Behavioural Determinants of Hand Washing and Glove Recontamination before Aseptic Procedures at Birth: A Time-and-Motion Study and Survey in Zanzibar Labour Wards
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Instruments
2.2. Variables and Their Operationalization
2.2.1. Variables Collected During Observation
Outcomes
Contextual Modifiable Determinants
Candidate Confounders
2.2.2. Variables Collected with the Questionnaire
Individual Modifiable Determinants
Training
Attitudes
Norms and Sanctioning
Self-Efficacy
Habit
Knowledge
Candidate Confounders
2.3. Analysis
2.4. Ethics Approval
2.5. Data Sharing
3. Results
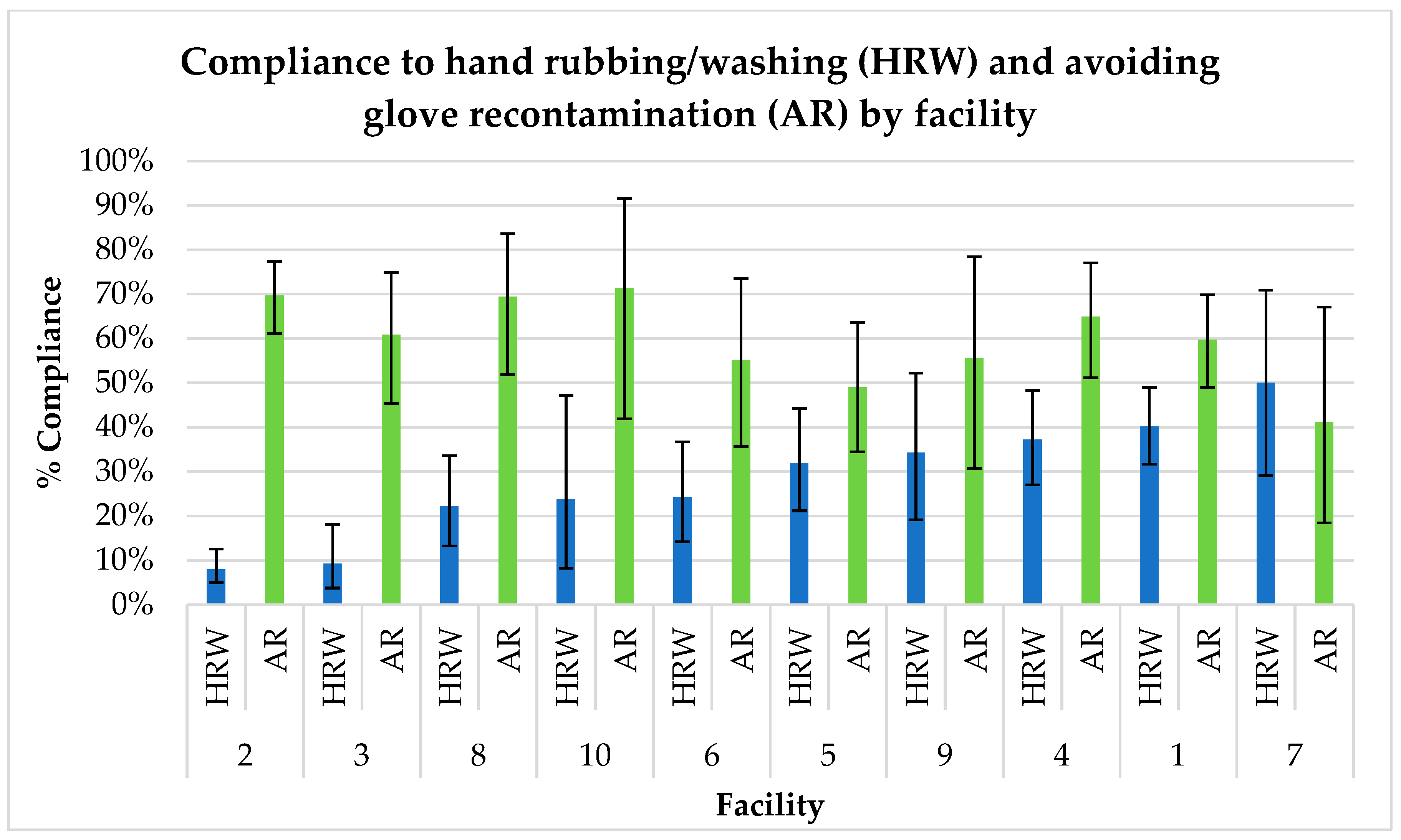
3.1. Descriptive
3.2. Analytical Models
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Blencowe, H.; Cousens, S.; Mullany, L.C.; Lee, A.C.C.; Kerber, K.; Wall, S.; Darmstadt, G.L.; Lawn, J.E. Clean birth and postnatal care practices to reduce neonatal deaths from sepsis and tetanus: A systematic review and Delphi estimation of mortality effect. BMC Public Health 2011, 11 (Suppl. S3), S11. [Google Scholar] [CrossRef]
- Winani, S.; Wood, S.; Coffey, P.; Chirwa, T.; Mosha, F.; Changalucha, J. Use of a clean delivery kit and factors associated with cord infection and puerperal sepsis in Mwanza, Tanzania. J. Midwifery Women’s Health 2007, 52, 37–43. [Google Scholar] [CrossRef]
- Gould, I.M. Alexander Gordon, puerperal sepsis, and modern theories of infection control—Semmelweis in perspective. Lancet Infect. Dis. 2010, 10, 275–278. [Google Scholar] [CrossRef]
- Allegranzi, B.; Pittet, D. Role of hand hygiene in healthcare-associated infection prevention. J. Hosp. Infect. 2009, 73, 305–315. [Google Scholar] [CrossRef]
- Allegranzi, B.; Nejad, S.B.; Combescure, C.; Graafmans, W.; Attar, H.; Donaldson, L.; Pittet, D. Burden of endemic health-care-associated infection in developing countries: Systematic review and meta-analysis. Lancet 2011, 377, 228–241. [Google Scholar] [CrossRef]
- Bagheri Nejad, S.; Allegranzi, B.; Syed, S.B.; Ellis, B.; Pittet, D. Health-care-associated infection in Africa: A systematic review. Bull. World Health Organ. 2011, 89, 757–765. [Google Scholar] [CrossRef]
- ECDC. Point Prevalence Survey of Healthcare-Associated Infections and Antimicrobial Use in European Acute Care Hospitals; Protocol Version 5.3; ECDC: Solna, Sweden, 2016. [Google Scholar]
- Zaidi, A.K.; Huskins, W.C.; Thaver, D.; Bhutta, Z.A.; Abbas, Z.; Goldmann, D.A. Hospital-acquired neonatal infections in developing countries. Lancet 2005, 365, 1175–1188. [Google Scholar] [CrossRef]
- ICF International STATcompiler, the DHS Program. Available online: http://www.statcompiler.com/en/ (accessed on 9 January 2018).
- Baker, U. Closing the Quality Gap. Investigating Health System Bottlenecks and Quality Improvement Strategies for Maternal and Newborn Care in Sub Saharan Africa, Focusing on Tanzania; EBA Dissertation Brief 2018:03; Expert Group for Aid Studies: Stockholm, Sweden, 2018. [Google Scholar]
- Erasmus, V.; Daha, T.J.; Brug, H.; Richardus, J.H.; Behrendt, M.D.; Vos, M.C.; van Beeck, E.F. Systematic review of studies on compliance with hand hygiene guidelines in hospital care. Infect. Control Hosp. Epidemiol. 2010, 31, 283–294. [Google Scholar] [CrossRef]
- World Health Organization. WHO Guidelines on Hand Hygiene in Health Care: First Global Patient Safety Challenge Clean Care Is Safer Care; WHO: Geneva, Switzerland, 2009. [Google Scholar]
- Gon, G.; de Bruin, M.; de Barra, M.; Ali, S.M.; Campbell, O.M.; Graham, W.J.; Juma, M.; Nash, S.; Kilpatrick, C.; Penn-Kekana, L.; et al. Hands washing, glove use, and avoiding recontamination before aseptic procedures at birth: A multicenter time-and-motion study conducted in Zanzibar. Am. J. Infect. Control 2018, 47, 149–156. [Google Scholar] [CrossRef] [PubMed]
- WHO. Hand Hygiene Technical Reference Manual; WHO: Geneva, Switzerland, 2009. [Google Scholar]
- Pittet, D.; Simon, A.; Hugonnet, S.; Pessoa-Silva, C.L.; Sauvan, V.; Perneger, T.V. Hand hygiene among physicians: Performance, beliefs, and perceptions. Ann. Intern. Med. 2004, 141, 1–8. [Google Scholar] [CrossRef] [PubMed]
- O’Boyle, C.A.; Henly, S.J.; Larson, E. Understanding adherence to hand hygiene recommendations: The theory of planned behavior. Am. J. Infect. Control 2001, 29, 352–360. [Google Scholar] [CrossRef] [PubMed]
- Smiddy, M.P.; O’ Connell, R.; Creedon, S.A. Systematic qualitative literature review of health care workers’ compliance with hand hygiene guidelines. Am. J. Infect. Control 2015, 43, 269–274. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Evidence of Hand Hygiene as the Building Block for Infection Prevention and Control; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Whitby, M.; McLaws, M.-L.; Ross, M.W. Why healthcare workers don’t wash their hands: A behavioral explanation. Infect. Control Hosp. Epidemiol. 2006, 27, 484–492. [Google Scholar] [CrossRef] [PubMed]
- De Bono, S.; Heling, G.; Borg, M.A. Organizational culture and its implications for infection prevention and control in healthcare institutions. J. Hosp. Infect. 2014, 86, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Jenner, E.A.; Watson, P.W.B.; Miller, L.; Jones, F.; Scott, G.M. Explaining hand hygiene practice: An extended application of the Theory of Planned Behaviour. Psychol. Health Med. 2002, 7, 311–326. [Google Scholar] [CrossRef]
- Montano, E.D.; Kasprzyk, D. Theory of Reasoned Action, Theory of Planned Behaviour, and the Integrated Behavioural Model. In Health Behaviour and Health Education. Theory, Research and Practice, 4th ed.; Jossey-Bass: San Francisco, CA, USA, 2008. [Google Scholar]
- Huis, A.; van Achterberg, T.; de Bruin, M.; Grol, R.; Schoonhoven, L.; Hulscher, M. A systematic review of hand hygiene improvement strategies: A behavioural approach. Implement. Sci. 2012, 7, 92. [Google Scholar] [CrossRef]
- Von Lengerke, T.; Lutze, B.; Krauth, C.; Lange, K.; Theodor Stahmeyer, J.; Freya Chaberny, I. Promoting Hand Hygiene Compliance. Dtsch. Arztebl. Int. 2017, 114, 29–36. [Google Scholar]
- Gon, G.; Ali, S.M.; Towriss, C.; Kahabuka, C.; Ali, A.O.; Cavill, S.; Dahoma, M.; Faulkner, S.; Haji, H.S.; Kabole, I.; et al. Unpacking the enabling factors for hand, cord and birth-surface hygiene in Zanzibar maternity units. Health Policy Plan. 2017, 32, 1220–1228. [Google Scholar] [CrossRef]
- Westbrook, J. Work Observation Method by Activity Timing: A guide to the Installation and Use of WOMBAT V2; Centre for Health Systems and Safety Research, Macquarie University: Sydney, NSW, Australia, 2016. [Google Scholar]
- Zheng, K.; Guo, M.H.; Hanauer, D.A. Using the time and motion method to study clinical work processes and workflow: Methodological inconsistencies and a call for standardized research. J. Am. Med. Inform. Assoc. 2011, 18, 704–710. [Google Scholar] [CrossRef]
- Aunger, R.; Curtis, V. The Anatomy of Motivation: An Evolutionary-Ecological Approach. Biol. Theory 2013, 8, 49–63. [Google Scholar] [CrossRef]
- Bicchieri, C.; Lindemans, J.W.; Jiang, T. A structured approach to a diagnostic of collective practices. Front. Psychol. 2014, 5, 1418. [Google Scholar] [CrossRef] [PubMed]
- Gardner, B.; Abraham, C.; Lally, P.; de Bruijn, G.-J. Towards parsimony in habit measurement: Testing the convergent and predictive validity of an automaticity subscale of the Self-Report Habit Index. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 102. [Google Scholar] [CrossRef] [PubMed]
- WHO. Hand Hygiene in Outpatient and Home-Based Care and Long-Term Care Facilities; WHO: Geneva, Switzerland, 2012. [Google Scholar]
- WHO. Pregnancy, Chilbirth, Postpartum and Newborn Care: A Guide for Essential Practice, 3rd ed.; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- Belela-Anacleto, A.S.C.; Kusahara, D.M.; Peterlini, M.A.S.; Pedreira, M.L.G. Hand hygiene compliance and behavioural determinants in a paediatric intensive care unit: An observational study. Aust. Crit. Care 2018, 32, 21–27. [Google Scholar] [CrossRef] [PubMed]
- Curtis, V.A.; Danquah, L.O.; Aunger, R.V. Planned, motivated and habitual hygiene behaviour: An eleven country review. Health Educ. Res. 2009, 24, 655–673. [Google Scholar] [CrossRef]
- Rabe-Hesketh, S.; Skrondal, A.; Pickles, A. Reliable Estimation of Generalized Linear Mixed Models Using Adaptive Quadrature. Stata J. 2002, 2, 1–21. [Google Scholar] [CrossRef]
- Yawson, A.E.; Hesse, A.A.J. Hand hygiene practices and resources in a teaching hospital in Ghana. J. Infect. Dev. Ctries. 2013, 7, 338–347. [Google Scholar] [CrossRef]
- Allegranzi, B.; Sax, H.; Bengaly, L.; Richet, H.; Minta, D.K.; Chraiti, M.-N.; Sokona, F.M.; Gayet-Ageron, A.; Bonnabry, P.; Pittet, D.; et al. Successful implementation of the World Health Organization hand hygiene improvement strategy in a referral hospital in Mali, Africa. Infect. Control Hosp. Epidemiol. 2010, 31, 133–141. [Google Scholar] [CrossRef]
- Saito, H.; Inoue, K.; Ditai, J.; Wanume, B.; Abeso, J.; Balyejussa, J.; Weeks, A. Alcohol-based hand rub and incidence of healthcare associated infections in a rural regional referral and teaching hospital in Uganda (‘WardGel’ study). Antimicrob. Resist. Infect. Control 2017, 6, 129. [Google Scholar] [CrossRef]
- Luangasanatip, N.; Hongsuwan, M.; Limmathurotsakul, D.; Lubell, Y.; Lee, A.S.; Harbarth, S.; Day, N.P.J.; Graves, N.; Cooper, B.S. Comparative efficacy of interventions to promote hand hygiene in hospital: Systematic review and network meta-analysis. BMJ 2015, 351, h3728. [Google Scholar] [CrossRef]
- Stone, S.P.; Fuller, C.; Savage, J.; Cookson, B.; Hayward, A.; Cooper, B.; Duckworth, G.; Michie, S.; Murray, M.; Jeanes, A.; et al. Evaluation of the national Cleanyourhands campaign to reduce Staphylococcus aureus bacteraemia and Clostridium difficile infection in hospitals in England and Wales by improved hand hygiene: Four year, prospective, ecological, interrupted time series study. BMJ 2012, 344, e3005. [Google Scholar] [CrossRef]
- Nicol, P.W.; Watkins, R.E.; Donovan, R.J.; Wynaden, D.; Cadwallader, H. The power of vivid experience in hand hygiene compliance. J. Hosp. Infect. 2009, 72, 36–42. [Google Scholar] [CrossRef] [PubMed]
- Srigley, J.A.; Furness, C.D.; Baker, G.R.; Gardam, M. Quantification of the Hawthorne effect in hand hygiene compliance monitoring using an electronic monitoring system: A retrospective cohort study. BMJ Qual. Saf. 2014, 23, 974–980. [Google Scholar] [CrossRef] [PubMed]
- McCambridge, J.; Witton, J.; Elbourne, D.R. Systematic review of the Hawthorne effect: New concepts are needed to study research participation effects. J. Clin. Epidemiol. 2014, 67, 267–277. [Google Scholar] [CrossRef] [PubMed]
| Construct | Number of Items | Cronbach’s alpha |
|---|---|---|
| Outcome 1 (hand rubbing/washing) | ||
| Instrumental attitudes | 5 | 0.27 * |
| Experiential attitudes | 4 | 0.31 * |
| Self-efficacy | 4 | 0.68 |
| Habit | 3 | 0.71 |
| Outcome 2 (avoiding glove recontamination) | ||
| Instrumental attitudes | 3 | 0.13 * |
| Experiential attitudes | 2 | 0.77 |
| Self-efficacy | 3 | 0.76 |
| Habit | 3 | 0.71 |
| Categorical Modifiable Determinants | Facility % (n) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | |
| N = 779 * | Hand rubbing/washing dataset | |||||||||
| Workload (lowest category) | 19.7 (26) | 11.9 (24) | 21.1 (15) | 15.1 (13) | 24.6 (17) | 24.2 (15) | 54.8 (13) | 19.4 (14) | 25.7 (9) | 38.1 (8) |
| Drying material (not available) | 21.2 (28) | 99.0 (200) | 100 (76) | 68.6 (59) | 7.3 (5) | 100 (62) | 100 (24) | 98.6 (71) | 16 (45.7) | 76.2 (16) |
| Knowledge (duration “>10 s”) | 94.7 (125) | 34.2 (69) | 35.5 (27) | 44.2 (38) | 36.2 (25) | 66.1 (41) | 100 (24) | 52.8 (38) | 54.3 (19) | 0 (0) |
| Instrumental beliefs (mentions hand hygiene) | 47.0 (62) | 55.5 (112) | 36.8 (28) | 37.2 (32) | 42 (60.8) | 80.7 (50) | 70.8 (17) | 81.9 (59) | 31.4 (11) | 81.0 (17) |
| Refresher training (yes) | 78.0 (103) | 64.4 (130) | 382 (29) | 24.4 (21) | 17.4 (12) | 71.0 (44) | 41.6 (10) | 77.8 (56) | 34.3 (12) | 71.4 (15) |
| N = 490 ** | Avoiding glove contamination dataset | |||||||||
| Time since donning gloves (<1 min) | 67.4 (62) | 59.9 (79) | 47.8 (22) | 54.4 (31) | 49.0 (24) | 62.1 (18) | 47.1 (8) | 69.4 (25) | 77.8 (25) | 35.7 (5) |
| Workload (lowest category) | 28.3 (26) | 15.9 (21) | 26.1 (19) | 21.1 (12) | 34.7 (17) | 37.9 (11) | 64.7 (11) | 33.3 (12) | 50.0 (9) | 50.0 (7) |
| Experiential attitudes (always yes a lot) | 97.8 (90) | 65.9 (87) | 82.6 (38) | 80.7 (46) | 87.8 (43) | 27.6 (8) | 100 (17) | 75.0 (27) | 83.3 (15) | 42.9 (6) |
| Instrumental beliefs (mentions hand hygiene) | 52.2 (48) | 58.3 (77) | 36.9 (17) | 43.9 (25) | 57.1 (28) | 72.4 (21) | 70.6 (12) | 86.1 (31) | 38.9 (7) | 92.9 (13) |
| Refresher training (yes) | 77.2 (71) | 64.4 (85) | 39.1 (18) | 26.3 (15) | 12.2 (6) | 65.5 (19) | 35.3 (6) | 80.6 (29) | 38.9 (7) | 78.6 (11) |
| Variable Name | Opportunities % (n) or Mean (s.d.) N = 779 | Rubbed/Washed % (n) or Mean (s.d.) N = 190 | Adjusted Odds Ratio * (95% CI) N = 751 ** | LRT p-Value |
|---|---|---|---|---|
| MAIN DETERMINANTS | ||||
| Workload *** | ||||
| Highest | 20.0 (156) | 7.1 (11) | 1 | <0.0001 |
| High | 20.0 (156) | 12.8 (20) | 1.63 (0.67–3.92) | |
| Medium | 20.0 (156) | 25.6 (40) | 4.29 (1.90–9.72) | |
| Low | 20.0 (156) | 14.7 (23) | 2.22 (0.94–5.24) | |
| Lowest | 19.9 (155) | 61.9 (96) | 29.39 (12.90–67.00) | |
| Availability of single use drying material | ||||
| No | 71.5 (557) | 19.9 (111) | 1 | 0.0009 |
| Yes | 26.7 (208) | 36.5 (76) | 2.85 (1.58–5.14) | |
| Missing | 1.7 (13) | 23.1 (3) | - | |
| Inconsistent info | 0.1 (1) | 0 | - | |
| Knowledge (duration) | ||||
| Less than 10 s | 47.8 (373) | 18.0 (67) | 1 | 0.0457 |
| 10 s or more | 52.1 (406) | 30.3 (123) | 1.89 (1.02–3.49) | |
| Habit ° (1–10) | 6.12 (2.50) | 6.56 (2.40) | 1.09 (0.96–1.24) | 0.1716 |
| Instrumental beliefs | ||||
| Does not mention HH | 44.8 (349) | 21.8 (76) | 1 | 0.8066 |
| Mentions HH | 55.2 (430) | 26.5 (114) | 1.09 (0.55–2.14) | |
| Self-efficacy ° (1–10) | 4.9 (3.2) | 4.9 (3.1) | 0.94 (0.83–1.07) | 0.3628 |
| Descriptive norms (colleagues) ° (1–10) | 5.7 (1.8) | 5.9 (1.7) | 1.07(0.86–1.32) | 0.5309 |
| Descriptive norms (managers) ° (1–10) | 6.7 (2.3) | 6.9 (2.4) | 0.95 (0.82–1.11) | 0.5646 |
| Reminders° (0–4) | 2.5 (1.59) | 2.9 (1.41) | 1.20 (0.98–1.46) | 0.0736 |
| Hand hygiene refresher training in the past 12 months | ||||
| No | 44.5 (347) | 21.3 (74) | 1 | 0.2390 |
| Yes | 55.5 (432) | 26.9 (116) | 1.43 (0.79–2.59) | |
| CONFOUNDERS | ||||
| Necessary material (water and soap, or gel) | ||||
| No | 6.2 (48) | 10.4 (5) | 1 | 0.6798 |
| Yes | 90.4 (704) | 25.1 (177) | 1.28 (0.40–412) | |
| Missing | 1.7 (13) | 23.1 (3) | ||
| Inconsistent info | 1.8 (14) | 35.7 (5) | ||
| Presence of the in charge | ||||
| No | 90.9 (708) | 23.7 (168) | 1 | 0.3655 |
| Yes | 7.5 (58) | 32.8 (19) | 1.54 (0.61–3.93) | |
| Missing | 1.7 (13) | 23.1 (3) | - | |
| Professional background | ||||
| Senior Nurse | 4.8 (37) | 16.2 (6) | 1 | 0.1344 |
| Nurse Midwife | 48.7 (379) | 23.0 (87) | 0.91 (0.21–4.03) | |
| Public Health Nurse B | 10.7 (83) | 31.3 (36) | 3.17 (0.63–15.87) | |
| Orderly | 9.9 (77) | 15.6 (12) | 1.89 (0.38–9.50) | |
| Other nurse or nurse assistant | 26.1 (203) | 29.1 (59) | 1.16 (0.23–5.91) | |
| Years since formal training | ||||
| 8 and over | 21.7(169) | 22.5 (38) | 1 | 0.0083 |
| 4–7 | 19.3150) | 17.3 (26) | 1.50 (0.49–4.58) | |
| 1–3 | 15.0 (117) | 24.8 (29) | 4.07 (1.50–11.09) | |
| No training | 9.9 (77) | 15.6(12) | - **** | |
| Years working in this specific maternity ° | 3.7 (5.2) | 3.4 (4.6) | 0.99 (0.92–1.06) | 0.7102 |
| Variable Name | Opportunities % (n) or Mean (s.d.) N = 490 | Clean % (n) or Mean (s.d.) N = 304 | Adjusted odds * Ratio (95% CI) N = 485 ** | LRT p-Value |
|---|---|---|---|---|
| MODIFIABLE DETERMINANTS | ||||
| Time since donning gloves | ||||
| 3 or more minutes | 16.9 (83) | 39.8 (33) | 1 | <0.0001 |
| 2–3 min | 8.0 (39) | 35.9 (14) | 0.75 (0.33–1.85) | |
| 1–2 min | 16.3 (80) | 53.8 (43) | 1.54 (0.77–3.09) | |
| Less than a minute | 58.8 (288) | 74.3 (214) | 4.49 (2.51–8.04) | |
| Workload *** | ||||
| Lowest | 28.2 (138) | 55.1 (76) | 1 | 0.4694 |
| Low | 227 (111) | 60.4 (67) | 1.29 (0.72–2.34) | Test for trend= 0.0641 |
| Medium | 19.4 (95) | 65.3 (62) | 1.42 (0.75–2.69) | |
| High | 17.8 (87) | 65.5 (57) | 1.64 (0.84–3.23) | |
| Highest | 12.0 (59) | 71.2 (42) | 1.87 (0.87–4.04) | |
| Habit ° (1–10) | 6.6 (2.5) | 6.6 (2.9) | 0.99 (0.89–1.10) | 0.8005 |
| Experiential attitudes | ||||
| Mixed responses | 23.1 (113) | 65.5 (74) | 1 | 0.6505 |
| Always responded yes a lot | 76.9 (377) | 61.0 (230) | 1.18 (0.57–2.45) | |
| Instrumental beliefs | ||||
| Does not mention HH | 56.9 (279) | 67.4 (188) | 1 | 0.1670 |
| Mentions HH | 43.1 (211) | 55.0 (116) | 1.52 (0.83–2.78) | |
| Self-efficacy ° (1–10) | 4.9 (3.2) | 4.9 (3.1) | 1.02 (0.94–1.11) | 0.6993 |
| Descriptive norms (colleagues) ° (1–10) | 6.0 (2.0) | 5.9 (2.1) | 1.06 (0.86–1.23) | 0.5551 |
| Descriptive norms (managers)° (1–10) | 6.9(2.4) | 6.8 (2.5) | 0.90 (0.76–1.05) | 0.1731 |
| Reminders° (0–4) | 2.6 (1.6) | 2.6 (1.6) | 1.03 (0.87–1.23) | 0.7831 |
| Hand hygiene refresher training in the past 12 months | ||||
| No | 54.5 (267) | 64.0 (171) | 1 | 0.6245 |
| Yes | 45.5 (223) | 59.6 (133) | 1.16 (0.65–2.05) | |
| CONFOUNDERS | ||||
| Knowledge (touching delivery surface one can pick up germs) | ||||
| Agree | 95.7 (469) | 61.2 (287) | 1 | 0.8171 |
| Disagree | 4.3 (21) | 81.0 (17) | 1.22 (0.23–6.53) | |
| Presence of the in-charge | ||||
| No | 90.8 (445) | 62.0 (276) | 1 | 0.4205 |
| Yes | 8.2 (40) | 67.5 (27) | 1.44 (0.59–3.56) | |
| Missing | 1.0 (5) | 20.0 (1) | ||
| Professional background | ||||
| Senior Nurse | 3.9 (19) | 68.4 (13) | 1 | 0.2252 |
| Nurse Midwife | 52.7 (258) | 59.7 (154) | 0.39 (0.10–1.68) | |
| Public Health Nurse B | 9.8 (48) | 58.3 (28) | 0.71 (0.15–3.38) | |
| Orderly | 6.7 (33) | 51.5 (17) | 0.35 (0.08–1.68) | |
| Other nurse or nurse assistant | 26.9 (132) | 69.7 (92) | 0.67 (0.13–3.39) | |
| Years since formal training | ||||
| 8 and over | 20.0 (98) | 64.3 (63) | 1 | 0.3938 |
| 4–7 | 22.2 (109) | 66.1 (72) | 0.82 (0.32–2.10) | |
| 1–3 | 51.0 (250) | 60.8 (152) | 1.40 (0.53–3.74) | |
| No training | 6.7 (33) | 51.5 (17) | - **** | |
| Years working in this specific maternity ° | 3.5 (4.2) | 3.24 (3.6) | 0.94 (0.87–1.02) | 0.1082 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gon, G.; Virgo, S.; de Barra, M.; Ali, S.M.; Campbell, O.M.; Graham, W.J.; Nash, S.; Woodd, S.L.; de Bruin, M. Behavioural Determinants of Hand Washing and Glove Recontamination before Aseptic Procedures at Birth: A Time-and-Motion Study and Survey in Zanzibar Labour Wards. Int. J. Environ. Res. Public Health 2020, 17, 1438. https://doi.org/10.3390/ijerph17041438
Gon G, Virgo S, de Barra M, Ali SM, Campbell OM, Graham WJ, Nash S, Woodd SL, de Bruin M. Behavioural Determinants of Hand Washing and Glove Recontamination before Aseptic Procedures at Birth: A Time-and-Motion Study and Survey in Zanzibar Labour Wards. International Journal of Environmental Research and Public Health. 2020; 17(4):1438. https://doi.org/10.3390/ijerph17041438
Chicago/Turabian StyleGon, Giorgia, Sandra Virgo, Mícheál de Barra, Said M. Ali, Oona M. Campbell, Wendy J. Graham, Stephen Nash, Susannah L. Woodd, and Marijn de Bruin. 2020. "Behavioural Determinants of Hand Washing and Glove Recontamination before Aseptic Procedures at Birth: A Time-and-Motion Study and Survey in Zanzibar Labour Wards" International Journal of Environmental Research and Public Health 17, no. 4: 1438. https://doi.org/10.3390/ijerph17041438
APA StyleGon, G., Virgo, S., de Barra, M., Ali, S. M., Campbell, O. M., Graham, W. J., Nash, S., Woodd, S. L., & de Bruin, M. (2020). Behavioural Determinants of Hand Washing and Glove Recontamination before Aseptic Procedures at Birth: A Time-and-Motion Study and Survey in Zanzibar Labour Wards. International Journal of Environmental Research and Public Health, 17(4), 1438. https://doi.org/10.3390/ijerph17041438





