The Health Consequences of Social Mobility in Contemporary China
Abstract
1. Introduction
2. Data, Variables, and Methods
2.1. Data and Sample
2.2. Variables
2.3. Analytical Procedures
3. Results
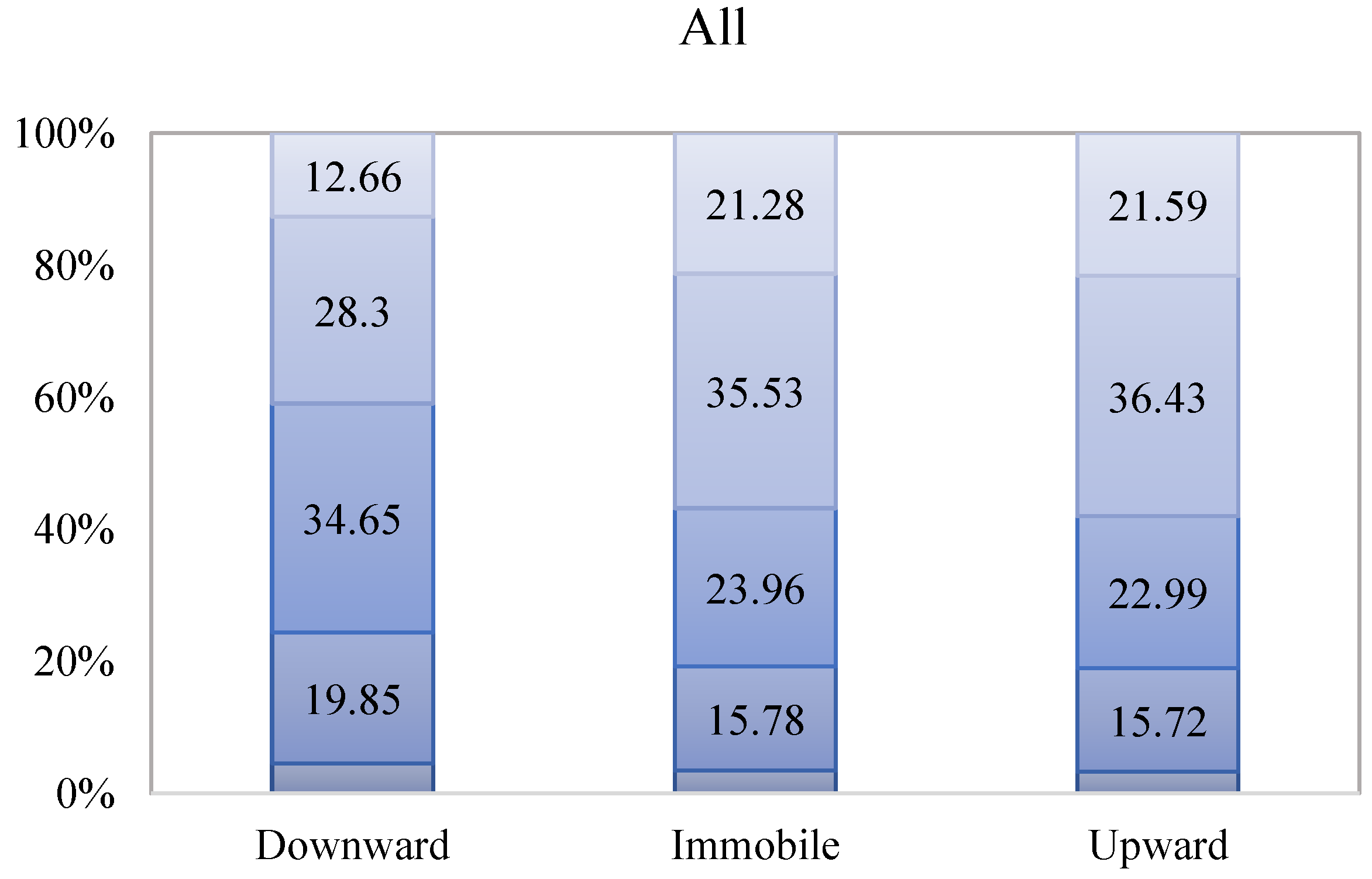
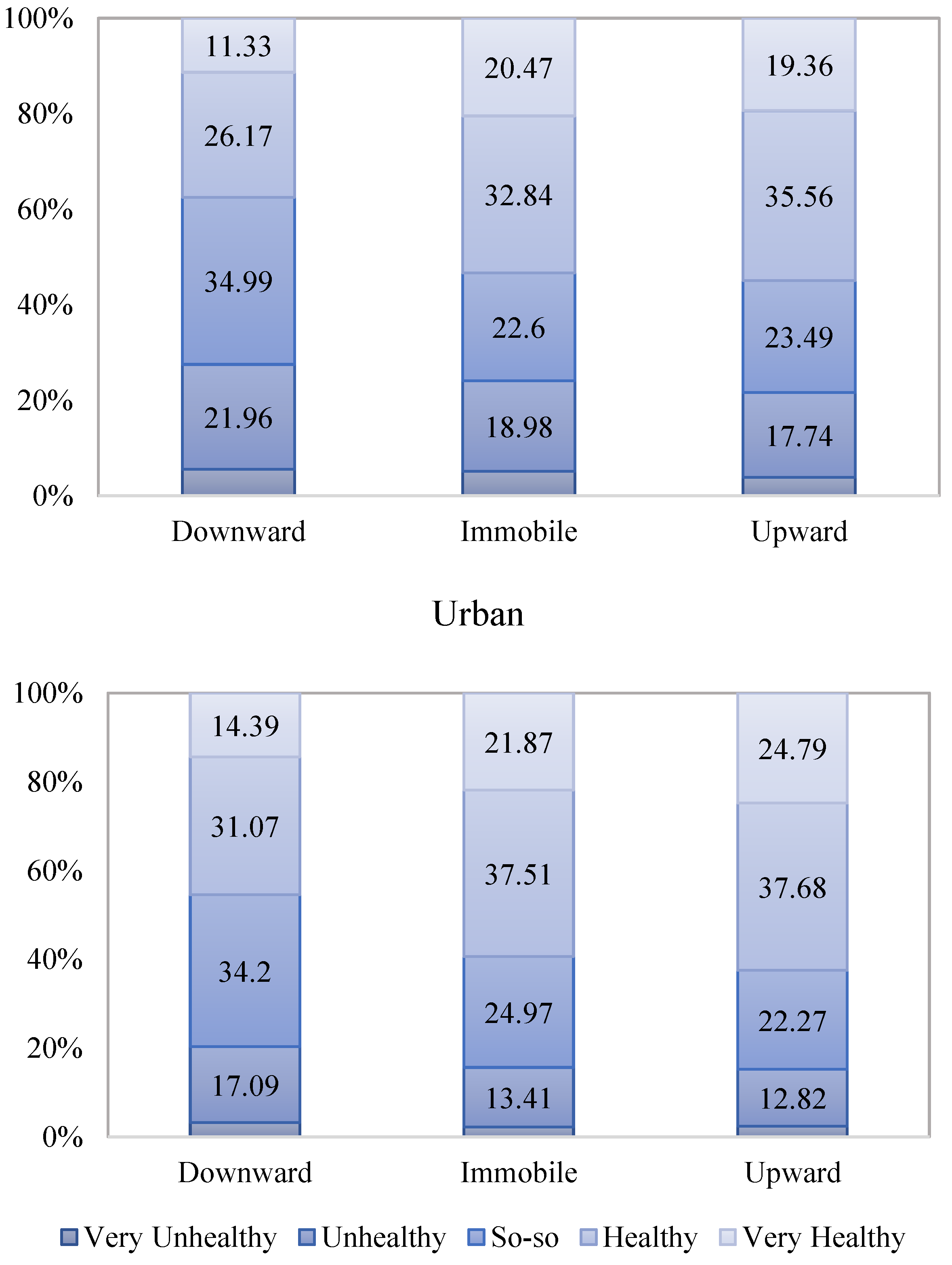
3.1. Distribution of Health Status
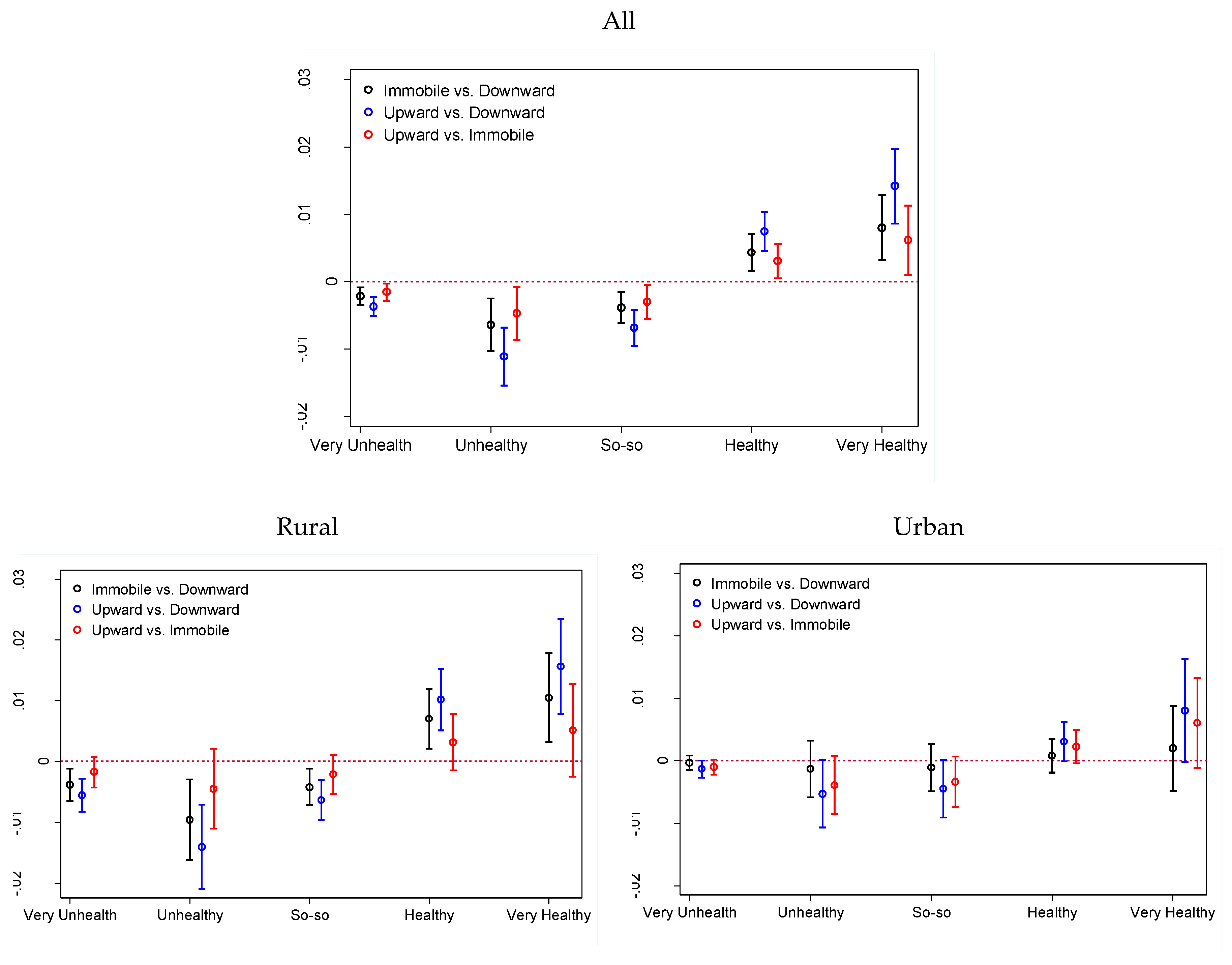
3.2. Individual-Level Analysis
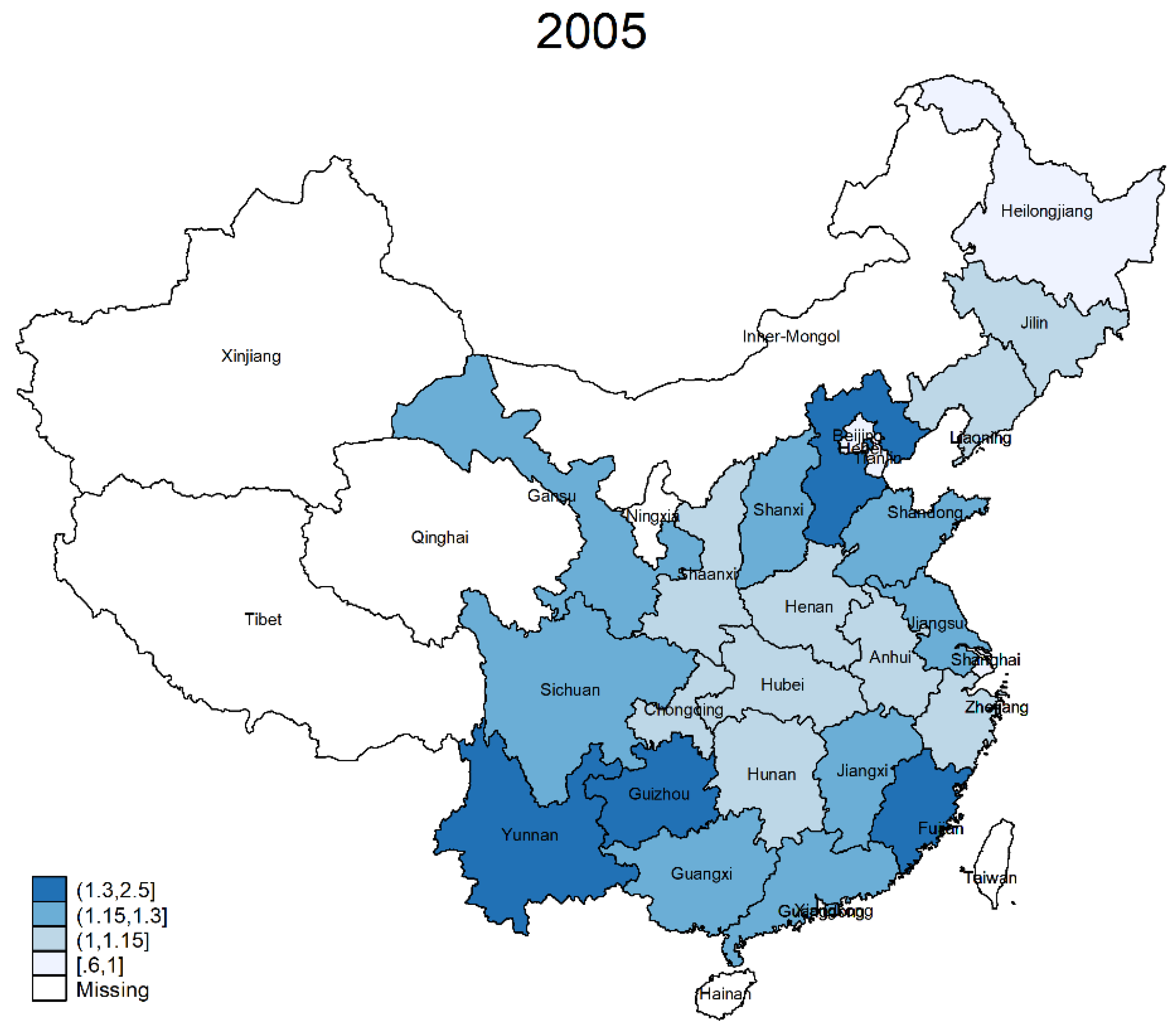
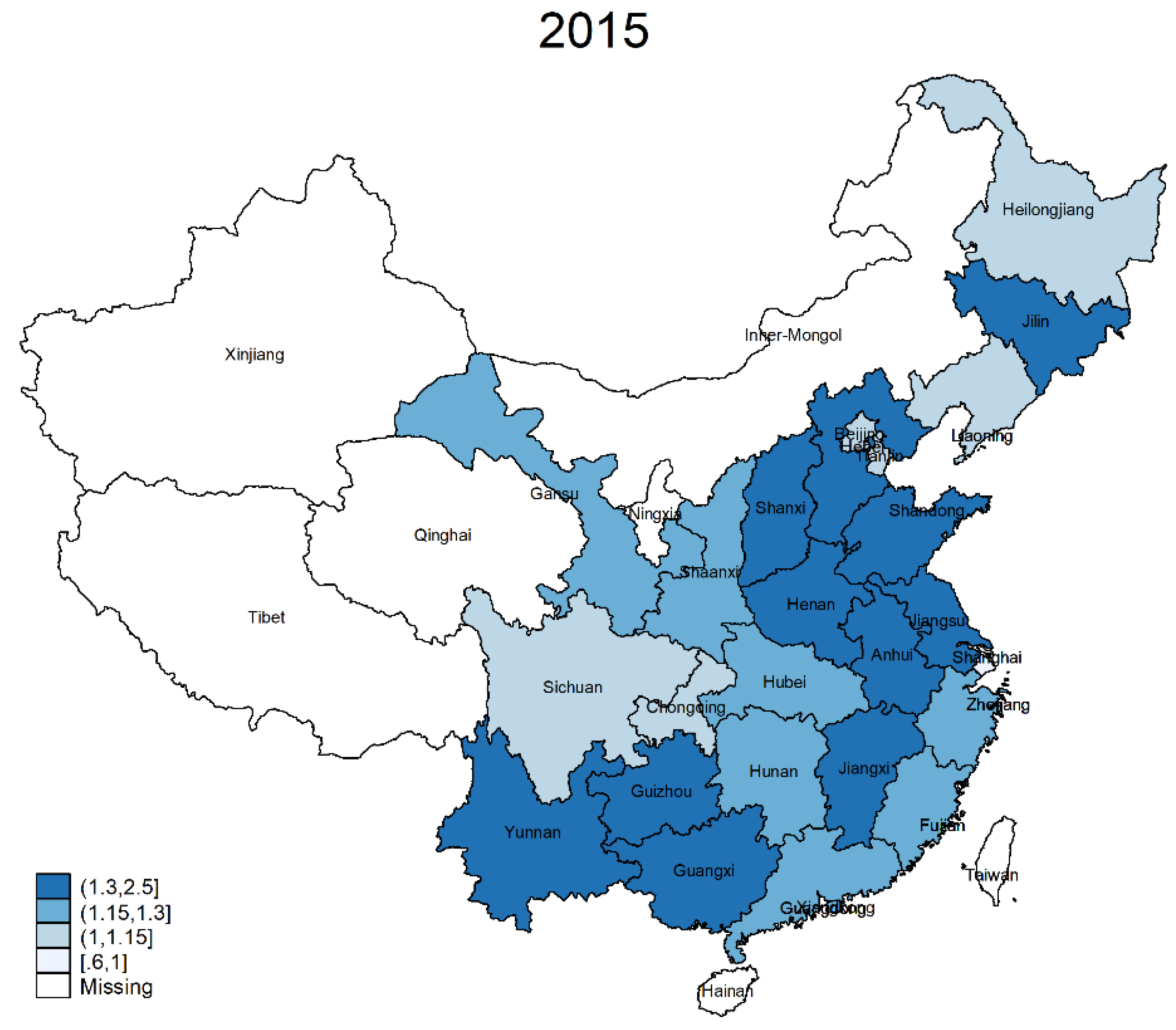
3.3. Provincial-Level Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Elliott, S.J. 50 years of medical health geography (ies) of health and wellbeing. Soc. Sci. Med. 2018, 196, 206–208. [Google Scholar] [CrossRef] [PubMed]
- Rosenberg, M. Health geography I: Social justice, idealist theory, health and health care. Prog. Hum. Geog. 2014, 38, 466–475. [Google Scholar] [CrossRef]
- Dorling, D. The mother of underlying causes—Economic ranking and health inequality. Soc. Sci. Med. 2015, 128, 327–330. [Google Scholar] [CrossRef] [PubMed]
- Simandan, D. Kinds of environments—A framework for reflecting on the possible contours of a better world. Can. Geogr. 2011, 55, 383–386. [Google Scholar] [CrossRef]
- Lundberg, O. Childhood living conditions, health status, and social mobility: A contribution to the health selection debate. Eur. Sociol. Rev. 1991, 7, 149–162. [Google Scholar] [CrossRef]
- Rodgers, B.; Mann, S.L. Re-thinking the analysis of intergenerational social mobility: A comment on John W. Fox’s social class, mental illness, and social mobility. J. Health Soc. Behav. 1993, 34, 165–172. [Google Scholar] [CrossRef] [PubMed]
- Wadsworth, M.E. Serious illness in childhood and its association with later-life achievement. In Class and Health: Research and Longitudinal Data; Wilkinson, R., Ed.; Tavistock Publications: London, UK, 1986; pp. 50–74. [Google Scholar]
- Wadsworth, M.E.J.; Kuh, D.J.L. Childhood influences on adult health: A review of recent work from the British 1846 national Birth cohort study, the RMC national survey of health and development. Pediatr. Perinat. Epidemiol. 1997, 11, 2–20. [Google Scholar] [CrossRef]
- Collins, J.W.; Rankin, K.M.; David, R.J. Downward economic mobility and preterm birth: An exploratory study of Chicago-born upper class white mothers. Matern. Child Health J. 2015, 19, 1601–1607. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.C.; Huang, N. Changes in self-perceived economic satisfaction and mortality at old ages: Evidence from a survey of middle-aged and elderly adults in Taiwan. Soc. Sci. Med. 2015, 130, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Bartley, M.; Plewis, I. Does health-selective mobility account for socioeconomic differences in health? Evidence from England and Wales, 1971 to 1991. J. Health Soc. Behav. 1997, 38, 376–386. [Google Scholar] [CrossRef] [PubMed]
- Bourdieu, P. Distinction: A Social Critique of the Judgment of Taste (Translated by Richard Nice); Harvard University Press: Cambridge, MA, USA, 1984. [Google Scholar]
- Simandan, D. Proximity, subjectivity, and space: Rethinking distance in human geography. Geoforum 2016, 75, 249–252. [Google Scholar] [CrossRef]
- Sorokin, P.A. Social and Cultural Mobility; The Free Press: New York, NY, USA, 1959. [Google Scholar]
- Dahl, E. Social mobility and health: Cause or effect? Brit. Med. J. 1996, 313, 435–436. [Google Scholar] [CrossRef] [PubMed]
- Hertz, T. Understanding Mobility in America; Center for American Progress Discussion Paper: Washington, DC, USA, 2006. [Google Scholar]
- Palloni, A. Reproducing inequalities: Luck, wallets, and the enduring effects of childhood health. Demography 2006, 43, 587–615. [Google Scholar] [CrossRef] [PubMed]
- Smith, J.P. Healthy bodies and thick wallets: The dual relation between health and economic status. J. Econ Perspect. 1999, 13, 145–166. [Google Scholar] [CrossRef]
- Currie, J.; Madrian, B.C. Health, health insurance and the labor market. Handb. Labor Econ. 1999, 3, 3309–3416. [Google Scholar]
- Mulatu, M.S.; Schooler, C. Causal connections between socio-economic status and health: Reciprocating effects and mediating mechanisms. J. Health Soc. Behav. 2002, 43, 22–41. [Google Scholar] [CrossRef] [PubMed]
- Miller, S.M. Comparative social mobility. Curr. Sociol. 1960, 9, 1–89. [Google Scholar] [CrossRef]
- Lipset, S.M.; Bendix, R. Social Mobility in Industrial Society; University of California Press: Berkeley, CA, USA, 1959. [Google Scholar]
- Wright, E.O.; Shin, K.Y. Temporality and class analysis: A comparative study of the effects of class trajectory and class structure on class consciousness in Sweden and the United States. Sociol. Thor. 1988, 6, 58–84. [Google Scholar] [CrossRef]
- Nieuwbeerta, P.; De Graaf, N.D.; Ultee, W. The effects of class mobility on class voting in post-war western industrialized countries. Eur. Sociol. Rev. 2000, 16, 327–348. [Google Scholar] [CrossRef]
- Clifford, P.; Heath, A. The political consequences of social mobility. J. R. Stat. Soc. Series B (Statistics in Society) 1993, 156, 51–61. [Google Scholar] [CrossRef]
- Simandan, D. Rethinking the health consequences of social class and social mobility. Soc. Sci. Med. 2018, 200, 258–261. [Google Scholar] [CrossRef] [PubMed]
- Reay, D.; Crozier, G.; Clayton, J. “Strangers in paradise?” Working-class students in elite universities. Sociology 2009, 43, 1103–1121. [Google Scholar] [CrossRef]
- Lehmann, W. Becoming middle class: How working-class university students draw and transgress moral class boundaries. Sociology 2009, 43, 631–647. [Google Scholar] [CrossRef]
- Norton, M.I. All ranks are local: Why humans are both (painfully) aware and (surprisingly) unaware of their lot in life. Psychol. Inq. 2013, 24, 124–125. [Google Scholar] [CrossRef]
- Cruces, G.; Perez-Truglia, R.; Tetaz, M. Biased perceptions of income distribution and preferences for redistribution: Evidence from a survey experiment. J. Public Econ. 2013, 98, 100–112. [Google Scholar] [CrossRef]
- Mishra, S.; Carleton, R.N. Subjective relative deprivation is associated with poorer physical and mental health. Soc. Sci. Med. 2015, 147, 144–149. [Google Scholar] [CrossRef] [PubMed]
- Bian, Y.J.; Li, L.L. The Chinese general social survey (2003–8): Sample designs and data evaluation. Chinese Sociol. Rev. 2012, 45, 70–97. [Google Scholar] [CrossRef]
- Jylhä, M. What is self-rated health and why does it predict mortality? Towards a unified conceptual model. Soc. Sci. Med. 2009, 69, 307–316. [Google Scholar] [CrossRef] [PubMed]
- Greene, W.H. Economic Analysis, 6th ed.; Prentice Hall: Upper Saddle River, NJ, USA, 2008. [Google Scholar]
- Cappellari, L. Earning mobility among Italian low-paid workers. J. Popul. Econ. 2007, 20, 465–482. [Google Scholar] [CrossRef]
- D’Addio, A.C.; Rosholm, M. Exits from temporary jobs in Europe: A competing risks analysis. Labour Econ. 2005, 12, 449–468. [Google Scholar] [CrossRef]
- Knabe, A.; Plum, A. Low-wage jobs-springboard to high-paid ones? Labour 2013, 27, 310–330. [Google Scholar] [CrossRef]
- Mood, C. Logistic regression: Why we cannot do what we think we can do, and what we can do about it. Eur. Sociol. Rev. 2010, 26, 67–82. [Google Scholar] [CrossRef]
- Bhurosy, T.; Jeewon, R. Overweight and obesity epidemic in developing countries: A problem with diet, physical activity, or socioeconomic status? Sci. World J. 2014, 964236. [Google Scholar] [CrossRef] [PubMed]
- Yatsuya, H.; Li, Y.; Hilawe, E.H.; Ota, A.; Wang, C.; Chiang, C.; Zhang, Y.; Uemura, M.; Osako, A.; Ozaki, Y.; et al. Global trend in overweight and obesity and its association with cardiovascular disease incidence. Circ. J. 2014, 78, 2807–2818. [Google Scholar] [CrossRef] [PubMed]
- Mirowsky, J.; Ross, C.E. Education and self-rated health: Cumulative advantage and its rising importance. Res. Aging 2008, 30, 93–122. [Google Scholar] [CrossRef]
- Zhang, W.; McCubbin, H.; McCubbin, L.; Chen, Q.; Foley, S.; Strom, I.; Kehl, L. Education and self-rated health: An individual and neighborhood level analysis of Asia Americans, Hawaiians, and Caucasians in Hawaii. Soc. Sci. Med. 2010, 70, 561–569. [Google Scholar] [CrossRef] [PubMed]
| Variable | Proportion (%) | Mean (SD) | |
|---|---|---|---|
| Dependent Variable | |||
| Health | Very Unhealthy = 1 | 3.75 | |
| Unhealthy = 2 | 17.05 | ||
| So-so = 3 | 26.94 | ||
| Healthy = 4 | 33.53 | ||
| Very Healthy = 5 | 18.72 | ||
| Independent Variable | |||
| Mobility | Downward = 1 | 30.26 | |
| Immobile = 2 | 44.79 | ||
| Upward =3 | 24.95 | ||
| Class | Lower = 1 | 20.37 | |
| Lower Middle = 2 | 31.43 | ||
| Middle = 3 | 41.46 | ||
| Upper Middle = 4 | 5.85 | ||
| Upper = 5 | 0.90 | ||
| Party Member | No = 0 | 89.13 | |
| Yes = 1 | 10.87 | ||
| Hukou | Rural = 0 | 50.99 | |
| Urban = 1 | 49.01 | ||
| Gender | Female = 0 | 51.10 | |
| Male = 1 | 48.90 | ||
| Marital Status | Married =1 | 86.23 | |
| Never Married = 2 | 5.74 | ||
| Divorced/Widowed = 3 | 8.03 | ||
| Work Status | Unemployed = 0 | 20.03 | |
| Employed = 1 | 61.92 | ||
| Retired = 2 | 18.05 | ||
| Wave | Year 2005 | 12.31 | |
| Year 2006 | 12.17 | ||
| Year 2008 | 12.67 | ||
| Year 2010 | 11.77 | ||
| Year 2011 | 11.99 | ||
| Year 2012 | 11.83 | ||
| Year 2013 | 13.62 | ||
| Year 2015 | 13.65 | ||
| Age (years old) | 45.93 (14.93) | ||
| Years of Schooling (years) | 8.40 (4.30) | ||
| Family Annual Income (RMB) | 41,608.78 (104,372.20) | ||
| Variable | Description | Mean | S.D. |
|---|---|---|---|
| Dependent Variable | |||
| Health | Average Self-Rated Health | 1.26 | 0.30 |
| Independent Variable | |||
| Class Mobility | Average Self-Perceived Mobility | 0.72 | 1.71 |
| Urbanization | Level of Urbanization | 0.42 | 0.16 |
| Class | Average Self-Perceived Class | 1.47 | 0.35 |
| Economic Development | GDP per capita (log value) | 0.17 | 0.59 |
| Economic Growth | GDP Annual Growth Rate (Log value) | 0.13 | 0.06 |
| Political Development | Percent of Party member | 0.11 | 0.05 |
| Social Development | Number of NGO Association (log value) | 1.10 | 0.46 |
| Inequality | Gini Coefficient (Household Income) | −0.78 | 0.18 |
| Marketization | Marketization Index | 1.85 | 0.25 |
| Labor Cost | Average Wage Level (Log value) | 10.30 | 0.80 |
| Education | College Students per 100,000 People (Log value) | 2.16 | 0.32 |
| Environment | PM10 | −2.31 | 0.26 |
| Medical Care Development | Number of Hospital Beds (log value) | −5.61 | 0.28 |
| Variables | Model 1 | Model 2 | Model 3 |
|---|---|---|---|
| Self-Rated Health | |||
| Immobile | 0.175 *** (0.019) | 0.073 *** (0.019) | 0.061 ** (0.019) |
| Upward | 0.309 *** (0.020) | 0.126 *** (0.021) | 0.107 *** (0.021) |
| Urban Residence | 0.123 *** (0.017) | ||
| Self-Rated Class (ref: Middle Class) | |||
| Lower | −0.755 *** (0.021) | −0.561 *** (0.021) | |
| Lower Middle | −0.366 *** (0.017) | −0.284 *** (0.017) | |
| Upper Middle | 0.163 *** (0.031) | 0.118 *** (0.032) | |
| Upper | 0.235 ** (0.080) | 0.447 *** (0.081) | |
| Age | −0.041 *** (0.001) | ||
| Male | 0.295 *** (0.015) | ||
| Party Member | 0.059 * (0.025) | ||
| Marital Status (ref: Married) | |||
| Never Married | 0.083 * (0.033) | ||
| Separated/Divorced/Widowed | −0.043 (0.030) | ||
| Work Status (ref: Employed) | |||
| Unemployed | −0.307 *** (0.021) | ||
| Retired | −0.099 *** (0.021) | ||
| Years of Schooling | 0.018 *** (0.002) | ||
| Logged Family Income | 0.139 *** (0.007) | ||
| Cut Point 1 | −3.630 *** (0.048) | −4.025 *** (0.050) | −4.278 *** (0.093) |
| Cut Point 2 | −1.645 *** (0.044) | −2.017 *** (0.046) | −2.146 *** (0.092) |
| Cut Point 3 | −0.275 *** (0.044) | −0.622 *** (0.045) | −0.615 *** (0.091) |
| Cut Point 4 | 1.417 *** (0.044) | 1.094 *** (0.046) | 1.275 *** (0.091) |
| N | 65,829 | 65,829 | 65,829 |
| Log-Likelihood | −91,928.407 | −91,118.680 | −86,318.460 |
| Variables | Rural | Urban | Sig |
|---|---|---|---|
| Self-rated Health | |||
| Immobile | 0.086 ** (0.030) | 0.014 (0.025) | * |
| Upward | 0.127 *** (0.032) | 0.057 † (0.030) | † |
| Self-Rated Class (ref: Middle Class) | |||
| Lower | −0.513 *** (0.033) | −0.630 *** (0.029) | |
| Lower Middle | −0.272 *** (0.028) | −0.304 *** (0.022) | |
| Upper Middle | 0.192 *** (0.055) | 0.067 † (0.038) | * |
| Upper | 0.697 *** (0.124) | 0.089 (0.109) | *** |
| Age | −0.039 *** (0.001) | −0.042 *** (0.001) | |
| male | 0.345 *** (0.024) | 0.214 *** (0.020) | *** |
| Party Member | 0.142 ** (0.048) | 0.071 * (0.028) | |
| Marital Status (ref: Married) | |||
| Never Married | 0.080 (0.053) | 0.057 (0.042) | † |
| Separated/Divorced/Widowed | −0.080 (0.052) | 0.013 (0.036) | |
| Work Status (ref: Employed) | |||
| Unemployed | −0.394 *** (0.037) | −0.316 *** (0.026) | * |
| Retired | −0.161 *** (0.041) | −0.158 *** (0.028) | |
| Years of Schooling | 0.030 *** (0.004) | 0.004 (0.003) | *** |
| Logged Familial Income | 0.168 *** (0.011) | 0.090 *** (0.010) | *** |
| Cut Point 1 | −3.003 *** (0.177) | −5.572 *** (0.129) | |
| Cut Point 2 | −0.927 *** (0.175) | −3.299 *** (0.126) | |
| Cut Point 3 | 0.516 ** (0.175) | −1.634 *** (0.125) | |
| Cut Point 4 | 2.341 *** (0.176) | 0.334 ** (0.124) | |
| N | 26,221 | 39,608 | |
| Log-Likelihood | −35,257.311 | −50,122.127 |
| Health | Immobile vs. Downward | Upward vs. Downward | Upward vs. Immobile |
|---|---|---|---|
| All | |||
| Very Unhealthy | −0.002 ** (0.001) | −0.004 *** (0.001) | −0.002 * (0.001) |
| Unhealthy | −0.006 ** (0.002) | −0.011 *** (0.002) | −0.005 * (0.002) |
| So-so | −0.004 ** (0.001) | −0.006 *** (0.001) | −0.003 * (0.001) |
| Healthy | 0.004 ** (0.001) | 0.007 *** (0.001) | 0.003 * (0.001) |
| Very Healthy | 0.008 ** (0.002) | 0.014 *** (0.003) | 0.006 * (0.003) |
| Rural | |||
| Very Unhealthy | −0.004 ** (0.001) | −0.006 *** (0.001) | −0.002 (0.001) |
| Unhealthy | −0.010 ** (0.003) | −0.014 *** (0.004) | −0.004 (0.003) |
| So-so | −0.004 ** (0.002) | −0.009 *** (0.002) | −0.002 (0.002) |
| Healthy | 0.007 ** (0.003) | 0.010 *** (0.002) | 0.003 (0.002) |
| Very Healthy | 0.011 ** (0.003) | 0.016 *** (0.004) | 0.005 (0.004) |
| Urban | |||
| Very Unhealthy | −0.000 (0.001) | −0.001 † (0.001) | −0.001 (0.001) |
| Unhealthy | −0.001 (0.002) | −0.005 † (0.003) | −0.004 (0.002) |
| So-so | −0.001 (0.002) | −0.004 † (0.002) | −0.003 (0.002) |
| Healthy | 0.001 (0.001) | 0.003 † (0.002) | 0.002 (0.001) |
| Very Healthy | 0.002 (0.003) | 0.008 † (0.004) | 0.006 (0.004) |
| Variables | OLS | RE | FE |
|---|---|---|---|
| Average Self-perceived Mobility | 0.167 *** (0.023) | 0.167 *** (0.023) | 0.156 *** (0.022) |
| Urbanization | −0.030 (0.075) | −0.030 (0.075) | −0.078 (0.071) |
| Average Subjective Social Class | 0.364 *** (0.060) | 0.364 *** (0.060) | 0.218 *** (0.061) |
| Political Party Structure | −0.327 * (0.162) | −0.327 * (0.162) | −0.503 ** (0.164) |
| GDP per capita (log value) | −0.064 * (0.029) | −0.064 * (0.029) | 0.053 (0.085) |
| GDP Annual Growth Rate (log value) | 0.035 (0.164) | 0.035 (0.164) | −0.256 (0.176) |
| Gini Index | −0.002 (0.030) | −0.002 (0.030) | 0.001 (0.030) |
| Marketization | 0.075 † (0.044) | 0.075 † (0.044) | 0.015 (0.081) |
| Average Wage Level (log value) | −0.026 (0.021) | −0.026 (0.021) | 0.032 (0.021) |
| Number of College Students (log value) | 0.313 *** (0.057) | 0.313 *** (0.057) | 0.337 *** (0.061) |
| PM10 | 0.023 (0.022) | 0.023 (0.022) | 0.020 (0.038) |
| Number of Hospital Bed (log value) | −0.033 (0.042) | −0.033 (0.042) | −0.092 (0.071) |
| NGO Association (log value) | 0.028 (0.022) | 0.028 (0.022) | 0.017 (0.041) |
| Constant | −0.300 (0.241) | −0.300 (0.241) | −0.783 † (0.402) |
| N | 200 | 200 | 200 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yan, F.; He, G.; Chen, Y. The Health Consequences of Social Mobility in Contemporary China. Int. J. Environ. Res. Public Health 2018, 15, 2644. https://doi.org/10.3390/ijerph15122644
Yan F, He G, Chen Y. The Health Consequences of Social Mobility in Contemporary China. International Journal of Environmental Research and Public Health. 2018; 15(12):2644. https://doi.org/10.3390/ijerph15122644
Chicago/Turabian StyleYan, Fei, Guangye He, and Yunsong Chen. 2018. "The Health Consequences of Social Mobility in Contemporary China" International Journal of Environmental Research and Public Health 15, no. 12: 2644. https://doi.org/10.3390/ijerph15122644
APA StyleYan, F., He, G., & Chen, Y. (2018). The Health Consequences of Social Mobility in Contemporary China. International Journal of Environmental Research and Public Health, 15(12), 2644. https://doi.org/10.3390/ijerph15122644






