Crying Therapy Intervention for Breast Cancer Survivors: Development and Effects
Abstract
1. Introduction
Objective and Hypotheses
2. Materials and Methods
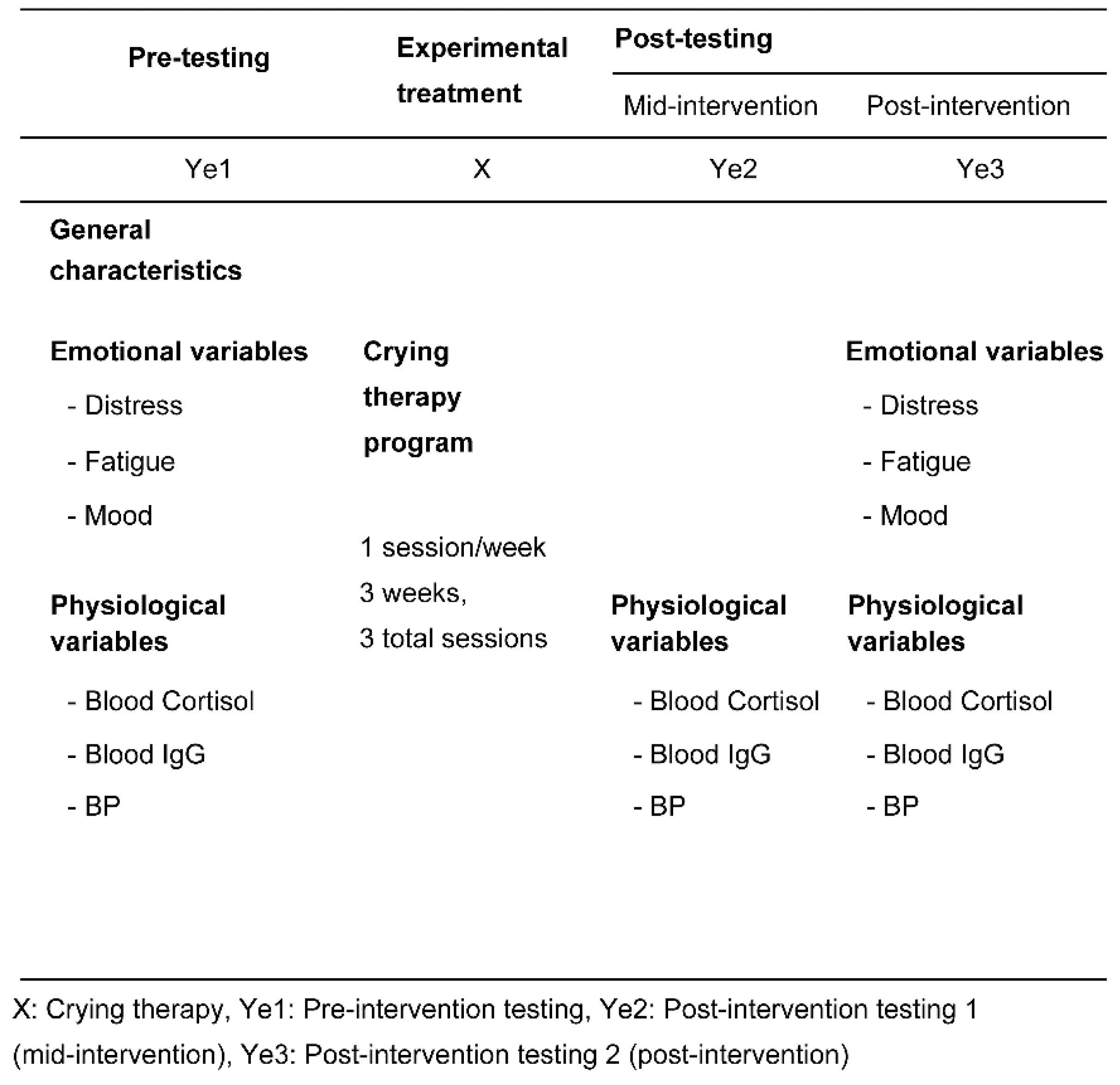
2.1. Design
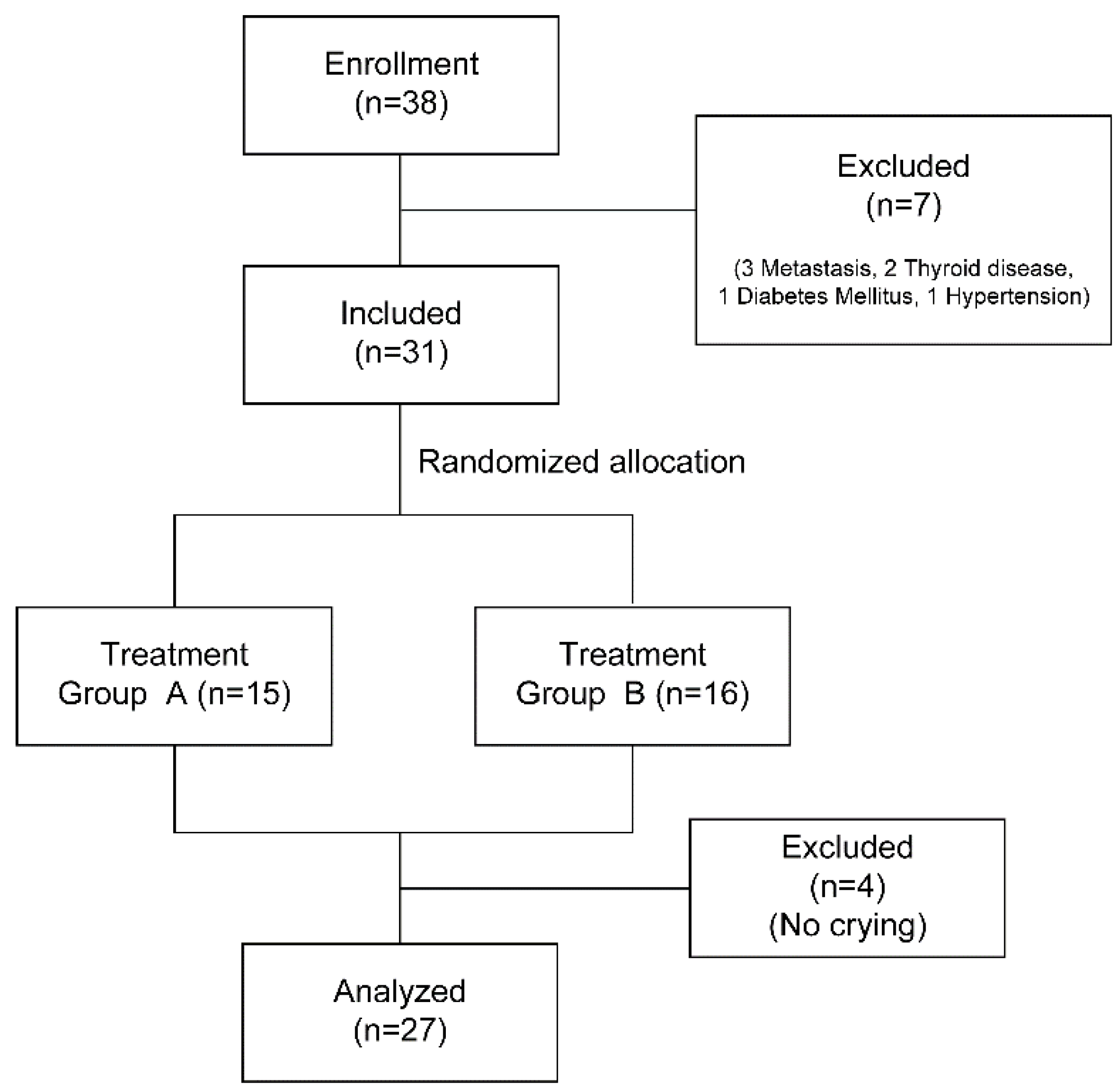
2.2. Sample and Setting
2.2.1. Variables
Emotional Effects
Physiological Effects
2.3. Experimental Intervention Program: Crying Therapy
2.3.1. Phase 1: Introductory Phase
2.3.2. Phase 2: Execution Phase
2.3.3. Phase 3: Closing Phase
2.4. Study Procedures
2.4.1. Ethical Considerations
2.4.2. Preliminary Study
2.4.3. Main Study
2.5. Data Analysis
3. Results
3.1. Participant Characteristics
3.2. Hypothesis Testing
3.2.1. Hypothesis 1
3.2.2. Hypothesis 2
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. All Cancers (Excluding Non-Melanoma Skin Cancer): Estimated Incidence, Mortality and Prevalence Worldwide in 2019. Available online: https://gco.iarc.fr/today/data/factsheets/populations/900-world-fact-sheets.pdf (accessed on 2 December 2019).
- Larson, M.R.; Duberstein, P.R.; Talbot, N.L.; Caldwell, C.; Moynihan, J.A. A presurgical psychosocial intervention for breast cancer patients: Psychological distress and the immune response. J. Psychosom. Res. 2000, 48, 187–194. [Google Scholar] [CrossRef]
- Lazarus, R.S.; Folkman, S. Stress, Appraisal, and Coping; Springer Publishing Company: New York, NY, USA, 1984. [Google Scholar]
- Park, J.H.; Bae, S.H.; Chun, M.S.; Jung, Y.S.; Jung, Y.M. Factors influencing elevated distress scores at the end of primary treatment of breast cancer. Asian Oncol. Nurs. 2015, 15, 132–139. [Google Scholar] [CrossRef]
- Burgess, C.; Cornelius, V.; Love, S.; Graham, J.; Richards, M.; Ramirez, A. Depression and anxiety in women with early breast cancer: Five-year observational cohort study. BMJ 2005, 330, 702. [Google Scholar] [CrossRef]
- Lee, J.H.; Byun, H.S.; Kim, G.D. Impacts of the mood state on the quality of life in breast cancer survivors. J. Korea Contents Assoc. 2014, 14, 356–366. [Google Scholar] [CrossRef]
- Seong, S.R.; Cho, M.K.; Kim, J.; Kim, Y.O. Effects of group coaching program on depression, anxiety and hope in women with breast cancer undergoing chemotherapy. Asian Oncol. Nurs. 2017, 17, 188–199. [Google Scholar] [CrossRef]
- Phillips, K.M.; Antoni, M.H.; Lechner, S.C.; Blomberg, B.B.; Llabre, M.M.; Avisar, E.; Glück, S.; DerHagopian, R.; Carver, C.S. Stress management intervention reduces serum cortisol and increases relaxation during treatment for nonmetastatic breast cancer. Psychosom. Med. 2008, 70, 1044–1049. [Google Scholar] [CrossRef]
- Antoni, M.H. Stress management effects on psychological, endocrinological, and immune functioning in men with HIV infection: Empirical support for a psychoneuroimmunological model. Stress 2003, 6, 173–188. [Google Scholar] [CrossRef] [PubMed]
- Jeon, S.I. Clinical Application and Practice of Complimentary Alternative Medicine; Korean Medicine Academies Press: Seoul, Korea, 2009. [Google Scholar]
- Qiu, J.; Keyser, B.; Lin, Z.T.; Wu, T. Autoantibodies as potential biomarkers in breast cancer. Biosensors 2018, 8, 67. [Google Scholar] [CrossRef]
- Han, H.J.; Park, A.; Kim, H.S.; Moon, H.K.; Park, Y.H. The effects of laughter therapy on stress responses in patients with preoperative breast cancer. J. Korean Oncol. Nurs. 2011, 11, 93–100. [Google Scholar] [CrossRef]
- Bylsma, L.M.; Gračanin, A.; Vingerhoets, A.J. The neurobiology of human crying. Clin. Auton. Res. 2019, 29, 63–73. [Google Scholar] [CrossRef]
- Hastrup, J.L.; Baker, J.G.; Kraemer, D.L.; Bornstein, R.F. Crying and depression among older adults. Gerontologist 1986, 26, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Lee, B.Y. You Have to Cry to Live; Jungang M & B: Seoul, Korea, 2011. [Google Scholar]
- Lee, J.Y.; Seo, Y.S. A phenomenological study of client’s meaningful tear experience in the therapy process. J. Korean Couns. Psychother. 2017, 29, 553–576. [Google Scholar] [CrossRef]
- Frey, W.H. Crying: The Mystery of Tears; Harper Row Press: New York, NY, USA, 1985. [Google Scholar]
- Fooladi, M.M. The healing effects of crying. Holist. Nurs. Pract. 2005, 19, 248–255. [Google Scholar] [CrossRef]
- Dugan, D.O. Laughter and tears: Best medicine for stress. Nurs. Forum 1989, 24, 18–26. [Google Scholar] [CrossRef]
- Gračanin, A.; Bylsma, L.; Vingerhoets, A.J. Why only humans shed emotional tears: Evolutionary and cultural perspectives. Hum. Nat. 2018, 29, 104–133. [Google Scholar] [CrossRef]
- Griffith, M.B.; Hall, J.M.; Fields, B. Crying that heals: Concept evaluation. J. Holist. Nurs. 2011, 29, 167–179. [Google Scholar] [CrossRef] [PubMed]
- Curtis, R.; Matise, M.; Glass, J.S. Counselling students’ views and concerns about weeping with clients: A pilot study. Couns. Psychother. Res. 2003, 3, 300–306. [Google Scholar] [CrossRef]
- Van de Ven, N.; Meijs, M.H.J.; Vingerhoets, A. What emotional tears convey: Tearful individuals are seen as warmer, but also less competent. Br. J. Soc. Psychol. 2017, 56, 146–160. [Google Scholar] [CrossRef] [PubMed]
- Vingerhoets, A.J.; Bylsma, L.; Rottenberg, J. Crying: A biopsychosocial phenomenon. In Tears in the Graeco-Roman World; Fogen, T., Ed.; De Guyter: Berlin, Germany, 2009; pp. 439–475. [Google Scholar]
- Vingerhoets, A.J.; Scheirs, J.G. Crying and health. In Adult Crying. A Biopsychosocial Approach; Vingerhoets, A.J., Cornelius, R.R., Eds.; Brunner-Routledge: Milton Park, UK, 2001; pp. 227–246. [Google Scholar]
- Vingerhoets, A.J.; Bylsma, L.M. The riddle of human emotional crying: A challenge for emotion researchers. Emot. Rev. 2015, 8, 207–217. [Google Scholar] [CrossRef]
- McFarland, D.C.; Shaffer, K.M.; Tiersten, A.; Holland, J. Prevalence of physical problems detected by the distress thermometer and problem list in patients with breast cancer. Psycho-Oncology 2018, 27, 1394–1403. [Google Scholar] [CrossRef]
- National Comprehensive Cancer Network. Distress Thermometer Screening Tool Figure (DIS-A), V.1.2013. Plymouth Meeting (PA): National Comprehensive Cancer Network. Available online: https://www.nccn.org/global/international_adaptations.aspx (accessed on 6 March 2017).
- Mitchell, A.J. Pooled results from 38 analyses of the accuracy of distress thermometer and other ultra-short methods of detecting cancer-related mood disorders. J. Clin. Oncol. 2007, 25, 4670–4681. [Google Scholar] [CrossRef] [PubMed]
- Byun, H.S.; Kim, E.K.; Kim, G.D. Impacts of stigma and distress on the quality of life in patients with lung cancer. Crisisonomy 2015, 11, 227–244. [Google Scholar]
- Functional Assessment of Chronic Illness Therapy. FACIT-Fatigue Scale Korean Version. Available online: https://www.2017.facit.org/FACITOrg/Questionnaires (accessed on 6 March 2017).
- Byun, H.S.; Kim, G.D. Impacts of fatigue, pain, anxiety, and depression on the quality of life in patients with breast cancer. Asian Oncol. Nurs. 2012, 12, 27–34. [Google Scholar] [CrossRef][Green Version]
- Han, K.I.; Kim, S.H. Crying: If You Hold Back, You Will Fall Sick; Samho Media Press: Incheon, Korea, 2012. [Google Scholar]
- Janov, A. The Biology of Love; Prometheus Books: New York, NY, USA, 2000. [Google Scholar]
- Choi, S.J. Korean Psychology; Hakjisa Press: Seoul, Korea, 2011. [Google Scholar]
- Freud, S.; Breuer, J. Studies in Hysteria; Penguin Books Press: London, UK, 2004. [Google Scholar]
- Vingerhoets, A.; Bylsma, L. Crying and health: Popular and scientific conceptions. Psychol. Top. 2007, 16, 275–296. [Google Scholar]
- Hendriks, M.C.; Croon, M.A.; Vingerhoets, A.J. Social reaction to adult crying: The help-soliciting function of tears. J. Soc. Psychol. 2008, 148, 22–41. [Google Scholar] [CrossRef]
| Week/Phase | Program Contents | Background Music | Time (mins) | ||
|---|---|---|---|---|---|
| Week 1 | Introductory phase | Developing intimacy, opening up, preparing for crying therapy | Exchanging greetings Explaining the effects of crying therapy Introducing the need for the program Introducing the procedure of the program | 120 min | |
| Week 2 | Execution phase | “Finding my wounded self” | Breathing methods to relieve physical and psychological tension - Abdominal breathing - Progressive muscle relaxation - Imagery training | 15 min | |
| “Finding another me” | Communal silent contemplation for emotional involvement Silent contemplation of photographs at different ages Silent contemplation on infancy Silent contemplation on preschool age Silent contemplation on school age Silent contemplation on adolescence | Sad piano pieces | 25 min | ||
| “Treating my wounded self” | Watching videos of terminal patients Writing a will Silent contemplation to cleanse wounds Reading the will aloud Hugging partners | Meditation music | 70 min | ||
| “Self-discovery of hope” | Final silent contemplation Stretching and shouting | Meditation music | 10 min | ||
| Week 3 | Closing phase | Sharing feelings | Introducing cases of overcoming cancer Final silent contemplation Reading poetry aloud Writing a letter to oneself Expressing one’s feelings and changes | Meditation music | 120 min |
| Variable | Category | n | % | Variable | Category | n | % |
|---|---|---|---|---|---|---|---|
| Sociodemographic Characteristics | |||||||
| Educational level | Middle school graduation or below | 5 | 18.5 | Household size (number of persons) | 1–2 | 6 | 22.2 |
| High school graduation | 16 | 59.3 | 3–4 | 14 | 51.9 | ||
| University graduation or above | 6 | 22.2 | 5 or more | 7 | 25.9 | ||
| Marital status | Married | 23 | 85.2 | Occupation | Unemployed | 25 | 92.6 |
| Widowed | 4 | 14.8 | Employed | 2 | 7.4 | ||
| Exercise (times per week) | Once or less | 4 | 14.8 | Religion | Yes | 21 | 77.8 |
| 2–3 times | 14 | 51.9 | No | 6 | 22.2 | ||
| 4 times or more | 9 | 33.3 | |||||
| Disease-related characteristics | |||||||
| Stage at diagnosis | 0 | 3 | 11.1 | Time since diagnosis (years) | 0–5 | 15 | 55.6 |
| 1 | 9 | 33.3 | 6–10 | 8 | 29.6 | ||
| 11–20 | 4 | 14.8 | |||||
| 2 | 13 | 48.1 | Family history of breast cancer | Yes | 2 | 7.4 | |
| 3 | 2 | 7.4 | No | 25 | 92.6 | ||
| Surgery | Partial mastectomy | 14 | 51.9 | Radiotherapy | Yes | 22 | 81.5 |
| Total mastectomy | 13 | 48.1 | No | 5 | 18.5 | ||
| Chemotherapy | Yes | 20 | 74.1 | Antihormone therapy | Yes | 9 | 33.3 |
| No | 7 | 25.9 | No | 18 | 66.6 | ||
| Variable | Possible Range | Pre | Post | t (p) | |
|---|---|---|---|---|---|
| M ± SD | M ± SD | ||||
| Distress | Thermometer | 0–10 | 4.63 ± 1.96 | 3.74 ± 2.54 | 2.884 (0.008) |
| Problem List | 0–39 | 9.93 ± 6.82 | 7.63 ± 6.66 | 2.820 (0.009) | |
| Fatigue | 0–52 | 15.15 ± 7.28 | 13.70 ± 8.17 | 1.257 (0.220) | |
| Mood conditions | Depression | 0–10 | 4.15 ± 2.66 | 3.04 ± 2.26 | 3.162 (0.004) |
| Anger | 0–10 | 3.89 ± 2.59 | 2.67 ± 2.11 | 2.877 (0.008) | |
| Anxiety | 0–10 | 3.93 ± 2.75 | 2.85 ± 2.91 | 3.108 (0.005) | |
| Variable | Pre a | Mid b | Post c | F (p) Bonferroni | |
|---|---|---|---|---|---|
| M ± SD | M ± SD | M ± SD | |||
| Cortisol (μg/dL) | 6.97 ± 2.54 | 7.11 ± 3.04 | 7.33 ± 3.90 | 0.176 (0.839) | |
| IgG (mg/dL) | 1268.37 ± 217.78 | 1307.70 ± 232.80 | 1346.96 ± 235.84 | 24.775 (<0.001) a < b (0.001); b < c (0.001); a < c (<0.001) | |
| Blood pressure (mm/Hg) | SBP | 126.22 ± 15.26 | 133.07 ± 14.27 | 127.00 ± 15.28 | 8.703 (0.001) a < b (0.001); b > c (0.009) |
| DBP | 80.89 ± 10.63 | 86.00 ± 9.34 | 84.70 ± 8.69 | 9.239 (<0.001) a < b (0.002); a < c (0.024) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Byun, H.-S.; Hwang, H.; Kim, G.-D. Crying Therapy Intervention for Breast Cancer Survivors: Development and Effects. Int. J. Environ. Res. Public Health 2020, 17, 4911. https://doi.org/10.3390/ijerph17134911
Byun H-S, Hwang H, Kim G-D. Crying Therapy Intervention for Breast Cancer Survivors: Development and Effects. International Journal of Environmental Research and Public Health. 2020; 17(13):4911. https://doi.org/10.3390/ijerph17134911
Chicago/Turabian StyleByun, Hye-Sun, Hyenam Hwang, and Gyung-Duck Kim. 2020. "Crying Therapy Intervention for Breast Cancer Survivors: Development and Effects" International Journal of Environmental Research and Public Health 17, no. 13: 4911. https://doi.org/10.3390/ijerph17134911
APA StyleByun, H.-S., Hwang, H., & Kim, G.-D. (2020). Crying Therapy Intervention for Breast Cancer Survivors: Development and Effects. International Journal of Environmental Research and Public Health, 17(13), 4911. https://doi.org/10.3390/ijerph17134911





