Impact of the Regional Network for AMI in the Management of STEMI on Care Processes, Outcomes and Health Inequities in the Veneto Region, Italy
Abstract
1. Introduction
2. Materials and Methods
2.1. Geographical and Socio-Demographic Context
2.2. Health Care System
2.3. The Veneto Region’s AMI Network
2.4. Materials
2.5. Performance Indicators
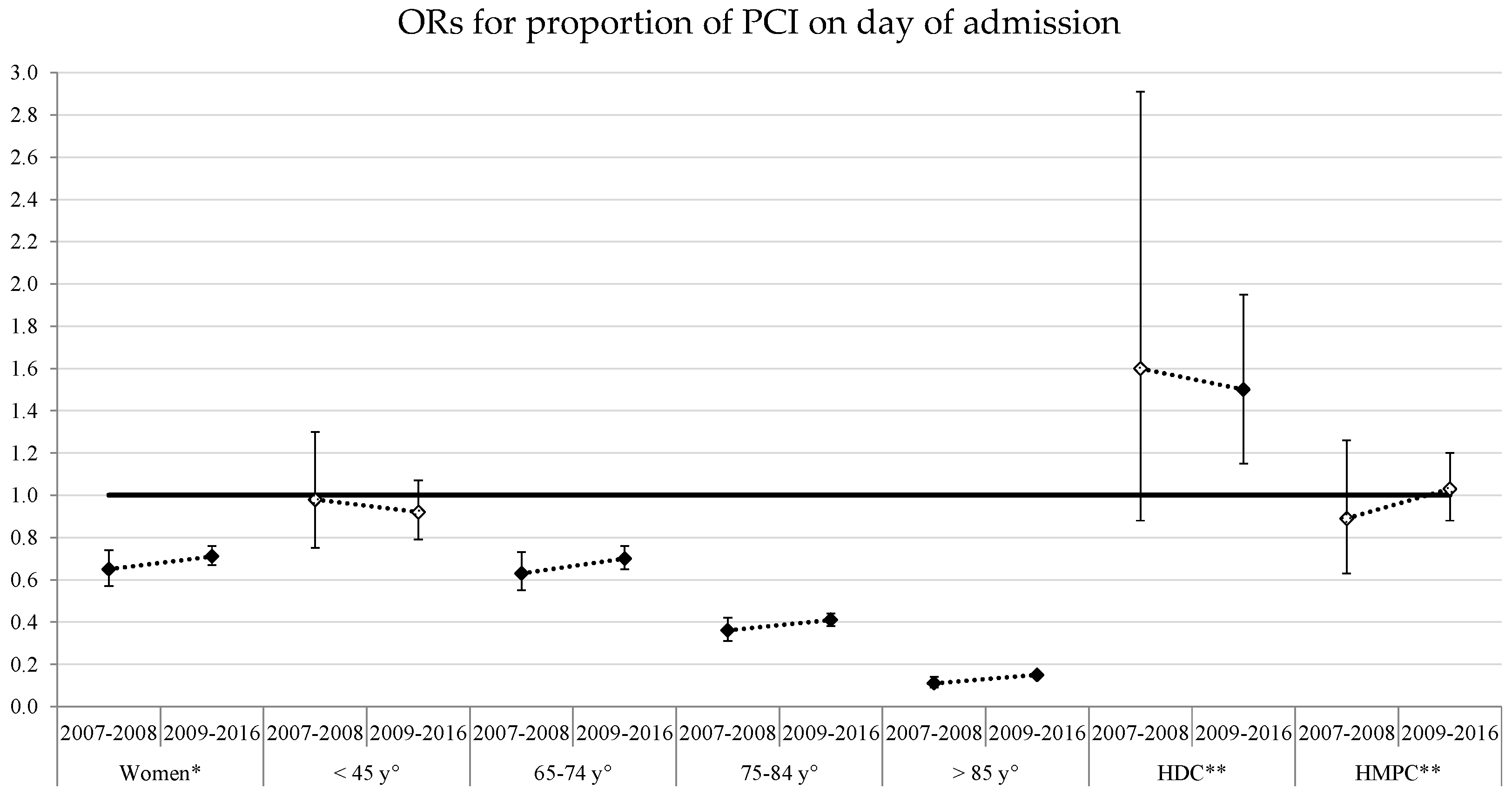
- The proportion of patients with STEMI treated with PCI within 24 h, since this was considered the treatment of choice in cases of STEMI; and
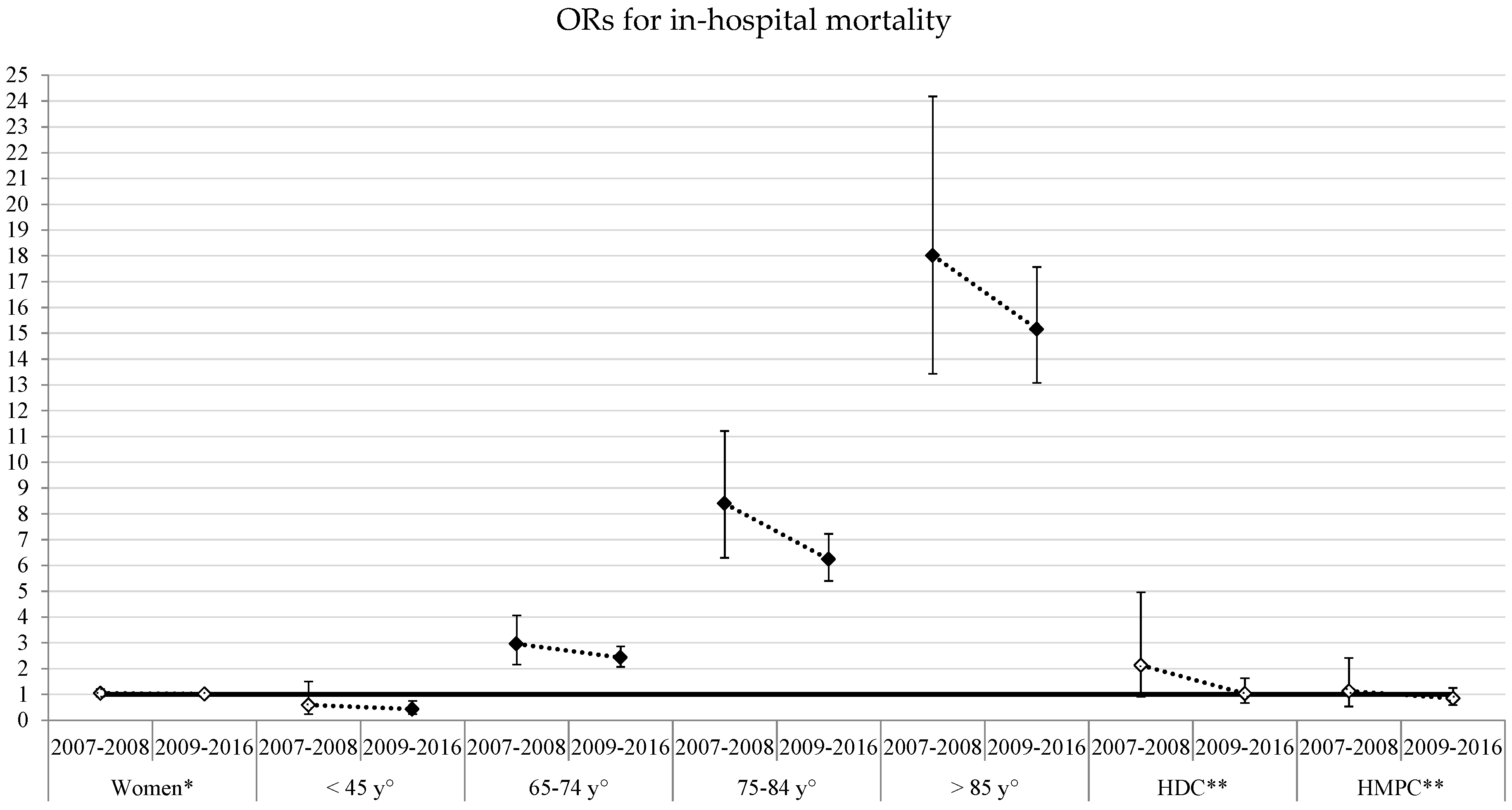
- The proportion of in-hospital deaths among patients treated for STEMI.
2.6. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- WHO Regional Office for Europe. Gaining Health: The European Strategy for the Prevention and Control of Noncommunicable Diseases; WHO Regional Office for Europe: Copenhagen, Denmark, 2006. [Google Scholar]
- Townsend, N.; Wilson, L.; Bhatnagar, P.; Wickramasinghe, K.; Rayner, M.; Nichols, M. Cardiovascular disease in Europe: Epidemiological update 2016. Eur. Heart J. 2016, 37, 3232–3245. [Google Scholar] [CrossRef] [PubMed]
- Hartley, A.; Marshall, D.C.; Salciccioli, J.D.; Sikkel, M.B.; Maruthappu, M.; Shalhoub, J. Trends in mortality from ischemic heart disease and cerebrovascular disease in Europe: 1980 to 2009. Circulation 2016, 133, 1916–1926. [Google Scholar] [CrossRef] [PubMed]
- Amit, G.; Cafri, C.; Gilutz, H.; Ilia, R.; Zahger, D. Benefit of direct ambulance to coronary care unit admission of acute myocardial infarction patients undergoing primary percutaneous intervention. Int. J. Cardiol. 2007, 119, 355–358. [Google Scholar] [CrossRef] [PubMed]
- Andersen, H.R.; Nielsen, T.T.; Rasmussen, K.; Thuesen, L.; Kelbaek, H.; Thayssen, P.; Abildgaard, U.; Pedersen, F.; Madsen, J.K.; Grande, P.; et al. DANAMI-2 Investigators. A comparison of coronary angioplasty with fibrinolytic therapy in acute myocardial infarction. N. Engl. J. Med. 2003, 349, 733–742. [Google Scholar] [CrossRef] [PubMed]
- Terkelsen, C.J.; Lassen, J.F.; Nørgaard, B.L.; Gerdes, J.C.; Poulsen, S.H.; Bendix, K.; Ankersen, J.P.; Gøtzsche, L.B.; Rømer, F.K.; Nielsen, T.T.; et al. Reduction of treatment delay in patients with ST-elevation myocardial infarction: Impact of pre-hospital diagnosis and direct referral to primary percutanous coronary intervention. Eur. Heart J. 2005, 26, 770–777. [Google Scholar] [CrossRef] [PubMed]
- Dorsch, M.F.; Greenwood, J.P.; Priestley, C.; Somers, K.; Hague, C.; Blaxill, J.M.; Wheatcroft, S.B.; Mackintosh, A.F.; McLenachan, J.M.; Blackman, D.J. Direct ambulance admission to the cardiac catheterization laboratory significantly reduces door-to-balloon times in primary percutaneous coronary intervention. Am. Heart J. 2008, 155, 1054–1058. [Google Scholar] [CrossRef] [PubMed]
- Brown, J.P.; Mahmud, E.; Dunford, J.V.; Ben-Yehuda, O. Effect of prehospital 12-lead electrocardiogram on activation of the cardiac catheterization laboratory and door-to-balloon time in ST-segment elevation acute myocardial infarction. Am. J. Cardiol. 2008, 101, 158–161. [Google Scholar] [CrossRef] [PubMed]
- Quinn, T.; Johnsen, S.; Gale, C.P.; Snooks, H.; McLean, S.; Woollard, M.; Weston, C.; Myocardial Ischaemia National Audit Project (MINAP) Steering Group. Effects of prehospital 12-lead ECG on processes of care and mortality in acute coronary syndrome: A linked cohort study from the Myocardial Ischaemia National Audit Project. Heart 2014, 100, 944–950. [Google Scholar] [CrossRef] [PubMed]
- Edmund Anstey, D.; Li, S.; Thomas, L.; Wang, T.Y.; Wiviott, S.D. Race and sex differences in management and outcomes of patients after ST-elevation and non-ST-elevation myocardial infarct: Results From the NCDR. Clin. Cardiol. 2016, 39, 585–595. [Google Scholar] [CrossRef] [PubMed]
- Canto, J.G.; Allison, J.J.; Kiefe, C.I.; Fincher, C.; Farmer, R.; Sekar, P.; Person, S.; Weissman, N.W. Relation of race and sex to the use of reperfusion therapy in Medicare beneficiaries with acute myocardial infarction. N. Engl. J. Med. 2000, 342, 1094–1100. [Google Scholar] [CrossRef] [PubMed]
- Vaccarino, V.; Rathore, S.S.; Wenger, N.K.; Frederick, P.D.; Abramson, J.L.; Barron, H.V.; Manhapra, A.; Mallik, S.; Krumholz, H.M.; National Registry of Myocardial Infarction Investigators. Sex and racial differences in the management of acute myocardial infarction, 1994 through 2002. N. Engl. J. Med. 2005, 353, 671–682. [Google Scholar] [CrossRef] [PubMed]
- Hagen, T.P.; Häkkinen, U.; Iversen, T.; Klitkou, S.T.; Moger, T.A.; EuroHOPE Study Group. Socio-economic inequality in the use of procedures and mortality among AMI patients: Quantifying the effects along different paths. Health Econ. 2015, 24, 102–115. [Google Scholar] [CrossRef] [PubMed]
- Mensah, G.A. Eliminating disparities in cardiovascular health: Six strategic imperatives and a framework for action. Circulation 2005, 111, 1332–1336. [Google Scholar] [CrossRef] [PubMed]
- Colais, P.; Agabiti, N.; Fusco, D.; Pinnarelli, L.; Sorge, C.; Perucci, C.A.; Davoli, M. Inequality in 30-day mortality and the wait for surgery after hip fracture: The impact of the regional health care evaluation program in Lazio (Italy). Int. J. Qual. Health Care 2013, 25, 239–247. [Google Scholar] [CrossRef] [PubMed]
- Huded, C.P.; Johnson, M.; Kravitz, K.; Menon, V.; Abdallah, M.; Gullett, T.C.; Hantz, S.; Ellis, S.G.; Podolsky, S.R.; Meldon, S.W. 4-Step Protocol for Disparities in STEMI Care and Outcomes in Women. J. Am. Coll. Cardiol. 2018, 71, 2122–2132. [Google Scholar] [CrossRef] [PubMed]
- Glickman, S.W.; Granger, C.B.; Ou, F.S.; O’Brien, S.; Lytle, B.L.; Cairns, C.B.; Mears, G.; Hoekstra, J.W.; Garvey, J.L.; Peterson, E.D.; et al. Impact of a statewide ST-segment-elevation myocardial infarction regionalization program on treatment times for women, minorities, and the elderly. Circ. Cardiovasc. Qual. Outcomes 2010, 514–521. [Google Scholar] [CrossRef] [PubMed]
- Evans, L.W.; van Woerden, H.; Davies, G.R.; Fone, D. Impact of service redesign on the socioeconomic inequity in revascularisation rates for patients with acute myocardial infarction: A natural experiment and electronic record-linked cohort study. BMJ Open 2016, 6, e011656. [Google Scholar] [CrossRef] [PubMed]
- Demografia in Cifre [Demography in Numbers][Website]; Rome: Istituto Nazionale di Statistica. 2018. Available online: http://demo.istat.it/ (accessed on 23 May 2018).
- Istituto Nazionale di Statistica [National Institute of Statistics][Website]. Rome: National Institute of Statistics. 2017. Available online: http://dati.istat.it (accessed on 25 May 2018).
- AUR—Anagrafe Unica Assistiti Regionale. Portale Sanità Regione del Veneto [Website]; Venice: Veneto Region, Italy. 2011. Available online: https://salute.regione.veneto.it/ web/bando-ssi/aur-anagrafe-unica-assistiti-regionale (accessed on 14 January 2015).
- World Health Organization. The Veneto Model—A Regional Approach to Tackling Global and European Health Challenges (2016). Available online: http://www.euro.who.int/en/publications/abstracts/the-veneto-model-a-regional-approach-to-tackling-global-and-european-health-challenges-2016 (accessed on 23 May 2018).
- Regione del Veneto; Bur n. 15 del 19 Febbraio 2008; Materia: Sanità e Igiene Pubblica; Deliberazione della Giunta Regionale n. 4550 del 28 Dicembre 2007 n.d. Available online: https://bur.regione.veneto.it/BurvServices/pubblica/DettaglioDgr.aspx?id=203192 (accessed on 28 February 2018).
- Documento di, Consenso. La rete interospedaliera per l’emergenza coronarica. Ital. Health J. 2005, 6, 56S–62S. Available online: http://www.giornaledicardiologia.it/allegati/00730_2005_12/fulltext/S6-05_02%205-26.pdf (accessed on 9 September 2018).
- Barchielli, A.; Profili, F.; Balzi, D.; Francesconi, P.; Zuppiroli, A.; Cipriani, F. Trends in occurrence, treatment, and outcomes of acute myocardial infarction in Tuscany Region (Central Italy), 1997–2010. Epidemiol. Prev. 2015, 39, 167–175. (In Italian) [Google Scholar] [PubMed]
- Sugiyama, T.; Hasegawa, K.; Kobayashi, Y.; Takahashi, O.; Fukui, T.; Tsugawa, Y. Differential time trends of outcomes and costs of care for acute myocardial infarction hospitalizations by ST elevation and type of intervention in the United States, 2001–2011. J. Am. Heart Assoc. 2015, 4, e001445. [Google Scholar] [CrossRef] [PubMed]
- McManus, D.D.; Gore, J.; Yarzebski, J.; Spencer, F.; Lessard, D.; Goldberg, R.J. Recent trends in the incidence, treatment, and outcomes of patients with STEMI and NSTEMI. Am. J. Med. 2011, 124, 40–47. [Google Scholar] [CrossRef] [PubMed]
- Yeh, R.W.; Sidney, S.; Chandra, M.; Sorel, M.; Selby, J.V.; Go, A.S. Population trends in the incidence and outcomes of acute myocardial infarction. N. Engl. J. Med. 2010, 362, 2155–2165. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Normand, S.L.; Wang, Y.; Drye, E.E.; Schreiner, G.C.; Krumholz, H.M. Recent declines in hospitalizations for acute myocardial infarction for Medicare fee-for-service beneficiaries: Progress and continuing challenges. Circulation 2010, 121, 1322–1328. [Google Scholar] [CrossRef] [PubMed]
- Luepker, R.V.; Berger, A.K. Is acute myocardial infarction disappearing? Circulation 2010, 121, 1280–1282. [Google Scholar] [CrossRef] [PubMed]
- Fordyce, C.B.; Al-Khalidi, H.R.; Jollis, J.G.; Roettig, M.L.; Gu, J.; Bagai, A.; Berger, P.B.; Corbett, C.C.; Dauerman, H.L.; Fox, K.; et al. STEMI Systems Accelerator Project. Association of rapid care process implementation on reperfusion times across multiple ST-segment-elevation myocardial infarction networks. Circ. Cardiovasc. Interv. 2017, 10, e004061. [Google Scholar] [CrossRef] [PubMed]
- Gersh, B.J.; Stone, G.W.; White, H.D.; Holmes, D.R. Pharmacological facilitation of primary percutaneous coronary intervention for acute myocardial infarction: Is the slope of the curve the shape of the future? JAMA 2005, 293, 979–986. [Google Scholar] [CrossRef] [PubMed]
- Reimer, K.A.; Lowe, J.E.; Rasmussen, M.M.; Jennings, R.B. The wavefront phenomenon of ischemic cell death. 1. Myocardial infarct size vs duration of coronary occlusion in dogs. Circulation 1977, 56, 786–794. [Google Scholar] [CrossRef] [PubMed]
- Flynn, A.; Moscucci, M.; Share, D.; Smith, D.; LaLonde, T.; Changezi, H.; Riba, A.; Gurm, H.S. Trends in door-to-balloon time and mortality in patients with ST-elevation myocardial infarction undergoing primary percutaneous coronary intervention. Arch. Intern. Med. 2010, 170, 1842–1849. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.Y.; Fonarow, G.C.; Hernandez, A.F.; Liang, L.; Ellrodt, G.; Nallamothu, B.K.; Shah, B.R.; Cannon, C.P.; Peterson, E.D. The dissociation between door-to-balloon time improvement and improvements in other acute myocardial infarction care processes and patient outcomes. Arch. Intern. Med. 2009, 169, 1411–1419. [Google Scholar] [CrossRef] [PubMed]
- Aday, L.A.; Begley, C.E.; Lairson, D.R.; Slater, C.H.; Richard, A.J.; Montoya, I.D. A framework for assessing the effectiveness, efficiency, and equity of behavioral healthcare. Am. J. Manag. Care 1999, 5, SP25–SP44. [Google Scholar] [PubMed]
- Van Oeffelen, A.A.; Rittersma, S.; Vaartjes, I.; Stronks, K.; Bots, M.L.; Agyemang, C. Are there ethnic inequalities in revascularisation procedure rate after an ST-elevation myocardial infarction? PLoS ONE 2015, 10, e0136415. [Google Scholar] [CrossRef] [PubMed]
- Bansal, N.; Fischbacher, C.M.; Bhopal, R.S.; Brown, H.; Steiner, M.F.; Capewell, S.; Scottish Health and Ethnicity Linkage Study. Myocardial infarction incidence and survival by ethnic group: Scottish Health and Ethnicity Linkage retrospective cohort study. BMJ Open 2013, 3, e003415. [Google Scholar] [CrossRef] [PubMed]
- Freund, K.M.; Jacobs, A.K.; Pechacek, J.A.; White, H.F.; Ash, A.S. Disparities by race, ethnicity, and sex in treating acute coronary syndromes. J. Womens Health 2012, 21, 126–132. [Google Scholar] [CrossRef] [PubMed]
- Iribarren, C.; Tolstykh, I.; Somkin, C.P.; Ackerson, L.M.; Brown, T.T.; Scheffler, R.; Syme, L.; Kawachi, I. Sex and racial/ethnic disparities in outcomes after acute myocardial infarction: A cohort study among members of a large integrated health care delivery system in northern California. Arch. Intern. Med. 2005, 165, 2105–2113. [Google Scholar] [CrossRef] [PubMed]
- Thomas, K.L.; Honeycutt, E.; Shaw, L.K.; Peterson, E.D. Racial differences in long-term survival among patients with coronary artery disease. Am. Heart J. 2010, 160, 744–751. [Google Scholar] [CrossRef] [PubMed]
- Buja, A.; Canavese, D.; Furlan, P.; Lago, L.; Saia, M.; Baldo, V. Are hospital process quality indicators influenced by socio-demographic health determinants. Eur. J. Public Health 2015, 25, 759–765. [Google Scholar] [CrossRef] [PubMed]
- Srichaiveth, B.; Ruengsakulrach, P.; Visudharom, K.; Sanguanwong, S.; Tangsubutr, W.; Insamian, P. Impact of gender on treatment and clinical outcomes in acute ST elevation myocardial infarction patients in Thailand. J. Med. Assoc. Thai. 2007, 90, 65–73. [Google Scholar] [PubMed]
- Falcone, M.; Del Santo, S.; Forni, S.; Pepe, P.; Marchi, M.; Rossi, G. Equity of access to percutaneous transluminal coronary angioplasty (PTCA) among patients with acute myocardial infarction in Tuscany Region (Central Italy), 2001–2008. Epidemiol. Prev. 2013, 37, 386–395. (In Italian) [Google Scholar] [PubMed]
- Pilgrim, T.; Heg, D.; Tal, K.; Erne, P.; Radovanovic, D.; Windecker, S.; Jüni, P.; AMIS Plus Investigators. Age- and gender-related disparities in primary percutaneous coronary interventions for acute ST-segment elevation myocardial infarction. PLoS ONE 2015, 10, e0137047. [Google Scholar] [CrossRef] [PubMed]
- Blair, I.V.; Steiner, J.F.; Havranek, E.P. Unconscious (implicit) bias and health disparities: Where do we go from here? Perm. J. 2011, 15, 71–78. [Google Scholar] [PubMed]
- Schulman, K.A.; Berlin, J.A.; Harless, W.; Kerner, J.F.; Sistrunk, S.; Gersh, B.J.; Dubé, R.; Taleghani, C.K.; Burke, J.E.; Williams, S.; et al. The effect of race and sex on physicians’ recommendations for cardiac catheterization. N. Engl. J. Med. 1999, 340, 618–626. [Google Scholar] [CrossRef] [PubMed]
- Peterson, E.D.; Shah, B.R.; Parsons, L.; Pollack, CV.; French, W.J.; Canto, J.G.; Gibson, C.M.; Rogers, W.J. Trends in quality of care for patients with acute myocardial infarction in the National Registry of Myocardial Infarction from 1990 to 2006. Am. Heart J. 2008, 156, 1045–1055. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.Y.; Dai, D.; Hernandez, A.F.; Bhatt, D.L.; Heidenreich, P.A.; Fonarow, G.C.; Peterson, E.D. The importance of consistent, high-quality acute myocardial infarction and heart failure care results from the American Heart Association’s Get with the Guidelines Program. J. Am. Coll. Cardiol. 2011, 58, 637–644. [Google Scholar] [CrossRef] [PubMed]
| Hospital Admissions | Mean Age | Average Hospital Stay | PCI on Day of Admission | In-Hospital Mortality | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | (y) ± SD | d ± SD | n | % | n | % | |
| Total | 36,035 | - | 70.1 ± 14.3 | 9.24 ± 8.80 | 16,075 | 44.6 | 4385 | 12.2 |
| Gender | ||||||||
| Male | 23,862 | 66.2 | 66.2 ± 13.5 | 8.82 ± 8.75 | 12,284 | 51.5 | 2162 | 9.1 |
| Female | 12,173 | 33.8 | 77.7 ± 12.7 | 10.04 ± 8.83 | 3791 | 31.1 | 2223 | 18.3 |
| Age | ||||||||
| <45 y | 1424 | 3.9 | 40.0 ± 4.4 | 7.34 ± 8.44 | 844 | 59.3 | 18 | 1.3 |
| 45–64 y | 11,415 | 31.7 | 55.9 ± 5.4 | 7.61 ± 6.51 | 7012 | 61.4 | 312 | 2.7 |
| 65–74 y | 7949 | 22.1 | 69.6 ± 2.9 | 9.19 ± 8.96 | 4039 | 50.8 | 536 | 6.7 |
| 75–84 y | 8771 | 24.3 | 79.6 ± 2.9 | 10.90 ± 10.63 | 3147 | 35.9 | 1432 | 16.3 |
| >84 y | 6476 | 18.0 | 89.4 ± 3.7 | 10.33 ± 8.86 | 1033 | 16.0 | 2087 | 32.2 |
| Citizenship | ||||||||
| Italian | 34,414 | 95.5 | 70.7 ± 14.0 | 8.4 ± 7.3 | 15,130 | 44.0 | 4314 | 12.5 |
| HDC | 394 | 10.9 | 62.9 ± 11.8 | 8.2 ± 10.4 | 262 | 66.5 | 29 | 7.4 |
| HMPC | 1127 | 3.1 | 52.7 ± 12.2 | 11.8 ± 10.9 | 645 | 57.2 | 38 | 3.4 |
| % of PCI Within 24 h | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 2007 (n = 4040) | 2008 (n = 4083) | 2009 (n = 3908) | 2010 (n = 3793) | 2011 (n = 3644) | 2012 (n = 3536) | 2013 (n = 3362) | 2014 (n = 3252) | 2015 (n = 3228) | 2016 (n = 3189) | APC (CI 95%) | |
| Gender | |||||||||||
| Male | 38.1 | 40.8 | 42.5 | 48.3 | 49.9 | 54.4 | 59.0 | 61.0 | 62.2 | 64.2 | 6.3 (5.4;7.3) ° |
| Female | 18.6 | 22.5 | 28.6 | 28.5 | 32.4 | 32.9 | 38.2 | 38.8 | 40.8 | 40.6 | 8.6 (6.2;11.1) ° |
| Age | |||||||||||
| <45 y | 51.3 | 47.0 | 60.9 | 53.0 | 58.8 | 63.4 | 69.4 | 69.7 | 66.7 | 59.6 | 3.3 (0.9;5.8) ° |
| 45–64 y | 47.8 | 49.9 | 53.2 | 61.2 | 60.9 | 63.2 | 68.7 | 68.9 | 71.8 | 71.9 | 4.9 (3.8;6.0) ° |
| 65–74 y | 35.2 | 39.2 | 43.6 | 44.5 | 50.6 | 54.8 | 59.2 | 61.4 | 63.4 | 64.5 | 7.2 (6.0;8.4) ° |
| 75–84 y | 22.0 | 25.9 | 27.5 | 32.8 | 35.9 | 37.7 | 44.9 | 47.5 | 47.8 | 50.5 | 9.8 (8.2;11.5) ° |
| >84 y | 8.0 | 9.4 | 12.6 | 14.9 | 14.9 | 19.3 | 17.3 | 21.9 | 22.1 | 24.2 | 12.5 (9.4;15.6) ° |
| Citizenship | |||||||||||
| Italian | 30.4 | 33.8 | 37.2 | 40.8 | 43.7 | 46.9 | 51.1 | 53.1 | 54.7 | 56.2 | 7.2 (6.1;8.3) ° |
| HDC | 50.0 | 46.4 | 68.3 | 46.0 | 62.9 | 61.3 | 92.5 | 77.3 | 74.5 | 76.3 | 6.1 (1.8;10.6) ° |
| HMPC | 41.1 | 44.6 | 45.5 | 60.0 | 54.3 | 52.3 | 65.3 | 66.1 | 63.4 | 70.9 | 5.9 (3.8;8.1) ° |
| % in-Hospital Mortality | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 2007 (n = 4040) | 2008 (n = 4083) | 2009 (n = 3908) | 2010 (n = 3793) | 2011 (n = 3644) | 2012 (n = 3536) | 2013 (n = 3362) | 2014 (n = 3252) | 2015 (n = 3228) | 2016 (n = 3189) | APC (CI 95%) | |
| Gender | |||||||||||
| Male | 9.9 | 8.7 | 9.8 | 9.0 | 9.6 | 9.3 | 8.5 | 9.8 | 8.2 | 7.5 | −1.9 (−3.7;0.0) |
| Female | 18.9 | 19.4 | 16.7 | 18.4 | 20.6 | 17.8 | 19.4 | 16.6 | 17.7 | 16.2 | −1.2 (−3.1;0.6) |
| Age | |||||||||||
| <45 y | 1.3 | 1.8 | - | 0.7 | 3.3 | 0.6 | 0.8 | 1.6 | 1.8 | 1.0 | −1.6 (−16.0;15.3) * |
| 45–64 y | 3.1 | 1.9 | 2.6 | 2.5 | 2.7 | 2.7 | 3.0 | 4.1 | 2.3 | 2.5 | 1.4 (−3.9;6.9) |
| 65–74 y | 7.7 | 6.5 | 6.4 | 7.2 | 8.1 | 7.3 | 6.0 | 7.2 | 5.9 | 4.8 | −3.0 (−6.2;0.3) |
| 75–84 y | 18.1 | 17.6 | 17.3 | 16.1 | 16.8 | 17.9 | 15.3 | 14.1 | 15.1 | 13.1 | −3.0 (−4.5;−1.6) ° |
| >84 y | 31.2 | 34.0 | 31.7 | 31.1 | 35.3 | 29.5 | 35.3 | 31.6 | 31.6 | 31.1 | −0.2 (−1.8;1.4) |
| Citizenship | |||||||||||
| Italian | 13.5 | 12.9 | 12.4 | 12.7 | 13.6 | 12.6 | 12.6 | 12.4 | 11.6 | 10.4 | −1.9 (−3.2;−0.6) ° |
| HDC | 15.6 | 7.1 | 7.3 | 4.0 | 8.6 | 6.5 | 7.5 | 6.8 | 7.3 | 5.3 | −4.9 (−12.6;3.5) |
| HMPC | 5.3 | 3.0 | 4.0 | 3.6 | 1.7 | 3.6 | 1.6 | 3.3 | 3.3 | 4.7 | −1.8 (−11.5;8.9) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Saia, M.; Mantoan, D.; Fonzo, M.; Bertoncello, C.; Soattin, M.; Sperotto, M.; Baldovin, T.; Furlan, P.; Scapellato, M.L.; Viel, G.; et al. Impact of the Regional Network for AMI in the Management of STEMI on Care Processes, Outcomes and Health Inequities in the Veneto Region, Italy. Int. J. Environ. Res. Public Health 2018, 15, 1980. https://doi.org/10.3390/ijerph15091980
Saia M, Mantoan D, Fonzo M, Bertoncello C, Soattin M, Sperotto M, Baldovin T, Furlan P, Scapellato ML, Viel G, et al. Impact of the Regional Network for AMI in the Management of STEMI on Care Processes, Outcomes and Health Inequities in the Veneto Region, Italy. International Journal of Environmental Research and Public Health. 2018; 15(9):1980. https://doi.org/10.3390/ijerph15091980
Chicago/Turabian StyleSaia, Mario, Domenico Mantoan, Marco Fonzo, Chiara Bertoncello, Marta Soattin, Milena Sperotto, Tatjana Baldovin, Patrizia Furlan, Maria Luisa Scapellato, Guido Viel, and et al. 2018. "Impact of the Regional Network for AMI in the Management of STEMI on Care Processes, Outcomes and Health Inequities in the Veneto Region, Italy" International Journal of Environmental Research and Public Health 15, no. 9: 1980. https://doi.org/10.3390/ijerph15091980
APA StyleSaia, M., Mantoan, D., Fonzo, M., Bertoncello, C., Soattin, M., Sperotto, M., Baldovin, T., Furlan, P., Scapellato, M. L., Viel, G., Baldo, V., Cocchio, S., & Buja, A. (2018). Impact of the Regional Network for AMI in the Management of STEMI on Care Processes, Outcomes and Health Inequities in the Veneto Region, Italy. International Journal of Environmental Research and Public Health, 15(9), 1980. https://doi.org/10.3390/ijerph15091980








