U.S. Trends of ED Visits for Pediatric Traumatic Brain Injuries: Implications for Clinical Trials
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Definition of Pediatric TBI
2.3. Definition of Pediatric Concussion
2.4. Definition of Pediatric Severe TBI
2.5. Definition of TBI Type
2.6. Study Variables
2.7. Statistical Analysis
2.8. Bootstrap Simulation Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Centers for Disease Control and Prevention. Rates of hospitalization related to traumatic brain injury—Nine states, 2003. MMWR Morb. Mortal. Wkly. Rep. 2007, 56, 167–170. [Google Scholar]
- Schneier, A.J.; Shields, B.J.; Hostetler, S.G.; Xiang, H.; Smith, G.A. Incidence of pediatric traumatic brain injury and associated hospital resource utilization in the United States. Pediatrics 2006, 118, 483–492. [Google Scholar] [CrossRef] [PubMed]
- Mandalis, A.; Kinsella, G.; Ong, B.; Anderson, V. Working memory and new learning following pediatric traumatic brain injury. Dev. Neuropsychol. 2007, 32, 683–701. [Google Scholar] [CrossRef] [PubMed]
- Pullela, R.; Raber, J.; Pfankuch, T.; Ferriero, D.M.; Claus, C.P.; Koh, S.E.; Yamauchi, T.; Rola, R.; Fike, J.R.; Noble-Haeusslein, L.J. Traumatic injury to the immature brain results in progressive neuronal loss, hyperactivity and delayed cognitive impairments. Dev. Neurosci. 2006, 28, 396–409. [Google Scholar] [CrossRef] [PubMed]
- Verger, K.; Junque, C.; Jurado, M.A.; Tresserras, P.; Bartumeus, F.; Nogués, P.; Poch, J.M. Age effects on long-term neuropsychological outcome in paediatric traumatic brain injury. Brain Inj. 2000, 14, 495–503. [Google Scholar] [PubMed]
- Umile, E.M.; Sandel, M.E.; Alavi, A.; Terry, C.M.; Plotkin, R.C. Dynamic imaging in mild traumatic brain injury: Support for the theory of medial temporal vulnerability. Arch. Phys. Med. Rehabil. 2002, 83, 1506–1513. [Google Scholar] [CrossRef] [PubMed]
- Stocchetti, N.; Zanier, E.R. Chronic impact of traumatic brain injury on outcome and quality of life: A narrative review. Crit. Care 2016, 20, 148. [Google Scholar] [CrossRef] [PubMed]
- Stanley, R.M.; Bonsu, B.K.; Zhao, W.; Ehrlich, P.F.; Rogers, A.J.; Xiang, H. US estimates of hospitalized children with severe traumatic brain injury: implications for clinical trials. Pediatrics 2012, 129, e24–e30. [Google Scholar] [CrossRef] [PubMed]
- ClinicalTrials.gov. Search for Studies. Available online: https://clinicaltrials.gov/ (accessed on 16 October 2016).
- Centers for Disease Control and Prevention. Report to Congress on Traumatic Brain Injury in the United States: Epidemiology and Rehabilitation. Available online: https://www.quantumunitsed.com/get-material.php?id=457 (accessed on 16 October 2016).
- Marr, A.; Coronado, V. Central Nervous System Injury Surveillance Data Submission Standards—2002. Available online: http://dshs.texas.gov/injury/registry/CoronadoAndMarrCNSDefinitions.doc (accessed on 30 March 2017).
- Copes, W.S.; Champion, H.R.; Sacco, W.J. Progress in characterizing anatomic injury. J. Trauma 1990, 30, 1200–1207. [Google Scholar] [CrossRef] [PubMed]
- United States Census Bureau. Annual Estimates of the Resident Population by Sex, Single Year of Age, Race and Hispanic Origin for the United States. Available online: https://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=PEP_2012_PEPALL6N&prodType=table (accessed on 16 October 2016).
- Centers for Disease Control and Prevention. Rates of TBI-Related Emergency Department Visits by Age Group—United States, 2001–2010. Available online: https://www.cdc.gov/traumaticbraininjury/data/rates_ed_byage.html (accessed on 16 October 2016).
- Marin, J.R.; Weaver, M.D.; Yealy, D.M.; Mannix, R.C. Trends in visits for traumatic brain injury to emergency departments in the United States. JAMA 2014, 311, 1917–1919. [Google Scholar] [CrossRef] [PubMed]
- Smith, N.A.; Chounthirath, T.; Xiang, H. Soccer-Related Injuries Treated in Emergency Departments: 1990–2014. Pediatrics 2016, 138. [Google Scholar] [CrossRef] [PubMed]
- HealthIT.gov. Benefits of Electronic Medical Records. Available online: https://www.healthit.gov/providers-professionals/electronic-medical-records-emr (accessed on 16 October 2016).
- World Health Organization. International Classification of Diseases (ICD). Available online: http://www.who.int/classifications/icd/en/ (accessed on 16 October 2016).
- Bazarian, J.J.; Veazie, P.; Mookerjee, S.; Lerner, E.B. Accuracy of mild traumatic brain injury case ascertainment using ICD-9 codes. Acad. Emerg. Med. 2006, 13, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Chan, V.; Mann, R.E.; Pole, J.D.; Colantonio, A. Children and youth with “unspecified injury to the head”: Implications for traumatic brain injury research and surveillance. Emerg. Themes Epidemiol. 2015, 12, 9. [Google Scholar] [CrossRef] [PubMed]
- Natale, J.E.; Joseph, J.G.; Pretzlaff, R.K.; Silber, T.J.; Guerguerian, A.M. Clinical trials in pediatric traumatic brain injury: Unique challenges and potential responses. Dev. Neurosci. 2006, 28, 276–290. [Google Scholar] [CrossRef] [PubMed]
- The Clinical Trials Subcommittee. Design and Conduct of Clinical Trials. Available online: http://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=0ahUKEwiDrIjbobrRAhWp34MKHUK5DVQQFggcMAA&url=http%3A%2F%2Fwww.tearfilm.org%2Fdewsreport%2Fpdfs%2FDesign%2520and%2520Conduct%2520of%2520Clinical%2520Trials.pdf&usg=AFQjCNHo_4As8HKb53kgh6zqhnL3h1iauQ&sig2=b9zOs9FQjEdgKl_cIaPr2A (accessed on 16 October 2016).
- Cook, A.; Weddle, J.; Baker, S.; Hosmer, D.; Glance, L.; Friedman, L.; Osler, T. A comparison of the Injury Severity Score and the Trauma Mortality Prediction Model. J. Trauma Acute Care Surg. 2014, 76, 47–52. [Google Scholar] [CrossRef] [PubMed]
- Kohn, M.A.; Hammel, J.M.; Bretz, S.W.; Stangby, A. Trauma team activation criteria as predictors of patient disposition from the emergency department. Acad. Emerg. Med. 2004, 11, 1–9. [Google Scholar] [CrossRef] [PubMed]
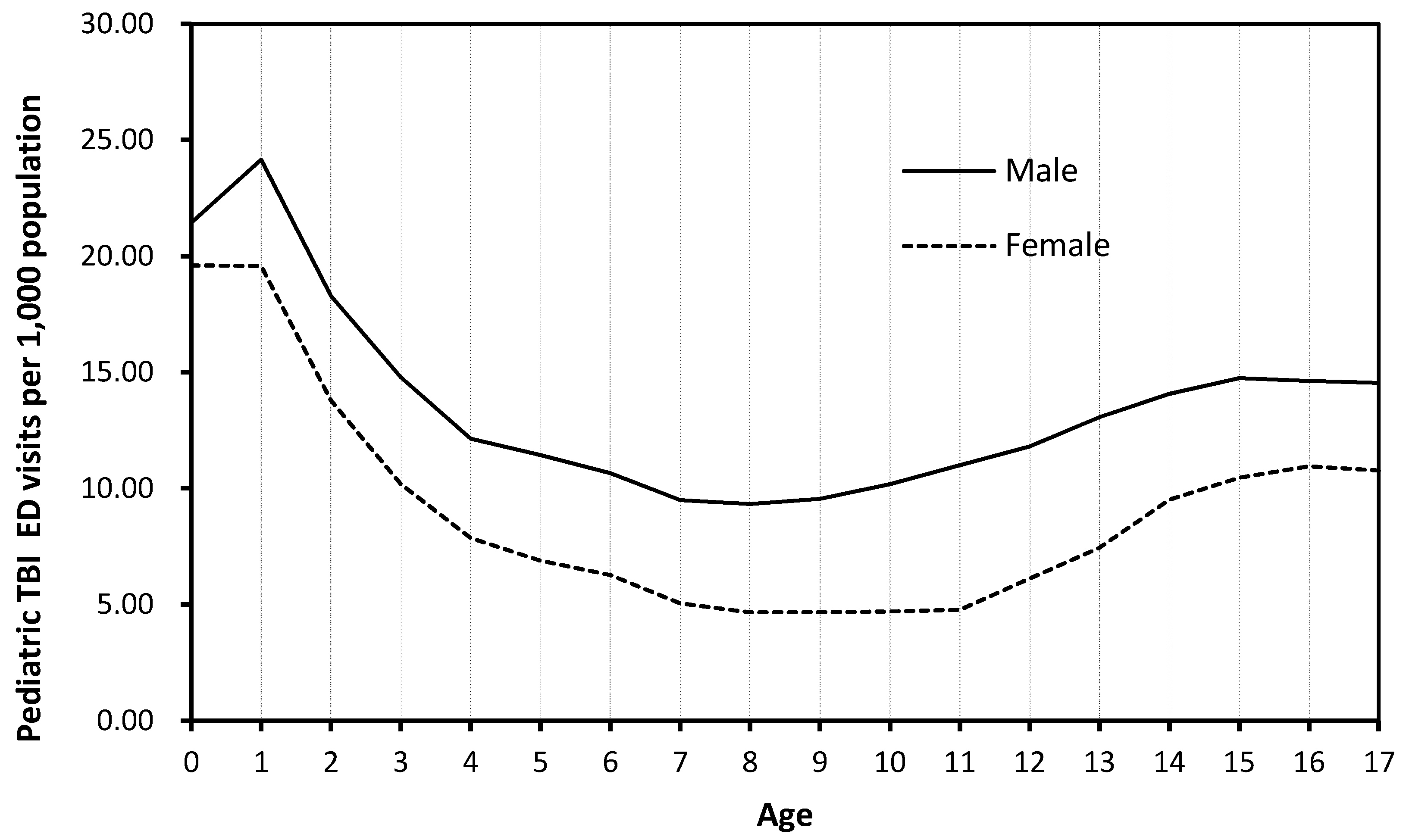
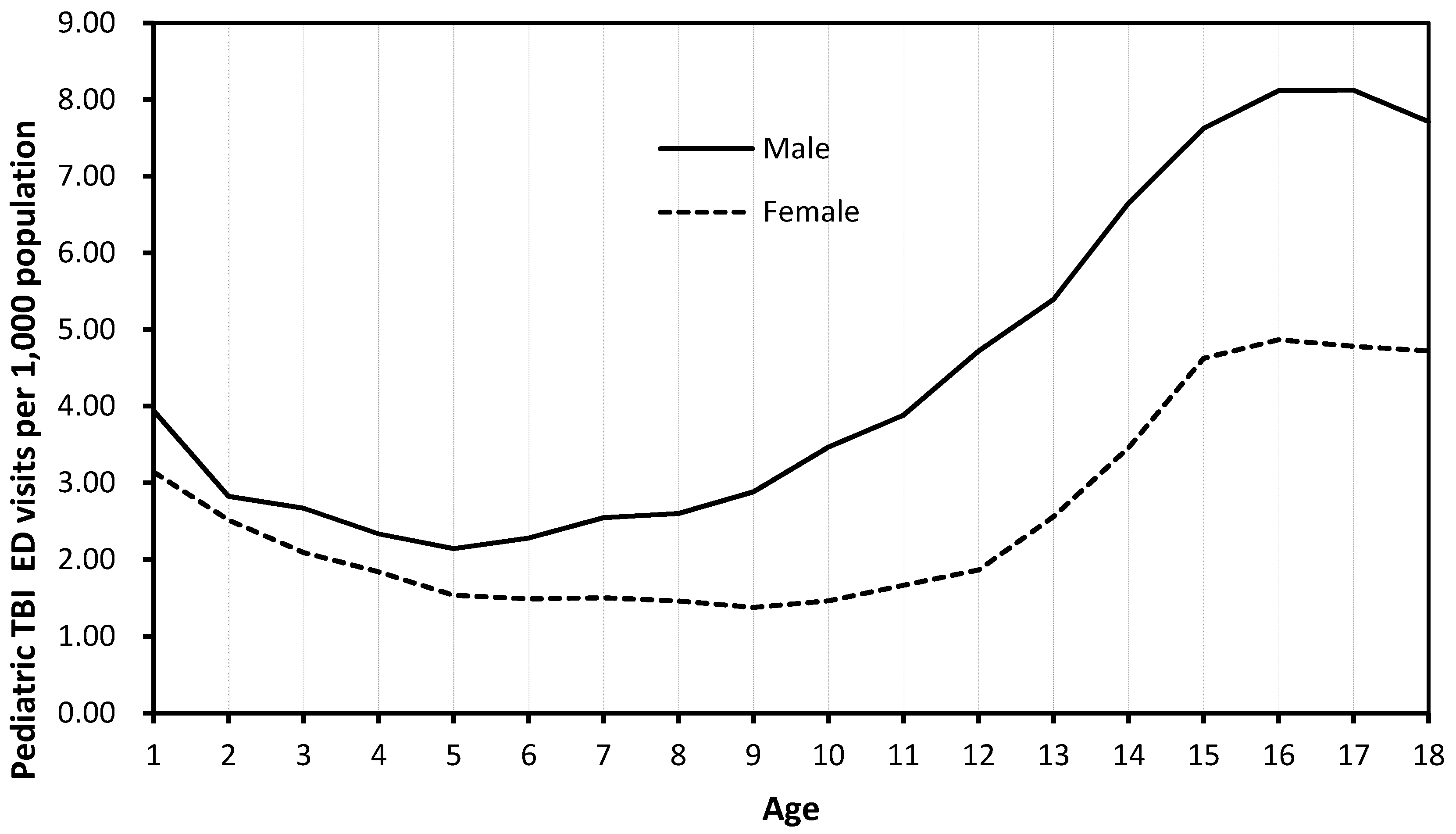
| Year | Pediatric ED Visits | Pediatric TBI (Including Code 959.01) 2 | Pediatric TBI (Excluding Code 959.01) | Pediatric Concussion | Pediatric Severe TBI | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Weighted Number | % Change 3 | Weighted Number | % Change | Weighted Number | % Change | Weighted Number | % Change | Weighted Number | % Change | |
| 2006 | 26,421,966 | 0.0 | 624,705 | 0.0 | 216,097 | 0.0 | 162,013 | 0.0 | 34,046 | 0.0 |
| 2007 | 26,952,590 | 2.0 | 638,088 | 2.1 | 224,657 | 4.0 | 168,717 | 4.1 | 35,311 | 3.7 |
| 2008 | 26,422,740 | 0.0 | 656,897 | 5.2 | 231,665 | 7.2 | 177,039 | 9.3 | 35,324 | 3.8 |
| 2009 | 28,411,936 | 7.5 | 798,044 | 27.7 | 243,015 | 12.5 | 193,538 | 19.5 | 31,893 | −6.3 |
| 2010 | 25,511,069 | −3.4 | 778,138 | 24.6 | 252,566 | 16.9 | 202,681 | 25.1 | 31,777 | −6.7 |
| 2011 | 27,010,706 | 2.2 | 851,405 | 36.3 | 255,072 | 18.0 | 209,917 | 29.6 | 28,575 | −16.1 |
| 2012 | 27,877,600 | 5.5 | 905,225 | 44.9 | 272,004 | 25.9 | 228,424 | 41.0 | 27,620 | −18.9 |
| 2013 | 26,596,325 | 0.7 | 837,428 | 34.1 | 262,826 | 21.6 | 218,984 | 35.2 | 27,787 | −18.4 |
| Total | 215,204,932 | 6,089,930 | 1,957,902 | 1,561,313 | 252,333 | |||||
| Pediatric TBI Including 959.01 2 (n = 837,428) | Pediatric TBI Excluding 959.01 2 (n = 262,826) | Pediatric Concussion (n = 218,984) | Pediatric Severe TBI (n = 12,370) | ||
|---|---|---|---|---|---|
| Gender, weighted % (95% CI) 3 | |||||
| Male | 61.2 (60.9–61.5) | 64.09 (63.6–64.6) | 64.0 (63.4–64.5) | 66.2 (64.4–68.1) | |
| Female | 38.9 (38.6–39.1) | 35.9 (35.4–36.4) | 36.0 (35.5–36.6) | 33.8 (31.9–35.6) | |
| Age (years), weighted % (95% CI) | |||||
| Age 0– | 9.7 (9.2–10.1) | 5.3 (4.6–6.1) | 1.5 (1.3–1.7) | 20.9 (18.3–23.4) | |
| Age 1–4 | 29.0 (28.3–29.6) | 13.7 (12–14.7) | 11.8 (10.9–12.7) | 19.7 (18.0–21.4) | |
| Age 5–9 | 19.2 (18.9–19.5) | 16.5 (16–17.1) | 16.6 (16.0–17.2) | 15.3 (13.8–16.9) | |
| Age 10–14 | 23.0 (22.5–23.6) | 33.7 (32–34.6) | 36.9 (35.9–37.8) | 19.5 (17.5–21.6) | |
| Age 15–17 | 19.1 (18.4–19.9) | 30.8 (29–32.3) | 33.2 (32.0–34.4) | 24.5 (20.3–28.8) | |
| TBI Type, weighted % (95% CI) | |||||
| Type 1 | 9.9 (8.5–11.4) | 9.9 (8.5–11.4) | 0.2 (0.1–0.2) | 88.0 (86.5–89.5) | |
| Type 2 | 85.6 (83.8–87.5) | 85.6 (83.8–87.5) | 99.8 (99.8–99.9) | 4.6 (3.7–5.5) | |
| Type 3 | 4.4 (3.8–5.0) | 4.4 (3.8–5.0) | - | 7.4 (6.3–8.5) | |
| ISS, weighted % (95% CI) | |||||
| ISS 1–3 | 3.1 (2.9–3.3) | 9.9 (9.3–10.6) | 11.0 (10.2–11.7) | - | |
| ISS 4–8 | 92.5 (91.8–93.1) | 77.5 (75.8–79.1) | 87.1 (86.3–87.9) | - | |
| ISS 9–15 | 2.9 (2.6–3.3) | 7.9 (6.9–8.9) | 1.6 (1.5–1.8) | - | |
| ISS 16–24 | 1.3 (1.1–1.4) | 3.9 (3.4–4.4) | 0.3 (0.2–0.4) | 84.3 (82.3–86.3) | |
| ISS 25–75 | 0.2 (0.2–0.3) | 0.7 (0.6–0.9) | 0.1 (0.0–0.1) | 15.7 (13.7–17.7) | |
| Major external cause, weighted % (95% CI) | |||||
| Fall | 47.8 (46.2–49.4) | 38.3 (36.7–40.0) | 37.0 (35.5–38.5) | 30.9 (28.4–33.4) | |
| Struck | 30.0 (29.0–31.1) | 34.1 (32.6–35.6) | 38.1 (36.7–39.5) | 10.0 (8.7–11.4) | |
| Motor vehicle crash | 6.6 (6.2–6.9) | 8.4 (7.8–9.0) | 7.3 (6.8–7.8) | 26.7 (23.7–29.8) | |
| Patient location, weighted % (95% CI) | |||||
| Large central metropolitan | 27.0 (22.7–31.2) | 22.7 (18.0–27.5) | 21.7 (17.0–26.3) | 23.7 (18.2–29.3) | |
| Large fringe metropolitan | 25.7 (22.1–29.3) | 26.0 (22.3–29.7) | 26.9 (23.1–30.8) | 20.9 (15.7–26.2) | |
| Medium metropolitan | 22.1 (18.9–25.4) | 21.6 (18.3–24.9) | 21.6 (18.4–24.9) | 21.6 (16.7–26.5) | |
| Small metropolitan | 8.4 (6.7–10.2) | 9.0 (7.2–10.8) | 8.9 (7.0–10.9) | 10.1 (7.8–12.4) | |
| Micropolitan | 11.0 (9.8–12.1) | 12.4 (11.2–13.7) | 12.5 (11.1–13.8) | 14.7 (12.2–17.2) | |
| Not metropolitan or micropolitan | 5.8 (5.2–6.5) | 8.2 (7.3–9.2) | 8.3 (7.3–9.4) | 8.9 (7.2–10.7) | |
| Primary expected payer, weighted % (95% CI) | |||||
| Medicare | 0.4 (0.1–0.6) | 0.4 (0.1–0.6) | 0.3 (0.1–0.5) | 0.3 (0.0–0.5) | |
| Medicaid | 43.1 (41.4–44.9) | 35.9 (34.1–37.7) | 33.7 (32.1–35.3) | 46.3 (42.2–50.3) | |
| Private including HMO | 46.3 (44.5–48.2) | 54.0 (52.0–55.9) | 56.1 (54.4–58.1) | 43.0 (39.0–47.1) | |
| Self-pay | 5.7 (5.4–6.1) | 5.2 (4.8–5.6) | 5.3 (4.8–5.7) | 4.2 (3.4–5.0) | |
| No charge | 0.0 (0.0–0.1) | 0.1 (0.0–0.1) | 0.1 (0.0–0.1) | 0.1 (0.0–0.2) | |
| Other | 4.4 (3.6–5.2) | 4.5 (3.8–5.2) | 4.3 (3.7–5.0) | 6.2 (3.5–8.8) | |
| Children’s hospital, weighted % (95% CI)4 | |||||
| No | 92.3 (86.2–98.4) | 89.1 (80.6–97.6) | 90.9 (83.3–98.5) | 80.2 (65.9–94.4) | |
| Yes | 7.7 (1.6–13.8) | 10.9 (2.4–19.4) | 9.1 (1.5–16.7) | 19.8 (5.6–34.1) | |
| Trauma center level designation, weighted % (95% CI) | |||||
| Non-trauma center | 37.8 (34.1–41.5) | 36.6 (32.2–41.0) | 39.5 (35.1–43.9) | 16.4 (12.7–20.2) | |
| Trauma center level I | 20.6 (15.0–26.2) | 24.9 (17.7–32.1) | 20.2 (13.5–26.9) | 53.8 (45.0–62.6) | |
| Trauma center level II | 10.9 (8.8–13.0) | 10.3 (8.2–12.4) | 10.4 (8.4–12.4) | 11.9 (8.2–15.7) | |
| Trauma center level III | 8.4 (6.8–9.9) | 8.7 (6.9–10.5) | 9.2 (7.3–11.2) | 5.2 (3.8–6.6) | |
| Non-trauma or trauma center level III, collapsed category | 17.1 (14.9–19.4) | 14.7 (12.2–17.3) | 16.0 (13.2–18.7) | 7.2 (5.7–8.8) | |
| Trauma center level I or II, collapsed category | 5.2 (3.6–6.9) | 4.8 (3.4–6.1) | 4.8 (3.5–6.0) | 5.5 (3.8–7.1) | |
| Hospital urban-rural designation, weighted % (95% CI) | |||||
| Large metropolitan areas with at least 1 million residents | 49.6 (45.3–54.0) | 46.4 (40.8–52.0) | 45.1 (39.8–50.5) | 51.4 (42.1–60.8) | |
| Small metropolitan areas with less than 1 million residents | 29.7 (26.1–33.3) | 30.9 (26.4–35.4) | 30.5 (26.6–34.4) | 35.4 (26.0–44.7) | |
| Micropolitan areas | 10.1 (8.7–11.4) | 10.4 (8.8–11.9) | 11.2 (9.6–12.9) | 5.4 (4.1–6.6) | |
| Not metropolitan or micropolitan | 4.6 (3.9–5.3) | 6.6 (5.6–7.7) | 7.3 (6.1–8.4) | 2.4 (1.9–2.9) | |
| Collapsed category of small metropolitan and micropolitan | 2.5 (1.5–3.5) | 2.2 (1.5–3.0) | 2.2 (1.4–3.0) | 2.7 (1.5–4.0) | |
| Metropolitan, collapsed category of large and small metropolitan | 2.8 (1.2–4.3) | 2.4 (1.1–3.7) | 2.5 (1.1–3.9) | 1.4 (0.6–2.2) | |
| Non-metropolitan, collapsed category of micropolitan and rural | 0.8 (0.5–1.1) | 1.1 (0.8–1.5) | 1.2 (0.8–1.6) | 1.3 (0.7–1.8) | |
| Control/ownership of hospital, weighted % (95% CI) | |||||
| Government or private, collapsed category | 68.9 (65.8–72.0) | 69.3 (65.5–73.1) | 67.0 (63.2–71.0) | 84.2 (81.1–87.4) | |
| Government, nonfederal, public | 5.5 (4.5–6.6) | 5.9 (4.7–7.1) | 6.4 (5.1–7.7) | 2.9 (2.2–3.7) | |
| Private, non-profit, voluntary | 16.0 (13.8–18.3) | 14.9 (12.2–17.6) | 16.0 (13.1–18.9) | 7.6 (6.0–9.3) | |
| Private, invest-own | 6.6 (5.5–7.7) | 5.7 (4.6–6.7) | 6.1 (5.0–7.2) | 3.3 (2.4–4.1) | |
| Private, collapsed category | 3.0 (2.5–3.5) | 4.2 (3.4–5.0) | 4.6 (3.7–5.4) | 1.9 (1.3–2.5) | |
| Region of hospital in US, weighted % (95% CI) | |||||
| Northeast | 20.6 (17.5–23.8) | 19.4 (16.0–22.7) | 20.8 (17.3–24.4) | 10.4 (6.8–13.9) | |
| Midwest | 22.9 (18.8–27.0) | 25.3 (19.8–30.7) | 25.7 (20.3–31.1) | 23.2 (15.6–30.8) | |
| South | 33.6 (29.7–37.5) | 31.9 (27.5–36.2) | 31.4 (27.3–35.4) | 36.8 (28.3–45.2) | |
| West | 22.9 (19.0–26.7) | 23.5 (18.2–28.9) | 22.1 (17.9–26.3) | 29.6 (19.3–39.9) | |
| Teaching status of hospital, weighted % (95% CI) | |||||
| Metropolitan non-teaching | 39.8 (36.0–43.5) | 36.2 (31.8–40.5) | 38.5 (34.2–42.8) | 21.2 (16.9–25.5) | |
| Metropolitan teaching | 44.8 (40.2–49.4) | 45.7 (40.0–51.5) | 41.8 (36.3–47.4) | 69.7 (63.8–75.6) | |
| Non-metropolitan | 15.5 (13.7–17.2) | 18.1 (15.8–20.4) | 19.7 (17.3–22.0) | 9.1 (7.1–11.0) | |
| Hospital Classification | No. of Hospitals in NEDS 2013 | No. of Hospitals Selected | Number of Pediatric TBIs (Excluding 959.01) 1 | Number of Pediatric Concussions | Number of Severe Pediatric TBIs | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Median | P5–P95 2 | Median | P5–P95 2 | Median | P5–P95 2 | |||||||||
| TBI ED visits > 500 | 408 | 5 | 457 | (202 | – | 1435) | 396 | (172 | – | 976) | 37 | (11 | – | 291) |
| TBI ED visits > 500 | 408 | 10 | 960 | (526 | – | 2429) | 813 | (465 | – | 1769) | 84 | (33 | – | 396) |
| TBI ED visits > 1000 | 211 | 5 | 694 | (355 | – | 2104) | 571 | (293 | – | 1503) | 67 | (22 | – | 330) |
| TBI ED visits > 1000 | 211 | 10 | 1429 | (847 | – | 3180) | 1183 | (719 | – | 2651) | 164 | (63 | – | 504) |
| Trauma center I | 49 | 5 | 1,184 | (389 | – | 3115) | 774 | (259 | – | 2334) | 251 | (67 | – | 651) |
| Trauma center I | 49 | 10 | 2493 | (1171 | – | 5190) | 1613 | (790 | – | 3778) | 522 | (209 | – | 1055) |
| Trauma center II | 46 | 5 | 657 | (394 | – | 1181) | 556 | (329 | – | 979) | 71 | (29 | – | 161) |
| Trauma center II | 46 | 10 | 1352 | (889 | – | 2067) | 1144 | (753 | – | 1717) | 147 | (79 | – | 271) |
| Pediatric hospital | 6 | 5 | 4496 | (2496 | – | 6876) | 3165 | (1691 | – | 5376) | 861 | (442 | – | 1270) |
| Adult hospital | 928 | 5 | 236 | (70 | – | 645) | 208 | (59 | – | 545) | 17 | (3 | – | 102) |
| Adult hospital | 928 | 10 | 507 | (221 | – | 1040) | 431 | (190 | – | 870) | 39 | (12 | – | 179) |
| Teaching hospital | 184 | 5 | 527 | (177 | – | 2108) | 424 | (149 | – | 1700) | 59 | (13 | – | 354) |
| Teaching hospital | 184 | 10 | 1151 | (510 | – | 2961) | 904 | (414 | – | 2335) | 153 | (39 | – | 538) |
| Non-teaching hospital | 363 | 5 | 265 | (18 | – | 1244) | 215 | (14 | – | 836) | 18 | (5 | – | 60) |
| Non-teaching hospital | 363 | 10 | 544 | (82 | – | 2011) | 425 | (64 | – | 1440) | 37 | (17 | – | 105) |
| Northeast region | 121 | 5 | 378 | (142 | – | 880) | 339 | (129 | – | 765) | 17 | (4 | – | 98) |
| Northeast region | 121 | 10 | 788 | (395 | – | 1439) | 705 | (352 | – | 1299) | 37 | (14 | – | 138) |
| Midwest region | 278 | 5 | 186 | (56 | – | 649) | 159 | (50 | – | 497) | 12 | (2 | – | 117) |
| Midwest region | 278 | 10 | 404 | (163 | – | 2087) | 348 | (145 | – | 1763) | 30 | (8 | – | 204) |
| Southern region | 358 | 5 | 220 | (62 | – | 837) | 189 | (55 | – | 633) | 18 | (4 | – | 140) |
| Southern region | 358 | 10 | 484 | (204 | – | 1295) | 411 | (172 | – | 959) | 42 | (12 | – | 294) |
| Western region | 183 | 5 | 278 | (89 | – | 1348) | 243 | (80 | – | 868) | 23 | (5 | – | 306) |
| Western region | 183 | 10 | 590 | (250 | – | 1759) | 508 | (223 | – | 1174) | 52 | (16 | – | 357) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, C.; Shi, J.; Stanley, R.M.; Sribnick, E.A.; Groner, J.I.; Xiang, H. U.S. Trends of ED Visits for Pediatric Traumatic Brain Injuries: Implications for Clinical Trials. Int. J. Environ. Res. Public Health 2017, 14, 414. https://doi.org/10.3390/ijerph14040414
Chen C, Shi J, Stanley RM, Sribnick EA, Groner JI, Xiang H. U.S. Trends of ED Visits for Pediatric Traumatic Brain Injuries: Implications for Clinical Trials. International Journal of Environmental Research and Public Health. 2017; 14(4):414. https://doi.org/10.3390/ijerph14040414
Chicago/Turabian StyleChen, Cheng, Junxin Shi, Rachel M. Stanley, Eric A. Sribnick, Jonathan I. Groner, and Henry Xiang. 2017. "U.S. Trends of ED Visits for Pediatric Traumatic Brain Injuries: Implications for Clinical Trials" International Journal of Environmental Research and Public Health 14, no. 4: 414. https://doi.org/10.3390/ijerph14040414
APA StyleChen, C., Shi, J., Stanley, R. M., Sribnick, E. A., Groner, J. I., & Xiang, H. (2017). U.S. Trends of ED Visits for Pediatric Traumatic Brain Injuries: Implications for Clinical Trials. International Journal of Environmental Research and Public Health, 14(4), 414. https://doi.org/10.3390/ijerph14040414






