Exploring Volatile Organic Compound Exposure and Its Association with Wheezing in Children under 36 Months: A Cross-Sectional Study in South Lisbon, Portugal
Abstract
1. Introduction
2. Materials and Methods
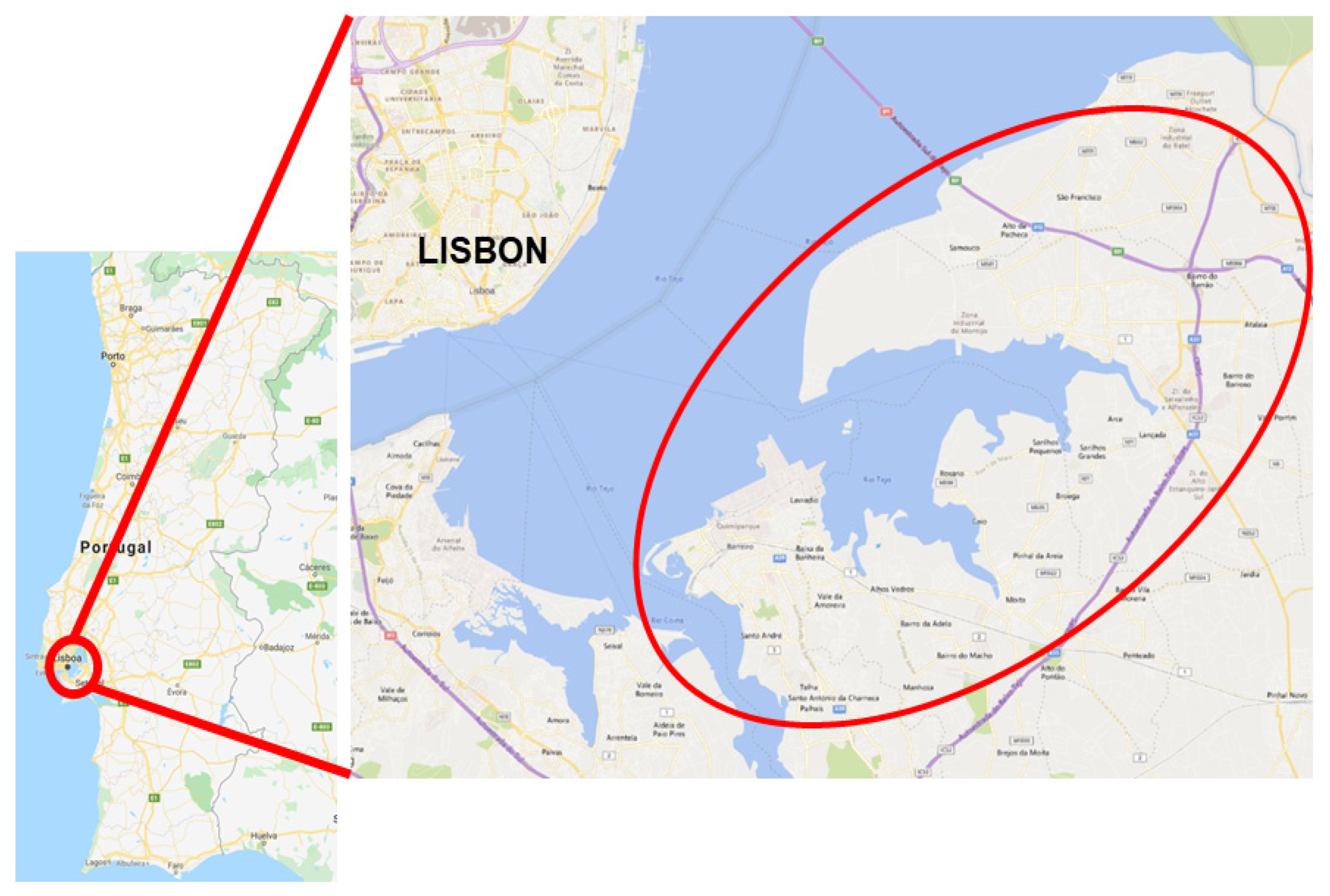
2.1. Study Setting
2.2. Sampling Strategy
2.3. Data Collection
2.4. Variables of Interest
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Nugent, R.; Bertram, M.Y.; Jan, S.; Niessen, L.W.; Sassi, F.; Jamison, D.T.; Pier, E.G.; Beaglehole, R. Investing in non-communicable disease prevention and management to advance the Sustainable Development Goals. Lancet 2018, 391, 2029–2035. [Google Scholar] [CrossRef]
- Nurmatov, U.B.; Tagiyeva, N.; Semple, S.; Devereux, G.; Sheikh, A. Volatile organic compounds and risk of asthma and allergy: A systematic review. Eur. Respir. Rev. 2015, 24, 92–101. [Google Scholar] [CrossRef] [PubMed]
- To, T.; Stanojevic, S.; Moores, G.; Gershon, A.S.; Bateman, E.D.; Cruz, A.A.; Boulet, L.-P. Global asthma prevalence in adults: Findings from the cross-sectional world health survey. BMC Public Health 2012, 12, 204. [Google Scholar] [CrossRef] [PubMed]
- Simpson, C.R.; Sheikh, A. Trends in the epidemiology of asthma in England: A national study of 333,294 patients. J. R. Soc. Med. 2010, 103, 98–106. [Google Scholar] [CrossRef] [PubMed]
- Le Blanc, D. Towards Integration at Last? The Sustainable Development Goals as a Network of Targets. Sustain. Dev. 2015, 23, 176–187. [Google Scholar] [CrossRef]
- To, T.; Wang, C.; Guan, J.; McLimont, S.; Gershon, A.S. What Is the Lifetime Risk of Physician-Diagnosed Asthma in Ontario, Canada? Am. J. Respir. Crit. Care Med. 2010, 181, 337–343. [Google Scholar] [CrossRef]
- Pickett, A.R.; Bell, M.L. Assessment of indoor air pollution in homes with infants. Int. J. Environ. Res. Public Health 2011, 8, 4502–4520. [Google Scholar] [CrossRef] [PubMed]
- Asher, M.I.; Montefort, S.; Björkstén, B.; Lai, C.K.; Strachan, D.P.; Weiland, S.K.; Williams, H. Worldwide time trends in the prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and eczema in childhood: ISAAC Phases One and Three repeat multicountry cross-sectional surveys. Lancet 2006, 368, 733–743. [Google Scholar] [CrossRef]
- Arif, A.A.; Shah, S.M. Association between personal exposure to volatile organic compounds and asthma among US adult population. Int. Arch. Occup. Environ. Health 2007, 80, 711–719. [Google Scholar] [CrossRef]
- Janson, C.; Anto, J.; Burney, P.; Chinn, S.; de Marco, R.; Heinrich, J.; Jarvis, D.; Kuenzli, N.; Leynaert, B.; Luczynska, C.; et al. The European Community Respiratory Health Survey: What are the main results so far? Eur. Respir. J. 2001, 18, 598–611. [Google Scholar] [CrossRef]
- Strachan, D.P. Hay fever, hygiene, and household size. BMJ 1989, 299, 1259–1260. [Google Scholar] [CrossRef] [PubMed]
- Ober, C.; Sperling, A.I.; von Mutius, E.; Vercelli, D. Immune development and environment: Lessons from Amish and Hutterite children. Curr. Opin. Immunol. 2017, 48, 51–60. [Google Scholar] [CrossRef] [PubMed]
- Sa-Sousa, A.; Morais-Almeida, M.; Azevedo, L.; Carvalho, R.; Jacinto, T.; Todo-Bom, A.; Loureiro, C.; Bugalho-Almeida, A.; Bousquet, J.; Fonseca, J. Prevalence of asthma in Portugal—The Portuguese National Asthma Survey. Clin. Transl. Allergy 2012, 2, 15. [Google Scholar] [CrossRef] [PubMed]
- De Sousa, J.C.; Santo, M.E.; Colaço, T.; Almada-Lobo, F.; Yaphe, J. Asthma in an urban population in Portugal: A prevalence study. BMC Public Health 2011, 11, 347. [Google Scholar] [CrossRef]
- Ferreira de Magalhães, M.; Amaral, R.; Pereira, A.M.; Sá-Sousa, A.; Azevedo, I.; Azevedo, L.F.; Fonseca, J.A. Cost of asthma in children: A nationwide, population-based, cost-of-illness study. Pediatr. Allergy Immunol. 2017, 28, 683–691. [Google Scholar] [CrossRef]
- Oz, K.; Merav, B.; Sara, S.; Yael, D. Volatile Organic Compound Emissions from Polyurethane Mattresses under Variable Environmental Conditions. Environ. Sci. Technol. 2019, 53, 9171–9180. [Google Scholar] [CrossRef]
- Fuentes-Leonarte, V.; Tenías, J.M.; Ballester, F. Levels of pollutants in indoor air and respiratory health in preschool children: A systematic review. Pediatr. Pulmonol. 2009, 44, 231–243. [Google Scholar] [CrossRef]
- Matz, C.; Stieb, D.; Davis, K.; Egyed, M.; Rose, A.; Chou, B.; Brion, O. Effects of Age, Season, Gender and Urban-Rural Status on Time-Activity: Canadian Human Activity Pattern Survey 2 (CHAPS 2). Int. J. Environ. Res. Public Health 2014, 11, 2108–2124. [Google Scholar] [CrossRef]
- Madureira, J.; Paciência, I.; Cavaleiro-Rufo, J.; Fernandes, E.D.O. Indoor air risk factors for schoolchildren’s health in Portuguese homes: Results from a case-control survey. J. Toxicol. Environ. Health Part A 2016, 79, 938–953. [Google Scholar] [CrossRef]
- Oliveira, M.; Slezakova, K.; Delerue-Matos, C.; Pereira, M.D.C.; Morais, S. Indoor air quality in preschools (3- to 5-year-old children) in the Northeast of Portugal during spring–summer season: Pollutants and comfort parameters. J. Toxicol. Environ. Health Part A 2017, 80, 740–755. [Google Scholar] [CrossRef]
- ISO. Ergonomics of the Thermal Environment—Analytical Determination and Interpretation of Thermal Comfort Using Calculation of the PMV and PPD Indices and Local Thermal Comfort Criteria; ISO 7730:2005; International Organization for Standardization: Geneva, Switzerland, 2005; p. 52. [Google Scholar]
- World Health Organization. WHO Guidelines for Indoor Air Quality: Selected Pollutants; World Health Organization, Regional Office for Europe: Geneva, Switzerland, 2010. [Google Scholar]
- Agência Portuguesa do Ambiente. Qualidade do Ar em Espaços Interiores; Agência Portuguesa do Ambiente: Lisbon, Portugal, 2009. [Google Scholar]
- Agência Portuguesa do Ambiente. Manual da Qualidade do Ar em Espaços Interiores—Um Guia Técnico; Agência Portuguesa do Ambiente: Lisbon, Portugal, 2010. [Google Scholar]
- Dos Santos, R.R.; Fernandes, A.S.; Castanheira, L. Development of a strategy to identify the characteristics of babie’s rooms associated with volatile organic compounds and with the occurrence of wheezing. J. Biomed. Biopharm. Res. 2017, 14, 16–22. [Google Scholar]
- Biscaia, A.R.; Heleno, L.C.V. Primary Health Care Reform in Portugal: Portuguese, modern and innovative. Cien Saude Colet 2017, 22, 701–712. [Google Scholar] [CrossRef] [PubMed]
- Asher, M.I. Worldwide variations in the prevalence of asthma symptoms: The International Study of Asthma and Allergies in Childhood (ISAAC). Eur. Respir. J. 1998, 12, 315–335. [Google Scholar]
- Da Silva, E.N.; Ribeiro, H. Ambiente atmosférico urbano e admissão hospitalar de crianças, na cidade de São Paulo, Brasil. Rev. Salud Ambient. 2013, 13, 30–36. [Google Scholar]
- Paciência, I.; Madureira, J.; Rufo, J.; Moreira, A.; Fernandes, E.D.O. A systematic review of evidence and implications of spatial and seasonal variations of volatile organic compounds (VOC) in indoor human environments. J. Toxicol. Environ. Health Part B 2016, 19, 47–64. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, R.R.; Gregório, J.; Castanheira, L.; Fernandes, A. The association of housing conditions with wheezing in children up to 36 month-old: An observational study in Arco Ribeirinho region. J. Biomed. Biopharm. Res. 2019, 16, 55–61. [Google Scholar]
- Neto, H.J.C.; Rosário, N.A.; Solé, D.; Mallol, J. Prevalence of recurrent wheezing in infants. J. Pediatr. 2007, 83, 357–362. [Google Scholar] [CrossRef][Green Version]
- Martins, P.C.; Valente, J.; Papoila, A.L.; Caires, I.; Araujo-Martins, J.; Mata, P.; Lopes, M.; Torres, S.; Rosado-Pinto, J.; Borrego, C.; et al. Airways changes related to air pollution exposure in wheezing children. Eur. Respir. J. 2012, 39, 246–253. [Google Scholar] [CrossRef]
- Cheraghi, M.; Salvi, S. Environmental tobacco smoke (ETS) and respiratory health in children. Eur. J. Pediatr. 2009, 168, 897–905. [Google Scholar] [CrossRef]
- Vanker, A.; Gie, R.P.; Zar, H.J. The association between environmental tobacco smoke exposure and childhood respiratory disease: A review. Expert Rev. Respir. Med. 2017, 11, 661–673. [Google Scholar] [CrossRef]
- Lu, C.; Norbäck, D.; Li, Y.; Deng, Q. Early-life exposure to air pollution and childhood allergic diseases: An update on the link and its implications. Expert Rev. Clin. Immunol. 2020, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Batterman, S.; Su, F.-C.; Li, S.; Mukherjee, B.; Jia, C.; HEI Health Review Committee. Personal exposure to mixtures of volatile organic compounds: Modeling and further analysis of the RIOPA data. Res. Rep. Health Eff. Inst. 2014, 181, 3–63. [Google Scholar]
- Montero-Montoya, R.; López-Vargas, R.; Arellano-Aguilar, O. Volatile Organic Compounds in Air: Sources, Distribution, Exposure and Associated Illnesses in Children. Ann. Glob. Health 2018, 84, 225–238. [Google Scholar] [CrossRef] [PubMed]
- Serrano-Trespalacios, P.I.; Ryan, L.; Spengler, J.D. Ambient, indoor and personal exposure relationships of volatile organic compounds in Mexico City Metropolitan Area. J. Expo. Sci. Environ. Epidemiol. 2004, 14, S118–S132. [Google Scholar] [CrossRef]
- Emenius, G.; Svartengren, M.; Korsgaard, J.; Nordvall, L.; Pershagen, G.; Wickman, M. Building characteristics, indoor air quality and recurrent wheezing in very young children (BAMSE). Indoor Air 2004, 14, 34–42. [Google Scholar] [CrossRef]
- Franklin, P.J. Indoor air quality and respiratory health of children. Paediatr. Respir. Rev. 2007, 8, 281–286. [Google Scholar] [CrossRef]
- DGS. Portugal Doenças Respiratórias em Números—2014; DGS: Lisboa, Portugal, 2015. [Google Scholar]
- Van Strien, R.T.; Gehring, U.; Belanger, K.; Triche, E.; Gent, J.; Bracken, M.B.; Leaderer, B.P. The influence of air conditioning, humidity, temperature and other household characteristics on mite allergen concentrations in the northeastern United States. Allergy 2004, 59, 645–652. [Google Scholar] [CrossRef]
- Neves, D.L. A CUF e o Barreiro: Responsabilidade social, empresarial e sustentabilidade. In Actas Do Colóquio Internacional Industrialização Em Portugal No Século XX: O Caso Do Barreiro; Faria, M.F., Mendes, J.A., Eds.; Ediual: Lisboa, Portugal, 2010. [Google Scholar]
- Gabriel, M.F.; Felgueiras, F.; Fernandes, M.; Ribeiro, C.; Ramos, E.; Mourão, Z.; de Oliveira Fernandes, E. Assessment of indoor air conditions in households of Portuguese families with newborn children. Implementation of the HEALS IAQ checklist. Environ. Res. 2020, 182, 108966. [Google Scholar] [CrossRef]
| Boys | Girls | p-Value | ||
|---|---|---|---|---|
| Mean age in months (SD) | 11.0 (8.8) | 12.3 (10.6) | 0.776 | |
| Wheezing | Never | 49 (72.1%) | 37 (58.7%) | 0.108 |
| From birth | 19 (27.9%) | 26 (41.3%) | ||
| Wheezing in the past 12 months | 16 (23.5%) | 23 (36.5%) | 0.267 | |
| Total | Boys | Girls | |||||
|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | p-Value | |
| Location | |||||||
| Rural | 14 | 10.7 | 4 | 5.9 | 10 | 15.9 | 0.064 |
| Urban | 117 | 89.3 | 64 | 94.1 | 53 | 84.1 | |
| Smokers in house | |||||||
| Yes | 40 | 30.5 | 20 | 29.4 | 20 | 31.7 | 0.772 |
| No | 91 | 69.5 | 48 | 70.6 | 43 | 68.3 | |
| Children’s bedrooms characteristics | |||||||
| Floor location | |||||||
| Ground Floor | 29 | 22.1 | 12 | 17.6 | 17 | 27.0 | 0.298 |
| 1st floor | 38 | 29.0 | 23 | 33.8 | 15 | 23.8 | |
| 2nd floor or more | 64 | 48.9 | 33 | 48.5 | 31 | 49.2 | |
| Visible mold | |||||||
| Yes | 39 | 29.8 | 18 | 26.5 | 21 | 33.3 | 0.391 |
| No | 92 | 70.2 | 50 | 73.5 | 42 | 66.7 | |
| Proximity to pollution site | |||||||
| Yes | 32 | 24.4 | 14 | 20.6 | 18 | 28.6 | 0.288 |
| No | 99 | 75.6 | 54 | 79.4 | 45 | 71.4 | |
| Decoration | |||||||
| Paint | 119 | 90.8 | 62 | 91.2 | 57 | 90.5 | 0.898 |
| Paint and paper | 10 | 7.6 | 5 | 7.4 | 5 | 7.9 | |
| Other | 2 | 1.5 | 1 | 1.5 | 1 | 1.6 | |
| Area m2 (SD) | 13.4 (2.8) | 13.0 (2.9) | 13.9 (2.8) | 0.088 | |||
| Room density m2/person (SD) | 5.9 (2.9) | 5.8 (3.1) | 6.15 (2.8) | 0.683 | |||
| Used in the past 48 h | |||||||
| Bedroom used for hygiene | |||||||
| Yes | 74 | 56.5 | 39 | 57.4 | 35 | 55.6 | 0.836 |
| No | 57 | 43.5 | 29 | 42.6 | 28 | 44.4 | |
| Air conditioned | |||||||
| Yes | 15 | 11.5 | 8 | 11.8 | 7 | 11.1 | 0.907 |
| No | 116 | 88.5 | 60 | 88.2 | 56 | 88.9 | |
| Oil radiator | |||||||
| Yes | 19 | 14.5 | 10 | 14.7 | 9 | 14.3 | 0.946 |
| No | 112 | 85.5 | 58 | 85.3 | 54 | 85.7 | |
| Floor cleaning products | |||||||
| Yes | 28 | 21.4 | 11 | 16.2 | 17 | 27.0 | 0.132 |
| No | 103 | 78.6 | 57 | 83.8 | 46 | 73.0 | |
| Furniture cleaning products | |||||||
| Yes | 8 | 6.1 | 4 | 5.9 | 4 | 6.3 | 0.911 |
| No | 123 | 93.9 | 64 | 94.1 | 59 | 93.7 | |
| Recently washed clothes | |||||||
| Yes | 41 | 31.3 | 24 | 35.3 | 17 | 27.0 | 0.305 |
| No | 90 | 68.7 | 44 | 64.7 | 46 | 73.0 | |
| Air cleaner/dehumidifier | |||||||
| Yes | 13 | 9.9 | 6 | 8.8 | 7 | 11.1 | 0.662 |
| No | 118 | 90.1 | 62 | 91.2 | 56 | 88.9 | |
| Use of anti-insect/anti-moth products | |||||||
| Yes | 6 | 4.6 | 1 | 1.5 | 5 | 7.9 | 0.077 |
| No | 125 | 95.4 | 67 | 98.5 | 58 | 92.1 | |
| Window opening frequency | |||||||
| No more than once a month | 4 | 3.1 | 1 | 1.5 | 3 | 4.8 | 0.155 |
| No more than once a week | 4 | 3.1 | 1 | 1.5 | 3 | 4.8 | |
| 2 or more per week | 33 | 25.2 | 19 | 27.9 | 14 | 22.2 | |
| Once a day | 69 | 52.7 | 40 | 58.8 | 29 | 46.0 | |
| 2 or more per day | 21 | 16.0 | 7 | 10.3 | 14 | 22.2 | |
| Temperature, °C | Relative Humidity, % | CO2, ppm | TVOC, mg/m3 | CO, mg/m3 | ||
|---|---|---|---|---|---|---|
| Reference Values: [21,22,23,24] | 20–24 | 30–70 | <1800 | <0.3 | <5.8 | |
| % rooms outside references | 77.9 | 88.5 | 19.8 | 48.1 | 0 | |
| Indoor | Mean (SD) | 18.4 (2.1) | 75.9 (6.8) | 1260.8 (1046.7) | 3.1 (4.9) | 0.2 (0.6) |
| Median | 18.3 | 75.5 | 951.0 | 0.2 | 0.0 | |
| Range (min–max) | 13.9–25.4 | 56.8–95.9 | 1.0–5545.0 | 0–23.1 | 0.0–3.5 | |
| P25–P75 | 16.9–19.8 | 71.8–80.8 | 597.0–1595.0 | 0.0–5.0 | 0.0–0.0 | |
| Outdoor | Mean (SD) | 18.5 (3.5) | 70.1 (10.9) | 614.9 (672.3) | 2.0 (3.7) | 0.1 (0.4) |
| Median | 18.1 | 70.2 | 449.0 | 0.0 | 0.0 | |
| Range (min–max) | 12.9–31.0 | 27.0–90.9 | 0–3229 | 0.0–13.3 | 0.0–2.3 | |
| P25–P75 | 16.3–20.0 | 65.4–77.5 | 276.0–542.0 | 0.0–1.4 | 0.0–0.0 | |
| I/O Ratio | Mean (SD) | 1.0 (0.2) | 1.1 (0.2) | 5.3 (12.9) § | 1.9 (2.8) ⸸ | 1.0 (0.2) ¥ |
| Median | 1.0 | 1.1 | 2.2 § | 1.0 ⸸ | 1.0 ¥ | |
| Range (min–max) | 0.5–1.4 | 0.8–2.7 | 0.2–127.5 § | 0.0–19.2 ⸸ | 0.0–2.0 ¥ | |
| P25–P75 | 0.9–1.1 | 1.0–1.1 | 1.5 §–3.3 § | 1.0 ⸸–1.3 ⸸ | 1.0 ¥–1.0 ¥ | |
| Episodes of Wheezing | Exposure to TVOC ≤ 0.3 mg/m3 n (%) | Exposure to TVOC > 0.3 mg/m3 n (%) | |
|---|---|---|---|
| Boys | Never | 25 (67.6%) | 24 (77.4%) |
| Between 1 and 3 episodes | 5 (13.5%) | 2 (6.5%) | |
| More than 3 episodes | 7 (18.9%) | 5 (16.1%) | |
| Girls | Never | 20 (64.5%) | 17 (53.1%) |
| Between 1 and 3 episodes | 5 (16.1%) | 8 (25.0%) | |
| More than 3 episodes | 6 (19.4%) | 7 (21.9%) |
| Presence of Indoor Smokers | TVOC above 0.3 mg/m3 | ||||
|---|---|---|---|---|---|
| OR | aOR | OR | aOR | ⸸ aOR | |
| Never | 1 | 1 | 1 | 1 | 1 |
| Between 1 and 3 episodes | 3.66 | 4.202 | 1.098 | 1.264 | 0.770 |
| [1.335–10.000] | [1.122–15.625] | [0.415–2.907] | [0.349–4.587] | [0.196–3.021] | |
| (p = 0.012) | (p = 0.033) | (p = 0.851) | (p = 0.721) | (p = 0.708) | |
| More than 3 episodes | n.a | n.a | 1.013 [0.415–2.469] (p = 0.977) | 0.927 [0.337–2.545] (p = 0.883) | 1.014 [0.355–2.899] (p = 0.979) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodrigues dos Santos, R.; Gregório, J.; Castanheira, L.; Fernandes, A.S. Exploring Volatile Organic Compound Exposure and Its Association with Wheezing in Children under 36 Months: A Cross-Sectional Study in South Lisbon, Portugal. Int. J. Environ. Res. Public Health 2020, 17, 6929. https://doi.org/10.3390/ijerph17186929
Rodrigues dos Santos R, Gregório J, Castanheira L, Fernandes AS. Exploring Volatile Organic Compound Exposure and Its Association with Wheezing in Children under 36 Months: A Cross-Sectional Study in South Lisbon, Portugal. International Journal of Environmental Research and Public Health. 2020; 17(18):6929. https://doi.org/10.3390/ijerph17186929
Chicago/Turabian StyleRodrigues dos Santos, Raquel, João Gregório, Liliana Castanheira, and Ana S. Fernandes. 2020. "Exploring Volatile Organic Compound Exposure and Its Association with Wheezing in Children under 36 Months: A Cross-Sectional Study in South Lisbon, Portugal" International Journal of Environmental Research and Public Health 17, no. 18: 6929. https://doi.org/10.3390/ijerph17186929
APA StyleRodrigues dos Santos, R., Gregório, J., Castanheira, L., & Fernandes, A. S. (2020). Exploring Volatile Organic Compound Exposure and Its Association with Wheezing in Children under 36 Months: A Cross-Sectional Study in South Lisbon, Portugal. International Journal of Environmental Research and Public Health, 17(18), 6929. https://doi.org/10.3390/ijerph17186929







