Norovirus Outbreak Associated with Swimming in a Recreational Lake Not Influenced by External Human Fecal Sources in The Netherlands, August 2012
Abstract
1. Introduction
2. Materials and Methods
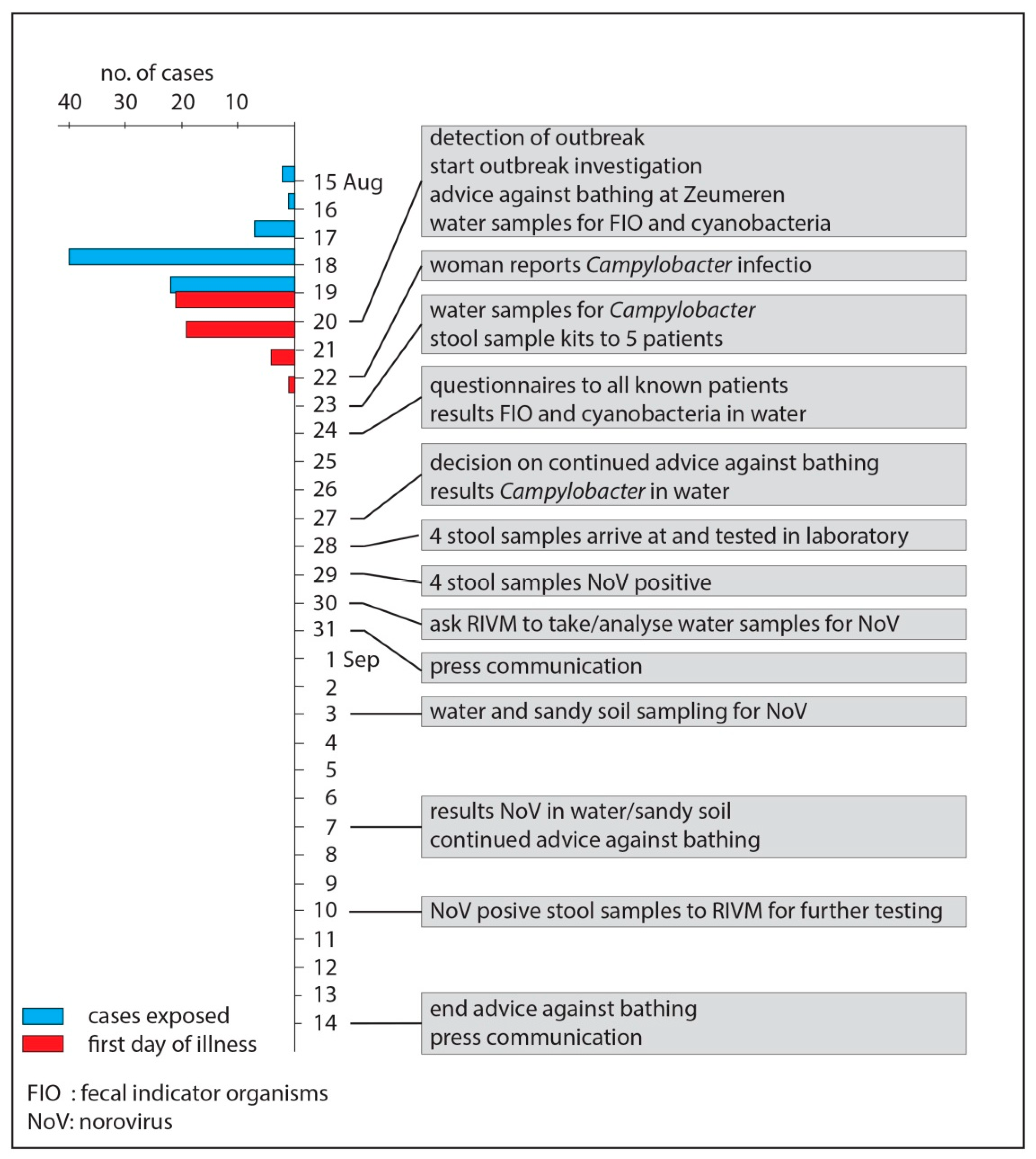
2.1. Outbreak Description
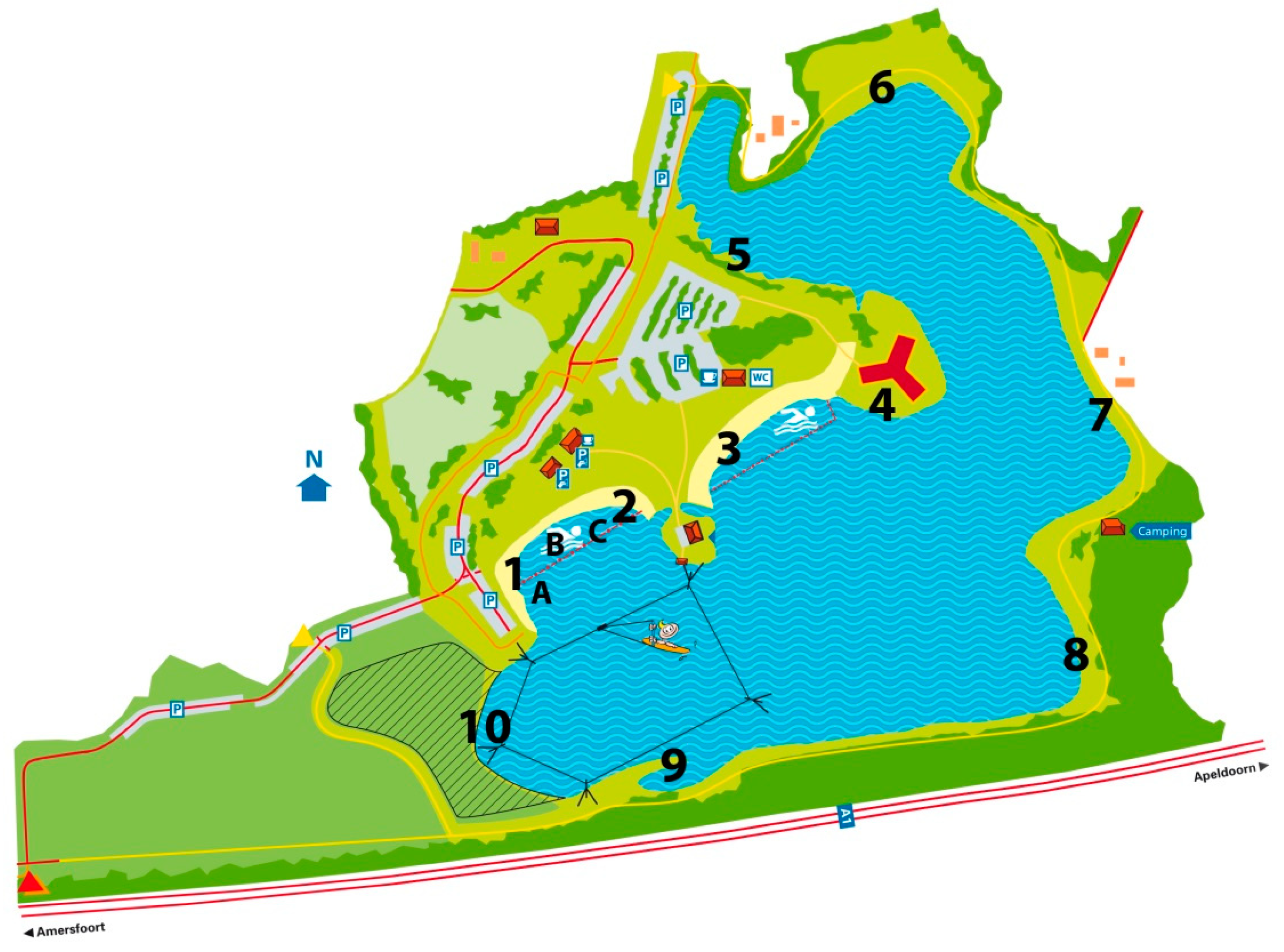
2.2. Site Description
2.3. Epidemiological Investigation
2.4. Microbiological Investigation of Clinical Samples
2.5. Environmental Investigation
3. Results
3.1. Epidemiological Investigation
3.2. Microbiological Investigation of Clinical Samples
3.3. Environmental Investigation
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Patel, M.M.; Hall, A.J.; Vinjé, J.; Parashar, U.D. Noroviruses: A comprehensive review. J. Clin. Virol. 2009, 44, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Teunis, P.F.M.; Moe, C.L.; Liu, P.; Miller, S.E.; Lindesmith, L.; Baric, R.S.; Le Pendu, J.; Calderon, R.L. Norwalk virus: How infectious is it? J. Med. Virol. 2008, 80, 1468–1476. [Google Scholar] [CrossRef] [PubMed]
- Atmar, R.L.; Opekum, A.R.; Gilger, M.A.; Estes, M.K.; Crawford, S.E.; Neill, F.H.; Graham, D.Y. Norwalk virus shedding after experimental human infection. Emerg. Infect. Dis. 2008, 14, 1553–1557. [Google Scholar] [CrossRef] [PubMed]
- Glass, R.I.; Parashar, U.D.; Estes, M.K. Norovirus gastroenteritis. N. Engl. J. Med. 2009, 361, 1776–1785. [Google Scholar] [CrossRef] [PubMed]
- Rockx, B.; De Wit, M.; Vennema, H.; Vinjé, J.; De Bruin, E.; Van Duynhoven, Y.; Koopmans, M. Natural history of human calicivirus infection: A prospective cohort study. Clin. Infect. Dis. 2002, 35, 246–253. [Google Scholar] [CrossRef] [PubMed]
- Zheng, D.P.; Ando, T.; Fankhauser, R.L.; Beard, R.S.; Glass, R.I.; Monroe, S.S. Norovirus classification and proposed strain nomenclature. Virology 2006, 346, 312–323. [Google Scholar] [CrossRef] [PubMed]
- Atmar, R.L.; Ramani, S.; Estes, M.K. Human noroviruses: recent advances in a 50-year history. Curr. Opin. Infect. Dis. 2018, 31, 422–432. [Google Scholar] [CrossRef] [PubMed]
- Matthews, J.E.; Dickey, B.W.; Miller, R.D.; Felzer, J.R.; Dawson, B.P.; Lee, A.S.; Rocks, J.J.; Kiel, J.; Montes, J.S.; Moe, C.L.; et al. The epidemiology of published norovirus outbreaks: A review of risk factors associated with attack rate and genogroup. Epidemiol. Infect. 2012, 140, 1161–1172. [Google Scholar] [CrossRef]
- Riera-Montes, M.; Sjölander, K.B.; Allestam, G.; Hallin, E.; Hedlund, K.O.; Löfdahl, M. Waterborne norovirus outbreak in a municipal drinking-water supply in Sweden. Epidemiol. Infect. 2011, 139, 1928–1935. [Google Scholar] [CrossRef] [PubMed]
- Ter Waarbeek, H.L.; Dukers-Muijrers, N.H.; Vennema, H.; Hoebe, C.J. Waterborne gastroenteritis outbreak at a scouting camp caused by two norovirus genogroups: GI and GII. J. Clin. Virol. 2010, 47, 268–272. [Google Scholar] [CrossRef] [PubMed]
- Cho, H.G.; Lee, S.G.; Kim, W.H.; Lee, J.S.; Park, P.H.; Cheon, D.S.; Jheong, W.H.; Jho, E.H.; Lee, J.B.; Paik, S.Y. Acute gastroenteritis outbreaks associated with ground-waterborne norovirus in South Korea during 2008–2012. Epidemiol. Infect. 2014, 142, 2604–2609. [Google Scholar] [CrossRef] [PubMed]
- Sinclair, R.G.; Jones, E.L.; Gerba, C.P. Viruses in recreational water-borne disease outbreaks: A review. J. Appl. Microbiol. 2009, 107, 1769–1780. [Google Scholar] [CrossRef] [PubMed]
- Hoebe, C.J.; Vennema, H.; De Roda Husman, A.M.; Van Duynhoven, Y.T. Norovirus outbreak among primary schoolchildren who had played in a recreational water fountain. J. Infect. Dis. 2004, 189, 699–705. [Google Scholar] [CrossRef] [PubMed]
- Podewils, L.J.; Zanardi Blevins, L.; Hagenbuch, M.; Itani, D.; Burns, A.; Otto, C.; Blanton, L.; Adams, A.; Monroe, S.S.; Beach, M.J.; et al. Outbreak of norovirus illness associated with a swimming pool. Epidemiol. Infect. 2007, 135, 827–833. [Google Scholar] [CrossRef] [PubMed]
- Zlot, A.; Simckes, M.; Vines, J.; Reynolds, L.; Sullivan, A.; Scott, M.K.; McLuckie, J.M.; Kromer, D.; Hill, V.R.; Yoder, J.S.; et al. Norovirus outbreak associated with a natural lake used for recreation–Oregon, 2014. Am. J. Transplant. 2015, 15, 2001–2005. [Google Scholar] [CrossRef] [PubMed]
- Polkowska, A.; Räsänen, S.; Al-Hello, H.; Bojang, M.; Lyytikäinen, O.; Nuorti, J.P.; Jalava, K. An outbreak of norovirus infections associated with recreational lake water in Western Finland, 2014. Epidemiol. Infect. 2018, 146, 544–550. [Google Scholar] [CrossRef] [PubMed]
- Kauppinen, A.; Al-Hello, H.; Zacheus, O.; Kilponen, J.; Maunula, L.; Huusko, S.; Lappalainen, M.; Miettinen, I.; Blomqvist, S.; Rimhanen-Finne, R. Increase in outbreaks of gastroenteritis linked to bathing water in Finland in summer 2014. Euro Surveill. 2017, 22, 30470. [Google Scholar] [CrossRef] [PubMed]
- The European Parliament and the Council of the European Union. Directive 2006/7/EC of the European Parliament and of the Council of 15 February 2006 concerning the management of bathing water quality and repealing Directive 76/160/EEC. Off. J. Europ. Union 2006, L64, 37–51. [Google Scholar]
- Verhaelen, K.; Bouwknegt, M.; Lodder-Verschoor, F.; Rutjes, S.A.; De Roda Husman, A.M. Persistence of human norovirus GII.4 and GI.4, murine norovirus, and human adenovirus on soft berries as compared with PBS at commonly applied storage conditions. Int. J. Food Microbiol. 2012, 160, 137–144. [Google Scholar] [CrossRef] [PubMed]
- Van Olphen, M.; Kapsenberg, J.G.; Van de Baan, E.; Kroon, W.A. Removal of enteric viruses from surface water at eight waterworks in The Netherlands. Appl. Environ. Microbiol. 1984, 47, 927–932. [Google Scholar] [PubMed]
- Rutjes, S.A.; Italiaander, R.; Van den Berg, H.H.; Lodder, W.J.; De Roda Husman, A.M. Isolation and detection of enterovirus RNA from large-volume water samples by using the NucliSens miniMAG system and real-time nucleic acid sequence-based amplification. Appl. Environ. Microbiol. 2005, 71, 3734–3740. [Google Scholar] [CrossRef] [PubMed]
- Skraber, S.; Schijven, J.; Italiaander, R.; De Roda Husman, A.M. Accumulation of enteric bacteriophage in fresh water sediments. J. Water Health 2009, 7, 372–379. [Google Scholar] [CrossRef] [PubMed]
- Schets, F.M.; De Roda Husman, A.M.; Havelaar, A.H. Disease outbreaks associated with untreated recreational water use. Epidemiol. Infect. 2011, 139, 1114–1125. [Google Scholar] [CrossRef] [PubMed]
- Bitler, E.J.; Matthews, J.E.; Dickey, B.W.; Eisenberg, J.N.; Leon, J.S. Norovirus outbreaks: a systematic review of commonly implicated transmission routes and vehicles. Epidemiol. Infect. 2013, 141, 1563–1571. [Google Scholar] [CrossRef] [PubMed]
- Wyn-Jones, A.P.; Carducci, A.; Cook, N.; D’Agostino, M.; Divizia, M.; Fleischer, J.; Gantzer, C.; Gawler, A.; Girones, R.; Höller, C.; et al. Surveillance of adenoviruses and noroviruses in European recreational waters. Water Res. 2011, 45, 1025–1038. [Google Scholar] [CrossRef] [PubMed]
- Schets, F.M.; Schijven, J.F.; De Roda Husman, A.M. Exposure assessment for swimmers in bathing waters and swimming pools. Water Res. 2011, 45, 2392–2400. [Google Scholar] [CrossRef] [PubMed]
- DeFlorio-Barker, S.; Arnold, B.F.; Sams, E.A.; Dufour, A.P.; Colford, J.M., Jr.; Weisberg, S.B.; Schiff, K.C.; Wade, T.J. 2017 Child environmental exposures to water and sand at the beach: Findings from studies of over 68,000 subjects at 12 beaches. J. Expo. Sci. Environ. Epidemiol. 2017, 28, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Arnold, B.F.; Wade, T.J.; Benjamin-Chung, J.; Schiff, K.C.; Griffith, J.F.; Dufour, A.P.; Weisberg, S.B.; Colford, J.M., Jr. Acute gastroenteritis and recreational water: highest burden among young US children. Am. J. Public Health 2016, 106, 1690–1697. [Google Scholar] [CrossRef] [PubMed]
- Teunis, P.F.; Sukhrie, F.H.; Vennema, H.; Bogerman, J.; Beersma, M.F.; Koopmans, M.P. Shedding of norovirus in symptomatic and asymptomatic infections. Epidemiol. Infect. 2015, 143, 1710–1717. [Google Scholar] [CrossRef] [PubMed]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schets, F.M.; Van den Berg, H.H.J.L.; Vennema, H.; Pelgrim, M.T.M.; Collé, C.; Rutjes, S.A.; Lodder, W.J. Norovirus Outbreak Associated with Swimming in a Recreational Lake Not Influenced by External Human Fecal Sources in The Netherlands, August 2012. Int. J. Environ. Res. Public Health 2018, 15, 2550. https://doi.org/10.3390/ijerph15112550
Schets FM, Van den Berg HHJL, Vennema H, Pelgrim MTM, Collé C, Rutjes SA, Lodder WJ. Norovirus Outbreak Associated with Swimming in a Recreational Lake Not Influenced by External Human Fecal Sources in The Netherlands, August 2012. International Journal of Environmental Research and Public Health. 2018; 15(11):2550. https://doi.org/10.3390/ijerph15112550
Chicago/Turabian StyleSchets, Franciska M., Harold H. J. L. Van den Berg, Harry Vennema, Manon T. M. Pelgrim, Cees Collé, Saskia A. Rutjes, and Willemijn J. Lodder. 2018. "Norovirus Outbreak Associated with Swimming in a Recreational Lake Not Influenced by External Human Fecal Sources in The Netherlands, August 2012" International Journal of Environmental Research and Public Health 15, no. 11: 2550. https://doi.org/10.3390/ijerph15112550
APA StyleSchets, F. M., Van den Berg, H. H. J. L., Vennema, H., Pelgrim, M. T. M., Collé, C., Rutjes, S. A., & Lodder, W. J. (2018). Norovirus Outbreak Associated with Swimming in a Recreational Lake Not Influenced by External Human Fecal Sources in The Netherlands, August 2012. International Journal of Environmental Research and Public Health, 15(11), 2550. https://doi.org/10.3390/ijerph15112550