An Integrative Review of How Healthcare Organizations Can Support Hospital Nurses to Thrive at Work
Abstract
1. Introduction
2. Methods
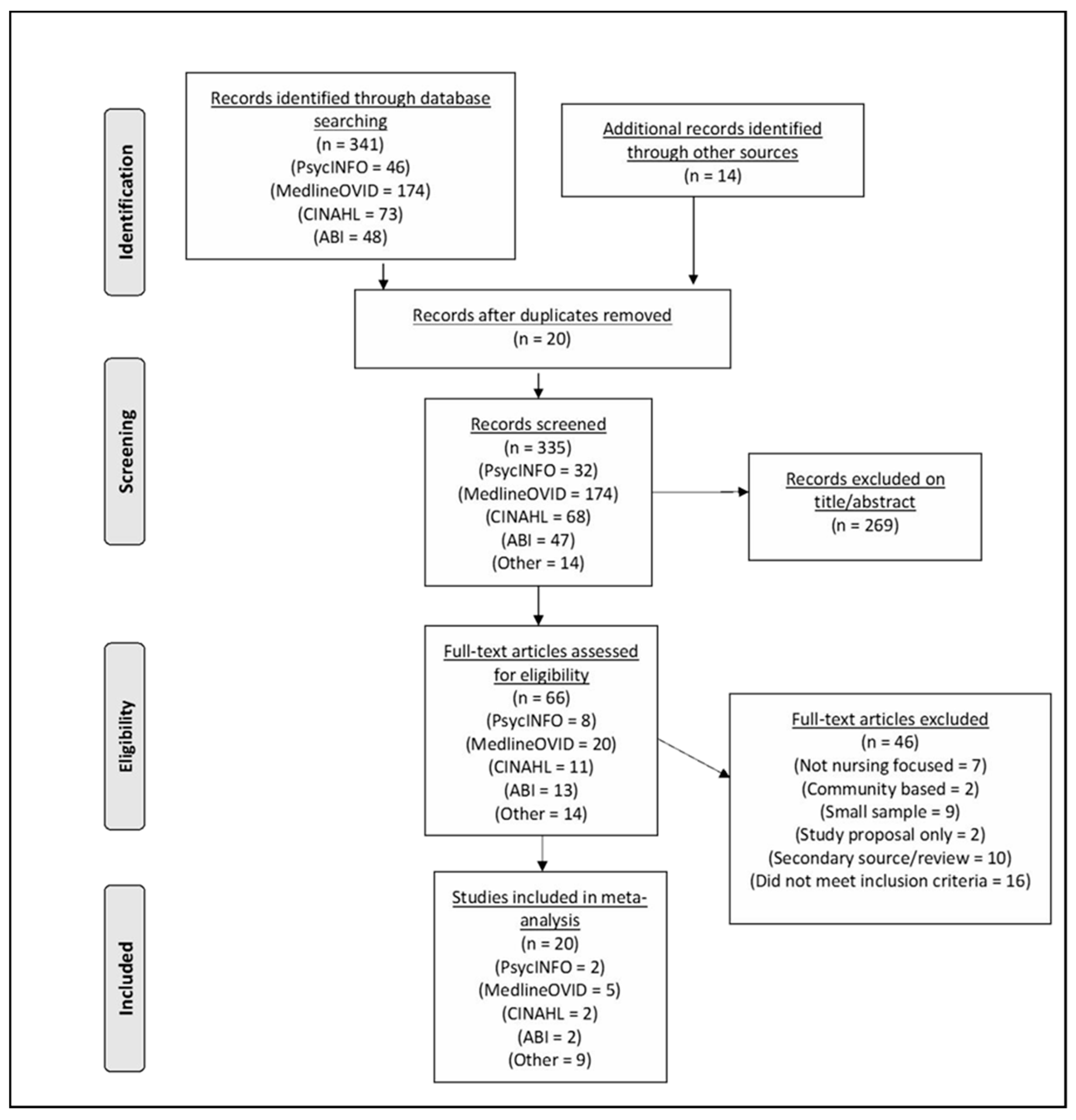
2.1. Search Strategy
2.2. Analysis
3. Results
3.1. Empowerment
3.1.1. Autonomy
3.1.2. Decision-Making Latitude
3.1.3. Motivation
3.2. Mood of the Organisation
3.2.1. Favorable Behaviors
3.2.2. Climate of Civility and Discretion
3.2.3. Employee Engagement
3.2.4. Organizational Justice
3.3. Enabling Environment
3.3.1. Job Demands/Stressors
3.3.2. Control/Demand
3.3.3. Professional Development
3.3.4. Quality of Care
3.3.5. Availability of Resources
3.4. Togetherness with Colleagues
3.4.1. Social Support Environment
3.4.2. Collegial Relations
3.4.3. Reciprocity
3.5. Leaders’ Connectivity
3.5.1. Support from Managers
3.5.2. Interpersonal Relationships between Management and Staff
3.5.3. Acknowledgment
4. Discussion
4.1. Thriving at Work and Nursing
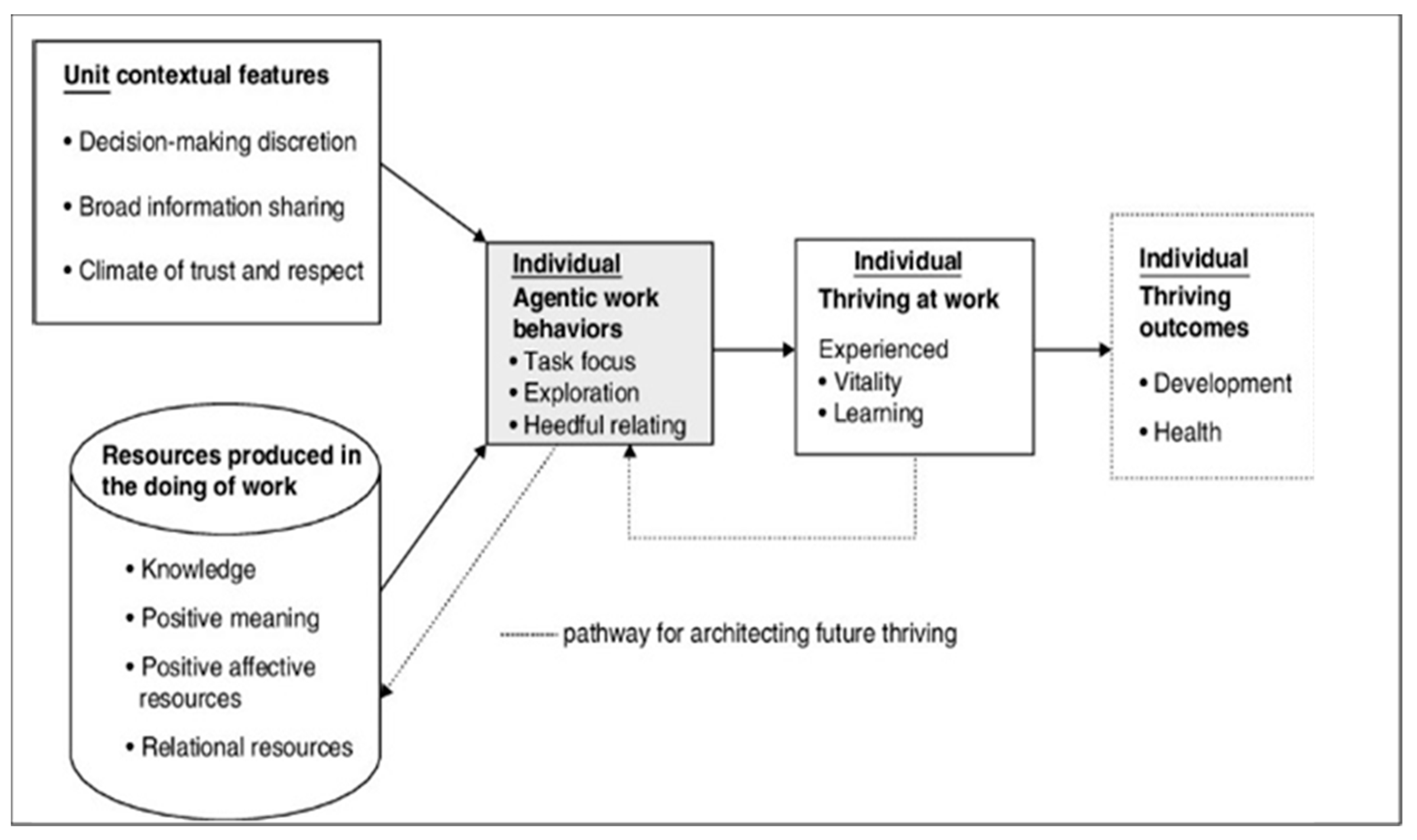
4.2. Unit Contextual Features
4.2.1. Decision-Making Discretion
4.2.2. Broad Information Sharing
4.2.3. Climate of Trust and Respect
4.3. Agentic Work Behaviours
4.3.1. Task Focus
Exploration
4.3.2. Heedful Relating
4.4. Organizational Factors to Enable Thriving at Work for Frontline Nurses
4.5. Thriving at Work: Outcomes for Nurse Sustainability and Wellbeing
5. Limitations
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- New Zealand Nurses Organisation. Nursing Matters; New Zealand Nurses Organisation: Wellington, New Zealand, 2017. [Google Scholar]
- Huntington, A.; Glimour, J.; Tuckett, A.; Neville, S.; Wilson, D.; Turner, C. Is anybody listening? A qualitative study of nurses’ reflections on practice. J. Clin. Nurs. 2010, 20, 1413–1422. [Google Scholar] [CrossRef] [PubMed]
- Geiger-Brown, J.; Lipscomb, J. The health care work environment and adverse health and safety consequences for nurses. Annu. Rev. Nursing Res. Workforce Issues 2010, 28, 191–231. [Google Scholar] [CrossRef] [PubMed]
- Szeto, G.P.Y.; Wong, T.K.T.; Law, R.K.Y.; Lee, E.W.C.; Lau, T.; So, B.C.L.; Law, S.W. The impact of a multifaceted ergonomic intervention program on promoting occupational health in community nurses. Appl. Ergonom. 2013, 44, 414–422. [Google Scholar]
- Nelson, K.; Boudrias, J.S.; Brunet, L.; Morin, D.; De Civita, M.; Savoie, A.; Alderson, M. Authentic leadership and psychological well-being at work of nurses: The mediating role of work climate at the individual level of analysis. Burnout Res. 2014, 1, 90–101. [Google Scholar] [CrossRef]
- Woods, M.; Rodgers, V.; Towers, A.; La Grow, S. Researching moral distress among New Zealand nurses: A national survey. Nurs. Ethics 2015, 22, 117–130. [Google Scholar] [CrossRef]
- Brunetto, Y.; Rodwell, J.; Shacklock, K.; Farr-Wharton, R.; Demir, D. The impact of individual and organizational resources on nurse outcomes and intent to quit. J. Adv. Nurs. 2016, 72, 3093–3103. [Google Scholar] [CrossRef]
- Moloney, W.; Gorman, D.; Parson, M.; Cheung, G. How to keep registered nurses working in New Zealand even as economic conditions improve. Human Res. Health 2018, 16. [Google Scholar] [CrossRef]
- Franks, S. Coronavirus: Nursing Students Dive into Career Early to Help with Pandemic. TCA Regional News. Available online: https://www.daytondailynews.com/gdpr.html (accessed on 12 April 2020).
- Labrague, L.J.; de los Santos, J.A.A. COVID-19 anxiety among front-line nurses: Predictive role of organisational support, personal resilience and social support. J. Nurs. Manag. 2020, 20, 1653–1661. [Google Scholar] [CrossRef]
- Labrague, L.J.; de los Santos, J.A.A. Fear of COVID-19, psychological distress, work satisfaction and turnover intention among frontline nurses. J. Nurs. Manag. 2020, 1–9. [Google Scholar] [CrossRef]
- Aburn, G.; Gott, M.; Hoare, K. What is resilience? An integrative review of the empirical literature. J. Adv. Nurs. 2016, 72, 980–1000. [Google Scholar]
- Spreitzer, G.; Sutcliffe, S.; Dutton, J.; Sonenshein, S.; Grant, A.M. A socially embedded model of thriving at work. Org. Sci. 2005, 16, 537–549. [Google Scholar] [CrossRef]
- Abid, G.; Zahra, I.; Ahmed, A. Promoting thriving at work and waning turnover intention: A relational perspective. Fut. Bus. J. 2016, 2, 127–137. [Google Scholar] [CrossRef]
- Kleine, A.K.; Rudolph, C.W.; Zacher, H. Thriving at work: A meta-analysis. J. Org. Beh. 2019, 40, 973–999. [Google Scholar] [CrossRef]
- Rodwell, J.; Munro, L. Relational regulation theory and the role of social support and organisational fairness for nurses in a general acute context. J. Clin. Nurs. 2013, 22, 3160–3169. [Google Scholar] [CrossRef] [PubMed]
- Sharif, S.P.; Ahadzadeh, A.S.; Nia, H.S. Mediating role of psychological well-being in the relationship between organizational support and nurses’ outcomes: A cross-sectional study. J. Adv. Nurs. 2018, 74, 887–899. [Google Scholar] [CrossRef]
- Utriainen, K.; Ala-Mursula, L.; Kyngäs, H. Hospital nurses’ wellbeing at work: A theoretical model. J. Nurs. Manag. 2015, 23, 736–743. [Google Scholar] [CrossRef]
- Koivu, A.; Saarinen, P.; Hyrkas, K. Who benefits from clinical supervision and how? The association between clinical supervision and the work-related well-being of female hospital nurses. J. Clin. Nurs. 2012, 21, 2567–2578. [Google Scholar]
- Päätalo, K.; Kyngäs, H. Measuring hospital nurses’ well-being at work–psychometric testing of the scale. Contem. Nurse 2016, 52, 722–735. [Google Scholar] [CrossRef]
- Setti, I.; Argentero, P. Organizational features of workplace and job engagement among Swiss healthcare workers. Nurs. Health Sci. 2011, 13, 425–432. [Google Scholar] [CrossRef]
- Weberg, D. Transformational leadership and staff retention: An evidence review with implications for healthcare systems. Nurs. Adm. Q. 2010, 34, 246–258. [Google Scholar] [CrossRef]
- Carmeli, A.; Spreitzer, G. Trust, connectivity, and thriving: Implications for innovative behaviors at work. J. Create. Beh. 2009, 43, 169–191. [Google Scholar] [CrossRef]
- Gillet, N.; Fouquerau, E.; Bonnaund-Antignac, A.; Mokounkolo, R.; Colombat, P. The mediating role of organizational justice in the relationship between transformational leadership and nurses’ quality of work life: A cross-sectional questionnaire survey. Int. J. Nur. Stud. 2013, 50, 1359–1367. [Google Scholar] [CrossRef] [PubMed]
- Laschinger, H.; Finegan, J. Empowering nurses for work engagement and health in hospital settings. J. Nurs. Adm. 2005, 35, 439–449. [Google Scholar] [CrossRef] [PubMed]
- Moloney, W.; Boxall, P.; Parsons, M.; Cheung, G. Factors predicting Registered Nurses’ intentions to leave their organization and profession: A job demands-resources framework. J. Adv. Nurs. 2018, 74, 864–875. [Google Scholar] [CrossRef]
- Spreitzer, G.; Porath, C. Self-determination as nutriment for thriving: Building an integrative model of human growth at work. In The Oxford Handbook of Work Engagement, Motivation, and Self-Determination Theory; Gagne, M., Ed.; Oxford University Press: New York, NY, USA, 2014. [Google Scholar]
- Whittemore, R.; Knafl, K. The integrative review: Updated methodology. J. Adv. Nurs. 2005, 52, 546–553. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gotzsche, P.C.; Ionnidis, J.P.A.; Clarke, M.; Deveraux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. BMJ Clin. Res. Ed. 2009, 339, b2700. [Google Scholar] [CrossRef]
- Dang, D.; Dearholt, S. Johns Hopkins Nursing Evidence-Based Practice: Model and Guidelines; Sigma Theta Tau International: Indianpolis, IL, USA, 2017. [Google Scholar]
- Mortier, A.V.; Vlerick, P.; Clays, E. Authentic leadership and thriving among nurses: The mediating role of empathy. J. Nurs. Manag. 2016, 24, 357–365. [Google Scholar] [CrossRef]
- Bensemmane, S.; Ohana, M.; Stinglhamber, F. Team justice and thriving: A dynamic approach. J. Manag. Psychol. 2018, 33, 229–242. [Google Scholar] [CrossRef]
- Brown, D.; Arnold, R.; Fletcher, D.; Standage, M. Human thriving. A conceptual debate and literature review. Eur. Psychol. 2017, 22, 167–179. [Google Scholar] [CrossRef]
- Fiabane, E.; Giorgi, I.; Sguzzin, C.; Argentero, P. Work engagement and occupational stress in nurses and other healthcare workers: The role of organisational and personal factors. J. Clin. Nurs. 2013, 22, 2614–2624. [Google Scholar] [CrossRef]
- Kowalczuk, K.; Krajewska-Kułak, E.; Sobolewski, M. The Reciprocal effect of psychosocial aspects on nurses’ working conditions. Front. Psychol. 2017, 8, 1386. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Liu, W.; Han, Y.; Zhang, P. Linking empowering leadership and change-oriented organizational citizenship behavior: The role of thriving at work and autonomy orientation. J. Org. Chan. Manag. 2016, 29, 732–750. [Google Scholar] [CrossRef]
- Mushtaq, M.; Abid, G.; Sarwar, K.; Ahmed, S. Forging ahead: How to thrive at the modern workplace. Iran. J. Manage. Stud. 2017, 10, 783–818. [Google Scholar]
- Paterson, T.A.; Luthans, F.; Jeung, W. Thriving at work: Impact of psychological capital and supervisor support. J. Org. Beh. 2014, 35, 3. [Google Scholar]
- Porath, C.; Spreitzer, G.; Gibson, C.; Garnett, F.G. Thriving at work: Toward its measurement, construct validation, and theoretical refinement. J. Org. Beh. 2012, 33, 250–275. [Google Scholar] [CrossRef]
- Sia, S.K.; Duari, P. Agentic work behaviour and thriving at work: Role of decision making authority. Benchmarking 2018, 25, 3225–3237. [Google Scholar] [CrossRef]
- Verhaeghe, R.; Vlerick, P.; Gemmel, P.; Maele, G.V.; Backer, G.D. Impact of recurrent changes in the work environment on nurses’ psychological well-being and sickness absence. J. Adv. Nurs. 2006, 56, 646–656. [Google Scholar] [CrossRef]
- Laschinger, H.; Heather, K.; Read, E.; Wilk, P.; Finegan, J. The influence of nursing unit empowerment and social capital on unit effectiveness and nurse perceptions of patient care quality. J. Nurs. Adm. 2014, 44, 347–352. [Google Scholar] [CrossRef]
- George, M. Stress in NHS staff triggers defensive inward-focussing and an associated loss of connection with colleagues: This is reversed by Schwartz Rounds. J. Compass. Health Care 2016, 31, 9–26. [Google Scholar] [CrossRef]
- Rickard, G.; Lenthall, S.; Dollard, M.; Opie, T.; Knight, S.; Dunn, S.; Wakerman, J.; MacLeod, M.; Seiler, J.; Webb-Brewster, D. Organisational intervention to reduce occupational stress and turnover in hospital nurses in the Northern Territory, Australia. Coll. J. Roy. Coll. Nurs. 2012, 19, 211–221. [Google Scholar] [CrossRef]
- Pabico, C. Creating supportive environments and thriving in a volatile, uncertain, complex, and ambiguous world. J. Nurs. Adm. 2015, 45, 471–473. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.; Bartram, T.; Karimi, L.; Leggat, S. Transformational leadership and social identity as predictors of team climate, perceived quality of care, burnout and turnover intention among nurses. Pers. Rev. 2016, 45, 1200–1216. [Google Scholar] [CrossRef]
- Prem, R.; Ohly, S.; Kubickek, B.; Korunka, C. Thriving on challenge stressors? Exploring time pressure and learning demands as antecedents of thriving at work. J. Org. Beh. 2017, 38, 108–123. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Siu, O.L.; Shi, K. Transformational leadership and employee well-being: The mediating role of trust in the leader and self-efficacy. Appl. Psychol. 2010, 59, 454–479. [Google Scholar] [CrossRef]
- Mcdonald, G.; Jackson, D.; Vickers, M.H.; Wilkes, L. Surviving workplace adversity: A qualitative study of nurses and midwives and their strategies to increase personal resilience. J. Nurs. Manag 2016, 24, 123–131. [Google Scholar] [CrossRef]
- Raelin, J. From leadership-as-practice to leaderful practice. Leadership-as-Practice to Leaderful Practice. Leadership 2011, 7, 195–211. [Google Scholar] [CrossRef]
- Laschinger, H. Positive working relationships matter for better nurse and patient outcomes. J. Nurs. Manag. 2010, 8, 875–877. [Google Scholar] [CrossRef]
- Brennan, E.J. Towards resilience and wellbeing in nurses. Br. J. Nurs. 2017, 26, 43–47. [Google Scholar] [CrossRef]
- Moloney, W.; Boxall, P.; Matthew, P.; Sheridan, N. Which factors influence New Zealand registered nurses to leave their profession? New Zealand J. Empl. Rel. 2018, 43, 1–13. [Google Scholar]
- Ginsburg, L.; Bain, L. The evaluation of a multifaceted intervention to promote “speaking up” and strengthen interprofessional teamwork climate perceptions. J. Interprof. Care 2017, 31, 207–217. [Google Scholar] [CrossRef]
- Gosselin, E.; Bourgault, P.; Lavoie, S. Association between job strain, mental health and empathy among intensive care nurses. Nurs. Crit. Care 2016, 3, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Garcia, A.B.; Rocha, F.L.R.; Pissinati, P.D.S.C.; Marziale, M.H.P.; Henriques, C.; do Carmo, M.; Haddad, F.L. The effects of organisational culture on nurses’ perceptions of their work. Br. J. Nurs. 2017, 26, 806–812. [Google Scholar] [CrossRef] [PubMed]
- Zhao, S.; Liu, L.; Chen, H. Factors influencing the occupational well-being of experienced nurses. Int. J. Nurs. Sci. 2015, 2, 378–382. [Google Scholar] [CrossRef][Green Version]
- Abid, G.; Ahmed, A. Multifacetedness of thriving: Its cognitive, affective, and behavioral dimensions. Int. J. Inform. Bus. Manag. 2016, 8, 121–130. [Google Scholar]
- Mihail, D.; Kloutsiniotis, P. The effects of high-performance work systems on hospital employees’ work-related well-being: Evidence from Greece. Eur. Manag. J. 2016, 34, 424–438. [Google Scholar] [CrossRef]
| Inclusion Criteria | Exclusion Criteria |
|---|---|
| English language | Community-based |
| 2005–2019 | Aged care |
| Hospital-based nurses | Maternity |
| Discussion on organizational factors | Student nurses |
| Human-related studies | Focus on individual factors |
| Business literature | Discussion on ‘failure to thrive’ rather than ‘thriving at work’ |
| Psychology literature | |
| Both components (learning and vitality) of thriving at work discussed |
| Reference | Purpose/Aim | Method | Findings | Evidence | Quality |
|---|---|---|---|---|---|
| Abid, G., Zahra, I., and Ahmed, A. (2016) [14]. Promoting thriving at work and waning turnover intention: A relational perspective. Future Business Journal, 2(2), 127–137. doi:10.1016/j.fbj.2016.08.001 | What are the antecedents of thriving at work and turnover intention? What is the relationship between perceived organizational support and relational resources? | Questionnaire. 128 software developers. | Heedful relating enhances thriving at work. Heedful relating minimizes intention to leave due to connectiveness among individuals. Perceived organizational support positively impacts heedful relating and thriving at work. | 3 | A |
| Bensemmane, S., Ohana, M., and Stinglhamber, F. (2018) [32]. Team justice and thriving: a dynamic approach. Journal of Managerial Psychology, 33(2), 229–242. doi:10.1108/JMP-07-2017-0223 | Perceived team justice is known to fluctuate within individuals over time, and in response to events at work Is transient team justice predictive of employees transient thriving at work? Is transient self-efficacy an underlying mechanism? | Questionnaire in four waves. 395 individuals completed the first wave, and at least 2 of the 3 subsequent questionnaires. Total 1412 cases. Business master’s students. | Transient overall team justice positively predicts self-efficacy, and therefore thriving at work. Team justice is related to thriving at work. Consideration of how team justice fluctuates is required. Self-efficacy is an important personal resource for team justice and thriving at work. Further mediators need identifying. | 3 | A |
| Brown, D., Arnold, R., Fletcher, D., and Standage, M. (2017) [33]. Human thriving. A conceptual Debate and Literature Review. European Psychologist. 22(3), 167–179. doi:10.1027/1016-9040/a000294 | To investigate key processes that underpin thriving at work. To propose a conceptualization of thriving applicable across different populations and domains. To identify personal and contextual enablers of thriving at work. | Literature Review. | Thriving at work is seen as multifactorial. To achieve thriving at work, subjective individual high-levels of wellbeing and holistic functioning is important. Important to distinguish differences between thriving, prospering, flourishing, growth. Psychosocial variables-personal and contextual enablers. Personal enablers: positive perspective, spirituality, motivation, proactive personality, knowledge and learning, resilience, social competence. Contextual enablers: challenge environment, attachment, trust, family support, colleague and employer support. | 5 | B |
| Carmeli, A., and Spreitzer, G. (2009) [23]. Trust, connectivity, and thriving: Implications for innovative behaviors at work. The Journal of Creative Behavior, 43(3), 169–191. doi:10.1002/j.21626057.2009.tb01313.x | Investigating the relationship between trust, connectivity, thriving and innovative behaviors? | Survey completed 3 weeks apart (same survey). Response rate 74.78%. 172 participants from a variety of organizations and industries. | Connectivity mediates the relationship between trust and thriving. Thriving mediates connectivity and innovative behaviors. Viewed as relational and psychological antecedents to how individuals engage in innovative work behaviors. Thriving increases individuals capability to demonstrate innovative, creative and momentum for ideas. Trust is viewed as a psychological contract that augments connectivity/collegial relationships. Results support the hypothesized theoretical model. | 3 | A |
| Fiabane, E., Giorgi, I., Sguazzin, C., and Argentero, P. (2013) [34]. Work engagement and occupational stress in nurses and other healthcare workers: the role of organisational and personal factors. Journal of Clinical Nursing, 22(17–18), 2614–2624. doi:10.1111/jocn.12084 | To identify the role of organizational and personal factors in predicting work engagement in healthcare workers. Compare work engagement and occupational stress perceptions of healthcare workers. | Cross-sectional survey. 110 hospital staff (registered nurses, nurse aides, physicians, physiotherapists). | Energy predicted by workload, mental health, job satisfaction. Professional efficacy predicted by values and job satisfaction. Physiotherapists had the highest levels of stress and disengagement. Improving psychological health requires a focus on workloads, personal expectations, and job satisfaction. | 3 | A |
| Kleine, A.K., Rudolph, C., and Zacher, H. (2019) [15]. Thriving at work: A meta-analysis. Journal of Organizational Behavior. 1–27. doi:10.1002/job.2375 | Using Spretizer et al.’s (2005) model for thriving at work as a basis, the constructs were investigated and organized into antecedents and outcomes of thriving. | Meta-analysis. | Individual characteristics associated with thriving at work are (a) psychological capital, (b) proactive personality, (c) positive affect, (d) work engagement. Relational characteristics positively associated with thriving at work are (a) supportive co-worker behavior, (b) supportive leadership behavior, (c) perceived organizational support. Thriving at work related to positive employee outcomes e.g., burnout, commitment, and task performance. Analysis supports the Spreitzer et al (2005) model and importance of thriving at work. | 3 | A |
| Kowalczuk, K., Krajewska-Kułak, E., and Sobolewski, M. (2017) [35]. The Reciprocal Effect of Psychosocial Aspects on Nurses’ Working Conditions. Frontiers in Psychology, 8, 1386. doi:10.3389/fpsyg.2017.01386 | Investigate the correlations between different aspects of nurses’ psychosocial working conditions and what factors affect well-being. Investigate what actions should be taken by management to ensure decent physical and mental conditions. | Questionnaire: Psychosocial aspects of work. 789 inpatient working nurses. | Well-being: Conflict and overload impact negatively. Control of work and cognitive control most strongly correlated. Social, supervisor, and collegial support are positively impacted. Physical well-being correlates with psychological well-being. Expectation of need for change: When work demands are perceived as being high. Low levels of social support were found. Psychosocial risk monitoring and stress prevention programs should be introduced. | 3 | B |
| Laschinger, H.K.S., and Finegan, J. (2005) [25]. Empowering nurses for work engagement and health in hospital settings. Journal of Nursing Administration, 35(10), 439–449. doi:10.1097/00005110-200510000-00005 | Relationship between empowerment, employee engagement, and physical and mental health outcomes. | Predictive non-experimental design. Random sample of 285 nurses. Test a theoretical model. | Empowerment strongly related to lower levels of burnout, greater work engagement and physical/mental health. Emotional exhaustion linked to overload, lack of reward/recognition, values congruence. | 3 | B |
| Li, M., Liu, W., Han, Y., and Zhang, P. (2016) [36]. Linking empowering leadership and change-oriented organizational citizenship behavior: The role of thriving at work and autonomy orientation. Journal of Organizational Change Management, 29(5), 732–750. doi:10.1108/JOCM-02-2015-0032 | Based on the theory of thriving at work, what is the link between empowering leadership and change orientated organizational behavior (OCB). | Questionnaires, 2 stages—203 employees. Structured interviews—80 supervisors. Information technology company. | Empowering leadership positively relates to thriving at work. Empowering leadership critically influences change-orientated OCBs. Employees with high autonomy direction were most positively stimulated by empowering leadership. Leaders need to adopt empowering behaviors, and provide suitable settings for thriving to occur. | 3 | A |
| Mortier, A.V., Vlerick, P., and Clays, E. 2016) [31]. Authentic leadership and thriving among nurses: the mediating role of empathy. Journal of Nursing Management, 24(3), 357–365. doi: 10.1111/jonm.12329 | Examine the relationship between perceived authentic leadership and two dimensions of thriving (learning and vitality). | Questionnaire, cross-sectional design. 360 nurses. | Authentic and empathic leadership enhances both indicators (learning and vitality) of thriving at work. Leadership positively related to vitality. Empathy mediates vitality but not learning. | 3 | B |
| Mushtaq, M., Abid, G., Sarwar, K., and Ahmed, S. (2017) [37]. Forging Ahead: How to Thrive at the Modern Workplace. Iranian Journal of Management Studies, 10(4). doi: 10.220059/ijms.2017.2355409/672704 | Investigation of contextual factors including organizational support, fairness perception, supervisor support, and civility on employee’s thriving at work. Simultaneously, what is the impact of individual characteristics? | Survey questionnaire. Purposive sampling on variety of occupations in service sector organizations: 221 participants. | Proactive personality, civility, fairness perception, organizational support and supervisor support are all antecedents to thriving. | 3 | A |
| Nelson, K., Boudrias, J.-S., Brunet, L., Morin, D., Civita, M. De, Savoie, A., and Alderson, M. (2014) [5]. Authentic leadership and psychological well-being at work of nurses: The mediating role of work climate at the individual level of analysis. Burnout Research, 1(2), 90–101. doi:10.1016/j.burn.2014.08.001 | Further understand the role of authentic leadership and work climate and associated relationship with psychological well-being. | Time-lagged questionnaire. 406 nurses. | Work climate is an important mediator for the relationship between authentic leadership and psychological well-being. Authentic leadership positively impacts work climate and increases psychological well-being. | 3 | A |
| Paterson, T.A., Luthans, F., and Jeung, W. (2014) [38]. Thriving at work: Impact of psychological capital and supervisor support. Journal of Organizational Behavior, 35(3), 434–446. doi:10.1002/job.1907 | Is thriving at work linked to self-development? What is the relationship between thriving at work and agentic work behaviors (task focus and heedful relating)? The aim was to explore the relationship between psychological capital (PsyCap) and supervisor support climate, with the outcome of thriving at work. | Online survey. 198 employee-supervisor dyads. Variety of part-time management students (full-time employed) and their direct supervisors. Employees completed the survey 1 month prior to supervisors. | Supervisor-rated employee self-development/performance supports Thriving. Agentic behaviors are positively related to thriving. PsyCap and supervisor support positively relates to agentic behaviors. PsyCap supports thriving via task focus. Supervisor support climate and thriving are affected by task focus. | 3 | B |
| Porath, C., Spreitzer, G., Gibson, C., and Garnett, F.G. (2012) [39]. Thriving at work: Toward its measurement, construct validation, and theoretical refinement. Journal of Organizational Behavior, 33(2), 250–275. doi: 10.1002/job.756 | Study 1: Investigate the construct validity of thriving at work in relation to affect, career orientation, proactive personality, self-evaluations. Study 2: Relationship between thriving and career development initiative, performance, burnout vs. job satisfaction, health, commitment. Study 3: Understanding the contextual embeddedness of thriving. | Study 1: Thriving survey. 175 undergraduates. 410 young professionals. Study 2: Thriving and Burnout Survey. Three samples: 1 = 276 respondents, 2 = 335 respondents, 3 = 136 respondents. Study 3: Thriving survey. 78 respondents (sample 3 in study 2: one month post university program completion). | Study 1: Evidence of convergent and discriminant validity of thriving in relation to hypothesized constructs. Study 2: Thriving positively related to general health, career development initiative, job performance, and leadership effectiveness. Negatively relates to burnout. Study 3: Thriving varies as individuals work life changes. Thriving is related to and varies across work and non-work contexts. | 3 | A |
| Sharif, S.P., Ahadzadeh, A.S., and Nia, H.S. (2018) [17]. Mediating role of psychological well-being in the relationship between organizational support and nurses’ outcomes: A cross-sectional study. Journal of Advanced Nursing, 74(4), 887–899. doi: 10.1111/jan.13501 | How does psychological well- being mediate the relationship between organizational support for nursing practice, quality of care, and, job satisfaction in the hospital setting? | Cross-sectional survey. 345 hospital-based nurses. | Psychological well-being and organizational support positively relate to quality of care and job satisfaction. Positive perceived organizational support generates favorable well-being, enhancing quality of care and individual outcomes. | 3 | A |
| Sia, S.K., and Duari, P. (2018) [40]. Agentic work behaviour and thriving at work: role of decision making authority. Benchmarking, 25(8), 3225-3237. doi:10.1108/BIJ-07-2017-0204 | Examining the contribution of agentic work behaviors and decision-making authority (DMA) to thriving at work. Does DMA have a moderating role in the relationship between agentic work behaviors and thriving at work? | Randomized sample. 330 manufacturing companies’ employees. Below the supervisory level. | The three dimensions of agentic work behaviors (task focus, exploration, and heedful relation), positively and directly contribute to thriving at work. Thriving is higher for employees experiencing DMA. | 3 | A |
| Spreitzer, G., and Porath, C. (2014) [27]. Self-determination as nutriment for thriving: Building an integrative model of human growth at work. In M. Gagne (Ed.), The Oxford handbook of work engagement, motivation, and self-determination theory. doi:10.1093/oxfordhb/9780199794911.016 | Discuss key outcomes and antecedents of thriving at work. Focus on self-determination theory and how thriving relates to autonomous motivation. | Book chapter | The three nutriments of autonomous motivation: (1) autonomy, (2) competence, and (3) relatedness, are powerful facilitators of thriving at work. Organizations wanting to promote thriving need to consider autonomy, competence, relatedness enhancement - starting with decision-making, sharing info, creating a culture of community/trust/respect, providing feedback, mitigating volatility to change, and providing flexible work hours. Individual and organizational outcomes of thriving are vast. | 5 | A |
| Spreitzer, G., Sutcliffe, K., Dutton, J., Sonenshein, S., and Grant, A.M. (2005) [13]. A socially embedded model of thriving at work. Organization Science, 16(5), 537–549. | Develop a model that explains the social embeddedness of thriving at work. How do work contexts affect individuals? | Model development. | Individuals who self-adapt to psychological states/internal feelings will thrive/undertake change. Organizations need to enable positive participation and well-being. Focus on producing and changing resources. Unit contextual features and resources created in ‘the doing of work’ cultivate agentic working behaviors. | 5 | A |
| Utriainen, K., Ala-Mursula, L., and Kyngäs, H. (2015) [18]. Hospital nurses’ wellbeing at work: a theoretical model. Journal of Nursing Management, 23(6), 736–743. doi: 10.1111/jonm.12203 | To develop a theoretical model of hospital nurses’ well-being at work. | Model development. Empirical data from 233 nurses. | Themes which support well-being: collegial relationships, enhancing high-quality patient care, supportive and fair leadership, challenging/meaningful and well organized work, opportunities for professional development. | 3 | A |
| Verhaeghe, R., Vlerick, P., Gemmel, P., Maele, G. Van, and Backer, G. De. (2006) [41]. Impact of recurrent changes in the work environment on nurses’ psychological well-being and sickness absence. Journal of Advanced Nursing, 56(6), 646–656. doi:10.1111/j.1365-2648.2006.04058.x | How is psychological well-being (job satisfaction, distress) and absence from work impacted by recurrent changes? | Cross-sectional questionnaire. 2094 hospital-based nurses. | Changes in the work environment negatively impact psychological well-being. Distress was high in nurses confronted with threatening changes—Job satisfaction was low, sickness rates were high. Challenging changes were positively related partially to wellbeing (job satisfaction, eustress) but did not change distress or sickness levels. | 3 | B |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moloney, W.; Fieldes, J.; Jacobs, S. An Integrative Review of How Healthcare Organizations Can Support Hospital Nurses to Thrive at Work. Int. J. Environ. Res. Public Health 2020, 17, 8757. https://doi.org/10.3390/ijerph17238757
Moloney W, Fieldes J, Jacobs S. An Integrative Review of How Healthcare Organizations Can Support Hospital Nurses to Thrive at Work. International Journal of Environmental Research and Public Health. 2020; 17(23):8757. https://doi.org/10.3390/ijerph17238757
Chicago/Turabian StyleMoloney, Willoughby, Jessica Fieldes, and Stephen Jacobs. 2020. "An Integrative Review of How Healthcare Organizations Can Support Hospital Nurses to Thrive at Work" International Journal of Environmental Research and Public Health 17, no. 23: 8757. https://doi.org/10.3390/ijerph17238757
APA StyleMoloney, W., Fieldes, J., & Jacobs, S. (2020). An Integrative Review of How Healthcare Organizations Can Support Hospital Nurses to Thrive at Work. International Journal of Environmental Research and Public Health, 17(23), 8757. https://doi.org/10.3390/ijerph17238757





