Incidence, Costs and Predictors of Non-Union, Delayed Union and Mal-Union Following Long Bone Fracture
Abstract
1. Introduction
2. Methods
3. Results
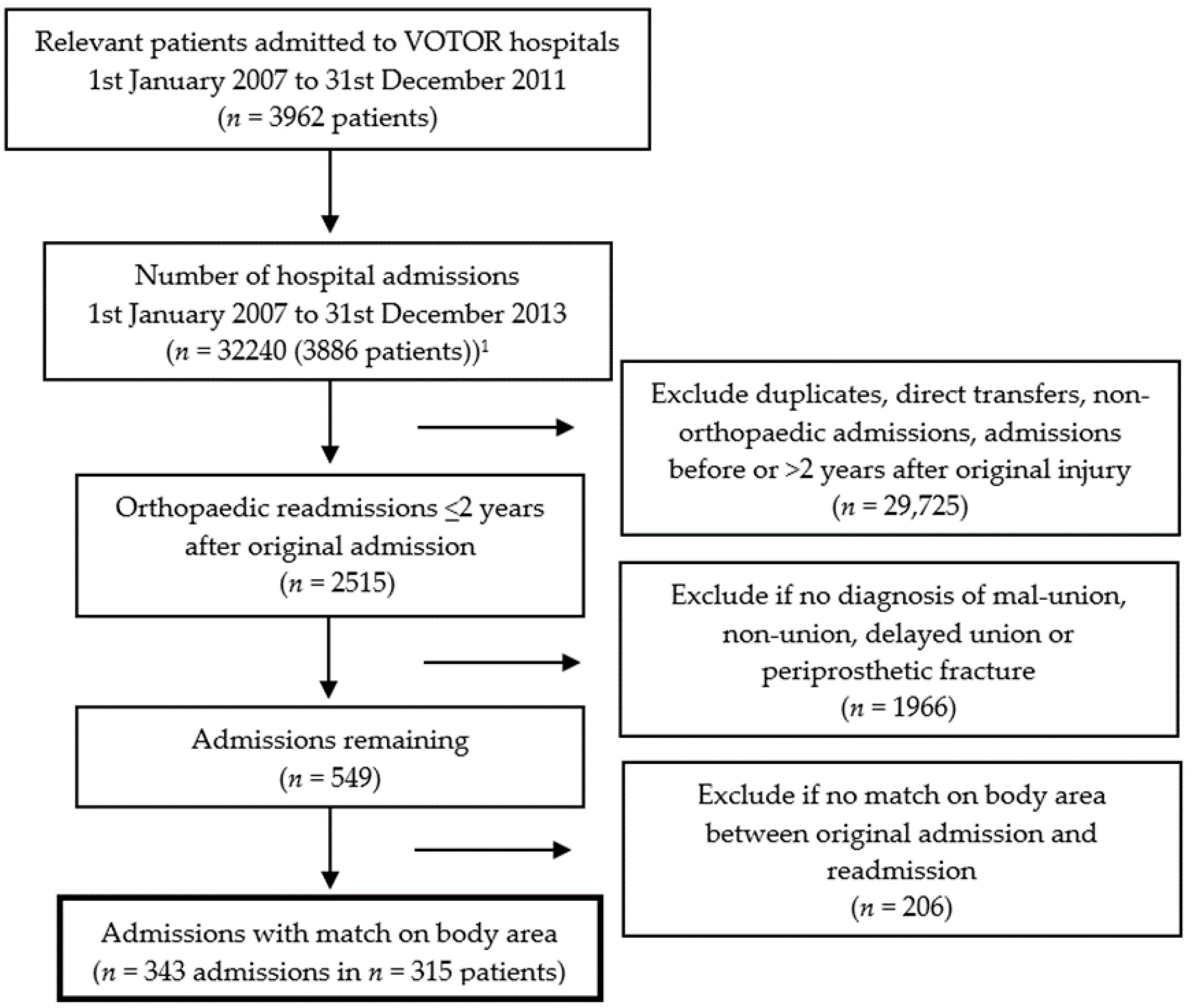
3.1. Patients Readmitted for Fracture Healing Complications
3.2. Time to Hospital Readmission, Length of Stay and Costs for Fracture Healing Complication Admissions
3.3. Type and Number of Readmissions for Fracure Healing Complications
3.4. Characteristics of Patients Admitted for Fracture Healing Complications
3.5. Factors Associated with the Admission for Fracture Healing Complications
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bradley, C.; Harrison, J. Descriptive Epidemiology of Traumatic Fractures in Australia; AIHW: Adelaide, Australia, 2004.
- Bonafede, M.; Espindle, D.; Bower, A.G. The direct and indirect costs of long bone fractures in a working age US population. J. Med. Econ. 2013, 16, 169–178. [Google Scholar] [CrossRef] [PubMed]
- Norton, L.; Harrison, J.E. Hospital Separations due to Injury and Poisoning, Australia 2007–08; Contract No: INJCAT 140; AIHW: Canberra, Australia, 2012.
- Hak, D.; Fitzpatrick, D.; Bishop, J.; Marsh, J.; Tilp, S.; Schnettler, R.; Simpson, H.; Alt, V. Delayed union and nonunions: Epidemiology, clinical issues, and financial aspects. Injury 2014, 45, S3–S7. [Google Scholar] [CrossRef] [PubMed]
- Lerner, R.K.; Esterhai, J.L., Jr.; Polomano, R.C.; Cheatle, M.D.; Heppenstall, R.B. Quality of life assessment of patients with posttraumatic fracture nonunion, chronic refractory osteomyelitis, and lower-extremity amputation. Clin. Orthop. Relat. Res. 1993, 28–36. [Google Scholar] [CrossRef]
- Mills, L.A.; Aitken, S.A.; Simpson, A. The risk of non-union per fracture: current myths and revised figures from a population of over 4 million adults. Acta Orthop. 2017, 88, 434–439. [Google Scholar] [CrossRef] [PubMed]
- Zimmermann, G.; Moghaddam, A. Trauma: Non-Union: New Trends. Eur. Instruct. Lect. 2010, 10, 10–19. [Google Scholar]
- Mills, L.; Simpson, A. The relative incidence of fracture non-union in the Scottish population (5.17 million): A 5-year epidemiological study. BMJ Open 2014, 3, e002276. [Google Scholar] [CrossRef] [PubMed]
- Kanakaris, N.; Giannoudis, P. The health economics of long-bone non-unions. Injury 2007, 38, S77–S84. [Google Scholar] [CrossRef]
- Antonova, E.; Le, T.; Burge, R.; Mershon, J. Tibia shaft fractures: costly burden of nonunions. BMC Musculoskelet. Disord. 2013, 14, 42. [Google Scholar] [CrossRef] [PubMed]
- Perumal, V.; Roberts, C.S. (ii) Factors contributing to non-union of fractures. Curr. Orthop. 2007, 21, 258–261. [Google Scholar] [CrossRef]
- Nandra, R.; Grover, L.; Porter, K. Fracture non-union epidemiology and treatment. Trauma 2015, 18, 3–11. [Google Scholar] [CrossRef]
- Brinker, M.R.; O’Connor, D.P. Nonunions: Evaluation and treatment. In Skeletal Trauma: Basic Science, Management, and Reconstruction, 4th ed.; Browner, B.D., Jupiter, J.B., Levine, A.M., Trafton, P.G., Krettek, C., Eds.; WB Saunders: Philadelphia, PA, USA, 2009; pp. 637–718. [Google Scholar]
- Beck, B.; Devlin, A.; Hart, M.; Gabbe, B. Victorian Orthopaedic Trauma Outcomes Registry (VOTOR) Annual Report; Monash University: Melbourne, Australia, 2018. [Google Scholar]
- National Centre for Classification in Health. International Statistical Classification of Diseases and Related Health Problems, Tenth Revision, Australian Modification (ICD-10-AM); Independent Hospital Pricing Authority: Sydney, Australia, 2010.
- Duckett, S. The development of Australian refined diagnosis related groups: The Australian inpatient casemix classification. Casemix Quart. 2000, 2, 115–120. [Google Scholar]
- World Health Organization. International Classification of Functioning, Disability and Health: ICF; World Health Organization: Geneva, Switzerland, 2001; Available online: http://www.who.int/classifications/icf/en/ (accessed on 11 September 2015).
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Socio-Economic Indexes for Areas (SEIFA) 2011. 2013. Available online: http://www.abs.gov.au/ausstats/abs@.nsf/mf/2039.0/ (accessed on 28 July 2015).
- Clay, F.; Ozanne-Smith, J. Private hospital insurance status among a state-wide injured population. Aust. Health Rev. 2006, 30, 252–258. [Google Scholar] [CrossRef] [PubMed]
- Independent Hospital Pricing Authority. National Hospital Cost Data Collection Cost Weight Tables 2018. Available online: https://www.ihpa.gov.au/publications?f%5B0%5D=field_publication_section%3A4 (accessed on 9 November 2015).
- Hosmer, J.D.W.; Lemeshow, S.; Sturdivant, R.X. Model-Building Strategies and Methods for Logistic Regression. In Applied Logistic Regression; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2013; pp. 89–151. [Google Scholar]
- Tzioupis, C.; Giannoudis, P.V. Prevalence of long-bone non-unions. Injury 2007, 38, S3–S9. [Google Scholar] [CrossRef]
- Giannoudis, P.; Tzioupis, C.; Almalki, T.; Buckley, R. Fracture healing in osteoporotic fractures: Is it really different? A basic science perspective. Injury 2007, 38 (Suppl. 1), S90–S99. [Google Scholar] [CrossRef] [PubMed]
- O’Halloran, K.; Coale, M.; Costales, T.; Zerhusen, T., Jr.; Castillo, R.C.; Nascone, J.W.; O’Toole, R.V. Will My Tibial Fracture Heal? Predicting Nonunion at the Time of Definitive Fixation Based on Commonly Available Variables. Clin. Orthop. Relat. Res. 2016, 474, 1385–1395. [Google Scholar] [CrossRef] [PubMed]
- MacKenzie, E.; Bosse, M.; Kellam, J.; Pollak, A.; Webb, L.; Swiontkowski, M.; Smith, D.G.; Sanders, R.W.; Jones, A.L.; Starr, A.J.; et al. Early predictors of long-term work disability after major limb trauma. J. Trauma 2006, 61, 688–694. [Google Scholar] [CrossRef] [PubMed]
- Gabbe, B.; Cameron, P.; Williamson, O.; Edwards, E.; Graves, S.; Richardson, M. The relationship between compensable status and long-term patient outcomes following orthopaedic trauma. Med. J. Aust. 2007, 187, 14–17. [Google Scholar] [PubMed]
- Harris, I.; Mulford, J.; Solomon, M.; van Gelder, J.; Young, J. Association between compensation status and outcome after surgery. JAMA 2005, 293, 1644–1652. [Google Scholar] [CrossRef] [PubMed]
- Harwood, P.J.; Newman, J.B.; Michael, A.L.R. (ii) An update on fracture healing and non-union. Orthop. Trauma 2010, 24, 9–23. [Google Scholar] [CrossRef]
- Bhandari, M.; Guyatt, G.; Swiontkowski, M.; Tornetta, P.; Sprague, S.; Schemitsch, E. A lack of consensus in the assessment of fracture healing among orthopaedic surgeons. J. Orthop. Trauma 2002, 16, 562–566. [Google Scholar] [CrossRef] [PubMed]
| 1st Admission | All Admissions (Range 1–3 per Patient) | ||
|---|---|---|---|
| Time to Admission (months) | Range per patient | 2–24 | |
| Median (IQR) per patient | 8 (5–12) | ||
| Length of stay (days) | Range per patient | 1–63 | 1–109 |
| Median (IQR) per patient | 2 (1–5) | 3 (1–6) | |
| Total days all patients | 1549 | 1792 | |
| Costs ($AUD) | Range per patient | $4788–$35,890 | $4788–$93,197 |
| Median (IQR) per patient | $14,957 ($9462–$15,520) | $14,957 ($9632–$19,887) | |
| Total costs all patients | $4,339,098 | $4,916,438 |
| Fracture Type | Fractures (n) | Admissions per Patient (n) | Total Admissions (n, % Fractures) | ||
|---|---|---|---|---|---|
| 1 | 2 | 3 | |||
| Proximal humerus fracture | 1117 | 26 | 26 (2.3) | ||
| Shaft of humerus fracture | 413 | 28 | 2 | 32 (7.8) | |
| Subtrochanteric fracture | 308 | 13 | 13 (4.2) | ||
| Shaft of femur fracture | 791 | 89 | 9 | 107 (13.5) | |
| Distal femur fracture | 465 | 25 | 7 | 39 (8.4) | |
| Shaft of tibia fracture | 1075 | 111 | 6 | 1 | 126 (11.7) |
| Total | 4169 1 | 343 (8.2) | |||
| Descriptor | Patients with Complications (n = 315) n (%) | Patients without complications (n = 3571) n (%) | |
|---|---|---|---|
| Age group | 15–24 years | 61 (19.4) | 566 (15.9) |
| 25–34 years | 61 (19.4) | 475 (13.3) | |
| 35–44 years | 49 (15.6) | 418 (11.7) | |
| 45–54 years | 41 (13.0) | 364 (10.2) | |
| 55–64 years | 53 (16.8) | 396 (11.1) | |
| 65–74 years | 23 (7.3) | 465 (13.0) | |
| 75–84 years | 20 (6.4) | 551 (15.4) | |
| 85+ years | 7 (2.2) | 336 (9.4) | |
| Sex | Male | 221 (70.2) | 1936 (54.2) |
| Female | 94 (29.8) | 1635 (45.8) | |
| Marital status | Never married | 116 (36.8) | 1183 (33.1) |
| Widowed | 19 (6.0) | 536 (15.0) | |
| Divorced/Separated | 14 (4.4) | 225 (6.3) | |
| Married | 122 (38.7) | 1281 (35.9) | |
| De Facto | 24 (7.6) | 203 (5.7) | |
| Not stated/inadequately described | 20 (6.4) | 143 (4.0) | |
| ARIA 1 | Major cities of Australia | 221 (70.8) | 2592 (74.4) |
| Inner regional Australia | 70 (22.4) | 769 (22.1) | |
| Outer regional and remote Australia | 21 (6.7) | 121 (3.5) | |
| IRSAD decile 2 | 10 (Most advantaged) | 40 (12.8) | 582 (16.7) |
| 9 | 4450 (16.0) | 570 (16.4 | |
| 8 | 46 (11.5) | 570 (16.4) | |
| 7 | 33 (14.1) | 462 (13.3) | |
| 6 | 33 (10.6) | 274 (7.9) | |
| 5 | 28 (9.0) | 238 (6.8) | |
| 4 | 25 (8.0) | 266 (7.6) | |
| 3 | 21 (6.7) | 100 (2.9) | |
| 2 | 19 (6.1) | 219 (6.3) | |
| 1 (Most disadvantaged) | 16 (5.1) | 203 (5.8) | |
| Comorbidities (CCI) | None | 235 (74.6) | 2545 (71.3) |
| CCI = 1 | 67 (21.3) | 736 (20.6) | |
| CCI > 1 | 13 (4.1) | 290 (8.1) | |
| Cause of injury | Low fall | 47 (14.9) | 1350 (37.8) |
| High fall | 23 (7.3) | 296 (8.3) | |
| Road trauma | 209 (66.4) | 1,401 (39.2) | |
| Other external cause | 36 (11.4) | 524 (14.7) | |
| Compensable status 3 | Medicare/Non compensable | 74 (23.6) | 1737 (48.9) |
| Private/DVA | 30 (9.6) | 515 (14.5) | |
| TAC/Worksafe/Other compensable | 210 (66.9) | 1301 (36.6) | |
| Head injury | No | 240 (76.2) | 3036 (85.0) |
| Yes | 75 (23.8) | 535 (15.0) | |
| Other non-orthopaedic injuries | No | 194 (61.6) | 2729 (76.4) |
| Yes | 121 (38.4) | 842 (23.6) | |
| Fracture readmission type | Proximal humerus | 26 (8.3) | 1021 (28.6) |
| Shaft of humerus | 30 (9.5) | 320 (9.0) | |
| Subtrochanteric | 13 (4.1) | 263 (7.4) | |
| Shaft of femur | 97 (30.8) | 560 (15.7) | |
| Distal femur | 31 (9.8) | 352 (9.9) | |
| Shaft of tibia | 116 (36.8) | 848 (23.8) | |
| Shaft of tibia and femur | 2 (0.6) | 207 (5.8) 4 | |
| Descriptor | Multivariable Analysis (n = 3775) | ||
|---|---|---|---|
| AOR (95% CI) | P | ||
| Age group | 15–24 years | 1.00 (ref.) | 0.004 |
| 25–34 years | 1.37 (0.91,2.07) | ||
| 35–44 years | 1.28 (0.81,2.02) | ||
| 45–54 years | 1.49 (0.91,2.46) | ||
| 55–64 years | 2.44 (1.48,4.02) | ||
| 65–74 years | 1.20 (0.64,2.22) | ||
| 75–84 years | 0.99 (0.50,1.97) | ||
| 85+ years | 0.67 (0.25,1.80) | ||
| Compensable status 1 | Medicare/Non compensable | 1.00 (ref.) | <0.001 |
| Private/DVA | 1.41 (0.90,2.22) | ||
| TAC/Worksafe/Other compensable | 2.43 (1.54,3.83) | ||
| Fracture type | Proximal humerus readmission | 1.00 (ref.) | <0.001 |
| Shaft of humerus readmission | 2.81 (1.60,4.92) | ||
| Subtrochanteric readmission | 2.62 (1.31,5.26) | ||
| Shaft of femur readmission | 4.67 (2.91,7.50) | ||
| Distal femur readmission | 2.56 (1.47,4.45) | ||
| Shaft of tibia readmission | 3.39 (2.13,5.38) | ||
| Shaft of tibia and femur readmission | 0.20 (0.05,0.88) | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ekegren, C.L.; Edwards, E.R.; De Steiger, R.; Gabbe, B.J. Incidence, Costs and Predictors of Non-Union, Delayed Union and Mal-Union Following Long Bone Fracture. Int. J. Environ. Res. Public Health 2018, 15, 2845. https://doi.org/10.3390/ijerph15122845
Ekegren CL, Edwards ER, De Steiger R, Gabbe BJ. Incidence, Costs and Predictors of Non-Union, Delayed Union and Mal-Union Following Long Bone Fracture. International Journal of Environmental Research and Public Health. 2018; 15(12):2845. https://doi.org/10.3390/ijerph15122845
Chicago/Turabian StyleEkegren, Christina L., Elton R. Edwards, Richard De Steiger, and Belinda J. Gabbe. 2018. "Incidence, Costs and Predictors of Non-Union, Delayed Union and Mal-Union Following Long Bone Fracture" International Journal of Environmental Research and Public Health 15, no. 12: 2845. https://doi.org/10.3390/ijerph15122845
APA StyleEkegren, C. L., Edwards, E. R., De Steiger, R., & Gabbe, B. J. (2018). Incidence, Costs and Predictors of Non-Union, Delayed Union and Mal-Union Following Long Bone Fracture. International Journal of Environmental Research and Public Health, 15(12), 2845. https://doi.org/10.3390/ijerph15122845






