Exploring Mechanisms of Action: Using a Testing Typology to Understand Intervention Performance in an HIV Self-Testing RCT in England and Wales
Abstract
1. Introduction
1.1. HIV Self-Testing in the UK
1.2. SELPHI HIV Self-Testing RCT
1.3. Understanding HIVST Interventions
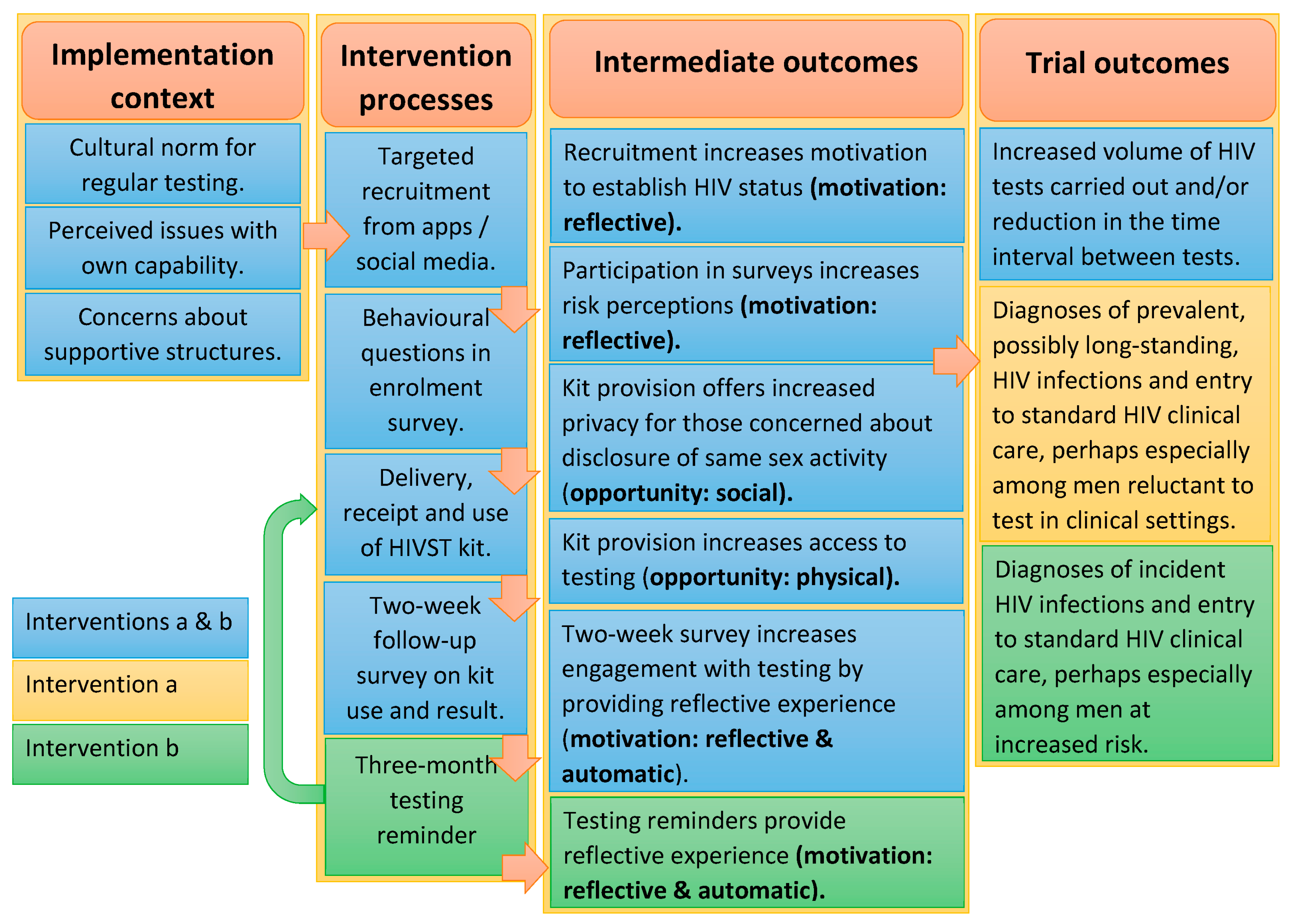
1.4. SELPHI Logic Model
2. Methods
2.1. Participants and Procedures
2.2. Analytic Procedures
3. Results
3.1. A Testing Typology
3.1.1. Inexperienced Testers
3.1.2. Pro Self-Testers
3.1.3. Opportunistic Adopters
3.2. Intervention Components and Behavioural Influences
3.2.1. Recruitment and Testing Motivation
Deep down, I knew that it was something that I should do anyway. And it was free. And I knew that not all people would get it. But it was free if I was selected. And it just seemed like I’d no excuse, really, to turn it down. It’s free. It would be in private. I wouldn’t have to go to the clinic. And I’d get a little bit of peace of mind if it came back negative. (23-year-old man, undisclosed sexual orientation, not previously tested, inexperienced tester).
For me, it was timing. It was just a case of like, ‘okay, it’s been a year’; I knew I had had some…maybe not the cleverest of sexual encounters a couple of months beforehand, and it literally landed at the right time in my thought processes so I was like ‘yep, we’ve got that whole World AIDS Day thing coming up again, and this is probably about the right time to get tested again’. (29-year-old gay man, tested in last 12 months, pro self-tester)
3.2.2. Surveys and Risk Perception
Some of the questions […] I felt might make some people worry, maybe […] The ones relating to having sex without protection. Also, having sex whilst taking drugs as well. That was another one. And I thought, ‘oh, okay, well, that’s half of gaydom’. (49-year-old man, undisclosed sexual orientation, tested in last 12 months, pro self-tester).
It doesn’t make me feel any different about myself. Because I have been actively gay for 20 years now. Maybe or definitely, in my early years, that would make me feel uncomfortable that I was promiscuous, so to speak. But having been active for 20 years now, it’s not something that bothers me anymore. (40-year-old gay man, tested in last 12 months, opportunistic adopter)
3.2.3. Kit Provision and Privacy to Test
The SELPHI thing actually appealed to me that I could be totally anonymous. […] I’ll say the shame and embarrassment. And I’ll put it that way because I’m in the closet and probably prefer to remain that way. So, it is the difficulty of taking that step [accessing a clinic]. […] (55-year-old bisexual man, not previously tested, inexperienced tester)
3.2.4. Kit Provision Increases HIV Testing Access
I started having sex with other men more frequently. And, at that point, I started to consider [testing for HIV]. And that was around the time when... about a month or so after that when, I think, the SELPHI thing came up on Grindr. And that’s when I thought, mmm, self-testing seemed like a better idea, I thought. (23-year-old man, undisclosed sexual orientation, not previously tested, inexperienced tester)
But when I had seen it, and doing it at home I thought it was a great idea, because you’re at home, you can sit and get your result there and then, you can take it from there, and go and get support if you needed to. (30-year-old gay man, tested in last three months, pro self-tester)
So, I think for me, whenever I found out about this I was like, ‘Okay, well that makes my life a lot easier,’ because I work long hours and I have quite an unpredictable job. So, trying to maybe get time off and having that time off assured so that I can go to an appointment is quite difficult, so this study was very helpful. (27-year old gay man, tested in last three months, opportunistic adopter)
3.2.5. Two-Week Survey and Testing Engagement
I’ve done the test and then there was nothing for a while, and then you get the survey back and you feel, ‘Oh yes, they are still thinking about me. I am still part of this study, I still feel included.’ Whereas I think if it’d just been left and there was nothing you have thought, ‘Well, okay, I’ve got a free test out of it but what’s the point?’ (35-year-old gay man, tested in last 12 months, inexperienced tester)
Interviewer: So, if you were getting the test from the NHS, you wouldn’t necessarily want to fill out one of those surveys?
Participant: I wouldn’t want to, but I think it would be good practice to. If you were going to distribute self-tests, it would be good to use a follow-up. If in my situation now, if I wasn’t studying it, if it was just a routine thing and it was negative, I probably wouldn’t fill it out, it’d go into the junk box. But I still think it’s probably a good thing to do. (32-year-old gay man, tested in last 12 months, pro self-tester).
I took it as a study. I felt like I was trialling something, I didn’t have any expectations of what it would be. Nothing stood out to me, but again, with my sexual health and dealing with sexual health services, there is a resilience or comfortability of having to share information, if that makes sense? (25-year-old gay man, tested in last 12 months, opportunistic adopter)
3.2.6. Testing Reminders and Reflection
Just made me think a bit harder of the past three months, what I’d been doing, yeah. It didn’t make me feel anything like I shouldn’t be asked this or this and that, yeah, it was just a questionnaire and it just made me think about all the movement I had in the last three months [...] (27-year-old bisexual man, tested in last six months, pro self-tester)
4. Discussion
4.1. Strength and Limitations
4.2. COM-B, HIVST, and Challenges for the Model
4.3. Considerations for Future HIVST Intervention Development
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Granich, R.M.; Gilks, C.F.; Dye, C.; De Cock, K.M.; Williams, B.G. Universal voluntary HIV testing with immediate antiretroviral therapy as a strategy for elimination of HIV transmission: A mathematical model. Lancet 2009, 373, 48–57. [Google Scholar] [CrossRef]
- Phillips, A.N.; Cambiano, V.; Miners, A.; Lampe, F.C.; Rodger, A.; Nakagawa, F.; Brown, A.; Gill, Q.N.; De Angelis, D.; Elford, J.; et al. Potential impact on HIV incidence of higher HIV testing rates and earlier antiretroviral therapy initiation in MSM. AIDS 2015, 29, 1855–1862. [Google Scholar] [CrossRef] [PubMed]
- Rodger, A.J.; Cambiano, V.; Bruun, T.; Vernazza, P.; Collins, S.; van Lunzen, J.; Corbelli, G.M.; Estrada, V.; Geretti, A.M.; Beloukas, A.; et al. Sexual Activity Without Condoms and Risk of HIV Transmission in Serodifferent Couples When the HIV-Positive Partner Is Using Suppressive Antiretroviral Therapy. JAMA 2016, 316, 171–181. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.C.; Rodger, A.J. New initiatives to develop self-testing for HIV. Curr. Opin. Infect. Dis. 2017, 30, 50–57. [Google Scholar] [CrossRef] [PubMed]
- Rodger, A.J.; Cambiano, V.; Bruun, T.; Vernazza, P.; Collins, S.; Degen, O.; Corbelli, G.M.; Estrada, V.; Geretti, A.M.; Beloukas, A.; et al. Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): Final results of a multicentre, prospective, observational study. Lancet 2019, 393, 2428–2438. [Google Scholar] [CrossRef]
- Witzel, T.C.; Melendez-Torres, G.J.; Hickson, F.; Weatherburn, P. HIV testing history and preferences or future tests among gay men, bisexual men and other MSM in England: Results from a cross-sectional study. BMJ Open 2016, 6, e011372. [Google Scholar] [CrossRef]
- Flowers, P.; Estcourt, C.; Sonnenberg, P.; Burns, F. HIV testing intervention development among men who have sex with men in the developed world. Sex. Health 2017, 14, 80–88. [Google Scholar] [CrossRef][Green Version]
- Flowers, P.; Knussen, C.; Li, J.; McDaid, L. Has testing been normalized? An analysis of changes in barriers to HIV testing among men who have sex with men between 2000 and 2010 in Scotland, UK. HIV Med. 2013, 14, 92–98. [Google Scholar] [CrossRef]
- Witzel, T.C.; Weatherburn, P.; Rodger, A.J.; Bourne, A.H.; Burns, F.M. Risk, reassurance and routine: A qualitative study of narrative understandings of the potential for HIV self-testing among men who have sex with men in England. BMC Public Health 2017, 17, 491. [Google Scholar] [CrossRef]
- Witzel, T.C.; Guise, A.; Nutland, W.; Bourne, A. It Starts With Me: Privacy concerns and stigma in the evaluation of a Facebook health promotion intervention. Sex. Health 2016, 13, 228–233. [Google Scholar] [CrossRef]
- Witzel, T.C.; Rodger, A.J.; Burns, F.M.; Rhodes, T.; Weatherburn, P. HIV Self-Testing among Men Who Have Sex with Men (MSM) in the UK: A Qualitative Study of Barriers and Facilitators, Intervention Preferences and Perceived Impacts. PLoS ONE 2016, 11, e0162713. [Google Scholar] [CrossRef] [PubMed]
- Vera, J.H.; Soni, S.; Pollard, A.; Llewellyn, C.; Peralta, C.; Rodriguez, L.; Dean, G. Acceptability and feasibility of using digital vending machines to deliver HIV self-tests to men who have sex with men. Sex. Transm. Infect. 2019, 95, 557–561. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, M.M.; Dunn, D.T.; Speakman, A.; McCabe, L.; Ward, D.; Witzel, T.C.; Harbottle, J.; Collins, S.; Gafos, M.; Burns, F.M.; et al. Protocol, rationale and design of SELPHI: A randomised controlled trial assessing whether offering free HIV self-testing kits via the internet increases the rate of HIV diagnosis. BMC Infect. Dis. 2018, 18, 531. [Google Scholar] [CrossRef]
- Witzel, T.C.; Gabriel, M.M.; Weatherburn, P.; Gafos, M.; Speakman, A.; Pebody, R.; Burns, F.M.; Bonell, C.; Lampe, F.C.; Dunn, D.T.; et al. Pilot phase of an internet-based RCT of HIVST targeting MSM and transgender people in England and Wales: Advertising strategies and acceptability of the intervention. BMC Infect. Dis. 2019, 699, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.C.; Bourne, A.; Burns, F.M.; Rodger, A.J.; McCabe, L.; Gabriel, M.M.; Gafos, D.; Ward, D.; Collaco-Moraes, Y.; Dunn, D.T.; et al. HIV self-testing intervention experiences and kit usability: Results from a qualitative study among men who have sex with men in the SELPHI (Self-Testing Public Health Intervention) randomized controlled trial in England and Wales. HIV Med. 2019. [Google Scholar] [CrossRef]
- Michie, S.; van Stralen, M.M.; West, R. The behaviour change wheel: A new method for characterising and designing behaviour change interventions. Implement. Sci. 2011, 6, 42. [Google Scholar] [CrossRef]
- Coulson, N.S.; Ferguson, M.A.; Henshaw, H.; Heffernan, E. Applying theories of health behaviour and change to hearing health research: Time for a new approach. Int. J. Audiol. 2016, 55, S99–S104. [Google Scholar] [CrossRef]
- Ogden, J. Celebrating variability and a call to limit systematisation: The example of the behaviour change technique taxonomy and the behaviour change wheel. Health Psychol. Rev. 2016, 10, 245–250. [Google Scholar] [CrossRef] [PubMed]
- Barker, F.; Atkins, L.; de Lusignan, S. Applying the COM-B behaviour model and behaviour change wheel to develop an intervention to improve hearing-aid use in adult auditory rehabilitation. Int. J. Audiol. 2016, 55, S90–S98. [Google Scholar] [CrossRef]
- Lister, C.; West, J.H.; Cannon, B.; Sax, T.; Brodegard, D. Just a fad? Gamification in health and fitness apps. JMIR Serious Games 2014, 2, e9. [Google Scholar] [CrossRef]
- Chiang, N.; Guo, M.; Amico, K.R.; Atkins, L.; Lester, R.T. Interactive two-way mHealth interventions for improving medication adherence: An evaluation using the behaviour change wheel framework. JMIR mHealth uHealth 2018, 6, e87. [Google Scholar] [CrossRef] [PubMed]
- Webster, R.; Bailey, J.V. Development of a theory-based interactive digital intervention to improve condom use in men in sexual health clinics: An application of qualitative methods using the behaviour change wheel. Lancet 2013, 382, S102. [Google Scholar] [CrossRef]
- Seguin, M.; Dodds, C.; Mugweni, E.; McDaid, L.; Flowers, P.; Wayal, S.; Zomer, E.; Weatherburn, P.; Fakoya, I.; Hartney, T.; et al. Self-sampling kits to increase HIV testing among black Africans in the UK: The HAUS mixed-methods study. Health Technol. Assess. 2018, 22. [Google Scholar] [CrossRef] [PubMed]
- Banda, J. Rapid Home HIV Testing: Risk and the Moral Imperatives of Biological Citizenship. Body Soc. 2014, 21, 24–47. [Google Scholar] [CrossRef]
- Bavinton, B.R.; Brown, G.; Hurley, M.; Bradley, J.; Keen, P.; Conway, D.P.; Guy, R.; Grulich, A.E.; Prestage, G. Which gay men would increase their frequency of HIV testing with home self-testing? AIDS Behav. 2013, 17, 2084–2092. [Google Scholar] [CrossRef] [PubMed]
- Figueroa, C.; Johnson, C.; Verster, A.; Baggaley, R. Attitudes and Acceptability on HIV Self-testing Among Key Populations: A Literature Review. AIDS Behav. 2015, 19, 1949–1965. [Google Scholar] [CrossRef]
- Bilardi, J.E.; Walker, S.; Read, T.; Prestage, G.; Chen, M.Y.; Guy, R.; Bradshaw, C.; Fairley, C.K. Gay and bisexual men’s views on rapid self-testing for HIV. AIDS Behav. 2013, 17, 2093–2099. [Google Scholar] [CrossRef]
- Nelson, M.C.; Cordray, D.S.; Hulleman, C.S.; Darrow, C.L.; Sommer, E.C. A procedure for assessing intervention fidelity in experiments testing educational and behavioral interventions. J. Behav. Health Serv. Res. 2012, 39, 374–396. [Google Scholar] [CrossRef]
- Witzel, T.C.; Weatherburn, P.; Burns, F.M.; Johnson, C.C.; Figueroa, C.; Rodger, A.J. Consolidating emerging evidence surrounding HIVST and HIVSS: A rapid systematic mapping protocol. Syst. Rev. 2017, 6, 72. [Google Scholar] [CrossRef]
- Witzel, T.C.; Burns, F.M.; Weatherburn, P.; Rodger, A.J. What are the perspectives of key informants on the implementation HIV self-testing (HIVST) in England? A qualitative study of barriers, facilitators and anticipated impacts. Sex. Transm. Infect. 2017, 93, A42. [Google Scholar]
- McCutcheon, A.L. Latent Class Analysis; Sage: Thousand Oaks, CA, USA, 1987. [Google Scholar]
- Vermunt, J.K.; Magidson, J. Latent class cluster analysis. Appl. Latent Cl. Anal. 2002, 11, 89–106. [Google Scholar]
- Flowers, P.; Riddell, J.; Park, C.; Ahmed, B.; Young, I.; Frankis, J.; Davis, M.; Gilbert, M.; Estcourt, C.; Wallace, L.; et al. Preparedness for use of the rapid result HIV self-test by gay men and other men who have sex with men (MSM): A mixed methods exploratory study among MSM and those involved in HIV prevention and care. HIV Med. 2016, 18, 245–255. [Google Scholar] [CrossRef] [PubMed]
- Ritchie, J.; Spencer, L. Qualitative Data Analysis for Applied Policy Research. In Analyzing Qualitative Data; Bryman, A., Burgess, R.G., Eds.; Taylor & Francis Books Ltd.: Abingdon, UK, 1994. [Google Scholar]
- Witzel, T.C.; Nutland, W.; Bourne, A. What qualities in a potential HIV pre-exposure prophylaxis service are valued by black men who have sex with men in London? A qualitative acceptability study. Int. J. STD AIDS 2018, 29, 760–765. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.C.; Nutland, W.; Bourne, A. What are the motivations and barriers to pre-exposure prophylaxis (PrEP) use among black men who have sex with men aged 18–45 in London? Results from a qualitative study. Sex. Transm. Infect. 2019, 95, 262–266. [Google Scholar] [CrossRef]
- Young, I.; Li, J.; McDaid, L. Awareness and willingness to use HIV pre-exposure prophylaxis amongst gay and bisexual men in Scotland: Implications for biomedical HIV prevention. PLoS ONE 2013, 8, e64038. [Google Scholar] [CrossRef]
- Bradshaw, J. Taxonomy of Social Need; Oxford University Press: London, UK, 1972. [Google Scholar]
- Carver, N.A.; Ward, B.M.; Talbot, L.A. Using Bradshaw’s Taxonomy of Needs: Listening to women in planning pregnancy care. Contemp. Nurse 2008, 30, 76–82. [Google Scholar] [CrossRef]



| Interventions | Definition |
|---|---|
| Education | Increasing knowledge or understanding |
| Persuasion | Using communication to induce positive or negative feelings or stimulate action |
| Incentivisation | Creating expectation of reward |
| Coercion | Creating expectation of punishment or cost |
| Training | Imparting skills |
| Restriction | Using rules to reduce the opportunity to engage in the target behaviour (or to increase the target behaviour by reducing the opportunity to engage in competing behaviours) |
| Environmental restructuring | Changing the physical or social context |
| Modelling | Providing an example for people to aspire to or imitate |
| Enablement | Increasing means/reducing barriers to increase capability or opportunity 1 |
| Model of behaviour: sources | Education | Persuasion | Incentivisation | Coercion | Training | Restriction | Environmental restructuring | Modelling | Enablement |
|---|---|---|---|---|---|---|---|---|---|
| C-Ph | √ | √ | |||||||
| C-Ps | √ | √ | √ | ||||||
| M-Re | √ | √ | √ | √ | |||||
| M-Au | √ | √ | √ | √ | √ | √ | |||
| O-Ph | √ | √ | √ | ||||||
| O-So | √ | √ | √ |
| Ethnicity | White | 29 |
| Black | 3 | |
| Asian | 2 | |
| Other/mixed | 3 | |
| Sexual orientation | Gay | 24 |
| Bisexual | 5 | |
| Don’t use a term | 1 | |
| Undisclosed | 7 | |
| Recency of HIV testing | Never tested | 7 |
| 12 months + | 17 | |
| <12 months | 13 | |
| Highest education qualification | Low 1 | 7 |
| Medium 2 | 11 | |
| High 3 | 19 | |
| Condomless anal intercourse partners in preceding three months | 0 | 12 |
| 1 | 14 | |
| 2–3 | 7 | |
| 4–10 | 4 | |
| 10+ | 0 | |
| Test outcome | Positive | 2 |
| Negative | 35 | |
| Intervention | Intervention A | 27 |
| Intervention B | 10 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Witzel, T.C.; Weatherburn, P.; Bourne, A.; Rodger, A.J.; Bonell, C.; Gafos, M.; Trevelion, R.; Speakman, A.; Lampe, F.; Ward, D.; et al. Exploring Mechanisms of Action: Using a Testing Typology to Understand Intervention Performance in an HIV Self-Testing RCT in England and Wales. Int. J. Environ. Res. Public Health 2020, 17, 466. https://doi.org/10.3390/ijerph17020466
Witzel TC, Weatherburn P, Bourne A, Rodger AJ, Bonell C, Gafos M, Trevelion R, Speakman A, Lampe F, Ward D, et al. Exploring Mechanisms of Action: Using a Testing Typology to Understand Intervention Performance in an HIV Self-Testing RCT in England and Wales. International Journal of Environmental Research and Public Health. 2020; 17(2):466. https://doi.org/10.3390/ijerph17020466
Chicago/Turabian StyleWitzel, T. Charles, Peter Weatherburn, Adam Bourne, Alison J. Rodger, Chris Bonell, Mitzy Gafos, Roy Trevelion, Andrew Speakman, Fiona Lampe, Denise Ward, and et al. 2020. "Exploring Mechanisms of Action: Using a Testing Typology to Understand Intervention Performance in an HIV Self-Testing RCT in England and Wales" International Journal of Environmental Research and Public Health 17, no. 2: 466. https://doi.org/10.3390/ijerph17020466
APA StyleWitzel, T. C., Weatherburn, P., Bourne, A., Rodger, A. J., Bonell, C., Gafos, M., Trevelion, R., Speakman, A., Lampe, F., Ward, D., Dunn, D. T., Gabriel, M. M., McCabe, L., Harbottle, J., Collaco Moraes, Y., Michie, S., Phillips, A. N., McCormack, S., & Burns, F. M. (2020). Exploring Mechanisms of Action: Using a Testing Typology to Understand Intervention Performance in an HIV Self-Testing RCT in England and Wales. International Journal of Environmental Research and Public Health, 17(2), 466. https://doi.org/10.3390/ijerph17020466





