Regular Doses of Nature: The Efficacy of Green Exercise Interventions for Mental Wellbeing
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Projects
2.2. Design, Measures and Data Processing
2.3. Categorising Wellbeing Scores
2.4. Creating a Single Variable for Analyses
2.5. Statistical Analysis
3. Results
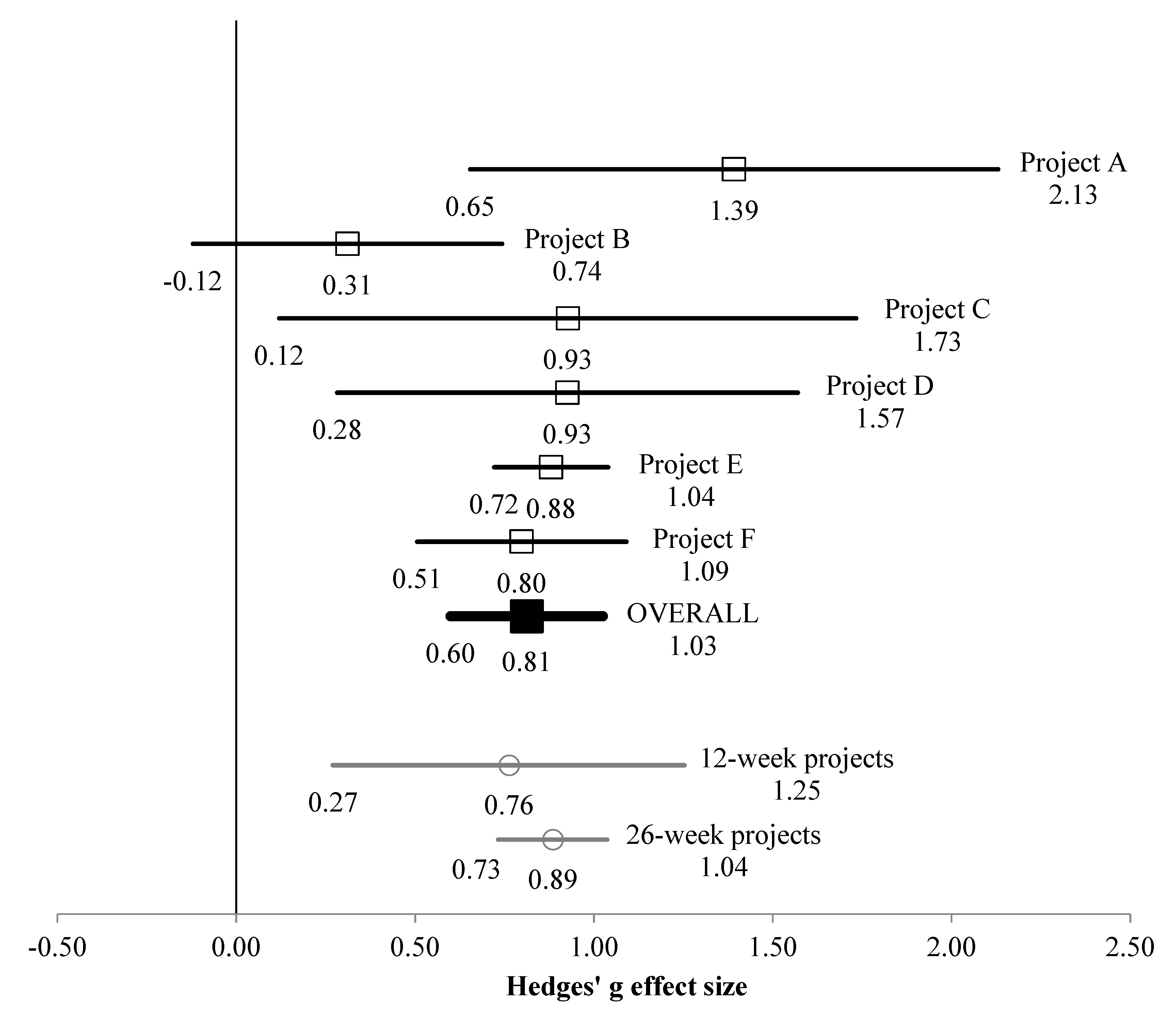
3.1. Whole Sample
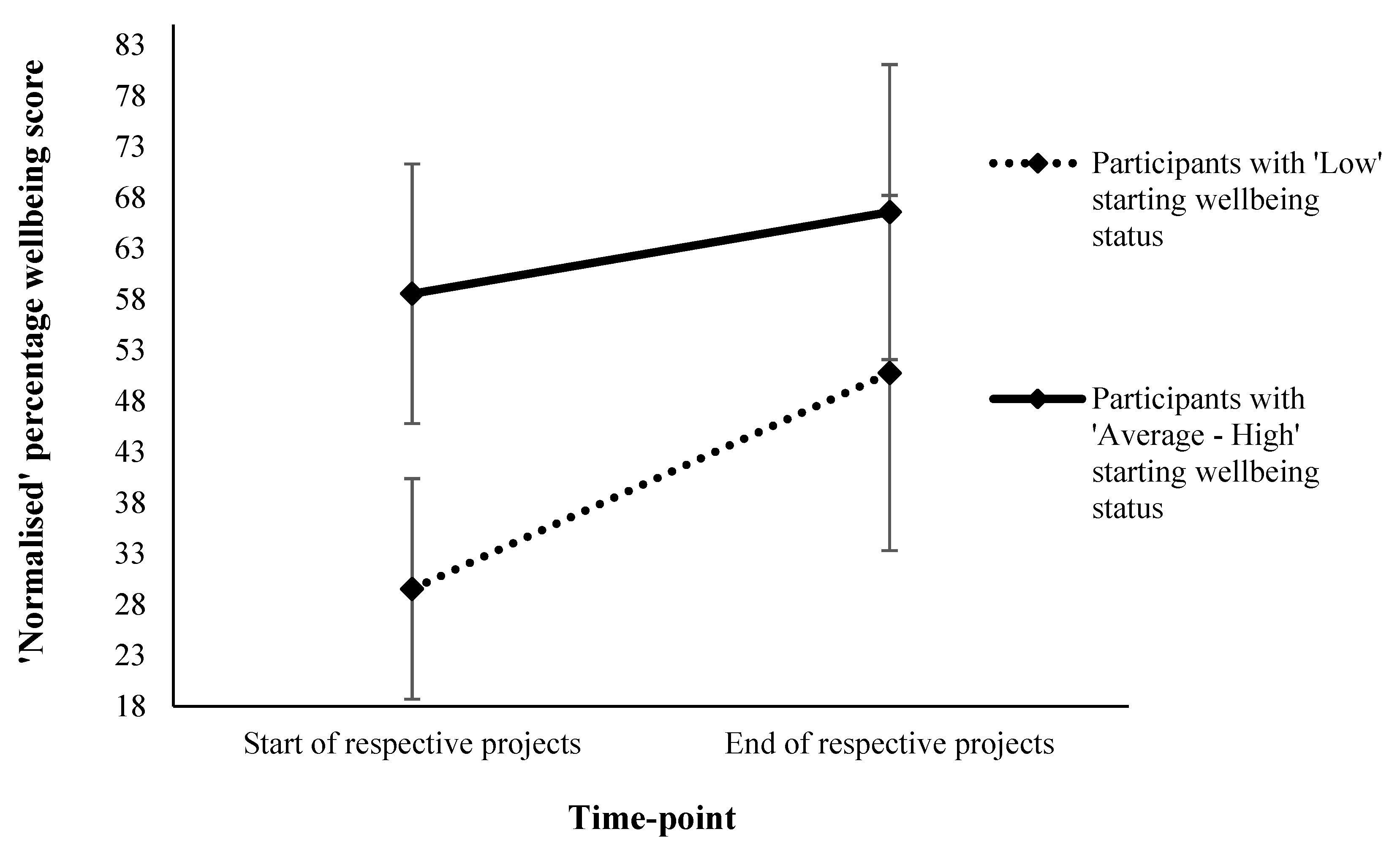
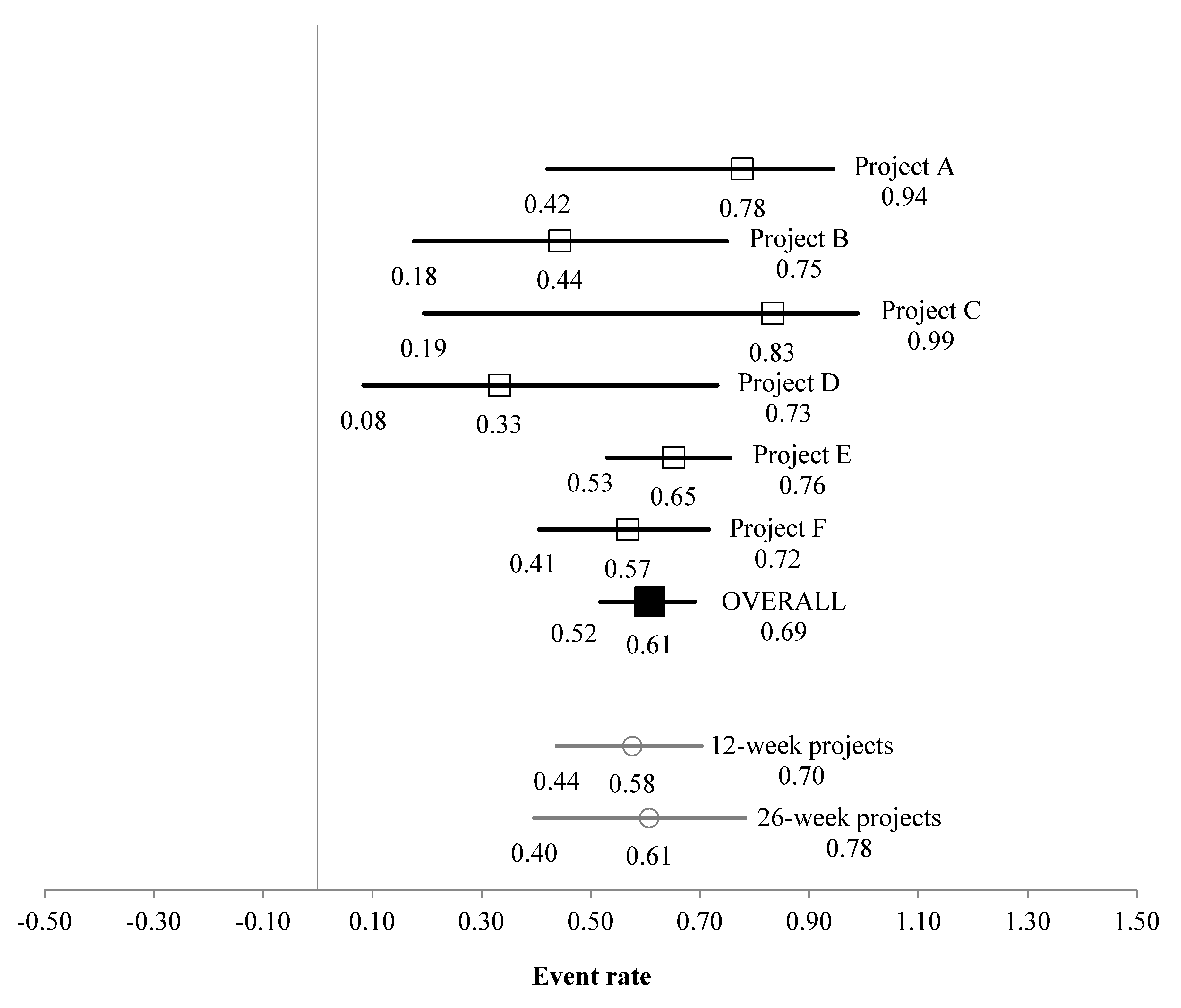
3.2. Low Wellbeing Subsample
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pretty, J.; Peacock, J.; Sellens, M.; Griffin, M. The mental and physical health outcomes of green exercise. Int. J. Environ. Health Res. 2005, 15, 319–337. [Google Scholar] [CrossRef]
- Barton, J.; Pretty, J. What is the best dose of nature and green exercise for improving mental health? A multi-study analysis. Environ. Sci. Technol. 2010, 44, 3947–3955. [Google Scholar] [CrossRef]
- Barton, J.; Bragg, R.; Wood, C.; Pretty, J. Green Exercise: Linking Nature, Health and Well-Being; Routledge: Abingdon, UK, 2016. [Google Scholar]
- Rogerson, M.; Brown, D.K.; Sandercock, G.; Wooller, J.J.; Barton, J. A comparison of four typical green exercise environments and prediction of psychological health outcomes. Perspect. Public Health 2015, 136, 171–180. [Google Scholar] [CrossRef] [PubMed]
- Thompson Coon, J.; Boddy, K.; Stein, K.; Whear, R.; Barton, J.; Depledge, M.H. Does participating in physical activity in outdoor natural environments have a greater effect on physical and mental wellbeing than physical activity indoors? A systematic review. Environ. Sci. Technol. 2011, 45, 1761–1772. [Google Scholar] [CrossRef] [PubMed]
- Bowler, D.E.; Buyung-Ali, L.M.; Knight, T.M.; Pullin, A.S. A systematic review of evidence for the added benefits to health of exposure to natural environments. BMC Public Health 2010, 10, 456. [Google Scholar] [CrossRef]
- Wood, C.J.; Pretty, J.; Griffin, M. A case–control study of the health and well-being benefits of allotment gardening. J. Public Health 2015, 38. [Google Scholar] [CrossRef]
- Brown, D.K.; Barton, J.L.; Gladwell, V.F. Viewing nature scenes positively affects recovery of autonomic function following acute-mental stress. Environ. Sci. Technol. 2013, 47, 5562–5569. [Google Scholar] [CrossRef] [PubMed]
- Barton, J.; Bragg, R.; Pretty, J.; Roberts, J.; Wood, C. The wilderness expedition an effective life course intervention to improve young people’s well-being and connectedness to nature. J. Exp. Educ. 2016. [Google Scholar] [CrossRef]
- Norton, C.L.; Tucker, A.; Russell, K.C.; Bettmann, J.E.; Gass, M.A.; Gillis, H.L.; Behrens, E. Adventure therapy with youth. J. Exp. Educ. 2014, 37, 46–59. [Google Scholar] [CrossRef]
- de Bruin, S.R.; Stoop, A.; Molema, C.C.; Vaandrager, L.; Hop, P.J.; Baan, C.A. Green care farms an innovative type of adult day service to stimulate social participation of people with dementia. Gerontol. Geriatr. Med. 2015, 1. [Google Scholar] [CrossRef]
- Vella, E.J.; Milligan, B.; Bennett, J.L. Participation in outdoor recreation program predicts improved psychosocial well-being among veterans with post-traumatic stress disorder: A pilot study. Mil. Med. 2013, 178, 254–260. [Google Scholar] [CrossRef] [PubMed]
- Lamers, S.M.; Bolier, L.; Westerhof, G.J.; Smit, F.; Bohlmeijer, E.T. The impact of emotional well-being on long-term recovery and survival in physical illness: A meta-analysis. J. Behav. Med. 2012, 35, 538–547. [Google Scholar] [CrossRef] [PubMed]
- De Neve, J.E.; Diener, E.; Tay, L.; Xuereb, C. The objective benefits of subjective well-being (6 August 2013). In World Happiness Report 2013; Helliwell, J., Layard, R., Sachs, J., Eds.; UN Sustainable Development Solutions Network: New York, NY, USA, 2013. [Google Scholar]
- Eurofound. European Quality of Life Survey 2016: Quality of Life, Quality of Public Services, and Quality of Society; Publications Office of the European Union: Luxembourg, 2017. [Google Scholar]
- Rogerson, M.; Barton, J.; Pretty, J.; Gladwell, V. The green exercise concept: Two intertwining pathways to health and well-being. In Physical Activity in Natural Settings: Green Exercise and Blue Mind; MacIntyre, T.E., Donnelly, A.A., Eds.; Routledge: Abingdon upon Thames, UK, in press.
- Brymer, E.; Davids, K.; Mallabon, L. Understanding the psychological health and well-being benefits of physical activity in nature: An ecological dynamics analysis. Ecopsychology 2014, 6, 189–197. [Google Scholar]
- Flowers, E.P.; Freeman, P.; Gladwell, V.F. A cross-sectional study examining predictors of visit frequency to local green space and the impact this has on physical activity levels. BMC Public Health 2016, 16, 420. [Google Scholar] [CrossRef] [PubMed]
- McMahan, E.A.; Estes, D. The effect of contact with natural environments on positive and negative affect: A meta-analysis. J. Posit. Psychol. 2015, 10, 507–519. [Google Scholar] [CrossRef]
- Roe, J.; Aspinall, P. The restorative benefits of walking in urban and rural settings in adults with good and poor mental health. Health Place 2011, 17, 103–113. [Google Scholar] [CrossRef]
- Mitchell, R.; Popham, F. Effect of exposure to natural environment on health inequalities: An observational population study. Lancet 2008, 372, 1655–1660. [Google Scholar] [CrossRef]
- Lachowycz, K.; Jones, A. Greenspace and obesity: A systematic review of the evidence. Obes. Rev. 2011, 12, e183–e189. [Google Scholar] [CrossRef]
- Wolch, J.R.; Byrne, J.; Newell, J.P. Urban green space, public health, and environmental justice: The challenge of making cities ‘just green enough’. Landsc. Urban Plan. 2014, 125, 234–244. [Google Scholar] [CrossRef]
- de Vries, S.; van Dillen, S.M.; Groenewegen, P.P.; Spreeuwenberg, P. Streetscape greenery and health: Stress, social cohesion and physical activity as mediators. Soc. Sci. Med. 2013, 94, 26–33. [Google Scholar] [CrossRef]
- van den Berg, M.M.; van Poppel, M.; van Kamp, I.; Ruijsbroek, A.; Triguero-Mas, M.; Gidlow, C.; Nieuwenhuijsen, M.J.; Gražulevičiene, R.; van Mechelen, W.; Kruize, H. Do physical activity, social cohesion, and loneliness mediate the association between time spent visiting green space and mental health? Environ. Behav. 2017. [Google Scholar] [CrossRef] [PubMed]
- McManus, S.; Bebbington, P.; Jenkins, R.; Brugha, T. Mental health and wellbeing in England: Adult psychiatric morbidity survey 2014; NHS Digital: Leeds, UK, 2016. [Google Scholar]
- Tennant, R.; Hiller, L.; Fishwick, R.; Platt, S.; Joseph, S.; Weich, S.; Parkinson, J.; Secker, J.; Stewart-Brown, S. The warwick-edinburgh mental well-being scale (wemwbs): Development and UK validation. Health Qual. Life Outcomes 2007, 5, 63. [Google Scholar] [CrossRef] [PubMed]
- Fat, L.N.; Scholes, S.; Boniface, S.; Mindell, J.; Stewart-Brown, S. Evaluating and establishing national norms for mental wellbeing using the short warwick–edinburgh mental well-being scale (swemwbs): Findings from the health survey for england. Qual. Life Res. 2017, 26, 1129–1144. [Google Scholar] [CrossRef] [PubMed]
- Stewart-Brown, S.; Tennant, A.; Tennant, R.; Platt, S.; Parkinson, J.; Weich, S. Internal construct validity of the warwick-edinburgh mental well-being scale (wemwbs): A rasch analysis using data from the scottish health education population survey. Health Qual. Life Outcomes 2009, 7, 15. [Google Scholar] [CrossRef]
- Deeks, J.; Higgins, J.; Altman, D. Analysing data and undertaking meta-analyses. In Cochrane Handbook for Systematic Reviews of Interventions 5.1.0 [Updated March 2011]; Higgins, J.P.T., Green, S., Eds.; The Cochrane Collaboration: London, UK, 2011. [Google Scholar]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates Inc.: Hillsdale, NJ, USA, 1988; Volume 13. [Google Scholar]
- Hedges, L.V. Distribution theory for glass’s estimator of effect size and related estimators. J. Educ. Stat. 1981, 6, 107–128. [Google Scholar] [CrossRef]
- Hedges, L.V.; Olkin, I. Statistical Methods for Meta-Analysis; Academic Press: San Diego, CA, USA, 1985. [Google Scholar]
- Funder, D.C.; Ozer, D.J. Evaluating effect size in psychological research: Sense and nonsense. Adv. Methods Pract. Psychol. Sci. 2019, 2, 156–168. [Google Scholar] [CrossRef]
- Higgins, J.P.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ Br. Med. J. 2003, 327, 557. [Google Scholar] [CrossRef]
- Soga, M.; Gaston, K.J.; Yamaura, Y. Gardening is beneficial for health: A meta-analysis. Prev. Med. Rep. 2017, 5, 92–99. [Google Scholar] [CrossRef]
- Clatworthy, J.; Hinds, J.; Camic, P.M. Gardening as a mental health intervention: A review. Ment. Health Rev. J. 2013. [Google Scholar] [CrossRef]
- Dodich, A.; Zollo, M.; Crespi, C.; Cappa, S.F.; Laureiro Martinez, D.; Falini, A.; Canessa, N. Short-term sahaja yoga meditation training modulates brain structure and spontaneous activity in the executive control network. Brain Behav. 2018. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, J.; Romero, V.L.; Elkin-Frankston, S.; Bezdek, M.A.; Schumacher, E.H.; Lazar, S.W. Reduced interference in working memory following mindfulness training is associated with increases in hippocampal volume. Brain Imaging Behav. 2018, 13, 1–11. [Google Scholar]
- Christie, M.A.; Cole, F. The impact of green exercise on volunteer’s mental health and wellbeing-findings from a community project in a woodland setting. J. Ther. Hortic. 2017, 27, 16–32. [Google Scholar] [CrossRef]
- Dadvand, P.; Bartoll, X.; Basagaña, X.; Dalmau-Bueno, A.; Martinez, D.; Ambros, A.; Cirach, M.; Triguero-Mas, M.; Gascon, M.; Borrell, C. Green spaces and general health: Roles of mental health status, social support, and physical activity. Environ. Int. 2016, 91, 161–167. [Google Scholar] [CrossRef] [PubMed]
- Lovell, R.; Husk, K.; Cooper, C.; Stahl-Timmins, W.; Garside, R. Understanding how environmental enhancement and conservation activities may benefit health and wellbeing: A systematic review. BMC Public Health 2015, 15, 864. [Google Scholar] [CrossRef] [PubMed]
- Maas, J.; Van Dillen, S.M.; Verheij, R.A.; Groenewegen, P.P. Social contacts as a possible mechanism behind the relation between green space and health. Health Place 2009, 15, 586–595. [Google Scholar] [CrossRef]
| Scale | Project | Sample Size | Mean Raw/Metric-Converted Scores for Respective Scale * | Normalised Percentage Scores | |||
|---|---|---|---|---|---|---|---|
| Start of Intervention | End of Intervention | Start of Intervention | End of Intervention | ||||
| Whole sample | WEMWBS (14–70) | A | 13 | 33.3 ± 12.2 | 46.2 ± 9.0 | 34.5 ± 21.7 | 57.4 ± 16.2 |
| C | 7 | 39.6 ± 12.8 | 57.9 ± 10.1 | 45.7 ± 22.9 | 78.3 ± 18.1 | ||
| D | 12 | 36.0 ± 5.7 | 43.4 ± 6.2 | 39.3 ± 10.2 | 52.5 ± 11.1 | ||
| F | 58 | 35.5 ± 13.1 | 45.6 ± 10.6 | 38.3 ± 23.4 | 56.4 ± 18.8 | ||
| SWEMWBS (7–35) | B | 20 | 19.4 ± 2.7 | 20.5 ± 3.5 | 44.3 ± 9.6 | 48.3 ± 12.6 | |
| E | 208 | 21.2 ± 4.7 | 24.5 ± 4.8 | 50.6 ± 16.6 | 62.4 ± 17.0 | ||
| Low wellbeing subsample | WEMWBS (14–70) | A | 9 | 27.0 ± 6.0 | 43.9 ± 6.6 | 23.2 ± 10.6 | 53.4 ± 11.8 |
| C | 2 | 23.0 ± 1.4 | 61.5 ± 12.0 | 16.1 ± 2.5 | 84.8 ± 21.5 | ||
| D | 6 | 30.8 ± 2.1 | 40.7 ± 7.2 | 30.1 ± 3.8 | 47.6 ± 12.9 | ||
| F | 37 | 27.2 ± 7.1 | 42.2 ± 10.3 | 23.6 ± 12.7 | 50.3 ± 18.3 | ||
| SWEMWBS (7–35) | B | 9 | 16.9 ± 1.3 | 19.1 ± 4.3 | 35.4 ± 4.5 | 43.3 ± 15.3 | |
| E | 66 | 16.3 ± 2.4 | 21.3 ± 4.9 | 33.3 ± 8.6 | 50.9 ± 17.4 | ||
| Test of Null (2-Tailed) | Heterogeneity between Projects/for Respective Moderator | Tau2 | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Z | P | Q | df (Q) | P | I2 | Tau2 | SE | Variance | ||
| Whole sample | Overall (in relation to Hedges g effect size) | 7.463 | <0.001 | 8.343 | 5 | 0.138 | 40.07 | 0.025 | 0.043 | 0.002 |
| Moderator effect for project duration | - | - | 0.215 | 1 | 0.643 | - | - | - | - | |
| 12 weeks | 3.053 | 0.002 | - | - | - | - | - | - | - | |
| 26 weeks | 11.393 | <0.001 | - | - | - | - | - | - | - | |
| Including moderator of wellbeing scale version | - | - | 1.086 | 1 | 0.297 | - | - | - | - | |
| WEMWBS | 7.287 | <0.001 | - | - | - | - | - | - | - | |
| SWEMWBS | 2.240 | 0.025 | - | - | - | - | - | - | - | |
| Low wellbeing subsample | Overall (in relation to Event Rate) | 2.345 | 0.019 | 5.060 | 5 | 0.409 | 1.19 | 0.003 | 0.169 | 0.029 |
| Including moderator of project duration | - | - | 0.061 | 1 | 0.805 | - | - | - | - | |
| 12 weeks | 1.081 | 0.280 | - | - | - | - | - | - | - | |
| 26 weeks | 1.000 | 0.317 | - | - | - | - | - | - | - | |
| Including moderator of wellbeing scale version | - | - | 0.017 | 1 | 0.895 | - | - | - | ||
| WEMWBS | 1.036 | 0.300 | - | - | - | - | - | - | - | |
| SWEMWBS | 1.188 | 0.235 | - | - | - | - | - | - | - | |
| Sex | Age Category (years) | Starting Wellbeing Status | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Male | Female | 18–30 | 31–50 | 51–70 | >70 | Low | Average–High | ||
| Whole sample | Starting | 47.2 ± 18.4 | 46.8 ± 17.5 | 48.6 ± 20.5 | 45.3 ± 16.2 | 49.8 ± 19.5 | 46.9 ± 12.4 | 29.5 ± 10.8 | 58.6 ± 12.8 |
| Δ | 15.0 ± 16.5 n = 125 | 13.4 ± 15.8 n = 177 | 13.9 ± 16.9 n = 67 | 14.6 ± 17.1 n = 122 | 12.2 ± 15.3 n = 77 | 19.0 ± 14.1 n = 15 | 21.2 ± 18.7 n = 129 | 8.0 ± 12.1 n = 189 | |
| Low wellbeing | Starting | 29.7 ± 11.0 | 30.7 ± 10.3 | 27.9 ± 11.0 | 30.4 ± 11.2 | 28.4 ± 11.0 | 36.5 ± 6.0 | - | - |
| Δ | 22.6 ± 18.9 n = 49 | 21.3 ± 19.4 n = 71 | 23.9 ± 20.0 n = 25 | 21.9 ± 21.8 n= 49 | 21.9 ± 17.7 n = 25 | 23.2 ± 12.0 n = 7 | - | - | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rogerson, M.; Wood, C.; Pretty, J.; Schoenmakers, P.; Bloomfield, D.; Barton, J. Regular Doses of Nature: The Efficacy of Green Exercise Interventions for Mental Wellbeing. Int. J. Environ. Res. Public Health 2020, 17, 1526. https://doi.org/10.3390/ijerph17051526
Rogerson M, Wood C, Pretty J, Schoenmakers P, Bloomfield D, Barton J. Regular Doses of Nature: The Efficacy of Green Exercise Interventions for Mental Wellbeing. International Journal of Environmental Research and Public Health. 2020; 17(5):1526. https://doi.org/10.3390/ijerph17051526
Chicago/Turabian StyleRogerson, Mike, Carly Wood, Jules Pretty, Patrick Schoenmakers, Dan Bloomfield, and Jo Barton. 2020. "Regular Doses of Nature: The Efficacy of Green Exercise Interventions for Mental Wellbeing" International Journal of Environmental Research and Public Health 17, no. 5: 1526. https://doi.org/10.3390/ijerph17051526
APA StyleRogerson, M., Wood, C., Pretty, J., Schoenmakers, P., Bloomfield, D., & Barton, J. (2020). Regular Doses of Nature: The Efficacy of Green Exercise Interventions for Mental Wellbeing. International Journal of Environmental Research and Public Health, 17(5), 1526. https://doi.org/10.3390/ijerph17051526







