Trends in Pediatric and Adolescent Anterior Cruciate Ligament Injuries in Victoria, Australia 2005–2015
Abstract
:1. Introduction
2. Materials and Methods
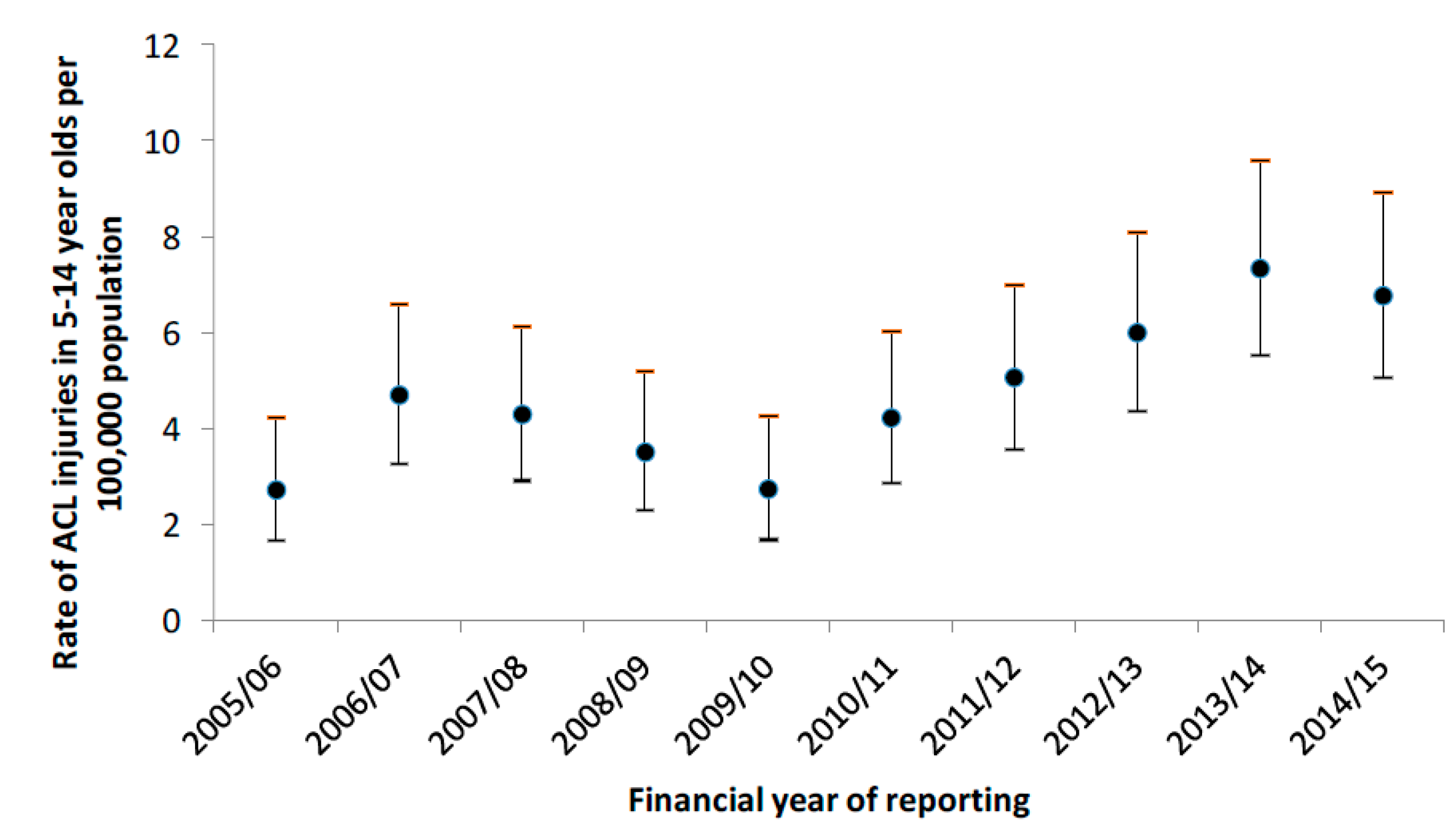
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Caine, D.; Purcell, L.; Maffulli, N. The child and adolescent athlete: A review of three potentially serious injuries. BMC Sports Sci. Med. Rehabil. 2014, 6, 22. [Google Scholar] [CrossRef] [PubMed]
- Dodwell, E.R.; LaMont, L.E.; Green, D.W.; Pan, T.J.; Marx, R.G.; Lyman, S. 20 Years of pediatric anterior cruciate ligament reconstruction in New York State. Am. J. Sports Med. 2014, 42, 675–680. [Google Scholar] [CrossRef] [PubMed]
- Frank, J.S.; Gambacorta, P.L. Anterior Cruciate Ligament injuries in the skeletally immature athlete: Diagnosis and management. J. Am. Acad. Orthop. Surg. 2013, 21, 78–87. [Google Scholar] [CrossRef] [PubMed]
- Griffiths, M. ACL Injuries: Growing Number of Child Cases Prompts Call for National Database. 2016. Available online: http://www.abc.net.au/news/2016-11-16/acl-revelations-spark-call-for-sports-injury-database/8027902 (accessed on 16 November 2016).
- Janssen, K.W.; Orchard, J.W.; Driscoll, T.R.; van Mechelen, W. High incidence and costs for Anterior Cruciate Ligament reconstructions performed in Australia from 2003–2004 to 2007–2008: Time for an Anterior Cruciate Ligament register by Scandinavian model? Scand. J. Med. Sci. Sports 2012, 22, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Schub, D.; Saluan, P. Anterior Cruciate Ligament injuries in the young athlete: Evaluation and treatment. Sports Med. Arthrosc. Rev. 2011, 19, 34–43. [Google Scholar] [CrossRef] [PubMed]
- Shea, K.G.; Grimm, N.L.; Ewing, C.K.; Aoki, S.K. Youth sports anterior cruciate ligament and knee injury epidemiology: Who is getting injured? In what sports? When? Clin. Sports Med. 2011, 30, 691–706. [Google Scholar] [CrossRef] [PubMed]
- Caine, D.J.; Golightly, Y.M. Osteoarthritis as an outcome of paediatric sport: An epidemiological perspective. Br. J. Sports Med. 2011, 45, 298–303. [Google Scholar] [CrossRef] [PubMed]
- Clanton, T.; DeLee, J.; Sanders, B.; Neidre, A. Knee ligament injuries in children. J. Bone Jt. Surg. 1979, 61, 1195–1201. [Google Scholar] [CrossRef]
- DeLEE, J.C.; Curtis, R. Anterior cruciate ligament insufficiency in children. Clin. Orthop. Relat. Res. 1983, 172, 112–118. [Google Scholar] [CrossRef]
- Lipscomb, A.B.; Anderson, A. Tears of the anterior cruciate ligament in adolescents. J. Bone Jt. Surg. Am. Vol. 1986, 68, 19–28. [Google Scholar] [CrossRef]
- McCarroll, J.R.; Rettig, A.C.; Shelbourne, K.D. Anterior Cruciate Ligament injuries in the young athlete with open physes. Am. J. Sports Med. 1988, 16, 44–47. [Google Scholar] [CrossRef] [PubMed]
- Milewski, M.D.; Beck, N.A.; Lawrence, J.T.; Ganley, T.J. Anterior Cruciate Ligament reconstruction in the young athlete: A treatment algorithm for the skeletally immature. Clin. Sports Med. 2011, 30, 801–810. [Google Scholar] [CrossRef] [PubMed]
- Werner, B.C.; Yang, S.; Looney, A.M.; Gwathmey, F.W., Jr. Trends in pediatric and adolescent Anterior Cruciate Ligament Injury and reconstruction. J. Pediatr. Orthop. 2016, 36, 447–452. [Google Scholar] [CrossRef] [PubMed]
- Kocher, M.S.; Smith, J.T.; Zoric, B.J.; Lee, B.; Micheli, L.J. Transphyseal anterior cruciate ligament reconstruction in skeletally immature pubescent adolescents. J. Bone Jt. Surg. Am. Vol. 2007, 89, 2632–2639. [Google Scholar] [CrossRef] [PubMed]
- Angel, K.R.; Hall, D.J. Anterior Cruciate Ligament injury in children and adolescents. Arthroscopy 1989, 5, 197–200. [Google Scholar] [CrossRef]
- Moksnes, H.; Grindem, H. Prevention and rehabilitation of paediatric anterior cruciate ligament injuries. Knee Surg. Sports Traumatol. Arthrosc. 2016, 24, 730–736. [Google Scholar] [CrossRef] [PubMed]
- Stracciolini, A.; Casciano, R.; Levey Friedman, H.; Meehan, W.P.; Micheli, L.J. Pediatric sports injuries: An age comparison of children versus adolescents. Am. J. Sports Med. 2013, 41, 1922–1929. [Google Scholar] [CrossRef] [PubMed]
- Monash University Accident Research Centre. Victorian Injury Surveillance Unit. 2017. Available online: https://www.monash.edu/muarc/research/research-areas/home-and-community/visu (accessed on 5 May 2017).
- National Centre for Classification in Health. The International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Australian Modification (ICD-10-AM); Uo, S., Ed.; Australian Institute of Health and Welfare: Canberra, Australia, 1998.
- Australian Sports Commission. AusPlay Participation Data for the Sport Sector: Summary of Key National Findings October 2015 to September 2016 Data; Australian Government: Canberra, Australia, 2016.
- Australian Bureau of Statistics. 3235.0 Population by Age and Sex, Regions of Australia, 2015. Available online: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/3235.02015?OpenDocument (accessed on 6 September 2016).
- Miettinen, O.S. Proportion of disease caused or prevented by a given exposure, trait or intervention. Am. J. Epidemiol. 1974, 99, 325–332. [Google Scholar] [CrossRef] [PubMed]
- Arbes, S.; Resinger, C.; Vécsei, V.; Nau, T. The functional outcome of total tears of the Anterior Cruciate Ligament (ACL) in the skeletally immature patient. Int. Orthop. 2007, 31, 471–475. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Wong Shee, A.; Clapperton, A. Time to add a new priority target for child injury prevention? The case for an excess burden associated with sport and exercise injury: Population-based study. BMJ Open 2014, 4, e005043. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Kemp, J.L.; Clapperton, A.J. The incidence and burden of hospital-treated sports-related injury in people aged 15+ years in Victoria, Australia, 2004–2010: A future epidemic of osteoarthritis? Osteoarthr. Cartil. 2015, 23, 1138–1143. [Google Scholar] [CrossRef] [PubMed]
- Hewett, T.E.; Myer, G.D.; Ford, K.R.; Paterno, M.V.; Quatman, C.E. The 2012 ABJS Nicolas Andry Award: The sequence of prevention: A systematic approach to prevent anterior cruciate ligament injury. Clin. Orthop. Relat. Res. 2012, 470, 2930–2940. [Google Scholar] [CrossRef] [PubMed]
- Fabricant, P.D.; Kocher, M.S. Anterior Cruciate Ligament Injuries in Children and Adolescents. Orthop. Clin. N. Am. 2016, 47, 777–788. [Google Scholar] [CrossRef] [PubMed]
- Moksnes, H.; Engebretsen, L.; Risberg, M.A. The current evidence for treatment of ACL injuries in children is low: A systematic review. J. Bone Jt. Surg. Am. Vol. 2012, 94, 1112–1119. [Google Scholar] [CrossRef] [PubMed]
- Quatman-Yates, C.C.; Quatman, C.E.; Meszaros, A.J.; Paterno, M.V.; Hewett, T.E. A systematic review of sensorimotor function during adolescence: A developmental stage of increased motor awkwardness? Br. J. Sports Med. 2012, 46, 649–655. [Google Scholar] [CrossRef] [PubMed]
- Hewett, T.E.; Myer, G.D.; Ford, K.R.; Heidt, R.S.; Colosimo, A.J.; McLean, S.G.; Van den Bogert, A.J.; Paterno, M.V.; Succop, P. Biomechanical measures of neuromuscular control and valgus loading of the knee predict Anterior Cruciate Ligament injury risk in female athletes a prospective study. Am. J. Sports Med. 2005, 33, 492–501. [Google Scholar] [CrossRef] [PubMed]
- Ford, K.R.; Myer, G.D.; Hewett, T.E. Longitudinal effects of maturation on lower extremity joint stiffness in adolescent athletes. Am. J. Sports Med. 2010, 38, 1829–1837. [Google Scholar] [CrossRef] [PubMed]
- Frosch, K.H.; Stengel, D.; Brodhun, T.; Stietencron, I.; Holsten, D.; Jung, C.; Reister, D.; Voigt, C. Outcomes and risks of operative treatment of rupture of the Anterior Cruciate Ligament in children and adolescents. Arthroscopy 2010, 26, 1539–1550. [Google Scholar] [CrossRef] [PubMed]
- Vavken, P.; Murray, M.M. Treating Anterior Cruciate Ligament tears in skeletally immature patients. Arthroscopy 2011, 27, 704–716. [Google Scholar] [CrossRef] [PubMed]
- Cohen, M.; Ferretti, M.; Quarteiro, M.; Marcondes, F.B.; de Hollanda, J.P.; Amaro, J.T.; Abdalla, R.J. Transphyseal Anterior Cruciate Ligament reconstruction in patients with open physes. Arthroscopy 2009, 25, 831–838. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.; Ahearne, D.; Hunt, D.M. Transphyseal Anterior Cruciate Ligament reconstruction in the skeletally immature: Follow-up to a minimum of sixteen years of age. J. Bone Jt. Surg. Am. Vol. 2013, 95, e1. [Google Scholar] [CrossRef] [PubMed]
- Hewett, T.E.; Myer, G.D.; Ford, K.R. Decrease in neuromuscular control about the knee with maturation in female athletes. J. Bone Jt. Surg. Am. Vol. 2004, 86, 1601–1608. [Google Scholar] [CrossRef]
- Waldén, M.; Atroshi, I.; Magnusson, H.; Wagner, P.; Hägglund, M. Prevention of acute knee injuries in adolescent female football players: Cluster randomised controlled trial. Br. Med. J. 2012, 344, e3042. [Google Scholar] [CrossRef] [PubMed]
- Quatman, C.E.; Ford, K.R.; Myer, G.D.; Hewett, T.E. Maturation leads to gender differences in landing force and vertical jump performance: A longitudinal study. Am. J. Sports Med. 2006, 34, 806–813. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Gabbe, B.J.; Lloyd, D.G.; Cook, J.; Young, W.; Nicholson, M.; Seward, H.; Donaldson, A.; Doyle, T.L.A. Towards a national sports safety strategy: Addressing facilitators and barriers towards safety guideline uptake. Inj. Prev. 2011, 17, e4. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F. Implementing studies into real life. In Sports Injury Research 16; Verhagen, E., van Mechelen, W., Eds.; Oxford University Press: Oxford, UK, 2010; p. 213. [Google Scholar]
- Hewett, T.E.; Johnson, D.L. ACL prevention programs: Fact or fiction? Orthopedics 2010, 33, 36–39. [Google Scholar] [CrossRef] [PubMed]
- Gilchrist, J.; Mandelbaum, B.R.; Melancon, H.; Ryan, G.W.; Silvers, H.J.; Griffin, L.Y.; Watanabe, D.S.; Dick, R.W.; Dvorak, J. A randomized controlled trial to prevent noncontact Anterior Cruciate Ligament injury in female collegiate soccer players. Am. J. Sports Med. 2008, 36, 1476–1483. [Google Scholar] [CrossRef] [PubMed]
- Mandelbaum, B.R.; Silvers, H.J.; Watanabe, D.S.; Knarr, J.F.; Thomas, S.D.; Griffin, L.Y.; kirkendall, D.T.; Garrett, W. Effectiveness of a neuromuscular and proprioceptive training program in preventing Anterior Cruciate Ligament injuries in female athletes 2-year follow-up. Am. J. Sports Med. 2005, 33, 1003–1010. [Google Scholar] [CrossRef] [PubMed]
- Myer, G.D.; Sugimoto, D.; Thomas, S.; Hewett, T.E. The influence of age on the effectiveness of neuromuscular training to reduce Anterior Cruciate Ligament injury in female athletes: A meta-analysis. Am. J. Sports Med. 2013, 41, 203–215. [Google Scholar] [CrossRef] [PubMed]
- Ladenhauf, H.N.; Graziano, J.; Marx, R.G. Anterior cruciate ligament prevention strategies: Are they effective in young athletes—Current concepts and review of literature. Curr. Opin. Pediatr. 2013, 25, 64–71. [Google Scholar] [CrossRef] [PubMed]
- Myer, G.D.; Ford, K.R.; Barber Foss, K.D.; Liu, C.; Nick, T.G.; Hewett, T.E. The relationship of hamstrings and quadriceps strength to Anterior Cruciate Ligament injury in female athletes. Clin. J. Sport Med. 2009, 19, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Lewis, D.A.; Kirkbride, B.; Vertullo, C.J.; Gordon, L.; Comans, T.A. Comparison of four alternative national universal anterior cruciate ligament injury prevention programme implementation strategies to reduce secondary future medical costs. Br. J. Sports Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Noyes, F.R.; Barber-Westin, S.D. Neuromuscular retraining intervention programs: Do they reduce noncontact anterior cruciate ligament injury rates in adolescent female athletes? Arthroscopy 2014, 30, 245–255. [Google Scholar] [CrossRef] [PubMed]
- Hägglund, M.; Atroshi, I.; Wagner, P.; Waldén, M. Superior compliance with a neuromuscular training programme is associated with fewer ACL injuries and fewer acute knee injuries in female adolescent football players: Secondary analysis of an RCT. Br. J. Sports Med. 2013, 47, 974–979. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Donaldson, A. A sports setting matrix for understanding the implementation context for community sport. Br. J. Sports Med. 2010, 44, 973–978. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F. No longer lost in translation: The art and science of sports injury prevention implementation research. Br. J. Sports Med. 2011, 45, 1253–1257. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F. Getting sports injury prevention on to public health agendas—Addressing the shortfalls in current information sources. Br. J. Sports Med. 2011, 46, 70–74. [Google Scholar] [CrossRef] [PubMed]
- Donaldson, A.; Finch, C. Planning for implementation and translation: Seek first to understand the end-users’ perspectives. Br. J. Sports Med. 2011, 46, 306–307. [Google Scholar] [CrossRef] [PubMed]
- Verhagen, E.; Finch, C.F. Setting our minds to implementation. Br. J. Sports Med. 2011, 45, 1015–1016. [Google Scholar] [CrossRef] [PubMed]
- Verhagen, E.; Voogt, N.; Bruinsma, A.; Finch, C.F. A knowledge transfer scheme to bridge the gap between science and practice: An integration of existing research frameworks into a tool for practice. Br. J. Sports Med. 2013. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Boufous, S. Do inadequacies in ICD-10-AM activity coded data lead to underestimates of the population frequency of sports/leisure injuries? Inj. Prev. 2008, 14, 202–204. [Google Scholar] [CrossRef] [PubMed]
- Cassell, E.P.; Finch, C.F.; Stathakis, V.Z. Epidemiology of medically treated sport and active recreation injuries in the Latrobe Valley, Victoria, Australia. Br. J. Sports Med. 2003, 37, 405–409. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, R.; Finch, C.; Boufous, S. Counting organised sport injury cases: Evidence of incomplete capture from routine hospital collections. J. Sci. Med. Sport 2010, 13, 304–308. [Google Scholar] [CrossRef] [PubMed]
| Australian Classification of Health Interventions (ACHI) for Admitted ACL Injuries amongst Victorian Children and Adolescents | Number | % |
|---|---|---|
| Arthroscopic reconstruction of knee | 106 | 33.1 |
| Reconstruction of knee | 87 | 27.2 |
| Arthroscopic reconstruction of cruciate ligament of knee with repair of meniscus | 55 | 17.2 |
| Reconstruction of cruciate ligament of knee with repair of meniscus | 18 | 5.6 |
| Arthroscopic debridement of knee | 9 | 2.8 |
| Arthroscopy of knee | 8 | 2.5 |
| Arthroscopic menisectomy of knee with debridement, osteoplasty or chondroplasty | 7 | 2.2 |
| Allied health intervention, physiotherapy | 5 | 1.6 |
| Other surgical procedures * | 25 | 7.8 |
| Total | 320 | 100 |
| Activity | Male | Female | Total | ||
|---|---|---|---|---|---|
| n | % | n | % | ||
| Team ball sports | 62 | 35.4 | 76 | 52.4 | 138 |
| Other activity (not specified) | 83 | 47.4 | 46 | 31.7 | 129 |
| Other specified activity with small cell counts grouped together (Team bat or stick sports, individual athletic activities, acrobatic sports, combative sports, equestrian activities, other school related recreational activities, other specified sport and exercise activity) | 6 | 3.4 | 11 | 7.6 | 17 |
| Other sport or leisure activities (Ice and snow sports, wheeled motor sports, wheeled non-motored sports, unspecified sport and exercise activity, leisure activity) | 24 | 13.7 | 12 | 8.3 | 36 |
| Totals | 175 | 100 | 145 | 100 | 320 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shaw, L.; Finch, C.F. Trends in Pediatric and Adolescent Anterior Cruciate Ligament Injuries in Victoria, Australia 2005–2015. Int. J. Environ. Res. Public Health 2017, 14, 599. https://doi.org/10.3390/ijerph14060599
Shaw L, Finch CF. Trends in Pediatric and Adolescent Anterior Cruciate Ligament Injuries in Victoria, Australia 2005–2015. International Journal of Environmental Research and Public Health. 2017; 14(6):599. https://doi.org/10.3390/ijerph14060599
Chicago/Turabian StyleShaw, Louise, and Caroline F. Finch. 2017. "Trends in Pediatric and Adolescent Anterior Cruciate Ligament Injuries in Victoria, Australia 2005–2015" International Journal of Environmental Research and Public Health 14, no. 6: 599. https://doi.org/10.3390/ijerph14060599
APA StyleShaw, L., & Finch, C. F. (2017). Trends in Pediatric and Adolescent Anterior Cruciate Ligament Injuries in Victoria, Australia 2005–2015. International Journal of Environmental Research and Public Health, 14(6), 599. https://doi.org/10.3390/ijerph14060599






