015, 31, 190–198. [Google Scholar] [CrossRef]
- Haraux, E.; Tourneux, P.; Kouakam, C.; Stephan-Blanchard, E.; Boudailliez, B.; Leke, A.; Klein, C.; Chardon, K. Isolated hypospadias: The impact of prenatal exposure to pesticides, as determined by meconium analysis. Environ. Int. 2018, 119, 20–25. [Google Scholar] [CrossRef]
- Roncati, L.; Piscioli, F.; Pusiol, T. The endocrine disruptors among the environmental risk factors for stillbirth. Sci. Total. Environ. 2016, 563–564, 1086–1087. [Google Scholar] [CrossRef]
- Sagiv, S.K.; Bruno, J.L.; Baker, J.M.; Palzes, V.; Kogut, K.; Rauch, S.; Gunier, R.; Mora, A.M.; Reiss, A.L.; Eskenazi, B. Prenatal exposure to organophosphate pesticides and functional neuroimaging in adolescents living in proximity to pesticide application. Proc. Natl. Acad. Sci. USA 2019, 116, 18347–18356. [Google Scholar] [CrossRef]
- Hood, E. Are EDCs Blurring Issues of Gender? Environ. Health Perspect. 2005, 113, A670–A677. [Google Scholar] [CrossRef]
- Teodoro, M.; Briguglio, G.; Fenga, C.; Costa, C. Genetic polymorphisms as determinants of pesticide toxicity: Recent advances. Toxicol. Rep. 2019, 6, 564–570. [Google Scholar] [CrossRef]
- Mackness, M.; Mackness, B. Human paraoxonase-1 (PON1): Gene structure and expression, promiscuous activities and multiple physiological roles. Gene 2015, 567, 12–21. [Google Scholar] [CrossRef]
- Costa, L.G.; Cole, T.B.; Furlong, C.E. Polymorphisms of Paraoxonase (PON1) and Their Significance in Clinical Toxicology of Organophosphates. J. Toxicol. Clin. Toxicol. 2003, 41, 37–45. [Google Scholar] [CrossRef]
- Mackness, B.; Durrington, P.; Povey, A.; Thomson, S.; Dippnall, M.; Mackness, M.; Smith, T.; Cherry, N. Paraoxonase and susceptibility to organophosphorus poisoning in farmers dipping sheep. Pharmacogenetics 2003, 13, 81–88. [Google Scholar] [CrossRef]
- Coombes, R.H.; Meek, E.C.; Dail, M.B.; Chambers, H.W.; Chambers, J.E. Human paraoxonase 1 hydrolysis of nanomolar chlorpyrifos-oxon concentrations is unaffected by phenotype or Q192R genotype. Toxicol. Lett. 2014, 230, 57–61. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Declerck, K.; Remy, S.; Wohlfahrt-Veje, C.; Main, K.M.; Van Camp, G.; Schoeters, G.; Berghe, W.V.; Andersen, H.R. Interaction between prenatal pesticide exposure and a common polymorphism in the PON1 gene on DNA methylation in genes associated with cardio-metabolic disease risk—An exploratory study. Clin. Epigenet. 2017, 9, 35. [Google Scholar] [CrossRef]
- Leviev, I.; James, R.W. Promoter polymorphisms of human paraoxonase PON1 gene and serum paraoxonase activities and concentrations. Arter. Thromb. Vasc. Biol. 2000, 20, 516–521. [Google Scholar] [CrossRef]
- Brophy, V.H.; Hastings, M.D.; Clendenning, J.B.; Richter, R.J.; Jarvik, G.P.; Furlong, C.E. Polymorphisms in the human paraoxonase (PON1) promoter. Pharmacogenetics 2001, 11, 77–84. [Google Scholar] [CrossRef] [PubMed]
- Davies, H.G.; Richter, R.J.; Keifer, M.; Broomfield, C.A.; Sowalla, J.; Furlong, C.E. The effect of the human serum paraoxonase polymorphism is reversed with diazoxon, soman and sarin. Nat. Genet. 1996, 14, 334–336. [Google Scholar] [CrossRef]
- Moreno-Banda, G.; Blanco-Muñoz, J.; Lacasaña, M.; Rothenberg, S.; Aguilar-Garduño, C.; Gamboa, R.; Pérez-Méndez, O. Maternal exposure to floricultural work during pregnancy, PON1 Q192R polymorphisms and the risk of low birth weight. Sci. Total. Environ. 2009, 407, 5478–5485. [Google Scholar] [CrossRef]
- Berkowitz, G.S.; Wetmur, J.G.; Birman-Deych, E.; Obel, J.; Lapinski, R.H.; Godbold, J.H.; Holzman, I.R.; Wolff, M.S. In utero pesticide exposure, maternal paraoxonase activity, and head circumference. Environ. Health Perspect. 2004, 112, 388–391. [Google Scholar] [CrossRef] [PubMed]
- Engel, S.M.; Wetmur, J.; Chen, J.; Zhu, C.; Barr, D.B.; Canfield, R.L.; Wolff, M.S. Prenatal Exposure to Organophosphates, Paraoxonase 1, and Cognitive Development in Childhood. Environ. Health Perspect. 2011, 119, 1182–1188. [Google Scholar] [CrossRef] [PubMed]
- Harley, K.G.; Huen, K.; Schall, R.A.; Holland, N.T.; Bradman, A.; Barr, D.B.; Eskenazi, B. Association of Organophosphate Pesticide Exposure and Paraoxonase with Birth Outcome in Mexican-American Women. PLoS ONE 2011, 6, e23923. [Google Scholar] [CrossRef]
- Cole, T.B.; Jampsa, R.L.; Walter, B.J.; Arndt, T.L.; Richter, R.J.; Shih, D.M.; Tward, A.; Lusis, A.J.; Jack, R.M.; Costa, L.G.; et al. Expression of human paraoxonase (PON1) during development. Pharmacogenetics 2003, 13, 357–364. [Google Scholar] [CrossRef]
- Furlong, C.E.; Holland, N.; Richter, R.J.; Bradman, A.; Ho, A.; Eskenazi, B. PON1 status of farmworker mothers and children as a predictor of organophosphate sensitivity. Pharm. Genom. 2006, 16, 183–190. [Google Scholar] [CrossRef]
- Chen, J.; Kumar, M.; Chan, W.; Berkowitz, G.; Wetmur, J.G. Increased influence of genetic variation on PON1 activity in neonates. Environ. Health Perspect. 2003, 111, 1403–1409. [Google Scholar] [CrossRef]
- Andersen, H.R.; Wohlfahrt-Veje, C.; Dalgård, C.; Christiansen, L.; Main, K.M.; Nellemann, C.; Murata, K.; Jensen, T.K.; Skakkebæk, N.E.; Grandjean, P. Paraoxonase 1 Polymorphism and Prenatal Pesticide Exposure Associated with Adverse Cardiovascular Risk Profiles at School Age. PLoS ONE 2012, 7, e36830. [Google Scholar] [CrossRef]
- Jørgensen, A.; Nellemann, C.; Wohlfahrt-Veje, C.; Jensen, T.K.; Main, K.M.; Andersen, H.R. Interaction between paraoxonase 1 polymorphism and prenatal pesticide exposure on metabolic markers in children using a multiplex approach. Reprod. Toxicol. 2015, 51, 22–30. [Google Scholar] [CrossRef]
- Tinggaard, J.; Wohlfahrt-Veje, C.; Husby, S.; Christiansen, L.; Skakkebaek, N.E.; Jensen, T.K.; Grandjean, P.; Main, K.M.; Andersen, H.R.; Skakkebæk, N.E. Prenatal pesticide exposure andPON1genotype associated with adolescent body fat distribution evaluated by dual X-ray absorptiometry (DXA). Andrology 2016, 4, 735–744. [Google Scholar] [CrossRef] [PubMed]
- Padungtod, C.; Niu, T.; Wang, Z.; Savitz, D.A.; Christiani, D.C.; Ryan, L.M.; Xu, X. Paraoxonase polymorphism and its effect on male reproductive outcomes among Chinese pesticide factory workers. Am. J. Ind. Med. 1999, 36, 379–387. [Google Scholar] [CrossRef]
- Pérez-Herrera, N.; Polanco-Minaya, H.; Salazar-Arredondo, E.; Solís-Heredia, M.; Hernández-Ochoa, I.; Rojas-García, E.; Alvarado-Mejía, J.; Borja-Aburto, V.; Quintanilla-Vega, B. PON1Q192R genetic polymorphism modifies organophosphorous pesticide effects on semen quality and DNA integrity in agricultural workers from southern Mexico. Toxicol. Appl. Pharmacol. 2008, 230, 261–268. [Google Scholar] [CrossRef] [PubMed]
- Cherry, N.; Mackness, M.; Durrington, P.; Povery, A.; Dippnall, M.; Smith, T.; Mackness, B. Paraoxonase (PON1) polymorphisms in farmers attributing ill health to sheep dip. Lancet 2002, 359, 763–764. [Google Scholar] [CrossRef]
- Lee, B.W.; London, L.; Paulauskis, J.; Myers, J.; Christiani, D.C. Association Between Human Paraoxonase Gene Polymorphism and Chronic Symptoms in Pesticide-Exposed Workers. J. Occup. Environ. Med. 2003, 45, 118–122. [Google Scholar] [CrossRef]
- Cooney, M.A.; Louis, G.M.B.; Sundaram, R.; McGuiness, B.M.; Lynch, C.D. Validity of Self-Reported Time to Pregnancy. Epidemiology 2009, 20, 56–59. [Google Scholar] [CrossRef] [PubMed]
- Olsen, J. Design options and sources of bias in time-to-pregnancy studies. Scand. J. Work. Environ. Health 1999, 25 (Suppl. 1), 5–7. [Google Scholar] [PubMed]
- Bloom, M.S.; Buck-Louis, G.M.; Schisterman, E.; Kostyniak, P.J.; Vena, J.E. Changes in maternal serum chlorinated pesticide concentrations across critical windows of human reproduction and development. Environ. Res. 2009, 109, 93–100. [Google Scholar] [CrossRef]
- Scacchi, R.; Corbo, R.M.; Rickards, O.; De Stefano, G.F. New data on the world distribution of paraoxonase (PON1 Gln 192 --> Arg) gene frequencies. Hum. Biol. 2003, 75, 365–373. [Google Scholar] [CrossRef]
- Kim, K.; Bloom, M.S.; Fujimoto, V.Y.; Browne, R.W. Associations between PON1 enzyme activities in human ovarian follicular fluid and serum specimens. PLoS ONE 2017, 12, e0172193. [Google Scholar] [CrossRef]
- Ali, S.M.; Chia, S.E. Interethnic variability of plasma paraoxonase (PON1) activity towards organophosphates and PON1 polymorphisms among Asian populations—A short review. Ind. Health 2008, 46, 309–317. [Google Scholar] [CrossRef]
- Rauh, V.A.; Perera, F.P.; Horton, M.K.; Whyatt, R.M.; Bansal, R.; Hao, X.; Liu, J.; Barr, D.B.; Slotkin, T.A.; Peterson, B.S. Brain anomalies in children exposed prenatally to a common organophosphate pesticide. Proc. Natl. Acad. Sci. USA 2012, 109, 7871–7876. [Google Scholar] [CrossRef]
- Salvador-Oliván, J.A.; Marco-Cuenca, G.; Arquero-Avilés, R. Errors in search strategies used in systematic reviews and their effects on information retrieval. J. Med. Libr. Assoc. 2019, 107, 210–221. [Google Scholar] [CrossRef] [PubMed]
- van Weijen, D. The Language of (Future) Scientific Communication. Available online: https://www.researchtrends.com/issue-31-november-2012/the-language-of-future-scientific-communication/ (accessed on 6 June 2021).
- Di Bitetti, M.S.; Ferreras, J.A. Publish (in English) or perish: The effect on citation rate of using languages other than English in scientific publications. Ambio 2016, 46, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Ohlander, J.; Fuhrimann, S.; Basinas, I.; Cherrie, J.W.; Galea, K.S.; Povey, A.C.; Van Tongeren, M.; Harding, A.-H.; Jones, K.; Vermeulen, R.; et al. Systematic review of methods used to assess exposure to pesticides in occupational epidemiology studies, 1993–2017. Occup. Environ. Med. 2020, 77, 357–367. [Google Scholar] [CrossRef] [PubMed]
- Jones, K.; Basinas, I.; Kromhout, H.; van Tongeren, M.; Harding, A.-H.; Cherrie, J.W.; Povey, A.; Ahmad, Z.N.S.; Fuhrimann, S.; Ohlander, J.; et al. Improving Exposure Assessment Methodologies for Epidemiological Studies on Pesticides: Study Protocol. JMIR Res. Protoc. 2020, 9, e16448. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fucic, A.; Duca, R.C.; Galea, K.S.; Maric, T.; Garcia, K.; Bloom, M.S.; Andersen, H.R.; Vena, J.E. Reproductive Health Risks Associated with Occupational and Environmental Exposure to Pesticides. Int. J. Environ. Res. Public Health 2021, 18, 6576. https://doi.org/10.3390/ijerph18126576
Fucic A, Duca RC, Galea KS, Maric T, Garcia K, Bloom MS, Andersen HR, Vena JE. Reproductive Health Risks Associated with Occupational and Environmental Exposure to Pesticides. International Journal of Environmental Research and Public Health. 2021; 18(12):6576. https://doi.org/10.3390/ijerph18126576
Chicago/Turabian StyleFucic, Aleksandra, Radu C. Duca, Karen S. Galea, Tihana Maric, Kelly Garcia, Michael S. Bloom, Helle R. Andersen, and John E. Vena. 2021. "Reproductive Health Risks Associated with Occupational and Environmental Exposure to Pesticides" International Journal of Environmental Research and Public Health 18, no. 12: 6576. https://doi.org/10.3390/ijerph18126576
APA StyleFucic, A., Duca, R. C., Galea, K. S., Maric, T., Garcia, K., Bloom, M. S., Andersen, H. R., & Vena, J. E. (2021). Reproductive Health Risks Associated with Occupational and Environmental Exposure to Pesticides. International Journal of Environmental Research and Public Health, 18(12), 6576. https://doi.org/10.3390/ijerph18126576








