Comorbidity of Symptoms of Alcohol and Cannabis Use Disorders among a Population-Based Sample of Simultaneous Users. Insight from a Network Perspective
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample and Procedures
2.2. Measures
2.3. Data Analysis
3. Results
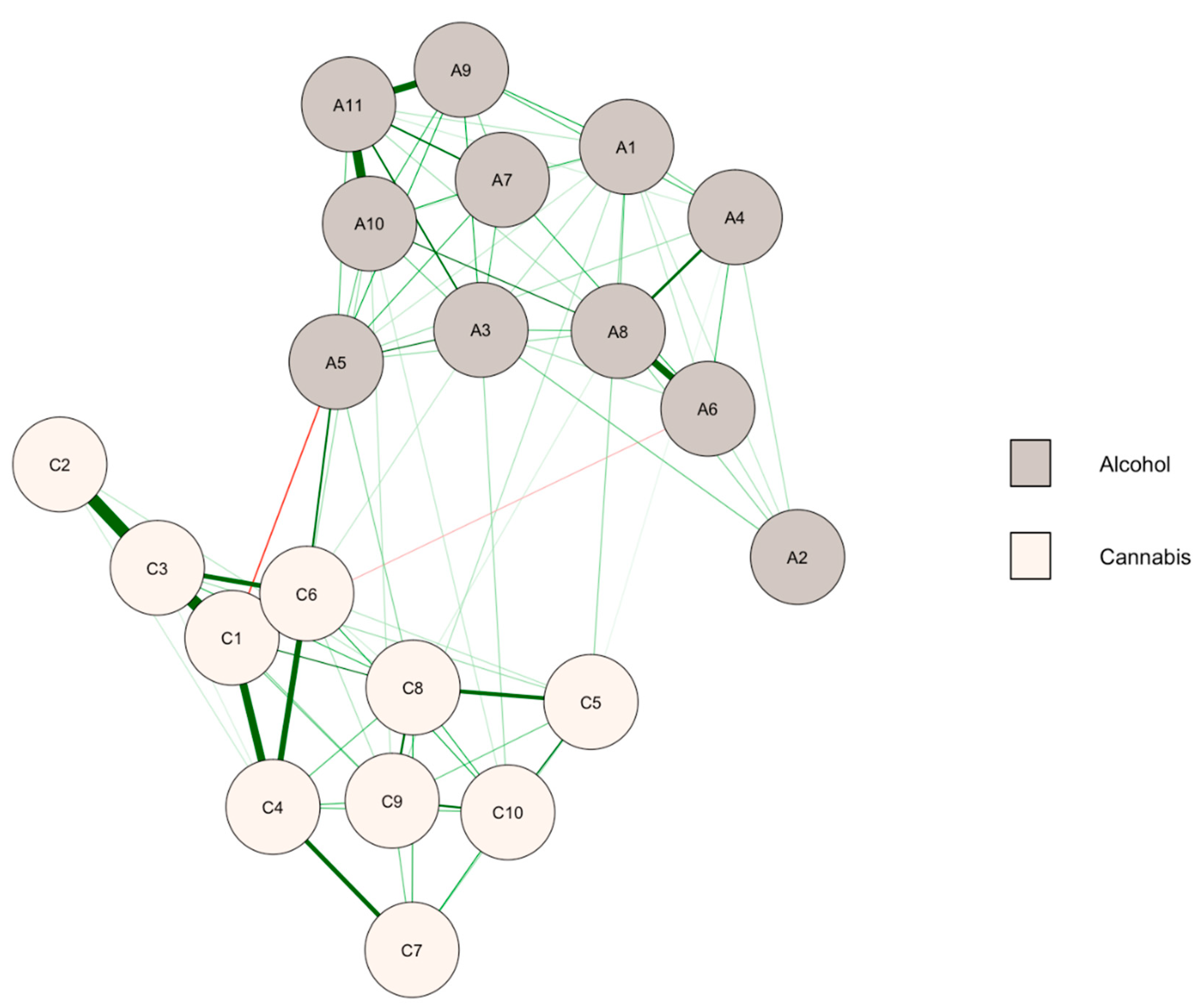
3.1. Baseline Network
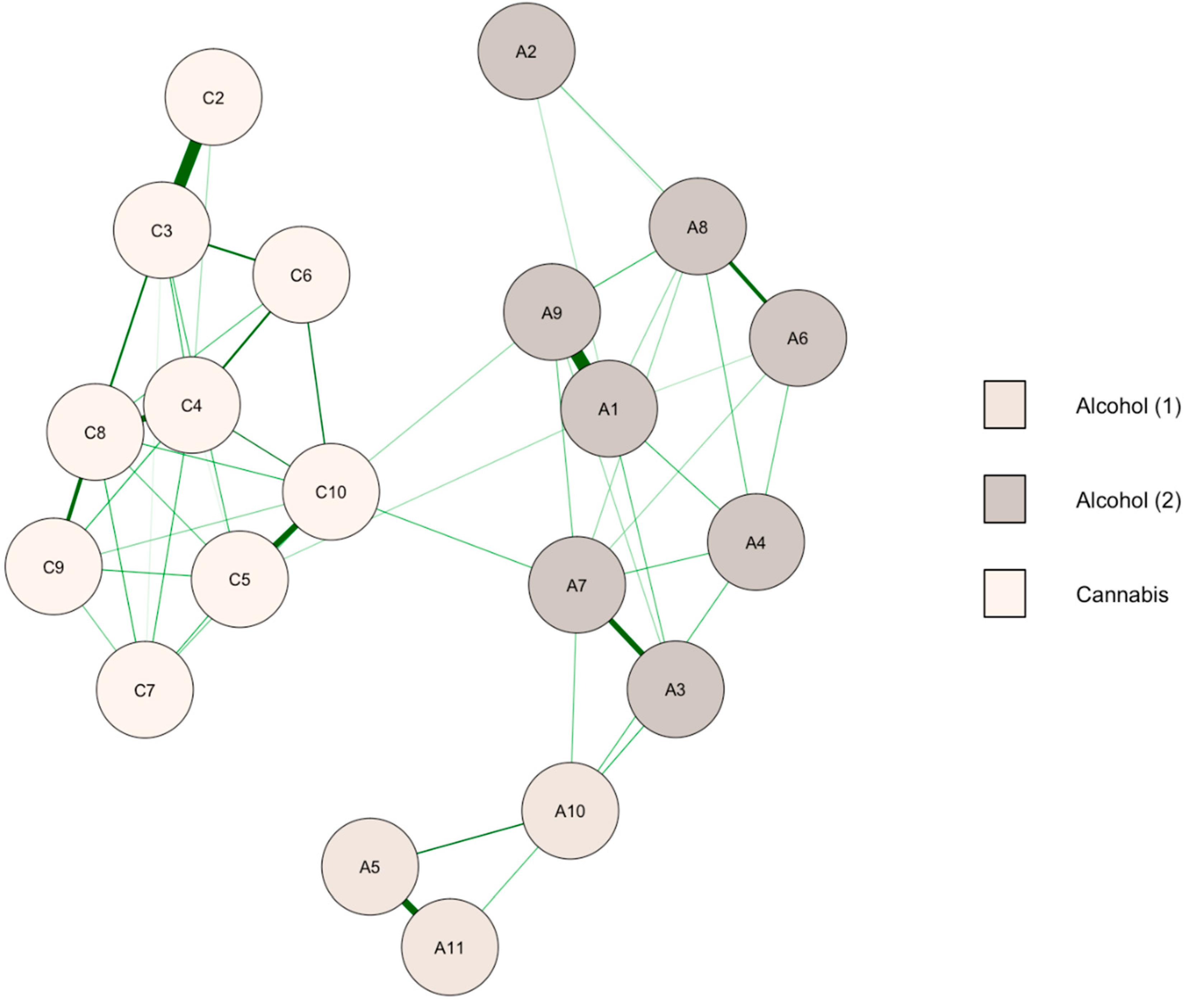
3.2. Follow-Up Network
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Midanik, L.T.; Tam, T.W.; Weisner, C. Concurrent and simultaneous drug and alcohol use: Results of the 2000 National Alcohol Survey. Drug Alcohol. Depend. 2007, 90, 72–80. [Google Scholar] [CrossRef] [PubMed]
- Patrick, M.E.; Terry-McElrath, Y.M.; Lee, C.M.; Schulenberg, J.E. Simultaneous alcohol and marijuana use among underage young adults in the United States. Addict. Behav. 2019, 88, 77–81. [Google Scholar] [CrossRef] [PubMed]
- Brière, F.N.; Fallu, J.S.; Descheneaux, A.; Janosz, M. Predictors and consequences of simultaneous alcohol and cannabis use in adolescents. Addict. Behav. 2011, 36, 785–788. [Google Scholar] [CrossRef] [PubMed]
- Pape, H.; Rossow, I.; Storvoll, E.E. Under double influence: Assessment of simultaneous alcohol and cannabis use in general youth populations. Drug Alcohol. Depend. 2009, 101, 69–73. [Google Scholar] [CrossRef] [PubMed]
- Subbaraman, M.S.; Kerr, W.C. Simultaneous versus concurrent use of alcohol and cannabis in the National Alcohol Survey. Alcohol. Clin. Exp. Res. 2015, 39, 872–879. [Google Scholar] [CrossRef] [PubMed]
- Terry-McElrath, Y.M.; O’Malley, P.M.; Johnston, L.D. Simultaneous alcohol and marijuana use among US high school seniors from 1976 to 2011: Trends, reasons, and situations. Drug Alcohol. Depend. 2013, 133, 71–79. [Google Scholar] [CrossRef] [PubMed]
- Terry-McElrath, Y.M.; O’Malley, P.M.; Johnston, L.D. Alcohol and Marijuana Use Patterns Associated with Unsafe Driving Among U.S. High School Seniors: High Use Frequency, Concurrent Use, and Simultaneous Use. J. Stud. Alcohol. Drugs 2014, 75, 378–389. [Google Scholar] [CrossRef]
- Baggio, S.; Studer, J.; Deline, S.; N’Goran, A.; Mohler-Kuo, M.; Daeppen, J.B.; Gmel, G. Simultaneous use of alcohol, tobacco and cannabis in relation to severity of substance dependence: A study among young Swiss men. J. Addict. Res. Therapy. 2014. [Google Scholar] [CrossRef]
- Subbaraman, M.S. Substitution and complementarity of alcohol and cannabis: A review of the literature. Subst. Use Misuse 2016, 51, 1399–1414. [Google Scholar] [CrossRef]
- Peters, E.N.; Hughes, J.R. Daily marijuana users with past alcohol problems increase alcohol consumption during marijuana abstinence. Drug Alcohol Depend. 2010, 106, 111–118. [Google Scholar] [CrossRef]
- Subbaraman, M.S.; Metrik, J.; Patterson, D.; Swift, R. Cannabis use during treatment for alcohol use disorders predicts alcohol treatment outcomes. Addiction 2017, 112, 685–694. [Google Scholar] [CrossRef] [PubMed]
- Blanco, C.; Okuda, M.; Wang, S.; Liu, S.-M.; Olfson, M. Testing the drug substitution switching-addictions hypothesis: A prospective study in a nationally representative sample. JAMA Psychiatry 2014, 71, 1246–1253. [Google Scholar] [CrossRef] [PubMed]
- Yurasek, A.M.; Aston, E.R.; Metrik, J. Co-use of Alcohol and Cannabis: A Review. Curr. Addict. Rep. 2017, 4, 184–193. [Google Scholar] [CrossRef]
- Yurasek, A.M.; Merrill, J.E.; Metrik, J.; Miller, M.B.; Fernandez, A.C.; Borsari, B. Marijuana use in the context of alcohol interventions for mandated college students. J. Subst. Abuse Treat. 2017, 79, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Borsboom, D. A network theory of mental disorders. World Psychiatry 2017, 16, 5–13. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, S.G.; Curtiss, J.; McNally, R.J. A complex network perspective on clinical science. Perspect. Psychol. Sci. 2016, 11, 597–605. [Google Scholar] [CrossRef] [PubMed]
- Cramer, A.O.J.; Waldorp, L.J.; van der Maas, H.L.J.; Borsboom, D. Comorbidity: A network perspective. Behav. Brain Sci. 2010, 33, 137–150; discussion 50–93. [Google Scholar] [CrossRef] [PubMed]
- Schmittmann, V.D.; Cramer, A.O.J.; Waldorp, L.J.; Epskamp, S.; Kievit, R.A.; Borsboom, D. Deconstructing the construct: A network perspective on psychological phenomena. New Ideas Psychol. 2013, 31, 43–53. [Google Scholar] [CrossRef]
- Borsboom, D.; Cramer, A.O.J. Network analysis: An integrative approach to the structure of psychopathology. Annu. Rev. Clin. Psychol. 2013, 9, 91–121. [Google Scholar] [CrossRef]
- Baggio, S.; Gainsbury, S.M.; Berchtold, A.; Iglesias, K. Co-morbidity of gambling and Internet use among Internet and land-based gamblers: Classic and network approaches. Int. Gambl. Stud. 2016, 16, 500–517. [Google Scholar] [CrossRef]
- Ruzzano, L.; Borsboom, D.; Geurts, H.M. Repetitive behaviors in autism and obsessive-compulsive disorder: New perspectives from a network analysis. J. Autism Dev. Disord. 2015, 45, 192–202. [Google Scholar] [CrossRef]
- Fried, E.I.; van Borkulo, C.D.; Cramer, A.O.J.; Boschloo, L.; Schoevers, R.A.; Borsboom, D. Mental disorders as networks of problems: A review of recent insights. Soc. Psychiatry Psychiatr. Epidemiol. 2017, 52, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Rhemtulla, M.; Fried, E.I.; Aggen, S.H.; Tuerlinckx, F.; Kendler, K.S.; Borsboom, D. Network analysis of substance abuse and dependence symptoms. Drug Alcohol. Depend. 2016, 161, 230–237. [Google Scholar] [CrossRef] [PubMed]
- Barrett, S.P.; Darredeau, C.; Pihl, R.O. Patterns of simultaneous polysubstance use in drug using university students. Hum. Psychopharmacol. 2006, 21, 255–263. [Google Scholar] [CrossRef] [PubMed]
- Somers, J.M.; Goldner, E.M.; Waraich, P.; Hsu, L. Prevalence studies of substance-related disorders: A systematic review of the literature. Can. J. Psychiatry 2004, 49, 373–384. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, M.; Steinley, D.; Trull, T.J.; Sher, K.J. Criteria definitions and network relations: The importance of criterion thresholds. Clin. Psychol. Sci. 2018, 6, 506–516. [Google Scholar] [CrossRef] [PubMed]
- Gmel, G.; Akre, C.; Astudillo, M.; Bähler, C.; Baggio, S.; Bertholet, N.; Clair, C.; Cornuz, J.; Daeppen, J.B.; Deline, S.; et al. The Swiss Cohort Study on Substance Use Risk Factors—Findings of two Waves. Sucht 2015, 61, 251–262. [Google Scholar] [CrossRef]
- Studer, J.; Baggio, S.; Mohler-Kuo, M.; Dermota, P.; Gaume, J.; Bertholet, N.; Daeppen, J.B.; Gmel, G. Examining non-response bias in substance use research—Are late respondents proxies for non-respondents? Drug Alcohol. Depend. 2013, 132, 316–323. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Publishing: Arlington, VA, USA, 2013. [Google Scholar]
- Annaheim, B.; Scotto, T.J.; Gmel, G. Revising the Cannabis Use Disorders Identification Test (CUDIT) by means of Item Response Theory. Int. J. Methods Psychiatr. Res. 2010, 19, 142–155. [Google Scholar] [CrossRef]
- Van Borkulo, C.D.; Borsboom, D.; Epskamp, S.; Blanken, T.F.; Boschloo, L.; Schoevers, R.A.; Waldorp, L.J. A new method for constructing networks from binary data. Sci. Rep. 2014, 4, 5918. [Google Scholar] [CrossRef]
- Kossakowski, J.; Cramer, A.O.J. Complex dynamical systems in psychology. In Network Science in Cognitive Psychology; Vitevitch, M., Ed.; Rutledge Taylor & Francis Group: Abingdon-on-Thames, UK, 2017. [Google Scholar]
- Pons, P.; Latapy, M. (Eds.) Computing communities in large networks using random walks. In International Symposium on Computer and Information Sciences; Springer: Berlin/Heidelberg, Germany, 2005. [Google Scholar]
- Payton, J. Package ‘Networktools’–Tools for Identifying Important Nodes in Networks. Available online: https://cran.r-project.org/web/packages/networktools/networktools.pdf (accessed on 11 December 2018).
- Epskamp, S.; Borsboom, D.; Fried, E.I. Estimating psychological networks and their accuracy: A tutorial paper. arXiv, 2016; arXiv:160408462. [Google Scholar]
- Epskamp, S.; Cramer, A.O.J.; Waldorp, L.J.; Schmittmann, V.D.; Borsboom, D. qgraph: Network Visualizations of Relationships in Psychometric Data. J. Stat. Softw. 2012, 48, 1–18. [Google Scholar] [CrossRef]
- Forbes, M.K.; Wright, A.G.C.; Markon, K.E.; Krueger, R.F. Evidence that psychopathology symptom networks have limited replicability. J. Abnorm. Psychol. 2017, 126, 969–988. [Google Scholar] [CrossRef] [PubMed]
- Borsboom, D.; Fried, E.I.; Epskamp, S.; Waldorp, L.J.; van Borkulo, C.D.; van der Maas, H.L.; Cramer, A.O. False alarm? A comprehensive reanalysis of “Evidence that psychopathology symptom networks have limited replicability” by Forbes, Wright, Markon, and Krueger (2017). J. Abnorm. Psychol. 2017, 126, 989–999. [Google Scholar] [CrossRef] [PubMed]
- Forbes, M.K.; Wright, A.G.C.; Markon, K.E.; Krueger, R.F. Further evidence that psychopathology networks have limited replicability and utility: Response to Borsboom et al. (2017) and Steinley et al. (2017). J. Abnorm. Psychol. 2017, 126, 1011–1016. [Google Scholar] [CrossRef] [PubMed]
- Metrik, J.; Spillane, N.S.; Leventhal, A.M.; Kahler, C.W. Marijuana use and tobacco smoking cessation among heavy alcohol drinkers. Drug Alcohol. Depend. 2011, 119, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Brache, K.; Stockwell, T.; Macdonald, S. Functions and harms associated with simultaneous polysubstance use involving alcohol and cocaine. J Subst. Use 2012, 17, 399–416. [Google Scholar] [CrossRef]
- Hyland, M.E. Network origins of anxiety and depression. Behav. Brain Sci. 2010, 33, 161–162. [Google Scholar] [CrossRef] [PubMed]
- Bos, E.H.; Wanders, R.B.K. Group-level symptom networks in depression. JAMA Psychiatry 2016, 73, 411. [Google Scholar] [CrossRef] [PubMed]
- Haslam, N. Symptom networks and psychiatric categories. Behav. Brain Sci. 2010, 33, 158–159. [Google Scholar] [CrossRef] [PubMed]
- Lal, R.; Deb, K.S.; Kedia, S. Substance use in women: Current status and future directions. Indian J. Psychiatry 2015, 57 (Suppl. 2), S275–S285. [Google Scholar] [CrossRef]
- Pabst, A.; Kraus, L.; Piontek, D.; Baumeister, S.E. Age differences in diagnostic criteria of DSM-IV alcohol dependence among adults with similar drinking behaviour. Addiction 2012, 107, 331–338. [Google Scholar] [CrossRef] [PubMed]
- Karriker-Jaffe, K.J.; Witbrodt, J.; Greenfield, T.K. Refining measures of alcohol problems for general population surveys. Alcohol. Clin. Exp. Res. 2015. [Google Scholar] [CrossRef] [PubMed]
- Saunders, J. What Is This Thing Called Addiction? Victoria, BC, Canada, 2014. [Google Scholar]
| Label | Items | Baseline (n = 1559) | Follow-up (n = 991) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| % | Bridge Strength | Bridge Betweenness | Bridge Closeness | % | Bridge Strength | Bridge Betweenness | Bridge Closeness | ||
| A1 | Neglect important activities | 20.9 | 0.60 | 8 | 0.23 | 19.5 | 0.33 | 5 | 0.24 |
| A2 | Increased chances of getting injured | 45.4 | 0.00 | 0 | 0.18 | 46.6 | 0.00 | 0 | 0.13 |
| A3 | Resume drinking habits despites problems with others | 8.1 | 0.50 | 11 | 0.28 | 6.5 | 0.00 | 0 | 0.27 |
| A4 | Tolerance | 34.2 | 0.07 | 0 | 0.19 | 27.4 | 0.00 | 0 | 0.22 |
| A5 | Withdrawal | 6.9 | 2.09 | 69 | 0.40 | 4.7 | 0.00 | 0 | 0.16 |
| A6 | Drink more/longer than intended | 43.0 | 0.28 | 0 | 0.18 | 51.2 | 0.00 | 0 | 0.17 |
| A7 | Try to cut down but couldn’t | 5.8 | 0.00 | 9 | 0.25 | 5.5 | 0.63 | 54 | 0.35 |
| A8 | Spend time obtaining, using, recovering from alcohol | 26.6 | 0.12 | 2 | 0.19 | 27.0 | 0.00 | 4 | 0.18 |
| A9 | Give up activities | 5.0 | 0.00 | 14 | 0.26 | 4.5 | 0.37 | 17 | 0.25 |
| A10 | Continue drinking despites health problems | 5.4 | 0.72 | 3 | 0.22 | 3.8 | 0.00 | 18 | 0.20 |
| A11 | Strong desire or urge to drink | 6.0 | 0.00 | 0 | 0.24 | 6.0 | 0.00 | 0 | 0.15 |
| C1 | Frequency of cannabis use previous 12 months | 48.6 | 1.11 | 0 | 0.24 | 100 * | - | - | - |
| C2 | Felt stoned after using cannabis ≥3 h | 37.4 | 0.00 | 0 | 0.21 | 47.4 | 0.00 | 0 | 0.16 |
| C3 | Felt stoned for ≥6 h | 46.3 | 0.00 | 11 | 0.24 | 52.3 | 0.00 | 11 | 0.18 |
| C4 | Being not able to stop using cannabis | 20.3 | 0.00 | 13 | 0.24 | 18.9 | 0.00 | 0 | 0.22 |
| C5 | Failed to do what is expected | 36.0 | 0.43 | 3 | 0.21 | 35.2 | 0.33 | 17 | 0.25 |
| C6 | Need of cannabis in the morning after a heavy cannabis intake | 16.6 | 1.36 | 64 | 0.31 | 12.9 | 0.00 | 18 | 0.22 |
| C7 | Felt guilty or remorseful | 29.3 | 0.00 | 0 | 0.20 | 27.6 | 0.00 | 0 | 0.18 |
| C8 | Had a problem with memory/concentration | 39.3 | 0.51 | 2 | 0.22 | 36.8 | 0.00 | 0 | 0.21 |
| C9 | Refrained from leisure activities | 18.4 | 0.47 | 0 | 0.20 | 18.9 | 0.00 | 0 | 0.18 |
| C10 | Had difficulties at work/school | 12.4 | 0.50 | 4 | 0.23 | 8.8 | 1.00 | 78 | 0.31 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baggio, S.; Sapin, M.; Khazaal, Y.; Studer, J.; Wolff, H.; Gmel, G. Comorbidity of Symptoms of Alcohol and Cannabis Use Disorders among a Population-Based Sample of Simultaneous Users. Insight from a Network Perspective. Int. J. Environ. Res. Public Health 2018, 15, 2893. https://doi.org/10.3390/ijerph15122893
Baggio S, Sapin M, Khazaal Y, Studer J, Wolff H, Gmel G. Comorbidity of Symptoms of Alcohol and Cannabis Use Disorders among a Population-Based Sample of Simultaneous Users. Insight from a Network Perspective. International Journal of Environmental Research and Public Health. 2018; 15(12):2893. https://doi.org/10.3390/ijerph15122893
Chicago/Turabian StyleBaggio, Stéphanie, Marlène Sapin, Yasser Khazaal, Joseph Studer, Hans Wolff, and Gerhard Gmel. 2018. "Comorbidity of Symptoms of Alcohol and Cannabis Use Disorders among a Population-Based Sample of Simultaneous Users. Insight from a Network Perspective" International Journal of Environmental Research and Public Health 15, no. 12: 2893. https://doi.org/10.3390/ijerph15122893
APA StyleBaggio, S., Sapin, M., Khazaal, Y., Studer, J., Wolff, H., & Gmel, G. (2018). Comorbidity of Symptoms of Alcohol and Cannabis Use Disorders among a Population-Based Sample of Simultaneous Users. Insight from a Network Perspective. International Journal of Environmental Research and Public Health, 15(12), 2893. https://doi.org/10.3390/ijerph15122893





