A Multisensory Multilevel Health Education Model for Diverse Communities
Abstract
1. Introduction
2. The Multisensory Multilevel Health Education Model
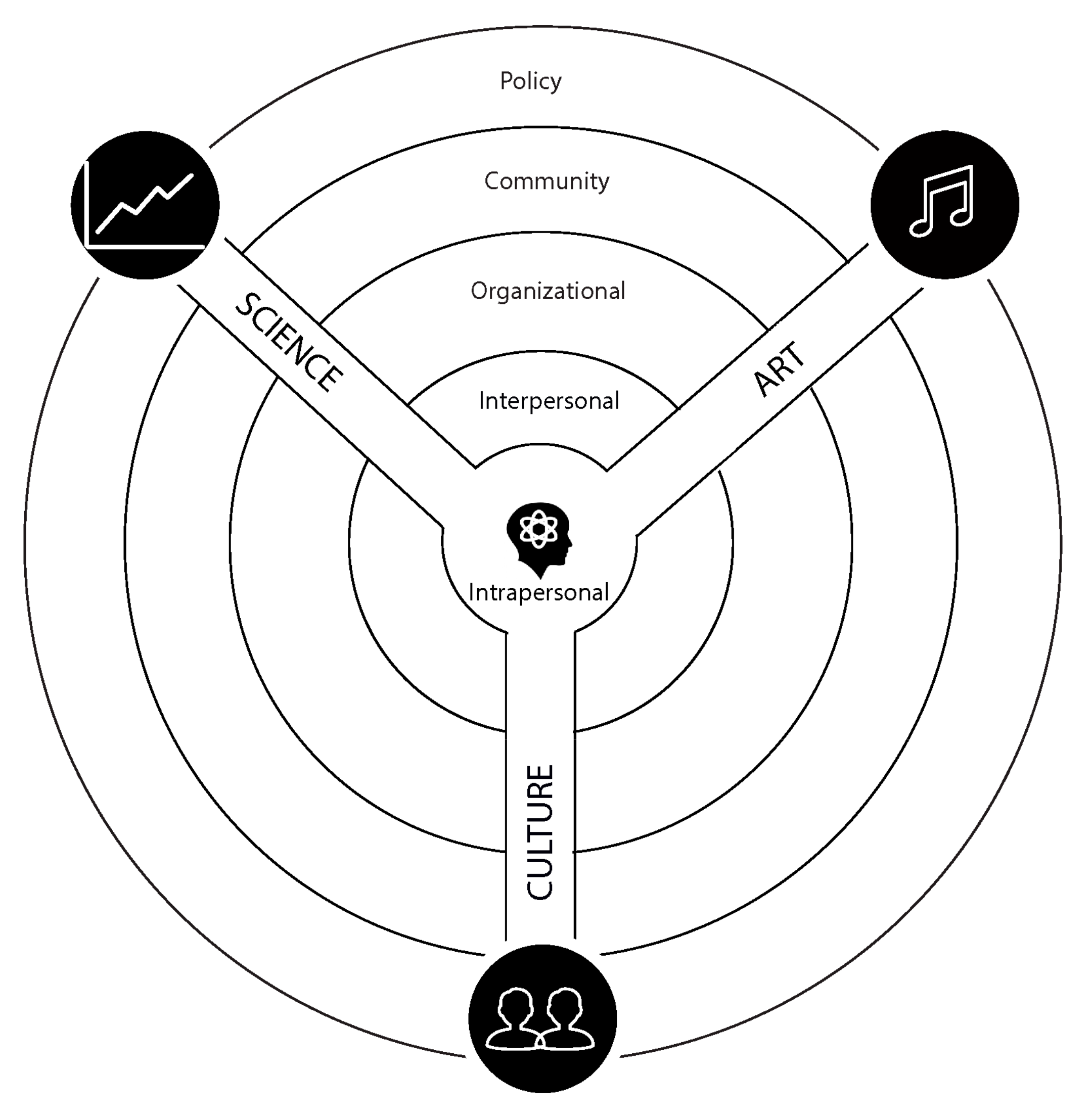
2.1. Socio-Ecological Model (SEM) and Health Education: Foundation of the Multisensory Multilevel Health Education Model (MMHEM)
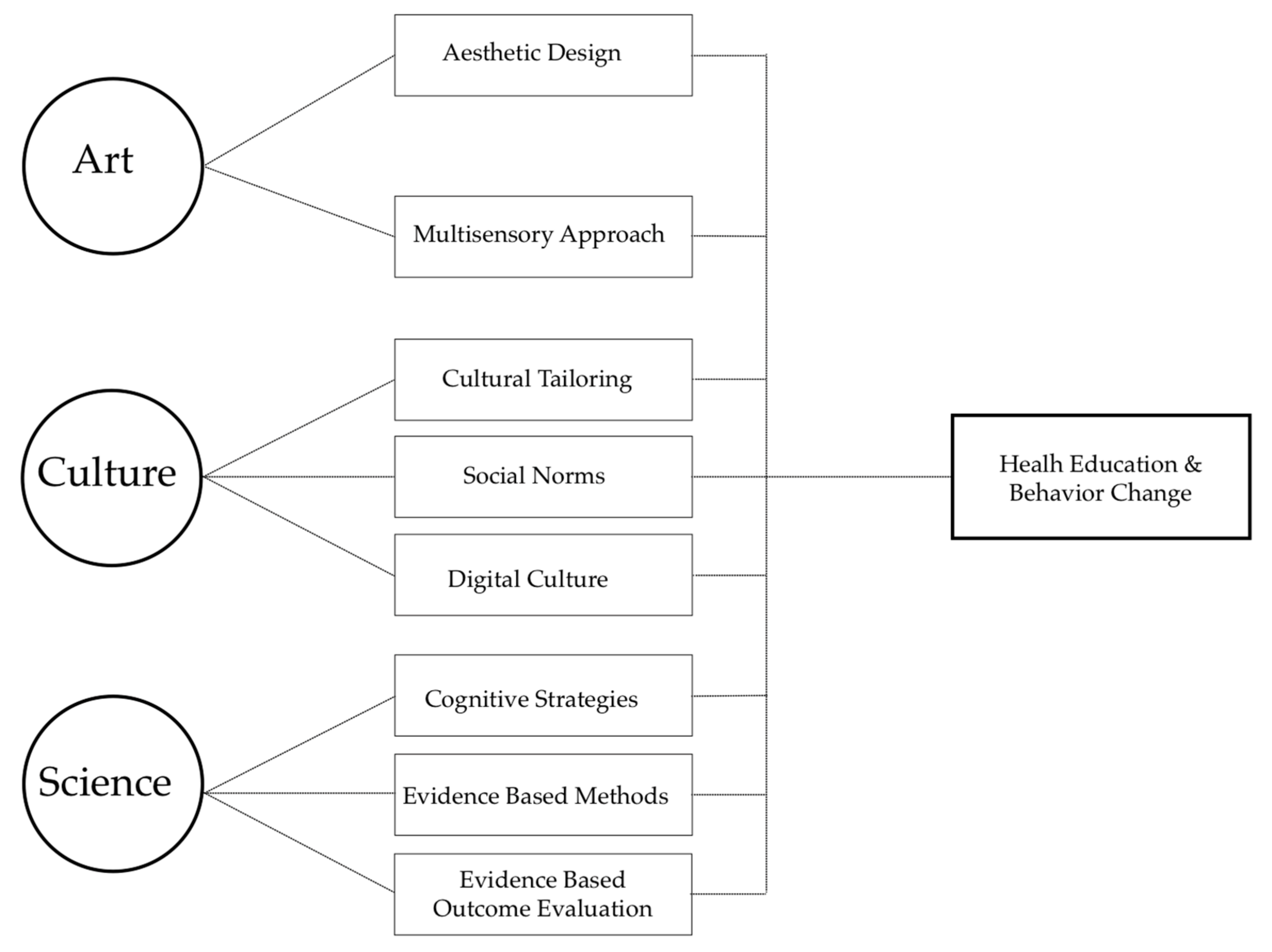
2.2. Art, Culture, and Science—Major Domains of the Multisensory Multilevel Health Education Model
2.2.1. Art
2.2.2. Culture
2.2.3. Science
2.3. The Interaction between Art, Culture, and Science
3. Hip Hop Stroke: An Illustration of MMHEM
3.1. General Overview of HHS
3.2. Art Domain of Hip Hop Stroke
3.3. Culture Domain of Hip Hop Stroke
3.4. Science Domain of Hip Hop Stroke
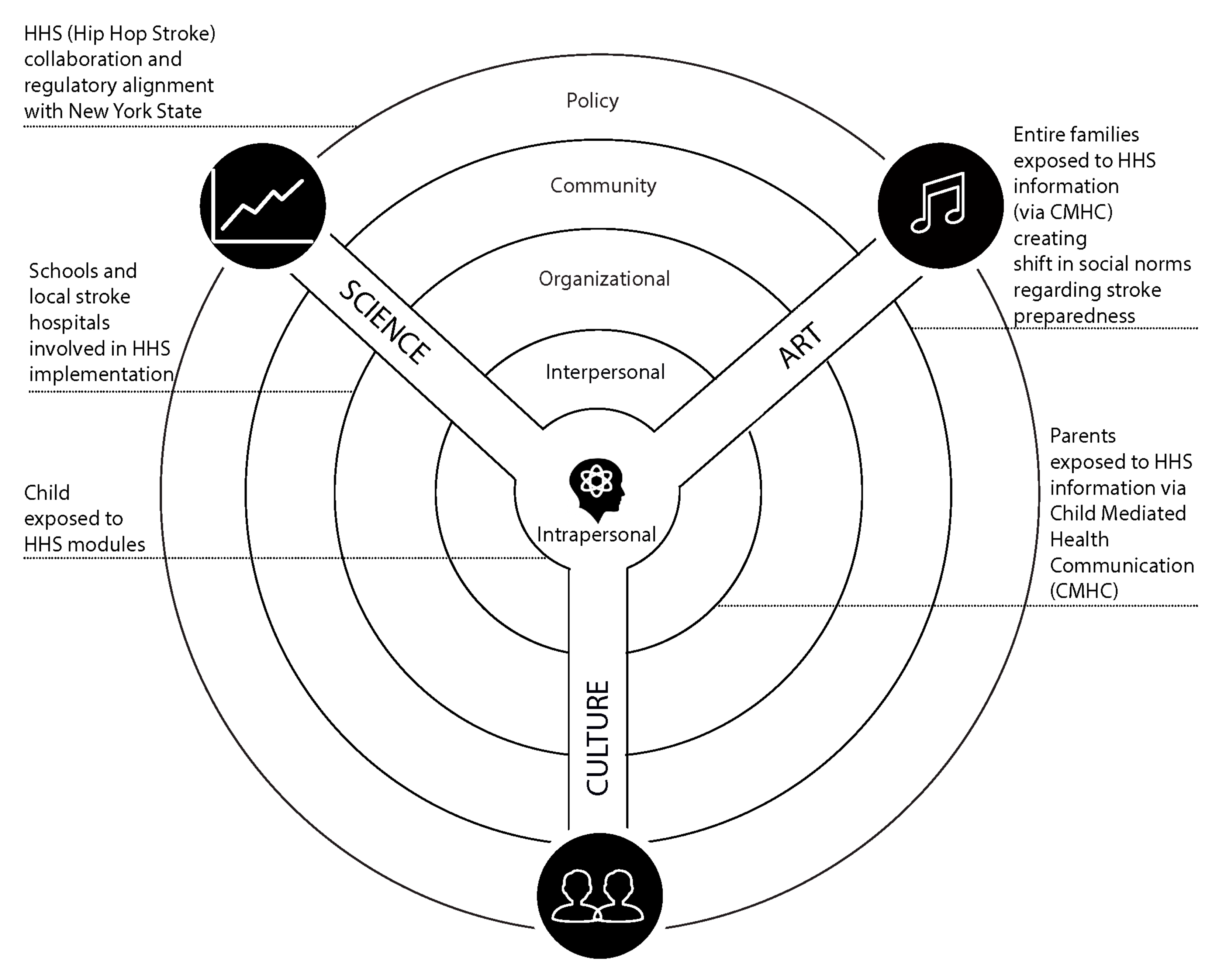
3.5. Levels of Behavioral Influence and Hip Hop Stroke
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Laverack, G. The challenge of the ‘art and science’ of health promotion. Challenges 2017, 8, 22. [Google Scholar] [CrossRef]
- Xiaoyan, O.; Diego, O.; Alireza, S.; Alessandro, F.; Filippo, M. Limited individual attention and online virality of low-quality information. Nat. Hum. Behav. 2017, 1, 0312. [Google Scholar]
- Falkinger, J. Attention economies. J. Econ. Theory 2007, 133, 266–294. [Google Scholar] [CrossRef]
- Thomson, K.; Hillier-Brown, F.; Todd, A.; Mcnamara, C.; Huijts, T.; Bambra, C. The effects of public health policies on health inequalities in high-income countries: An umbrella review. BMC Public Health 2018, 18, 869. [Google Scholar] [CrossRef] [PubMed]
- Baum, F.; Fisher, M. Why behavioral health promotion endures despite its failure to reduce health inequities. Sociol. Health Illn. 2014, 36, 213–225. [Google Scholar] [CrossRef] [PubMed]
- Frieden, T.R. Six components necessary for effective public health program implementation. Am. J. Public Health 2014, 104, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Gill, T.; Boylan, S. Public health messages: Why are they ineffective and what can be done? Curr. Obes. Rep. 2012, 1, 50–58. [Google Scholar] [CrossRef]
- Jepson, R.G.; Harris, F.M.; Platt, S.; Tannahill, C. The effectiveness of interventions to change six health behaviours: A review of reviews. BMC Public Health 2010, 10, 538. [Google Scholar] [CrossRef] [PubMed]
- Debarr, K. A Review of Current Health Education Theories. Calif. J. Health Promot. 2004, 2, 74–87. [Google Scholar]
- Rosenstock, I.M.; Strecher, V.J.; Becker, M.H. Social Learning Theory and the Health Belief Model. Health Educ. Q. 1998, 15, 175–183. [Google Scholar] [CrossRef]
- Ajzen, I. The theory of planned behavior. Organ. Behav. Hum. Decis. Process. 1991, 50, 179–211. [Google Scholar] [CrossRef]
- Bandura, A. Social cognitive theory: An agentive perspective. Annu. Rev. Psychol. 2001, 52, 1–26. [Google Scholar] [CrossRef] [PubMed]
- Petty, R.E.; Caciopo, J.T. The elaboration likelihood model of persuasion. Adv. Exp. Soc. Psychol. 1986, 19, 123–205. [Google Scholar]
- Caplan, G. Support. Systems and Community Mental Health; Behavioral Publications: New York, NY, USA, 1974. [Google Scholar]
- Prochaska, J.O.; Diclemente, C.C. Stages and processes of self-change of smoking: Toward an integrative model of change. J. Consult. Clin. Psychol. 1983, 51, 390–395. [Google Scholar] [CrossRef] [PubMed]
- Rogers, E.M. Diffusion of Innovations; Free Press: New York, NY, USA, 1995. [Google Scholar]
- Singhal, A. A Theoretical agenda for entertainment-education. Commun. Theory 2002, 12, 117–135. [Google Scholar]
- McLeroy, K.; Bibeau, D.; Steckler, A.; Glanz, K. An ecology perspective on health promotion programs. Health Educ. Q. 1988, 15, 351–377. [Google Scholar] [CrossRef] [PubMed]
- Langille, J.; Rodgers, W.M. Exploring the influence of a Social Ecological Model on school-based physical activity. Health Educ. Behav. 2010, 37, 879–894. [Google Scholar] [CrossRef] [PubMed]
- Stokols, D.; Allen, J.; Bellingham, R.L. The social ecology of health promotion: Implications for research and practice. Am. J. Health Promot. 1996, 10, 247–251. [Google Scholar] [CrossRef] [PubMed]
- Williams, O.; Noble, J.M. Hip-Hop Stroke: A stroke educational program for elementary school children living in a high-risk community. Stroke 2008, 39, 2809–2816. [Google Scholar] [CrossRef] [PubMed]
- Williams, O.; DeSorbo, A.; Noble, J.; Gerin, W. Child Mediated Stroke Communication: Findings from Hip Hop Stroke. Stroke 2012, 43, 163–169. [Google Scholar] [CrossRef] [PubMed]
- Williams, O.; Leighton-Herrmann, E.; DeSorbo, A.; Hecht, M.; Hedmann, M.; Huq, S.; Gerin, W.; Chinchilli, V.; Ogedegbe, G.; Noble, J. Hip Hop Stroke: Study protocol for a randomized controlled trial to address stroke literacy. J. Clin. Trials 2015, 5, 242. [Google Scholar] [PubMed]
- Williams, O.; Leighton-Hermann, E.; Hecht, M.; DeSorbo, A.; Gerin, W.; Hedmann, M.; Shelton, R.; Tolchin, B.; Noble, J. Child Mediated Health Communication: A conceptual framework for increasing stroke literacy in hard to reach populations. J. Health Disparities Res. Pract. 2016, 9, 82–97. [Google Scholar]
- Williams, O.; Leighton-Herrmann, E.; Teresi, J.; Eimicke, J.K.; Kong, J.; Ogedegbe, G.; Noble, J. Improving community stroke preparedness in the HHS (Hip-Hop Stroke) randomized clinical trial. Stroke 2018, 49, 972–979. [Google Scholar] [CrossRef] [PubMed]
- Hayslip, B.; Kaminski, P.L. Grandparents raising their grandchildren: A review of the literature and suggestions for practice. Gerontologist 2005, 45, 262–269. [Google Scholar] [CrossRef] [PubMed]
- Spence, J.C.; Lee, R.E. Toward a comprehensive model of physical activity. Psychol. Sport Exerc. 2003, 4, 7–24. [Google Scholar] [CrossRef]
- Lewis, M.A.; Fitzgerald, T.M.; Zulkiewicz, B.; Peinado, S.; Williams, P. Identifying synergies in multilevel interventions. Converg. Strategy. Health Educ. Behav. 2017, 44, 236–244. [Google Scholar] [CrossRef] [PubMed]
- Golden, S.D.; Earp, J.A.L. Social ecological approaches to individuals and their contexts: Twenty years of health education & behavior health promotion interventions. Health Educ. Behav. 2012, 39, 364–372. [Google Scholar] [PubMed]
- Batra, R.; Keller, P.A.; Strecher, V.J. Leveraging Consumer Psychology for Effective Health Communications: The Obesity Challenge; M.E. Sharpe: Armonk, NY, USA, 2012. [Google Scholar]
- Stuckey, H.L.; Nobel, J. The connection between art, healing, and public health: A review of current literature. Am. J. Public Health 2010, 100, 254–263. [Google Scholar] [CrossRef] [PubMed]
- Yom-Tov, E.; Shembekar, J.; Barclay, S.; Muenning, P. The effectiveness of public health advertisements to promote health: A randomized-controlled trial on 794,000 participants. Digit. Med. 2018, 1, 24. [Google Scholar] [CrossRef]
- Kreuter, M.; Lukwago, S.; Bucholtz, R.D.; Clark, E.M.; Sanders-Thompson, V. Achieving cultural appropriateness in health promotion programs. Health Educ. Behav. 2003, 30, 133–146. [Google Scholar] [CrossRef] [PubMed]
- Resnicow, K.; Baranowski, T.; Ahluwahlia, J.S.; Braithwaite, R.L. Cultural sensitivity in public health: Defined and demystified. Ethn. Dis. 1999, 9, 10–21. [Google Scholar] [PubMed]
- Mann, C. Behaviour Changing Campaigns: Success and Failure Factors. Transparency International. 2011. Available online: https://www.transparency.org/whatwedo/answer/behaviour_changing_campaigns_success_and_failure_factors (accessed on 1 December 2018).
- Jacobs, J.A.; Clayton, P.F.; Dove, C.; Funchess, T.; Jones, E.; Perveen, G.; Skidmore, B.; Sutton, V.; Worthington, S.; Baker, E.A.; et al. A survey tool for measuring evidence-based decision- making capacity in public health agencies. BMC Health Serv. Res. 2012, 12, 57. [Google Scholar] [CrossRef] [PubMed]
- Baldwin, S.; Ching, Y.H. Interactive storytelling: Opportunities for online course design. Technol. Trends 2016, 61, 179–187. [Google Scholar] [CrossRef]
- Lehmann, S.; Murray, M.M. The role of multisensory memories in unisensory object discrimination. Cogn. Brain Res. 2005, 24, 326–334. [Google Scholar] [CrossRef] [PubMed]
- Murray, M.M.; Michel, C.M.; Grave de Peralta, R.; Ortigue, S.; Brunet, D.; Gonzalez Andino, S.; Schnider, A. Rapid discrimination of visual and multisensory memories revealed by electrical neuroimaging. Neuroimage 2004, 21, 125–135. [Google Scholar] [CrossRef] [PubMed]
- Shams, L.; Seitz, A. Benefits of multisensory learning. Trends Cogn. Sci. 2008, 12, 411–417. [Google Scholar] [CrossRef] [PubMed]
- Xie, Y.; Bian, C.; Li, M. Semantic congruent audiovisual integration during the encoding stage of working memory: An ERP and sLORETA study. Sci. Rep. 2017, 7, 5112–5127. [Google Scholar] [CrossRef] [PubMed]
- Elder, R.S.; Krishna, E.A. The effects of advertising copy on sensory thoughts and perceived taste. J. Consum. Res. 2010, 36, 748–756. [Google Scholar] [CrossRef]
- Shi, Z.; Müller, H.J. Multisensory perception and action: Development, decision-making, and neural mechanisms. Front. Integr. Neurosci. 2013, 7, 81. [Google Scholar] [CrossRef] [PubMed]
- Quak, L.; London, R.E.; Talsma, D. A multisensory perspective of working memory. Front. Hum. Neurosci. 2015, 9, 197. [Google Scholar] [CrossRef] [PubMed]
- Mayer, K.M.; Yildiz, I.B.; Macedonia, M.; von Kriegstein, K. Visual and motor cortices differentially support the translation of foreign language words. Curr. Biol. 2015, 25, 530–535. [Google Scholar] [CrossRef] [PubMed]
- Shimojo, S.; Shams, L. Sensory modalities are not separate modalities: Plasticity and interactions. Curr. Opin. Neurobiol. 2001, 11, 505–509. [Google Scholar] [CrossRef]
- Voto, D.; Viñas, L.M.; D’Auria, L. Multisensory interactive installation. In Proceedings of the Sound and Music Computing ’05, XV CIM, Salerno, Italy, 24–26 November 2015. [Google Scholar]
- Seitz, A.; Kim, R.; Shams, L. Sound Facilitates Visual Learning. Curr. Biol. 2005, 16, 1422–1427. [Google Scholar] [CrossRef] [PubMed]
- Steslow, D.M.; Gardner, C. More than one way to tell a story: Integrating storytelling into your law course. J. Leg. Stud. Educ. 2011, 28, 249–271. [Google Scholar] [CrossRef]
- Heikkilä, J. Audiovisual semantic congruency during encoding enhances memory performance. Exp. Psychol. 2014, 62, 123–130. [Google Scholar] [CrossRef] [PubMed]
- Delp, C.; Jones., J. Communicating information to patients: The use of cartoon illustrations to improve comprehension of instructions. Acad. Emerg. Med. 1996, 3, 264–270. [Google Scholar] [CrossRef] [PubMed]
- Houts, P.S.; Witmer, J.T.; Egeth, H.E.; Loscalzo, M.J.; Zabora, J.R. Using pictographs to enhance recall of spoken medical instructions II. Patient Educ. Couns. 2001, 43, 231–242. [Google Scholar] [CrossRef]
- George, S.; Moran, E.; Duran, N.; Jenders, R.A. Using animation as an information tool to advance health research literacy among minority participants. Amia Annu. Symp. Proc. 2013, 475–484. [Google Scholar]
- Clift, S. Creative arts as a public health resource: Moving from practice-based research to evidence-based practice. Perspect. Public Health 2012, 132, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Padilla, A.M.; Borsato, G.N. Issues in culturally appropriate psychoeducational assessment. In Handbook of Multicultural Assessment: Clinical, Psychological, and Educational Applications, 3rd ed.; Suzuki, L.A., Ponterotto, J.G., Eds.; Jossey-Bass: San Francisco, CA, USA, 2008; pp. 5–21. [Google Scholar]
- Lewis, N.A.; Oyserman, D. Using identity-based motivation to improve the nation’s health without breaking the bank. Behav. Sci. Policy 2016, 2, 25–38. [Google Scholar] [CrossRef]
- Kreuter, M.; Mcclure, S. The role of culture in health communication. Annu. Rev. Public Health 2004, 25, 439–455. [Google Scholar] [CrossRef] [PubMed]
- Oyserman, D.; Smith, G.C.; Elmore, K. Identity-Based Motivation: Implications for health and health disparities. J. Soc. Issues 2014, 70, 206–225. [Google Scholar] [CrossRef]
- Norman, C.D. Social media and health promotion. Glob. Health Promot. 2012, 19, 3–6. [Google Scholar] [CrossRef] [PubMed]
- Jane, M.; Hagger, M.; Foster, J.; Ho, S.; Pal, S. Social media for health promotion and weight management: A critical debate. BMC Public Health 2018, 18, 932. [Google Scholar] [CrossRef] [PubMed]
- Pew Research Center—Social Media Use in 2018. Available online: http://www.pewinternet.org/2018/03/01/social-media-use-in-2018/ (accessed on 9 January 2019).
- Lewis, J.J. Use of social media for the delivery of health promotion on smoking, nutrition, and physical activity: A systematic review. Lancet 2017, 390, S49. [Google Scholar]
- Welch, V.; Petkovic, J.; Pardo, J.; Rader, T.; Tugwell, P. Interactive social media interventions to promote health equity: An overview of reviews. Health Promot. Chronic Dis. Prev. 2016, 36, 63–75. [Google Scholar] [CrossRef]
- Berger, J. Identity-signalling, social influence, and social contagion. In Understanding Peer Influence in Children and Adolescents; Prinstein, M.J., Dodge, K.A., Eds.; Guilford: New York, NY, USA, 2008. [Google Scholar]
- Berger, J.; Heath, C. Idea habitats: How the prevalence of environmental cues influences the success of ideas. Cogn. Sci. 2005, 29, 195–221. [Google Scholar] [CrossRef] [PubMed]
- Berger, J.; Rand, L. Shifting signals to help health: Using identity signaling to reduce risky health behaviors. J. Consum. Res. 2008, 35, 509–518. [Google Scholar] [CrossRef]
- Rimal, R.N.; Real, K. How behaviors are influenced by perceived norms: A test of the theory of normative social behavior. Commun. Res. 2005, 32, 389–414. [Google Scholar] [CrossRef]
- Templeton, E.M.; Stanton, M.V.; Zaki, J. Social norms shift preferences for healthy and unhealthy foods. PLoS ONE 2016, 11, e0166286. [Google Scholar] [CrossRef] [PubMed]
- Cross, I. Musicality and the human capacity for cultures. Music. Sci. 2008, 12 (Suppl. 1), 147–167. [Google Scholar] [CrossRef]
- Murray, N.M.; Murray, S.B. Music and lyrics in commercials: A cross-cultural comparison between commercials run in the Dominican Republic and in the United States. J. Advert. 1996, 25, 51–63. [Google Scholar] [CrossRef]
- Schlosser, M.J.; Aoyagi, N.; Fulbright, R.K.; Gore, J.C.; McCarthy, G. Functional MRI studies of auditory comprehension. Hum. Brain Mapp. 1998, 6, 1–13. [Google Scholar] [CrossRef]
- Morrison, J.; Demorest, S.M.; Aylward, E.H.; Cramer, S.C.; Maravilla, K.R. FMRI investigation of cross-cultural music comprehension. NeuroImage 2003, 20, 378–384. [Google Scholar] [CrossRef]
- North, A.C.; Mackenzie, L.C.; Law, R.M.; Hargreaves, D.J. The effects of musical and voice “fit” on responses to advertisements1. J. Appl. Soc. Psychol. 2004, 34, 1675–1708. [Google Scholar] [CrossRef]
- Yeoh, P.S.; North, A.C. The Effect of musical fit on consumers’ memory. Psychol. Music 2010, 38, 68–378. [Google Scholar] [CrossRef]
- Brownson, R.C.; Fielding, J.E.; Maylahn, C.M. Evidence-based decision making to improve public health practice. Front. Public Health Serv. Syst. Res. 2013, 2, 2. [Google Scholar]
- Heath, C.; Heath, D. Made to Stick: Why Some Ideas Survive and Others Die; Random House: New York, NY, USA, 2007. [Google Scholar]
- Berger, J. Contagious: Why Things Catch On; Simon & Schuster: New York, NY, USA, 2013. [Google Scholar]
- Milkman, K.; Berger, J. The Science of sharing and the sharing of science. Proc. Natl. Acad. Sci. USA 2014, 111, 13642–13649. [Google Scholar] [CrossRef] [PubMed]
- Brownson, R.C.; Chriqui, J.F.; Stamatakis, K.A. Understanding evidence-based public health policy. Am. J. Public Health 2009, 99, 1576–1583. [Google Scholar] [CrossRef] [PubMed]
- Burns, P.; Rohrich, R.; Chung, K. The levels of evidence and their role in evidence-based medicine. Plast. Reconstr. Surg. 2011, 128, 305–310. [Google Scholar] [CrossRef] [PubMed]
- Rychetnik, L.; Hawe, P.; Waters, E.; Barratt, A.; Frommer, M. A glossary for evidence based public health. J. Epidemiol. Community Health 2004, 58, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Bernal, G.; Bonilla, J.; Bellido, C. Ecological validity and cultural sensitivity for outcome research: Issues for the cultural adaptation and development of psychosocial treatments with Hispanics. J. Abnorm. Child. Psychol. 1995, 23, 67–82. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.K.; Hecht, M.L.; Miller-Day, M.; Elek, E. Evaluating mediated perception of narrative health messages: The perception of Narrative Performance Scale. Commun. Methods Meas. 2011, 5, 126–145. [Google Scholar] [CrossRef] [PubMed]
- Miller, M.; Hecht, M.; Stiff, J. An exploratory measurement of engagement with live and film media. J. Ill. Speech Theatre Assoc. 1998, 49, 69–97. [Google Scholar]
- Naples, M.J. Effective frequency—Then and now. J. Advert. Res. 1997, 37, 7–13. [Google Scholar]
- DeSorbo, A.; Noble, J.; Shafer, M.; Gerin, W.; Williams, O. The use of an audience response system in an elementary school-based health education program. Health Educ. Behav. J. 2013, 40, 531–535. [Google Scholar] [CrossRef] [PubMed]
- Simmons, C.; Noble, J.M.; Leighton-Herrmann, E.; Hecht, M.F.; Williams, O. Community-level measures of stroke knowledge among children: Findings from Hip Hop Stroke. J. Stroke Cerebrovasc. Dis. 2017, 26, 139–142. [Google Scholar] [CrossRef] [PubMed]
- Saver, J.L. Time is brain—Quantified. Stroke 2005, 37, 263–266. [Google Scholar] [CrossRef] [PubMed]

| Domains | Subdomains | Examples | Functions | SEM Level of Influence |
|---|---|---|---|---|
| Art | 1. Aesthetic Design 2. Multisensory Approach (visual, auditory, tactile kinesthetic) | (a) Music (b) Storytelling (c) Multimedia (e.g., animation, video) (d) Pictographs (e) Gamification (f) Acting (dramatization) (g) Movement (e.g., dance) (h) Virtual Reality | Enhance attention Facilitate immersion Trigger emotions Inspire action Overcome illiteracy barriers Enhance learning | Intrapersonal Interpersonal |
| Culture | 1. Cultural Tailoring 2. Social Norms 3. Digital Culture | (a) Qualitative research (e.g., focus groups, community advisory boards, use of a narrative performance scale) (b) Cultural adaptation frameworks (e.g., ecological validity model) (c) Identity Signaling (d) Role of social media and digital platforms | Increase cultural relevance Increase personal relevance Facilitate acceptance Leverage social networks through digital platforms | Intrapersonal Interpersonal Organizational Community |
| Science | 1. Cognitive Strategies (memory and learning) | (a) Stickiness (including the properties of a sticky message) (b) Contagiousness (including the properties of a contagious message) (c) Repetition (d) Rehearsal (e) Role Play (f) Rhymes (g) Acronyms | Facilitate learning Facilitate retention | Intrapersonal Interpersonal Organizational Community |
| 2. Evidence Based Methods | (a) Scientific Advisory Boards (b) Literature reviews/Subject Matter Experts (c) Best practices (d) Use of Conceptual Frameworks (e) Multidisciplinary or Transdisciplinary teams | Ensure scientific rigor including strong scientific premise | Intrapersonal Interpersonal Organizational Community | |
| 3. Evidence Based Outcome Evaluation | (a) Psychometrically Reliable and Validated Outcomes Measures (b) Rigorous Research designs to test for Efficacy and Effectiveness | Facilitates internal and external validity | Intrapersonal Interpersonal Organizational Community Policy |
| Health Education Framework | WHY/WHAT (e.g., Self-efficacy, Perception, Normative beliefs, Persuasion, Social Norms etc.) | WHO/WHERE (i.e., Individuals, Family/Friends, Community, Organizations, Public Policy) | HOW (i.e., the Incorporation of Art, Cultural Adaptation, Scientific Evidence based Methods) |
|---|---|---|---|
| Existing Models of Health Education * (individual, interpersonal, stage-based frameworks) | × | ||
| Socio-Ecological Model | × | ||
| Educational Entertainment | × | × | |
| MMHEM | × | × | × |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Williams, O.; Swierad, E.M. A Multisensory Multilevel Health Education Model for Diverse Communities. Int. J. Environ. Res. Public Health 2019, 16, 872. https://doi.org/10.3390/ijerph16050872
Williams O, Swierad EM. A Multisensory Multilevel Health Education Model for Diverse Communities. International Journal of Environmental Research and Public Health. 2019; 16(5):872. https://doi.org/10.3390/ijerph16050872
Chicago/Turabian StyleWilliams, Olajide, and Ewelina M. Swierad. 2019. "A Multisensory Multilevel Health Education Model for Diverse Communities" International Journal of Environmental Research and Public Health 16, no. 5: 872. https://doi.org/10.3390/ijerph16050872
APA StyleWilliams, O., & Swierad, E. M. (2019). A Multisensory Multilevel Health Education Model for Diverse Communities. International Journal of Environmental Research and Public Health, 16(5), 872. https://doi.org/10.3390/ijerph16050872




