A Conceptual Model Map on Health and Nutrition Behavior (CMMHB/NB)
Abstract
1. Introduction
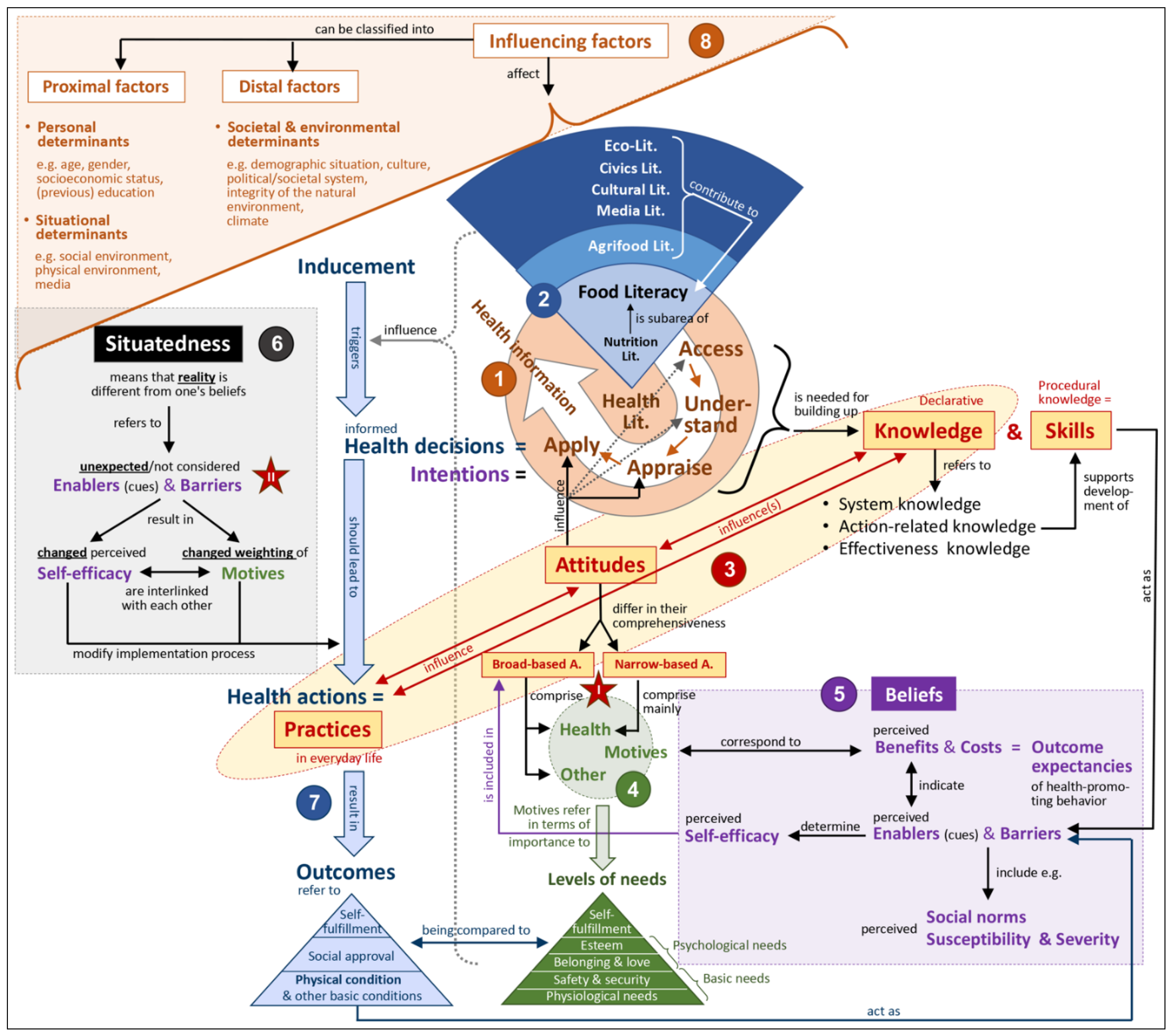
2. The Conceptual Model Map
2.1. The Orange Circle (No. 1)/Health Literacy
2.2. The Blue Circle Segment (No. 2)/Food Literacy
2.3. The Yellow Ellipse with Red Writing (No. 3)/KAP
2.4. The Green Components (No. 4)/Decision Motives and Pyramid of Needs
2.5. The Lilac Rectangle (No. 5)/Beliefs in Behavior Change Theories
2.6. The Grey Rectangle (No. 6)/Situatedness of Actions
2.7. The Line of Blue Arrows (No. 7)/Phases of an Action Episode
2.8. The Orange Triangle (No. 8)/Proximal and Distal Influencing Factors
3. Implications for Research and Practice
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Noar, S.M.; Zimmerman, R.S. Health Behavior Theory and cumulative knowledge regarding health behaviors: Are we moving in the right direction? Health Educ. Res. 2005, 20, 275–290. [Google Scholar] [CrossRef]
- Ruiz-Primo, M.A.; Shavelson, R.J. Problems and issues in the use of concept maps in science assessment. J. Res. Sci. Teach. 1996, 33, 569–600. [Google Scholar] [CrossRef]
- Glanz, K.; Rimer, B.K.; Viswanath, K. (Eds.) Health Behavior and Health Education: Theory, Research, and Practice, 4th ed.; Jossey-Bass: San Francisco, CA, USA, 2008. [Google Scholar]
- Nutbeam, D.; Harris, E.; Wise, M. Theory in a Nutshell: A Practical Guide to Health Promotion Theories, 3rd ed.; McGraw-Hill: North Ryde NSW, Australia, 2010. [Google Scholar]
- Gellman, M.D.; Turner, J.R. (Eds.) Encyclopedia of Behavioral Medicine; Springer: New York, NY, USA, 2013. [Google Scholar]
- Goldstein, S.; Naglieri, J.A. (Eds.) Encyclopedia of Child Behavior and Development; Springer: New York, NY, USA, 2011. [Google Scholar]
- Benes, S.; Alperin, H. The Essentials of Teaching Health Education: Curriculum, Instruction, and Assessment; Human Kinetics: Champaign, IL, USA, 2016. [Google Scholar]
- Sørensen, K.; Van den Broucke, S.; Fullam, J.; Doyle, G.; Pelikan, J.; Slonska, Z.; Brand, H.; Consortium Health Literacy Project European. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health 2012, 12, 80. [Google Scholar] [CrossRef] [PubMed]
- Krause, C.; Sommerhalder, K.; Beer-Borst, S.; Abel, T. Just a subtle difference? Findings from a systematic review on definitions of nutrition literacy and food literacy. Health Promot. Int. 2016, 33, 378–389. [Google Scholar] [CrossRef] [PubMed]
- Fautsch Macías, Y.; Glasauer, P. Guidelines for Assessing Nutrition-Related Knowledge, Attitudes and Practices: KAP Manual; Food and Agriculture Organization of the United Nations: Rome, Italy, 2014. [Google Scholar]
- Sproesser, G.; Ruby, M.B.; Arbit, N.; Rozin, P.; Schupp, H.T.; Renner, B. The Eating Motivation Survey: Results from the USA, India and Germany. Public Health Nutr. 2018, 21, 515–525. [Google Scholar] [CrossRef]
- Sørensen, K. Defining health literacy: Exploring differences and commonalities. In International Handbook of Health Literacy: Research, Practice and Policy across the Lifespan; Okan, O., Bauer, U., Pinheiro, P., Sørensen, K., Levin, D., Eds.; Policy Press: Bristol, UK, 2019; pp. 5–20. [Google Scholar]
- Joint Committee on National Health Education Standards. National Health Education Standards, Second Edition: Achieving Excellence; The American Cancer Society: Washington, DC, USA, 2007. [Google Scholar]
- Hernandez, K.J. Exploring Food Literacy in Nova Scotia Public Schools: A Critical Analysis. Ph.D. Thesis, Dalhousie University, Halifax, NS, Canada, 2019. [Google Scholar]
- Hernandez, K.J.; Gillis, D.; Kevany, K.; Kirk, S.F.L. Towards a common understanding of food literacy. 2020; manuscript in progress. [Google Scholar]
- Azevedo Perry, E.; Thomas, H.; Samra, H.R.; Edmonstone, S.; Davidson, L.; Faulkner, A.; Petermann, L.; Manafò, E.; Kirkpatrick, S.I. Identifying attributes of food literacy: A scoping review. Public Health. Nutr. 2017, 20, 2406–2415. [Google Scholar] [CrossRef]
- Bisogni, C.; Bostic, S.; Sobal, J.; Jastran, M. Food literacy and food choice: A constructionist perspective. In Food Literacy; Vidgen, H., Ed.; Routledge: London, UK, 2016; pp. 102–117. [Google Scholar]
- Vidgen, H.A.; Gallegos, D. Defining food literacy and its components. Appetite 2014, 76, 50–59. [Google Scholar] [CrossRef]
- Gillis, D.E. Using a health literacy frame to conceptualize food literacy. In Food Literacy; Vidgen, H., Ed.; Routledge: London, UK, 2016; pp. 85–101. [Google Scholar]
- Truman, E.; Bischoff, M.; Elliott, C. Which literacy for health promotion: Health, food, nutrition or media? Health Promot. Int. 2020, 35, 432–444. [Google Scholar] [CrossRef]
- Vettori, V.; Lorini, C.; Milani, C.; Bonaccorsi, G. Towards the implementation of a conceptual framework of food and nutrition literacy: Providing healthy eating for the population. Int. J. Environ. Res. Public Health 2019, 16, 5041. [Google Scholar] [CrossRef]
- Sumner, J. Food literacy and adult education: Learning to read the world by eating. Can. J. Study Adult Educ. 2013, 25, 79–92. [Google Scholar]
- Cullen, T.; Hatch, J.; Martin, W.; Higgins, J.W.; Sheppard, R. Food Literacy: Definition and Framework for Action. Can. J. Diet. Pract. Res. 2015, 76, 140–145. [Google Scholar] [CrossRef] [PubMed]
- Frick, M.J.; Kahler, A.A.; Miller, W.W. A definition and the concepts of agricultural literacy. J. Agric. Educ. 1991, 32, 49–57. [Google Scholar] [CrossRef]
- Yeatman, H. Developing food literacy through food production. In Food Literacy; Vidgen, H., Ed.; Routledge: London, UK, 2016; pp. 205–220. [Google Scholar]
- Bachmair, B.; Bazalgette, C. The European Charter for Media Literacy: Meaning and potential. Res. Comp. Int. Educ. 2007, 2, 80–87. [Google Scholar] [CrossRef]
- National Association for Media Literacy Education. The Core Principles of Media Literacy Education. Available online: https://namle.net/publications/core-principles/ (accessed on 11 August 2020).
- Zarcadoolas, C.; Pleasant, A.; Greer, D.S. Understanding health literacy: An expanded model. Health Promot. Int. 2005, 20, 195–203. [Google Scholar] [CrossRef]
- Orr, D.W. Environmental education and ecological literacy. Educ. Dig. 1990, 55, 49–53. [Google Scholar]
- Puk, T.; Stibbards, A. Ecological concept development of preservice teacher candidates: Opaque empty shells. Int. J. Environ. Sci. Educ. 2010, 5, 461–476. [Google Scholar]
- Nutbeam, D. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promot. Int. 2000, 15, 259–267. [Google Scholar] [CrossRef]
- Slater, J. Is cooking dead? The state of Home Economics Food and Nutrition education in a Canadian province. Int. J. Consum. Stud. 2013, 37, 617–624. [Google Scholar] [CrossRef]
- Squire, L.R. Memory systems of the brain: A brief history and current perspective. Neurobiol. Learn. Mem. 2004, 82, 171–177. [Google Scholar] [CrossRef]
- Arnold, J.C. An integrated model of decision-making in health contexts: The role of science education in health education. Int. J. Sci. Educ. 2018, 40, 519–537. [Google Scholar] [CrossRef]
- Frick, J.; Kaiser, F.G.; Wilson, M. Environmental knowledge and conservation behavior: Exploring prevalence and structure in a representative sample. Personal. Individ. Differ. 2004, 37, 1597–1613. [Google Scholar] [CrossRef]
- Iverson, D.C.; Portnoy, B. Reassessment of the knowledge/attitude/behavior triad. Health Educ. 1977, 8, 31–34. [Google Scholar] [CrossRef] [PubMed]
- Wicker, A.W. Attitudes versus actions: The relationship of verbal and overt behavioral responses to attitude objects. J. Soc. Issues 1969, 25, 41–78. [Google Scholar] [CrossRef]
- Maslow, A.H. A Theory of Human Motivation. Psychol. Rev. 1943, 50, 370–396. [Google Scholar] [CrossRef]
- Rosenstock, I.M. Historical origins of the health belief model. Health Educ. Monogr. 1974, 2, 328–335. [Google Scholar] [CrossRef]
- Rosenstock, I.M.; Strecher, V.J.; Becker, M.H. Social learning theory and the health belief model. Health Educ. Q. 1988, 15, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Ajzen, I.; Madden, T.J. Prediction of goal-directed behavior: Attitudes, intentions, and perceived behavioral control. J. Exp. Soc. Psychol. 1986, 22, 453–474. [Google Scholar] [CrossRef]
- Bandura, A. Health promotion from the perspective of social cognitive theory. Psychol. Health 1998, 13, 623–649. [Google Scholar] [CrossRef]
- Truman, E.; Elliott, C. Barriers to food literacy: A conceptual model to explore factors inhibiting proficiency. J. Nutr. Educ. Behav. 2019, 51, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Schwarzer, R. Modeling health behavior change: How to predict and modify the adoption and maintenance of health behaviors. Appl. Psychol. 2008, 57, 1–29. [Google Scholar] [CrossRef]
- Carrington, M.J.; Neville, B.A.; Whitwell, G.J. Why ethical consumers don’t walk their talk: Towards a framework for understanding the gap between the ethical purchase intentions and actual buying behaviour of ethically minded consumers. J. Bus. Ethics 2010, 97, 139–158. [Google Scholar] [CrossRef]
- Brown, J.S.; Collins, A.; Duguid, P. Situated cognition and the culture of learning. Educ. Res. 1989, 18, 32–42. [Google Scholar] [CrossRef]
- Wahl, D.R.; Villinger, K.; Blumenschein, M.; König, L.M.; Ziesemer, K.; Sproesser, G.; Schupp, H.T.; Renner, B. Why We Eat What We Eat: Assessing Dispositional and In-the-Moment Eating Motives by Using Ecological Momentary Assessment. JMIR Mhealth Uhealth 2020, 8, e13191. [Google Scholar] [CrossRef]
- Hill, J.O.; Wyatt, H.R.; Reed, G.W.; Peters, J.C. Obesity and the environment: Where do we go from here? Science 2003, 299, 853–855. [Google Scholar] [CrossRef] [PubMed]
- Hill, J.O. Can a small-changes approach help address the obesity epidemic? A report of the Joint Task Force of the American Society for Nutrition, Institute of Food Technologists, and International Food Information Council. Am. J. Clin. Nutr. 2009, 89, 477–484. [Google Scholar] [CrossRef]
- Rosenbaum, M.E.; Franc, D.E. Opinion change as a function of external commitment and amount of discrepancy from the opinion of another. J. Abnorm. Soc. Psychol. 1960, 61, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Gollwitzer, P.M.; Sheeran, P. Implementation Intentions and Goal Achievement: A Meta-analysis of Effects and Processes. In Advances in Experimental Social Psychology; Academic Press: Cambridge, MA, USA, 2006; Volume 38, pp. 69–119. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schlüter, K.; Vamos, S.; Wacker, C.; Welter, V.D.E. A Conceptual Model Map on Health and Nutrition Behavior (CMMHB/NB). Int. J. Environ. Res. Public Health 2020, 17, 7829. https://doi.org/10.3390/ijerph17217829
Schlüter K, Vamos S, Wacker C, Welter VDE. A Conceptual Model Map on Health and Nutrition Behavior (CMMHB/NB). International Journal of Environmental Research and Public Health. 2020; 17(21):7829. https://doi.org/10.3390/ijerph17217829
Chicago/Turabian StyleSchlüter, Kirsten, Sandra Vamos, Corinne Wacker, and Virginia D. E. Welter. 2020. "A Conceptual Model Map on Health and Nutrition Behavior (CMMHB/NB)" International Journal of Environmental Research and Public Health 17, no. 21: 7829. https://doi.org/10.3390/ijerph17217829
APA StyleSchlüter, K., Vamos, S., Wacker, C., & Welter, V. D. E. (2020). A Conceptual Model Map on Health and Nutrition Behavior (CMMHB/NB). International Journal of Environmental Research and Public Health, 17(21), 7829. https://doi.org/10.3390/ijerph17217829




