Calcium Channel Blocker-Associated Chyloperitoneum in Patients Receiving Peritoneal Dialysis: A Systematic Review
Abstract
1. Introduction
2. Methods
2.1. Search Strategy
2.2. Study Selection
2.3. Data Extraction and Analysis
3. Results
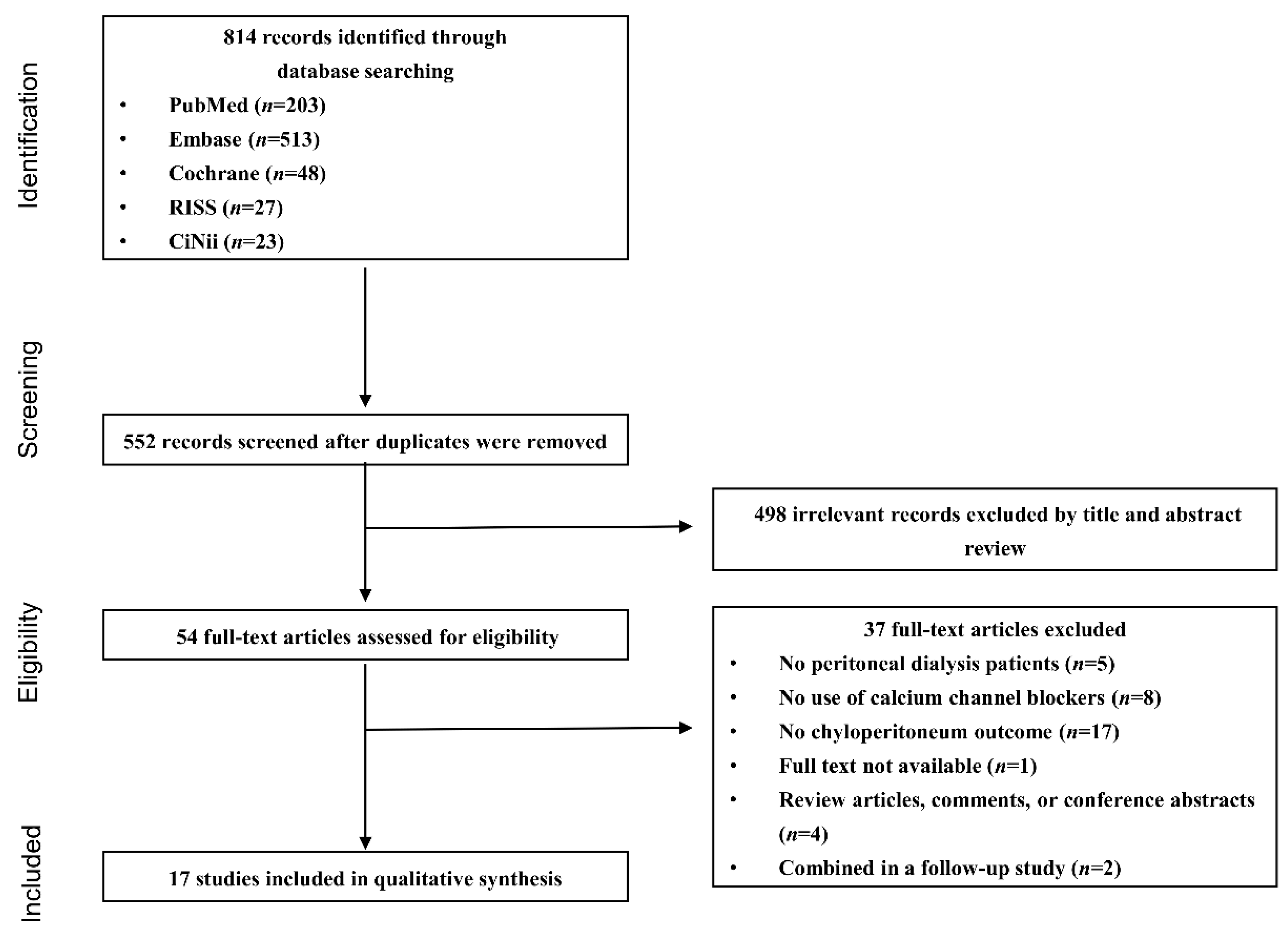
3.1. Literature Search and Study Characteristics
3.2. Characteristics of Chyloperitoneum
3.3. Study Quality
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Sarafidis, P.A.; Persu, A.; Agarwal, R.; Burnier, M.; De Leeuw, P.; Ferro, C.J.; Halimi, J.M.; Heine, G.H.; Jadoul, M.; Jarraya, F.; et al. Hypertension in dialysis patients: A consensus document by the European Renal and Cardiovascular Medicine (EURECA-m) working group of the European Renal Association-European Dialysis and Transplant Association (ERA-EDTA) and the Hypertension and the Kidney working group of the European Society of Hypertension (ESH). Nephrol. Dial. Transplant. 2017, 32, 620–640. [Google Scholar]
- Saran, R.; Li, Y.; Robinson, B.; Ayanian, J.; Balkrishnan, R.; Bragg-Gresham, J.; Chen, J.T.; Cope, E.; Gipson, D.; He, K.; et al. US Renal Data System 2014 Annual Data Report: Epidemiology of Kidney Disease in the United States. Am. J. Kidney Dis. 2015, 66, S1–S305. [Google Scholar] [CrossRef]
- Griffith, T.F.; Chua, B.S.; Allen, A.S.; Klassen, P.S.; Reddan, D.N.; Szczech, L.A. Characteristics of treated hypertension in incident hemodialysis and peritoneal dialysis patients. Am. J. Kidney Dis. 2003, 42, 1260–1269. [Google Scholar] [CrossRef] [PubMed]
- Kestenbaum, B.; Gillen, D.L.; Sherrard, D.J.; Seliger, S.; Ball, A.; Stehman-Breen, C. Calcium channel blocker use and mortality among patients with end-stage renal disease. Kidney Int. 2002, 61, 2157–2164. [Google Scholar] [CrossRef] [PubMed]
- Steinemann, D.C.; Dindo, D.; Clavien, P.-A.; Nocito, A. Atraumatic Chylous Ascites: Systematic Review on Symptoms and Causes. J. Am. Coll. Surg. 2011, 212, 899–905. [Google Scholar] [CrossRef] [PubMed]
- Vasko, J.S.; Tapper, R.I. The surgical significance of chylous ascites. Arch. Surg. 1967, 95, 355–368. [Google Scholar] [CrossRef]
- Press, O.W.; Press, N.O.; Kaufman, S.D. Evaluation and management of chylous ascites. Ann. Intern. Med. 1982, 96, 358–364. [Google Scholar] [CrossRef]
- Lizaola, B.; Bonder, A.; Trivedi, H.D.; Tapper, E.B.; Cardenas, A. Review article: The diagnostic approach and current management of chylous ascites. Aliment. Pharmacol. Ther. 2017, 46, 816–824. [Google Scholar] [CrossRef]
- Saka, Y.; Tachi, H.; Sakurai, H.; Tawada, M.; Sawai, A.; Shimamura, Y.; Mizuno, M.; Maruyama, S.; Matsuo, S.; Ito, Y. Aliskiren-induced chyloperitoneum in a patient on peritoneal dialysis. Perit. Dial. Int. 2012, 32, 111–113. [Google Scholar] [CrossRef] [PubMed]
- Yoshimoto, K.; Saima, S.; Nakamura, Y. Manidipine hydrochloride induced peritoneal fluid turbidity in two patients on continuous peritoneal dialysis. Ther. Apher. Dial. 1991, 24, 1171–1173. [Google Scholar]
- Yoshimoto, K.; Saima, S.; Nakamura, Y.; Nakayama, M.; Kubo, H.; Kawaguchi, Y.; Nishitani, H.; Nakamura, Y.; Yasui, A.; Yokoyama, K.; et al. Dihydropyridine type calcium channel blocker-induced turbid dialysate in patients undergoing peritoneal dialysis. Clin. Nephrol. 1998, 50, 90–93. [Google Scholar]
- Lopez, M.C.V.; Rivas, P.C.G.; Canada, A.L.; Cunquero, J.M.G.; Garcia, E.M. Clinical case: Peritoneal dialysis patient with cloudy peritoneal fluid following administration of calcium antagonists. Nefrologia 2011, 31, 624. [Google Scholar]
- Gupta, S.; Lahori, M.; Bhat, S. Amlodipine induced chylous ascites in a patient undergoing peritoneal dialysis: A case report. Ann. Appl. Biosci. 2016, 3, C50–C52. [Google Scholar]
- Davenport, A. Peritonitis remains the major clinical complication of peritoneal dialysis: The London, UK, peritonitis audit 2002–2003. Perit. Dial. Int. 2009, 29, 297–302. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Dekkers, O.M.; Egger, M.; Altman, D.G.; Vandenbroucke, J.P. Distinguishing case series from cohort studies. Ann. Intern. Med. 2012, 156, 37–40. [Google Scholar] [CrossRef]
- The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-Analyses 2000. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 28 June 2018).
- Mohammadi, S.; Jalaludin, M.Y.; Su, T.T.; Dahlui, M.; Azmi Mohamed, M.N.; Abdul Majid, H. Determinants of Diet and Physical Activity in Malaysian Adolescents: A Systematic Review. Int. J. Environ. Res. Public Health 2019, 16, 603. [Google Scholar] [CrossRef]
- World Health Organization-Uppsala Monitoring Centre. The Use of the WHO-UMC System for Standardised Case Causality Assessment. Available online: https://www.who-umc.org/media/2768/standardised-case-causality-assessment.pdf (accessed on 28 June 2018).
- Naranjo, C.A.; Busto, U.; Sellers, E.M.; Sandor, P.; Ruiz, I.; Roberts, E.A.; Janecek, E.; Domecq, C.; Greenblatt, D.J. A method for estimating the probability of adverse drug reactions. Clin. Pharmacol. Ther. 1981, 30, 239–245. [Google Scholar] [CrossRef]
- Hsiao, P.J.; Lin, H.W.; Sung, C.C.; Wang, C.W.; Chu, P.; Lin, S.H. Incidence and clinical course of lercanidipine-associated cloudy effluent in continuous ambulatory peritoneal dialysis. Clin. Nephrol. 2010, 74, 217–222. [Google Scholar] [CrossRef]
- Topal, C.; Sayarlioglu, H.; Dogan, E.; Erkoc, R.; Soyoral, Y. Cloudy dialysate due to lercanidipine. Nephrol. Dial. Transplant. 2006, 21, 2997–2998. [Google Scholar] [CrossRef][Green Version]
- Yang, W.S.; Huang, J.W.; Chen, H.W.; Tsai, T.J.; Wu, K.D. Lercanidipine-induced chyloperitoneum in patients on peritoneal dialysis. Perit. Dial. Int. 2008, 28, 632–636. [Google Scholar]
- Betancourt-Castellanos, L.; Ponz-Clemente, E.; Otero-Lopez, M.S.; Blasco-Cabanas, C.; Marquina-Parra, D.; Garcia-Garcia, M. Turbid acellular peritoneal fluid and the use of calcium antagonists in peritoneal dialysis. Nefrologia 2013, 33, 377–380. [Google Scholar]
- Kugiyama, A.; Simomura, T.; Miura, H.; Hayano, K.; Fukui, H. A case of continuous ambulatory peritoneal dialysis with significantly increased ultrafiltration and peritoneal fluid turbidity by Manidipine hydrochloride. Ther. Apher. Dial. 1993, 26, 1553–1556. [Google Scholar]
- Kato, A.; Hishida, A.; Nakajima, T.; Ohtake, T.; Furuya, R.; Arai, T.; Kumagai, H.; Kimura, M.; Kaneko, E. Manidipine hydrochloride-induced chyloperitoneum in a patient on continuous ambulatory peritoneal dialysis. Ther. Apher. Dial. 1994, 27, 1185–1188. [Google Scholar]
- Fujii, Y.; Horii, Y.; Kishimoto, K.; Iwano, M.; Dohi, K. Three cases of continuous ambulatory peritoneal dialysis with chylous peritoneal dialysate. Ther. Apher. Dial. 1995, 28, 1179–1184. [Google Scholar]
- Tsurusaki, T.; Kiyokawa, S.; Miyata, Y.; Sawase, K.; Nishikido, M.; Matsuya, F.; Kanetake, H.; Saito, Y. Manidipine hydrochloride-induced chyloperitoneum in a cadaver renal transplant patient on continuous ambulatory peritoneal dialysis. Ther. Apher. Dial. 1995, 28, 383–387. [Google Scholar]
- Roh, H.J.; Yoo, T.H.; Ryu, D.R.; Hwang, J.H.; Song, H.Y.; Noh, H.J.; Shin, S.K.; Kang, S.W.; Choi, K.H.; Han, D.S.; et al. A Case of Drug-Induced Chylous Ascites in a Patient Undergoing Continuous Ambulatory Peritoneal Dialysis. Kidney. Res. Clin. Pract. 1999, 18, 1013–1016. [Google Scholar]
- Tsao, Y.T.; Chen, W.L. Calcium channel blocker-induced chylous ascites in peritoneal dialysis. Kidney Int. 2009, 75, 868. [Google Scholar] [CrossRef]
- Ram, R.; Swarnalatha, G.; Pai, B.H.S.; Rao, C.S.S.; Dakshinamurty, K.V. Cloudy Peritoneal Fluid Attributable to Non-Dihydropyridine Calcium Channel Blocker. Perit. Dial. Int. 2012, 32, 110–111. [Google Scholar] [CrossRef] [PubMed]
- Moreiras-Plaza, M.; Fernández-Fleming, F.; Martín-Báez, I.; Blanco-García, R.; Beato-Coo, L. Non-infectious cloudy peritoneal fluid secondary to lercanidipine. Nefrologia 2014, 34, 683–685. [Google Scholar]
- Nicotera, R.; Chiarella, S.; Placida, G.; De Paola, L.; D’Onofrio, G.; Panzino, M.T.; Panzino, A.; Mileti, S.; Pinciaroli, A.R.; Coppolino, G. Possible role of Lercanidipine in Chiloperitoneum occurrence in CAPD: A case-report. G. Ital. Nefrol. 2018, 35, 6. [Google Scholar]
- Mallett, T.; Culligan, C.; Plant, N.; McKeever, K. Chyloperitoneum post peritonitis and the role of calcium channel blockade in an infant. Research 2014, 1, 995. [Google Scholar] [CrossRef]
- Tsauo, J.; Shin, J.H.; Han, K.; Yoon, H.K.; Ko, G.Y.; Ko, H.K.; Gwon, D.I. Transjugular Intrahepatic Portosystemic Shunt for the Treatment of Chylothorax and Chylous Ascites in Cirrhosis: A Case Report and Systematic Review of the Literature. J. Vasc. Interv. Radiol. 2016, 27, 112–116. [Google Scholar] [CrossRef]
- Baiocchi, G.; Faloppa, C.C.; Araujo, R.L.; Fukazawa, E.M.; Kumagai, L.Y.; Menezes, A.N.; Badiglian-Filho, L. Chylous ascites in gynecologic malignancies: Cases report and literature review. Arch. Gynecol. Obstet. 2010, 281, 677–681. [Google Scholar] [CrossRef]
- Cardenas, A.; Chopra, S. Chylous ascites. Am. J. Gastroenterol. 2002, 97, 1896–1900. [Google Scholar] [CrossRef]
- McKeage, K.; Scott, L.J. Manidipine: A review of its use in the management of hypertension. Drugs 2004, 64, 1923–1940. [Google Scholar] [CrossRef]
- van Zwieten, P.A. The pharmacological properties of lipophilic calcium antagonists. Blood. Press. Suppl. 1998, 2, 5–9. [Google Scholar] [CrossRef]
- Campisi, C.; Bellini, C.; Eretta, C.; Zilli, A.; da Rin, E.; Davini, D.; Bonioli, E.; Boccardo, F. Diagnosis and management of primary chylous ascites. J. Vasc. Surg. 2006, 43, 1244–1248. [Google Scholar] [CrossRef]
- Jungst, D.; Gerbes, A.L.; Martin, R.; Paumgartner, G. Value of ascitic lipids in the differentiation between cirrhotic and malignant ascites. Hepatology 1986, 6, 239–243. [Google Scholar] [CrossRef]
- Basualdo, J.E.; Rosado, I.A.; Morales, M.I.; Fernandez-Ros, N.; Huerta, A.; Alegre, F.; Landecho, M.F.; Lucena, J.F. Lercanidipine-induced chylous ascites: Case report and literature review. J. Clin. Pharm. Ther. 2017, 42, 638–641. [Google Scholar] [CrossRef]
| Study | Country | Study Design | Number of Patients | Drug Name | Dose (mg) | Prevalence of CP | Age (mean ± SD, year) | Sex (men, %) | TGs in Dialysate (mean ± SD, mg/dL) | TGs in Serum (mean ± SD, mg/dl) | Duration of PD Treatment (mean ± SD, months) | Time-to-Onset of CP (mean ± SD, days) | Result of Withdrawal | Result of Rechallenge | QA Score (0–7) a | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| T | Non-T | T | Non-T | T | Non-T | T | Non-T | T | Non-T | |||||||||||
| Hsiao 2010 [21] | Taiwan | P | 40 | Lercanidipine | 5 | 22.5% (9/40) | 39.4 ± 14.3 | 47.5 ± 12.5 | 44.4 | 38.7 | 19.3 ± 6.3 | 0 | 123 ± 43 | 151 ± 52 | 33 ± 21 | 39 ± 24 | 1.2 ± 0.4 | Dialysate clear within 24 h | Cloudy again | 5 |
| Yang 2008 [23] | Taiwan | R | 14 | Lercanidipine | - | 57.14% (8/14) | 52.6 ± 18.5 | 46.0 ± 10.8 | 62.5 | 33.3 | 128.4 | 6.5 | 218.0 ± 176.6 | 115.8 ± 3.2 | 20.4 ± 21.6 | 33.6 ± 24 | 38.5 ± 60.8 | Dialysate clear within 24 h | Cloudy again | 6 |
| Topal 2006 b [22] | Turkey | R | 23 | Lercanidipine | 5 | 13.04% (3/23) | 45.3 ± 17.6 | 39.1 | - | - | 15.9±11.6 | 1 | - | - | 3 | |||||
| Yoshimoto 1998 [11] | Japan | R | 251 | Various CCBs c | - | 7.57% (19/251) | 55 ± 17 | 50 ± 12 | 52.6 | 67.7 | - | - | - | - | Dialysate clear | Cloudy again | 4 | |||
| Study | Country | Study Design | Number of Patients | Drug Name | Dose | Age | Sex | TGs in Dialysate (mg/dL) | TGs in Serum (mg/dL) | Duration of PD Treatment | Time-to-Onset of CP | Result of Withdrawal | Result of Rechallenge | Causality a |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Betancourt 2013 [24] | Spain | Case series | 4 | Manidipine | - | 60 y | M | 52 | - | 2 mo | - | Dialysate clear | - | Probable |
| Verapamil | - | 41 y | M | 9 | - | 4 mo | - | Dialysate clear | - | Probable | ||||
| Manidipine | - | 70 y | F | 745 | - | 4 d | - | Dialysate clear | - | Probable | ||||
| Manidipine | - | 52 y | M | 452 | - | 5 mo | - | Dialysate clear | - | Probable | ||||
| Nicotera 2018 [33] | Italy | Case report | 1 | Lercanidipine | 20 mg | 53 y | - | 150 | - | 2 y | - | Dialysate clear immediately | - | Probable |
| Gupta 2016 [13] | India | Case report | 1 | Amlodipine | 5 mg | 65 y | M | 293.8 | 88.4 | 8 d | 3 d | Dialysate clear within 24 h | Not-rechallenged | Probable |
| Moreiras 2014 [32] | Spain | Case report | 1 | Lercanidipine | 5 mg | 59 y | F | 20 | 182 | - | 3 d | Dialysate clear within 24 h | Cloudy again | Certain (or definite) |
| Mallett 2012 [34] | Northern Ireland | Case report | 1 | Amlodipine | 0.6 mg/kg | 7 mo | M | 57.5 | 164.6 | 5 mo | 2 d | Dialysate clear before withdrawal b | TG slightly increased in dialysate | Probable |
| Ram 2012 [31] | India | Case report | 1 | Diltiazem | - | 55y | M | 61 | 134 | - | - | Dialysate clear after 1 d | Cloudy again | Certain (or definite) |
| Lopez 2011 [12] | Spain | Case report | 1 | Manidipine (from nifedipine OROS) | - | 44 y | F | 119 | 76 | - | 1 d | Dialysate clear within 24 h | - | Probable |
| Tsao 2009 [30] | Taiwan | Case report | 1 | Lercanidipine | 10 mg | 41 y | F | 251 | - | 2 wk | 3 d | Dialysate clear within 24 h | Cloudy again | Certain (or definite) |
| Roh 1999 [29] | Korea | Case report | 1 | Manidipine | 40 mg | 47 y | M | 28 | 111 | 9 d | 1 d | Dialysate clear after 1 d | Not-rechallenged | Probable |
| Tsurusaki 1995 [28] | Japan | Case report | 1 | Manidipine | 20 mg | 36 y | M | 27.2 | - | 32 mo | 4 d | Dialysate clear within 24 h | - | Probable |
| Fujii 1995 [27] | Japan | Case report | 1 | Manidipine | 10 mg | 58 y | M | 26 | - | 2 mo | 3 d | Dialysate clear within 24 h | - | Probable |
| Kato 1994 [26] | Japan | Case report | 1 | Manidipine | 40 mg (From 20 mg) | 51 y | F | 29 | 121 | 4 mo | 1 d | Dialysate clear within 12 h | - | Probable |
| Atsuko 1993 [25] | Japan | Case report | 1 | Manidipine | 20 mg | 44 y | M | 24 | 81 | 6 mo | 8 h | Dialysate clear within 1 d | Cloudy again | Certain (or definite) |
| Study | Criteria of modified Newcastle–Ottawa Scale | ||||||
|---|---|---|---|---|---|---|---|
| Prior Criteria; Representativeness | Ascertainment of Exposure | Starting Condition Prior to Outcome | Adjustment for Confounding Factors a | Ascertainment of Outcome | Sufficiency of Follow-Up Period | Adequacy of Follow-Up | |
| Hsiao 2010 [21] | Lack of detailed description of selection criteria | Medical records | Chyloperitoneum was not pre sent | Infection and other causes | Standardised assessment | No statement | Complete follow-up |
| Yang 2008 [23] | Lack of detailed description of selection criteria | Medical records | Chyloperitoneum was not present | Infection and other causes | Standardised assessment | Follow-up period ≥ 30 d | More than 90% |
| Topal 2006 [22] | Unclear | Medical records | Chyloperitoneum was not present | Infection | Visual observation; Turbidity of peritoneal dialysate | Not sufficient; 1 d | Complete follow-up |
| Yoshimoto 1998 [11] | Participant selection by researchers | Medical records | Chyloperitoneum was not present | Infection and other causes | Standardised assessment | Not sufficient; 2 d | Subsequent observation by a biochemical test was performed on 53% of the patients |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, S.; Yu, Y.M.; Kwon, J.; Yoo, H.; Jung, S.H.; Lee, E. Calcium Channel Blocker-Associated Chyloperitoneum in Patients Receiving Peritoneal Dialysis: A Systematic Review. Int. J. Environ. Res. Public Health 2019, 16, 1333. https://doi.org/10.3390/ijerph16081333
Kim S, Yu YM, Kwon J, Yoo H, Jung SH, Lee E. Calcium Channel Blocker-Associated Chyloperitoneum in Patients Receiving Peritoneal Dialysis: A Systematic Review. International Journal of Environmental Research and Public Health. 2019; 16(8):1333. https://doi.org/10.3390/ijerph16081333
Chicago/Turabian StyleKim, Seungyeon, Yun Mi Yu, Jeongyoon Kwon, Hyejin Yoo, Sun Hoi Jung, and Euni Lee. 2019. "Calcium Channel Blocker-Associated Chyloperitoneum in Patients Receiving Peritoneal Dialysis: A Systematic Review" International Journal of Environmental Research and Public Health 16, no. 8: 1333. https://doi.org/10.3390/ijerph16081333
APA StyleKim, S., Yu, Y. M., Kwon, J., Yoo, H., Jung, S. H., & Lee, E. (2019). Calcium Channel Blocker-Associated Chyloperitoneum in Patients Receiving Peritoneal Dialysis: A Systematic Review. International Journal of Environmental Research and Public Health, 16(8), 1333. https://doi.org/10.3390/ijerph16081333




