Integrating Digital Technologies and Public Health to Fight Covid-19 Pandemic: Key Technologies, Applications, Challenges and Outlook of Digital Healthcare
Abstract
1. Introduction
2. Background Information
2.1. The Concept of Digital Health
2.2. The Digital Technologies Behind Digital Health
2.2.1. Internet of Things
2.2.2. Artificial Intelligence
2.2.3. Blockchain
2.2.4. Cloud Computing
2.2.5. Big Data
2.2.6. 5G Communication Network
2.3. Digital Tool of Digital Health
2.3.1. Mobile Devices
2.3.2. Wearable Devices
2.3.3. Surveillance Cameras
3. Bibliometric Analysis of Digital Medical Research
3.1. Methods and Data
3.2. Bibliometric Analysis
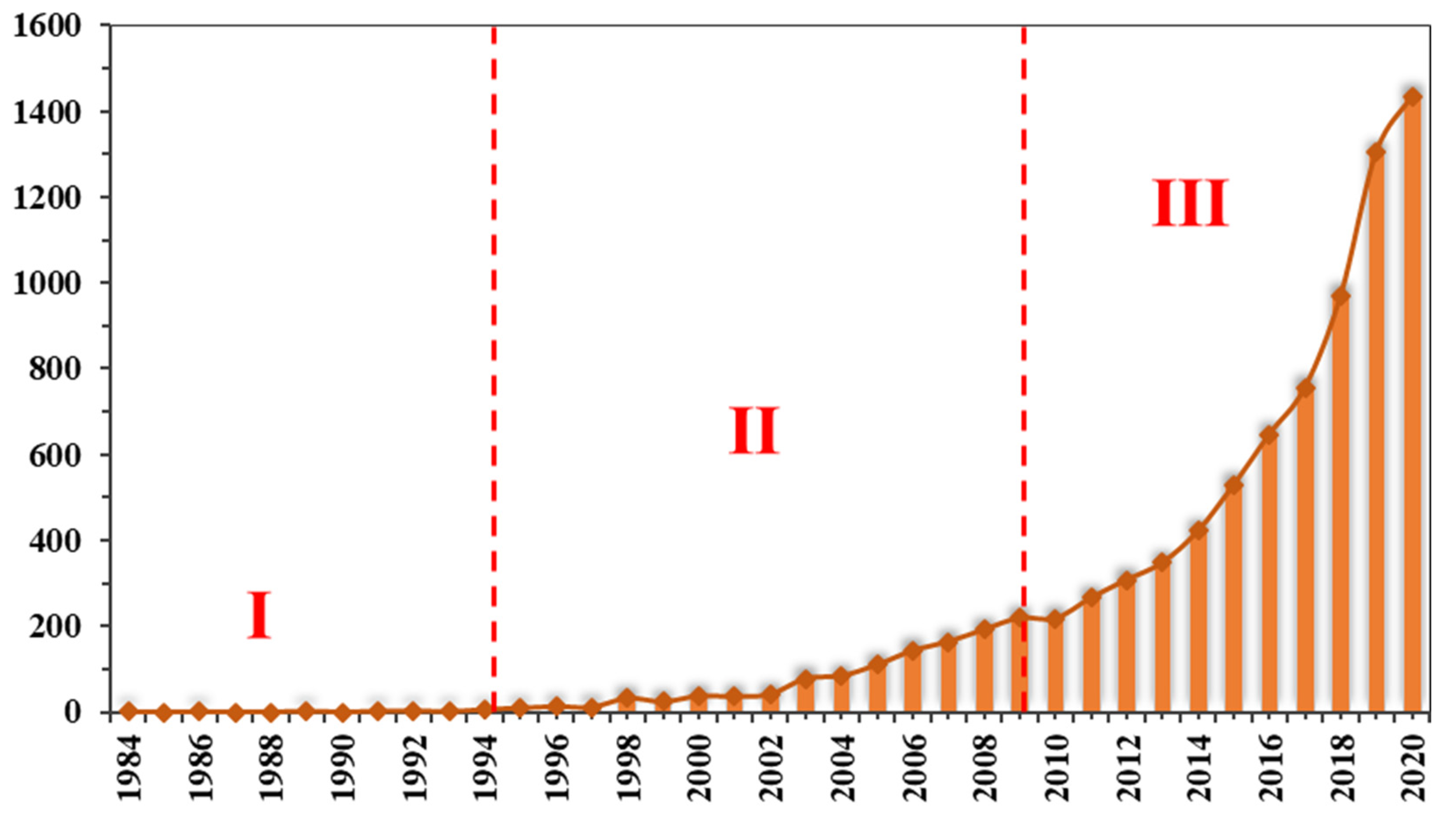
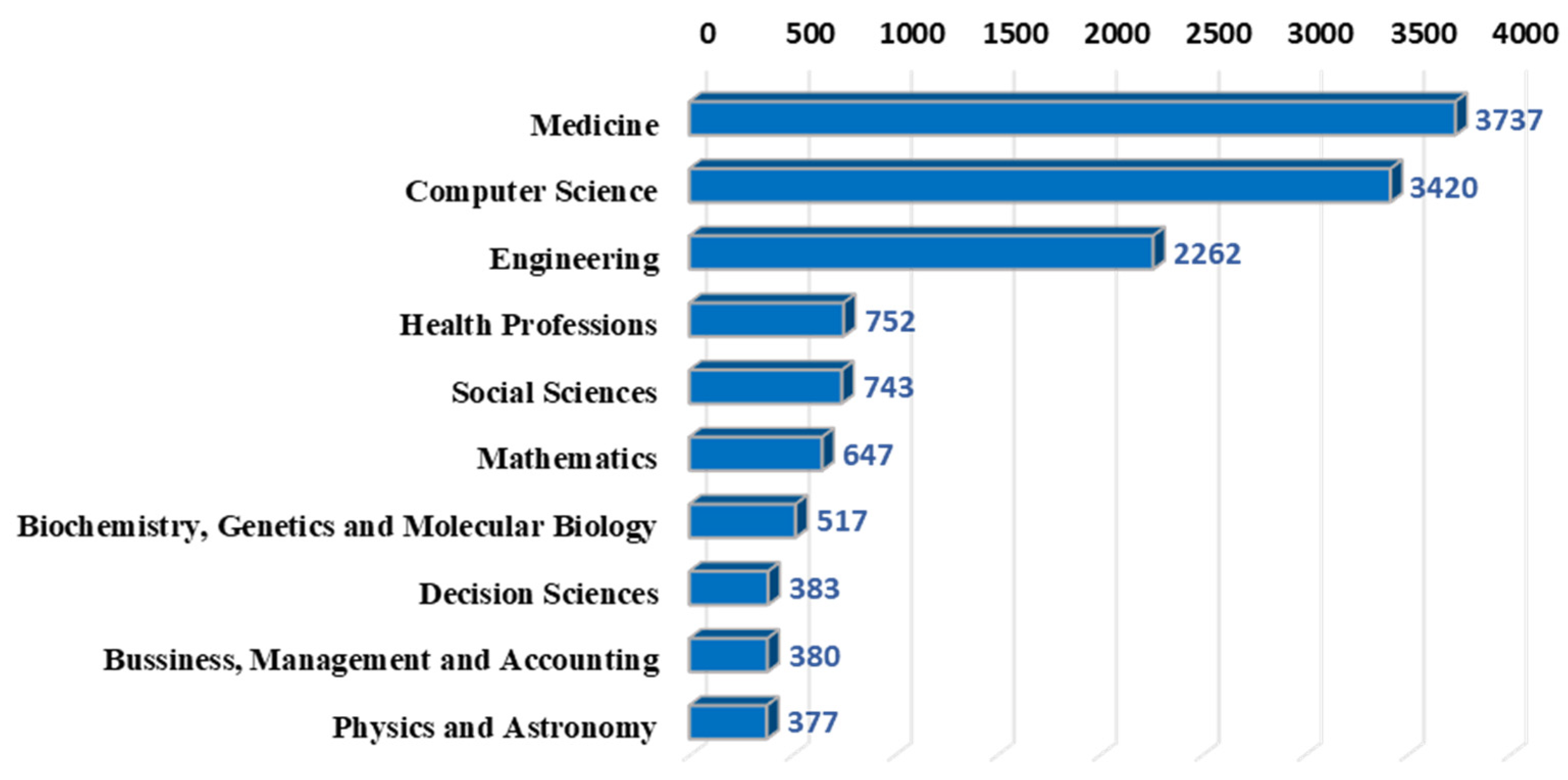
3.2.1. Descriptive Analysis
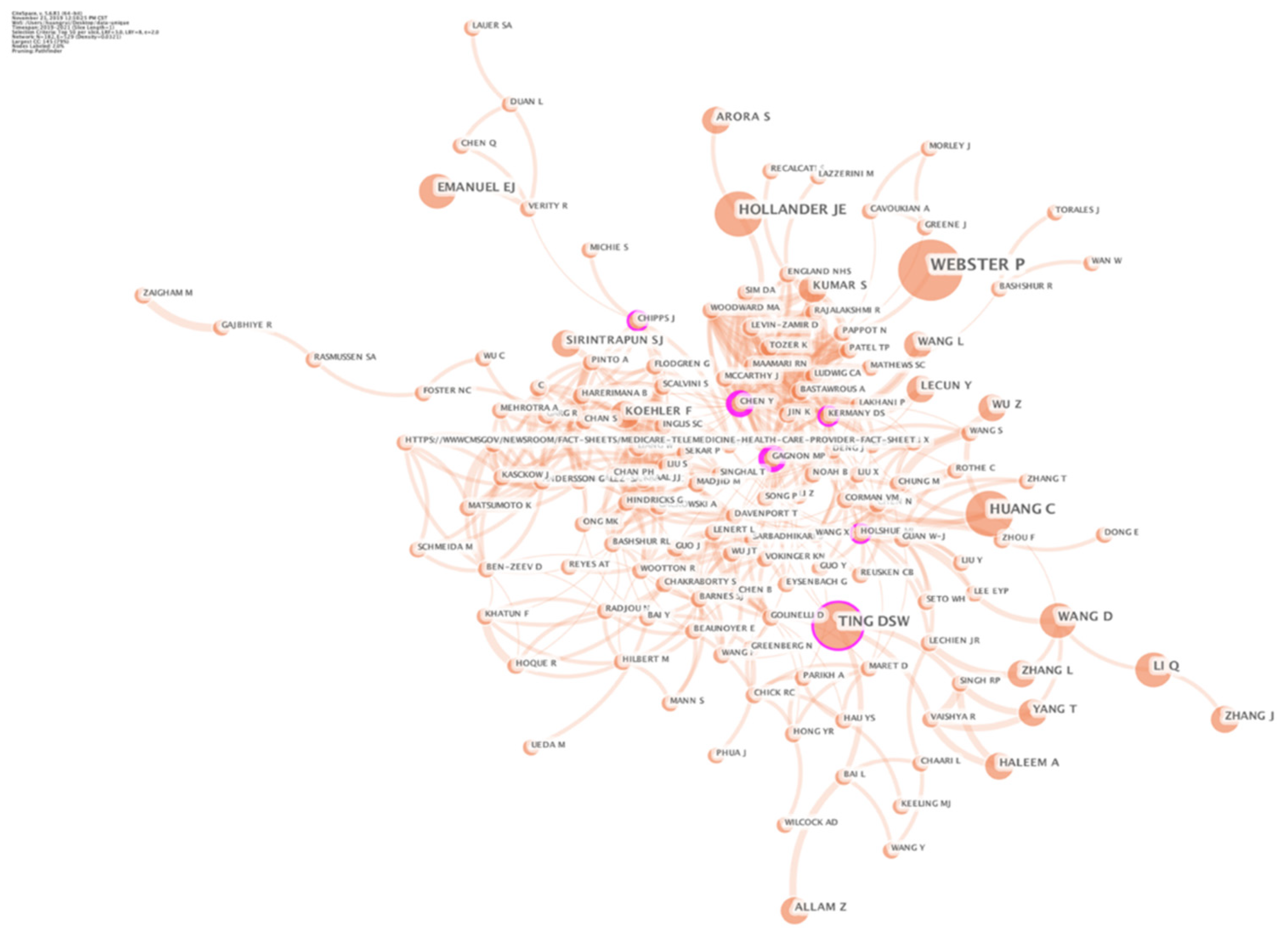
3.2.2. Cited Authors Analysis
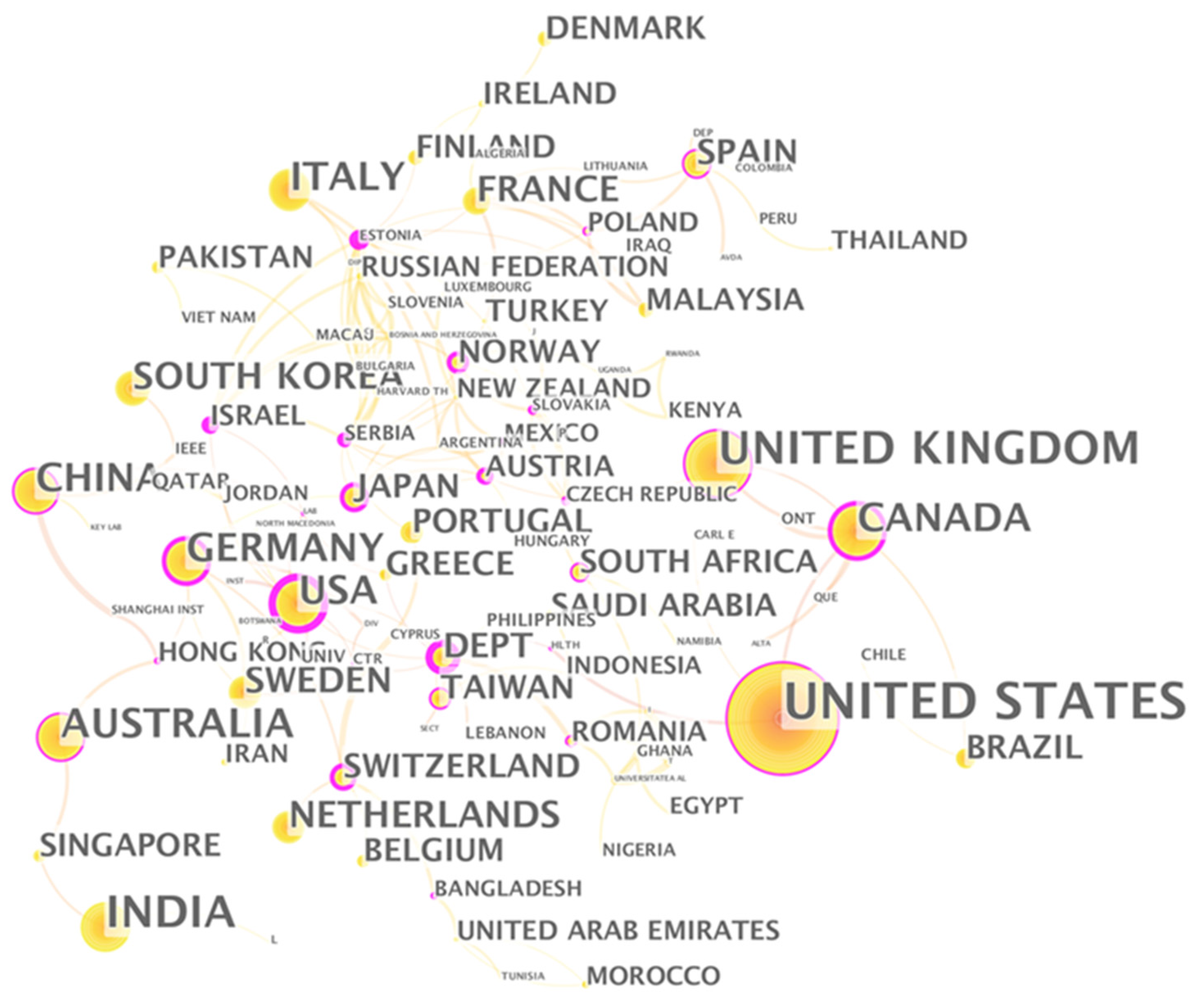
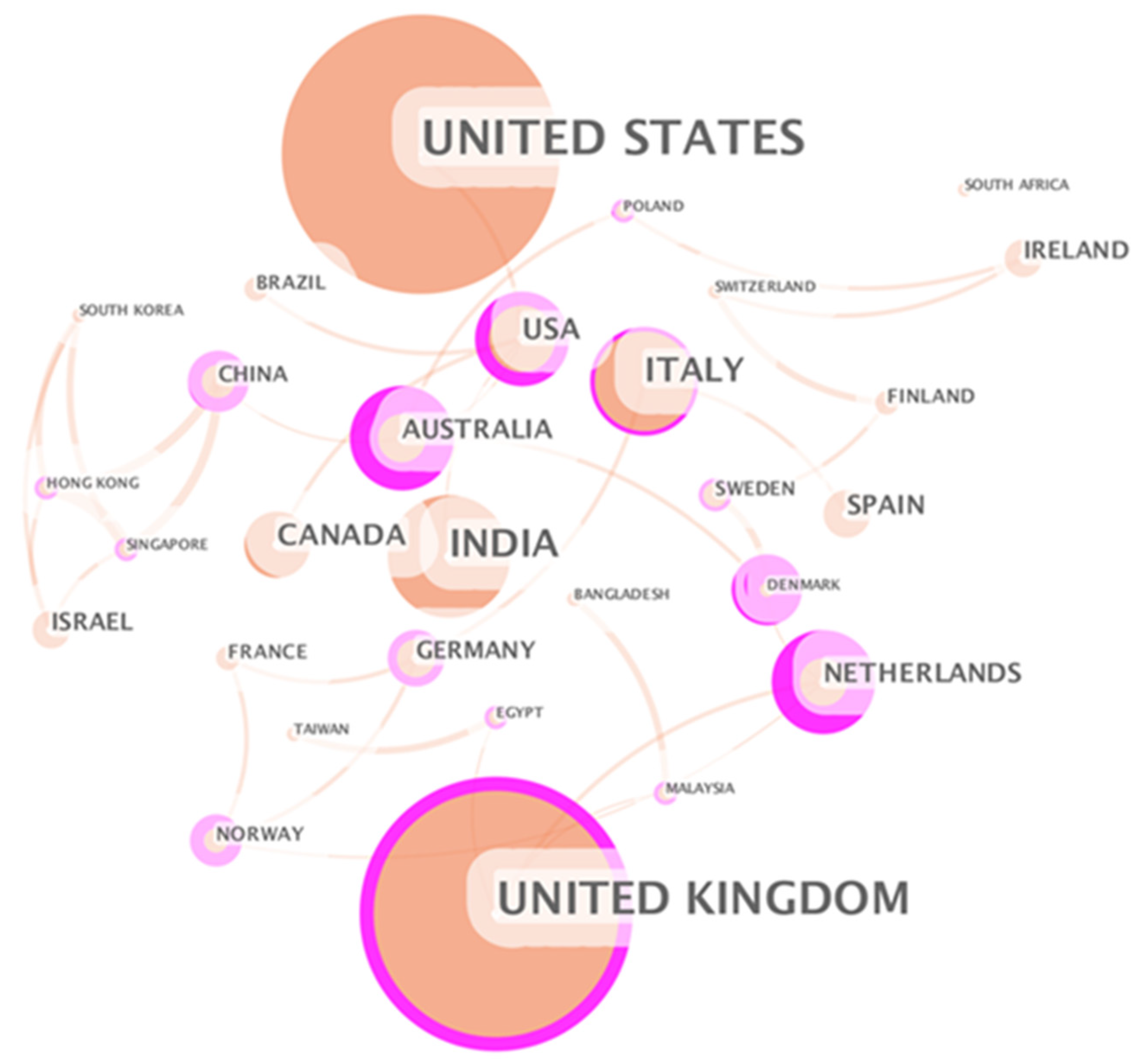
3.2.3. Country Analysis
3.2.4. Funding Agency Analysis
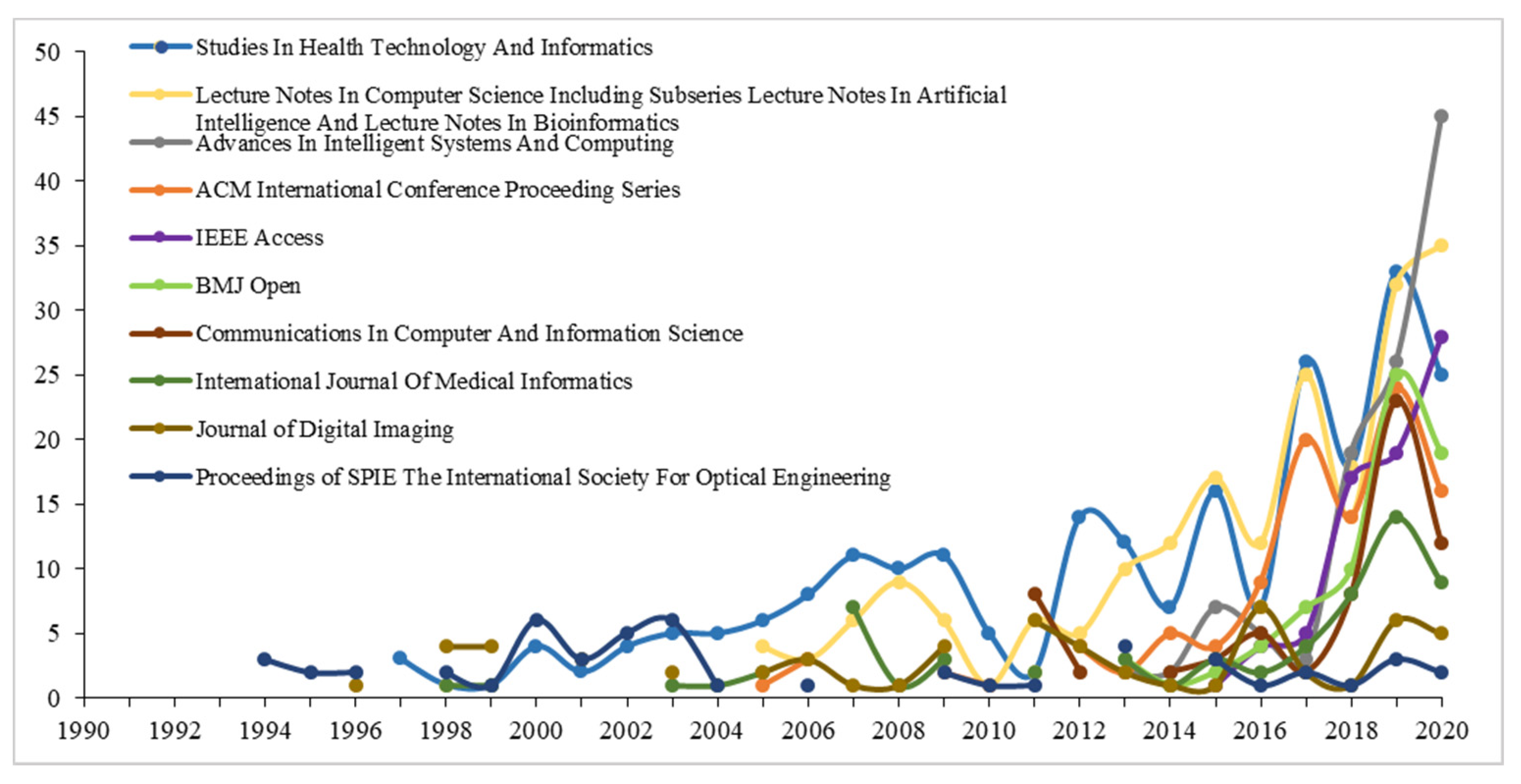
3.2.5. Source Journal Analysis
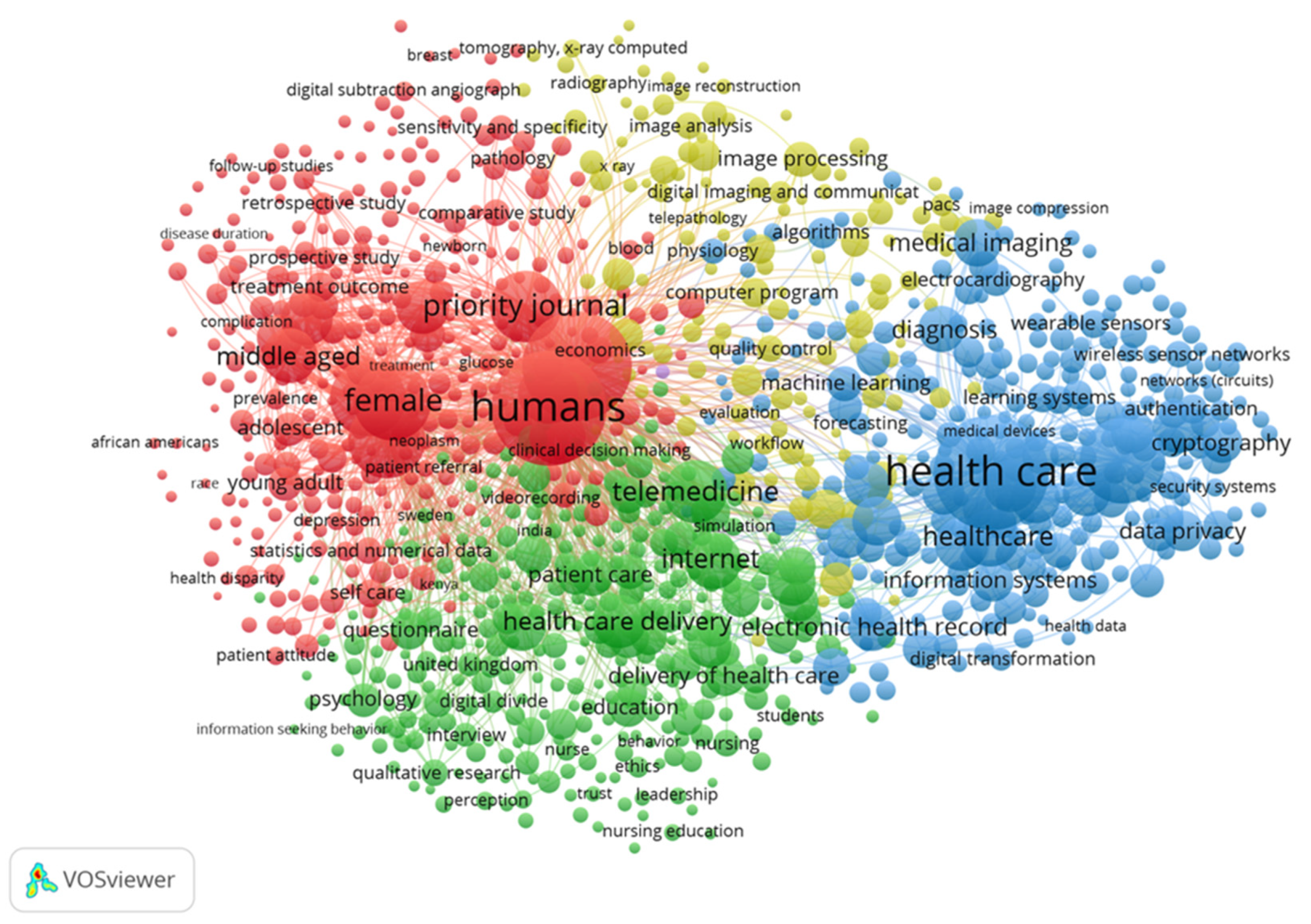
3.2.6. Keyword Co-Occurrence Analysis
- (1)
- For the red clusters with humans, female, adolescent, and middle aged as the main keywords, the keyword nodes all have high total link strength. The publications in this part mainly focus on the target groups and research objects of digital healthcare. The age and gender of digital healthcare research objects are relatively wide, and they are not limited to the research of a particular group. Note that “female” has a higher total link strength. Rock Health pointed out in the investment and financing report released in 2019 that the public market for digital medical enterprise IPOs consists of two hot investment areas-behavioral health and women’s health [100]. Women are considered to be the largest group of buyers and decision makers in healthcare.
- (2)
- A green cluster with telemedicine, internet, questionnaire, and digital divide as the main keywords. This group of the keywords mainly focuses on digital medical treatment methods and analysis tools. Blockchain, AI and genome editing are key technologies used in digital medicine. One of the main advantages of blockchain in the field of digital healthcare is that the technology can provide a higher degree of security, privacy, and confidentiality of healthcare data [101]. AI can automatically solve labor-intensive tasks, read radiological images, and analyze patients’ symptoms and vital signs [102].
- (3)
- The blue clusters with data privacy, cryptography, information systems, health record, and medical imaging as the main keywords mainly describe the data technology of digital medical treatment. The emergence of big data provides a cost-effective prospect for the improvement of health care [103]. Many scholars have proposed new digital technologies, such as convolutional neural network (CNN) [104], lot in healthcare [105], electronic medical records (EMR) [106], etc. At the same time, the application of digital technology in the medical field is also facing challenges. On the one hand, the unbalanced development of infrastructure and human capital between developing and developed countries has created a new dimension of the digital divide. These differences hinder developing countries’ attempts to use digital healthcare to provide medical care [107]. On the other hand, the proliferation of big data also brings security and privacy issues [108].
- (4)
- Yellow clusters with image processing, image analysis, and image reconstruction as the main keywords. These keywords are focused on the analysis of medical images. Digital medicine can change the imaging informatics known in the medical world today, thereby providing more accurate, timely and effective treatment plans [109]. As of 2020, the artificial intelligence medical imaging market is the second largest market segment in artificial intelligence medical applications, second only to drug research and development, accounting for 35%.
3.2.7. Keyword Evolution Analysis
3.3. Digital Healthcare Research during COVID-19
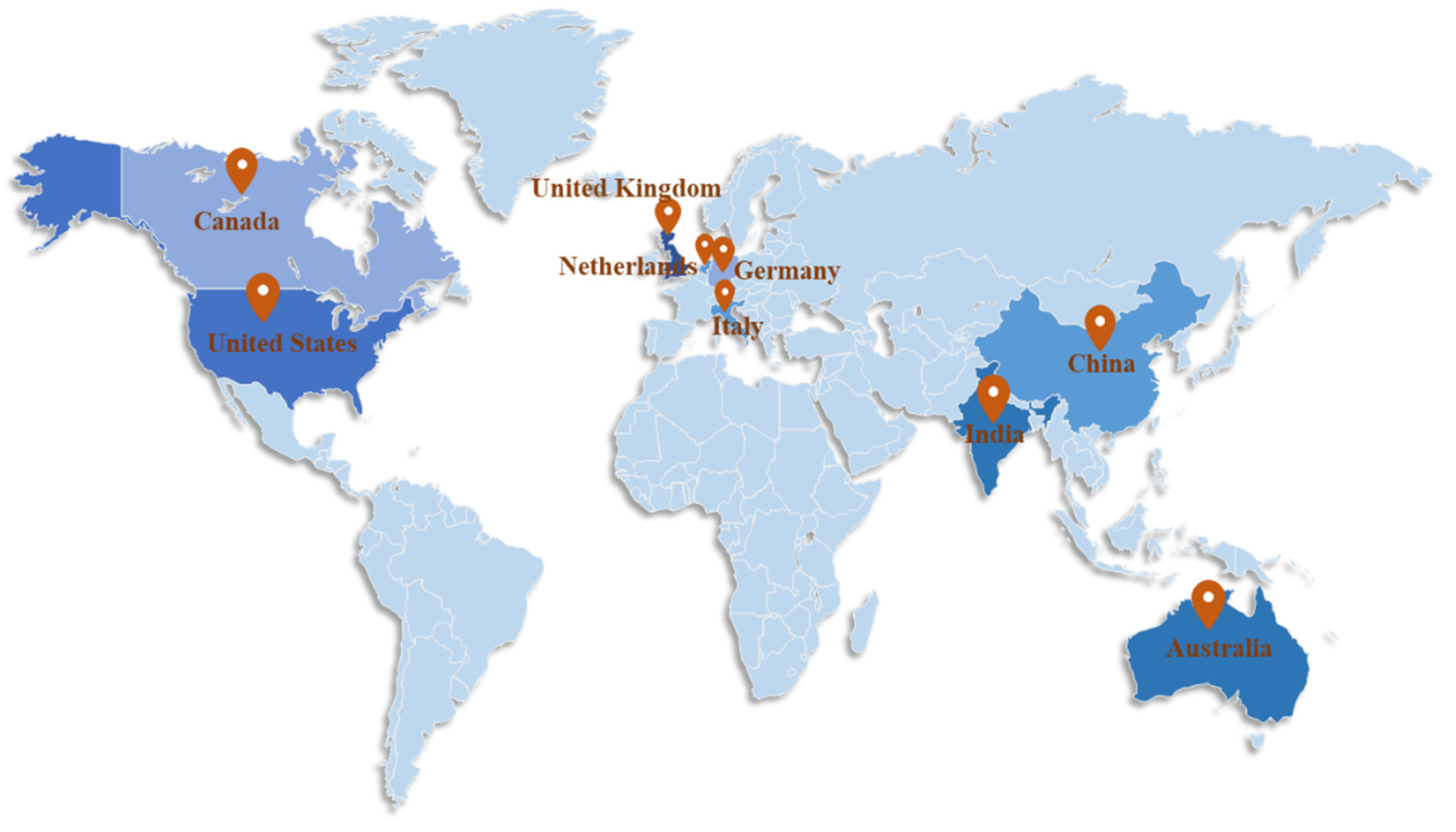
3.3.1. Country Analysis
3.3.2. Keyword Analysis
- (1)
- Disease risk management and prediction
- (2)
- Hospital management
- (3)
- Adjuvant treatment
- (4)
- Health Management
- (5)
- Complementary medical research
- (6)
- Information data management
4. Applications and Impacts of Digital Technology in Fighting COVID-19
4.1. Digital Technology in Epidemic Surveillance
4.1.1. Epidemic Screening and Case Identification
4.1.2. Contact Tracking
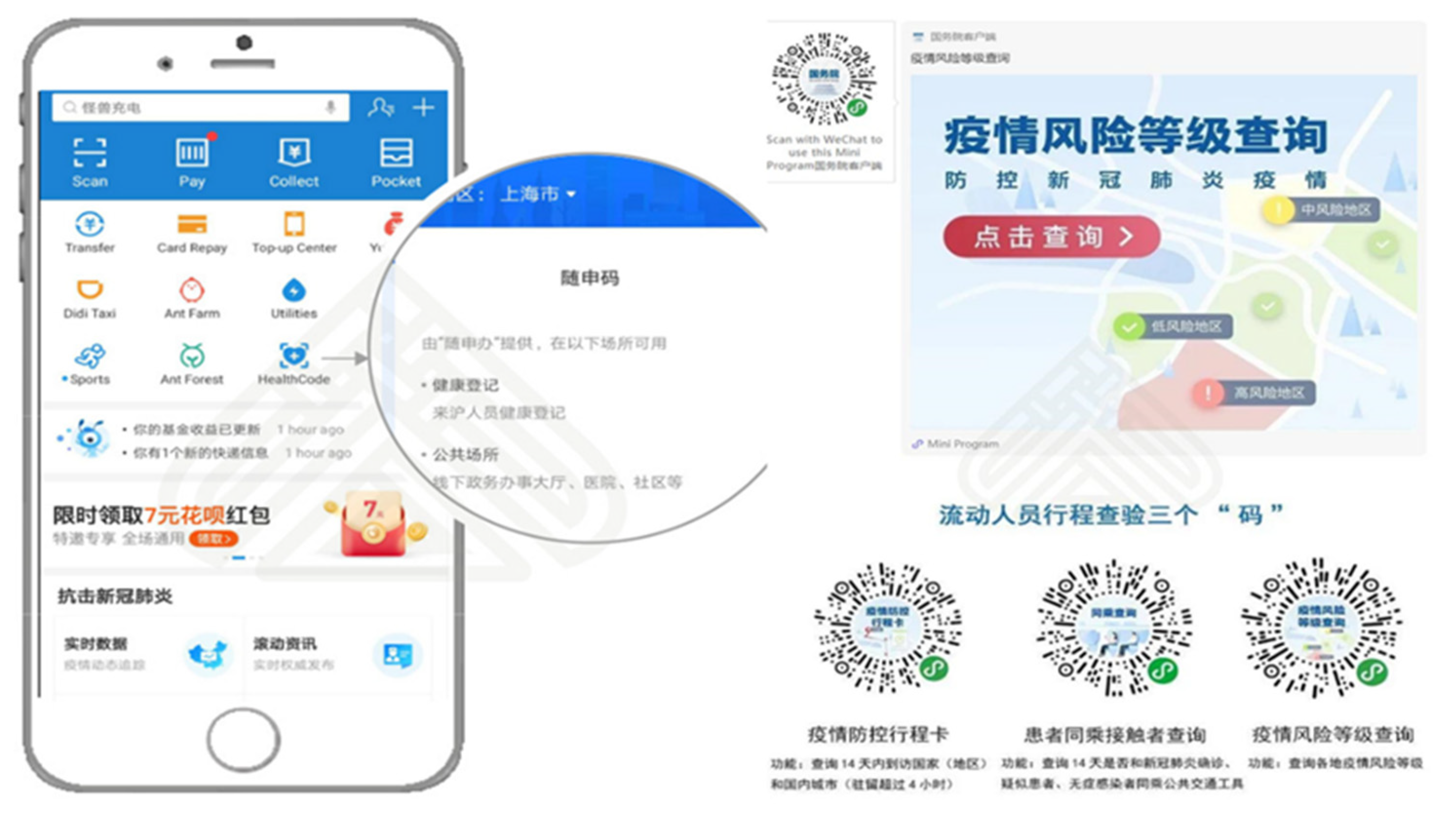
Case Study 1: Health Code
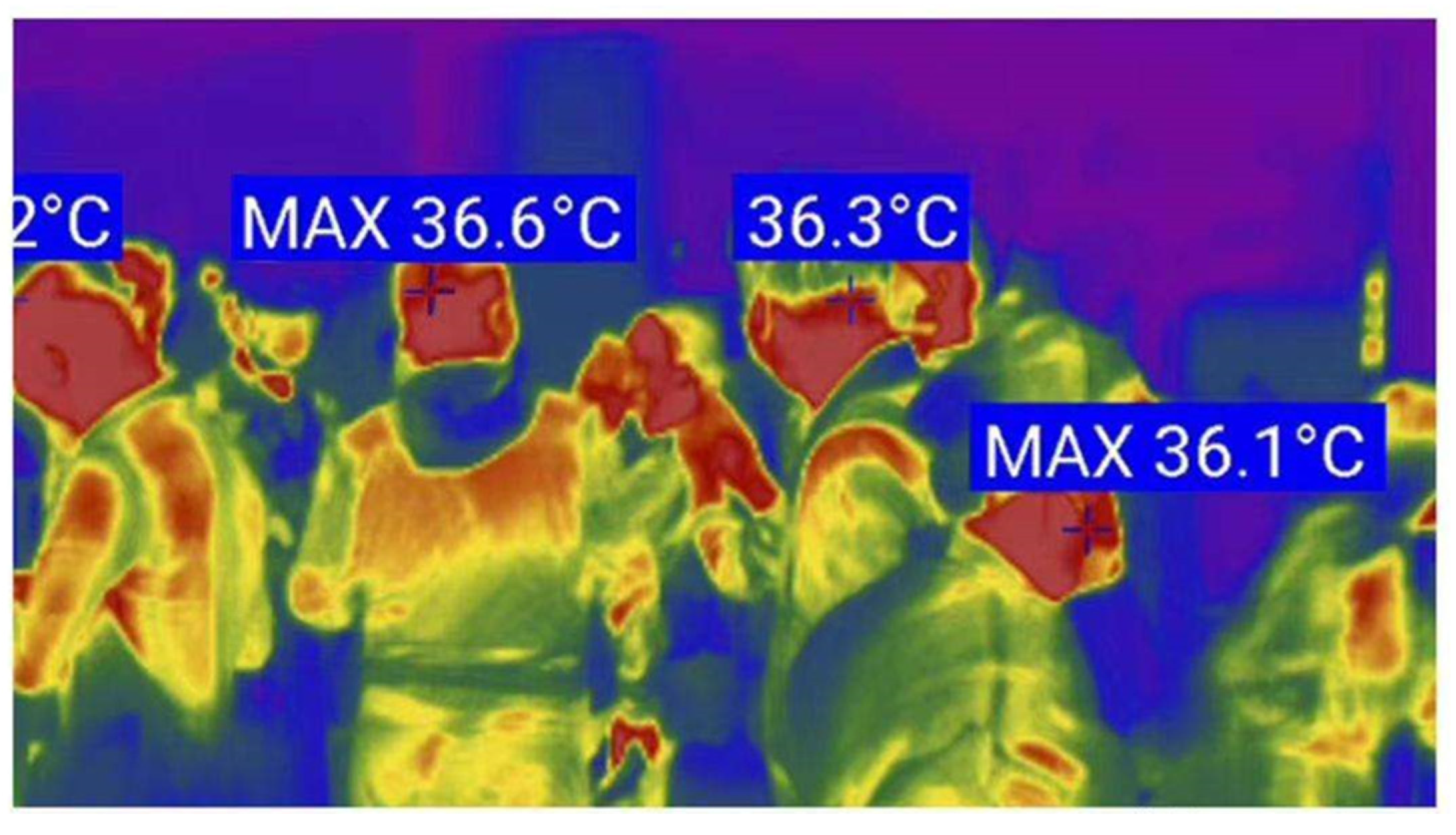
Case Study 2: Infrared Thermal Imaging Thermometer
4.2. Digital Technology in Diagnosis and Treatment
4.2.1. Telemedicine
4.2.2. Remote Health Management
4.2.3. Ai-Assisted Diagnosis
4.2.4. Intelligent Robots
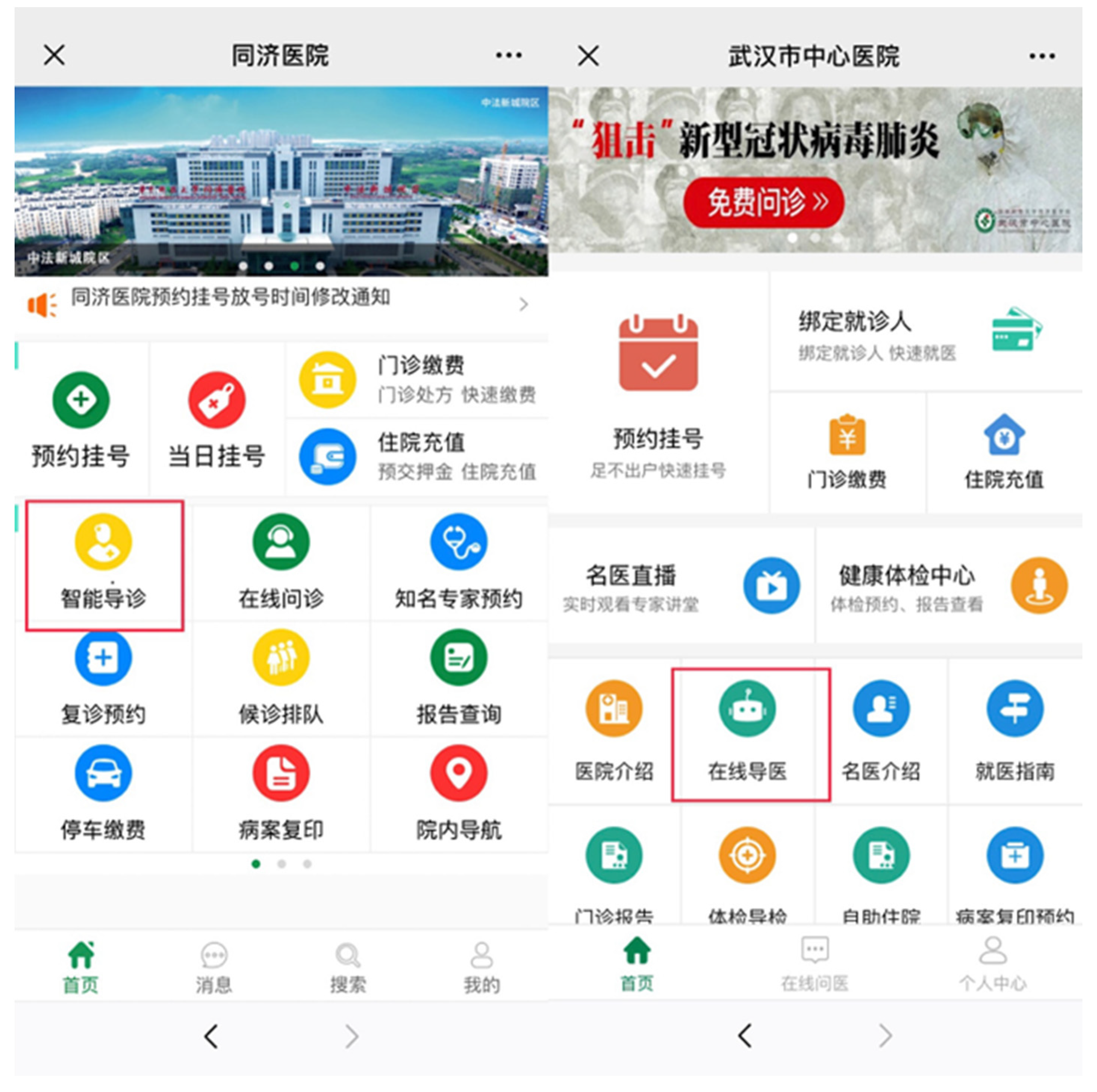
Case Study 1: WeDoctor
Case Study 2: Left-Hand Doctor APP
4.3. Digital Technology in Covid-19 Epidemic Management
4.3.1. Real-Time Epidemic Monitoring System
4.3.2. Medical Materials Online Allocation System
Case Study 1: COVID-19 Map of Johns Hopkins University
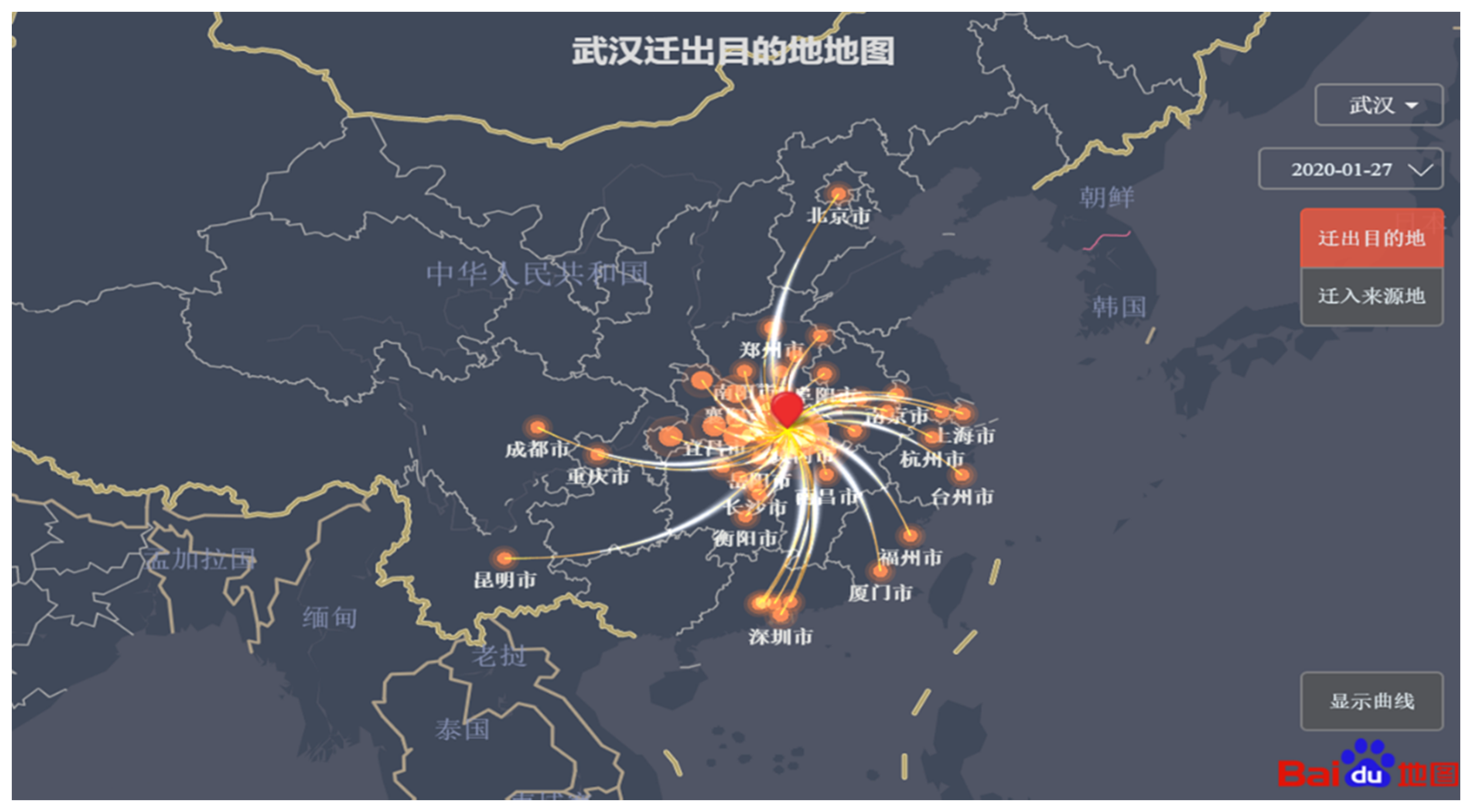
Case Study 2: Baidu Map
4.4. Digital Technology in Drug Development
4.4.1. SARS-CoV-2 Gene Sequencing
4.4.2. Drug and Vaccine Development
5. Challenges
5.1. Data Lag
5.2. Data Fragmentation
5.3. Personal Privacy
5.4. Digital Security Breaches
5.5. Regulatory System
6. Outlook and Implications
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bai, Y.; Yao, L.; Wei, T.; Tian, F.; Jin, D.-Y.; Chen, L.; Wang, M. Presumed Asymptomatic Carrier Transmission of COVID-19. JAMA 2020, 323, 1406–1407. [Google Scholar] [CrossRef]
- Sohrabi, C.; Alsafi, Z.; O’Neill, N.; Khan, M.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, R. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020, 76, 71–76. [Google Scholar] [CrossRef]
- Bi, Q.; Wu, Y.; Mei, S.; Ye, C.; Zou, X.; Zhang, Z.; Liu, X.; Wei, L.; Truelove, S.A.; Zhang, T.; et al. Epidemiology and transmission of COVID-19 in 391 cases and 1286 of their close contacts in Shenzhen, China: A retrospective cohort study. Lancet Infect. Dis. 2020, 20, 911–919. [Google Scholar] [CrossRef]
- Ghanbari, B. On forecasting the spread of the COVID-19 in Iran: The second wave. Chaos Solitons Fractals 2020, 140, 110176. [Google Scholar] [CrossRef]
- U.S. News. America Sees Daily COVID Cases Pass 60,000 Once Again. Available online: https://www.usnews.com/news/health-news/articles/2020-10-16/america-sees-daily-covid-cases-pass-60-000-once-again (accessed on 16 October 2020).
- Wang, Q.; Han, X. Spillover effects of the United States economic slowdown induced by COVID-19 pandemic on energy, economy, and environment in other countries. Environ. Res. 2021, 196, 110936. [Google Scholar] [CrossRef]
- China News. How to Deal with the Second Wave of the Global Epidemic. Available online: https://m.chinanews.com/wap/detail/chs/zw/9319189.shtml (accessed on 22 October 2020). (In Chinese).
- Higgins-Dunn, N.; Rattner, N. U.S. Reports More than 71,600 New Covid Cases as New Infections near Record Highs and Hospitalizations Rise. Available online: https://www.cnbc.com/2020/10/23/covid-us-reports-more-than-71600-new-cases-as-hospitalizations-rise.html (accessed on 23 October 2020).
- World Pop. Effect of Non-Pharmaceutical Interventions for Containing the COVID-19 Outbreak. Available online: https://www.worldpop.org/events/COVID_NPI (accessed on 4 March 2020).
- Wang, Q.; Su, M. A preliminary assessment of the impact of COVID-19 on environment—A case study of China. Sci. Total Environ. 2020, 728, 138915. [Google Scholar] [CrossRef] [PubMed]
- Leung, K.; Wu, J.T.; Liu, D.; Leung, G.M. First-wave COVID-19 transmissibility and severity in China outside Hubei after control measures, and second-wave scenario planning: A modelling impact assessment. Lancet 2020, 395, 1382–1393. [Google Scholar] [CrossRef]
- Aleta, A.; Martín-Corral, D.; Pastore y Piontti, A.; Ajelli, M.; Litvinova, M.; Chinazzi, M.; Dean, N.E.; Halloran, M.E.; Longini Jr, I.M.; Merler, S.; et al. Modelling the impact of testing, contact tracing and household quarantine on second waves of COVID-19. Nat. Hum. Behav. 2020, 4, 964–971. [Google Scholar] [CrossRef] [PubMed]
- Tian, H.; Liu, Y.; Li, Y.; Wu, C.-H.; Chen, B.; Kraemer, M.U.G.; Li, B.; Cai, J.; Xu, B.; Yang, Q.; et al. An investigation of transmission control measures during the first 50 days of the COVID-19 epidemic in China. Science 2020, 368, 638. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Niu, P.; Chen, L.; Wang, L.; Zhao, L.; Huang, B.; Ma, J.; Hu, S.; Wu, L.; Wu, G.; et al. Genetic tracing of HCoV-19 for the re-emerging outbreak of COVID-19 in Beijing, China. Protein Cell 2020. [Google Scholar] [CrossRef]
- Jia, J.; Hu, X.; Yang, F.; Song, X.; Dong, L.; Zhang, J.; Jiang, F.; Gao, R. Epidemiological Characteristics on the Clustering Nature of COVID-19 in Qingdao City, 2020: A Descriptive Analysis. Disaster Med. Public Health Prep. 2020, 14, 643–647. [Google Scholar] [CrossRef] [PubMed]
- CCTV News. Why Did the Second Wave of Epidemics Not Occur in China? Available online: https://www.thepaper.cn/newsDetail_forward_9805469 (accessed on 1 November 2020).
- Gousseff, M.; Penot, P.; Gallay, L.; Batisse, D.; Benech, N.; Bouiller, K.; Collarino, R.; Conrad, A.; Slama, D.; Joseph, C.; et al. Clinical recurrences of COVID-19 symptoms after recovery: Viral relapse, reinfection or inflammatory rebound? J. Infect. 2020, 81, 816–846. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Zhang, F. What does the China’s economic recovery after COVID-19 pandemic mean for the economic growth and energy consumption of other countries? J. Clean. Prod. 2021, 295, 126265. [Google Scholar] [CrossRef] [PubMed]
- Qiu, Y.; Chen, X.; Shi, W. Impacts of social and economic factors on the transmission of coronavirus disease (COVID-19) in China. medRxiv 2020. [Google Scholar] [CrossRef]
- Flaxman, S.; Mishra, S.; Gandy, A.; Unwin, H.J.T.; Mellan, T.A.; Coupland, H.; Whittaker, C.; Zhu, H.; Berah, T.; Eaton, J.W.; et al. Estimating the effects of non-pharmaceutical interventions on COVID-19 in Europe. Nature 2020, 584, 257–261. [Google Scholar] [CrossRef]
- Lau, H.; Khosrawipour, V.; Kocbach, P.; Mikolajczyk, A.; Schubert, J.; Bania, J.; Khosrawipour, T. The positive impact of lockdown in Wuhan on containing the COVID-19 outbreak in China. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef]
- WHO. WHO Guideline: Recommendations on Digital Interventions for Health System Strengthening: Web Supplement 2: Summary of Findings and GRADE Tables; World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- WHO. Draft Global Strategy on Digital Health 2020–2024; World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- Sonnier, P. The Fourth Wave: Digital Health; Independently published: Washington, DC, USA, 2017. [Google Scholar]
- Lupton, D. Critical Perspectives on Digital Health Technologies. Sociol. Compass 2014, 8, 1344–1359. [Google Scholar] [CrossRef]
- Taylor, K. How Digital Technology is Transforming Health and Social Care; Deloitte Centre for Health Solutions: London, UK, 2014. [Google Scholar]
- Ashton, K. That ‘internet of things’ thing. RFID J. 2009, 22, 97–114. [Google Scholar]
- Gharote, M.S.; Sodani, A.; Palshikar, G.K.; Tibrewala, P.A.; Saproo, K.; Bendre, A. Efficient Vaccine Distribution Planning Using IoT; TATA Consultancy Services: Mumbai, India, 2015. [Google Scholar]
- Ahmadi, H.; Arji, G.; Shahmoradi, L.; Safdari, R.; Nilashi, M.; Alizadeh, M. The application of internet of things in healthcare: A systematic literature review and classification. Univers. Access Inf. Soc. 2019, 18, 837–869. [Google Scholar] [CrossRef]
- Esteban-Cartelle, H.; Gutierrez, R.V.; Fernández-Ferreiro, A. Technology and Telemedicine in Hospital Pharmacy, It has Come to Stay; SMG: Chicago, IL, USA, 2017. [Google Scholar]
- Banta, H.D. Future health care technology and the hospital. Health Policy 1990, 14, 61–73. [Google Scholar] [CrossRef]
- Kulkarni, A.; Sathe, S. Healthcare applications of the Internet of Things: A Review. Int. J. Comput. Sci. Inf. Technol. 2014, 5, 6229–6232. [Google Scholar]
- Catarinucci, L.; Donno, D.d.; Mainetti, L.; Palano, L.; Patrono, L.; Stefanizzi, M.L.; Tarricone, L. An IoT-Aware Architecture for Smart Healthcare Systems. IEEE Internet Things J. 2015, 2, 515–526. [Google Scholar] [CrossRef]
- Branger, J.; Pang, Z. From automated home to sustainable, healthy and manufacturing home: A new story enabled by the Internet-of-Things and Industry 4.0. J. Manag. Anal. 2015, 2, 314–332. [Google Scholar] [CrossRef]
- Stefik, M. Introduction to Knowledge Systems; Elsevier: Amsterdam, The Netherlands, 2014. [Google Scholar]
- Haenlein, M.; Kaplan, A. A Brief History of Artificial Intelligence: On the Past, Present, and Future of Artificial Intelligence. Calif. Manag. Rev. 2019, 61, 5–14. [Google Scholar] [CrossRef]
- Nadarzynski, T.; Miles, O.; Cowie, A.; Ridge, D. Acceptability of artificial intelligence (AI)-led chatbot services in healthcare: A mixed-methods study. Digit. Health 2019, 5, 2055207619871808. [Google Scholar] [CrossRef]
- Liu, R.; Rong, Y.; Peng, Z. A review of medical artificial intelligence. Global Health J. 2020, 4, 42–45. [Google Scholar] [CrossRef]
- Wang, Q.; Zhang, C. Can COVID-19 and environmental research in developing countries support these countries to meet the environmental challenges induced by the pandemic? Environ. Sci. Pollut. Res. 2021. [Google Scholar] [CrossRef]
- Yang, Y.; Zheng, X.; Liu, X.; Zhong, S.; Chang, V. Cross-domain dynamic anonymous authenticated group key management with symptom-matching for e-health social system. Future Gener. Comput. Syst. 2018, 84, 160–176. [Google Scholar] [CrossRef]
- Zhu, R.; Niu, H.; Yin, N.; Wu, T.; Zhao, Y. Analysis of Varicose Veins of Lower Extremities Based on Vascular Endothelial Cell Inflammation Images and Multi-Scale Deep Learning. IEEE Access 2019, 7, 174345–174358. [Google Scholar] [CrossRef]
- Liu, Y.; Zhang, W.; Pan, S.; Li, Y.; Chen, Y. Analyzing the robotic behavior in a smart city with deep enforcement and imitation learning using IoRT. Comput. Commun. 2020, 150, 346–356. [Google Scholar] [CrossRef]
- Randall, D.; Goel, P.; Abujamra, R. Blockchain Applications and Use Cases in Health Information Technology. J. Health Med. Inform. 2017, 8, 8–11. [Google Scholar] [CrossRef]
- Agbo, C.C.; Mahmoud, Q.H.; Eklund, J.M. Blockchain Technology in Healthcare: A Systematic Review. Healthcare 2019, 7, 56. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; White, J.; Schmidt, D.; Lenz, G. Applying Software Patterns to Address Interoperability in Blockchain-based Healthcare Apps. arXiv 2017, arXiv:1706.03700. Available online: https://arxiv.org/abs/1706.03700 (accessed on 5 June 2017).
- Li, H.; Zhu, L.; Shen, M.; Gao, F.; Liu, S. Blockchain-Based Data Preservation System for Medical Data. J. Med Syst. 2018, 42, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Cheng, X.; Chen, F.; Xie, D.; Sun, H.; Huang, C.; Qi, Z. Blockchain-Based Secure Authentication Scheme for Medical Data Sharing. In Proceedings of the International Conference of Pioneering Computer Scientists, Engineers and Educators, Guilin, China, 20–23 September 2019; Springer: Berlin/Heidelberg, Germany, 2019; pp. 409–411. [Google Scholar]
- Lee, T.-F.; Li, H.-Z.; Hsieh, Y.-P. A blockchain-based medical data preservation scheme for telecare medical information systems. Int. J. Inf. Secur. 2020. [Google Scholar] [CrossRef]
- Yue, X.; Wang, H.; Jin, D.; Li, M.; Jiang, W. Healthcare Data Gateways: Found Healthcare Intelligence on Blockchain with Novel Privacy Risk Control. J. Med Syst. 2016, 40, 218. [Google Scholar] [CrossRef]
- Liang, X.; Shetty, S.; Tosh, D.; Kamhoua, C.; Kwiat, K.; Njilla, L. ProvChain: A Blockchain-Based Data Provenance Architecture in Cloud Environment with Enhanced Privacy and Availability. In Proceedings of the 2017 17th IEEE/ACM International Symposium on Cluster, Cloud and Grid Computing (CCGRID), Madrid, Spain, 14–17 May 2017; pp. 468–477. [Google Scholar]
- Dorri, A.; Kanhere, S.S.; Jurdak, R.; Gauravaram, P. Blockchain for IoT Security and Privacy: The Case Study of a Smart Home. In Proceedings of the 2017 IEEE International Conference on Pervasive Computing and Communications Workshops (PerCom Workshops), Kona, HI, USA, 13–17 March 2017; pp. 618–623. [Google Scholar]
- Attili, S.; Ladwa, S.; Sharma, U.; Trenkle, A. Blockchain: The Chain of Trust and Its Potential to Transform Healthcare–Our Point of View. In Proceedings of the ONC/NIST Use of Blockchain for Healthcare and Research Workshop, Gaithersburg, MD, USA, 8 August 2016. [Google Scholar]
- Botta, A.; de Donato, W.; Persico, V.; Pescapé, A. Integration of Cloud computing and Internet of Things: A survey. Future Gener. Comput. Syst. 2016, 56, 684–700. [Google Scholar] [CrossRef]
- Laplante, P.A.; Laplante, N. The internet of things in healthcare: Potential applications and challenges. It Prof. 2016, 18, 2–4. [Google Scholar] [CrossRef]
- Kuo, M.-H. Opportunities and challenges of cloud computing to improve health care services. J. Med Internet Res. 2011, 13, e67. [Google Scholar] [CrossRef] [PubMed]
- Narayan, S.; Gagné, M.; Safavi-Naini, R. Privacy Preserving EHR System Using Attribute-Based Infrastructure. In Proceedings of the 2010 ACM Workshop on Cloud Computing Security Workshop, Chicago, IL, USA, 8 October 2010; pp. 47–52. [Google Scholar]
- Sultan, N. Making use of cloud computing for healthcare provision: Opportunities and challenges. Int. J. Inf. Manag. 2014, 34, 177–184. [Google Scholar] [CrossRef]
- Santos, J.; Rodrigues, J.J.P.C.; Silva, B.M.C.; Casal, J.; Saleem, K.; Denisov, V. An IoT-based mobile gateway for intelligent personal assistants on mobile health environments. J. Netw. Comput. Appl. 2016, 71, 194–204. [Google Scholar] [CrossRef]
- Hiremath, S.; Yang, G.; Mankodiya, K. Wearable Internet of Things: Concept, Architectural Components and Promises for Person-Centered Healthcare. In Proceedings of the 2014 4th International Conference on Wireless Mobile Communication and Healthcare—Transforming Healthcare Through Innovations in Mobile and Wireless Technologies (MOBIHEALTH), Athens, Greece, 3–5 November 2014; pp. 304–307. [Google Scholar]
- Rolim, C.O.; Koch, F.L.; Westphall, C.B.; Werner, J.; Fracalossi, A.; Salvador, G.S. A Cloud Computing Solution for Patient’s Data Collection in Health Care Institutions. In Proceedings of the 2010 Second International Conference on eHealth, Telemedicine, and Social Medicine, Saint Maarten, Netherlands Antilles, 10–16 February 2010; pp. 95–99. [Google Scholar]
- Joyia, G.J.; Liaqat, R.M.; Farooq, A.; Rehman, S. Internet of Medical Things (IOMT): Applications, benefits and future challenges in healthcare domain. J. Commun. 2017, 12, 240–247. [Google Scholar] [CrossRef]
- Istepanian, R.S.H.; Hu, S.; Philip, N.Y.; Sungoor, A. The Potential of Internet of m-Health Things “m-IoT” for Non-Invasive Glucose Level Sensing. In Proceedings of the 2011 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Boston, MA, USA, 30 August–3 September 2011; pp. 5264–5266. [Google Scholar]
- Vidhyalakshmi, A.; Priya, C. Chapter 1—Medical big data mining and processing in e-health care. In An Industrial IoT Approach for Pharmaceutical Industry Growth; Balas, V.E., Solanki, V.K., Kumar, R., Eds.; Academic Press: Cambridge, MA, USA, 2020; pp. 1–30. [Google Scholar]
- Moharana, M.; Pandey, M.; Routaray, S.S. Chapter 8—Why big data, and what it is: Basics to advanced big data journey for the medical industry. In Handbook of Data Science Approaches for Biomedical Engineering; Balas, V.E., Solanki, V.K., Kumar, R., Khari, M., Eds.; Academic Press: Cambridge, MA, USA, 2020; pp. 221–249. [Google Scholar]
- Shakhovska, N.; Fedushko, S.; Greguš ml, M.; Melnykova, N.; Shvorob, I.; Syerov, Y. Big Data analysis in development of personalized medical system. Procedia Comput. Sci. 2019, 160, 229–234. [Google Scholar] [CrossRef]
- Arata, J.; Takahashi, H.; Pitakwatchara, P.; Warisawa, S.; Tanoue, K.; Konishi, K.; Ieiri, S.; Shimizu, S.; Nakashima, N.; Okamura, K.; et al. A Remote Surgery Experiment between Japan and Thailand over Internet Using a Low Latency CODEC System. In Proceedings of the 2007 IEEE International Conference on Robotics and Automation, Rome, Italy, 10–14 April 2007; pp. 953–959. [Google Scholar]
- Meshram, D.A.; Patil, D.D. 5G Enabled Tactile Internet for Tele-Robotic Surgery. Procedia Comput. Sci. 2020, 171, 2618–2625. [Google Scholar] [CrossRef]
- Jones, C. Apple and Google Continue to Gain US Smartphone Market Share. 2013. Available online: https://www.forbes.com/sites/chuckjones/2013/01/04/apple-and-google-continue-to-gain-us-smartphone-market-share/?sh=6ff6f0154717 (accessed on 4 January 2013).
- Balapour, A.; Reychav, I.; Sabherwal, R.; Azuri, J. Mobile technology identity and self-efficacy: Implications for the adoption of clinically supported mobile health apps. Int. J. Inf. Manag. 2019, 49, 58–68. [Google Scholar] [CrossRef]
- Marques, G.; Pitarma, R.M.; Garcia, N.; Pombo, N. Internet of Things architectures, technologies, applications, challenges, and future directions for enhanced living environments and healthcare systems: A review. Electronics 2019, 8, 1081. [Google Scholar] [CrossRef]
- Hong, Y.-J.; Kim, I.-J.; Ahn, S.C.; Kim, H.-G. Mobile health monitoring system based on activity recognition using accelerometer. Simul. Model. Pract. Theory 2010, 18, 446–455. [Google Scholar] [CrossRef]
- Wang, Q.; Wang, S. Preventing carbon emission retaliatory rebound post-COVID-19 requires expanding free trade and improving energy efficiency. Sci. Total Environ. 2020, 746, 141158. [Google Scholar] [CrossRef]
- Pires, I.M.; Marques, G.; Garcia, N.M.; Flórez-Revuelta, F.; Ponciano, V.; Oniani, S. A Research on the Classification and Applicability of the Mobile Health Applications. J. Pers. Med. 2020, 10, 11. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.; Ma, Y.; Song, J.; Lai, C.-F.; Hu, B. Smart Clothing: Connecting Human with Clouds and Big Data for Sustainable Health Monitoring. Mob. Netw. Appl. 2016, 21, 825–845. [Google Scholar] [CrossRef]
- Balandina, E.; Balandin, S.; Koucheryavy, Y.; Mouromtsev, D. IoT Use Cases in Healthcare and Tourism. In Proceedings of the 2015 IEEE 17th Conference on Business Informatics, Lisbon, Portugal, 13–16 July 2015; pp. 37–44. [Google Scholar]
- Abro, Z.A.; Hong, C.; Chen, N.; Zhang, Y.; Lakho, R.A.; Yasin, S. A fiber Bragg grating-based smart wearable belt for monitoring knee joint postures. Text. Res. J. 2019, 90, 386–394. [Google Scholar] [CrossRef]
- Rachim, V.P.; Chung, W.-Y. Wearable-band type visible-near infrared optical biosensor for non-invasive blood glucose monitoring. Sens. Actuators B Chem. 2019, 286, 173–180. [Google Scholar] [CrossRef]
- Ching, K.W.; Singh, M.M. Wearable technology devices security and privacy vulnerability analysis. Int. J. Netw. Secur. Appl. 2016, 8, 19–30. [Google Scholar] [CrossRef]
- Bing-jin, L.; Jian, Y.; Yan-jun, L. Design and Implementation of Medical Ultrasound Remote Video Aided Diagnosis System. In Proceedings of the 2020 IEEE 6th International Conference on Control Science and Systems Engineering (ICCSSE), Beijing, China, 17–19 July 2020; pp. 1–4. [Google Scholar]
- Costanzo, I.M.; Sen, D.; Rhein, L.; Guler, U. Respiratory Monitoring: Current State of the Art and Future Roads. IEEE Rev. Biomed. Eng. 2020. [Google Scholar] [CrossRef]
- Kiani, M.J.E.; Al-Ali, A.; Muhsin, B.; Sampath, A.; Olsen, G.A. Medical Monitoring System. U.S. Patent US 9,218,454 B2, 22 December 2015. [Google Scholar]
- Wu, J.T.; Leung, K.; Bushman, M.; Kishore, N.; Niehus, R.; de Salazar, P.M.; Cowling, B.J.; Lipsitch, M.; Leung, G.M. Estimating clinical severity of COVID-19 from the transmission dynamics in Wuhan, China. Nat. Med. 2020, 26, 506–510. [Google Scholar] [CrossRef]
- Wang, Q.; Li, R.; Zhan, L. Blockchain technology in the energy sector: From basic research to real world applications. Comput. Sci. Rev. 2021, 39, 100362. [Google Scholar] [CrossRef]
- Rupasinghe, T.; Burstein, F.; Rudolph, C. Blockchain Based Dynamic Patient Consent: A Privacy-Preserving Data Acquisition Architecture for Clinical Data Analytics. In Proceedings of the 40th International Conference on Information Systems, ICIS 2019, Munich, Germany, 15–18 December 2019. [Google Scholar]
- WHO. Coronavirus Disease (COVID-19) Situation Report—120. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200519-covid-19-sitrep-120.pdf?sfvrsn=515cabfb_4 (accessed on 19 May 2020).
- Xue, J.-Y.; Zhu, Y..-M.; Yu, J.; Yin, W. Application of various communication means in isolation wards for coronavirus disease 2019. Acad. J. Second Mil. Med. Univ. 2020, 41. [Google Scholar] [CrossRef]
- Nelson, H.D.; Tyne, K.; Naik, A.; Bougatsos, C.; Chan, B.K.; Humphrey, L. Screening for breast cancer: An update for the U.S. Preventive Services Task Force. Ann. Intern. Med. 2009, 151, 727–737. [Google Scholar] [CrossRef]
- Abella, B.S.; Sandbo, N.; Vassilatos, P.; Alvarado, J.P.; O’Hearn, N.; Wigder, H.N.; Hoffman, P.; Tynus, K.; Vanden Hoek, T.L.; Becker, L.B. Chest compression rates during cardiopulmonary resuscitation are suboptimal: A prospective study during in-hospital cardiac arrest. Circulation 2005, 111, 428–434. [Google Scholar] [CrossRef]
- Martinez, A.W.; Phillips, S.T.; Carrilho, E.; Thomas Iii, S.W.; Sindi, H.; Whitesides, G.M. Simple telemedicine for developing regions: Camera phones and paper-based microfluidic devices for real-time, off-site diagnosis. Anal. Chem. 2008, 80, 3699–3707. [Google Scholar] [CrossRef]
- Azaria, A.; Ekblaw, A.; Vieira, T.; Lippman, A. MedRec: Using Blockchain for Medical Data Access and Permission Management. In Proceedings of the 2016 2nd International Conference on Open and Big Data, OBD 2016, Vienna, Austria, 22–24 August 2016; pp. 25–30. [Google Scholar]
- Zhang, Y.; Qiu, M.; Tsai, C.W.; Hassan, M.M.; Alamri, A. Health-CPS: Healthcare cyber-physical system assisted by cloud and big data. IEEE Syst. J. 2017, 11, 88–95. [Google Scholar] [CrossRef]
- Agarwal, R.; Gao, G.G.; DesRoches, C.; Jha, A.K. The digital transformation of healthcare: Current status and the road ahead. Inf. Syst. Res. 2010, 21, 796–809. [Google Scholar] [CrossRef]
- Wang, Q.; Su, M.; Li, R. Is China the world’s blockchain leader? Evidence, evolution and outlook of China’s blockchain research. J. Clean. Prod. 2020, 264, 121742. [Google Scholar] [CrossRef]
- Foster, R.N. Available online: https://www.cn-healthcare.com/article/20190906/content-523327.html (accessed on 6 September 2019).
- Ministry of Health and Family Welfare Government of India. Available online: https://www.mohfw.gov.in/ (accessed on 3 June 2021).
- The State Council of China. “13th Five-Year” National Science and Technology Innovation Plan. Available online: http://www.gov.cn/xinwen/2016-08/08/content_5098259.htm (accessed on 8 August 2016).
- Saluse, J.; Aaviksoo, A.; Ross, P.; Tiik, M.; Parv, L.; Sepper, R.; Pohjonen, H.; Jakovlev, Ü.; Enni, K. Assessing the Economic Impact/Net Benefi ts of the Estonian Electronic Health Record System. Available online: http://www.praxis.ee/fileadmin/tarmo/Projektid/Tervishoid/Digimoju/Digimpact.pdf (accessed on 3 June 2021).
- Leitsalu, L.; Metspalu, A. From Biobanking to Precision Medicine. In Genomic and Precision Medicine, 3rd ed.; Academic Press: Cambridge, MA, USA, 2017; pp. 119–129. [Google Scholar]
- Sogomonjan, M. Challenges and opportunities for e-mental health policy: An Estonian case study. Contemp. Soc. Sci. 2020. [Google Scholar] [CrossRef]
- Health Rock. Rock Health’s 2019 Digital Health Market Insights. Available online: https://rockhealth.com/reports/in-2019-digital-health-celebrated-six-ipos-as-venture-investment-edged-off-record-highs/ (accessed on 3 June 2021).
- Kshetri, N. Blockchain’s roles in strengthening cybersecurity and protecting privacy. Telecommun. Policy 2017, 41, 1027–1038. [Google Scholar] [CrossRef]
- Bayram, M.; Springer, S.; Garvey, C.K.; Özdemir, V. COVID-19 Digital Health Innovation Policy: A Portal to Alternative Futures in the Making. OMICS J. Integr. Biol. 2020, 24, 460–469. [Google Scholar] [CrossRef] [PubMed]
- Hilbert, M. Big Data for Development: A Review of Promises and Challenges. Dev. Policy Rev. 2016, 34, 135–174. [Google Scholar] [CrossRef]
- Faust, O.; Hagiwara, Y.; Hong, T.J.; Lih, O.S.; Acharya, U.R. Deep learning for healthcare applications based on physiological signals: A review. Comput. Methods Programs Biomed. 2018, 161, 1–13. [Google Scholar] [CrossRef]
- Farahani, B.; Firouzi, F.; Chang, V.; Badaroglu, M.; Constant, N.; Mankodiya, K. Towards fog-driven IoT eHealth: Promises and challenges of IoT in medicine and healthcare. Future Gener. Comput. Syst. 2017, 78, 659–676. [Google Scholar] [CrossRef]
- Yang, J.-J.; Li, J.; Mulder, J.; Wang, Y.; Chen, S.; Wu, H.; Wang, Q.; Pan, H. Emerging information technologies for enhanced healthcare. Comput. Ind. 2015, 69, 3–11. [Google Scholar] [CrossRef]
- Sharma, R.; Kshetri, N. Digital healthcare: Historical development, applications, and future research directions. Int. J. Inf. Manag. 2020, 53, 102105. [Google Scholar] [CrossRef]
- Abouelmehdi, K.; Beni-Hssane, A.; Khaloufi, H.; Saadi, M. Big data security and privacy in healthcare: A Review. Procedia Comput. Sci. 2017, 113, 73–80. [Google Scholar] [CrossRef]
- Panayides, A.S.; Amini, A.; Filipovic, N.D.; Sharma, A.; Tsaftaris, S.A.; Young, A.; Foran, D.J.; Do, N.; Golemati, S.; Kurc, T.; et al. AI in Medical Imaging Informatics: Current Challenges and Future Directions. IEEE J. Biomed. Health Inform. 2020, 24, 1837–1857. [Google Scholar] [CrossRef]
- Raghupathi, W.; Kesh, S. Designing electronic health records versus total digital health systems: A systemic analysis. Syst. Res. Behav. Sci. 2009, 26, 63–79. [Google Scholar] [CrossRef]
- Leslie, H. Commentary: The patient’s memory stick may complement electronic health records. Aust. Health Rev. 2005, 29, 401–405. [Google Scholar] [CrossRef]
- Cohen, A.B.; Mathews, S.C.; Dorsey, E.R.; Bates, D.W.; Safavi, K. Direct-to-consumer digital health. Lancet Digit. Health 2020, 2, e163–e165. [Google Scholar] [CrossRef]
- Aceto, G.; Persico, V.; Pescapé, A. Industry 4.0 and Health: Internet of Things, Big Data, and Cloud Computing for Healthcare 4.0. J. Ind. Inf. Integr. 2020, 18, 100129. [Google Scholar] [CrossRef]
- Lytras, M.D.; Papadopoulou, P.; Sarirete, A. Smart Healthcare: Emerging technologies, best practices, and sustainable policies. In Innovation in Health Informatics; Academic Press: Cambridge, MA, USA, 2020. [Google Scholar]
- Raghupathi, W.; Raghupathi, V. Big data analytics in healthcare: Promise and potential. Health Inf. Sci. Syst. 2014, 2, 3. [Google Scholar] [CrossRef]
- Albahri, A.S.; Alwan, J.K.; Taha, Z.K.; Ismail, S.F.; Hamid, R.A.; Zaidan, A.A.; Albahri, O.S.; Zaidan, B.B.; Alamoodi, A.H.; Alsalem, M.A. IoT-based telemedicine for disease prevention and health promotion: State-of-the-Art. J. Netw. Comput. Appl. 2021, 173, 102873. [Google Scholar] [CrossRef]
- Li, H.; Gupta, A.; Zhang, J.; Sarathy, R. Examining the decision to use standalone personal health record systems as a trust-enabled fair social contract. Decis. Support Syst. 2014, 57, 376–386. [Google Scholar] [CrossRef]
- Kaffash, S.; Azizi, R.; Huang, Y.; Zhu, J. A survey of data envelopment analysis applications in the insurance industry 1993–2018. Eur. J. Oper. Res. 2020, 284, 801–813. [Google Scholar] [CrossRef]
- Treskes, R.W.; van Winden, L.A.M.; van Keulen, N.; van der Velde, E.T.; Beeres, S.L.M.A.; Atsma, D.E.; Schalij, M.J. Effect of Smartphone-Enabled Health Monitoring Devices vs. Regular Follow-up on Blood Pressure Control Among Patients After Myocardial Infarction: A Randomized Clinical Trial. JAMA Netw. Open 2020, 3, e202165. [Google Scholar] [CrossRef]
- Lai, L.; Wittbold, K.A.; Dadabhoy, F.Z.; Sato, R.; Landman, A.B.; Schwamm, L.H.; He, S.; Patel, R.; Wei, N.; Zuccotti, G.; et al. Digital triage: Novel strategies for population health management in response to the COVID-19 pandemic. Healthcare 2020, 8, 100493. [Google Scholar] [CrossRef] [PubMed]
- Schwamm, L.H.; Erskine, A.; Licurse, A. A Digital Embrace to Blunt the Curve of COVID19 Pandemic. Available online: https://www.nature.com/articles/s41746-020-0279-6.pdf (accessed on 4 May 2020).
- Wootton, R. Telemedicine. Br. Med. J. 2001, 323, 557–560. [Google Scholar] [CrossRef] [PubMed]
- Merry, S.N.; Cargo, T.; Christie, G.; Donkin, L.; Hetrick, S.; Fleming, T.; Holt-Quick, C.; Hopkins, S.; Stasiak, K.; Warren, J. Debate: Supporting the mental health of school students in the COVID-19 pandemic in New Zealand—A digital ecosystem approach. Child Adolesc. Ment. Health 2020, 25, 267–269. [Google Scholar] [CrossRef]
- Barnes, S.J.; Pressey, A.D.; Scornavacca, E. Mobile ubiquity: Understanding the relationship between cognitive absorption, smartphone addiction and social network services. Comput. Hum. Behav. 2019, 90, 246–258. [Google Scholar] [CrossRef]
- Aluisio, A.R.; Zhu, E.; Gil, G.; Kenyon, T.; Uzevski, V.; Levine, A.C. Academic-humanitarian partnerships: Leveraging strengths to combat COVID-19. Glob. Health Action 2020, 13, 1797296. [Google Scholar] [CrossRef]
- Hiffler, L.; Rakotoambinina, B. Selenium and RNA Virus Interactions: Potential Implications for SARS-CoV-2 Infection (COVID-19). Front. Nutr. 2020, 7. [Google Scholar] [CrossRef]
- Chen, D.; Xu, W.; Lei, Z.; Huang, Z.; Liu, J.; Gao, Z.; Peng, L. Recurrence of positive SARS-CoV-2 RNA in COVID-19: A case report. Int. J. Infect. Dis. 2020, 93, 297–299. [Google Scholar] [CrossRef] [PubMed]
- Marian, A.J. Current state of vaccine development and targeted therapies for COVID-19: Impact of basic science discoveries. Cardiovasc. Pathol. 2021, 50. [Google Scholar] [CrossRef]
- Verma, S.; Gazara, R.K. Big Data Analytics for Understanding and Fighting COVID-19; Springer Science and Business Media Deutschland GmbH: Berlin/Heidelberg, Germany, 2021; Volume 923. [Google Scholar]
- Siyal, A.A.; Junejo, A.Z.; Zawish, M.; Ahmed, K.; Khalil, A.; Soursou, G. Applications of Blockchain Technology in Medicine and Healthcare: Challenges and Future Perspectives. Cryptography 2019, 3, 3. [Google Scholar] [CrossRef]
- Kuo, T.-T.; Kim, H.-E.; Ohno-Machado, L. Blockchain distributed ledger technologies for biomedical and health care applications. J. Am. Med. Inform. Assoc. 2017, 24, 1211–1220. [Google Scholar] [CrossRef] [PubMed]
- Khatoon, A. A Blockchain-Based Smart Contract System for Healthcare Management. Electronics 2020, 9, 94. [Google Scholar] [CrossRef]
- Clauson, K.A.; Breeden, E.A.; Davidson, C.; Mackey, T.K. Leveraging Blockchain Technology to Enhance Supply Chain Management in Healthcare. Blockchain Healthc. Today 2018. [Google Scholar] [CrossRef]
- Boccardi, F.; Heath, R.W.; Lozano, A.; Marzetta, T.L.; Popovski, P.J. Five disruptive technology directions for 5G. IEEE Commun. Mag. 2014, 52, 74–80. [Google Scholar] [CrossRef]
- Patwary, M.N.; Nawaz, S.J.; Rahman, A.; Sharma, S.K.; Rashid, M.; Barnes, S.J. The Potential Short- and Long-Term Disruptions and Transformative Impacts of 5G and Beyond Wireless Networks: Lessons Learnt From the Development of a 5G Testbed Environment. IEEE Access 2020, 8, 11352–11379. [Google Scholar] [CrossRef]
- Siriwardhana, Y.; Gür, G.; Ylianttila, M.; Liyanage, M. The role of 5G for digital healthcare against COVID-19 pandemic: Opportunities and challenges. ICT Express 2020. [Google Scholar] [CrossRef]
- Gupta, R.; Tanwar, S.; Tyagi, S.; Kumar, N.J.I.N. Tactile-Internet-Based Telesurgery System for Healthcare 4.0: An Architecture, Research Challenges, and Future Directions. IEEE Netw. 2019, 33, 22–29. [Google Scholar] [CrossRef]
- Osseiran, A.; Monserrat, J.F.; Marsch, P. 5G Mobile and Wireless Communications Technology; Cambridge University Press: Cambridge, UK, 2016. [Google Scholar]
- Peeri, N.C.; Shrestha, N.; Rahman, M.S.; Zaki, R.; Tan, Z.; Bibi, S.; Baghbanzadeh, M.; Aghamohammadi, N.; Zhang, W.; Haque, U. The SARS, MERS and novel coronavirus (COVID-19) epidemics, the newest and biggest global health threats: What lessons have we learned? Int. J. Epidemiol. 2020, 49, 717–726. [Google Scholar] [CrossRef]
- Chakraborty, I.; Maity, P. COVID-19 outbreak: Migration, effects on society, global environment and prevention. Sci. Total Environ. 2020, 728, 138882. [Google Scholar] [CrossRef]
- Song, Y.; Liu, P.; Shi, X.L.; Chu, Y.L.; Zhang, J.; Xia, J.; Gao, X.Z.; Qu, T.; Wang, M.Y. SARS-CoV-2 induced diarrhoea as onset symptom in patient with COVID-19. Gut 2020, 69, 1143. [Google Scholar] [CrossRef]
- Saurabh, A.; Nelson, G.-T.; Gaurav, A.; Carl, L.; Giuseppe, L.; Brandon Michael, H. Clinical features, laboratory characteristics, and outcomes of patients hospitalized with coronavirus disease 2019 (COVID-19): Early report from the United States. Diagnosis 2020, 7, 91–96. [Google Scholar] [CrossRef]
- Wang, C.J.; Ng, C.Y.; Brook, R.H. Response to COVID-19 in Taiwan: Big Data Analytics, New Technology, and Proactive Testing. JAMA 2020, 323, 1341–1342. [Google Scholar] [CrossRef] [PubMed]
- Lai, S.; Ruktanonchai, N.W.; Zhou, L.; Prosper, O.; Luo, W.; Floyd, J.R.; Wesolowski, A.; Santillana, M.; Zhang, C.; Du, X. Effect of non-pharmaceutical interventions to contain COVID-19 in China. Nature 2020, 585, 410–413. [Google Scholar] [CrossRef]
- Lewnard, J.A.; Lo, N.C. Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet Infect. Dis 2020, 20, 631–633. [Google Scholar] [CrossRef]
- Sun, J.; Shi, Z.; Xu, H. Non-pharmaceutical interventions used for COVID-19 had a major impact on reducing influenza in China in 2020. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- WHO. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—13 April 2020. Available online: https://www.who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19--13-april-2020 (accessed on 13 April 2020).
- He, Z. What further should be done to control COVID-19 outbreaks in addition to cases isolation and contact tracing measures? BMC Med. 2020, 18, 80. [Google Scholar] [CrossRef]
- Zhang, J.; Litvinova, M.; Liang, Y.; Wang, Y.; Wang, W.; Zhao, S.; Wu, Q.; Merler, S.; Viboud, C.; Vespignani, A.; et al. Changes in contact patterns shape the dynamics of the COVID-19 outbreak in China. Science 2020, 368, 1481. [Google Scholar] [CrossRef]
- Lai, C.-C.; Shih, T.-P.; Ko, W.-C.; Tang, H.-J.; Hsueh, P.-R. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19): The epidemic and the challenges. Int. J. Antimicrob. Agents 2020, 55, 105924. [Google Scholar] [CrossRef]
- Hellewell, J.; Abbott, S.; Gimma, A.; Bosse, N.I.; Jarvis, C.I.; Russell, T.W.; Munday, J.D.; Kucharski, A.J.; Edmunds, W.J.; Sun, F.; et al. Feasibility of controlling COVID-19 outbreaks by isolation of cases and contacts. Lancet Glob. Health 2020, 8, e488–e496. [Google Scholar] [CrossRef]
- Yang, Z.; Zeng, Z.; Wang, K.; Wong, S.-S.; Liang, W.; Zanin, M.; Liu, P.; Cao, X.; Gao, Z.; Mai, Z.; et al. Modified SEIR and AI prediction of the epidemics trend of COVID-19 in China under public health interventions. J. Thorac. Dis. 2020, 12, 165–174. [Google Scholar] [CrossRef]
- Bragazzi, N.L.; Dai, H.; Damiani, G.; Behzadifar, M.; Martini, M.; Wu, J. How Big Data and Artificial Intelligence Can Help Better Manage the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 3176. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.-K.; Liu, X.F.; Wu, Y.; Ali, S.T.; Du, Z.; Bosetti, P.; Lau, E.H.Y.; Cowling, B.J.; Wang, L. Reconstruction of Transmission Pairs for Novel Coronavirus Disease 2019 (COVID-19) in Mainland China: Estimation of Superspreading Events, Serial Interval, and Hazard of Infection. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- Bouchnita, A.; Jebrane, A. A hybrid multi-scale model of COVID-19 transmission dynamics to assess the potential of non-pharmaceutical interventions. Chaos Solitons Fractals 2020, 138, 109941. [Google Scholar] [CrossRef] [PubMed]
- Ting, D.S.W.; Carin, L.; Dzau, V.; Wong, T.Y. Digital technology and COVID-19. Nat. Med. 2020, 26, 459–461. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Su, M.; Li, R.; Ponce, P. The effects of energy prices, urbanization and economic growth on energy consumption per capita in 186 countries. J. Clean. Prod. 2019, 225, 1017–1032. [Google Scholar] [CrossRef]
- Chen, S.; Yang, J.; Yang, W.; Wang, C.; Bärnighausen, T. COVID-19 control in China during mass population movements at New Year. Lancet 2020, 395, 764–766. [Google Scholar] [CrossRef]
- Lin, L.; Hou, Z. Combat COVID-19 with artificial intelligence and big data. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef]
- He, P.; Niu, H.; Sun, Z.; Li, T. Accounting Index of COVID-19 Impact on Chinese Industries: A Case Study Using Big Data Portrait Analysis. Emerg. Mark. Financ. Trade 2020, 56, 2332–2349. [Google Scholar] [CrossRef]
- Zhu, B.; Zheng, X.; Liu, H.; Li, J.; Wang, P. Analysis of spatiotemporal characteristics of big data on social media sentiment with COVID-19 epidemic topics. Chaos Solitons Fractals 2020, 140, 110123. [Google Scholar] [CrossRef]
- Wu, J.; Wang, J.; Nicholas, S.; Maitland, E.; Fan, Q. Application of Big Data Technology for COVID-19 Prevention and Control in China: Lessons and Recommendations. J. Med. Internet Res. 2020, 22, e21980. [Google Scholar] [CrossRef] [PubMed]
- Wosik, J.; Fudim, M.; Cameron, B.; Gellad, Z.F.; Cho, A.; Phinney, D.; Curtis, S.; Roman, M.; Poon, E.G.; Ferranti, J.; et al. Telehealth transformation: COVID-19 and the rise of virtual care. J. Am. Med. Inform. Assoc. 2020, 27, 957–962. [Google Scholar] [CrossRef]
- Siriwardhana, Y.; Alwis, C.D.; Gür, G.; Ylianttila, M.; Liyanage, M. The Fight against the COVID-19 Pandemic With 5G Technologies. IEEE Eng. Manag. Rev. 2020, 48, 72–84. [Google Scholar] [CrossRef]
- Pandya, S.; Sur, A.; Kotecha, K. Smart epidemic tunnel: IoT-based sensor-fusion assistive technology for COVID-19 disinfection. Int. J. Pervasive Comput. Commun. 2020. [Google Scholar] [CrossRef]
- Carfì, A.; Bernabei, R.; Landi, F.; for the Gemelli against COVID-19 Post-Acute Care Study Group. Persistent Symptoms in Patients after Acute COVID-19. JAMA 2020, 324, 603–605. [Google Scholar] [CrossRef]
- Menni, C.; Valdes, A.M.; Freidin, M.B.; Sudre, C.H.; Nguyen, L.H.; Drew, D.A.; Ganesh, S.; Varsavsky, T.; Cardoso, M.J.; El-Sayed Moustafa, J.S.; et al. Real-time tracking of self-reported symptoms to predict potential COVID-19. Nat. Med. 2020, 26, 1037–1040. [Google Scholar] [CrossRef]
- Qilu Evening News. Intelligent Epidemic Prevention, Infrared Thermal Imaging Thermometer “On Duty”. Available online: http://baijiahao.baidu.com/s?id=1659591504293794902&wfr=spider&for=pc (accessed on 26 February 2020). (In Chinese).
- Scarano, A.; Inchingolo, F.; Lorusso, F. Facial skin temperature and discomfort when wearing protective face masks: Thermal infrared imaging evaluation and hands moving the mask. Int. J. Environ. Res. Public Health 2020, 17, 4624. [Google Scholar] [CrossRef] [PubMed]
- Rane, K.P. Design and development of low cost humanoid robot with thermal temperature scanner for COVID-19 virus preliminary identification. Int. J. Adv. Trends Comput. Sci. Eng. 2020, 9, 3485–3493. [Google Scholar] [CrossRef]
- Allam, Z.; Dey, G.; Jones, D.S. Artificial intelligence (AI) provided early detection of the coronavirus (COVID-19) in China and will influence future Urban health policy internationally. AI 2020, 1, 156–165. [Google Scholar] [CrossRef]
- Wang, Q.; Wang, S.; Jiang, X.-T. Preventing a rebound in carbon intensity post-COVID-19—Lessons learned from the change in carbon intensity before and after the 2008 financial crisis. Sustain. Prod. Consum. 2021, 27, 1841–1856. [Google Scholar] [CrossRef]
- Lauer, S.A.; Grantz, K.H.; Bi, Q.; Jones, F.K.; Zheng, Q.; Meredith, H.R.; Azman, A.S.; Reich, N.G.; Lessler, J. The Incubation Period of Coronavirus Disease 2019 (COVID-19) From Publicly Reported Confirmed Cases: Estimation and Application. Ann. Intern. Med. 2020, 172, 577–582. [Google Scholar] [CrossRef]
- Li, Q.; Guan, X.; Wu, P.; Wang, X.; Zhou, L.; Tong, Y.; Ren, R.; Leung, K.S.M.; Lau, E.H.Y.; Wong, J.Y.; et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus–Infected Pneumonia. N. Engl. J. Med. 2020, 382, 1199–1207. [Google Scholar] [CrossRef]
- Zhang, J.; Litvinova, M.; Wang, W.; Wang, Y.; Deng, X.; Chen, X.; Li, M.; Zheng, W.; Yi, L.; Chen, X.; et al. Evolving epidemiology and transmission dynamics of coronavirus disease 2019 outside Hubei province, China: A descriptive and modelling study. Lancet Infect. Dis. 2020, 20, 793–802. [Google Scholar] [CrossRef]
- Chen, J.; Qi, T.; Liu, L.; Ling, Y.; Qian, Z.; Li, T.; Li, F.; Xu, Q.; Zhang, Y.; Xu, S.; et al. Clinical progression of patients with COVID-19 in Shanghai, China. J. Infect. 2020, 80, e1–e6. [Google Scholar] [CrossRef]
- Brooke, J.; Jackson, D. Older people and COVID-19: Isolation, risk and ageism. J. Clin. Nurs. 2020, 29, 2044–2046. [Google Scholar] [CrossRef]
- State Administration of Science, Technology and Industry for National Defense. COVID-19 Close Contact Measuring Instrument. Available online: http://www.sastind.gov.cn/n112/n117/c6808819/content.html (accessed on 10 February 2020). (In Chinese)
- People’s Daily Online. In This Way, Close Contacts Are Detected. Available online: http://paper.people.com.cn/rmrb/html/2020-02/14/nw.D110000renmrb_20200214_1-12.htm (accessed on 14 February 2020). (In Chinese).
- National Health Commission of the People’s Republic of China. Contact Inquiry of the Same Vehicle. Available online: http://bmfw.www.gov.cn/ggjtmqjczcx/index.html (accessed on 3 June 2021). (In Chinese)
- Zhang, Z. China’s Travel Restrictions due to COVID-19: An Explainer. Available online: https://www.china-briefing.com/news/chinas-travel-restrictions-due-to-covid-19-an-explainer/ (accessed on 23 April 2021).
- Tang, B.; Xia, F.; Tang, S.; Bragazzi, N.L.; Li, Q.; Sun, X.; Liang, J.; Xiao, Y.; Wu, J. The effectiveness of quarantine and isolation determine the trend of the COVID-19 epidemics in the final phase of the current outbreak in China. Int. J. Infect. Dis. 2020, 95, 288–293. [Google Scholar] [CrossRef] [PubMed]
- Shen, J.; Duan, H.; Zhang, B.; Wang, J.; Ji, J.S.; Wang, J.; Pan, L.; Wang, X.; Zhao, K.; Ying, B.; et al. Prevention and control of COVID-19 in public transportation: Experience from China. Environ. Pollut. 2020, 266, 115291. [Google Scholar] [CrossRef] [PubMed]
- Cai, J.; Sun, W.; Huang, J.; Gamber, M.; Wu, J.; He, G. Indirect Virus Transmission in Cluster of COVID-19 Cases, Wenzhou, China, 2020. Emerg. Infect. Dis. J. 2020, 26, 1343. [Google Scholar] [CrossRef] [PubMed]
- Whitworth, J. COVID-19: A fast evolving pandemic. Trans. R. Soc. Trop.Med. Hyg. 2020, 114, 241–248. [Google Scholar] [CrossRef] [PubMed]
- Kucharski, A.J.; Klepac, P.; Conlan, A.; Kissler, S.M.; Tang, M.; Fry, H.; Gog, J.; Edmunds, J. Effectiveness of isolation, testing, contact tracing and physical distancing on reducing transmission of SARS-CoV-2 in different settings. Lancet Infect. Dis. 2020, 20, 1151–1160. [Google Scholar] [CrossRef]
- Hu, M.; Lin, H.; Wang, J.; Xu, C.; Tatem, A.J.; Meng, B.; Zhang, X.; Liu, Y.; Wang, P.; Wu, G.; et al. Risk of Coronavirus Disease 2019 Transmission in Train Passengers: An Epidemiological and Modeling Study. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Morley, J.; Cowls, J.; Taddeo, M.; Floridi, L. Ethical guidelines for COVID-19 tracing apps. Nat. Cell Biol. 2020, 582, 29–31. [Google Scholar] [CrossRef]
- Ahmed, N.; Michelin, R.A.; Xue, W.; Ruj, S.; Malaney, R.; Kanhere, S.S.; Seneviratne, A.; Hu, W.; Janicke, H.; Jha, S.K. A Survey of COVID-19 Contact Tracing Apps. IEEE Access 2020, 8, 134577–134601. [Google Scholar] [CrossRef]
- Whitelaw, S.; Mamas, M.A.; Topol, E.; Van Spall, H.G.C. Applications of digital technology in COVID-19 pandemic planning and response. Lancet Digit. Health 2020, 2, e435–e440. [Google Scholar] [CrossRef]
- Liu, W.; Yue, X.-G.; Tchounwou, P.B. Response to the COVID-19 Epidemic: The Chinese Experience and Implications for Other Countries. Int. J. Environ. Res. Public Health 2020, 17, 2304. [Google Scholar] [CrossRef]
- Huang, H.; Peng, Z.; Wu, H.; Xie, Q. A big data analysis on the five dimensions of emergency management information in the early stage of COVID-19 in China. J. Chin. Gov. 2020, 5, 213–233. [Google Scholar] [CrossRef]
- Macau News. Health Bureau Launches 3-Colour Code to Stem COVID-19 Spread. Available online: https://macaonews.org/health-bureau-launches-3-colour-code-to-stem-covid-19-spread/ (accessed on 22 November 2020).
- Wang, Q.; Su, M.; Li, R. Toward to economic growth without emission growth: The role of urbanization and industrialization in China and India. J. Clean. Prod. 2018, 205, 499–511. [Google Scholar] [CrossRef]
- Cortese, R.; Tur, C.; Prados, F.; Schneider, T.; Kanber, B.; Moccia, M.; Wheeler-Kingshott, C.A.M.G.; Thompson, A.J.; Barkhof, F.; Ciccarelli, O. Ongoing microstructural changes in the cervical cord underpin disability progression in early primary progressive multiple sclerosis. Mult. Scler. J. 2020, 27, 28–38. [Google Scholar] [CrossRef]
- Xinhuanet. Industrial Pulse under the Epidemic: 5G Releases Technological Dividends, Digital Medical Treatment has Emerged. Available online: http://www.xinhuanet.com/tech/2020-02/26/c_1125624838.htm (accessed on 26 February 2020). (In Chinese).
- Health Leaders. Coronavirus: Virtual Hospital at Home Program Used for Low-Acuity Patients. Available online: https://www.healthleadersmedia.com/clinical-care/coronavirus-virtual-hospital-home-program-used-low-acuity-patients (accessed on 28 September 2020).
- Song, X.; Liu, X.; Wang, C. The role of telemedicine during the COVID-19 epidemic in China—Experience from Shandong province. Crit. Care 2020, 24, 178. [Google Scholar] [CrossRef]
- Bokolo Anthony, J. Use of Telemedicine and Virtual Care for Remote Treatment in Response to COVID-19 Pandemic. J. Med. Syst. 2020, 44, 132. [Google Scholar] [CrossRef]
- Philips. eICU Program—Telehealth for the Intensive Care Unit. Available online: https://www.philips.com.hk/healthcare/product/HC865325ICU/eicu-program-telehealth-for-the-intensive-care-unit (accessed on 3 June 2021).
- Jefferies, J.G.; Bishop, S.; Hibbert, S. Customer boundary work to navigate institutional arrangements around service interactions: Exploring the case of telehealth. J. Bus. Res. 2019, 105, 420–433. [Google Scholar] [CrossRef]
- News Break. Swedish Health Services Taps Microsoft to Build App That Tracks COVID-19 Patients, Hospital Capacity. Available online: https://www.newsbreak.com/news/1539889832861/swedish-health-services-taps-microsoft-to-build-app-that-tracks-covid-19-patients-hospital-capacity (accessed on 3 June 2021).
- U.S. News. Germany Launches Smartwatch App to Monitor Coronavirus Spread. Available online: https://www.usnews.com/news/technology/articles/2020-04-07/germany-launches-smartwatch-app-to-monitor-coronavirus-spread (accessed on 7 April 2020).
- Gozes, O.; Frid-Adar, M.; Greenspan, H.; Browning, P.D.; Zhang, H.; Ji, W.; Bernheim, A.; Siegel, E. Rapid ai development cycle for the coronavirus (covid-19) pandemic: Initial results for automated detection & patient monitoring using deep learning ct image analysis. arXiv 2020, arXiv:2003.05037. Available online: https://arxiv.org/abs/2003.05037 (accessed on 24 March 2020).
- Chowdhury, M.E.; Rahman, T.; Khandakar, A.; Mazhar, R.; Kadir, M.A.; Mahbub, Z.B.; Islam, K.R.; Khan, M.S.; Iqbal, A.; Al-Emadi, N. Can AI help in screening viral and COVID-19 pneumonia? arXiv 2020, arXiv:2003.13145. Available online: https://arxiv.org/pdf/2003.13145v1.pdf (accessed on 3 June 2021). [CrossRef]
- Lessmann, N.; Sánchez, C.I.; Beenen, L.; Boulogne, L.H.; Brink, M.; Calli, E.; Charbonnier, J.-P.; Dofferhoff, T.; van Everdingen, W.M.; Gerke, P.K.; et al. Automated Assessment of CO-RADS and Chest CT Severity Scores in Patients with Suspected COVID-19 Using Artificial Intelligence. Radiology 2020, 298, E18–E28. [Google Scholar] [CrossRef]
- Bai, H.X.; Wang, R.; Xiong, Z.; Hsieh, B.; Chang, K.; Halsey, K.; Tran, T.M.L.; Choi, J.W.; Wang, D.-C.; Shi, L.-B.; et al. Artificial Intelligence Augmentation of Radiologist Performance in Distinguishing COVID-19 from Pneumonia of Other Origin at Chest CT. Radiology 2020, 296, E156–E165. [Google Scholar] [CrossRef]
- European Commission. Using AI to Fast and Effectively Diagnose COVID-19 in Hospitals. Available online: https://ec.europa.eu/digital-single-market/en/news/using-ai-fast-and-effectively-diagnose-covid-19-hospitals (accessed on 8 March 2021).
- Yang, G.-Z.J.; Nelson, B.; Murphy, R.R.; Choset, H.; Christensen, H.H.; Collins, S.; Dario, P.; Goldberg, K.; Ikuta, K.; Jacobstein, N.; et al. Combating COVID-19—The role of robotics in managing public health and infectious diseases. Sci. Robot. 2020, 5, eabb5589. [Google Scholar] [CrossRef]
- Zeng, Z.; Chen, P.-J.; Lew, A.A. From high-touch to high-tech: COVID-19 drives robotics adoption. Tour. Geogr. 2020, 22, 724–734. [Google Scholar] [CrossRef]
- Jat, D.S.; Singh, C. Artificial Intelligence-Enabled Robotic Drones for COVID-19 Outbreak. In Intelligent Systems and Methods to Combat Covid-19; Springer: Berlin/Heidelberg, Germany, 2020; pp. 37–46. [Google Scholar]
- Chen, B.; Marvin, S.; While, A. Containing COVID-19 in China: AI and the robotic restructuring of future cities. Dialogues Hum. Geogr. 2020, 10, 238–241. [Google Scholar] [CrossRef]
- Duan, Y.; Edwards, J.S.; Dwivedi, Y.K. Artificial intelligence for decision making in the era of Big Data—Evolution, challenges and research agenda. Int. J. Inf. Manag. 2019, 48, 63–71. [Google Scholar] [CrossRef]
- Ahir, S.; Telavane, D.; Thomas, R. The Impact of Artificial Intelligence, Blockchain, Big Data and Evolving Technologies in Coronavirus Disease—2019 (COVID-19) Curtailment. In Proceedings of the 2020 International Conference on Smart Electronics and Communication (ICOSEC), Trichy, India, 10–12 September 2020; pp. 113–120. [Google Scholar]
- Yan, A.; Zou, Y.; Mirchandani, D.A. How hospitals in mainland China responded to the outbreak of COVID-19 using information technology–enabled services: An analysis of hospital news webpages. J. Am. Med. Inform. Assoc. 2020, 27, 991–999. [Google Scholar] [CrossRef]
- Khan, Z.H.; Siddique, A.; Lee, C.W. Robotics Utilization for Healthcare Digitization in Global COVID-19 Management. Int. J. Environ. Res. Public Health 2020, 17, 3819. [Google Scholar] [CrossRef]
- European Commission. Coronavirus: Commission to Provide 200 Disinfection Robots to European Hospitals. Available online: https://ec.europa.eu/digital-single-market/en/news/coronavirus-commission-provide-200-disinfection-robots-european-hospitals (accessed on 8 March 2021).
- OpenKG.CN. Knowledge Graphs about COVID-19. Available online: http://openkg.cn/group/coronavirus (accessed on 3 June 2021). (In Chinese).
- Daughton, C. The international imperative to rapidly and inexpensively monitor community-wide Covid-19 infection status and trends. Sci. Total Environ. 2020, 726, 138149. [Google Scholar] [CrossRef]
- Braithwaite, I.; Callender, T.; Bullock, M.; Aldridge, R.W. Automated and partly automated contact tracing: A systematic review to inform the control of COVID-19. Lancet Digit. Health 2020, 2, e607–e621. [Google Scholar] [CrossRef]
- Abeler, J.; Bäcker, M.; Buermeyer, U.; Zillessen, H. COVID-19 Contact Tracing and Data Protection Can Go Together. JMIR mHealth uHealth 2020, 8, e19359. [Google Scholar] [CrossRef] [PubMed]
- Jonker, M.; de Bekker-Grob, E.; Veldwijk, J.; Goossens, L.; Bour, S.; Rutten-Van Mölken, M. COVID-19 Contact Tracing Apps: Predicted Uptake in the Netherlands Based on a Discrete Choice Experiment. JMIR mHealth uHealth 2020, 8, e20741. [Google Scholar] [CrossRef]
- Sun, Z.; Zhang, H.; Yang, Y.; Wan, H.; Wang, Y. Impacts of geographic factors and population density on the COVID-19 spreading under the lockdown policies of China. Sci. Total Environ. 2020, 746, 141347. [Google Scholar] [CrossRef]
- Normal Business Daily. Public Health Surveillance is Moving into Phase 2.0. Available online: http://www.nbd.com.cn/articles/2020-06-24/1450223.html (accessed on 24 June 2020). (In Chinese).
- Bai, X.; Fang, C.; Zhou, Y.; Bai, S.; Liu, Z.; Xia, L.; Chen, Q.; Xu, Y.; Xia, T.; Gong, S.; et al. Predicting COVID-19 malignant progression with AI techniques. 2020. Available online: https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3557984 (accessed on 31 March 2020).
- Jia, J.S.; Lu, X.; Yuan, Y.; Xu, G.; Jia, J.; Christakis, N.A. Population flow drives spatio-temporal distribution of COVID-19 in China. Nature 2020, 582, 389–394. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.A.; Atangana, A.; Alzahrani, E. The dynamics of COVID-19 with quarantined and isolation. Adv. Differ. Equ. 2020, 2020, 425. [Google Scholar] [CrossRef]
- Al-Qaness, M.A.; Ewees, A.A.; Fan, H.; Abd El Aziz, M. Optimization method for forecasting confirmed cases of COVID-19 in China. J. Clin. Med. 2020, 9, 674. [Google Scholar] [CrossRef]
- Tuli, S.; Tuli, S.; Tuli, R.; Gill, S.S. Predicting the growth and trend of COVID-19 pandemic using machine learning and cloud computing. Internet Things 2020, 11, 100222. [Google Scholar] [CrossRef]
- DX Doctor. COVID-19 Global Pandemic Real-time Report. Available online: https://ncov.dxy.cn/ncovh5/view/en_pneumonia?from=dxy&source=&link=&share (accessed on 3 June 2021).
- European Commission. Digital Solutions during the Pandemic. Available online: https://ec.europa.eu/info/live-work-travel-eu/coronavirus-response/digital-solutions-during-pandemic_en#innovative-solutions (accessed on 3 June 2021).
- Zhao, S.; Chen, H. Modeling the epidemic dynamics and control of COVID-19 outbreak in China. Quant. Biol. 2020, 8, 1–9. [Google Scholar] [CrossRef]
- Sun, G.-Q.; Wang, S.-F.; Li, M.-T.; Li, L.; Zhang, J.; Zhang, W.; Jin, Z.; Feng, G.-L. Transmission dynamics of COVID-19 in Wuhan, China: Effects of lockdown and medical resources. Nonlinear Dyn. 2020, 101, 1981–1993. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Yao, W.; Wang, Y.; Long, C.; Fu, X. Wuhan and Hubei COVID-19 mortality analysis reveals the critical role of timely supply of medical resources. J. Infect. 2020, 81, 147–178. [Google Scholar] [CrossRef]
- Emanuel, E.J.; Persad, G.; Upshur, R.; Thome, B.; Parker, M.; Glickman, A.; Zhang, C.; Boyle, C.; Smith, M.; Phillips, J.P. Fair Allocation of Scarce Medical Resources in the Time of Covid-19. N. Engl. J. Med. 2020, 382, 2049–2055. [Google Scholar] [CrossRef]
- Ying, S.; Li, F.; Geng, X.; Li, Z.; Du, X.; Chen, H.; Chen, S.; Zhang, M.; Shao, Z.; Wu, Y.; et al. Spread and control of COVID-19 in China and their associations with population movement, public health emergency measures, and medical resources. medRxiv 2020. [Google Scholar] [CrossRef]
- Wang, H.; Wang, S.; Yu, K. COVID-19 infection epidemic: The medical management strategies in Heilongjiang Province, China. Crit. Care 2020, 24, 107. [Google Scholar] [CrossRef] [PubMed]
- The Cyberspace Administration of China. COVID-19 Accelerates Digital Transformation. Available online: http://www.cac.gov.cn/2020-03/19/c_1586163219396289.htm (accessed on 19 March 2020). (In Chinese)
- Xinhuanet. New Generation Information Technology Presses “Fast Forward” Button for Epidemic Prevention and Control and Return to Work and Production. Available online: http://www.xinhuanet.com/tech/2020-03/05/c_1125667595.htm (accessed on 5 March 2020). (In Chinese).
- Johns Hopkins University. Global Tracking Map: COVID-19 Cases and Data Visualization. Available online: https://coronavirus.jhu.edu/map.html (accessed on 12 January 2021).
- Zhou, Y.; Xu, R.; Hu, D.; Yue, Y.; Li, Q.; Xia, J. Effects of human mobility restrictions on the spread of COVID-19 in Shenzhen, China: A modelling study using mobile phone data. Lancet Digit. Health 2020, 2, e417–e424. [Google Scholar] [CrossRef]
- Oliver, N.; Lepri, B.; Sterly, H.; Lambiotte, R.; Deletaille, S.; De Nadai, M.; Letouzé, E.; Salah, A.A.; Benjamins, R.; Cattuto, C.; et al. Mobile phone data for informing public health actions across the COVID-19 pandemic life cycle. Sci. Adv. 2020, 6, eabc0764. [Google Scholar] [CrossRef]
- Walrave, M.; Waeterloos, C.; Ponnet, K. Adoption of a Contact Tracing App for Containing COVID-19: A Health Belief Model Approach. JMIR Public Health Surveill 2020, 6, e20572. [Google Scholar] [CrossRef]
- Cai, X.; Zheng, Z.; Su, Q.; Huang, J. Visualization analysis of the characteristics of COVID-19 clinical trial. Res. Sq. 2020. [Google Scholar] [CrossRef]
- Baidu. Baidu migration map. Available online: https://qianxi.baidu.com/2020/ (accessed on 15 March 2020). (In Chinese).
- New Europe. European Commission Launches Covid-19 Data Platform. Available online: https://www.neweurope.eu/article/european-commission-launches-covid-19-data-platform/ (accessed on 21 April 2020).
- Nour, M.; Cömert, Z.; Polat, K. A Novel Medical Diagnosis model for COVID-19 infection detection based on Deep Features and Bayesian Optimization. Appl. Soft Comput. 2020, 97, 106580. [Google Scholar] [CrossRef] [PubMed]
- Raza, K. Artificial Intelligence Against COVID-19: A Meta-analysis of Current Research. In Big Data Analytics and Artificial Intelligence Against COVID-19: Innovation Vision and Approach; Hassanien, A.-E., Dey, N., Elghamrawy, S., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 165–176. [Google Scholar]
- Allen, W.E.; Altae-Tran, H.; Briggs, J.; Jin, X.; McGee, G.; Shi, A.; Raghavan, R.; Kamariza, M.; Nova, N.; Pereta, A.; et al. Population-scale longitudinal mapping of COVID-19 symptoms, behaviour and testing. Nat. Hum. Behav. 2020, 4, 972–982. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, M.; Kneifel, C.; Orlikowski, V.; Dorff, J.; Newton, M.; Howard, A.; Shinn, D.; Bishawi, M.; Chidyagwai, S.; Balogh, P.; et al. Cloud Computing for COVID-19: Lessons Learned From Massively Parallel Models of Ventilator Splitting. Comput. Sci. Eng. 2020, 22, 37–47. [Google Scholar] [CrossRef]
- Mohanty, S.; Harun Ai Rashid, M.; Mridul, M.; Mohanty, C.; Swayamsiddha, S. Application of Artificial Intelligence in COVID-19 drug repurposing. Diabetes Metab. Syndr. Clin. Res. Rev. 2020, 14, 1027–1031. [Google Scholar] [CrossRef] [PubMed]
- Vaishya, R.; Javaid, M.; Khan, I.H.; Haleem, A. Artificial Intelligence (AI) applications for COVID-19 pandemic. Diabetes Metab. Syndr. Clin. Res. Rev. 2020, 14, 337–339. [Google Scholar] [CrossRef] [PubMed]
- Xinhuanet. They are Here to fight the “epidemic”!—Science and technology companies and scientific research institutions are fully invested in the Fight against COVID-19. Available online: http://www.xinhuanet.com/politics/2020-03/01/c_1125646570.htm (accessed on 1 March 2020). (In Chinese).
- European Commission. Coronavirus: EU-Funded Project Launches a Clinical Trial for Coronavirus Treatment in Italy. Available online: https://ec.europa.eu/digital-single-market/en/news/coronavirus-eu-funded-project-launches-clinical-trial-coronavirus-treatment-italy (accessed on 27 October 2020).
- Naudé, W. Artificial intelligence vs. COVID-19: Limitations, constraints and pitfalls. AI Soc. 2020, 35, 761–765. [Google Scholar] [CrossRef]
- Zhou, C.; Su, F.; Pei, T.; Zhang, A.; Du, Y.; Luo, B.; Cao, Z.; Wang, J.; Yuan, W.; Zhu, Y.; et al. COVID-19: Challenges to GIS with Big Data. Geogr. Sustain. 2020, 1, 77–87. [Google Scholar] [CrossRef]
- Grantz, K.H.; Meredith, H.R.; Cummings, D.A.T.; Metcalf, C.J.E.; Grenfell, B.T.; Giles, J.R.; Mehta, S.; Solomon, S.; Labrique, A.; Kishore, N.; et al. The use of mobile phone data to inform analysis of COVID-19 pandemic epidemiology. Nat. Commun. 2020, 11, 4961. [Google Scholar] [CrossRef]
- Wu, J.; Xie, X.; Yang, L.; Xu, X.; Cai, Y.; Wang, T.; Xie, X. Mobile health technology combats COVID-19 in China. J. Infect. 2020. [Google Scholar] [CrossRef]
- Pan, X.-B. Application of personal-oriented digital technology in preventing transmission of COVID-19, China. Ir. J. Med. Sci. 2020, 189, 1145–1146. [Google Scholar] [CrossRef]
- Srinivasa Rao, A.S.R.; Vazquez, J.A. Identification of COVID-19 can be quicker through artificial intelligence framework using a mobile phone–based survey when cities and towns are under quarantine. Infect. Control Hosp. Epidemiol. 2020, 41, 826–830. [Google Scholar] [CrossRef]
- Price, W.N.; Cohen, I.G. Privacy in the age of medical big data. Nat. Med. 2019, 25, 37–43. [Google Scholar] [CrossRef]
- Jeong, Y.-S.; Shin, S.-S. An efficient authentication scheme to protect user privacy in seamless big data services. Wirel. Pers. Commun. 2016, 86, 7–19. [Google Scholar] [CrossRef]
- Dwork, C. Differential Privacy: A Survey of Results. In Proceedings of the Theory and Applications of Models of Computation, Xi’an, China, 25–29 April 2008; Springer: Berlin, Heidelberg, 2008; pp. 1–19. [Google Scholar]
- Yaqoob, T.; Abbas, H.; Atiquzzaman, M. Security Vulnerabilities, Attacks, Countermeasures, and Regulations of Networked Medical Devices—A Review. IEEE Commun. Surv. Tutor. 2019, 21, 3723–3768. [Google Scholar] [CrossRef]
- Loncar-Turukalo, T.; Zdravevski, E.; da Silva, J.M.; Chouvarda, I.; Trajkovik, V. Literature on wearable technology for connected health: Scoping review of research trends, advances, and barriers. J. Med. Internet Res. 2019, 21, e14017. [Google Scholar] [CrossRef]
- Greenleaf, G. Global Data Privacy Laws 2017: 120 National Data Privacy Laws, Including Indonesia and Turkey; 145 Privacy Laws & Business International Report; UNSW: Sydney, Australia, 2017; Volume 145, pp. 10–13. [Google Scholar]
- Ienca, M.; Vayena, E. On the responsible use of digital data to tackle the COVID-19 pandemic. Nat. Med. 2020, 26, 463–464. [Google Scholar] [CrossRef]
- Javaid, M.; Haleem, A.; Vaishya, R.; Bahl, S.; Suman, R.; Vaish, A. Industry 4.0 technologies and their applications in fighting COVID-19 pandemic. Diabetes Metab. Syndr. Clin. Res. Rev. 2020, 14, 419–422. [Google Scholar] [CrossRef] [PubMed]
- Chamola, V.; Hassija, V.; Gupta, V.; Guizani, M. A Comprehensive Review of the COVID-19 Pandemic and the Role of IoT, Drones, AI, Blockchain, and 5G in Managing its Impact. IEEE Access 2020, 8, 90225–90265. [Google Scholar] [CrossRef]
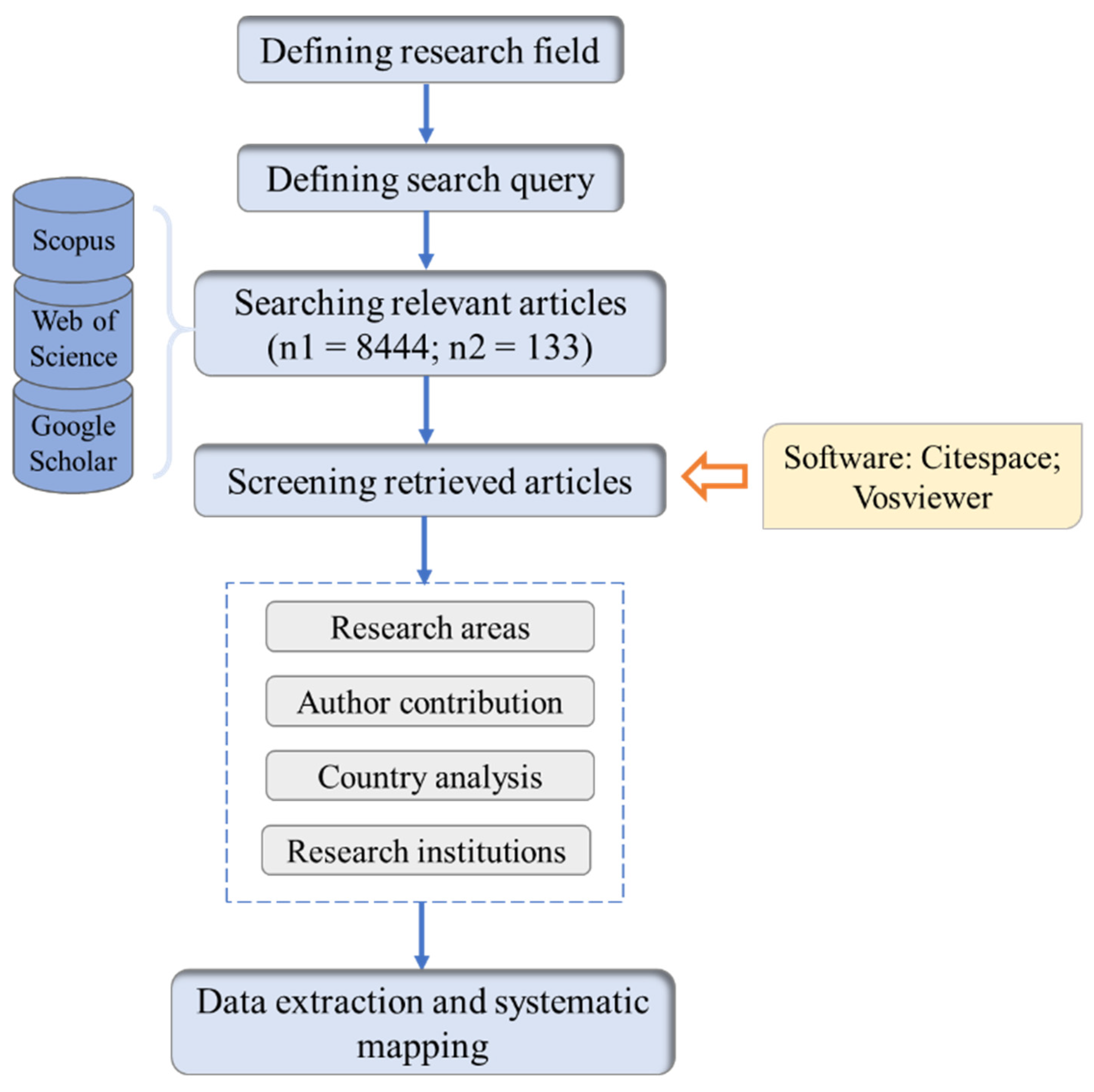






| Topic | Search Strategy | Publications |
|---|---|---|
| Digital healthcare | TITLE-ABS-KEY (digital AND healthcare) | 8444 |
| COVID-19&Digital healthcare | (TITLE-ABS-KEY (covid-19) OR TITLE-ABS-KEY (2019-ncov) OR TITLE-ABS-KEY (2019 novel AND coronavirus *) OR TITLE-ABS-KEY (2019 novel-cov) AND TITLE-ABS-KEY (digital AND healthcare)) | 133 |
| Funding Agency | Country/Region | Type |
|---|---|---|
| National Institutes of Health | United States | public funding |
| National Natural Science Foundation of China | China | public funding |
| National Science Foundation | United States | public funding |
| National Institute for Health Research | United States | public funding |
| European Commission | Europe | public funding |
| Horizon 2020 Framework Programme | Europe | public funding |
| European Regional Development Fund | Europe | public funding |
| Medical Research Council | United Kingdom | public funding |
| National Cancer Institute | China | public funding |
| Engineering and Physical Sciences Research Council | United Kingdom | public funding |
| Source Publication | Country | Subject Area and Category | H-Index | SJR 2019 | SNIP 2019 |
|---|---|---|---|---|---|
| Studies in Health Technology and Informatics | Netherlands | Engineering; Health Professions; Medicine | 56 | 0.267 | 0.457 |
| Lecture Notes in Computer Science | Germany | Computer Science; Mathematics | 356 | 0.427 | 0.776 |
| Advances in Intelligent Systems and Computing | Germany | Computer Science; Engineering | 34 | 0.184 | 0.429 |
| ACM International Conference Proceeding Series | United States | Computer Science | 109 | 0.2 | 0.333 |
| IEEE Access | United States | Computer Science; Engineering; Materials Science | 86 | 0.775 | 1.734 |
| BMJ Open | United Kingdom | Medicine | 84 | 1.247 | 1.359 |
| Communications in Computer and Information Science | Germany | Computer Science; Mathematics | 45 | 0.188 | 0.403 |
| International Journal of Medical Informatics | Ireland | Medicine | 99 | 0.954 | 1.958 |
| Journal of Digital Imaging | United States | Computer Science; Health Professions; Medicine | 51 | 0.967 | 1.641 |
| Proceedings of SPIE The International Society for Optical Engineering | United States | Computer Science; Engineering; Materials Science; Mathematics; Physics and Astronomy | 162 | 0.215 | 320 |
| Securities Code | Market Value (2020/5, Billion USD) | Quote Change (January–May) | Business Profile |
|---|---|---|---|
| LVGO.O | 57.74 | 135.55 | Chronic disease management |
| TDOC.N | 128.21 | 105.69 | Telemedicine |
| SMED.O | 1.14 | 65.88 | Medical waste treatment |
| AHCO.O | 12.22 | 50.27 | Respiratory equipment rental and sales |
| INFU.A | 2.3 | 34.47 | Medical Supplies |
| CATS.O | 3.61 | 30.35 | Psychological intervention-Insurance |
| PRSC.O | 8.65 | 16.52 | Pharmaceutical logistics |
| LHCG.O | 50.6 | 16.27 | Hospice care + Home care |
| AMED.O | 62.56 | 15.74 | Hospice care + Home rehabilitation |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, Q.; Su, M.; Zhang, M.; Li, R. Integrating Digital Technologies and Public Health to Fight Covid-19 Pandemic: Key Technologies, Applications, Challenges and Outlook of Digital Healthcare. Int. J. Environ. Res. Public Health 2021, 18, 6053. https://doi.org/10.3390/ijerph18116053
Wang Q, Su M, Zhang M, Li R. Integrating Digital Technologies and Public Health to Fight Covid-19 Pandemic: Key Technologies, Applications, Challenges and Outlook of Digital Healthcare. International Journal of Environmental Research and Public Health. 2021; 18(11):6053. https://doi.org/10.3390/ijerph18116053
Chicago/Turabian StyleWang, Qiang, Min Su, Min Zhang, and Rongrong Li. 2021. "Integrating Digital Technologies and Public Health to Fight Covid-19 Pandemic: Key Technologies, Applications, Challenges and Outlook of Digital Healthcare" International Journal of Environmental Research and Public Health 18, no. 11: 6053. https://doi.org/10.3390/ijerph18116053
APA StyleWang, Q., Su, M., Zhang, M., & Li, R. (2021). Integrating Digital Technologies and Public Health to Fight Covid-19 Pandemic: Key Technologies, Applications, Challenges and Outlook of Digital Healthcare. International Journal of Environmental Research and Public Health, 18(11), 6053. https://doi.org/10.3390/ijerph18116053