Evaluating the Implementation of a Twitter-Based Foodborne Illness Reporting Tool in the City of St. Louis Department of Health
Abstract
:1. Introduction
2. Materials and Methods
2.1. Sample Selection
2.2. Interview Guide
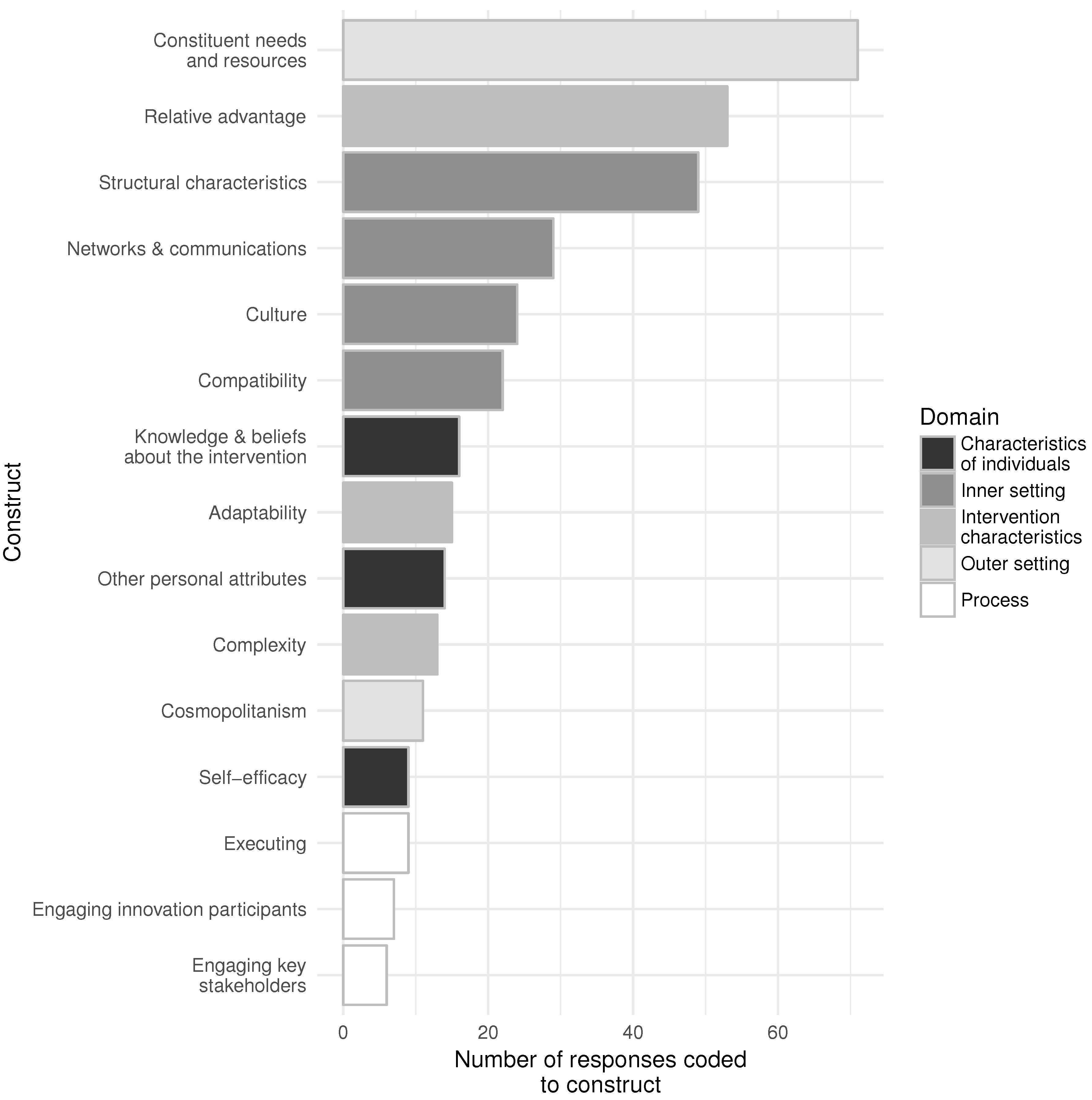
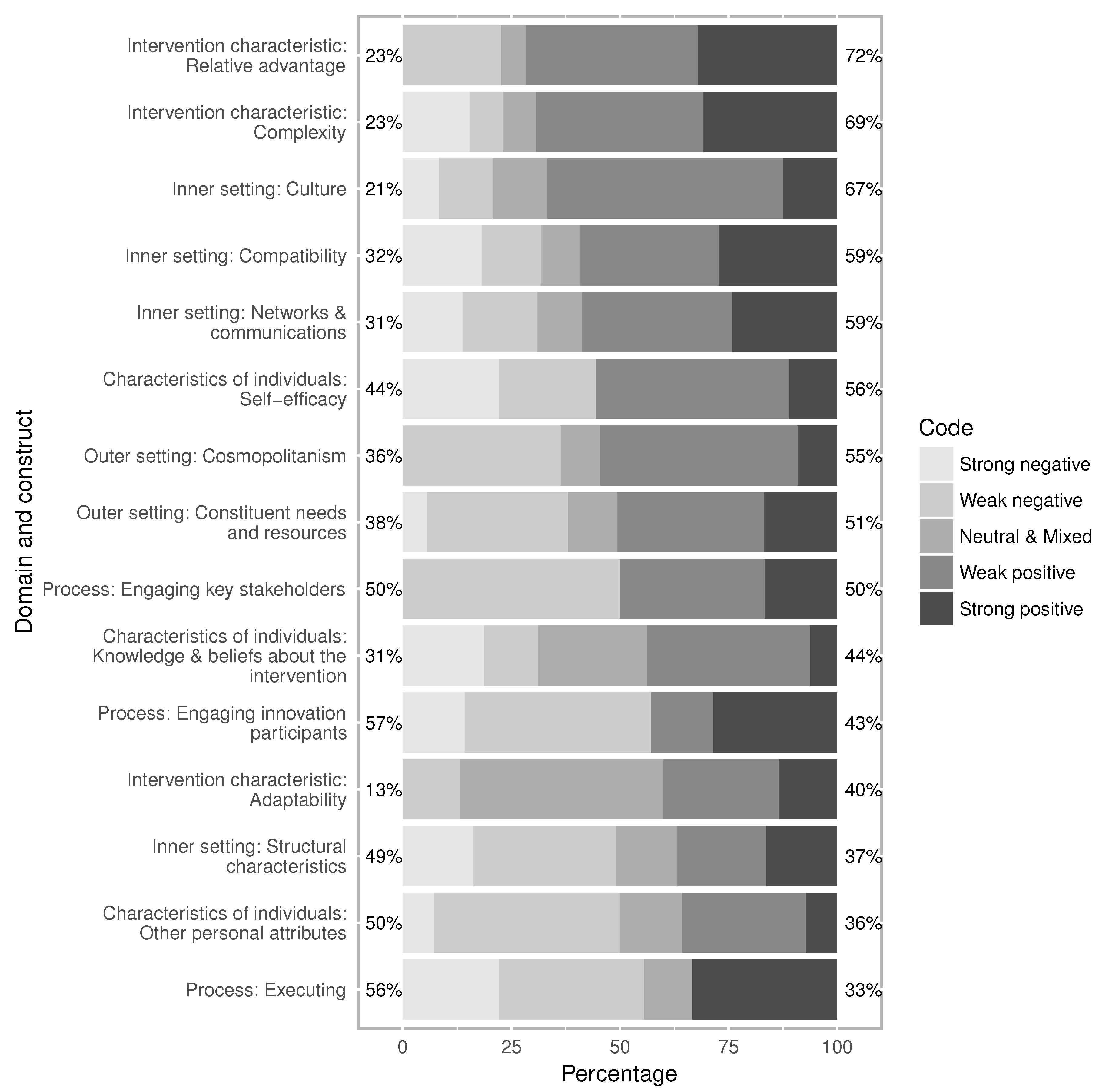
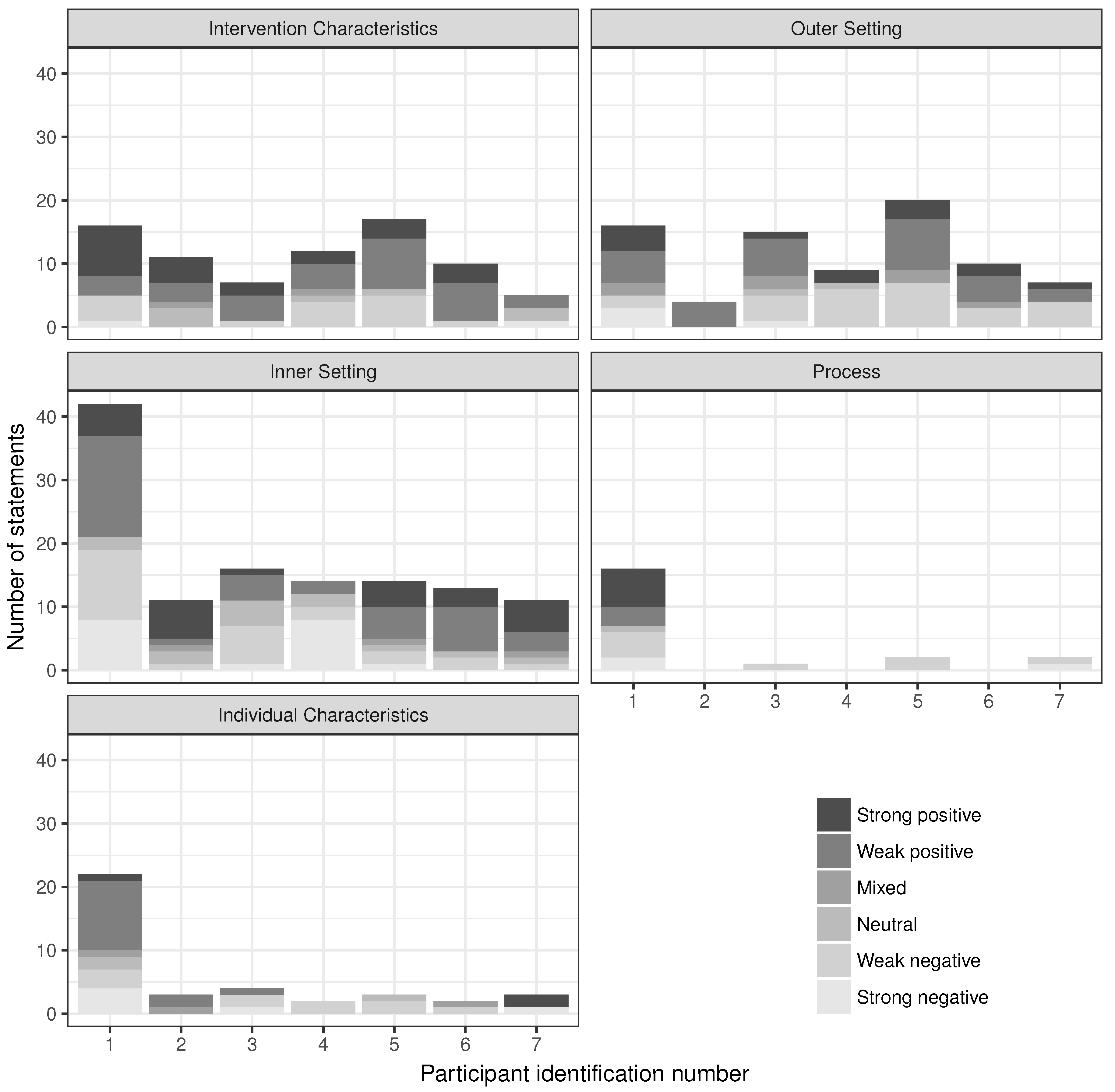
3. Results
3.1. Intervention Characteristics
Honestly, I think its goal is really big, but honestly, you guys have narrowed it down to a pretty simple procedure. This is even easier than if they call and then I have to go through the interview process. This is easier than what we normally do. So as far as intricacy goes, I think it doesn’t have too many steps. It’s really pretty streamlined. I really do. And I think for people who are afraid to pick up the phone and call but are willing to text or follow the steps online it makes it easier for them.
Probably because we’re interested in reaching the public, and this is a way to capture another segment of the population that we might not capture. That’s the medium that they use, so that’s the medium that we want to get out there in.
We were knocking on their doors to say, “Hey this blood lead level indicates that you have … your child has been exposed to lead in the last 30 to 60 days.” I think in those cases people were really quite happy to have the outreach and to learn about the services that were available in the city to address that. I think this could be very similar in that reaching out to somebody who complained of a foodborne illness that the city is proactive and that we want to address any issues that were coming up that we don’t have to just wait for you to come to us with a complaint.
I think you should involve other social media platforms or links, if there aren’t already. So I think it’s great that we’re giving people a channel to say, Hey, fill out this form. We’ll follow up with you. I think that shows a greater presence in the community that we’re reaching out to people, but I also think there is ... there’s always an opportunity for health promotion and education. So if there were a way for us to ... and I don’t know if you guys do this now … but to send out educational Tweets and so to kind of get a discussion about foodborne illness.
There is this idea that people don’t use social media. So one of the inspectors told me, “Nobody uses Twitter. Why are you doing this project? Nobody uses Twitter.”
I think the only disadvantage at this point is that perception that it could potentially be harmful to food and beverage control providers … food and beverage providers in the city. But I think we’re addressing that hurdle.
3.2. Outer Setting
I think it’s important that our residents feel like they can connect with us. I think a lot of the younger residents, they live on Twitter and social media, my generation, I guess, and so I think it allows a greater depth of communication. Yes, it’s just a Tweet, but that’s just another presence of the Health Department. In terms of people who would prefer more face-to-face contact, I think they still get that because there’s an inspector who’s going to come out and going to take a look, or we’re going to call you up, and so you still have that personal interaction, and so you feel like, hey, the Health Department cares.
I think that some of the barriers is that they receive ... say they receive a tweet from us asking them to report their illness. A hesitancy for not submitting that form or interacting is questioning the credibility of our handle. I think that’s probably one of the main things, and hesitancy with submitting their personal information.
Another disadvantage that it has compared to existing practices is that it’s also ... that we might also pick up on complaints that are defamatory or people who are tweeting about being sick but then putting another restaurant down. And I think that is a concern.
So there’s sort of a perception in the administration that this may target food and beverage providers in the city and that that may create some anxiety on their part and some tension between the public administration and the private citizens and businesses in the city.
It would also be nice if we could somehow get the actual doctors and clinics involved, because they don’t educate. They don’t ask for a stool sample. They don’t ask for a blood sample. They just go with self-defeating, “Drink some water, you’ll be better in 24 h.”
3.3. Inner Setting
The only thing that anybody had thoughts of was, oh my God, does this mean that we’re going to have a 50 percent increase in the number of complaints that we get? And people were freaking out for a very short second about that, but then when they realized that it’s not going to ... it’s not going to create that much more work, and actually we want that work because if people are sick, we need to know about it. Everybody calmed down; they just went about their business as usual.
The size of the department means that communicable disease and food and beverage control and epidemiology can work easily together because we know each other and we’re in close contact.
3.4. Characteristics of Individuals
Well I’m sure that people that just are reluctant to use any kinds of social media that are not technology savvy, and that population is just ... whether it’s age or just fear of the medium ... I don’t know what we could do to change that type of ... that part of the culture of the organization because they don’t use it personally and...
I think all of us food inspectors are fascinated by the idea. There were also some that were terrified that we would receive a whole bunch more bogus complaints, but that didn’t happen and that’s a good thing.
3.5. Process
I remember a couple months ago when the press release initially went to the mayor’s office, the first thing that they asked was like, “So now you’re asking citizens to tweet to you?” And I said, “No, no, no. We don’t want citizens to tweet to Food Safety STL.”
There is a hesitancy to initially report or submit that report form. And I think that citizens are still a little bit leery of the project, but I think as we continue to use it they are aware that the department is using alternative ways of surveillance to identify food-borne illness or outbreaks.
I think one barrier is that right now that we don’t have ... there’s yet to be a press release that has gone out, and if someone, whenever they get the questionnaire, at the same time, there could be a link that they could click on that would take them to an official press release that’s gone out or something that takes them to a city website that says, This is approved, this is legitimate, that would probably make the project more successful.
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Scallan, E.; Hoekstra, R.M.; Angulo, F.J.; Tauxe, R.V.; Widdowson, M.A.; Roy, S.L.; Jones, J.L.; Griffin, P.M. Foodborne Illness Acquired in the United States—Major Pathogens. Emerg. Infect. Dis. 2011, 17, 7–15. [Google Scholar] [CrossRef] [PubMed]
- Scharff, R.L. Economic Burden from Health Losses Due to Foodborne Illness in the United States. J. Food Prot. 2012, 75, 123–131. [Google Scholar] [CrossRef] [PubMed]
- Arendt, S.; Rajagopal, L.; Strohbehn, C.; Stokes, N.; Meyer, J.; Mandernach, S. Reporting of Foodborne Illness by US Consumers and Healthcare Professionals. Int. J. Environ. Res. Public Health 2013, 10, 3684–3714. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Smith, K.; Kaehler, D.; Everstine, K.; Rounds, J.; Hedberg, C. Evaluation of a Statewide Foodborne Illness Complaint Surveillance System in Minnesota, 2000 through 2006. J. Food Prot. 2010, 73, 2059–2064. [Google Scholar] [CrossRef] [PubMed]
- Mead, P.S.; Slutsker, L.; Dietz, V.; Mccaig, L.F.; Bresee, J.S.; Shapiro, C.; Griffin, P.M.; Tauxe, R.V. Food-Related Illness and Death in the United States. Emerg. Infect. Dis. 1999, 5, 607–625. [Google Scholar] [CrossRef] [PubMed]
- Lee, P.; Hedberg, C.W. Understanding the Relationships between Inspection Results and Risk of Foodborne Illness in Restaurants. Foodborne Pathog. Dis. 2016, 13, 582–586. [Google Scholar] [CrossRef] [PubMed]
- Irwin, K.; Ballard, J.; Grendon, J.; Kobayashi, J. Results of Routine Restaurant Inspections Can Predict Outbreaks of Foodborne Illness: The Seattle-King County Experience. Am. J. Public Health 1989, 79, 586–590. [Google Scholar] [CrossRef] [PubMed]
- Harrison, C.; Jorder, M.; Stern, H.; Stavinsky, F.; Reddy, V.; Hanson, H.; Waechter, H.; Lowe, L.; Gravano, L.; Balter, S.; et al. Using Online Reviews by Restaurant Patrons to Identify Unreported Cases of Foodborne Illness—New York City, 2012–2013. Morb. Mortal. Wkly. Rep. 2014, 63, 441–445. [Google Scholar]
- Harris, J.K.; Mansour, R.; Choucair, B.; Olson, J.; Nissen, C.; Bhatt, J. Health Department Use of Social Media to Identify Foodborne Illness—Chicago, Illinois, 2013–2014. Morb. Mortal. Wkly. Rep. 2014, 63, 681–685. [Google Scholar]
- Hawkins, J.B.; Tuli, G.; Kluberg, S.; Harris, J.; Brownstein, J.S.; Nsoesie, E. A Digital Platform for Local Foodborne Illness and Outbreak Surveillance. Online J. Public Health Inf. 2016, 8. [Google Scholar] [CrossRef]
- Song, C.; Lee, J. Citizens’ Use of Social Media IN Government, Perceived Transparency, and Trust in Government. Public Perform. Manag. Rev. 2016, 39, 430–453. [Google Scholar] [CrossRef]
- Bertot, J.C.; Jaeger, P.T.; Grimes, J.M. Using Icts to Create a Culture of Transparency: E-Government and Social Media as Openness and Anti-Corruption Tools for Societies. Gov. Inf. Q. 2010, 27, 264–271. [Google Scholar] [CrossRef]
- Stetler, C.B.; Legro, M.W.; Wallace, C.M.; Bowman, C.; Guihan, M.; Hagedorn, H.; Kimmel, B.; Sharp, N.D.; Smith, J.L. The Role of Formative Evaluation in Implementation Research and the QUERI Experience. J. Gen. Internal Med. 2006, 21, S1–S8. [Google Scholar] [CrossRef]
- Harris, J.K.; Hawkins, J.B.; Nguyen, L.; Nsoesie, E.O.; Tuli, G.; Mansour, R.; Brownstein, J.S. Using Twitter to Identify and Respond to Food Poisoning in Real Time: The Food Safety STL Project. J. Public Health Manag. Pract. 2017, 23, 577–580. [Google Scholar] [CrossRef] [PubMed]
- CFIR Guide. Available online: http://www.cfirguide.org/guide/app/index.html#/ (accessed on 3 April 2018).
- Consolidated Framework for Implementation Research. Available online: http://cfirguide.org/qual.html (accessed on 3 April 2018).
- Data and Statistical Code for the Evaluation of Food Safety STL. Available online: https://github.com/coding2share/foodsafety (accessed on 3 April 2018).
- Facebook Usage and Engagement Is on the Rise, While Adoption of Other Platforms Holds Steady. Available online: http://www.pewinternet.org/2016/11/11/social-media-update-2016/ (accessed on 3 April 2018).
- Liss-Levinson, R.; Bharthapudi, K.; Leider, J.P.; Sellers, K. Loving and Leaving Public Health: Predictors of Intentions to Quit among State Health Agency Workers. J. Public Health Manag. Pract. 2015, 21 (Suppl. 6), S91–S101. [Google Scholar] [CrossRef] [PubMed]
- Veil, S.R.; Buehner, T.; Palenchar, M.J. A Work-In-Process Literature Review: Incorporating Social Media in Risk and Crisis Communication. J. Contingencies Crisis Manag. 2011, 19, 110–122. [Google Scholar] [CrossRef]
| Domain | Constructs | Interview Questions |
|---|---|---|
| Intervention characteristics | Relative advantage | How does Food Safety STL compare to other similar existing practices related to foodborne illness reporting at the DOH? What advantages does Food Safety STL have compared to existing practices? What disadvantages does Food Safety STL have compared to existing practices? |
| Adaptability: the degree to which Food Safety STL could be adapted, tailored, refined, or reinvented to meet local needs | What kinds of changes or alterations do you think would be needed to make Food Safety STL work more effectively at the DOH? Do you think the DOH is capable of making these changes? Why or why not? | |
| Complexity: perceived difficulty of implementation of Food Safety STL | How complicated is Food Safety STL? Please consider the following aspects of Food Safety STL: duration, scope, intricacy and number of steps involved and whether Food Safety STL reflects a clear departure from previous practices. | |
| Outer setting | Patient needs & resources | How well do you think Food Safety STL meets the needs of the individuals served by the DOH? In what ways did Food Safety STL meet their needs? E.g., convenient way of reporting? How do you think the citizens who used Food Safety STL responded to the service? What do you think are the barriers for the citizens participating or interacting with Food Safety STL? |
| Inner setting | Structural | How does the infrastructure of your organization (work hierarchy, age, maturity, size, or physical layout) affect the implementation of Food Safety STL? How does the infrastructure facilitate/hinder the implementation of Food Safety STL? How do you work around these structural challenges? What kinds of infrastructure changes are needed to further accommodate Food Safety STL? Changes in scope of practice? Changes in formal policies? Changes in information systems or electronic records systems? Other? What kind of approvals are needed? Who needs to be involved? Can you describe the process needed to make these changes? |
| Culture: Norms, values, and basic assumptions of a given organization | How do you think your organization’s culture (general beliefs, values, assumptions that people have) affect the implementation of Food Safety STL? Can you describe an example that highlights this? | |
| Implementation climate | What is the general level of receptivity at the DOH to implementing Food Safety STL? Why? |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Harris, J.K.; Hinyard, L.; Beatty, K.; Hawkins, J.B.; Nsoesie, E.O.; Mansour, R.; Brownstein, J.S. Evaluating the Implementation of a Twitter-Based Foodborne Illness Reporting Tool in the City of St. Louis Department of Health. Int. J. Environ. Res. Public Health 2018, 15, 833. https://doi.org/10.3390/ijerph15050833
Harris JK, Hinyard L, Beatty K, Hawkins JB, Nsoesie EO, Mansour R, Brownstein JS. Evaluating the Implementation of a Twitter-Based Foodborne Illness Reporting Tool in the City of St. Louis Department of Health. International Journal of Environmental Research and Public Health. 2018; 15(5):833. https://doi.org/10.3390/ijerph15050833
Chicago/Turabian StyleHarris, Jenine K., Leslie Hinyard, Kate Beatty, Jared B. Hawkins, Elaine O. Nsoesie, Raed Mansour, and John S. Brownstein. 2018. "Evaluating the Implementation of a Twitter-Based Foodborne Illness Reporting Tool in the City of St. Louis Department of Health" International Journal of Environmental Research and Public Health 15, no. 5: 833. https://doi.org/10.3390/ijerph15050833
APA StyleHarris, J. K., Hinyard, L., Beatty, K., Hawkins, J. B., Nsoesie, E. O., Mansour, R., & Brownstein, J. S. (2018). Evaluating the Implementation of a Twitter-Based Foodborne Illness Reporting Tool in the City of St. Louis Department of Health. International Journal of Environmental Research and Public Health, 15(5), 833. https://doi.org/10.3390/ijerph15050833





