Transdisciplinary Research Priorities for Human and Planetary Health in the Context of the 2030 Agenda for Sustainable Development
Abstract
1. Introduction
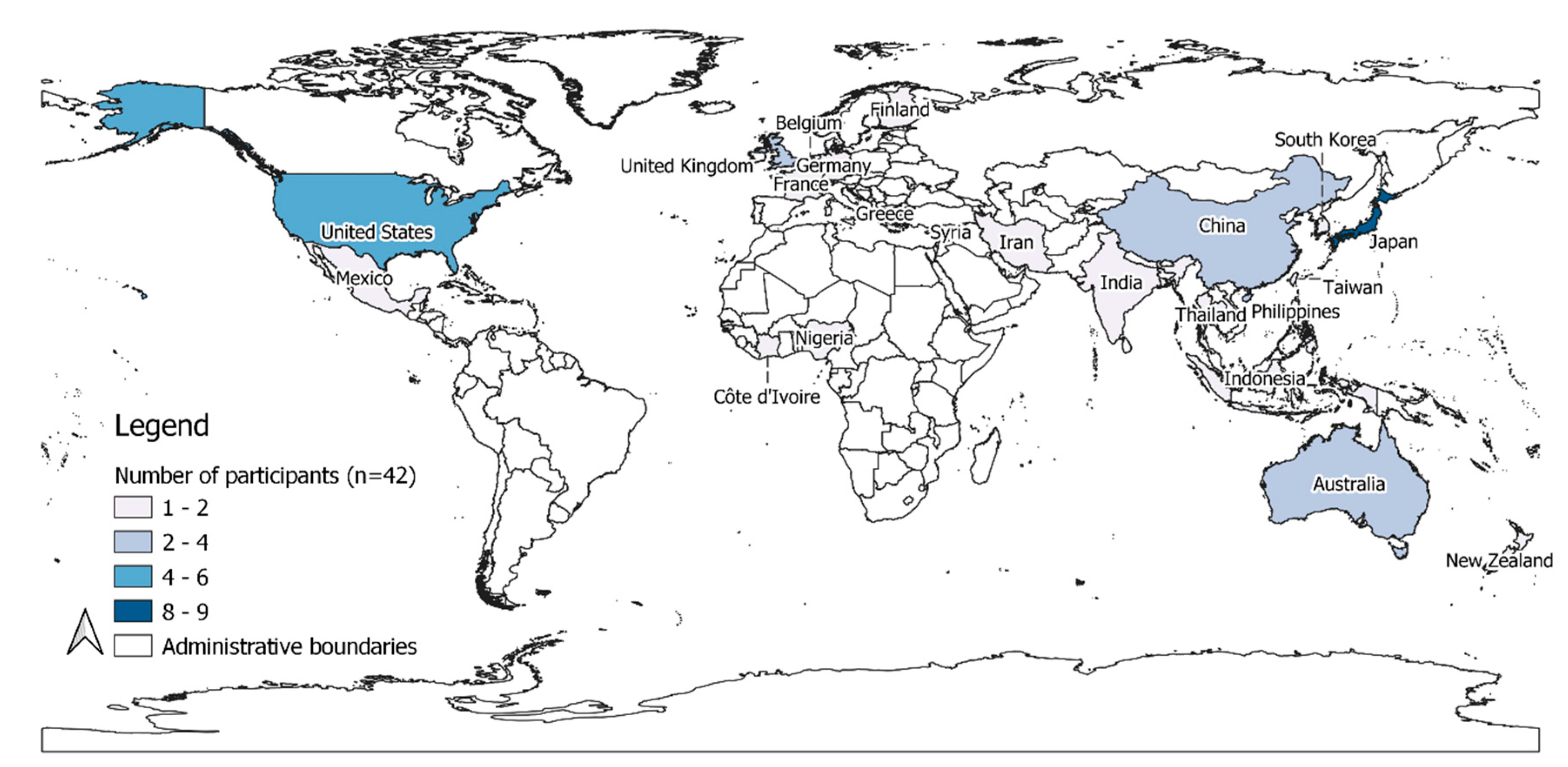
2. Materials and Methods
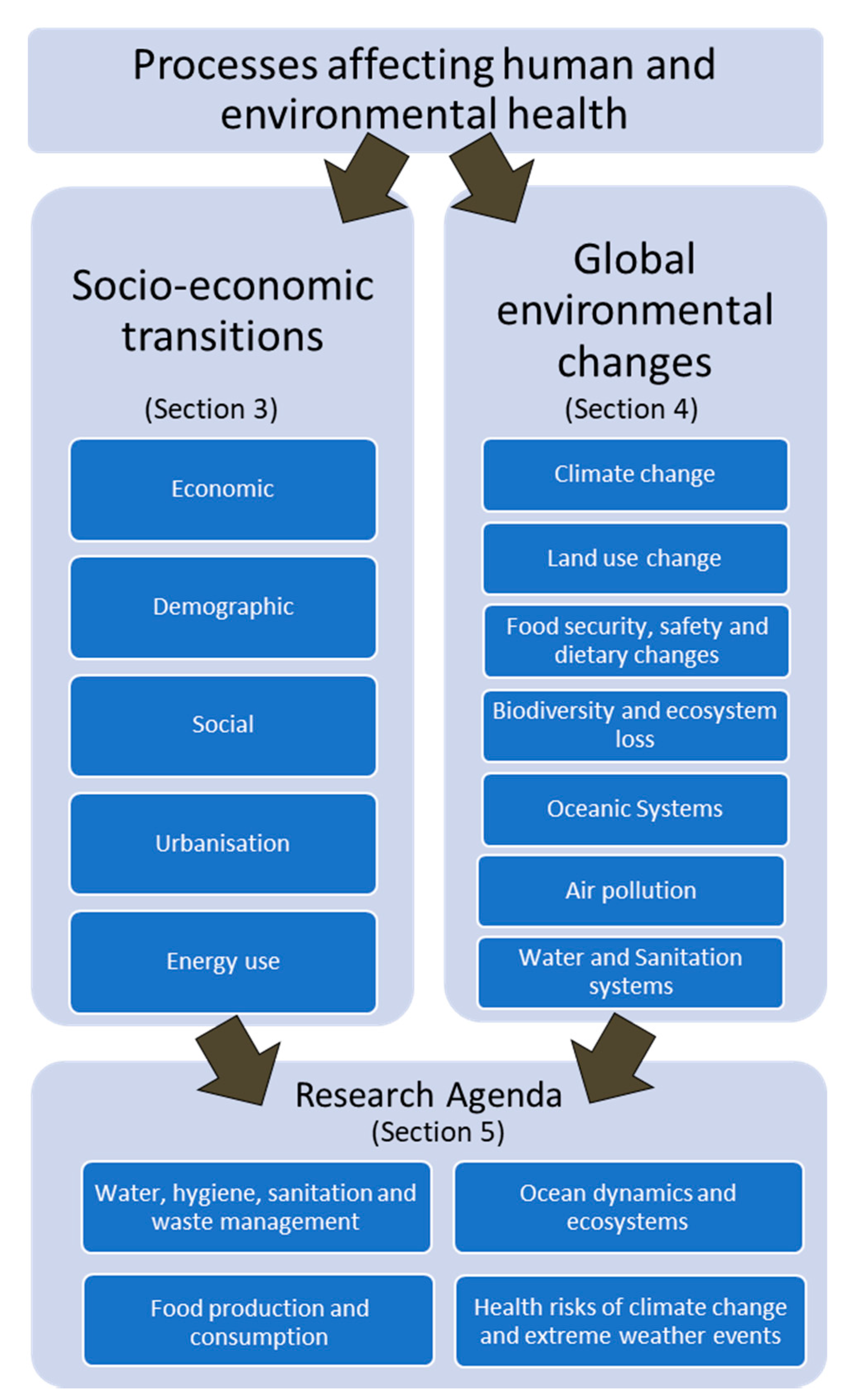
3. Socioeconomic Transitions Affecting Human and Planetary Health
3.1. Economic
3.2. Demographic and Social
3.3. Energy Systems
3.4. Urban Systems
4. Global Environmental Changes Affecting Human and Planetary Health
4.1. Climate Change
4.2. Land Use
4.3. Food Safety and Security, and Dietary Changes
4.4. Biodiversity and Ecosystem Service Loss
4.5. Change in the Global Ocean
4.6. Air Pollution
4.7. Water and Sanitation Systems
5. Research Agenda to Protect and Promote Human in the Context of Global Environmental Changes
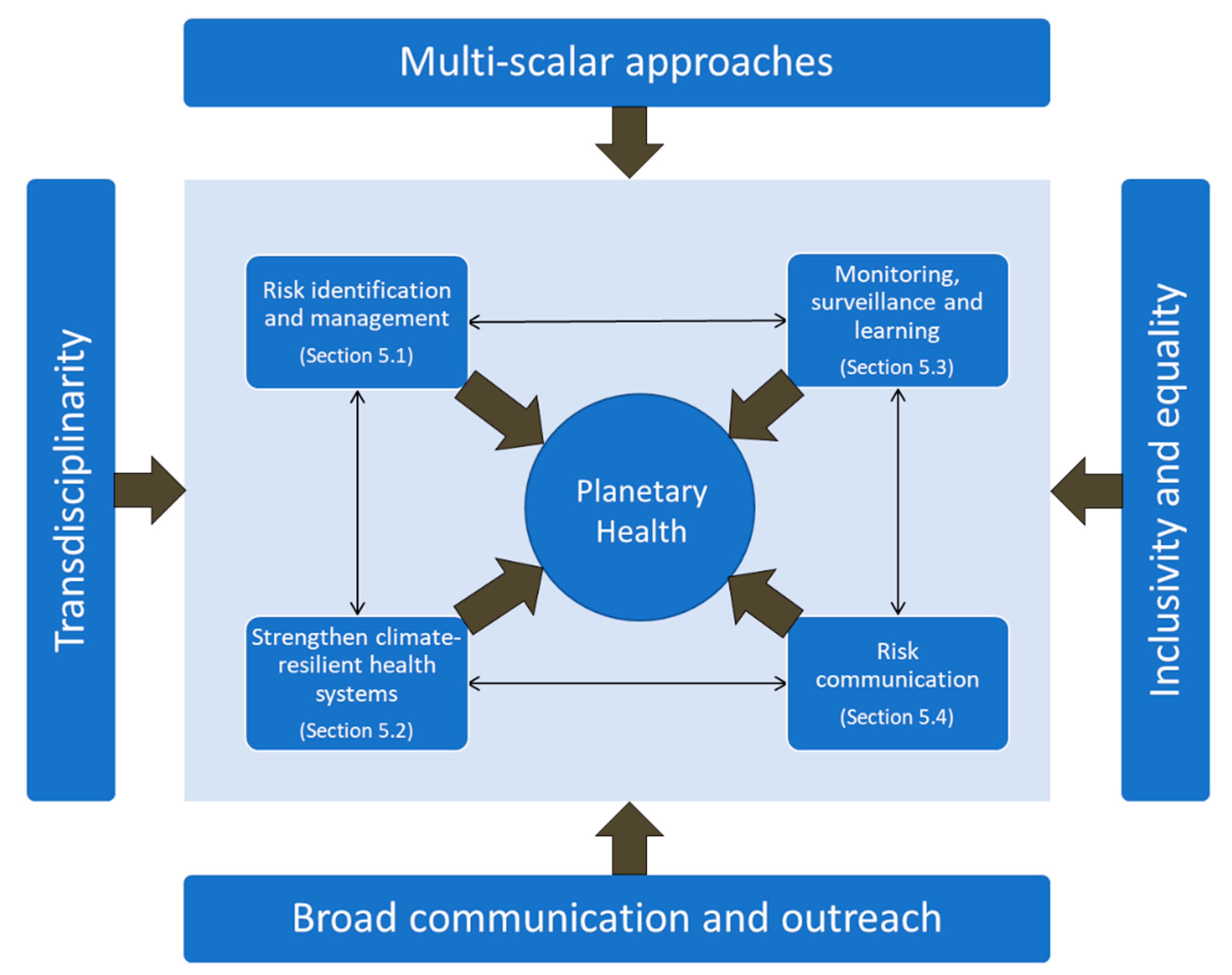
5.1. Risk Identification and Management
5.1.1. Water, Hygiene, Sanitation, and Waste Management
5.1.2. Food Production and Consumption
5.1.3. Oceans
5.1.4. Extreme Weather Events and Climate Change
5.2. Strengthen Climate-Resilient Health Systems
5.3. Monitoring, Surveillance, and Evaluation
5.4. Risk Communication
6. Discussion: Pathways toward Sustainability
- Transdisciplinary, inviting stakeholders to co-design research and implement interventions [148,149]. Transdisciplinary research into reducing vulnerability and enhancing resilience should cut across several domains, including (but not limited to) the built environment, natural ecosystems and biodiversity, social and cultural contexts, economics, and governance. Such research could inform policymaking for all relevant sectors and actors including governments, businesses, and civil society organizations. This approach could also inform mainstreaming health into national strategies and action plans to implement relevant multi-hazard international frameworks (e.g., the New Urban Agenda, the Sendai Framework for Disaster Risk Reduction and the Paris Agreement for Climate, and the Biodiversity Framework), and promoting international collaborations, information sharing, and capacity building. Moreover, the SDGs provide a comprehensive framework for a more integrated and preventive risk reduction approach in health.
- Multi-scalar, understanding historical patterns of planetary health impacts to establish causal relationships from the local to the global and projecting the possible magnitude and pattern of future risks under different development pathways. This knowledge is necessary for designing, implementing, and monitoring solutions to improve population health in the short-, mid-, and long-term.
- Inclusive and equitable by being responsive to intersectional aspects such as gender, age, social status, and ethnicity, in how research is conducted and in how solutions are developed. The intergenerational justice impacts of global environmental health research are considered. Equitable research includes searching for funding structures that enable South-South and North-South cooperation and that aim for diverse representation in research projects.
- Communicated broadly, sharing newly generated knowledge with different audiences. This includes dissemination beyond academia and experimenting with creative communication approaches to inform policy development in adaptation and mitigation.
7. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Appendix B
| No. | Family Name | Name (s) | Affiliation |
|---|---|---|---|
| 1 | Anyamba | Assaf | USRA and NASA Goddard Space Flight Center |
| 2 | Bi | Peng | University of Adelaide, Australia |
| 3 | Boeckmann | Melanie | Bielefeld University, Research Group Environment and Health, Germany |
| 4 | Bowen | Kathryn | Australian National University/University of Melbourne |
| 5 | Capon | Anthony | University of Sydney (Future Earth Health KAN Co-chair) |
| 6 | Charles-Ayinde | Makyba K S | AAAS, Future Earth, National Science Foundation |
| 7 | Cheong | Hae-Kwan | Sungkyunkwan University School of Medicine |
| 8 | Cissé | Guéladio | Swiss Tropical and Public Health Institute |
| 9 | Dasgupta | Purnamita | Institute of Economic Growth, Delhi, India |
| 10 | Daszak | Peter | EcoHealth Alliance (Future Earth GRP oneHEALTH) |
| 11 | Ebi | Kristie L. | University of Washington (Future Earth Health KAN Co-chair) |
| 12 | Gasparatos | Alexandros | The University of Tokyo |
| 13 | Hashizume | Masahiro | Nagasaki University |
| 14 | Honda | Yasushi | University of Tsukuba |
| 15 | Javadi | Firouzeh | Institute of Decision Science for a Sustainable Society, Kyushu University |
| 16 | Kanbara | Sakiko | University of Kochi |
| 17 | Kasuga | Fumiko | Future Earth |
| 18 | Kim | Ho | Seoul National University |
| 19 | Koné | Brama | Centre Suisse de Recherches Scientifiques en Côte d’Ivoire & Université péléforo Gon Coulibaly of Korhogo |
| 20 | Kovats | Sari | London School of Hygiene and Tropical Medicine |
| 21 | Kusuma | Parama Tirta Wulandari Wening | Indonesian Institute of Sciences, Bureau for Financial Planning |
| 22 | Lee | Shihyu | Research Center for Environmental Changes |
| 23 | Lee | Chia-Hsing Jeffery | Center for Sustainability Science, Academia Sinica, and Future Earth-Taipei |
| 24 | Lung | Shih-Chun Candice | Research Center for Environmental Changes, Academia Sinica |
| 25 | Mallee | Hein | Regional Centre for Future Earth in Asia, Research Institute for Humanity and Nature |
| 26 | Maycock | Bruce | Curtin University |
| 27 | Morse | Andy | University of Liverpool |
| 28 | Murakami | Takahiro | Institution of Decision Science for a Sustainable Society, Kyushu University |
| 29 | Mustapha | Adetoun | Nigerian Institute for Medical Research; Imperial College London and International Society for Environmental Epidemiology, Africa Chapter |
| 30 | Nagashima | Miki | Malaria No More Japan |
| 31 | Onofre | Edwin A. Merilles Jr. | The Pacific Community (SPC) |
| 32 | Pongsiri | Montira | Oxford University |
| 33 | Raivio | Kari Olavi | University of Helsinki |
| 34 | Sioen | Giles B. | Future Earth, Institute for Future Initiatives, The University of Tokyo, The United Nations University Institute for the Advanced Study of Sustainability |
| 35 | Sobral | Bruno Walther Santos | One Health Institute, Colorado State University |
| 36 | Suzán | Gerardo | National Autonomous University of Mexico UNAM |
| 37 | Tanimoto | Hiroshi | National Institute for Environmental Studies |
| 38 | Wannous | Chadia | TASW Network, Health KAN Development Team |
| 39 | Watanabe | Chiho | National Institute for Environmental Studies |
| 40 | Wegerdt | Johannah | Green Climate Fund |
| 41 | Wu | Pei-Chih, Peggy | Chang Jung Christian University |
| 42 | Yamauchi | Taro | Hokkaido University/Research Institute for Humanity and Nature |
References
- Steffen, W.; Rockström, J.; Richardson, K.; Lenton, T.M.; Folke, C.; Liverman, D.; Summerhayes, C.P.; Barnosky, A.D.; Cornell, S.E.; Crucifix, M.; et al. Trajectories of the Earth System in the Anthropocene. Proc. Natl. Acad. Sci. USA 2018, 115, 8252–8259. [Google Scholar] [CrossRef] [PubMed]
- Whitmee, S.; Haines, A.; Beyrer, C.; Boltz, F.; Capon, A.G.; Dias, B.F.D.S.; Ezeh, A.; Frumkin, H.; Gong, P.; Head, P.; et al. Safeguarding human health in the Anthropocene epoch: Report of The Rockefeller Foundation–Lancet Commission on planetary health. Lancet 2015, 386, 1973–2028. [Google Scholar] [CrossRef]
- Steffen, W.; Richardson, K.; Rockström, J.; Cornell, S.E.; Fetzer, I.; Bennett, E.M.; Biggs, R.; Carpenter, S.R.; Vries, W.D.; Wit, C.A.D.; et al. Planetary boundaries: Guiding human development on a changing planet. Science 2015, 347, 1259855. [Google Scholar] [CrossRef]
- Horton, R.; Lo, S. Planetary health: A new science for exceptional action. Lancet 2015, 386, 1921–1922. [Google Scholar] [CrossRef]
- Lenton, T.M.; Rockström, J.; Gaffney, O.; Ramstorf, S.; Richardson, K.; Steffen, W.; Schellnhuber, H.J. Climate tipping points—Too risky to bet against. Nature 2019, 575, 592–595. [Google Scholar] [CrossRef] [PubMed]
- Watts, N.; Amann, M.; Arnell, N.; Ayeb-Karlsson, S.; Belesova, K.; Berry, H.; Bouley, T.; Boykoff, M.; Byass, P.; Cai, W.; et al. The 2018 report of the Lancet Countdown on health and climate change: Shaping the health of nations for centuries to come. Lancet 2018, 392, 2479–2514. [Google Scholar] [CrossRef]
- Ebi, K.L.; Semenza, J.C.; Rocklöv, J. Current medical research funding and frameworks are insufficient to address the health risks of global environmental change. Environ. Health A Glob. Access Sci. Source 2016, 15, 108. [Google Scholar] [CrossRef]
- Green, D.; Pitman, A.; Barnet, A.; Kaldor, J.; Doherty, P.; Stanley, F. Advancing Australia’s role in climate change and health research. Nat. Clim. Chang. 2017, 7, 103–106. [Google Scholar] [CrossRef]
- Our History. Available online: https://futureearth.org/about/history/ (accessed on 26 November 2020).
- IPSP. Summary. Rethinking society for the 21st Century. In 2018 Report of the Inter. Panel Social Progress; Cambridge University Press: Cambridge, UK, 2018. [Google Scholar]
- Fosu, A.K. Growth, inequality and poverty in Sub-Saharan Africa: Recent progress in a global context. Oxf. Dev. Stud. 2014, 43, 44–59. [Google Scholar] [CrossRef]
- Dollar, D.; Kraay, A. Growth is Good for the Poor. J. Econ. Growth 2002, 7, 195–225. [Google Scholar] [CrossRef]
- Dollar, D.; Kleineberg, T.; Kraay, A. Growth still is good for the poor. Eur. Econ. Rev. 2016, 81, 68–85. [Google Scholar] [CrossRef]
- Watts, N.N.; Adger, W.M.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and climate change: Policy responses to protect public health. Lancet 2015, 386, 1861–1914. [Google Scholar] [CrossRef]
- WHO. WHO Guidance to Protect Health from Climate Change through Health Adaptation Planning; World Health Organization: Geneva, Switzerland, 2014. [Google Scholar]
- Stiglitz, J.E.; Sen, A.; Fitoussi, J.P. Report by the Commission on the Measurement of Economic Performance and Social Progress. 2009. Available online: http://ec.europa.eu/eurostat/documents/118025/118123/Fitoussi+Commission+report (accessed on 26 November 2020).
- Stiglitz, J.E.; Sen, A.; Fitoussi, J.P. Mismeasuring Our Lives: Why GDP does not Add Up; Final Report of the WHO Commission on Social Determinants of Health; The New Press: New York, NY, USA, 2010. [Google Scholar]
- Sud, S.R.; Brenner, J.E.; Shaffer, E.R. Trading away health: The influence of trade policy on youth tobacco control. J. Pediatrics 2015, 166, 1303–1307. [Google Scholar] [CrossRef] [PubMed]
- Ostrom, E. A Polycentric Approach for Coping with Climate Change. Ann. Econ. Financ. 2014, 15, 71–108. [Google Scholar]
- Settele, J.; Díaz, S.; Brondizio, E.; Daszak, P. Stimulus Measures Must Save Lives, Protect. Livelihoods, and Safeguard Nature to Reduce the Risk of Future Pandemics. Available online: https://ipbes.net/covid19stimulus (accessed on 26 November 2020).
- Galor, O. Unified Growth Theory; Princeton University Press: Princeton, NJ, USA, 2011. [Google Scholar]
- Cervellati, M.; Sunde, U. Human capital formation, life expectancy, and the process of development. Am. Econ. Rev. 2005, 95, 1653–1672. [Google Scholar] [CrossRef] [PubMed]
- Croix, D.D.L.; Licandro, O. The Child is father of the man: Implications for the Demographic Transition. Econ. J. 2012. [Google Scholar] [CrossRef]
- Smith, K.R.; Frumkin, H.; Balakrishnan, K.; Butler, C.D.; Chafe, Z.A.; Fairlie, I.; Kinney, P.; Kjellstrom, T.; Mauzerall, D.L.; McKone, T.E.; et al. Energy and human health. Annu. Rev. Public Health 2013, 34, 159–188. [Google Scholar] [CrossRef]
- Perera, F. Pollution from fossil-fuel combustion is the leading environmental threat to global pediatric health and equity: Solutions exist. Int. J. Env. Res. Public Health 2017, 15, 16. [Google Scholar] [CrossRef]
- Godri, K.J.; Harrison, R.M.; Evans, T.; Baker, T.; Dunster, C.; Mudway, I.S.; Kelly, F.J. Increased oxidative burden associated with traffic component of ambient particulate matter at roadside and urban background schools sites in London. PLoS ONE 2011, 6, e21961. [Google Scholar] [CrossRef]
- Kheirbek, I.; Haney, J.; Douglas, S.; Ito, K.; Matte, T. The contribution of motor vehicle emissions to ambient fine particulate matter public health impacts in New York City: A health burden assessment. Environ. Health 2016, 15. [Google Scholar] [CrossRef]
- Pieprzyk, B.; Hilje, P.R. Influence of methane emissions on the GHG emissions of fossil fuels. Biofuels Bioprod. Bioref. 2018, 13, 535–551. [Google Scholar] [CrossRef]
- Landrigan, P.J.; Fuller, R.; Acosta, N.J.R.; Adeyi, O.; Arnold, R.; Basu, N.N.; Baldé, A.B.; Bertollini, R.; Bose-O’Reilly, S.; Boufford, J.I.; et al. The Lancet Commission on pollution and health. Lancet 2018, 391, 462–512. [Google Scholar] [CrossRef]
- Gordon, S.B.; Bruce, N.G.; Grigg, J.; Hibberd, P.L.; Kurmi, O.P.; Lam, K.-B.H.; Mortimer, K.; Asante, K.P.; Balakrishnan, K.; Balmes, J.; et al. Respiratory risks from household air pollution in low and middle income countries. Lancet Respir. Med. 2014, 2, 823–860. [Google Scholar] [CrossRef]
- World Health Organization. Burning Opportunity: Clean Household Energy for Health, Sustainable Development and Well-Being of Women and Children. 2016. Available online: https://apps.who.int/iris/bitstream/handle/10665/204717/9789241565233_eng.pdf;jsessionid=4F3BA629F3397497C2D8DDB4B38583B6?sequence=1 (accessed on 23 November 2020).
- Chang, K.M.; Hess, J.J.; Balbus, J.M.; Buonocore, J.J.; Cleveland, D.A.; Grabow, M.L.; Neff, R.; Saari, R.K.; Tessum, C.W.; Wilkinson, P.; et al. Ancillary health effects of climate mitigation scenarios as drivers of policy uptake: A review of air quality, transportation and diet co-benefits modeling studies. Environ. Res. Lett. 2017, 12, 113001. [Google Scholar] [CrossRef]
- Gao, Y.; Gao, X.; Zhang, X. The 2 °C global temperature target and the evolution of the long-term goal of addressing climate change—From the United Nations Framework Convention on Climate Change to the Paris Agreement. Engineering 2017, 3, 272–278. [Google Scholar] [CrossRef]
- McMichael, A.J. The urban environment and health in a world of increasing globalization: Issues for developing countries. Bull. World Health Organ. 2000, 78, 1117–1126. [Google Scholar]
- United Nations Department of Economic and Social Affairs Population Division. World Urbanization Prospects: The 2015 Revision; United Nations: New York, NY, USA, 2015. [Google Scholar]
- Swilling, M.; Robinson, B.; Marvin, S.; Hodson, M. City-Level Decoupling: Urban. Resource Flows and the Governance of Infrastructure Transitions. Summary for Policy Makers; UNEP: Nairobi, Kenya, 2013. [Google Scholar]
- WHO. Health as the Pulse of the New Urban Agenda. In United Nations Conference on Housing and Sustainable Urban Development; World Health Organization: Quito, Ecuador, 2017. [Google Scholar]
- Eckert, S.; Kohler, S. Urbanization and Health in Developing Countries: A Systematic Review. World Health Popul. 2014, 15, 7–20. [Google Scholar] [CrossRef]
- Rao, K.D.; Peters, D.H. Urban health in India: Many challenges, few solutions. Lancet Glob. Health 2015, 3, 729–730. [Google Scholar] [CrossRef]
- Li, X.; Song, J.; Lin, T.; Dixon, J.; Zhang, G.; Ye, H. Urbanization and health in China, thinking at the national, local and individual levels. Environ. Health 2016, 15, 113–123. [Google Scholar] [CrossRef]
- Oni, T.; Smith, W.; Matzopoulos, R.; Adams, J.H.; Pentecost, M.; Rother, H.-A.A.; Albertyn, Z.; Behroozi, F.; Alaba, O.; Kaba, M.; et al. Urban Health Research in Africa: Themes and Priority Research Questions. J. Urban. Health 2016, 93, 722–730. [Google Scholar] [CrossRef]
- Gatzweiler, F.; Fu, B.; Rozenblat, C.; Su, H.J.J.; Luginaah, I.; Corburn, J.; Boufford, J.I.; Valdes, J.V.; Nguendo-Yongsi, B.; Howden-Chapman, P.; et al. COVID-19 reveals the systemic nature of urban health globally. Cities Health 2020, 1–5. [Google Scholar] [CrossRef]
- UNDRR. Global Assessment Report on Disaster Risk Reduction; United Nations Office for Disaster Risk Reduction (UNDRR): Geneva, Switzerland, 2019. [Google Scholar]
- Koomen, E.; Diogo, V. Assessing potential future urban heat island patterns following climate scenarios, socio-economic developments and spatial planning strategies. Mitig. Adapt. Strat. Glob. Chang. 2017, 22, 287–306. [Google Scholar] [CrossRef] [PubMed]
- World Economic Forum. Global Risk Report 2019. Available online: https://www.weforum.org/reports/the-global-risks-report-2019 (accessed on 26 November 2020).
- Jevrejeva, S.; Jackson, L.P.; Riva, R.E.; Grinsted, A.; Moore, J.C. Coastal Sea Level Rise with Warming above 2 °C. Proc. Natl. Acad. Sci. USA 2016, 113, 13342–13347. [Google Scholar] [CrossRef] [PubMed]
- Ramirez-Rubio, O.; Daher, C.; Fanjul, G.; Gascon, M.; Mueller, N.; Pajín, L.; Plasencia, A.; Rojas-Rueda, D.; Thondoo, M.; Nieuwenhuijsen, M.J. Urban health: An example of a “health in all policies” approach in the context of SDGs implementation. Glob. Health 2019, 15, 87. [Google Scholar] [CrossRef] [PubMed]
- IFRC. Leaving No One Behind; World Disasters Report; IFRC: Geneva, Switzerland, 2018. [Google Scholar]
- UN HABITAT. Cities 2030, Cities for All: Implementing the New Urban. Agenda; UN HABITAT: Nairobi, Kenya, 2017. [Google Scholar]
- UN HABITAT. Working for a Better Urban. Future; Annual Report UN HABITAT: Nairobi, Kenya, 2018. [Google Scholar]
- WHO. Communicable Diseases following Natural Disasters—Risk Assessment and Priority Interventions. 2006. Available online: https://www.who.int/diseasecontrol_emergencies/publications/who_cds_ntd_dce_2006.4/en/ (accessed on 26 November 2020).
- Anyamba, A.; Chretien, J.-P.; Britch, S.C.; Soebiyanto, R.P.; Small, J.L.; Jepsen, P.; Forshey, B.M.; Sanchez, J.L.; Smith, R.D.; Harris, R.; et al. Global Disease Outbreaks Associated with the 2015-2016 El Niño Event. Nat. Sci. Rep. 2019, 9, 1930. [Google Scholar] [CrossRef] [PubMed]
- Newbold, T.; Hudson, L.N.; Arnell, A.P.; Contu, S.; Palma, A.D.; Ferrier, S.; Hill, S.L.L.; Hoskins, A.J.; Lysenko, I.; Phillips, H.R.P.; et al. Has land use pushed terrestrial biodiversity beyond the planetary boundary? A global assessment. Science 2016, 353, 288–291. [Google Scholar] [CrossRef]
- Scholes, R.; Montanarella, L.; Brainich, A.; Barger, N.; Brink, B.; Cantele, M.; Fisher, J.; Gardner, T.; Holland, T.; Kohler, F.; et al. IPBES: Summary for Policymakers of the Assessment Report on Land Degradation and Restoration of the Intergovernmental Science Policy Platform on Biodiversity and Ecosystem Services. 2018. Available online: https://ipbes.net/sites/default/files/spm_3bi_ldr_digital.pdf (accessed on 23 November 2020).
- Costanza, R.; Groot, R.D.; Sutton, P.; Ploeg, S.V.D.; Anderson, S.J.; Kubiszewski, I.; Farber, S.; Turner, R.K. Changes in the global value of ecosystem services. Glob. Environ. Chang. 2014, 26, 152–158. [Google Scholar] [CrossRef]
- Nkonya, E.; Anderson, W.; Kato, E.; Koo, J.; Mirzabaev, A.; von Braun, J. Economics of Land Degradation and Improvement—A Global Assessment for Sustainable Development; Springer International Publishing: Cham, Switzerland, 2016. [Google Scholar]
- Loh, E.H.; Zambrana-Torrelio, C.; Olival, K.J.; Bogich, T.L.; Johnson, C.K.; Mazet, J.A.K.; Karesh, W.; Daszak, P. Targeting transmission pathways for emerging zoonotic disease surveillance and control. Vector Borne Zoonotic Dis. 2015, 15, 432–437. [Google Scholar] [CrossRef]
- Schmid, K.A.; Ostfeld, R.S. Biodiversity and the dilution effect in disease ecology. Ecology 2001, 82, 609–619. [Google Scholar] [CrossRef]
- Vittor, A.Y.; Gilman, R.H.; Tielsch, J.; Glass, G.; Shields, T.I.M.; Lozano, W.S.; Patz, J.A. The effect of deforestation on the human biting rate of Anopheles Darlingi, the primary vector of Falciparum malaria in the Peruvian Amazon. Am. J. Trop. Med. Hyg. 2006, 74, 3–11. [Google Scholar] [CrossRef]
- Willett, W.; Rockstrom, J.; Loken, B.; Springmann, M.; Lang, T.; Vermeulen, S.; Garnett, T.; Tilman, D.; De Clerck, F.; Wood, A.; et al. Food in the Anthropocene: The EAT—Lancet Commission on healthy diets from sustainable food systems. Lancet 2019, 393, 447–492. [Google Scholar] [CrossRef]
- FAO. State of Food Security and Nutrition in the World 2019. Available online: http://www.fao.org/3/ca5162en/ca5162en.pdf (accessed on 26 November 2020).
- FAO; IFAD; UNICEF; WFP; WHO. The State of Food Security and Nutrition in the World 2020. In Transforming Food Systems for Affordable Healthy Diets; FAO: Rome, Italy, 2020. [Google Scholar]
- HLPE. Nutrition and Food Systems. In A Report by the High Level Panel of Experts on Food Security and Nutrition of the Committee on World Food Security; FAO: Rome, Italy, 2017. [Google Scholar]
- Kearney, J. Food consumption: Trends and driers. Philos. Trans. R. Soc. B 2010, 365, 2793–2804. [Google Scholar] [CrossRef] [PubMed]
- IPBES. Global Assessment Report on Biodiversity and Ecosystem Services of the Intergovernmental Science-Policy Platform on Biodiversity and Ecosystem Services; Brondizio, E.S., Settele, J., Díaz, S., Ngo, H.T., Eds.; IPBES Secretariat: Bonn, Germany, 2019. [Google Scholar]
- Hallström, E.; Annika, C.K.; Börjesson, P. Environmental impact of dietary change: A systematic review. J. Clean. Prod. 2015, 91, 1–11. [Google Scholar] [CrossRef]
- Springmann, M.; Godfray, H.C.; Rayner, M.; Scarborough, P. Analysis and valuation of the health and climate change cobenefits of dietary change. Proc. Natl. Acad. Sci. USA 2016, 113, 4146–4151. [Google Scholar] [CrossRef]
- Tilman, D.; Clark, M. Global diets link environmental sustainability and human health. Nature 2014, 515, 518–522. [Google Scholar] [CrossRef]
- Hoegh-Guldberg, O.; Jacob, D.; Bindi, M.; Brown, S.; Camilloni, I.; Diedhiou, A.; Djalante, R.; Ebi, K.; Engelbrecht, F.; Guiot, J.; et al. Global Warming of 1.5 °C: An. IPCC Special Report; IPCC Secretariat: Geneva, Switzerland, 2018; pp. 175–311. [Google Scholar]
- Thrupp, L.N. Linking agricultural biodiversity and food security: The valuable role of agrobiodiversity for sustainable agriculture. Int. Aff. 2002, 76, 265–281. [Google Scholar] [CrossRef]
- FAO. Agricultural Biodiversity, Multifunctional Character of Agriculture and Land Conference; 1999 Background Paper 1; FAO: Maastricht, The Netherlands, 1999. [Google Scholar]
- Bhandari, H.R.; Bhanu, A.N.; Srivastava, K.; Singh, M.N. Assessment of Genetic Diversity in Crop Plants—An Overview. Adv. Plants Agric. Res. 2017, 7, 255. [Google Scholar] [CrossRef]
- Adjimoti, G.O.; Kwadzo, G.T. Crop diversification and household food security status: Evidence from rural Benin. Agric. Food Secur. 2018, 7, 82. [Google Scholar] [CrossRef]
- Newman, D.J. Natural products as leads to potential drugs: An old process or the new hope for drug discovery? J. Med. Chem. 2008, 51, 2589–2599. [Google Scholar] [CrossRef]
- Beghyn, T.; Deprez-Poulain, R.; Willand, N.; Folleas, B.; Deprez, B. Natural compounds: Leads or ideas? Bioinspired molecules for drug discovery. Chem. Biol. Drug Des. 2008, 72, 3–15. [Google Scholar] [CrossRef]
- Desai, M.C.; Chackalamannil, S. Rediscovering the role of natural products in drug discovery. Curr. Opin. Drug Discov. Dev. 2008, 11, 436–437. [Google Scholar]
- Keesing, F.; Belden, L.K.; Daszak, P.; Dobson, A.; Harvell, C.D.; Holt, R.D.; Hudson, P.; Jolles, A.; Jones, K.E.; Mitchell, C.E.; et al. Impacts of biodiversity on the emergence and transmission of infectious diseases. Nature 2010, 468, 647–652. [Google Scholar] [CrossRef] [PubMed]
- Ostfeld, R.S.; Keesing, F. Effects of host diversity on infectious disease. Annu. Rev. Ecol. Evol. Syst. 2012, 43, 157–182. [Google Scholar] [CrossRef]
- Dobson, A. Population dynamics of pathogens with multiple host species. Am. Nat. 2004, 164, S64–S78. [Google Scholar] [CrossRef] [PubMed]
- Logiudice, K.; Duerr, S.T.K.; Newhouse, M.J.; Schmidt, K.A.; Killilea, M.E.; Ostfeld, R.S. Impact of host community composition on Lyme disease risk. Ecology 2008, 89, 2841–2849. [Google Scholar] [CrossRef]
- Roche, B.; Dobson, A.P.; Guégan, J.-F.; Rohani, P. Linking community and disease ecology: The impact of biodiversity on pathogen transmission. Philos. Trans. R. Soc. B Biol. Sci. 2012, 367, 2807–2813. [Google Scholar] [CrossRef]
- Tersago, K.; Schreurs, A.; Linard, C.; Verhagen, R.; Dongen, S.V.; Leirs, H. Population, environmental, and community effects on local bank vole (Myodes glareolus) puumala virus infection in an area with low human incidence. Vector Borne Zoonotic Dis. 2008, 8, 235–244. [Google Scholar] [CrossRef]
- Suzán, G.; García-Peña, G.E.; Castro-Arellano, I.; Rico, O.; Rubio, A.V.; Tolsa, M.J.; Roche, B.; Hosseini, P.R.; Rizzoli, A.; Murray, K.A.; et al. Metacommunity and phylogenetic structure determine wildlife and zoonotic infectious disease patterns in time and space. Ecol. Evol. 2015, 5, 865–873. [Google Scholar] [CrossRef]
- Swaddle, J.P.; Calos, S.E. Increased avian diversity is associated with lower incidence of human West Nile infection: Observation of the dilution effect. PLoS ONE 2008, 3, e2488. [Google Scholar] [CrossRef]
- Johnson, P.T.J.; Preston, D.L.; Hoverman, J.T.; Richgels, K.L.D. Biodiversity decreases disease through predictable changes in host community competence. Nature 2013, 494, 230–233. [Google Scholar] [CrossRef]
- Ostfeld, R.S.; Keesing, F. Biodiversity series: The function of biodiversity in the ecology of vector-borne zoonotic diseases. Can. J. Zool. 2000, 78, 2061–2078. [Google Scholar] [CrossRef]
- Gibb, R.; Redding, D.W.; Chin, K.Q.; Donnelly, C.A.; Blackburn, T.M.; Newbold, T.; Jones, K.E. Zoonotic host diversity increases in human-dominated ecosystems. Nature 2020, 584, 398–402. [Google Scholar] [CrossRef] [PubMed]
- Doherty, T.S.; Glen, A.S.; Nimmo, D.G.; Ritchie, E.G.; Dickman, C.R. Invasive predators and global biodiversity loss. Proc. Natl. Acad. Sci. USA 2016, 113, 11261–11265. [Google Scholar] [CrossRef] [PubMed]
- Hooper, D.U.; Adair, E.C.; Cardinale, B.J.; Byrnes, J.E.K.; Hungate, B.A.; Matulich, K.L.; Gonzalez, A.; Duffy, J.E.; Gamfeldt, L.; O’Connor, M.I. A global synthesis reveals biodiversity loss as a major driver of ecosystem change. Nature 2012, 486, 105–108. [Google Scholar] [CrossRef]
- Doherty, T.S.; Davis, R.A.; Etten, E.J.B.V.; Algar, D.; Collier, N.; Dickman, C.R.; Edwards, G.; Masters, P.; Palmer, R.; Robinson, S. A continental-scale analysis of feral cat diet in Australia. J. Biogeogr. 2015, 42, 964–975. [Google Scholar] [CrossRef]
- Harris, D.B.; Macdonald, D.W. Interference competition between introduced black rats and endemic Galápagos rice rats. Ecology 2007, 88, 2330–2344. [Google Scholar] [CrossRef]
- Wyatt, K.B.; Campos, P.F.; Gilbert, M.T.P.; Kolokotronis, S.-O.; Hynes, W.H.; Desalle, R.; Ball, S.J.; Daszak, P.; Macphee, R.D.E.; Greenwood, A.D. Correction: Historical mammal extinction on Christmas Island (Indian Ocean) correlates with introduced infectious disease. PLoS ONE 2008, 3, e3602. [Google Scholar] [CrossRef]
- Rubio, A.V.; Ávila-Flores, R.; Suzán, G. Responses of small mammals to habitat fragmentation: Epidemiological considerations for rodent-borne Hantaviruses in the Americas. EcoHealth 2014, 11, 526–533. [Google Scholar] [CrossRef]
- Fleming, L.; Maycock, B.; White, M.; Depledge, M. Fostering human health through ocean sustainability in the 21st century. People Nat. 2019, 1, 276–283. [Google Scholar] [CrossRef]
- FAO. The State of World Fisheries and Aquaculture 2020. In Sustainability in Action; FAO: Rome, Italy, 2020. [Google Scholar]
- Allen, J. Marine Environment and Human health: An Overview. In Issues in Environmental Science & Technology; Hester, R., Harrison, R., Eds.; London Royal Society of Chemistry: London, UK, 2011. [Google Scholar]
- Cicin-Sain, B.; Berna, P.; Vandeweerd, V.; Belfiore, S.; Goldstein, K. A Guide to Oceans, Coasts and Islands at the World Summit on Sustainable Development; UNESCO: Paris, France, 2002. [Google Scholar]
- Leonard, A.F.; Zhang, L.; Balfour, A.J.; Garside, R.; Hawkey, P.M.; Murray, A.K.; Ukoumunne, O.C.; Gaze, W.H. Exposure to and colonisation by antibiotic-resistant E. coli in UK coastal water users: Environmental surveillance, exposure assessment, and epidemiological study (Beach Bum Survey). Environ. Int. 2018, 114, 326–333. [Google Scholar] [CrossRef]
- Sunderland, E.M.; Li, M.; Bullard, K. Decadal changes in the edible supply of seafood and methylmercury exposure in the United States. Environ. Health Perspect. 2018, 126, 17006. [Google Scholar] [CrossRef] [PubMed]
- Paz, S.; Rubio, C.; Frías, I.; Gutiérrez, A.J.; González-Weller, D.; Revert, C.; Hardisson, A. Metal concentrations in wild-harvested phaeophyta seaweed from the Atlantic Ocean (Canary Islands, Spain). J. Food Prot. 2018, 81, 1165–1170. [Google Scholar] [CrossRef] [PubMed]
- Woodall, L.C.; Sanchez-Vidal, A.; Canals, M.; Paterson, G.L.J.; Coppock, R.; Sleight, V.; Calafat, A.; Rogers, A.D.; Narayanaswamy, B.E.; Thompson, R.C. The deep sea is a major sink for microplastic debris. R. Soc. Open Sci. 2014, 1, 140317. [Google Scholar] [CrossRef] [PubMed]
- Lamb, J.B.; Willis, B.L.; Fiorenza, E.A.; Couch, C.S.; Howard, R.; Rader, D.N.; True, J.D.; Kelly, L.A.; Ahmad, A.; Jompa, J.; et al. Plastic waste associated with disease on coral reefs. Science 2018, 359, 460–462. [Google Scholar] [CrossRef] [PubMed]
- Spijkers, J.; Morrison, T.H.; Blasiak, R.; Cumming, G.S.; Osborne, M.; Watson, J.; Österblom, H. Marine fisheries and future ocean conflict. Fish. Fish. 2018, 19, 798–806. [Google Scholar] [CrossRef]
- Costello, C.; Cao, L.; Gelcich, S.; Cisneros-Mata, M.Á.; Free, C.M.; Froehlich, H.E.; Golden, C.D.; Ishimura, G.; Maier, J.; Macadam-Somer, I.; et al. The future of food from the sea. Nature 2020, 1–6. [Google Scholar] [CrossRef] [PubMed]
- International Energy Agency. Energy Air Pollution; World Energy Outlook Special Report 2016. Available online: http://pure.iiasa.ac.at/id/eprint/13467/1/WorldEnergyOutlookSpecialReport2016EnergyandAirPollution.pdf (accessed on 26 November 2020).
- Wilkinson, P.; Smith, K.R.; Joffe, M.; Haines, A. A global perspective on energy: Health effects and injustices. Lancet 2007, 370, 965–978. [Google Scholar] [CrossRef]
- Beggs, P.J. Adaptation to impacts of climate change on aeroallergens and allergic respiratory diseases. Int. J. Environ. Res. Public Health 2010, 7, 3006–3021. [Google Scholar] [CrossRef]
- WHO (2018) Diarrheal Disease. Available online: https://www.who.int/news-room/fact-sheets/detail/diarrhoeal-disease (accessed on 26 November 2020).
- WHO (2018) Drinking-Water. Available online: https://www.who.int/news-room/fact-sheets/detail/drinking-water (accessed on 26 November 2020).
- UN-Water (2018) Water and Climate Change. Available online: http://www.unwater.org/water-facts/climate-change/ (accessed on 26 November 2020).
- Khalid, S.; Shahid, M.; Bibi, I.; Sarwar, T.; Shah, A.H.; Niazi, N.K. A review of environmental contamination and health risk assessment of wastewater use for crop irrigation with a focus on low and high-income countries. Int. J. Environ. Res. Public Health 2018, 15, 895. [Google Scholar] [CrossRef]
- Jaramillo, M.F.; Restrepo, I. Wastewater reuse in agriculture: A review about its limitations and benefits. Sustainability 2017, 9, 1734. [Google Scholar] [CrossRef]
- Yapo, R.I.; Koné, B.; Bonfoh, B.; Cissé, G.; Zinsstag, J.; Nguyen-Viet, H. Quantitative microbial risk assessment related to urban wastewater and lagoon water reuse in Abidjan, Côte d’Ivoire. J. Water Health 2013, 12, 301–309. [Google Scholar] [CrossRef] [PubMed]
- Mpandeli, S.; Naidoo, D.; Mabhaudhi, T.; Nhemachena, C.; Nhamo, L.; Liphadzi, S.; Hlahla, S.; Modi, A.T. Climate change adaptation through the water-energy-food nexus in Southern Africa. Int. J. Environ. Res. Public Health 2018, 15, 2306. [Google Scholar] [CrossRef] [PubMed]
- Nkhonjera, G.K.; Dinka, M.O. Significance of direct and indirect impacts of climate change on groundwater resources in the Olifants River basin: A review. Glob. Planet. Chang. 2017, 158, 72–82. [Google Scholar] [CrossRef]
- Ahmed, T.; Scholz, M.; Al-Faraj, F.; Niaz, W. Water-related impacts of climate change on agriculture and subsequently on public health: A review for generalists with particular reference to Pakistan. Int. J. Environ. Res. Public Health 2016, 13, 1051. [Google Scholar] [CrossRef]
- Tong, S.; Berry, H.L.; Ebi, K.; Bambrick, H.; Hu, W.; Green, D.; Hanna, E.; Wang, Z.; Butler, C.D. Climate change, food, water and population health in China. Bull. World Health Organ. 2016, 94, 759–765. [Google Scholar] [CrossRef]
- Faour-Klingbeil, D.; Todd, E.C.D. The impact of climate change on raw and untreated wastewater use for agriculture, especially in arid regions: A review. Foodborne Pathog. Dis. 2018, 15, 61–72. [Google Scholar] [CrossRef]
- Hutton, G.; Chase, C. The knowledge base for achieving the sustainable development goal targets on water supply, sanitation and hygiene. Int. J. Environ. Res. Public Health 2016, 13, 536. [Google Scholar] [CrossRef]
- Howard, G.; Calow, R.; Macdonald, A.; Bartram, J. Climate change and water and sanitation: Likely impacts and emerging trends for action. Annu. Rev. Environ. Resour. 2016, 41, 253–276. [Google Scholar] [CrossRef]
- Smith, K.R.; Woodward, A.; Campbell-Lendrum, D.; Chadee, D.D.; Honda, Y.; Liu, Q.Y.; Olwoch, J.M.; Revich, B.; Sauerborn, R.; Aranda, C.; et al. Human health: Impacts, adaptation, and co-benefits. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part A: Global and Sectoral Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Cambridge University Press: Cambridge, UK, 2014; pp. 709–754. [Google Scholar]
- Kimbrough, D.E. Changes in temperature and rainfall as a result of local climate change in Pasadena, California. Hydrology 2018, 5, 25. [Google Scholar] [CrossRef]
- Kimbrough, D.E. Impact of local climate change on drinking water quality in a distribution system. Water Qual. Res. J. 2019, 54, 179–192. [Google Scholar] [CrossRef]
- United Nations General Assembly the Human Rights to Safe Drinking Water and Sanitation. 2015. Available online: https://undocs.org/A/RES/70/169 (accessed on 26 November 2020).
- Oates, N.; Ross, I.; Calow, R.; Carter, R.; Doczi, J. Adaptation to Climate Change in Water, Sanitation and Hygiene: Assessing Risks and Appraising Options in AFRICA. 2014. Available online: https://www.odi.org/publications/8154-adaptation-climate-change-water-sanitation-and-hygiene-assessing-risks-appraising-options-africa (accessed on 26 November 2020).
- Depledge, M.H.; White, M.P.; Maycock, D.; Fleming, L.E. Time and tide. BMJ 2019, 366, 14671. [Google Scholar] [CrossRef] [PubMed]
- Poussin, J.K.; Bubeck, P.; Aerts, J.C.J.H.; Ward, P. Impact of Climate Change, Land Use Change, and Residential Mitigation Measures on Damage and Risk Assessment 2012. Available online: https://edepot.wur.nl/319652 (accessed on 26 November 2020).
- World Health Organization. Protecting Health from Climate Change: Vulnerability and Adaptation Assessment. 2013. Available online: https://www.who.int/globalchange/publications/Final_Climate_Change.pdf (accessed on 26 November 2020).
- World Health Organization. Piloting Climate Change Adaptation to Protect Human Health 2004. Available online: https://www.who.int/globalchange/climate/gefproject/en/ (accessed on 26 November 2020).
- WHO Operational Framework for Building Climate Resilient Health Systems. 2015. Available online: https://www.who.int/globalchange/publications/building-climate-resilient-health-systems/en/ (accessed on 26 November 2020).
- Ceccato, P.; Ramirez, B.; Manyangadze, T.; Gwakisa, P.; and Thomson, M.C. Data and tools to integrate climate and environmental information into public health. Infect. Dis. Poverty 2018, 7, 126. [Google Scholar] [CrossRef] [PubMed]
- Nuttall, M. Tipping points and the human world: Living with change and thinking about the future. Ambio 2012, 41, 96–105. [Google Scholar] [CrossRef] [PubMed]
- TAR. Climate Change 2001: Impacts, Adaptation, and Vulnerability. 2001. Available online: https://www.ipcc.ch/report/ar3/wg2/ (accessed on 26 November 2020).
- World Bank. Climate-Smart Healthcare: Low-Carbon and Resilience Strategies for the Health Sector; World Bank: Washington, DC, USA, 2017; Available online: https://openknowledge.worldbank.org/handle/10986/27809 (accessed on 26 November 2020).
- WHO. Urban Green Space Interventions and Health: A Review of Impacts and Effectiveness. 2017. Available online: https://www.euro.who.int/__data/assets/pdf_file/0010/337690/FULL-REPORT-for-LLP.pdf (accessed on 23 November 2020).
- Ebikeme, C.; Gatzweiler, F.; Oni, T.; Liu, J.; Oyuela, A.; Siri, J. Xiamen Call for Action: Building the Brain of the City-Universal Principles of Urban Health. J. Urban. Health Bull. N. Y. Acad. Med. 2019, 96, 507–509. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Communicating Risk in Public Health Emergencies: A WHO Guideline for Emergency Risk Communication (ERC) Policy and Practice. 2017. Available online: https://apps.who.int/iris/bitstream/handle/10665/259807/9789241550208-eng.pdf?sequence=2 (accessed on 26 November 2020).
- Walker, R.; Hassall, J.; Chaplin, S.; Congues, J.; Bajayo, R.; Mason, W. Health promotion interventions to address climate change using a primary health care approach: A literature review. Health Promot. J. Aust. 2011, 22, 6–12. [Google Scholar] [CrossRef]
- Kreslake, J.M.; Sarfaty, M.; Roser-Renouf, C.; Leiserowitz, A.A.; Maibach, E.W. The critical roles of health professionals in climate change prevention and preparedness. Am. J. Public Health 2018, 108, S68–S69. [Google Scholar] [CrossRef]
- Buonocore, J.J.; Luckow, P.; Norris, G.; Spengler, J.D.; Biewald, B.; Fisher, J.; Levy, J.I. Health and climate benefits of different energy-efficiency and renewable energy choices. Nat. Clim Chang. 2015, 6, 100–105. [Google Scholar] [CrossRef]
- Rosenthal, J.; Balakrishnan, K.; Bruce, N.; Chambers, D.; Graham, J.; Jack, D.; Kline, L.; Masera, O.; Mehta, S.; Mercado, I.R.; et al. Implementation science to accelerate clean cooking for public health. Environ. Health Perspect 2017, 125, 3–7. [Google Scholar] [CrossRef]
- Haines, A.; McMichael, A.J.; Smith, K.R.; Roberts, I.; Woodcock, J.; Markandya, A.; Armstrong, B.G.; Campbell-Lendrum, D.; Dangour, A.D.; Davies, M.; et al. Public health benefits of strategies to reduce greenhouse-gas emissions: Overview and implications for policy makers. Lancet 2009, 374, 2104–2114. [Google Scholar] [CrossRef]
- Smith, K.R.; Jerrett, M.; Anderson, H.R.; Burnett, R.T.; Stone, V.; Derwent, R.; Atkinson, R.W.; Cohen, A.; Shonkoff, S.B.; Krewski, D.; et al. Public health benefits of strategies to reduce greenhouse-gas emissions: Health implications of short-lived greenhouse pollutants. Lancet 2009, 374, 2091–2103. [Google Scholar] [CrossRef]
- UNEP. The Adaptation Gap Report; United Nations Environment Programme: Nairobi, Kenya, 2018. [Google Scholar]
- Bowen, K.; Ebi, K. Governing the health risks of climate change: Towards multi-sector responses. Curr. Opin. Environ. Sustain. 2015, 12, 80–85. [Google Scholar] [CrossRef]
- Buse, C.G.; Smith, M.; Silva, D.S. Attending to scalar ethical issues in emerging approaches to environmental health research and practice. Monash Bioeth. Rev. 2018, 37, 4–21. [Google Scholar] [CrossRef] [PubMed]
- Haines, A.; Ebi, K. The imperative for climate action to protect health. N. Engl. J. Med. 2019, 380, 263–273. [Google Scholar] [CrossRef] [PubMed]
- Harris, F.; Lyon, F. Transdisciplinary Environmental Research: A Review of Approaches to Knowledge Co-Production. 2014. Available online: http://thenexusnetwork.org/wp-content/uploads/2014/11/Harris-and-Lyon-Transdisciplinary-Research-002_Nexus-Thinkpiece-2014.pdf (accessed on 26 November 2020).
- Harris, F.; Lyon, F. Transdisciplinary environmental research: Building trust across professional boundaries. Environ. Sci. Policy 2013, 31, 109–119. [Google Scholar] [CrossRef]
- Future Earth. Science-Based Pathways for Sustainability. 2020. Available online: https://futureearth.org/initiatives/earth-targets-initiatives/science-based-pathways/ (accessed on 26 November 2020).
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ebi, K.L.; Harris, F.; Sioen, G.B.; Wannous, C.; Anyamba, A.; Bi, P.; Boeckmann, M.; Bowen, K.; Cissé, G.; Dasgupta, P.; et al. Transdisciplinary Research Priorities for Human and Planetary Health in the Context of the 2030 Agenda for Sustainable Development. Int. J. Environ. Res. Public Health 2020, 17, 8890. https://doi.org/10.3390/ijerph17238890
Ebi KL, Harris F, Sioen GB, Wannous C, Anyamba A, Bi P, Boeckmann M, Bowen K, Cissé G, Dasgupta P, et al. Transdisciplinary Research Priorities for Human and Planetary Health in the Context of the 2030 Agenda for Sustainable Development. International Journal of Environmental Research and Public Health. 2020; 17(23):8890. https://doi.org/10.3390/ijerph17238890
Chicago/Turabian StyleEbi, Kristie L., Frances Harris, Giles B. Sioen, Chadia Wannous, Assaf Anyamba, Peng Bi, Melanie Boeckmann, Kathryn Bowen, Guéladio Cissé, Purnamita Dasgupta, and et al. 2020. "Transdisciplinary Research Priorities for Human and Planetary Health in the Context of the 2030 Agenda for Sustainable Development" International Journal of Environmental Research and Public Health 17, no. 23: 8890. https://doi.org/10.3390/ijerph17238890
APA StyleEbi, K. L., Harris, F., Sioen, G. B., Wannous, C., Anyamba, A., Bi, P., Boeckmann, M., Bowen, K., Cissé, G., Dasgupta, P., Dida, G. O., Gasparatos, A., Gatzweiler, F., Javadi, F., Kanbara, S., Kone, B., Maycock, B., Morse, A., Murakami, T., ... Capon, A. (2020). Transdisciplinary Research Priorities for Human and Planetary Health in the Context of the 2030 Agenda for Sustainable Development. International Journal of Environmental Research and Public Health, 17(23), 8890. https://doi.org/10.3390/ijerph17238890










