Vulnerable Populations Exposed to Lead-Contaminated Drinking Water within Houston Ship Channel Communities
Abstract
1. Introduction
2. Materials and Methods
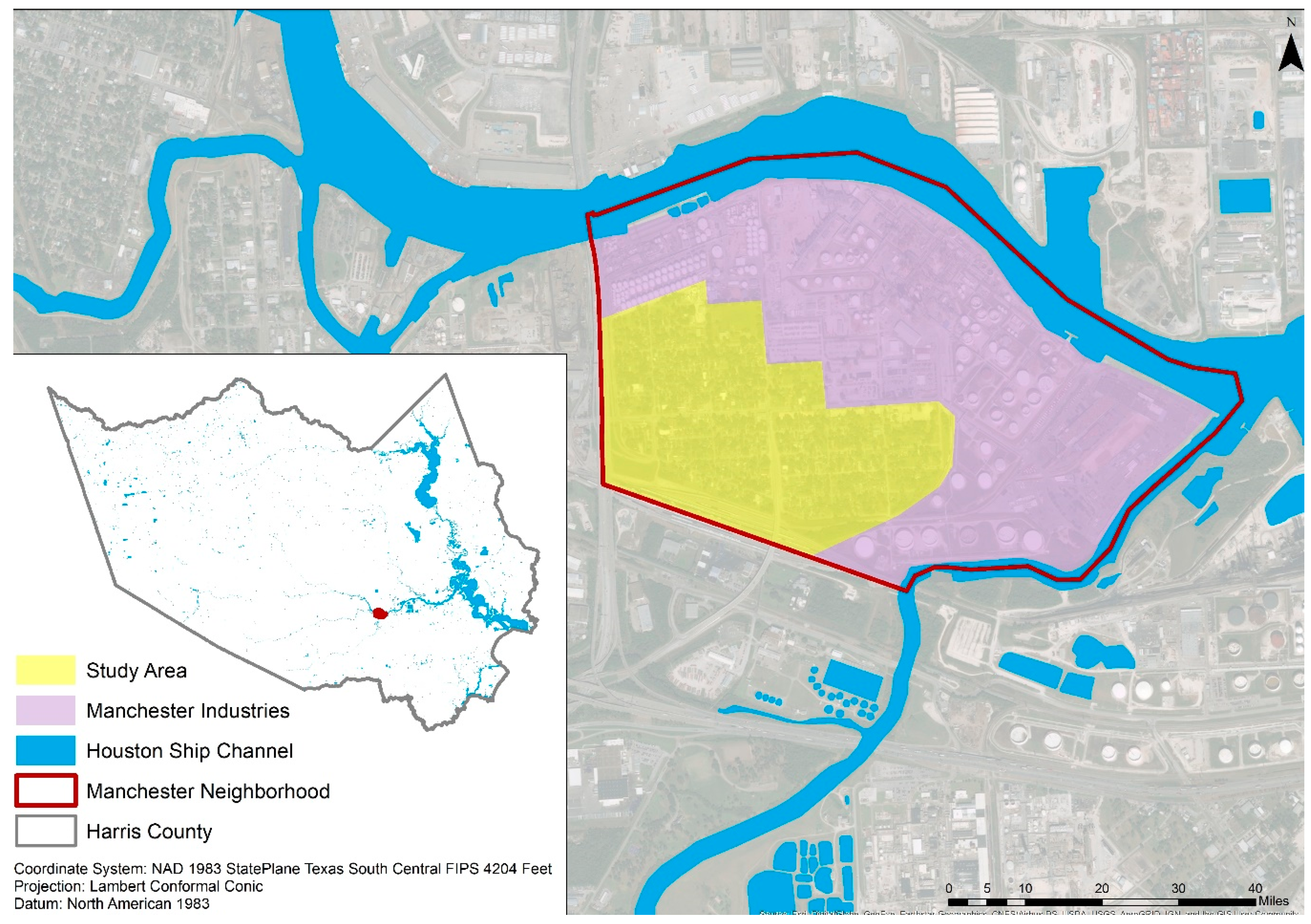
2.1. Study Location and Population
2.2. Household Survey
2.3. Household Tap Water
3. Results and Discussion
3.1. Household Survey
3.2. Household Tap Water
3.3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- International Agency for Research on Cancer. Summaries & Evaluations: Inorganic and Organic Lead Compounds; World Health Organization: Lyon, France, 2006. [Google Scholar]
- World Health Organization (WHO). Lead Poisoning and Health. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/lead-poisoning-and-health (accessed on 12 May 2019).
- Agency for Toxic Substances and Disease Registry. Toxicological Profile for Lead. Available online: https://www.atsdr.cdc.gov/toxprofiles/tp13.pdf (accessed on 10 April 2019).
- Environmental Protection Agency (EPA). Basic Information about Lead in Drinking Water. 2016. Available online: https://www.epa.gov/ground-water-and-drinking-water/basic-information-about-lead-drinking-water#getinto (accessed on 12 May 2019).
- Roberts, J.R.; Roberts, J.; Reigart, J.R.; Ebeling, M.; Hulsey, T.C. Time required for blood lead levels to decline in non-chelated children. J. Toxicol. Clin. Toxicol. 2001, 39, 153–160. [Google Scholar] [CrossRef] [PubMed]
- Canfield, R.L.; Henderson, C.R.; Cory-Slechta, D.A.; Cox, C.; Jusko, T.A.; Lanphear, B.P. Intellectual impairment in children with blood lead concentrations below 10 mg per deciliter. N. Engl. J. Med. 2003, 348, 1517–1526. [Google Scholar] [CrossRef] [PubMed]
- Centeno, J.A.; Mullick, F.G.; Martinez, L.; Page, N.P.; Gibb, H.; Longfellow, D.; Ladich, E.R. Pathology related to chronic lead exposure. Environ. Health Perspect. 2002, 110 (Suppl. S5), 883–886. [Google Scholar] [CrossRef]
- Bullard, R.D.; Johnson, G.S. Environmental justice: Grassroots activism and its impact on public policy decision making. J. Soc. Issues 2000, 56, 555–578. [Google Scholar] [CrossRef]
- Sampson, R.J.; Winter, A.S. The racial ecology of lead poisoning. Du Bois Rev. Soc. Sci. Res. Race 2016, 1, 1–23. [Google Scholar] [CrossRef]
- Whitehead, L.S.; Buchanan, S.D. Childhood lead poisoning: A perpetual environmental justice issue? J. Public Health Manag. Pract. 2019, 25, S115–S120. [Google Scholar] [CrossRef] [PubMed]
- Hauptman, M.; Bruccoleri, R.; Woolf, A.D. An update on childhood lead poisoning. Clin. Pediatr. Emerg. Med. 2017, 18, 181–192. [Google Scholar] [CrossRef] [PubMed]
- Kodras, K.; Ravenscroft, J.; McLean, E.V. Lead exposure in low and middle-income countries: Perspectives and lessons on patterns, injustices, economics, and politics. Int. J. Environ. Res. Public Health 2018, 15, 2351. [Google Scholar] [CrossRef]
- Wright, R.O.; Tsaih, S.W.; Schwartz, J.; Wright, R.J.; Hu, H. Association between iron deficiency and blood lead level in a longitudinal analysis of children followed in an urban primary care clinic. J. Pediatr. 2003, 142, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention [CDC]. Sources of Lead. 2013. Available online: https://www.cdc.gov/nceh/lead/tips/water.htm (accessed on 12 May 2019).
- Environmental Protection Agency (EPA). Understanding the Safe Drinking Water Act. 2004. Available online: https://www.epa.gov/sites/production/files/2015-04/documents/epa816f04030.pdf (accessed on 12 May 2019).
- Miranda, M.L.; Kim, D.; Hull, A.P.; Paul, C.J.; Galeano, M.A. Changes in blood lead levels associated with use of chloramines in water treatment systems. Environ. Health Perspect. 2006, 115, 221–225. [Google Scholar] [CrossRef] [PubMed]
- Renner, R. Out of plumb: When water treatment causes lead contamination. Environ. Health Perspect. 2009, 117, A542–A547. [Google Scholar] [CrossRef] [PubMed]
- Troesken, W. The Great Lead Water Pipe Disaster; MIT Press: Cambridge, MA, USA, 2006. [Google Scholar]
- Rabin, R. The lead industry and lead water pipes “A Modest Campaign”. Am. J. Public Health 2008, 98, 1584–1592. [Google Scholar] [CrossRef] [PubMed]
- Environmental Protection Agency (EPA). Alternative Disinfectants and Oxidants Guidance Manual; EPA 815-R99-014; United States Environmental Protection Agency: Washington, DC, USA, 1999. [Google Scholar]
- Environmental Protection Agency (EPA). Stage 1 Disinfectants and Disinfection Byproducts Rule; EPA 815-F-98-010; United States Environmental Protection Agency: Washington, DC, USA, 1998. [Google Scholar]
- Environmental Protection Agency (EPA). Basic Information about Chloramines. 2009. Available online: https://www.epa.gov/sites/production/files/2015-09/documents/q1.pdf (accessed on 18 January 2019).
- Environmental Protection Agency (EPA). Water Systems, Disinfection Byproducts, and the Use of Monochloramine. 2009. Available online: https://www.epa.gov/sites/production/files/2015-09/documents/why_are_water_utilities_switching_to_monochloramine.pdf (accessed on 8 December 2018).
- City of Houston Department of Health and Human Services. Community Health Profiles; Harrisburg/Manchester Super Neighborhood: Houston, TX, USA, 1999–2003. Available online: https://www.houstontx.gov/health/chs/Harrisburg-Manchester.pdf (accessed on 10 June 2019).
- A Closer Look at Air Pollution in Houston: Identifying Priority Health Risks. Available online: https://www3.epa.gov/ttnchie1/conference/ei16/session6/bethel.pdf (accessed on 30 July 2019).
- Kleiner, D.J. Handbook of Texas Online; Texas State Historical Association (TSHA): Manchester, TX, USA, 1952; Available online: https://tshaonline.org/handbook/online/articles/hvm20 (accessed on 1 April 2019).
- Environmental Protection Agency (EPA). TRI Basic Data Files. 2019. Available online: https://www.epa.gov/toxics-release-inventory-tri-program/tri-basic-data-files-calendar-years-1987-2017 (accessed on 10 June 2019).
- City of Houston Department of Public Works & Engineering. Water Quality Report. 2008. Available online: https://edocs.publicworks.houstontx.gov/documents/divisions/utilities/water_quality_report_2008.pdf (accessed on 1 January 2019).
- City of Houston Planning and Development Department. Harrisburge/Manchester Super Neighborhood. Available online: http://www.houstontx.gov/superneighborhoods/65.html (accessed on 20 February 2019).
- Ordonez, L. The Effect of Urbanization on the Streamflow’s of the Sims Bayou Watershed. Ph.D. Thesis, Office of Graduate and Professional Studies of Texas A&M University, College Station, TX, USA, 2015. [Google Scholar]
- Texas A&M University School of Public Health. EpiAssist. Available online: https://sph.tamhsc.edu/epi-bio/epi-assist.html (accessed on 30 July 2019).
- Environmental Protection Agency (EPA). 3Ts for Reducing Lead in Drinking Water Toolkit; EPA 815-F-18-022; United States Environmental Protection Agency: Washington, DC, USA, 2018. [Google Scholar]
- Environmental Protection Agency (EPA). Method 2007: Determination of Metals and Trace Elements in Water and Wastes by Inductively Coupled Plasma-Atomic Emission Spectrometry. 1994. Available online: https://www.epa.gov/homeland-security-research/method-2007-determination-metals-and-trace-elements-water-and-wastes (accessed on 12 June 2016).
- Manton, W.I.; Angle, C.R.; Stanek, K.L.; Reese, Y.R.; Kuehnemann, T.J. Acquisition and retention of lead by young children. Environ. Res. 2000, 82, 60–80. [Google Scholar] [CrossRef] [PubMed]
- National Center for Environmental Health (NCEH). CDC’s Childhood Lead and Prevention Program; CDC: Atlanta, GA, USA, 2013. [Google Scholar]
- Hanna-Attisha, M.; LaChance, J.; Sadler, R.C.; Schnepp, A.C. Elevated blood lead levels in children associated with the Flint drinking water crisis: A spatial analysis of risk and public health response. Am. J. Public Health 2016, 106, 283–290. [Google Scholar] [CrossRef] [PubMed]
- Campbell, C.; Greenberg, R.; Mankikar, D.; Ross, R.D. A case study of environmental injustice: The failure in Flint. Int. J. Environ. Res. Public Health 2016, 13, 951. [Google Scholar] [CrossRef] [PubMed]
- Sansom, G.; Berke, P.; McDonald, T.; Shipp, E.; Horney, J. Confirming the Environmental Concerns of Community Members Utilizing Participatory-Based Research in the Houston Neighborhood of Manchester. Int. J. Environ. Res. Public Health 2016, 13, 839. [Google Scholar] [CrossRef] [PubMed]
- Horney, J.; Casillas, G.; Baker, S.; Stone, K.; Kirsch, K.; Camargo, K.; Wade, T.; McDonald, T. Comparing residential contamination in a Houston environmental justice neighborhood before and after Hurricane Harvey. PLoS ONE 2018, 13, e192660. [Google Scholar] [CrossRef]
| Characteristics | N (%) |
|---|---|
| Gender | |
| Male | 2 (15.4%) |
| Female | 7 (53.8%) |
| Prefer not to answer | 4 (30.8%) |
| Race and Ethnicity | |
| Non-Hispanic White | 0 (0%) |
| Hispanic or Latino | 13 (100%) |
| African American | 0 (0%) |
| Other | 0 (0%) |
| Age (years) | |
| Mean (SD) | 53 (21.68) |
| Age in Groups (years) | |
| <35 | 2 (22.2%) |
| 36–50 | 3 (33.3%) |
| 51–69 | 2 (22.2%) |
| 70+ | 2 (22.2%) |
| Language Preference | |
| Spanish | 10 (76.9%) |
| English | 3 (23.1%) |
| N | % | |
|---|---|---|
| Tap Water Quality Concern | ||
| Yes, concerned | 4 | 30.8 |
| No, not concerned | 9 | 69.2 |
| Perceived Tap Water Problems among Concerned | ||
| The water is contaminated | 1 | 7.7 |
| The water has a bad smell | 3 | 23.1 |
| The water looks cloudy/dirty | 3 | 23.1 |
| The water is unhealthy | 2 | 15.4 |
| Sample No | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Lead (µg/L) | 1.2 | 2.4 | 1.0 | 0.6 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sansom, G.; Cizmas, L.; Aarvig, K.; Dixon, B.; Kirsch, K.R.; Katare, A.; Sansom, L. Vulnerable Populations Exposed to Lead-Contaminated Drinking Water within Houston Ship Channel Communities. Int. J. Environ. Res. Public Health 2019, 16, 2745. https://doi.org/10.3390/ijerph16152745
Sansom G, Cizmas L, Aarvig K, Dixon B, Kirsch KR, Katare A, Sansom L. Vulnerable Populations Exposed to Lead-Contaminated Drinking Water within Houston Ship Channel Communities. International Journal of Environmental Research and Public Health. 2019; 16(15):2745. https://doi.org/10.3390/ijerph16152745
Chicago/Turabian StyleSansom, Garett, Leslie Cizmas, Kathleen Aarvig, Benika Dixon, Katie R. Kirsch, Anjali Katare, and Lindsay Sansom. 2019. "Vulnerable Populations Exposed to Lead-Contaminated Drinking Water within Houston Ship Channel Communities" International Journal of Environmental Research and Public Health 16, no. 15: 2745. https://doi.org/10.3390/ijerph16152745
APA StyleSansom, G., Cizmas, L., Aarvig, K., Dixon, B., Kirsch, K. R., Katare, A., & Sansom, L. (2019). Vulnerable Populations Exposed to Lead-Contaminated Drinking Water within Houston Ship Channel Communities. International Journal of Environmental Research and Public Health, 16(15), 2745. https://doi.org/10.3390/ijerph16152745





