Effect of Training Load on Post-Exercise Cardiac Troponin T Elevations in Young Soccer Players
Abstract
1. Introduction
2. Experimental Section
2.1. Participants
2.2. Design
2.3. Instruments
2.4. Variables
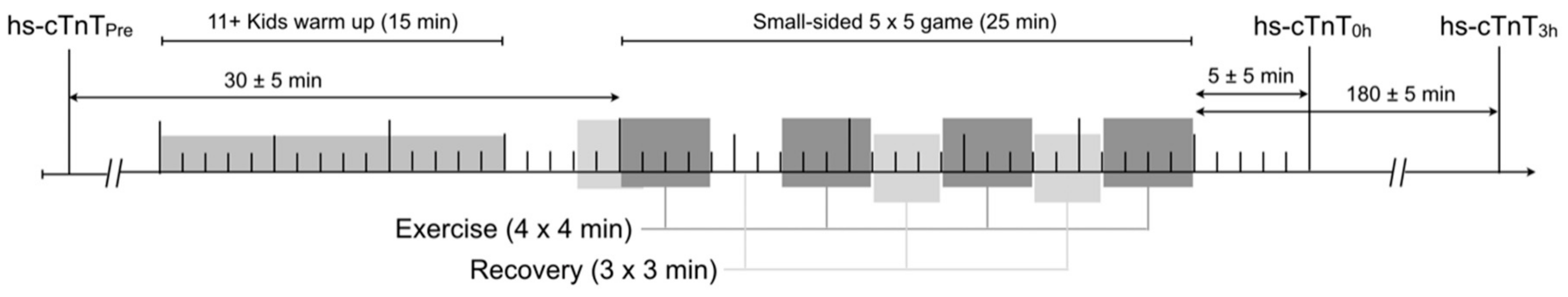
2.5. Experimental Setup and Protocol
2.6. Statistical analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- FIFA Communications Division FIFA Big Count 2006: 270 Million People Active in Football. Available online: https://www.fifa.com/mm/document/fifafacts/bcoffsurv/bigcount.statspackage_7024.pdf (accessed on 1 October 2019).
- Bourdon, P.C.; Cardinale, M.; Murray, A.; Gastin, P.; Kellmann, M.; Varley, M.C.; Gabbett, T.J.; Coutts, A.J.; Burgess, D.J.; Gregson, W.; et al. Monitoring Athlete Training Loads: Consensus Statement. Int. J. Sports Physiol. Perform. 2017, 12, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Impellizzeri, F.M.; Marcora, S.M.; Coutts, A.J. Internal and External Training Load: 15 Years On. Int. J. Sports Physiol. Perform. 2019, 14, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Buchheit, M. Monitoring training status with HR measures: Do all roads lead to Rome? Front. Physiol. 2014, 5, 73. [Google Scholar] [CrossRef] [PubMed]
- Modena, R.; Ferraresi, I.; Schena, F.; Impellizzeri, F.M.; Fanchini, M.; Coutts, A.J.; Ferraresi, I.; Modena, R.; Schena, F.; Coutts, A.J.; et al. Use of the CR100 Scale for Session Rating of Perceived Exertion in Soccer and Its Interchangeability with the CR10. Int. J. Sports Physiol. Perform. 2016, 11, 388–392. [Google Scholar]
- Edwards, S. The Heart Rate Monitor Book; Polar CIC: Sacramento, CA, USA, 1992. [Google Scholar]
- Stølen, T.; Chamari, K.; Castagna, C.; Wisløff, U. Physiology of Soccer. Sports Med. 2005, 35, 501–536. [Google Scholar] [CrossRef]
- Akubat, I.; Barrett, S.; Sagarra, M.L.; Abt, G. The Validity of External:Internal Training Load Ratios in Rested and Fatigued Soccer Players. Sports 2018, 6, 44. [Google Scholar] [CrossRef]
- Odqvist, M.; Andersson, P.O.; Tygesen, H.; Eggers, K.M.; Holzmann, M.J. High-Sensitivity Troponins and Outcomes After Myocardial Infarction. J. Am. Coll. Cardiol. 2018, 71, 2616–2624. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D. Fourth Universal Definition of Myocardial Infarction. J. Am. Coll. Cardiol. 2018, 33, 2551–2567. [Google Scholar] [CrossRef]
- Shave, R.; George, K.; Atkinson, G.; Hart, E.; Middleton, N.; Whyte, G.; Gaze, D.; Collinson, P.O. Exercise-induced cardiac troponin T release: A meta-analysis. Med. Sci. Sports Exerc. 2007, 39, 2099–2106. [Google Scholar] [CrossRef]
- Cirer-Sastre, R.; Legaz-Arrese, A.; Corbi, F.; George, K.; Nie, J.; Carranza-García, L.E.; Reverter-Masià, J. Cardiac Biomarker Release After Exercise in Healthy Children and Adolescents: A Systematic Review and Meta-Analysis. Pediatr. Exerc. Sci. 2019, 31, 28–36. [Google Scholar] [CrossRef]
- Eijsvogels, T.M.H.; Fernandez, A.B.; Thompson, P.D. Are There Deleterious Cardiac Effects of Acute and Chronic Endurance Exercise? Physiol. Rev. 2016, 96, 99–125. [Google Scholar] [CrossRef] [PubMed]
- Aakre, K.M.; Omland, T. Physical activity, exercise and cardiac troponins: Clinical implications. Prog. Cardiovasc. Dis. 2019, 52, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Whitehead, S.; Till, K.; Weaving, D.; Jones, B. The Use of Microtechnology to Quantify the Peak Match Demands of the Football Codes: A Systematic Review. Sports Med. 2018, 48, 2549–2575. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, F.A. Spanish version of the Physical Activity Readiness Questionnaire (C-AAF/rPAR-Q). Apunts 1994, 31, 301–310. [Google Scholar]
- World Medical Association World Medical Association Declaration of Helsinki: Ethical principles for medical research involving human subjects. JAMA 2013, 310, 2191–2194. [CrossRef] [PubMed]
- Molina, I.; Gómez, C.; Bastida, A.; Pino, J. Validez del dispositivo inercial WIMU PRO para el registro de la frecuencia cardiaca en un test de campo. SPORT TK Rev. Euroam. Cienc. Deporte 2018, 7, 81–86. [Google Scholar] [CrossRef]
- Muñoz-Lopez, A.; Granero-Gil, P.; Pino-Ortega, J.; Hoyo, M. The validity and reliability of a 5-hz GPS device for quantifying athletes’ sprints and movement demands specific to team sports. J. Hum. Sport Exerc. 2017, 12, 156–166. [Google Scholar] [CrossRef]
- Giannitsis, E.; Kurz, K.; Hallermayer, K.; Jarausch, J.; Jaffe, A.S.; Katus, H.A. Analytical validation of a high-sensitivity cardiac troponin T assay. Clin. Chem. 2010, 56, 254–261. [Google Scholar] [CrossRef]
- Borg, E.; Borg, G. A comparison of AME and CR100 for scaling perceived exertion. Acta Psychol. 2002, 109, 157–175. [Google Scholar] [CrossRef]
- Fox, S.M.; Naughton, J.P.; Haskell, W.L. Physical activity and the prevention of coronary heart disease. Ann. Clin. Res. 1971, 3, 404–432. [Google Scholar] [CrossRef]
- Tanner, J.M. Growth and maturation during adolescence. Nutr. Rev. 1981, 39, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Rössler, R.; Verhagen, E.; Rommers, N.; Dvorak, J.; Junge, A.; Lichtenstein, E.; Donath, L.; Faude, O. Comparison of the 11+ Kids’ injury prevention programme and a regular warmup in children’s football (soccer): A cost effectiveness analysis. Br. J. Sports Med. 2018, 53, 309–314. [Google Scholar] [CrossRef] [PubMed]
- Mascarin, R.B.; De Andrade, V.L.; Barbieri, R.A.; Loures, J.P.; Kalva-Filho, C.A.; Papoti, M. Dynamics of Recovery of Physiological Parameters After a Small-Sided Game in Women Soccer Players. Front. Physiol. 2018, 9, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, B.; Gelman, A.; Hoffman, M.D.; Lee, D.; Goodrich, B.; Betancourt, M.; Brubaker, M.; Guo, J.; Li, P.; Riddell, A. Stan: A Probabilistic Programming Language. J. Stat. Softw. 2017, 76, 1–32. [Google Scholar] [CrossRef]
- Bürkner, P.-C. brms: An R Package for Bayesian Multilevel Models Using Stan. J. Stat. Softw. 2017, 80, 1–28. [Google Scholar] [CrossRef]
- López-Laval, I.; Legaz-Arrese, A.; George, K.; Serveto-Galindo, O.; González-Rave, J.M.; Reverter-Masia, J.; Munguía-Izquierdo, D. Cardiac troponin I release after a basketball match in elite, amateur and junior players. Clin. Chem. Lab. Med. 2016, 54, 333–338. [Google Scholar] [CrossRef]
- Nie, J.; Tong, T.K.; Shi, Q.; Lin, H.; Zhao, J.; Tian, Y. Serum cardiac troponin response in adolescents playing basketball. Int. J. Sports Med. 2008, 29, 449–452. [Google Scholar] [CrossRef]
- Hosseini, S.M.; Azizi, M.; Samadi, A.; Talebi, N.; Hannes, G.; Burtscher, M. Impact of a Soccer Game on Cardiac Biomarkers in Adolescent Players. Pediatr. Exerc. Sci. 2018, 30, 90–95. [Google Scholar] [CrossRef]
- Ma, G.; Liu, Y.; Liu, K. Influence of repeated bouts of table tennis training on cardiac biomarkers in children. Pediatr. Cardiol. 2014, 35, 711–718. [Google Scholar] [CrossRef]
- Gresslien, T.; Agewall, S. Troponin and exercise. Int. J. Cardiol. 2016, 221, 609–621. [Google Scholar] [CrossRef]
- Tian, Y.; Nie, J.; Huang, C.; George, K.P. The kinetics of highly sensitive cardiac troponin T release after prolonged treadmill exercise in adolescent and adult athletes. J. Appl. Physiol. 2012, 113, 418–425. [Google Scholar] [CrossRef] [PubMed]
- Fu, F.H.; Nie, J.; George, K.; Tong, T.K.; Lin, H.; Shi, Q. Impact of a 21-km Run on Cardiac Biomarkers in Adolescent Runners. J. Exerc. Sci. Fit. 2010, 8, 61–66. [Google Scholar] [CrossRef]
- Legaz-Arrese, A.; Carranza-García, L.E.; Navarro-Orocio, R.; Valadez-Lira, A.; Mayolas-Pi, C.; Munguía-Izquierdo, D.; Reverter-Masía, J.; George, K. Cardiac Biomarker Release after Endurance Exercise in Male and Female Adults and Adolescents. J. Pediatr. 2017, 191, 96–102. [Google Scholar] [CrossRef] [PubMed]
- Fu, F.; Nie, J.; Tong, T. Serum Cardiac Troponin T in Adolescent Runners: Effects of Exercise Intensity and Duration. Int. J. Sports Med. 2009, 30, 168–172. [Google Scholar] [CrossRef]
- Peretti, A.; Mauri, L.; Masarin, A.; Annoni, G.; Corato, A.; Maloberti, A.; Giannattasio, C.; Vignati, G. Cardiac Biomarkers Release in Preadolescent Athletes After an High Intensity Exercise. High Blood Press. Cardiovasc. Prev. 2017, 25, 89–96. [Google Scholar] [CrossRef]
- Van Brussel, M.; Bongers, B.C.; Hulzebos, E.H.J.; Burghard, M.; Takken, T. A Systematic Approach to Interpreting the Cardiopulmonary Exercise Test in Pediatrics. Pediatr. Exerc. Sci. 2019, 31, 194–203. [Google Scholar] [CrossRef]
- Akubat, I.; Barrett, S.; Abt, G. Integrating the internal and external training loads in soccer. Int. J. Sports Physiol. Perform. 2014, 9, 457–462. [Google Scholar] [CrossRef]
| Variable | Mean ± SD |
|---|---|
| Age (years) | 11.9 ± 2 |
| Tanner stage (n) | II = 8, III = 8, IV = 4 |
| Height (cm) | 151.2 ± 13.1 |
| Weight (kg) | 43.1 ± 13 |
| BMI (kg/m2) | 18.4 ± 2.62 |
| Experience (years) | 5.9 ± 1.7 |
| HR max (bpm) | 208 ± 2 |
| Variable | Mean ± SD |
|---|---|
| Internal Training Load | |
| HR av (bpm) | 181.17 ± 8.97 |
| rHR av (% HR max) | 87.15 ± 4.46 |
| HR peak (bpm) | 198.5 ± 7.32 |
| rHR peak (% HR max) | 95.48 ± 3.46 |
| Time HR Zone 5 (min: s) | 13:23 ± 1:15 |
| ∆HR 1 min recovery (bpm) | −49.86 ± 7.61 |
| RPE (AU) | 17.25 ± 0.91 |
| External Training Load | |
| Distance (m) | 2101.22 ± 217.31 |
| rDistance (m min−1) | 131.33 ± 13.58 |
| Speed av (km h−1) | 7.34 ± 0.79 |
| Speed peak (km h−1) | 22.15 ± 1.86 |
| Time Speed Zone 4 (min) | 6.48 ± 5.02 |
| Distance Speed Zone 4 (min) | 40.04 ± 31.42 |
| Mixed Metrics of Training Load | |
| Session RPE (AU) | 431.25 ± 22.76 |
| Edwards’ TRIMP (AU) | 6013 ± 381.64 |
| Hs-cTnT | |
| Pre (ng/L) | 1.5 (IQR = 1.5–1.5) |
| 0 h (ng/L) | 1.5 (IQR = 1.5–1.94) |
| 3 h (ng/L) | 7.46 (IQR = 4.17–12.57) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cirer-Sastre, R.; Legaz-Arrese, A.; Corbi, F.; López-Laval, I.; Puente-Lanzarote, J.; Hernández-González, V.; Reverter-Masià, J. Effect of Training Load on Post-Exercise Cardiac Troponin T Elevations in Young Soccer Players. Int. J. Environ. Res. Public Health 2019, 16, 4853. https://doi.org/10.3390/ijerph16234853
Cirer-Sastre R, Legaz-Arrese A, Corbi F, López-Laval I, Puente-Lanzarote J, Hernández-González V, Reverter-Masià J. Effect of Training Load on Post-Exercise Cardiac Troponin T Elevations in Young Soccer Players. International Journal of Environmental Research and Public Health. 2019; 16(23):4853. https://doi.org/10.3390/ijerph16234853
Chicago/Turabian StyleCirer-Sastre, Rafel, Alejandro Legaz-Arrese, Francisco Corbi, Isaac López-Laval, Jose Puente-Lanzarote, Vicenç Hernández-González, and Joaquín Reverter-Masià. 2019. "Effect of Training Load on Post-Exercise Cardiac Troponin T Elevations in Young Soccer Players" International Journal of Environmental Research and Public Health 16, no. 23: 4853. https://doi.org/10.3390/ijerph16234853
APA StyleCirer-Sastre, R., Legaz-Arrese, A., Corbi, F., López-Laval, I., Puente-Lanzarote, J., Hernández-González, V., & Reverter-Masià, J. (2019). Effect of Training Load on Post-Exercise Cardiac Troponin T Elevations in Young Soccer Players. International Journal of Environmental Research and Public Health, 16(23), 4853. https://doi.org/10.3390/ijerph16234853









