Evaluation of Implementing TOM: A Group-Based Fall Prevention Programme among Community-Dwelling Older Adults in The Netherlands
Abstract
1. Introduction
2. Materials and Methods
2.1. Phases and Components of the Programme
2.1.1. Information Meeting and Screening
2.1.2. Exercise Component
2.1.3. Nutrition Component
2.1.4. Social Component
2.1.5. Closing Event
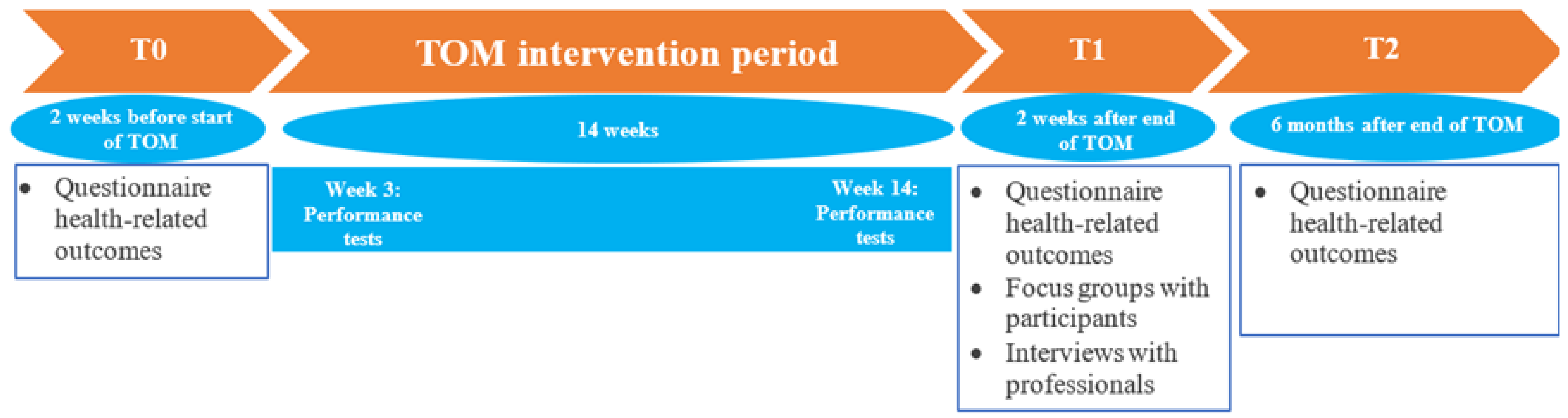
2.2. Study Design
2.3. Programme Evaluation
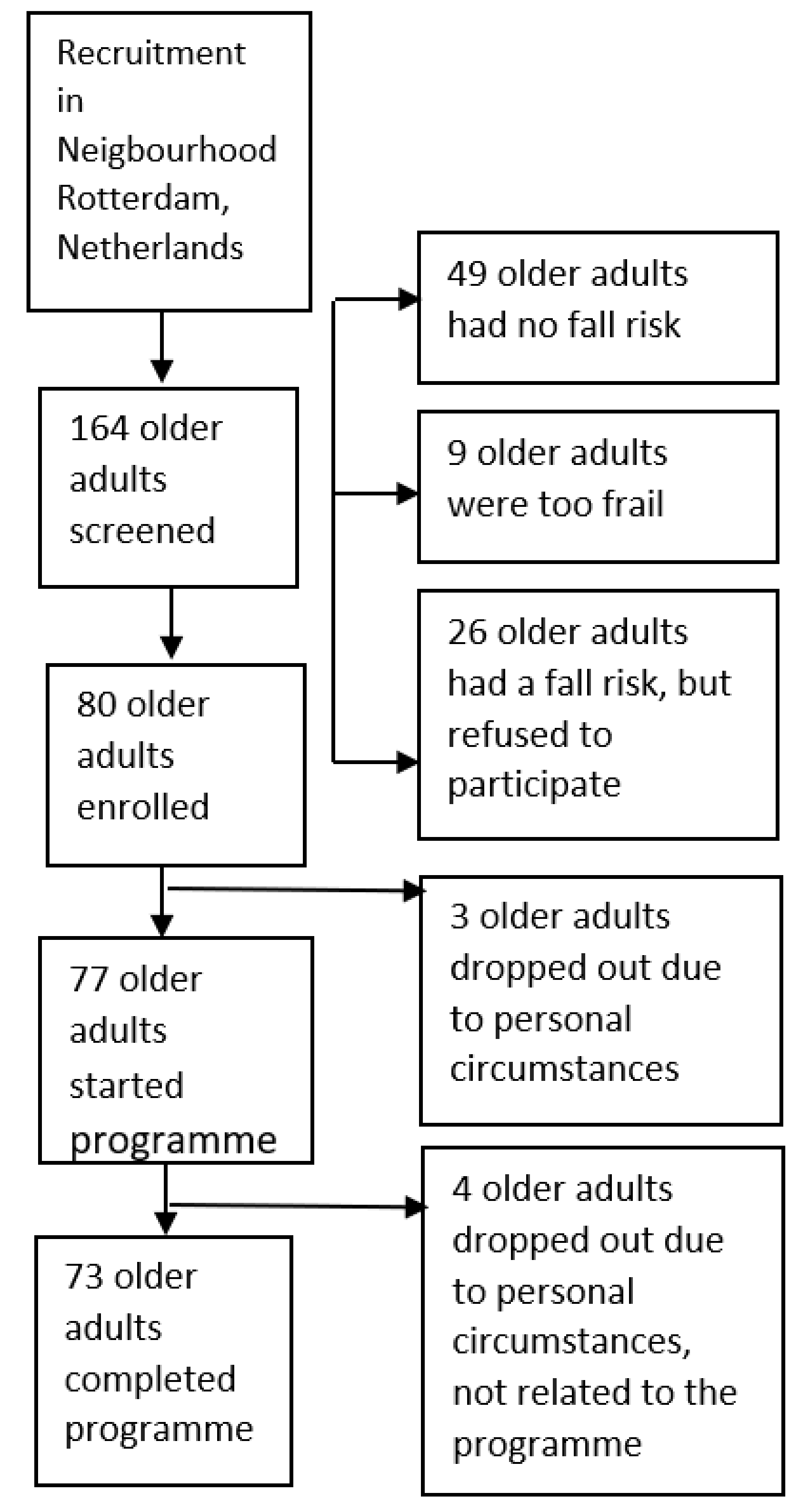
2.3.1. Recruitment of Participants
2.3.2. Impact
2.3.3. Barriers and Facilitators of Implementation
3. Results
3.1. Rectruitment
3.2. Impact
3.3. Barriers and Facilitators of Implementation
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Source | Baseline/Start (T0) | Post-Intervention/End (T1) | 6 Months Follow-Up (T2) | ||
|---|---|---|---|---|---|
| Socio-demographic information | Age, gender, education, marital status, living situation | Self-report | x | x | x |
| Falls history | Number of falls past period | Self-report | x | x | x |
| Quantitative/impact measures | |||||
| Clinical performance-based measures | Physiotherapist | ||||
| Static balance | 4-balance test [29,30] | x | x | ||
| Dynamic balance/mobility | Timed Up-and-Go [25,26] | x | x | ||
| Stability/static balance | Functional reach test (Duncan) | x | x | ||
| Strength | Chair-stand test [28] | x | x | ||
| Self-report | |||||
| Subjective health | Self-report | x | x | x | |
| Fear of falling | FES-I [24] | Self-report | x | x | x |
| Quality of life | EQ-5D [23] | Self-report | x | x | x |
| Physical functioning | SF-36 pfs [22] | Self-report | x | x | x |
| Costs | Costs of preperation, delivery, closing activities, and organisation of the programme | Physiotherapists, dieticians, TOM buddy, local coordinators | x | x | |
| Programme acceptability | |||||
| Adherence | Self-report | x | |||
| Satisfaction | Self-report | x | |||
| Qualitative measures | |||||
| Participants | Focus group; barriers and facilitators | x | |||
| Professionals | Semi-structured interviews; barriers and facilitators | x |
References
- Sherrington, C.; Fairhall, N.; Wallbank, G.; Tiedemann, A.; Michaleff, Z.A.; Howard, K.; Clemson, L.; Hopewell, S.; Lamb, S. Exercise for preventing falls in older people living in the community: An abridged Cochrane systematic review. Br. J. Sports Med. 2020, 54, 885–891. [Google Scholar] [CrossRef] [PubMed]
- GBD Causes of Death Collaborators. Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1736–1788. [Google Scholar] [CrossRef]
- Juckett, L.A.; Bunger, A.C.; Jarrott, S.E.; Dabelko-Schoeny, H.I.; Krok-Schoen, J.; Poling, R.M.; Mion, L.C.; Tucker, S. Determinants of Fall Prevention Guideline Implementation in the Home- and Community-Based Service Setting. Gerontologist 2020. [Google Scholar] [CrossRef] [PubMed]
- Stenhagen, M.; Ekström, H.; Nordell, E.; Elmståhl, S. Accidental falls, health-related quality of life and life satisfaction: A prospective study of the general elderly population. Arch. Gerontol. Geriatr. 2014, 58, 95–100. [Google Scholar] [CrossRef]
- Yoshikawa, A.; Ramirez, G.; Smith, M.L.; Lee, S.; Ory, M.G. Systematic review and meta-analysis of fear of falling and fall-related efficacy in a widely disseminated community-based fall prevention program. Arch. Gerontol. Geriatr. 2020, 91, 104235. [Google Scholar] [CrossRef]
- Schoene, D.; Heller, C.; Aung, Y.N.; Sieber, C.C.; Kemmler, W.; Freiberger, E. A systematic review on the influence of fear of falling on quality of life in older people: Is there a role for falls? Clin. Interv. Aging 2019, 14, 701–719. [Google Scholar] [CrossRef]
- Petersen, N.; König, H.-H.; Hajek, A. The link between falls, social isolation and loneliness: A systematic review. Arch. Gerontol. Geriatr. 2020, 88, 104020. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Ros, P.; Martínez-Arnau, F.M.; Tarazona-Santabalbina, F.J. Risk Factors and Number of Falls as Determinants of Quality of Life of Community-Dwelling Older Adults. J. Geriatr. Phys. Ther. 2019, 42, 63–72. [Google Scholar] [CrossRef]
- Hopewell, S.; Adedire, O.; Copsey, B.J.; Boniface, G.J.; Sherrington, C.; Clemson, L.; Close, J.C.; Lamb, S. Multifactorial and multiple component interventions for preventing falls in older people living in the community. Cochrane Database Syst. Rev. 2018, 7, CD012221. [Google Scholar] [CrossRef] [PubMed]
- Elizabeth, E.; Eckstrom, E.; Harmer, P.; Fitzgerald, K.; Voit, J.; Cameron, K.A. Exercise and Fall Prevention: Narrowing the Research-to-Practice Gap and Enhancing Integration of Clinical and Community Practice. J. Am. Geriatr. Soc. 2016, 64, 425–431. [Google Scholar] [CrossRef]
- Hicks, G.E. Addressing Balance, Mobility, and Falls: Are We Moving the Needle on Fall Prevention? J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2019, 74, 1487–1488. [Google Scholar] [CrossRef]
- Haines, T.P.; Day, L.; Hill, K.D.; Clemson, L.; Finch, C. “Better for others than for me”: A belief that should shape our efforts to promote participation in falls prevention strategies. Arch. Gerontol. Geriatr. 2014, 59, 136–144. [Google Scholar] [CrossRef]
- Lukaszyk, C.; Coombes, J.; Sherrington, C.; Tiedemann, A.; Keay, L.; MacKean, T.; Clemson, L.; Cumming, R.; Broe, T.; Ivers, R. The Ironbark program: Implementation and impact of a community-based fall prevention pilot program for older Aboriginal and Torres Strait Islander people. Heal. Promot. J. Aust. 2018, 29, 189–198. [Google Scholar] [CrossRef]
- Faber, M.J.; Bosscher, R.J.; Paw, M.J.C.A.; van Wieringen, P.C. Effects of Exercise Programs on Falls and Mobility in Frail and Pre-Frail Older Adults: A Multicenter Randomized Controlled Trial. Arch. Phys. Med. Rehabil. 2006, 87, 885–896. [Google Scholar] [CrossRef]
- In Balans: Valpreventie Programma Voor Ouderen|Loketgezondleven.nl. Available online: https://interventies.loketgezondleven.nl/leefstijlinterventies/interventies-zoeken/1400740 (accessed on 28 July 2020).
- Bukman, A.J.; Ronteltap, A.; Lebrun, M. Interpersonal determinants of eating behaviours in Dutch older adults living independently: A qualitative study. BMC Nutr. 2020, 6, 1–12. [Google Scholar] [CrossRef] [PubMed]
- City of Rotterdam—Database. Available online: https://onderzoek010.nl//jive (accessed on 6 March 2021).
- Faber, M.J.; Bosscher, R.J.; Van Wieringen, P.C.W. Clinimetric Properties of the Performance-Oriented Mobility Assessment. Phys. Ther. 2006, 86, 944–954. [Google Scholar] [CrossRef] [PubMed]
- Tinetti, M.E. Performance-Oriented Assessment of Mobility Problems in Elderly Patients. J. Am. Geriatr. Soc. 1986, 34, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Pin, T.W. Psychometric Properties of 2-Minute Walk Test: A Systematic Review. Arch. Phys. Med. Rehabil. 2014, 95, 1759–1775. [Google Scholar] [CrossRef]
- Selman, J.P.; De Camargo, A.A.; Santos, J.; Lanza, F.C.; Corso, S.D. Reference Equation for the 2-Minute Walk Test in Adults and the Elderly. Respir. Care 2013, 59, 525–530. [Google Scholar] [CrossRef] [PubMed]
- Wijnhoven, H.; Schilp, J.; Schueren, M.A.V.B.-D.V.D.; De Vet, H.C.; Kruizenga, H.M.; Deeg, R.J.; Ferrucci, L.; Visser, M. Development and validation of criteria for determining undernutrition in community-dwelling older men and women: The Short Nutritional Assessment Questionnaire 65+. Clin. Nutr. 2012, 31, 351–358. [Google Scholar] [CrossRef]
- Bohannon, R.W.; De Pasquale, L. Physical Functioning Scale of the Short-Form (SF) 36: Internal consistency and validity with older adults. J. Geriatr. Phys. Ther. 2010, 33, 16–18. [Google Scholar]
- Versteegh, M.M.; Vermeulen, K.M.; Evers, S.M.A.A.; de Wit, G.A.; Prenger, R.; Stolk, E.A. Dutch Tariff for the Five-Level Version of EQ-5D. Value Health 2016, 19, 343–352. [Google Scholar] [CrossRef]
- Kempen, G.I.J.M.; Yardley, L.; Van Haastregt, J.C.M.; Zijlstra, G.A.R.; Beyer, N.; Hauer, K.; Todd, C. The Short FES-I: A shortened version of the falls efficacy scale-international to assess fear of falling. Age Ageing 2007, 37, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Bohannon, R.W. Reference Values for the Timed Up and Go Test. J. Geriatr. Phys. Ther. 2006, 29, 64–68. [Google Scholar] [CrossRef] [PubMed]
- Podsiadlo, D.; Richardson, S. The Timed “Up & Go”: A Test of Basic Functional Mobility for Frail Elderly Persons. J. Am. Geriatr. Soc. 1991, 39, 142–148. [Google Scholar] [CrossRef]
- Duncan, P.; Weiner, D.K.; Chandler, J.; Studenski, S. Functional Reach: A New Clinical Measure of Balance. J. Gerontol. 1990, 45, M192–M197. [Google Scholar] [CrossRef] [PubMed]
- Rikli, R.E.; Jones, C.J. Functional Fitness Normative Scores for Community-Residing Older Adults, Ages 60–94. J. Aging Phys. Act. 1999, 7, 162–181. [Google Scholar] [CrossRef]
- Renfro, M.; Bainbridge, D.B.; Smith, M.L. Validation of Evidence-Based Fall Prevention Programs for Adults with Intellectual and/or Developmental Disorders: A Modified Otago Exercise Program. Front. Public Health 2016, 4, 261. [Google Scholar] [CrossRef]
- The Four Stage Balance Test. Available online: https://www.cdc.gov/steadi/materials.html (accessed on 23 February 2021).
- CBS. CBS Stateline. Available online: https://opendata.cbs.nl/#/CBS/nl/navigatieScherm/thema?themaNr=52050 (accessed on 23 February 2021).
- Olij, B.F.; Erasmus, V.; Barmentloo, L.M.; Burdorf, A.; Smilde, D.; Schoon, Y.; Van Der Velde, N.; Polinder, S. Evaluation of Implementing a Home-Based Fall Prevention Program among Community-Dwelling Older Adults. Int. J. Environ. Res. Public Heal. 2019, 16, 1079. [Google Scholar] [CrossRef]
- Nkimbeng, M.; Roberts, L.; Thorpe, J.R.J.; Gitlin, L.N.; Delaney, A.; Tanner, E.; Szanton, S.L. Recruiting Older Adults with Functional Difficulties Into a Community-Based Research Study: Approaches and Costs. J. Appl. Gerontol. 2020, 39, 644–650. [Google Scholar] [CrossRef]
- Barmentloo, L.M.; Olij, B.F.; Erasmus, V.; Smilde, D.; Schoon, Y.; Polinder, S. Personal preferences of participation in fall prevention programmes: A descriptive study. BMC Geriatr. 2020, 20, 185. [Google Scholar] [CrossRef] [PubMed]
- Shandro, J.R.; Spain, D.A.; Dicker, R.A. Recruitment Strategies for a Fall Prevention Program: If We Build It, Will They Really Come? J. Trauma Inj. Infect. Crit. Care 2007, 63, 142–146. [Google Scholar] [CrossRef]
- Di Lorito, C.; Long, A.; Byrne, A.; Harwood, R.H.; Gladman, J.R.; Schneider, S.; Logan, P.; Bosco, A.; van der Wardt, V. Exercise interventions for older adults: A systematic review of meta-analyses. J. Sport Health Sci. 2021, 10, 29–47. [Google Scholar] [CrossRef] [PubMed]
- Bunn, F.; Dickinson, A.; Barnett-Page, E.; McInnes, E.; Horton, K. A systematic review of older people’s perceptions of facilitators and barriers to participation in falls-prevention interventions. Ageing Soc. 2008, 28, 449–472. [Google Scholar] [CrossRef]
- Stormacq, C.; Broucke, S.V.D.; Wosinski, J. Does health literacy mediate the relationship between socioeconomic status and health disparities? Integrative review. Heal. Promot. Int. 2019, 34, e1–e17. [Google Scholar] [CrossRef] [PubMed]
- Bergen, G.; Stevens, M.R.; Kakara, R.; Burns, E.R. Understanding Modifiable and Unmodifiable Older Adult Fall Risk Factors to Create Effective Prevention Strategies. Am. J. Lifestyle Med. 2019. [Google Scholar] [CrossRef]
- Jin, A.; Brussoni, M.; George, M.A.; Lalonde, C.; McCormick, R. Risk of Hospitalization Due to Unintentional Fall Injury in British Columbia, Canada, 1999–2008: Ecological Associations with Socioeconomic Status, Geographic Place, and Aboriginal Ethnicity. J. Racial Ethn. Health Disparities 2016, 4, 558–570. [Google Scholar] [CrossRef]
- Peel, N.M.; Travers, C.; Bell, R.A.R.; Smith, K. Evaluation of a health service delivery intervention to promote falls prevention in older people across the care continuum. J. Eval. Clin. Pr. 2010, 16, 1254–1261. [Google Scholar] [CrossRef]
- Nilsen, P. Making sense of implementation theories, models and frameworks. Implement. Sci. 2015, 10, 1–13. [Google Scholar] [CrossRef]
- VeiligheidNL. Thuis Onbezorgd Mobiel. Available online: https://www.veiligheid.nl/valpreventie/interventies/integrale-aanpak/thuis-onbezorgd-mobiel (accessed on 23 February 2021).

| Self-Reported Health-Related Variables | T0 | T1 | T2 |
|---|---|---|---|
| Self-reported health—av (SD) | 3.16 (±0.75) | 2.51 (±0.78) * | 2.81 (±0.83) ±, α |
| Much better than previous measurement—% (#) | 3.5% (2) | 12.1% (7) | 10.3% (6) |
| Somewhat better previous measurement—% (#) | 8.8% (5) | 32.8% (19) | 17.2% (10) |
| Roughly the same as previous measurement—% (#) | 57.9% (33) | 51.7% (30) | 58.6% (34) |
| Somewhat worse than previous measurement —% (#) | 28.1% (16) | 1.7% (1) | 12.1% (7) |
| Much worse than previous measurement—% (#) | 1.8% (1) | 1.7% (1) | 1.7% (1) |
| VAS score self-reported health—av (SD) | 70.2 (±13.2) (range 40–95) | 75.2 (±11.0) * (range 50–98) | 73.8 (±11.0) ± (range 45–100) |
| EQ5-DL total score—av (SD) | 0.7578 (±0.17) | 0.7873 (±0.17) * | 0.8123 (±0.16) ± |
| SF-36 score—av (SD) | 68.0 (±21.12) | 72.5 (±21.4) * | 65.8 (±24.3) |
| Short FES-I score—av SD | 10.7 (±3.6) | 10.3 (±3.3) | 10.1 (±3.3) |
| Suffered a fall? | |||
| Yes—% (#) | 31.0% (18) | 29.3% (17) | 22.4% (13) |
| No—% (#) | 69.0% (40) | 70.7% (41) | 77.6% (45) |
| Number of falls | |||
| Fell once—# | 7 | 10 | 10 |
| Fell twice—# | 8 | 8 | 3 |
| Fell three times—# | 12 | 6 | |
| Fell four times—# | 4 | ||
| Total number of falls—# | 31 | 24 | 16 |
| Per faller—falls/# fallers | 1.94 | 1.5 | 1.2 |
| Performance Test | Week 3 | Week 14 | p-Value | % Progress between Week 3 and 4 of Total Participants |
|---|---|---|---|---|
| Timed Up-and-Go (mobility/dynamic balance) (s) (n = 66) | 9.9 s (±2.5) | 8.8 (±3.0) | p < 0.01 | 77.3% |
| Reach test (stability/static balance) (cm) (n = 66) | 21.3 cm (±5.9) | 26.1 (±6.4) | p < 0.01 | 78.8% |
| Chair-stand test (strength) (s)(n = 65) | 16.4 (±5.1) | 12.4 (±3.8) | p < 0.01 | 89.2% |
| Balance; parallel stance (s) (n = 66) | 10 (±0) | 10 (±0) | -- | -- |
| Balance; semi-parallel stance (s) (n = 66) | 9.7 (±1.6) | 9.98 (±0.18) | p = 0.203 | 3.0% (95.5% same) |
| Balance; tandem stance (s) (n = 66) | 8.7 (±3.0) | 9.7 (±1.4) | p < 0.01 | 18.2% (80.3% same) |
| Balance; one-legged stance (s) (n = 66) | 6.0 (±3.9) | 7.7 (±3.3) | p < 0.01 | 45.5% (43.9% same) |
| Facilitators | Participants | Physiotherapists | Dieticians | Volunteers | Local Coordinator |
|---|---|---|---|---|---|
| Group dynamic/social contact | x | x | x | x | x |
| Clear communication | x | x | X | x | x |
| Visible effect | x | x | n.a. | n.a. | x |
| Set duration | x | n.a. | n.a. | x | n.a. |
| Acquiring knowledge/informative | x | n.a. | n.a. | x | x |
| Physical support | x | n.a. | n.a. | n.a. | n.a. |
| Not feeling under any obligation to take part | x | n.a. | n.a. | n.a. | n.a. |
| Organisational support from volunteer | n.a. | x | x | x | n.a. |
| Contact with clients in own neighbourhood | n.a. | x | n.a. | x | n.a. |
| Barriers | |||||
| Lack of follow-up after programme | x | x | x | n.a. | x |
| Groups at nutrition information session too big/hard to understand | x | n.a. | x | n.a. | n.a. |
| Costs/financing | x | x | x | n.a. | X |
| Difference in physical level | x | x | n.a. | n.a. | n.a. |
| Absence of participants | x | n.a. | n.a. | n.a. | n.a. |
| Lack of collaboration between physiotherapist/dietician | n.a. | x | x | n.a. | n.a. |
| Not enough visible effect | n.a. | n.a. | x | n.a. | n.a. |
| Lack of materials/proper timetable | n.a. | x | x | x | x |
| Big time investment | n.a. | n.a. | n.a. | x | x |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Frazer, S.W.T.; van der Veen, R.; Baan, A.; Hermans, M.E.W.; Olij, B.F. Evaluation of Implementing TOM: A Group-Based Fall Prevention Programme among Community-Dwelling Older Adults in The Netherlands. Int. J. Environ. Res. Public Health 2021, 18, 6360. https://doi.org/10.3390/ijerph18126360
Frazer SWT, van der Veen R, Baan A, Hermans MEW, Olij BF. Evaluation of Implementing TOM: A Group-Based Fall Prevention Programme among Community-Dwelling Older Adults in The Netherlands. International Journal of Environmental Research and Public Health. 2021; 18(12):6360. https://doi.org/10.3390/ijerph18126360
Chicago/Turabian StyleFrazer, Sanne W. T., Rozan van der Veen, Anneloes Baan, Mariëlle E. W. Hermans, and Branko F. Olij. 2021. "Evaluation of Implementing TOM: A Group-Based Fall Prevention Programme among Community-Dwelling Older Adults in The Netherlands" International Journal of Environmental Research and Public Health 18, no. 12: 6360. https://doi.org/10.3390/ijerph18126360
APA StyleFrazer, S. W. T., van der Veen, R., Baan, A., Hermans, M. E. W., & Olij, B. F. (2021). Evaluation of Implementing TOM: A Group-Based Fall Prevention Programme among Community-Dwelling Older Adults in The Netherlands. International Journal of Environmental Research and Public Health, 18(12), 6360. https://doi.org/10.3390/ijerph18126360





