Food Retail Environments in Greater Melbourne 2008–2016: Longitudinal Analysis of Intra-City Variation in Density and Healthiness of Food Outlets
Abstract
1. Introduction
- How did the density of food outlets change in Melbourne between 2008 and 2016?
- Did the ‘healthiness’ of food outlets in Melbourne vary with distance from Central Business District; and, how has this changed over time between 2008 and 2016?
- Did the density of different types of food outlets vary with distance from Central Business District in Melbourne; and, how has this changed over time between 2008 and 2016?
2. Materials and Methods
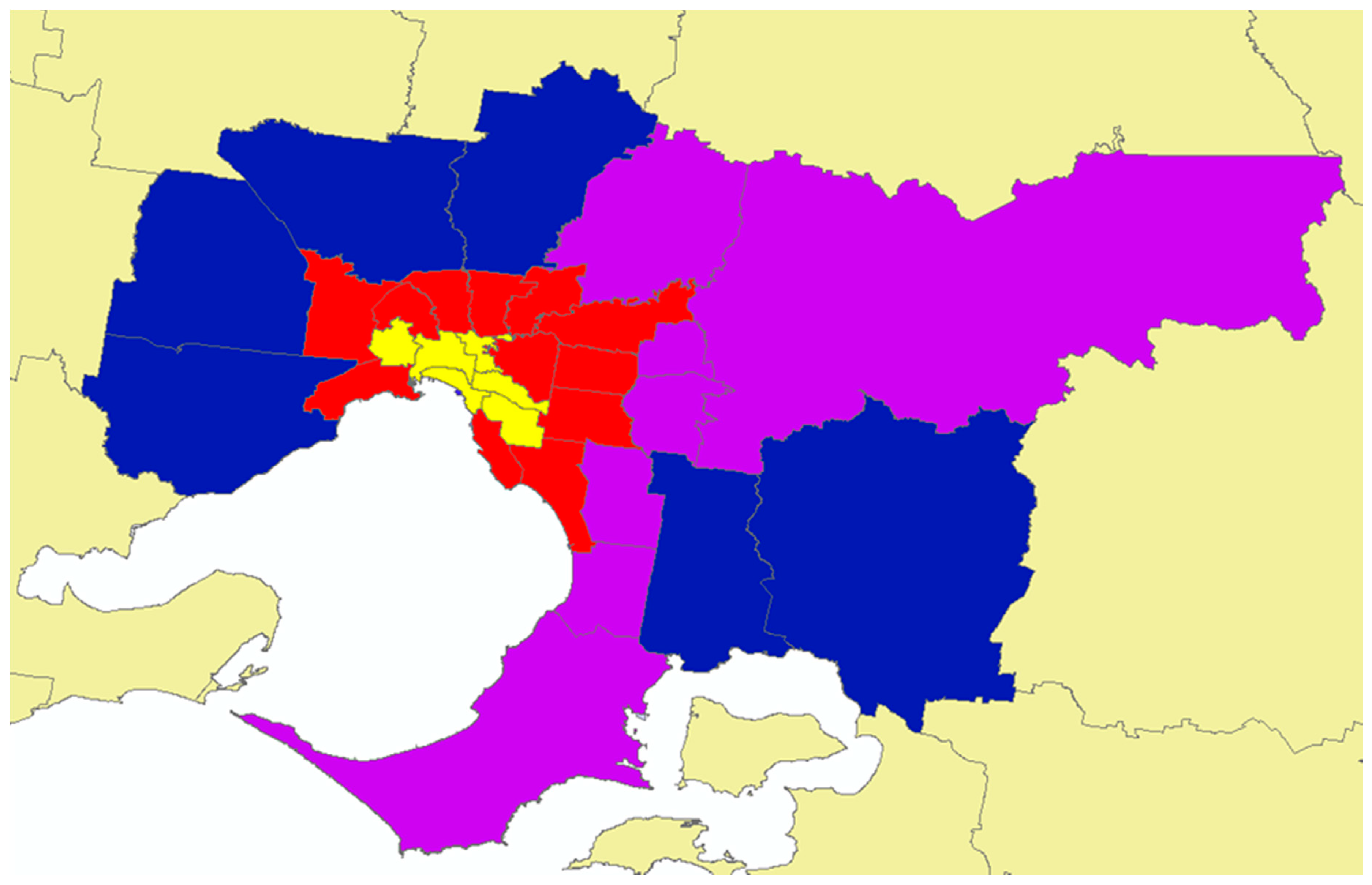
2.1. Study Design
2.2. Food Outlet Data Collection and Management
2.3. Food Outlet Data Preparation
2.3.1. Food Outlet Classification Tool
2.3.2. Food Outlet Classification
2.4. Classification of Local Government Areas (LGAs)
2.5. Food Environment Measures
2.6. Statistical Analysis
3. Results
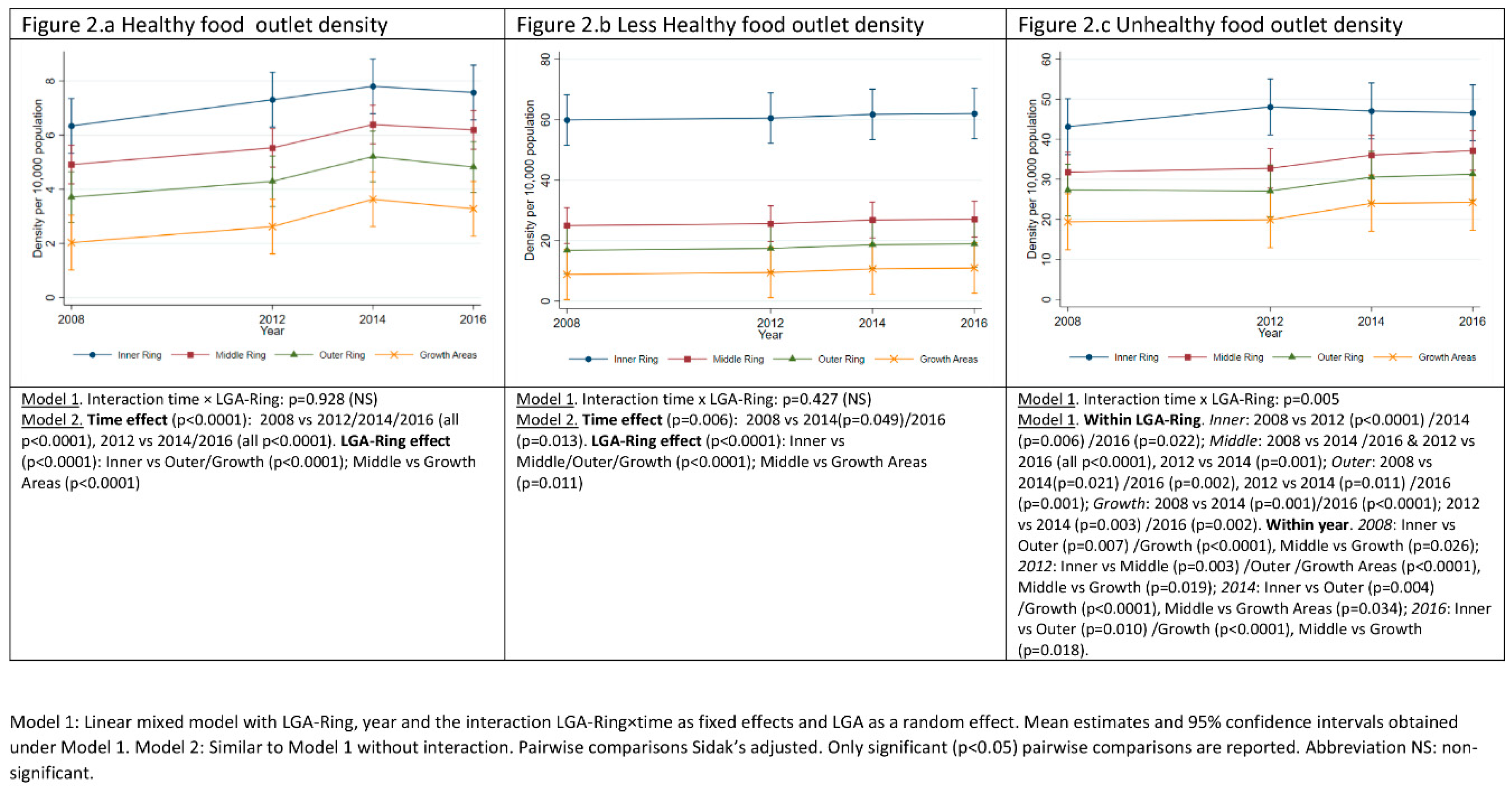
3.1. Food Outlets Grouped by Healthiness: Density over Time and across LGA-Rings
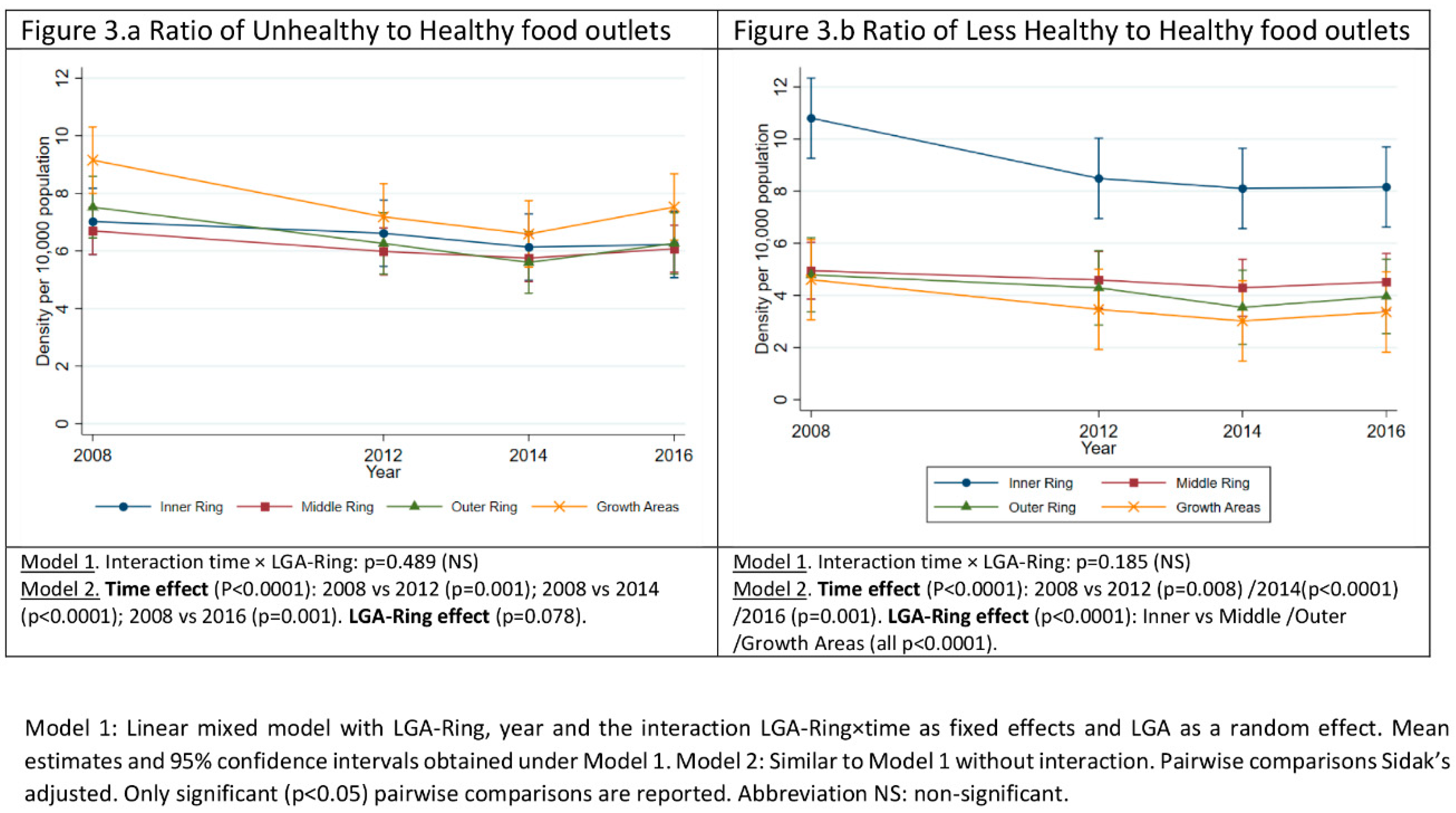
3.2. Ratio of Unhealthy or Less Healthy Food Outlets to Healthy Food Outlets over Time and across LGA-Rings
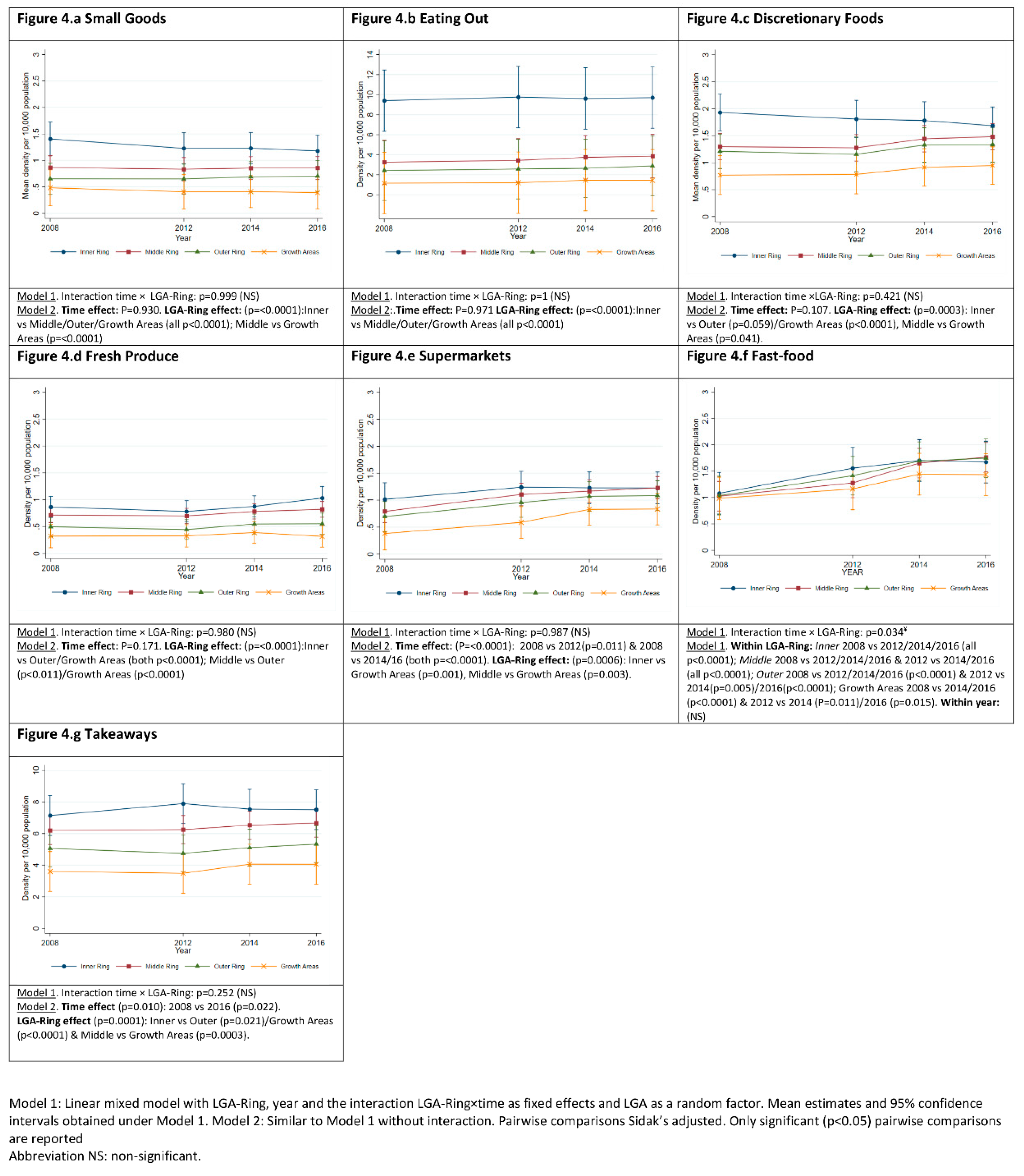
3.3. Food Outlets Grouped by Store Type: Density over Time and across LGA-Rings
4. Discussion
4.1. Strengths
4.2. Limitations
4.3. Implications for Practice
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Swinburn, B.A.; Kraak, V.I.; Allender, S.; Atkins, V.J.; Baker, P.I.; Bogard, J.R.; Brinsden, H.; Calvillo, A.; De Schutter, O.; Devarajan, R.; et al. The global syndemic of obesity, undernutrition, and climate change: The Lancet Commission report. Lancet N. Am. Ed. 2019, 39, 791–846. [Google Scholar] [CrossRef]
- Kelly, T.; Yang, W.; Chen, C.S.; Reynolds, K.; He, J. Global burden of obesity in 2005 and projections to 2030. IJO 2008, 32, 1431–1437. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Diet, Nutrition and the Prevention of Chronic Diseases; WHO Technical Report Series; World Health Organization (WHO): Geneva, Switzerland, 2003. [Google Scholar]
- Swinburn, B.A.; Sacks, G.; Hall, K.D.; McPherson, K.; Finegood, D.T.; Moodie, M.L.; Gortmaker, S.L. The global obesity pandemic: Shaped by global drivers and local environments. Lancet 2011, 378, 804–814. [Google Scholar] [CrossRef]
- Swinburn, B.; Vandevijvere, S.; Kraak, V.; Sacks, G.; Snowdon, W.; Hawkes, C.; Barquera, S.; Friel, S.; Kelly, B.; Kumanyika, S.; et al. Monitoring and benchmarking government policies and actions to improve the healthiness of food environments: A proposed Government Healthy Food Environment Policy Index. Obes. Rev. 2013, 14 (Suppl. 1), 24–37. [Google Scholar] [CrossRef] [PubMed]
- Giskes, K.; van Lenthe, F.; Avendano-Pabon, M.; Brug, J. A systematic review of environmental factors and obesogenic dietary intakes among adults: Are we getting closer to understanding obesogenic environments? Obes. Rev. 2011, 12, e95–e106. [Google Scholar] [CrossRef]
- Morland, K.; Wing, S.; Roux, A.D.; Poole, C. Neighborhood characteristics associated with the location of food stores and food service places. Am. J. Prev. Med. 2002, 22, 23–29. [Google Scholar] [CrossRef]
- Keeble, M.; Adams, J.; White, M.; Summerbell, C.; Cummins, S.; Burgoine, T. Correlates of English local government use of the planning system to regulate hot food takeaway outlets: A cross-sectional analysis. IJBNPA 2019, 16, 127. [Google Scholar] [CrossRef]
- Sacks, G.; Robinson, E.; Cameron, A. Issues in measuring the healthiness of food environments and interpreting relationships with diet, obesity and related health outcomes. Curr. Obes. Rep. 2019, 8, 98–111. [Google Scholar] [CrossRef]
- Gamba, R.; Schuchter, J.; Rutt, C.; Seto, E. Measuring the food environment and its effects on obesity in the united states: A systematic review of methods and results. J. Community Health 2015, 40, 464–475. [Google Scholar] [CrossRef]
- Miller, L.J.; Joyce, S.; Carter, S.; Yun, G. Associations between childhood obesity and the availability of food outlets in the local environment: A retrospective cross-sectional study. AJHP 2014, 28, e137–e145. [Google Scholar] [CrossRef]
- Feng, X.; Astell-Burt, T.; Badland, H.; Mavoa, S.; Giles-Corti, B. Modest ratios of fast food outlets to supermarkets and green grocers are associated with higher body mass index: Longitudinal analysis of a sample of 15,229 Australians aged 45 years and older in the Australian National Liveability Study. Health Place 2018, 49, 101–110. [Google Scholar] [CrossRef] [PubMed]
- Paquet, C.; Coffee, N.T.; Haren, M.T.; Howard, N.J.; Adams, R.J.; Taylor, A.W.; Daniel, M. Food environment, walkability, and public open spaces are associated with incident development of cardio-metabolic risk factors in a biomedical cohort. Health Place 2014, 28, 173–176. [Google Scholar] [CrossRef] [PubMed]
- Moayyed, H.; Kelly, B.; Feng, X.; Flood, V. Is living near healthier food stores associated with better food intake in regional Australia? Int. J. Environ. Res. Public Health 2017, 14, 884. [Google Scholar] [CrossRef] [PubMed]
- Crawford, D.A.; Timperio, A.F.; Salmon, J.A.; Baur, L.; Giles-Corti, B.; Roberts, R.J.; Jackson, M.L.; Andrianopoulos, N.; Ball, K. Neighbourhood fast food outlets and obesity in children and adults: The CLAN study. Int. J. Pediatr. Obes. 2008, 3, 249–256. [Google Scholar] [CrossRef] [PubMed]
- Pearce, J.; Hiscock, R.; Blakely, T.; Witten, K. A national study of the association between neighbourhood access to fast-food outlets and the diet and weight of local residents. Health Place 2009, 15, 193–197. [Google Scholar] [CrossRef] [PubMed]
- De Vogli, R.; Kouvonen, A.; Gimeno, D. Globesization: Ecological evidence on the relationship between fast food outlets and obesity among 26 advanced economies: Corrigendum. Crit. Public Health 2012, 22, 117–119. [Google Scholar] [CrossRef]
- Minaker, L.M.; Shuh, A.; Olstad, D.L.; Engler-Stringer, R.; Black, J.L.; Mah, C.L. Retail food environments research in Canada: A scoping review. Can. J. Public Health. 2016, 107 (Suppl. 1), eS4–eS13. [Google Scholar] [CrossRef]
- Hilmers, A.; Hilmers, D.C.; Dave, J. Neighborhood disparities in access to healthy foods and their effects on environmental justice. Am. J. Public Health 2012, 102, 1644–1654. [Google Scholar] [CrossRef]
- Vandevijvere, S.; D’Souza, E.; Swinburn, B. How Healthy are New Zealand Food Environements? A Comprehensive Assessment 2014–2017; International Network for Food and Obesity/non-communicable diseases Research, Monitoring and Action Support (INFORMAS): Auckland, New Zealand, 2018. [Google Scholar]
- Needham, C.; Sacks, G.; Orellana, L.; Robinsone, E.; Allender, S.; Strugnell, C. A systematic review of the Australian food retail environment: Characteristics, variation by geographic area, socioeconomic position and associations with diet and obesity. Obes. Rev. 2019, 21, 1–22. [Google Scholar] [CrossRef]
- Moayyed, H.; Kelly, B.; Feng, X.; Flood, V. Evaluation of a ’healthiness’ rating system for food outlet types in Australian residential communities. Nutr. Diet. 2017, 74, 29–35. [Google Scholar] [CrossRef]
- Thornton, L.E.; Kavanagh, A.M. Association between fast food purchasing and the local food environment. Nutr. Diabetes 2012, 2, e53. [Google Scholar] [CrossRef] [PubMed]
- United Nations. World Urbanization Prospects: The 2018 Revision (Key Facts); Department of Economic and Social Affairs: Geneva, Switzerland, 2019. [Google Scholar]
- Hooper, P.; Giles-Corti, B.; Knuiman, M. Evaluating the implementation and active living impacts of a State Government planning policy designed to create walkable neighborhoods in Perth, Western Australia. AJHP 2014, 28, S5–S18. [Google Scholar] [CrossRef] [PubMed]
- Murphy, M.; Badland, H.; Jordan, H.; Koohsari, M.J.; Giles-Corti, B. Local food environments, suburban development, and BMI: A mixed methods study. Int. J. Environ. Res. Public Health 2018, 15, 1392. [Google Scholar] [CrossRef] [PubMed]
- Brain, P.; Stanley, J.; Stanley, J. Melbourne: How Big, How Fast and at What Cost? Melbourne Sustainable Society Institute, The University of Melbourne: Melbourne, Australia, 2019. [Google Scholar]
- Walker, R.E.; Keane, C.R.; Burke, J.G. Disparities and access to healthy food in the United States: A review of food deserts literature. Health Place 2010, 16, 876–884. [Google Scholar] [CrossRef] [PubMed]
- Beaulac, J.; Kristjansson, E.; Cummins, S. A systematic review of food deserts, 1966–2007. Prev. Chronic Dis. 2009, 6, A105. [Google Scholar] [PubMed]
- Australian Bureau of Statistics (ABS). Estimated Resident Population (ERP) and Components by LGA (ASGS 2018) 2001–2018; Commonwealth of Australia: Canberra, Australia, 2018.
- Victorian State Government. Plan Melbourne 2017–2050: Metropolitan Planning Strategy; Department of Environment Land Water and Planning, Victorian State Government: Melbourne, Australia, 2017.
- Australian Bureau of Statistics (ABS). 3218.0—Regional Population Growth, Australia, 2017–2018; Commonwealth of Australia: Canberra, Australia, 2019.
- Victorian State Government. Victoria in Future 2016: Population and Household Projections to 2051; Department of Environment Land Water and Planning: Melbourne, Australia, 2016.
- Victorian State Government. Precinct Structure Planning Guidelines Part Two: Preparing the Pricnct Strucutre Plan; Australian Growth Authority: Melbourne, Australia; Victorian State Government: Melbourne, Australia, 2013.
- Murphy, M.; Koohsari, M.J.; Badland, H.; Giles-Corti, B. Supermarket access, transport mode and BMI: The potential for urban design and planning policy across socio-economic areas. Public Health Nutr. 2017, 20, 3304–3315. [Google Scholar] [CrossRef]
- Rossimel, A.; Han, S.S.; Larsen, K.; Palermo, C. Access and affordability of nutritious food in metropolitan Melbourne. Nutr. Diet 2016, 73, 13–18. [Google Scholar] [CrossRef]
- Gunn, L.D.; Mavoa, S.; Boulangé, C.; Hooper, P.; Kavanagh, A.; Giles-Corti, B. Designing healthy communities: Creating evidence on metrics for built environment features associated with walkable neighbourhood activity centres. IJBMPA 2017, 14. [Google Scholar] [CrossRef]
- Cameron, A.J. The shelf space and strategic placement of healthy and discretionary foods in urban, urban-fringe and rural/non-metropolitan Australian supermarkets. Public Health Nutr. 2018, 21, 593–600. [Google Scholar] [CrossRef]
- Victorian State Government. Victorian Electors by Locality, Postcode and Electorates Melbourne, Austalia. 2019. Available online: https://discover.data.vic.gov.au/dataset/victorian-electors-by-locality-postcode-and-electorates (accessed on 7 January 2019).
- Victorian State Government. Victorian Population Health Survey 2014: Modifiable Risk Factors Contributing to Chronic Diseases in Victoria. A Snapshot by Local Government Area; Department of Health and Human Services: Melbourne, Australia, 2016.
- Sensis Data. Frequently Asked Questions. Available online: https://www.sensis.com.au/help/faqs-yellow-pages-print (accessed on 16 August 2019).
- Thornton, L.E.; Lamb, K.E.; Ball, K. Fast food restaurant locations according to socioeconomic disadvantage, urban-regional locality, and schools within Victoria, Australia. SSM Popul. Health 2016, 2, 1–9. [Google Scholar] [CrossRef]
- National Health and Medical Research Council (NHMRC). Australian Dietary Guidelines; National Health and Medical Research Council (NHMRC): Canberra, Australia, 2013.
- Victorian State Government. A Plan for Melbourne’s Growth Areas; Department of Sustainability and Environment: Melbourne, Australia, 2005.
- Maguire, E.R.; Burgoine, T.; Monsivais, P. Area deprivation and the food environment over time: A repeated cross-sectional study on takeaway outlet density and supermarket presence in Norfolk, UK, 1990–2008. Health Place 2015, 33, 142–147. [Google Scholar] [CrossRef] [PubMed]
- StataCorp. Stata Statistical Software: Release 15; StataCorp LLC: College Station, TX, USA, 2017. [Google Scholar]
- Burgoine, T.; Lake, A.A.; Stamp, E.; Alvanides, S.; Mathers, J.C.; Adamson, A.J. Changing foodscapes 1980–2000, using the ASH30 study. Appetite 2009, 53, 157–165. [Google Scholar] [CrossRef] [PubMed]
- Bivoltsis, A.; Trapp, G.; Knuiman, M.; Hooper, P.; Ambrosini, G.L. The evolution of local food environments within established neighbourhoods and new developments in Perth, Western Australia. Health Place 2019, 57, 204–217. [Google Scholar] [CrossRef] [PubMed]
- Hui, L.; Law, J.; Quick, M. Identifying food deserts and swamps based on relative healthy food access: A spatio-temporal Bayesian approach. Int. J. Health Geogr. 2015, 14, 1–11. [Google Scholar]
- Rose, R.; Swalm, C.M.; Rice, J.; Farley, T.; Hutchinson, P. Deserts in New Orleans? Illustrations of Urban Food Access and Implications for Policy; School of Public Health and Tropical Medicine, Tulane University: New Orleans, LA, USA, 2009. [Google Scholar]
- Cooksey-Stowers, K.; Schwartz, M.B.; Brownell, K.D. Food swamps predict obesity rates better than food deserts in the United States. Int. J. Environ. Res. Public Health 2017, 14, 1366. [Google Scholar] [CrossRef] [PubMed]
- Lopez, R. Urban sprawl and risk for being overweight or obese. Am. J. Public Health 2004, 94, 1574–1579. [Google Scholar] [CrossRef]
- Victorian State Government Department of Environment Land Water and Planning. Melbourne 2030; Audit Expert Group Report; Victorian State Government: Melbourne, Australia, 2008.
- Lake, A.A.; Burgoine, T.; Greenhalgh, F.; Stamp, E.; Tyrrell, R. The foodscape: Classification and field validation of secondary data sources. Health Place 2010, 16, 666–673. [Google Scholar] [CrossRef]
- Glanz, K.; Sallis, J.F.; Saelens, B.E.; Frank, L.D. Nutrition environment measures survey in stores (NEMS-S): Development and evaluation. Am. J. Prev. Med. 2007, 32, 282–289. [Google Scholar] [CrossRef]
- Rosenheck, R. Fast food consumption and increased caloric intake: A systematic review of a trajectory towards weight gain and obesity risk. Obes. Rev. 2008, 9, 535–547. [Google Scholar] [CrossRef]
- Zorbas, C.; Gilham, B.; Boelsen-Robinson, T.; Blake, M.R.C.; Peeters, A.; Cameron, A.J.; Wu, J.H.Y.; Backholer, K. The frequency and magnitude of price-promoted beverages available for sale in Australian supermarkets. Aust. N. Z. J. Public Health 2019, 43, 346–351. [Google Scholar] [CrossRef]
- Riesenberg, D.; Backholer, K.; Zorbas, C.; Sacks, G.; Paix, A.; Marshall, J.; Blake, M.R.; Bennett, R.; Peeters, A.; Cameron, A.J. Price promotions by food category and product healthiness in an Australian supermarket chain, 2017–2018. Am. J. Public Health 2019, 109, 1434–1439. [Google Scholar] [CrossRef] [PubMed]
- Thornton, L.E.; Cameron, A.J.; McNaughton, S.A.; Waterlander, W.E.; Sodergren, M.; Svastisalee, C.; Blanchard, L.; Liese, A.D.; Battersby, S.; Carter, M.; et al. Does the availability of snack foods in supermarkets vary internationally? IJBNPA 2013, 10, 56. [Google Scholar] [CrossRef] [PubMed]
- Spencer, S. FOODmap: An Analysis of the Australian Food Supply Chain; Department of Agriculture, Fisheries and Forestry: Canberra, Australia, 2012. [Google Scholar]
- Communities CGHC. Weekly Affordable Fresh Food Markets to Support Healthy Connected Communities. 2019. Available online: https://www.thecommunitygrocer.com.au/ (accessed on 6 September 2019).
| Food Outlets Grouped by ‘Type’ | Food Outlets Grouped by ‘Healthiness’ Score | |
|---|---|---|
| 1. Supermarkets: Minor and Major Supermarkets |  | 1. Healthy (FES range: +5 to +10): Supermarkets, Fruit and greengrocer, Butcher, Fish, Poultry shop, Salad/Sandwich/Sushi bar. |
| 2. Fresh Produce: Fruit and greengrocer, Butcher, Fish, Poultry shop | ||
| 3. Eating Out: Cafes and Restaurants (Independent and Franchise), and Pubs | 2. Less Healthy (FES range: −4 to +4): Cafes and Restaurants (Independent and Franchise), Bakers, Delis. | |
| 4. Small Goods: Bakers, Delis, Sandwich and Sushi | ||
| 5. Fast-food: Takeaway Franchise | 3. Unhealthy (FES range: −10 to −5): Fast-food, Takeaway independent, Pubs, General stores and Specialty extra. | |
| 6. Takeaways: Takeaway Independent | ||
| 7. Discretionary Foods *: General stores and Specialty extra |
| Measures | Year | ||||
|---|---|---|---|---|---|
| 2008 | 2012 | 2014 | 2016 | % Change # | |
| Greater Melbourne population | 4,020,094 | 4,356,752 | 4,566,216 | 4,851,674 | 20.7 |
| Food outlet classification (healthiness value): | Number of outlets (density per 10,000 population) | ||||
| Total | 10,077 (25) | 11,415 (26.2) | 12,943 (28.4) | 13,580 (28) | +34.8(11.7) |
| Baker (0) | 804 (2) | 841 (1.93) | 879 (1.93) | 911 (1.88) | +13 (−6.11) |
| Butcher (+9) | 386 (0.96) | 422 (0.97) | 489 (1.07) | 502 (1.03) | +30 (7.76) |
| General Stores (−5) | 532 (1.32) | 523 (1.2) | 664 (1.45) | 687 (1.42) | +29 (7) |
| Delicatessen (0) | 297 (0.74) | 262 (0.6) | 255 (0.56) | 253 (0.52) | −15 (−29.42) |
| Fruit & Greengrocer (+10) | 304 (0.76) | 278 (0.64) | 330 (0.72) | 337 (0.69) | +11 (−8.15) |
| Fish Shop (+9) | 110 (0.27) | 118 (0.27) | 177 (0.39) | 181 (0.37) | +65 (36.34) |
| Major Supermarkets (+5) | 99 (0.25) | 309 (0.71) | 394 (0.86) | 390 (0.8) | +294 (226.42) |
| Minor Supermarkets (+5) | 440 (1.09) | 508 (1.17) | 552 (1.21) | 639 (1.32) | +45 (20.34) |
| Poultry Shop (+9) | 97 (0.24) | 90 (0.21) | 128 (0.28) | 19 (0.04) | −80 (−83.77) |
| Pubs (−5) | 290 (0.72) | 339 (0.78) | 323 (0.71) | 357 (0.74) | +23.1 (2) |
| Restaurant Café Franchise (0) | 98 (0.24) | 152 (0.35) | 247 (0.54) | 198 (0.41) | +102 (67.41) |
| Restaurant Café Independent (0) | 3468 (8.63) | 3910 (8.97) | 4317 (9.45) | 4672 (9.63) | +35 (11.63) |
| Sandwich shop (+5) | 78 (0.19) | 48 (0.11) | 58 (0.13) | 57 (0.12) | −27 (−39.45) |
| Specialty Core (+5) | 106 (0.26) | 149 (0.34) | 230 (0.5) | 245 (0.5) | +131 (91.52) |
| Specialty Extra (−8) | 427 (1.06) | 486 (1.12) | 520 (1.14) | 550 (1.13) | +29 (6.73) |
| Sushi bar (+5) | 17 (0.04) | 112 (0.26) | 136 (0.3) | 117 (0.24) | +588 (470.27) |
| Fast-food Franchise (−10) | 405 (1.01) | 560 (1.29) | 720 (1.58) | 779 (1.61) | +92 (59.38) |
| Takeaway Independent (−8) | 2119 (5.27) | 2308 (5.3) | 2524 (5.53) | 2686 (5.54) | +27 (5.03) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Needham, C.; Orellana, L.; Allender, S.; Sacks, G.; Blake, M.R.; Strugnell, C. Food Retail Environments in Greater Melbourne 2008–2016: Longitudinal Analysis of Intra-City Variation in Density and Healthiness of Food Outlets. Int. J. Environ. Res. Public Health 2020, 17, 1321. https://doi.org/10.3390/ijerph17041321
Needham C, Orellana L, Allender S, Sacks G, Blake MR, Strugnell C. Food Retail Environments in Greater Melbourne 2008–2016: Longitudinal Analysis of Intra-City Variation in Density and Healthiness of Food Outlets. International Journal of Environmental Research and Public Health. 2020; 17(4):1321. https://doi.org/10.3390/ijerph17041321
Chicago/Turabian StyleNeedham, Cindy, Liliana Orellana, Steven Allender, Gary Sacks, Miranda R. Blake, and Claudia Strugnell. 2020. "Food Retail Environments in Greater Melbourne 2008–2016: Longitudinal Analysis of Intra-City Variation in Density and Healthiness of Food Outlets" International Journal of Environmental Research and Public Health 17, no. 4: 1321. https://doi.org/10.3390/ijerph17041321
APA StyleNeedham, C., Orellana, L., Allender, S., Sacks, G., Blake, M. R., & Strugnell, C. (2020). Food Retail Environments in Greater Melbourne 2008–2016: Longitudinal Analysis of Intra-City Variation in Density and Healthiness of Food Outlets. International Journal of Environmental Research and Public Health, 17(4), 1321. https://doi.org/10.3390/ijerph17041321





