Depression and Anxiety Symptoms of British Adoptive Parents: A Prospective Four-Wave Longitudinal Study
Abstract
:1. Introduction
1.1. Risk Factors for Depression and Anxiety in Adoptive Parents
1.2. The Current Study
2. Method
2.1. Design
2.2. Procedure
2.2.1. Questionnaire Data
2.2.2. Case File Data
2.3. Participants
2.4. Measures
2.4.1. Parent Symptoms of Depression and Anxiety
2.4.2. Parent Sense of Competency
2.4.3. Age Placed for Adoption
2.4.4. Child Internalizing Symptoms and Externalizing Problems
2.5. Data Analysis
2.5.1. Missingness
2.5.2. Model Fit
3. Results
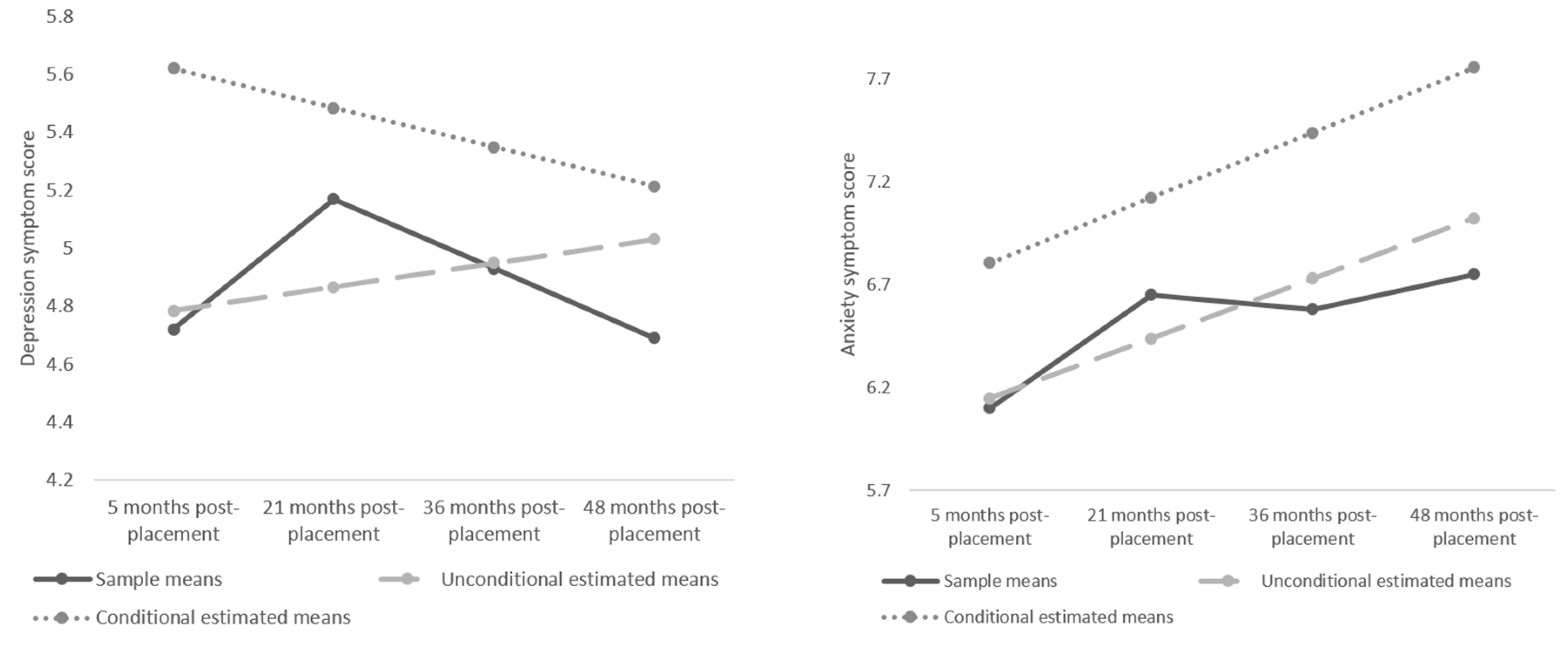
3.1. Growth Curve Models
3.1.1. Unconditional Depression Model
3.1.2. Conditional Depression Model
3.1.3. Unconditional Anxiety Model
3.1.4. Conditional Anxiety Model
4. Discussions
Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Cowan, C.P.; Cowan, P.A. Interventions to ease the transition to parenthood: Why they are needed and what they can do. Fam. Relat. Interdiscip. J. Appl. Fam. Stud. 1995, 44, 412–423. [Google Scholar] [CrossRef]
- Shrivastava, S.R.; Shrivastava, P.S.; Ramasamy, J. Antenatal and postnatal depression: A public health perspective. J. Neurosci. Rural Pract. 2015, 6, 116–119. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Natsuaki, M.N.; Shaw, D.S.; Neiderhiser, J.M.; Ganiban, J.M.; Harold, G.T.; Reiss, D.; Leve, L.D. Raised by depressed parents: Is it an environmental risk? Clin. Child Fam. Psychol. Rev. 2014, 17, 357–367. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Payne, J.L.; Fields, E.S.; Meuchel, J.M.; Jaffe, C.J.; Jha, M. Post adoption depression. Arch. Women’s Ment. Health 2010, 13, 147–151. [Google Scholar] [CrossRef] [PubMed]
- McKay, K.; Ross, L.E. The transition to adoptive parenthood: A pilot study of parents adopting in Ontario, Canada. Child. Youth Serv. Rev. 2010, 32, 604–610. [Google Scholar] [CrossRef]
- Goodman, S.H.; Rouse, M.H.; Connell, A.M.; Broth, M.R.; Hall, C.M.; Heyward, D. Maternal depression and child psychopathology: A Meta-Analytic Review. Clin. Child Fam. Psychol. Rev. 2011, 14, 1–27. [Google Scholar] [CrossRef]
- Selwyn, J.; Wijedesa, D.; Meakings, S. Beyond the Adoption Order. In Challenges, Interventions and Adoption Disruption; BAAF: London, UK, 2014. [Google Scholar]
- Dean, C.; Dean, N.R.; White, A.; Liu, W.Z. An adoption study comparing the prevalence of psychiatric illness in women who have adoptive and natural children compared with women who have adoptive children only. J. Affect. Disord. 1995, 34, 55–60. [Google Scholar] [CrossRef]
- Foli, K.J.; South, S.C.; Lim, E.; Hebdon, M. Maternal postadoption depression, unmet expectations, and personality traits. J. Am. Psychiatr. Nurses Assoc. 2012, 18, 267–277. [Google Scholar] [CrossRef]
- Foli, K.J.; South, S.C.; Lim, E.; Jarnecke, A.M. Post-adoption depression: Parental classes of depressive symptoms across time. J. Affect. Disord. 2016, 200, 293–302. [Google Scholar] [CrossRef] [Green Version]
- Gair, D. Distress and depression in new motherhood: Research with adoptive mothers highlights important contributing factors. Child Fam. Soc. Work 1999, 4, 55–66. [Google Scholar] [CrossRef]
- Mott, S.L.; Schiller, C.E.; Richards, J.G.; O’Hara, M.W.; Stuart, S. Depression and anxiety among postpartum and adoptive mothers. Arch. Women’s Ment. Health 2011, 14, 335–343. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Senecky, Y.; Agassi, H.; Inbar, D.; Horesh, N.; Diamond, G.; Bergman, Y.S.; Apter, A. Post-adoption depression among adoptive mothers. J. Affect. Disord. 2009, 115, 62–68. [Google Scholar] [CrossRef] [PubMed]
- O’Hara, M.W.; Swain, A.M. Rates and risk of postpartum depression-A meta-analysis. Int. Rev. Psychiatry 1996, 8, 37–54. [Google Scholar] [CrossRef]
- Adoption and Foster Care Analysis and Reporting System (AFCARS). Preliminary Estimates for FY 2012 as for July 2013. Available online: https://www.acf.hhs.gov/program/cb (accessed on 10 September 2019).
- Ivaldi, G. Surveying Adoption: A Comprehensive Analysis of Local Authority Adoptions 1998–1999 (England); British Association of Adoption and Fostering: London, UK, 2000. [Google Scholar]
- Rushton, A. The Adoption of Looked after Children: A Scoping Review of Research; Social Care Institute for Excellence: London, UK, 2003. [Google Scholar]
- Kohler, J.K.; Grotevant, H.D.; McRoy, R.G. Adopted adolescents’ preoccupation with adoption: Impact of adoptive family dynamics. J. Marriage Fam. 2002, 64, 93–104. [Google Scholar] [CrossRef]
- Department for Education. Adoption: National Minimum Standards; Crown Copyright; Department for Education: London, UK, 2014.
- Brodzinsky, D.M. Children’s understanding of adoption: Developmental and clinical implications. Prof. Psychol. Res. Pract. 2011, 42, 200–207. [Google Scholar] [CrossRef] [Green Version]
- Brodzinsky, D.M.; Schechter, M.D. The Psychology of Adoption; Oxford University Press: Oxford, UK, 1990. [Google Scholar]
- Daniluk, J.C.; Hurtig-Mitchell, J. Themes of hope and healing: Infertile couples’ experiences of adoption. J. Couns. Dev. 2003, 81, 389–399. [Google Scholar] [CrossRef]
- Dance, C.; Farmer, E. Changing lives and changing minds: The experiences of adoptive parents from application to approval. Adopt. Fostering 2014, 38, 101–114. [Google Scholar] [CrossRef]
- Anthony, R.E.; Meakings, S.; Doughty, J.; Ottaway, H.; Holland, S.; Shelton, K.H. Factors affecting adoption in Wales: Predictors of variation in time between entry to care and adoptive placement. Child. Youth Serv. Rev. 2016, 184–190. [Google Scholar] [CrossRef]
- Lavner, J.A.; Waterman, J.; Peplau, L.A. Parent adjustment over time in gay, lesbian, and heterosexual parent families adopting from foster care. Am. J. Orthopsychiatry 2014, 84, 46–53. [Google Scholar] [CrossRef] [Green Version]
- Brooker, R.J.; Neiderhiser, J.M.; Leve, L.D.; Shaw, D.S.; Scaramella, L.V.; Reiss, D. Associations between infant negative affect and parent anxiety symptoms are bidirectional: Evidence from mothers and fathers. Front. Psychol. 2015, 6, 1875. [Google Scholar] [CrossRef]
- Anthony, R.E.; Paine, A.L.; Shelton, K.H. Adverse childhood experiences of children adopted from care: The importance of adoptive parental warmth for future child adjustment. Int. J. Environ. Res. Public. Health 2019, 16, 2212. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Simmel, C.; Barth, R.P.; Brooks, D. Adopted foster youths’ psychosocial functioning: A longitudinal perspective. Child Fam. Soc. Work 2007, 12, 336–348. [Google Scholar] [CrossRef]
- Barnett, E.R.; Cleary, S.E.; Butcher, R.L.; Jankowski, M.K. Children’s behavioral health needs and satisfaction and commitment of foster and adoptive parents: Do trauma-informed services make a difference? Psychol. Trauma Theory Res. Pract. Policy 2019, 11, 73–81. [Google Scholar] [CrossRef] [PubMed]
- Brannan, A.M.; Heflinger, C.A. Caregiver, Child, Family, and Service System Contributors to Caregiver Strain in Two Child Mental Health Service Systems. J. Behav. Health Serv. Res. 2006, 33, 408–422. [Google Scholar] [CrossRef]
- Judge, S. Determinants of parental stress in families adopting children from Eastern Europe. Fam. Relat. Interdiscip. J. Appl. Fam. Stud. 2003, 52, 241–248. [Google Scholar] [CrossRef]
- Viana, A.G.; Welsh, J.A. Correlates and predictors of parenting stress among internationally adopting mothers: A longitudinal investigation. Int. J. Behav. Dev. 2010, 34, 363–373. [Google Scholar] [CrossRef] [Green Version]
- Brodzinsky, D. Understanding and treating adoptive families. In Contemporary families: Translating Research into Practice; Browning, S., Pasley, K., Eds.; Routledge/Taylor Francis Group: New York, NY, USA, 2015; pp. 35–52. [Google Scholar]
- Hegar, R.L. Sibling placement in foster care and adoption: An overview of international research. Child. Youth Serv. Rev. 2005, 27, 717–739. [Google Scholar] [CrossRef]
- Meakings, S.; Sebba, J.; Luke, N. What is Known about the Placement and Outcomes of Siblings in Foster Care? An International Literature Review; Rees Centre: Oxford, UK, 2017. [Google Scholar]
- Johnston, C.; Mash, E.J. A measure of parenting satisfaction and efficacy. J. Clin. Child Psychol. 1989, 18, 167–175. [Google Scholar] [CrossRef]
- Gross, D.; Conrad, B.; Fogg, L.; Wothke, W. A longitudinal model of maternal self-efficacy, depression, and difficult temperament during toddlerhood. Res. Nurs. Health 1994, 17, 207–215. [Google Scholar] [CrossRef]
- Lipscomb, S.T.; Leve, L.D.; Harold, G.T.; Neiderhiser, J.M.; Shaw, D.S.; Ge, X.; Reiss, D. Trajectories of parenting and child negative emotionality during infancy and toddlerhood: A longitudinal analysis. Child Dev. 2011, 82, 1661–1675. [Google Scholar] [CrossRef] [Green Version]
- Foli, K.J. Depression in adoptive parents: A model of understanding through grounded theory. West. J. Nurs. Res. 2010, 32, 379–400. [Google Scholar] [CrossRef] [PubMed]
- Statistics, O.F.N. Gross Household Income, UK, Financial Year Ending 2018. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/personalandhouseholdfinances/incomeandwealth/adhocs/009772grosshouseholdincomeukfinancialyearending2018 (accessed on 10 September 2019).
- Goodman, R. The strengths and difficulties questionnaire: A research note. J. Child Psychol. Psychiatry 1997, 38, 581–586. [Google Scholar] [CrossRef] [PubMed]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bjelland, I.; Dahl, A.A.; Haug, T.T.; Neckelmann, D. The validity of the hospital anxiety and depression scale. J. Psychosom. Res. 2002, 52, 69–77. [Google Scholar] [CrossRef]
- Gibaud-Wallston, J.; Wandersman, L.P. Parenting Sense of Competence Scale; Lawrence Erlbaum Associates: Toronto, ON, Canada, 1978. [Google Scholar]
- Shumow, L.; Lowmax, R. Parental efficacy: Predictor of parenting behavior and adolescent outcomes. Parent. Sci. Pract. 2002, 2, 127–150. [Google Scholar] [CrossRef] [Green Version]
- Muthén, L.K.; Muthén, B. Mplus user’s guide [Computer Software Manual]; Muthén Muthén: Los Angeles, CA, USA, 2012. [Google Scholar]
- Bollen, K.A.; Curran, P.J. Latent Curve Models: A Structural Equation Perspective; John Wiley Sons: Hoboken, NJ, USA, 2006; Volume 467. [Google Scholar]
- Muthén, B.O.; Curran, P.J. General longitudinal modeling of individual differences in experimental designs: A latent variable framework for analysis and power estimation. Psychol. Methods 1997, 2, 371–402. [Google Scholar] [CrossRef]
- Diggle, P.; Kenward, M.G. Informative drop-out in longitudinal data analysis. J. R. Stat. Soc. 1994, 43, 49–93. [Google Scholar] [CrossRef]
- Enders, C.K. Analyzing longitudinal data with missing values. Rehabil. Psychol. 2011, 56, 267–288. [Google Scholar] [CrossRef]
- Li, M.; Chen, N.; Cui, Y.; Liu, H. Comparison of different LGM-based methods with MAR and MNAR dropout data. Front. Psychol. 2017, 8, 722. [Google Scholar] [CrossRef] [Green Version]
- Schafer, J.L.; Graham, J.W. Missing data: Our view of the state of the art. Psychol. Methods 2002, 7, 147–177. [Google Scholar] [CrossRef]
- Carmines, E.G.; McIver, J.P. Social Measurement: Current Issues; Sage: Beverly Hills, CA, USA, 1981. [Google Scholar]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equ. Modelling 1999, 6, 1–55. [Google Scholar] [CrossRef]
- MacCallum, R.C.; Browne, M.W.; Sugawara, M. Power analysis and determination of sample size for covariance structure modeling. Psychol. Methods 1996, 1, 130–149. [Google Scholar] [CrossRef]
- Burnham, K.P.; Anderson, D.R. Multimodel inference. Sociol. Methods Res. 2004, 33, 261–304. [Google Scholar] [CrossRef]
- Frigon, J.; Laurencelle, L. Analysis of covariance: A proposed algorithm. Educ. Psychol. Meas. 1993, 53, 1–18. [Google Scholar] [CrossRef]
- Crawford, J.R.; Henry, J.S.; Crombie, C.; Taylor, E.P. Brief report. Normative data for the HADS from a large non-clinical sample. Br. J. Clin. Psychol. 2001, 40, 429–434. [Google Scholar] [CrossRef]
- Woolhouse, H.; Gartland, D.; Mensah, F.; Brown, S. Maternal depression from early pregnancy to 4 years postpartum in a prospective pregnancy cohort study: Implications for primary health care. BJOG Int. J. Obstet. Gynaecol. 2015, 122, 312–321. [Google Scholar] [CrossRef]
- Cox, M.J.; Paley, B. Families as systems. Annu. Rev. Psychol. 1997, 48, 243–267. [Google Scholar] [CrossRef]
- Teti, D.M.; Gelfand, D.M. Behavioral competence among mothers of infants in the first year: The mediational role of maternal self-efficacy. Child Dev. 1991, 62, 918–929. [Google Scholar] [CrossRef]
- Latham, R.M.; Mark, K.M.; Oliver, B.R. Coparenting and children’s disruptive behavior: Interacting processes for parenting sense of competence. J. Fam. Psychol. 2018, 32, 151–156. [Google Scholar] [CrossRef]
- Al-Yagon, M. Maternal personal resources and children’s socioemotional and behavioral adjustment. Child Psychiatry Hum. Dev. 2008, 39, 283–298. [Google Scholar] [CrossRef]
- Min, J.; Jin Yu, J.; Lee, C.; Chae, J. Cognitive emotion regulation strategies contributing to resilience in patients with depression and/or anxiety disorders. Compr. Psychiatry 2013, 54, 1190–1197. [Google Scholar] [CrossRef] [PubMed]
- Rutter, M. Psychosocial resilience and protective mechanisms. Am. J. Orthopsychiatry 1987, 57, 316–331. [Google Scholar] [CrossRef] [PubMed]
- Tasker, F.; Wood, S. The transition into adoptive parenthood: Adoption as a process of continued unsafe uncertainty when family scripts collide. Clin. Child Psychol. Psychiatry 2016, 21, 520–535. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McQuillan, J.; Greil, A.L.; White, L.; Jacob, M.C. Frustrated fertility: Infertility and psychological distress among women. J. Marriage Fam. 2003, 65, 1007–1018. [Google Scholar] [CrossRef]
- International Labour Office. Maternity and Paternity at Work: Law and Practice across the World; International Labour Organization: Geneva, Switzerland, 2014. [Google Scholar]
- NHS After Adoption: What Help Can We Get? Available online: https://www.nhs.uk/live-well/healthy-body/after-adoption-what-help-can-we-get/ (accessed on 5 December 2019).
- Morgan, J.; Robinson, D.; Aldridge, J. Parenting stress and externalizing child behaviour. Child Fam. Soc. Work 2002, 7, 219–225. [Google Scholar] [CrossRef]
- Whelan-Goodinson, R.; Ponsford, J.; Schönberger, M. Validity of the Hospital Anxiey and Depression Scale to assess depression and anxiety following traumatic brain injury as compared with the Structured Clinical Interview for DSM-IV. J. Affect. Disord. 2009, 114, 94–102. [Google Scholar] [CrossRef]
- Lugg-Widger, F.V.; Angel, L.; Cannings-John, R.; Hood, K.; Hughes, K.; Moody, G.; Robling, M. Challenges in accessing routinely collected data from multiple providers in the UK for primary studies: Managing the morass. Int. J. Popul. Data Sci. 2018, 3, 2. [Google Scholar] [CrossRef] [Green Version]
- Stoolmiller, M. Implications of the restricted range of family environments for estimates of heritability and nonshared environment in behavior–genetic adoption studies. Psychol. Bull. 1999, 125, 392–409. [Google Scholar] [CrossRef]
- Harold, G.; Hampden-Thompson, G.; Rodic, M.; Sellers, R. An Evaluation of the AdOpt Parenting Programme. 2017. Available online: https://www.gov.uk/government/publications/adopt-parenting-programme-evaluation (accessed on 13 November 2019).
| N | Mean | SD | 1. | 2. | 3. | 4. | 5. | 6. | 7. | |
|---|---|---|---|---|---|---|---|---|---|---|
| 1. W1 depression score | 96 | 4.72 | 3.43 | - | ||||||
| 2. W1 anxiety score | 96 | 6.10 | 3.48 | 0.611 ** | - | |||||
| 3. Age child placed for adoption | 84 | 2.32 | 2.23 | 0.254 * | 0.252 * | - | ||||
| 4. W1 child internalizing | 58 | 5.28 | 3.35 | 0.340 * | 0.209 | 0.315 * | - | |||
| 5. W1 child externalizing | 58 | 8.33 | 3.97 | 0.321 * | 0.153 | 0.338 * | 0.513 ** | - | ||
| 6. Sibling group adoption | 84 | 0.27 | 0.45 | 0.398 ** | 0.309 ** | 0.513 ** | 0.205 | 0.188 | - | |
| 7. W1 sense of competency | 94 | 74.11 | 12.62 | −0.562 ** | −0.531 ** | −0.428 ** | −0.223 | −0.312 * | −0.364 ** | - |
| χ2 | df | RMSEA | TLI | CFI | AIC | BIC | |
|---|---|---|---|---|---|---|---|
| Depression | |||||||
| M1 intercept only | 17.006 * | 8 | 0.108 | 0.887 | 0.849 | 1574.821 | 1590.207 |
| M2 Unconditional linear | 1.436 | 5 | 0.000 | 1.072 | 1.000 | 1564.875 | 1587.955 |
| M3 Unconditional quadratic | 0.754 | 1 | 0.000 | 1.025 | 1.000 | 1572.164 | 1605.501 |
| M4 Conditional linear | 14.300 | 17 | 0.000 | 1.061 | 1.000 | 798.148 | 838.300 |
| Anxiety | |||||||
| M1 intercept only | 22.167 * | 8 | 0.136 | 0.905 | 0.874 | 1629.025 | 1644.411 |
| M2 Unconditional linear | 3.191 | 5 | 0.000 | 1.019 | 1.000 | 1615.244 | 1638.323 |
| M3 Unconditional quadratic | 0.440 | 1 | 0.000 | 1.030 | 1.000 | 1620.664 | 1654.000 |
| M4 Conditional linear | 13.347 | 17 | 0.000 | 1.063 | 1.000 | 837.734 | 877.887 |
| Depression | Anxiety | |||
|---|---|---|---|---|
| Unconditional Linear Model Parameter Estimate (SE) | Conditional Linear Model Parameter Estimate (SE) | Unconditional Linear Model Parameter Estimate (SE) | Conditional Linear Model Parameter Estimate (SE) | |
| Intercept on | ||||
| W1 Anxiety score a | 0.223 (0.156) | |||
| W1 Depression score a | 0.277 (0.161) | |||
| Age placed a | −0.267 (0.146) | −0.219 (0.125) | ||
| W1 Internalizing a | 0.401 (0.152) | 0.209 (0.190) | ||
| W1 Externalizing a | 0.004 (0.139) | −0.098 (0.197) | ||
| Sibling group a | 0.137 (0.132) | 0.050 (0.125) | ||
| W1 Parental sense of competency a | −0.546 (0.144) | −0.383 (0.152) | ||
| Slope on | ||||
| W1 Anxiety score a | 0.243 (0.119) | |||
| W1 Depression score a | −0.316 (0.234) | |||
| Age placed a | 0.439 (0.137) | 0.002 (0.253) | ||
| W1 Internalizing a | −0.235 (0.174) | −0.257 (0.289) | ||
| W1 Externalizing a | −0.294 (0.164) | 0.446 (0.271) | ||
| Sibling group a | 0.111 (0.164) | 0.013 (0.212) | ||
| W1 Parental sense of competency a | 0.347 (0.164) | −0.054 (0.256) | ||
| Means/intercept | ||||
| Intercept | 4.785 (0.337) | 13.997 (3.774) | 5.250 (0.318) | 14.675 (4.527) |
| Slope | 0.082 (0.126) | −3.600 (1.515) | 0.639 (0.126) | 0.604 (2.299) |
| Variances | ||||
| Intercept | 7.794 (2.134) | 2.451 (2.135) | 3.228 (2.318) | 6.986 (2.480) |
| Slope | 0.963 (0.378) | 1.142 (0.426) | −0.569 (0.349) | 0.994 (0.438) |
| Intercept-slope correlationa | −0.382 (0.149) | −0.262 (0.228) | −0.331 (0.225) | −0.076 (0.339) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Anthony, R.E.; Paine, A.L.; Shelton, K.H. Depression and Anxiety Symptoms of British Adoptive Parents: A Prospective Four-Wave Longitudinal Study. Int. J. Environ. Res. Public Health 2019, 16, 5153. https://doi.org/10.3390/ijerph16245153
Anthony RE, Paine AL, Shelton KH. Depression and Anxiety Symptoms of British Adoptive Parents: A Prospective Four-Wave Longitudinal Study. International Journal of Environmental Research and Public Health. 2019; 16(24):5153. https://doi.org/10.3390/ijerph16245153
Chicago/Turabian StyleAnthony, Rebecca E., Amy L. Paine, and Katherine H. Shelton. 2019. "Depression and Anxiety Symptoms of British Adoptive Parents: A Prospective Four-Wave Longitudinal Study" International Journal of Environmental Research and Public Health 16, no. 24: 5153. https://doi.org/10.3390/ijerph16245153
APA StyleAnthony, R. E., Paine, A. L., & Shelton, K. H. (2019). Depression and Anxiety Symptoms of British Adoptive Parents: A Prospective Four-Wave Longitudinal Study. International Journal of Environmental Research and Public Health, 16(24), 5153. https://doi.org/10.3390/ijerph16245153





