HIV, Other Blood-Borne Viruses and Sexually Transmitted Infections amongst Expatriates and Travellers to Low- and Middle-Income Countries: A Systematic Review
Abstract
:1. Introduction
2. Materials and Methods
3. Results
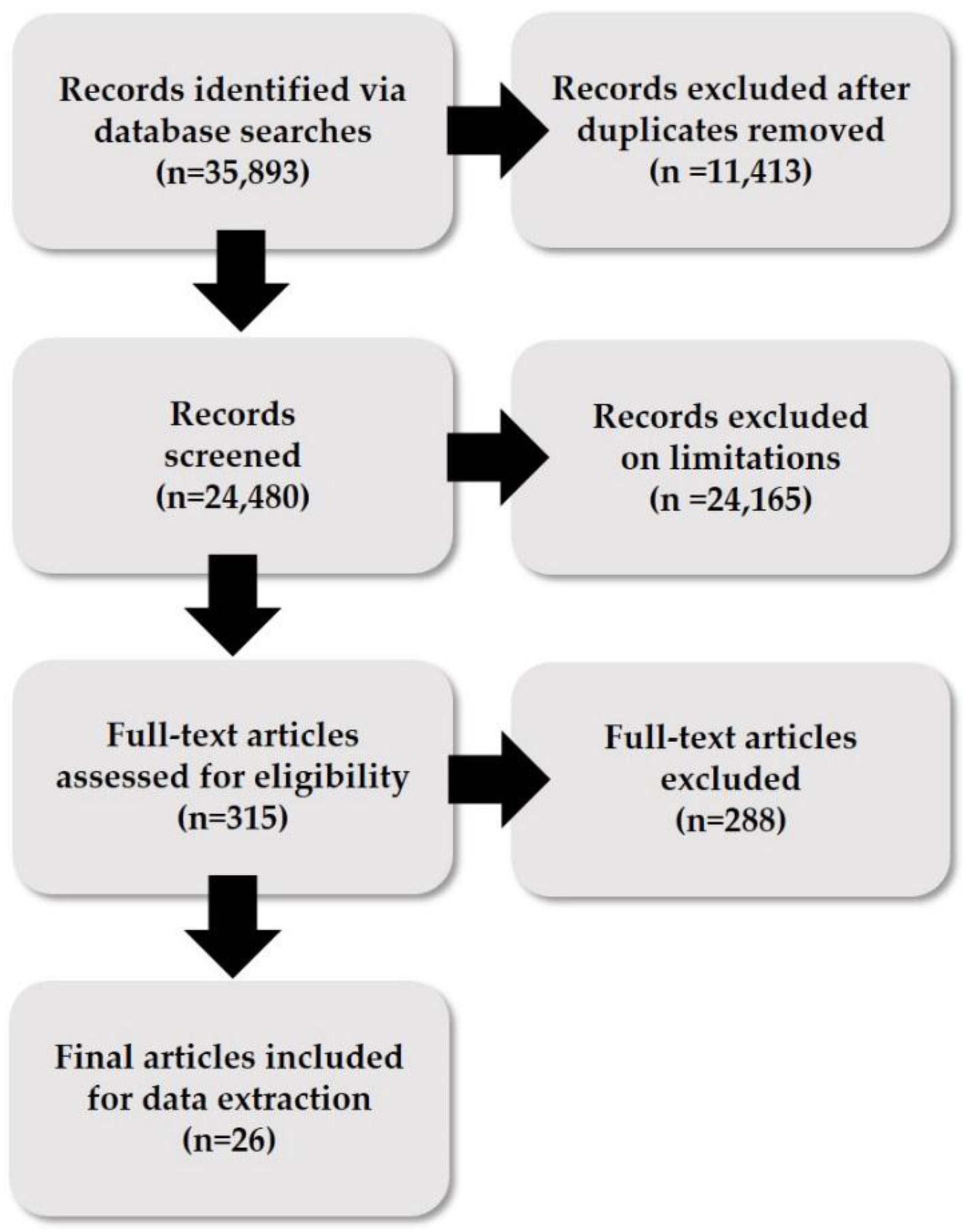
- Study Overview—design, setting, participant type and number
- Traveller and Travel Characteristics—gender, sexuality and age; participant country of origin and destination; purpose of travel, length of stay and frequency of travel
- Knowledge, Attitudes and Beliefs—perceptions of travel and destination countries; sexual expectations; knowledge of HIV, other BBVs or STIs
- Sexual Partner Acquisition—influencing factors; sexual mixing; commercial sex; number of sexual partners
- Alcohol and Other Drug Use—frequency of use, type, role as risk factor
- Condom Use—consistency of condom use; influencing factors
- Pre-Travel Health Consultation-use and experience; advice given
- Vaccination—knowledge and vaccination coverage
- Acquisition of HIV, other BBV or STI—risk behavior; diagnosis and related symptoms; place of acquisition; influencing factors
- Study Recommendations—policy, practice (clinical and health promotion) and research
3.1. Study Design and Setting
3.2. Traveller and Travel Characteristics
3.2.1. Gender, Sexuality and Age
3.2.2. Origin
3.2.3. Destination
3.2.4. Purpose of Travel
3.2.5. Length of Stay and Frequency of Travel
3.3. Knowledge, Attitudes and Beliefs
3.3.1. Perceptions of Travel and Destination Countries
3.3.2. Sexual Expectations
3.3.3. Knowledge of HIV, Other BBVs or STIs
3.4. Sexual Partner Acquisition
3.4.1. Sexual Mixing
3.4.2. Commercial Sex
3.4.3. Number of Sexual Partners
3.5. Alcohol and Other Drug Use
3.6. Condom Use
3.6.1. Consistency of Condom Use
3.6.2. Factors Influencing Condom Use
3.7. Pre-Travel Health Consultation
3.8. Vaccination
3.9. Acquisition of HIV, Other BBVs or STIs
3.9.1. Risk Behavior
3.9.2. Diagnosis and Related Symptoms
3.9.3. Place of Acquisition
3.9.4. Influencing Factors
3.10. Study Recommendations
4. Discussion
4.1. Overview of Findings
4.2. Study Design and Reporting Limitations
4.3. Strengths and Limitations of the Review
4.4. Implications for Research, Policy and Practice
4.4.1. Research Opportunities
4.4.2. Clinical Practice Opportunities
4.4.3. Health Promotion Opportunities
4.4.4. Policy and Advocacy Opportunities
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- UNAIDS. Background Paper: People on the Move-Forced Displacement and Migrant Populations; UNAIDS: Geneva, Switzerland, 2009; pp. 1–31. [Google Scholar]
- Chapman, A.R. Globalization, human rights, and the social determinants of health. Bioethics 2009, 23, 97–111. [Google Scholar] [CrossRef] [PubMed]
- International Air Transport Association. Air Passenger Forecast Shows Dip in Long-Term Demand. Available online: http://www.iata.org/pressroom/pr/Pages/2015-11-26-01.aspx (accessed on 10 September 2016).
- Simon, H. Travel to Developing Countries. Available online: http://umm.edu/health/medical/reports/articles/travel-to-developing-countries (accessed on 10 September 2016).
- Department of Economic and Social Affairs Population Division. Population Distribution, Urbanization, Internal Migration and Development: An International Perspective; United Nations: Geneva, Switzerland, 2011. [Google Scholar]
- Gushulak, B.D.; MacPherson, D.W. Population mobility and health: An overview of the relationships between movement and population health. J. Travel Med. 2004, 11, 171–178. [Google Scholar] [CrossRef] [PubMed]
- Acevedo-Garcia, D.; Almeida, J. Special issue introduction: Place, migration and health. Soc. Sci. Med. 2012, 75, 2055–2059. [Google Scholar] [CrossRef] [PubMed]
- Deane, K.D.; Parkhurst, J.O.; Johnston, D. Linking migration, mobility and HIV. Trop Med. Int. Health 2010, 15, 1458–1463. [Google Scholar] [CrossRef] [PubMed]
- Crawford, G.; Lobo, R.; Brown, G.; Langdon, P. HIV and Mobility in Australia: Road Map for Action; Western Australian Centre for Health Promotion Research and Australian Research Centre in Sex, Health and Society: Melbourne, Australia, 2014. [Google Scholar]
- Newman, L.; Rowley, J.; Vander Hoorn, S.; Wijesooriya, N.S.; Unemo, M.; Low, N.; Stevens, G.; Gottlieb, S.; Kiarie, J.; Temmerman, M. Global estimates of the prevalence and incidence of four curable sexually transmitted infections in 2012 based on systematic review and global reporting. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Incidence and Prevalence of Selected Curable Sexually Transmitted Infections—2008; World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- UNAIDS. Global Statistics 2015; UNAIDS: Geneva, Switzerland, 2016. [Google Scholar]
- World Health Organization. Sexually Transmitted Infections (STIs); World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- Centers for Disease Control and Prevention. Incidence, Prevalence, and Cost of Sexually Transmitted Infections in the United States; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2013.
- World Tourism Organization. Tourism Highlights 2014; World Tourism Organization: Madrid, Spain, 2014. [Google Scholar]
- Office for National Statistics. Travel Trends, 2011; UK Statistics Authority: London, UK, 2012.
- Australian Bureau of Statistics. Overseas Arrivals and Departures, Australia, June 2015; Australian Bureau of Statistics: Canberra, Australia, 2015.
- Haour-Knipe, M.; de Zalduondo, B.; Samuels, F.; Molesworth, K.; Sehgal, S. HIV and “people on the move”: Six strategies to reduce risk and vulnerability during the migration process. Int. Migr. 2013, 3, 17. [Google Scholar] [CrossRef]
- Howard, R. The migration of westerners to Thailand: An unusual flow from developed to developing world. Int. Migr. 2009, 47, 193–225. [Google Scholar] [CrossRef]
- Richens, J. Sexually transmitted infections and HIV among travellers: A review. Travel Med. Infect. Dis. 2006, 4, 184–195. [Google Scholar] [CrossRef] [PubMed]
- Crawford, G.; Lobo, R.; Brown, G.; Maycock, B. The influence of population mobility on changing patterns of HIV acquisition: Lessons for and from Australia. Health Promot. J. Aust. 2016. [Google Scholar] [CrossRef] [PubMed]
- Memish, Z.; Osoba, A. International travel and sexually transmitted diseases. Travel Med. Infect. Dis. 2006, 4, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Auerbach, J.; Parkhurst, J.; Caceres, C.; Keller, K. Addressing Social Drivers of HIV/AIDS: Some Conceptual, Methodological, and Evidentiary Considerations; Working Paper 24; AIDS2031 Social Drivers Working Group: New York, NY, USA, 2009. [Google Scholar]
- Health and Development Network. Risk and Vulnerabilities of Migrants and Mobile Populations in Southern Africa; Health and Development Networks (HDN) and the International Organization for Migration Partnership on HIV/AIDS and Mobile Populations in Southern Africa: Arcadia, South Africa, 2006. [Google Scholar]
- Butler, A.; Hallett, T. Migration and the transmission of STIs. In The New Public Health and STD/HIV Prevention: Personal, Public and Health Systems Approaches; Aral, S., Fenton, K., Lipshutz, J., Eds.; Springer: New York, NY, USA, 2013; pp. 65–75. [Google Scholar]
- Woolley, I.; Bialy, C. Visiting friends and relatives may be a risk for non-adherence for HIV-positive travellers. Int. J. STD AIDS 2012, 23, 833–834. [Google Scholar] [CrossRef] [PubMed]
- Fenton, K.A.; Chinouya, M.; Davidson, O.; Copas, A. HIV transmission risk among Sub-Saharan Africans in London travelling to their countries of origin. AIDS 2001, 15, 1442–1445. [Google Scholar] [CrossRef] [PubMed]
- Ward, B.J.; Plourde, P. Travel and sexually transmitted infections. J. Travel Med. 2006, 13, 300–317. [Google Scholar] [CrossRef] [PubMed]
- Yokota, F. Sex behaviour of male Japanese tourists in Bangkok, Thailand. Cult. Health Sex. 2006, 8, 115–131. [Google Scholar] [CrossRef] [PubMed]
- Hamlyn, E.; Peer, A.; Easterbrook, P. Sexual health and HIV in travellers and expatriates. Occup. Med. 2007, 57, 313–321. [Google Scholar] [CrossRef] [PubMed]
- Rice, B.; Gilbart, V.L.; Lawrence, J.; Smith, R.; Kall, M.; Delpech, V. Safe travels? HIV transmission among Britons travelling abroad. HIV Med. 2012, 13, 315–317. [Google Scholar] [CrossRef] [PubMed]
- Boggild, A.K.; Geduld, J.; Libman, M.; Ward, B.J.; McCarthy, A.E.; Doyle, P.W.; Ghesquiere, W.; Vincelette, J.; Kuhn, S.; Freedman, D.O.; et al. Travel-acquired infections and illnesses in Canadians: Surveillance report from CanTravNet surveillance data, 2009–2011. Open Med. 2014, 8, e20–e32. [Google Scholar] [PubMed]
- Western Australian Government. HIV Notifications by Sex and Place of Birth and Acquisition 2010 to 2015, WA Residents; Epidemiology and Surveillance Program, Department of Health Western Australia: Perth, Australia, 2016.
- Government of South Australia. Surveillance of Sexually Transmitted Infections and Blood-Borne Viruses in South Australia, 2014; Department of Health South Australia: Adelaide, Australia, 2014.
- New South Wales Government. NSW HIV Strategy 2012–2015, Annual and Quarter 4 Data Report; New South Wales Ministry of Health: North Sydney, Australia, 2015.
- Crawford, G.; Bowser, N.J.; Brown, G.E.; Maycock, B.R. Exploring the potential of expatriate social networks to reduce HIV and STI transmission: A protocol for a qualitative study. BMJ Open 2013, 3. [Google Scholar] [CrossRef] [PubMed]
- Australian Government Department of Health. Seventh National HIV Strategy 2014–2017; Australian Government Department of Health: Canberra, Australia, 2014.
- Memish, Z.A.; Osoba, A.O. Sexually transmitted diseases and travel. Int. J. Antimicrob. Agent. 2003, 21, 131–134. [Google Scholar] [CrossRef]
- Rogstad, K.E. Sex, sun, sea, and STIs: Sexually transmitted infections acquired on holiday. BMJ 2004, 329, 214–217. [Google Scholar] [CrossRef] [PubMed]
- Patel, D. Occupational travel. Occup. Med. 2011, 61, 6–18. [Google Scholar] [CrossRef] [PubMed]
- Korzeniewski, K.; Juszczak, D. Travel-related sexually transmitted infections. Int. Marit. Health 2015, 66, 238–246. [Google Scholar] [CrossRef] [PubMed]
- Jones, S. Medical aspects of expatriate health: Health threats. Occup. Med. 2000, 50, 572–578. [Google Scholar] [CrossRef]
- Hynes, N.A. Sexually transmitted diseases in travelers. Curr. Infect. Dis. Rep. 2005, 7, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6. [Google Scholar] [CrossRef] [PubMed]
- Crawford, G.; Leavy, J.; Portsmouth, L.; Jancey, J.; Leaversuch, F.; Nimmo, L.; Reid-Dornbusch, L.; Hills, E. Development of a systematic review of public health interventions to prevent children drowning. Open J. Prev. Med. 2014, 4, 100–106. [Google Scholar] [CrossRef]
- Leavy, J.E.; Crawford, G.; Portsmouth, L.; Jancey, J.; Leaversuch, F.; Nimmo, L.; Hunt, K. Recreational drowning prevention interventions for adults, 1990–2012: A review. J. Community Health 2015, 40, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Leavy, J.E.; Crawford, G.; Leaversuch, F.; Nimmo, L.; McCausland, K.; Jancey, J. A review of drowning prevention interventions for children and young people in high, low and middle income countries. J. Community Health 2016, 41, 424–441. [Google Scholar] [CrossRef] [PubMed]
- World Bank Country and Lending Groups 2015. Available online: https://datahelpdesk.worldbank.org/knowledgebase/articles/906519-world-bank-country-and-lending-groups (accessed on 10 January 2016).
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions 5.1.0; Higgins, J.P.T., Green, S., Eds.; The Cochrane Collaboration: London, UK, 2011. [Google Scholar]
- Joanna Briggs Institute. Joanna Briggs Institute Reviewers’ Manual; Joanna Briggs Institute: Adelaide, Australia, 2014. [Google Scholar]
- National Institute for Health and Clinical Excellence (NICE). Methods for the Development of NICE Public Health Guidance; NICE: London, UK, 2009. [Google Scholar]
- National Institute for Health and Clinical Excellence. The Guidelines Manual; NICE: London, UK, 2012. [Google Scholar]
- The Cochrane Public Health Group. Guide for Developing a Cochrane Protocol 2011. Available online: http://ph.cochrane.org/sites/ph.cochrane.org/files/uploads/Guide%20for%20PH%20protocol_Nov%202011_final%20for%20website.pdf (accessed on 10 January 2016).
- Alcedo, S.; Kossuth-Cabrejos, S.; Piscoya, A.; Mayta-Tristan, P. Factors associated with non-use of condoms in an online community of frequent travellers. Travel Med. Infect. Dis. 2014, 12, 750–756. [Google Scholar] [CrossRef] [PubMed]
- Angelin, M.; Evengard, B.; Palmgren, H. Travel health advice: Benefits, compliance, and outcome. Scand. J. Infect. Dis. 2014, 46, 447–453. [Google Scholar] [CrossRef] [PubMed]
- Bhatta, P.; Simkhada, P.; Van Teijlingen, E.; Maybin, S. A questionnaire study of voluntary service overseas (VSO) volunteers: Health risk and problems encountered. J. Travel Med. 2009, 16, 332–337. [Google Scholar] [CrossRef] [PubMed]
- Cabada, M.M.; Echevarria, J.I.; Seas, C.R.; Narvarte, G.; Samalvides, F.; Freedman, D.O.; Gotuzzo, E. Sexual behavior of international travelers visiting Peru. J. Sex. Trans. Dis. 2002, 29, 510–513. [Google Scholar] [CrossRef]
- Cabada, M.M.; Montoya, M.; Echevarria, J.I.; Verdonck, K.; Seas, C.; Gotuzzo, E. Sexual behavior in travelers visiting Cuzco. J. Travel Med. 2003, 10, 214–218. [Google Scholar] [CrossRef] [PubMed]
- Croughs, M.; Van Gompel, A.; de Boer, E.; Van den Ende, J. Sexual risk behavior of travelers who consulted a pretravel clinic. J. Travel Med. 2008, 15, 6–12. [Google Scholar] [CrossRef] [PubMed]
- Dahlgren, A.L.; DeRoo, L.; Avril, J.; Bise, G.; Loutan, L. Health risks and risk-taking behaviors among International Committee of the Red Cross (ICRC) expatriates returning from humanitarian missions. J. Travel Med. 2009, 16, 382–390. [Google Scholar] [CrossRef] [PubMed]
- Hamer, D.H.; Ruffing, R.; Callahan, M.V.; Lyons, S.H.; Abdullah, A.S. Knowledge and use of measures to reduce health risks by corporate expatriate employees in Western Ghana. J. Travel Med. 2008, 15, 237–242. [Google Scholar] [CrossRef] [PubMed]
- Kaehler, N.; Piyaphanee, W.; Kittitrakul, C.; Kyi, Y.P.; Adhikari, B.; Sibunruang, S.; Jearraksuwan, S.; Tangpukdee, N.; Silachamroon, U.; Tantawichien, T. Sexual behavior of foreign backpackers in the Khao San Road area, Bangkok. Southeast Asian J. Trop. Med. Public Health 2013, 44, 690–696. [Google Scholar] [PubMed]
- Manieri, M.; Svensson, H.; Stafstrom, M. Sex tourist risk behaviour-an on-site survey among Swedish men buying sex in Thailand. Scand. J. Public Health 2013, 41, 392–397. [Google Scholar] [CrossRef] [PubMed]
- Matteelli, A.; Schlagenhauf, P.; Carvalho, A.C.; Weld, L.; Davis, X.M.; Wilder-Smith, A.; Barnett, E.D.; Parola, P.; Pandey, P.; Han, P.; et al. Travel-associated sexually transmitted infections: An observational cross-sectional study of the GeoSentinel surveillance database. Lancet Infect. Dis. 2013, 13, 205–213. [Google Scholar] [CrossRef]
- Mercer, C.H.; Fenton, K.A.; Wellings, K.; Copas, A.J.; Erens, B.; Johnson, A.M. Sex partner acquisition while overseas: Results from a British national probability survey. Sex. Transm. Infect. 2007, 83, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Streeton, C.L.; Zwar, N. Risk of exposure to hepatitis B and other blood-borne viruses among Australians who travel abroad. J. Travel Med. 2006, 13, 345–350. [Google Scholar] [CrossRef] [PubMed]
- Whelan, J.; Belderok, S.; van den Hoek, A.; Sonder, G. Unprotected casual sex equally common with local and western partners among long-term Dutch travelers to (sub) tropical countries. J. Sex. Transm. Dis. 2013, 40, 797–800. [Google Scholar] [CrossRef] [PubMed]
- Zuckerman, J.N.; Hoet, B. Hepatitis B immunisation in travellers: Poor risk perception and inadequate protection. Travel Med. Infect. Dis. 2008, 6, 315–320. [Google Scholar] [CrossRef] [PubMed]
- Zuckerman, J.N.; Steffen, R. Risks of hepatitis B in travelers as compared to immunization status. J. Travel Med. 2000, 7, 170–174. [Google Scholar] [CrossRef] [PubMed]
- Combs, B.C.; Giele, C.M. An increase in overseas acquired HIV infections among heterosexual people in Western Australia. Sex. Health 2009, 6, 35–39. [Google Scholar] [CrossRef] [PubMed]
- Ansart, S.; Hochedez, P.; Perez, L.; Bricaire, F.; Caumes, E. Sexually transmitted diseases diagnosed among travelers returning from the tropics. J. Travel Med. 2009, 16, 79–83. [Google Scholar] [CrossRef] [PubMed]
- Bauer, I. Understanding sexual relationships between tourists and locals in Cuzco/Peru. Travel Med. Infect. Dis. 2007, 5, 287–294. [Google Scholar] [CrossRef] [PubMed]
- Brown, G.; Ellard, J.; Mooney-Somers, J.; Hildebrand, J.; Langdon, T. HIV risk among Australian men travelling overseas: Networks and context matter. Cult. Health Sex. 2012, 14, 677–690. [Google Scholar] [CrossRef] [PubMed]
- Brown, G.; Ellard, J.; Mooney-Somers, J.; Prestage, G.; Crawford, G.; Langdon, T. “Living a life less ordinary”: Exploring the experiences of Australian men who have acquired HIV overseas. Sex. Health 2014, 11, 547–555. [Google Scholar] [CrossRef] [PubMed]
- Collins, D. “We’re there and queer”: Homonormative mobility and lived experience among gay expatriates in Manila. Gend. Soc. 2009, 23, 465–493. [Google Scholar] [CrossRef]
- Kelly, D.; Hughes, K.; Bellis, M. Work hard, party harder: Drug use and sexual behaviour in young British casual workers in Ibiza, Spain. Int. J. Environ. Res. Public Health 2014, 11, 10051–10061. [Google Scholar] [CrossRef] [PubMed]
- Dias, S.; Marques, A.; Gama, A.; Martins, M. HIV risky sexual behaviors and HIV infection among immigrants: A cross-sectional study in Lisbon, Portugal. Int. J. Environ. Res. Public Health 2014, 11, 8552–8566. [Google Scholar] [CrossRef] [PubMed]
- Davidson, J.O.C. The sex tourist, the expatriate, his ex-wife and her other’: The politics of loss, difference and desire. Sexualities 2001, 4, 5–24. [Google Scholar] [CrossRef]
- Croughs, M.; Remmen, R.; Van den Ende, J. The effect of pre-travel advice on sexual risk behavior abroad: A systematic review. J. Travel Med. 2014, 21, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Bauer, I. Australian senior adventure travellers to Peru: Maximising older tourists’ travel health experience. Travel Med. Infect. Dis. 2012, 10, 59–68. [Google Scholar] [CrossRef] [PubMed]
| Databases | PsycINFO, MEDLINE, ProQuest, Scopus, Global Health, Web of Science, Embase |
| Search Terms | Sexual health related terms (“sexually transmitted infection” OR “sexually transmissible infection” OR “sexually transmitted disease” OR “sexually transmissible disease” OR “human immunodeficiency virus” OR “blood borne virus” OR STI OR HIV OR BBV OR STD OR sex OR “condom use” OR “sexual health” OR “sexual behavior” OR “sexual behavior” OR “sexual health risk” OR “sexual risk” OR “unsafe sex” OR “unprotected sex” OR “casual sex” OR “sexual intercourse” OR “sexual health behavior” OR “sexual health behavior” OR “venereal disease”) |
| Expatriate and traveler related terms (expatriate OR traveler OR traveler OR “overseas volunteering” OR “military personnel” OR “aid work” OR “humanitarian aid” OR “lifestyle migration” OR “residential tourism” OR “international retirement migration” OR retirement OR retirees OR relocate OR relocation OR “transnational travel” OR “corporate travel” OR “business travel” OR “occupational travel” OR mining) | |
| Target group related terms (male OR men) |
| Overview | Twenty-six peer reviewed articles. Published between 2000 and 2015. High degree of variability in the study design and demographics. |
| Risk factors for acquisition of HIV or other STIs | Travel to a low-income region or region perceived to be less repressive, longer duration of stay. |
| Single relationship status, travel specifically for romance or sex, (commercial or non-commercial). | |
| Alcohol and other drug use and not receiving pre-travel advice. | |
| Being male having a higher number of sexual partners and a lack of, or inconsistent condom use. | |
| Other key findings in relation to HIV or other STIs | Levels of knowledge were poor. |
| Few studies comprehensively discussed pre-travel advice. | |
| Protective factors | Vaccinations and pre-travel health advice (particularly for older travelers). |
| Being female and fewer sexual partners. | |
| Recommendations | Lack of policy ready recommendations and only a third provided recommendations for research. |
| Focus on education and travel health advice, for example prevention opportunities to increase vaccination rates. |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Crawford, G.; Lobo, R.; Brown, G.; Macri, C.; Smith, H.; Maycock, B. HIV, Other Blood-Borne Viruses and Sexually Transmitted Infections amongst Expatriates and Travellers to Low- and Middle-Income Countries: A Systematic Review. Int. J. Environ. Res. Public Health 2016, 13, 1249. https://doi.org/10.3390/ijerph13121249
Crawford G, Lobo R, Brown G, Macri C, Smith H, Maycock B. HIV, Other Blood-Borne Viruses and Sexually Transmitted Infections amongst Expatriates and Travellers to Low- and Middle-Income Countries: A Systematic Review. International Journal of Environmental Research and Public Health. 2016; 13(12):1249. https://doi.org/10.3390/ijerph13121249
Chicago/Turabian StyleCrawford, Gemma, Roanna Lobo, Graham Brown, Chloe Macri, Hannah Smith, and Bruce Maycock. 2016. "HIV, Other Blood-Borne Viruses and Sexually Transmitted Infections amongst Expatriates and Travellers to Low- and Middle-Income Countries: A Systematic Review" International Journal of Environmental Research and Public Health 13, no. 12: 1249. https://doi.org/10.3390/ijerph13121249
APA StyleCrawford, G., Lobo, R., Brown, G., Macri, C., Smith, H., & Maycock, B. (2016). HIV, Other Blood-Borne Viruses and Sexually Transmitted Infections amongst Expatriates and Travellers to Low- and Middle-Income Countries: A Systematic Review. International Journal of Environmental Research and Public Health, 13(12), 1249. https://doi.org/10.3390/ijerph13121249







