Lung Health in Children in Sub-Saharan Africa: Addressing the Need for Cleaner Air
Abstract
1. Introduction
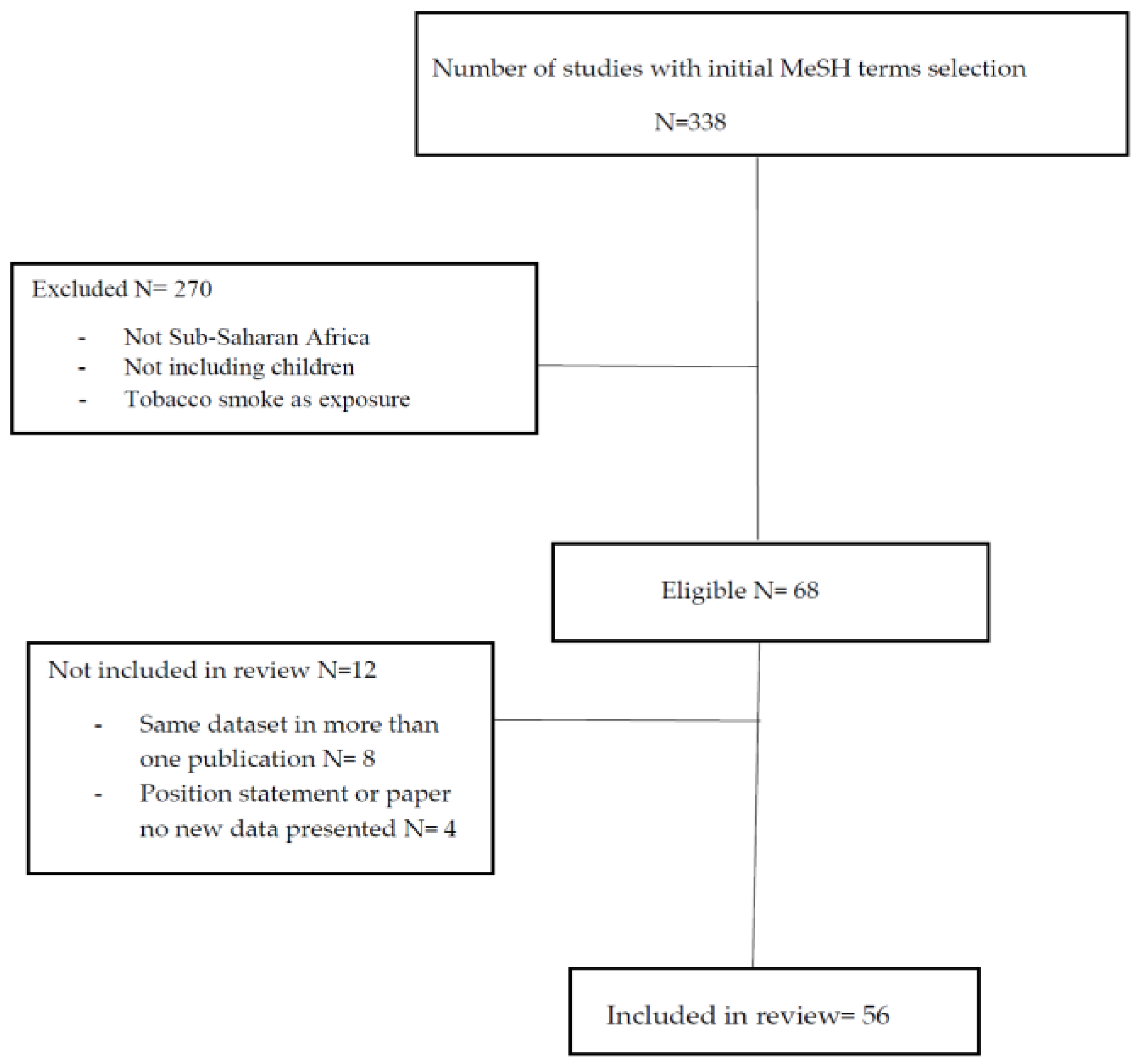
2. Methodology
3. Epidemiology
4. Pathophysiology
5. Exposure Assessments
6. Lung Health Impacts
6.1. Acute
6.2. Long-Term Lung Health Effects and Asthma
7. Impact of Interventions to Reduce Air Pollution
8. Discussion
9. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Landrigan, P.J.; Fuller, R.; Acosta, N.J.R.; Adeyi, O.; Arnold, R.; Basu, N.N.; Blade’, A.D.; Bertollilni, R.; Bose- O’ Reilly, S.; Boufford, J.I.; et al. The lancet commission on pollution and health. Lancet 2018, 391, 462–512. [Google Scholar] [CrossRef]
- Kim, D.; Chen, Z.; Zhou, L.F.; Huang, S.X. Air pollutants and early origins of respiratory diseases. ChronicDis. Trans. Med. 2018, 4, 75–94. [Google Scholar] [CrossRef] [PubMed]
- Sly, P.D.; Bush, A. From the cradle to the grave: The early-life origins of chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 2015, 193, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Schraufnagel, D.E.; Balmes, J.R.; De Matteis, S.; Hoffman, B.; Kim, W.J.; Perez-Padilla, R.; Rice, M.; Sood, A.; Vanker, A.; Wuebbles, D.J. Health benefits of air pollution reduction. Ann. Am. Thor. Soc. 2019, 16, 1478–1487. [Google Scholar] [CrossRef] [PubMed]
- Vardoulakis, S.; Kettle, R.; Cosford, P.; Lincoln, P.; Holgate, S.; Grigg, J.; Kelly, F.; Pencheon, D. Local action on outdoor air pollution to improve public health. Int. J. Public Health 2018, 63, 557–565. [Google Scholar] [CrossRef] [PubMed]
- Ackermann-Liebrich, U.; Leuenberger, P.; Schwartz, J.; Schindler, C.; Monn, C.; Bolognini, G.; Elsasser, S.; Grize, L.; Karrer, W.; Keller, R. Lung function and long term exposure to air pollutants in Switzerland. Study on Air Pollution and Lung Diseases in Adults (SAPALDIA) team. Am. J. Respir. Crit. Care Med. 1997, 155, 122–129. [Google Scholar] [CrossRef]
- Nordgren, T.M.; Bailey, K.L. Pulmonary health effects of agriculture. Curr. Opin. Pulm. Med. 2016, 22, 144. [Google Scholar] [CrossRef]
- Grigg, J. Traffic-derived air pollution and lung function growth. Am. J. Respir. Crit. Care Med. 2012, 186, 1208–1209. [Google Scholar] [CrossRef]
- Cooper, C.W.; Mira, M.; Danforth, M.; Abraham, K.; Fasher, B.; Bolton, P. Acute exacerbations of asthma and bushfires. Lancet 1994, 343, 1509. [Google Scholar] [CrossRef]
- Goudie, A.S. Desert dust and human health disorders. Environ. Int. 2014, 63, 1–13. [Google Scholar] [CrossRef]
- Schraufnagel, D.E.; Balmes, J.R.; Cowl, C.T.; De Matteis, S.; Jung, S.H.; Mortimer, K.; Perez-Padilla, R.; Rice, M.B.; Riojas-Rodriguez, H.; Sood, A. Air pollution and noncommunicable diseases: A review by the forum of international respiratory societies’ environmental committee, part 1, the damaging effects of air pollution. Chest 2019, 155, 409–416. [Google Scholar] [CrossRef] [PubMed]
- Forbes, L.; Jarvis, D.; Potts, J.; Baxter, P.J. Volcanic ash and respiratory symptoms in children on the island of Montserrat, British West Indies. Occup. Environ. Med. 2003, 60, 207–211. [Google Scholar] [CrossRef]
- Johnson, K.G.; Loftsgaarden, D.O.; Gideon, R.A. The effects of Mount St. Helens volcanic ash on the pulmonary function of 120 elementary school children. Am. Rev. Respir. Dis. 1982, 126, 1066–1069. [Google Scholar] [PubMed]
- Gordon, S.B.; Bruce, N.G.; Grigg, J.; Hibberd, P.L.; Kurmi, O.P.; Lam, K.B.; Mortimer, K.; Asante, K.P.; Balakrishnan, K.; Balmes, J. Respiratory risks from household air pollution in low and middle income countries. Lancet Respir. Med. 2014, 2, 823–860. [Google Scholar] [CrossRef]
- Naeher, L.; Leaderer, B.; Smith, K.R. Particulate matter and carbon monoxide in highland Guatemala: Indoor and outdoor levels from traditional and improved wood stoves and gas stoves. Indoor Air 2000, 10, 200–205. [Google Scholar] [CrossRef] [PubMed]
- Naeher, L.P.; Brauer, M.; Lipsett, M.; Zelikoff, J.T.; Simpson, C.D.; Koenig, J.Q.; Smith, K.R. Woodsmoke health effects: A review. Inhal. Toxicol 2007, 19, 67–106. [Google Scholar] [CrossRef]
- Olaniyan, T.; Dalvie, M.A.; Roosli, M.; Naidoo, R.; Kunzli, N.; de Hoogh, K.; Parker, B.; Leaner, J.; Jeebhay, M. Asthma-related outcomes associated with indoor air pollutants among schoolchildren from four informal settlements in two municipalities in the Western Cape Province of South Africa. Indoor Air 2019, 29, 89–100. [Google Scholar] [CrossRef]
- World Health Organisation. Air Pollution and Child Health: Prescribing Clean Air. Summary; Contract No.: (WHO/CED/PHE/18.01); World Health Organisation: Geneva, Switzerland, 2018. [Google Scholar]
- World Health Organisation. Burden of Disease from Household and Ambient Air Pollution for 2012 Summary of Results; World Health Organisation: Geneva, Switzerland, 2014; Available online: http://www.who.int/phe/health_topics/outdoorair/databases/FINAL_HAP_AAP_BoD_24March2014.pdf (accessed on 1 May 2020).
- World Health Organization. WHO Guidelines for Indoor Air Quality: Selected Pollutants; Report No.: Null; Regional Office for Europe: Bonn, Germany, 2010. [Google Scholar]
- Myllyvirta, L. Air Quality and Health Impacts of Doubling the South African Standards for SO2 Emissions from Power Plants. Greepeace International. 2019. Available online: https://cer.org.za/wp-content/uploads/2019/07/Annexure-3_Lauri-Myllyvirta_Report_July-2019.pdf (accessed on 27 April 2020).
- Atani, M. Air Pollution: Africa’s Invisible, Silent Killer. 2019. Available online: https://www.unenvironment.org/news-and-stories/story/air-pollution-africas-invisible-silent-killer-1 (accessed on 1 May 2020).
- McAllister, D.A.; Liu, L.; Shi, T.; Chu, Y.; Reed, C.; Burrows, J.; Adeloye, D.; Rudan, I.; Black, R.E.; Campbell, H. Global, regional, and national estimtes of pneumonia morbidity and mortality in children younger than 5 years between 2000 and 2015, a systematic analysis. Lancet Glob. Health. 2019, 7, e47–e57. [Google Scholar] [CrossRef]
- Adeloye, D.; Chan, K.Y.; Rudan, I.; Campbell, H. An estimate of asthma prevalence in Africa: A systematic analysis. Croat. Med. J. 2013, 54, 519–531. [Google Scholar] [CrossRef]
- Goldizen, F.C.; Sly, P.D.; Knibbs, L.D. Respiratory effects of air pollution on children. Pediatr. Pulmonol. 2016, 51, 94–108. [Google Scholar] [CrossRef]
- Nhung, N.T.T.; Amini, H.; Schindler, C.; Kutlar Joss, M.; Dien, T.M.; Probst-Hensch, N.; Perez, L.; Künzli, N. Short-term association between ambient air pollution and pneumonia in children: A systematic review and meta-analysis of time-series and case-crossover studies. Environ. Pollut. 2017, 230, 1000–1008. [Google Scholar] [CrossRef] [PubMed]
- Adaji, E.E.; Ekezie, W.; Clifford, M.; Phalkey, R. Understanding the effect of indoor air pollution on pneumonia in children under 5 in low- and middle-income countries: A systematic review of evidence. Environ. Sci. Pollut. Res. 2019, 26, 3208–3225. [Google Scholar] [CrossRef] [PubMed]
- Seaton, A.; MacNee, W.; Donaldson, K.; Godden, D. Particulate air pollution and acute health effects. Lancet 1995, 345, 176–178. [Google Scholar] [CrossRef]
- Ashmore, M.R.; Dimitroulopoulou, C. Personal exposure of children to air pollution. Atmos. Environ. 2009, 43, 128–141. [Google Scholar] [CrossRef]
- Joubert, B.R.; Mantooth, S.N.; McAllister, K.A. Environmental health research in Africa: Important progress and promising opportunities. Front. Genet. 2020, 10, 1166. [Google Scholar] [CrossRef]
- Bo, M.; Salizzoni, P.; Clerico, M.; Buccolieri, R. Assessment of indoor-outdoor particulate matter air pollution: A review. Atmosphere 2017, 8, 136. [Google Scholar] [CrossRef]
- Kim, K.H.; Kabir, E.; Kabir, S. A review on the human health impact of airborne particulate matter. Environ. Int. 2015, 74, 136–143. [Google Scholar] [CrossRef]
- Suk, W.; Ruchirawat, M.; Stein, R.T.; Diaz-Barriga, F.; Carpenter, D.O.; Neira, M.; Sly, P.D. Health consequences of environmental exposures in early life: Coping with a changing world in the post-MDG era. Ann. Glob. Health 2016, 82, 20–27. [Google Scholar] [CrossRef]
- Karanasiou, A.; Moreno, N.; Moreno, T.; Viana, M.; de Leeuw, F.; Querol, X. Health effects from Sahara dust episodes in Europe: Literature review and research gaps. Environ. Int. 2012, 47, 107–114. [Google Scholar] [CrossRef]
- Gotschi, T.; Heinrich, J.; Sunyer, J.; Kunzli, N. Long-term effects of ambient air pollution on lung function: A review. Epidemiology 2008, 19, 690–701. [Google Scholar] [CrossRef]
- Arku, R.E.; Birch, A.; Shupler, M.; Yusuf, S.; Hystad, P.; Brauer, M. Characterizing exposure to household air pollution within the Prospective Urban Rural Epidemiology (PURE) study. Environ. Int. 2018, 114, 307–317. [Google Scholar] [CrossRef] [PubMed]
- Shupler, M.; Godwin, W.; Frostad, J.; Gustafson, P.; Arku, R.E.; Brauer, M. Global estimation of exposure to fine particulate matter (PM2.5) from household air pollution. Environ. Int. 2018, 120, 354–363. [Google Scholar] [CrossRef]
- Kirenga, B.J.; Meng, Q.; van Gemert, F.; Aanyu-Tukamuhebwa, H.; Chavannes, N.; Katamba, A.; Obai, G.; van der Molen, T.; Schwander, S.; Mohsenin, V. The state of ambient air quality in two ugandan cities: A pilot cross-sectional spatial assessment. Int. J. Environ. Res. Public Health 2015, 12, 8075–8091. [Google Scholar] [CrossRef] [PubMed]
- Katoto, P.; Byamungu, L.; Brand, A.S.; Mokaya, J.; Strijdom, H.; Goswami, N.; De Boever, P.; Nawrot, T.S.; Nemery, B. Ambient air pollution and health in Sub-Saharan Africa: Current evidence, perspectives and a call to action. Environ. Res. 2019, 173, 174–188. [Google Scholar] [CrossRef] [PubMed]
- Piddock, K.C.; Gordon, S.B.; Ngwira, A.; Msukwa, M.; Nadeau, G.; Davis, K.J.; Nyirenda, M.J.; Mortimer, K. A cross-sectional study of household biomass fuel use among a periurban population in Malawi. Ann. Am. Thor. Soc. 2014, 11, 915–924. [Google Scholar] [CrossRef] [PubMed]
- Korten, I.; Ramsey, K.; Latzin, P. Air pollution during pregnancy and lung development in the child. Paediatr. Respir. Rev. 2017, 21, 38–46. [Google Scholar] [CrossRef]
- Gray, D.; Willemse, L.; Visagie, A.; Czovek, D.; Nduru, P.; Vanker, A.; Stein, D.J.; Koen, N.; Sly, P.D.; Hantos, Z. Determinants of early-life lung function in African infants. Thorax 2017, 72, 445–450. [Google Scholar] [CrossRef]
- Vanker, A.; Barnett, W.; Workman, L.; Nduru, P.M.; Sly, P.D.; Gie, R.P.; Zar, H.J. Early-life exposure to indoor air pollution or tobacco smoke and lower respiratory tract illness and wheezing in African infants: A longitudinal birth cohort study. Lancet Planet Health 2017, 1, e328–e336. [Google Scholar] [CrossRef]
- Voynow, J.A.; Auten, R. Environmental pollution and the developing lung. Clin. Pulm. Med. 2015, 22, 177–184. [Google Scholar] [CrossRef]
- Ober, C. Asthma genetics in the post-GWAS era. Ann. Am. Thor. Soc. 2016, 13, S85–S90. [Google Scholar]
- He, L.; Li, Z.; Teng, Y.; Cui, X.; Barkjohn, K.K.; Norris, C.; Fang, L.; Lin, L.; Wang, Q.; Zhou, X. Associations of personal exposure to air pollutants with airway mechanics in children with asthma. Environ. Int. 2020, 138, 105647. [Google Scholar] [CrossRef] [PubMed]
- Hüls, A.; Vanker, A.; Gray, D.; Koen, N.; MacIsaac, J.L.; Lin, D.T.S.; Ramadori, K.E.; Sly, P.D.; Stein, D.J.; Kobor, M.S. Genetic susceptibility to asthma increases the vulnerability to indoor air pollution. Eur. Respir. J. 2020, 55, 1901831. [Google Scholar] [CrossRef] [PubMed]
- Gall, E.T.; Carter, E.M.; Matt Earnest, C.; Stephens, B. Indoor air pollution in developing countries: Research and implementation needs for improvements in global public health. Am. J. Public Health 2013, 103, e67–e72. [Google Scholar] [CrossRef] [PubMed]
- Ezzati, M.; Kammen, D.M. The health impacts of exposure to indoor air pollution from solid fuels in developing countries: Knowledge, gaps, and data needs. Environ. Health Perspect. 2002, 110, 1057–1068. [Google Scholar] [CrossRef] [PubMed]
- Okello, G.; Devereux, G.; Semple, S. Women and girls in resource poor countries experience much greater exposure to household air pollutants than men: Results from Uganda and Ethiopia. Environ. Int. 2018, 119, 429–437. [Google Scholar] [CrossRef]
- Vanker, A.; Barnett, W.; Nduru, P.M.; Gie, R.P.; Sly, P.D.; Zar, H.J. Home environment and indoor air pollution exposure in an African birth cohort study. Sci. Total Environ. 2015, 536, 362–367. [Google Scholar] [CrossRef]
- Dionisio, K.L.; Howie, S.R.; Dominici, F.; Fornace, K.M.; Spengler, J.D.; Adegbola, R.A.; Ezzati, M. Household concentrations and exposure of children to particulate matter from biomass fuels in The Gambia. Environ. Sci. Tech. 2012, 46, 3519–3527. [Google Scholar] [CrossRef]
- Havens, D.; Wang, D.; Grigg, J.; Gordon, S.B.; Balmes, J.; Mortimer, K. The Cooking and Pneumonia Study (CAPS) in Malawi: A cross-sectional assessment of carbon monoxide exposure and carboxyhemoglobin levels in children under 5 years old. Int. J. Environ. Res. Public Health 2018, 15, 1936. [Google Scholar] [CrossRef]
- Nsoh, M.; Mankollo, B.O.Y.; Ebongue, M.; Cyprien, K.N.; Likeng, J.L.N.; Islam, S.M.S.; Collier, A.; Tsoka-Gwegweni, J.M.; Cumber, S.N. Acute respiratory infection related to air pollution in Bamenda, North West Region of Cameroon. Pan. Afr. Med. J. 2019, 32, 99. [Google Scholar] [CrossRef]
- Kilabuko, J.H.; Matsuki, H.; Satoshi Nakai, S. Air quality and acute respiratory illness in biomass fuel using homes in Bagamoyo, Tanzania. Int. J. Environ. Res. Public Health 2007, 4, 39–44. [Google Scholar] [CrossRef]
- Admasie, A.; Kumie, A.; Worku, A. Children under five from houses of unclean fuel sources and poorly ventilated houses have higher odds of suffering from acute respiratory infection in Wolaita-Sodo, Southern Ethiopia: A case-control study. J. Environ. Public Health 2018. [Google Scholar] [CrossRef] [PubMed]
- Sanbata, H.; Asfaw, A.; Kumie, A. Association of biomass fuel use with acute respiratory infections among under- five children in a slum urban of Addis Ababa, Ethiopia. BMC Public Health 2014, 14, 1122. [Google Scholar] [CrossRef]
- Mishra, V. Indoor air pollution from biomass combustion and acute respiratory illness in preschool age children in Zimbabwe. Int. J. Epidemiol. 2003, 32, 847–853. [Google Scholar] [CrossRef] [PubMed]
- Van Zyl Smit, R.N.; Pai, M.; Yew, W.W.; Leung, C.C.; Zumla, A.; Bateman, E.D.; Dheda, K. Global lung health: The colliding epidemics of tuberculosis, tobacco smoking, HIV and COPD. Eur. Respir. J. 2010, 35, 27–33. [Google Scholar] [CrossRef] [PubMed]
- Mustapha, B.A.; Blangiardo, M.; Briggs, D.J.; Hansell, A. Traffic air pollution and other risk factors for respiratory illness in schoolchildren in the Niger-Delta Region of Nigeria. Environ. Health Perspect. 2011, 119, 1478–1482. [Google Scholar] [CrossRef] [PubMed]
- Po, J.Y.; FitzGerald, J.M.; Carlsten, C. Respiratory disease associated with solid biomass fuel exposure in rural women and children: Systematic review and meta-analysis. Thorax 2011, 66, 232–239. [Google Scholar] [CrossRef]
- Thacher, J.D.; Emmelin, A.; Madaki, A.J.K.; Thacher, T.D. Biomass fuel use and the risk of asthma in Nigerian children. Respir. Med. 2013, 107, 1845–1851. [Google Scholar] [CrossRef]
- Foote, E.M.; Gieraltowski, L.; Ayers, T.; Sadumah, I.; Faith, S.H.; Silk, B.J.; Cohen, A.L.; Were, V.; Hughes, J.M.; Quick, R.E. Impact of locally-produced, ceramic cookstoves on respiratory disease in children in rural western Kenya. Am. J. Trop. Med. Hyg. 2013, 88, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Barnes, B.R. Behavioural change, indoor air pollution and child respiratory health in developing countries: A review. Int. J. Environ. Res. Public Health 2014, 11, 4607–4618. [Google Scholar] [CrossRef]
- Shirinde, J.; Wichmann, J.; Voyi, K. Association between wheeze and selected air pollution sources in an air pollution priority area in South Africa: A cross-sectional study. Environ. Health 2014, 13, 32. [Google Scholar] [CrossRef]
- Heinzerling, A.P.; Guarnieri, M.J.; Mann, J.K.; Diaz, J.V.; Thompson, L.M.; Diaz, A.; Bruce, N.G.; Smith, K.R.; Balmes, J.R. Lung function in woodsmoke-exposed Guatemalan children following a chimney stove intervention. Thorax 2016, 71, 421–428. [Google Scholar] [CrossRef] [PubMed]
- Mortimer, K.; Ndamala, C.B.; Naunje, A.W.; Malava, J.; Katundu, C.; Weston, W.; Havens, D.; Pope, D.; Bruce, N.G.; Nyirenda, M. A cleaner burning biomass-fuelled cookstove intervention to prevent pneumonia in children under 5 years old in rural Malawi (the Cooking and Pneumonia Study): A cluster randomised controlled trial. Lancet 2017, 389, 167–175. [Google Scholar] [CrossRef]
- Olutola, B.G.; Claassen, N.; Wichmann, J.; Voyi, K. Factors associated with parent-reported wheeze and cough in children living in an industrial area of Gauteng, South Africa. Environ. Sci. Pollut. Res. 2018, 25, 33455–33463. [Google Scholar] [CrossRef] [PubMed]
- Kirby, M.A.; Nagel, C.L.; Rosa, G.; Zambrano, L.D.; Musafiri, S.; Ngirabega, J.D.; Thomas, E.A.; Clasen, T. Effects of a large-scale distribution of water filters and natural draft rocket-style cookstoves on diarrhea and acute respiratory infection: A cluster-randomized controlled trial in Western Province, Rwanda. PLoS Med. 2019, 16, e1002812. [Google Scholar] [CrossRef]
- Mentz, G.; Robins, T.G.; Batterman, S.; Naidoo, R.N. Effect modifiers of lung function and daily air pollutant variability in a panel of schoolchildren. Thorax 2019, 74, 1055–1062. [Google Scholar] [CrossRef]
- Rylance, S.; Nightingale, R.; Naunje, A.; Mbalume, F.; Jewell, C.; Balmes, J.R.; Grigg, J.; Mortimer, K. Lung health and exposure to air pollution in Malawian children (CAPS): A cross-sectional study. Thorax 2019, 74, 1070–1077. [Google Scholar] [CrossRef]
- Vanker, A.; Nduru, P.M.; Barnett, W.; Dube, F.S.; Sly, P.D.; Gie, R.P.; Nicol, M.P.; Zar, H.J. Indoor air pollution and tobacco smoke exposure: Impact on nasopharyngeal bacterial carriage in mothers and infants in an African birth cohort study. Eur. Respir. J. Open Res. 2019, 5, 00052–2018. [Google Scholar] [CrossRef]
- Olaniyan, T.; Jeebhay, M.; Röösli, M.; Naidoo, R.N.; Künzli, N.; de Hoogh, K.; Saucy, A.; Badpa, M.; Baatjies, R.; Parker, B. The association between ambient NO2 and PM2.5 with the respiratory health of school children residing in informal settlements: A prospective cohort study. Environ. Res. 2020, 186, 109606. [Google Scholar] [CrossRef]
- World Health Organization. Inheriting a Sustainable World? Report No.: Licence: CC BY-NC-SA 3.0 IGO; World Health Organisation: Geneva, Switzerland, 2017. [Google Scholar]
| Publication Year | No Publications | Author | Summary |
|---|---|---|---|
| 2002 | 1 | Ezzati M [49] | Solid fuels and health impacts. |
| 2003 | 1 | Mishra V [58] | BMF and ARIs in presechool children. |
| 2007 | 1 | Kilabuko JH [55] | Air quality and ARSs in chldren. |
| 2010 | 1 | Van Zyl-Smit R [59] | TB, smoking, HIV and COPD. |
| 2011 | 2 | Mustapha BA [60] | Air pollution and respiratory illnesses. |
| Po JY [61] | Respiratory diseases and BMF exposure. | ||
| 2012 | 1 | Dionisio KL [52] | Exposure of children to PM in household. |
| 2013 | 4 | Adeloye D [24] | Asthma prevalence in Africa. |
| Gall ET [48] | Air pollution in developing countries. | ||
| Thacher JD [62] | BMF and asthma risk. | ||
| Foote [63] | Cookstoves and impact on lung health | ||
| 2014 | 6 | Barnes BR [64] | Behavioural factors and air pollution. |
| Gordon SB [14] | Respiratory risk for HAP. | ||
| Piddock KC [40] | BMF in Malawi. | ||
| Sanbata H [57] | BMF and ARI in children under 5 years. | ||
| Shirinde J [65] | Wheeze and air pollution in children. | ||
| WHO [19] | Air pollution and burden of disease | ||
| 2015 | 4 | Kirenga BJ [38] | Air quality in two Ugandan cities. |
| Sly PD [3] | Early origins of COPD. | ||
| Vanker A [51] | Home environment and air pollution exposure. | ||
| Voynow JA [44] | Air pollution and the developing lung. | ||
| 2016 | 3 | Heinzerling AP [66] | Lung function and wood exposure. |
| Goldizen FC [25] | Respiratory effect of air pollution on children. | ||
| Ober C [45] | Asthma and GWAS studies. | ||
| 2017 | 5 | Gray D [42] | Early lung function determinants. |
| Korten I [41] | Air pollution in pregnancy and lung development. | ||
| Mortimer K [67] | Cleaner cookstoves and impact on pneumonia. | ||
| Vanker A [43] | Early life exposures and ARI and wheezing. | ||
| WHO [18] | Inheriting a sustainable world. | ||
| 2018 | 9 | Admasie A [56] | Under 5 years and air pollution. |
| Arku RE [36] | HAP exposure and rural-urban differences. | ||
| Havens D [53] | Carbon monoxide exposure in children under 5 years. | ||
| Kim D [2] | Early origins of lung disease and air pollution. | ||
| Landrigan [1] | Pollution and health. | ||
| Okello G [50] | Women and girls increased pollution exposure. | ||
| Olutola BG [68] | Cough and wheeze and outdoor air pollution. | ||
| Shupler M [37] | Global estimates of HAP. | ||
| WHO [19] | Air pollution and child health | ||
| 2019 | 11 | Atani M [21] | Air pollution and mortality. |
| Katoto P [39] | Ambient air pollution and health in sSA. | ||
| Kirby MA [69] | Cookstoves and ARI. | ||
| Mentz G [70] | Effect modifiers of lung function and air pollution. | ||
| McAllister DA [23] | Global, regional and national estimates of LRTI mortality. | ||
| Myllyvirth L [21] | Air quality and health impacts. | ||
| Nsoh M [54] | ARI and air pollution. | ||
| Olaniyan T [18] | Air pollution and respiratory health of children. | ||
| Rylance S [71] | Lung health and air pollution in children. | ||
| Schraufnagel DE [4] | Health benefits of air pollution reduction. | ||
| Vanker A [72] | Indoor air pollution and bacterial carriage. | ||
| 2020 | 3 | Hüls A. [47] | Genetic susceptibility to asthma and air pollution. |
| He L. [46] | Perinatal air pollution exposure and respiratory mechanics in children. | ||
| Olaniyan T [73] | PM exposure and NO on respiratory health of children. | ||
| Country | Indoor vs. Outdoor Source | Pollutant | Timing of Exposure | Age of Effect | Effect | Study |
|---|---|---|---|---|---|---|
| South Africa | Indoor | Benzene | Prenatal | 6 weeks | Altered lung function (lower time to peak tidal expiratory flow over total expiratory time ratios; 3.0% (95% CI −5.2% to −0.7%, p = 0.01)) | Determinants of early-life lung function in African infants [42]. |
| Zimbabwe | Indoor | Biomass | Infancy | 6–11 months | Increased risk of Acute Respiratory Infections (two-fold) | Indoor air pollution from biomass combustion and acute respiratory illness in preschool age children in Zimbabwe [58]. |
| Cameroon | Indoor | Infants | Mean age 9 years | Increased risk of Acute Respiratory Infections (OR 3.62, 95% CI 1.45–4.90) | Acute respiratory infection related to air pollution in Bamenda, North West Region of Cameroon [54]. | |
| Tanzania | Indoor | Biomass PM10, NO2, and CO | Children under 5years and household | Under 5 years and exposed women cooks | ARI prevalence for cooks and children under age 5 making up the exposed group—54.7% (OR 5.5; 95% CI 3.6 to 8.5) | Air quality and acute respiratory illness in biomass fuel using homes in Bagamoyo, Tanzania [55]. |
| South Africa | Indoor | Particulate matter (PM10) | Postnatal | Infants | Nasopharyngeal carriage of H. influenzae (aRR 1.68 (95% CI 1.10–2.57)) or Moraxella catarrhalis (aRR 1.42 (95% CI 1.03–1.97)) | Indoor air pollution and tobacco smoke exposure: impact on nasopharyngeal bacterial carriage in mothers and infants in an African birth cohort study [72]. |
| South Africa | Outdoor | TRAP | Children under 5 years | Aged 1 to 26 months | Children with trucks passing on streets frequently, dry cough more likely (aOR 3.88; 95% CI 2.29–6.57). | Factors associated with parent-reported wheeze and cough in children living in an industrial area of Gauteng, South Africa [68]. |
| South Africa | Indoor and Outdoor | Gas heating and cooking TRAP | School going children | 13–14 years | Gas used for residential heating —“wheeze ever” increased by 47% (OR 1.47 95% CI: 1.15–1.88). Trucks passing near homes—increased “wheeze ever” (OR 1.32 95% CI: 1.01–1.73), “current wheeze” (OR 1.61 95% CI: 1.15–2.24) and “current severe wheeze” (OR 2.22 95% CI: 1.28–3.77). | Association between wheeze and selected air pollution sources in an air pollution priority area in South Africa: a cross-sectional study [65]. |
| Nigeria | Outdoor | TRAP | School going children | 7–14 years | Traffic disturbance at home (noise or fumes) associated with wheeze (OR = 2.16; 95% CI 1.28–3.64); Night cough (OR 1.37; 95% CI 1.03–1.82) Phlegm (OR1.49; 95% CI 1.09–2.04) | Traffic air pollution and other risk factors for respiratory illness in schoolchildren in the Niger-delta region of Nigeria [60]. |
| Malawi | Indoor | Carbon monoxide–household air pollution | School going children | 6–8 years | Spirometric abnormalities (7.1% low forced vital capacity (FVC); 6.3% obstruction) were seen in 13.0% of children | Lung health and exposure to air pollution in Malawian children (CAPS): a cross-sectional study [71]. |
| South Africa | Indoor | PM10 | Prenatal and postnatal exposure | Infants 6 weeks and 1 year | Pre- and postnatal PM10 exposure reduced lung function at 6 weeks and 1 year and lower respiratory tract infection in the first year. Infants with asthma-related risk alleles more susceptible to PM10-associated reduced lung function. | Genetic susceptibility to asthma increases the vulnerability to indoor air pollution [47]. |
| South Africa | Indoor | Kerosene (paraffin) | School going children | 9–11 years | Kerosene use associated significant airway inflammation (FeNO > 35 ppb) (aOR: 2.31, 95% CI: 1.05–5.06). | Asthma-related outcomes associated with indoor air pollutants among schoolchildren from four informal settlements in two municipalities in the Western Cape Province of South Africa [17]. |
| South Africa | Outdoor | NO2 and PM2.5 | School going children | Grade 4 pupils | NO2 associated with increased risk of: new onset of ocular-nasal symptoms (aOR: 1.63, 95% CI: 1.01–2.60), wheezing (aOR: 3.57, 95% CI: 1.18–10.92), ≥2 asthma symptom score (aOR: 1.71, 95% CI: 1.02–2.86), and airway inflammation FeNO > 35 ppb (aOR: 3.10, 95% CI: 1.10–8.71), independent of PM2.5 exposures. | The association between ambient NO2 and PM2.5 with the respiratory health of school children residing in informal settlements: A prospective cohort study [73]. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Masekela, R.; Vanker, A. Lung Health in Children in Sub-Saharan Africa: Addressing the Need for Cleaner Air. Int. J. Environ. Res. Public Health 2020, 17, 6178. https://doi.org/10.3390/ijerph17176178
Masekela R, Vanker A. Lung Health in Children in Sub-Saharan Africa: Addressing the Need for Cleaner Air. International Journal of Environmental Research and Public Health. 2020; 17(17):6178. https://doi.org/10.3390/ijerph17176178
Chicago/Turabian StyleMasekela, Refiloe, and Aneesa Vanker. 2020. "Lung Health in Children in Sub-Saharan Africa: Addressing the Need for Cleaner Air" International Journal of Environmental Research and Public Health 17, no. 17: 6178. https://doi.org/10.3390/ijerph17176178
APA StyleMasekela, R., & Vanker, A. (2020). Lung Health in Children in Sub-Saharan Africa: Addressing the Need for Cleaner Air. International Journal of Environmental Research and Public Health, 17(17), 6178. https://doi.org/10.3390/ijerph17176178





