A Comprehensive Evaluation of the Burden of Heat-Related Illness and Death within the Florida Population
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Defining HRI
2.3. Variable Selection
2.4. Analysis
3. Results
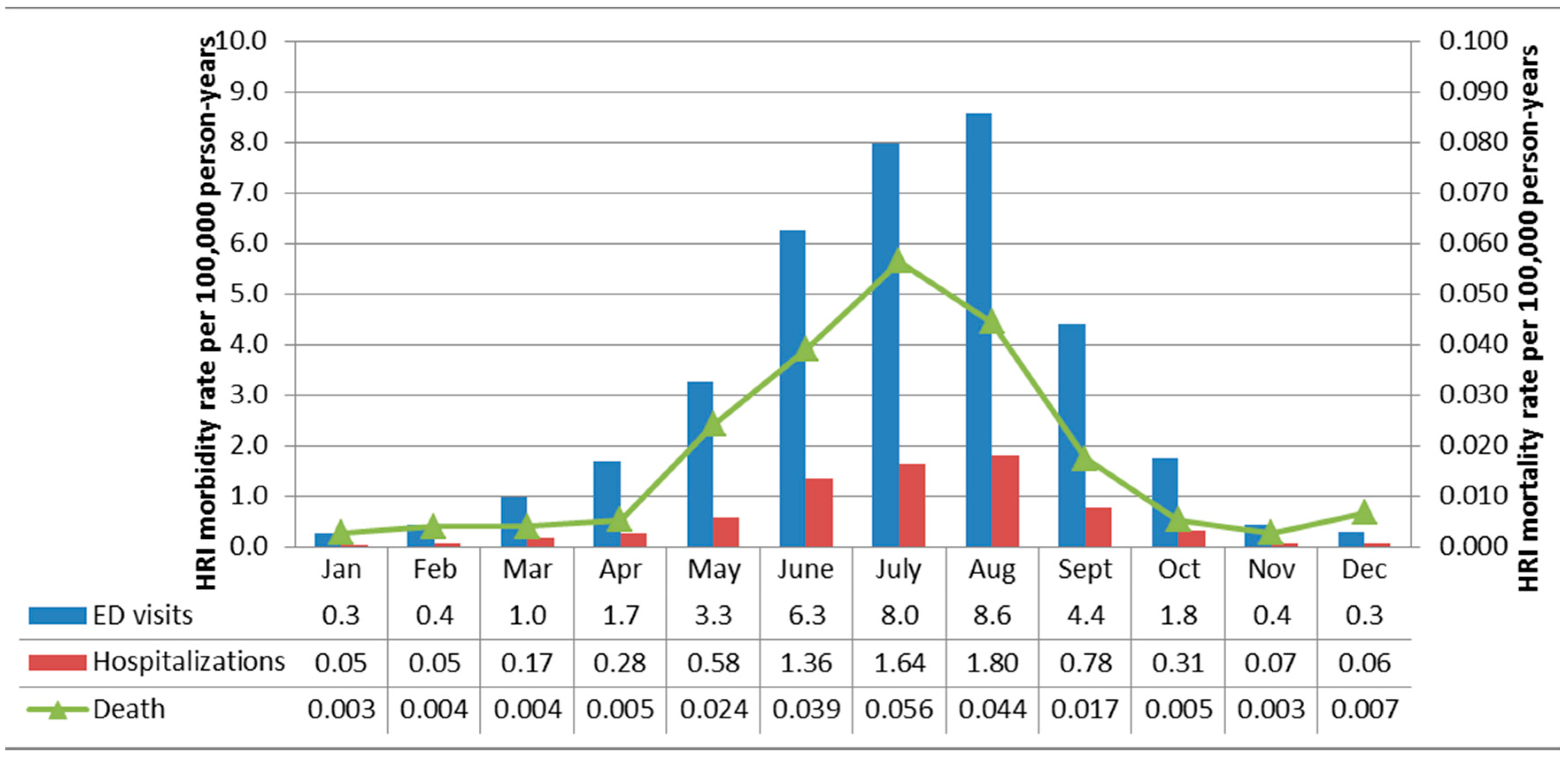
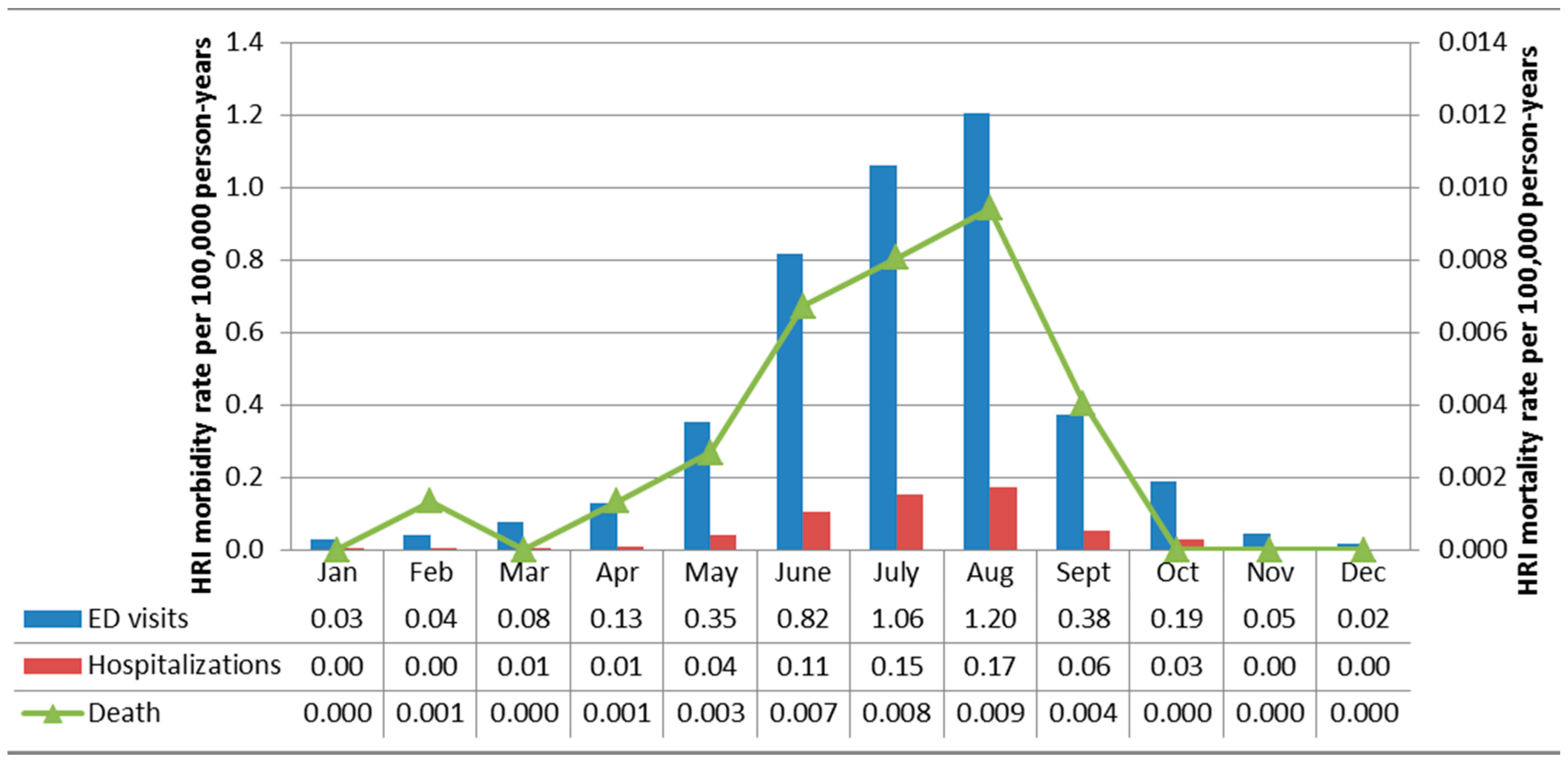
3.1. HRI Seasonality
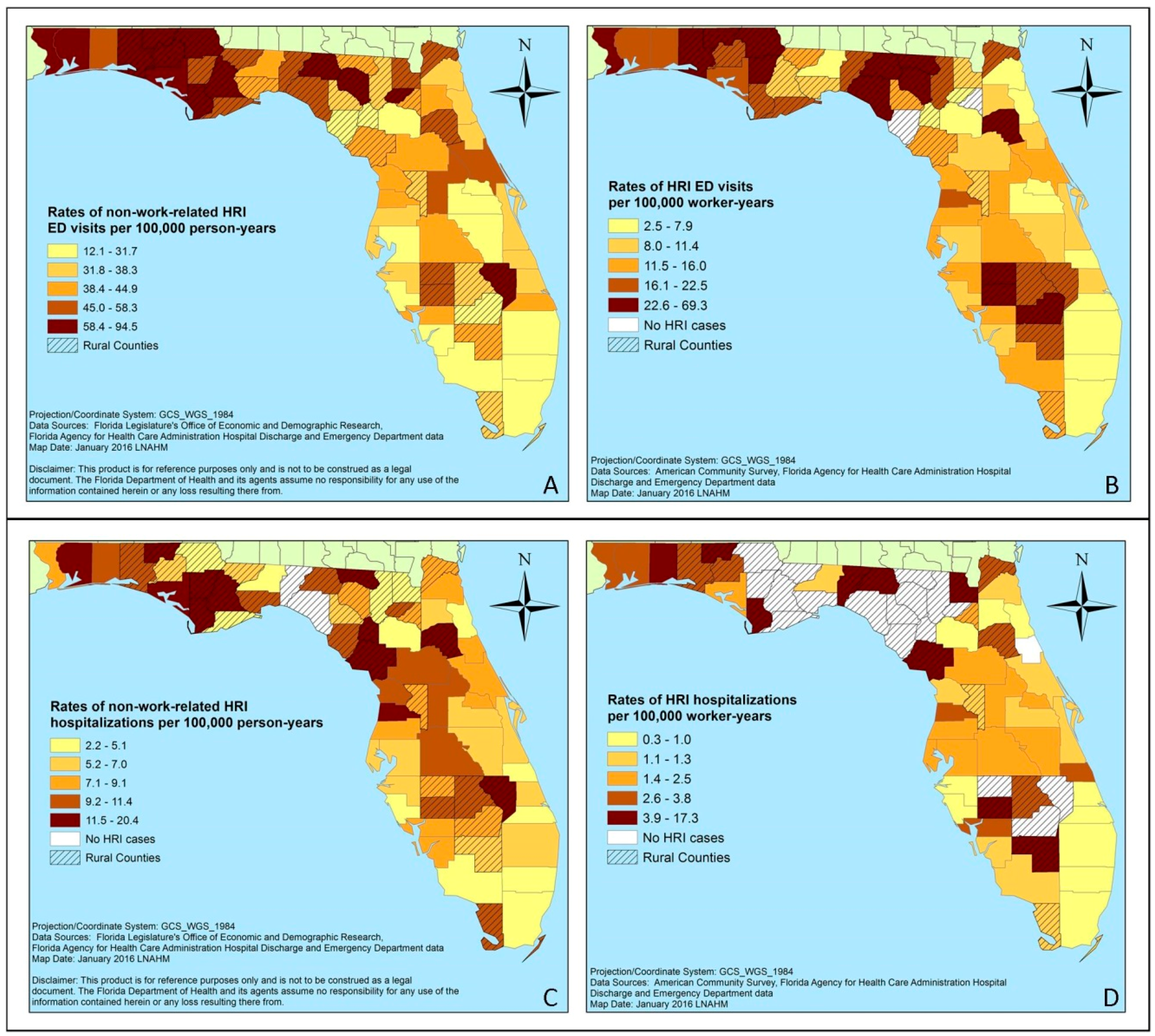
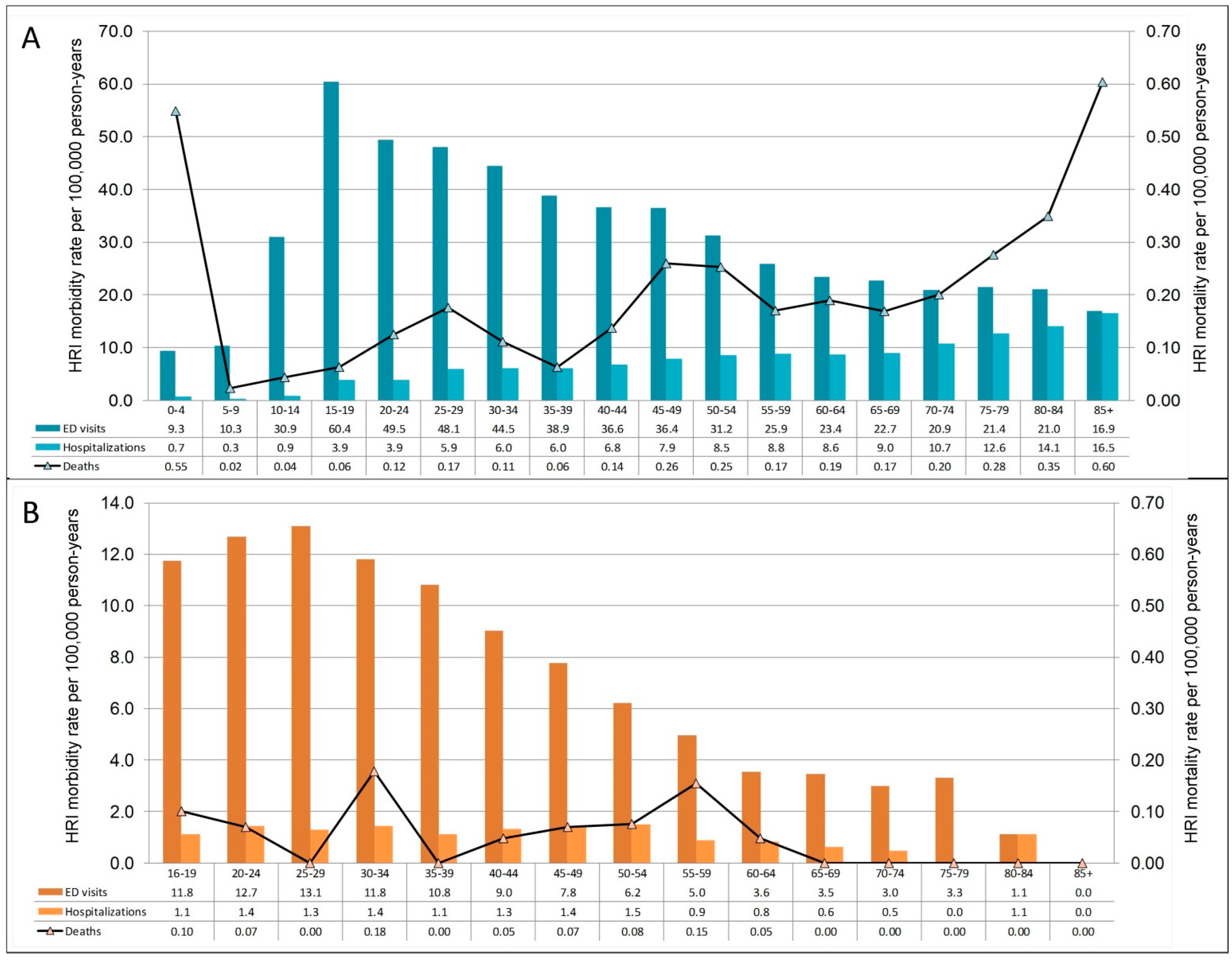
3.2. HRI Occurance
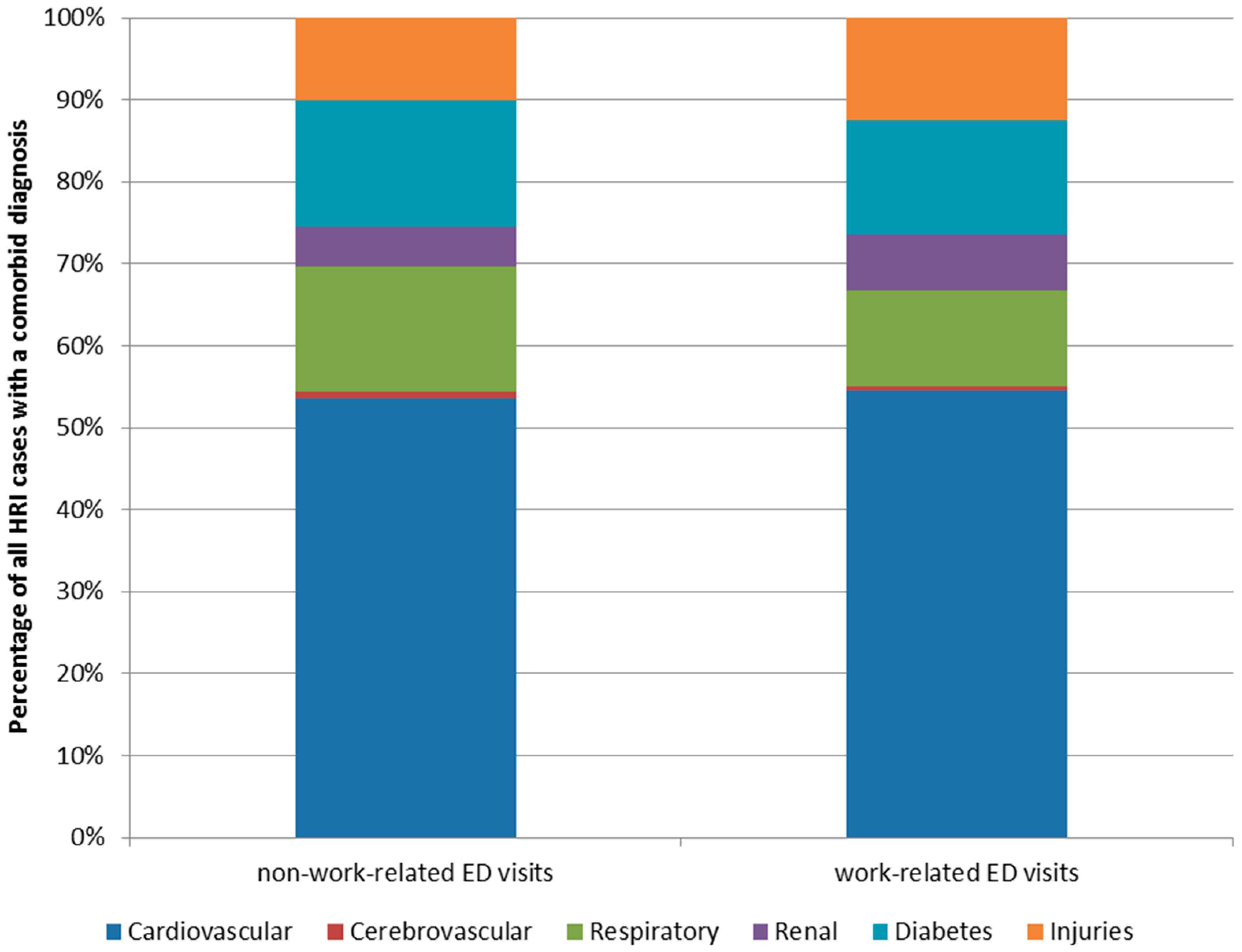
3.3. Emergency Department Visits
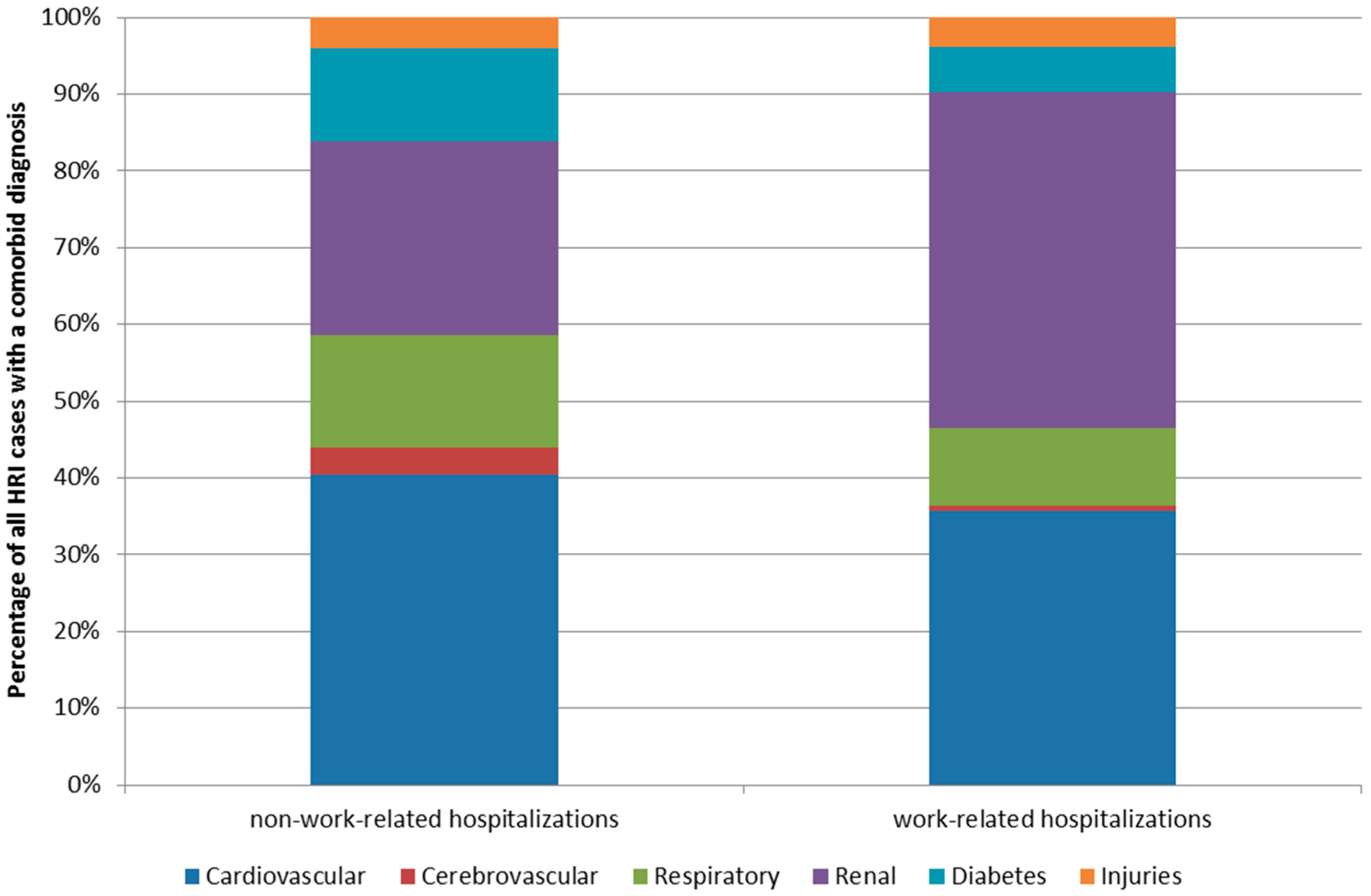
3.4. Hospitalizations
3.5. Deaths
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| ACS | American Community Survey |
| CDC | Centers for Disease Control and Prevention |
| CI | Confidence interval |
| CPS | Current Population Survey |
| Ecode | External cause of injury |
| ED | Emergency Department |
| FDOH | Florida Department of Health |
| ICD-9-CM | International Classification of Diseases, Ninth Revision, Clinical Modification |
| ICD-10 | International Classification of Diseases, Tenth Revision |
| HRI | Heat-related illness |
| LOS | Length of stay |
| RR | Rate ratio |
| SE | Standard error |
| SES | Socio-economic status |
| U.S. | United States |
References
- Hall, J.E.; Guyton, A.C. Guyton and Hall Textbook of Medical Physiology, 12th ed.; Saunders/Elsevier: Philadelphia, PA, USA, 2011. [Google Scholar]
- Lugo-Amador, N.M.; Rothenhaus, T.; Moyer, P. Heat-related illness. Emerg. Med. Clin. N. Am. 2004, 22, 315–327. [Google Scholar] [CrossRef] [PubMed]
- Simon, H.B. Hyperthermia. N. Engl. J. Med. 1993, 329, 483–487. [Google Scholar] [PubMed]
- Bouchama, A.; Knochel, J.P. Heat stroke. N. Engl. J. Med. 2002, 346, 1978–1988. [Google Scholar] [CrossRef] [PubMed]
- Epstein, Y. Heat intolerance: Predisposing factor or residual injury? Med. Sci. Sports Exerc. 1990, 22, 29–35. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, F.G.; Casa, D.J.; Bergeron, M.F.; Carter, R., 3rd; Deuster, P.; Heled, Y.; Kark, J.; Leon, L.; McDermott, B.; O’Brien, K.; et al. American college of sports medicine roundtable on exertional heat stroke--return to duty/return to play: Conference proceedings. Curr. Sports Med. Rep. 2010, 9, 314–321. [Google Scholar]
- Shapiro, Y.; Magazanik, A.; Udassin, R.; Ben-Baruch, G.; Shvartz, E.; Shoenfeld, Y. Heat intolerance in former heatstroke patients. Ann. Intern. Med. 1979, 90, 913–916. [Google Scholar] [CrossRef] [PubMed]
- Jackson, L.L.; Rosenberg, H.R. Preventing heat-related illness among agricultural workers. J. Agromed. 2010, 15, 200–215. [Google Scholar] [CrossRef] [PubMed]
- Joubert, D.; Thomsen, J.; Harrison, O. Safety in the heat: A comprehensive program for prevention of heat illness among workers in Abu Dhabi, United Arab Emirates. Am. J. Public Health 2011, 101, 395–398. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J.; Wilkinson, P.; Kovats, R.S.; Pattenden, S.; Hajat, S.; Armstrong, B.; Vajanapoom, N.; Niciu, E.M.; Mahomed, H.; Kingkeow, C.; et al. International study of temperature, heat and urban mortality: The ”isothurm“ project. Int. J. Epidemiol. 2008, 37, 1121–1131. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Heat-related deaths—Dallas, wichita, and cooke counties, texas, and united states, 1996. Morb. Mortal. Wkly. Rep. 1997, 46, 528–531. [Google Scholar]
- Romero-Lankao, P.; Qin, H.; Dickinson, K. Urban vulnerability to temperature-related hazards: A meta-analysis and meta-knowledge approach. Glob. Environ. Chang. 2012, 22, 670–683. [Google Scholar] [CrossRef]
- Kravchenko, J.; Abernethy, A.P.; Fawzy, M.; Lyerly, H.K. Minimization of heatwave morbidity and mortality. Am. J. Prev. Med. 2013, 44, 274–282. [Google Scholar] [CrossRef] [PubMed]
- Harlan, S.L.; Declet-Barreto, J.H.; Stefanov, W.L.; Petitti, D.B. Neighborhood effects on heat deaths: Social and environmental predictors of vulnerability in maricopa county, Arizona. Environ. Health Perspect. 2013, 121, 197–204. [Google Scholar] [PubMed]
- Klinenberg, E. Heat Wave: A Social Autopsy of Disaster in Chicago; University of Chicago Press: Chicago, IL, USA, 2002. [Google Scholar]
- Kerr, Z.Y.; Casa, D.J.; Marshall, S.W.; Comstock, R.D. Epidemiology of exertional heat illness among U.S. high school athletes. Am. J. Prev. Med. 2013, 44, 8–14. [Google Scholar] [CrossRef] [PubMed]
- Jay, O.; Kenny, G.P. Heat exposure in the Canadian workplace. Am. J. Ind. Med. 2010, 53, 842–853. [Google Scholar] [CrossRef] [PubMed]
- Basu, R. High ambient temperature and mortality: A review of epidemiologic studies from 2001 to 2008. Environ. Health Glob. Access Sci. Sour. 2009, 8, 40. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Samet, J.M. Relation between elevated ambient temperature and mortality: A review of the epidemiologic evidence. Epidemiol. Rev. 2002, 24, 190–202. [Google Scholar] [CrossRef] [PubMed]
- Ye, X.; Wolff, R.; Yu, W.; Vaneckova, P.; Pan, X.; Tong, S. Ambient temperature and morbidity: A review of epidemiological evidence. Environ. Health Perspect. 2012, 120, 19–28. [Google Scholar] [CrossRef] [PubMed]
- Lundgren, K.; Kuklane, K.; Gao, C.; Holmer, I. Effects of heat stress on working populations when facing climate change. Ind. Health 2013, 51, 3–15. [Google Scholar] [CrossRef] [PubMed]
- Winsberg, M.D.; Simmons, M. An Analysis of the Beginning, End, Length, and Strength of Florida’s Hot Season. Available online: http://climatecenter.fsu.edu/topics/specials/floridas-hot-season (accessed on 6 March 2015).
- Wellenius, G.A.; Burger, M.R.; Coull, B.A.; Schwartz, J.; Suh, H.H.; Koutrakis, P.; Schlaug, G.; Gold, D.R.; Mittleman, M.A. Ambient air pollution and the risk of acute ischemic stroke. Arch. Intern. Med. 2012, 172, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Yip, F.Y.; Flanders, W.D.; Wolkin, A.; Engelthaler, D.; Humble, W.; Neri, A.; Lewis, L.; Backer, L.; Rubin, C. The impact of excess heat events in Maricopa County, Arizona: 2000–2005. Int. J. Biometeorol. 2008, 52, 765–772. [Google Scholar] [CrossRef] [PubMed]
- Harduar Morano, L.; Bunn, T.L.; Lackovic, M.; Lavender, A.; Dang, G.T.; Chalmers, J.J.; Li, Y.; Zhang, L.; Flammia, D.D. Occupational heat-related illness emergency department visits and inpatient hospitalizations in the southeast region, 2007–2011. Am. J. Ind. Med. 2015, 58, 1114–1125. [Google Scholar] [CrossRef] [PubMed]
- Fechter-Leggett, E.D.; Vaidyanathan, A.; Choudhary, E. Heat stress illness emergency department visits in national environmental public health tracking states, 2005–2010. J. Community Health 2015, 41, 57–69. [Google Scholar] [CrossRef] [PubMed]
- Gubernot, D.M.; Anderson, G.B.; Hunting, K.L. The epidemiology of occupational heat exposure in the United States: A review of the literature and assessment of research needs in a changing climate. Int. J. Biometeorol. 2014, 58, 1779–1788. [Google Scholar] [CrossRef] [PubMed]
- Alamgir, H.; Koehoorn, M.; Ostry, A.; Tompa, E.; Demers, P. An evaluation of hospital discharge records as a tool for serious work related injury surveillance. Occup. Environ. Med. 2006, 63, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Koken, P.J.; Piver, W.T.; Ye, F.; Elixhauser, A.; Olsen, L.M.; Portier, C.J. Temperature, air pollution, and hospitalization for cardiovascular diseases among elderly people in Denver. Environ. Health Perspect. 2003, 111, 1312–1317. [Google Scholar] [CrossRef] [PubMed]
- Ye, F.; Piver, W.T.; Ando, M.; Portier, C.J. Effects of temperature and air pollutants on cardiovascular and respiratory diseases for males and females older than 65 years of age in Tokyo, July and August 1980–1995. Environ. Health Perspect. 2001, 109, 355–359. [Google Scholar] [CrossRef] [PubMed]
- Piver, W.T.; Ando, M.; Ye, F.; Portier, C.J. Temperature and air pollution as risk factors for heat stroke in Tokyo, July and August 1980–1995. Environ. Health Perspect. 1999, 107, 911–916. [Google Scholar] [CrossRef] [PubMed]
- Nelson, N.G.; Collins, C.L.; Comstock, R.D.; McKenzie, L.B. Exertional heat-related injuries treated in emergency departments in the U.S., 1997–2006. Am. J. Prev. Med. 2011, 40, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Stafoggia, M.; Forastiere, F.; Agostini, D.; Biggeri, A.; Bisanti, L.; Cadum, E.; Caranci, N.; de Donato, F.; De Lisio, S.; De Maria, M.; et al. Vulnerability to heat-related mortality: A multicity, population-based, case-crossover analysis. Epidemiology 2006, 17, 315–323. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Vaneckova, P.; Mengersen, K.; Pan, X.; Tong, S. Is the association between temperature and mortality modified by age, gender and socio-economic status? Sci. Total Environ. 2010, 408, 3513–3518. [Google Scholar] [CrossRef] [PubMed]
- Son, J.Y.; Lee, J.T.; Anderson, G.B.; Bell, M.L. The impact of heat waves on mortality in seven major cities in Korea. Environ. Health Perspect. 2012, 120, 566–571. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, M.S.; Zanobetti, A.; Schwartz, J. Disparities by race in heat-related mortality in four U.S. cities: The role of air conditioning prevalence. J. Urban Health Bull. N.Y. Acad. Med. 2005, 82, 191–197. [Google Scholar] [CrossRef] [PubMed]
- Knowlton, K.; Rotkin-Ellman, M.; King, G.; Margolis, H.G.; Smith, D.; Solomon, G.; Trent, R.; English, P. The 2006 California heat wave: Impacts on hospitalizations and emergency department visits. Environ. Health Perspect. 2009, 117, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Mirabelli, M.C.; Richardson, D.B. Heat-related fatalities in North Carolina. Am. J. Public Health 2005, 95, 635–637. [Google Scholar] [CrossRef] [PubMed]
- Sawaka, M.N.; Wenoer, C.B.; Pandolf, K.B. Thermoregulatory responses to acute exercise-heat stress and heat acclimation. In Handbook of Physiology: Environmental Physiology; Fregly, M.J., Blatteis, C.M., Eds.; Oxford University Press: New York, NY, USA, 1996; Volume 2, pp. 157–185. [Google Scholar]
- Gronlund, C.J. Racial and socioeconomic disparities in heat-related health effects and their mechanisms: A review. Curr. Epidemiol. Rep. 2014, 1, 165–173. [Google Scholar] [CrossRef] [PubMed]
- Cabanac, M. Heat stress and behavior. In Handbook of Physiology, Environmental Physiology; Fregly, M.J., Blatteis, C.M., Eds.; Oxford University Press: Oxford, UK, 1996; Volume 2, pp. 261–284. [Google Scholar]
- Yu, W.; Mengersen, K.; Wang, X.; Ye, X.; Guo, Y.; Pan, X.; Tong, S. Daily average temperature and mortality among the elderly: A meta-analysis and systematic review of epidemiological evidence. Int. J. Biometeorol. 2012, 56, 569–581. [Google Scholar] [CrossRef] [PubMed]
- Vandentorren, S.; Bretin, P.; Zeghnoun, A.; Mandereau-Bruno, L.; Croisier, A.; Cochet, C.; Riberon, J.; Siberan, I.; Declercq, B.; Ledrans, M. August 2003 heat wave in France: Risk factors for death of elderly people living at home. Eur. J. Public Health 2006, 16, 583–591. [Google Scholar] [CrossRef] [PubMed]
- Semenza, J.C.; Rubin, C.H.; Falter, K.H.; Selanikio, J.D.; Flanders, W.D.; Howe, H.L.; Wilhelm, J.L. Heat-related deaths during the july 1995 heat wave in Chicago. N. Engl. J. Med. 1996, 335, 84–90. [Google Scholar] [CrossRef] [PubMed]
- Bonauto, D.; Rauser, E.; Lim, L. Occupational Heat Illness in Washington State, 2000–2009; Technical Report Number 59-2-2010. Available online: http://www.lni.wa.gov/safety/research/files/occheatrelatedillnesswa20002009.pdf (accessed on 26 July 2010).
- Wu, P.C.; Lin, C.Y.; Lung, S.C.; Guo, H.R.; Chou, C.H.; Su, H.J. Cardiovascular mortality during heat and cold events: Determinants of regional vulnerability in taiwan. Occup. Environ. Med. 2011, 68, 525–530. [Google Scholar] [CrossRef] [PubMed]
- Reid, C.E.; O’Neill, M.S.; Gronlund, C.J.; Brines, S.J.; Brown, D.G.; Diez-Roux, A.V.; Schwartz, J. Mapping community determinants of heat vulnerability. Environ. Health Perspect. 2009, 117, 1730–1736. [Google Scholar] [CrossRef] [PubMed]
- Josseran, L.; Caillere, N.; Brun-Ney, D.; Rottner, J.; Filleul, L.; Brucker, G.; Astagneau, P. Syndromic surveillance and heat wave morbidity: A pilot study based on emergency departments in France. BMC Med. Inform. Decis. Mak. 2009, 9, 14. [Google Scholar] [CrossRef] [PubMed]
- Prudhomme, J.C.; Neidhardt, A. Cal/Osha Investigations of Heat Related Illnesses 2005; State of California Memorandum: Sacramento, CA, USA, 2006. [Google Scholar]
- Florida Department of Health Office of Rural Health. Rural County List. Available online: http://www.floridahealth.gov/programs-and-services/community-health/rural-health/_documents/rual-counties-2000-2010.pdf (accessed on 28 January 2015).
- Yeo, T.P. Heat stroke: A comprehensive review. AACN Clin. Issues 2004, 15, 280–293. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, J. Who is sensitive to extremes of temperature? Epidemiology 2005, 16, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Ostro, B.D. A multicounty analysis identifying the populations vulnerable to mortality associated with high ambient temperature in California. Am. J. Epidemiol. 2008, 168, 632–637. [Google Scholar] [CrossRef] [PubMed]
- Rey, G.; Jougla, E.; Fouillet, A.; Pavillon, G.; Bessemoulin, P.; Frayssinet, P.; Clavel, J.; Hemon, D. The impact of major heat waves on all-cause and cause-specific mortality in France from 1971 to 2003. Int. Arch. Occup. Environ. Health 2007, 80, 615–626. [Google Scholar] [CrossRef] [PubMed]
- Keatinge, W.R.; Coleshaw, S.R.; Easton, J.C.; Cotter, F.; Mattock, M.B.; Chelliah, R. Increased platelet and red cell counts, blood viscosity, and plasma cholesterol levels during heat stress, and mortality from coronary and cerebral thrombosis. Am. J. Med. 1986, 81, 795–800. [Google Scholar] [CrossRef]
- Noakes, T.D. A modern classification of the exercise-related heat illnesses. J. Sci. Med. Sport Sports Med. Aust. 2008, 11, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Kenny, G.P.; Yardley, J.; Brown, C.; Sigal, R.J.; Jay, O. Heat stress in older individuals and patients with common chronic diseases. Can. Med. Assoc. J. 2010, 182, 1053–1060. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, L.E.; Casa, D.J.; Millard-Stafford, M.; Moran, D.S.; Pyne, S.W.; Roberts, W.O.; American College of Sports Medicine. American College of Sports Medicine position stand. Exertional heat illness during training and competition. Med. Sci. Sports Exerc. 2007, 39, 556–572. [Google Scholar] [CrossRef] [PubMed]
- Yardley, J.E.; Stapleton, J.M.; Carter, M.R.; Sigal, R.J.; Kenny, G.P. Is whole-body thermoregulatory function impaired in type 1 diabetes mellitus? Curr. Diabetes Rev. 2013, 9, 126–136. [Google Scholar] [CrossRef] [PubMed]
- Anderson, B.G.; Bell, M.L. Weather-related mortality: How heat, cold, and heat waves affect mortality in the United States. Epidemiology 2009, 20, 205–213. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Occupational Safety and Health. Heat Stress. Available online: http://www.cdc.gov/niosh/topics/heatstress/ (accessed on 20 Feburary 2013).
- Morabito, M.; Cecchi, L.; Crisci, A.; Modesti, P.A.; Orlandini, S. Relationship between work-related accidents and hot weather conditions in Tuscany (Central Italy). Ind. Health 2006, 44, 458–464. [Google Scholar] [CrossRef] [PubMed]
- Fogleman, M.; Fakhrzadeh, L.; Bernard, T.E. The relationship between outdoor thermal conditions and acute injury in an aluminum smelter. Int. J. Ind. Ergon. 2005, 35, 47–55. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Warning Signs and Symptoms of Heat-Related Illness. Available online: http://www.cdc.gov/extremeheat/warning.html (accessed on 26 May 2015).
- Occupational Safety & Health Administration. Occupational Heat Exposure: Heat Illness and First Aid. Available online: https://www.osha.gov/SLTC/heatstress/heat_illnesses.html (accessed on 27 May 2015).
- Rhea, S.; Ising, A.; Fleischauer, A.T.; Deyneka, L.; Vaughan-Batten, H.; Waller, A. Using near real-time morbidity data to identify heat-related illness prevention strategies in North Carolina. J. Community Health 2012, 37, 495–500. [Google Scholar] [CrossRef] [PubMed]
- The Bureau of Epidemiology and Disease Control Office of Environmental Health; Bureau of Public Health Statistics Health Status and Vital Statistics Section. Trends in Morbidity and Mortality from Exposure to Excessive Natural Heat in Arizona, 2012 Report; Arizona Department of Health and Human Services: Phoenix, Arizona, 2014. [Google Scholar]
- Carter, R., 3rd; Cheuvront, S.N.; Williams, J.O.; Kolka, M.A.; Stephenson, L.A.; Sawka, M.N.; Amoroso, P.J. Epidemiology of hospitalizations and deaths from heat illness in soldiers. Med. Sci. Sports Exerc. 2005, 37, 1338–1344. [Google Scholar] [CrossRef] [PubMed]
- Kark, J.A.; Burr, P.Q.; Wenger, C.B.; Gastaldo, E.; Gardner, J.W. Exertional heat illness in marine corps recruit training. Aviat. Space Environ. Med. 1996, 67, 354–360. [Google Scholar] [PubMed]
- Bonauto, D.; Anderson, R.; Rauser, E.; Burke, B. Occupational heat illness in Washington State, 1995–2005. Am. J. Ind. Med. 2007, 50, 940–950. [Google Scholar] [CrossRef] [PubMed]
- Gubernot, D.M.; Anderson, G.B.; Hunting, K.L. Characterizing occupational heat-related mortality in the United States, 2000–2010: An analysis using the census of fatal occupational injuries database. Am. J. Ind. Med. 2015, 58, 203–211. [Google Scholar] [CrossRef] [PubMed]
- Hess, J.J.; Saha, S.; Luber, G. Summertime acute heat illness in U.S. emergency departments from 2006 through 2010: Analysis of a nationally representative sample. Environ. Health Perspect. 2014, 122, 1209–1215. [Google Scholar] [CrossRef] [PubMed]
- Pillai, S.K.; Noe, R.S.; Murphy, M.W.; Vaidyanathan, A.; Young, R.; Kieszak, S.; Freymann, G.; Smith, W.; Drenzek, C.; Lewis, L.; et al. Heat illness: Predictors of hospital admissions among emergency department visits-georgia, 2002–2008. J. Community Health 2014, 39, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Choudhary, E.; Vaidyanathan, A. Heat stress illness hospitalizations—Environmental public health tracking program, 20 states, 2001–2010. Morb. Mortal. Wkly. Rep. Surveill. Summ. 2014, 63, 1–10. [Google Scholar]
- Winsberg, M.D. Florida Weather, 2nd ed.; University Press of Florida: Gainesville, FL, USA, 2003. [Google Scholar]
- Florida Department of Agriculture and Consumer Services. Florida Agricultural Statistical Directory; Florida Department of Agriculture and Consumer Services: Tallahassee, FL, USA, 2009. [Google Scholar]
- Calvin, L.; Philip, M. The U.S. Produce Industry and Labor: Facing the Future in a Global Economy; U.S. Department of Agriculture Economic Research Service: Washington, DC, USA, 2010. [Google Scholar]
- Sheridan, S.C.; Dolney, T.J. Heat, mortality, and level of urbanization: Measuring vulnerability across Ohio, USA. Clim. Res. 2003, 24, 255–265. [Google Scholar] [CrossRef]
- Prudhomme, J.C.; Neidhardt, A. Cal/Osha Investigations of Heat Related Illnesses 2006; State of California Memorandum: Sacramento, CA, USA, 2007. [Google Scholar]
- Kovach, M.M.; Konrad, C.E.; Fuhrmann, C.M. Area-level risk factors for heat-related illness in rural and urban locations across North Carolina, USA. Appl. Geogr. 2015, 60, 175–183. [Google Scholar] [CrossRef]
- US EPA Climate Protection Partnership Division. Reducing Urban Heat Islands: Compendium of Strategies; Office of Atmospheric Programs: Washington, DC, USA, 2008. [Google Scholar]
- Hajat, S.; Kovats, R.S.; Lachowycz, K. Heat-related and cold-related deaths in England and Wales: Who is at risk? Occup. Environ. Med. 2007, 64, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Heat-related illnesses, deaths, and risk factors—Cincinnati and Dayton, Ohio, 1999, and United States, 1979–1997. Morb. Mortal. Wkly. Rep. 2000, 49, 470–473. [Google Scholar]
- Centers for Disease Control Prevention. Heat-related deaths—United States, 1999–2003. Morb. Mortal. Wkly. Rep. 2006, 55, 796–798. [Google Scholar]
- Basagana, X.; Sartini, C.; Barrera-Gomez, J.; Dadvand, P.; Cunillera, J.; Ostro, B.; Sunyer, J.; Medina-Ramon, M. Heat waves and cause-specific mortality at all ages. Epidemiology 2011, 22, 765–772. [Google Scholar] [CrossRef] [PubMed]
- Grubenhoff, J.A.; du Ford, K.; Roosevelt, G.E. Heat-related illness. Clin. Pediatr. Emerg. Med. 2007, 8, 59–64. [Google Scholar] [CrossRef]
- Bureau of Labor Statistics. 2009 Annual Averages—Household Data—Tables from Employment and Earnings. Available online: http://www.bls.gov/cps/cps_aa2009.htm (accessed on 10 March 2014).
- Medina-Ramon, M.; Zanobetti, A.; Cavanagh, D.P.; Schwartz, J. Extreme temperatures and mortality: Assessing effect modification by personal characteristics and specific cause of death in a multi-city case-only analysis. Environ. Health Perspect. 2006, 114, 1331–1336. [Google Scholar] [CrossRef] [PubMed]
- D’Ippoliti, D.; Michelozzi, P.; Marino, C.; de’Donato, F.; Menne, B.; Katsouyanni, K.; Kirchmayer, U.; Analitis, A.; Medina-Ramon, M.; Paldy, A.; et al. The impact of heat waves on mortality in 9 European cities: Results from the euroheat project. Environ. Health Glob. Access Sci. Sour. 2010, 9, 37. [Google Scholar] [CrossRef] [PubMed]
- Mississippi State Department of Health. Heat-Related Illness; Mississippi State Department of Health: Jackson, MS, USA, 2008; Volume 24. [Google Scholar]
- Culp, K.; Tonelli, S.; Ramey, S.L.; Donham, K.; Fuortes, L. Preventing heat-related illness among Hispanic farmworkers. AAOHN J. 2011, 59, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Utterback, D.F.; Schnorr, T.M. Use of Workers’ Compensation Data for Occupational Injury & Illness Prevention; Department of Health and Human Services, Centers for Disease Control, National Institute for Occupational Safety and Health: Cincinnati, OH, USA, 2010. [Google Scholar]
- Brown, A.; Lopez, M.H. Mapping the Latino population, by state, county, and city. In Pew Research Center’s Hispanic Trends Project; PewResearchCenter: Washington, DC, USA, 2013. [Google Scholar]
- Pew Research Center’s Hispanic Trends Project. Population Distribution of Hispanic Origin Groups by County, 2010; PewResearchCenter: Washington, DC, USA, 2012. [Google Scholar]
- Xiang, J.; Bi, P.; Pisaniello, D.; Hansen, A. Health impacts of workplace heat exposure: An epidemiological review. Ind. Health 2014, 52, 91–101. [Google Scholar] [CrossRef] [PubMed]
- Emrich, C.T.; Morath, D.P.; Morath, G.C.; Reeves, R. Climate-Sensitive Hazards in Florida: Identifying and Prioritizing Threats to Build Resilience against Climate Effects; Hazard and Vulnerability Research Institute: Columbia, SC, USA, 2014. [Google Scholar]
- Xiang, J.; Hansen, A.; Pisaniello, D.; Bi, P. Extreme heat and occupational heat illnesses in South Australia, 2001–2010. Occup. Environ. Med. 2015, 72, 580–586. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A.; Armstrong, B.; Kovats, S.; Wilkinson, P. The effect of high temperatures on cause-specific mortality in England and Wales. Occup. Environ. Med. 2012, 69, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Gosling, S.N.; Lowe, J.A.; McGregor, G.R.; Pelling, M.; Malamud, B.D. Associations between elevated atmospheric temperature and human mortality: A critical review of the literature. Clim. Chang. 2008, 92, 299–341. [Google Scholar] [CrossRef]
- Basu, R.; Feng, W.Y.; Ostro, B.D. Characterizing temperature and mortality in nine California counties. Epidemiology 2008, 19, 138–145. [Google Scholar] [CrossRef] [PubMed]
- Johnson, R.F.; Kobrick, J.L. Psychological aspects of military performance in hot environments. In Medical Aspects of Harsh Environments; Pandolf, K.B., Burr, R.E., Wenger, C.B., Office of the Surgeon General, United States Department of the Army, Eds.; Office of The Surgeon General, Department of the Army, United States of America: Washington, DC, USA, 2001; Volume 1, pp. 135–159. [Google Scholar]
- Dixon, D. Florida Tourism Numbers Break Records Again for the Third Quarter of This Year. Available online: http://jacksonville.com/news/metro/2015-11-19/story/florida-tourism-numbers-break-records-again-third-quarter-year (accessed on 12 February 2016).
- U.S. Census Bureau. Longitudinal Employer Household Dynamics Survey Accessed via on the Map Application and LEHD Origin-Destination Employment Statistics (2005–2014). Available online: http://onthemap.ces.census.gov/ (accessed on 10 April 2016).
- Davis, L.K.; Hunt, P.R.; Hackman, H.H.; McKeown, L.N.; Ozonoff, V.V. Use of statewide electronic emergency department data for occupational injury surveillance: A feasibility study in Massachusetts. Am. J. Ind. Med. 2012, 55, 344–352. [Google Scholar] [CrossRef] [PubMed]
- Groenewold, M.R.; Baron, S.L. The proportion of work-related emergency department visits not expected to be paid by workers’ compensation: Implications for occupational health surveillance, research, policy, and health equity. Health Serv. Res. 2013, 48, 1939–1959. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Proportion of workers who were work-injured and payment by workers’ compensation systems—10 states, 2007. Morb. Mortal. Wkly. Rep. 2010, 59, 897–900. [Google Scholar]
- Shen, T.; Howe, H.L.; Alo, C.; Moolenaar, R.L. Toward a broader definition of heat-related death: Comparison of mortality estimates from medical examiners’ classification with those from total death differentials during the July 1995 heat wave in Chicago, Illinois. Am. J. Forensic Med. Pathol. 1998, 19, 113–118. [Google Scholar] [CrossRef] [PubMed]
- Luber, G.; McGeehin, M. Climate change and extreme heat events. Am. J. Prev. Med. 2008, 35, 429–435. [Google Scholar] [CrossRef] [PubMed]
- Hajat, S.; Kosatky, T. Heat-related mortality: A review and exploration of heterogeneity. J. Epidemiol. Community Health 2010, 64, 753–760. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.; Cody, S. Methodology for Constructing Estimates of Total Population for Counties and Subcounty Areas in Florida; Bureau of Economic and Business Research, University of Florida: Gainesville, FL, USA, 2014. [Google Scholar]
| ICD-9-CM | Definition |
|---|---|
| - | Principal payer is workers’ compensation |
| E000.0 | Civilian activity done for income or pay |
| E000.1 | Military activity |
| E800-E807 | Railway accident among railway employee (4th digit = 0) |
| E830-E838 | Water transport accident among crew, dockers and stevedores (4th digit = 2 or 6) |
| E840-E845 | Air and space transport accidents among crew and ground crew (4th digit = 2 or 8) |
| E846 | Accidents involving powered vehicles used solely within the buildings and premises of industrial or commercial establishment |
| E849.1 | Place of occurrence: farm building/land under cultivation |
| E849.2 | Place of occurrence: mine or quarry |
| E849.3 | Place of occurrence: industrial place and premises |
| Characteristic | Florida Residents | HRI ED Visits | HRI Hospitalizations | HRI Deaths | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N (%) | N (%) | Rate * | Rate Ratio (95% CI) | N (%) | Rate * | Rate Ratio (95% CI) | N (%) | Rate * | Rate Ratio (95% CI) | |
| Gender | ||||||||||
| Male | 72,742,430 (48.9) | 17,405 (72.6) | 47.85 | 2.77 (2.69, 2.85) | 3807 (79) | 10.47 | 3.94 (3.68, 4.23) | 94 (67.6) | 0.26 | 2.18 (1.53, 3.11) |
| Female | 76,018,379 (51.1) | 6576 (27.4) | 17.30 | Reference | 1009 (21) | 2.65 | Reference | 45 (32.4) | 0.12 | Reference |
| Race † | ||||||||||
| White | 117,671,057 (79.1) | 17,511 (73.5) | 29.76 | Reference | 3649 (76.5) | 6.20 | Reference | 101 (72.7) | 0.17 | Reference |
| Black | 24,114,183 (16.2) | 5129 (21.5) | 42.54 | 1.43 (1.39, 1.47) | 870 (18.2) | 7.22 | 1.16 (1.08, 1.25) | 36 (25.9) | 0.30 | 1.74 (1.19, 2.54) |
| Other | 6,975,569 (4.7) | 1182 (5) | 33.89 | 1.14 (1.07, 1.21) | 253 (5.3) | 7.25 | 1.17 (1.03, 1.33) | 2 (1.4) | 0.06 | 0.33 (0.08, 1.35) |
| Ethnicity ‡ | ||||||||||
| Non-Hispanic | 116,393,541 (78.2) | 21,033 (88.6) | 36.14 | Reference | 4194 (88.3) | 7.21 | Reference | 124 (89.2) | 0.21 | Reference |
| Hispanic | 32,367,268 (21.8) | 2716 (11.4) | 16.78 | 0.46 (0.45, 0.48) | 557 (11.7) | 3.44 | 0.48 (0.44, 0.52) | 15 (10.8) | 0.09 | 0.44 (0.25, 0.74) |
| Rural/Urban | ||||||||||
| Urban | 139,458,520 (93.7) | 21,636 (90.2) | 31.03 | Reference | 4379 (90.9) | 6.28 | Reference | 127 (91.4) | 0.18 | Reference |
| Rural | 9,302,289 (6.3) | 2345 (9.8) | 50.42 | 1.62 (1.56, 1.70) | 437 (9.1) | 9.40 | 1.50 (1.36, 1.65) | 12 (8.6) | 0.26 | 1.42 (0.78, 2.56) |
| Characteristic | Florida Residents | HRI ED Visits | HRI Hospitalizations | HRI Deaths | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N (%) | N (%) | Rate * | Rate Ratio (95% CI) | N (%) | Rate * | Rate Ratio (95% CI) | N (%) | Rate * | Rate Ratio (95% CI) | |
| Gender | ||||||||||
| Male | 35,690,570 (52.7) | 2586 (86.8) | 14.49 | 5.91 (5.32, 6.58) | 396 (95.4) | 2.22 | 18.73 (11.82, 29.69) | 22 (95.7) | 0.12 | 19.77 (2.67, 146.71) |
| Female | 32,080,314 (47.3) | 393 (13.2) | 2.45 | Reference | 19 (4.6) | 0.12 | Reference | 1 (4.3) | 0.01 | Reference |
| Race † | ||||||||||
| White | 55,638,157 (82.1) | 2348 (79.3) | 8.44 | Reference | 298 (72) | 1.07 | Reference | 16 (69.6) | 0.06 | Reference |
| Black | 9,547,987 (14.1) | 474 (16) | 9.93 | 1.18 (1.07, 1.3) | 88 (21.3) | 1.84 | 1.72 (1.36, 2.18) | 7 (30.4) | 0.15 | 2.55 (1.05, 6.2) |
| Other | 2,584,739 (3.8) | 138 (4.7) | 10.68 | 1.27 (1.07, 1.5) | 28 (6.8) | 2.17 | 2.02 (1.37, 2.98) | (0) | 0.00 | - |
| Ethnicity ‡ | ||||||||||
| Non-Hispanic | 53,220,195 (78.5) | 2560 (86.8) | 9.62 | Reference | 324 (78.5) | 1.22 | Reference | 14 (60.9) | 0.05 | Reference |
| Hispanic | 14,550,689 (21.5) | 389 (13.2) | 5.35 | 0.56 (0.5, 0.62) | 89 (21.5) | 1.22 | 1.00 (0.79, 1.27) | 9 (39.1) | 0.12 | 2.35 (1.02, 5.43) |
| Rural/Urban | ||||||||||
| Urban | 62,309,645 (93.7) | 2613 (87.7) | 8.39 | Reference | 366 (88.2) | 1.17 | Reference | 21 (91.3) | 0.07 | Reference |
| Rural | 3,479,229 (6.3) | 366 (12.3) | 21.04 | 2.51 (2.25, 2.8) | 49 (11.8) | 2.82 | 2.4 (1.78, 3.23) | 2 (8.7) | 0.11 | 1.71 (0.40, 7.27) |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Harduar Morano, L.; Watkins, S.; Kintziger, K. A Comprehensive Evaluation of the Burden of Heat-Related Illness and Death within the Florida Population. Int. J. Environ. Res. Public Health 2016, 13, 551. https://doi.org/10.3390/ijerph13060551
Harduar Morano L, Watkins S, Kintziger K. A Comprehensive Evaluation of the Burden of Heat-Related Illness and Death within the Florida Population. International Journal of Environmental Research and Public Health. 2016; 13(6):551. https://doi.org/10.3390/ijerph13060551
Chicago/Turabian StyleHarduar Morano, Laurel, Sharon Watkins, and Kristina Kintziger. 2016. "A Comprehensive Evaluation of the Burden of Heat-Related Illness and Death within the Florida Population" International Journal of Environmental Research and Public Health 13, no. 6: 551. https://doi.org/10.3390/ijerph13060551
APA StyleHarduar Morano, L., Watkins, S., & Kintziger, K. (2016). A Comprehensive Evaluation of the Burden of Heat-Related Illness and Death within the Florida Population. International Journal of Environmental Research and Public Health, 13(6), 551. https://doi.org/10.3390/ijerph13060551





