A Comparison of Direct and Two-Stage Transportation of Patients to Hospital in Poland
Abstract
:1. Introduction
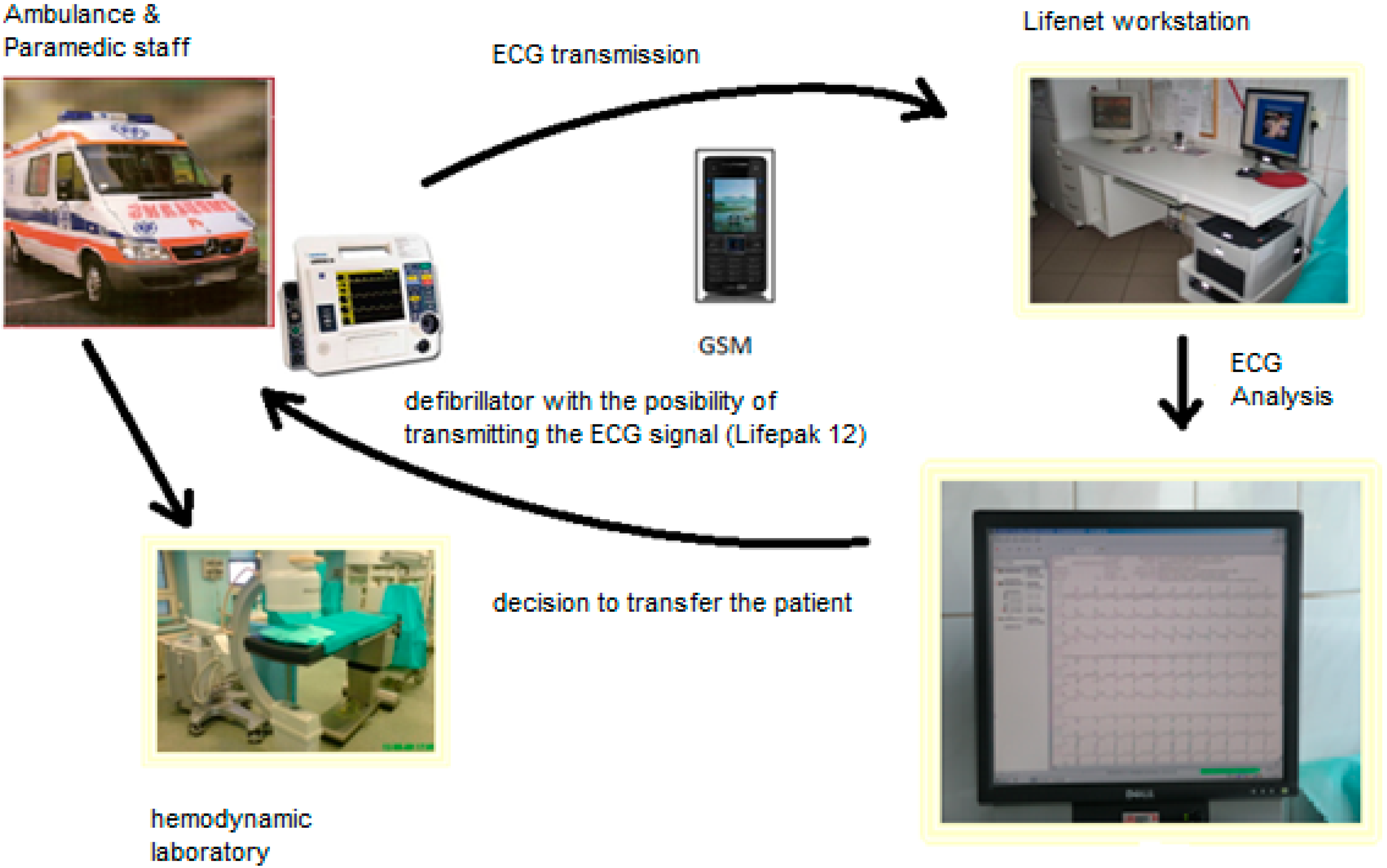
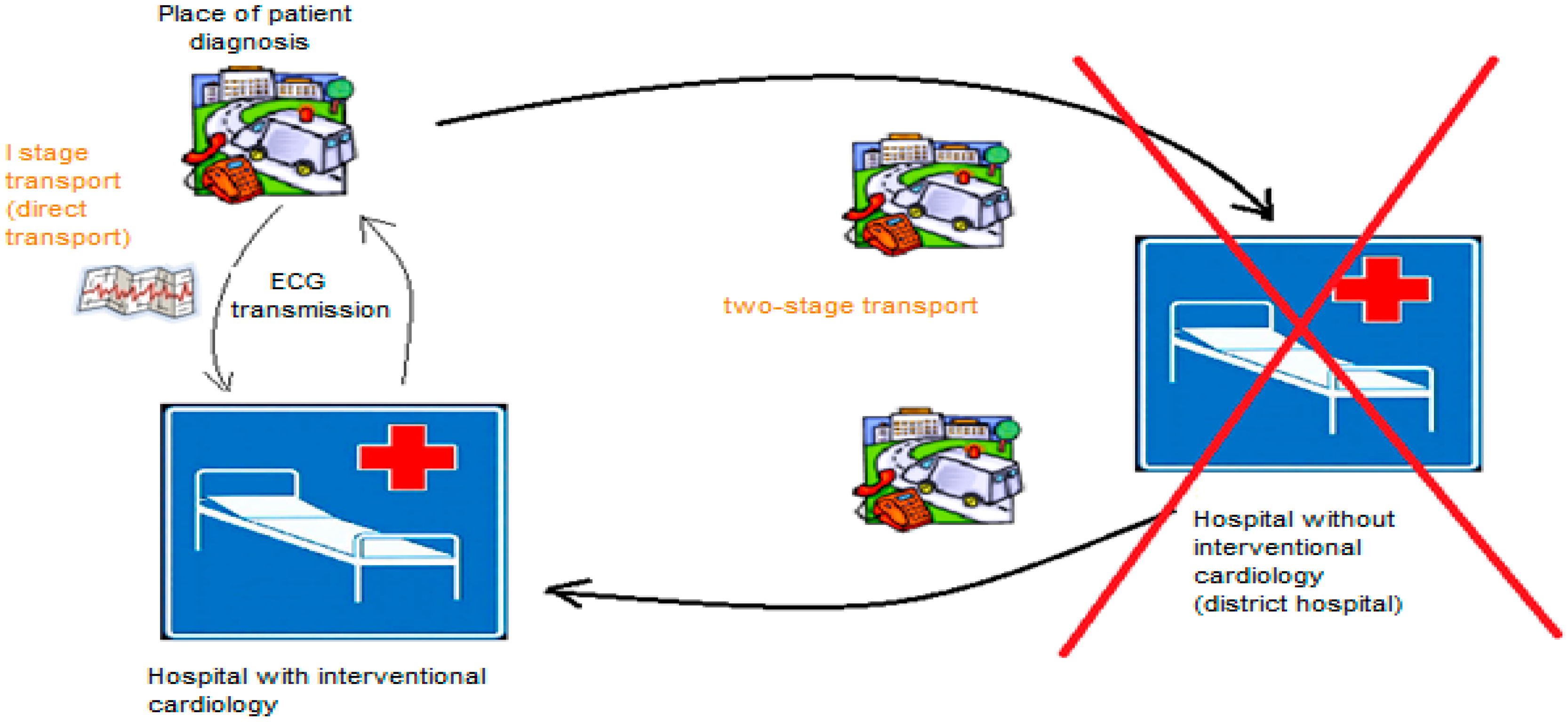
2. Materials and Methods
| Two-Stage Transport to a Referral Hospital | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Sex | STEMI | NSTEMI | UA | Sum | p | ||||
| No. | % | No. | % | No. | % | No. | % | ||
| Female | 10 | 14.9 | 10 | 14.9 | 2 | 3.0 | 22 | 32.8 | p < 0.05 |
| Male | 21 | 31.4 | 23 | 34.3 | 1 | 1.5 | 45 | 67.2 | |
| Sum | 31 | 46.3 | 33 | 49.2 | 3 | 4.5 | 67 | 100 | |
| Education Level | STEMI | NSTEMI | UA | Sum | p | ||||
| No. | % | No. | % | No. | % | No. | % | ||
| Elementary Level | 8 | 12.0 | 11 | 16.4 | 1 | 1.5 | 20 | 29.9 | p > 0.05 |
| Basic Technical | 16 | 23.9 | 13 | 19.4 | 2 | 3.0 | 31 | 46.3 | |
| High School | 6 | 8.9 | 2 | 3.0 | 0 | 0 | 8 | 11.9 | |
| University Level | 1 | 1.5 | 7 | 10.4 | 0 | 0 | 8 | 11.9 | |
| Sum | 31 | 46.3 | 33 | 49.2 | 3 | 4.5 | 67 | 100 | |
- -
- the time of admission to the hospital (time from the beginning of transportation from district hospital to reference center ) and the start of coronary angiography—average time was 140 min and,
- -
- the time of admission to the hospital and the start of coronary angioplasty—average time was 95 min.
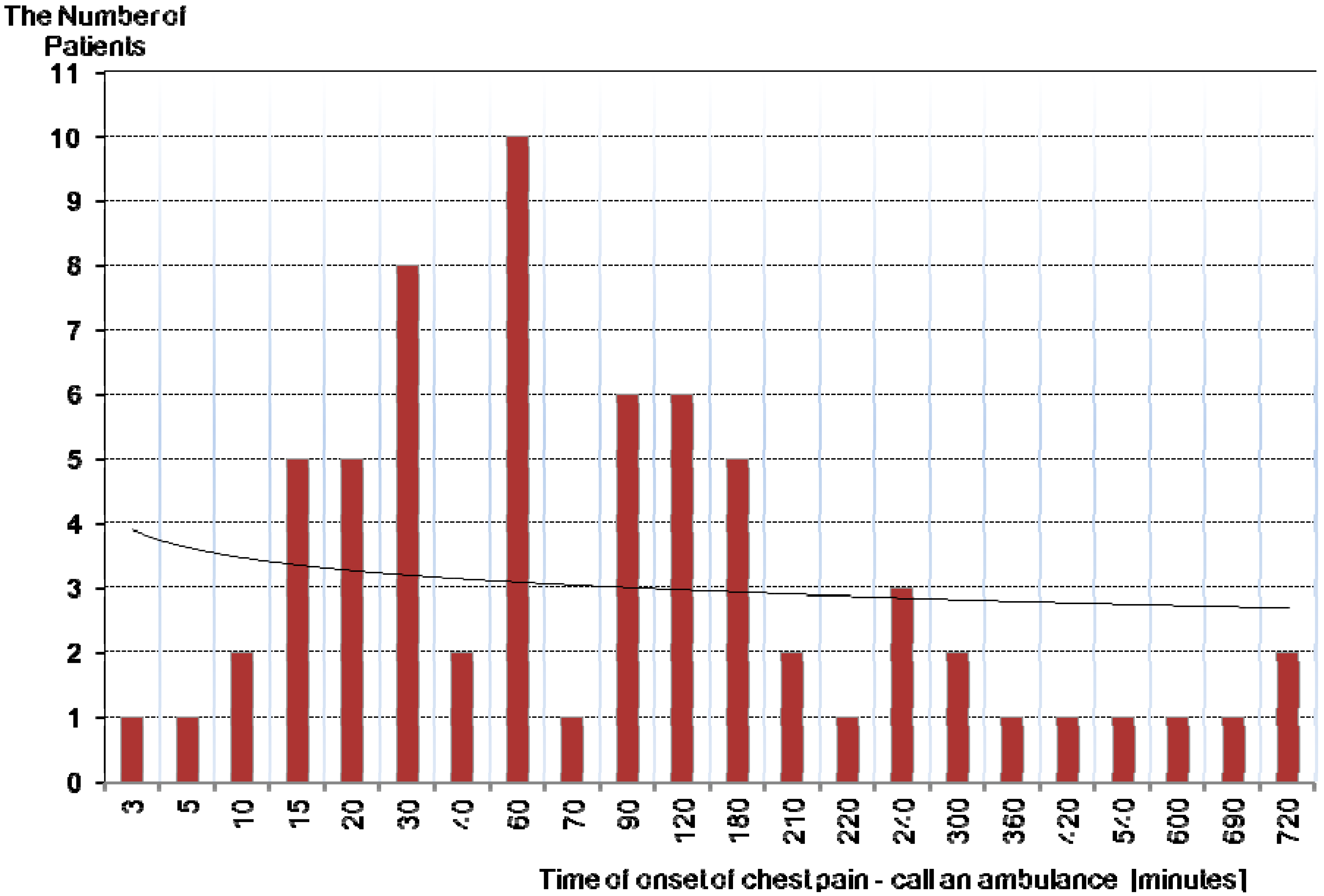
3. Results
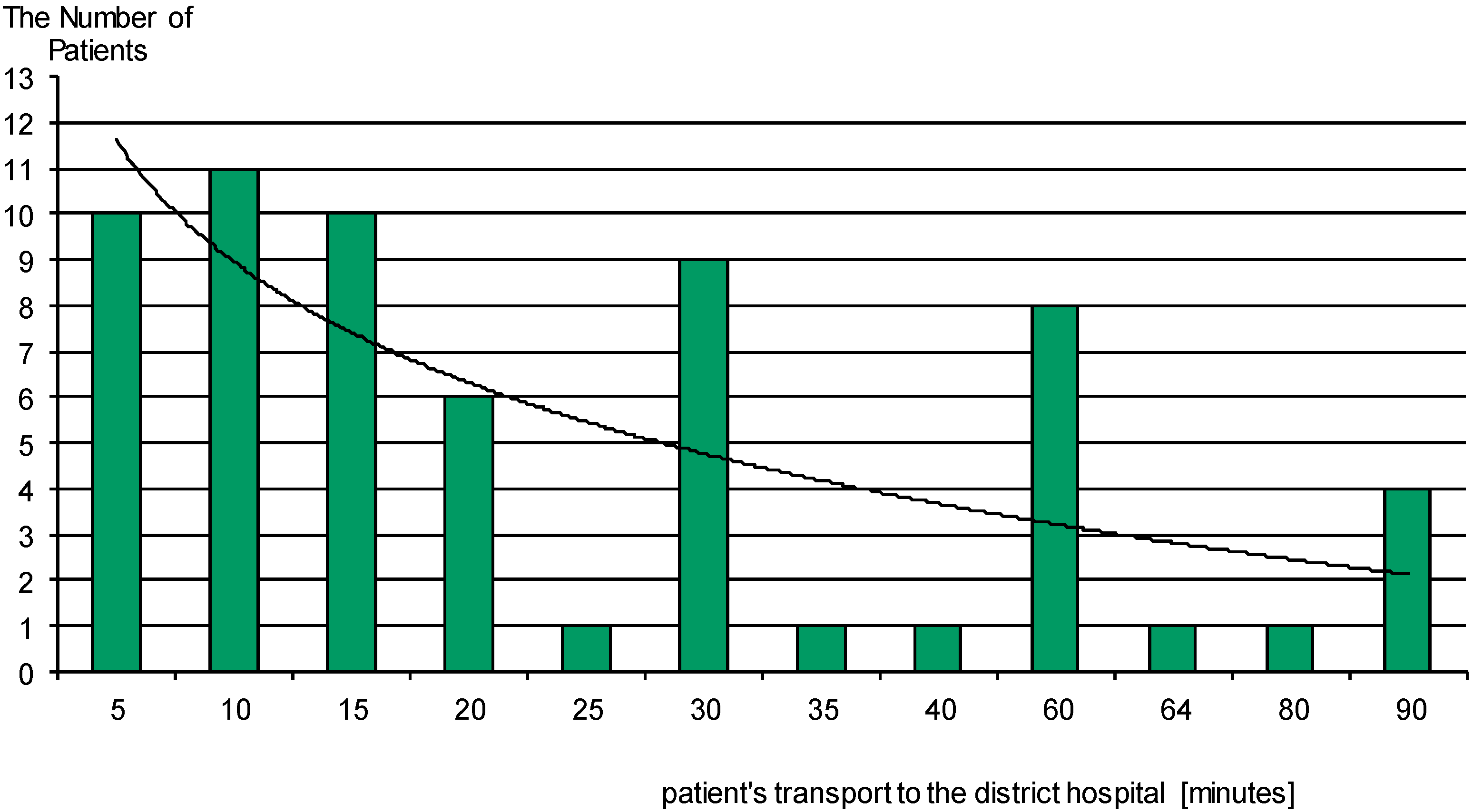
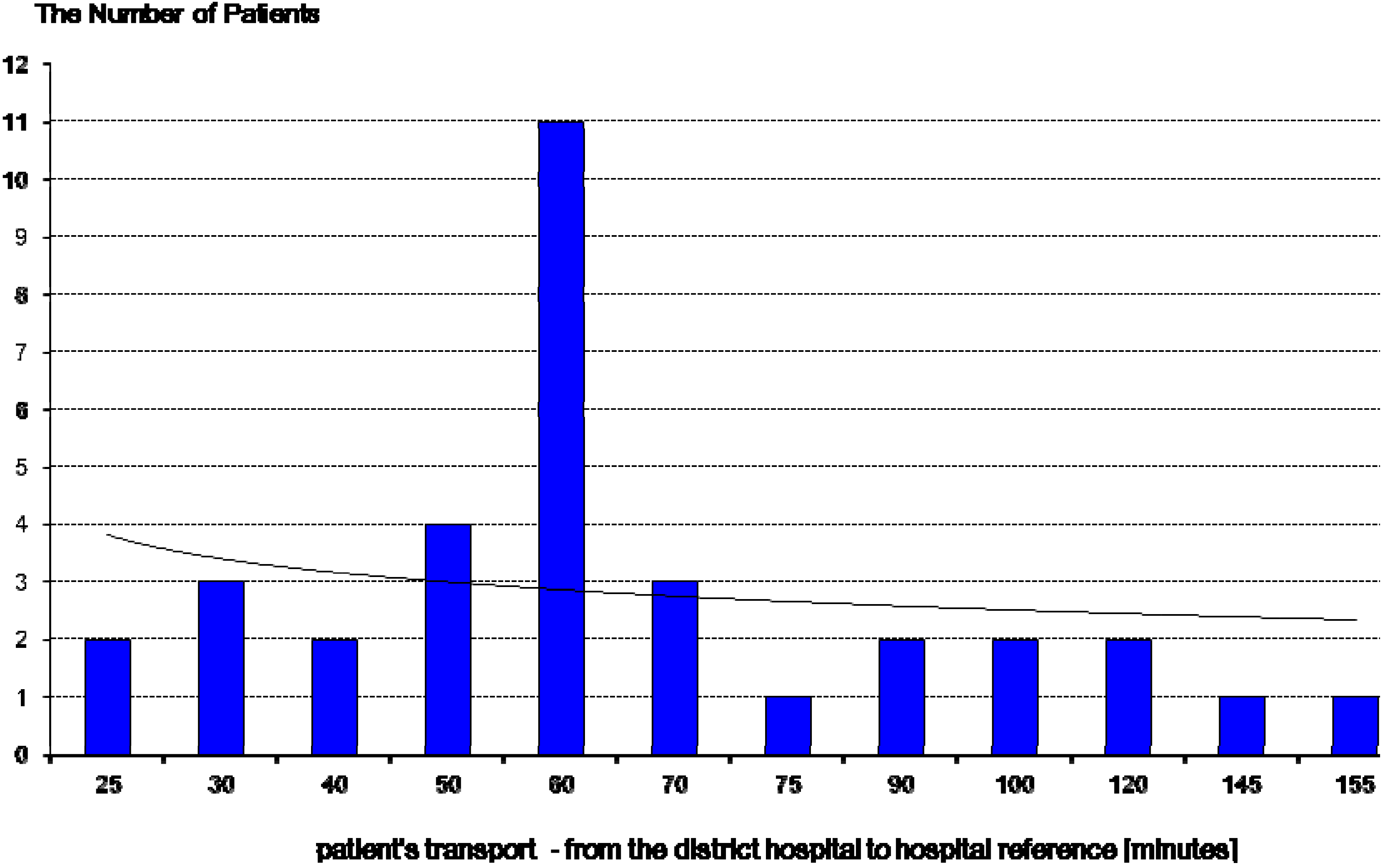
| Two-Stage Transport to a Referral Hospital | Timedelays Sume (Dependent and Independent) | Group | p |
|---|---|---|---|
| N = 67 | |||
| STEMI | 95 min | 31 | <0.0001 |
| NSTEMI | N/A | 33 | 0.2692 |
| UA | 140 min | 3 | <0.0001 |
| Diagnosis with using technology (One-stage transport) | 28 min | 67 | N/A |
4. Discussion
- -
- The most critical moment occurs at an early stage when the patient is in pain and is at risk of sudden cardiac arrest.
- -
- Early reperfusion minimizes the effects of the so-called myocardial infarction (infarction scar).
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Gaseau, M. Corrections technology options are expanding. Corr. Today 1999, 61, 22–26. [Google Scholar]
- Wright, L.B. The use of telemedicine in correctional facilities. Acad. Exchange Quart. 2002, 6, 16–24. [Google Scholar]
- Buntin, M.B.; Burke, M.F.; Hoaglin, M.C.; Blumenthal, D. The benefits of health information technology: A review of the literature shows predominantly positive results. Health Aff. (Millwood) 2011, 30, 464–471. [Google Scholar] [CrossRef]
- Johansson, I.; Stromberg, A.; Swahn, E. Ambulance use in patients with acute myocardial infarction. J. Cardiovasc. Nurs. 2004, 19, 5–12. [Google Scholar] [CrossRef] [PubMed]
- Steg, P.G.; James, S.K.; Atar, D.; Badano, L.P.; Blomstrom-Lundqvist, C.; Borger, M.A.; di Mario, C.; Dickstein, K.; Ducrocq, G.; Fernandez-Aviles, F.; et al. ESC Guidelines for the management of acute mycocardial infraction in patients presenting with ST-segment elevation. Eur. Heart J. 2012, 20, 2569–2619. [Google Scholar]
- American Telemedicine Association. Available online: http://atmed.org (accessed on 20 April 2015).
- Mencl, F.; Wilber, S.; Frey, J.; Zalewski, J.; Maiers, J.F.; Bhalla, M.C. Paramedic ability to recognize ST-segment elevation myocardial infarction on prehospital electrocardiograms. Prehosp. Emerg. Care 2013, 17, 203–210. [Google Scholar] [CrossRef] [PubMed]
- Ryan, D.; Craig, A.M.; Turner, L.; Verbeek, P.R. Clinical events and treatment in prehospital patients with ST-segment elevation myocardial infarction. Prehosp. Emerg. Care 2013, 17. [Google Scholar] [CrossRef]
- Terkelsen, C.J.; Lassen, J.F.; Norgaard, B.L.; Gerdes, J.C.; Poulsen, S.H.; Bendix, K.; Ankersen, J.P.; Gotzsche, L.B.; Romer, F.K.; Nielsen, T.T.; et al. Reduction of treatment delay in patients with ST-elevation myocardial infarction: impact of pre-hospital diagnosis and direct referral to primary percutaneous coronary intervention. Eur. Heart J. 2005, 26, 770–777. [Google Scholar] [CrossRef]
- Hess, D.C.; Wang, S.; Hamilton, W.; Lee, S.; Pardue, C.; Waller, J.L.; Gross, H.; Nichols, F.; Hall, C.; Adams, R.J. REACH: Clinical feasibility of a rural telestroke network. Stroke 2005, 36. [Google Scholar] [CrossRef]
- Waite, K.; Silver, F.; Jaigobin, C.; Black, S.; Lee, L.; Murray, B.; Danyliuk, P.; Brown, E.M. Telestroke: A multi-site, emergency-based telemedicine service in Ontario. J. Telemed. Telecare 2006, 12. [Google Scholar] [CrossRef] [PubMed]
- Liman, T.G.; Winter, B.; Waldschmidt, C.; Zerbe, N.; Hufnagl, P.; Audebert, H.J.; Endres, M. Telestroke ambulances in prehospital stroke management: Concept and pilot feasibility study. Stroke 2012, 43. [Google Scholar] [CrossRef]
- Puetz, V.; Bodechtel, U.; Gerber, J.C.; Dzialowski, I.; Kunz, A.; Wolz, M.; Hentschel, H.; Schultheiss, T.; Kepplinger, J.; Schneider, H.; et al. Reliability of brain CT evaluation by stroke neurologists in telemedicine. Neurology 2013, 80. [Google Scholar] [CrossRef]
- Emergency Telemedicine in Wielkopolska, Termedia. Available online: http://www.termedia.pl/telemedycyna-ratunkowa-w-wielkopolsce.1174.html (accessed on 1 July 2013).
- Zanini, R.; Aroldi, M.; Bonatti, S.; Buffoli, F.; Izzo, A.; Lettieri, C.; Romano, M.; Tomasi, L.; Ferrari, M.R. Impact of prehospital diagnosis in the management of ST elevation myocardial infarction in the era of primary percutaneous coronary intervention: Reduction of treatment delay and mortality. J. Cardiovasc. Med. 2008, 9. [Google Scholar] [CrossRef]
- Sanchez-Ross, M.; Oghlakian, G.; Maher, J.; Patel, B.; Mazza, V.; Hom, D.; Dhruva, V.; Langley, D.; Palmaro, J.; Ahmed, S.; et al. The STAT-MI (ST-Segment Analysis Using Wireless Technology in Acute Myocardial Infarction) trial improves outcomes. J. Am. Coll. Cardiol. Intv. 2011, 4. [Google Scholar] [CrossRef]
- LaMonte, M.P.; Xiao, Y.; Hu, P.F.; et al. Shortening time to stroke treatment using ambulance telemedicine: TeleBAT. J. Stroke Cerebrovasc. Dis. 2004, 13, 148–154. [Google Scholar] [CrossRef]
- Levine, S.R.; Gorman, M. “Telestroke”: The application of telemedicine for stroke. Stroke 1999, 30, 464–469. [Google Scholar] [CrossRef] [PubMed]
- European Stroke Organisation (ESO) Executive Committee; ESO Writing Committee. Guidelines for management of ischaemic stroke and transient ischaemic attack 2008. Cerebrovasc. Dis. 2008, 25, 457–507. [Google Scholar]
- Evenson, K.R.; Rosamond, W.D.; Morris, D.L. Prehospital and in-hospital delays in acute stroke care. Neuroepidemiology 2001, 20, 65–76. [Google Scholar] [CrossRef] [PubMed]
- Moser, D.; Kimble, L.; Alberts, M.; Alonzo, A.; Croft, J.; Dracup, K.; Evenson, K.; Go, A.; Hand, M.; Kothari, R.; et al. Reducing delay in seeking treatment by patients with acute coronary syndrome and stroke: A scientific statement from the American Heart Association Council on cardiovascular nursing and stroke council. Circulation 2006, 114, 168–182. [Google Scholar] [CrossRef]
- Mosley, I.; Nicol, M.; Donnan, G.; Patrick, I.; Kerr, F.; Dewey, H. The impact of ambulance practice on acute stroke care. Stroke 2007, 38, 2765–2770. [Google Scholar] [CrossRef] [PubMed]
- Burges Watson, D.L.; Sanoff, R.; Mackintosh, J.E.; et al. Evidence from the scene: Paramedic perspectives on involvement in out-of-hospital research. Ann. Emerg. Med. 2012, 60, 641–650. [Google Scholar] [CrossRef]
- Demaerschalk, B.M.; Bobrow, B.J.; Raman, R.; Ernstrom, K.; Hoxworth, J.M.; Patel, A.C.; Kiernan, T.E.; Aguilar, M.I.; Ingall, T.J.; Dodick, D.W.; et al. CT interpretation in a telestroke network: Agreement among a spoke radiologist, hub vascular neurologist, and hub neuroradiologist. Stroke 2012, 43, 3095–3097. [Google Scholar] [CrossRef]
- Schwamm, L.H.; Holloway, R.G.; Amarenco, P.; Audebert, H.J.; Bakas, T.; Chumbler, N.R.; Handschu, R.; Jauch, E.C.; Knight, W.A., 4th; Levine, S.R.; et al. A review of the evidence for the use of telemedicine within stroke systems of care: A scientific statement from the American Heart Association/American Stroke Association. Stroke 2009, 40, 2616–2634. [Google Scholar] [CrossRef]
- Schwamm, L.H.; Audebert, H.J.; Amarenco, P.; Chumbler, N.R.; Frankel, M.R.; George, M.G.; Gorelick, P.B.; Horton, K.B.; Kaste, M.; Lackland, D.T.; et al. Recommendations for the implementation of telemedicine within stroke systems of care: A policy statement from the American Heart Association. Stroke 2009, 40, 2635–2660. [Google Scholar] [CrossRef] [PubMed]
- Meyer, B.C.; Raman, R.; Hemmen, T.; Obler, R.; Zivin, J.A.; Rao, R.; Thomas, R.G.; Lyden, P.D. Efficacy of site-independent telemedicine in the STRokE DOC trial: A randomised, blinded, prospective study. Lancet Neurol. 2008, 7, 787–795. [Google Scholar] [CrossRef] [PubMed]
- Pervez, M.A.; Silva, G.; Masrur, S.; Betensky, R.A.; Furie, K.L.; Hidalgo, R.; Lima, F.; Rosenthal, E.S.; Rost, N.; Viswanathan, A.; Schwamm, L.H. Remote supervision of IV-tPA for acute ischemic stroke by telemedicine or telephone before transfer to a regional stroke center is feasible and safe. Stroke 2010, 41, e18–e24. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Lee, S.B.; Pardue, C.; Ramsingh, D.; Waller, J.; Gross, H.; Nichols, F.T., 3rd; Hess, D.C.; Adams, R.J. Remote evaluation of acute ischemic stroke: Reliability of National Institutes of Health Stroke Scale via telestroke. Stroke 2003, 34, e188–e191. [Google Scholar] [CrossRef]
- Wiborg, A.; Widder, B.; for the TESS Study Group. Teleneurology to improve stroke care in rural areas: The Telemedicine in Stroke in Swabia (TESS) project. Stroke 2003, 34, 2951–2956. [Google Scholar] [CrossRef]
- Kwan, J.; Hand, P.; Sandercock, P. A systematic review of barriers to delivery of thrombolysis for acute stroke. Age Ageing 2004, 33, 116–121. [Google Scholar] [CrossRef] [PubMed]
- Pedragosa, A.; Alvarez-Sabin, J.; Molina, C.A.; Sanclemente, C.; Martín, M.C.; Alonso, F.; Ribo, M. Impact of a telemedicine system on acute stroke care in a community hospital. J. Telemed. Telecare 2009, 15. [Google Scholar] [CrossRef] [PubMed]
- Reid, J. A telemedicine primer: Understanding the issues; Innovative Medical Communications: Topeka, KS, USA, 1996. [Google Scholar]
- Utterback, K. Supporting A New Model of Care with Telehealth Technology. Telemedicine Information Exchange. January/February 2005. Available online: http://tie.telemed.org/articles/article.asp?path=articles&article=telehealthTechnology_ku_tpr05.xml (accessed on 31 May 2008).
- Ahmed, B.; Lischke, S.; Straight, F.; Gogo, P.; Leffler, S.; Kutler, M.; Schneider, D.J.; Dauerman, H.L. Consistent door-to-balloon times of less than 90 minutes for STEMI patients transferred for primary PCI. J. Invasive Cardiol. 2009, 21, 429–433. [Google Scholar] [PubMed]
- Le May, M.R.; So, D.Y.; Dionne, R.; Glover, C.A.; Froeschl, M.P.; Wells, G.A.; Davies, R.F.; Sherrard, H.L.; Maloney, J.; Marquis, J.-F.; et al. A citywide protocol for primary PCI in ST-segment elevation myocardial infarction. N. Engl. J. Med. 2008, 358, 231–240. [Google Scholar] [CrossRef]
- Neumar, R.W.; Nolan, J.P.; Adrie, C.; Aibiki, M.; Berg, R.A.; Bottiger, B.W.; Callaway, C.; Clark, R.S.; Geocadin, R.G.; Jauch, E.C.; et al. Post-cardiac arrest syndrome: Epidemiology, pathophysiology, treatment, and prognostication. A consensus statement from the International Liaison Committee on Resuscitation (American Heart Association, Australian and New Zealand Council on Resuscitation, European Resuscitation Council, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Council of Asia, and the Resuscitation Council of Southern Africa); the American Heart Association Emergency Cardiovascular Care Committee; the Council on Cardiovascular Surgery and Anesthesia; the Council on Cardiopulmonary, Perioperative, and Critical Care; the Council on Clinical Cardiology; and the Stroke Council. Circulation 2008, 118, 2452–2483. [Google Scholar] [CrossRef]
- Goldberg, R.J.; Steg, P.G.; Sadiq, I.; Granger, C.B.; Jackson, E.A.; Budaj, A.; Brieger, D.; Avezum, A.; Goodman, S. Extent of, and factors associated with, delay to hospital presentation in patients with acute coronary disease (the GRACE registry). Am. J. Cardiol. 2002, 89, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Rosenfeld, A.G. Women’s risk of decision delay in acute myocardial infarction: Implications for research and practice. AACN Clin. Iss. 2001, 12, 29–39. [Google Scholar] [CrossRef]
- O’Gara, P.T.; Kushner, F.G.; Ascheim, D.D.; et al. ACCF/AHA Guidelines for the management of ST-Elevation of Mycocardial infraction: A report of American College of Cardiology Fundation/American Heart Association task force on practice guidelines. Circulation 2012. [Google Scholar] [CrossRef]
- Peberdy, M.A.; Callaway, C.W.; Neumar, R.W.; Geocadin, R.G.; Zimmerman, J.L.; Donnino, M.; Gabrielli, A.; Silvers, S.M.; Zaritsky, A.L.; Merchant, R.; et al. Part 9: Post–Cardiac Arrest Care 2010 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 2010, 122. [Google Scholar] [CrossRef] [PubMed]
- Safar, P. Resuscitation from clinical death: Pathophysiologic limits and therapeutic potentials. Crit. Care Med. 1988, 16, 923–941. [Google Scholar] [CrossRef] [PubMed]
- Hypothermia After Cardiac Arrest Study Group. Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N. Engl. J. Med. 2002, 346, 549–556. [Google Scholar]
- Gaieski, D.F.; Band, R.A.; Abella, B.S.; Neumar, R.W.; Fuchs, B.D.; Kolansky, D.M.; Merchant, R.M.; Carr, B.G.; Becker, L.B.; Maguire, C.; et al. Early goal-directed hemodynamic optimization combined with therapeutic hypothermia in comatose survivors of out-of-hospital cardiac arrest. Resuscitation 2009, 80, 418–424. [Google Scholar] [CrossRef] [PubMed]
- Kirves, H.; Skrifvars, M.B.; Vahakuopus, M.; Ekstrom, K.; Martikainen, M.; Castren, M. Adherence to resuscitation guidelines during prehospital care of cardiac arrest patients. Eur. J. Emerg. Med. 2007, 14, 75–81. [Google Scholar] [CrossRef] [PubMed]
- Sunde, K.; Pytte, M.; Jacobsen, D.; Mangschau, A.; Jensen, L.P.; Smedsrud, C.; Draegni, T.; Steen, P.A. Implementation of a standardised treatment protocol for post resuscitation care after out-of-hospital cardiac arrest. Resuscitation 2007, 73, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Kosiński, S.; Darocha, T.; Gałązkowski, R.; Drwiła, R. Accidental hypothermia in Poland—Estimation of prevalence, diagnostic methods and treatment. Scand. J. Trauma Resusc. Emerg. Med. 2015, 23. [Google Scholar] [CrossRef]
- Moser, D.K.; Kimble, L.P.; Alberts, M.J.; Alonzo, A.; Croft, J.B.; Dracup, K.; Evenson, K.R.; Go, A.S.; Hand, M.M.; Kothari, R.U.; et al. Reducing delay in seeking treatment by patients with acute coronary syndrome and stroke. Circulation 2006, 114, 168–182. [Google Scholar] [CrossRef] [PubMed]
- Van de Werf, F.; Bax, J.; Betriu, A.; Blomstrom-Lundqvist, C.; Crea, F.; Falk, V.; Filippatos, G.; Fox, K.; Huber, K.; Kastrati, A.; et al. Management of acute myocardial infarction in patients presenting with persistent ST-segment elevation. The Task Force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology. Eur. Heart J. 2008, 29, 2909–2945. [Google Scholar] [CrossRef] [PubMed]
- Fukuoka, Y.; Dracup, K.; Ohno, M.; Kobayashi, F.; Hirayama, H. Symptom severity as a predictor of reported differences of prehospital delay between medical records and structured interviews among patients with AMI. Eur. J. Cardiovasc. Nurs. 2005, 4, 171–176. [Google Scholar] [CrossRef] [PubMed]
- Report Ambulancecare in Europe; Ambulancezorg Nederland: Veerallee, Netherlands, 2010; p. 30.
- Bashshur, R.; Sanders, J.; Shannon, G. Telemedicine: Theory and Practice; Charles C. Thomas: Springfield, IL, USA, 1997. [Google Scholar]
- Demiris, G. Introducing telemedicine within a health informatics curriculum. Acad. Exchange Quart. 2002, 6, 5–11. [Google Scholar]
- Spetz, J.; Keane, D. Information technology implementation in a rural hospital: A cautionary tale. Health Manag. 2009, 54, 337–347, discussion 348. [Google Scholar]
- Yellowlees, P.M.; Chorba, K.; Parish, M.B.; Wynn-Jones, H.; Nafiz, N. Telemedicine can make healthcare greener. Telemed. J. E-Health 2010, 16, 229–232. [Google Scholar] [CrossRef] [PubMed]
- Darkins, A.W.; Cary, M.A. Regulatory, legislative, and political considerations in telehealth. In Telemedicine and Telehealth; Springer: New York, NY, USA, 2002. [Google Scholar]
- Bassand, J.P.; Danchin, N.; Filippatos, G.; Gitt, A.; Hamm, C.; Silber, S.; Tubaro, M.; Weidinger, F. Implementation of reperfusion therapy in acute myocardial infarction. A policy statement from the European Society of Cardiology. Eur. Heart J. 2005, 26, 2733–2741. [Google Scholar] [CrossRef] [PubMed]
- Telemedicine Research Center. Telemedicine Information Exchange. 1997. Available online: http://208.129.211.51 (accessed on 20 April 2015).
- U.S. Department of Health and Human Services. Health Resources Services Administration. What is Telehealth? Available online: http://www.hrsa.gov/telehealth/default.htm (accessed on 10 May 2008).
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rosiek, A.; Rosiek-Kryszewska, A.; Leksowski, Ł.; Leksowski, K. A Comparison of Direct and Two-Stage Transportation of Patients to Hospital in Poland. Int. J. Environ. Res. Public Health 2015, 12, 4572-4586. https://doi.org/10.3390/ijerph120504572
Rosiek A, Rosiek-Kryszewska A, Leksowski Ł, Leksowski K. A Comparison of Direct and Two-Stage Transportation of Patients to Hospital in Poland. International Journal of Environmental Research and Public Health. 2015; 12(5):4572-4586. https://doi.org/10.3390/ijerph120504572
Chicago/Turabian StyleRosiek, Anna, Aleksandra Rosiek-Kryszewska, Łukasz Leksowski, and Krzysztof Leksowski. 2015. "A Comparison of Direct and Two-Stage Transportation of Patients to Hospital in Poland" International Journal of Environmental Research and Public Health 12, no. 5: 4572-4586. https://doi.org/10.3390/ijerph120504572
APA StyleRosiek, A., Rosiek-Kryszewska, A., Leksowski, Ł., & Leksowski, K. (2015). A Comparison of Direct and Two-Stage Transportation of Patients to Hospital in Poland. International Journal of Environmental Research and Public Health, 12(5), 4572-4586. https://doi.org/10.3390/ijerph120504572





