Depression and Objectively Measured Physical Activity: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Information Sources and Search Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Study Selection and Data Extraction
2.4. Quality Evaluation
2.5. Meta-Analysis
3. Results
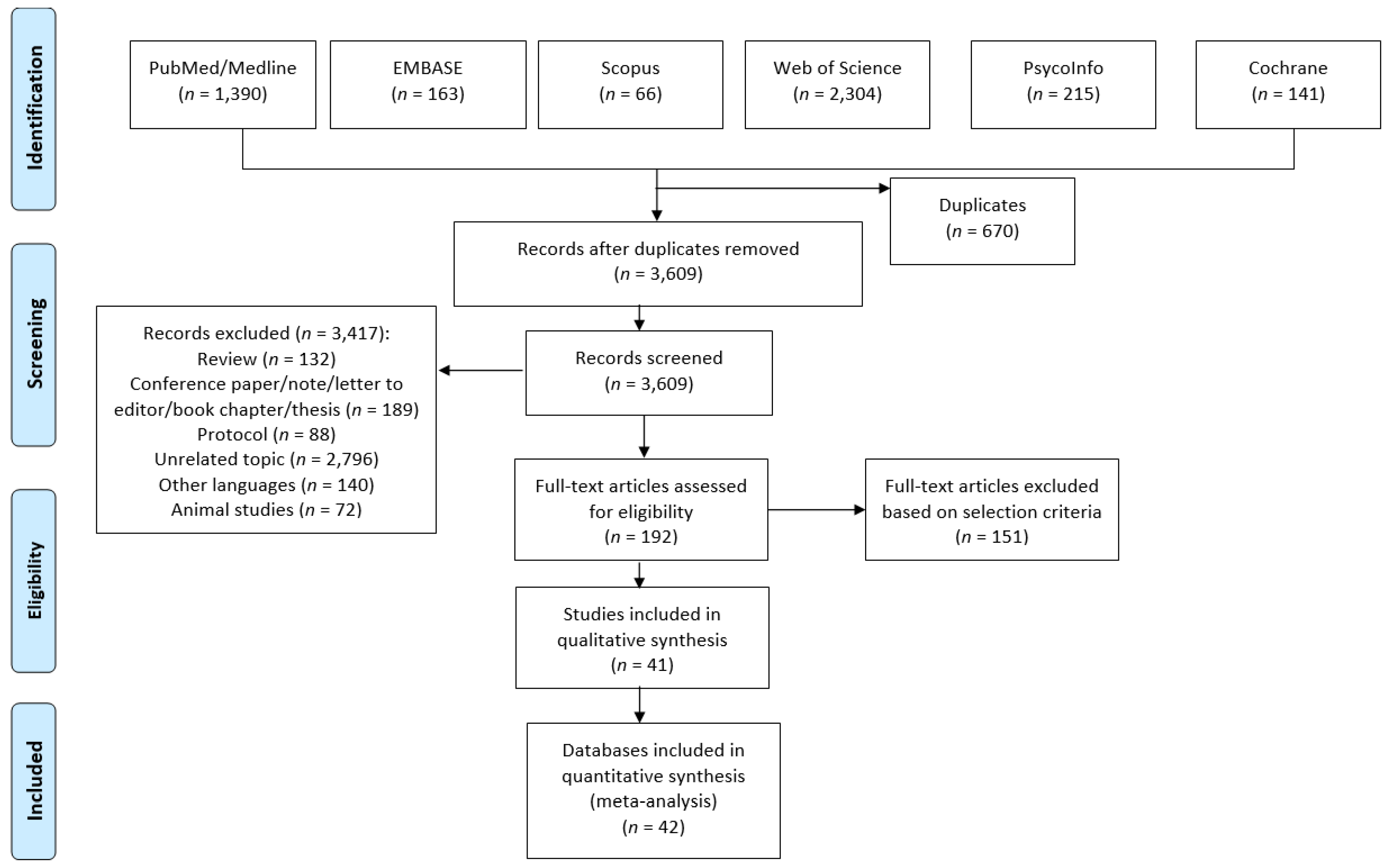
3.1. Literature Search
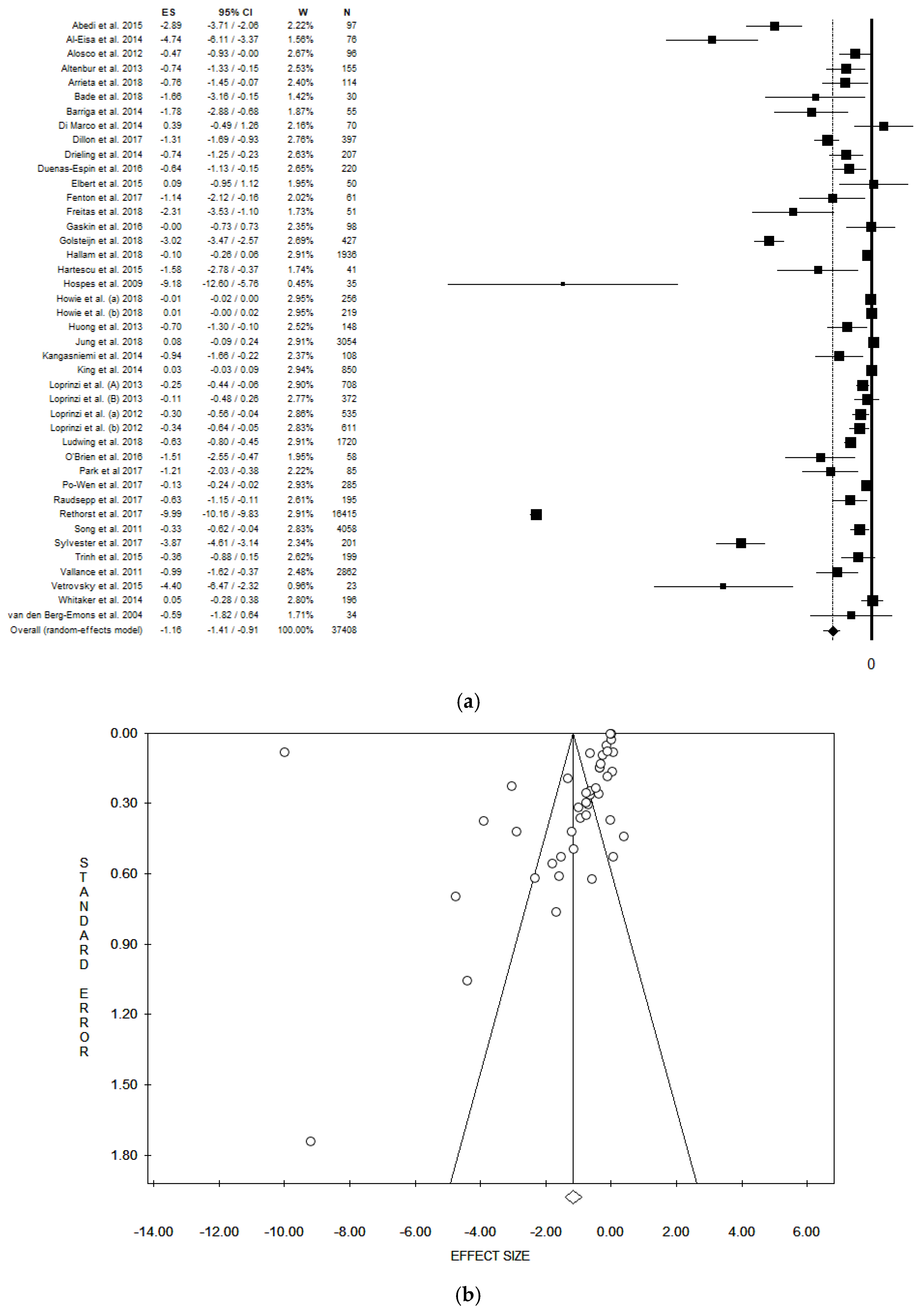
3.2. Results of Meta-Analysis
3.3. Sensitivity Analysis by Participants’ Comorbidities
3.4. Sensitivity Analysis by Study Design
3.5. Subgroup Analysis by Gender
4. Discussion
Limitantions and Strengths
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. The Global Burden of Disease: 2004 Update; Health Statistics and Information Systems: Geneva, Switzerland, 2008. [Google Scholar]
- Peveler, R.; Carson, A.; Rodin, G. Depression in medical patients. BMJ 2002, 325, 149–152. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Arlington, VA, USA, 2013. [Google Scholar]
- Odone, A.; Landriscina, T.; Amerio, A.; Costa, G. The impact of the current economic crisis on mental health in Italy: Evidence from two representative national surveys. Eur. J. Public Health 2018, 28, 490–495. [Google Scholar] [CrossRef] [PubMed]
- Burcusa, S.L.; Iacono, W.G. Risk for Recurrence in Depression. Clin. Psychol. Rev. 2007, 27, 959–985. [Google Scholar] [CrossRef] [PubMed]
- Amerio, A.; Odone, A.; Marchesi, C.; Ghaemi, S.N. Is depression one thing or many? Br. J. Psychiatry 2014, 204, 488. [Google Scholar] [CrossRef]
- Belvederi Murri, M.; Ekkekakis, P.; Magagnoli, M.; Zampogna, D.; Cattedra, S.; Capobianco, L.; Serafini, G.; Calcagno, P.; Zanetidou, S.; Amore, M. Physical Exercise in Major Depression: Reducing the Mortality Gap While Improving Clinical Outcomes. Front. Psychiatry 2018, 9, 762. [Google Scholar] [CrossRef]
- Meeusen, R.; De Meirleir, K. Exercise and brain neurotransmission. Sports Med. 1995, 20, 160–188. [Google Scholar] [CrossRef]
- Rimmele, U.; Zellweger, B.C.; Marti, B.; Seiler, R.; Mohiyeddini, C.; Ehlert, U.; Heinrichs, M. Trained men show lower cortisol, heart rate and psychological responses to psychosocial stress compared with untrained men. Psychoneuroendocrinology 2007, 32, 627–635. [Google Scholar] [CrossRef]
- Szuhany, K.L.; Bugatti, M.; Otto, M.W. A meta-analytic review of the effects of exercise on brain-derived neurotrophic factor. J. Psychiatr. Res. 2015, 60, 56–64. [Google Scholar] [CrossRef]
- Van Agtmaal, M.J.M.; Houben, A.; Pouwer, F.; Stehouwer, C.D.A.; Schram, M.T. Association of Microvascular Dysfunction with Late-Life Depression: A Systematic Review and Meta-analysis. JAMA Psychiatry 2017, 74, 729–739. [Google Scholar] [CrossRef]
- Taylor, W.D.; Aizenstein, H.J.; Alexopoulos, G.S. The vascular depression hypothesis: Mechanisms linking vascular disease with depression. Mol. Psychiatry 2013, 18, 963–974. [Google Scholar] [CrossRef]
- Schuch, F.; Vancampfort, D.; Firth, J.; Rosenbaum, S.; Ward, P.; Reichert, T.; Bagatini, N.C.; Bgeginski, R.; Stubbs, B. Physical activity and sedentary behavior in people with major depressive disorder: A systematic review and meta-analysis. J. Affect. Disord. 2017, 210, 139–150. [Google Scholar] [CrossRef] [PubMed]
- Krogh, J.; Hjorthoj, C.; Speyer, H.; Gluud, C.; Nordentoft, M. Exercise for patients with major depression: A systematic review with meta-analysis and trial sequential analysis. BMJ Open 2017, 7, e014820. [Google Scholar] [CrossRef] [PubMed]
- Strath, S.J.; Kaminsky, L.A.; Ainsworth, B.E.; Ekelund, U.; Freedson, P.S.; Gary, R.A.; Richardson, C.R.; Smith, D.T.; Swartz, A.M.; American Heart Association Physical Activity Committee of the Council on Lifestyle; et al. Guide to the assessment of physical activity: Clinical and research applications: A scientific statement from the American Heart Association. Circulation 2013, 128, 2259–2279. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions, Version 5.1.0; The Cochrane Collaboration, 2013. Available online: www.training.cochrane.org/handbook (accessed on 1 November 2018).
- Stroup, D.F.; Berlin, J.A.; Morton, S.C.; Olkin, I.; Williamson, G.D.; Rennie, D.; Moher, D.; Becker, B.J.; Sipe, T.A.; Thacker, S.B.; et al. Meta-analysis of observational studies in epidemiology: A proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000, 283, 2008–2012. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gotzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. Ann. Intern. Med. 2009, 151, W65–W94. [Google Scholar] [CrossRef]
- Gianfredi, V.; Blandi, L.; Cacitti, S.; Minelli, M. Physical Activity and Depression: A Systematic Review and Meta-Analysis on the Association between Patterns of Objectively Measured Physical Activity and Risk of Depression in Adults. CRD42020132860, Prospero 2020. Available online: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020132860 (accessed on 29 April 2020).
- Amerio, A.; Stubbs, B.; Odone, A.; Tonna, M.; Marchesi, C.; Ghaemi, S.N. Bipolar I and II Disorders; A Systematic Review and Meta-Analysis on Differences in Comorbid Obsessive-Compulsive Disorder. Iran. J. Psychiatry Behav. Sci. 2016, 10, e3604. [Google Scholar] [CrossRef]
- Amerio, A.; Ossola, P.; Scagnelli, F.; Odone, A.; Allinovi, M.; Cavalli, A.; Iacopelli, J.; Tonna, M.; Marchesi, C.; Ghaemi, S.N. Safety and efficacy of lithium in children and adolescents: A systematic review in bipolar illness. Eur. Psychiatry 2018, 54, 85–97. [Google Scholar] [CrossRef]
- Brown, P.; Brunnhuber, K.; Chalkidou, K.; Chalmers, I.; Clarke, M.; Fenton, M.; Forbes, C.; Glanville, J.; Hicks, N.J.; Moody, J.; et al. How to formulate research recommendations. BMJ 2006, 333, 804–806. [Google Scholar] [CrossRef]
- Gianfredi, V.; Nucci, D.; Abalsamo, A.; Acito, M.; Villarini, M.; Moretti, M.; Realdon, S. Green Tea Consumption and Risk of Breast Cancer and Recurrence-A Systematic Review and Meta-Analysis of Observational Studies. Nutrients 2018, 10, 1886. [Google Scholar] [CrossRef]
- Gianfredi, V.; Bragazzi, N.L.; Nucci, D.; Villarini, M.; Moretti, M. Cardiovascular diseases and hard drinking waters: Implications from a systematic review with meta-analysis of case-control studies. J. Water Health 2017, 15, 31–40. [Google Scholar] [CrossRef]
- Gianfredi, V.; Nucci, D.; Fatigoni, C.; Salvatori, T.; Villarini, M.; Moretti, M. Extent of Primary DNA Damage Measured by the Comet Assay in Health Professionals Exposed to Antineoplastic Drugs: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2020, 17, 523. [Google Scholar] [CrossRef] [PubMed]
- Wells, G.A.; Shea, B.; O’Connell, D.; Paterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses. 2014. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 1 November 2018).
- Higgins, J.P.; Altman, D.G.; Gotzsche, P.C.; Juni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.; et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [PubMed]
- Begg, C.B.; Mazumdar, M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994, 50, 1088–1101. [Google Scholar] [CrossRef] [PubMed]
- Egger, M.; Davey Smith, G.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef]
- Abedi, P.; Nikkhah, P.; Najar, S. Effect of pedometer-based walking on depression, anxiety and insomnia among postmenopausal women. Climacteric 2015, 18, 841–845. [Google Scholar] [CrossRef]
- Al-Eisa, E.; Buragadda, S.; Melam, G.R. Association between physical activity and psychological status among Saudi female students. BMC Psychiatry 2014, 14, 238. [Google Scholar] [CrossRef]
- Alosco, M.L.; Spitznagel, M.B.; Miller, L.; Raz, N.; Cohen, R.; Sweet, L.H.; Colbert, L.H.; Josephson, R.; Waechter, D.; Hughes, J.; et al. Depression is associated with reduced physical activity in persons with heart failure. Health Psychol. 2012, 31, 754–762. [Google Scholar] [CrossRef]
- Altenburg, W.A.; Bossenbroek, L.; De Greef, M.H.; Kerstjens, H.A.; Ten Hacken, N.H.; Wempe, J.B. Functional and psychological variables both affect daily physical activity in COPD: A structural equations model. Respir. Med. 2013, 107, 1740–1747. [Google Scholar] [CrossRef]
- Arrieta, H.; Rezola-Pardo, C.; Echeverria, I.; Iturburu, M.; Gil, S.M.; Yanguas, J.J.; Irazusta, J.; Rodriguez-Larrad, A. Physical activity and fitness are associated with verbal memory, quality of life and depression among nursing home residents: Preliminary data of a randomized controlled trial. BMC Geriatr. 2018, 18, 80. [Google Scholar] [CrossRef]
- Bade, B.C.; Brooks, M.C.; Nietert, S.B.; Ulmer, A.; Thomas, D.D.; Nietert, P.J.; Scott, J.B.; Silvestri, G.A. Assessing the Correlation between Physical Activity and Quality of Life in Advanced Lung Cancer. Integr. Cancer Ther. 2018, 17, 73–79. [Google Scholar] [CrossRef]
- Barriga, S.; Rodrigues, F.; Barbara, C. Factors that influence physical activity in the daily life of male patients with chronic obstructive pulmonary disease. Rev. Port. Pneumol. 2014, 20, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Di Marco, F.; Terraneo, S.; Roggi, M.A.; Repossi, A.C.; Pellegrino, G.M.; Veronelli, A.; Santus, P.; Pontiroli, A.E.; Centanni, S. Physical activity impairment in depressed COPD subjects. Respir. Care 2014, 59, 726–734. [Google Scholar] [CrossRef] [PubMed]
- Dillon, C.B.; McMahon, E.; O’Regan, G.; Perry, I.J. Associations between physical behaviour patterns and levels of depressive symptoms, anxiety and well-being in middle-aged adults: A cross-sectional study using isotemporal substitution models. BMJ Open 2018, 8, e018978. [Google Scholar] [CrossRef] [PubMed]
- Drieling, R.L.; Goldman Rosas, L.; Ma, J.; Stafford, R.S. Community resource utilization, psychosocial health, and sociodemographic factors associated with diet and physical activity among low-income obese Latino immigrants. J. Acad. Nutr. Diet. 2014, 114, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Duenas-Espin, I.; Demeyer, H.; Gimeno-Santos, E.; Polkey, M.I.; Hopkinson, N.S.; Rabinovich, R.A.; Dobbels, F.; Karlsson, N.; Troosters, T.; Garcia-Aymerich, J. Depression symptoms reduce physical activity in COPD patients: A prospective multicenter study. Int. J. Chron. Obstruct. Pulmon. Dis. 2016, 11, 1287–1295. [Google Scholar] [CrossRef] [PubMed]
- Elbelt, U.; Ahnis, A.; Riedl, A.; Burkert, S.; Schuetz, T.; Ordemann, J.; Strasburger, C.J.; Klapp, B. F Associations of physical activity with depressiveness and coping in subjects with high-grade obesity aiming at bariatric surgery: A cross-sectional study. Biopsychosoc. Med. 2015, 9, 16. [Google Scholar] [CrossRef]
- Fenton, S.A.M.; Van Zanten, J.; Metsios, G.S.; Rouse, P.C.; Yu, C.A.; Kitas, G.D.; Dudaa, J.L. Autonomy support, light physical activity and psychological well-being in Rheumatoid Arthritis: A cross-sectional study. Ment. Health Phys. Act. 2018, 14, 11–18. [Google Scholar] [CrossRef]
- Freitas, P.D.; Silva, A.G.; Ferreira, P.G.; Silva, D.A.; Salge, J.M.; Carvalho-Pinto, R.M.; Cukier, A.; Brito, C.M.; Mancini, M.C.; Carvalho, C.R.F. Exercise Improves Physical Activity and Comorbidities in Obese Adults with Asthma. Med. Sci. Sports Exerc. 2018, 50, 1367–1376. [Google Scholar] [CrossRef]
- Gaskin, C.J.; Craike, M.; Mohebbi, M.; Salmon, J.; Courneya, K.S.; Broadbent, S.; Livingston, P.M. Associations of objectively measured moderate-to-vigorous physical activity and sedentary behavior with quality of life and psychological well-being in prostate cancer survivors. Cancer Causes Control. 2016, 27, 1093–1103. [Google Scholar] [CrossRef]
- Golsteijn, R.H.J.; Bolman, C.; Volders, E.; Peels, D.A.; De Vries, H.; Lechner, L. Short-term efficacy of a computer-tailored physical activity intervention for prostate and colorectal cancer patients and survivors: A randomized controlled trial. Int. J. Behav. Nutr. Phys. Act. 2018, 15, 106. [Google Scholar] [CrossRef]
- Hallam, K.T.; Bilsborough, S.; De Courten, M. “Happy feet”: Evaluating the benefits of a 100-day 10,000 step challenge on mental health and wellbeing. BMC Psychiatry 2018, 18, 19. [Google Scholar] [CrossRef] [PubMed]
- Hartescu, I.; Morgan, K.; Stevinson, C.D. Increased physical activity improves sleep and mood outcomes in inactive people with insomnia: A randomized controlled trial. J. Sleep Res. 2015, 24, 526–534. [Google Scholar] [CrossRef] [PubMed]
- Hospes, G.; Bossenbroek, L.; Ten Hacken, N.H.; Van Hengel, P.; De Greef, M.H. Enhancement of daily physical activity increases physical fitness of outclinic COPD patients: Results of an exercise counseling program. Patient Educ. Couns. 2009, 75, 274–278. [Google Scholar] [CrossRef]
- Howie, E.K.; McVeigh, J.A.; Winkler, E.A.H.; Healy, G.N.; Bucks, R.S.; Eastwood, P.R.; Straker, L.M. Correlates of physical activity and sedentary time in young adults: The Western Australian Pregnancy Cohort (Raine) Study. BMC Public Health 2018, 18, 916. [Google Scholar] [CrossRef] [PubMed]
- Jung, S.; Lee, S.; Lee, S.; Bae, S.; Imaoka, M.; Harada, K.; Shimada, H. Relationship between physical activity levels and depressive symptoms in community-dwelling older Japanese adults. Geriatr. Gerontol. Int. 2018, 18, 421–427. [Google Scholar] [CrossRef] [PubMed]
- Kangasniemi, A.; Lappalainen, R.; Kankaanpaa, A.; Tammelin, T. Mindfulness skills, psychological flexibility, and psychological symptoms among physically less active and active adults. Ment. Health Phys. Act. 2014, 7, 121–127. [Google Scholar] [CrossRef]
- King, W.C.; Kalarchian, M.A.; Steffen, K.J.; Wolfe, B.M.; Elder, K.A.; Mitchell, J.E. Associations between physical activity and mental health among bariatric surgical candidates. J. Psychosom. Res. 2013, 74, 161–169. [Google Scholar] [CrossRef]
- Po-Wen, K.; Steptoe, A.; Liao, Y.; Sun, W.J.; Chen, L.J. Prospective relationship between objectively measured light physical activity and depressive symptoms in later life. Int. J. Geriatr. Psychiatry 2018, 33, 58–65. [Google Scholar]
- Loprinzi, P.D.; Cardinal, B.J. Interrelationships among physical activity, depression, homocysteine, and metabolic syndrome with special considerations by sex. Prev Med. 2012, 54, 388–392. [Google Scholar] [CrossRef]
- Loprinzi, P.D.; Franz, C.; Hager, K.K. Accelerometer-assessed physical activity and depression among US adults with diabetes. Ment. Health Phys. Act. 2013, 6, 79–82. [Google Scholar] [CrossRef]
- Loprinzi, P.D. Objectively measured light and moderate-to-vigorous physical activity is associated with lower depression levels among older US adults. Aging Ment. Health 2013, 17, 801–805. [Google Scholar] [CrossRef] [PubMed]
- Ludwig, V.M.; Bayley, A.; Cook, D.G.; Stahl, D.; Treasure, J.L.; Asthworth, M.; Greenough, A.; Winkley, K.; Bornstein, S.R.; Ismail, K. Association between depressive symptoms and objectively measured daily step count in individuals at high risk of cardiovascular disease in South London, UK: A cross-sectional study. BMJ Open 2018, 8, e020942. [Google Scholar] [PubMed]
- Huong, N.Q.; Fan, V.S.; Herting, J.; Lee, J.; Fu, M.; Chen, Z.; Borson, S.; Kohen, R.; Matute-Bello, G.; Pagalilauan, G.; et al. Patients with COPD with higher levels of anxiety are more physically active. Chest 2013, 144, 145–151. [Google Scholar]
- O’Brien, J.T.; Gallagher, P.; Stow, D.; Hammerla, N.; Ploetz, T.; Firbank, M.; Ladha, C.; Ladha, K.; Jackson, D.; McNaney, R.; et al. A study of wrist-worn activity measurement as a potential real-world biomarker for late-life depression. Psychol. Med. 2017, 47, 93–102. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Thogersen-Ntoumani, C.; Ntoumanis, N.; Stenling, A.; Fenton, S.A.; Veldhuijzen van Zanten, J.J. Profiles of Physical Function, Physical Activity, and Sedentary Behavior and their Associations with Mental Health in Residents of Assisted Living Facilities. Appl. Psychol. Health Well Being 2017, 9, 60–80. [Google Scholar] [CrossRef] [PubMed]
- Raudsepp, L.; Riso, E.M. Longitudinal Association between Objectively Measured Walking and Depressive Symptoms among Estonian Older Adults. J. Aging Phys. Act. 2017, 25, 639–645. [Google Scholar] [CrossRef]
- Rethorst, C.D.; Moncrieft, A.E.; Gellman, M.D.; Arredondo, E.M.; Buelna, C.; Castaneda, S.F.; Daviglus, M.L.; Khan, U.I.; Perreira, K.M.; Sotres-Alvarez, D.; et al. Isotemporal Analysis of the Association of Objectively Measured Physical Activity with Depressive Symptoms: Results from Hispanic Community Health Study/Study of Latinos (HCHS/SOL). J. Phys. Act. Health 2017, 14, 733–739. [Google Scholar] [CrossRef]
- Song, M.R.; Lee, Y.S.; Baek, J.D.; Miller, M. Physical activity status in adults with depression in the National Health and Nutrition Examination Survey, 2005–2006. Public Health Nurs. 2012, 29, 208–217. [Google Scholar] [CrossRef]
- Sylvester, B.D.; Lee, Y.S.; Baek, J.D.; Miller, M. Changes in light-, moderate-, and vigorous-intensity physical activity and changes in depressive symptoms in breast cancer survivors: A prospective observational study. Support. Care Cancer 2017, 25, 3305–3312. [Google Scholar] [CrossRef]
- Trinh, L.; Amireault, S.; Lacombe, J.; Sabiston, C.M. Physical and psychological health among breast cancer survivors: Interactions with sedentary behavior and physical activity. Psychooncology 2015, 24, 1279–1285. [Google Scholar] [CrossRef]
- Vallance, J.K.; Winkler, E.A.; Gardiner, P.A.; Healy, G.N.; Lynch, B.M.; Owen, N. Associations of objectively-assessed physical activity and sedentary time with depression: NHANES (2005–2006). Prev. Med. 2011, 53, 284–288. [Google Scholar] [CrossRef] [PubMed]
- Vallance, J.K.; Boyle, T.; Courneya, K.S.; Lynch, B.M. Accelerometer-assessed physical activity and sedentary time among colon cancer survivors: Associations with psychological health outcomes. J. Cancer Surviv. 2015, 9, 404–411. [Google Scholar] [CrossRef] [PubMed]
- Van den Berg-Emons, R.; Balk, A.; Bussmann, H.; Stam, H. Does aerobic training lead to a more active lifestyle and improved quality of life in patients with chronic heart failure? Eur. J. Heart Fail 2004, 6, 95–100. [Google Scholar] [CrossRef] [PubMed]
- Whitaker, K.M.; Sharpe, P.A.; Wilcox, S.; Hutto, B.E. Depressive symptoms are associated with dietary intake but not physical activity among overweight and obese women from disadvantaged neighborhoods. Nutr. Res. 2014, 34, 294–301. [Google Scholar] [CrossRef]
- Vetrovsky, T.; Cupka, J.; Dudek, M.; Kuthanova, B.; Vetrovska, K.; Capek, V.; Bunc, V. A pedometer-based walking intervention with and without email counseling in general practice: A pilot randomized controlled trial. BMC Public Health 2018, 18, 635. [Google Scholar] [CrossRef]
- Romano-Spica, V.; Macini, P.; Fara, G.M.; Giammanco, G.; GSMS Working Group on Movement Sciences for Health Italian Society of Hygiene Preventive Medicine Public Health. Adapted Physical Activity for the Promotion of Health and the Prevention of Multifactorial Chronic Diseases: The Erice Charter. Ann. Ig 2015, 27, 406–414. [Google Scholar]
- Nebiker, L.; Lichtenstein, E.; Minghetti, A.; Zahner, L.; Gerber, M.; Faude, O.; Donath, L. Moderating Effects of Exercise Duration and Intensity in Neuromuscular vs. Endurance Exercise Interventions for the Treatment of Depression: A Meta-Analytical Review. Front. Psychiatry 2018, 9, 305. [Google Scholar] [CrossRef]
- Paolucci, E.M.; Loukov, D.; Bowdish, D.M.E.; Heisz, J.J. Exercise reduces depression and inflammation but intensity matters. Biol. Psychol. 2018, 133, 79–84. [Google Scholar] [CrossRef]
- Gianfredi, V.; Monarca, S.; Moretti, M.; Villarini, M. Health education, what is the role for pharmacist? Results from a cross sectional study in Umbria, Italy. Recent. Prog. Med. 2017, 108, 433–441. [Google Scholar]
- Gianfredi, V.; Grisci, C.; Nucci, D.; Parisi, V.; Moretti, M. Communication in health. Recent. Prog. Med. 2018, 109, 374–383. [Google Scholar]
- Gianfredi, V.; Balzarini, F.; Gola, M.; Mangano, S.; Carpagnano, L.F.; Colucci, M.E.; Gentile, L.; Piscitelli, A.; Quattrone, F.; Scuri, S.; et al. Leadership in Public Health: Opportunities for Young Generations within Scientific Associations and the Experience of the “Academy of Young Leaders”. Front. Public Health 2019, 7, 378. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Physical Activity. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/physical-activity (accessed on 2 April 2020).
- Huedo-Medina, T.B.; Sánchez-Meca, J.; Marín-Martínez, F.; Botella, J. Assessing heterogeneity in meta-analysis: Q statistic or I2 index? Psychol. Methods 2006, 11, 193–206. [Google Scholar] [CrossRef] [PubMed]
- Gianfredi, V.; Nucci, D.; Salvatori, T.; Dallagiacoma, G.; Fatigoni, C.; Moretti, M.; Realdon, S. Rectal Cancer: 20% Risk Reduction Thanks to Dietary Fibre Intake. Systematic Review and Meta-Analysis. Nutrients 2019, 11, 1579. [Google Scholar] [CrossRef] [PubMed]
| Search Strategy | Details |
|---|---|
| Inclusion criteria | P: adults (men and women) E: physical activity objectively measured O: Depressive disorder S: Trials, cohort studies, case-control, cross-sectional |
| Exclusion criteria | P: people < 18 years old E: physical activity not objectively measured (self-reported) O: other psychological disorders S: not original papers (opinion paper, review article, commentary, letter, protocols, article without quantitative data) |
| Language filter | English |
| Time filter | No filter (from inception) |
| Database | PubMed/Medline; EMBASE, Web of Science; Scopus, PsycoInfo, Cochrane |
| Author Year [Reference] | Country | Characteristics | Study Period | Age and Gender | Sample Size and Gender | Depressed Subjects | Attrition + | Device Used | Duration of Measurement | Tool Used for Depression Diagnosis | PA | Results | QS |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Cross-sectional studies | |||||||||||||
| Al-Eisa, 2014 [31] | Saudi Arabia | Female students | 2014 | Mean: 20.9 ± 1.4 y, F | 76 | 52% | 29 | Pedometer | 3 weeks | BDI-II | PA = 8715 steps/day | R = −0.78 p ≤ 0.01; | 4 |
| Alosco, 2012 [32] | USA | Persons with heart failure | n.a. | Mean: 68.81 ± 8.8 y, M, F | 96 (M = 63, 5%, F = 36, 5%) | n.a. | 27 | GT1M+ accelerometer (ActiGraph, Pensacola, Florida) | 7 days at baseline, 3 months, 12 months | BDI-II | MVPA = 3.24 ± 9.0 min/day | β = −64.35 p < 0.05 t = −2.32 | 6 |
| Altenburg, 2013 [33] | The Netherlands | Patients with stable chronic obstructive pulmonary disease (COPD) | n.a. | Mean: 62 (54–69) y M, F | 155 (M = 102, F = 53) | n.a. | 0 | Yamax-Digiwalker pedometer (SW-200) | 2 weeks | HADS | PA = 4206 (2387–6284) steps/day | R = −0.191 p < 0.05 | 4 |
| Arrieta, 2018 [34] | Spain | Partecipants from nursing home | October 2016–June 2017 | 84.9 ± 6.9 years | 114 (81 F, 33 M) | 25% (at risk of depression | 0 | Actigraph GT3X model | 7 days | GDS | MVPA = 0.9 ± 1.2 min/day | β = 1.142 p = 0.028 | 7 |
| Bade, 2018 [35] | USA | Lung Cancer Patients | 2014–2015 | Mean: 66 ± 7.75(SD) y (51–80) M, F | 30 (M = 20, F = 10) | n.a. | 43 | Accelerometer (Fitbit Zip) | 7 days | PHQ-9 | PA = 4877 ± 305 | R = −0.40 | 5 |
| Barriga, 2014 [36] | Portugal | COPD patients | n.a. | Mean: 67 ± 9.6 y, M | 55 (sex n.s.) | n.a. | 0 | Pedometer | Number of steps per day, on three consecutive days | HADS | PA = 4972.4 ± 2242.3 | R = −0.424 p < 0.01 | 3 |
| Di Marco, 2014 [37] | Italy | COPD patients | n.a. | Mean: 71 ± 6 y M, F | 70 (M = 52, F = 18); No Depression = 51 (18% F) | 19 (47% F) | 0 | Accelerometer (SenseWear Pro Armband, BodyMedia) | 5 days | HADS | No Depression PA = 6950 ± 2431 Depresed PA = 5055 ± 2576 | β = 0.106 p = 0.84 | 6 |
| Dillon, 2017 [38] | Ireland | Patients in the 50–69 year age group. | 2011 | Mean: 59.6 ± 5.5 y M, F | 397 (M = 182, F = 214) | 18.2% | 78 | Accelerometer (ActivInsights Ltd.) | 7 days | CESD-20 | Mean Light PA No Depression = 103 min/day Depressed = 105 min/day | β = −0.34 (95% CI = −0.64 to −0.04) | 7 |
| Drieling, 2014 [39] | USA | Obese latino immigrants | July 2009–September 2010 | n.a. | 207 (48 M, 159 F) | 36.7% | 0 | Pedometer | 7 days | CESD | 6.3 ± 3.1 steps/day in thousands | β = −0.02 SE 0.01 p = 0.03 | 6 |
| Elbelt, 2015 [41] | Germany | High grade obesity | 2008–2010 | Mean: 42 ± 12 y | 50 (10 M, 40 F) | 36% | 0 | Accelerometer | 3 days | PHQ-9 | No depressed: 6023 ± 2459 steps/day Depressed: 6532 ± 3085 steps/day | r = 0.023 | 7 |
| Fenton, 2017 [42] | England | Rheumatoid Arthritis patients | n.a. | Mean: 54.92 ± 12.39 y | 61 (F = 67.2%) | n.a. | 36 | Actigraph GT3X+, accelerometer (Pensacola, FL) | 7 days | HADS | LPA = 269.35 ± 69.35 min/day | β = −0.30 p < 0.05 | 10 |
| Gaskin, 2016 [44] | Australia | Prostate cancer survivors | n.a. | 65.6 ± 8.5 y | 98 (M) | n.a. | n.a. | ActiGraph GT1 M (Pensacola, FL) | 7 days | CESD | MVPA = 38 min/day | β = ·0.00 p = 0.97 | 10 |
| Howie, 2018 [49] | Australia | Subsample of the 22th follow-up measurement of the Raine cohort Study. | 2011 | n.a. | 475 (256 F, 219 M) | 1.3% | 299 | Actigraph GT3X+, accelerometer Pensacola, FL | 7 days | DASS-21 | MVPA F = 27 min/day M = 34.1 min/day | F: RR = 0.99 (95% CI = 0.98–1.00), p = 0.078 M: RR= 1.01 (95% CI = 0.99–1.02), p = 0.300 | 10 |
| Huong, 2013 [58] | USA | COPD patients | n.a. | Mean: 66.5 ± 8.8 y M, F | 148 (M = 115, F = 33) | 29% | 0 | Accelerometer Stepwatch 3 Activity Monitor (OrthoCare Innovations LLC) | 7 days | HADS | Mean = 6.079 ± 3718 | β = −0.19 p = 0.02) | 7 |
| Jung, 2018 [50] | Japan | Community-dwelling older Japanese adults. | 2013 | Mean: >75 y M, F | 3054 (M = 1491, F = 1563) | 598 | 2.203 | Accelerometer (GT40-020) | 7–40 days | GDS | No Depression = 5059.6 ± 53.7 steps/day Depressed = 5003.0 ± 112.1 steps/day | Coehns = 0.03 p = 0.359 | 7 |
| Kangasniemi, 2014 [51] | Finland | Adults, general population | 2011 | Mean 43 ± 5.2 y, | 108 (58 F, 50 M) | n.a. | 109 | ActiGraph-GT1M, accelerometer LLC, Pensacola, Florida | 7 days | BDI- II | Less Active: 24.3 ± 12.4 min/day More active: 62.7 ± 24.7 min/day | r = −0.24, (95% CI 0.38, 0.08) | 7 |
| King, 2014 [52] | USA | Adults with ≥class 2 obesity. | 2009 | Mean 45 (18–78) y | 850 (673 F, 177 M) | 31.8% | 3626 | StepWatch™ 3 Activity Monitor (OrthoCare Innovations, Washington, D.C.) | 7 days | BDI- II | PA ≥ 1000 steps/day Mean: 7321.0 steps/day | OR = 1.03 (95% CI 0.97–1.09)c | 7 |
| Loprinzi, 2012 [54] | USA | non-institutionalized U.S. civilians | 2005–2006 | 48.4 ± 0.8 y | 1146 (611 M) | 9.5% | n.a. | ActiGraph AM-7164, accelerometer Walton, Beach, FL. | 7 days | PHQ-9 | MVPA = 2020–5998 steps/min | M: OR 0.71 (95% CI 0.53–0.95) F:OR = 0.74 (95% CI 0.57–0.96) | 10 |
| Loprinzi 2013 (A) [55] | USA | non-institutionalized USA civilians | 2006 | Mean: 73.5 ± 0.2 y | 708 (57.2% M) | 14.9% | n.a. | ActiGraph AM-7164, accelerometer Walton, Beach, FL. | 7 days | PHQ-9 | MVPA = 10.0 ± 0.9 min/day | OR = 0.78 (95% CI 0.64–0.94) | 9 |
| Loprinzi, 2013 (B) [56] | USA | Diabetic non-institutionalized USA civilians | 2006 | Mean: 59.6 ± 1.2 y | 372 (51.4% F) | 3.1% | n.a. | ActiGraph AM-7164, accelerometer Walton, Beach, FL. | 7 days | PHQ-9 | MVPA = 12.2 ± 1.3 min/day | β = −0.03 (95% CI −0.05—−0.006) p < 0.05 | 10 |
| Ludwig, 2018 [57] | UK | UK residents | 2013–2015 | 69 ± 4.1 y | 1720 (M = 85.5%) | 4% | 20 | ActiGraph GT3X accelerometer (ActiGraph, Florida, USA) | 7 days | PHQ-9 | PA = 6151 steps/day | β = −0.170 p < 0.001 | 7 |
| Park, 2017 [60] | UK | Subjects living facilities across England | n.a. | 77.5 ± 8.2 y | 85 (M = 31.8%) | n.a. | 0 | GT3X+, WGT3X-BT; ActiGraph, Pensacola, FL, USA | n.a. | HADS | MVPA = 9.74 min/day | Χ2 = 8.45 p = 0.004 | 5 |
| Song, 2011 [64] | USA | community residents older than 20 years | 2006 | ≥20 y | 4058 (51.32% F) | 19.5% | 6290 | ActiGraph® AM-7164, accelerometer Walton, Beach, FL. | 7 days | PHQ-9 | MPA = 30 min daily and more than 3 days a week | OR = 0.72 (95% CI 0.54–0.97) p < 0.05 | 7 |
| Vallance JK, 2011 [66] | USA | non-institutionalized civilian US citizens | 2005–2006 | 45.7 ± 13.7 y | 2862 (1417 M) | 195 | n.a. | ActiGraph AM-7164, accelerometer Walton, Beach, FL. | 7 days | PHQ-9 | MVPA = 20.2 ± 0.2 min/day | OR = 0.37, (95% CI, 0.20 to 0.70) p < 0.01 | 9 |
| Vallance J.K, 2015 [67] | Canada | Colon cancer survivors | n.a. | Mean: 64.3 ± 10.3 y M, F | 180 (M = 99, F = 81) | 8.5% | 17 | Actigraph GT3X+ accelerometer | 7 days | PHQ-9 | non-extrapolatable | non-extrapolatable | 8 |
| Whitaker, 2014 [69] | USA | Overweight and obese women | n.a. | Mean: 38.3 ± 7.6 y | 196 (F) | n.a. | 34 | ActiGraph-GT1M, accelerometer LLC, Pensacola, Florida | 7 days | CESD-10 | MVPA ≥ 2400 steps/min | t = 0.30 p = 0.77 | 9 |
| Case-control studies | |||||||||||||
| O’Brien JT, 2016 [59] | UK | adults > 60yo | 2015 | 74 ± 6 y | 58 (43 F) | 29 | 0 | Accelerometer | 7 days | Montgomery–Åsberg Depression Rating Scale (MADRS); GDS-15 | 0.17 acceleration/min/day | r = −0.37 p ≤ 0.05 | 7 |
| Cohort studies | |||||||||||||
| Duenas-Espin, 2016 [40] | Europe (Athens, Leuven, London, Groningen). | COPD patients | July–November 2011 | M, F Mean: 67 ± 8y | 220 (149 M, 71 F) | 5% | n.a. | Accelerometer Dynaport MoveMonitor (McRoberts BV, The Hague, the Netherlands). | 7 days at baseline, 6 and 12 months | HADS hospital anxiety and depression scale) (depression>11 points) | 4812 ± 3147 steps/day | β = 0.6 (95% CI 0.5 to 0.8) p = 0.01 | 5 |
| Follow-up = 1 y | |||||||||||||
| Po-Wen, 2017 [53] | Taiwan | community-dwelling older adults | 2012–2014 | Mean: 74.5 y M, F | 285 (M = 125, F = 149) | n.a. | 11 | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 7 day at baseline | 15-item Geriatric Depression Scale | MVPA>1951 steps/min | RR: 0.88 95% CI (0.79–0.98) p = 0.021 | 8 |
| Follow-up = 2 y | |||||||||||||
| Raudsepp, 2017 [61] | Estonia | generally healthy community-dwelling individuals aged 67–74 years | 2011–2013 | 67–74 y M, F | 195 (M = 85, F = 110) | n.a. | 23 | Yamax-Digiwalker pedometer (SW-200-024) | 1 week each year, per 3 years | 15-Item Geriatric Depression Scale | 6394.5 daily walking steps | β = −0.17 Χ2 = 83.27 | 6 |
| Follow-up = 3 y | |||||||||||||
| Rethorst, 2017 [62] | USA | Hispanic/Latino men and women, age 18 to 74 years at time | 2008–2011 | Mean: 41.06 ± 0.25 y M, F | 16,415 (52.13% F) | n.a. | n.a. | Actical B-1 version accelerometer | 7 days at baseline | Center for Epidemiological Studies Depression Scale 10 | VPA≥3962 steps/min | β = −0.936 | 4 |
| Follow-up = 7 days | |||||||||||||
| Sylvester, 2017 [64] | Canada | Breast cancer women over 1 year post-treatment | n.a. | 55.01 ± 10.96 y | 201 F | n.a. | 0 | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 7 days every 3 months | 10-item Center for Epidemiologic Studies Depression Scale | MPA = 14.73 ± 11.6 min/day | β = −0.73; p = 0.03 | 8 |
| Follow-up = 1 y | |||||||||||||
| Trinh, 2015 [65] | Canada | Patients with breast cancer in stage I–III without metastatic disease | 2010–2012 | Mean: 55 ± 11 y F | 199 (F) | n.a. | 4 | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 7 days at baseline | CES-D10 | MVPA mean 107.1 ± 81.3 min/week) | β = −0.10 p = 0.19 | 4 |
| Follow-up = 7 days | |||||||||||||
| Trial studies | |||||||||||||
| Author Year | Country | Characteristics | Study Period | Age and Gender | Sample Size | Depressed Subjects | Attrition + | Device Used | Duration of Measurement | Tool Used for Depression Diagnosis | PA | Results | Follow-up |
| Abedi, 2015 [30] | Iran | Post-menopausal women | n.a. | n.a. | 106 F | n.a. | n.a. | Pedometer | 12 weeks | BDI-II | Before 76,377 steps/months; after: 106398/month | Intervention vs. control group 13.7 ± 5 vs. 19.6 ± 4.79 p < 0.001 | 12 weeks |
| Freitas, 2018 [43] | Brazil | Obese adults with asthma | n.a. | 30–60 y | 51 F | 58.8% | n.a | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 7 days | HADS | Training group (after): 10,000 steps/day Control group(after): ~8000 steps/day | r = 0.52 p < 0.01 | 3 months |
| Golsteijn, 2018 [45] | Holland | prostate and colorectal cancer patients survivors | 2015–2016 | 66.5 ± 7.1 y | 427 (M, F) | n.a. | na | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 7 days | HADS | MVPA > 3 MET MVPA = 271 ± 211 min/week | β = −0.64 p = 0.005 | 6 months |
| Hallam, 2018 [46] | India, Australia, and 21 other countries | General Population, of Stepathlon corporate challenge | 2015/16 | 16–74 y | 1963 (1458 M, 505 F) | n.a. | na | own personal pedometer, or activity monitoring device | 100 days | DASS | n.a. | r = − 0.026 p = 0.254 | 100 days |
| Hartescu I, 2015 [47] | UK | Inactive people with insomnia | 2014 | 59.8 ± 9.46 yo | 41 (30 F, 11 M) | n.a. | n.a. | ActiGraph GT3X-BT (ActiGraph, Pensacola, FL) | 6 months | BDI-II | Intervention group 66.50 ± 30.37 (min per week) | Cohen: 0.87 (0.19–1.56) | 6 months |
| Hospes G, 2009 [48] | Netherlands | COPD patients | 2008 | 63.1 ± 8.3 y | 35 (21 M) | n.a. | n.a. | Pedometer Digiwalker SW-2000 (Yamax; Tokyo, Japan) | 12 weeks | BDI-II | Intervention group Before 7087 ± 4058 After 7872 ± 3962 | β = 0.93 p = 0.01 | 12 weeks |
| van den Berg-Emons, 2004 [68] | Netherlands | Patients with stable chronic heart failure | n.a. | 58.6 ± 12.1 | 34 (25 M e 9 F) | n.a. | n.a. | Accelerometer (AM, Temec Instruments, Kerkrade | 48 h | HADS | Intervention group: 9.9% (of 24 h) Control group: 7.4% | Intervention group: 3.4(±4.0); Control group: 4.8 ± (3.1) | 3 months |
| Vetrovsky T, 2017 [70] | Czech Republic | inactive people from general population in primary care setting | 2015 | 41 ± 10 y | 23 (12 M, 11 F) | 0 at baseline | 0 | tri- axial pedometer (eVito 3D Step Counter SL; HMM Diagnostics GmbH, Dossenheim, Germany) | 7 days | HADS | After = +1676 | Mean difference = −2.4 [95% CI −3.7, −1.2] p = 0.001 | 3 months |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gianfredi, V.; Blandi, L.; Cacitti, S.; Minelli, M.; Signorelli, C.; Amerio, A.; Odone, A. Depression and Objectively Measured Physical Activity: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2020, 17, 3738. https://doi.org/10.3390/ijerph17103738
Gianfredi V, Blandi L, Cacitti S, Minelli M, Signorelli C, Amerio A, Odone A. Depression and Objectively Measured Physical Activity: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health. 2020; 17(10):3738. https://doi.org/10.3390/ijerph17103738
Chicago/Turabian StyleGianfredi, Vincenza, Lorenzo Blandi, Stefano Cacitti, Mirko Minelli, Carlo Signorelli, Andrea Amerio, and Anna Odone. 2020. "Depression and Objectively Measured Physical Activity: A Systematic Review and Meta-Analysis" International Journal of Environmental Research and Public Health 17, no. 10: 3738. https://doi.org/10.3390/ijerph17103738
APA StyleGianfredi, V., Blandi, L., Cacitti, S., Minelli, M., Signorelli, C., Amerio, A., & Odone, A. (2020). Depression and Objectively Measured Physical Activity: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 17(10), 3738. https://doi.org/10.3390/ijerph17103738







