A Scoping Review of Epidemiological, Ergonomic, and Longitudinal Cohort Studies Examining the Links between Stair and Bathroom Falls and the Built Environment
Abstract
1. Introduction
- What specific environmental features and dimensions of stairs and bathrooms have been assessed in epidemiological studies examining risk factors for falls and/or fall-related morbidity or mortality among seniors in community settings?
- What specific environmental features and dimensions of stairs and bathrooms have been assessed in ergonomic studies examining the kinematic measures associated with the risk of falling?
- How does the data collected on the environmental features and dimensions of stairs and bathrooms differ between epidemiological and ergonomic studies?
- Do national longitudinal studies on aging include questions related to falls, the location of falls, and features of the built environment?
2. Materials and Methods
2.1. Epidemiological and Ergonomic Studies
2.1.1. Search Strategy
2.1.2. Eligibility Criteria
2.1.3. Additional Inclusion Criteria for Epidemiological Studies
2.1.4. Additional Inclusion Criteria for Ergonomic Studies
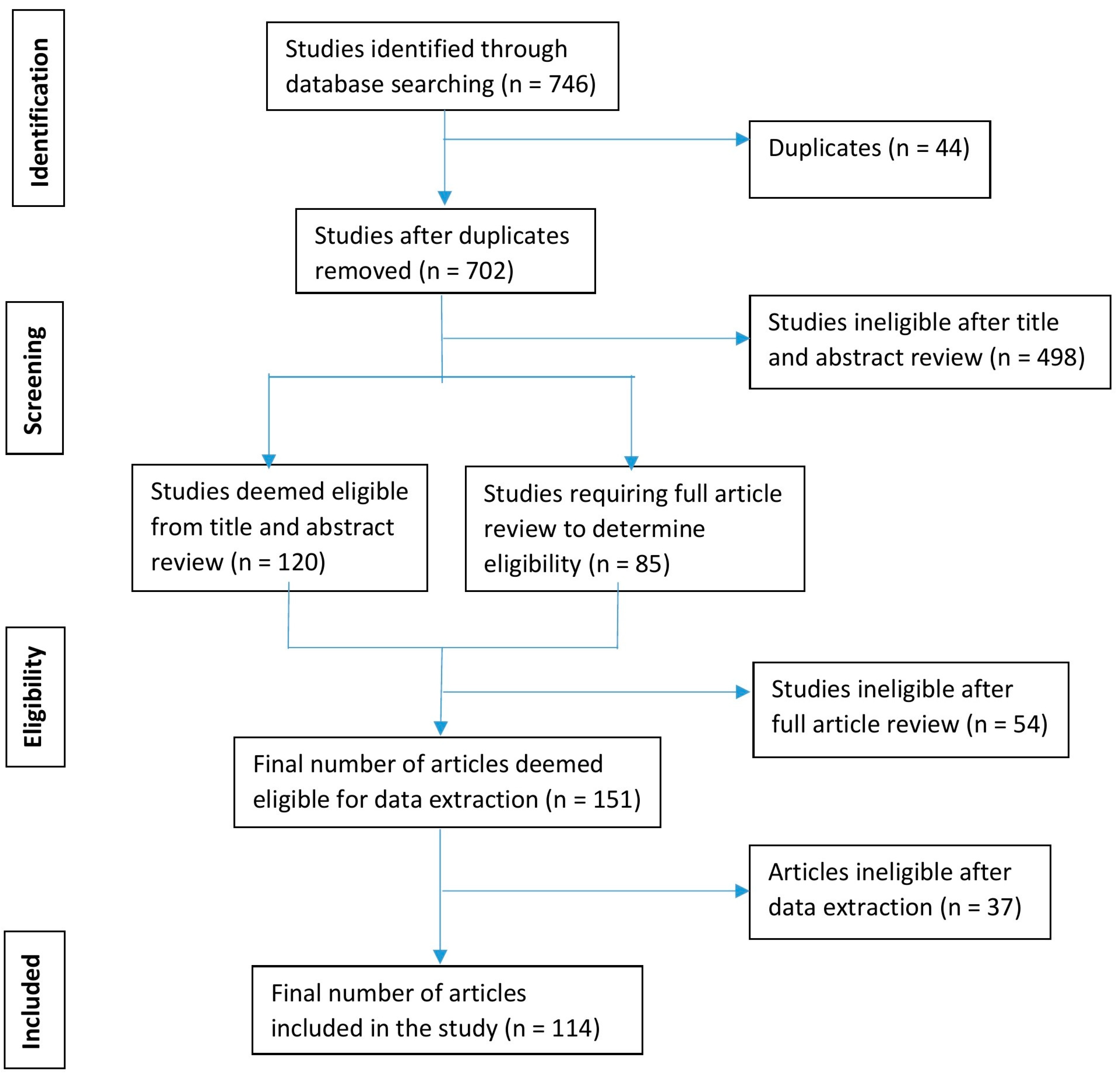
2.1.5. Study Selection Process
2.1.6. Data Collection
- Study information (author(s) and year of publication);
- Study setting (country for both epidemiological studies and ergonomic studies, and laboratory versus community setting for ergonomic studies);
- Study characteristics (type of study design, study aims, sample size, and age of study participants);
- Outcomes for epidemiological studies, namely: data source for falls; measures of falls reported (falls, fall-related injuries, and fall-related deaths); location of falls described (proportion of falls on stairs, in bathrooms or in another location, or location of falls not disaggregated; indoor versus outdoor falls);
- Outcomes for ergonomic studies, namely: type of kinematic and kinetic variables assessed (e.g., gait, balance, and muscle strength); included question(s) about falls in their study (yes or no);
- Environmental features for epidemiological studies, namely: data source(s) used for environmental hazards; environmental features and dimensions of stairs and bathrooms recorded (yes or no), and if recorded, the features and dimensions described; individual versus cumulative set of environmental hazards used in analysis of relationship to measure(s) of falls; and,
- Environmental features for ergonomic studies, namely: environmental features and dimensions of stairs and bathrooms recorded (yes or no), and if recorded, features and dimensions described.
2.2. Longitudinal Studies on Aging
2.2.1. Search Strategy
2.2.2. Eligibility
2.2.3. Data Extraction
3. Results
3.1. Eligible Epidemiological and Ergonomic Studies
3.2. Characteristics of Epidemiological and Ergonomic Studies
3.3. Features of Stairs and Bathrooms Described in Epidemiological and Ergonomic Studies
3.3.1. Epidemiological Studies
3.3.2. Association between Falls and Features of Stairs and/or Bathrooms in Epidemiological Studies
3.3.3. Ergonomic Studies
3.4. National Longitudinal Studies on Ageing
Studies Retrieved and Study Characteristics
3.5. Comparison of Epidemiological, Ergonomic, and Longitudinal Studies on Aging
4. Discussion
4.1. Limitations
4.2. Recommendations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
- Aged/
- Senior *
- Older adults
- Elderly
- Stair *
- Toilet *
- Bath *
- Accidents, home or
- Fall *
- Gait
- Balance
- Accessibility
- (Aged/OR senior* OR older adults OR elderly) AND
- (Stair* OR toilet* OR bath*) AND
- (Gait OR balance OR accessibility OR fall* OR accidents, home)
References
- Public Health Agency of Canada Seniors’ Falls in Canada: Second Report. Available online: https://www.canada.ca/en/public-health/services/health-promotion/aging-seniors/publications/publications-general-public/seniors-falls-canada-second-report.html (accessed on 29 September 2017).
- Parachute. The Cost of Injury in Canada; Parachute: Toronto, ON, Canada, 2015. [Google Scholar]
- Bergen, G. Falls and Fall Injuries Among Adults Aged ≥65 Years—United States, 2014. Mmwr. Morb. Mortal. Wkly. Rep. 2016, 65, 993–998. Available online: https://www.cdc.gov/mmwr/volumes/65/wr/mm6537a2.htm (accessed on 20 March 2018). [CrossRef] [PubMed]
- Bohl, A.A.; Fishman, P.A.; Ciol, M.A.; Williams, B.; LoGerfo, J.; Phelan, E.A. A longitudinal analysis of total 3-year healthcare costs for older adults who experience a fall requiring medical care. J. Am. Geriatr. Soc. 2010, 58, 853–860. [Google Scholar] [CrossRef] [PubMed]
- Davis, J.C.; Robertson, M.C.; Ashe, M.C.; Liu-ambrose, T.; Khan, K.M.; Marra, C.A. International comparison of cost of falls in older adults living in the community: A systematic review. Osteoporos. Int. Lond. 2010, 21, 1295–1306. [Google Scholar] [CrossRef]
- Burns, E.R.; Stevens, J.A.; Lee, R. The direct costs of fatal and non-fatal falls among older adults—United States. J. Saf. Res. 2016, 58, 99–103. [Google Scholar] [CrossRef]
- Public Health Agency of Canada. The Safe Living Guide—A Guide to Home Safety for Seniors; Public Health Agency of Canada: Ottawa, ON, Canada, 2015.
- Larson, E.B. Evidence supports action to prevent injurious falls in older adults. JAMA 2017, 318, 1659–1660. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Nonfatal bathroom injuries among persons aged >=15 years–United States, 2008. Morb. Mortal. Wkly. Rep. 2011, 60, 729–733. [Google Scholar]
- Edwards, N. Chapter 15: Knowledge translation for intersectoral action: The case of Canada’s building codes. In Population Health in Canada: Issues, Research, and Action; Bourgeault, I.L., Labonte, R., Packer, C., Runnels, V., Eds.; Canada Scholars Press: Toronto, ON, Canada, 2017; pp. 156–160. [Google Scholar]
- PRISMA the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA). Available online: http://prisma-statement.org/ (accessed on 21 March 2018).
- Dobson, F.; Bennell, K.L.; Hinman, R.S.; Abbott, J.H.; Roos, E.M. Recommended Performance-Based Tests to Assess Physical Function in People Diagnosed with Hip or Knee Osteoarthritis. Available online: https://www.oarsi.org/sites/default/files/docs/2013/manual.pdf (accessed on 21 March 2018).
- Zotero. Available online: https://www.zotero.org/ (accessed on 23 March 2018).
- Gateway to Global Aging Data Surveys at a Glance. Available online: https://g2aging.org/?section=surveyOverview (accessed on 23 March 2018).
- ILifespan Links to Longitudinal Studies. Available online: https://www.ilifespan.org/?q=links_to_longitudinal_studies (accessed on 23 March 2018).
- IALSA Research Network IALSA—Integrative Analysis of Longitudinal Studies of Aging and Dementia | Maelstrom Research. Available online: https://www.maelstrom-research.org/mica/network/ialsa#/ (accessed on 23 March 2018).
- Hanba, C.; Gupta, A.; Svider, P.F.; Folbe, A.J.; Eloy, J.A.; Zuliani, G.F.; Carron, M.A. Forgetful but not forgotten: Bathroom-related craniofacial trauma among the elderly: Elderly Bathroom Craniofacial Trauma. Laryngoscope 2017, 127, 820–827. [Google Scholar] [CrossRef] [PubMed]
- Pereira, S.G.; Santos, C.B.D.; Doring, M.; Portella, M.R. Prevalence of household falls in long-lived adults and association with extrinsic factors. Rev. Dépidémiologie St. Publique 2017, 25, 3–11. [Google Scholar] [CrossRef]
- Stessman, J. Climbing Stairs, Handrail Use, and Survival. Available online: https://link.springer.com/article/10.1007/s12603-016-0763-5 (accessed on 15 January 2018).
- Keall, M.D.; Pierse, N.; Howden-Chapman, P.; Cunningham, C.; Cunningham, M.; Guria, J.; Baker, M.G. Home modifications to reduce injuries from falls in the Home Injury Prevention Intervention (HIPI) study: A cluster-randomised controlled trial. Lancet 2015, 385, 231–238. [Google Scholar] [CrossRef]
- Shi, J.; Zhou, B.Y.; Tao, Y.K.; Yu, P.L.; Zhang, C.F.; Qin, Z.H.; Sun, Z.Q. Incidence and associated factors for single and recurrent falls among the elderly in an urban community of Beijing. Biomed Environ. Sci. 2014, 27, 939–949. [Google Scholar] [PubMed]
- Kamel, M.H.; Abdulmajeed, A.A.; Ismail, S.E.S. Risk factors of falls among elderly living in urban Suez–Egypt. Pan Afr. Med. J. 2013, 14, 26. [Google Scholar] [CrossRef]
- Kuhirunyaratn, P.; Prasomrak, P.; Jindawong, B. Factors related to falls among community dwelling elderly. Southeast Asian J. Trop. Med. Public Health 2013, 44, 906–915. [Google Scholar] [PubMed]
- Lim, Y.M.; Sung, M.H. Home environmental and health-related factors among home fallers and recurrent fallers in community dwelling older Korean women. Int. J. Nurs. Pract. 2012, 18, 481–488. [Google Scholar] [CrossRef]
- Sophonratanapokin, B.; Sawangdee, Y.; Soonthorndhada, K. Effect of the living environment on falls among the elderly in Thailand. Southeast Asian J. Trop. Med. Public Health 2012, 43, 1537–1547. [Google Scholar] [PubMed]
- Leclerc, B.-S.; Bégin, C.; Cadieux, É.; Goulet, L.; Allaire, J.-F.; Meloche, J.; Leduc, N.; Kergoat, M.-J. Relationship between home hazards and falling among community-dwelling seniors using home-care services. Rev. D’épidémiologie Et De St. Publique 2010, 58, 3–11. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.Y.Y.; Kim, J.H.; Griffiths, S.M.; Lau, J.T.F.; Yu, I. Does living density matter for nonfatal unintentional home injury in Asian urban settings? Evidence from Hong Kong. J. Urban Health 2009, 86, 872–886. [Google Scholar] [CrossRef]
- van Hensbroek, P.B.; Mulder, S.; Luitse, J.S.K.; van Ooijen, M.R.; Goslings, J.C. Staircase falls: High-risk groups and injury characteristics in 464 patients. Injury 2009, 40, 884–889. [Google Scholar] [CrossRef] [PubMed]
- Yu, P.L.; Qin, Z.H.; Shi, J.; Zhang, J.; Xin, M.Z.; Wu, Z.L.; Sun, Z.Q. Prevalence and related factors of falls among the elderly in an urban community of Beijing. Biomed. Environ. Sci. 2009, 22, 179–187. [Google Scholar] [CrossRef]
- Edwards, N.; Birkett, N.; Nair, R.; Murphy, M.; Roberge, G.; Lockett, D. Access to bathtub grab bars: Evidence of a policy gap. Can. J. Aging 2006, 25, 295–304. [Google Scholar] [CrossRef]
- Johnson, D.A.; Pauls, J. Systemic Stair Step Geometry Defects, Increased Injuries, and Public Health Plus Regulatory Responses. In Contemporary Ergonomics and Human Factors 2010, Proceedings of the International Conference on Contemporary Ergonomics and Human Factors, Keele, UK, 2010; Anderson, M., Ed.; CRC Press: Boca Raton, FL, USA, 2010; pp. 453–461. [Google Scholar]
- Johannsson, J.; Duchateau, J.; Baudry, S. Spinal and corticospinal pathways are differently modulated when standing at the bottom and the top of a three-step staircase in young and older adults. Eur. J. Appl. Physiol. 2017, 117, 1165–1174. [Google Scholar] [CrossRef]
- King, E.C.; Novak, A.C. Effect of bathroom aids and age on balance control during bathing transfers. Am. J. Occup. Ther. 2017, 71, 106165030. [Google Scholar] [CrossRef] [PubMed]
- Kunzler, M.R.; da Rocha, E.S.; Bobbert, M.F.; Duysens, J.; Carpes, F.P. Acute effects of walking exercise on stair negotiation in sedentary and physically active older adults. J. Phys. Act. Health 2017, 14, 532–538. [Google Scholar] [CrossRef] [PubMed]
- Song, Q.; Tian, X.; Wong, D.; Zhang, C.; Sun, W.; Cheng, P.; Mao, D. Effects of Tai Chi exercise on body stability among the elderly during stair descent under different levels of illumination. Res. Sports Med. 2017, 25, 197–208. [Google Scholar] [CrossRef]
- Song, Q.; Wang, S.; Wong, D.P.; Zhou, J.; Sun, W.; Zhang, C.; Gu, H.; Mao, D. Long-term Tai Chi exercise increases body stability of the elderly during stair ascent under high and low illumination. Sports Biomech. 2017, 17, 402–413. [Google Scholar] [CrossRef]
- Swanenburg, J.; Bäbler, E.; Adelsberger, R.; Straumann, D.; de Bruin, E.D. Patients with chronic peripheral vestibular hypofunction compared to healthy subjects exhibit differences in gaze and gait behaviour when walking on stairs and ramps. PLoS ONE 2017, 12, e0189037. [Google Scholar] [CrossRef]
- Wang, K.; Delbaere, K.; Brodie, M.A.D.; Lovell, N.H.; Kark, L.; Lord, S.R.; Redmond, S.J. Differences between gait on stairs and flat surfaces in relation to fall risk and future falls. IEEE J. Biomed. Health Inf. 2017, 21, 1479–1486. [Google Scholar] [CrossRef]
- Handsaker, J.C.; Brown, S.J.; Bowling, F.L.; Maganaris, C.N.; Boulton, A.J.M.; Reeves, N.D. Resistance exercise training increases lower limb speed of strength generation during stair ascent and descent in people with diabetic peripheral neuropathy. Diabet. Med. 2016, 33, 97–104. [Google Scholar] [CrossRef]
- Lyytinen, T.; Bragge, T.; Hakkarainen, M.; Liikavainio, T.; Karjalainen, P.A.; Arokoski, J.P. Repeatability of knee impulsive loading measurements with skin-mounted accelerometers and lower limb surface electromyographic recordings during gait in knee osteoarthritic and asymptomatic individuals. J. Musculoskelet. Neuronal. Interact. 2016, 16, 63–74. [Google Scholar] [PubMed]
- Novak, A.C.; Komisar, V.; Maki, B.E.; Fernie, G.R. Age-related differences in dynamic balance control during stair descent and effect of varying step geometry. Appl. Ergon. 2016, 52, 275–284. [Google Scholar] [CrossRef]
- Shin, S.-S.; Yoo, W.-G. The effects of gait time and trunk acceleration ratio during stair climbing in old-old adult females. J. Phys. Ther. Sci. 2016, 28, 2025–2026. [Google Scholar] [CrossRef][Green Version]
- Spolaor, F.; Sawacha, Z.; Guarneri, G.; Del Din, S.; Avogaro, A.; Cobelli, C. Altered EMG patterns in diabetic neuropathic and not neuropathic patients during step ascending and descending. J. Electromyogr. Kinesiol. 2016, 31, 32–39. [Google Scholar] [CrossRef]
- Weiss, A.; Brozgol, M.; Giladi, N.; Hausdorff, J.M. Can a single lower trunk body-fixed sensor differentiate between level-walking and stair descent and ascent in older adults? Preliminary findings. Med. Eng. Phys. 2016, 38, 1146–1151. [Google Scholar] [CrossRef] [PubMed]
- Alcock, L.; O’Brien, T.D.; Vanicek, N. Biomechanical demands of the 2-step transitional gait cycles linking level gait and stair descent gait in older women. J. Biomech. 2015, 48, 4191–4197. [Google Scholar] [CrossRef] [PubMed]
- Brodie, M.A.; Wang, K.; Delbaere, K.; Persiani, M.; Lovell, N.H.; Redmond, S.J.; Rosario, M.B.D.; Lord, S.R. New methods to monitor stair ascents using a wearable pendant device reveal how behavior, fear, and frailty influence falls in octogenarians. IEEE Trans. Biomed. Eng. 2015, 62, 2595–2601. [Google Scholar] [CrossRef]
- Chiu, S.-L.; Chang, C.-C.; Dennerlein, J.T.; Xu, X. Age-related differences in inter-joint coordination during stair walking transitions. Gait Posture 2015, 42, 152–157. [Google Scholar] [CrossRef]
- Foster, R.J.; Whitaker, D.; Scally, A.J.; Buckley, J.G.; Elliott, D.B. What you see is what you step: The horizontal-vertical illusion increases toe clearance in older adults during stair ascent. Invest. Ophthalmol. Vis. Sci. 2015, 56, 2950–2957. [Google Scholar] [CrossRef]
- Kennedy, M.J.; Arcelus, A.; Guitard, P.; Goubran, R.A.; Sveistrup, H. Toilet grab-bar preference and center of pressure deviation during toilet transfers in healthy seniors, seniors with hip replacements, and seniors having suffered a stroke. Assist. Technol. 2015, 27, 78–87. [Google Scholar] [CrossRef]
- Laudanski, A.; Brouwer, B.; Li, Q. Activity classification in persons with stroke based on frequency features. Med. Eng. Phys. 2015, 37, 180–186. [Google Scholar] [CrossRef]
- Paquette, M.R.; Klipple, G.; Zhang, S. Greater step widths reduce internal knee abduction moments in medial compartment knee osteoarthritis patients during stair ascent. J. Appl. Biomech. 2015, 31, 229–236. [Google Scholar] [CrossRef]
- Singhal, K.; Kim, J.; Casebolt, J.; Lee, S.; Han, K.-H.; Kwon, Y.-H. Gender difference in older adult’s utilization of gravitational and ground reaction force in regulation of angular momentum during stair descent. Hum. Mov. Sci. 2015, 41, 230–239. [Google Scholar] [CrossRef]
- Alcock, L.; O’Brien, T.D.; Vanicek, N. Biomechanical demands differentiate transitioning vs. continuous stair ascent gait in older women. Clin. Biomech. 2014, 29, 111–118. [Google Scholar] [CrossRef]
- Antonio, P.J.; Perry, S.D. Quantifying stair gait stability in young and older adults, with modifications to insole hardness. Gait Posture 2014, 40, 429–434. [Google Scholar] [CrossRef]
- Foster, R.J.; Asha, A.R.D.; Reeves, N.D.; Maganaris, C.N.; Buckley, J.G. Stair-specific algorithms for identification of touch-down and foot-off when descending or ascending a non-instrumented staircase. Gait Posture 2014, 39, 816–821. [Google Scholar] [CrossRef][Green Version]
- Foster, R.J.; Hotchkiss, J.; Buckley, J.G.; Elliott, D.B. Safety on stairs: Influence of a tread edge highlighter and its position. Exp. Gerontol. 2014, 55, 152–158. [Google Scholar] [CrossRef]
- Handsaker, J.C.; Brown, S.J.; Bowling, F.L.; Cooper, G.; Maganaris, C.N.; Boulton, A.J.M.; Reeves, N.D. Contributory factors to unsteadiness during walking up and down stairs in patients with diabetic peripheral neuropathy. Diabetes Care 2014, 37, 3047–3053. [Google Scholar] [CrossRef][Green Version]
- Hinman, M.R.; O’Connell, J.K.; Dorr, M.; Hardin, R.; Tumlinson, A.B.; Varner, B. Functional predictors of stair-climbing speed in older adults. J. Geriatr. Phys. Ther. 2014, 37, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Hsue, B.-J.; Su, F.-C. Effects of age and gender on dynamic stability during stair descent. Arch. Phys. Med. Rehabil. 2014, 95, 1860–1869. [Google Scholar] [CrossRef]
- Singhal, K.; Kim, J.; Casebolt, J.; Lee, S.; Han, K.H.; Kwon, Y.H. Kinetic comparison of older men and women during walk-to-stair descent transition. Gait Posture 2014, 40, 600–604. [Google Scholar] [CrossRef]
- Telonio, A.; Blanchet, S.; Maganaris, C.N.; Baltzopoulos, V.; Villeneuve, S.; McFadyen, B.J. The division of visual attention affects the transition point from level walking to stair descent in healthy, active older adults. Exp. Gerontol. 2014, 50, 26–33. [Google Scholar] [CrossRef]
- Wang, K.; Lovell, N.H.; Rosario, M.B.D.; Liu, Y.; Wang, J.; Narayanan, M.R.; Brodie, M.A.D.; Delbaere, K.; Menant, J.; Lord, S.R.; et al. Inertial Measurements of Free-Living Activities: Assessing Mobility To Predict Falls. In Proceedings of the 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Chicago, IL, USA, 26–30 August 2014; pp. 6892–6895. [Google Scholar]
- Buckley, J.G.; Cooper, G.; Maganaris, C.N.; Reeves, N.D. Is stair descent in the elderly associated with periods of high centre of mass downward accelerations? Exp. Gerontol. 2013, 48, 283–289. [Google Scholar] [CrossRef]
- Guitard, P.; Sveistrup, H.; Fahim, A.; Leonard, C. Smart grab bars: A potential initiative to encourage bath grab bar use in community dwelling older adults. Assist. Technol. 2013, 25, 139–148. [Google Scholar] [CrossRef]
- Novak, A.C.; Brouwer, B. Kinematic and kinetic evaluation of the stance phase of stair ambulation in persons with stroke and healthy adults: A pilot study. J. Appl. Biomech. 2013, 29, 443–452. [Google Scholar] [CrossRef] [PubMed]
- Samuel, D.; Rowe, P.; Nicol, A. The Functional Demand (FD) placed on the knee and hip of older adults during everyday activities. Arch. Gerontol. Geriatr. 2013, 57, 192–197. [Google Scholar] [CrossRef][Green Version]
- Bosse, I.; Oberländer, K.D.; Savelberg, H.H.; Meijer, K.; Brüggemann, G.-P.; Karamanidis, K. Dynamic stability control in younger and older adults during stair descent. Hum. Mov. Sci. 2012, 31, 1560–1570. [Google Scholar] [CrossRef]
- Hicks-Little, C.A.; Peindl, R.D.; Fehring, T.K.; Odum, S.M.; Hubbard, T.J.; Cordova, M.L. Temporal-spatial gait adaptations during stair ascent and descent in patients with knee osteoarthritis. J. Arthroplast. 2012, 27, 1183–1189. [Google Scholar] [CrossRef] [PubMed]
- Novak, A.C.; Brouwer, B. Strength and aerobic requirements during stair ambulation in persons with chronic stroke and healthy adults. Arch. Phys. Med. Rehabil. 2012, 93, 683–689. [Google Scholar] [CrossRef]
- Samuel, D.; Rowe, P.; Hood, V.; Nicol, A. The relationships between muscle strength, biomechanical functional moments and health-related quality of life in non-elite older adults. Age Ageing 2012, 41, 224–230. [Google Scholar] [CrossRef]
- Guitard, P.; Sveistrup, H.; Edwards, N.; Lockett, D. Use of different bath grab bar configurations following a balance perturbation. Assist. Technol. 2011, 23, 205–215. [Google Scholar] [CrossRef] [PubMed]
- Hicks-Little, C.A.; Peindl, R.D.; Hubbard, T.J.; Scannell, B.P.; Springer, B.D.; Odum, S.M.; Fehring, T.K.; Cordova, M.L. Lower extremity joint kinematics during stair climbing in knee osteoarthritis. Med. Sci. Sports Exerc. 2011, 43, 516–524. [Google Scholar] [CrossRef]
- Karamanidis, K.; Arampatzis, A. Altered control strategy between leading and trailing leg increases knee adduction moment in the elderly while descending stairs. J. Biomech. 2011, 44, 706–711. [Google Scholar] [CrossRef]
- Leitner, M.; Schmid, S.; Hilfiker, R.; Radlinger, L. Test–retest reliability of vertical ground reaction forces during stair climbing in the elderly population. Gait Posture 2011, 34, 421–425. [Google Scholar] [CrossRef]
- Lin, C.-F.; Chang, C.-L.; Kuo, L.C.; Lin, C.J.; Chen, C.Y.; Su, F.C. Postural control while dressing on two surfaces in the elderly. Age 2011, 33, 187–196. [Google Scholar] [CrossRef]
- Novak, A.C.; Brouwer, B. Sagittal and frontal lower limb joint moments during stair ascent and descent in young and older adults. Gait Posture 2011, 33, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Oh-Park, M.; Wang, C.; Verghese, J. Stair negotiation time in community-dwelling older adults: Normative values and association with functional decline. Arch. Phys. Med. Rehabil. 2011, 92, 2006–2011. [Google Scholar] [CrossRef] [PubMed]
- Reid, S.M.; Graham, R.B.; Costigan, P.A. Differentiation of young and older adult stair climbing gait using principal component analysis. Gait Posture 2010, 31, 197–203. [Google Scholar] [CrossRef]
- Zietz, D.; Johannsen, L.; Hollands, M. Stepping characteristics and Centre of Mass control during stair descent: Effects of age, fall risk and visual factors. Gait Posture 2011, 34, 279–284. [Google Scholar] [CrossRef]
- Fujita, T.; Fujii, Y.; Munezane, H.; Ohue, M.; Takagi, Y. Analgesic effect of raloxifene on back and knee pain in postmenopausal women with osteoporosis and/or osteoarthritis. J. Bone Min. Metab. 2010, 28, 477–484. [Google Scholar] [CrossRef]
- Liikavainio, T.; Bragge, T.; Hakkarainen, M.; Karjalainen, P.A.; Arokoski, J.P. Gait and muscle activation changes in men with knee osteoarthritis. Knee 2010, 17, 69–76. [Google Scholar] [CrossRef]
- Pua, Y.-H.; Clark, R.A.; Bryant, A.L. Physical function in hip osteoarthritis: Relationship to isometric knee extensor steadiness. Arch. Phys. Med. Rehabil. 2010, 91, 1110–1116. [Google Scholar] [CrossRef]
- Reid, S.M.; Novak, A.C.; Brouwer, B.; Costigan, P.A. Relationship between stair ambulation with and without a handrail and centre of pressure velocities during stair ascent and descent. Gait Posture 2011, 34, 529–532. [Google Scholar] [CrossRef]
- Siegmund, G.P.; Flynn, J.; Mang, D.W.; Chimich, D.D.; Gardiner, J.C. Utilized friction when entering and exiting a dry and wet bathtub. Gait Posture 2010, 31, 473–478. [Google Scholar] [CrossRef]
- Arcelus, A.; Holtzman, M.; Goubran, R.; Sveistrup, H.; Guitard, P.; Knoefel, F. Analysis of commode grab bar usage for the monitoring of older adults in the smart home environment. In Proceedings of the 2009 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Minneapolis, MN, USA, 3–6 September 2009; pp. 6155–6158. [Google Scholar]
- Asay, J.L.; Mündermann, A.; Andriacchi, T.P. Adaptive patterns of movement during stair climbing in patients with knee osteoarthritis. J. Orthop. Res. 2009, 27, 325–329. [Google Scholar] [CrossRef]
- Bertucco, M.; Cesari, P. Dimensional analysis and ground reaction forces for stair climbing: Effects of age and task difficulty. Gait Posture 2009, 29, 326–331. [Google Scholar] [CrossRef]
- Hsue, B.-J.; Su, F.-C. Kinematics and kinetics of the lower extremities of young and elder women during stairs ascent while wearing low and high-heeled shoes. J. Electromyogr. Kinesiol. 2009, 19, 1071–1078. [Google Scholar] [CrossRef]
- Karamanidis, K.; Arampatzis, A. Evidence of mechanical load redistribution at the knee joint in the elderly when ascending stairs and ramps. Ann. Biomed. Eng. 2009, 37, 467–476. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.J. Prevention of falls during stairway descent in older adults. Appl Ergon. 2009, 40, 348–352. [Google Scholar] [CrossRef] [PubMed]
- Misic, M.M.; Valentine, R.J.; Rosengren, K.S.; Woods, J.A.; Evans, E.M. Impact of training modality on strength and physical function in older adults. Gerontology 2009, 55, 411–416. [Google Scholar] [CrossRef] [PubMed]
- Ojha, H.A.; Kern, R.W.; Lin, C.-H.J.; Winstein, C.J. Age affects the attentional demands of stair ambulation: Evidence from a dual-task approach. Phys. Ther. 2009, 89, 1080–1088. [Google Scholar] [CrossRef] [PubMed]
- Reeves, N.D.; Spanjaard, M.; Mohagheghi, A.A.; Baltzopoulos, V.; Maganaris, C.N. Older adults employ alternative strategies to operate within their maximum capabilities when ascending stairs. J. Electromyogr. Kinesiol. 2009, 19, e57–e68. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, I.; Sajin, A.; Fisher, I.; Neeb, M.; Shochina, M.; Katz-Leurer, M.; Meiner, Z. The effectiveness of locomotor therapy using robotic-assisted gait training in subacute stroke patients: A randomized controlled trial. PMR 2009, 1, 516–523. [Google Scholar] [CrossRef]
- Zietz, D.; Hollands, M. Gaze behavior of young and older adults during stair walking. J. Mot. Behav. 2009, 41, 357–365. [Google Scholar] [CrossRef]
- Fabio, D.; P, R.; Zampieri, C.; Tuite, P. Gaze Control and Foot Kinematics During Stair Climbing: Characteristics Leading to Fall Risk in Progressive Supranuclear Palsy. Phys. Ther. 2008, 88, 240–250. [Google Scholar] [CrossRef]
- Larsen, A.H.; Puggaard, L.; Hämäläinen, U.; Aagaard, P. Comparison of ground reaction forces and antagonist muscle coactivation during stair walking with ageing. J. Electromyogr. Kinesiol. 2008, 18, 568–580. [Google Scholar] [CrossRef]
- Reeves, N.D.; Spanjaard, M.; Mohagheghi, A.A.; Baltzopoulos, V.; Maganaris, C.N. Influence of light handrail use on the biomechanics of stair negotiation in old age. Gait Posture 2008, 28, 327–336. [Google Scholar] [CrossRef]
- Guo, M.; Axe, M.J.; Manal, K. The influence of foot progression angle on the knee adduction moment during walking and stair climbing in pain free individuals with knee osteoarthritis. Gait Posture 2007, 26, 436–441. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.-J.; Chou, L.-S. Balance control during stair negotiation in older adults. J. Biomech. 2007, 40, 2530–2536. [Google Scholar] [CrossRef]
- Liikavainio, T.; Isolehto, J.; Helminen, H.J.; Perttunen, J.; Lepola, V.; Kiviranta, I.; Arokoski, J.P.A.; Komi, P.V. Loading and gait symmetry during level and stair walking in asymptomatic subjects with knee osteoarthritis: Importance of quadriceps femoris in reducing impact force during heel strike? Knee 2007, 14, 231–238. [Google Scholar] [CrossRef]
- Mian, O.S.; Thom, J.M.; Narici, M.V.; Baltzopoulos, V. Kinematics of stair descent in young and older adults and the impact of exercise training. Gait Posture 2007, 25, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Misic, M.M.; Rosengren, K.S.; Woods, J.A.; Evans, E.M. Muscle quality, aerobic fitness and fat mass predict lower-extremity physical function in community-dwelling older adults. Gerontology 2007, 53, 260–266. [Google Scholar] [CrossRef] [PubMed]
- Murphy, S.L.; Nyquist, L.V.; Strasburg, D.M.; Alexander, N.B. Bath transfers in older adult congregate housing residents: Assessing the person–environment interaction. J. Am. Geriatr. Soc. 2006, 54, 1265–1270. [Google Scholar] [CrossRef] [PubMed]
- Flinders Centre for Ageing Studies the Australian Longitudinal Study of Ageing (ALSA). Available online: http://www.flinders.edu.au/ (accessed on 20 March 2018).
- Canadian Longitudinal Study on Aging Canadian Longitudinal Study on Aging (CLSA). Available online: https://www.clsa-elcv.ca/researchers/data-collection (accessed on 20 March 2018).
- Costa Rican Longevity and Healthy Aging Study (CRELES). Available online: http://www.creles.berkeley.edu/documentation.html (accessed on 20 March 2018).
- English Longitudinal Study of Ageing (ELSA). Available online: http://www.elsa-project.ac.uk/documentation (accessed on 20 March 2018).
- Engstler, H.; Schmiade, N. The German Ageing Survey (DEAS)—A longitudinal and time-series study of people in the second half of life. Schmollers Jahrb. 2013, 133, 97–107. [Google Scholar] [CrossRef]
- Interview Questionnaires: Health and Retirement Study. Available online: https://hrs.isr.umich.edu/documentation/questionnaires (accessed on 20 March 2018).
- Research Institute of Economy, Trade and Industry Japanese Study of Aging and Retirement (JSTAR). Available online: https://www.rieti.go.jp/en/projects/jstar/ (accessed on 20 March 2018).
- Korean Longitudinal Study of Ageing (KLoSA). Available online: http://survey.keis.or.kr/eng/klosa/klosa01.jsp (accessed on 20 March 2018).
- Mexican Health and Aging Study Data files and Documentation. Available online: http://www.mhasweb.org/DocumentationQuestionnaire.aspx (accessed on 20 March 2018).
- New Zealand Health, Work and Retirement Study. Available online: https://www.massey.ac.nz/massey/learning/departments/school-of-psychology/research/hart/new-zealand-health-work-and-retirement-study/health-work-and-retirement-questionnaires.cfm (accessed on 20 March 2018).
- The Survey of Health, Ageing and Retirement in Europe (SHARE). Available online: http://www.share-project.org/data-documentation.html (accessed on 20 March 2018).
- Code books: The Swedish National study on Aging and Care in Kungsholmen (SNAC-K). Available online: http://www.snac-k.se/for-researchers/code-books/ (accessed on 20 March 2018).
- Welmer, A.-K.; Rizzuto, D.; Laukka, E.J.; Johnell, K.; Fratiglioni, L. Cognitive and Physical Function in Relation to the Risk of Injurious Falls in Older Adults: A Population-Based Study. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 669–675. [Google Scholar] [CrossRef]
- Trinity College Dublin Documentation: The Irish Longitudinal Study on Ageing (TILDA). Available online: http://tilda.tcd.ie/data/documentation/ (accessed on 20 March 2018).
- Soriano, T.A.; DeCherrie, L.V.; Thomas, D.C. Falls in the community-dwelling older adult: A review for primary-care providers. Clin. Interv. Aging 2007, 2, 545–553. [Google Scholar] [CrossRef]
- Nyberg, L.; Gustafson, Y.; Berggren, D.; Brännström, B.; Bucht, G. Falls Leading to Femoral Neck Fractures in Lucid Older People. J. Am. Geriatr. Soc. 1996, 44, 156–160. [Google Scholar] [CrossRef]
- Northridge, M.E.; Nevitt, M.C.; Kelsey, J.L.; Link, B. Home hazards and falls in the elderly: The role of health and functional status. Am. J. Public Health 1995, 85, 509–515. [Google Scholar] [CrossRef] [PubMed]
- Weinberg, L.E.; Strain, L.A. Community-dwelling older adults’ attributions about falls. Arch. Phys. Med. Rehabil. 1995, 76, 955–960. [Google Scholar] [CrossRef]
- Nevitt, M.C.; Cummings, S.R.; Hudes, E.S. Risk Factors for Injurious Falls: A Prospective Study. J. Gerontol. 1991, 46, M164–M170. [Google Scholar] [CrossRef]
- Nevitt, M.C.; Cummings, S.R.; Kidd, S.; Black, D. Risk Factors for Recurrent Nonsyncopal Falls: A Prospective Study. JAMA 1989, 261, 2663–2668. [Google Scholar] [CrossRef]
- Tinetti, M.E.; Speechley, M.; Ginter, S.F. Risk Factors for Falls among Elderly Persons Living in the Community. N. Engl. J. Med. 1988, 319, 1701–1707. [Google Scholar] [CrossRef] [PubMed]
- O’Loughlin, J.L.; Boivin, J.F.; Robitaille, Y.; Suissa, S. Falls among the elderly: Distinguishing indoor and outdoor risk factors in Canada. J. Epidemiol. Community Health 1994, 48, 488–489. [Google Scholar] [CrossRef] [PubMed]
- Bergland, A.; Jarnlo, G.-B.; Laake, K. Predictors of falls in the elderly by location. Aging Clin. Exp. Res. 2003, 15, 43–50. [Google Scholar] [CrossRef] [PubMed]
- Kelsey, J.L.; Berry, S.D.; Procter-Gray, E.; Quach, L.; Nguyen, U.-S.D.T.; Li, W.; Kiel, D.P.; Lipsitz, L.A.; Hannan, M.T. Indoor and outdoor falls in older adults are different: The maintenance of balance, independent living, intellect, and Zest in the Elderly of Boston Study. J. Am. Geriatr. Soc. 2010, 58, 2135–2141. [Google Scholar] [CrossRef]
- Rio Rico Medical & Fire District. Operational Policy Manual: Community Healthcare Integrated Paramedicine Program (CHIPP); Rio Rico Medical & Fire District: Rio Rico, AZ, USA, 2016. [Google Scholar]
- World Health Organization Falls: Fact sheet. Available online: http://www.who.int/mediacentre/factsheets/fs344/en/ (accessed on 23 March 2018).
- Blanchet, R.; Edwards, N. A need to improve the assessment of environmental hazards for falls on stairs and in bathrooms. BMC Geriatr. 2018, 18, 272. [Google Scholar] [CrossRef]
- Cumming, R.G.; Thomas, M.; Szonyi, G.; Salkeld, G.; O’Neill, E.; Westbury, C.; Frampton, G. Home visits by an occupational therapist for assessment and modification of environmental hazards: A randomized trial of falls prevention. J. Am. Geriatr. Soc. 1999, 47, 1397–1402. [Google Scholar] [CrossRef] [PubMed]
- Blazewick, D.H.; Chounthirath, T.; Hodges, N.L.; Collins, C.L.; Smith, G.A. Stair-related injuries treated in United States emergency departments. Am. J. Emerg. Med. 2018, 36, 608–614. [Google Scholar] [CrossRef] [PubMed]
- Anonymous. The prevention of falls in later life. A report of the Kellogg International Work Group on the Prevention of Falls by the Elderly. Dan Med. Bull. 1987, 34, 1–24. [Google Scholar]
| Articles by Author and Year | Quantitative Measure of Environmental Features of Stairs (n = 9 Stair Studies) | Quantitative Measure of Environmental Features of Bathrooms (n = 10 Bathroom Studies) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Lighting | Handrail | Stair Rise or Run Dimensions | Uneven Stairs | Tread Edge Contrast | Landing Size | Other 1 | Lighting | Shower or Bathtub Grab Bar | Toilet Grab Bar | Other 2 | |
| Hanba et al. (2017) [17] | ✓ | ||||||||||
| Pereira et al. (2017) [18] | ✓ | ✓ | ✓ | ✓ | |||||||
| Stessman (2017) [19] | ✓ | ||||||||||
| Keall et al. (2015) [20] | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||
| Shi et al. (2014) [21] | ✓ | ✓ | |||||||||
| Kamel et al. (2013) [22] | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||
| Kuhirunyaratn et al. (2013) [23] | ✓ | ||||||||||
| Lim and Sung (2012) [24] | ✓ | ||||||||||
| Sophonratanapokin et al. (2012) [25] | ✓ | ✓ | ✓ | ✓ | |||||||
| Leclerc et al. (2010) [26] | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||
| Chan et al. (2009) [27] | ✓ | ✓ | |||||||||
| Hensbroek et al. (2009) [28] | ✓ | ||||||||||
| Yu et al. (2009) [29] | ✓ | ||||||||||
| Edwards et al. (2006) [30] | ✓ | ✓ | ✓ | ||||||||
| Total N (% of all epidemiological studies) | 5/38 (13.2%) | 5/38 (13.2%) | 3/38 (7.9%) | 2/38 (5.3%) | 0/38 3 (0.0%) | 0/38 3 (0.0%) | 3/38 (8.8%) | 3/38 (7.9%) | 6/38 (15.8%) | 6/38 (15.8%) | 9/38 (23.6%) |
| Articles by Author and Year | Quantitative Measure of Environmental Features of Stairs | Quantitative Measure of Environmental Features of Bathrooms | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Lighting | Handrail | Stair Rise or Run Dimensions | Uneven Stairs | Tread Edge Contrast | Landing Size | Other 1 | Lighting | Shower or Bathtub Grab Bar | Toilet Grab Bar | Other 2 | |
| Johannsson et al. (2017) [32] | ✓ | ||||||||||
| King and Novak (2017) [33] | ✓ | ||||||||||
| Kunzler et al. (2017) [34] | ✓ | ||||||||||
| Song et al. (2017a) [35] | ✓ | ||||||||||
| Song et al. (2017b) [36] | ✓ | ||||||||||
| Swanenburg et al. (2017) [37] | ✓ | ✓ | |||||||||
| Wang et al. (2017) [38] | ✓ | ✓ | |||||||||
| Handsaker et al. (2016) [39] | ✓ | ||||||||||
| Lyytinen et al. (2016) [40] | ✓ | ||||||||||
| Novak et al. (2016) [41] | ✓ | ✓ | |||||||||
| Shin and Yoo (2016) [42] | ✓ | ||||||||||
| Spolaor et al. (2016) [43] | ✓ | ||||||||||
| Weiss et al. (2016) [44] | ✓ | ||||||||||
| Alcock et al. (2015) [45] | ✓ | ✓ | |||||||||
| Brodie et al. (2015) [46] | ✓ | ||||||||||
| Chiu et al. (2015) [47] | ✓ | ✓ | |||||||||
| Foster et al. (2015) [48] | ✓ | ✓ | ✓ | ||||||||
| Kennedy et al. (2015) [49] | ✓ | ||||||||||
| Laudanski et al. (2015) [50] | ✓ | ||||||||||
| Paquette et al. (2015) [51] | ✓ | ||||||||||
| Singhal et al. (2015) [52] | ✓ | ✓ | |||||||||
| Alcock et al. (2014) [53] | ✓ | ✓ | |||||||||
| Antonio and Perry (2014) [54] | ✓ | ✓ | |||||||||
| Foster et al. (2014a) [55] | ✓ | ||||||||||
| Foster et al (2014b) [56] | ✓ | ✓ | |||||||||
| Handsaker et al. (2014) [57] | ✓ | ||||||||||
| Hinman et al. (2014) [58] | ✓ | ✓ | |||||||||
| Hsue and Su (2014) [59] | ✓ | ||||||||||
| Singhal et al. (2014) [60] | ✓ | ✓ | |||||||||
| Telonio et al. (2014) [61] | ✓ | ✓ | ✓ | ||||||||
| Wang et al. (2014) [62] | ✓ | ||||||||||
| Buckley et al. (2013) [63] | ✓ | ||||||||||
| Guitard et al. (2013) [64] | ✓ | ||||||||||
| Novak and Brouwer (2013) [65] | ✓ | ||||||||||
| Samuel et al. (2013) [66] | ✓ | ✓ | |||||||||
| Bosse et al. (2012) [67] | ✓ | ||||||||||
| Hicks-Little et al. (2012) [68] | ✓ | ||||||||||
| Novak and Brouwer (2012) [69] | ✓ | ✓ | |||||||||
| Samuel et al. (2012) [70] | ✓ | ✓ | |||||||||
| Guitard et al. (2011) [71] | ✓ | ||||||||||
| Hicks-Little et al. (2011) [72] | ✓ | ✓ | |||||||||
| Karamanidis and Arampatzis (2011) [73] | ✓ | ✓ | |||||||||
| Leitner et al. (2011) [74] | ✓ | ✓ | |||||||||
| Lin et al. (2011) [75] | ✓ | ||||||||||
| Novak and Brouwer (2011) [76] | ✓ | ||||||||||
| Oh-Park et al. (2011) [77] | ✓ | ✓ | ✓ | ✓ | |||||||
| Reid et al. (2011) [78] | ✓ | ✓ | |||||||||
| Zietz et al. (2011) [79] | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||
| Fujita et al. (2010) [80] | ✓ | ||||||||||
| Liikavainio et al. (2010) [81] | ✓ | ✓ | |||||||||
| Pua et al. (2010) [82] | ✓ | ✓ | |||||||||
| Reid et al. (2010) [83] | ✓ | ||||||||||
| Siegmund et al. (2010) [84] | ✓ | ✓ | |||||||||
| Arcelus et al. (2009) [85] | ✓ | ||||||||||
| Asay et al. (2009) [86] | ✓ | ✓ | |||||||||
| Bertucco and Cesari (2009) [87] | ✓ | ||||||||||
| Hsue and Su (2009) [88] | ✓ | ||||||||||
| Karamanidis and Arampatzis (2009) [89] | ✓ | ||||||||||
| Kim (2009) [90] | ✓ | ✓ | |||||||||
| Misic et al. (2009) [91] | ✓ | ✓ | |||||||||
| Ojha et al. (2009) [92] | ✓ | ||||||||||
| Reeves et al. (2009) [93] | ✓ | ||||||||||
| Schwartz et al. (2009) [94] | ✓ | ✓ | ✓ | ||||||||
| Zietz and Hollands (2009) [95] | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||
| Di Fabio et al. (2008) [96] | ✓ | ✓ | |||||||||
| Larsen et al. (2008) [97] | ✓ | ||||||||||
| Reeves et al. (2008) [98] | ✓ | ✓ | |||||||||
| Guo et al. (2007) [99] | ✓ | ✓ | |||||||||
| Lee and Chou (2007) [100] | ✓ | ||||||||||
| Liikavainio et al. (2007) [101] | ✓ | ||||||||||
| Mian et al. (2007) [102] | ✓ | ||||||||||
| Misic et al. (2007) [103] | ✓ | ✓ | |||||||||
| Murphy et al. (2006) [104] | ✓ | ✓ | |||||||||
| Total N (%) | 3/67 (4.5%) | 30/67 (44.8%) | 64/67 (95.5%) | 0/67 3 (0.0%) | 5/67 (7.5%) | 4/67 (6.0%) | 3/67 (4.5%) | 0/9 3 (0.0%) | 5/9 (55.6%) | 2/9 (22.2%) | 2/9 (22.2%) |
| Name of Study | Falls in all Locations Assessed | Assistive Device Use Recorded | Quantitative Measure of Environmental Features of Stairs | Quantitative Measure of Environmental Features of Bathrooms | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Lighting | Handrail | Stair Rise or Run Dimensions | Uneven Stairs | Tread Edge Contrast | Landing Size | Other 1 | Lighting | Shower or Bathtub Grab Bar | Toilet Grab Bar | Other 2 | |||
| Australian Longitudinal Study of Ageing (1992–2014) [105] | ✓ | ✓ | |||||||||||
| Canadian Longitudinal Study on Aging (2013–present) [106] | ✓ | ✓ | |||||||||||
| Costa Rican Longevity and Health Aging Study (2005–present) [107] | ✓ | ✓ | ✓ | ✓ | |||||||||
| English Longitudinal Study of Aging (2002–present) [108] | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||
| German Ageing Survey (199–present) [109] | ✓ | ✓ | ✓ | ✓ | |||||||||
| Health & Retirement Study (USA; 1992–present) [110] | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||
| Japanese Study on Aging and Retirement (2007–present) [111] | ✓ | ||||||||||||
| Korean Longitudinal Study of Aging (2006–present) [112] | ✓ | ||||||||||||
| Mexican Health and Aging Study (2001–present) [113] | ✓ | ✓ | |||||||||||
| New Zealand Longitudinal Study of Ageing (2006–present) [114] | ✓ | ||||||||||||
| Survey of Health, Ageing, and Retirement in Europe (2004–present) [115] | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||
| Swedish National Study on Aging and Care in Kungsholmen (2001–present) [116,117] | ✓3 | ✓ | |||||||||||
| The Irish Longitudinal Study on Ageing (2009–present) [118] | ✓ | ✓ | ✓ | ||||||||||
| Total N (%) | 13/13 (100.0%) | 10/13 (76.9%) | 0/13 (0.0%) | 4/13 (30.8%) | 0/13 (0.0%) | 0/13 (0.0%) | 0/13 (0.0%) | 0/13 (0.0%) | 4/13 (30.8%) | 0/13 (0.0%) | 2/13 (15.4%) | 0/13 (0.0%) | 5/13 (38.5%) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Edwards, N.; Dulai, J.; Rahman, A. A Scoping Review of Epidemiological, Ergonomic, and Longitudinal Cohort Studies Examining the Links between Stair and Bathroom Falls and the Built Environment. Int. J. Environ. Res. Public Health 2019, 16, 1598. https://doi.org/10.3390/ijerph16091598
Edwards N, Dulai J, Rahman A. A Scoping Review of Epidemiological, Ergonomic, and Longitudinal Cohort Studies Examining the Links between Stair and Bathroom Falls and the Built Environment. International Journal of Environmental Research and Public Health. 2019; 16(9):1598. https://doi.org/10.3390/ijerph16091598
Chicago/Turabian StyleEdwards, Nancy, Joshun Dulai, and Alvi Rahman. 2019. "A Scoping Review of Epidemiological, Ergonomic, and Longitudinal Cohort Studies Examining the Links between Stair and Bathroom Falls and the Built Environment" International Journal of Environmental Research and Public Health 16, no. 9: 1598. https://doi.org/10.3390/ijerph16091598
APA StyleEdwards, N., Dulai, J., & Rahman, A. (2019). A Scoping Review of Epidemiological, Ergonomic, and Longitudinal Cohort Studies Examining the Links between Stair and Bathroom Falls and the Built Environment. International Journal of Environmental Research and Public Health, 16(9), 1598. https://doi.org/10.3390/ijerph16091598





