Sleep Valuation Is Associated with Components of Sleep Health and Daytime Functioning in a College Sample: A Survey Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedures
2.3. Measures
2.3.1. Sleep Valuation
2.3.2. Sleep Health Variables
2.3.3. Daytime Functioning Variables
2.3.4. Preliminary Analyses
2.3.5. Main Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kahneman, D.; Tversky, A. Prospect Theory: An analysis of decision under risk. Econometrica 1979, 47, 263–291. [Google Scholar] [CrossRef]
- Weiss, G.L.; Larsen, D.L. Health value, health locus of control, and the prediction of health protective behaviors. Soc. Behav. Personal. Int. J. 1990, 18, 121–135. [Google Scholar] [CrossRef]
- Kristiansen, C.M. Value correlates of preventive health behavior. J. Pers. Soc. Psychol. 1985, 49, 748–758. [Google Scholar] [CrossRef] [PubMed]
- Jackson, E.S.; Tucker, C.M.; Herman, K.C. Health value, perceived social support, and health self-efficacy as factors in a health-promoting lifestyle. J. Am. Coll. Health 2007, 56, 69–74. [Google Scholar] [CrossRef] [PubMed]
- Buysse, D.J. Sleep health: Can we define it? Does it matter? Sleep 2014, 37, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Cappuccio, F.P.; Cooper, D.; D’Elia, L.; Strazzullo, P.; Miller, M.A. Sleep duration predicts cardiovascular outcomes: A systematic review and meta-analysis of prospective studies. Eur. Heart J. 2011, 32, 1484–1492. [Google Scholar] [CrossRef]
- Jennings, J.R.; Muldoon, M.F.; Hall, M.; Buysse, D.J.; Manuck, S.B. Self-reported sleep quality is associated with the metabolic syndrome. Sleep 2007, 30, 219–223. [Google Scholar] [CrossRef]
- Newman, A.B.; Spiekerman, C.F.; MD, P.E.; Lefkowitz, D.; Manolio, T.; Reynolds, C.F.; Robbins, J. Daytime sleepiness predicts mortality and cardiovascular disease in older adults. J. Am. Geriatr. Soc. 2000, 48, 115–123. [Google Scholar] [CrossRef]
- Van Dongen, H.P.; Maislin, G.; Mullington, J.M.; Dinges, D.F. The cumulative cost of additional wakefulness: Dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep 2003, 26, 117–126. [Google Scholar] [CrossRef] [PubMed]
- Dew, M.A.; Hoch, C.C.; Buysse, D.J.; Monk, T.H.; Begley, A.E.; Houck, P.R.; Hall, M.; Kupfer, D.J.; Reynolds, C.F.I. Healthy older adults’ sleep predicts all-cause mortality at 4 to 19 years of follow-up. Psychosom. Med. 2003, 65, 63–73. [Google Scholar] [CrossRef] [PubMed]
- Wallace, M.L.; Stone, K.; Smagula, S.F.; Hall, M.H.; Simsek, B.; Kado, D.M.; Redline, S.; Vo, T.N.; Buysse, D.J. Which sleep health characteristics predict all-cause mortality in older men? An application of flexible multivariable approaches. Sleep 2018, 41. [Google Scholar] [CrossRef]
- Wallace, M.L.; Yu, L.; Buysse, D.J.; Stone, K.L.; Redline, S.; Smagula, S.F.; Stefanick, M.L.; Kritz-Silverstein, D.; Hall, M.H. Multidimensional sleep health domains in older men and women: An actigraphy factor analysis. Sleep 2021, 44. [Google Scholar] [CrossRef]
- Ravyts, S.G.; Dzierzewski, J.M.; Perez, E.; Donovan, E.K.; Dautovich, N.D. Sleep Health as measured by RU SATED: A psychometric evaluation. Behav. Sleep Med. 2021, 19, 48–56. [Google Scholar] [CrossRef]
- Cappuccio, F.P.; Elia, L.; Strazzullo, P.; Miller, M.A. Quantity and quality of sleep and incidence of Type 2 Diabetes. Diabetes Care 2010, 33, 414. [Google Scholar] [CrossRef]
- Hoevenaar-Blom, M.P.; Spijkerman, A.M.W.; Kromhout, D.; van den Berg, J.F.; Verschuren, W.M.M. Sleep duration and sleep quality in relation to 12-Year cardiovascular disease incidence: The MORGEN study. Sleep 2011, 34, 1487–1492. [Google Scholar] [CrossRef]
- Haseli-Mashhadi, N.; Dadd, T.; Pan, A.; Yu, Z.; Lin, X.; Franco, O.H. Sleep quality in middle-aged and elderly Chinese: Distribution, associated factors and associations with cardio-metabolic risk factors. BMC Public Health 2009, 9, 130. [Google Scholar] [CrossRef]
- Troxel, W.M.; Buysse, D.J.; Matthews, K.A.; Kip, K.E.; Strollo, P.J.; Hall, M.; Drumheller, O.; Reis, S.E. Sleep symptoms predict the development of the metabolic syndrome. Sleep 2010, 33, 1633–1640. [Google Scholar] [CrossRef]
- Sabanayagam, C.; Shankar, A.; Buchwald, D.; Goins, R.T. Insomnia symptoms and cardiovascular disease among older American Indians: The Native Elder Care Study. J. Env. Public Health 2011, 2011, 964617. [Google Scholar] [CrossRef]
- Dinges, D.F.; Pack, F.; Williams, K.; Gillen, K.A.; Powell, J.W.; Ott, G.E.; Aptowicz, C.; Pack, A.I. Cumulative Sleepiness, Mood Disturbance, and Psychomotor Vigilance Performance Decrements During a Week of Sleep Restricted to 4–5 Hours per Night. Sleep 1997, 20, 267–277. [Google Scholar] [CrossRef]
- Åkerstedt, T.; Kecklund, G.; Johansson, S.-E. Shift work and mortality. Chronobiol. Int. 2004, 21, 1055–1061. [Google Scholar] [CrossRef]
- Kawachi, I.; Colditz, G.A.; Stampfer, M.J.; Willett, W.C.; Manson, J.E.; Speizer, F.E.; Hennekens, C.H. Prospective study of shift work and risk of coronary heart disease in women. Circulation 1995, 92, 3178–3182. [Google Scholar] [CrossRef] [PubMed]
- Buxton, O.M.; Cain, S.W.; O’Connor, S.P.; Porter, J.H.; Duffy, J.F.; Wang, W.; Czeisler, C.A.; Shea, S.A. Adverse metabolic consequences in humans of prolonged sleep restriction combined with circadian disruption. Sci. Transl. Med. 2012, 4, 129ra143. [Google Scholar] [CrossRef]
- Huang, T.; Mariani, S.; Redline, S. Sleep irregularity and risk of cardiovascular events: The multi-ethnic study of Atherosclerosis. J. Am Coll. Cardiol. 2020, 75, 991–999. [Google Scholar] [CrossRef]
- Grandner, M.A.; Jackson, N.J.; Pak, V.M.; Gehrman, P.R. Sleep disturbance is associated with cardiovascular and metabolic disorders. J. Sleep Res. 2012, 21, 427–433. [Google Scholar] [CrossRef] [PubMed]
- Brindle, R.C.; Yu, L.; Buysse, D.J.; Hall, M.H. Empirical derivation of cutoff values for the sleep health metric and its relationship to cardiometabolic morbidity: Results from the Midlife in the United States (MIDUS) study. Sleep 2019, 42. [Google Scholar] [CrossRef]
- Dalmases, M.; Benítez, I.D.; Mas, A.; Garcia-Codina, O.; Medina-Bustos, A.; Escarrabill, J.; Saltó, E.; Buysse, D.J.; Roure, N.; Sánchez-de-la-Torre, M.; et al. Assessing sleep health in a European population: Results of the Catalan Health Survey 2015. PLoS ONE 2018, 13, e0194495. [Google Scholar] [CrossRef]
- Dong, L.; Martinez, A.J.; Buysse, D.J.; Harvey, A.G. A composite measure of sleep health predicts concurrent mental and physical health outcomes in adolescents prone to eveningness. Sleep Health 2019, 5, 166–174. [Google Scholar] [CrossRef]
- Brindle, R.C.; Cribbet, M.R.; Samuelsson, L.B.; Gao, C.; Frank, E.; Krafty, R.T.; Thayer, J.F.; Buysse, D.J.; Hall, M.H. The relationship between childhood trauma and poor sleep health in adulthood. Psychosom. Med. 2018, 80, 200–207. [Google Scholar] [CrossRef]
- Furihata, R.; Hall, M.H.; Stone, K.L.; Ancoli-Israel, S.; Smagula, S.F.; Cauley, J.A.; Kaneita, Y.; Uchiyama, M.; Buysse, D.J. An aggregate measure of sleep health is associated with prevalent and incident clinically significant depression symptoms among community-dwelling older women. Sleep 2017, 40. [Google Scholar] [CrossRef]
- Drummond, S.P.; Bischoff-Grethe, A.; Dinges, D.F.; Ayalon, L.; Mednick, S.C.; Meloy, M.J. The neural basis of the psychomotor vigilance task. Sleep 2005, 28, 1059–1068. [Google Scholar]
- Philip, P.; Sagaspe, P.; Lagarde, E.; Leger, D.; Ohayon, M.M.; Bioulac, B.; Boussuge, J.; Taillard, J. Sleep disorders and accidental risk in a large group of regular registered highway drivers. Sleep Med. 2010, 11, 973–979. [Google Scholar] [CrossRef]
- Swanson, L.M.; Arnedt, J.T.; Rosekind, M.R.; Belenky, G.; Balkin, T.J.; Drake, C. Sleep disorders and work performance: Findings from the 2008 National Sleep Foundation Sleep in America poll. J. Sleep Res. 2011, 20, 487–494. [Google Scholar] [CrossRef] [PubMed]
- Sunwoo, J.S.; Hwangbo, Y.; Kim, W.J.; Chu, M.K.; Yun, C.H.; Yang, K.I. Sleep characteristics associated with drowsy driving. Sleep Med. 2017, 40, 4–10. [Google Scholar] [CrossRef]
- Powell, N.B.; Schechtman, K.B.; Riley, R.W.; Guilleminault, C.; Chiang, R.P.; Weaver, E.M. Sleepy driver near-misses may predict accident risks. Sleep 2007, 30, 331–342. [Google Scholar] [CrossRef] [PubMed]
- Toyoshima, K.; Inoue, T.; Shimura, A.; Uchida, Y.; Masuya, J.; Fujimura, Y.; Higashi, S.; Kusumi, I. Mediating roles of cognitive complaints on relationships between insomnia, state anxiety, and presenteeism in Japanese adult workers. Int. J. Env. Res. Public Health 2021, 18, 4516. [Google Scholar] [CrossRef]
- Bistricky, S.L.; Walther, C.; Balderas, J.; Prudon, J.; Ward, C.P.; Ingram, R.E.; Atchley, R.A. Dysfunctional sleep insufficiency and reduced P3 attentional response to positive social information. Sleep Biol. Rhythm. 2021. [Google Scholar] [CrossRef]
- Lallukka, T.; Sivertsen, B.; Kronholm, E.; Bin, Y.S.; Øverland, S.; Glozier, N. Association of sleep duration and sleep quality with the physical, social, and emotional functioning among Australian adults. Sleep Health 2018, 4, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Tavernier, R.; Willoughby, T. Bidirectional associations between sleep (quality and duration) and psychosocial functioning across the university years. Dev. Psychol. 2014, 50, 674–682. [Google Scholar] [CrossRef] [PubMed]
- Dorrian, J.; Centofanti, S.; Smith, A.; McDermott, K.D. Chapter 4—Self-regulation and social behavior during sleep deprivation. In Progress in Brain Research; Van Dongen, H.P.A., Whitney, P., Hinson, J.M., Honn, K.A., Chee, M.W.L., Eds.; Elsevier: Amsterdam, The Netherlands, 2019; Volume 246, pp. 73–110. [Google Scholar]
- Ko, P.R.; Kientz, J.A.; Choe, E.K.; Kay, M.; Landis, C.A.; Watson, N.F. Consumer sleep technologies: A review of the landscape. J. Clin. Sleep Med. 2015, 11, 1455–1461. [Google Scholar] [CrossRef]
- Cardon, J.H.; Eide, E.R.; Phillips, K.L.; Showalter, M.H. A model of sleep, leisure and work over the business cycle. J. Econ. Dyn. Control 2018, 95, 19–36. [Google Scholar] [CrossRef]
- Léger, D.; Bayon, V. Societal costs of insomnia. Sleep Med. Rev. 2010, 14, 379–389. [Google Scholar] [CrossRef]
- Hillman, D.; Mitchell, S.; Streatfeild, J.; Burns, C.; Bruck, D.; Pezzullo, L. The economic cost of inadequate sleep. Sleep 2018, 41. [Google Scholar] [CrossRef]
- Daley, M.; Morin, C.M.; LeBlanc, M.; Grégoire, J.P.; Savard, J. The economic burden of insomnia: Direct and indirect costs for individuals with insomnia syndrome, insomnia symptoms, and good sleepers. Sleep 2009, 32, 55–64. [Google Scholar] [PubMed]
- Craig, B.M.; Reeve, B.B.; Brown, P.M.; Cella, D.; Hays, R.D.; Lipscomb, J.; Simon Pickard, A.; Revicki, D.A. US valuation of health outcomes measured using the PROMIS-29. Value Health 2014, 17, 846–853. [Google Scholar] [CrossRef] [PubMed]
- Council, B.S. Survey: Americans Don’t Value Sleep. Available online: https://bettersleep.org/research/survey-americans-dont-value-sleep/ (accessed on 14 May 2021).
- Hershner, S.D.; Chervin, R.D. Causes and consequences of sleepiness among college students. Nat. Sci. Sleep 2014, 6, 73–84. [Google Scholar] [CrossRef]
- Okano, K.; Kaczmarzyk, J.R.; Dave, N.; Gabrieli, J.D.E.; Grossman, J.C. Sleep quality, duration, and consistency are associated with better academic performance in college students. NPJ Sci. Learn 2019, 4, 16. [Google Scholar] [CrossRef] [PubMed]
- Mohammadbeigi, A.; Absari, R.; Valizadeh, F.; Saadati, M.; Sharifimoghadam, S.; Ahmadi, A.; Mokhtari, M.; Ansari, H. Sleep quality in medical students; the impact of over-use of mobile cell-phone and social networks. J. Res. Health Sci. 2016, 16, 46–50. [Google Scholar]
- Taylor, D.J.; Bramoweth, A.D. Patterns and consequences of inadequate sleep in college students: Substance use and motor vehicle accidents. J. Adolesc. Health 2010, 46, 610–612. [Google Scholar] [CrossRef]
- Gloger, E.M.; Suhr, J.A. Correlates of poor sleep and subsequent risk of misdiagnosis in college students presenting with cognitive complaints. Arch. Clin. Neuropsychol. 2020, 35, 692. [Google Scholar] [CrossRef]
- Becker, S.P.; Jarrett, M.A.; Luebbe, A.M.; Garner, A.A.; Burns, G.L.; Kofler, M.J. Sleep in a large, multi-university sample of college students: Sleep problem prevalence, sex differences, and mental health correlates. Sleep Health 2018, 4, 174–181. [Google Scholar] [CrossRef]
- Orzech, K.M.; Salafsky, D.B.; Hamilton, L.A. The state of sleep among college students at a large public university. J. Am. Coll. Health 2011, 59, 612–619. [Google Scholar] [CrossRef] [PubMed]
- Valerio, T.D.; Kim, M.J.; Sexton-Radek, K. Association of stress, general health, and alcohol use with poor sleep quality among U.S. college students. Am. J. Health Educ. 2016, 47, 17–23. [Google Scholar] [CrossRef]
- Taylor, D.J.; Bramoweth, A.D.; Grieser, E.A.; Tatum, J.I.; Roane, B.M. Epidemiology of insomnia in college students: Relationship with mental health, quality of life, and substance use difficulties. Behav. Ther. 2013, 44, 339–348. [Google Scholar] [CrossRef]
- Trockel, M.T.; Barnes, M.D.; Egget, D.L. Health-related variables and academic performance among first-year college students: Implications for sleep and other behaviors. J. Am. Coll. Health 2000, 49, 125–131. [Google Scholar] [CrossRef] [PubMed]
- Ge, Y.; Xin, S.; Luan, D.; Zou, Z.; Liu, M.; Bai, X.; Gao, Q. Association of physical activity, sedentary time, and sleep duration on the health-related quality of life of college students in Northeast China. Health Qual. Life Outcomes 2019, 17, 124. [Google Scholar] [CrossRef]
- Huckins, J.F.; DaSilva, A.W.; Wang, W.; Hedlund, E.; Rogers, C.; Nepal, S.K.; Wu, J.; Obuchi, M.; Murphy, E.I.; Meyer, M.L.; et al. Mental health and behavior of college students during the early phases of the COVID-19 pandemic: Longitudinal smartphone and ecological momentary assessment study. J. Med. Internet Res. 2020, 22, e20185. [Google Scholar] [CrossRef]
- Son, C.; Hegde, S.; Smith, A.; Wang, X.; Sasangohar, F. Effects of COVID-19 on college students’ mental health in the United States: Interview survey study. J. Med. Internet Res. 2020, 22, e21279. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhang, H.; Ma, X.; Di, Q. Mental health problems during the COVID-19 pandemics and the mitigation effects of exercise: A longitudinal study of college students in China. Int. J. Env. Res. Public Health 2020, 17, 3722. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds, C.F., 3rd; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Carpenter, J.S.; Andrykowski, M.A. Psychometric evaluation of the Pittsburgh Sleep Quality Index. J. Psychosom. Res. 1998, 45, 5–13. [Google Scholar] [CrossRef]
- Johns, M.W. A new method for measuring daytime sleepiness: The Epworth sleepiness scale. Sleep 1991, 14, 540–545. [Google Scholar] [CrossRef]
- Akerstedt, T.; Gillberg, M. Subjective and objective sleepiness in the active individual. Int. J. Neurosci. 1990, 52, 29–37. [Google Scholar] [CrossRef]
- Johns, M.W. Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep 1992, 15, 376–381. [Google Scholar] [CrossRef]
- Beaudreau, S.A.; Spira, A.P.; Stewart, A.; Kezirian, E.J.; Lui, L.Y.; Ensrud, K.; Redline, S.; Ancoli-Israel, S.; Stone, K.L. Validation of the Pittsburgh Sleep Quality Index and the Epworth Sleepiness Scale in older black and white women. Sleep Med. 2012, 13, 36–42. [Google Scholar] [CrossRef]
- Kaida, K.; Takahashi, M.; Akerstedt, T.; Nakata, A.; Otsuka, Y.; Haratani, T.; Fukasawa, K. Validation of the Karolinska sleepiness scale against performance and EEG variables. Clin. Neurophysiol. 2006, 117, 1574–1581. [Google Scholar] [CrossRef]
- McGee, D.L.; Liao, Y.; Cao, G.; Cooper, R.S. Self-reported health status and mortality in a multiethnic US cohort. Am. J. Epidemiol. 1999, 149, 41–46. [Google Scholar] [CrossRef]
- Miilunpalo, S.; Vuori, I.; Oja, P.; Pasanen, M.; Urponen, H. Self-rated health status as a health measure: The predictive value of self-reported health status on the use of physician services and on mortality in the working-age population. J. Clin. Epidemiol. 1997, 50, 517–528. [Google Scholar] [CrossRef]
- Mawani, F.N.; Gilmour, H. Validation of self-rated mental health. Health Rep. 2010, 21, 61–75. [Google Scholar] [PubMed]
- Teresi, J.A.; Ocepek-Welikson, K.; Kleinman, M.; Ramirez, M.; Kim, G. Measurement equivalence of the Patient Reported Outcomes Measurement Information System® (PROMIS®) Anxiety short forms in ethnically diverse groups. Psychol. Test Assess Model. 2016, 58, 183–219. [Google Scholar] [PubMed]
- Radloff, L.S. The CES-D scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Schoemann, A.M.; Boulton, A.J.; Short, S.D. Determining power and sample size for simple and complex mediation models. Soc. Psychol. Personal. Sci. 2017, 8, 379–386. [Google Scholar] [CrossRef]
- Council, B.S. Survey: Starving for Sleep. Available online: https://bettersleep.org/research/survey-starving-for-sleep/ (accessed on 14 May 2021).
- Morin, C.M.; Stone, J.; Trinkle, D.; Mercer, J.; Remsberg, S. Dysfunctional beliefs and attitudes about sleep among older adults with and without insomnia complaints. Psychol. Aging 1993, 8, 463–467. [Google Scholar] [CrossRef]
- Espie, C.A.; Inglis, S.J.; Harvey, L.; Tessier, S. Insomniacs’ attributions. psychometric properties of the Dysfunctional Beliefs and Attitudes about Sleep Scale and the Sleep Disturbance Questionnaire. J. Psychosom. Res. 2000, 48, 141–148. [Google Scholar] [CrossRef]
- Harvey, A.G. A cognitive model of insomnia. Behav. Res. Ther. 2002, 40, 869–893. [Google Scholar] [CrossRef]
- Yang, C.M.; Hung, C.Y.; Lee, H.C. Stress-related sleep vulnerability and maladaptive sleep beliefs predict insomnia at long-term follow-up. J. Clin. Sleep Med. 2014, 10, 997–1001. [Google Scholar] [CrossRef][Green Version]
- Crönlein, T.; Wagner, S.; Langguth, B.; Geisler, P.; Eichhammer, P.; Wetter, T.C. Are dysfunctional attitudes and beliefs about sleep unique to primary insomnia? Sleep Med. 2014, 15, 1463–1467. [Google Scholar] [CrossRef]
- Janati Idrissi, A.; Lamkaddem, A.; Benouajjit, A.; Ben El Bouaazzaoui, M.; El Houari, F.; Alami, M.; Labyad, S.; Chahidi, A.; Benjelloun, M.; Rabhi, S.; et al. Sleep quality and mental health in the context of COVID-19 pandemic and lockdown in Morocco. Sleep Med. 2020, 74, 248–253. [Google Scholar] [CrossRef] [PubMed]
- Zhou, J.; Jin, L.R.; Tao, M.J.; Peng, H.; Ding, S.S.; Yuan, H. The underlying characteristics of sleep behavior and its relationship to sleep-related cognitions: A latent class analysis of college students in Wuhu city, China. Psychol. Health Med. 2020, 25, 887–897. [Google Scholar] [CrossRef]
- Jin, L.; Zhou, J.; Peng, H.; Ding, S.; Yuan, H. Investigation on dysfunctional beliefs and attitudes about sleep in Chinese college students. Neuropsychiatr. Dis. Treat. 2018, 14, 1425–1432. [Google Scholar] [CrossRef] [PubMed]
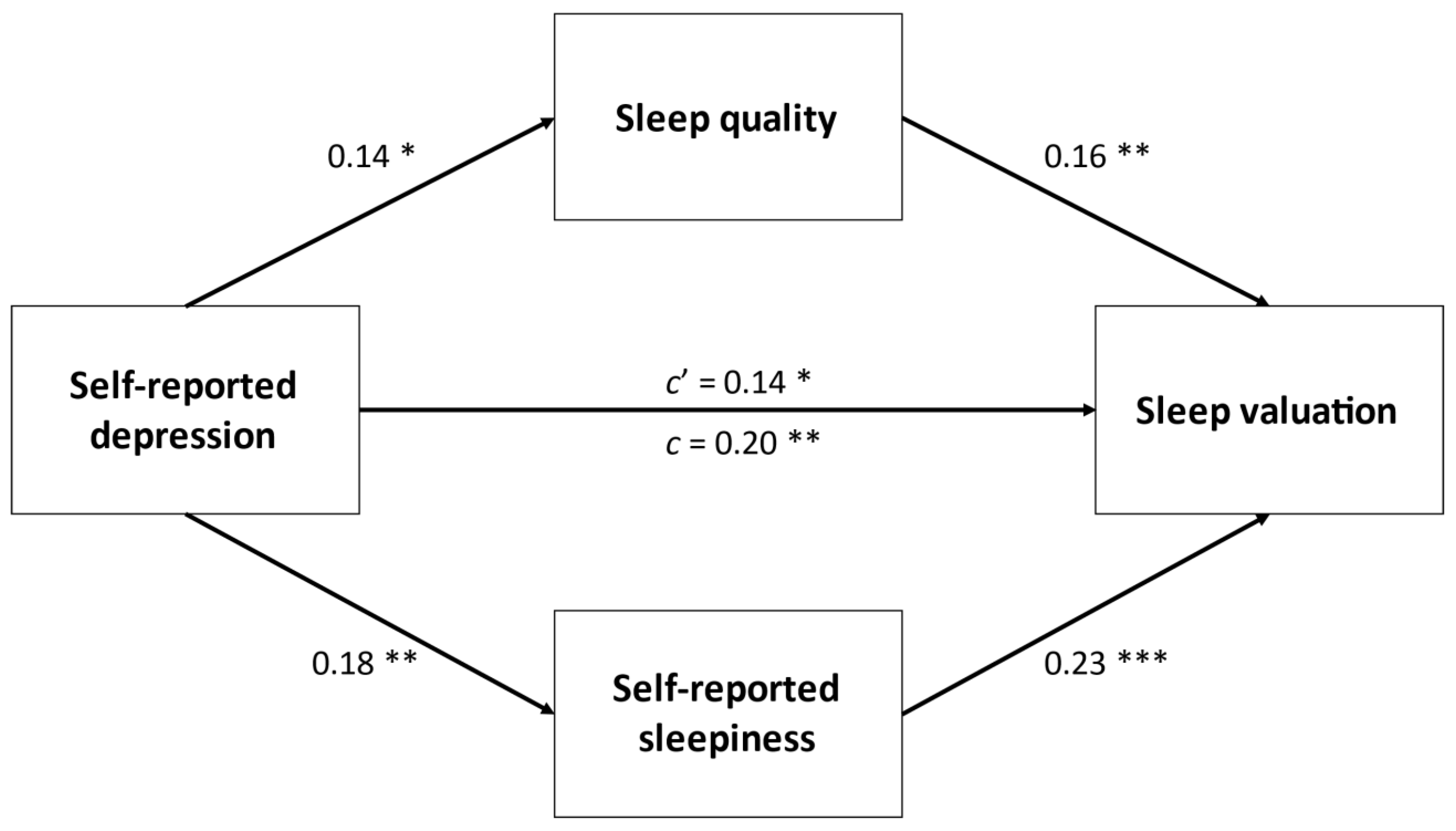
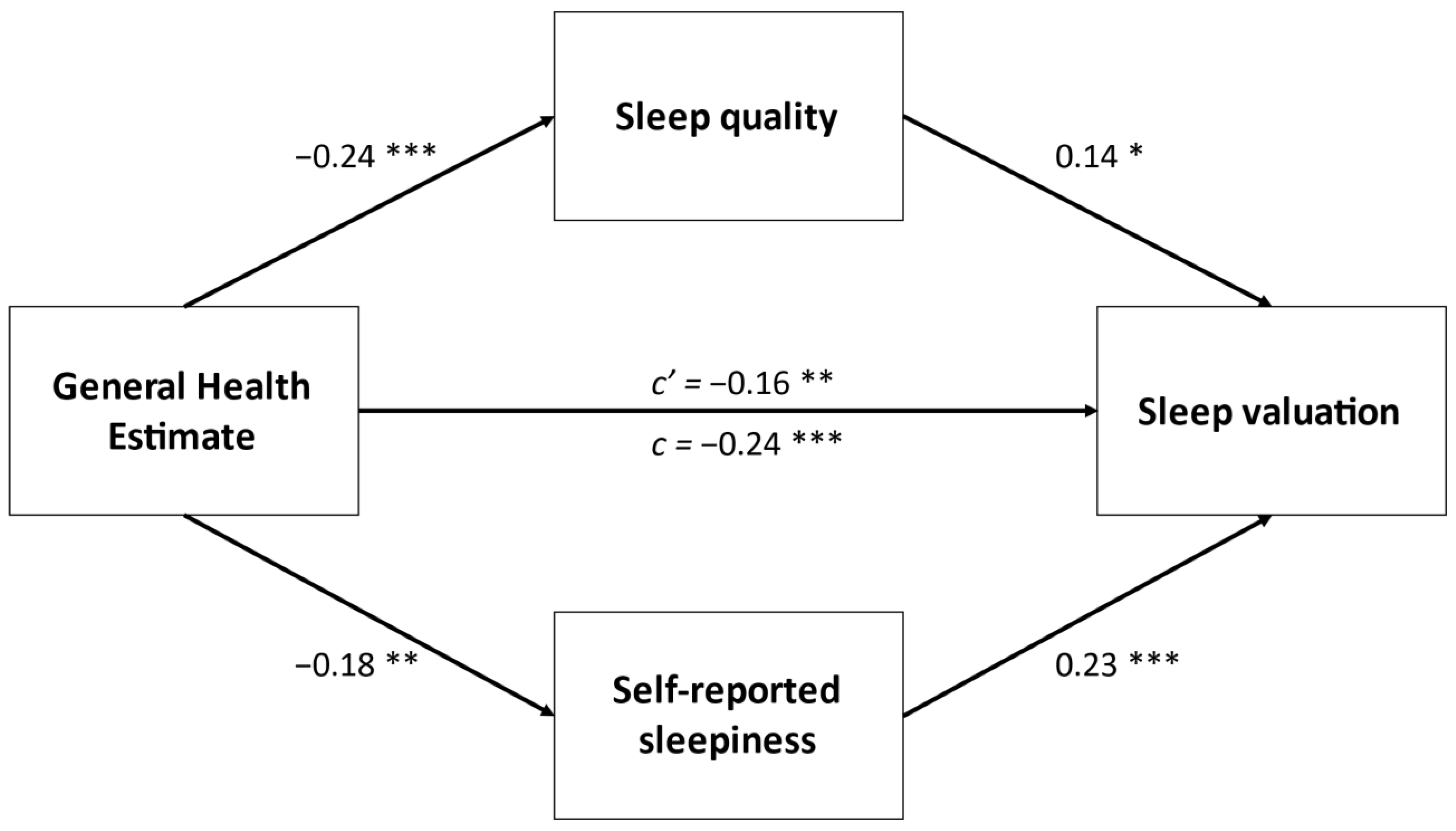
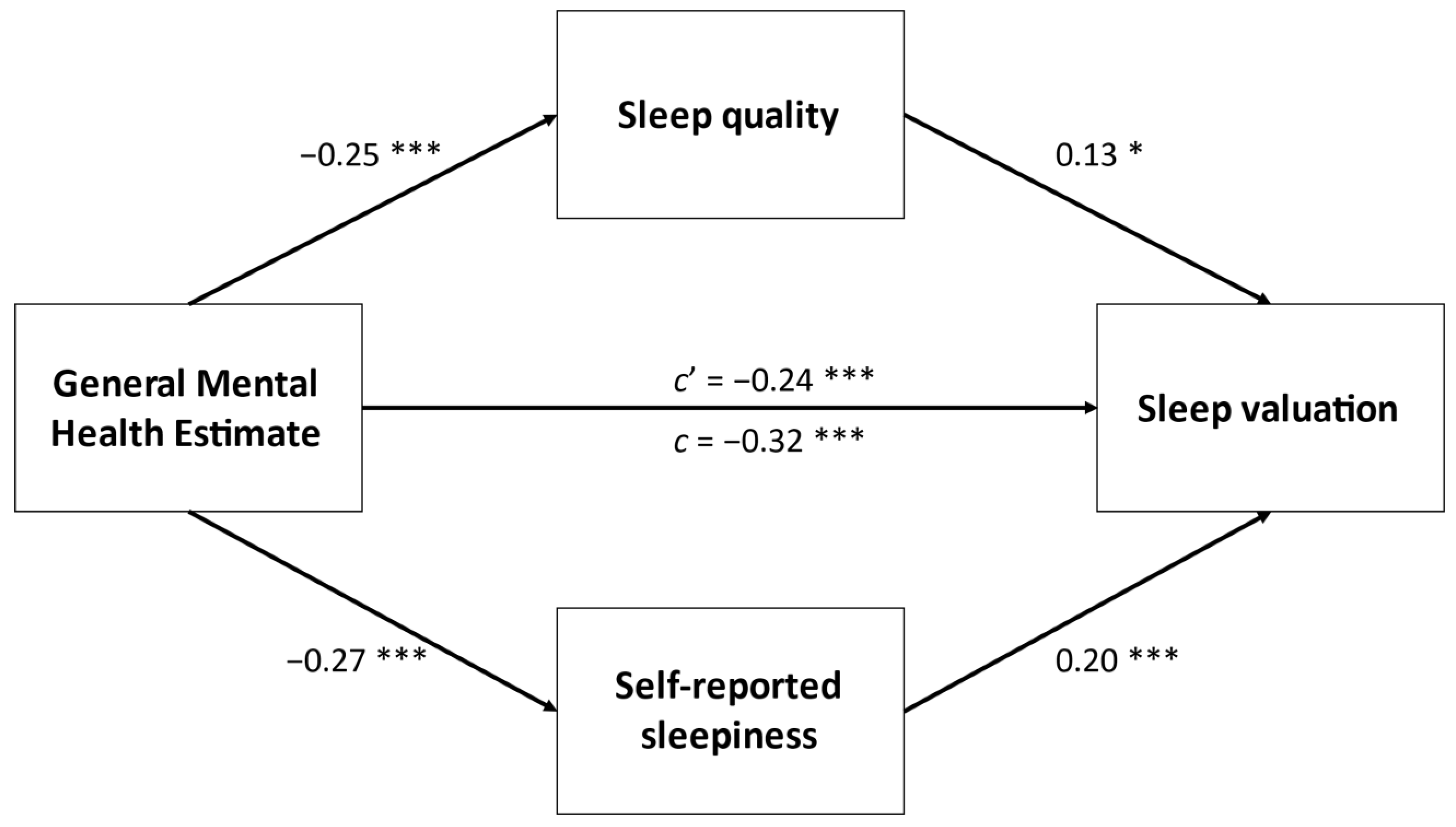
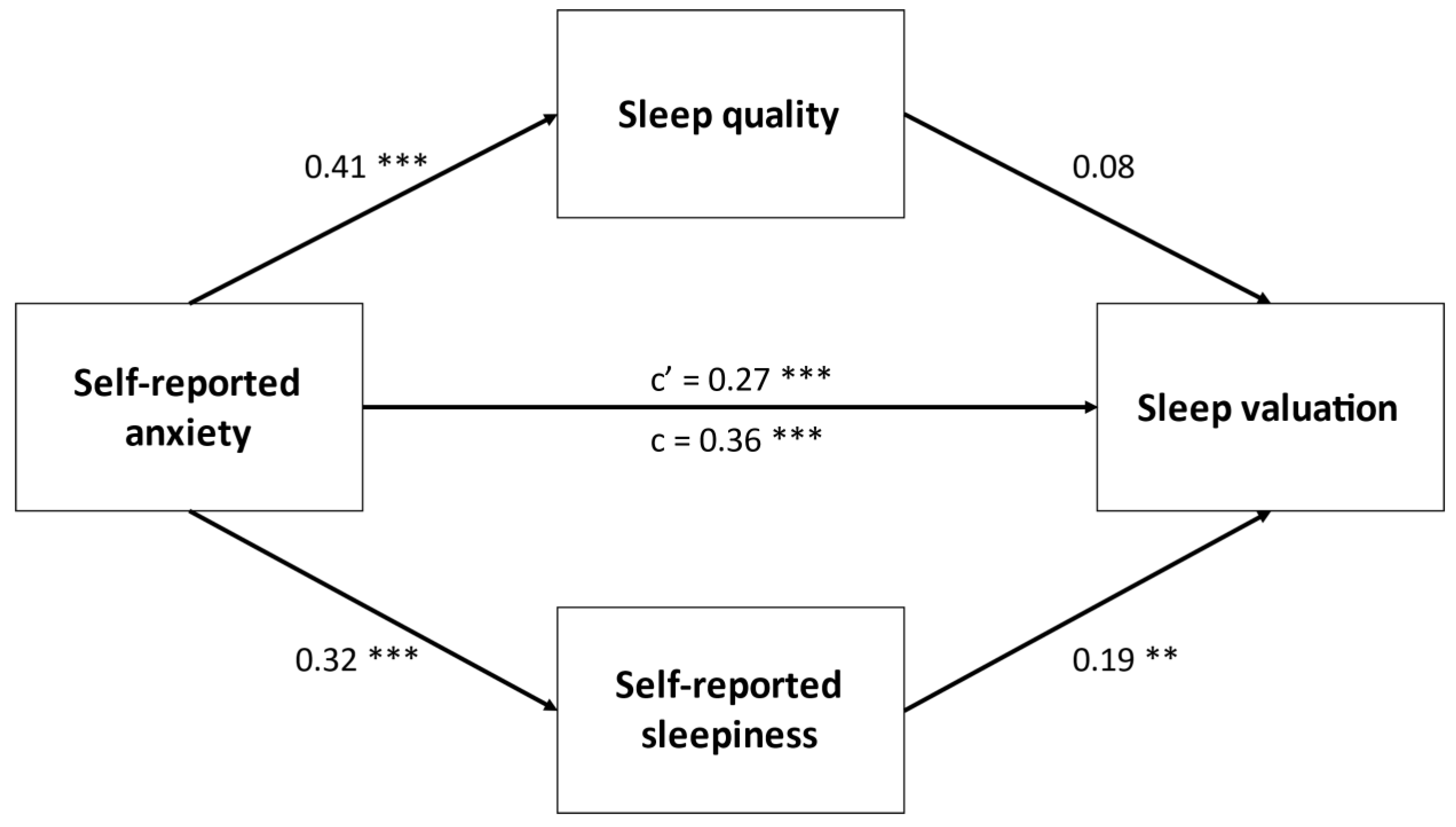
| Age, y | 19 (1) |
| Gender | |
| Male | 43 (17%) |
| Female | 203 (82%) |
| Other | 1 (<1%) |
| Race | |
| White | 209 (85%) |
| Black/African American | 17 (7%) |
| Asian/Asian American | 4 (2%) |
| Hispanic/Latino | 5 (2%) |
| Mixed race | 12 (5%) |
| Marital Status | |
| Married | 1 (<1%) |
| Never married | 238 (96%) |
| Cohabitating | 8 (3%) |
| Education | |
| Graduated high school | 115 (47%) |
| Graduated high school equivalent | 21 (9%) |
| Some college | 107 (43%) |
| Graduated 2-year college | 1 (<1%) |
| Graduated 4-year college | 3 (1%) |
| Household Income | |
| <$10,000 | 17 (7%) |
| $10,000-$40,000 | 15 (6%) |
| $40,001–$90,000 | 55 (22%) |
| $90,001–$190,000 | 98 (40%) |
| >$190,000 | 61 (25%) |
| # | Item | Mean | SD | Range | Reverse Scored | Skewness | Kurtosis | α | Item-Total Correlation |
|---|---|---|---|---|---|---|---|---|---|
| 1 | I generally desire more sleep | 80.17 | 18.39 | 19–100 | −0.89 | 3.50 | 0.89 | 0.51 | |
| 2 | When I have nothing to do, I would prefer to sleep | 60.06 | 28.30 | 0–100 | −0.28 | 2.07 | 0.89 | 0.74 | |
| 3 | I put off going to sleep at night, even when I am sleepy | 51.42 | 30.24 | 0–100 | Yes | −0.02 | 1.82 | 0.89 | 0.06 |
| 4 | I generally prefer to sleep in | 75.70 | 25.69 | 0–100 | −1.07 | 3.34 | 0.89 | 0.44 | |
| 5 | When I wake up in the morning or my alarm goes off, I generally try to go back to sleep | 61.23 | 29.74 | 0–100 | −0.43 | 2.07 | 0.89 | 0.36 | |
| 6 | If I had to choose between sleep in a little longer or eating breakfast, I would choose to sleep in | 73.72 | 30.44 | 0–100 | −1.08 | 3.01 | 0.89 | 0.40 | |
| 7 | I try to sleep as much as I can | 73.11 | 23.67 | 2–100 | −0.75 | 2.87 | 0.89 | 0.55 | |
| 8 | I take every opportunity I can to sleep | 53.59 | 30.22 | 0–100 | 0.07 | 1.86 | 0.89 | 0.72 | |
| 9 | I would rather stay asleep than wake up | 63.45 | 28.62 | 0–100 | −0.44 | 2.18 | 0.89 | 0.65 | |
| 10 | I would rather get in bed to sleep at night than stay up to do household tasks | 66.75 | 26.28 | 0–100 | −0.40 | 2.25 | 0.89 | 0.66 | |
| 11 | I would rather get in bed to sleep at night than stay up later to do my hobbies | 51.77 | 27.06 | 0–100 | 0.05 | 2.20 | 0.89 | 0.67 | |
| 12 | I would rather get in bed to sleep at night than stay up to engage in social activities | 43.58 | 28.66 | 0–100 | 0.41 | 2.22 | 0.89 | 0.60 | |
| 13 | I avoid doing things that might disrupt my sleep | 49.41 | 25.13 | 0–100 | 0.20 | 2.35 | 0.89 | 0.48 | |
| 14 | Sleep is less pleasant than being awake | 65.07 | 22.53 | 0–100 | Yes | −0.32 | 2.92 | 0.89 | 0.41 |
| 15 | I want to sleep more even when I feel rested | 46.36 | 27.39 | 0–100 | 0.28 | 2.21 | 0.89 | 0.61 | |
| 16 | When I’m sleep, I would rather surf the web, watch a movie, engage in social media, or play a video game than go to sleep | 50.56 | 27.45 | 0–100 | Yes | 0.08 | 2.10 | 0.90 | 0.11 |
| 17* | I want to sleep because I don’t like being awake | 26.14 | 26.77 | 0–100 | 0.91 | 2.77 | 0.89 | 0.48 | |
| 18 | I would want to sleep more if my sleep were more restful | 49.45 | 25.84 | 0–100 | −0.04 | 2.44 | 0.89 | 0.18 | |
| 19 | I want to sleep more because I enjoy it so much | 55.96 | 25.14 | 0–100 | −0.08 | 2.53 | 0.89 | 0.72 | |
| 20 | When I feel sleepy at night, I try to go to sleep | 71.60 | 22.89 | 2–100 | −0.70 | 2.88 | 0.89 | 0.25 | |
| 21 | When I feel sleepy at night, I push through it so I can stay awake longer | 56.59 | 25.90 | 0–100 | Yes | −0.20 | 2.17 | 0.90 | 0.21 |
| 22 | I don’t mind feeling sleepy during the day | 70.74 | 24.46 | 0–100 | Yes | −0.70 | 2.63 | 0.90 | 0.07 |
| 23 | I want to sleep more because I feel sleepy | 67.80 | 24.44 | 0–100 | −0.84 | 3.37 | 0.89 | 0.60 | |
| 24 | I would rather sleep an extra hour than work an extra hour at my current rate of pay (or if not currently employed, I would rather sleep an extra hour than work an extra hour at minimum wage) | 54.57 | 30.63 | 0–100 | −0.19 | 2.00 | 0.89 | 0.49 | |
| 25 | I would rather sleep an extra hour than spend an extra hour doing the things I enjoy | 37.90 | 25.45 | 0–100 | 0.42 | 2.69 | 0.89 | 0.59 | |
| 26 | I want to sleep even when I am not sleepy | 39.52 | 27.68 | 0–100 | 0.41 | 2.37 | 0.89 | 0.65 | |
| 27 | I want to sleep more because I am not getting enough restful sleep | 57.83 | 27.36 | 0–100 | −0.30 | 2.32 | 0.89 | 0.40 | |
| 28 | If I can’t sleep, I would rather take a sleep aid than remain awake | 51.28 | 32.71 | 0–100 | −0.15 | 1.75 | 0.89 | 0.45 | |
| 29 | I wish I could sleep less | 67.89 | 25.88 | 0–100 | Yes | −0.57 | 2.46 | 0.90 | 0.12 |
| 30 * | I dread waking up in the morning | 59.69 | 29.63 | 0–100 | −0.46 | 2.23 | 0.89 | 0.51 | |
| 31 | I dread going to sleep at night | 75.94 | 23.03 | 1–100 | Yes | −0.69 | 2.50 | 0.89 | 0.10 |
| 32 * | I want to sleep my life away | 24.17 | 28.02 | 0–100 | 1.17 | 3.33 | 0.89 | 0.55 | |
| 33 | If I could function without sleep, I would sleep less than I do | 46.36 | 31.45 | 0–100 | Yes | 0.13 | 1.85 | 0.90 | 0.15 |
| 34 | I’m likely to wake up earlier than usual to do something I look forward to | 28.81 | 25.48 | 0–100 | Yes | 1.04 | 3.45 | 0.89 | 0.30 |
| 35 | I look forward to going to sleep | 72.05 | 20.61 | 0–100 | −0.44 | 2.93 | 0.89 | 0.66 | |
| 36 | I schedule my day around my sleep | 33.43 | 26.72 | 0–100 | 0.64 | 2.66 | 0.89 | 0.51 | |
| 37 | I modify my daytime activities to accommodate my sleep | 36.41 | 27.50 | 0–100 | 0.37 | 2.15 | 0.89 | 0.50 | |
| 38 | I keep track of how much sleep I’ve lost and how much sleep I hope to make up later | 33.90 | 28.95 | 0–100 | 0.63 | 2.40 | 0.89 | 0.27 | |
| 39 | If I lose sleep on one night, I try to make it up by napping or sleep more another night | 56.43 | 29.22 | 0–100 | −0.53 | 2.20 | 0.89 | 0.44 | |
| 40 | If I need more sleep, I am likely to sleep in even if that means I will be late | 30.17 | 29.20 | 0–100 | 0.70 | 2.36 | 0.89 | 0.40 | |
| 41 | I enjoy sleeping | 82.12 | 18.02 | 4–100 | −0.95 | 3.83 | 0.89 | 0.61 | |
| 42 | I feel that sleep is a waste of time | 72.19 | 25.66 | 0–100 | Yes | −0.65 | 2.45 | 0.89 | 0.34 |
| 43 | I try to catch up on sleep on days off | 72.00 | 22.72 | 0–100 | −0.92 | 3.76 | 0.89 | 0.52 |
| Measure | Correlation | β | t | 95% CI | p |
|---|---|---|---|---|---|
| General Health Estimate | −0.24 *** | −6.18 | −3.12 | −10.07–−2.28 | 0.002 ** |
| General Mental Health Estimate | −0.32 *** | −5.40 | −4.54 | −7.74–−3.06 | <0.001 *** |
| Karolinska Sleepiness Scale (KSS) | 0.30 *** | 55.27 | 3.86 | 27.02–83.51 | <0.001 *** |
| Pittsburgh Sleep Quality Index (PSQI) | 0.35 *** | 40.08 | 5.37 | 25.39–54.78 | <0.001 *** |
| Center for Epidemiologic Studies Depression Scale (CES-D) | 0.20 ** | 7.50 | 2.50 | 1.58–13.42 | 0.013 * |
| PROMIS Emotional Distress–Anxiety | 0.36 *** | 16.86 | 5.19 | 10.46–23.27 | <0.001 *** |
| Overall sleep quality (PSQI item 6) | 0.24 *** | 133.83 | 3.42 | 56.69–210.97 | 0.001 ** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nielson, S.A.; Taylor, J.; Simmons, Z.; Decker, A.N.; Kay, D.B.; Cribbet, M.R. Sleep Valuation Is Associated with Components of Sleep Health and Daytime Functioning in a College Sample: A Survey Study. Int. J. Environ. Res. Public Health 2021, 18, 5644. https://doi.org/10.3390/ijerph18115644
Nielson SA, Taylor J, Simmons Z, Decker AN, Kay DB, Cribbet MR. Sleep Valuation Is Associated with Components of Sleep Health and Daytime Functioning in a College Sample: A Survey Study. International Journal of Environmental Research and Public Health. 2021; 18(11):5644. https://doi.org/10.3390/ijerph18115644
Chicago/Turabian StyleNielson, Spencer A., Jordan Taylor, Zach Simmons, Andrea N. Decker, Daniel B. Kay, and Matthew R. Cribbet. 2021. "Sleep Valuation Is Associated with Components of Sleep Health and Daytime Functioning in a College Sample: A Survey Study" International Journal of Environmental Research and Public Health 18, no. 11: 5644. https://doi.org/10.3390/ijerph18115644
APA StyleNielson, S. A., Taylor, J., Simmons, Z., Decker, A. N., Kay, D. B., & Cribbet, M. R. (2021). Sleep Valuation Is Associated with Components of Sleep Health and Daytime Functioning in a College Sample: A Survey Study. International Journal of Environmental Research and Public Health, 18(11), 5644. https://doi.org/10.3390/ijerph18115644






