Optimal Time of Thermotherapy for Reducing Pain, Anxiety, and Side Effects in Arteriovenous Fistula Puncture Patients: A Randomized Controlled Trial
Abstract
1. Introduction
2. Materials and Method
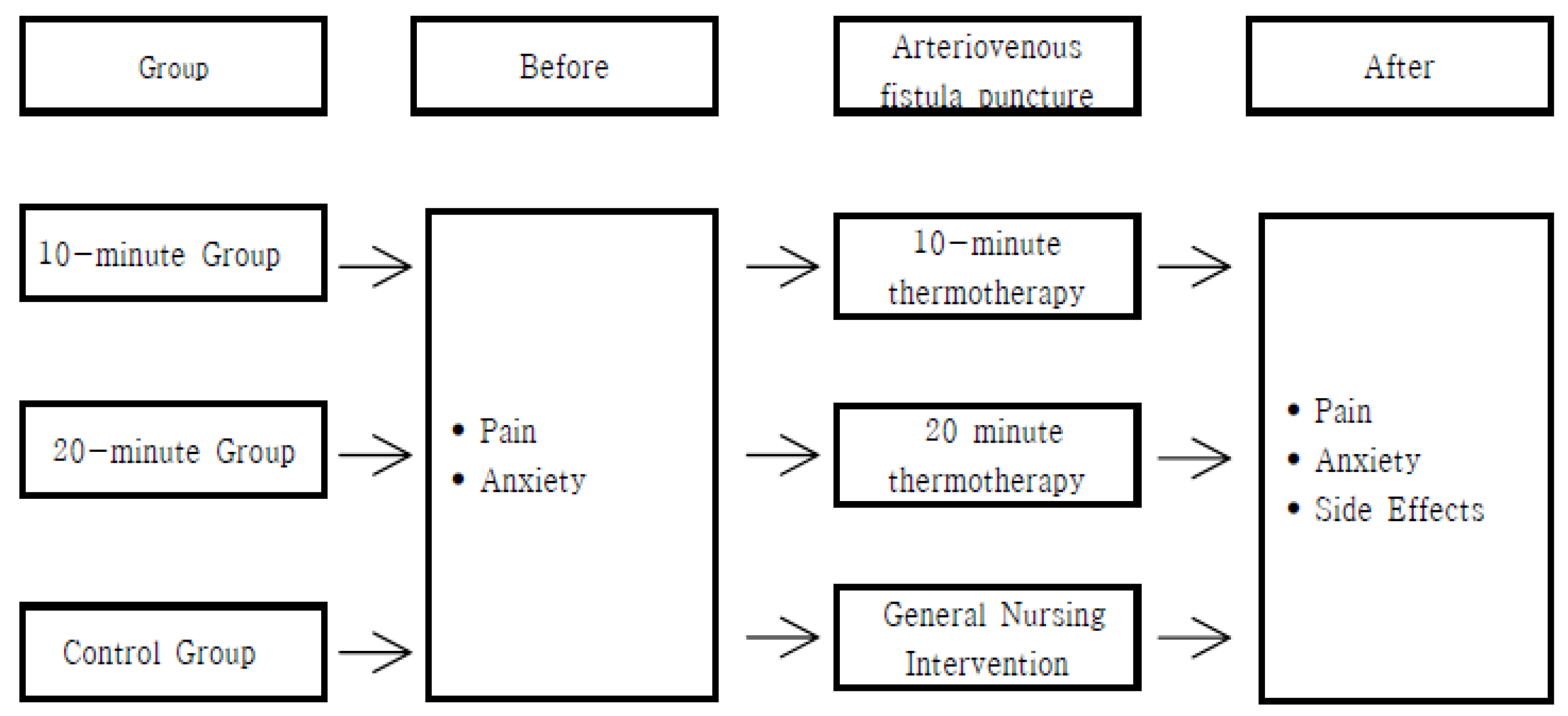
2.1. Study Design
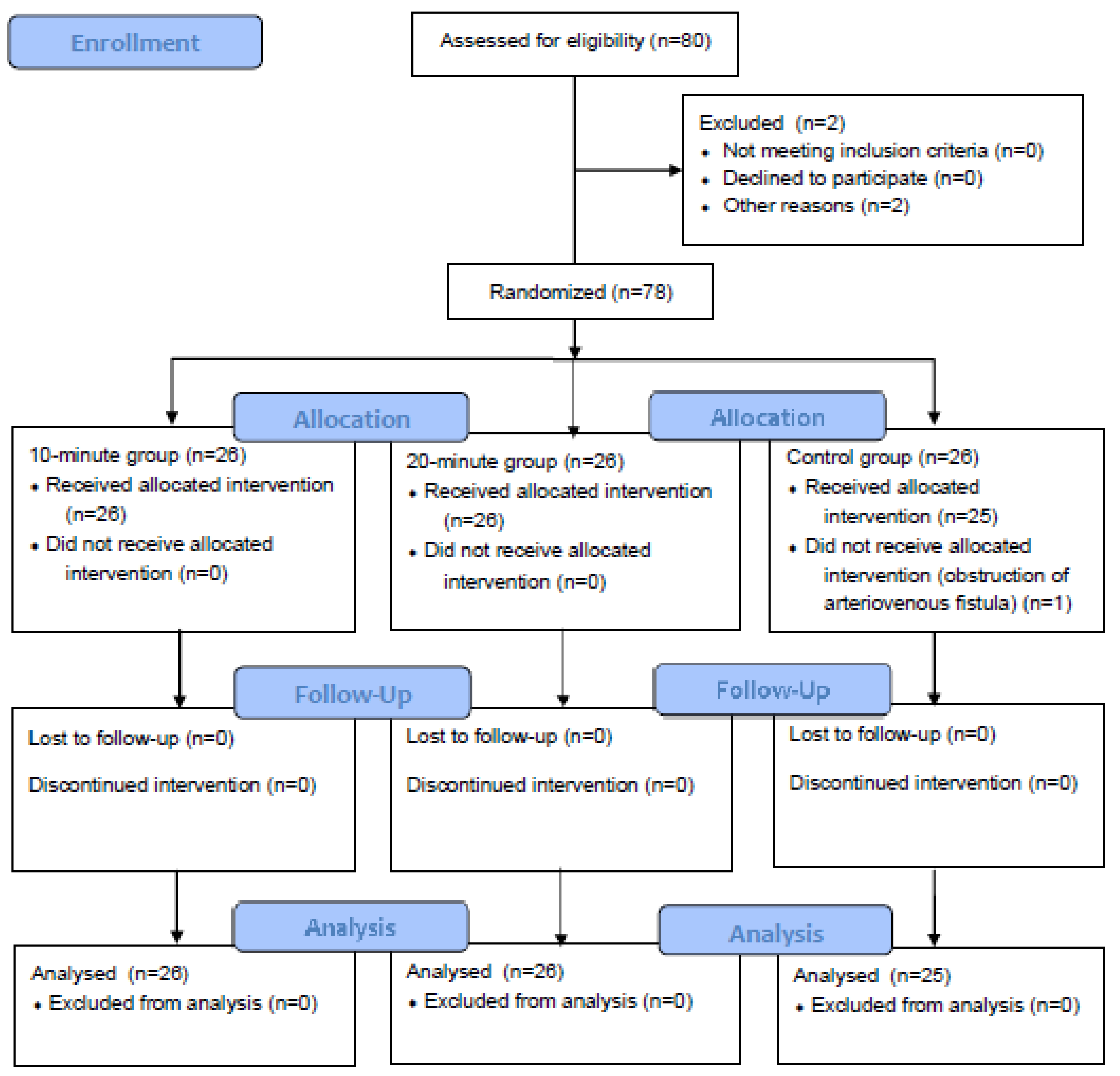
2.2. Participants
2.3. Randomization and Blinding
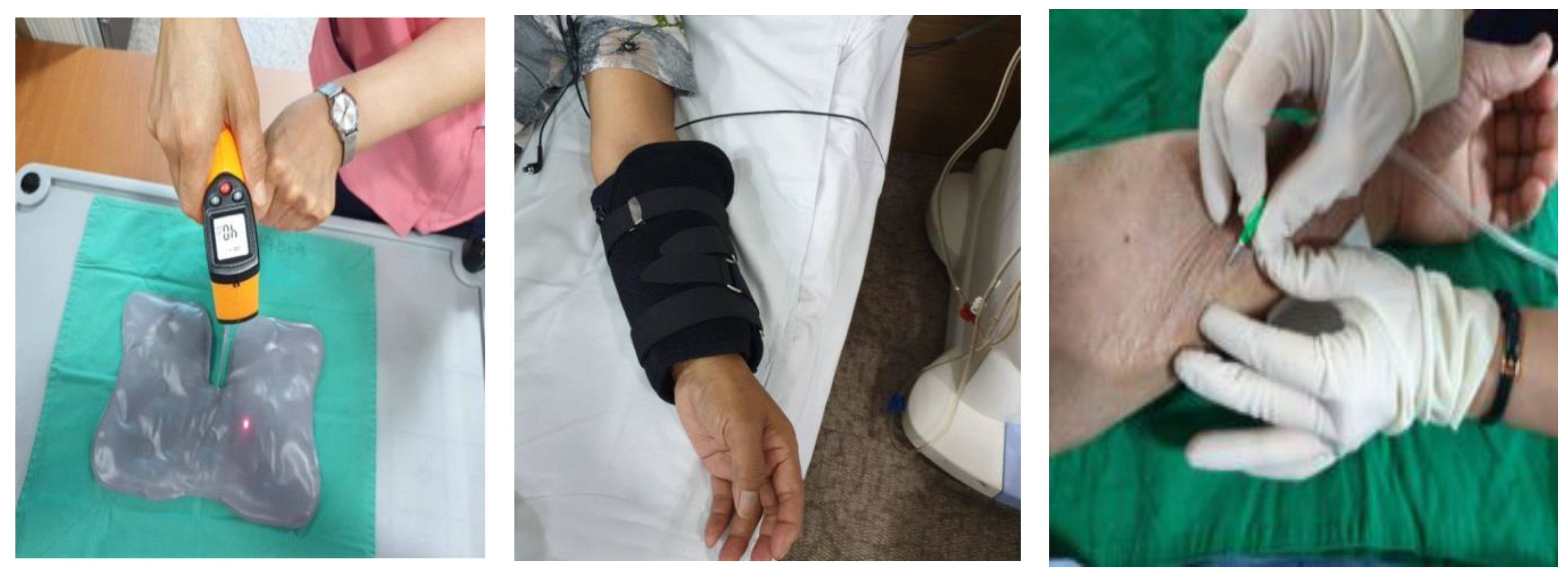
2.4. Intervention
2.5. Outcome
2.6. Ethical Considerations
2.7. Data Analysis
3. Results
3.1. Characteristics of Subjects and Homogeneity
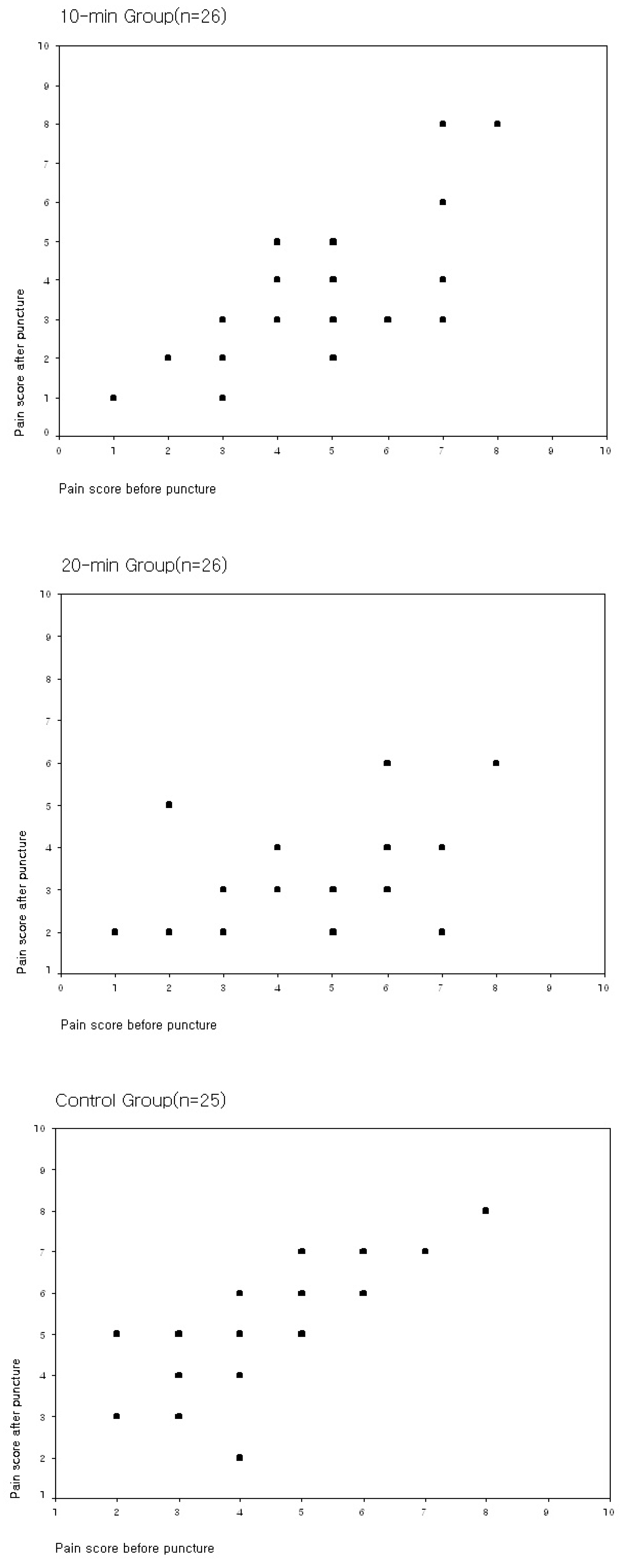
3.2. Difference in Pain Experienced by the Three Groups According to the Application Time of Thermotherapy
3.3. Difference in Anxiety Felt by the Three Groups According to the Application Time of Thermotherapy
3.4. Difference in Adverse Events of the Three Groups According to the Application Time of Thermotherapy
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Figueiredo, A.E.; Viegas, A.; Monteiro, M.; Poli-de-Figueiredo, C.E. Research into pain perception with arteriovenous fistula (avf) cannulation. J. Ren. Care 2008, 34, 169–172. [Google Scholar] [CrossRef] [PubMed]
- Attia, A.A.M.; Hassan, A.M. Effect of cryotherapy on pain management at the puncture site of arteriovenous fistula among children undergoing hemodialysis. Int. J. Nurs. Sci. 2017, 4, 46–51. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.H.; Baek, K.H.; Lee, J.Y.; Lim, H.B.; Kim, H.J.; Kim, Y.S.; Lee, R.G.; Kweon, Y.E. The effect of warm and ice application for pain control caused by arteriovenous fistula needling under hemodialysis. Clin. Nurs. Res. 2006, 12, 179–189. [Google Scholar]
- Arslan, D.E.; Akca, N.K. Pain following needle insertion into a hemodialysis fistula and influencing factors. Int. J. Caring Sci. 2018, 11, 1662–1670. [Google Scholar]
- Lee, Y.H.; Kim, N.C. The comparison of effects of 2% lidocaine intradermal injection and 10% lidocaine spray for pain and anxiety relief on arteriovenous fistula puncture in hemodialysis patients. Clin. Nurs. Res. 2007, 13, 169–177. [Google Scholar]
- Kang, H.Y.; Chae, Y.R. Comparison of skin stimulation method and topical anesthetic cream on pain and heart rate variability during arteriovenous fistula puncture in hemodialysis patients. J. Korean Biol. Nurs. Sci. 2019, 21, 207–216. [Google Scholar] [CrossRef]
- No, I.S.; Kim, S.Y. Assessment of the influence of application time of lidocaine patch on pain intensity after venipuncture. J. Korean Acad. Fundam. Nurs. 2018, 25, 250–258. [Google Scholar] [CrossRef]
- Song, J.M.; Park, H.J. Effects of 10% lidocaine spray and aroma hand massage on pain, anxiety, blood pressure, and pulse during arteriovenous fistula needling in hemodialysis patients. Korean Acad. Soc. Rehabil. Nurs. 2016, 19, 1–11. [Google Scholar]
- Yu, Y.M.; Moon, S.M.; Kim, J.Y.; Bae, H.J.; Ha, H.R. Comparison of the degree of pain according to nursing intervention method during arteriovenous fistula needle insertion for patients on hemodialysis. J. Korean Clin. Nurs. Res. 2011, 17, 286–296. [Google Scholar]
- Kim, K.S. Comparison of Local Anesthetic Ointment to Warm Pack Therapy for Pain Relief during Arteriovenous Fistula Puncture in Hemodialysis Patients. Master’s Thesis, Ajou University, Suwon, Korea, 2011. [Google Scholar]
- Nurcan, C.; Karadag, M. Osteoarthritis Progress in Basic Research and Treatment; InTech: Rijeka, Croatia, 2015; pp. 249–264. [Google Scholar]
- Jung, M.A. The Effect of Warm and Ice Application on the Pain and Stress in Needling under Hemodialysis. Master’s Thesis, Kwandong University, Gangneung, Korea, 2002. [Google Scholar]
- Abramson, D.I.; Chu, L.S.; Tuck, S., Jr.; Lee, S.W.; Richardson, G.; Levin, M. Effect of tissue temperatures and blood flow on motor nerve conduction velocity. J. Am. Med. Assoc. 1966, 198, 1082–1088. [Google Scholar] [CrossRef]
- Wadsworth, H.; Changmugam, A.P.P. Electrophysical Agents in Physiotherapy, 2nd ed.; Science Press: Marrickville, Sydney, 1983; pp. 1–49. [Google Scholar]
- Lehmann, J.F.; DeLaterur, B.J. Therapeutic Heat. In Therapeutic Heat and Cold, 3rd ed.; Williams and Wilkins: Baltmore, MD, USA, 1982. [Google Scholar]
- Aciksoz, S.; Akyuz, A.; Tunay, S. The effect of self-administered superficial local hot and cold application methods on pain, functional status and quality of life in primary knee osteoarthritis patients. J. Clin. Nurs. 2017, 26, 5179–5190. [Google Scholar] [CrossRef] [PubMed]
- Mohamed, H.G.; Mohamed, M.A.F. Effect of Local Heat Application on Complaints of Patients with Moderate Knee Osteoarthritis. Am. J. Nurs. Res. 2019, 7, 148–159. [Google Scholar]
- Kim, S.Y.; Yi, S.H.; Cho, J.H.; Yin, C.S.; Lee, H.; Park, H.J. Heat Stimulation on the Skin for Medical Treatment: Can It Be Controlled? Altern. Complement Med. 2011, 7, 497–504. [Google Scholar] [CrossRef]
- Jun, J.H.; Lee, Y.O.; Lee, S.N. Effect of Abdominal Skin Massage and Warming Therapy on the Pain and Anxiety in Breast Cancer Patients who Underwent Hormone Injections. Asian Oncol. Nurs. 2016, 16, 226–233. [Google Scholar] [CrossRef]
- Brosseau, L.; Yonge, K.A.; Robinson, V.; Marchand, S.; Judd, M.; Wells, G.; Tugwell, P. Thermotherapy for treatment of osteoarthritis. Cochrane Database Syst. Rev. 2003, 2003, CD004522. [Google Scholar] [CrossRef] [PubMed]
- Yun, S.Y.; Cho, B.H. The Effects of Heat Therapy on Low Back Pain, Blood Pressure and Pulse Rate after Percutaneous Coronary Intervention. J. Korean Acad. Fundam. Nurs. 2011, 18, 348–355. [Google Scholar]
- Mirzaei, S.; Javadi, M.; Eftekhari, A.; Hatami, M.; Hemayati, R. Efficacy of application of eutectic mixture of local anesthetics and lidocaine spray in pain management of arteriovenous fistula cannulation in hemodialysis patients. J. Renal. Inj. Prev. 2017, 6, 269–274. [Google Scholar] [CrossRef]
- Jeong, E.S. Effect of Warm Therapy and Topical Anesthetic Cream on the Pain and Anxiety of Patients under Hemodialysis during Arteriovenous Fistula Needling. Master’s Thesis, Eulji University, Daejeon, Korea, 2014. [Google Scholar]
- Choi, H.M.; Choi, E.D.; Jang, S.H.; Kim, E.H.; Choi, M.J.; Back, S.Y.; Han, B.H. The Effect of Far Infrared Heat Therapy on Vascular Access Function of Patients receiving Hemodialysis. J. Korean Clin. Nurs. Res. 2015, 21, 215–222. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: New York, NY, USA, 1988. [Google Scholar]
- Furlan, R.M.M.M.; Raquel Safar Giovanardi, R.S.; de Oliveira e Britto, A.T.B.; de Oliveira e Britto, D.B. The use of superficial heat for treatment of temporomandibular disorders: An integrative review. CoDAS 2015, 27, 207–212. [Google Scholar] [CrossRef]
- Kim, J.S.; Kwon, J.Y.; Ko, Y.J.; Kang, S.Y.; Whang, I.S. Comparison of Skin Temperature between Supine and Prone Position during Application of Hot Packs on the Back. J. Korean Acad. Rehabil. Med. 2003, 27, 778–781. [Google Scholar]
- Sherman, K.J.; Ludman, E.J.; Cook, A.J.; Hawkes, R.J.; Roy-Byrne, P.P.; Bentley, S.; Brooks, M.Z.; Cherkin, D.C. Effectiveness of therapeutic massage for generalized anxiety disorder: A randomized controlled trial. Depress Anxiety 2010, 27, 441–450. [Google Scholar] [CrossRef] [PubMed]
- Kwak, H.; Lee, S.; Kim, S.B. Therapeutic heat and cryotherapy in family medicine. J. Korean Acad. Fam. Med. 2003, 24, 877–883. [Google Scholar]
- Taşan, E.; Ovayolu, O.; Ovayolu, N. The effect of diluted lavender oil inhalation on pain development during vascular access among patients undergoing haemodialysis. Complement. Ther. Clin. Pract. 2019, 35, 177–182. [Google Scholar] [CrossRef]
- Vasilopoulou, C.; Bourtsi, E.; Giaple, S.; Koutelekos, I.; Theofilou, P.; Polikandrioti, M. The impact of anxiety and depression on the quality of life of hemodialysis patients. Glob. J. Health Sci. 2016, 8, 45–55. [Google Scholar] [CrossRef] [PubMed]
- Jang, H.S.; Lee, C.S.; Yang, Y.H. Influence of uncertainty and uncertainty appraisal on self- management in hemodialysis patients. J. Korean Acad. Nurs. 2015, 45, 271–279. [Google Scholar] [CrossRef]
| Variables | 10-min Group (n = 26) | 20-min Group (n = 26) | Control Group (n = 25) | F or χ2 | p | |
|---|---|---|---|---|---|---|
| N(%) or M ± SD | N(%) or M ± SD | N(%) or M ± SD | ||||
| Age (year) | 60.2 ± 10.8 | 63.7 ± 8.9 | 56.7 ± 13.5 | 2.528 | 0.087 | |
| Sex | Male | 15 (57.7) | 14 (53.9) | 17 (68.0) | 1.130 | 0.568 |
| Female | 11 (42.3) | 12 (46.2) | 8 (32.0) | |||
| Diabetes Mlietus | Yes | 12 (46.2) | 16 (61.5) | 8 (32.0) | 4.473 | 0.107 |
| No | 14 (53.8) | 10 (38.5) | 17 (68.0) | |||
| Hypertension | Yes | 5 (19.2) | 7 (26.9) | 8 (32.0) | 1.099 | 0.577 |
| No | 21 (80.8) | 19 (73.1) | 17 (68.0) | |||
| Glomerulo-nephritis | Yes | 1 (3.8) | 2 (7.7) | 4 (16.0) | 2.371 | 0.306 |
| No | 25 (96.2) | 24 (92.3) | 21 (84.0) | |||
| Treatment period of hemodialysis (year) | 38.9 ± 49.6 | 57.6 ± 63.6 | 66.3 ± 63.0 | 1.437 | 0.244 | |
| Cycle of hemodialysis | 3 times per week | 26 (100.0) | 25 (96.1) | 25 (100.0) | 1.987 | 0.370 |
| 2 times per week | 0 (0) | 1 (3.9) | 0 (0) | |||
| Type of arteriovenous fistula | Fistula | 23 (88.5) | 20 (76.9) | 24 (96.0) | 4.177 | 0.124 |
| Graft | 3 (11.5) | 6 (23.1) | 1 (4.0) | |||
| Site of arteriovenous fistula | Upper arm | 15 (57.7) | 11 (42.3) | 11 (44.0) | 1.748 | 0.782 |
| Forearm | 9 (34.6) | 11 (42.3) | 11 (44.0) | |||
| Upper arm and forearm | 2 (7.7) | 4 (15.4) | 3 (12.0) | |||
| Use of lidocaine cream | Yes | 0 (0) | 0 (0) | 0 (0) | ||
| No | 26 (100) | 26 (100) | 25 (100) | |||
| Pain before arteriovenous fistula puncture | 4.4 ± 1.9 | 4.5 ± 1.9 | 4.3 ± 1.7 | 0.038 | 0.963 | |
| Anxiety before arteriovenous fistula puncture | 4.0 ± 1.9 | 3.6 ± 1.9 | 3.2 ± 1.3 | 1.587 | 0.211 |
| Variables | 10-min Group a (n = 26) | 20-min Group b (n = 26) | Control Group c (n = 25) | F | p |
|---|---|---|---|---|---|
| Mean ± SD | Mean ± SD | Mean ± SD | |||
| Pain | 3.4 ± 1.8 | 3.2 ± 1.1 | 5.1 ± 1.6 | 11.457 | <0.001 |
| Anxiety | 3.3 ± 1.8 | 3.0 ± 1.6 | 3.2 ± 1.4 | 0.255 | 0.775 |
| Side Effects | 10-min Group (n = 26) n (%) | 20-min Group (n = 26) n (%) | Control Group (n = 25) n (%) | |
|---|---|---|---|---|
| Redness | Yes | 0 (0) | 0 (0) | 0 (0) |
| No | 26 (100) | 26 (100) | 25 (100) | |
| Itching | Yes | 0 (0) | 4 (15) | 0 (0) |
| No | 26 (100) | 22 (85) | 25 (100) | |
| Edema | Yes | 0 (0) | 0 (0) | 0 (0) |
| No | 26 (100) | 26 (100) | 25 (100) | |
| Bullous | Yes | 0 (0) | 0 (0) | 0 (0) |
| No | 26 (100) | 26 (100) | 25 (100) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Back, Y.; Lee, Y. Optimal Time of Thermotherapy for Reducing Pain, Anxiety, and Side Effects in Arteriovenous Fistula Puncture Patients: A Randomized Controlled Trial. Int. J. Environ. Res. Public Health 2020, 17, 7147. https://doi.org/10.3390/ijerph17197147
Back Y, Lee Y. Optimal Time of Thermotherapy for Reducing Pain, Anxiety, and Side Effects in Arteriovenous Fistula Puncture Patients: A Randomized Controlled Trial. International Journal of Environmental Research and Public Health. 2020; 17(19):7147. https://doi.org/10.3390/ijerph17197147
Chicago/Turabian StyleBack, Yangok, and Yoonyoung Lee. 2020. "Optimal Time of Thermotherapy for Reducing Pain, Anxiety, and Side Effects in Arteriovenous Fistula Puncture Patients: A Randomized Controlled Trial" International Journal of Environmental Research and Public Health 17, no. 19: 7147. https://doi.org/10.3390/ijerph17197147
APA StyleBack, Y., & Lee, Y. (2020). Optimal Time of Thermotherapy for Reducing Pain, Anxiety, and Side Effects in Arteriovenous Fistula Puncture Patients: A Randomized Controlled Trial. International Journal of Environmental Research and Public Health, 17(19), 7147. https://doi.org/10.3390/ijerph17197147





