Flood-Exposure is Associated with Higher Prevalence of Child Undernutrition in Rural Eastern India
Abstract
:1. Introduction
2. Materials and Methods
2.1. Analysis Plan
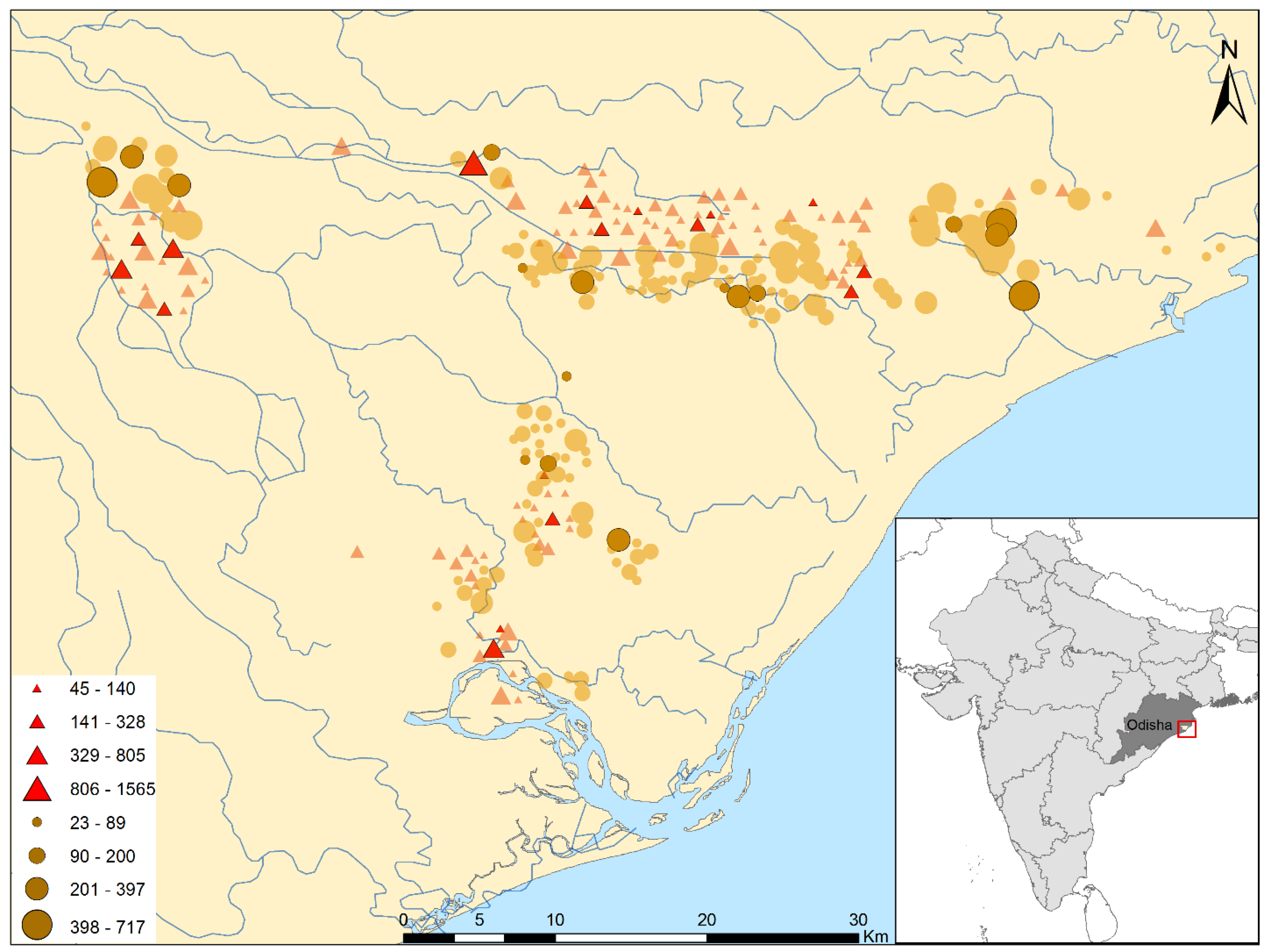
2.2. Exposure Data
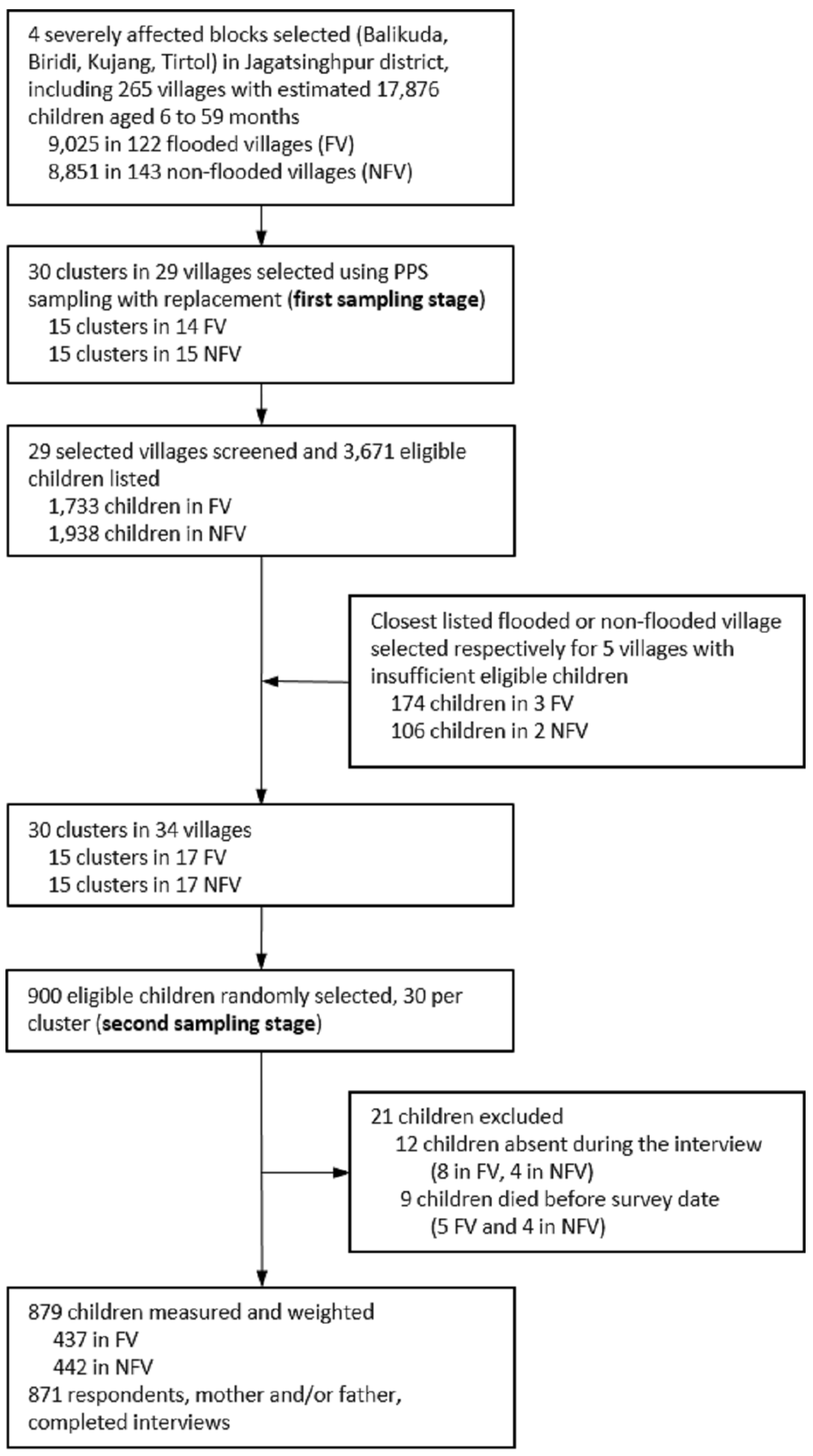
2.3. Study Design and Participants
2.4. Ethical Considerations
2.5. Procedures
2.6. Statistical Methods
2.7. Estimates of Population Size
3. Results
3.1. Sample and Determinants of Child Undernutrition in Flooded and Non-Flooded Communities
3.2. Effect of Floods on Child Undernutrition
3.3. Effect of Age on Undernutrition
| Variables | Flooded (n = 370) | Non-Flooded (n = 394) | |||
|---|---|---|---|---|---|
| n | % (95% CI) | n | % (95% CI) | p | |
| Child characteristics | |||||
| Child female | 171 | 44.8 (38.7, 50.8) | 179 | 44.9 (39.1, 50.1) | 0.97 |
| Mean birthweight, g 1 | 370 | 2783.6 (2734.3, 2832.9) | 394 | 2748 (2707.2, 2788.7) | 0.28 |
| Child age, months | 0.16 | ||||
| 6–11 | 38 | 8.5 (5.8, 11.2) | 47 | 12.0 (8.4, 15.5) | |
| 12–23 | 85 | 25.1 (19.5, 30.7) | 100 | 24.3 (19.4, 29.3) | |
| 24–35 | 74 | 19.7 (15.0, 24.5) | 81 | 21.4 (16.3, 26.5) | |
| 36–47 | 89 | 24.6 (19.2, 30.0) | 69 | 17.1 (13.0, 21.2) | |
| 48–59 | 84 | 22.0 (17.0, 27.1) | 97 | 25.2 (20.0, 30.5) | |
| Immediate Causes | |||||
| Dietary intake | |||||
| Household did experience food shortage due to 2008 flood | 314 | 86.4 (82.4, 90.3) | 56 | 5.6 (3.3, 7.9) | <0.0001 |
| Mean number of daily meals (last week) 2 | 370 | 2.07 (2.04, 2.09) | 394 | 2.05 (2.02, 2.08) | 0.37 |
| Mean weekly vegetable consumption (last week) 3 | 370 | 7.7 (7.3, 8.0) | 394 | 7.5 (7.1, 7.8) | 0.40 |
| Child’s disease | |||||
| Diarrhea (last two weeks) | 127 | 33.5 (27.9, 39.2) | 113 | 28.2 (22.8, 33.5) | 0.18 |
| Respiratory symptoms (last two weeks) | 207 | 58.6 (52.7, 64.6) | 199 | 47.3 (41.4, 53.1) | 0.007 |
| Underlying Causes | |||||
| Food insecurity (related to flood in 2008) | |||||
| Crop washed away | 157 | 48.9 (42.8, 55.1) | 0 | 0.0 (0.0, 0.0) | <0.0001 |
| Lack of earning opportunities | 50 | 13.5 (9.7, 17.3) | 0 | 0.0 (0.0, 0.0) | <0.0001 |
| Increase in food price | 37 | 7.9 (4.9, 10.9) | 9 | 2.0 (0.7, 3.4) | <0.001 |
| Grain stock washed away | 26 | 5.9 (3.5, 8.3) | 0 | 0.0 (0.0, 0.0) | <0.0001 |
| Food unavailable in market | 26 | 5.6 (3.4, 7.8) | 15 | 3.6 (1.7, 5.4) | 0.17 |
| Household members migrated | 16 | 4.1 (2.1, 6.1) | 0 | 0.0 (0.0, 0.0) | <0.0001 |
| Care of mother and children | |||||
| Mean age at marriage of the mother, y 4 | 370 | 21.9 (21.6, 22.3) | 394 | 21.5 (21.2, 21.9) | 0.10 |
| Mean age of the mother at first delivery, y 5 | 370 | 23.7 (23.4, 24.1) | 394 | 23.4 (23.1, 23.8) | 0.19 |
| Mean age of the mother at birth of child, y 6 | 370 | 26.1 (25.7, 26.5) | 394 | 25.9 (25.5, 26.3) | 0.55 |
| Mean age of the father at birth of child, y 7 | 370 | 31.3 (30.8, 31.8) | 394 | 31.1 (30.6, 31.7) | 0.61 |
| Two or more children underfive eating from same kitchen | 142 | 38.0 (32.1, 43.9) | 168 | 39.8 (34.2, 45.4) | 0.66 |
| Mean number of child visits to ICDS (last month) 8 | 370 | 1.2 (0.9, 1.5) | 394 | 1.2 (0.9, 1.5) | 0.96 |
| Mother was a member of self-help group/Mahila Mandal | 68 | 17.8 (13.6, 22.0) | 70 | 17.1 (13.0, 21.2) | 0.82 |
| Mean number of mother’s conceptions 9 | 370 | 1.9 (1.8, 2.1) | 394 | 2.0 (1.9, 2.1) | 0.51 |
| Mother had one or more miscarriages, stillbirths | 50 | 12.8 (9.0, 16.7) | 61 | 15.5 (11.1, 19.9) | 0.37 |
| Child received deworming treatment in past 6 months | 132 | 35.8 (29.9, 41.6) | 145 | 37.3 (31.5, 43.0) | 0.72 |
| Child breastfed at least 2 years | 123 | 31.9 (26.3, 37.5) | 131 | 35.0 (29.3, 40.7) | 0.65 |
| Supplementary feeding started after 6 months of child’s age | 251 | 66.8 (60.9, 72.8) | 265 | 68.7 (63.3, 74.0) | 0.65 |
| Child breastfed at least 2 years and supplemented after 6 months of age | 81 | 20.7 (15.9, 25.4) | 98 | 26.7 (21.3, 32.1) | 0.10 |
| Mother washes hands with soap before feeding child | 72 | 17.5 (13.1, 21.9) | 82 | 22.7 (17.3, 28.0) | 0.14 |
| Mother washes hands with soap before preparing food for the family | 51 | 12.4 (8.5, 16.3) | 68 | 19.5 (14.2, 24.7) | 0.035 |
| Mother washes hands with soap before lunch | 71 | 18.5 (13.9, 23.2) | 80 | 21.9 (16.5, 27.2) | 0.36 |
| Mother washes hands with soap after attending the child who defecated | 121 | 29.2 (23.9, 34.5) | 121 | 31.9 (26.1, 37.6) | 0.51 |
| Child received BCG vaccine | 254 | 66.4 (60.4, 72.3) | 274 | 68.4 (62.8, 74.1) | 0.62 |
| Child received measles vaccine | 224 | 58.8 (52.7, 64.9) | 232 | 57.9 (52.1, 63.8) | 0.84 |
| Child received all three doses of polio vaccine | 245 | 64.4 (58.4, 70.4) | 260 | 65.9 (60.2, 71.6) | 0.73 |
| Child received all three doses of B-hepatitis vaccine | 41 | 10.6 (6.9, 14.4) | 35 | 8.9 (5.8, 12.1) | 0.50 |
| Child received all three doses of DPT vaccine | 247 | 64.8 (58.8, 70.8) | 261 | 66.1 (60.4, 71.8) | 0.76 |
| Public health | |||||
| Improved latrine (before floods) | 126 | 32.6 (26.7, 38.4) | 341 | 86.4 (81.9, 90.9) | <0.0001 |
| Improved latrine (after floods) | 58 | 13.3 (9.4, 17.2) | 341 | 86.4 (81.9, 90.9) | <0.0001 |
| Improved drinking water (before floods) | 361 | 98.2 (97.0, 99.4) | 341 | 86.7 (83.0, 90.3) | <0.0001 |
| Improved drinking water (after floods) | 232 | 60.6 (54.5, 66.8) | NA | NA | NA |
| Mother gave birth at hospital | 306 | 84.2 (80.1, 88.4) | 324 | 82.4 (78.2, 86.6) | 0.54 |
| Child received treatment at private medical consultation, community healthcare or hospital of diarrhea or respiratory symptoms | 160 | 44.8 (38.6, 50.9) | 178 | 43.1 (37.4, 48.9) | 0.70 |
| Number of individuals eating from same kitchen | 0.15 | ||||
| <5 | 69 | 19.7 (14.6, 24.7) | 103 | 25.2 (20.2, 30.2) | |
| ≥5 and <6 | 55 | 14.4 (10.0, 18.8) | 75 | 18.3 (14.1, 22.4) | |
| ≥6 and <8 | 121 | 32.2 (26.7, 37.8) | 99 | 29.2 (23.4, 35.1) | |
| ≥8 | 125 | 33.6 (27.8, 39.5) | 117 | 27.3 (22.4, 32.3) | |
| Capital | |||||
| Mean annual income per household Capita 10 | 370 | 7642.6 (6582.3, 8702.9) | 394 | 7554.4 (6316.1, 8792.6) | 0.40 |
| Household did borrow money (loan, credit, micro-credit) | 31 | 8.1 (4.9, 11.2) | 22 | 5.2 (3.0, 7.4) | 0.70 |
| Maternal education | 0.011 | ||||
| None | 20 | 5.0 (2.8, 7.2) | 37 | 9.2 (5.8, 12.7) | |
| Primary school | 64 | 16.7 (12.2, 21.2) | 96 | 22.7 (18.1, 27.4) | |
| Middle school | 126 | 35.3 (29.3, 41.2) | 105 | 25.2 (20.5, 29.9) | |
| High school | 116 | 32.1 (26.2, 38.0) | 110 | 28.4 (23.1, 33.7) | |
| College or more | 44 | 10.9 (7.4, 14.5) | 46 | 14.4 (9.4, 19.5) | |
| Paternal education | 0.014 | ||||
| None | 7 | 2.2 (0.5, 4.0) | 15 | 4.0 (1.3, 6.6) | |
| Primary school | 32 | 7.3 (4.6, 10.0) | 55 | 13.8 (9.8, 17.7) | |
| Middle school | 103 | 24.9 (20.0, 29.8) | 116 | 28.6 (23.5, 30.7) | |
| High school | 143 | 40.7 (34.6, 46.8) | 123 | 29.9 (24.7, 35.0) | |
| College or more | 85 | 24.8 (19.3, 30.4) | 85 | 23.8 (18.3, 29.3) | |
| Land ownership, hectare | 0.003 | ||||
| <0.04 | 74 | 17.1 (13.0, 21.2) | 115 | 29.7 (24.1, 35.3) | |
| ≥0.04 and <0.2 | 84 | 21.1 (16.4, 25.9) | 89 | 21.9 (17.2, 26.5) | |
| ≥0.2 and <0.8 | 92 | 26.6 (21.0, 32.3) | 98 | 23.2 (18.7, 27.8) | |
| ≥0.8 | 120 | 35.2 (29.2, 41.2) | 92 | 25.2 (19.9, 30.6) | |
| Household did own any livestock or poultry | 236 | 64.7 (58.9, 70.6) | 213 | 55.2 (49.3, 61.0) | 0.024 |
| Basic causes | |||||
| Religion | 0.55 | ||||
| Hindu | 318 | 91.9 (89.6, 94.1) | 366 | 93.0 (90.1, 95.8) | |
| Muslim | 52 | 8.1 (5.9, 10.4) | 28 | 7.0 (4.2, 9.9) | |
| Caste | 0.001 | ||||
| General | 116 | 38.4 (32.1, 44.7) | 73 | 22.2 (16.8, 27.5) | |
| Other backward | 134 | 33.7 (28.2, 39.2) | 186 | 41.3 (35.7, 47.0) | |
| Scheduled caste | 69 | 20.1 (15.2, 24.9) | 107 | 29.5 (24.0, 35.0) | |
| No caste | 51 | 7.9 (5.7, 10.1) | 28 | 7.0 (4.2, 9.9) | |
4. Discussion
| Flooded Twice (n = 303) | Flooded Once (n = 67) | Non-Flooded (n = 394) | Adjusted Model 1 | Adjusted Model 2 | Unadjusted model | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Indicator | Variable | n | % (95% CI) | n | % (95% CI) | n | % (95% CI) | Twice vs. None aPR (95% CI) | Once vs. None aPR (95% CI) | Twice vs. None aPR (95% CI) | Once vs. None aPR (95% CI) | Twice vs. None PR (95% CI) | Once vs. None PR (95% CI) |
| Wasting (weight-for-height, WHZ) | |||||||||||||
| Moderate | 93 | 30.5 (24.5, 36.6) | 22 | 31.3 (17.0, 45.6) | 42 | 14.3 (9.2, 19.4) | 2.06 (1.43, 2.97) | 2.22 (1.42, 3.48) | 2.04 (1.29, 3.24) | 2.23 (1.39, 3.57) | 2.14 (1.42, 3.21) | 2.19 (1.23, 3.91) | |
| Severe | 63 | 21.1 (15.9, 26.3) | 9 | 10.1 (3.3, 16.8) | 28 | 6.9 (4.2, 9.6) | 3.37 (2.34, 4.86) | 1.76 (0.83, 3.72) | 3.06 (1.79, 5.21) | 1.46 (0.64, 3.33) | 3.04 (1.92, 4.81) | 1.45 (0.67, 3.13) | |
| Total | 156 | 51.6 (45.0, 58.2) | 31 | 41.4 (26.4, 56.4) | 70 | 21.2 (15.8, 26.6) | 2.30 (1.86, 2.85) | 1.94 (1.43, 2.63) | 2.36 (1.73, 3.20) | 1.93 (1.32, 2.82) | 2.43 (1.83, 3.23) | 1.95 (1.25, 3.04) | |
| Stunting (height-for-age, HAZ) | |||||||||||||
| Moderate | 58 | 20.1 (14.6, 25.6) | 9 | 9.4 (3.1, 15.8) | 75 | 17.2 (13.0, 21.4) | 1.03 (0.73, 1.47) | 0.47 (0.29, 1.09) | 0.92 (0.57, 1.47) | 0.45 (0.20, 1.04) | 1.17 (0.81, 1.69) | 0.55 (0.27, 1.12) | |
| Severe | 27 | 10.0 (5.8, 14.1) | 3 | 7.3 (0.0, 17.3) | 44 | 11.2 (7.5, 15.0) | 1.66 (0.81, 3.40) | 1.83 (0.54, 6.17) | 1.72 (0.85, 3.47) | 2.00 (0.63, 6.37) | 0.89 (0.52, 1.51) | 0.65 (0.16, 2.66) | |
| Total | 85 | 30.0 (23.8, 36.3) | 12 | 16.7 (10.9, 30.3) | 119 | 28.4 (23.3, 33.6) | 0.90 (0.72, 1.14) | 0.63 (0.31, 1.29) | 1.00 (0.70, 1.42) | 0.67 (0.31, 1.43) | 1.06 (0.80, 1.39) | 0.59 (0.29, 1.18) | |
| Underweight (weight-for-age, WAZ) | |||||||||||||
| Moderate | 81 | 29.4 (23.1, 35.8) | 20 | 33.1 (17.8, 48.4) | 76 | 20.6 (15.6, 25.7) | 1.77 (1.22, 2.58) | 2.12 (1.35, 3.33) | 1.73 (1.20, 2.49) | 2.21 (1.43, 3.43) | 1.43 (1.03, 1.98) | 1.60 (0.95, 2.71) | |
| Severe | 65 | 22.4 (16.9, 28.0) | 7 | 8.0 (2.0, 13.9) | 40 | 10.4 (6.8, 14.0) | 2.48 (1.77, 3.49) | 1.09 (0.61, 1.97) | 2.73 (1.68, 4.43) | 1.18 (0.55, 2.54) | 2.17 (1.42, 3.32) | 0.76 (0.33, 1.75) | |
| Total | 146 | 51.9 (45.3, 58.4) | 27 | 41.0 (25.6, 56.5) | 116 | 31.0 (25.4, 36.6) | 1.48 (1.21, 1.81) | 1.53 (1.09, 2.13) | 1.76 (1.36, 2.29) | 1.89 (1.31, 2.72) | 1.67 (1.34, 2.09) | 1.32 (0.87, 2.01) | |
| Repeatedly Flooded (2006, 2008) | Flooded Once (2008) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| n | aPR (95% CI) | P | PR (95% CI) | P | aPR (95% CI) | P | PR (95% CI) | p | ||
| Flooded vs. non-flooded | 764 | 2.07 (1.44, 2.99) | <0.001 | 1.79 (1.23, 2.62) | 0.002 | 1.26 (0.69, 2.31) | 0.45 | 1.69 (0.93, 3.07) | 0.084 | |
| Child age, months | ||||||||||
| 6–11 | 85 | Reference | Reference | Reference | Reference | |||||
| 12–23 | 185 | 0.59 (0.38, 0.93) | 0.024 | 0.59 (0.33, 1.04) | 0.07 | 0.59 (0.38, 0.93) | 0.024 | 0.59 (0.33, 1.04) | 0.07 | |
| 24–35 | 155 | 0.28 (0.14, 0.55) | <0.001 | 0.22 (0.10, 0.48) | <0.001 | 0.28 (0.14, 0.55) | <0.001 | 0.22 (0.10, 0.48) | <0.001 | |
| 36–47 | 158 | 0.16 (0.06, 0.40) | <0.001 | 0.11 (0.03, 0.39) | <0.001 | 0.16 (0.06, 0.40) | <0.001 | 0.11 (0.03, 0.39) | <0.001 | |
| 48–59 | 181 | 0.66 (0.41, 1.06) | 0.09 | 0.53 (0.29, 0.97) | 0.04 | 0.66 (0.41, 1.06) | 0.09 | 0.53 (0.29, 0.97) | 0.04 | |
| Child age x flooding | ||||||||||
| 6–11 | 85 | Reference | Reference | Reference | Reference | |||||
| 12–23 | 185 | 0.75 (0.42, 1.34) | 0.33 | 0.80 (0.40, 1.61) | 0.54 | 0.54 (0.14, 2.09) | 0.37 | 0.39 (0.10, 1.47) | 0.16 | |
| 24–35 | 155 | 2.00 (0.97, 4.15) | 0.06 | 2.94 (1.26, 6.84) | 0.012 | 2.54 (0.88, 7.32) | 0.08 | 1.94 (0.59, 6.33) | 0.27 | |
| 36–47 | 158 | 4.01 (1.51, 10.63) | 0.005 | 5.62 (1.57, 20.12) | 0.008 | 5.71 (1.78, 18.24) | 0.003 | 5.60 (1.25, 25.15) | 0.024 | |
| 48–59 | 181 | 0.88 (0.52, 1.51) | 0.65 | 1.19 (0.60, 2.37) | 0.61 | 1.57 (0.71, 3.53) | 0.27 | 1.46 (0.60, 3.52) | 0.4 | |
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| aPR | adjusted prevalence ratio |
| ENA | emergency nutrition assessment |
| ICDS | Integrated Child Development Scheme |
| OSDMA | Odisha state disaster mitigation authority |
| PR | prevalence ratio |
| PSU | primary sampling unit |
| SSU | secondary sampling unit |
| SMART | standardized monitoring and assessment of relief and transitions |
| UNICEF | United Nations children’s fund |
Appendix A
| Flooded vs. Non-Flooded | Confounders (p ≤ 0.2) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Variables | Wasting | Stunting | Underweight | |||||||
| Child characteristics | Moderate | Severe | Total | Moderate | Severe | Total | Moderate | Severe | Total | |
| Child female | NS | No | Yes | Yes | Yes | No | Yes | No | No | No |
| Mean birthweight, g | NS | Yes | Yes | Yes | No | Yes | Yes | No | Yes | Yes |
| Child age, months | p ≤ 0.2 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | No |
| Underlying Causes | ||||||||||
| Care of mother and children | ||||||||||
| Mean age at marriage of the mother, y | p ≤ 0.2 | No | No | No | No | No | No | Yes | Yes | Yes |
| Mean age of the mother at first delivery, y | p ≤ 0.2 | Yes | Yes | Yes | Yes | No | Yes | No | Yes | No |
| Mean age of the mother at birth of child, y | NS | Yes | Yes | No | No | No | Yes | Yes | No | Yes |
| Mean age of the father at birth of child, y | NS | No | Yes | Yes | Yes | No | No | No | Yes | No |
| Two or more children underfive eating from same kitchen | NS | No | No | No | No | No | No | No | No | No |
| Mother was a member of self-help group/Mahila Mandal | NS | Yes | Yes | No | No | No | No | No | No | No |
| Mean number of mother‘s conceptions | NS | Yes | Yes | No | Yes | No | Yes | Yes | No | Yes |
| Mother had one or more miscarriages, stillbirths | NS | No | No | Yes | Yes | Yes | Yes | No | No | No |
| Child breastfed at least 2 years | NS | No | No | No | No | No | No | No | Yes | No |
| Supplementary feeding started after 6 months of child‘s age | NS | Yes | Yes | No | No | Yes | Yes | No | Yes | No |
| Child breastfed at least 2 years and supplemented after 6 months of age | p ≤ 0.2 | Yes | No | Yes | No | No | No | No | No | No |
| Mother washes hands with soap before feeding child | p ≤ 0.2 | No | No | No | No | No | No | No | No | No |
| Mother washes hands with soap before preparing food for the family | p ≤ 0.2 | Yes | No | Yes | No | No | No | No | No | No |
| Mother washes hands with soap before lunch | NS | No | Yes | Yes | Yes | Yes | No | No | No | No |
| Mother washes hands with soap after attending the child who defecated | NS | Yes | No | Yes | Yes | Yes | Yes | Yes | No | Yes |
| Child received BCG vaccine | NS | No | Yes | Yes | No | Yes | No | Yes | Yes | Yes |
| Child received measles vaccine | NS | No | Yes | No | No | Yes | Yes | No | Yes | Yes |
| Child received all three doses of polio vaccine | NS | Yes | Yes | Yes | Yes | No | Yes | No | No | No |
| Child received all three doses of B-hepatitis vaccine | NS | No | Yes | No | No | Yes | No | Yes | No | Yes |
| Child received all three doses of DPT vaccine | NS | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | No |
| Public health | ||||||||||
| Improved latrine (before floods) | p ≤ 0.2 | No | No | No | No | Yes | No | Yes | No | No |
| Improved drinking water (before floods) | p ≤ 0.2 | No | No | No | No | No | No | No | Yes | No |
| Mother gave birth at hospital | NS | No | No | No | No | No | No | Yes | No | Yes |
| Number of individuals eating from same kitchen | p ≤ 0.2 | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Yes |
| Capital | ||||||||||
| Household did borrow money (loan, credit, micro-credit) | NS | No | No | No | Yes | No | Yes | Yes | Yes | No |
| Maternal education | p ≤ 0.2 | Yes | Yes | Yes | Yes | Yes | Yes | No 1 | Yes | Yes |
| Paternal education | p ≤ 0.2 | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes |
| Land ownership, hectare | p ≤ 0.2 | No | Yes | No | Yes | Yes | Yes | No | Yes | Yes |
| Basic causes | ||||||||||
| Religion | NS | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Caste | p ≤ 0.2 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Model 1 | Model 2 | ||||
|---|---|---|---|---|---|
| aPR (95% CI) | p | aPR (95% CI) | p | ||
| Flooded vs. non-flooded | 1.93 (1.34, 2.79) | <0.001 | 2.22 (1.45, 3.40) | <0.001 | |
| Child age, months | |||||
| 6–11 | Reference | Reference | |||
| 12–23 | 0.46 (0.25, 0.87) | 0.02 | 0.60 (0.32, 1.14) | 0.12 | |
| 24–35 | 0.25 (0.11, 0.57) | 0.009 | 0.31 (0.14, 0.71) | 0.006 | |
| 36–47 | 0.13 (0.04, 0.51) | 0.003 | 0.15 (0.04, 0.54) | 0.004 | |
| 48–59 | 0.65 (0.39, 1.07) | 0.095 | 0.70 (0.36, 1.35) | 0.29 | |
| Child age x flooding | |||||
| 6–11 | Reference | Reference | |||
| 12–23 | 0.92 (0.44, 1.92) | 0.83 | 0.73 (0.36, 1.50) | 0.40 | |
| 24–35 | 2.31 (0.94, 5.65) | 0.07 | 1.99 (0.82, 4.83) | 0.13 | |
| 36–47 | 5.16 (1.31, 20.35) | 0.02 | 4.29 (1.19, 15.48) | 0.03 | |
| 48–59 | 0.95 (0.55, 1.64) | 0.84 | 0.88 (0.45, 1.71) | 0.70 | |
Appendix B
| Item No. | Recommendation | ||
|---|---|---|---|
| Title and abstract | 1✓ p1–2 | (a) Indicate the study’s design with a commonly used term in the title or the abstract | |
| (b) Provide in the abstract an informative and balanced summary of what was done and what was found | |||
| Introduction | |||
| Background/rationale | 2✓ p3–4 | Explain the scientific background and rationale for the investigation being reported | |
| Objectives | 3✓ p4 | State specific objectives, including any prespecified hypotheses | |
| Methods | |||
| Study design | 4✓ p4–5 | Present key elements of study design early in the paper | |
| Setting | 5✓ p6 | Describe the setting, locations, and relevant dates, including periods of recruitment, exposure, follow-up, and data collection | |
| Participants | 6✓ p5–8 | (a) Give the eligibility criteria, and the sources and methods of selection of participants | |
| Variables | 7✓ p5, 8–9 | Clearly define all outcomes, exposures, predictors, potential confounders, and effect modifiers. Give diagnostic criteria, if applicable | |
| Data sources/measurement | 8✓ p8–9 | For each variable of interest, give sources of data and details of methods of assessment (measurement). Describe comparability of assessment methods if there is more than one group | |
| Bias | 9✓ p5, 9, 10 and SOM | Describe any efforts to address potential sources of bias | |
| Study size | 10✓ p7 | Explain how the study size was arrived at | |
| Quantitative variables | 11✓ p5, 8 and tables | Explain how quantitative variables were handled in the analyses. If applicable, describe which groupings were chosen and why | |
| Statistical methods | 12✓ p9–10 | (a) Describe all statistical methods, including those used to control for confounding | |
| (b) Describe any methods used to examine subgroups and interactions | |||
| (c) Explain how missing data were addressed | |||
| (d) If applicable, describe analytical methods taking account of sampling strategy | |||
| (e) Describe any sensitivity analyses | |||
| Results | |||
| Participants | 13✓ p10 | (a) Report numbers of individuals at each stage of study—e.g., numbers potentially eligible, examined for eligibility, confirmed eligible, included in the study, completing follow-up, and analysed | |
| (b) Give reasons for non-participation at each stage ✓ Figure 1 | |||
| (c) Consider use of a flow diagram ✓ Figure 1 | |||
| Descriptive data | 14✓ p10, table 1 | (a) Give characteristics of study participants (e.g., demographic, clinical, social) and information on exposures and potential confounders | |
| (b) Indicate number of participants with missing data for each variable of interest | |||
| Outcome data | 15✓ p10, table 2 | Report numbers of outcome events or summary measures | |
| Main results | 16✓ p10–11, tables 2–3 tables 1–3 p5 n/a | (a) Give unadjusted estimates and, if applicable, confounder-adjusted estimates and their precision (eg, 95% confidence interval). Make clear which confounders were adjusted for and why they were included ✓ (p10) | |
| (b) Report category boundaries when continuous variables were categorized | |||
| (c) If relevant, consider translating estimates of relative risk into absolute risk for a meaningful time period | |||
| Other analyses | 11✓ p7 | Report other analyses done—e.g., analyses of subgroups and interactions, and sensitivity analyses | |
| Discussion | |||
| Key results | 18✓ p12 | Summarise key results with reference to study objectives | |
| Limitations | 19✓ p14–15 | Discuss limitations of the study, taking into account sources of potential bias or imprecision. Discuss both direction and magnitude of any potential bias | |
| Interpretation | 20✓ p14–16 | Give a cautious overall interpretation of results considering objectives, limitations, multiplicity of analyses, results from similar studies, and other relevant evidence | |
| Generalisability | 21✓ p15–16 | Discuss the generalisability (external validity) of the study results | |
| Other information | |||
| Funding | 22✓ p1 | Give the source of funding and the role of the funders for the present study and, if applicable, for the original study on which the present article is based | |
References
- EM-DAT. The OFDA/CRED International Disaster Database. Available online: http://www.emdat.be/database (accessed on 1 November 2014).
- Ahern, M.; Kovats, R.S.; Wilkinson, P.; Few, R.; Matthies, F. Global health impacts of floods: Epidemiologic evidence. Epidemiol. Rev. 2005, 27, 36–46. [Google Scholar] [CrossRef] [PubMed]
- Alderman, K.; Turner, L.R.; Tong, S. Floods and human health: A systematic review. Environ. Int. 2012, 47, 37–47. [Google Scholar] [CrossRef] [PubMed]
- Milojevic, A.; Armstrong, B.; Hashizume, M.; McAllister, K.; Faruque, A.; Yunus, M.; Kim, S.P.; Moji, K.; Wilkinson, P. Health effects of flooding in rural Bangladesh. Epidemiology 2011, 23, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Stephenson, J.; Vaganay, M.; Cameron, R.; Joseph, P. The long-term health impacts of repeated flood events. In Flood Recovery, Innovation and Response IV; Proverbs, D., Brebbia, C.A., Eds.; WITpress: Southampton, UK, 2014; pp. 201–215. [Google Scholar]
- Del Ninno, C.; Lundberg, M. Treading water. The long-term impact of the 1998 flood on nutrition in Bangladesh. Econ. Hum. Biol. 2005, 3, 67–96. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Llanes, J.M.; Ranjan-Dash, S.; Degomme, O.; Mukhopadhyay, A.; Guha-Sapir, D. Child malnutrition and recurrent flooding in rural eastern India: A community-based survey. BMJ Open 2011, 1, e000109. [Google Scholar] [CrossRef] [PubMed]
- Goudet, S.M.; Faiz, S.; Bogin, B.A.; Griffiths, P.L. Pregnant women’s and community health workers’ perceptions of root causes of malnutrition among infants and young children in the slums of Dhaka, Bangladesh. Am. J. Public Health 2011, 101, 1225–1233. [Google Scholar] [CrossRef] [PubMed]
- Haines, A.; Kovats, R.S.; Campbell-Lendrum, D.; Corvalan, C. Climate change and human health: impacts, vulnerability and public health. Public Health 2006, 120, 585–596. [Google Scholar] [CrossRef] [PubMed]
- Few, R. Health and climatic hazards: Framing social research on vulnerability, response and adaptation. Glob. Environ. Chang. 2007, 17, 281–295. [Google Scholar] [CrossRef]
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; De Onis, M.; Ezzati, M.; Grantham-McGregor, S.; Katz, J.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- Dilley, M.; Chen, R.S.; Deichmann, U.; Lerner-Lam, A.L.; Arnold, M.; Agwe, J.; Buys, P.; Kjevstad, O.; Lyon, B.; Yetman, G. Natural Disaster Hotspots: A Global Risk Analysis; The World Bank and Columbia University: Washington, DC, USA, 2005. [Google Scholar]
- Department of Economic and Social Affairs, United Nations. Population Division. Available online: http://www.un.org/en/development/desa/population/publications/database (accessed on 1 November 2014).
- Coumou, D.; Rahmstorf, S. A decade of weather extremes. Nature Clim. Chang. 2012, 2, 491–496. [Google Scholar] [CrossRef]
- Mechler, R.; Bouwer, L.M. Understanding trends and projections of disaster losses and climate change: Is vulnerability the missing link? Clim. Chang. 2015, 133, 23–35. [Google Scholar] [CrossRef]
- Bunyavanich, S.; Landrigan, C.P.; McMichael, A.J.; Epstein, P.R. The impact of climate change on child health. Ambul. Pediatr. 2003, 3, 44–52. [Google Scholar] [CrossRef]
- Krishnamurthy, P.K.; Lewis, K.; Choularton, R.J. A methodological framework for rapidly assessing the impacts of climate risk on national-level food security through a vulnerability index. Glob. Environ. Chang. 2014, 25, 121–132. [Google Scholar] [CrossRef]
- Government of Orissa. Memorandum on Floods 2008; Special Relief Commissioner, Orissa Revenue and Disaster Management Department: Odisha, India, 2008.
- Phalkey, R.; Dash, S.R.; Mukhopadhyay, A.; Runge-Ranzinger, S.; Marx, M. Prepared to react? Assessing the functional capacity of the primary health care system in rural Orissa, India to respond to the devastating flood of September 2008. Glob. Health Action 2012, 5, 10964. [Google Scholar]
- Schisterman, E.; Cole, S.; Platt, R. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology 2009, 20, 488–495. [Google Scholar] [CrossRef] [PubMed]
- United Nations Children’s Fund. The State of the World’s Children 1998; Oxford University Press for UNICEF: New York, NY, USA, 1997. [Google Scholar]
- Vittinghoff, E.; Glidden, D.V.; Shiboski, S.C.; McCulloch, C.E. Regression Methods in Biostatistics: Linear, logistic, Survival, and Repeated Measures Models; Springer: New York, NY, USA, 2005. [Google Scholar]
- Lumley, T. Complex Surveys: A Guide to Analysis Using R; John Wiley & Sons: Hoboken, NJ, USA, 2010. [Google Scholar]
- Odisha State Disaster Mitigation Authority (OSDMA). Available online: http://www.osdma.org (accessed on 3 April 2009).
- The Census of India 2011. Available online: http://www.censusindia.gov.in (accessed on 9 September 2014).
- Groves, R.M.; Fowler, F.J.; Couper, M.P.; Lepkowski, J.M.; Singer, E.; Tourangeau, R. Survey Methodology; Wiley-Blackwell: Oxford, UK, 2009. [Google Scholar]
- The Census of India 2001. Available online: http://www.censusindia.gov.in (accessed on 3 April 2009).
- Sullivan, K.M.; Dean, A.; Soe, M.M. OpenEpi: A web-based epidemiologic and statistical calculator for public health. Public Health Rep. 2009, 124, 471–474. [Google Scholar] [PubMed]
- World Medical Association. Declaration of Helsinki: Recommendations guiding physicians in biomedical research involving human subjects. JAMA 1997, 277, 925–926. [Google Scholar]
- Emergency Nutrition Assessment (ENA) Software for Standardized Monitoring and Assessment of Relief and Transitions (SMART), Version November 2008. Available online: http://www.nutrisurvey.de/ena/ena.html (accessed on November 2010).
- R: A Language and Environment for Statistical Computing. Available online: http://www.R-project.org (accessed on 25 September 2013).
- Ho, D.; Imai, K.; King, G.; Stuart, E. MatchIt: Nonparametric Preprocessing for Parametric Causal Inference. Available online: https://cran.r-project.org/web/packages/MatchIt/MatchIt.pdf (accessed on 19 February 2015).
- De Onis, M.; Blössner, M. WHO Global Database on Child Growth and Malnutrition; World Health Organization: Geneva, Switzerland, 1997. [Google Scholar]
- Danysh, H.E.; Gilman, R.H.; Wells, J.C.; Pan, W.; Zaitchik, B.; Gonzalvez, G.; Alvarez, M.; Checkley, W. El Niño adversely affected childhood stature and lean mass in northern Peru. Clim. Chang. Resp. 2014, 1, 10–20. [Google Scholar] [CrossRef]
- Rosales, M.F. Impact of Early Life Shocks on Human Capital Formation: El Nino Floods in Ecuador. Available online: http://dx.doi.org/10.2139/ssrn.2559634 (accessed on 1 June 2015).
- Pörtner, C.C. Natural Hazards and Child Health, 2010. Available online: http://dx.doi.org/10.2139/ssrn.1599432 (accessed on 1 June 2015).
- Hossain, S.M.; Kolsteren, P. The 1998 flood in Bangladesh: Is different targeting needed during emergencies and recovery to tackle malnutrition? Disasters 2003, 27, 172–184. [Google Scholar] [CrossRef] [PubMed]
- Catani, C.; Jacob, N.; Schauer, E.; Kohila, M.; Neuner, F. Family violence, war, and natural disasters: A study of the effect of extreme stress on children’s mental health in Sri Lanka. BMC Psychiat. 2008, 8, 33. [Google Scholar] [CrossRef] [PubMed]
- Black, R.E.; Allen, L.H.; Bhutta, Z.A.; Caulfield, L.E.; De Onis, M.; Ezzati, M.; Mathers, C.; Rivera, J. Maternal and child undernutrition: Global and regional exposures and health consequences. Lancet 2008, 371, 243–260. [Google Scholar] [CrossRef]
- Gray, C.; Mueller, V. Natural disasters and population mobility in Bangladesh. Proc. Natl. Acad. Sci. U.S. 2012, 109, 6000–6005. [Google Scholar] [CrossRef] [PubMed]
- UNICEF Office of Research. The Challenges of Climate Change: Children on the Front Line; Innocenti Insight: Florence, Italy, 2014. [Google Scholar]
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodriguez-Llanes, J.M.; Ranjan-Dash, S.; Mukhopadhyay, A.; Guha-Sapir, D. Flood-Exposure is Associated with Higher Prevalence of Child Undernutrition in Rural Eastern India. Int. J. Environ. Res. Public Health 2016, 13, 210. https://doi.org/10.3390/ijerph13020210
Rodriguez-Llanes JM, Ranjan-Dash S, Mukhopadhyay A, Guha-Sapir D. Flood-Exposure is Associated with Higher Prevalence of Child Undernutrition in Rural Eastern India. International Journal of Environmental Research and Public Health. 2016; 13(2):210. https://doi.org/10.3390/ijerph13020210
Chicago/Turabian StyleRodriguez-Llanes, Jose Manuel, Shishir Ranjan-Dash, Alok Mukhopadhyay, and Debarati Guha-Sapir. 2016. "Flood-Exposure is Associated with Higher Prevalence of Child Undernutrition in Rural Eastern India" International Journal of Environmental Research and Public Health 13, no. 2: 210. https://doi.org/10.3390/ijerph13020210
APA StyleRodriguez-Llanes, J. M., Ranjan-Dash, S., Mukhopadhyay, A., & Guha-Sapir, D. (2016). Flood-Exposure is Associated with Higher Prevalence of Child Undernutrition in Rural Eastern India. International Journal of Environmental Research and Public Health, 13(2), 210. https://doi.org/10.3390/ijerph13020210





