Assessing the Acceptability and Usability of an Internet-Based Intelligent Health Assistant Developed for Use among Turkish Migrants: Results of a Study Conducted in Bremen, Germany
Abstract
:1. Introduction
2. Methods
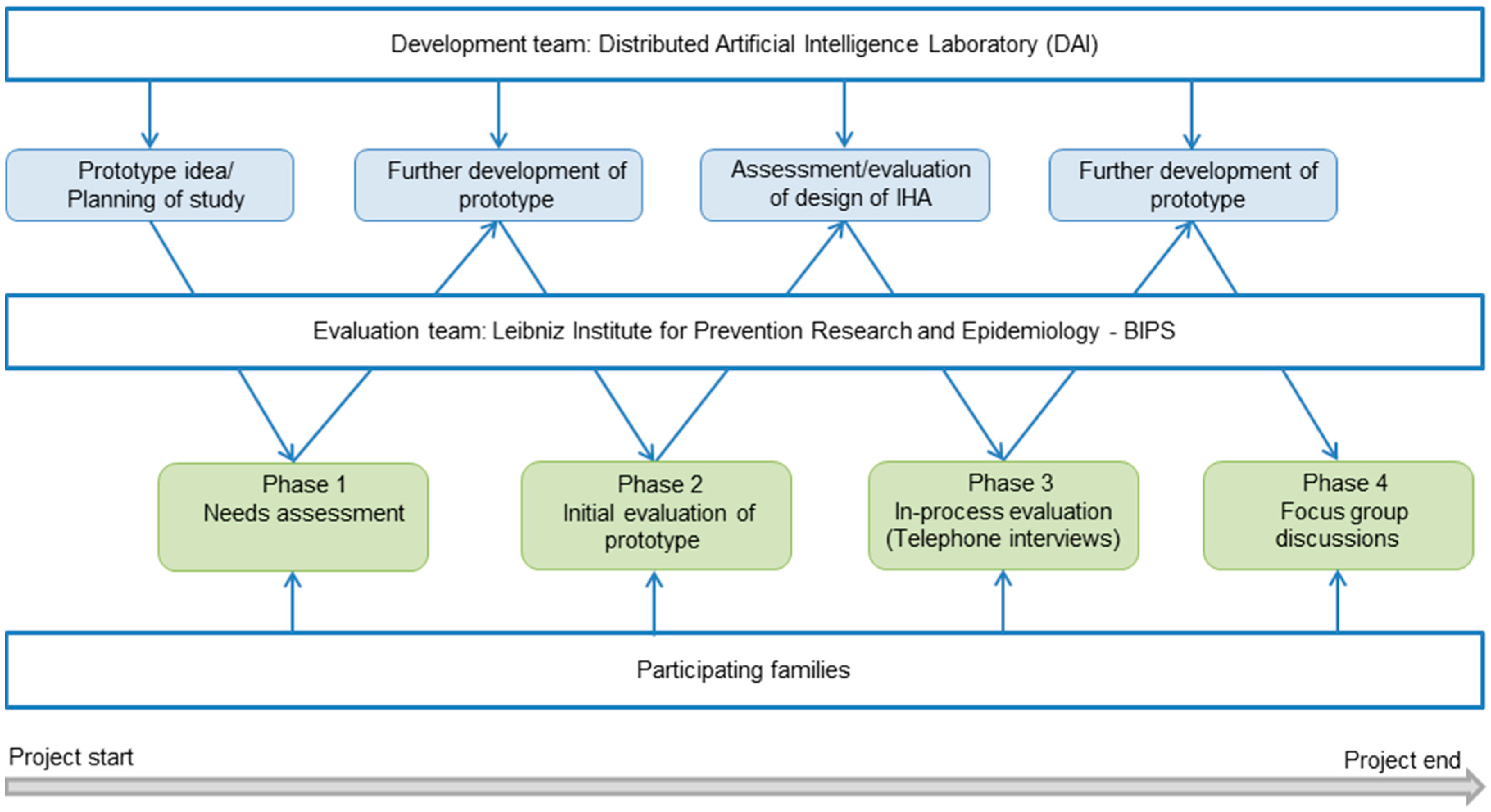

3. Results
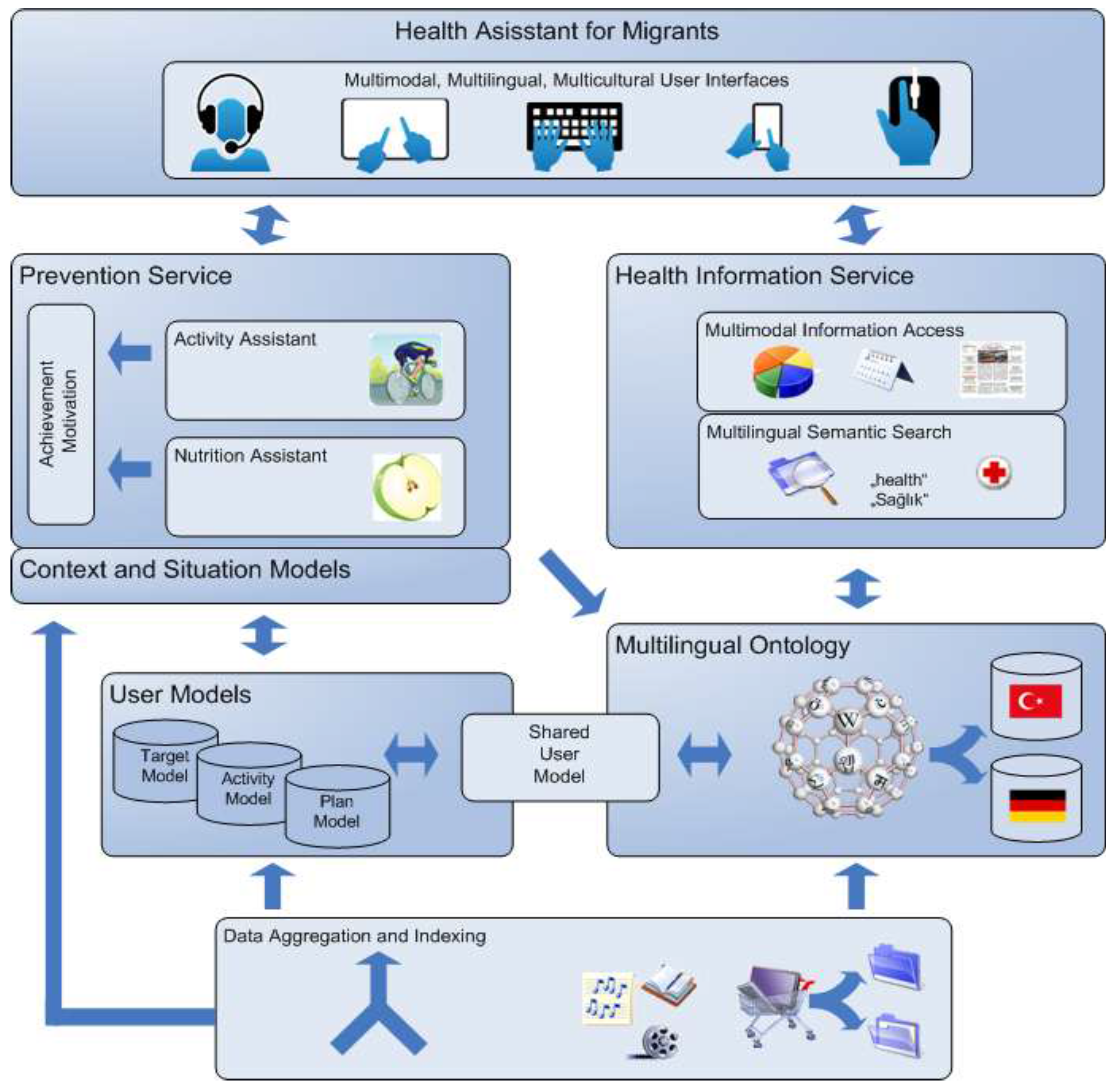
3.1. Features of the IHA
3.1.1. Health Information Service
3.1.2. Prevention Service
3.2. Description of Study Participants
| N = 28 | No Turkish Migrant Background (n = 9) 1 | Turkish Migrant Background (n = 19) |
|---|---|---|
| Age (in years) | ||
| 11–20 | 4 | 6 |
| 21–30 | 1 | 2 |
| 31–50 | 4 | 8 |
| 51–60 | - | 1 |
| 61–70 | - | 3 |
| Sex | ||
| Male | 3 | 6 |
| Female | 6 | 13 |
| School education | ||
| University entrance | 1 | 2 |
| Upper secondary school | 3 | 1 |
| Lower secondary school | 1 | 3 |
| College entrance | - | 1 |
| Still at school | 4 | 6 |
| No school certificate | - | 3 |
| Missing | - | 3 |
| Occupational status | ||
| Employed | 1 | 4 |
| Maternity leave | 2 | - |
| Unemployed | 2 | 9 |
| Still at school | 4 | 6 |
| Nationality | ||
| German | 8 | 4 |
| Turkish | - | 15 |
| Other | 1 | - |
| Country of birth | ||
| Germany | 8 | - |
| Turkey | - | 5 |
| Other | 1 | 14 |
| Length of stay in Germany (in years) | ||
| 4–10 | - | 3 |
| 11–20 | - | 3 |
| 21–41 | 1 | 8 |
| Not applicable | 8 | 5 |
3.2.1. Phase 1: Needs Assessment for Sources of Health Information
“It’s exactly what I need.” (Female, 38 years, no migrant background)“Yes well, if I had it, I would use it.” (Male, 13 years, Turkish migrant background)“That I really could picture well to myself, because that’s how it really is when one has questions I mean, that one can access Information quickly and informally.” (Female, 41 years, no migrant background)“Yes, well, for health. Just looking at a medical book is enough to make me lose interest in leafing through it, because it’s so thick. And when I just imagine that I have just this thing and can simply do this, I find that great.” (Female, 41 years, no migrant background)“…oh, maybe I would get so attached to it and ask it everything (laughs)—Should I eat this, should I not eat that? Would I be able to tolerate it (the food)?” (Female, 34 years, Turkish migrant background)“So, I imagine that questions which concern you come, e.g., in Summer, do you feel tired and are you lethargic? Then one thinks well, actually yes and then the answer would immediately appear, somehow a picture with a strawberry salad.” (Male, 29 years, Brazilian migrant background)“The assistant should tell one to drink something or to eat fruit, and in the evening tell you that you have taken too much sugar or fat, eaten too little fruit and drunk too little.” (Male, 40 years, Turkish migrant background)
3.2.2. Phase 2: Initial Evaluation of Prototype
“I can’t write Turkish well and can only read very slowly. One doesn’t even want to read if it’s written in German. Pictures would be good—videos too.” (Female, 34 years, Turkish migrant background).
3.2.3. Phase 3: Telephone Interviews
3.2.4. Focus Group Discussion
3.3. Cultural Sensitivity
“If it is in Turkish, I understand everything.” (Female, 51 years, Turkish migrant background)“If I don’t understand, I can switch to Turkish.” (Female, 43 years, Turkish migrant background)“It’s good when you don’t understand something or the whole text, for example, you can read it and see it in another language.” (Male, 16 years, Turkish migrant background)
“I mean Turkish people are—there are Turkish people who eat pork and drink alcohol. If these are included in the ingredients, one could highlight this or restrict the search.” (Female, 40 years, Turkish migrant background).
“That’s a nice pleasant thing—she doesn’t have to go somewhere where she will encounter difficulties. It’s comfortable—she can go in and inform herself about everything. That’s a nice thing.” (Female, 51 years old, Turkish migrant background)“It’s something which happens often. I mean, I’ve had similar experiences very often. I’ve observed this in my surrounding quite often. For example quite often I go along as a translator because of such things, because they need information, have some questions they can’t ask because they don’t speak and understand German well. That’s why it’s necessary—it is better in Bremen, there are two Turkish gynecologists—the women can inform themselves better, but such a thing would be natural—I mean she could inform herself from her home and needn’t go all the way to the doctor for every little thing. She can ask everything there and get the necessary information.” (Female, 23 years, Turkish migrant background)“Pregnancy needs life, I mean needs interaction, needs closeness, needs trust, the talks. I can’t even imagine using that thing in such circumstances.” (Female, 41 years, no migrant background)“I could well imagine that it would help someone who is new here and is not familiar with the structures.” (Female, 32 years, no migrant background)
“But where is the difference, I ask you. Is a pregnant Turkish woman different to a pregnant German woman?” (Female, 40 years, Turkish migrant background)
“I don’t know, it is easy and—if the person gets the right answer immediately, it is easier than going to the doctor.” (Female, 34 years, Turkish migrant background)
4. Discussion
Strengths and Limitations
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- International Telecommunication Union. The World in 2014. ICT Facts and Figures. Available online: http://www.itu.int/en/ITU-D/Statistics/Documents/facts/ICTFactsFigures2014-e.pdf (accessed on 1 April 2015).
- Srivastava, A. 2 Billion Smart Phone Users by 2015: 83% of Internet Usage from Mobiles (Study). Available online: http://dazeinfo.com/2014/01/23/smartphone-users-growth-mobile-internet-2014–2017/ (accessed on 1 April 2015).
- eMarketer Smartphone Users Worldwide Will Total 1.75 Billion in 2014: Mobile Users Pick up Smartphones as They Become More Affordable, 3G and 4G Networks Advance. Available online: http://www.emarketer.com/Article/Smartphone-Users-Worldwide-Will-Total-175-Billion-2014/1010536 (accessed on 1 April 2015).
- Tsai, C.C.; Lee, G.; Raab, F.; Norman, G.J.; Sohn, T.; Griswold, W.G.; Patrick, K. Usability and feasibility of PmEB: A mobile phone application for monitoring real time caloric balance. Mob. Netw. Appl. 2007, 12, 173–184. [Google Scholar] [CrossRef]
- Fjeldsoe, B.S.; Marshall, A.L.; Miller, Y.D. Behavior change interventions delivered by mobile telephone short-message service. Am. J. Prev. Med. 2009, 36, 165–173. [Google Scholar] [CrossRef] [PubMed]
- Haapala, I.; Barengo, N.C.; Biggs, S.; Surakka, L.; Manninen, P. Weight loss by mobile phone: A 1-year effectiveness study. Public Health Nutr. 2009, 12, 2382–2391. [Google Scholar] [CrossRef] [PubMed]
- Lopez, C. Faszination Mobile: Verbreitung, Nutzungsmuster und Trends. Bundesverband Digitale Wirtschaft in Kooperation mit Google und TNS Infratest. Available online: http://www.bvdw.org/presseserver/studie_faszination_mobile/BVDW_Faszination_Mobile_2014.pdf (accessed on 2 April 2015).
- Spallek, J.; Zeeb, H.; Razum, O. Prevention among immigrants: The example of Germany. BMC Public Health 2010, 10, 92. [Google Scholar] [CrossRef] [PubMed]
- Brzoska, P.; Razum, O. Versorgungsprobleme und mögliche Lösungsstrategien bei Menschen mit Migrationshintergrund. DMW-Deutsch. Med. Wochenschr. 2014, 139, 1895–1897. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.A.; Saboor, H.T.; Qayyum, Z.; Khan, I.; Habib, Z.; Waheed, H.T. Barriers to accessing the German health-care system for Pakistani immigrants in Berlin, Germany: A qualitative exploratory study. Lancet 2013. [Google Scholar] [CrossRef]
- Henderson, S.; Kendall, E. Culturally and linguistically diverse peoples' knowledge of accessibility and utilisation of health services: Exploring the need for improvement in health service delivery. Aust. J. Prim. Health 2011, 17, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Povlsen, L.; Olsen, B.; Ladelund, S. Diabetes in children and adolescents from ethnic minorities: Barriers to education, treatment and good metabolic control. J. Adv. Nurs. 2005, 50, 576–582. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Yoon, J. The Use of an Online Forum for Health Information by Married Korean Women in the United States. Available online: http://search.ebscohost.com/login.aspx?direct=true&db=lih&AN=84397187&site=ehost-live (accessed on 27 November 2015).
- Van der Veen, Y.; van Empelen, P.; Richardus, J. Development of a culturally tailored Internet intervention promoting hepatitis B screening in the Turkish community in the Netherlands. Health Promot. Int. 2011, 27, 342–355. [Google Scholar] [CrossRef] [PubMed]
- Friedman, D.B.; Kao, E.K. Peer Reviewed: A Comprehensive Assessment of the Difficulty Level and Cultural Sensitivity of Online Cancer Prevention Resources for Older Minority Men. Available online: http://www.cdc.gov/pcd/issues/2008/jan/07_0146.htm (accessed on 27 November 2015).
- Daraz, L.; MacDermid, J.C.; Wilkins, S.; Gibson, J.; Shaw, L. The quality of websites addressing fibromyalgia: An assessment of quality and readability using standardised tools. BMJ Open 2011. [Google Scholar] [CrossRef] [PubMed]
- Mayring, P. Qualitative Inhaltsanalyse: Grundlagen und Techniken; Beltz Verlag: Weinheim, Germany, 2007. [Google Scholar]
- Pandey, A.; Hasan, S.; Dubey, D.; Sarangi, S. Smartphone apps as a source of cancer information: Changing trends in health information-seeking behavior. J. Cancer Educ. 2013, 28, 138–142. [Google Scholar] [CrossRef] [PubMed]
- Rosser, B.A.; Eccleston, C. Smartphone applications for pain management. J. Telemed. Telecare 2011, 17, 308–312. [Google Scholar] [CrossRef] [PubMed]
- Ingleby, D. Good practice in health service provision for migrants. In Migration and Health in the European Union; Rechel, B., Ed.; MacGraw-Hill Education: Boston, MA, USA, 2011; pp. 227–242. [Google Scholar]
- Mladovsky, P.; Ingleby, D.; Rechel, B. Good practices in migrant health: The European experience. Clin. Med. 2012, 12, 248–252. [Google Scholar] [CrossRef] [PubMed]
- Flores, G. The impact of medical interpreter services on the quality of health care: A systematic review. Med. Care Res. Rev. 2005, 62, 255–299. [Google Scholar] [CrossRef] [PubMed]
- Razum, O.; Zeeb, H.; Meesmann, U.; Schenk, L.; Bredehorst, M.; Brzoska, P.; Dercks, T.; Glodny, S.; Menkhaus, B.; Salman, R.; Saß, A.C.; Ulrich, R. Migration und Gesundheit. Schwerpunktbericht der Gesundheitsberichterstattung des Bundes; Robert Koch Institute: Berlin, Germany, 2008; pp. 122–126. [Google Scholar]
- Khaylis, A.; Yiaslas, T.; Bergstrom, J.; Gore-Felton, C. A review of efficacious technology-based weight-loss interventions: five key components. Telemed. J. E-Health 2010, 16, 931–938. [Google Scholar] [CrossRef] [PubMed]
- Leeman-Castillo, B.; Beaty, B.; Raghunath, S.; Steiner, J.; Bull, S. Luchar: using computer technology to battle heart disease among Latinos. Am. J. Public Health 2010, 100, 272–275. [Google Scholar] [CrossRef] [PubMed]
- Padilla, R.; Bull, S.; Raghunath, S.G.; Fernald, D.; Havranek, E.P.; Steiner, J.F. Designing a cardiovascular disease prevention web site for Latinos: Qualitative community feedback. Health Promot. Pract. 2010, 11, 140–147. [Google Scholar] [CrossRef] [PubMed]
- Boulos, M.N.; Wheeler, S.; Tavares, C.; Jones, R. How smartphones are changing the face of mobile and participatory healthcare: an overview, with example from eCAALYX. Biomed. Eng. Online 2011. [Google Scholar] [CrossRef] [PubMed]
- Mosa, A.S.M.; Yoo, I.; Sheets, L. A systematic review of healthcare applications for smartphones. BMC Med. Inform. Decis. Mak. 2012. [Google Scholar] [CrossRef] [PubMed]
- Dubey, D.; Amritphale, A.; Sawhney, A.; Amritphale, N.; Dubey, P.; Pandey, A. Smart phone applications as a source of information on stroke. J. Stroke 2014, 16, 86–90. [Google Scholar] [CrossRef] [PubMed]
- Wallace, L.S.; Dhingra, L.K. A systematic review of smartphone applications for chronic pain available for download in the United States. J. Opioid Manag. 2013, 10, 63–68. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Samkange-Zeeb, F.; Ernst, S.A.; Klein-Ellinghaus, F.; Brand, T.; Reeske-Behrens, A.; Plumbaum, T.; Zeeb, H. Assessing the Acceptability and Usability of an Internet-Based Intelligent Health Assistant Developed for Use among Turkish Migrants: Results of a Study Conducted in Bremen, Germany. Int. J. Environ. Res. Public Health 2015, 12, 15339-15351. https://doi.org/10.3390/ijerph121214987
Samkange-Zeeb F, Ernst SA, Klein-Ellinghaus F, Brand T, Reeske-Behrens A, Plumbaum T, Zeeb H. Assessing the Acceptability and Usability of an Internet-Based Intelligent Health Assistant Developed for Use among Turkish Migrants: Results of a Study Conducted in Bremen, Germany. International Journal of Environmental Research and Public Health. 2015; 12(12):15339-15351. https://doi.org/10.3390/ijerph121214987
Chicago/Turabian StyleSamkange-Zeeb, Florence, Sinja Alexandra Ernst, Funda Klein-Ellinghaus, Tilman Brand, Anna Reeske-Behrens, Till Plumbaum, and Hajo Zeeb. 2015. "Assessing the Acceptability and Usability of an Internet-Based Intelligent Health Assistant Developed for Use among Turkish Migrants: Results of a Study Conducted in Bremen, Germany" International Journal of Environmental Research and Public Health 12, no. 12: 15339-15351. https://doi.org/10.3390/ijerph121214987
APA StyleSamkange-Zeeb, F., Ernst, S. A., Klein-Ellinghaus, F., Brand, T., Reeske-Behrens, A., Plumbaum, T., & Zeeb, H. (2015). Assessing the Acceptability and Usability of an Internet-Based Intelligent Health Assistant Developed for Use among Turkish Migrants: Results of a Study Conducted in Bremen, Germany. International Journal of Environmental Research and Public Health, 12(12), 15339-15351. https://doi.org/10.3390/ijerph121214987






