Social Interactions Sparked by Pictorial Warnings on Cigarette Packs
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedures

2.3. Measures
2.4. Data Analysis
3. Results
| Characteristic | Pilot Study 1 (n = 30) % | Pilot Study 2 (n = 46) % |
|---|---|---|
| Age | ||
| 18–24 years | 40 | 4 |
| 25–39 years | 33 | 37 |
| 40–54 years | 27 | 33 |
| 55+ years | 0 | 26 |
| Mean (SD) | 30 (11) | 43 (12) |
| Female | 40 | 57 |
| Gay or bisexual | 10 | 11 |
| Hispanic | 10 | 13 |
| Race | ||
| Asian | 7 | 4 |
| Black | 27 | 35 |
| White | 43 | 44 |
| Other/Multiracial | 23 | 17 |
| Education | ||
| High school degree or less | 33 | 20 |
| Some college | 50 | 50 |
| College graduate | 10 | 24 |
| Graduate or professional degree | 7 | 7 |
| Low income (≤200% of poverty level) | 69 | 59 |
| Cigarettes smoked per day, mean (SD) | 12 (9) | 11 (8) |
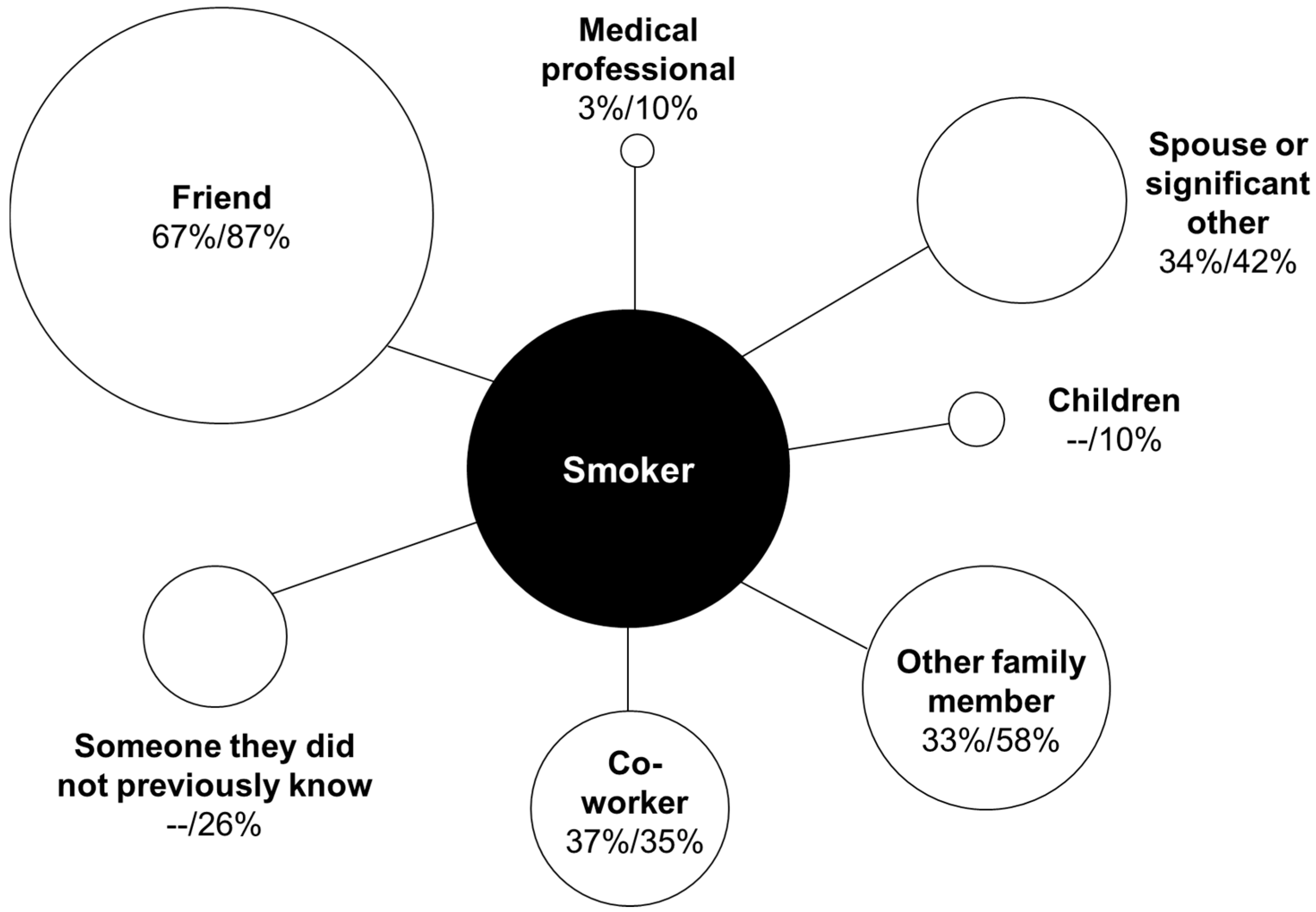
| Conversation Partners | About Warnings n (%) | About Health Effects of Smoking n (%) | About Quitting Smoking n (%) |
|---|---|---|---|
| Only smokers | 5 (17) | 3 (9) | 6 (18) |
| Mostly smokers | 10 (34) | 7 (21) | 6 (18) |
| Mix of smokers and non-smokers | 11 (38) | 17 (52) | 15 (45) |
| Mostly non-smokers | 2 (7) | 3 (9) | 1 (3) |
| Only non-smokers | 1 (3) | 3 (9) | 5 (15) |
| n | 29 | 33 | 33 |
| Content of Conversations | n (%) |
|---|---|
| Topics discussed in conversations | |
| Whether warning would encourage smokers to quit smoking | 24 (77) |
| Whether warning would make me want to quit smoking | 22 (71) |
| Discussed this research study | 22 (71) |
| Whether warning would discourage people from starting to smoke | 21 (68) |
| Whether warnings like this should be on cigarette packs | 20 (65) |
| Made fun of warning | 4 (13) |
| Descriptions of warnings in conversations | |
| Scary | 22 (71) |
| Informative, useful | 17 (55) |
| Gross | 17 (55) |
| Depressing, gloomy | 16 (52) |
| Interesting, engaging | 13 (42) |
| Stupid, pointless | 6 (19) |
| Judgmental, controlling | 3 (10) |
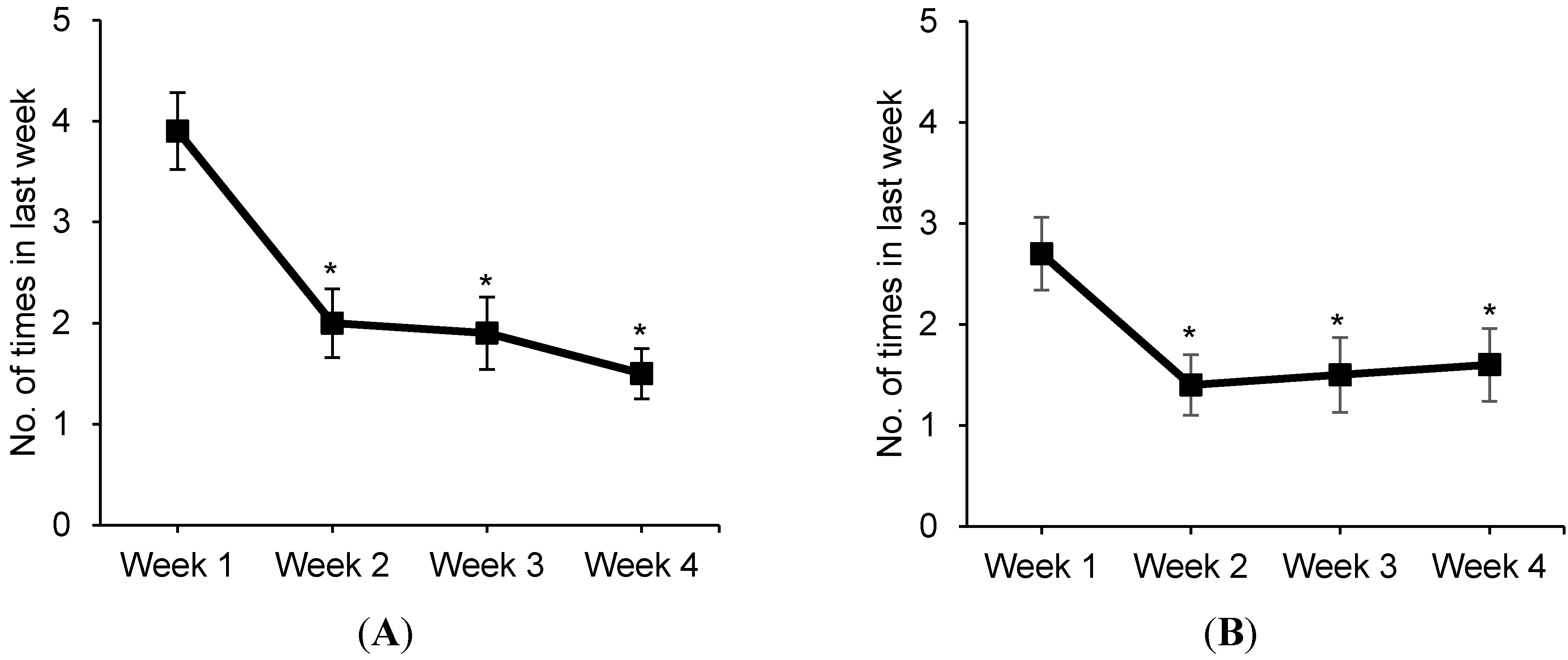
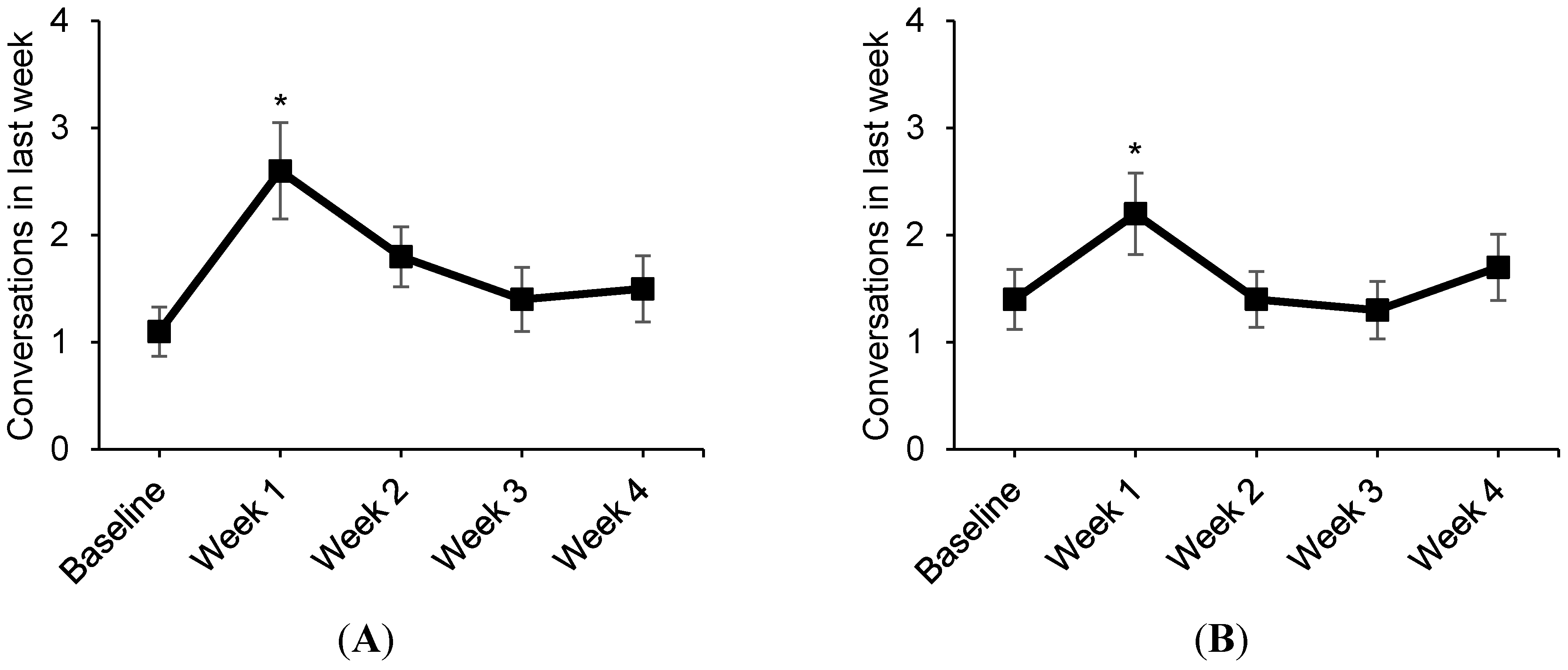
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization. Who Report on the Global Tobacco Epidemic, 2013: Enforcing Bans on Tobacco Advertising, Promotion and Sponsorship; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- Noar, S.M.; Hall, M.G.; Brewer, N.T. Pictorial cigarette pack warnings have important effects. Am. J. Public Health 2015. [CrossRef]
- Noar, S.M.; Hall, M.G.; Francis, D.; Ribisl, K.M.; Pepper, J.; Brewer, N.T. Pictorial cigarette pack warnings: A meta-analysis of experimental studies. Tob. Control 2015. [CrossRef] [PubMed]
- Hammond, D. Health warning messages on tobacco products: A review. Tob. Control 2011, 20, 327–337. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Framework Convention on Tobacco Control. Available online: http://www.who.int/fctc/en/ (accessed on 20 April 2015).
- Canadian Cancer Society. Cigarette Package Health Warnings: International Status Report; Canadian Cancer Society: Toronto, ON, Canada, 2014. [Google Scholar]
- Katz, E.; Lazarsfeld, P.F. Personal Influence, the Part Played by People in the Flow of Mass Communications; Transaction Publishers: Piscataway, NJ, USA, 1955. [Google Scholar]
- Southwell, B.G.; Yzer, M.C. The roles of interpersonal communication in mass media campaigns. Commun. Yearb. 2007, 31, 420–462. [Google Scholar]
- Southwell, B.G.; Yzer, M.C. When (and why) interpersonal talk matters for campaigns. Commun. Theory 2009, 19, 1–8. [Google Scholar] [CrossRef]
- Hornik, R.C.; Yanovitzky, I. Using theory to design evaluations of communication campaigns: The case of the national youth anti-drug media campaign. Commun. Theory 2003, 13, 204–224. [Google Scholar] [CrossRef] [PubMed]
- Noar, S.M. A 10-year retrospective of research in health mass media campaigns: Where do we go from here? J. Health Commun. 2006, 11, 21–42. [Google Scholar] [CrossRef] [PubMed]
- Thrasher, J.F.; Abad-Vivero, E.N.; Huang, L.; O’Connor, R.J.; Hammond, D.; Bansal-Travers, M.; Yong, H.H.; Borland, R.; Markovsky, B.; Hardin, J. Interpersonal communication about pictorial health warnings on cigarette packages: Policy-related influences and relationships with smoking cessation attempts. Soc. Sci. Med. 2015. [CrossRef] [PubMed]
- White, V.; Webster, B.; Wakefield, M. Do graphic health warning labels have an impact on adolescents’ smoking-related beliefs and behaviours? Addiction 2008, 103, 1562–1571. [Google Scholar] [CrossRef] [PubMed]
- Helme, D.W.; Noar, S.M.; Allard, S.; Zimmerman, R.S.; Palmgreen, P.; McClanahan, K.J. In-depth investigation of interpersonal discussions in response to a safer sex mass media campaign. Health Commun. 2011, 26, 366–378. [Google Scholar] [CrossRef] [PubMed]
- Jeong, M.; Tan, A.S.; Brennan, E.; Gibson, L.; Hornik, R.C. Talking about quitting: Interpersonal communication as a mediator of campaign effects on smokers’ quit behaviors. J. Health Commun. 2015, 20, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.H.; White, H.R.; Pandina, R.J. Predictors of smoking cessation from adolescence into young adulthood. Addict. Behav. 2001, 26, 517–529. [Google Scholar] [CrossRef]
- Powell, L.M.; Tauras, J.A.; Ross, H. The importance of peer effects, cigarette prices and tobacco control policies for youth smoking behavior. J. Health Econ. 2005, 24, 950–968. [Google Scholar] [CrossRef] [PubMed]
- Christakis, N.A.; Fowler, J.H. The collective dynamics of smoking in a large social network. N. Engl. J. Med. 2008, 358, 2249–2258. [Google Scholar] [CrossRef] [PubMed]
- Dunlop, S.; Wakefield, M.; Kashima, Y. Can you feel it? Negative emotion, risk, and narrative in health communication. Media Psychol. 2008, 11, 52–75. [Google Scholar]
- Durkin, S.; Wakefield, M. Maximizing the impact of emotive antitobacco advertising: Effects of interpersonal discussion and program placement. Soc. Mark. Q. 2006, 12, 3–14. [Google Scholar] [CrossRef]
- Hafstad, A.; Aarø, L.; Langmark, F. Evaluation of an anti-smoking mass media campaign targeting adolescents: The role of affective responses and interpersonal communication. Health Educ. Res. 1996, 11, 29–38. [Google Scholar] [CrossRef]
- Hafstad, A.; Aaro, L.E.; Engeland, A.; Andersen, A.; Langmark, F.; Stray-Pedersen, B. Provocative appeals in anti-smoking mass media campaigns targeting adolescents—The accumulated effect of multiple exposures. Health Educ. Res. 1997, 12, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Van den Putte, B.; Yzer, M.; Southwell, B.G.; de Bruijn, G.J.; Willemsen, M.C. Interpersonal communication as an indirect pathway for the effect of antismoking media content on smoking cessation. J. Health Commun. 2011, 16, 470–485. [Google Scholar] [CrossRef] [PubMed]
- Schuster, D.V.; Valente, T.W.; Skara, S.N.; Wenten, M.R.; Unger, J.B.; Cruz, T.B.; Rohrbach, L.A. Intermedia processes in the adoption of tobacco control activities among opinion leaders in california. Commun. Theory 2006, 16, 91–117. [Google Scholar] [CrossRef]
- Dunlop, S.M.; Wakefield, M.; Kashima, Y. The contribution of antismoking advertising to quitting: Intra- and interpersonal processes. J. Health Commun. 2008, 13, 250–266. [Google Scholar] [CrossRef] [PubMed]
- Kraemer, J.D.; Baig, S.A. Analysis of legal and scientific issues in court challenges to graphic tobacco warnings. Am. J. Prev. Med. 2013, 45, 334–342. [Google Scholar] [CrossRef] [PubMed]
- Brewer, N.T.; Hall, M.G.; Lee, J.G.; Peebles, K.; Noar, S.M.; Ribisl, K.M. Testing warning messages on smokers’ cigarette packages: A standardised protocol. Tob. Control 2015. [CrossRef] [PubMed]
- Willis, G.B. Cognitive Interviewing: A tool for Improving Questionnaire Design; Sage Publications Incorporated: Thousand Oaks, CA, USA, 2004. [Google Scholar]
- Strahan, E.J.; White, K.; Fong, G.T.; Fabrigar, L.R.; Zanna, M.P.; Cameron, R. Enhancing the effectiveness of tobacco package warning labels: A social psychological perspective. Tob. Control 2002, 11, 183–190. [Google Scholar] [CrossRef] [PubMed]
- McAfee, T.; Davis, K.C.; Alexander, R.L., Jr.; Pechacek, T.F.; Bunnell, R. Effect of the first federally funded us antismoking national media campaign. Lancet 2013, 382, 2003–2011. [Google Scholar] [CrossRef]
- Hammond, D.; Fong, G.T.; Borland, R.; Cummings, K.M.; McNeill, A.; Driezen, P. Text and graphic warnings on cigarette packages: Findings from the international tobacco control four country study. Am. J. Prev. Med. 2007, 32, 202–209. [Google Scholar] [CrossRef] [PubMed]
- Borland, R.; Wilson, N.; Fong, G.T.; Hammond, D.; Cummings, K.M.; Yong, H.-H.; Hosking, W.; Hastings, G.; Thrasher, J.; McNeill, A. Impact of graphic and text warnings on cigarette packs: Findings from four countries over five years. Tob. Control 2009, 18, 358–364. [Google Scholar] [CrossRef] [PubMed]
- Hitchman, S.C.; Driezen, P.; Logel, C.; Hammond, D.; Fong, G.T. Changes in effectiveness of cigarette health warnings over time in canada and the united states, 2002–2011. Nicotin Tob. Res. 2014, 16, 536–543. [Google Scholar] [CrossRef] [PubMed]
- Bell, K.; Dennis, S.; Robinson, J.; Moore, R. Does the hand that controls the cigarette packet rule the smoker? Findings from ethnographic interviews with smokers in canada, australia, the united kingdom and the USA. Soc. Sci. Med. 2015, 142, 136–144. [Google Scholar] [PubMed]
- Maynard, O.M.; Attwood, A.; O’Brien, L.; Brooks, S.; Hedge, C.; Leonards, U.; Munafo, M.R. Avoidance of cigarette pack health warnings among regular cigarette smokers. Drug Alcohol. Depend. 2014, 136, 170–174. [Google Scholar] [CrossRef] [PubMed]
- Hardcastle, S.J.; Chan, D.C.; Caudwell, K.M.; Sultan, S.; Cranwell, J.; Chatzisarantis, N.L.; Hagger, M.S. Larger and more prominent graphic health warnings on plain-packaged tobacco products and avoidant responses in current smokers: A qualitative study. Int. J. Behav. Med. 2015. [CrossRef] [PubMed]
- Hammond, D. Tobacco labelling and packaging toolkit. Available online: http://www.tobaccolabels.ca/toolkit (accessed on 10 December 2014).
- Kornfield, R.; Smith, K.C. Earned media and public engagement with cdc’s “tips from former smokers” campaign: An analysis of online news and blog coverage. J. Med. Internet Res. 2015. [CrossRef] [PubMed]
- Hammond, D.; Wakefield, M.; Durkin, S.; Brennan, E. Tobacco packaging and mass media campaigns: Research needs for articles 11 and 12 of the who framework convention on tobacco control. Nicotin Tob. Res. 2013, 15, 817–831. [Google Scholar] [CrossRef] [PubMed]
- Thrasher, J.F.; Murukutla, N.; Perez-Hernandez, R.; Alday, J.; Arillo-Santillan, E.; Cedillo, C.; Gutierrez, J.P. Linking mass media campaigns to pictorial warning labels on cigarette packages: A cross-sectional study to evaluate effects among mexican smokers. Tob. Control 2013, 22, e57–e65. [Google Scholar] [CrossRef] [PubMed]
- Brennan, E.; Durkin, S.J.; Cotter, T.; Harper, T.; Wakefield, M.A. Mass media campaigns designed to support new pictorial health warnings on cigarette packets: Evidence of a complementary relationship. Tob. Control 2011, 20, 412–418. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hall, M.G.; Peebles, K.; Bach, L.E.; Noar, S.M.; Ribisl, K.M.; Brewer, N.T. Social Interactions Sparked by Pictorial Warnings on Cigarette Packs. Int. J. Environ. Res. Public Health 2015, 12, 13195-13208. https://doi.org/10.3390/ijerph121013195
Hall MG, Peebles K, Bach LE, Noar SM, Ribisl KM, Brewer NT. Social Interactions Sparked by Pictorial Warnings on Cigarette Packs. International Journal of Environmental Research and Public Health. 2015; 12(10):13195-13208. https://doi.org/10.3390/ijerph121013195
Chicago/Turabian StyleHall, Marissa G., Kathryn Peebles, Laura E. Bach, Seth M. Noar, Kurt M. Ribisl, and Noel T. Brewer. 2015. "Social Interactions Sparked by Pictorial Warnings on Cigarette Packs" International Journal of Environmental Research and Public Health 12, no. 10: 13195-13208. https://doi.org/10.3390/ijerph121013195
APA StyleHall, M. G., Peebles, K., Bach, L. E., Noar, S. M., Ribisl, K. M., & Brewer, N. T. (2015). Social Interactions Sparked by Pictorial Warnings on Cigarette Packs. International Journal of Environmental Research and Public Health, 12(10), 13195-13208. https://doi.org/10.3390/ijerph121013195





