Nature-Based Interventions and Mind–Body Interventions: Saving Public Health Costs Whilst Increasing Life Satisfaction and Happiness
Abstract
1. Introduction
1.1. Prevent to Save
1.2. Social Models of Health
1.3. Social Prescribing and Psychological Therapy Models
1.4. Nature-Based Interventions (NBIs) and Mind–Body Interventions (MBIs)
1.5. Theory of Change for Interventions
- (i)
- Opportunity: A logic of adherence—there need to be incentives and motivations for individuals to complete the course or programme.
- (ii)
- Motivation: The ability of individuals to incorporate the new behaviours, habits and activities into their lives beyond the course/programme in order to sustain health and well-being benefits over the long term, resulting in reductions in demand for public health and other public services (e.g., education support, criminal justice actions and support).
- (iii)
- Capability: A programme design that is intended to produce long-term and positive changes in individuals.
2. Materials and Methods
2.1. Four NBI and MBI Programmes of Intervention
2.1.1. Green Light Trust (NBI)
2.1.2. Ecominds (NBI)
2.1.3. Trust Links Growing Together (NBI)
2.1.4. Living Movement Tai Chi (MBI)
2.2. Assumptions
- We use the guidance and methods set out by the government’s Treasury Green Book [147] for benefits appraisal. The unit costs saved for public services are drawn from the New Economy Manchester cost–benefit analysis spreadsheets and unit costs database (v 2.0 updated April 2019), and draw upon costs in Pretty et al. [6]. We use best practice recommended in the Treasury Green Book by calculating cost savings over 1 and 10 years. We use a discount rate of 3.5% (costs saved today are worth more than those in the future), and a standard 2% GDP deflator (to take account of inflation). This permits creation of a net present social value (NPSV) for interventions.
- We use the norm of “reliable improvement” as an outcome measure [56,67]. Evaluations of Improving Access to Psychological Therapies (IAPT) programmes show that 40–50% of individuals make complete recoveries, and some 63–67% make reliable improvements over the long term. This suggests that some 30% of individuals do not benefit from the designed interventions. We thus differentiate where data exist between participants who make “reliable improvements” to their well-being and those who receive no benefit.
- A number of biases may be inherent in these analyses [147]. There may be an optimism bias of observers and deliverers of programmes that unintentionally inflates beneficial outcomes. There may be an unmeasured counterfactual of natural recovery: some improvements to individuals would have occurred regardless of the intervention, as would some adverse outcomes. Displacement may also occur: where one benefit achieved may be at the cost to another service. Regional variations in economic costs of programmes and service delivery are not included, nor can account be taken of cultural norms of behaviours and habits that may vary across social classes and at different locations in the UK. We also do not make adjustments for gender differences in uptake of programmes (SP typically shows a gender bias in uptake of 60% women, 40% men) or of outcomes (NBI programmes have found no differences in outcomes according to gender). Finally, no specific adjustments have been made for the substantial social, economic and cultural changes occurring since the worldwide outbreak of the Covid-19 virus.
- Economic evaluations of SP and NBI programmes have often included in their benefits register the costs saved from reductions in benefits payments (on the assumption that individuals have returned to work), and the increase tax contributions from such employment. The evidence is also compelling that these types of programmes can result in measurable improvements to self-esteem and mood, improved sleep patterns, and changed habits that would lead to greater happy longevity. Here we focus on costs saved from three types of public services: health and social care, police and criminal justice, and education. We also analyse the marginal improvements in life satisfaction and happiness, and indicate the substantial changes required in society to achieve similar benefits. We conclude that economic benefits measured by these interventions are minima, as not all changes have been monetised.
3. Results
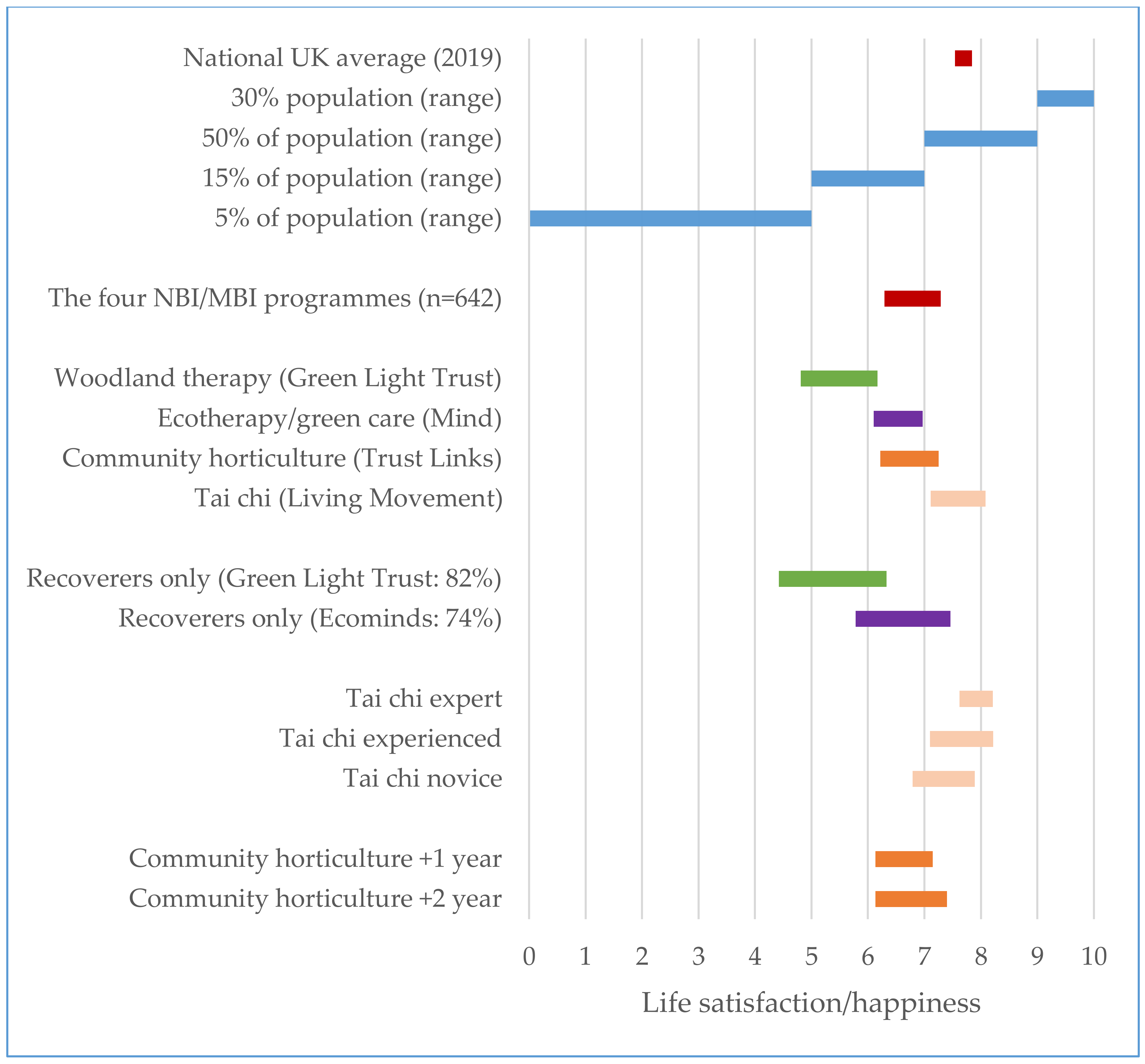
3.1. Impacts on Changes to Life Satisfaction/Happiness
3.2. Impacts on Costs Saved
- (a)
- Some evaluations of social prescribing programmes have recorded outcomes on service use, again though over variable time periods after intervention. The ranges for improvements after one year are 15–25% reductions in GP appointments, 20–25% reductions in A&E appointments, and 35–50% reductions in secondary treatments in hospitals [58]. We only have data on the use of public services from the GLT NBI (Table 2). These show changes in the use of GP appointments, A&E visits to hospitals, and recorded engagements with police and criminal justice systems.
- (b)
- We assume that the NBI programmes reduced loneliness and social isolation, as there are explicit aims to increase both nature and social connectedness. Loneliness increases annual GP visits by 1.8-fold and annual A&E visits by 1.6-fold [8]. We assume that these are reduced to the levels found in the GLT cohort. This results in additional Y1 savings of £714 and Y10 NPSV (savings) of £5317 (Table 3).
- (c)
- A third approach is to benchmark the changes in income that would be needed to achieve the equivalent improvements in LS/H observed in these NBI/MBI programmes [87,146,149]. Collins [150] has calculated that a 1 pt increase in LS/H produces higher economic benefits to individuals starting at lower LS/H: for those on the median income of £23 k, an increase of 1 pt from 4 to 5 is equal to +£13,100 of income; for those on 5 to 6, £9230 of income; for those on 6 to 7, £7140 of income, and for those on 7 to 8, £5920 of income. We assume that these benefits accrue only once, so are counted only in year 1. Taking the mean LS/H increase of +0.97 pt, after one year, the NBI of the Green Light Trust thus adds £12,097 of value to each individual; Ecominds and Trust Links add £6550, and the Living Movement tai chi £5430. The 10 year benefits are smaller, as both discount rates and inflation are added each year (Table 3).
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Friedman, H.S.; Martin, L.R. The Longevity Project; Hay House: London, UK, 2011. [Google Scholar]
- Gratton, L.; Scott, A. The 100 Year Life; Bloomsbury: London, UK, 2018. [Google Scholar]
- WHO. A Healthy Diet Sustainably Produced; WHO/NMH/NHD 18.18 Technical Report; WHO: Copenhagen, Denmark, 2018. [Google Scholar]
- Foresight. Mental Health—Future Challenge; Government Office of Science: London, UK, 2008.
- Royal Society. People and the Planet; Royal Society: London, UK, 2012. [Google Scholar]
- Pretty, J.; Barton, J.; Bharucha, Z.P.; Bragg, R.; Wood, C.; Pencheon, D. Improving health and well-being independently of GDP: Dividends of greener and prosocial economies. Int. J. Environ. Health Res. 2015, 11, 1–26. [Google Scholar] [CrossRef] [PubMed]
- Lancet. Planetary health: From concept to decisive action. Lancet 2019, 3, e402. [Google Scholar]
- CMO (Chief Medical Officer). Annual Report 2018: Better Health Within Reach; UK Government: London, UK, 2018.
- DHSC. Prevention Is Better than Cure; Department of Health and Social Care: London, UK, 2018. [Google Scholar]
- CMO (Chief Medical Officer). Chief Medical Officer’s Annual Report 2012: Our Children Deserve Better: Prevention Pays; UK Government: London, UK, 2013.
- AMS (Academy of Medical Sciences). Health of the Public in 2040; AMS: London, UK, 2018; Available online: https://acmedsci.ac.uk/policy/policy-projects/health-of-the-public-in-2040 (accessed on 1 July 2020).
- NHS. Social Prescribing. 2019. Available online: https://www.england.nhs.uk/personalisedcare/social-prescribing/ (accessed on 1 July 2020).
- Pretty, J.; Barton, J.; Rogerson, M. Green Mind Theory: How brain-body-behaviour links into natural and social environments for healthy habits. Int. J. Environ. Res. Public Health 2017, 14, 706. [Google Scholar] [CrossRef] [PubMed]
- Jackson, T. Prosperity without Growth; Earthscan: London, UK, 2009. [Google Scholar]
- Pretty, J. The consumption of a finite planet: Well-being, convergence, divergence, and the nascent green economy. Environ. Resour. Econ. 2013, 55, 475–499. [Google Scholar] [CrossRef]
- Dorling, D. Slowdown; Yale University Press: New Haven, CT, USA, 2020. [Google Scholar]
- Layard, R. Can We Be Happier? Pelican: London, UK, 2020. [Google Scholar]
- Easterlin, R.A. Does economic growth improve the human lot? Some empirical evidence. In Nations and Households in Economic Growth; Academic Press: Cambridge, MA, USA, 1974; pp. 89–125. [Google Scholar]
- Diener, E. Subjective well-being. The science of happiness and a proposal for a national index. Am. Psychol. 2000, 55, 34–43. [Google Scholar] [CrossRef] [PubMed]
- Raworth, K. Doughnut Economics: Seven Ways to Think like a 21st-Century Economist; Chelsea Green Publishing: White River Junction, VT, USA, 2017. [Google Scholar]
- Helliwell, J.F.; Layard, R.; Sachs, J.D. (Eds.) World Happiness Report 2019; Sustainable Development Solutions Network: New York, NY, USA, 2019. [Google Scholar]
- Helliwell, J.F.; Layard, R.; Sachs, J.D.; De Neve, J.-E. (Eds.) World Happiness Report 2020; Sustainable Development Solutions Network: New York, NY, USA, 2020. [Google Scholar]
- Kasser, T. The High Price of Materialism; MIT Press: Cambridge, MA, USA, 2002. [Google Scholar]
- Wilkinson, R.; Pickett, K. The Spirit Level; Penguin: London, UK; New York, NY, USA, 2009. [Google Scholar]
- Wilkinson, R.; Pickett, K. The Inner Level; Allen Lane: London, UK, 2016. [Google Scholar]
- Piketty, T.; Saez, E. Inequality in the long run. Science 2014, 344, 838–843. [Google Scholar] [CrossRef]
- Mitchell, R.; Popham, F. Effect of exposure to natural environment on health inequalities: An observational population study. Lancet 2008, 372, 1655–1660. [Google Scholar] [CrossRef]
- Mitchell, R.J.; Richardson, E.A.; Shortt, N.K.; Pearce, J.R. Neighborhood environments and socioeconomic inequalities in mental well-being. Am. J. Prev. Med. 2015, 49, 80–84. [Google Scholar] [CrossRef]
- Kim, S.H.; Kim, M.S.; Lee, M.S.; Park, Y.S.; Lee, H.J.; Kang, S.A.; Lee, H.S.; Lee, K.E.; Yang, H.J.; Kim, M.J.; et al. Korean diet: Characteristics and historical background. J. Ethn. Foods 2016, 3, 26–31. [Google Scholar] [CrossRef]
- Cacioppo, J.T.; Hawkley, L.C.; Berntson, G.G. The anatomy of loneliness. Curr. Dir. Psychol. Sci. 2003, 12, 71–74. [Google Scholar] [CrossRef]
- Hawkley, L.C.; Cacioppo, J.T. Aging and loneliness. Downhill quickly? Curr. Dir. Psychol. Sci. 2007, 16, 187–191. [Google Scholar] [CrossRef]
- Holt-Lunstad, J.; Smith, T.B.; Layton, J.B. Social relationships and mortality risk: A meta-analytic review. PLoS Med. 2010, 7, e1000316. [Google Scholar] [CrossRef] [PubMed]
- Holt-Lunstad, J.; Smith, T.B.; Baker, M.; Harris, T.; Stephenson, D. Loneliness and social isolation as risk factors for mortality: A meta-analytic review. Perspect. Psychol. Sci. 2015, 10, 227–237. [Google Scholar] [CrossRef] [PubMed]
- Holt-Lunstad, J.; Robles, T.F.; Sbarra, D.A. Advancing social connection as a public health priority in the United States. Am. Psychol. 2017, 72, 517. [Google Scholar] [CrossRef]
- Borgonovi, F. Doing well by doing good. The relationship between formal volunteering and self-reported health and happiness. Soc. Sci. Med. 2008, 66, 2321–2334. [Google Scholar] [CrossRef]
- Borgonovi, F. A life-cycle approach to the analysis of the relationship between social capital and health in Britain. Soc. Sci. Med. 2010, 71, 1927–1934. [Google Scholar] [CrossRef]
- Anderson, N.D.; Damianakis, T.; Kröger, E.; Wagner, L.M.; Dawson, D.R.; Binns, M.A.; Bernstein, S.; Caspi, E.; Cook, S.L. The benefits associated with volunteering among seniors: A critical review and recommendations for future research. Psychol. Bull. 2014, 140, 1505. [Google Scholar] [CrossRef]
- Rojas-Rueda, D.; Nieuwenhuijsen, M.J.; Gascon, M.; Perez-Leon, D.; Mudu, P. Green spaces and mortality: A systematic review and meta-analysis of cohort studies. Lancet Planet. Health 2019, 3, e469–e477. [Google Scholar] [CrossRef]
- Ward Thompson, C.; Silveirinha de Oliveira, E.; Tilley, S.; Elizalde, A.; Botha, W.; Briggs, A.; Cummins, S.; Leyland, A.H.; Roe, J.J.; Aspinall, P.; et al. Health impacts of environmental and social interventions designed to increase deprived communities’ access to urban woodlands: A mixed-methods study. Public Health Res. 2019, 7, 1–172. [Google Scholar] [CrossRef]
- Rogerson, M.; Brown, D.; Sandercock, G.; Wooler, J.; Barton, J. A comparison of four typical green exercise environments and prediction of psychological health outcomes. Perspect. Public Health 2015. [Google Scholar] [CrossRef]
- Micha, R.; Peñalvo, J.L.; Cudhea, F.; Imamura, F.; Rehm, C.D.; Mozaffarian, D. Association between dietary factors and mortality from heart disease, stroke, and type 2 diabetes in the United States. JAMA 2017, 317, 912–924. [Google Scholar] [CrossRef] [PubMed]
- Ji, J.S.; Zhu, A.; Bai, C.; Wu, C.D.; Yan, L.; Tang, S.; Zeng, Y.; James, P. Residential greenness and mortality in oldest-old women and men in China: A longitudinal cohort study. Lancet Planet. Health 2019, 3, e17–e25. [Google Scholar] [CrossRef]
- Marseglia, A.; Wang, H.X.; Rizzuto, D.; Fratiglioni, L.; Xu, W. Participating in mental, social, and physical leisure activities and having a rich social network reduce the incidence of diabetes-related dementia in a cohort of Swedish older adults. Diabetes Care 2019, 2, 232–239. [Google Scholar] [CrossRef] [PubMed]
- Lee, I.-M.; Paffenbarger, R.S. Associations of light, moderate, and vigorous intensity physical activity with longevity the harvard alumni health study. Am. J. Epidemiol. 2000, 151, 293–299. [Google Scholar] [CrossRef] [PubMed]
- Willcox, D.C.; Scapagnini, G.; Willcox, B.J. Healthy aging diets other than the Mediterranean: A focus on the Okinawan diet. Mech. Ageing Dev. 2014, 136, 148–162. [Google Scholar] [CrossRef]
- Steptoe, A.; Wardle, J. Enjoying life and living longer. Arch. Intern. Med. 2012, 172, 273–275. [Google Scholar] [CrossRef] [PubMed]
- Danner, D.D.; Snowdon, D.A.; Friesen, W.V. Positive emotions in early life and longevity: Findings from the nun study. J. Personal. Soc. Psychol. 2001, 80, 804–813. [Google Scholar] [CrossRef]
- Elwood, P.; Galante, J.; Pickering, J.; Palmer, S.; Bayer, A.; Ben-Shlomo, Y.; Longley, M.; Gallagher, J. Healthy lifestyles reduce the incidence of chronic diseases and dementia: Evidence from the Caerphilly Cohort Study. PLoS ONE 2013, 8, e81877. [Google Scholar] [CrossRef]
- Vaillant G, E. Aging Well; Little, Brown and Co.: Boston, MA, USA, 2002. [Google Scholar]
- Lee, H.S.; Duffey, K.J.; Popkin, B.M. South Korea’s entry to the global food economy: Shifts in consumption of food between 1998 and 2009. Asia Pac. J. Clin. Nutr. 2012, 21, 618. [Google Scholar]
- Levitin, D. The Changing Mind: A Neuroscientist’s Guide to Ageing Well; Penguin: London, UK, 2020. [Google Scholar]
- Bratman, G.N.; Hamilton, J.P.; Daily G, C. The impacts of nature experience on human cognitive function and mental health. Ann. N. Y. Acad. Sci. 2012, 1249, 118–136. [Google Scholar] [CrossRef]
- Bratman, G.N.; Anderson, C.B.; Berman, M.G.; Cochran, B.; De Vries, S.; Flanders, J.; Folke, C.; Frumkin, H.; Gross, J.J.; Hartig, T.; et al. Nature and mental health: An ecosystem service perspective. Sci. Adv. 2019, 5, eaax0903. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, L.; Ambrose-Oji, B.; Waite, S.; Aronsson, J.; Clark, M. Learning on the move: Green exercise for children and young people. In Green Exercise: Linking Nature, Health and Well-Being; Barton, J., Bragg, R., Wood, C., Pretty, J., Eds.; Routledge: Abingdon, UK, 2016. [Google Scholar]
- Clark, D.M. Realizing the mass public benefit of evidence-based psychological therapies: The IAPT program. Annu. Rev. Clin. Psychol. 2018, 14, 159–183. [Google Scholar] [CrossRef] [PubMed]
- IAPT. Psychological Therapies: Annual Report on the Use of IAPT Services 2018–19; NHS: London, UK, 2019. [Google Scholar]
- Chatterjee, H.J.; Camic, P.M.; Lockyer, B.; Thomson, L.J. Non-clinical community interventions: A systematised review of social prescribing schemes. Arts Health 2018, 10, 97–123. [Google Scholar] [CrossRef]
- NASP. National Academy for Social Prescribing 2020–2023 Strategic Plan; NASP: London, UK, 2019. [Google Scholar]
- Dayson, C.; Bashir, N.; Bennett, E.; Sanderson, E. The Rotherham Social Prescribing Service for People with Long-Term Health Conditions; Annual Evaluation Report; The Centre for Regional Economic and Social Research, Sheffield Hallam University: Sheffield, UK, 2016. [Google Scholar]
- Polley, M.J.; Pilkington, K. A Review of the Evidence Assessing Impact of Social Prescribing on Healthcare Demand and Cost Implications; University of Westminster: London, UK, 2017. [Google Scholar]
- Bickerdike, L.; Booth, A.; Wilson, P.M.; Farley, K.; Wright, K. Social prescribing: Less rhetoric and more reality. A systematic review of the evidence. BMJ Open 2017, 7. [Google Scholar] [CrossRef]
- Laing, K.; Steer, M.; Lawson, S.; Penn, L.; O’Brien, N.; Wildman, J. “It Was the Turning Point in My Life” How Ways to Wellness Social Prescribing Is Improving the Health and Wellbeing of People with Long Term Conditions; Newcastle University: Newcastle, UK, 2017. [Google Scholar]
- Alderwick, H.A.; Gottlieb, L.M.; Fichtenberg, C.M.; Adler, N.E. Social prescribing in the US and England: Emerging interventions to address patients’ social needs. Am. J. Prev. Med. 2018, 54, 715–718. [Google Scholar] [CrossRef]
- Bromley by Bow Centre. Annual Review 2018; Bromley by Bow: London, UK, 2018. [Google Scholar]
- Bragg, R.; Leck, C. Good Practice in Social Prescribing for Mental Health: The Role of Nature-Based Interventions; Natural England Commissioned Reports, Number 228; Natural England: York, UK, 2017. [Google Scholar]
- Robinson, J.M.; Jorgensen, A.; Cameron, R.; Brindley, P. Let Nature Be Thy Medicine: A Socioecological Exploration of Green Prescribing in the UK. Int. J. Environ. Res. Public Health 2020, 17, 3460. [Google Scholar] [CrossRef]
- Gyani, A.; Shafran, R.; Layard, R.; Clark, D.M. Enhancing recovery rates: Lessons from year one of IAPT. Behav. Res. Ther. 2013, 51, 597–606. [Google Scholar] [CrossRef]
- Radhakrishnan, M.; Hammond, G.; Jones, P.B.; Watson, A.; McMillan-Shields, F.; Lafortune, L. Cost of Improving Access to Psychological Therapies (IAPT) programme: An analysis of cost of session, treatment and recovery in selected Primary Care Trusts in the East of England region. Behav. Res. Ther. 2013, 51, 37–45. [Google Scholar] [CrossRef]
- Pigott, H.E.; Leventhal, A.M.; Alter, G.S.; Boren, J.J. Efficacy and effectiveness of antidepressants: Current status of research. Psychother. Psychosom. 2010, 79, 267–279. [Google Scholar] [CrossRef]
- McCormack, J.; Korownyk, C. Effectiveness of antidepressants. BMJ 2018, 360, k1073. [Google Scholar] [CrossRef]
- Pretty, J.; Peacock, J.; Sellens, M.; Griffin, M. The mental and physical health outcomes of green exercise. Int. J. Environ. Health Res. 2005, 15, 319–337. [Google Scholar] [CrossRef] [PubMed]
- Barton, J.; Bragg, R.; Wood, C.; Pretty, J. Green Exercise: Linking Nature, Health and Well-Being; Routledge: Oxon, UK, 2017. [Google Scholar]
- Barton, J.; Hine, R.E.; Pretty, J. The health benefits of walking in greenspaces of high natural and heritage value. J. Integr. Environ. Sci. 2009, 6, 261–278. [Google Scholar] [CrossRef]
- Barton, J.; Pretty, J. What is the best dose of nature and green exercise for mental health? A meta-study analysis. Environ. Sci. Technol. 2010, 44, 3947–3955. [Google Scholar] [CrossRef] [PubMed]
- Shanahan, D.F.; Bush, R.; Gaston, K.J.; Lin, B.B.; Dean, J.; Barber, E.; Fuller, R.A. Health benefits from nature experiences depend on dose. Sci. Rep. 2016, 6, 28551. [Google Scholar] [CrossRef]
- Rogerson, M.; Wood, C.; Pretty, J.; Schoenmakers, P.; Bloomfield, D.; Barton, J. Regular doses of nature: The efficacy of green exercise interventions for mental well-being. Int. J. Environ. Res. Public Health 2020, 17, 1526. [Google Scholar] [CrossRef]
- NEA. National Ecosystem Assessment; Defra: London, UK, 2011. [Google Scholar]
- Kubiszewski, I.; Costanza, R.; Anderson, S.; Sutton, P. The future value of ecosystem services: Global scenarios and national implications. Ecosyst. Serv. 2017, 26, 289–301. [Google Scholar] [CrossRef]
- Defra. The 25 Year Environment Plan; Department for Environment, Food and Rural Affairs: London, UK, 2019. [Google Scholar]
- Natural England. An Estimate of the Value and Cost Effectiveness of the Expanded Walking the Way to Health Initiative Scheme 2009 (TIN055); Natural England: London, UK, 2009. [Google Scholar]
- Hamann, G.A.; Ivtzan, I. 30 minutes in nature a day can increase mood, well-being, meaning in life and mindfulness: Effects of a pilot programme. Soc. Inq. Well-Being 2016, 2, 34–46. [Google Scholar]
- Bloomfield, D. What makes nature-based interventions for mental health successful? BJPsych Int. 2017, 14, 82–85. [Google Scholar] [CrossRef]
- Wolsko, C.; Lindberg, K.; Reese, R. Nature-based physical recreation leads to psychological well-being: Evidence from five studies. Ecopsychology 2019, 11, 222–235. [Google Scholar] [CrossRef]
- Cooley, S.J.; Jones, C.R.; Kurtz, A.; Robertson, N. ‘Into the Wild’: A meta-synthesis of talking therapy in natural outdoor spaces. Clin. Psychol. Rev. 2020, 77, 101841. [Google Scholar] [CrossRef]
- Hubbard, G.; Thompson, C.W.; Locke, R.; Jenkins, D.; Munoz, S.A.; Van Woerden, H.; Maxwell, M.; Yang, Y.; Gorely, T. Co-production of “nature walks for wellbeing” public health intervention for people with severe mental illness: Use of theory and practical know-how. BMC Public Health 2020, 20, 1–12. [Google Scholar] [CrossRef]
- Fields in Trust. Revaluing Parks and Green Space. 2019. Available online: http://www.fieldsintrust.org/revaluing (accessed on 1 July 2020).
- Wildlife Trusts. Social Return on Investment Analysis of the Health and Wellbeing Impacts of Wildlife Trust Programmes; Wildlife Trusts: Newark-on-Trent, UK, 2019; Available online: https://www.wildlifetrusts.org/news/new-report-reveals-prescribing-nature (accessed on 1 July 2020).
- Forest School Association. Available online: https://www.forestschoolassociation.org/what-is-forest-school/ (accessed on 1 July 2020).
- Barton, J.; Bragg, R.; Pretty, J.; Roberts, J.; Wood, C. The wilderness expedition: An effective life course intervention to improve young people’s well-being and connectedness to nature. J. Exp. Educ. 2016, 39, 59–72. [Google Scholar] [CrossRef]
- Wilderness Foundation. Available online: https://wildernessfoundation.org.uk/ (accessed on 1 July 2020).
- Bragg, R.; Barton, J.; Wood, C. (Eds.) Ecominds Effects on Mental Well-Being. An Evaluation for Mind; Mind: London, UK, 2013. [Google Scholar]
- Mind. Ecotherapy Works. Available online: https://www.mind.org.uk/news-campaigns/campaigns/ecotherapy-works/ (accessed on 1 July 2020).
- Ahlskog, J.E.; Geda, Y.E.; Graff-Radford, N.R.; Petersen, R.C. Physical exercise as a preventive or disease-modifying treatment of dementia and brain aging. Mayo Clin. Proc. 2011, 86, 876–884. [Google Scholar] [CrossRef] [PubMed]
- Dementia Adventure. Available online: https://dementiaadventure.co.uk/ (accessed on 1 July 2020).
- Jahnke, R.; Larkey, L.; Rogers, C.; Etnier, J.; Lin, F. A comprehensive review of health benefits of qigong and tai chi. Am. J. Health Promot. 2010, 24, e1–e25. [Google Scholar] [CrossRef]
- Bhasin, M.K.; Dusek, J.A.; Chang, B.H.; Joseph, M.G.; Denninger, J.W.; Fricchione, G.L.; Benson, H.; Libermann, T.A. Relaxation response induces temporal transcriptome changes in energy metabolism, insulin secretion and inflammatory pathways. PLoS ONE 2013, 8, e62817. [Google Scholar] [CrossRef]
- Wayne, P.M.; Fuerst, M.L. The Harvard Medical School Guide to Tai Chi; Shambhala: Boston, MA, USA, 2013. [Google Scholar]
- Villemure, C.; Čeko, M.; Cotton, V.A.; Bushnell, M.C. Insular cortex mediates increased pain tolerance in yoga practitioners. Cereb. Cortex 2014, 24, 2732–2740. [Google Scholar] [CrossRef] [PubMed]
- Villemure, C.; Ceko, M.; Cotton, V.A.; Bushnell, M.C. Neuroprotective effects of yoga practice: Age-, experience-, and frequency-dependent plasticity. Front. Hum. Neurosci. 2015, 9, 281. [Google Scholar] [CrossRef]
- Kuyken, W.; Hayes, R.; Barrett, B.; Byng, R.; Dalgleish, T.; Kessler, D.; Lewis, G.; Watkins, E.; Brejcha, C.; Cardy, J.; et al. Effectiveness and cost-effectiveness of mindfulness-based cognitive therapy compared with maintenance antidepressant treatment in the prevention of depressive relapse or recurrence (PREVENT): A randomised controlled trial. Lancet 2015, 386, 63–73. [Google Scholar] [CrossRef]
- Yang, G.Y.; Wang, L.Q.; Ren, J.; Zhang, Y.; Li, M.L.; Zhu, Y.T.; Luo, J.; Cheng, Y.J.; Li, W.Y.; Wayne, P.M.; et al. Evidence base of clinical studies on Tai Chi: A bibliometric analysis. PLoS ONE 2015, 10, e0120655. [Google Scholar] [CrossRef]
- Osypiuk, K.; Thompson, E.; Wayne, P.M. Can Tai Chi and Qigong postures shape our mood? Toward an embodied cognition framework for mind-body research. Front. Hum. Neurosci. 2018, 12, 174. [Google Scholar] [CrossRef]
- Walther, A.; Lacker, T.J.; Ehlert, U. Everybody was Kung-Fu fighting—The beneficial effects of Tai Chi Qigong and self-defense Kung-Fu training on psychological and endocrine health in middle aged and older men. Complementary Ther. Med. 2018, 36, 68–72. [Google Scholar] [CrossRef]
- Xiang, Y.; Lu, L.; Chen, X.; Wen, Z. Does Tai Chi relieve fatigue? A systematic review and meta-analysis of randomized controlled trials. PLoS ONE 2017, 12, e0174872. [Google Scholar] [CrossRef] [PubMed]
- Nisbet, E.K.; Zelenski, J.M.; Grandpierre, Z. Mindfulness in nature enhances connectedness and mood. Ecopsychology 2019, 11, 81–91. [Google Scholar] [CrossRef]
- Wang, C.; Li, K.; Choudhury, A.; Gaylord, S. Trends in yoga, Tai Chi, and Qigong use among US adults, 2002–2017. Am. J. Public Health 2019, 109, 755–761. [Google Scholar] [CrossRef]
- Fabjański, M.; Brymer, E. Enhancing health and wellbeing through immersion in nature: A conceptual perspective combining the Stoic and Buddhist traditions. Front. Psychol. 2017, 8, 1573. [Google Scholar] [CrossRef]
- Duvall, J.; Sullivan, W.C. How to get more out of the green exercise experience: Insights from attention restoration theory. In Green Exercise; Barton, J., Bragg, R., Wood, C., Pretty, J., Eds.; Routledge: Abingdon, UK, 2016. [Google Scholar]
- Pagnoni, G.; Cekic, M.; Guo, Y. “Thinking about not-thinking”: Neural correlates of conceptual processing during Zen meditation. PLoS ONE 2008, 3, e3083. [Google Scholar] [CrossRef]
- Goleman, D.; Davidson, R.J. Altered Traits: Science Reveals How Meditation Changes Your Mind, Brain, and Body; Penguin: London, UK, 2017. [Google Scholar]
- Kotler, S.; Wheal, J. Stealing Fire: How Silicon Valley, the Navy SEALs, and Maverick Scientists Are Revolutionizing the Way We Live and Work; HarperCollins: London, UK, 2017. [Google Scholar]
- Csikszentmihali, M. Flow: The Psychology of Happiness; Rider: London, UK, 2002. [Google Scholar]
- Brewer, J. The Craving Mind; Yale University Press: New Haven, CT, USA, 2017. [Google Scholar]
- Kahneman, D. Thinking, Fast and Slow; Macmillan: New York, NY, USA, 2011. [Google Scholar]
- Goleman, D. Focus: The Hidden Driver of Excellence; Bloomsbury: London, UK, 2013. [Google Scholar]
- Ricard, M. Happiness: A Guide to Developing Life’s Most Important Skill; Atlantic Books: London, UK, 2015. [Google Scholar]
- Esch, T.; Fricchione, G.L.; Stefano, G.B. The therapeutic use of the relaxation response in stress-related diseases. Med. Sci. Monit. 2003, 9, RA23–RA34. [Google Scholar]
- Dusek, J.A.; Otu, H.H.; Wohlhueter, A.L.; Bhasin, M.; Zerbini, L.F.; Joseph, M.G.; Benson, H.; Libermann, T.A. Genomic counter-stress changes induced by the relaxation response. PLoS ONE 2008, 3, e2576. [Google Scholar] [CrossRef]
- Dietrich, A. Functional neuroanatomy of altered states of consciousness: The transient hypofrontality hypothesis. Conscious. Cogn. 2003, 12, 231–256. [Google Scholar] [CrossRef]
- Dietrich, A. Transient hypofrontality as a mechanism for the psychological effects of exercise. Psychiatry Res. 2006, 145, 79–83. [Google Scholar] [CrossRef]
- Del Giorno, J.M.; Hall, E.E.; O’Leary, K.C.; Bixby, W.R.; Miller, P.C. Cognitive function during acute exercise: A test of the transient hypofrontality theory. J. Sport Exerc. Psychol. 2010, 32, 312–323. [Google Scholar] [CrossRef]
- Peres, J.F.; Moreira-Almeida, A.; Caixeta, L.; Leao, F.; Newberg, A. Neuroimaging during trance state: A contribution to the study of dissociation. PLoS ONE 2012, 7, e49360. [Google Scholar] [CrossRef]
- Pagnoni, G.; Guareschi, F.T. Remembrance of things to come: A conversation between Zen and neuroscience on the predictive nature of the mind. Mindfulness 2017, 8, 27–37. [Google Scholar] [CrossRef]
- Goyal, M.; Singh, S.; Sibinga, E.M.; Gould, N.F.; Rowland-Seymour, A.; Sharma, R.; Berger, Z.; Sleicher, D.; Maron, D.D.; Shihab, H.M.; et al. Meditation programs for psychological stress and well-being: A systematic review and meta-analysis. JAMA Intern. Med. 2014, 174, 357–368. [Google Scholar] [CrossRef]
- Buric, I.; Farias, M.; Jong, J.; Mee, C.; Brazil, I.A. What is the molecular signature of mind–body interventions? A systematic review of gene expression changes induced by meditation and related practices. Front. Immunol. 2017, 8, 670. [Google Scholar] [CrossRef]
- Duhigg, C. The Power of Habit; Random House: London, UK, 2012. [Google Scholar]
- Ouellette, J.A.; Wood, W. Habit and intention in everyday life: The multiple processes by which past behavior predicts future behavior. Psychol. Bull. 1998, 124, 54. [Google Scholar] [CrossRef]
- Verplanken, B.; Melkevik, O. Predicting habit: The case of physical exercise. Psychol. Sport Exerc. 2008, 9, 15–26. [Google Scholar] [CrossRef]
- Miltenberger, R.G.; Fuqua, R.W.; Woods, D.W. Applying behavior analysis to clinical problems: Review and analysis of habit reversal. J. Appl. Behav. Anal. 1998, 31, 447–469. [Google Scholar] [CrossRef] [PubMed]
- Miltenberger, R.G. Behavior Modification: Principles and Procedures; Cengage Learning: Boston, MA, USA, 2011. [Google Scholar]
- Judah, G.; Gardner, B.; Aunger, R. Forming a flossing habit: An exploratory study of the psychological determinants of habit formation. Br. J. Health Psychol. 2013, 18, 338–353. [Google Scholar] [CrossRef] [PubMed]
- Gardner, B.; Lally, P.; Wardle, J. Making health habitual: The psychology of ‘habit-formation’and general practice. Br. J. Gen. Pract. 2012, 62, 664–666. [Google Scholar] [CrossRef] [PubMed]
- Lally, P.; Van Jaarsveld, C.H.; Potts, H.W.; Wardle, J. How are habits formed: Modelling habit formation in the real world. Eur. J. Soc. Psychol. 2010, 40, 998–1009. [Google Scholar] [CrossRef]
- Pollan, M. In Defense of Food: An Eater’s Manifesto; Penguin: London, UK, 2008. [Google Scholar]
- Wilson, B. The Way We Eat Now; Basic Books: New York, NY, USA, 2020. [Google Scholar]
- Defra. Food Statistics in Your Pocket; Department for Environment, Food and Rural Affairs: London, UK, 2020. [Google Scholar]
- Lang, T. Feeding Britain; Penguin: London, UK, 2020. [Google Scholar]
- Barker, F.; Atkins, L.; de Lusignan, S. Applying the COM-B behaviour model and behaviour change wheel to develop an intervention to improve hearing-aid use in adult auditory rehabilitation. Int. J. Audiol. 2016, 55 (Suppl. S3), S90–S98. [Google Scholar] [CrossRef] [PubMed]
- West, R.; Michie, S. A brief introduction to the COM-B Model of behaviour and the PRIME Theory of motivation [v1]. Qeios 2020. [Google Scholar] [CrossRef]
- NEF. The Economic Benefits of Ecominds; New Economics Foundation: London, UK, 2013. [Google Scholar]
- Living Movement. Available online: https://www.livingmovement.com/ (accessed on 1 July 2020).
- Cheng, M.-C. Master Cheng’s New Method of Taichi Ch’uan Self-Cultivation; Hennessy, M., Translator; Blue Snake Books: Berkeley, CA, USA, 1999. [Google Scholar]
- Clark, A. The Complete Illustrated Guide to Tai Chi: A Practical Approach to the Ancient Chinese Movement for Health and Well-Being; Barnes and Noble: London, UK, 2001. [Google Scholar]
- DCMS. Taking Part Survey; Department for Digital, Culture, Media and Sport: London, UK, 2019. [Google Scholar]
- Clark, A.E.; Georgellis, Y. Back to baseline in Britain: Adaptation in the British household panel survey. Economica 2013, 80, 496–512. [Google Scholar] [CrossRef]
- Clark, A.E.; Fleche, S.; Layard, R.; Powdthavee, N.; Ward, G. The Origins of Happiness; Princeton University Press: Princeton, NJ, USA, 2018. [Google Scholar]
- HM Treasury. Treasury Green Book; HM Treasury: London, UK, 2019. [Google Scholar]
- ONS. Measuring National Well-Being, October 2019 Release; Office for National Statistics: London, UK, 2019.
- Fujiwara, D. General Method for Valuing Non-Market Goods Using Wellbeing Data: Three-Stage Wellbeing Valuation; CEP Discussion Paper No 1233; LSE: London, UK, 2013. [Google Scholar]
- Collins, B. How Do We Value Wellbeing? Combining Data to Put an Economic Value on the Change in Short Warwick Edinburgh Wellbeing Scale (SWEMWBS) Scores; University of Liverpool: Liverpool, UK, 2015. [Google Scholar]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.; Taylor, S.; Commission on Social Determinants of Health. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef]
- Sun, W.; Watanabe, M.; Tanimoto, Y.; Shibutani, T.; Kono, R.; Saito, M.; Usuda, K.; Kono, K. Factors associated with good self-rated health of non-disabled elderly living alone in Japan: A cross-sectional study. BMC Public Health 2007, 7, 297. [Google Scholar] [CrossRef]
- Willcox, B.J.; Willcox, D.C.; Ferrucci, L. Secrets of healthy aging and longevity from exceptional survivors around the globe: Lessons from octogenarians to supercentenarians. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2008, 63, 1181–1185. [Google Scholar] [CrossRef]
- Bergsma, A.; Buijt, I.; Veenhoven, R. Will happiness-trainings make us happier? A research synthesis using an online findings-archive. Front. Psychol. 2020, 11, 1953. [Google Scholar]
- Frumkin, H. The Health of Places, the Wealth of Evidence. In Urban Place, Reconnecting with the Natural World; Massachusetts Institute of Technology Press: Cambridge, MA, USA, 2005; pp. 253–269. [Google Scholar]
- UNEP. Towards a Green Economy: Pathways to Sustainable Development and Eradication of Poverty; UNEP: Nairobi, Kenya, 2011. [Google Scholar]
- Lang, T.; Rayner, G. Ecological public health: The 21st century’s big idea? An essay by Tim Lang and Geoff Rayner. BMJ 2012, 345, e5466. [Google Scholar] [CrossRef]
- IPCC. Climate Change and Land; IPCC: Geneva, Switzerland, 2019. [Google Scholar]
- CCC. Reducing UK Emissions: 2020 Progress Report; Committee on Climate Change, UK Government: London, UK, 2020. [Google Scholar]
- Enough Is Enough. Ideas for a Sustainable Economy in a World of Finite Resources; Report of the Steady State Economy Conference; O’Neill, D.W., Dietz, R., Jones, N., Eds.; Centre for the Advancement of the Steady State Economy; Economic Justice for All: Leeds, UK, 2010. [Google Scholar]
- Klein, N. This Changes Everything; Penguin: London, UK, 2015. [Google Scholar]
| NBI/MBI | Sample Size | Start LS/H Score (Mean Standard Deviation) | End LS/H Score (Mean Standard Deviation) | Margin of Change | Significance (Bonferroni-Adjusted t-Test) |
|---|---|---|---|---|---|
| All Participants | |||||
| Woodland Therapy: Green Light Trust | 32 | 2.12 | +1.36 | (p < 0.01) | |
| Horticulture: Trust Links | 328 | +1.03 | (p < 0.001) | ||
| Green Care: Ecominds | 154 | 2.33 | +0.87 | (p < 0.001) | |
| Tai Chi: Living Movement | 128 | +0.97 | (p < 0.01) | ||
| Summary: All Interventions | 642 | 2.12 | +1.00 | (p < 0.001) | |
| Segmented: Responders Only | |||||
| Woodland Therapy: Green Light Trust | 26 | +1.91 | (p < 0.001) | ||
| Horticulture: Trust Links | 285 | +1.60 | (p < 0.001) | ||
| Green Care: Ecominds | 122 | +1.68 | (p < 0.001) | ||
| Segmented: Negative Responders Only | |||||
| Woodland Therapy: Green Light Trust | 6 | −1.00 | (p = 0.28) | ||
| Horticulture: Trust Links | 43 | −1.35 | (p < 0.001) | ||
| Green Care: Ecominds | 32 | −2.32 | (p < 0.001) | ||
| Impact over 2 years | Mixed ANOVA | ||||
| Horticulture: Trust Links (0–12 months) | 166 | +1.02 | (p < 0.001) a | ||
| Horticulture: Trust Links (12–24 months) | 60 | +1.27 | |||
| Impact of Prior Practice/Expertise | Mixed ANOVA | ||||
| Tai Chi—Novice (0–49 h) | 53 | +1.10 | (p = 0.046) b | ||
| Tai Chi—Experienced (50–499 h) | 42 | +1.12 | (p < 0.001) c | ||
| Tai Chi—Expert (500–8000 h) | 33 | +0.59 |
| Changes in Number of GP Visits (over 12 Weeks of Programme Compared with Previous 12 Weeks) | Changes in Number of A&E Hospital Visits | Changes in Police Incidents | |
|---|---|---|---|
| GLT—whole cohort | −2.50 | −0.44 | +0.03 |
| GLT—responders only | −2.84 | −0.75 | −0.06 |
| Costs and Benefits | NBI/MBI | Benefits after Year 1 | Benefits after Year 10 |
|---|---|---|---|
| A: Costs prevented from reduced public services use (n = 32 or 26) | Green Light Trust | ||
| Full cohort | £831 | £6456 | |
| Responders only | £1521 | £11,980 | |
| B: Costs prevented from reduced loneliness (n = 671) | Green Light Trust, Ecominds, Trust Links, Living Movement | £714 | £5317 |
| C: Benefits created from increased LS/H (income equivalent) per individual | Green Light Trust | £12,097 | £7271 |
| Trust Links | £6550 | £3963 | |
| Ecominds | £6550 | £3963 | |
| Living Movement | £5430 | £3285 | |
| Total economic benefits per person (A + B + C) | Green Light Trust | ||
| Full cohort | £13,642 | £14,332 | |
| Responders only | £14,332 | £24,568 | |
| Trust Links * | £7264 | £9280 | |
| Ecominds * | £7264 | £9280 | |
| Living Movement * | £6144 | £8602 |
| Programme | Length of Programme | Intervention Time for each Individual | Cost (£) per Person | Sources |
|---|---|---|---|---|
| Green Light Trust: Earth | 12 weeks | 72 h | 960 | Green Light Trust (pers comm) |
| Green Light Trust: Air | 10 weeks | 60 h | 845 | |
| Nature-Based Interventions (general) | Variable | 24–36 h | 320 | [82] |
| Trust Links Growing Together | Open access all year | Uptake: 1–2 sessions per week (50–100 per year) | 1130 per year | Trust Links (pers comm) |
| Social Prescribing | Variable | 153 | [61] | |
| Mindfulness-Based Cognitive Therapy for Depression | 8 weeks + refreshers over months 5–14 | 18 h + 4 refresher hours | 112 | [100] |
| IAPT—Low Intensity | 7 weeks | 7 | 493 | [68] |
| IAPT—High Intensity | 7 weeks | 20 | 1416 | |
| IAPT—All | 7–20 sessions (x 1 hr) | 680 | [55,56] |
| End Y1 | End Y10 | |
|---|---|---|
| Green Light Trust (prevented public health and services costs only) | ||
| Full cohort | 1.71 | 12.9 |
| Responders only | 2.47 | 19.1 |
| Green Light Trust (total benefits) | ||
| Full cohort | 15.1 | 15.8 |
| Responders only | 15.8 | 27.1 |
| Trust Links (total benefits) | ||
| All | 6.42 | 7.61 |
| Changes in Life Satisfaction/Happiness (LS/H) across Whole Populations | Number of Countries | Number of Cities | |
|---|---|---|---|
| 2005–2006 to 2016–2018 | 2008–2012 to 2017–2019 | 2005 to 2013 | |
| Increases >1.0 | 5 | 10 | 0 |
| 0.5–0.99 | 30 | 31 | 22 |
| 0.0–0.49 | 43 | 34 | 66 |
| Falls by −0.01 to −1.5 | 50 | 71 | 81 |
| Significant Life Event | Women/Men | Effect on LS/Happiness (on 1–10 Scale) | Changes in 5 Years after the Life Event |
|---|---|---|---|
| Partnership | Women | +0.5 to +0.7 | Stable |
| Men | +0.4 to +0.5 | ||
| Parenthood | Women | +0.4 | Stable |
| Men | +0.2 | ||
| Separation/Divorce | Women | −0.5 to −1.0 | Then rising by +0.5 after 4–5 years |
| Men | −1.0 to −1.3 | ||
| Widowhood | Women | −0.6 to −1.0 | Then returning completely after 1 year |
| Men | −0.5 to −1.0 | ||
| Loss of Employment | Women | −0.4 | Then falling to −1.2 after 5 years |
| Men | −0.4 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pretty, J.; Barton, J. Nature-Based Interventions and Mind–Body Interventions: Saving Public Health Costs Whilst Increasing Life Satisfaction and Happiness. Int. J. Environ. Res. Public Health 2020, 17, 7769. https://doi.org/10.3390/ijerph17217769
Pretty J, Barton J. Nature-Based Interventions and Mind–Body Interventions: Saving Public Health Costs Whilst Increasing Life Satisfaction and Happiness. International Journal of Environmental Research and Public Health. 2020; 17(21):7769. https://doi.org/10.3390/ijerph17217769
Chicago/Turabian StylePretty, Jules, and Jo Barton. 2020. "Nature-Based Interventions and Mind–Body Interventions: Saving Public Health Costs Whilst Increasing Life Satisfaction and Happiness" International Journal of Environmental Research and Public Health 17, no. 21: 7769. https://doi.org/10.3390/ijerph17217769
APA StylePretty, J., & Barton, J. (2020). Nature-Based Interventions and Mind–Body Interventions: Saving Public Health Costs Whilst Increasing Life Satisfaction and Happiness. International Journal of Environmental Research and Public Health, 17(21), 7769. https://doi.org/10.3390/ijerph17217769






