Mental Health Interventions for Parent Carers of Children with Autistic Spectrum Disorder: Practice Guidelines from a Critical Interpretive Synthesis (CIS) Systematic Review
Abstract
:1. Introduction
Objectives of Study
2. Method
2.1. Critical Interpretative Synthesis
2.2. Search Criteria and Literature Search
2.3. Search Procedure
2.4. Quality Appraisal
3. Results
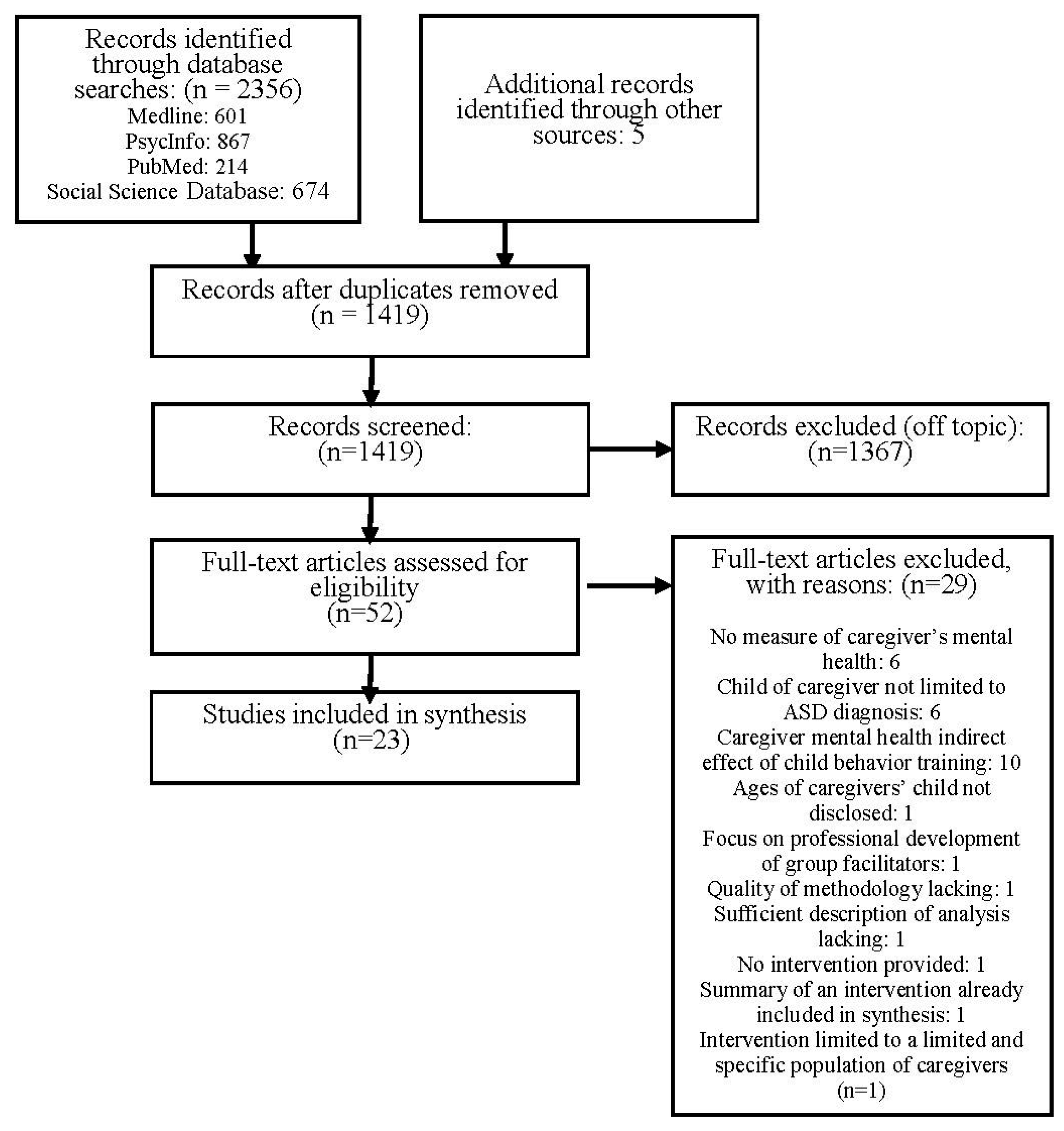
3.1. Search Results
3.2. Study Characteristics
3.3. Data Extraction
3.4. Synthesis
3.4.1. Social Support
Informal Networks
Reduced Isolation
Validation by Peers
3.4.2. Professional Training in Skill Development
Stress Management Strategies
Problem-Solving Skills
3.4.3. Gaining Knowledge Regarding ASD
Understanding Autism Spectrum Disorder
Resources and Services
4. Discussion
4.1. Strengths and Limitations of the Review
4.2. Implications of the Review and Practice Guidelines
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Brobst, J.B.; Clopton, J.R.; Hendrick, S.S. Parenting children with autism spectrum disorders: The couple’s relationship. Focus Autism Other Dev. Disabil. 2009, 24, 38–49. [Google Scholar] [CrossRef]
- Hoffman, C.D.; Sweeney, D.P.; Hodge, D.; Lopez-Wagner, M.D.; Looney, L. Parenting stress and closeness: Mothers of typically developing children and mothers of children with autism. Focus Autism Other Dev. Disabil. 2009, 24, 178–187. [Google Scholar] [CrossRef]
- Lee, G.K.; Lopata, C.; Volker, M.A.; Thomeer, M.L.; Nida, R.E.; Toomey, J.A.; Chow, S.Y.; Smerbeck, A.M. Health-Related quality of life of parents of children with high-functioning autism spectrum disorders. Focus Autism Other Dev. Disabil. 2009, 24, 227–239. [Google Scholar] [CrossRef]
- Abbeduto, L.; Seltzer, M.M.; Shattuck, P.; Krauss, M.W.; Orsmond, G.; Murphy, M.M. Psychological well-being and coping in mothers of youths with autism, Down syndrome, or fragile X syndrome. Am. J. Ment. Retard. 2004, 109, 237–254. [Google Scholar] [CrossRef]
- Pisula, E. A comparative study of stress profiles in mothers of children with autism and those of children with Down’s syndrome. J. Appl. Res. Intellect. Disabil. 2007, 20, 274–278. [Google Scholar] [CrossRef]
- Cochrane, J.J.; Goering, P.N.; Rogers, J.M. The mental health of information caregivers in Ontario: An epidemiological survey. Am. J. Public Health 1997, 87, 2002–2007. [Google Scholar] [CrossRef] [PubMed]
- Pinquart, M.; Sörensen, S. Differences between caregivers and noncaregivers in psychological health and physical health: A meta-analysis. Psychol. Aging 2003, 18, 250–267. [Google Scholar] [CrossRef] [PubMed]
- Davis, N.O.; Carter, A.S. Parenting stress in mothers and fathers of toddlers with autism spectrum disorders: Association with child characteristics. J. Autism Dev. Disord. 2008, 38, 1278–1291. [Google Scholar] [CrossRef] [PubMed]
- Hayes, S.A.; Watson, S.L. The impact of parenting stress: A meta-analysis of studies comparing the experience of parenting stress in parents of children with and without autism spectrum disorder. J. Autism Dev. Disord. 2013, 43, 629–642. [Google Scholar] [CrossRef] [PubMed]
- Lovell, B.; Moss, M.; Wetherell, M. The psychosocial, endocrine and immune consequences of caring for a child with autism or DAH. Psychoneuroendocrinology 2012, 17, 534–542. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Robledillo, N.; Moya-Albiol, L. Self-Reported health and cortisol awakening response in parents of people with Asperger syndrome: The role of trait anger and anxiety, coping and burden. Psychol. Health 2013, 28, 1246–1264. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Neurodevelopmental disorders: Autism spectrum disorder. In Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychological Association: Arlington, VA, USA, 2013. [Google Scholar]
- World Health Organization. Available online: http://www.who.int/mediacentre/factsheets/autism-spectrum-disorders/en/ (accessed on 19 January 2018).
- Statistia. Available online: https://www.statista.com/statistics/676354/autism-rate-among-children-select-countries-worldwide/ (accessed on 19 January 2018).
- Centers for Disease Control and Prevention. Available online: https://www.cdc.gov/ncbddd/autism/addm.html (accessed on 19 January 2018).
- Gray, D.E. Gender and coping: The parents of children with high functioning autism. Soc. Sci. Med. 2003, 56, 631–642. [Google Scholar] [CrossRef]
- Exhaustion, Anger of Caregiving Get a Name. Available online: http://www.cnn.com/2007/HEALTH/conditions/08/13/caregiver.syndrome/index.html (accessed on 20 September 2017).
- Killian, D. Helping ill it hurts? A multimethod study of compassion fatigue, burnout, and self-care in clinicians working with trauma survivors. Traumatology 2008, 14, 32–44. [Google Scholar] [CrossRef]
- Lawton, M.P.; Moss, M.; Kleban, M.H.; Glicksman, A.; Rovine, M. A two-factor model of caregiving appraisal and psychological well-being. J. Gerontol. 1991, 46, 181–189. [Google Scholar] [CrossRef]
- Quintero, N.; McIntyre, L.L. Sibling adjustment and maternal well-being: An examination of families with and without a child with an autism spectrum disorder. Focus Autism Other Dev. Disabil. 2010, 25, 37–46. [Google Scholar] [CrossRef] [PubMed]
- Baker, J.K.; Seltzer, M.M.; Greenberg, J.S. Longitudinal effects of adaptability on behavior problems and maternal depression I families of adolescents with autism. J. Fam. Psychol. 2011, 25, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Bitsika, V.; Sharpley, C. An exploratory examination of the effects of support groups on the well-being of parents of children with autism-I: General counselling. J. Appl. Health Behav. Sci. 1999, 1, 16–22. [Google Scholar]
- Eisenhower, A.S.; Baker, B.L.; Blacher, J. Preschool children with intellectual disability: Syndrome specificity, behavior problems, and maternal well-being. J. Intellect. Disabil. Res. 2005, 49, 657–671. [Google Scholar] [CrossRef] [PubMed]
- Estes, A.; Munson, J.; Dawson, G.; Koehler, E.; Zhou, X.; Abbott, R. Parenting stress and psychological functioning among mothers of preschool children with autism and developmental delay. Autism 2009, 13, 375–387. [Google Scholar] [CrossRef] [PubMed]
- Hamlyn-Wright, S.; Draghi-Lorenz, R.; Ellis, J. Locus of control fails to mediate between stress and anxiety and depression in parents of children with a developmental disorder. Autism 2007, 11, 489–501. [Google Scholar] [CrossRef] [PubMed]
- Mugno, D.; Ruta, L.; D-Arrigo, V.G.; Mazzone, L. Impairment of quality of life in parents of children and adolescents with pervasive developmental disorder. Health Qual. Life Outcomes 2007, 5. [Google Scholar] [CrossRef] [PubMed]
- Weiss, M.J. Hardiness and social support as predictors of stress in mothers of typical children, children with autism, and children with mental retardation. Autism 2002, 6, 115–130. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.E.; Hong, J.; Seltzer, M.M.; Greenberg, J.S.; Almeida, D.M.; Bishop, S.L. Daily experiences among mothers of adolescents and adults with autism spectrum disorder. J. Autism Dev. Disord. 2010, 40, 167–178. [Google Scholar] [CrossRef] [PubMed]
- Khanna, R.; Madhavan, S.S.; Smith, M.J.; Patrick, J.H.; Tworek, C.; Becker-Cottrill, B. Assessment of health-related quality of life among primary caregivers of children with autism spectrum disorders. J. Autism Dev. Disord. 2011, 41, 1214–1227. [Google Scholar] [CrossRef] [PubMed]
- Allik, H.; Larsson, J.-O.; Smedje, H. Health-Related quality of life in parents of school-age children with Asperger syndrome or high-functioning autism. Health Qual. Life Outcomes 2006, 4. [Google Scholar] [CrossRef] [PubMed]
- Fong, L.; Wilgosh, L.S.; Sobsey, D. The experience of parenting an adolescent with autism. Int. J. Disabil. Dev. Educ. 1993, 40, 105–113. [Google Scholar] [CrossRef]
- Kuhaneck, H.M.; Madonna, S.; Novak, A.; Pearson, E. Effectiveness of interventions for children with Autism Spectrum Disorder and their parents: A systematic review of family outcomes. Am. J. Occup. Ther. 2015, 69, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Meltzer, L.J. Factors associated with depressive symptoms in parents of children with Autism Spectrum Disorders. Res. Autism Spectr. Disord. 2011, 5, 361–367. [Google Scholar] [CrossRef]
- Serrata, C.A. Psychosocial aspects of parenting a child with autism. J. Appl. Rehabil. Couns. 2012, 43, 29–35. [Google Scholar]
- Campbell, J.M. Efficacy of behavioral intervention for reducing problematic behaviors in persons with autism: A quantitative synthesis of single-subject research. Res. Dev. Disabil. 2003, 24, 120–138. [Google Scholar] [CrossRef]
- Leyfer, O.T.; Folstein, S.E.; Bacalman, S.; Davis, N.O.; Dinh, E.; Morgan, J.; Tager-Flusberg, H.; Lainhart, J.E. Comorbid psychiatric disorders in children with autism: Interview development and rates of disorders. J. Autism Dev. Disord. 2006, 36, 849–861. [Google Scholar] [CrossRef] [PubMed]
- Baker, J.K.; Seltzer, M.M.; Greenberg, J.S. Behavior problems, maternal internalizing symptoms and family relations in families of adolescents and adults with fragile X syndrome. J. Intellect. Disabil. Res. 2012, 56, 984–995. [Google Scholar] [CrossRef] [PubMed]
- Jellett, R.; Wood, C.E.; Giallo, R.; Seymour, M. Family functioning and behavior problems in children with Autism Spectrum Disorders: The mediating role of parent mental health. Clin. Psychol. 2015, 19, 39–48. [Google Scholar] [CrossRef]
- Ooi, K.L.; Ong, Y.S.; Jacob, S.A.; Khan, T.M. A meta-synthesis on parenting a child with autism. Neuropsychiatr. Dis. Treat. 2016, 12, 745–762. [Google Scholar] [PubMed]
- Osborne, L.A.; McHugh, L.; Saunders, J.; Reed, P. Parenting stress reduces the effectiveness of early teaching interventions for autistic spectrum disorders. J. Autism Dev. Disord. 2008, 38, 1092–1103. [Google Scholar] [CrossRef] [PubMed]
- McInnes, E.; Wimpenny, P. Using qualitative assessment and review instrument software to synthesise studies on older people’s views and experiences of fall prevention. Int. J. Evid. Based Healthc. 2008, 6, 337–344. [Google Scholar] [CrossRef] [PubMed]
- Dixon-Woods, M.; Bonas, S.; Booth, A.; Jones, D.R.; Miller, T.; Sutton, A.J.; Shaw, R.L.; Smith, J.A.; Young, B. How can systematic reviews incorporate qualitative research? A critical perspective. Qual. Res. 2006, 6, 27–44. [Google Scholar] [CrossRef]
- World Health Organization. Mental Health: A State of Well-Being. Available online: http://www.who.int/features/factfiles/mental_health/en/ (accessed on 20 September 2017).
- Flemming, K. Synthesis of quantitative and qualitative research: An example using Critical Interpretive Synthesis. J. Adv. Nurs. 2009, 66, 201–217. [Google Scholar] [CrossRef] [PubMed]
- Hawker, S.; Payne, S.; Kerr, C.; Hardy, M.; Powell, J. Appraising the evidence reviewing disparate data systematically. Qual. Health Res. 2002, 12, 1284–1299. [Google Scholar] [CrossRef] [PubMed]
- Bitsika, V.; Sharpley, C. Development and testing of the effects of support groups on the well-being of parents of children with autism-II: Specific stress management techniques. J. Appl. Health Behav. 2000, 2, 8–15. [Google Scholar]
- Zung, W. A rating instrument for anxiety disorders. Psychosomatics 1973, XII, 371–379. [Google Scholar] [CrossRef]
- Zung, W. A self-rating depression scale. Arch. Gen. Psychiatry 1965, 12, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Blackledge, J.T.; Hayes, S.C. Using acceptance and commitment training in the support of parents of children diagnosed with autism. Child Fam. Behav. Ther. 2006, 28, 1–18. [Google Scholar] [CrossRef]
- Hayes, S.C.; Strosahl, K.D.; Wilson, K.G.; Bissett, R.T.; Pistorello, J.; Toarmino, D.; Polusny, M.A.; Dykstra, T.A.; Batten, S.V.; Bergan, J.; et al. Measuring experimental avoidance: A preliminary test of a working model. Psychol. Rec. 2004, 54, 553–578. [Google Scholar] [CrossRef]
- Hollon, S.D.; Kendall, P.C. Cognitive self-statements in depression: Development of an Automatic Thoughts Questionnaire. Cogn. Ther. Res. 1980, 4, 383–395. [Google Scholar] [CrossRef]
- Beck, A.T.; Steer, R.A.; Brown, G.K. Manual for the Beck Depression Inventory-II; Psychological Corporation: San Antonio, TX, USA, 1996. [Google Scholar]
- Goldbert, D.P. Manual of the General Health Questionnaire; National Foundation for Educational Research: Windsor, UK, 1978. [Google Scholar]
- Campis, L.K.; Lyman, R.D.; Prentice-Dunn, S. The Parental Locus of Control Scale: Development and validation. J. Clin. Child Psychiatry 1986, 15, 260–267. [Google Scholar] [CrossRef]
- Derogatis, L.R.; Melisaratos, N. The Brief Symptom Inventory: An introductory report. Psychol. Med. 1983, 13, 596–605. [Google Scholar] [CrossRef]
- Clifford, T.; Minnes, P. Logging on: Evaluating an online support group for parents of children with autism spectrum disorders. J. Autism Dev. Disord. 2013, 43, 1662–1675. [Google Scholar] [CrossRef] [PubMed]
- Spielberger, C.D. Manual for the State-Trait Anxiety Inventory; Consulting Psychologists Press: Palo Alto, CA, USA, 1983. [Google Scholar]
- Spielberger, C.D.; Ritterband, L.M.; Reheiser, E.S.; Brunner, T.M. The nature and measurement of depression. Int. J. Clin. Health Psychol. 2003, 3, 209–234. [Google Scholar]
- Behr, S.K.; Murphy, D.L.; Summers, J.A. User’s Manual: Kansas Inventory of Parental Perceptions (KIPP); Beach Center on Families and Disability, University of Kansas: Lawrence, KS, USA, 1992. [Google Scholar]
- Nachshen, J.; Woodford, L.; Minnes, P. The family stress and coping interview for families of individuals with developmental disabilities: A lifespan perspective on family adjustment. J. Intellect. Disabil. Res. 2003, 47, 285–290. [Google Scholar] [CrossRef] [PubMed]
- Ergüner-Tekinalp, B.; Akkök, F. The effects of a coping skills training program on the coping skills, hopelessness, and stress levels of mothers of children with autism. Int. J. Adv. Couns. 2004, 26, 257–269. [Google Scholar] [CrossRef]
- Amirkhan, J.H. A factor analytically derived measure of coping: The coping strategy indicator. J. Personal. Soc. Psychol. 1990, 59, 1066–1074. [Google Scholar] [CrossRef]
- Beck, A.T.; Lester, L.; Tresler, L. The Hopelessness Scale. J. Consult. Clin. Psychol. 1974, 42, 861–874. [Google Scholar] [CrossRef] [PubMed]
- Holroyd, J. The questionnaire on resources and stress: An instrument to measure family response to a handicapped family member. J. Community Psychol. 1987, 2, 92–94. [Google Scholar] [CrossRef]
- Farmer, J.; Reupert, A. Understanding autism and understanding my child with autism: An evaluation of a group parent education program in rural Australia. Aust. J. Rural Health 2013, 21, 20–27. [Google Scholar] [CrossRef] [PubMed]
- Feinberg, E.; Augustyn, M.; Fitzgerald, E.; Sandler, J.; Suarez, Z.F.; Chen, N.; Cabral, H.; Beardslee, W.; Silverstein, M. Improving maternal mental health after a child’s diagnosis of autism spectrum disorder: Results from a randomized clinical trial. JAMA Pediatr. 2014, 168, 40–46. [Google Scholar] [CrossRef] [PubMed]
- Carver, C.S. You want to measure coping but your protocol’s too long. Int. J. Behav. Med. 1997, 4, 92–100. [Google Scholar] [CrossRef] [PubMed]
- Rush, A.J.; Trivedi, M.H.; Ibrahim, H.M.; Carmody, T.J.; Arnow, B.; Klein, D.N.; Markowitz, J.C.; Ninan, P.T.; Kornstein, S.; Manber, R.; et al. The 16-item Quick Inventory of Depressive Symptomology (QIDS), clinical rating (QIDS-C), and self-report (QIDS-SR): A psychometric evaluation in patients with chronic major depression. Biol. Psychiatry 2003, 54, 573–583. [Google Scholar] [CrossRef]
- Abidin, R.R. Parenting Stress Index Professional Manual, 4th ed.; Psychological Assessment Resources: Lutz, FL, USA, 2012. [Google Scholar]
- Ferraioli, S.; Harris, S.L. Comparative effects of mindfulness and skills-based parent training programs for parents of children with autism: Feasibility and preliminary outcome data. Mindfulness 2012, 4, 89–101. [Google Scholar] [CrossRef]
- Brown, K.W.; Ryan, R.M. The benefits of being present: Mindfulness and its role in psychological well-being. J. Personal. Soc. Psychol. 2003, 84, 822–848. [Google Scholar] [CrossRef]
- Giarelli, E.; Bloch, J.; Souders, M.; Levy, S.E.; Pinto-Martin, J. Intervention pilot for parents of children with autism spectrum disorder. Pediatr. Nurs. 2005, 31, 389–399. [Google Scholar] [PubMed]
- Cohen, S.; Williamson, G.M. Perceived stress in probability sample of the United States. In The Social Psychology of Health; Spacapan, S., Oscamp, E., Eds.; Sage: Newbury Park, CA, USA, 1988; pp. 307–326. [Google Scholar]
- Zilberg, N.; Weiss, D.; Horowitz, M. Impact of events scale: A cross validation study and some empirical evidence supporting a conceptual model of stress response syndromes. J. Consult. Clin. Psychol. 1982, 50, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Gika, D.M.; Artemiadis, A.K.; Alexopoulos, E.C.; Darviri, C.; Papanikolaou, K.; Chrousos, G.P. Use of a relaxation technique by mothers of children with autism: A case-series study. Psychol. Rep. 2012, 111, 797–804. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Izadi-Mazidi, M.; Riahi, F.; Khajeddin, H. Effect of cognitive behavior group therapy on parenting stress in mothers of children with autism. Iran J. Psychiatry Behav. Sci. 2015, 9. [Google Scholar] [CrossRef] [PubMed]
- Jamison, J.M.; Fourie, E.; Siper, P.M.; Trelles, M.P.; George-Jones, J.; Grice, A.B.; Krata, J.; Holl, E.; Shaoul, J.; Hernandez, B.; et al. Examining the efficacy of a family peer advocate model for Black and Hispanic caregivers of children with autism spectrum disorder. J. Autism Dev. Disord. 2017, 47, 1314–1322. [Google Scholar] [CrossRef] [PubMed]
- Brannan, A.M.; Heflinger, C.A.; Brickman, L. The caregiver strain questionnaire: Measuring the impact on the family of living with a child with serious emotional disturbance. J. Emot. Behav. Disord. 1997, 5, 212–222. [Google Scholar] [CrossRef]
- Koren, P.D.; DeChillo, N.; Friesen, B.J. Measuring empowerment in families whose children have emotional disabilities: A brief questionnaire. Rehabil. Psychol. 1992, 37, 305–321. [Google Scholar] [CrossRef]
- Sherbourne, C.D.; Stewart, A.L. The MOS social support survey. Soc. Sci. Med. 1991, 32, 704–714. [Google Scholar] [CrossRef]
- Ji, B.; Sun, M.; Yi, R.; Tang, S. Multidisciplinary parent education for caregivers of children with autism spectrum disorders. Arch. Psychiatr. Nurs. 2014, 28, 319–326. [Google Scholar] [CrossRef] [PubMed]
- Novak, M.; Guest, C. Application of a multidimensional caregiver burden inventory. Gerontologist 1989, 29, 798–803. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.D.; Wang, X.L.; Ma, H. Rating Scales for Mental Health; Chinese Mental Health Journal Press: Beijing, China, 2009; pp. 187–190. [Google Scholar]
- Epstein, N.B.; Baldwin, L.; Bishop, D.S. The McMaster family assessment device. J. Marital. Fam. Ther. 1983, 9, 171–180. [Google Scholar] [CrossRef]
- General Health: 36-Item Short Form Health Survey (SF-36). Rand: Santa Monica, CA, USA. Available online: https://www.rand.org/health/surveys_tools/mos/36-item-short-form/survey-instrument.html (accessed on 13 February 2018).
- Schwarzer, R.; Jerusalem, M. Generalized Self-Efficacy scale. In Measures in Health Psychology: A User’s Portfolio. Casual and Control Beliefs; Weinman, J., Wright, S., Johnston, M., Eds.; NFER-Nelson: Windsor, UK, 1994; pp. 35–37. [Google Scholar]
- Zimet, G.D.; Powell, S.S.; Farley, G.K.; Werkman, S.; Berkoff, K.A. Psychometric characteristics of the Multidimensional Scale of Perceived Social Support. J. Personal. Assess. 1990, 55, 610–617. [Google Scholar] [CrossRef] [PubMed]
- Joekar, S.; Farid, A.A.; Birashk, B.; Gharraee, B.; Mohammadian, M. Effectiveness of acceptance and commitment therapy in the support of parents of children with high-functioning autism. Int. J. Humanit. Cult. Stud. 2016, 2, 2763–2772. [Google Scholar]
- Bond, F.W.; Hayes, S.C.; Baer, R.A.; Carpenter, K.M.; Orcutt, H.K.; Waltz, T.; Zettle, R.D. Preliminary psychometric properties of the Acceptance and Action Questionnaire–II: A revised measure of psychological inflexibility and experiential avoidance. Behav. Ther. 2011, 42, 676–688. [Google Scholar] [CrossRef] [PubMed]
- Ware, J.E., Jr.; Kosinski, M.; Keller, S.D. A 12-item short form health survey: Construction of scales and preliminary tests of reliability and validity. Med. Care 1996, 34, 220–233. [Google Scholar] [CrossRef] [PubMed]
- Kim, J. Effects of Buddhist Ontology Focused (BOF) meditation: Pilot studies with mothers of children with developmental disabilities on their EEG and psychological well-beings. Asia Pac. J. Couns. Psychother. 2016, 7, 82–100. [Google Scholar] [CrossRef]
- Watson, D.; Clark, L.A.; Tellegen, A. Development and validation of brief measures of positive and negative affect: The PANAS scales. J. Personal. Soc. Psychol. 1988, 54, 1063–1070. [Google Scholar] [CrossRef]
- Lovibond, S.H.; Lovibond, P.F. Manual for the Depression Anxiety Stress Scales, 2nd ed.; Psychological Foundation: Sydney, Australia, 1995; ISBN 7334-1423-0. [Google Scholar]
- Cartwright-Hatton, S.; Wells, A. Belifs about worry and intrusions: The meta-cognitions questionnaire and its correlates. J. Anxiety Disord. 1997, 11, 279–296. [Google Scholar] [CrossRef]
- Lovell, B.; Moss, M.; Wetherell, M.A. Assessing the feasibility and efficacy of written benefit-finding for caregivers of children with autism: A pilot study. J. Fam. Stud. 2016, 22, 32–42. [Google Scholar] [CrossRef]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, C.T.; Fairclough, D.L.; Noll, R.B. Problem-Solving skills training for mothers of children recently diagnosed with autism spectrum disorder: A pilot feasibility study. Autism 2016, 20, 55–64. [Google Scholar] [CrossRef] [PubMed]
- McNair, D.M.; Lorr, M.; Droppleman, L.F. Revised Manual for the Profile of Moods States; Educational and Industrial Testing Services: San Diego, CA, USA, 1992. [Google Scholar]
- Creamer, M.; Bell, R.; Failla, S. Psychometric properties of the impact of event scale—Revised. Behav. Res. Ther. 2003, 41, 1489–1496. [Google Scholar] [CrossRef] [PubMed]
- Niinomi, K.; Asano, J.; Kadoma, A.; Yoshida, K.; Ohashi, Y.; Furuzawa, A.; Yamamoto, M.; Yamakita, N.; Mori, A. Developing the “Skippu-Mama” program for mothers of children with autism spectrum disorder. Nurs. Health Sci. 2016, 18, 283–291. [Google Scholar] [CrossRef] [PubMed]
- The WHOQOL Group. The World Health Organization Quality of Life assessment (WHOQOL): Position paper from the World Health Organization. Soc. Sci. Med. 1995, 41, 1403–1409. [Google Scholar]
- Patra, S.; Arun, P.; Chavan, B.S. Impact of psychoeducation intervention module on parents of children with autism spectrum disorders: A preliminary study. J. Neurosci. Rural Pract. 2015, 6, 529–535. [Google Scholar] [CrossRef] [PubMed]
- Girimaji, S.C.; Srinath, S.; Seshadri, D.K.; Krishna, D.K. Family interview for stress and coping in mental retardation (FISC-MR): A tool to study stress and coping in families of children with mental retardation. Indian J. Psychiatry 1999, 41, 341–349. [Google Scholar] [PubMed]
- Rayan, A.; Ahmad, M. Effectiveness of mindfulness-based interventions on quality of life and positive reappraisal coping among parents of children with autism spectrum disorder. Res. Dev. Disabil. 2016, 55, 185–196. [Google Scholar] [CrossRef] [PubMed]
- Gamefski, N.; Kraaij, V.; Spinhoven, P. Manual for the Use of the Cognitive Emotion Regulation Questionnaire; DATEC: Leiderdorp, The Netherlands, 2002. [Google Scholar]
- WHOQOL Group. Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol. Med. 1998, 28, 551–558. [Google Scholar]
- Ruiz-Robledillo, N.; Sariñana-González, P.; Pérez-Blasco, J.; González-Bono, E.; Moya-Albiol, L. A mindfulness-based program improves health in caregivers of people with autism spectrum disorder: A pilot study. Mindfulness 2015, 6, 767–777. [Google Scholar] [CrossRef]
- Miguel-Tobal, J.J.; Casado, M.I.; Cano-Vindel, A.; Spielberger, C.D. Inventario de Expression de Ira Estado-Raso: STAXI-2; TEA Ediciones: Madrid, Spain, 2001. [Google Scholar]
- Zarit, S.H.; Reever, K.E.; Bach-Peterson, J. Relatives of the impaired elderly: Correlates of feelings of burden. Gerontologist 1980, 20, 649–654. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Steer, R.A. Beck Depression Inventory Manual; The Psychological Corporation: San Antonio, TX, USA, 1993. [Google Scholar]
- Sandin, B.; Chorot, P. Escala de Síntomas Somáticos-Revisada (ESS-R); Universidad Nacional de Educación a Distancia (UNED): Madrid, Spain, 1995. [Google Scholar]
- Samadi, S.A.; McConkey, R.; Kelly, G. Enhancing parental well-being and coping through a family-centered short course for Iranian parents of children with an autism spectrum disorder. Autism 2012, 17, 27–43. [Google Scholar] [CrossRef] [PubMed]
- Roger, D.; Jervis, G.; Najarian, B. Detachment and coping: The construction and validation of a new scale for measuring coping strategies. Personal. Individ. Differ. 1993, 15, 619–626. [Google Scholar] [CrossRef]
- McConkey, R.; Samadi, S.A. The impact of mutual support on Iranian parents of children with an autism spectrum disorder: A longitudinal study. Disabil. Rehabil. 2013, 35, 775–784. [Google Scholar] [CrossRef] [PubMed]
- Tonge, B.; Brereton, A.; Kiomall, M.; Mackinnon, A.; King, N.; Rinehart, N. Effects on parental mental health of an education and skills training program for parents of young children with autism: A randomized controlled trial. J. Am. Acad. Child Adolesc. Psychiatry 2006, 45, 561–569. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Yan, T.; Du, Y.; Liu, X. Brief report: Effects of solution-focused brief therapy group-work on promoting post-traumatic growth of mothers who have a child with ASD. J. Autism Dev. Disord. 2014, 44, 2052–2056. [Google Scholar] [CrossRef] [PubMed]
- Tedeschi, R.G.; Calhoun, L.G. The posttaumatic growth inventory: Measuring the positive legacy of trauma. J. Trauma. Stress 1996, 9, 455–471. [Google Scholar] [CrossRef] [PubMed]
| Reference, Year, Country | Aim | Design/Data Collection/Analysis Psychological Construct Measured: Instrument | Participants | Findings |
|---|---|---|---|---|
| Bitsika and Sharpley [46], 2000, Australia | To explore effect of parent support program providing specific stress management strategies | Mixed design, within-subject/questionnaires, written feedback/MANOVA content analysis Anxiety: Self-Rating Anxiety Scale (SAS; Zung [47]) Depression: Self-rating Depression Scale (SDS; Zung [48]) | n = 11 mothers | No significant change in stress, anxiety, or depression but measure of group cohesion increased; parent’s written feedback supported benefits gained from learning specific stress management technique (biofeedback) |
| Blackledge and Hayes [49], 2006, United States | To determine effectiveness of Acceptance and Commitment Therapy (ACT) on parent carers’ coping and mental health | Within-subject, repeated measures/questionnaires/Non-parametric Wilcoxon signed-ranked test Acceptance: Acceptance and Action Questionnaire (AAQ; Hayes, Strosahl, et al. [50]) Cognitions and automatic thoughts: Automatic Thoughts Questionnaire (ATQ; Hollon and Kendall [51]) Depression: Beck Depression Inventory II (BDI-II; Beck, Steer, and Brown [52]) General health: General Health Questionnaire-12 item (GHQ-12; Goldberg [53]) Locus of control: Parental Locus of Control Scale (PLOS; Campis, Lyman, Prentice-Dunn [54]) Psychological distress: Global Severity Index (GSI) from the Brief Symptom Inventory (BSI; Derogatis and Melisaratos [55]) | n = 20 (15 mothers; 5 fathers) | Improved psychological outcomes retained at three month follow-up, general distress and depression decreased significantly, was most pronounced among participants in clinical range of depression |
| Clifford and Minnes [56], 2013, Canada | To investigate changes in parent well-being following involvement in on-line support group | uasi-experimental between-group/questionnaires/MANOVA Anxiety: State-Trait Anxiety Inventory (STAI; Spielberger [57]) Depression: State-Trait Depression Scales (STADS; Spielberger et al. [58]) Family functioning: Kansas Inventory of Parental Perceptions (KIPP; Behr et al. [59]) Perceived stress: Family Stress and Coping Interview (FSCI; Nachshen et al. [60]) | n = 45 (43 mothers, 2 fathers) treatment group: n = 20, control group: n = 25 | No significant differences on parenting stress, anxiety, or depression |
| Erguner-Tekinalp and Akkok [61], 2004, Turkey | To explore effectiveness of coping skills training on stress, coping skills, and hopelessness among mothers | Mixed method, between-group/questionnaires, interviews/Mann Whitney U Test, content analysis Coping: Coping Strategy Indicator (CSI; Amirkhan [62]) Hopelessness: Beck Hopelessness Scale (BHS; Beck, Lester, and Trexler [63]) Parenting stress: Questionnaire on Resources and Stress (QRS; Holroyd [64]) | n = 20 mothers; Treatment group: n = 10, control group: n = 10 | No significant difference on stress level, but mothers in treatment group reported an increase in use of social support as a coping strategy, and felt a lower sense of hopelessness |
| Farmer and Reupert [65], 2013, Australia | To decrease parent carers’ anxiety and increase confidence by improving knowledge of ASD | Mixed method, within-subjects/questionnaires/paired t-test, inductive thematic analysis, Self-efficacy and parenting anxiety: Understanding Autism and Understanding my Child with Autism (Farmer and Reupert [65]) | n = 98 (63 mothers, 23 fathers); 86 participants were parents of child, 12 were other famly members | Parental knowledge of ASD, and confidence significantly increased, along with a significant decrease in anxiety |
| Feinberg et al. [66], 2013, United States | To explore if maternal stress and depressive symptoms would be reduced as the result of strengthening problem-solving skills | Experimental design/questionnaires, interviews/comparison of mean scores, Chronbach alpha Coping: Brief Coping Orientation to Problems (BCOP; Carver [67]) Depression: Quick Inventory of Depressive Symptomatology (QIDS; Rush et al. [68]) Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) | n = 110 mothers; Treatment group: n = 59, Control group: n = 61 | At three-month follow-up, mothers in the problem-solving education group reported higher use of social coping (both instrumental and emotional), and were significantly less likely than mothers in the control group to report clinically significant stress and depressive symptoms. No change in using problem-focused or avoidance coping skills |
| Ferraioli and Harris [70], 2013, United States | To evaluate benefits of mindfulness-based training approach compared to skills-based parentental training program on parental stress | Experimental design, between-group, within-subjects/questionnaires/independent t-tests, paired samples t-test General health: General Health Questionnaire-28 item (GHQ-28; Goldberg and Williams [53]) Mindfulness: Mindful Attention Awareness Scale (MAAS; Brown and Ryan [71]) Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) | n = 15 (10 mothers, 5 fathers) Mindfulness-based group: n = 6, Skills-based group: n = 9 | Parents in mindfulness-based group had significant improvement over skills-based group on measures of parental stress and general health at conclusion of training, and improved general health at 3-month follow-up |
| Giarelli et al. [72], 2005, United States | To refine a parent-focused nursing intervention and examine effects of post-diagnosis nursing intervention on parental psychological distress and use of services | Mixed methods, pretest-posttest experimental design, observations and survey/questionnaires, interview/non-parametric Wilcoxon test, content analysis Perceived stress: Perceived Stress Scale (PSS; Cohen and Williamson [73]) Psychological distress: Impact of Events Scale (IES; Zilberg et al. [74]) | n = 31 (16 mothers, 15 fathers), treatment group: n = 18, control: n = 13 | No significant differences on measures of parental distress but parents in intervention group reported being less upset due to unexpected event of child’s diagnosis, the intervention group increased their use of services when compared to treatment-as-usual group (control group). |
| Gika et al. [75], 2012, Greece | To examine impact of progressive muscle/breathing relaxation intervention on reduction of parental and perceived stress | Within-subjects, repeated measures/questionnaires/non-parametric Wilcoxon signed-rank test for dependent samples Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) Perceived stress: Perceived Stress Scale-14 items (PSS-14; Cohen, Kamarck and Mermelstein [76]) | n = 11mothers | Both parental stress and perceived stress was significantly reduced following intervention |
| Izadi-Mazidi et al. [77], 2015, Iran | To examine the effectiveness of a cognitive-behavior group therapy intervention on parenting stress | Within-subjects, repeated measures/questionnaires/Independent samples t-test Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) | n = 16 mothers | Parenting stress and distress was significantly reduced after intervention, which included education about ASD, discussions on cognitions and cognitive errors, and the practice of relaxation |
| Jamison et al. [78], 2017, United States | To evaluate a Family Peer Advocate (FPA) model on improving parent carers’ utilization of services, knowlege of ASD, and sense of empowerment, and reducing parenting stress | Experimental design/questionnaires/Repeated measures ANOVA Caregiver stress or burden: Caregiver-Strain Questionnaire (CSQ; Brannan et al. [79]) Family functioning: Family Empowerment Scale (FES; Karen et al. [80]) Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) Social support: Social Support Survey (SSS; Sherbourne and Steward [81]) | n = 39 racial/ethnic minority parents; Treatment group (i.e., FPA assigned to family): n = 19 Control group: n = 20 | Parenting stress in the treatment group was significantly decreased as compared to control group. No change was noted in caregiver’s sense of empowerment, or use of services, although a lack of available services in the community was noted. Parent knowledge of ASD in both groups increased |
| Ji et al. [82], 2014, China | To determine effectiveness of multi-disciplinary parent education program on improving health-related quality of life (HRQOL) of parent carers | Quasi-experimental between-groups/questionnaires/independent t-test and paired samples t-test Caregiver stress or burden: Caregiver Burden Index (CBI; Novak and Guest [83]) Coping: Simplified Coping Style Questionnaire (SCSQ; Wang, Wang, and Ma [84]) Family functioning: McMaster Family Assessment Device (FAD; Epstein, Baldwin and Bishop [85]) General health: Short Form Health Survey-36 items (SF-36, Rand Health [86]) Self-efficacy: General Self-Efficacy Scale (GSE; Jerusalem and Schwarzer [87]) Social support: Multidimensional Scale of Perceived Social Support (MSPSS; Zimet, Powell, Farley, Werkman, and Berkoff [88]) | n = 42 (38 mothers, 4 fathers) Treatment group: n = 22, Control group: n = 20 | Significant improvement in mental HRQOL, family functioning, self-efficacy, and positive coping style were reflected among participants in the intervention group |
| Joekar et al. [89], 016, Iran | To determine effectiveness of Acceptance and Commitment Therapy (ACT) on Iranian parent carers’ coping and mental health | Quasi-experimental between-group design/questionnaires/MANCOVA Acceptance: Acceptance and Action Questionnaire II (AAQ-II; Bond et al. [90]) General health: Short Form Health Survey-12 items (SF-12, Rand Health [91]) | n = 24 mothers; treatment group: n = 12, control group: n = 12 | ACT was found to be effective in decreasing symptoms of depression and increasing psychological flexibility |
| Kim [92], 2016, South Korea | To examine the effects of the Buddhist ontology focused meditation programme on the psychological health and well-being of mothers of children with ASD | Mixed methods, repeated measures, within-subjects/questionnaires, interview/ANOVA, content analysis Affect: Positive and Negative Affect Schedule (PANAS; Watson, Clark, and Tellegen [93]) Depression: Depression, Anxiety, and Stress Scale (DASS; Lovibond, and Lovibond [94]) Anxiety: State-Trait Anxiety Inventory (STAI; Spielberger [57]) Cognitions and automatic thoughts: Metacognitions Questionnaire (MCQ; Cartwright-Hatton and Wells [95]) Depression: Beck Depression Inventory II (BDI-II; Beck, Steer, and Brown [52]) | n = 9 mothers | A statistically significant improvement was found in psychological health well-being and positive affect. No changed was noted in anxiety or negative affect. Participants reported that the intervention helped them in relieving feelings of guilt that they had done wrong to accumulate bad karma and they were more aware of trying to accept people and things as they are. |
| Lovell et al. [96], 2016, UK | To examine the effectiveness of an intervention on reducing psychological distress in caregivers through written emotional disclosure regarding the benefits of caregiving | Experimental design/questionnaires, written essays/univariate ANOVA, chi square Depression: Hospital Anxiety and Depression Scale (HADS; Zigmond and Snaith [97]) Perceived stress: Perceived Stress Scale (PSS; Cohen and Williamson [73]) | n = 33 (28 mothers, 5 fathers) treatment group: n = 16, control group: n = 17 | Anxiety scores for parent carers in the benefit-finding condition were less likely to be in the clinical range 3-months post intervention |
| Nguyen et al. [98], 2016, United States | To determine if distress is reduced in mothers of children recently diagnosed with ASD following a problem-solving skills training program | Within-group, repeated measures/questionnaires/Mixed model analysis for repeated measures Depression: Beck Depression Inventory-Revised (BDI-R; Beck, Steer, and Brown [52]) Mood: Profile of Mood States (POMS; McNair et al. [99]) Psychological distress: Impact of Events Scale-Revised (IES-R; Creamer, Bell, and Failla [100]) | n = 24 mothers | Mothers increased their effectiveness to solve problems and experienced fewer depressive symptoms over the course of the study, less post-traumatic stress symptoms and less disturbance of mood was reported at 3-month follow-up but problem-solving skills had decreased |
| Niimomi et al. [101], 2016, Japan | To determine the effectiveness of a parenting support group program in reducing parental stress and improving quality of life | Within-subjects design/questionnaires/Repeated-measure multivariate analysis Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) Quality of life: World Health Organization Quality of Life 26 item (WHOQOL-26; WHOQOL Group [102]) | n = 24 mothers | A significant increase in quality of life was reported among participants at the conclusion of the program and at 3-months post follow-up. No change was noted in reducing parental stress. |
| Patra et al. [103], 2015, India | To develop a psycho-educational intervention for parents and to determine it’s impact on parent stress and knowledge of ASD | Mixed design, within-subjects/questionnaires, interview/Wilcoxon-signed rank test, nominal group technique Parenting stress: Family Interview for Stress and Coping (FISC-MR; Girimaji, et al. [104]) | n = 36 married parents (18 mothers, 18 fathers) | Parents’ social stress and total stress decreased by the conclusion of intervention. |
| Ryan and Ahman [105], 2016, Jordan | To examine effectiveness of brief mindfulness-based intervention on parent carers perceived quality of life (QoL) and positive stress reappraisal | Quasi-experimental with non-equivalent control group/questionnaires/Paired sample t-test, pre-post test Coping: Cognitive Emotion Regulation Questionnaire (CERQ; Garnefski, Kraaij, and Spinhoven [106]) Mindfulness: Mindful Attention Awareness Scale (MAAS; Brown and Ryan [71]) Quality of life: World Health Organization Quality of Life-Brief Version (WHOQOL-BREF; WHOQOL Group [107]) | n = 110 (73 mothers; 31 fathers) treatment group: n = 52 control group: n = 52 | Physical health and environmental health domains of QoL were not significant between groups, but there was a significant difference on psychological health, social relationship health, and overall QoL among participants in the mindfulness intervention group |
| Ruiz-Robledillo et al. [108], 2015, Spain | To assess the effects of a mindfulness intervention on the mood disturbances and health complaints among parent caregivers in comparison to non-caregivers | Quasi-experiemental, within-group, between-group Anger; State-Trait Anger Expression Inventory-2 (STAXI-2; Miguel-Tobal et al. [109]) Anxiety: State-Trait Anxiety Inventory (STAI; Spielberger [57]) Caregiver stress or burden: Zarit Burden Inventory (ZBI; Zarit et al. [110]) Depression: Beck Depression Inventory (BDI; Beck and Steer [111]) General health: General Health Questionnaire-28 item (GHQ-28; Goldberg and Williams [53]) Mood: Profile of Mood States (POMS; McNair et al. [99]) Somatic symptoms: Somatic Symptoms Scale-Revised (Spanish Version) (ESS-R; Sandin and Chorot [112]) | n = 13 (13 mothers; 1 father) Caregiver group: n = 6 (5 mothers, 1 father) Non-Caregiver group: n = 7 (7 mothers) | A significant reduction in mood disturbances and afternoon cortisol levels occurred for all participants, but were more pronounced in the caregiver group of parents. All participants reported a decrease in depressive and somatic symptoms at the end of the program and improved self-perceived general health. |
| Samadi et al. [113], 2012, Iran | To determine the effectiveness of a short group-based support course designed to increase parent’s knowledge of ASD and interventions to promote child’s development, boost parent’s confidence and sense of empowerment, and encourage parents to provide informal support to each other | Mixed design included pre-post, crossover design, within-group differences, between-group differences, questionnaires, interviews, paired t-tests, independent t-tests, content analysis Coping: Coping Styles Questionnaire (CSQ; Roger, Jervis and Najarian [114]) Family functioning: McMaster Family Assessment Device (FAD; Epstein, Baldwin and Bishop [85]) General health: General Health Questionnaire-28 item (GHQ-28; Goldberg and Williams [53]) Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) | n = 37 (24 mothers, 13 fathers) | Intervention resulted in significant improvements on parental ratings of health, stress, and family functioning, and a significant increase in use of problem-focused coping strategies up to 4-months post intervention |
| McConkey and Samadi [115], 2013, IranNOTE: This study is a 12-month follow-up study to Samadi et al. [113] and thus was not counted as a separate intervention study in the overall number of studies. | To determine the extent of informal support among Iranian parents who had a child with ASD following a group-based training course and if indicators of parental well-being and use of problem-focused and emotional focused coping strategies were maintained 12 months post-intervention | Mixed design included pre-post, crossover design, within-group differences, between-group differences/questionnaires, interviews/paired t-tests, independent t-tests, thematic analysis Coping: Coping Styles Questionnaire (CSQ; Roger, Jervis and Najarian [114]) Family functioning: McMaster Family Assessment Device (FAD; Epstein, Baldwin and Bishop [85]) Family health: General Health Questionnaire-28 item (GHQ-28; Goldberg and Williams [53]) Parenting stress: Parenting Stress Index-Short Form (PSI-SF; Abidin [69]) | n = 28 (17 mothers, 11 fathers) | Improved family functioning and better health of parents was maintained up to 12 months post-intervention, particularly among those parents who had maintained contact with others in the initial group-based intervention; child-related stress levels returned to baseline regardless if contact had been maintained; problem-focused coping strategies were not maintained 12 months-post intervention |
| Tongue et al. [116], 2006, Australia | To determine the impact of a parent education and behavior management intervention (PEBM), and a parent education and counseling intervention (PEC) on the mental health and adjustment of parent carers with preschool children with autism | Experimental design/questionnaires/Analysis of Covariance Family functioning: McMaster Family Assessment Device (FAD; Epstein, Baldwin and Bishop [85]) Family health: General Health Questionnaire-28 item (GHQ-28; Goldberg and Williams [53]) Parenting stress: Parenting Stress Thermometer [116] [visual analogue rating of general stress from 0 (none) to 4 (very, very much)] | n = 105 (info on gender of sample not reported) PEBM group: n = 35, PEC group: n = 35, Control group: n = 35 | Both the PEBM and PEC interventions contained the same educational material, however the PEBM intervention included sessions that were skills based and action oriented while the PEC intervention emphasized nondirective, interactive discussion and counseling. There were no significant differences between the outcomes of the PEBM and PEC groups-both interventions reduced overall symptoms of parental distress, although the PEC intervention reduced the depressive symptoms in a larger percentage of parents. |
| Zhang et al. [117], 2014, China | To evaluate the effectiveness of a group-based solution-focused brief therapy on promoting post-traumatic growth | Experimental design/questionnaires/independent samples t-test Post-traumatic growth: Post-Traumatic Growth Inventory-Chinese version (PTGI-C; Tedeschi and Calhoun [118]) | n = 45 mothers; Treatment groups = 20 (2 groups of 10), Control group = 25 | Post-traumatic growth was significantly higher among mothers in the intervention groups compared to control group. The difference was maintained at a 3-months follow-up. |
| Theme and Subthemes | 47 | 50 | 57 | 62 | 66 | 67 | 71 | 74 | 77 | 79 | 80 | 84 | 91 | 94 | 98 | 100 | 104 | 106 | 108 | 111 | 116/118 | 119 | 120 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Importance of social support | |||||||||||||||||||||||
| Informal networks | + | + | + | + | + | + | + | ||||||||||||||||
| Reduced isolation | + | + | + | + | + | + | |||||||||||||||||
| Validation by peers | + | + | + | + | + | + | + | + | |||||||||||||||
| Skill development | |||||||||||||||||||||||
| Acceptance/Stress management | + | + | + | + | + | + | + | + | + | + | |||||||||||||
| Problem-solving | + | + | + | + | + | + | + | + | + | ||||||||||||||
| Gaining knowledge | |||||||||||||||||||||||
| ASD | + | + | + | + | + | ||||||||||||||||||
| Resources, services | + | + | + | + |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Catalano, D.; Holloway, L.; Mpofu, E. Mental Health Interventions for Parent Carers of Children with Autistic Spectrum Disorder: Practice Guidelines from a Critical Interpretive Synthesis (CIS) Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 341. https://doi.org/10.3390/ijerph15020341
Catalano D, Holloway L, Mpofu E. Mental Health Interventions for Parent Carers of Children with Autistic Spectrum Disorder: Practice Guidelines from a Critical Interpretive Synthesis (CIS) Systematic Review. International Journal of Environmental Research and Public Health. 2018; 15(2):341. https://doi.org/10.3390/ijerph15020341
Chicago/Turabian StyleCatalano, Denise, Linda Holloway, and Elias Mpofu. 2018. "Mental Health Interventions for Parent Carers of Children with Autistic Spectrum Disorder: Practice Guidelines from a Critical Interpretive Synthesis (CIS) Systematic Review" International Journal of Environmental Research and Public Health 15, no. 2: 341. https://doi.org/10.3390/ijerph15020341
APA StyleCatalano, D., Holloway, L., & Mpofu, E. (2018). Mental Health Interventions for Parent Carers of Children with Autistic Spectrum Disorder: Practice Guidelines from a Critical Interpretive Synthesis (CIS) Systematic Review. International Journal of Environmental Research and Public Health, 15(2), 341. https://doi.org/10.3390/ijerph15020341






