Perceived Health Impacts of Watershed Development Projects in Southern India: A Qualitative Study
Abstract
1. Introduction
2. Materials and Methods
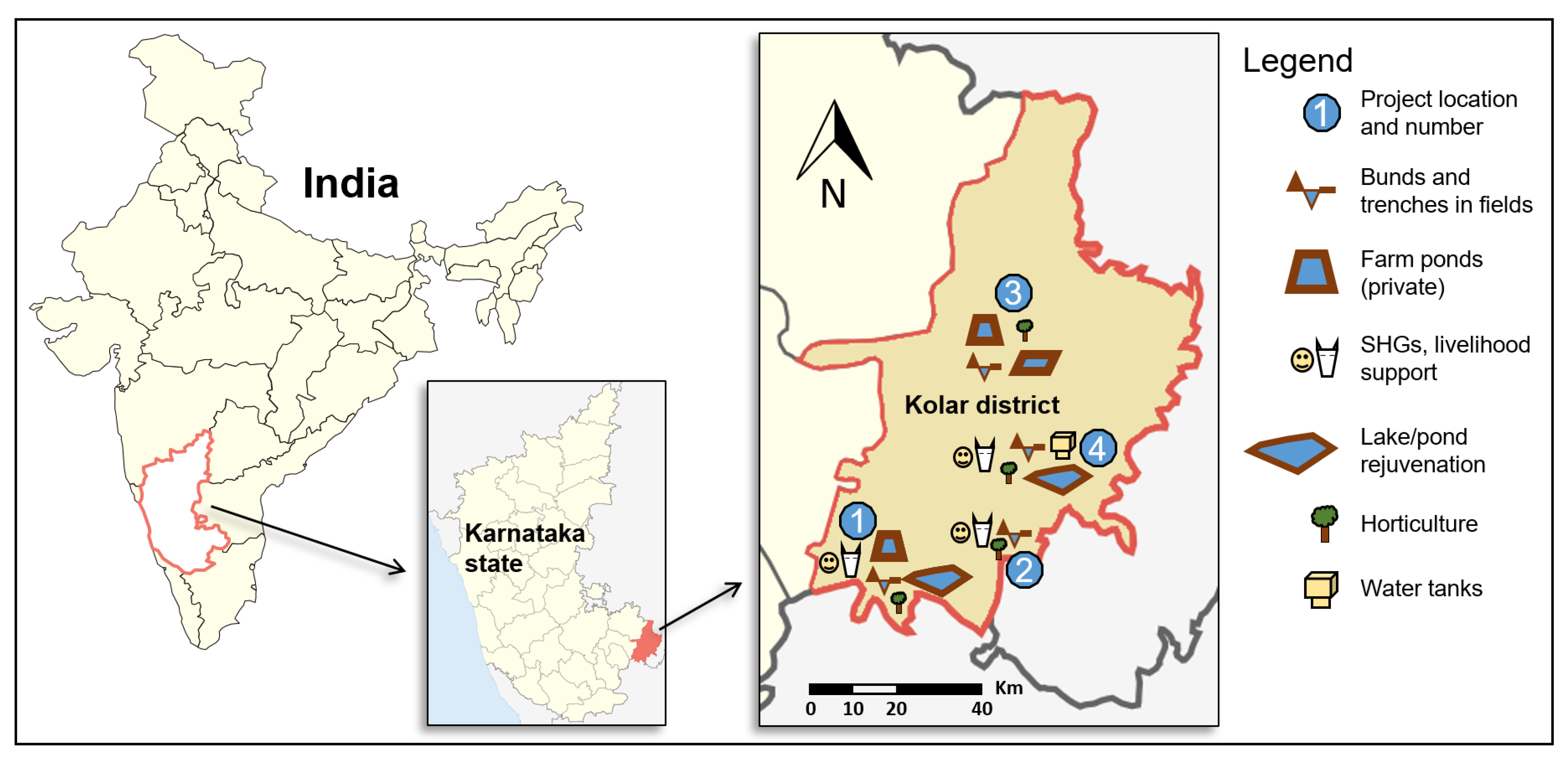
2.1. Design and Study Setting
2.2. Data Collection
2.3. Data Management and Analysis
2.4. Ethical Considerations
3. Results
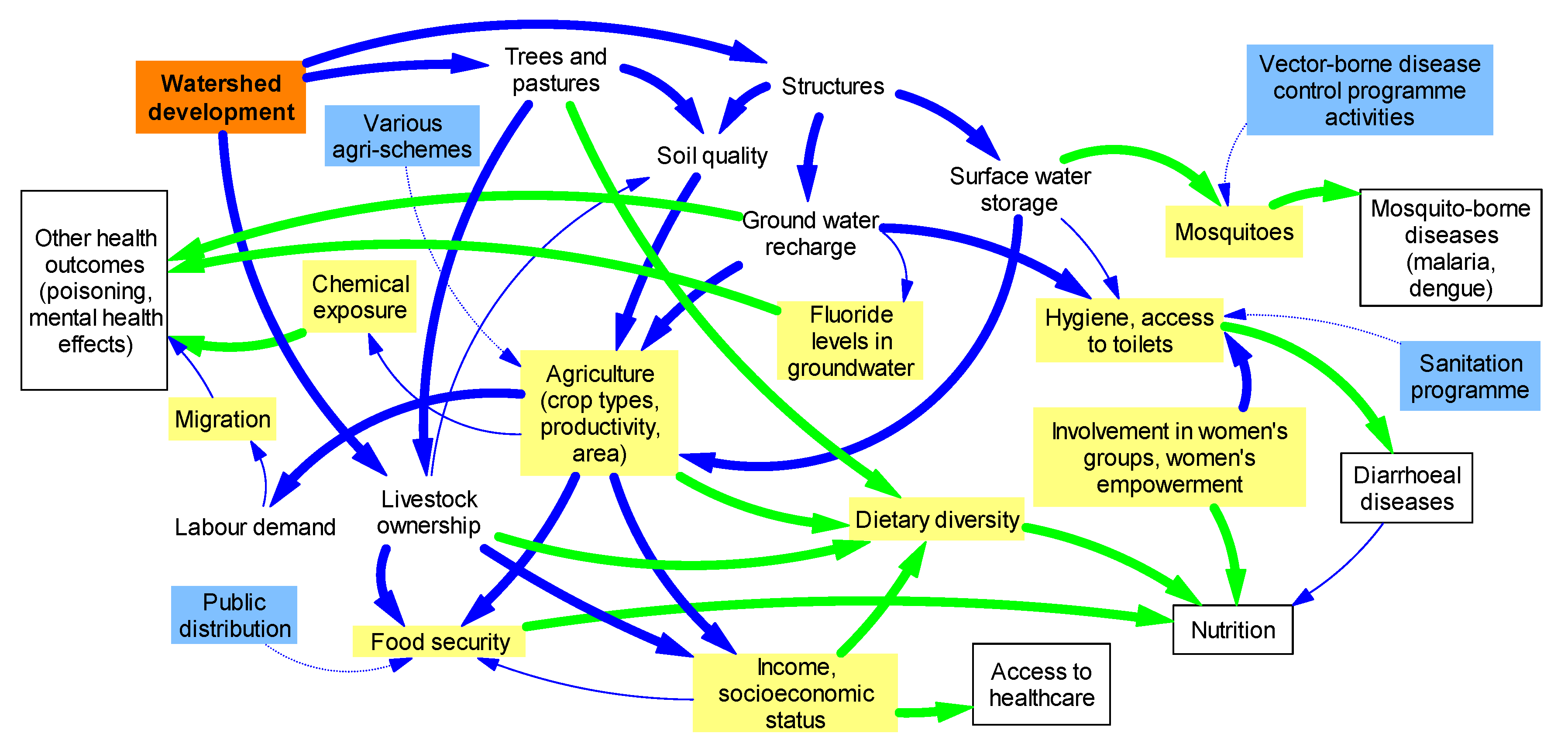
3.1. Pathways towards Nutritional Impacts
3.1.1. Direct Impacts on Food Security and Nutrition
“For home use, we grow finger millet surely, and pigeon peas and flat beans. If we ignore that, and plant other crops in those lands and don’t get returns…it will be difficult.”(land-owning male, GC, 35 years)
3.1.2. Income-Mediated Impacts on Food Security and Nutrition
“I had bought one (cow), and eventually bought four. Now I have two, but have kept 20 sheep too. I didn’t have cows or sheep earlier. I only worked for daily wage.”(landless female, ST, 37 years)
“They gave us Rs. 7,000…told us to buy a goat and grow the money...but we didn’t …we just used it for our regular expenses.”(landless female, SC, 68 years)
“We put bunds in 10 acres of mango plantation. I was not getting good yield earlier. Once it rained next year, the water was held in the soil in my field and the plants developed well. We got 5 tonnes earlier, then we got 10–15 tonnes and now we get even up to 25 tonnes.”(land-owning male, GC, 63 years)
3.2. Impacts on Disease Vector Ecology
“They can use carpio, which is edible and can grow to 600–700 g and is a protein source, and use gambusia along with that.”(Health academician 1)
3.3. Health Impacts of Opportunistic Activities during WSD Projects
“We bought it (gas connection) through the SHG itself. Earlier we used firewood. When it rained, we couldn’t cook. The kerosene stove was also difficult to use. Now it is much better.”(landless female, ST, 37 years)
4. Discussion
4.1. Size and Distribution of Impacts of WSD Projects
4.2. Interpreting Nutritional Impacts
4.3. Interpreting Other Health Impacts
4.4. Challenges in Eliciting Health Impacts
4.5. Strengths of the Study
4.6. Limitations, and Scope for Further Research
4.7. Future Action
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Government of India. Agricultural Statistics at a Glance 2018; Government of India: New Delhi, India, 2019.
- Government of India. Drought Management Plan; Government of India: New Delhi, India, 2017.
- Reddy, V.R. Land degradation in India: Extent, costs and determinants. Econ. Polit. Wkly. 2003, 38, 4700–4713. [Google Scholar]
- Arya, A.S.; Dhinwa, P.S.; Pathan, S.K.; Raj, K.G. Desertification/land degradation status mapping of India. Curr. Sci. 2009, 97, 1478–1483. [Google Scholar]
- Shiferaw, B.; Reddy, V.R.; Wani, S.P. Watershed externalities, shifting cropping patterns and groundwater depletion in Indian semi-arid villages: The effect of alternative water pricing policies. Ecol. Econ. 2008, 67, 327–340. [Google Scholar] [CrossRef]
- Hijioka, Y.; Lin, E.; Pereira, J.J.; Corlett, R.T.; Cui, X.; Insarov, G.E.; Lasco, R.D.; Lindgren, E.; Surjan, A. Asia. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part B: Regional Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Barros, V.R., Field, C.B., Dokken, D.J., Mastrandrea, M.D., Mach, K.J., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 1327–1370. [Google Scholar]
- O’Brien, K.; Leichenko, R.; Kelkar, U.; Venema, H.; Aandahl, G.; Tompkins, H.; Javed, A.; Bhadwal, S.; Barg, S.; Nygaard, L. Mapping vulnerability to multiple stressors: Climate change and globalization in India. Glob. Environ. Chang. 2004, 14, 303–313. [Google Scholar] [CrossRef]
- INCCA. Climate Change and India: A 4X4 Assessment; Government of India: New Delhi, India, 2010.
- Panda, A. Vulnerability to climate variability and drought among small and marginal farmers: A case study in Odisha, India. Clim. Dev. 2017, 9, 605–617. [Google Scholar] [CrossRef]
- IISc. Transitioning Towards Climate Resilient Development in Karnataka—Summary for Policy Makers; Indian Institute of Science: Bengaluru, India, 2014. [Google Scholar]
- Integrated Wasteland Development Programme. Available online: https://dolr.gov.in/integrated-wasteland-development-programme (accessed on 21 April 2020).
- Meenakshi, A.K.; Ramanathan, S. Evaluation of Watershed Programmes and LEISA; MYRADA: Bengaluru, India, 2010. [Google Scholar]
- Government of India. Common Guidelines for Watershed Development Projects—2008 (Revised 2011); Government of India: New Delhi, India, 2011.
- Lele, S.; Latha, G.M.; Badiger, S.; Vadivelu, A. Watershed Development in Karnataka: A Large-Scale Assessment of Processes, Sustainability and Impacts; Centre for Interdisciplinary Studies in Environment and Development: Bengaluru, India, 2007. [Google Scholar]
- Bunch, M.J.; Parkes, M.; Zubrycki, K.; Venema, H.; Hallstrom, L.; Neudorffer, C.; Berbés-Blázquez, M.; Morrison, K. Watershed management and public health: An exploration of the intersection of two fields as reported in the literature from 2000 to 2010. Environ. Manag. 2014, 54, 240–254. [Google Scholar] [CrossRef]
- Kolok, A.S.; Beseler, C.L.; Chen, X.-H.; Shea, P.J. The watershed as a conceptual framework for the study of environmental and human health. Environ. Health Insights 2009, 3, EHI.S1925. [Google Scholar] [CrossRef]
- Jordan, S.J.; Benson, W.H. Sustainable watersheds: Integrating ecosystem services and public health. Environ. Health Insights 2015, 9, EHI.S19586. [Google Scholar] [CrossRef]
- Herrera, D.; Ellis, A.; Fisher, B.; Golden, C.D.; Johnson, K.; Mulligan, M.; Pfaff, A.; Treuer, T.; Ricketts, T.H. Upstream watershed condition predicts rural children’s health across 35 developing countries. Nat. Commun. 2017, 8, 811. [Google Scholar] [CrossRef]
- Davies, J.-M.; Mazumder, A. Health and environmental policy issues in Canada: The role of watershed management in sustaining clean drinking water quality at surface sources. J. Environ. Manag. 2003, 68, 273–286. [Google Scholar] [CrossRef]
- Schmidt, P.J.; Pintar, K.D.M.; Fazil, A.M.; Flemming, C.A.; Lanthier, M.; Laprade, N.; Sunohara, M.D.; Simhon, A.; Thomas, J.L.; Topp, E.; et al. Using Campylobacter spp. and Escherichia coli data and Bayesian microbial risk assessment to examine public health risks in agricultural watersheds under tile drainage management. Water Res. 2013, 47, 3255–3272. [Google Scholar] [CrossRef] [PubMed]
- Wolka, K.; Moges, A.; Yimer, F. Farmers’ perception of the effects of soil and water conservation structures on crop production: The case of Bokole watershed, Southern Ethiopia. Afr. J. Environ. Sci. Technol. 2013, 7, 990–1000. [Google Scholar] [CrossRef]
- Joshi, P.K.; Jha, A.K.; Wani Suhas, P.; Sreedevi, T.K.; Shaheen, F.A. Impact of Watershed Program and Conditions for Success: A Meta-Analysis Approach. Global Theme on Agroecosystems. Report no. 46; International Crops Research Institute for the Semi-Arid Tropics: Patancheru, India, 2008. [Google Scholar]
- Pandit, A. Watershed Development Inputs and Social Change; Rawat Publications, Watershed Organisation Trust: Jaipur, India, 2010. [Google Scholar]
- Pandit, A.; Zade, D. Watershed Development and Health—Study of Child Nutrition in Rural Semi-Arid Region; Watershed Organisation Trust, Rawat Publications: Pune, India, 2012. [Google Scholar]
- James, A.J.; Pangtey, V.K.; Singh, P.; Virgo, K. Bringing people’s perceptions to project management desktops: A quantified participatory assessment of the Doon Valley Watershed Project in North India. Impact Assess. Proj. Apprais. 2002, 20, 201–214. [Google Scholar] [CrossRef][Green Version]
- Nerkar, S.S.; Pathak, A.; Lundborg, C.S.; Tamhankar, A.J. Can integrated watershed management contribute to improvement of public health? A cross-sectional study from hilly tribal villages in India. Int. J. Environ. Res. Public Health 2015, 12, 2653–2669. [Google Scholar] [CrossRef] [PubMed]
- Nerkar, S.S.; Tamhankar, A.J.; Johansson, E.; Lundborg, C.S. Improvement in health and empowerment of families as a result of watershed management in a tribal area in India—A qualitative study. BMC Int. Health Hum. Rights 2013, 13, 42. [Google Scholar] [CrossRef]
- Nerkar, S.S.; Tamhankar, A.J.; Johansson, E.; Lundborg, C.S. Impact of integrated watershed management on complex interlinked factors influencing health: Perceptions of professional stakeholders in a hilly tribal area of India. Int. J. Environ. Res. Public Health 2016, 13, 285. [Google Scholar] [CrossRef]
- Mishra, P.K.; Saxena, R. Integrated impact assessment model for explaining differential impact of watershed development projects. Impact Assess. Proj. Apprais. 2009, 27, 175–184. [Google Scholar] [CrossRef][Green Version]
- Technical Committee on Watershed Programmes in India. From Hariyali to Neeranchal—Report of the Technical Committee on Watershed Programmes in India; Government of India: New Delhi, India, 2006.
- Winkler, M.S.; Divall, M.J.; Krieger, G.R.; Balge, M.Z.; Singer, B.H.; Utzinger, J. Assessing health impacts in complex eco-epidemiological settings in the humid tropics: Advancing tools and methods. Environ. Impact Assess. Rev. 2010, 30, 52–61. [Google Scholar] [CrossRef]
- Green, J.; Thorogood, N. Qualitative Methods for Health Research; SAGE Publications Ltd.: London, UK, 2004. [Google Scholar]
- University of Agricultural Sciences—Bangalore. Impact on agricultural sector. In Karnataka Climate Change Action Plan—Final Report Submitted by Bangalore Climate Change Initiative—Karnataka to Government of Karnataka; BCCI-K, Ed.; Bangalore Climate Change Initiative—Karnataka (BCCI-K): Bengaluru, India, 2011. [Google Scholar]
- Office of the Registrar General & Census Commissioner. District census hand book: Village amenities (for Karnataka). In Census of India; Government of India: New Delhi, India, 2011. [Google Scholar]
- Van Eeuwijk, P.; Angehrn, Z. How to Conduct a Focus Group Discussion (FGD)—Methodological Manual; Swiss Tropical and Public Health Institute (Swiss TPH): Basel, Switzerland, 2015. [Google Scholar]
- Britten, N. Qualitative research: Qualitative interviews in medical research. BMJ 1995, 311, 251–253. [Google Scholar] [CrossRef]
- Marshall, M.N. Sampling for qualitative research. Fam. Pract. 1996, 13, 522–526. [Google Scholar] [CrossRef]
- Phillippi, J.; Lauderdale, J. A guide to field notes for qualitative research: Context and conversation. Qual. Health Res. 2018, 28, 381–388. [Google Scholar] [CrossRef] [PubMed]
- Loewenson, R.; Laurell, A.; Hogstedt, C.; D’Ambruoso, L.; Shroff, Z. Participatory Action Research in Health Systems—A Methods Reader; TARSC; AHPSR; WHO; IDRC Canada; EQUINET: Harare, Zimbabwe, 2014. [Google Scholar]
- Institute of Medicine (IOM); National Research Council (NRC). A Framework for Assessing Effects of the Food System; The National Academies Press: Washington, DC, USA, 2015. [Google Scholar]
- Gale, N.K.; Heath, G.; Cameron, E.; Rashid, S.; Redwood, S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med. Res. Methodol. 2013, 13, 117. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- ICT Services and System Development and Division of Epidemiology and Global Health. OpenCode 4.03; Umeå University: Umeå, Sweden, 2013. [Google Scholar]
- Tong, A.; Sainsbury, P.; Craig, J. Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 2007, 19, 349–357. [Google Scholar] [CrossRef] [PubMed]
- Kerr, J. Watershed development, environmental services, and poverty alleviation in India. World Dev. 2002, 30, 1387–1400. [Google Scholar] [CrossRef]
- Borooah, V.K.; Diwakar, D.; Mishra, V.K.; Naik, A.K.; Sabharwal, N.S. Caste, inequality, and poverty in India: A re-assessment. Dev. Stud. Res. 2014, 1, 279–294. [Google Scholar] [CrossRef]
- Singh, P.; Behera, H.C.; Singh, A. Impact and Effectiveness of Watershed Development Programmes in India—Review and Analysis Based on the Studies Conducted by Various Government Agencies and Other Organisations; Lal Bahadur Shastre National Academy of Administration: Musoorie, India, 2010.
- Kadiyala, S.; Harris, J.; Headey, D.; Yosef, S.; Gillespie, S. Agriculture and nutrition in India: Mapping evidence to pathways. Ann. N. Y. Acad. Sci. 2014, 1331, 43–56. [Google Scholar] [CrossRef] [PubMed]
- Padmaja, R.; Pramanik, S.; Pingali, P.; Bantilan, C.; Kavitha, K. Understanding nutritional outcomes through gendered analysis of time-use patterns in semi-arid India. Glob. Food Sec. 2019, 23, 49–63. [Google Scholar] [CrossRef]
- Ghosh, S.K.; Tiwari, S.N.; Sathyanarayan, T.S.; Sampath, T.R.R.; Sharma, V.P.; Nanda, N.; Joshi, H.; Adak, T.; Subbarao, S.K. Larvivorous fish in wells target the malaria vector sibling species of the Anopheles culicifacies complex in villages in Karnataka, India. Trans. R. Soc. Trop. Med. Hyg. 2005, 99, 101–105. [Google Scholar] [CrossRef]
- Balakrishnan, N.; Katyal, R.; Mittal, V.; Chauhan, L.S. Prevalence of Aedes aegypti—The vector of dengue/chikungunya fevers in Bangalore City, Urban and Kolar districts of Karnataka state. J. Commun. Dis. 2015, 47, 19–23. [Google Scholar]
- Shoba, S.; Amita, M.; Saraswathi, S. A clinico-epidemiological study of the burden and outcome of vector borne diseases in a tertiary care hospital, Bengaluru. Natl. J. Res. Community Med. 2019, 8, 108–111. [Google Scholar] [CrossRef]
- Shruthi, M.N.; Santhuram, A.; Arun, H.; Kishore Kumar, B. A comparative study of skeletal fluorosis among adults in two study areas of Bangarpet taluk, Kolar. Indian J. Public Health 2016, 60, 203–209. [Google Scholar] [CrossRef]
- Shruthi, M.N.; Anil, N.S. A comparative study of dental fluorosis and non-skeletal manifestations of fluorosis in areas with different water fluoride concentrations in rural Kolar. J. Fam. Med. Prim. Care 2018, 7, 1222–1228. [Google Scholar] [CrossRef]
- Saeed, M.; Malik, R.N.; Kamal, A. Fluorosis and cognitive development among children (6–14 years of age) in the endemic areas of the world: A review and critical analysis. Environ. Sci. Pollut. Res. 2019. [Google Scholar] [CrossRef] [PubMed]
- Bhagavan, S.V.B.K.; Raghu, V. Utility of check dams in dilution of fluoride concentration in ground water and the resultant analysis of blood serum and urine of villagers, Anantapur District, Andhra Pradesh, India. Environ. Geochem. Health 2005, 27, 97–108. [Google Scholar] [CrossRef] [PubMed]
- Jacks, G.; Bhattacharya, P.; Chaudhary, V.; Singh, K.P. Controls on the genesis of some high-fluoride groundwaters in India. Appl. Geochem. 2005, 20, 221–228. [Google Scholar] [CrossRef]
- State’s Drought Ponds Turn into Death Traps for Kids, Animals. Available online: https://timesofindia.indiatimes.com/city/bengaluru/states-drought-ponds-turn-into-death-traps-for-kids-animals/articleshow/61192066.cms (accessed on 21 April 2020).
- Rao, N.; Singh, C.; Solomon, D.; Camfield, L.; Sidiki, R.; Angula, M.; Poonacha, P.; Sidibé, A.; Lawson, E.T. Managing risk, changing aspirations and household dynamics: Implications for wellbeing and adaptation in semi-arid Africa and India. World Dev. 2020, 125, 104667. [Google Scholar] [CrossRef]
- Berry, H.L.; Bowen, K.; Kjellstrom, T. Climate change and mental health: A causal pathways framework. Int. J. Public Health 2010, 55, 123–132. [Google Scholar] [CrossRef]
- Cairns, M.R.; Cox, C.E.; Zambrana, J.; Flotemersch, J.; Lan, A.; Phillips, A.; Kozhuharova, G.; Qirjo, M.; Szigeti, B.M.; Kadeli, L. Building multi-country collaboration on watershed management: Lessons on linking environment and public health from the Western Balkans. Rev. Environ. Health 2017, 32, 15–22. [Google Scholar] [CrossRef]
- Obrist, B.; Iteba, N.; Lengeler, C.; Makemba, A.; Mshana, C.; Nathan, R.; Alba, S.; Dillip, A.; Hetzel, M.W.; Mayumana, I.; et al. Access to Health Care in Contexts of Livelihood Insecurity: A Framework for Analysis and Action. PLoS Med. 2007, 4, e308. [Google Scholar] [CrossRef]
- WHO; ECHP. Health Impact Assessment: Main Concepts and Suggested Approach—Gothenburg Consensus Paper; WHO Regional Office Europe: Copenhagen, Denmark, 1999. [Google Scholar]
- Government of India. National Health Policy 2017; Government of India: New Delhi, India, 2017.

| Village Characteristics | Village 1 | Village 2 | Village 3 | Village 4 |
|---|---|---|---|---|
| Sub-district | Malur | Bangarpet | Kolar | Bangarpet |
| Distance to sub-district headquarters (km) | 26 | 44 | 10 | 20 |
| Total households | 181 | 187 | 92 | 46 |
| Total population | 879 | 676 | 454 | 211 |
| Scheduled caste population (%) | 15.6 | 47.0 | 15.4 | 0.0 |
| Scheduled tribe population (%) | 24.6 | 6.5 | 0.0 | 100.0 |
| Geographical area of village (ha) | 440.6 | 777.6 | 87.2 | 151.8 |
| Distance to primary health centre (km) | 5–10 | 5–10 | 5–10 | 5–10 |
| Water supply | Available | Available | Available | Available |
| Governmental crèche (anganwadi) | Available | Available | Available | At nearby village |
| Themes | Sub-Themes | Codes |
|---|---|---|
| Pathways towards nutritional impacts | Direct impacts on food security and nutrition; income-mediated impacts on food security and nutrition | Crop choices, irrigated agriculture, rain-fed agriculture, financing agriculture, agri-inputs, wildlife and pests, surface water irrigation, food security, diet, wage labour, livestock, self-help groups, common lands, migration, nutrition, chemical toxicity, participation in WSD project, tree-planting, livelihood activities, impact on water and soil conservation, impact on food production, impact on wage labour, impact on livelihood and impact on nutrition |
| Impacts on disease vector ecology | Mosquitoes, vector-borne diseases, watershed structures, impact on local environment, impact on mosquitoes and vector control activities | |
| Health impacts of opportunistic activities | Hygiene, drinking water quality, diarrhoeal diseases, other work-related health problems, access to healthcare, creating local institutions, other structures created, health activities, water for domestic use, impact on awareness, impact on sanitation and other health impacts |
| Participants | Number (%) | Average Duration - Minutes (SD) |
|---|---|---|
| Local people (n = 26) | ||
| Men [average age (SD): 40.5 years (11.4 years)] | 13 (50) | 23.4 (10.1) |
| Women [average age (SD): 46.2 years (12.7 years)] | 13 (50) | 19.6 (7.9) |
| Scheduled caste | 4 (15) | 15.5 (2.4) |
| Scheduled tribe | 9 (35) | 16.8 (6.4) |
| Other caste | 13 (50) | 26.6 (9.4) |
| Land-owning, with irrigation | 12 (46) | 25.4 (7.9) |
| Land-owning, without irrigation | 5 (19) | 21.5 (15.7) |
| Landless | 9 (35) | 19 (2.5) |
| Key informants (n = 14) | ||
| Field health-worker | 5 (35.7) | 16.8 (4.6) |
| Field project staff (liaison) | 4 (28.6) | 29 (6.2) |
| Project managerial officials | 3 (21.4) | 37.3 (18.5) |
| WSD expert (other region) | 1 (7.1) | 92 |
| Environmental health academician | 1 (7.1) | 81 |
| FGD participants (n = 2; with 12 participants) | ||
| Female [average age (SD): 42.5 years (14.5 years)] | 12 (100) | 27 (5.7) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pradyumna, A.; Mishra, A.; Utzinger, J.; Winkler, M.S. Perceived Health Impacts of Watershed Development Projects in Southern India: A Qualitative Study. Int. J. Environ. Res. Public Health 2020, 17, 3448. https://doi.org/10.3390/ijerph17103448
Pradyumna A, Mishra A, Utzinger J, Winkler MS. Perceived Health Impacts of Watershed Development Projects in Southern India: A Qualitative Study. International Journal of Environmental Research and Public Health. 2020; 17(10):3448. https://doi.org/10.3390/ijerph17103448
Chicago/Turabian StylePradyumna, Adithya, Arima Mishra, Jürg Utzinger, and Mirko S. Winkler. 2020. "Perceived Health Impacts of Watershed Development Projects in Southern India: A Qualitative Study" International Journal of Environmental Research and Public Health 17, no. 10: 3448. https://doi.org/10.3390/ijerph17103448
APA StylePradyumna, A., Mishra, A., Utzinger, J., & Winkler, M. S. (2020). Perceived Health Impacts of Watershed Development Projects in Southern India: A Qualitative Study. International Journal of Environmental Research and Public Health, 17(10), 3448. https://doi.org/10.3390/ijerph17103448





