Vitamin D Status and Analysis of Specific Correlates in Preschool Children: A Cross-Sectional Study in Southern Croatia
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Variables
2.3. Statistics
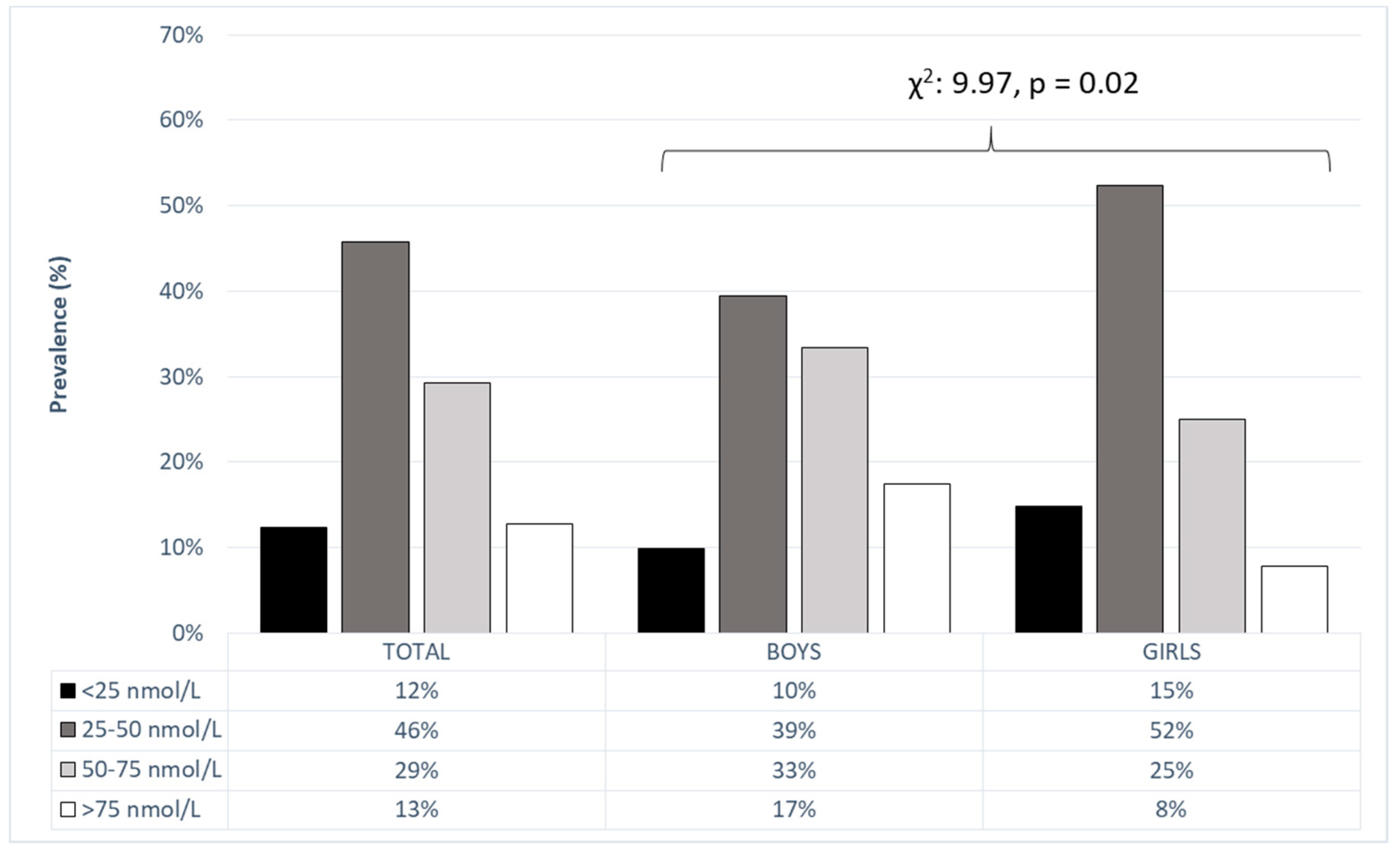
3. Results
4. Discussion
4.1. 25(OH)D Level in Croatian Preschool Children
4.2. Gender Differences in the 25(OH)D and Physical Activity Levels
4.3. Lack of Association of Body Mass Index, Physical Activity and Time Spent Outdoors with 25(OH)D Levels
4.4. Limitations and Strengths
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Dobnig, H. A review of the health consequences of the vitamin D deficiency pandemic. J. Neurol. Sci. 2011, 311, 15–18. [Google Scholar] [CrossRef] [PubMed]
- Prentice, A.; Schoenmakers, I.; Jones, K.S.; Jarjou, L.M.; Goldberg, G.R. Vitamin D Deficiency and Its Health Consequences in Africa. Clin. Rev. Bone Miner. Metab. 2009, 7, 94–106. [Google Scholar] [CrossRef] [PubMed]
- Norval, M.; Coussens, A.K.; Wilkinson, R.J.; Bornman, L.; Lucas, R.M.; Wright, C.Y. Vitamin D Status and Its Consequences for Health in South Africa. Int. J. Environ. Res. Public Health 2016, 13, 1019. [Google Scholar] [CrossRef] [PubMed]
- Kheiri, B.; Abdalla, A.; Osman, M.; Ahmed, S.; Hassan, M.; Bachuwa, G. Vitamin D deficiency and risk of cardiovascular diseases: A narrative review. Clin. Hypertens. 2018, 24, 9. [Google Scholar] [CrossRef] [PubMed]
- Mpandzou, G.; Ait Ben Haddou, E.; Regragui, W.; Benomar, A.; Yahyaoui, M. Vitamin D deficiency and its role in neurological conditions: A review. Rev. Neurol. 2016, 172, 109–122. [Google Scholar] [CrossRef] [PubMed]
- Misra, M.; Pacaud, D.; Petryk, A.; Collett-Solberg, P.F.; Kappy, M.; Drug and Therapeutics Committee of the Lawson Wilkins Pediatric Endocrine Society. Vitamin D deficiency in children and its management: Review of current knowledge and recommendations. Pediatrics 2008, 122, 398–417. [Google Scholar] [CrossRef] [PubMed]
- Yeum, K.J.; Song, B.C.; Joo, N.S. Impact of Geographic Location on Vitamin D Status and Bone Mineral Density. Int. J. Environ. Res. Public Health 2016, 13, 184. [Google Scholar] [CrossRef] [PubMed]
- Alaklabi, A.M.; Alsharairi, N.A. Current Evidence on Vitamin D Deficiency and Metabolic Syndrome in Obese Children: What Does the Evidence from Saudi Arabia Tell Us? Children 2018, 5, 11. [Google Scholar] [CrossRef] [PubMed]
- Al-Othman, A.; Al-Musharaf, S.; Al-Daghri, N.M.; Krishnaswamy, S.; Yusuf, D.S.; Alkharfy, K.M.; Al-Saleh, Y.; Al-Attas, O.S.; Alokail, M.S.; Moharram, O.; et al. Effect of physical activity and sun exposure on vitamin D status of Saudi children and adolescents. BMC Pediatr. 2012, 12, 92. [Google Scholar] [CrossRef] [PubMed]
- Bjarnadottir, A.; Kristjansdottir, A.G.; Hrafnkelsson, H.; Johannsson, E.; Magnusson, K.T.; Thorsdottir, I. Insufficient autumn vitamin D intake and low vitamin D status in 7-year-old Icelandic children. Public Health Nutr. 2015, 18, 208–217. [Google Scholar] [CrossRef] [PubMed]
- Esmaeili Dooki, M.R.; Moslemi, L.; Moghadamnia, A.A.; Alijanpour Aghamaleki, M.; Bijani, A.; Pornasrollah, M.; Ashrafianamiri, H. Vitamin D status in preschool children: Should vitamin D supplementation, preventing vitamin D deficiency be continued in children over 2 years? J. Public Health 2018, fdy147. [Google Scholar] [CrossRef] [PubMed]
- Flores, A.; Flores, M.; Macias, N.; Hernández-Barrera, L.; Rivera, M.; Contreras, A.; Villalpando, S. Vitamin D deficiency is common and is associated with overweight in Mexican children aged 1–11 years. Public Health Nutr. 2017, 20, 1807–1815. [Google Scholar] [CrossRef] [PubMed]
- Wakayo, T.; Whiting, S.J.; Belachew, T. Vitamin D Deficiency is Associated with Overweight and/or Obesity among Schoolchildren in Central Ethiopia: A Cross-Sectional Study. Nutrients 2016, 8, 190. [Google Scholar] [CrossRef] [PubMed]
- Zadka, K.; Palkowska-Gozdzik, E.; Rosolowska-Huszcz, D. The State of Knowledge about Nutrition Sources of Vitamin D, Its Role in the Human Body, and Necessity of Supplementation among Parents in Central Poland. Int. J. Environ. Res. Public Health 2018, 15, 1489. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, A.C.M.; Cureau, F.V.; de Oliveira, C.L.; Giannini, D.T.; Bloch, K.V.; Kuschnir, M.C.C.; Dutra, E.S.; Schaan, B.D.; de Carvalho, K.M.B. Physical activity but not sedentary time is associated with vitamin D status in adolescents: Study of cardiovascular risk in adolescents (ERICA). Eur. J. Clin. Nutr. 2018. [Google Scholar] [CrossRef] [PubMed]
- Mortensen, C.; Molgaard, C.; Hauger, H.; Kristensen, M.; Damsgaard, C.T. Sun behaviour and physical activity associated with autumn vitamin D status in 4–8-year-old Danish children. Public Health Nutr. 2018, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Saki, F.; Dabbaghmanesh, M.H.; Omrani, G.R.; Bakhshayeshkaram, M. Vitamin D deficiency and its associated risk factors in children and adolescents in southern Iran. Public Health Nutr. 2017, 20, 1851–1856. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, M.R.; Barreto, W.D.R.J. Association between physical activity and vitamin D: A narrative literature review. Rev. Assoc. Med. Bras. 2017, 63, 550–556. [Google Scholar] [CrossRef] [PubMed]
- Brown, H.E.; Pearson, N.; Braithwaite, R.E.; Brown, W.J.; Biddle, S.J. Physical activity interventions and depression in children and adolescents: A systematic review and meta-analysis. Sports Med. 2013, 43, 195–206. [Google Scholar] [CrossRef] [PubMed]
- Warburton, D.E.R.; Bredin, S.S.D. Health benefits of physical activity: A systematic review of current systematic reviews. Curr. Opin. Cardiol. 2017, 32, 541–556. [Google Scholar] [CrossRef] [PubMed]
- Scragg, R.K.; Camargo, C.A., Jr.; Simpson, R.U. Relation of serum 25-hydroxyvitamin D to heart rate and cardiac work (from the National Health and Nutrition Examination Surveys). Am. J. Cardiol. 2010, 105, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Millen, A.E.; Wactawski-Wende, J.; Pettinger, M.; Melamed, M.L.; Tylavsky, F.A.; Liu, S.; Robbins, J.; LaCroix, A.Z.; LeBoff, M.S.; Jackson, R.D. Predictors of serum 25-hydroxyvitamin D concentrations among postmenopausal women: The Women’s Health Initiative Calcium plus Vitamin D clinical trial. Am. J. Clin. Nutr. 2010, 91, 1324–1335. [Google Scholar] [CrossRef] [PubMed]
- Kluczynski, M.A.; Lamonte, M.J.; Mares, J.A.; Wactawski-Wende, J.; Smith, A.W.; Engelman, C.D.; Andrews, C.A.; Snetselaar, L.G.; Sarto, G.E.; Millen, A.E. Duration of physical activity and serum 25-hydroxyvitamin D status of postmenopausal women. Ann. Epidemiol. 2011, 21, 440–449. [Google Scholar] [CrossRef] [PubMed]
- Tseng, M.; Giri, V.; Bruner, D.W.; Giovannucci, E. Prevalence and correlates of vitamin D status in African American men. BMC Public Health 2009, 9, 191. [Google Scholar] [CrossRef] [PubMed]
- Bidzan-Bluma, I.; Lipowska, M. Physical Activity and Cognitive Functioning of Children: A Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 800. [Google Scholar] [CrossRef] [PubMed]
- Czyz, S.H.; Toriola, A.L.; Starosciak, W.; Lewandowski, M.; Paul, Y.; Oyeyemi, A.L. Physical Fitness, Physical Activity, Sedentary Behavior, or Diet—What Are the Correlates of Obesity in Polish School Children? Int. J. Environ. Res. Public Health 2017, 14, 664. [Google Scholar] [CrossRef] [PubMed]
- Maalouf, J.; Nabulsi, M.; Vieth, R.; Kimball, S.; El-Rassi, R.; Mahfoud, Z.; El-Hajj Fuleihan, G. Short- and long-term safety of weekly high-dose vitamin D3 supplementation in school children. J. Clin. Endocrinol. Metab. 2008, 93, 2693–2701. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.A.; Dalskov, S.M.; Sorensen, L.B.; Hjorth, M.F.; Andersen, R.; Tetens, I.; Krarup, H.; Ritz, C.; Astrup, A.; Michaelsen, K.F.; et al. Vitamin D status is associated with cardiometabolic markers in 8–11-year-old children, independently of body fat and physical activity. Br. J. Nutr. 2015, 114, 1647–1655. [Google Scholar] [CrossRef] [PubMed]
- Lammle, L.; Bergmann, K.; Bos, K.; Koletzko, B. Predictors of differences in vitamin D levels in children and adolescents and their relation to endurance performance. Ann. Nutr. Metab. 2013, 62, 55–62. [Google Scholar] [CrossRef] [PubMed]
- Absoud, M.; Cummins, C.; Lim, M.J.; Wassmer, E.; Shaw, N. Prevalence and predictors of vitamin D insufficiency in children: A Great Britain population based study. PLoS ONE 2011, 6, e22179. [Google Scholar] [CrossRef] [PubMed]
- Dong, Y.; Pollock, N.; Stallmann-Jorgensen, I.S.; Gutin, B.; Lan, L.; Chen, T.C.; Keeton, D.; Petty, K.; Holick, M.F.; Zhu, H. Low 25-hydroxyvitamin D levels in adolescents: Race, season, adiposity, physical activity, and fitness. Pediatrics 2010, 125, 1104–1111. [Google Scholar] [CrossRef] [PubMed]
- Grazio, S.; Naglic, D.B.; Anic, B.; Grubisic, F.; Bobek, D.; Bakula, M.; Kavanagh, H.S.; Kuna, A.T.; Cvijetic, S. Vitamin D serum level, disease activity and functional ability in different rheumatic patients. Am. J. Med. Sci. 2015, 349, 46–49. [Google Scholar] [CrossRef] [PubMed]
- Laktasic-Zerjavic, N.; Korsic, M.; Crncevic-Orlic, Z.; Kovac, Z.; Polasek, O.; Soldo-Juresa, D. Vitamin D status, dependence on age, and seasonal variations in the concentration of vitamin D in Croatian postmenopausal women initially screened for osteoporosis. Clin. Rheumatol. 2010, 29, 861–867. [Google Scholar] [CrossRef] [PubMed]
- Boraska, V.; Skrabic, V.; Zeggini, E.; Groves, C.J.; Buljubasic, M.; Peruzovic, M.; Zemunik, T. Family-based analysis of vitamin D receptor gene polymorphisms and type 1 diabetes in the population of South Croatia. J. Hum. Genet. 2008, 53, 210–214. [Google Scholar] [CrossRef] [PubMed]
- Zemunik, T.; Skrabic, V.; Boraska, V.; Diklic, D.; Terzic, I.M.; Capkun, V.; Peruzovic, M.; Terzic, J. FokI polymorphism, vitamin D receptor, and interleukin-1 receptor haplotypes are associated with type 1 diabetes in the Dalmatian population. J. Mol. Diagn. 2005, 7, 600–604. [Google Scholar] [CrossRef]
- Vranesic Bender, D.; Giljevic, Z.; Kusec, V.; Laktasic Zerjavic, N.; Bosnjak Pasic, M.; Vrdoljak, E.; Lkinas Kelecic, D.; Reiner, Z.; Anic, B.; Krznaric, Z. Guidelines for the Prevention, Detection and Therapy of Vitamin D Deficiency in Adults. Lijec. Vjesn. 2016, 138, 121–132. [Google Scholar] [PubMed]
- Sokolovic, S.; Alimanovic-Alagic, R.; Dzananovic, L.; Cavaljuga, S.; Beslic, N.; Ferhatbegovic-Opankovic, E. Vitamin D status in Bosnia and Herzegovina: The cross-sectional epidemiological analysis. Osteoporos. Int. 2017, 28, 1021–1025. [Google Scholar] [CrossRef] [PubMed]
- Dovnik, A.; Mujezinovic, F.; Treiber, M.; Pecovnik Balon, B.; Gorenjak, M.; Maver, U.; Takac, I. Determinants of maternal vitamin D concentrations in Slovenia: A prospective observational study. Wiener Klinische Wochenschr. 2017, 129, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Stokic, E.; Kupusinac, A.; Tomic-Naglic, D.; Zavisic, B.K.; Mitrovic, M.; Smiljenic, D.; Soskic, S.; Isenovic, E. Obesity and vitamin D deficiency: Trends to promote a more proatherogenic cardiometabolic risk profile. Angiology 2015, 66, 237–243. [Google Scholar] [CrossRef] [PubMed]
- Sempos, C.T.; Vesper, H.W.; Phinney, K.W.; Thienpont, L.M.; Coates, P.M.; Vitamin, D.S.P. Vitamin D status as an international issue: National surveys and the problem of standardization. Scand. J. Clin. Lab. Investig. 2012, 243, 32–40. [Google Scholar] [CrossRef]
- Thienpont, L.M.; Stepman, H.C.; Vesper, H.W. Standardization of measurements of 25-hydroxyvitamin D3 and D2. Scand. J. Clin. Lab. Investig. 2012, 243, 41–49. [Google Scholar] [CrossRef]
- Franca Gois, P.H.; Wolley, M.; Ranganathan, D.; Seguro, A.C. Vitamin D Deficiency in Chronic Kidney Disease: Recent Evidence and Controversies. Int. J. Environ. Res. Public Health 2018, 15, 1773. [Google Scholar] [CrossRef] [PubMed]
- Mansbach, J.M.; Ginde, A.A.; Camargo, C.A., Jr. Serum 25-hydroxyvitamin D levels among US children aged 1 to 11 years: Do children need more vitamin D? Pediatrics 2009, 124, 1404–1410. [Google Scholar] [CrossRef] [PubMed]
- Kondric, M.; Trajkovski, B.; Strbad, M.; Foretic, N.; Zenic, N. Anthropometric influence on physical fitness among preschool children: Gender-specific linear and curvilinear regression models. Coll. Antropol. 2013, 37, 1245–1252. [Google Scholar] [PubMed]
- Dwyer, G.M.; Hardy, L.L.; Peat, J.K.; Baur, L.A. The validity and reliability of a home environment preschool-age physical activity questionnaire (Pre-PAQ). Int. J. Behav. Nutr. Phys. Act. 2011, 8, 86. [Google Scholar] [CrossRef] [PubMed]
- Vollmer, R.L.; Adamsons, K.; Gorin, A.; Foster, J.S.; Mobley, A.R. Investigating the Relationship of Body Mass Index, Diet Quality, and Physical Activity Level between Fathers and Their Preschool-Aged Children. J. Acad. Nutr. Diet. 2015, 115, 919–926. [Google Scholar] [CrossRef] [PubMed]
- Skouteris, H.; Hill, B.; McCabe, M.; Swinburn, B.; Busija, L. A parent-based intervention to promote healthy eating and active behaviours in pre-school children: Evaluation of the MEND 2-4 randomized controlled trial. Pediatr. Obes. 2016, 11, 4–10. [Google Scholar] [CrossRef] [PubMed]
- Dwyer, G.M.; Walker, K.; Baur, L.; Badawi, N. Developmental outcomes and physical activity behaviour in children post major surgery: An observational study. BMC Pediatr. 2016, 16, 123. [Google Scholar] [CrossRef] [PubMed]
- Akeson, P.K.; Lind, T.; Hernell, O.; Silfverdal, S.A.; Ohlund, I. Serum Vitamin D Depends Less on Latitude Than on Skin Color and Dietary Intake During Early Winter in Northern Europe. J. Pediatr. Gastroenterol. Nutr. 2016, 62, 643–649. [Google Scholar] [CrossRef] [PubMed]
- Katic, M.; Pirsl, F.; Steinberg, S.M.; Dobbin, M.; Curtis, L.M.; Pulanic, D.; Desnica, L.; Titarenko, I.; Pavletic, S.Z. Vitamin D levels and their associations with survival and major disease outcomes in a large cohort of patients with chronic graft-vs-host disease. Croat. Med. J. 2016, 57, 276–286. [Google Scholar] [CrossRef] [PubMed]
- Culic, S.; Markic, J.; Petrovic, D.; Konjevoda, P.; Pavelic, J. Serum vitamin D levels in children with newly diagnosed and chronic immune thrombocytopenia. Semin. Hematol. 2016, 53 (Suppl. 1), S67–S69. [Google Scholar] [CrossRef]
- Zhu, Z.; Zhan, J.; Shao, J.; Chen, W.; Chen, L.; Li, W.; Ji, C.; Zhao, Z. High prevalence of vitamin D deficiency among children aged 1 month to 16 years in Hangzhou, China. BMC Public Health 2012, 12, 126. [Google Scholar] [CrossRef] [PubMed]
- Sanghera, D.K.; Sapkota, B.R.; Aston, C.E.; Blackett, P.R. Vitamin D Status, Gender Differences, and Cardiometabolic Health Disparities. Ann. Nutr. Metab. 2017, 70, 79–87. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Xiao, J.; Liao, X.; Cai, L.; Xu, F.; Chen, D.; Xiang, J.; Fang, R. Vitamin D Status among Young Children Aged 1–3 Years: A Cross-Sectional Study in Wuxi, China. PLoS ONE 2015, 10, e0141595. [Google Scholar] [CrossRef] [PubMed]
- Mandlik, R.; Kajale, N.; Ekbote, V.; Patwardhan, V.; Khadilkar, V.; Chiplonkar, S.; Khadilkar, A. Determinants of Vitamin D Status in Indian School-children. Indian J. Endocrinol. Metab. 2018, 22, 244–248. [Google Scholar] [CrossRef] [PubMed]
- Soininen, S.; Eloranta, A.M.; Lindi, V.; Venalainen, T.; Zaproudina, N.; Mahonen, A.; Lakka, T.A. Determinants of serum 25-hydroxyvitamin D concentration in Finnish children: The Physical Activity and Nutrition in Children (PANIC) study. Br. J. Nutr. 2016, 115, 1080–1091. [Google Scholar] [CrossRef] [PubMed]
- Pate, R.R.; Pfeiffer, K.A.; Trost, S.G.; Ziegler, P.; Dowda, M. Physical activity among children attending preschools. Pediatrics 2004, 114, 1258–1263. [Google Scholar] [CrossRef] [PubMed]
- Cleland, V.; Crawford, D.; Baur, L.A.; Hume, C.; Timperio, A.; Salmon, J. A prospective examination of children’s time spent outdoors, objectively measured physical activity and overweight. Int. J. Obes. 2008, 32, 1685–1693. [Google Scholar] [CrossRef] [PubMed]
- Kato, N.; Isojima, T.; Yokoya, S.; Tanaka, T.; Ono, A.; Yokomichi, H.; Yamagata, Z.; Tanaka, S.; Matsubara, H.; Ishikuro, M.; et al. Earlier BMI rebound and lower pre-rebound BMI as risk of obesity among Japanese preschool children. Int. J. Obes. 2018, 42, 52–58. [Google Scholar] [CrossRef] [PubMed]
- Alemzadeh, R.; Kichler, J.; Babar, G.; Calhoun, M. Hypovitaminosis D in obese children and adolescents: Relationship with adiposity, insulin sensitivity, ethnicity, and season. Metab. Clin. Exp. 2008, 57, 183–191. [Google Scholar] [CrossRef] [PubMed]
- Smotkin-Tangorra, M.; Purushothaman, R.; Gupta, A.; Nejati, G.; Anhalt, H.; Ten, S. Prevalence of vitamin D insufficiency in obese children and adolescents. J. Pediatr. Endocrinol. Metab. 2007, 20, 817–823. [Google Scholar] [CrossRef] [PubMed]
- Kumar, J.; Muntner, P.; Kaskel, F.J.; Hailpern, S.M.; Melamed, M.L. Prevalence and associations of 25-hydroxyvitamin D deficiency in US children: NHANES 2001–2004. Pediatrics 2009, 124, e362–e370. [Google Scholar] [CrossRef] [PubMed]
- Gilbert-Diamond, D.; Baylin, A.; Mora-Plazas, M.; Marin, C.; Arsenault, J.E.; Hughes, M.D.; Willett, W.C.; Villamor, E. Vitamin D deficiency and anthropometric indicators of adiposity in school-age children: A prospective study. Am. J. Clin. Nutr. 2010, 92, 1446–1451. [Google Scholar] [CrossRef] [PubMed]
- Motlaghzadeh, Y.; Sayarifard, F.; Allahverdi, B.; Rabbani, A.; Setoodeh, A.; Sayarifard, A.; Abbasi, F.; Haghi-Ashtiani, M.T.; Rahimi-Froushani, A. Assessment of Vitamin D Status and Response to Vitamin D3 in Obese and Non-Obese Iranian Children. J. Trop. Pediatr. 2016, 62, 269–275. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Dehli, A.C.; Riaño-Galán, I.R.; Fernández-Somoano, A.; Navarrete-Muñoz, E.M.; Espada, M.; Vioque, J.; Tardón, A. Hipovitaminosis D y factores asociados a los 4 años en el norte de España. Anales de Pediatría 2017, 86, 188–196. [Google Scholar] [CrossRef] [PubMed]
- Klesges, L.M.; Baranowski, T.; Beech, B.; Cullen, K.; Murray, D.M.; Rochon, J.; Pratt, C. Social desirability bias in self-reported dietary, physical activity and weight concerns measures in 8- to 10-year-old African-American girls: Results from the Girls Health Enrichment Multisite Studies (GEMS). Prev. Med. 2004, 38, S78–S87. [Google Scholar] [CrossRef] [PubMed]
- Lips, P.; van Schoor, N. Worldwide vitamin D status. In Vitamin D, 3rd ed.; Elsevier: Amsterdam, The Netherlands, 2011; pp. 947–963. [Google Scholar]
| Total | Boys | Girls | t-Test | |
|---|---|---|---|---|
| (n = 260) | (n = 132) | (n = 128) | ||
| Mean ± SD | Mean ± SD | Mean ± SD | t-Value (p) | |
| 25(OH)D (nmol/L) | 46.55 ± 20.16 | 49.62 ± 19.68 | 43.38 ± 20.24 | 2.52 (0.01) |
| BMI (kg/m2) | 15.91 ± 2.16 | 15.91 ± 2.14 | 15.92 ± 2.19 | −0.04 (0.97) |
| Pre-PAQ/L1 (score) | 1.15 ± 0.83 | 1.11 ± 0.79 | 1.18 ± 0.88 | −0.66 (0.51) |
| Pre-PAQ/L2 (score) | 0.80 ± 0.68 | 0.90 ± 0.69 | 0.71 ± 0.65 | 2.34 (0.02) |
| Pre-PAQ/L1 + L2 (score) | 1.95 ± 1.16 | 2.02 ± 1.15 | 1.89 ± 1.17 | 0.87 (0.38) |
| Pre-PAQ/L3 (score) | 0.96 ± 0.67 | 0.94 ± 0.69 | 0.98 ± 0.65 | −0.52 (0.60) |
| Pre-PAQ/L4 (score) | 0.92 ± 0.73 | 0.94 ± 0.77 | 0.89 ± 0.69 | 0.65 (0.52) |
| Pre-PAQ/L5 (score) | 0.32 ± 0.45 | 0.39 ± 0.49 | 0.26 ± 0.4 | 2.25 (0.03) |
| Time spent outdoors (hours/week) | 17.42 ± 7.12 | 17.94 ± 7.61 | 16.88 ± 6.57 | 1.21 (0.23) |
| Independent Variables | 25(OH)D (nmol/L) | |||||
|---|---|---|---|---|---|---|
| Total | Boys | Girls | ||||
| (n = 260) | (n = 132) | (n = 128) | ||||
| r | p | r | p | r | p | |
| BMI (kg/m2) | −0.04 | 0.49 | 0.01 | 0.85 | −0.01 | 0.25 |
| Pre-PAQ/L1 (score) | −0.03 | 0.59 | −0.08 | 0.38 | 0.02 | 0.86 |
| Pre-PAQ/L2 (score) | −0.07 | 0.25 | −0.07 | 0.42 | −0.12 | 0.17 |
| Pre-PAQ/L1 + L2 (score) | −0.06 | 0.29 | −0.09 | 0.28 | −0.06 | 0.53 |
| Pre-PAQ/L3 (score) | −0.12 | 0.06 | −0.15 | 0.08 | −0.08 | 0.35 |
| Pre-PAQ/L4 (score) | −0.02 | 0.74 | −0.06 | 0.47 | −0.01 | 0.88 |
| Pre-PAQ/L5 (score) | −0.04 | 0.54 | −0.07 | 0.44 | −0.05 | 0.55 |
| Time spent outdoors (hours/week) | −0.05 | 0.42 | 0.01 | 0.90 | −0.15 | 0.09 |
| 25(OH)D Deficiency (<50 nmol/L) | 25(OH)D Insufficiency (50–75 nmol/L) | |||
|---|---|---|---|---|
| Independent Variables | OR | 95% CI | OR | 95% CI |
| Gender | ||||
| Male | 0.33 | 0.15–0.74 | 0.60 | 0.25–1.43 |
| Female | REF | REF | ||
| BMI cont | 1.08 | 0.89–1.31 | 1.08 | 0.88–1.31 |
| Pre-PAQ/L1 cont | 1.15 | 0.71–1.86 | 1.00 | 0.59–1.70 |
| Pre-PAQ/L2 cont | 1.49 | 0.81–2.75 | 1.14 | 0.59–2.20 |
| Pre-PAQ/L1 + L2 cont | 1.22 | 0.86–1.75 | 1.05 | 0.72–1.54 |
| Pre-PAQ/L3 cont | 1.40 | 0.76–2.58 | 0.95 | 0.49–1.85 |
| Pre-PAQ/L4 cont | 1.15 | 0.68–1.94 | 0.88 | 0.49–1.56 |
| Pre-PAQ/L5 cont | 2.35 | 0.84–6.68 | 1.92 | 0.65–5.69 |
| Time spent outdoors cont | 1.04 | 0.98–1.10 | 1.03 | 0.97–1.10 |
| 25(OH)D Deficiency (<50 nmol/L) | 25(OH)D Insufficiency (50–75 nmol/L) | |||
|---|---|---|---|---|
| Independent Variables | OR | 95% CI | OR | 95% CI |
| BMI | 1.04 | 0.82–1.31 | 1.13 | 0.88–1.44 |
| Pre-PAQ/L1 | 1.33 | 0.71–2.49 | 0.88 | 0.44–1.76 |
| Pre-PAQ/L2 | 1.21 | 0.59–2.47 | 1.23 | 0.58–2.61 |
| Pre-PAQ/L1 + L2 | 1.22 | 0.79–1.88 | 1.02 | 0.64–1.63 |
| Pre-PAQ/L3 | 1.45 | 0.69–3.04 | 0.85 | 0.37–1.95 |
| Pre-PAQ/L4 | 1.05 | 0.57–1.93 | 0.83 | 0.43–1.62 |
| Pre-PAQ/L5 | 1.96 | 0.63–6.12 | 1.88 | 0.57–6.16 |
| Time spent outdoors | 1.01 | 0.94–1.08 | 1.02 | 0.95–1.09 |
| 25(OH)D Deficiency (<50 nmol/L) | 25(OH)D Insufficiency (50–75 nmol/L) | |||
|---|---|---|---|---|
| Independent Variables | OR | 95% CI | OR | 95% CI |
| BMI | 1.13 | 0.81–1.57 | 1.01 | 0.71–1.45 |
| Pre-PAQ/L1 | 0.99 | 0.47–2.13 | 1.1 | 0.49–2.47 |
| Pre-PAQ/L2 | 2.21 | 0.62–7.94 | 1.07 | 0.27–4.35 |
| Pre-PAQ/L1 + L2 | 1.25 | 0.66–2.36 | 1.09 | 0.55–2.17 |
| Pre-PAQ/L3 | 1.39 | 0.46–4.17 | 1.11 | 0.34–3.68 |
| Pre-PAQ/L4 | 1.46 | 0.52–4.08 | 1.06 | 0.35–3.26 |
| Pre-PAQ/L5 | 4.29 | 0.33–56.45 | 2.65 | 0.18–39.51 |
| Time spent outdoors | 1.14 | 0.99–1.30 | 1.1 | 0.95–1.27 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Karin, Z.; Gilic, B.; Supe Domic, D.; Sarac, Z.; Ercegovic, K.; Zenic, N.; Uljevic, O.; Peric, M.; Markic, J. Vitamin D Status and Analysis of Specific Correlates in Preschool Children: A Cross-Sectional Study in Southern Croatia. Int. J. Environ. Res. Public Health 2018, 15, 2503. https://doi.org/10.3390/ijerph15112503
Karin Z, Gilic B, Supe Domic D, Sarac Z, Ercegovic K, Zenic N, Uljevic O, Peric M, Markic J. Vitamin D Status and Analysis of Specific Correlates in Preschool Children: A Cross-Sectional Study in Southern Croatia. International Journal of Environmental Research and Public Health. 2018; 15(11):2503. https://doi.org/10.3390/ijerph15112503
Chicago/Turabian StyleKarin, Zeljka, Barbara Gilic, Daniela Supe Domic, Zdenko Sarac, Katarina Ercegovic, Natasa Zenic, Ognjen Uljevic, Mia Peric, and Josko Markic. 2018. "Vitamin D Status and Analysis of Specific Correlates in Preschool Children: A Cross-Sectional Study in Southern Croatia" International Journal of Environmental Research and Public Health 15, no. 11: 2503. https://doi.org/10.3390/ijerph15112503
APA StyleKarin, Z., Gilic, B., Supe Domic, D., Sarac, Z., Ercegovic, K., Zenic, N., Uljevic, O., Peric, M., & Markic, J. (2018). Vitamin D Status and Analysis of Specific Correlates in Preschool Children: A Cross-Sectional Study in Southern Croatia. International Journal of Environmental Research and Public Health, 15(11), 2503. https://doi.org/10.3390/ijerph15112503







