Does Sleep Mediate the Association between School Pressure, Physical Activity, Screen Time, and Psychological Symptoms in Early Adolescents? A 12-Country Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Sample and Protocol
2.2. Measures
2.3. Statistical Analysis
3. Results
3.1. Descriptive Characteristics of the Analytic Sample
3.2. Direct Relationship of School Pressure, Physical Activity, and Screen Time with Psychological Symptoms
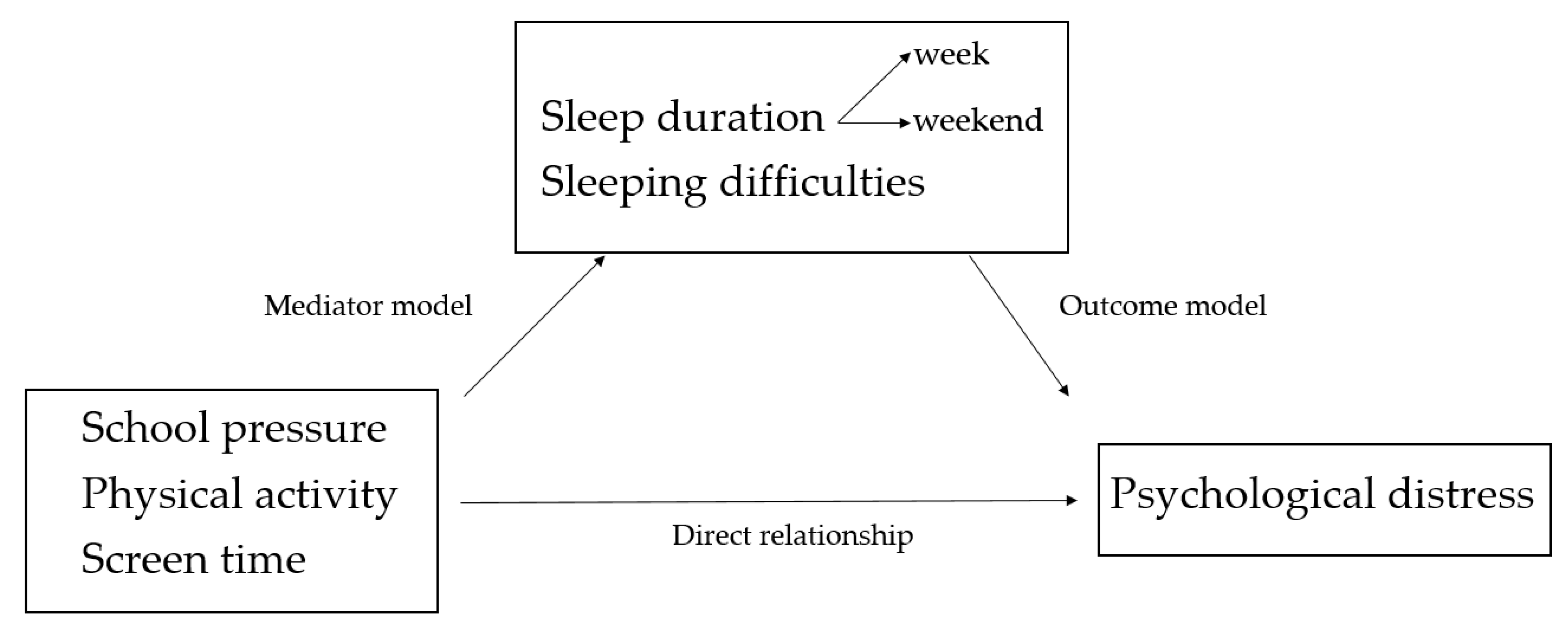
3.3. Mediation Analysis
3.3.1. Sleep Duration on Weekdays
3.3.2. Sleep Duration on Weekend Days
3.3.3. Difficulties in Getting to Sleep
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Braddick, F.; Carral, V.; Jenkins, R.; Jané-Llopis, E. Child and Adolescent Mental Health in Europe: Infrastructures, Policy and Programmes; European Communities: Luxembourg, 2009. [Google Scholar]
- Collishaw, S.; Maughan, B.; Goodman, R.; Pickles, A. Time trends in adolescent mental health. J. Child Psychol. Psychiatr. 2004, 45, 1350–1362. [Google Scholar] [CrossRef]
- Balazs, J.; Miklósi, M.; Keresztény, Á.; Apter, A.; Bobes, J.; Brunner, R.; Corcoran, P.; Cosman, D.; Haring, C.; Kahn, J.-P.; et al. P-259-Prevalence of adolescent depression in Europe. Eur. Psychiatr. 2012, 27 (Suppl. 1), 1. [Google Scholar] [CrossRef]
- Kessler, R.C.; Amminger, G.P.; Aguilar-Gaxiola, S.; Alonso, J.; Lee, S.; Ustün, T.B. Age of onset of mental disorders: A review of recent literature. Curr. Opin. Psychiatry 2007, 20, 359–364. [Google Scholar] [CrossRef] [PubMed]
- Mazur, J.; Nalecz, H.; Kleszczewska, D.; Malkowska-Szkutnik, A.; Borraccino, A. Behavioural factors enhancing mental health—Preliminary results of the study on its association with physial activity in 15 to 16 year olds. Dev. Period Med. 2016, 20, 315–324. [Google Scholar]
- Natvig, G.K.; Albrektsen, G.; Qvarnstrøm, U. Associations between psychosocial factors and happiness among school adolescents. Int. J. Nurs. Pract. 2003, 9, 166–175. [Google Scholar] [CrossRef]
- Undheim, A.M.; Sund, A.M. School factors and the emergence of depressive symptoms among young Norwegian adolescents. Eur. Child Adolesc. Psychiatry 2005, 14, 446–453. [Google Scholar] [CrossRef]
- Biddle, A. Physical activity and mental health in children and adolescents: A review of reviews. Br. J. Sports Med. 2011, 45, 886–895. [Google Scholar] [CrossRef]
- Khouja, J.N.; Munafò, M.R.; Tilling, K.; Wiles, N.J.; Joinson, C.; Etchells, P.J.; John, A.; Hayes, F.M.; Gage, S.H.; Cornish, R.P. Is screen time associated with anxiety or depression in young people? Results from a UK birth cohort. BMC Public Health 2019, 19, 82. [Google Scholar] [CrossRef]
- McMahon, E.M.; Corcoran, P.; O’Regan, G.; Keeley, H.; Cannon, M.; Carli, V.; Wasserman, C.; Hadlaczky, G.; Sarchiapone, M.; Apter, A.; et al. Physical activity in European adolescents and associations with anxiety, depression and well-being. Eur. Child Adolesc. Psychiatry 2017, 26, 111–122. [Google Scholar] [CrossRef]
- Cain, N.; Gradisar, M. Electronic media use and sleep in school-aged children and adolescents: A review. Sleep Med. 2010, 11, 735–742. [Google Scholar] [CrossRef]
- Van den Bulck, J. Adolescent use of mobile phones for calling and for sending text messages after lights out: Results from a prospective cohort study with a one-year follow-up. Sleep 2007, 30, 1220–1223. [Google Scholar] [CrossRef] [PubMed]
- Hale, L.; Guan, S. Screen time and sleep among school-aged children and adolescents: A systematic literature review. Sleep Med. Rev. 2015, 21, 50–58. [Google Scholar] [CrossRef]
- Gerber, M.; Pühse, U. “Don’t crack under pressure!”—Do leisure time physical activity and self-esteem moderate the relationship between school-based stress and psychosomatic complaints? J. Psychosom. Res. 2008, 65, 363–369. [Google Scholar] [CrossRef] [PubMed]
- Foti, K.E.; Eaton, D.K.; Lowry, R.; McKnight-Ely, L.R. Sufficient Sleep, Physical Activity, and Sedentary Behaviors. Am. J. Prev. Med. 2011, 41, 596–602. [Google Scholar] [CrossRef] [PubMed]
- Marino, C.; Vieno, A.; Lenzi, M.; Borraccino, A.; Lazzeri, G.; Lemma, P. Computer Use, Sleep Difficulties, and Psychological Symptoms Among School-Aged Children: The Mediating Role of Sleep Difficulties. Int. J. Sch. Health 2016, in press. [Google Scholar] [CrossRef]
- Nuutinen, T.; Roos, E.; Ray, C.; Villberg, J.; Valimaa, R.; Rasmussen, M.; Holstein, B.; Godeau, E.; Beck, F.; Léger, D.; et al. Computer use, sleep duration and health symptoms: A cross-sectional study of 15-year olds in three countries. Int. J. Public Health 2014, 59, 619–628. [Google Scholar] [CrossRef] [PubMed]
- Lemola, S.; Perkinson-Gloor, N.; Brand, S.; Dewald-Kaufmann, J.F.; Grob, A. Adolescents’ electronic media use at night, sleep disturbance, and depressive symptoms in the smartphone age. J. Youth Adolesc. 2015, 44, 405–418. [Google Scholar] [CrossRef]
- Kessler, R.; Berglund, P.; Demler, O.; Jin, R.; Merikangas, K.R.; Walters, E.E. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch. Gen. Psychiatry 2005, 62, 593–602. [Google Scholar] [CrossRef]
- Currie, C.; Inchley, J.; Molcho, M.; Lenzi, M.; Veselska, Z.; Wild, F. Health Behaviour in School-Aged Children (HBSC) Study Protocol: Background, Methodology and Mandatory items for the 2013/14 Survey; Child and Adolescent Health Research Unit (CAHRU): St Andrews, UK, 2014. [Google Scholar]
- Roberts, C.; Freeman, J.; Samdal, O.; Schnohr, C.W.; de Looze, M.E.; Nic Gabhainn, S.; Iannotti, R.; Rasmussen, M.; International HBSC Study Group. The Health Behaviour in School-aged Children (HBSC) study: Methodological developments and current tensions. Int. J. Public Health 2009, 54 (Suppl. 2), 140–150. [Google Scholar] [CrossRef] [PubMed]
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Currie, C.E.; Elton, R.A.; Todd, J.; Platt, S. Indicators of socioeconomic status for adolescents: The WHO Health Behaviour in School-aged Children Survey. Health Educ. Res. 1997, 12, 385–397. [Google Scholar] [CrossRef]
- Hartley, J.E.K.; Levin, K.; Currie, C. A new version of the HBSC Family Affluence Scale—FAS III: Scottish Qualitative Findings from the International FAS Development Study. Child Indic. Res. 2016, 9, 233–245. [Google Scholar] [CrossRef]
- Biddle, S.J.; Gorely, T.; Pearson, N.; Bull, F.C. An assessment of self-reported physical activity instruments in young people for population surveillance: Project ALPHA. Int. J. Behav. Nutr. Phys. Act. 2011, 8, 1. [Google Scholar] [CrossRef]
- Prochaska, J.J.; Sallis, J.F.; Long, B. A physical activity screening measure for use with adolescents in primary care. Arch. Pediatr. Adolesc. Med. 2001, 155, 554–559. [Google Scholar] [CrossRef] [PubMed]
- Rey-López, J.P.; Vicente-Rodriguez, G.; Ortega, F.B.; Ruiz, J.R.; Martinez-Gómez, D.; De Henauw, S.; Manios, Y.; Molnar, D.; Polito, A.; Verloigne, M.; et al. Sedentary patterns and media availability in European adolescents: The HELENA study. Prev. Med. 2010, 51, 50–55. [Google Scholar] [CrossRef]
- Gariepy, G.; McKinnon, B.; Sentenac, M.; Elgar, F.J. Validity and Reliability of a Brief Symptom Checklist to Measure Psychological Health in School-Aged Children. Child Indicators Res. 2016, 9, 471–484. [Google Scholar] [CrossRef]
- Wolfson, A.R.; Carskadon, M.A.; Acebo, C.; Seifer, R.; Fallone, G.; Labyak, S.E.; Martin, J.L. Evidence for the validity of a sleep habits survey for adolescents. Sleep 2003, 26, 213–216. [Google Scholar] [CrossRef] [PubMed]
- Imai, K.; Keele, L.; Tingley, D. A general approach to causal mediation analysis. Psychol. Methods 2010, 15, 309–334. [Google Scholar] [CrossRef] [PubMed]
- Tingley, D.; Yamamoto, T.; Hirose, K.; Keele, L.; Imai, K. Mediation: R Package for Causal Mediation Analysis; UCLA Statistics/American Statistical Association: Los Angeles, CA, USA, 2014. [Google Scholar]
- Cairns, K.E.; Yap, M.B.; Pilkington, P.D.; Jorm, A.F. Risk and protective factors for depression that adolescents can modify: A systematic review and meta-analysis of longitudinal studies. J. Affect. Disord. 2014, 169, 61–75. [Google Scholar] [CrossRef] [PubMed]
- Lovato, N.; Gradisar, M. A meta-analysis and model of the relationship between sleep and depression in adolescents: Recommendations for future research and clinical practice. Sleep Med. Rev. 2014, 18, 521–529. [Google Scholar] [CrossRef]
- Bei, B.; Wiley, J.F.; Allen, N.B.; Trinder, J. A cognitive vulnerability model of sleep and mood in adolescents under naturalistically restricted and extended sleep opportunities. Sleep 2015, 38, 453. [Google Scholar] [CrossRef] [PubMed]
- Dewald, J.F.; Meijer, A.M.; Oort, F.J.; Kerkhof, G.A.; Bögels, S.M. The influence of sleep quality, sleep duration and sleepiness on school performance in children and adolescents: A meta-analytic review. Sleep Med. Rev. 2010, 14, 179–189. [Google Scholar] [CrossRef]
- Murberg, T.A.; Bru, E. School-Related Stress and Psychosomatic Symptoms among Norwegian Adolescents. Sch. Psychol. Int. 2004, 25, 317–332. [Google Scholar] [CrossRef]
- Thomsen, D.K.; Mehsen, M.Y.; Christensen, S.; Zachariae, R. Rumination—Relationship with negative mood and sleep quality. Pers. Individ. Differ. 2003, 34, 1293–1301. [Google Scholar] [CrossRef]
- Driver, H.S.; Taylor, S.R. Exercise and sleep. Sleep Med. Rev. 2000, 4, 387–402. [Google Scholar] [CrossRef]
- Youngstedt, S.D.; Kripke, D.F.; Elliott, J.A. Is sleep disturbed by vigorous late-night exercise? Med. Sci. Sports Exerc. 1999, 31, 864–869. [Google Scholar] [CrossRef] [PubMed]
- Asare, M. Sedentary Behaviour and Mental Health in Children and Adolescents: A Meta-analysis. J. Child Adolesc. Behav. 2015, 3. [Google Scholar] [CrossRef]
- Hamer, M.; Yates, T.; Sherar, L.B.; Clemes, S.A.; Shankar, A. Association of after school sedentary behaviour in adolescence with mental wellbeing in adulthood. Prev. Med. 2016, 87, 6–10. [Google Scholar] [CrossRef]
- Higuchi, S.; Motohashi, Y.; Liu, Y.; Maeda, A. Effects of playing a computer game using a bright display on presleep physiological variables, sleep latency, slow wave sleep and REM sleep. J. Sleep Res. 2005, 14, 267–273. [Google Scholar] [CrossRef]
- Rosen, L.D.; Lim, A.F.; Felt, J.; Carrier, L.M.; Cheever, N.A.; Lara-Ruiz, J.M.; Mendoza, J.S.; Rokkum, J. Media and technology use predicts ill-being among children, preteens and teenagers independent of the negative health impacts of exercise and eating habits. Comput. Hum. Behav. 2014, 35, 364–375. [Google Scholar] [CrossRef]
- Chen, M.-Y.; Wang, E.K.; Jeng, Y.-J. Adequate sleep among adolescents is positively associated with health status and health-related behaviors. BMC Public Health 2006, 6, 59. [Google Scholar] [CrossRef] [PubMed]
- Das, J.K.; Salam, R.A.; Lassi, Z.S.; Khan, M.N.; Mahmood, W.; Patel, V.; Bhutta, A.Z. Interventions for Adolescent Mental Health: An Overview of Systematic Reviews. J. Adolesc. Health 2016, 59 (Suppl. 4), S49–S60. [Google Scholar] [CrossRef] [PubMed]
- Lovibond, P.F.; Lovibond, S.H. The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav. Res. 1995, 33, 335–343. [Google Scholar] [CrossRef]
- Ravens-Sieberer, U.; Erhart, M.; Rajmil, L.; Herdman, M.; Auquier, P.; Bruil, J.; Power, M.; Duer, W.; Abel, T.; Czemy, L.; et al. Reliability, construct and criterion validity of the KIDSCREEN-10 score: A short measure for children and adolescents’ well-being and health-related quality of life. Qual. Life Res. 2010, 19, 1487–1500. [Google Scholar] [CrossRef] [PubMed]
| Variable | Question | Response Categories | Data Processing | Reference |
|---|---|---|---|---|
| Socio-economic status (SES) | Family Affluence Scale III consisting of six items: number of cars family owns, having own bedroom, number of computers family owns, number of bathrooms at home, having a dishwasher at home, and number of travels for a vacation last year. | Number of cars family owns: None (0), one (1), two or more (2) Own bedroom: No (0), yes (1) Number of computers: None (0), one (1), two (2), more than two (3) Number of bathrooms: None (0), one (1), two (2), more than two (3) Dishwasher: No (0), yes (1) Family holidays: Not at all (0), once (1), twice (2), more than twice (3) | A sum score was calculated (range 0–9) and transformed into a continuous variable by performing a ridit transformation (range 0–1). In that way, the Family Affluence Scale indicates the relative material position within society (i.e. country). The scale also takes population heterogeneity for age and gender into account. Higher values reflect higher SES. | Material affluence was used as a measure of SES [23], using the Family Affluence Scale III [24]. The sum score of the six items showed high test–retest reliability (r = 0.90) and consistency between child and parent report (r = 0.80) |
| School pressure | “How pressured do you feel by the schoolwork you have to do?” | Not at all or a little (1), some (2), a lot (3) | ||
| Physical activity | “Over the past 7 days, on how many days were you physically active for a total of at least 60 min per day?” | None (0) to seven (7) days | Biddle et al. [25] report a reasonable validity and moderate reliability for this index. Prochaska et al. [26] validated this measure for use with children and adolescents. | |
| Screen time | “How many h a day, in your free time, do you usually spend watching television (TV), videos (including YouTube or similar services), DVDs, and other entertainment on a screen?”; “How many h a day, in your free time, do you usually spend playing games on a computer, games console, tablet (like iPad), smartphone or other electronic device (not including moving or fitness games)?”; and “How many h a day, in your free time, do you usually spend using electronic devices such as computers, tablets (like iPad) or smart phones for other purposes, for example, homework, emailing, tweeting, Facebook, chatting, surfing the Internet?” | None at all (1), “half an hour a day” (2), “1 h a day” (3), “2 h a day” (4), “3 h a day” (5), “4 h a day” (6), “5 h a day” (7), “6 h a day” (8), “7 h or more a day” (9) | Assessed separately for week- and weekend days. Response categories were transformed to number of h using the midpoint method. To represent the overall amount of screen time per day, the three screen time behaviours were summed for week- and weekend days separately. Finally, the mean screen time on weekdays and weekends together was calculated ((5 × weekdays) + (2 × weekend days)/7). | Rey-López JP et al (2010) [27] |
| Psychological symptoms | “In the last 6 months: how often have you had the following… (1) feeling low, (2) irritability or bad temper, and (3) feeling nervous?” | Five: “about every day” (1), “more than once a week” (2), “about every week” (3), “about every month” (4), and “rarely or never” (5) | Response categories were reversely scored to facilitate interpretation of the results. | Three psychological symptoms of the Health Behaviour in School-Aged Children (HBSC) Symptom Check List (HBSC-SCL) were used [28]. The HBSC-SCL consists of four questions on somatic and four questions on psychological symptom load. The internal validity of the psychological subscale was good (α = 0.78) [28]. When leaving out the symptom of sleep onset difficulties from the psychological symptom load generated by the HBSC-SCL, the internal consistency of the psychological dimension slightly improved (Cronbach’s alpha increased from 0.78 to 0.79). |
| Sleep onset difficulties | “In the last 6 months: how often have you had the following… difficulties in getting to sleep?” | Five: “about every day” (1), “more than once a week” (2), “about every week” (3), “about every month” (4), and “rarely or never” (5) | Response categories were reversely scored to facilitate interpretation of the results. | This is the fourth psychological symptom of the HBSC-SCL [28]. |
| Sleep duration week | “When do you usually go to bed if you have to go to school the next morning?” | Eleven: ranging from “no later than 21.00” to “02.00 or later” | Response categories were transformed to h using the midpoint method. | Wolfson et al. found that school and weekend nights survey variables were significantly correlated with actigraphy and diary variables [29]. |
| “When do you usually wake up on school mornings?” | Seven: ranging from no later than 05.00” to “08.00 or later” | Sleep duration was calculated by subtracting the reported bedtime from the wake-up time. | ||
| Sleep duration weekend | “When do you usually go to bed at weekends or during holidays?” | Fifteen: ranging from “no later than 21.00” to “04.00 or later” | ||
| “When do you usually wake up at weekends or during holidays?” | Fifteen: ranging from “no later than 05.00” to “14.00 or later” |
| Sleep Duration on Weekdays | Sleep Duration on Weekend Days | Sleep Onset Difficulties | ||
|---|---|---|---|---|
| Mediator model 1 | β (95% CI) | β (95% CI) | β (95% CI) | |
| School pressure (ref. none or a little) | Some | −0.09 (−0.11; −0.07) * | −0.08 (−0.11; −0.04) * | 0.32 (0.30; 0.35) * |
| A lot | −0,25 (−0.28; −0.22) * | -0.20 (-0.24; -0.15) * | 0.73 (0.69; 0.77) * | |
| Physical activity | −0.01 (−0.01; −0.01) * | −0.03 (−0.04; −0.02) * | −0.03 (−0.03; −0.02) * | |
| Screen time | −0.07 (−0.07; −0.07) * | −0.05 (−0.05; −0.05) * | 0.04 (0.04; 0.05) * | |
| Outcome model 2 | −0.13 (−0.13; −0.12) * | −0.035 (−0.04; −0.03) * | 0.30 (0.30; −0.31) * | |
| Mediating relationship | ||||
| School pressure (ref. none or a little) | Some | 0.01 (0.01; 0.01) * | 0.003 (0.001; 0.004) * | 0.10 (0.09; 0.11) * |
| A lot | 0.03 (0.03; 0.04) * | 0.007 (0.005; 0.009) * | 0.22 (0.21; 0.23) * | |
| Physical activity | 0.001 (0.001; 0.002) * | 0.001 (0.001; 0.001) * | −0.01 (−0.01; −0.01) * | |
| Screen time | 0.009 (0.008; 0.009) * | 0.002 (0.001; 0.002) * | 0.01 (0.01; 0.01) * | |
| Direct relationship 3 | ||||
| School pressure (ref. none or a little) | Some | 0.39 (0.37; 0.41) * | 0.40 (0.38; 0.42) * | 0.30 (0.28; 0.32) * |
| A lot | 0.83 (0.80; 0.85) * | 0.85 (0.83; 0.89) * | 0.64 (0.61; 0.66) * | |
| Physical activity | −0.03 (−0.03; −0.02) * | −0.03 (−0.03; −0.02) * | −0.02 (−0.02; −0.01) * | |
| Screen time | 0.03 (0.03; 0.03) * | 0.04 (0.04; 0.04) * | 0.03 (0.02; 0.03) * | |
| % mediated | % | % | % | |
| School pressure (ref. none or a little) | Some | 2.85 (2.21; 3.56) * | 0.66 (0.37; 1.02) * | 24.60 (22.28; 26.58) * |
| A lot | 3.62 (3.15; 4.08) * | 0.79 (0.60; 1.03) * | 25.80 (24.60; 27.20) * | |
| Physical activity | Inconsistent mediation | Inconsistent mediation | 33.56 (26.36; 41.61) * | |
| Screen time | 22.16 (20.29; 24.30) * | 4.49 (3.73; 5.37) * | 34.13 (31.74; 36.63) * | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vandendriessche, A.; Ghekiere, A.; Van Cauwenberg, J.; De Clercq, B.; Dhondt, K.; DeSmet, A.; Tynjälä, J.; Verloigne, M.; Deforche, B. Does Sleep Mediate the Association between School Pressure, Physical Activity, Screen Time, and Psychological Symptoms in Early Adolescents? A 12-Country Study. Int. J. Environ. Res. Public Health 2019, 16, 1072. https://doi.org/10.3390/ijerph16061072
Vandendriessche A, Ghekiere A, Van Cauwenberg J, De Clercq B, Dhondt K, DeSmet A, Tynjälä J, Verloigne M, Deforche B. Does Sleep Mediate the Association between School Pressure, Physical Activity, Screen Time, and Psychological Symptoms in Early Adolescents? A 12-Country Study. International Journal of Environmental Research and Public Health. 2019; 16(6):1072. https://doi.org/10.3390/ijerph16061072
Chicago/Turabian StyleVandendriessche, Ann, Ariane Ghekiere, Jelle Van Cauwenberg, Bart De Clercq, Karlien Dhondt, Ann DeSmet, Jorma Tynjälä, Maïté Verloigne, and Benedicte Deforche. 2019. "Does Sleep Mediate the Association between School Pressure, Physical Activity, Screen Time, and Psychological Symptoms in Early Adolescents? A 12-Country Study" International Journal of Environmental Research and Public Health 16, no. 6: 1072. https://doi.org/10.3390/ijerph16061072
APA StyleVandendriessche, A., Ghekiere, A., Van Cauwenberg, J., De Clercq, B., Dhondt, K., DeSmet, A., Tynjälä, J., Verloigne, M., & Deforche, B. (2019). Does Sleep Mediate the Association between School Pressure, Physical Activity, Screen Time, and Psychological Symptoms in Early Adolescents? A 12-Country Study. International Journal of Environmental Research and Public Health, 16(6), 1072. https://doi.org/10.3390/ijerph16061072





