Eating Habits and Their Association with Weight Status in Chinese School-Age Children: A Cross-Sectional Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample and Design
2.2. Data Collection
2.2.1. Questionnaires
2.2.2. Anthropometric Measurements
2.3. Statistical Analysis
3. Results
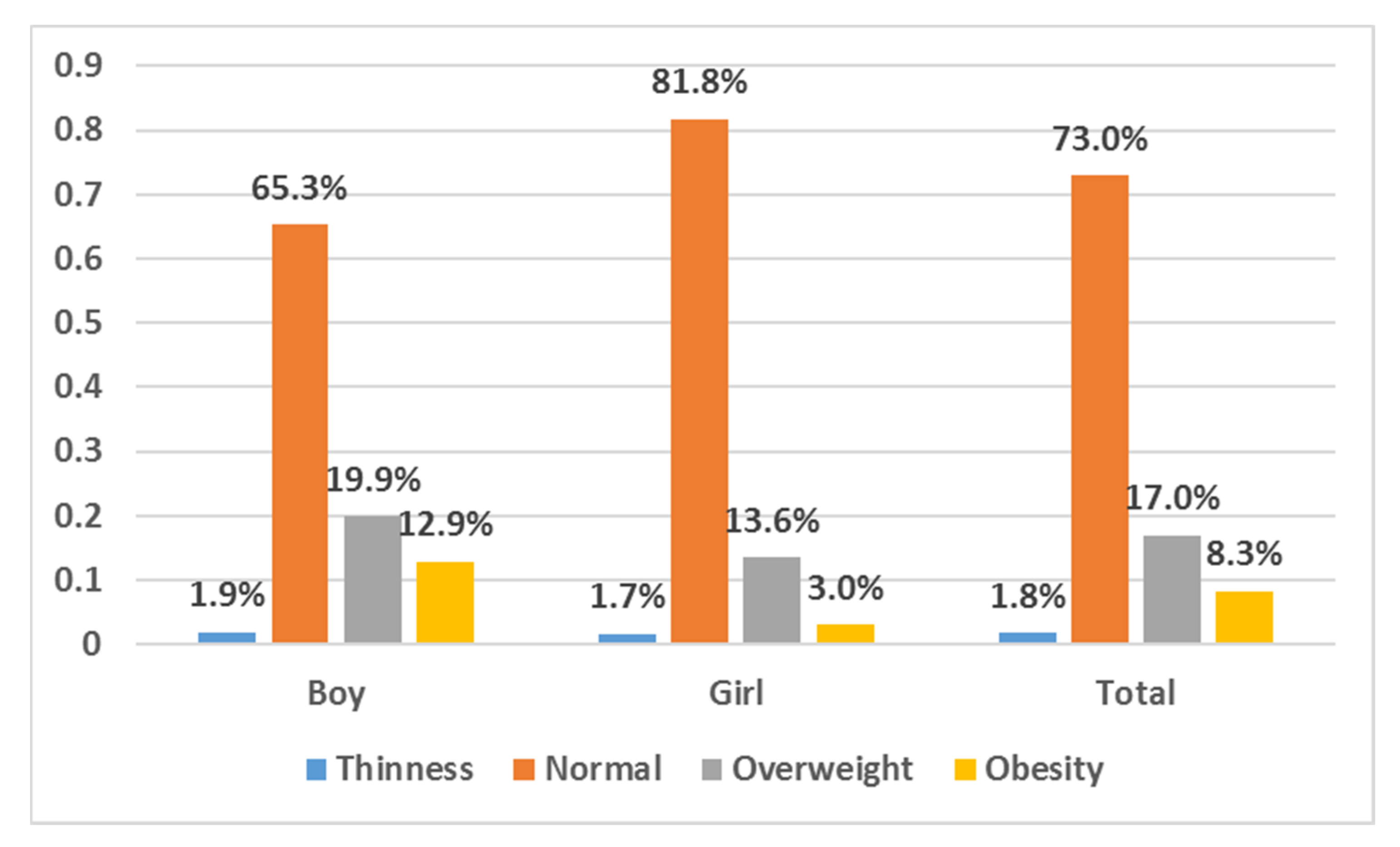
3.1. General Information of the Participants
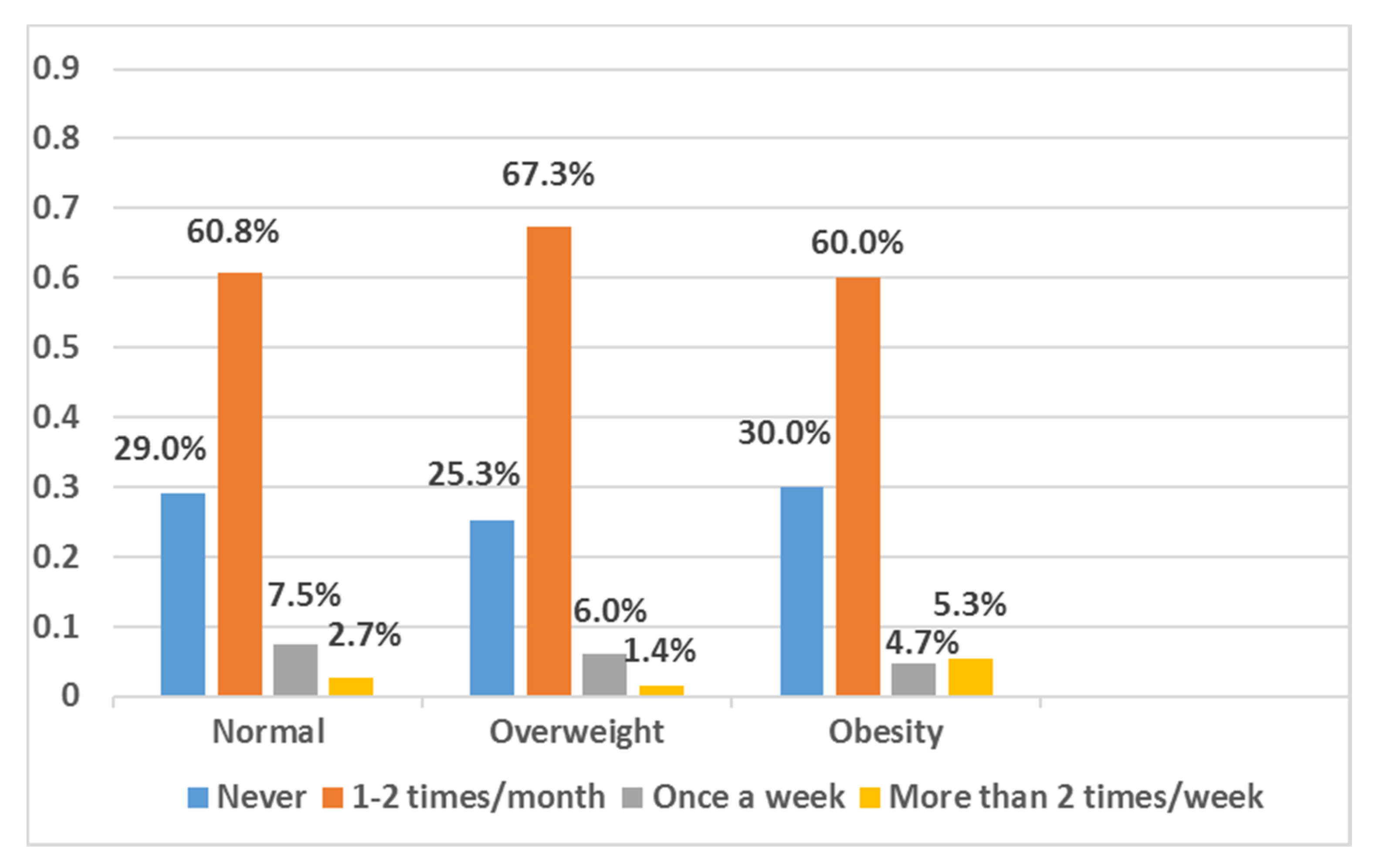
3.2. Eating Habits
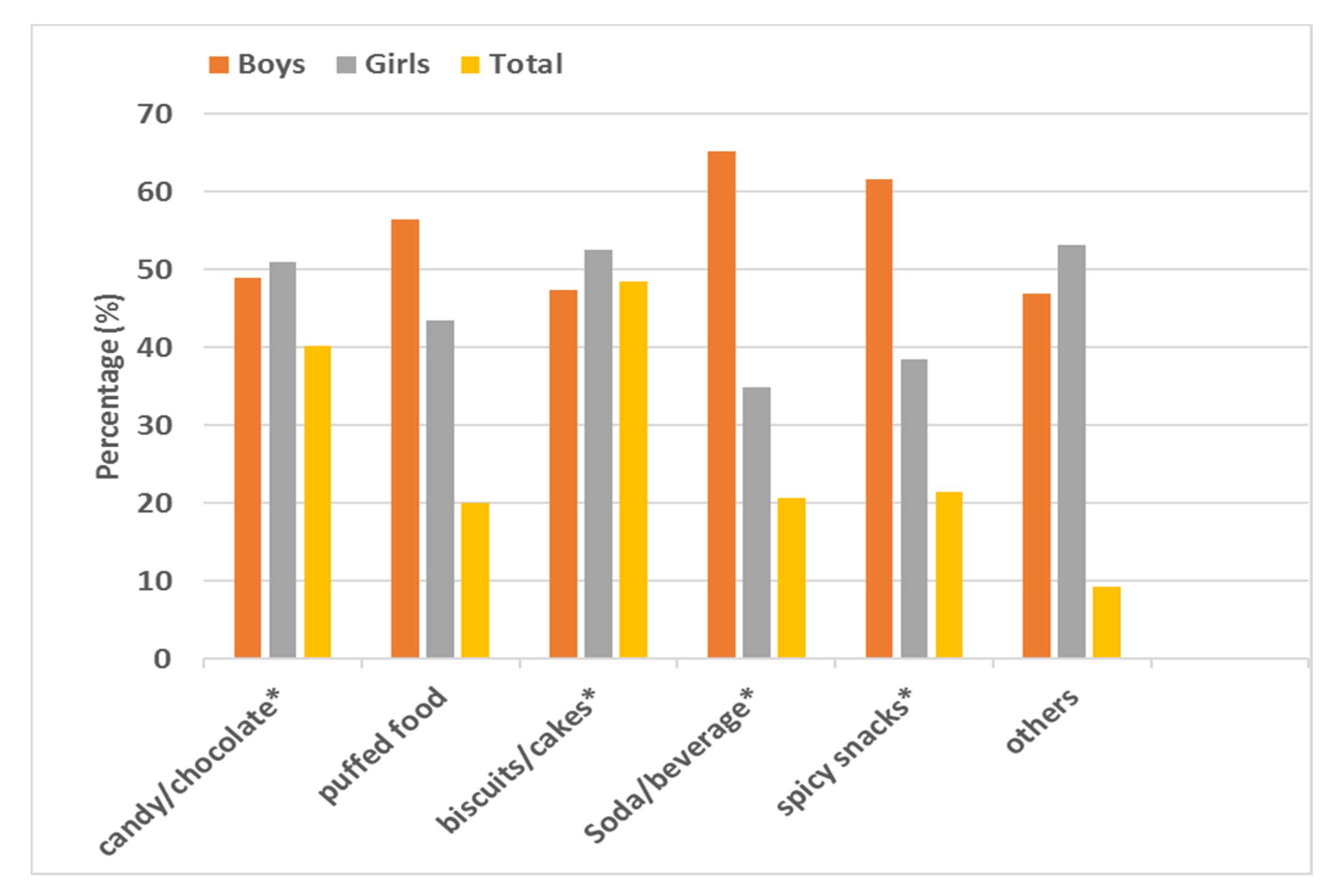
3.3. Types and Percentages of Snacks
3.4. Factors Related to Children’s Weight Status
4. Discussion
5. Strengths and Limitations
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| BMI | body mass index |
| RMB | renminbi |
| Cm | centimeters |
| Kg | kilograms |
References
- NCD Risk Factor Collaboration. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128.9 million children, adolescents, and adults. Lancet (London, England) 2017, 390, 2627–2642. [Google Scholar] [CrossRef]
- Qiuying, C.; Xianli, L.; Yiping, L. Research Progress of Obesity in Children and Adolescents. Drug Eval. 2019, 16, 3–6, 14. [Google Scholar]
- Yishan, C.; Yimin, Z.; Zhenxing, K.; Jingjing, Y.; Tingting, S.; Hanyue, Z. Survey on Prevalence of Overweight and Obesity among Children and Adolescents in China. Chin. J. Dis. Control 2017, 21, 866–869, 878. [Google Scholar]
- Wang, Y.; Beydoun, M.A.; Liang, L.; Caballero, B.; Kumanyika, S.K. Will all Americans become overweight or obese? estimating the progression and cost of the US obesity epidemic. Obesity (Silver Spring) 2008, 16, 2323–2330. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Wang, Q.; Venugopal, J.; Wang, J.; Kleiman, K.; Guo, C.; Eitzman, D.T. Obesity-induced Endothelial Dysfunction is Prevented by Neutrophil Extracellular Trap Inhibition. Sci. Rep. 2018, 8, 4881. [Google Scholar] [CrossRef] [PubMed]
- Skrypnik, D.; Mostowska, A.; Jagodzinski, P.P.; Bogdanski, P. Association of rs699947 (−2578 C/A) and rs2010963 (−634 G/C) Single Nucleotide Polymorphisms of the VEGF Gene, VEGF-A and Leptin Serum Level, and Cardiovascular Risk in Patients with Excess Body Mass: A Case-Control Study. J. Clin. Med. 2020, 9, 469. [Google Scholar] [CrossRef]
- Reilly, J.J.; Kelly, J. Long-term impact of overweight and obesity in childhood and adolescence on morbidity and premature mortality in adulthood: Systematic review. Int. J. Obes. 2011, 35, 891–898. [Google Scholar] [CrossRef]
- Guo, S.S.; Wu, W.; Chumlea, W.C.; Roche, A.F. Predicting overweight and obesity in adulthood from body mass index values in childhood and adolescence. Am. J. Clin. Nutr. 2002, 76, 653–658. [Google Scholar] [CrossRef]
- Skrypnik, D.; Bogdanski, P.; Zawiejska, A.; Wender-Ozegowska, E. Role of gestational weight gain, gestational diabetes, breastfeeding, and hypertension in mother-to-child obesity transmission. Pol. Arch. Intern. Med. 2019, 129, 267–275. [Google Scholar] [CrossRef]
- Karney, A.; Bragoszewska, H.; Soluch, L.; Oltarzewski, M. Risk factors for atherosclerosis in obese children aged 6–12 years. Dev. Period Med. 2017, 21, 259–265. [Google Scholar]
- Singh, R.K.; Kumar, P.; Mahalingam, K. Molecular genetics of human obesity: A comprehensive review. C. R. Biol. 2017, 340, 87–108. [Google Scholar] [CrossRef] [PubMed]
- Xuwei, Z. Clinical Intervention on Children’s Bad Dietary Behavior. J. Shandong Med. Coll. 2018, 40, 281–282. [Google Scholar]
- Stevenson, J. Dietary influences on cognitive development and behaviour in children. Proc. Nutr. Soc. 2006, 65, 361–365. [Google Scholar] [CrossRef] [PubMed]
- Kostecka, M. The influence of preschool children’s diets on the risk of lifestyle diseases. A pilot study. Rocz. Panstw. Zakl. Hig. 2018, 69, 139–145. [Google Scholar] [PubMed]
- Xianjun, Y.; Xun, J.; Yuhai, Z.; Lijun, S.; Changjun, W.; Lei, S. Development and Evaluation of Dietary Behavior Scale for Preschool Children. Chin. J. Child Health 2012, 20, 682–685. [Google Scholar]
- Ruonan, D.; Hongmei, X.; Yan, L.; Mingji, Y.; Guo, C. Study on the dietary behavior of children and adolescents in Chengdu and its relationship with overweight and obesity. J. Hyg. Res. 2015, 44, 576–580. [Google Scholar]
- Gadiraju, T.V.; Patel, Y.; Gaziano, J.M.; Djousse, L. Fried Food Consumption and Cardiovascular Health: A Review of Current Evidence. Nutrients 2015, 7, 8424–8430. [Google Scholar] [CrossRef]
- Shih, Y.H.; Chang, H.Y.; Wu, H.C.; Stanaway, F.F.; Pan, W.H. High sugar-sweetened beverage intake frequency is associated with smoking, irregular meal intake and higher serum uric acid in Taiwanese adolescents. J. Nutr. Sci. 2020, 9, e7. [Google Scholar] [CrossRef]
- Rodenbach, K.E.; Schneider, M.F.; Furth, S.L.; Moxey-Mims, M.M.; Mitsnefes, M.M.; Weaver, D.J.; Warady, B.A.; Schwartz, G.J. Hyperuricemia and Progression of CKD in Children and Adolescents: The Chronic Kidney Disease in Children (CKiD) Cohort Study. Am. J. Kidney Dis. 2015, 66, 984–992. [Google Scholar] [CrossRef]
- Yong, X.; Yun, C.; Ai, Z.; Peiyu, W.; Yumei, Z.; Zhishen, M. The influence of unhealthy dietary behavior on overweight and obesity in school children. J. Hyg. Res. 2014, 43, 764–767. [Google Scholar]
- Pesch, M.H.; Bauer, K.W.; Christoph, M.J.; Larson, N.; Neumark-Sztainer, D. Young adult nutrition and weight correlates of picky eating during childhood. Public Health Nutr. 2020, 23, 987–995. [Google Scholar] [CrossRef] [PubMed]
- De Onis, M.; Onyango, A.W.; Borghi, E.; Siyam, A.; Nishida, C.; Siekmann, J. Development of a WHO growth reference for school-aged children and adolescents. Bull. World Health Organ. 2007, 85, 660–667. [Google Scholar] [CrossRef] [PubMed]
- Shuo, W.; Yanhui, D.; Zhenghe, W.; Zhiyong, Z.; Jun, M. Epidemiological Trends of Overweight and Obesity among Students Aged 7–18 in China from 1985 to 2014. Chin. J. Prev. Med. 2017, 51, 300–305. [Google Scholar]
- Lingyi, W.; Hong, W.; Yao, T.; Peiyu, G.; Baocheng, Y.; Jing, G. Analysis of Overweight and Obesity Status and Dietary Behavioral Factors among Primary and Secondary School Students in Chongqing. School Health China 2016, 37, 194–196. [Google Scholar]
- Yuxin, B.; Ruonan, D.; Mingzhe, Y.; Yanrong, C.; Guo, T.; Jiao, L.; Guo, C. The Relationship between Meat, Fat and Fatty Acid Intake and Overweight and Obesity in Children and Adolescents in Chengdu. J. Sichuan Univ. 2017, 48, 96–100, 123. [Google Scholar]
- Lili, Y.; Bo, X. Prevalence of Overweight and Obesity among Children and Adolescents Aged 6–17 years in Urban Areas of Jinan. Chin. J. Child Health 2017, 25, 1108–1112. [Google Scholar]
- Lu, L. Investigation of Overweight and Obesity among Middle School Students in Changsha and Exploration of Intervention Measures. Master’s Thesis, Central South University, Changsha, China, 2007. [Google Scholar]
- Meiying, G.; Minjia, Y.; Hongwei, G.; Jian, Z.; Kun, X. Study on the correlation between overweight and obesity and dietary behavior in school-age children. J. Nutr. 2018, 40, 554–558. [Google Scholar]
- Cai, L.; Zhang, T.; Ma, J.; Ma, L.; Jing, J.; Chen, Y. Self-perception of weight status and its association with weight-related knowledge, attitudes, and behaviors among Chinese children in Guangzhou. J. Epidemiol. 2017, 27, 338–345. [Google Scholar] [CrossRef]
- Lu, C.; Stolk, R.P.; Sauer, P.J.; Sijtsma, A.; Wiersma, R.; Huang, G.; Corpeleijn, E. Factors of physical activity among Chinese children and adolescents: A systematic review. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 36. [Google Scholar] [CrossRef]
- Wei, L.; Rong, L.; Siyu, C.; Lihua, X.; Lin, L.; Chongshan, G.; Weijia, L. Prevalence of obesity and cognition of somatotype among primary school students of grade 3–5 in Guangzhou City. Chin. J. School Health 2017, 38, 190–192, 196. [Google Scholar]
- Jing, Z.; Juan, Z.; Jie, Y.; Yan, W.; Xiyan, Z.; Fengyun, Z. Current Situation and Influencing Factors of Overweight and Obesity among Children and Adolescents in Jiangsu Province. School Health China 2019, 40, 778–780. [Google Scholar]
- Min, J.; Xue, H.; Wang, V.H.C.; Li, M.; Wang, Y. Are single children more likely to be overweight or obese than those with siblings? The influence of China’s one-child policy on childhood obesity. Prev. Med. 2017, 103, 8–13. [Google Scholar] [CrossRef] [PubMed]
- Skrypnik, D.; Bogdanski, P.; Skrypnik, K.; Madry, E.; Karolkiewicz, J.; Szulinska, M.; Suliburska, J.; Walkowiak, J. Influence of endurance and endurance-strength training on mineral status in women with abdominal obesity: A randomized trial. Medicine 2019, 98, e14909. [Google Scholar] [CrossRef] [PubMed]
- Zhenmin, H. Carry out one hour of campus physical education every day to improve the physical health level of primary and secondary school students significantly. China School Phys. Educ. 2019, 5, 8–9. [Google Scholar]
- Bellisle, F. Effects of diet on behaviour and cognition in children. Br. J. Nutr. 2004, 92 (Suppl. 2), S227–S232. [Google Scholar] [CrossRef] [PubMed]
- Maynard, M.; Gunnell, D.; Emmett, P.; Frankel, S.; Daveysmith, G. Fruit, vegetables, and antioxidants in childhood and risk of adult cancer: The boyd orr cohort. J. Epidemiol. Community Health 2003, 57, 218–225. [Google Scholar] [CrossRef]
- Nurul-Fadhilah, A.; Teo, P.S.; Huybrechts, I.; Foo, L.H. Infrequent breakfast consumption is associated with higher body adiposity and abdominal obesity in Malaysian school-aged adolescents. PLoS ONE 2013, 8, e59297. [Google Scholar] [CrossRef]
- Smith, K.J.; Gall, S.L.; McNaughton, S.A.; Blizzard, L.; Dwyer, T.; Venn, A.J. Skipping breakfast: Longitudinal associations with cardiometabolic risk factors in the Childhood Determinants of Adult Health Study. Am. J. Clin. Nutr. 2010, 92, 1316–1325. [Google Scholar] [CrossRef]
- Guerreiro, S.; Alcada, M.; Azevedo, I. Sugary drinks and glycemia. Acta Med. Port. 2010, 23, 567–578. [Google Scholar]
- Popkin, B.M. Sugary beverages represent a threat to global health. Trends Endocrinol. Metab. 2012, 23, 591–593. [Google Scholar] [CrossRef]
- Fangyuan, J.; Yingjun, L.; Chunhong, F. Study on the Correlation between Sugary Beverage Consumption and Obesity in Chinese Children and Adolescents. Prev. Med. 2018, 30, 494–497, 501. [Google Scholar]
- Aburto, T.C.; Poti, J.M.; Popkin, B.M. Patterns and trends in the intake distribution of manufactured and homemade sugar-sweetened beverages in pre-tax Mexico, 1999–2012. Public Health Nutr. 2018, 21, 3296–3306. [Google Scholar] [CrossRef] [PubMed]
- Nicklas, T.A.; Yang, S.-J.; Baranowski, T.; Zakeri, I.; Berenson, G. Eating patterns and obesity in children. Am. J. Prev. Med. 2003, 25, 9–16. [Google Scholar] [CrossRef]
- Skinner, J.; Byun, R.; Blinkhorn, A.; Johnson, G. Sugary drink consumption and dental caries in New South Wales teenagers. Aust. Dent. J. 2015, 60, 169–175. [Google Scholar] [CrossRef]
- Chaput, J.P.; Tremblay, M.S.; Katzmarzyk, P.T.; Fogelholm, M.; Hu, G.; Maher, C.; Maia, J.; Olds, T.; Onywera, V.; Sarmiento, O.L.; et al. Sleep patterns and sugar-sweetened beverage consumption among children from around the world. Public Health Nutr. 2018, 21, 2385–2393. [Google Scholar] [CrossRef] [PubMed]
- Malik, V.S.; Pan, A.; Willett, W.C.; Hu, F.B. Sugar-sweetened beverages and weight gain in children and adults: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2013, 98, 1084–1102. [Google Scholar] [CrossRef]
- Deren, K.; Weghuber, D.; Caroli, M.; Koletzko, B.; Thivel, D.; Frelut, M.L.; Socha, P.; Grossman, Z.; Hadjipanayis, A.; Wyszynska, J.; et al. Consumption of Sugar-Sweetened Beverages in Paediatric Age: A Position Paper of the European Academy of Paediatrics and the European Childhood Obesity Group. Ann. Nutr. Metab. 2019, 74, 296–302. [Google Scholar] [CrossRef]
- Liang, T.; Kuhle, S.; Veugelers, P.J. Nutrition and body weights of Canadian children watching television and eating while watching television. Public Health Nutr. 2009, 12, 2457–2463. [Google Scholar] [CrossRef]
- Avery, A.; Anderson, C.; McCullough, F. Associations between children’s diet quality and watching television during meal or snack consumption: A systematic review. Matern. Child Nutr. 2017, 13, e12428. [Google Scholar] [CrossRef]
- Samuel, T.M.; Musa-Veloso, K.; Ho, M.; Venditti, C.; Shahkhalili-Dulloo, Y. A Narrative Review of Childhood Picky Eating and Its Relationship to Food Intakes, Nutritional Status, and Growth. Nutrients 2018, 10, 1992. [Google Scholar] [CrossRef]
- Finistrella, V.; Manco, M.; Ferrara, A.; Rustico, C.; Presaghi, F.; Morino, G. Cross-sectional exploration of maternal reports of food neophobia and pickiness in preschooler-mother dyads. J. Am. Coll. Nutr. 2012, 31, 152–159. [Google Scholar] [CrossRef] [PubMed]
- Taylor, C.M.; Emmett, P.M. Picky eating in children: Causes and consequences. Proc. Nutr. Soc. 2019, 78, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Guansheng, M.; Xiaoqi, H.; Wenjun, M.; Jin, W. A Survey on the Dietary Behavior of Children and Adolescents in Four Cities of China. Food Nutr. China 2001, 1, 16–18. [Google Scholar]
- Jing, L.; Guo, Z.; Xuan, D.; Min, F.; Gaiping, C.; Hongxia, G. Study on Snacking Behavior of School-age Children in Chengdu. School Health China 2008, 10, 893–894, 897. [Google Scholar]
- Bellisle, F. Meals and snacking, diet quality and energy balance. Physiol. Behav. 2014, 134, 38–43. [Google Scholar] [CrossRef]
- Tripicchio, G.L.; Kachurak, A.; Davey, A.; Bailey, R.L.; Dabritz, L.J.; Fisher, J.O. Associations between Snacking and Weight Status among Adolescents 12–19 Years in the United States. Nutrients 2019, 11, 1486. [Google Scholar] [CrossRef]
- Wang, D.; van der Horst, K.; Jacquier, E.; Eldridge, A.L. Snacking Among US Children: Patterns Differ by Time of Day. J. Nutr. Educ. Behav. 2016, 48, 369–375.e1. [Google Scholar] [CrossRef]
- Kerr, M.A.; Rennie, K.L.; McCaffrey, T.A.; Wallace, J.M.; Hannon-Fletcher, M.P.; Livingstone, M.B. Snacking patterns among adolescents: A comparison of type, frequency and portion size between Britain in 1997 and Northern Ireland in 2005. Br. J. Nutr. 2009, 101, 122–131. [Google Scholar] [CrossRef]
- Samuelson, G. Dietary habits and nutritional status in adolescents over Europe. An overview of current studies in the Nordic countries. Eur. J. Clin. Nutr. 2000, 54 (Suppl. 1), S21–S28. [Google Scholar] [CrossRef]
- Ailing, L.; Yifan, D.; Xiaoqi, H.; Shurong, Z.; Aiping, Q.; Guansheng, M. An Analysis of the Ten-Year Change of Snack Consumption Behavior of Urban Children. School Health China 2011, 32, 1415–1417. [Google Scholar]
| N | Normal | Overweight/Obesity | p-Value | |
|---|---|---|---|---|
| n, % | n, % | |||
| All | 1174 | 767 (65.3) | 385 (32.8) | |
| Age (y) | 0.043 | |||
| 7~9 | 262 | 185 (70.6) | 73 (27.9) | |
| 10~12 | 902 | 574 (63.6) | 311(34.5) | |
| 13~15 | 10 | 8 (80.8) | 4 (10.0) | |
| Only child # | 0.011 | |||
| Yes | 708 | 442 (62.4) | 253 (35.7) | |
| No | 404 | 287 (71.0) | 109 (27.0) | |
| Single-parent family # | 0.177 | |||
| Yes | 113 | 70 (61.9) | 43 (38.1) | |
| No | 1004 | 656 (65.3) | 327 (32.6) | |
| Living area | <0.001 | |||
| Urban | 749 | 451 (60.2) | 292 (39.0) | |
| Town | 425 | 316 (74.4) | 93 (21.9) | |
| Attended boarding school # | <0.001 | |||
| Yes | 84 | 64 (76.2) | 14 (16.7) | |
| No | 1029 | 658 (63.9) | 355 (34.5) | |
| Snack cost (RMB) # | 0.155 | |||
| <5 | 713 | 480 (67.3) | 221 (31.0) | |
| ≥5 | 409 | 252 (61.6) | 149 (36.4) | |
| Physical activity duration per day (hour) # | 0.010 | |||
| ≥1 | 624 | 384 (61.5) | 228 (36.5) | |
| <1 | 522 | 365 (69.9) | 147 (28.2) | |
| N | Normal | Overweight/Obesity | p-Value | |
|---|---|---|---|---|
| n, % | n, % | |||
| All | 1011 | 827 (81.8) | 167 (16.5) | |
| Age (y) | 0.102 | |||
| 7~9 | 270 | 224 (83.0) | 43 (15.9) | |
| 10~12 | 732 | 598 (81.7) | 121 (16.5) | |
| 13~15 | 9 | 5 (55.6) | 3 (33.3) | |
| Only child # | 0.001 | |||
| Yes | 495 | 390 (78.8) | 100 (20.2) | |
| No | 486 | 414 (85.2) | 60 (12.3) | |
| Single-parent family # | 0.094 | |||
| Yes | 75 | 55 (73.3) | 19 (25.3) | |
| No | 913 | 755 (82.7) | 143 (15.7) | |
| Living area | 0.001 | |||
| Urban | 669 | 532 (79.5) | 129 (19.3) | |
| Town | 342 | 295 (86.3) | 38 (11.1) | |
| Attended boarding school # | 0.988 | |||
| Yes | 49 | 40 (81.6) | 8 (16.3) | |
| No | 916 | 748 (81.7) | 152 (16.6) | |
| Snack cost (RMB) # | 0.140 | |||
| <5 | 678 | 573 (70.0) | 105 (15.5) | |
| ≥5 | 300 | 243 (81.0) | 55 (18.3) | |
| Physical activity duration per day (hour) # | 0.521 | |||
| ≥1 | 457 | 371 (81.2) | 76 (16.6) | |
| <1 | 533 | 442 (82.9) | 84 (15.8) | |
| Normal | Overweight/Obesity | Total | p-Value | |
|---|---|---|---|---|
| (n = 1633) | (n = 552) | (n = 2185) | ||
| Skip breakfast # | 0.032 | |||
| Every day | 10 (55.6) | 8 (44.4) | 18 (0.8) | |
| 1–2 times/week | 88 (72.7) | 31 (25.6) | 121 (5.6) | |
| 3–4 times/week | 78 (62.4) | 43 (34.4) | 125 (5.8) | |
| 5–6 times/week | 126 (67.4) | 56 (29.9) | 187 (8.6) | |
| Never | 1285 (74.6) | 409 (23.8) | 1722 (79.2) | |
| Eat out # | 0.129 | |||
| ≥2 times/week | 490 (74.9) | 149 (22.8) | 654 (30.5) | |
| Once a week or less | 1074 (72.2) | 391 (26.3) | 1488 (69.5) | |
| What to choose to quench their thirst # | 0.039 | |||
| Carbonated drinks (coke, sprite, etc.) | 95 (69.3) | 37 (27.0) | 137 (6.4) | |
| Mineral water | 164 (64.3) | 86 (33.7) | 255 (12.0) | |
| Fruit juice | 108 (74.0) | 35 (24.0) | 146 (6.8) | |
| Tea drinks | 89 (76.1) | 26 (22.2) | 117 (5.5) | |
| Plain boiled water | 1105 (74.8) | 348 (23.6) | 1477 (69.3) | |
| Eat while watching television # | 0.112 | |||
| Often | 154 (67.0) | 74 (32.2) | 230 (10.7) | |
| Occasionally | 958 (73.7) | 316 (24.3) | 1300 (60.3) | |
| Never | 460 (73.4) | 156 (24.9) | 627 (29.1) | |
| Picky eaters # | <0.001 | |||
| Never | 391 (65.5) | 198 (33.2) | 597 (28.4) | |
| Occasionally | 1053 (76.1) | 307 (22.2) | 1384 (65.7) | |
| Often | 98 (79.0) | 22 (17.7) | 124 (5.9) | |
| Eating speed # | 0.141 | |||
| ≤10 min | 284 (70.8) | 113 (28.2) | 401 (18.7) | |
| >10 min | 1286 (73.5) | 428 (24.5) | 1749 (81.3) | |
| Frequency of eating fast food (KFC, McDonalds, etc.) # | 0.583 | |||
| Never | 441 (74.6) | 140 (23.7) | 591 (28.5) | |
| 1–2 times/month | 923 (71.9) | 339 (26.4) | 1283 (61.9) | |
| Once a week | 114 (79.2) | 29 (20.1) | 144 (6.9) | |
| More than 2 times/week | 41 (73.2) | 14 (25.0) | 56 (2.7) | |
| Have late-night snacks # | 0.685 | |||
| Never | 678 (71.1) | 257 (27.0) | 953 (44.9) | |
| Occasionally | 829 (74.1) | 270 (24.1) | 1119 (52.7) | |
| Often | 38 (73.1) | 13 (25.0) | 52 (2.4) | |
| Eating meals at irregular times # | 0.782 | |||
| Yes | 849 (73.1) | 289 (24.9) | 1161 (53.8) | |
| No | 729 (73.0) | 254 (25.4) | 999 (46.3) | |
| Variables | Reference Group | Adjusted OR (95% CI) | p-Value |
|---|---|---|---|
| Boys | Girls | 2.913 (2.239~3.790) | 0.000 |
| Urban | Town | 1.958 (1.465~2.618) | 0.000 |
| Only child | No | 1.370 (1.055~1.781) | 0.018 |
| Snack cost < 5 RMB/day | ≥5 RMB | 0.714 (0.548~0.932) | 0.013 |
| Skip breakfast | No | 1.507 (1.116~2.035) | 0.007 |
| Picky eaters | No | 0.559 (0.427~0.733) | 0.000 |
| Eat puffed food ≥ 3 times/week | No | 1.571 (1.170~2.110) | 0.003 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sun, M.; Hu, X.; Li, F.; Deng, J.; Shi, J.; Lin, Q. Eating Habits and Their Association with Weight Status in Chinese School-Age Children: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2020, 17, 3571. https://doi.org/10.3390/ijerph17103571
Sun M, Hu X, Li F, Deng J, Shi J, Lin Q. Eating Habits and Their Association with Weight Status in Chinese School-Age Children: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2020; 17(10):3571. https://doi.org/10.3390/ijerph17103571
Chicago/Turabian StyleSun, Minghui, Xiangying Hu, Fang Li, Jing Deng, Jingcheng Shi, and Qian Lin. 2020. "Eating Habits and Their Association with Weight Status in Chinese School-Age Children: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 17, no. 10: 3571. https://doi.org/10.3390/ijerph17103571
APA StyleSun, M., Hu, X., Li, F., Deng, J., Shi, J., & Lin, Q. (2020). Eating Habits and Their Association with Weight Status in Chinese School-Age Children: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 17(10), 3571. https://doi.org/10.3390/ijerph17103571






