Intersections of Adverse Childhood Experiences, Race and Ethnicity and Asthma Outcomes: Findings from the Behavioral Risk Factor Surveillance System
Abstract
1. Introduction
1.1. The Disproportionate Burden of Asthma
1.2. Social Determinants of Asthma
1.3. Adverse Childhood Experiences as Social Determinants of Health
1.4. Adverse Experiences and Asthma: The Intersection of Race/Ethnicity and Sex
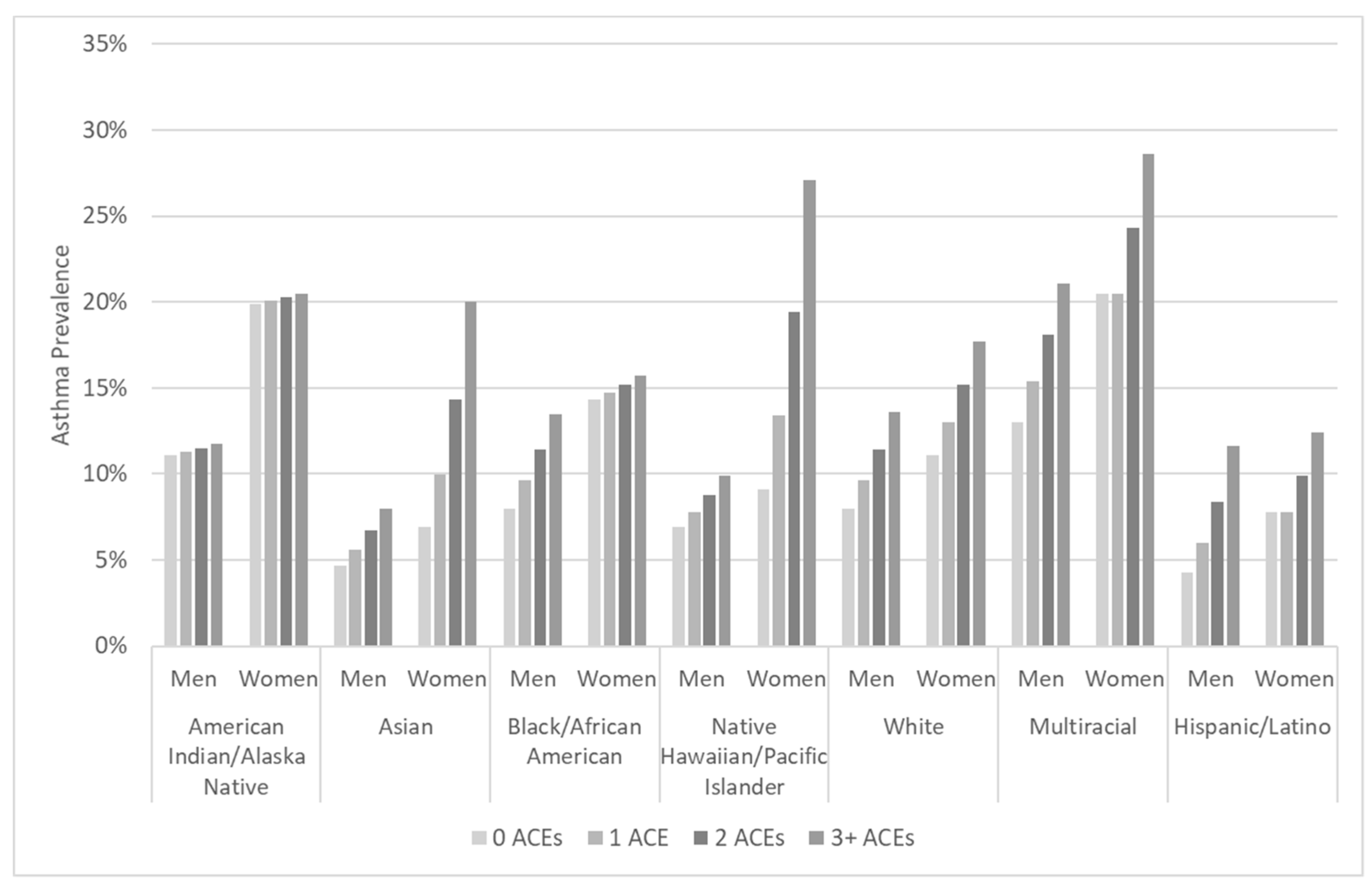
- ACE scores have a positively graded relationship with asthma;
- The positive relationship between ACEs and asthma varies by race/ethnicity, with a stronger relationship experienced by racial/ethnic minority groups with higher rates of asthma and ACEs, such as Black/African American, Hispanic/Latino, AIAN, and multiracial individuals;
- The positive relationship between ACEs and asthma varies by race/ethnicity and sex, with a disproportionate burden on Black/African American, Hispanic/Latino, AIAN, and multiracial women.
2. Materials and Methods
2.1. Data Source
2.2. Study Variables
2.2.1. Outcome Variable
2.2.2. Exposure Variable
2.2.3. Moderators
2.2.4. Control Variables
2.3. Data Analysis
3. Results
3.1. Sample Characteristics
3.2. Asthma
3.3. Adverse Childhood Experiences
3.4. The Intersection of Adverse Childhood Experiences and Race/Ethnicity
3.4.1. Model 1: Main Effects Model
3.4.2. Model 2: Interactional Model
3.4.3. Models 3a and 3b: Sex-Stratified Interactional Models
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Zahran, H.S.; Bailey, C.M.; Damon, S.A.; Garbe, P.L.; Breysse, P.N. Vital Signs: Asthma in Children—United States, 2001–2016. MMWR Morb. Mortal. Wkly. Rep. 2018, 67, 149–155. [Google Scholar] [CrossRef]
- National Health Interview Survey, Current Asthma Prevalence Percents by Age, United States: National Health Interview Survey, 2017; National Center for Health Statistics, Centers for Disease Control and Prevention: Atlanta, GA, USA, 2019.
- Shonkoff, J.P.; Garner, A.S. The lifelong effects of early childhood adversity and toxic stress. Pediatrics 2012, 129, e232–e246. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, R.G.; Marmot, M. Social Determinants of Health: The Solid Facts; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Akinbami, L.J.; Moorman, J.E.; Liu, X. Asthma prevalence, health care use, and mortality: United States, 2005–2009. Natl. Health Stat. Rep. 2011, 12, 1–14. [Google Scholar]
- Urquhart, A.; Clarke, P. US racial/ethnic disparities in childhood asthma emergent health care use: National Health Interview Survey, 2013–2015. J. Asthma 2019, 57, 510–520. [Google Scholar] [CrossRef] [PubMed]
- Blackwell, D.; Villarroel, M. Selected Respiratory Diseases Among Adults Aged 18 and Over, by Selected Characteristics: United States; National Center for Health Statistics: Hyattsville, MD, USA, 2017. [Google Scholar]
- Murphy, S.L.; Xu, J.Q.; Kochanek, K.D.; Arias, E. Mortality in the United States, 2017; National Center for Health Statistics: Hyattsville, MD, USA, 2018. [Google Scholar]
- Rosa, M.J.; Lee, A.; Wright, R.J. Evidence establishing a link between prenatal and early-life stress and asthma development. Curr. Opin. Allergy Clin. Immunol. 2018, 18, 148–158. [Google Scholar] [CrossRef] [PubMed]
- Von Korff, M.; Alonso, J.; Ormel, J.; Angermeyer, M.; Bruffaerts, R.; Fleiz, C.; de Girolamo, G.; Kessler, R.C.; Kovess-Masfety, V.; Posada-Villa, J.; et al. Childhood psychosocial stressors and adult onset arthritis: Broad spectrum risk factors and allostatic load. Pain 2009, 143, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Carger, E.; Westen, D. A New Way to Talk about the Social Determinants of Health; Robert Wood Johnson Foundation: Princeton, NJ, USA, 2010. [Google Scholar]
- Clark, N.A.; Demers, P.A.; Karr, C.J.; Koehoorn, M.; Lencar, C.; Tamburic, L.; Brauer, M. Effect of early life exposure to air pollution on development of childhood asthma. Environ. Health Perspec. 2009, 118, 284–290. [Google Scholar] [CrossRef] [PubMed]
- Ege, M.J.; Mayer, M.; Normand, A.-C.; Genuneit, J.; Cookson, W.O.; Braun-Fahrländer, C.; Heederik, D.; Piarroux, R.; von Mutius, E. Exposure to environmental microorganisms and childhood asthma. N. Engl. J. Med. 2011, 364, 701–709. [Google Scholar] [CrossRef]
- Bhan, N.; Glymour, M.M.; Kawachi, I.; Subramanian, S.V. Childhood adversity and asthma prevalence: Evidence from 10 US states (2009–2011). BMJ Open Respir. Res. 2014, 1, e000016. [Google Scholar] [CrossRef]
- Anda, R.F.; Brown, D.W.; Dube, S.R.; Bremner, J.D.; Felitti, V.J.; Giles, W.H. Adverse childhood experiences and chronic obstructive pulmonary disease in adults. Am. J. Prev. Med. 2008, 34, 396–403. [Google Scholar] [CrossRef]
- Williams, D.R.; Sternthal, M.; Wright, R.J. Social determinants: Taking the social context of asthma seriously. Pediatrics 2009, 123, S174. [Google Scholar] [CrossRef] [PubMed]
- CDC. Adverse childhood experiences reported by adults—Five states, 2009. MMWR Morb. Mortal. Wkly. Rep. 2010, 59, 1609–1613. [Google Scholar]
- Mersky, J.P.; Janczewski, C.E. Racial and ethnic differences in the prevalence of adverse childhood experiences: Findings from a low-income sample of US women. Child. Abuse Negl. 2018, 76, 480–487. [Google Scholar] [CrossRef] [PubMed]
- Hughes, K.; Bellis, M.A.; Hardcastle, K.A.; Sethi, D.; Butchart, A.; Mikton, C.; Jones, L.; Dunne, M.P. The effect of multiple adverse childhood experiences on health: A systematic review and meta-analysis. Lancet Public Health 2017, 2, e356–e366. [Google Scholar] [CrossRef]
- Brown, D.W.; Anda, R.F.; Felitti, V.J.; Edwards, V.J.; Malarcher, A.M.; Croft, J.B.; Giles, W.H. Adverse childhood experiences are associated with the risk of lung cancer: A prospective cohort study. BMC Public Health 2010, 10, 20. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.F.; Huang, B.; Simmons, J.M.; Moncrief, T.; Sauers, H.S.; Chen, C.; Ryan, P.H.; Newman, N.C.; Kahn, R.S. Role of financial and social hardships in asthma racial disparities. Pediatrics 2014, 133, 431. [Google Scholar] [CrossRef]
- Chen, E.; Hanson, M.D.; Paterson, L.Q.; Griffin, M.J.; Walker, H.A.; Miller, G.E. Socioeconomic status and inflammatory processes in childhood asthma: The role of psychological stress. J. Allergy Clin. Immunol. 2006, 117, 1014–1020. [Google Scholar] [CrossRef] [PubMed]
- Shuey, K.M.; Willson, A.E. Cumulative disadvantage and black-white disparities in life-course health trajectories. Res. Aging 2008, 30, 200–225. [Google Scholar] [CrossRef]
- Bauer, G.R. Incorporating intersectionality theory into population health research methodology: Challenges and the potential to advance health equity. Soc. Sci. Med. 2014, 110, 10–17. [Google Scholar] [CrossRef]
- Collins, P.H.; Bilge, S. Intersectionality; Polity Press: Cambridge, UK, 2016. [Google Scholar]
- Bowleg, L. The problem with the phrase women and minorities: Intersectionality-an important theoretical framework for public health. Am. J. Public Health 2012, 102, 1267–1273. [Google Scholar] [CrossRef]
- Oraka, E.; Iqbal, S.; Flanders, W.D.; Brinker, K.; Garbe, P. Racial and ethnic disparities in current asthma and emergency department visits: Findings from the National Health Interview Survey, 2001–2010. J. Asthma 2013, 50, 488–496. [Google Scholar] [CrossRef]
- Warner, D.F.; Brown, T.H. Understanding how race/ethnicity and gender define age-trajectories of disability: An intersectionality approach. Soc. Sci. Med. 2011, 72, 1236–1248. [Google Scholar] [CrossRef]
- CDC. Behavioral Risk Factor Surveillance System ACE Data. Available online: https://www.cdc.gov/violenceprevention/childabuseandneglect/acestudy/ace-brfss.html (accessed on 26 December 2019).
- CDC. Behavioral Risk Factor Surveillance System Survey Data; U.S. Department of Health and Human Services, Centers for Disease Control and Prevention: Atlanta, GA, USA, 2009–2012.
- CDC. Annual Survey Data. Available online: https://www.cdc.gov/brfss/annual_data/annual_data.htm (accessed on 26 December 2019).
- CDC. The BRFSS Data User Guide; Department of Health and Human Services: Atlanta, GA, USA, 2013.
- Williams, D.R.; Lavizzo-Mourey, R.; Warren, R.C. The concept of race and health status in America. Public Health Rep. 1994, 109, 26. [Google Scholar] [PubMed]
- Krieger, N. Refiguring “race”: Epidemiology, racialized biology, and biological expressions of race relations. Int. J. Health Serv. 2000, 30, 211–216. [Google Scholar] [CrossRef]
- Pedersen, A.B.; Mikkelsen, E.M.; Cronin-Fenton, D.; Kristensen, N.R.; Pham, T.M.; Pedersen, L.; Petersen, I. Missing data and multiple imputation in clinical epidemiological research. Clin. Epidemiol. 2017, 9, 157. [Google Scholar] [CrossRef] [PubMed]
- United States Census Bureau Geographic Levels. Available online: https://www.census.gov/programs-surveys/economic-census/guidance-geographies/levels.html#par_textimage_34 (accessed on 30 May 2020).
- Krstić, G. Asthma prevalence associated with geographical latitude and regional insolation in the United States of America and Australia. PLoS ONE 2011, 6, e18492. [Google Scholar] [CrossRef] [PubMed]
- Akinbami, L.J.; Santo, L.; Williams, S.; Rechtsteiner, E.A.; Strashny, A. Characteristics of Asthma Visits to Physician Offices in the United States: 2012–2015 National Ambulatory Medical Care Survey; National Center for Health Statistics: Hyattsville, MD, USA, 2019.
- StataCorp. Stata Statistical Software; StataCorp LLC: College Station, TX, USA, 2017. [Google Scholar]
- CDC. National Health Interview Survey (NHIS) Data; National Center for Health Statistics, CDC: Atlanta, GA, USA, 2011–2014.
- United States Census Bureau. 2008–2012 American Community Survey 5-Year Estimates; U.S. Census Bureau’s American Community Survey Office: Lakewood, CO, USA, 2014.
- United States Census Bureau. Annual Estimates of the Resident Population for the United States, Regions, States, and Puerto Rico; United States Census Bureau: Lakewood, CO, USA, 2012.
- Bowleg, L. When Black+ lesbian+ woman≠ Black lesbian woman: The methodological challenges of qualitative and quantitative intersectionality research. Sex. Roles 2008, 59, 312–325. [Google Scholar] [CrossRef]
- Cronholm, P.F.; Forke, C.M.; Wade, R.; Bair-Merritt, M.H.; Davis, M.; Harkins-Schwarz, M.; Pachter, L.M.; Fein, J.A. Adverse Childhood Experiences: Expanding the Concept of Adversity. Am. J. Prev. Med. 2015, 49, 354–361. [Google Scholar] [CrossRef]
- Brockie, T.N.; Elm, J.H.; Walls, M.L. Examining protective and buffering associations between sociocultural factors and adverse childhood experiences among American Indian adults with type 2 diabetes: A quantitative, community-based participatory research approach. BMJ Open 2018, 8, e022265. [Google Scholar] [CrossRef]
- John-Henderson, N.A.; Henderson-Matthews, B.; Ollinger, S.R.; Racine, J.; Gordon, M.R.; Higgins, A.A.; Horn, W.C.; Reevis, S.A.; Running Wolf, J.A.; Grant, D. Adverse Childhood Experiences and Immune System Inflammation in Adults Residing on the Blackfeet Reservation: The Moderating Role of Sense of Belonging to the Community. Ann. Behav. Med. 2019. [Google Scholar] [CrossRef]
- Cushing, L.; Faust, J.; August, L.M.; Cendak, R.; Wieland, W.; Alexeeff, G. Racial/Ethnic Disparities in Cumulative Environmental Health Impacts in California: Evidence From a Statewide Environmental Justice Screening Tool (CalEnviroScreen 1.1). Am. J. Public Health 2015, 105, 2341–2348. [Google Scholar] [CrossRef]
- Whitrow, M.J.; Harding, S. Asthma in Black African, Black Caribbean and South Asian adolescents in the MRC DASH study: A cross sectional analysis. BMC Pediatr. 2010, 10, 18. [Google Scholar] [CrossRef]
- Ebell, M.H.; Marchello, C.; Meng, L.; O’Connor, J. The Burden and Social Determinants of Asthma Among Children in the State of Georgia. J. Community Health 2019, 44, 1–7. [Google Scholar] [CrossRef]
- Warne, D.; Dulacki, K.; Spurlock, M.; Meath, T.; Davis, M.M.; Wright, B.; McConnell, K.J. Adverse Childhood Experiences (ACE) among American Indians in South Dakota and Associations with Mental Health Conditions, Alcohol Use, and Smoking. J. Health Care Poor Underserved 2017, 28, 1559–1577. [Google Scholar] [CrossRef] [PubMed]
- Beasley, R.; Semprini, A.; Mitchell, E.A. Risk factors for asthma: Is prevention possible? Lancet 2015, 386, 1075–1085. [Google Scholar] [CrossRef]
- Morgan, W.J.; Crain, E.F.; Gruchalla, R.S.; O’Connor, G.T.; Kattan, M.; Evans, R., III; Stout, J.; Malindzak, G.; Smartt, E.; Plaut, M. Results of a home-based environmental intervention among urban children with asthma. N. Engl. J. Med. 2004, 351, 1068–1080. [Google Scholar] [CrossRef]
- Wu, F.; Takaro, T.K. Childhood asthma and environmental interventions. Environ. Health Perspec. 2007, 115, 971–975. [Google Scholar] [CrossRef]
- Yorke, J.; Fleming, S.L.; Shuldham, C. Psychological interventions for adults with asthma: A systematic review. Respir. Med. 2007, 101, 1–14. [Google Scholar] [CrossRef]
- Guevara, J.P.; Wolf, F.M.; Grum, C.M.; Clark, N.M. Effects of educational interventions for self management of asthma in children and adolescents: Systematic review and meta-analysis. BMJ 2003, 326, 1308–1309. [Google Scholar] [CrossRef]
- Clark, N.M.; Mitchell, H.E.; Rand, C.S. Effectiveness of educational and behavioral asthma interventions. Pediatrics 2009, 123, S185–S192. [Google Scholar] [CrossRef]
- National Institute of Environmental Health Sciences Asthma. Available online: https://www.niehs.nih.gov/health/topics/conditions/asthma/index.cfm (accessed on 28 June 2020).
- Garg, A.; Jack, B.; Zuckerman, B. Addressing the social determinants of health within the patient-centered medical home: Lessons from pediatrics. JAMA 2013, 309, 2001–2002. [Google Scholar] [CrossRef]
- DeVoe, J.E.; Bazemore, A.W.; Cottrell, E.K.; Likumahuwa-Ackman, S.; Grandmont, J.; Spach, N.; Gold, R. Perspectives in primary care: A conceptual framework and path for integrating social determinants of health into primary care practice. Ann. Fam. Med. 2016, 14, 104–108. [Google Scholar] [CrossRef]
- Bryan, R.H. Getting to why: Adverse childhood experiences’ impact on adult health. J. Nurse Pract. 2019, 15, 153–157. [Google Scholar] [CrossRef]
- Larkin, H.; Shields, J.J.; Anda, R.F. The health and social consequences of adverse childhood experiences (ACE) across the lifespan: An introduction to prevention and intervention in the community. J. Prev. Interv. Community 2012, 40, 263–270. [Google Scholar] [CrossRef]
- Oral, R.; Ramirez, M.; Coohey, C.; Nakada, S.; Walz, A.; Kuntz, A.; Benoit, J.; Peek-Asa, C. Adverse childhood experiences and trauma informed care: The future of health care. Pediatr. Res. 2016, 79, 227. [Google Scholar] [CrossRef]
- Larkin, H.; Felitti, V.J.; Anda, R.F. Social work and adverse childhood experiences research: Implications for practice and health policy. Soc. Work Public Health 2014, 29, 1–16. [Google Scholar] [CrossRef]
- Britto, P.R.; Lye, S.J.; Proulx, K.; Yousafzai, A.K.; Matthews, S.G.; Vaivada, T.; Perez-Escamilla, R.; Rao, N.; Ip, P.; Fernald, L.C. Nurturing care: Promoting early childhood development. Lancet 2017, 389, 91–102. [Google Scholar] [CrossRef]
- Srivastav, A.; Strompolis, M.; Moseley, A.; Daniels, K. The Empower Action Model: A Framework for Preventing Adverse Childhood Experiences by Promoting Health, Equity, and Well-Being Across the Life Span. Health Promot. Pract. 2019, 21, 525–534. [Google Scholar] [CrossRef] [PubMed]
- Merrick, M.T.; Ford, D.C.; Ports, K.A.; Guinn, A.S.; Chen, J.; Klevens, J.; Metzler, M.; Jones, C.M.; Simon, T.R.; Daniel, V.M.; et al. Vital Signs: Estimated Proportion of Adult Health Problems Attributable to Adverse Childhood Experiences and Implications for Prevention—25 States, 2015–2017. MMWR Morb. Mortal. Wkly. Rep. 2019, 68, 999–1005. [Google Scholar] [CrossRef]
| Survey Question | Response Options and Coding for Analysis |
|---|---|
| 1. Did you live with anyone who was depressed, mentally ill, or suicidal? | 0—No 1—Yes |
| 2. Did you live with anyone who was a problem drinker or alcoholic? | |
| 3. Did you live with anyone who used illegal street drugs or who abused prescription medications? | |
| 4. Did you live with anyone who served time or was sentenced to serve time in a prison, jail, or other correctional facility? | |
| 5. Were your parents separated or divorced? | |
| 6. How often did your parents or adults in your home ever slap, hit, kick, punch or beat each other up? | 0—Never 1—Once 1—More than once |
| 7. Before age 18, how often did a parent or adult in your home ever hit, beat, kick, or physically hurt you in any way? Do not include spanking. | |
| 8. How often did a parent or adult in your home ever swear at you, insult you, or put you down? | |
| 9. How often did anyone at least 5 years older than you or an adult, ever touch you sexually? | |
| 10. How often did anyone at least 5 years older than you or an adult, try to make you touch them sexually? | |
| 11. How often did anyone at least 5 years older than you or an adult, force you to have sex? |
| Sample Characteristics | Percentage or Mean (SD) |
|---|---|
| N = 114,015 | |
| Asthma | 12.70% |
| Adverse Childhood Experiences | |
| Any | 57.10% |
| Number | 1.5 (2.0) |
| Sex | |
| Male | 39.70% |
| Female | 60.30% |
| Age (years) | 55.7 (16.8) |
| 18–64 | 68.20% |
| 65+ | 31.80% |
| Race/Ethnicity | |
| American Indian/Alaska Native | 1.70% |
| Asian | 2.70% |
| Black/African American | 7.60% |
| Native Hawaiian/Pacific Islander | 0.30% |
| White | 81.90% |
| Multiracial | 2.70% |
| Hispanic | 3.20% |
| Level of Education | |
| HS/GED or less | 36.90% |
| Some college/tech. school | 27.80% |
| College/tech. school grad | 35.20% |
| Annual Income | |
| USD <20,000 | 15.80% |
| USD 20,000 – <35,000 | 20.20% |
| USD 35,000 – <75,000 | 28.30% |
| USD 75,000+ | 23.30% |
| [Missing/Refused] | 12.40% |
| Smoking History | |
| Ever Smoker | 47.50% |
| Geographic Region | |
| Midwest | 28.90% |
| Northeast | 11.30% |
| South | 31.70% |
| West | 28.10% |
| Asthma | Any ACE | # ACEs | |||||||
|---|---|---|---|---|---|---|---|---|---|
| All | Men | Women | All | Men | Women | All | Men | Women | |
| Overall | 12.3 (11.9–12.7) | 10.1 (9.6–10.7) | 14.0 (13.5–14.5) | 60.2 (59.7–60.7) | 59.6 (58.8–60.5) | 60.7 (60.0–61.3) | 1.7 (1.7–1.7) | 1.5 (1.5–1.6) | 1.8 (1.8–1.8) |
| American Indian/Alaska Native | 17.6 (14.1–21.0) | 12.6 (7.8–17.3) | 21.8 (16.8–26.8 | 69.2 (65.1–73.3) | 69.3 (62.7–75.9) | 69.1 (63.9–74.3) | 2.4 (2.2–2.6) | 2.3 (2.0–2.7) | 2.5 (2.2–2.8) |
| Asian | 8.2 (6.1–10.3) | 5.9 (3.0–8.7) | 10.1 (7.1–13.2) | 43.7 (39.3–48.1) | 43.1 (36.3–50.0) | 44.1 (38.5–49.8) | 0.9 (0.8–1.0) | 0.8 (0.6–1.0) | 1.0 (0.8–1.2) |
| Black/African American | 14.2 (12.8–15.5) | 11.1 (8.8–13.3) | 16.0 (14.2–17.7) | 64.8 (63.0–66.5) | 64.6 (61.5–67.7) | 64.8 (62.7–67.0) | 1.9 (1.8–2.0) | 1.8 (1.6–1.9) | 2.0 (1.8–2.1) |
| Native Hawaiian/Pacific Islander | 13.2 (7.2–19.3) | 8.1 (0.8–15.3) | 19.9 (10.9–28.8) | 57.9 (43.7–72.0) | 49.6 (27.2–71.9) | 68.6 (56.9–80.3) | 1.7 (1.2–2.1) | 1.1 (0.6–1.5) | 2.4 (1.8–3.0) |
| White | 12.0 (11.6–12.4) | 9.9 (9.3–10.5) | 13.7 (13.1–14.2) | 59.2 (58.6–59.8) | 58.7 (57.8–59.6) | 59.6 (58.9–60.4) | 1.6 (1.6–1.7) | 1.5 (1.4–1.5) | 1.8 (1.7–1.8) |
| Multiracial | 23.8 (20.3–27.3) | 20.1 (15.2–25.0) | 27.1 (22.2–32.0) | 74.7 (71.5–78.0) | 75.4 (70.6–80.2) | 74.2 (69.7–78.7) | 2.9 (2.7–3.2) | 2.8 (2.5–3.1) | 3.1 (2.8–3.4) |
| Hispanic/Latino | 9.6 (8.0–11.3) | 9.1 (6.7–11.5) | 10.2 (7.9–12.4) | 68.1 (65.6–70.6) | 66.1 (62.3–69.9) | 69.9 (66.6–73.3) | 2.1 (1.9–2.2) | 1.9 (1.7–2.1) | 2.3 (2.0–2.4) |
| Predictor Variables | Model 1–Main Effects 1 | Model 2–Interaction 1 | Model 3a–Interaction, Men 1 | Model 3b–Interaction, Women 1 | ||||
|---|---|---|---|---|---|---|---|---|
| OR (95% CI) | p > |t| | OR (95% CI) | p > |t| | OR (95% CI) | p > |t| | OR (95% CI) | p > |t| | |
| # ACEs | 1.12 (1.10–1.13) | <0.001 * | 1.25 (1.06–1.49) | 0.009 * | 1.11 (0.93–1.32) | 0.25 | 1.30 (1.05–1.59) | 0.014 * |
| Race/Ethnicity (Reference = Asian) | ||||||||
| American Indian/Alaska Native | 1.91 (1.30–2.81) | 0.001 * | 2.97 (1.89–4.65) | <0.001 * | 2.58 (1.14–5.84) | 0.023 * | 3.12 (1.85–5.25) | <0.001 * |
| Black/African American | 1.57 (1.15–2.14) | 0.004 * | 2.06 (1.49–2.85) | <0.001 * | 1.80 (0.98–3.32) | 0.058 | 2.07 (1.45–2.95) | <0.001 * |
| Native Hawaiian/Pacific Islander | 1.57 (0.89–2.78) | 0.123 | 1.51 (0.73–3.13) | 0.266 | 1.37 (0.38–5.02) | 0.63 | 1.71 (0.81–3.59) | 0.158 |
| White | 1.47 (1.11–1.96) | 0.008 * | 1.69 (1.26–2.26) | <0.001 * | 1.77 (1.04–3.01) | 0.037 * | 1.57 (1.14–2.16) | 0.005 * |
| Multiracial | 2.54 (1.80–3.59) | <0.001 * | 2.74 (1.79–4.19) | <0.001 * | 2.70 (1.28–5.68) | 0.009 * | 2.61 (1.58–4.30) | <0.001 * |
| Hispanic/Latino | 0.97 (0.68–1.36) | 0.843 | 1.06 (0.72–1.56) | 0.774 | 1.18 (0.62–2.22) | 0.619 | 0.92 (0.57–1.49) | 0.739 |
| Interaction: ACEs by Race/Ethnicity | ||||||||
| American Indian/Alaska Native | 0.80 (0.67–0.97) | 0.021 * | 0.89 (0.71–1.12) | 0.32 | 0.78 (0.62–0.98) | 0.034 * | ||
| Black/African American | 0.84 (0.71–1.01) | 0.058 | 1.01 (0.82–1.24) | 0.954 | 0.80 (0.65–0.99) | 0.041 * | ||
| Native Hawaiian/Pacific Islander | 0.96 (0.75–1.23) | 0.771 | 1.03 (0.65–1.63) | 0.892 | 0.92 (0.70–1.21) | 0.548 | ||
| White | 0.90 (0.76–1.06) | 0.205 | 1.01 (0.85–1.21) | 0.887 | 0.87 (0.70–1.07) | 0.18 | ||
| Multiracial | 0.91 (0.76–1.09) | 0.315 | 1.04 (0.83–1.30) | 0.713 | 0.88 (0.70–1.10) | 0.25 | ||
| Hispanic/Latino | 0.91 (0.76–1.09) | 0.305 | 1.04 (0.85–1.27) | 0.694 | 0.88 (0.70–1.10) | 0.257 | ||
| Sex (Reference = Women) | ||||||||
| Men | 0.73 (0.67–0.78) | <0.001 * | 0.73 (0.67–0.79) | <0.001 * | -- | -- | -- | -- |
| Constant | 0.13 (0.10–0.19) | 0.12 (0.08–0.16) | <0.001 * | 0.08 (0.05–0.15) | <0.001 * | 0.12 (0.08–0.17) | <0.001 * | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hall, T.; Rooks, R.; Kaufman, C. Intersections of Adverse Childhood Experiences, Race and Ethnicity and Asthma Outcomes: Findings from the Behavioral Risk Factor Surveillance System. Int. J. Environ. Res. Public Health 2020, 17, 8236. https://doi.org/10.3390/ijerph17218236
Hall T, Rooks R, Kaufman C. Intersections of Adverse Childhood Experiences, Race and Ethnicity and Asthma Outcomes: Findings from the Behavioral Risk Factor Surveillance System. International Journal of Environmental Research and Public Health. 2020; 17(21):8236. https://doi.org/10.3390/ijerph17218236
Chicago/Turabian StyleHall, Tristen, Ronica Rooks, and Carol Kaufman. 2020. "Intersections of Adverse Childhood Experiences, Race and Ethnicity and Asthma Outcomes: Findings from the Behavioral Risk Factor Surveillance System" International Journal of Environmental Research and Public Health 17, no. 21: 8236. https://doi.org/10.3390/ijerph17218236
APA StyleHall, T., Rooks, R., & Kaufman, C. (2020). Intersections of Adverse Childhood Experiences, Race and Ethnicity and Asthma Outcomes: Findings from the Behavioral Risk Factor Surveillance System. International Journal of Environmental Research and Public Health, 17(21), 8236. https://doi.org/10.3390/ijerph17218236






