Learning and Action in Community Health: Using the Health Belief Model to Assess and Educate African American Community Residents about Participation in Clinical Research
Abstract
1. Introduction
The Learning and Action in Community Health Project
2. Materials and Methods
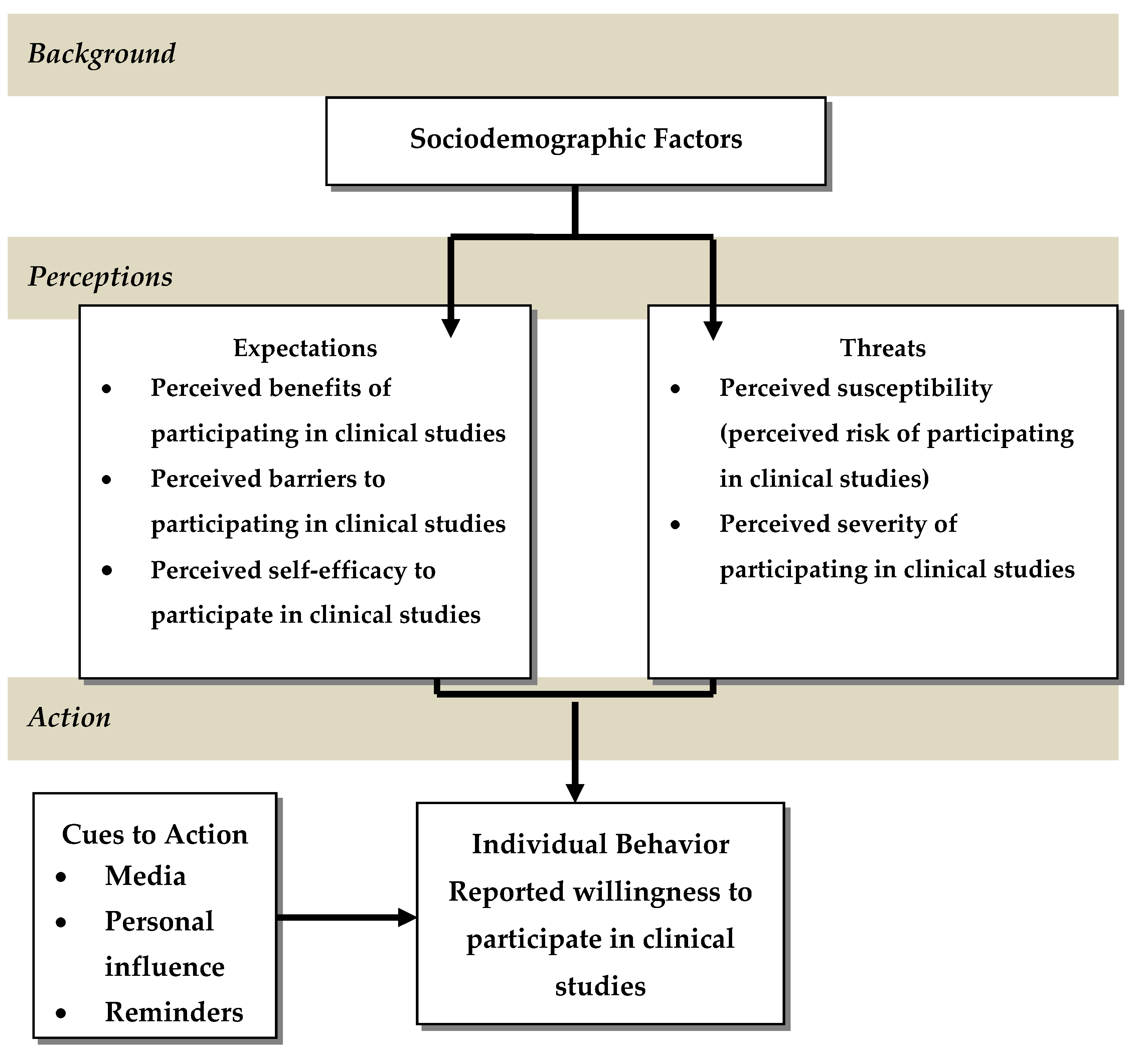
2.1. Theoretical Framework
2.2. Study Design
2.3. Study Population
2.4. Intervention
2.5. Quantitative Data Collection
2.6. Quantitative Data Analysis
2.7. Qualitative Data Collection
2.8. Qualitative Data Analysis
3. Results
3.1. Quantitative Results
3.2. Qualitative Results: Descriptive Analysis of Focus Group Data
3.2.1. Perceived Benefits of Clinical Research Participation
I am not a proponent of drug use as the treatment of choice, but some drugs do help some people in certain situations and it’s absolutely essential that those drugs be tested before they’re released to the public. So it has its place. I believe it is important.
Each generation, each age, each color, there’s the benefits of knowing that it can help somebody else out. But the main compensation coming from the hood would be getting paid.
With these studies that are prevalent now and targeted for minority environments, the way I see it is that {it} affords them an opportunity to get medical attention that perhaps they couldn’t have gotten earlier because they did not have proper medical attention.
3.2.2. Perceived Barriers to Clinical Research Participation
Prior to this experience I would never have considered participating because I would feel like a guinea pig. Like they’re wanting me to sample something that they don’t even know what the effects are. So I wouldn’t have considered it because I was afraid.
I think we have a checkered past here in the United States. They gave Indians smallpox. They gave black guys syphilis and then refused to give them the treatment. So a lot of people in our community think about things like that before they will go somewhere and get stuck or give blood.
I think too is just where like my age group just don’t want to take the time to really participate.
3.2.3. Cues to Action
Many proposals for the various studies are written from the academic perspective, and meeting their standards. However, I think it was at a sixth or eighth grade level that every proposal should be—somebody in that region should be able to see it, read it, and say okay this is what I’m going to be a part of.
So to me social media, I’m not going to say is the media, but it is a reliable platform for me. If you think past just a quick selfie that people are posting or just a quick little videos that are being passed on every day, it can be helpful and beneficial to engage people directly like in groups or have a video that’s shared from a group or something like that. So it can be a useful platform.
So if a black person knows that their auntie is going a lot and she’s getting all of these benefits or perks or whatever you want to call them, then maybe she’ll go, she’ll tell her friend, and that cycle will continue.
And you have health fairs. A lot of people don’t have insurance even with the Obamacare and I know a friend of mine, she goes to health fairs to get her mammogram and blood work and everything because she doesn’t have the money. So a lot of times health fairs, that’s what people are going for now—for health fairs because they’re offering to check your diabetes, check this, check that. When you don’t have the funds and you want to stay as healthy as you possibly can but sometimes your pocketbook doesn’t let you. You know what I mean?
A few years ago I went to the job fair hosted by the City of Atlanta. And out of the 80 vendors that were there, 20 of them were actually selling products. What would be great is if people had this knowledge {of clinical research opportunities}.
Culturally we’re very social so that’s certainly a good place to start. I think any time you make something lecture style you’re going to lose quite a bit of people. It’s just—that’s just how it is.
Because a lot of us attend church and we listen to our pastors and church leaders. We trust them
I’m 18, so …we could also go to schools … and they would have people … come to the school and talk to them about it.
Maybe presidents of our homeowners associations or like the neighborhood watch leaders, Boys and Girls Club presidents, things like that.
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Murphy, F.; Jackson, P.; Johnson, P.; Ofili, E.; Cashmire, N.; Quarshie, A. Informing and Consenting Disadvantaged Populations for Clinical and Community Research. Am. J. Health Stud. 2005, 19, 246–253. [Google Scholar]
- Yancey, A.K.; Ortega, A.N.; Kumanyika, S.K. Effective recruitment and retention of minority research participants. Annu. Rev. Public Health 2006, 27, 1–28. [Google Scholar] [CrossRef] [PubMed]
- Roundtable on the Promotion of Health Equity and the Elimination of Health Disparities; Board on Population Health and Public Health Practice; Health and Medicine Division; National Academies of Sciences, Engineering, and Medicine. Strategies for Ensuring Diversity, Inclusion, and Meaningful Participation in Clinical Trials: Proceedings of a Workshop. Available online: https://www.ncbi.nlm.nih.gov/books/NBK384602/ (accessed on 13 July 2018).
- George, S.; Duran, N.; Norris, K. A systematic review of barriers and facilitators to minority research participation among African Americans, Latinos, Asian Americans, and Pacific Islanders. Am. J. Public Health 2014, 104, e16–e31. [Google Scholar] [CrossRef] [PubMed]
- Nicholson, L.M.; Schwirian, P.M.; Groner, J.A. Recruitment and retention strategies in clinical studies with low-income and minority populations: Progress from 2004–2014. Contemp. Clin. Trials 2015, 45, 34–40. [Google Scholar] [CrossRef] [PubMed]
- Hagiwara, N.; Berry-Bobovski, L.; Francis, C.; Ramsey, L.; Chapman, R.A.; Albrecht, T.L. Unexpected findings in the exploration of African American underrepresentation in biospecimen collection and biobanks. J. Cancer Educ. 2014, 29, 580–587. [Google Scholar] [CrossRef] [PubMed]
- Cain, G.E.; Kalu, N.; Kwagyan, J.; Marshall, V.J.; Ewing, A.T.; Bland, W.P.; Hesselbrock, V.; Taylor, R.E.; Scott, D.M. Beliefs and preferences for medical research among African-Americans. J. Racial Ethn. Health Dispar. 2016, 3, 74–82. [Google Scholar] [CrossRef] [PubMed]
- Cortés, Y.I.; Arcia, A.; Kearney, J.; Luchsinger, J.; Lucero, R.J. Urban-Dwelling Community Members’ Views on Biomedical Research Engagement. Qual. Health Res. 2017, 27, 130–137. [Google Scholar] [CrossRef] [PubMed]
- Castillo-Mancilla, J.R.; Cohn, S.E.; Krishnan, S.; Cespedes, M.; Floris-Moore, M.; Schulte, G.; Pavlov, G.; Mildvan, D.; Smith, K.Y.; ACTG Underrepresented Populations Survey Group. Minorities remain underrepresented in HIV/AIDS research despite access to clinical trials. HIV Clin. Trials 2014, 15, 14–26. [Google Scholar] [CrossRef] [PubMed]
- Coakley, M.; Fadiran, E.O.; Parrish, J.; Griffith, R.A.; Weiss, E.; Carter, C. Dialogues on diversifying clinical trials: Successful strategies for engaging women and minorities in clinical trials. J. Women’s Health 2012, 21, 713–716. [Google Scholar] [CrossRef] [PubMed]
- Johnson, D.A.; Joosten, Y.A.; Wilkins, C.H.; Shibao, C.A. Case Study: Community engagement and clinical trial success: Outreach to African American Women. Clin. Trans. Sci. 2015, 8, 388–390. [Google Scholar] [CrossRef] [PubMed]
- Wendler, D.; Kington, R.; Madans, J.; Van Wye, G.; Christ-Schmidt, H.; Pratt, L.A.; Brawley, O.W.; Gross, C.P.; Emanuel, E. Are racial and ethnic minorities less willing to participate in health research? PLoS Med. 2005, 3, 201–210. [Google Scholar] [CrossRef] [PubMed]
- Ford, J.G.; Howerton, M.W.; Lai, G.Y.; Gary, T.L.; Bolen, S.; Gibbons, M.C.; Tilburt, J.; Baffi, C.; Tanpitukpongse, T.P.; Wilson, R.F.; et al. Barriers to recruiting underrepresented populations to cancer clinical trials: A systematic review. Cancer Interdiscip. Int. J. Am. Cancer Soc. 2008, 112, 228–242. [Google Scholar] [CrossRef] [PubMed]
- Dickerson, D.O.; MPH, D.L.; Leeman, R.F.; Mazure, C.M.; O’Malley, S.S. The inclusion of women and minorities in smoking cessation clinical trials: A systematic review. Am. J. Addict. 2009, 18, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Rivers, D.; August, E.M.; Ivana, S.; Green, B.L.; Quinn, G.P. A systematic review of the factors influencing African Americans’ participation in cancer clinical trials. Contemp. Clin. Trials 2013, 35, 13–32. [Google Scholar] [CrossRef] [PubMed]
- Frew, P.M.; Schamel, J.T.; O’Connell, K.A.; Randall, L.A.; Boggavarapu, S. Results of a community randomized study of a faith-based education program to improve clinical trial participation among African Americans. Int. J. Environ. Res. Public Health 2015, 13, 41. [Google Scholar] [CrossRef] [PubMed]
- Dash, C.; Wallington, S.F.; Muthra, S.; Dodson, E.; Mandelblatt, J.; Adams-Campbell, L.L. Disparities in knowledge and willingness to donate research biospecimens: A mixed-methods study in an underserved urban community. J. Community Genet. 2014, 5, 329–336. [Google Scholar] [CrossRef] [PubMed]
- Lang, R.; Kelkar, V.A.; Byrd, J.R.; Edwards, C.L.; Pericak-Vance, M.; Byrd, G.S. African American participation in health-related research studies: Indicators for effective recruitment. J. Public Health Manag. Pract. 2013, 19, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Napoles, A.; Cook, E.; Ginossar, T.; Knight, K.D.; Ford, M.E. Applying a conceptual framework to maximize the participation of diverse populations in cancer clinical trials. Adv. Cancer Res. 2017, 133, 77–94. [Google Scholar] [PubMed]
- Luebbert, R.; Perez, A. Barriers to clinical research participation among African Americans. J. Transcult. Nurs. 2016, 27, 456–463. [Google Scholar] [CrossRef] [PubMed]
- RCMI Translational Research Network Website. Available online: http://www.rtrn.net/rtrn-aims-goals/ (accessed on 29 June 2018).
- Glanz, K.; Rimer, B.K.; Viswanath, K. Health Behavior and Health Education: Theory, Research, and Practice; John Wiley & Sons: Hoboken, NJ, USA, 2008. [Google Scholar]
- Kirscht, J.P. The health belief model and illness behavior. Health Educ. Monogr. 1974, 2, 387–408. [Google Scholar] [CrossRef]
- Becker, M.H. The health belief model and sick role behavior. Health Educ. Monogr. 1974, 2, 409–419. [Google Scholar] [CrossRef]
- Becker, M.H.; Radius, S.M.; Rosenstock, I.M.; Drachman, R.H.; Schuberth, K.C.; Teets, K.C. Compliance with a medical regimen for asthma: A test of the health belief model. Public Health Rep. 1978, 93, 268–277. [Google Scholar] [PubMed]
- Seligman, M.E. Helplessness: On Depression, Development, and Death. A Series of Books in Psychology; WH Freeman/Times Books/Henry Holt & Co.: New York, NY, USA, 1975. [Google Scholar]
- Haggstrom, D.A.; Schapira, M.M. Black-white differences in risk perceptions of breast cancer survival and screening mammography benefit. J. Gen. Intern. Med. 2006, 21, 371–377. [Google Scholar] [CrossRef] [PubMed]
- Gale, N.K.; Heath, G.; Cameron, E.; Rashid, S.; Redwood, S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med. Res. Methodol. 2013, 13, 117. [Google Scholar] [CrossRef] [PubMed]
- Rivers, D.A.; Pal, T.; Vadaparampil, S.T.; Adams, L.A.; Dash-Pitts, L.; Quinn, G.P. A community-academic partnership to explore informational needs of African American women as a primer for cancer clinical trial recruitment. Ethn. Health 2017, 22, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Glaser, B.G. The constant comparative method of qualitative analysis. Soc. Probl. 1965, 12, 436–445. [Google Scholar] [CrossRef]
- Duncan, D.F. Content analysis in health education research: An introduction to purposes and methods. Health Educ. 1989, 20, 27–31. [Google Scholar] [CrossRef] [PubMed]
- Patton, M.Q. Qualitative Evaluation and Research Methods; SAGE Publications, Inc.: Thousand Oaks, CA, USA, 1990. [Google Scholar]
- Freimuth, V.S.; Quinn, S.C.; Thomas, S.B.; Cole, G.; Zook, E.; Duncan, T. African Americans’ views on research and the Tuskegee Syphilis Study. Soc. Sci. Med. 2001, 52, 797–808. [Google Scholar] [CrossRef]
- Ohmann, C.; Deimling, A. Attitude towards clinical trials: Results of a survey of persons interested in research. Inflamm. Res. 2004, 53 (Suppl. 2), S142–S147. [Google Scholar] [CrossRef] [PubMed]
| Constructs | Operationally Defined in this Study by the Corresponding Survey Question(s) |
|---|---|
| Cues to action leading to individual behavior |
|
| Perceived susceptibility |
|
| Perceived benefits |
|
| Perceived barriers |
|
| Perceived severity |
|
| Self-efficacy |
|
| Characteristics | Number | Percent |
|---|---|---|
| Age | ||
| 18–30 | 12 | 20.00 |
| 31–40 | 9 | 15.00 |
| 41–50 | 14 | 23.33 |
| 51–60 | 14 | 23.33 |
| 61+ | 11 | 18.33 |
| Sex | ||
| Male | 28 | 46.67 |
| Female | 32 | 53.33 |
| Race/ethnicity | ||
| Black or African American | 58 | 100.00 |
| Highest grade or year of school completed | ||
| Grades 9 through 11 (Some high school) | 1 | 1.72 |
| Grade 12 or GED (High school graduate) | 13 | 22.41 |
| College 1 year to 3 years (some college or technical school) | 24 | 41.38 |
| College 4 years (College graduate) | 11 | 18.97 |
| Graduate school (Advanced degree) | 9 | 15.52 |
| Language most frequently written | ||
| English | 58 | 96.67 |
| Language most frequently spoken | ||
| English | 57 | 95.00 |
| Survey Items | Pre-Test N (%) | Post-Test N (%) | Fisher Exact Test p Value | |
|---|---|---|---|---|
| Are you willing to take part in a clinical research study? | Yes | 47 (51.6) | 44 (48.4) | 0.8850 |
| No | 3 (50.0) | 3 (50.0) | ||
| Maybe | 10 (45.5) | 12 (54.5) | ||
| Are you willing to give your biological samples to a registry or biorepository? | Yes | 36 (48.0) | 39 (52.0) | 0.4771 |
| No | 3 (37.5) | 5 (62.5) | ||
| Maybe | 21 (58.3) | 15 (41.7) | ||
| Survey Items | Pre-Test | Post-Test | Wilcoxon-Mann-Whitney Test |
|---|---|---|---|
| Mean (SD) | Mean (SD) | p Value | |
| I need to agree before joining a clinical research study. | 4.53 (0.87) | 4.59 (0.75) | 0.8472 |
| I need to agree before joining a research registry or biorepository. | 4.55 (0.78) | 4.65 (0.66) | 0.5486 |
| I know how to join a registry or biorepository. | 2.69 (1.17) | 3.83 (1.04) | <0.0001 * |
| I know how to join a clinical research study. | 3.10 (1.19) | 4.00 (1.00) | <0.0001 * |
| The risks of taking part in a clinical research study are more than the benefits. | 2.84 (1.13) | 2.76 (1.03) | 0.5839 |
| Joining a clinical research study will help me get new health treatments that the public can’t get yet. | 3.35 (1.00) | 3.53 (0.83) | 0.2991 |
| Joining a clinical research study may help me get better medical care. | 3.48 (0.83) | 3.40 (0.98) | 0.8103 |
| Joining a clinical research study gives me more control over the health care I get. | 3.12 (0.97) | 3.25 (0.96) | 0.4592 |
| Joining a clinical research study allows me to help others by giving to medical research. | 4.13 (0.89) | 4.10 (0.93) | 0.8575 |
| There may be serious side effects from taking part in a clinical research study. | 3.27 (1.07) | 3.34 (1.12) | 0.6069 |
| Taking part in a clinical research study could put my life at risk. | 2.75 (1.06) | 2.91 (1.10) | 0.4446 |
| Treatment given to me for a clinical research study may not help me. | 3.21 (1.08) | 3.51 (1.08) | 0.1115 |
| Taking part in a clinical research study will take too much of my time. | 2.41 (1.02) | 2.25 (0.89) | 0.4946 |
| When I think about joining a clinical research study it scares me. | 2.16 (1.02) | 2.25 (1.08) | 0.6178 |
| I’m able to get transportation to take part in a clinical research study. | 4.03 (0.99) | 3.93 (1.10) | 0.7090 |
| My health insurance will not pay for me to take part in a clinical research study. | 3.51 (1.02) | 3.48 (0.95) | 0.8599 |
| People who oversee clinical research studies may not tell me all the risks of taking part in the study. | 2.62 (1.12) | 2.37 (1.07) | 0.2471 |
| My personal information is protected when I join a research study. | 3.81 (1.04) | 4.08 (0.87) | 0.1684 |
| I can talk to my doctor about joining a research study. | 3.92 (1.00) | 4.18 (0.85) | 0.1307 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rollins, L.; Sy, A.; Crowell, N.; Rivers, D.; Miller, A.; Cooper, P.; Teague, D.; Jackson, C.; Henry Akintobi, T.; Ofili, E. Learning and Action in Community Health: Using the Health Belief Model to Assess and Educate African American Community Residents about Participation in Clinical Research. Int. J. Environ. Res. Public Health 2018, 15, 1862. https://doi.org/10.3390/ijerph15091862
Rollins L, Sy A, Crowell N, Rivers D, Miller A, Cooper P, Teague D, Jackson C, Henry Akintobi T, Ofili E. Learning and Action in Community Health: Using the Health Belief Model to Assess and Educate African American Community Residents about Participation in Clinical Research. International Journal of Environmental Research and Public Health. 2018; 15(9):1862. https://doi.org/10.3390/ijerph15091862
Chicago/Turabian StyleRollins, Latrice, Angela Sy, Nicole Crowell, Desiree Rivers, Assia Miller, Pamela Cooper, Debra Teague, Cassandra Jackson, Tabia Henry Akintobi, and Elizabeth Ofili. 2018. "Learning and Action in Community Health: Using the Health Belief Model to Assess and Educate African American Community Residents about Participation in Clinical Research" International Journal of Environmental Research and Public Health 15, no. 9: 1862. https://doi.org/10.3390/ijerph15091862
APA StyleRollins, L., Sy, A., Crowell, N., Rivers, D., Miller, A., Cooper, P., Teague, D., Jackson, C., Henry Akintobi, T., & Ofili, E. (2018). Learning and Action in Community Health: Using the Health Belief Model to Assess and Educate African American Community Residents about Participation in Clinical Research. International Journal of Environmental Research and Public Health, 15(9), 1862. https://doi.org/10.3390/ijerph15091862








