Research Priorities for NCD Prevention and Climate Change: An International Delphi Survey
Abstract
:1. Introduction
Objective
2. Experimental Section
2.1. Step 1: Initial Identification of Priority Research Areas
- (a)
- had the capacity to impact positively one or more negative aspects of the interface between climate change and NCDs
- (b)
- were amenable to mitigation through legal and ethical frameworks and governance systems
- (c)
- had the potential to address critical deficits in our knowledge and understanding of how to mitigate and/or manage effects of the current NCD and climate change crises.
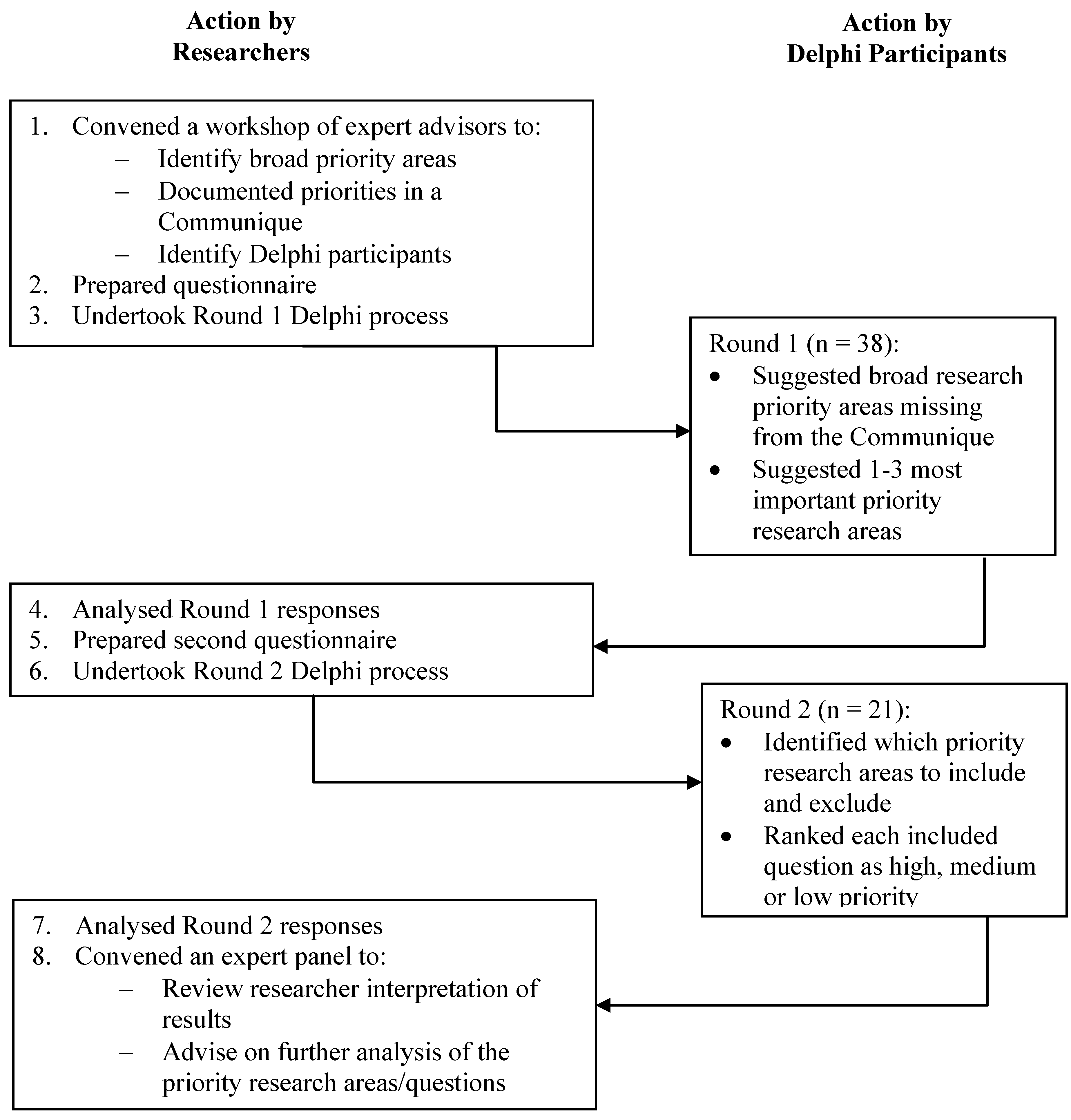
2.2. Step 2: An International Delphi Process
2.2.1. Identification of Priority Research Questions
2.2.2. Delphi Participants
2.2.3. Data Collection
- -
- were of central importance to the global response to NCD prevention and climate change;
- -
- addressed a knowledge or evidence deficit that is preventing progress in an area of high importance to the overlap between mitigating or adapting to climate change and preventing or significantly reducing the impact of NCDs and/or which focused on social and health justice issues;
- -
- addressed problems at the interface between NCDs and climate change which may be amenable to modification through legal interventions;
- -
- had a degree of urgency or immediacy.
2.2.4. Analysis
- -
- majority agreement to include as a high priority;
- -
- ranking of order of importance as a high priority;
- -
- majority agreement to identify as a low priority.
2.3. Step 3: Verification and Deconstruction of the Final Priority Questions
3. Results
3.1. Workshop Participants
3.2. Workshop Output
3.3. Delphi Process
3.4. Round 1 Results
3.5. Round 2 Results
| Characteristic | Round 1 | Round 2 |
|---|---|---|
| n-size | n-size | |
| Response rate | 46 | 22 |
| Subjects | ||
| Male / Female | 30/8 | 15/6 |
| Location | ||
| Europe | 18 | 9 |
| Oceania | 8 | 5 |
| United States | 5 | 4 |
| Caribbean | 2 | 1 |
| Canada | 1 | - |
| Africa | 1 | 1 |
| South America | 1 | 1 |
| India | 1 | - |
| South East Asia | 1 | - |
| Discipline | ||
| Public health(incl.epidemiology) | 21 | 11 |
| Law (public health/social justice) | 4 | 3 |
| Geography | 3 | 2 |
| Agriculture | 2 | 2 |
| Transport | 2 | 1 |
| Policy | 1 | 1 |
| Nutrition | 1 | 1 |
| Environmental health | 1 | - |
| Planning (urban) | 2 | - |
| Economics | 1 | - |
| Sector | ||
| Academia | 22 | 10 |
| Not-for profit organisation | 3 | 3 |
| Government | 12 | 7 |
| Industry | 1 | 1 |
| Question | Area | n | % |
|---|---|---|---|
| Access to potable water for human consumption and agriculture: what current best practices are needed to provide equitable access to water between geographic regions and usage demands? Are new best practices needed given climate change? | F | 20 | 95 |
| How do national agricultural policies affect urban food security in different regions? | F | 20 | 95 |
| What are the most effective ways to shift consumer demand from the “western” diet to a more diverse predominantly plant-based diet? | BCI | 20 | 95 |
| What are the likely environmental effects of a fat tax/healthy subsidy to encourage healthier diet? | RGP | 20 | 95 |
| What are the most appropriate policies to shift from private motorized transport to healthier and cleaner transport alternatives? | U | 19 | 90.5 |
| How can the harms that lead to NCDs be described and conceptualised in a way that more easily supports policy formation? | BCI | 19 | 90.5 |
| How can housing policies contribute to climate change adaptation and mitigation? | U | 19 | 90.5 |
| What are the methodologies to measure the impact of sustainable urban development and transport on health? | U | 19 | 90.5 |
| What are effective incentives and disincentives for healthy and unhealthy food consumption which also promote low-carbon solutions? | F | 19 | 90.5 |
| What metrics, policies and governance structures are needed to address tough trade-offs needed in shifting agricultural patterns underway, especially aimed at reducing long term demand for meat and palm and developing a more diverse diet? | F | 19 | 90.5 |
- -
- best practices for access to potable water
- -
- policies for shifting motorised transport to cleaner healthy transport
- -
- describing NCDS in a way that supports policy change
| Question | Area | n | % |
|---|---|---|---|
| How can car-dependent cities shrink their carbon footprints in a way that reduces health inequalities? | U | 12 | 75 |
| What are the cost-benefits of fiscal policies such as a fat tax/ healthy subsidies, taking into account the potential benefits or costs that they might have in terms of environmental effects? | ETB | 9 | 75 |
| Access to potable water for human consumption and agriculture: what current best practices are needed to provide equitable access to water between geographic regions and usage demands? Are new best practices needed given climate change? | F | 13 | 68 |
| Which strategies are the most appropriate to improve food security through small-scale farming and environmentally sustainable food production? | F | 11 | 65 |
| How can the health and climate change agendas be better aligned with those of urban planners and real estate developers? | U | 11 | 65 |
| What are the most appropriate policies to shift from private motorized transport to healthier and cleaner transport alternatives? | U | 11 | 65 |
| How can food needs be defined to meet optimal nutrition within an environmentally sustainable agricultural program? | F | 9 | 64 |
| How can we effectively predict crop production changes due to climate change and effects on food security (crop adaptation in regions most likely affected)? | F | 9 | 64 |
| What joint mechanisms can countries put in place to reduce the negative impacts of trade on climate change and NCDs? | ETB | 9 | 64 |
| How to change behaviour (as a collective rather than as individuals) to a highly active, low carbon transport system- (a question for primary research and for systems modelling). How to minimise rebound effects for a behaviour change? | BCI | 10 | 62.5 |
| How to develop evaluation tools for social decision making that go beyond cost benefit analysis approaches? | RGP | 10 | 62.5 |
| How can the harms that lead to NCDs be described and conceptualised in a way that more easily supports policy formation? | BCI | 11 | 61 |
4. Discussion
5. Conclusions
Supplementary Files
Supplementary File 1Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ban, K.-M. Ban Ki-Moon’s Speeches: Opening Remarks at 2014 Climate Summit. Available online: http://www.un.org/apps/news/infocus/sgspeeches/statments_full.asp?statID=2355#.VVW XllJBCuJ (accessed on 15 May 2015).
- United Nations. The Future We Want: Outcome Document Adopted at Rio+20; United Nations: New York, NY, USA, 2013. [Google Scholar]
- Intergovernmental Panel on Climate Change (IPCC). Climate Change 2007: Working Group I: The Physical Science Basis. Available online: www.ipcc.ch/publications_and_data/ar4/syr/en/mains1.html (accessed on 8 May 2015).
- World Health Organization. Preventing Chronic Diseases: A Vital Investment; WHO: Geneva, Switzerland, 2005. [Google Scholar]
- Stuckler, D.; Basu, S.; McKee, M. Drivers of inequality in millennium development goal progress: A statistical analysis. PLoS Med. 2010. [Google Scholar] [CrossRef] [PubMed]
- Horton, R. Non-communicable diseases: 2015 to 2025. Lancet 2013, 381, 509–510. [Google Scholar] [CrossRef]
- Alleyne, G.; Binagwaho, A.; Haines, A.; Jahan, S.; Nugent, R.; Rojhani, A.; Stuckler, D. Embedding non-communicable diseases in the post-2015 development agenda. Lancet 2013, 381, 566–574. [Google Scholar] [CrossRef]
- Beaglehole, R.; Horton, R. Chronic diseases: Global action must match global evidence. Lancet 2010, 376, 1619–1621. [Google Scholar] [CrossRef]
- Strong, K.; Mathers, C.; Leeder, S.; Beaglehole, R. Preventing chronic diseases: How many lives can we save? Lancet 2005, 366, 1578–1582. [Google Scholar] [CrossRef]
- Chaker, L.; Falla, A.; van der Lee, S.J.; Muka, T.; Imo, D.; Jaspers, L.; Colpani, V.; Mendis, S.; Chowdhury, R.; Bramer, W.M.; et al. The global impact of non-communicable diseases on macro-economic productivity: A systematic review. Eur. J. Epidemiol. 2015, 30, 357–395. [Google Scholar] [CrossRef] [PubMed]
- Bloom, D.E.; Cafiero, E.T.; Jané-Llopis, E.; Abrahams-Gessel, S.; Bloom, L.R.; Fathima, S.; Feigl, A.B.; Gaziano, T.; Mowafi, M.; Pandya, A.; et al. The Global Economic Burden of Non-communicable Diseases; World Economic Forum: Geneva, Switzerland, 2011. [Google Scholar]
- Patz, J.; Gibbs, H.; Foley, J.; Rogers, J.; Smith, K. Climate change and global health: Quantifying a growing ethical crisis. EcoHealth 2007, 4, 397–405. [Google Scholar] [CrossRef]
- United Nations General Assembly. Political Declaration of the High-Level Meeting of the General Assembly on the Prevention and Control of Non-Communicable Diseases; United Nations: New York, NY, USA, 2011. [Google Scholar]
- Gibbs, E.P. The evolution of one health: A decade of progress and challenges for the future. Vet. Rec. 2014, 174, 85–91. [Google Scholar] [CrossRef] [PubMed]
- Marais, B.; Crawford, J.; Iredell, J.; Ward, M.; Simpson, S.; Gilbert, L.; Griffiths, P.; Kamradt-Scott, A.; Colagiuri, R.; Jones, C.; et al. One world, one health: Beyond the Millennium Development Goals. Lancet 2012, 380, 805–806. [Google Scholar] [CrossRef]
- Haines, A.; McMichael, A.J.; Smith, K.R.; Roberts, I.; Woodcock, J.; Markandya, A.; Armstrong, B.G.; Campbell-Lendrum, D.; Dangour, A.D.; Davies, M.; et al. Public health benefits of strategies to reduce greenhouse-gas emissions: Overview and implications for policy makers. Lancet 2009, 374, 2104–2114. [Google Scholar] [CrossRef]
- Watts, N.; Adger, W.N.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and climate change: Policy responses to protect public health. Lancet 2015. [Google Scholar] [CrossRef]
- Marais, B.J.; Lonnroth, K.; Lawn, S.D.; Migliori, G.B.; Mwaba, P.; Glaziou, P.; Bates, M.; Colagiuri, R.; Zijenah, L.; Swaminathan, S.; et al. Tuberculosis comorbidity with communicable and non-communicable diseases: Integrating health services and control efforts. Lancet Infect. Dis. 2013, 13, 436–448. [Google Scholar] [CrossRef]
- World Health Organization. Quantitative Risk Assessment of the Effects of Climate Change on Selected Causes of Death, 2030s and 2050s; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- Edwards, P.; Roberts, I. Population adiposity and climate change. Int. J. Epidemiol. 2009, 38, 1137–1140. [Google Scholar] [CrossRef] [PubMed]
- Douglas, M.J.; Watkins, S.J.; Gorman, D.R.; Higgins, M. Are cars the new tobacco? J. Public Health 2011, 33, 160–169. [Google Scholar] [CrossRef] [PubMed]
- Van der Ploeg, H.P.; Chey, T.; Korda, R.J.; Banks, E.; Bauman, A. Sitting time and all-cause mortality risk in 222,497 Australian adults. Arch. Intern. Med. 2012, 172, 494–500. [Google Scholar] [CrossRef] [PubMed]
- Davis, D.R. Declining fruit and vegetable nutrient composition: What is the evidence? HortScience 2009, 44, 15–19. [Google Scholar]
- Fan, M.S.; Zhao, F.J.; Fairweather-Tait, S.J.; Poulton, P.R.; Dunham, S.J.; McGrath, S.P. Evidence of decreasing mineral density in wheat grain over the last 160 years. J. Trace Elem. Med. Biol. 2008, 22, 315–324. [Google Scholar] [CrossRef] [PubMed]
- Welch, R.M.; Graham, R.D. Agriculture: The real nexus for enhancing bioavailable micronutrients in food crops. J. Trace Elem. Med. Biol. 2005, 18, 299–307. [Google Scholar] [CrossRef] [PubMed]
- Kjellstrom, T.; Butler, A.J.; Lucas, R.M.; Bonita, R. Public health impact of global heating due to climate change: Potential effects on chronic non-communicable diseases. Int. J. Public Health 2010, 55, 97–103. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Protecting Health from Climate Change: Global Research Priorities; WHO: Geneva, Switzerland, 2009. [Google Scholar]
- Hales, S.; Woodward, A.; Guest, C. Climate change in the south pacific region: Priorities for public health research. Aust. J. Public Health 1995, 19, 543–545. [Google Scholar] [CrossRef] [PubMed]
- Glass, R.; Rosenthal, J.; Jessup, C.M.; Birnbaum, L.; Portier, C. Tackling the research challenges of health and climate change. Environ. Health Perspect. 2009. [Google Scholar] [CrossRef] [PubMed]
- Friel, S.; Hancock, T.; Kjellstrom, T.; McGranahan, G.; Monge, P.; Roy, J. Urban health inequities and the added pressure of climate change: An action-oriented research agenda. J. Urban Health 2011, 88, 886–895. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J. Impediments to comprehensive research on climate change and health. Int. J. Environ. Res. Public Health 2013, 10, 6096–6105. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; Sheffield, P.E.; Hu, W.; Su, H.; Yu, W.; Qi, X.; Tong, S. Climate change and children’s health—A call for research on what works to protect children. Int. J. Environ. Res. Public Health 2012, 9, 3298–3316. [Google Scholar] [CrossRef] [PubMed]
- Frumkin, H.; George, L. Climate change: A public health framework. Northwest Public Health 2008, 25, 6–7. [Google Scholar]
- Marinucci, G.D.; Luber, G.; Uejio, C.K.; Saha, S.; Hess, J.J. Building resilience against climate effects—A novel framework to facilitate climate readiness in public health agencies. Int. J. Environ. Res. Public Health 2014, 11, 6433–6458. [Google Scholar] [CrossRef] [PubMed]
- Daar, A.S.; Singer, P.A.; Persad, D.L.; Pramming, S.K.; Matthews, D.R.; Beaglehole, R.; Bernstein, A.; Borysiewicz, L.K.; Colagiuri, S.; Ganguly, N.; et al. Grand challenges in chronic non-communicable diseases. Nature 2007, 450, 494–496. [Google Scholar] [CrossRef] [PubMed]
- Beaglehole, R.; Bonita, R.; Horton, R.; Adams, C.; Alleyne, G.; Asaria, P.; Baugh, V.; Bekedam, H.; Billo, N.; Casswell, S.; et al. Priority actions for the non-communicable disease crisis. Lancet 2011, 377, 1438–1447. [Google Scholar] [CrossRef]
- Boylan, S.; Syrett, K.; Colagiuri, R. Role of law at the non-communicable diseases-climate change interface: Considerations for planetary and population health policy. Public Health 2013, 127, 579–581. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Health in all Policies: Helskini Statement, Framework for Country Action; WHO: Geneva, Switzerland, 2013. [Google Scholar]
- World Health Organization (WHO). Health Impact Assessment. Available online: http://www.who.int/hia/en/ (accessed on 15 May 2015).
- Winkler, M.S.; Krieger, G.R.; Divall, M.J.; Cisse, G.; Wielga, M.; Singer, B.H.; Tanner, M.; Utzinger, J. Untapped potential of health impact assessment. Bull. World Health Organ. 2013, 91, 298–305. [Google Scholar] [CrossRef] [PubMed]
- Haines, A.; McMichael, A.J. Climate change and health: Implications for research, monitoring, and policy. BMJ 1997, 315, 870–874. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J. Environmental change, climate and population health: A challenge for inter-disciplinary research. Environ. Health Prev. Med. 2008, 13, 183–186. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Finegood, D.T.; Karanfil, O.; Matteson, C.L. Getting from analysis to action: Framing obesity research, policy and practice with a solution-oriented complex systems lens. Healthc. Pap. 2008, 9, 36–41. [Google Scholar] [CrossRef] [PubMed]
- OxHA. The Sydney Resolution; Oxford Health Alliance: London, UK, 2008; Available online: http://archive.oxha.org/meetings/08-summit/sydney-resolution (accessed on 29 July 2015).
- Okoli, C.; Pawlowski, S.D. The delphi method as a research tool: An example, design considerations and applications. Inf. Manag. 2004, 42, 15–29. [Google Scholar] [CrossRef]
- De Meyrick, J. The delphi method and health research. Health Educ. 2003, 103, 7–16. [Google Scholar] [CrossRef]
- James, D.; Warren-Forward, H. Research methods for formal consensus development. Nurse Res. 2015, 22, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Fink, A.; Kosecoff, J.; Chassin, M.; Brook, R.H. Consensus methods: Characteristics and guidelines for use. Am. J. Public Health 1984, 74, 979–983. [Google Scholar] [CrossRef] [PubMed]
- Hasson, F.; Keeney, S.; McKenna, H. Research guidelines for the delphi survey technique. J. Adv. Nurs. 2000, 32, 1008–1015. [Google Scholar] [PubMed]
- Cooke, R.M.; Wittmann, M.E.; Lodge, D.M.; Rothlisberger, J.D.; Rutherford, E.S.; Zhang, H.; Mason, D.M. Out-of-sample validation for structured expert judgment of asian carp establishment in lake erie. Integr. Environ. Assess. Manag. 2014, 10, 522–528. [Google Scholar] [CrossRef] [PubMed]
- Akins, R.B.; Tolson, H.; Cole, B.R. Stability of response characteristics of a delphi panel: Application of bootstrap data expansion. BMC Med. Res. Methodol. 2005. [Google Scholar] [CrossRef] [PubMed]
- Ford, J.D.; Smith, T.R.; Berrang-Ford, L. Canadian federal support for climate change and health research compared with the risks posed. Am. J. Public Health 2011, 101, 814–821. [Google Scholar] [CrossRef] [PubMed]
- Friel, S.; Bowen, K.; Campbell-Lendrum, D.; Frumkin, H.; McMichael, A.J.; Rasanathan, K. Climate change, noncommunicable diseases, and development: The relationships and common policy opportunities. Ann. Rev. Public Health 2011, 32, 133–147. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization Framework Convention on Tobacco Control (WHO FCTC). Who Framework Convention on Tobacco Control; WHO: Geneva, Switzerland, 2003. [Google Scholar]
- Campbell-Lendrum, D.; Bertollini, R.; Neira, M.; Ebi, K.; McMichael, A. Health and climate change: A roadmap for applied research. Lancet 2009, 373, 1663–1665. [Google Scholar] [CrossRef]
- Tong, S.; Mackenzie, J.; Pitman, A.J.; FitzGerald, G.; Nicholls, N.; Selvey, L. Global climate change: Time to mainstream health risks and their prevention on the medical research and policy agenda. Intern. Med. J. 2008, 38, 445–447. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J.; Wilcox, B.A. Climate change, human health, and integrative research: A transformative imperative. EcoHealth 2009, 6, 163–164. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Colagiuri, R.; Boylan, S.; Morrice, E. Research Priorities for NCD Prevention and Climate Change: An International Delphi Survey. Int. J. Environ. Res. Public Health 2015, 12, 12941-12957. https://doi.org/10.3390/ijerph121012941
Colagiuri R, Boylan S, Morrice E. Research Priorities for NCD Prevention and Climate Change: An International Delphi Survey. International Journal of Environmental Research and Public Health. 2015; 12(10):12941-12957. https://doi.org/10.3390/ijerph121012941
Chicago/Turabian StyleColagiuri, Ruth, Sinead Boylan, and Emily Morrice. 2015. "Research Priorities for NCD Prevention and Climate Change: An International Delphi Survey" International Journal of Environmental Research and Public Health 12, no. 10: 12941-12957. https://doi.org/10.3390/ijerph121012941
APA StyleColagiuri, R., Boylan, S., & Morrice, E. (2015). Research Priorities for NCD Prevention and Climate Change: An International Delphi Survey. International Journal of Environmental Research and Public Health, 12(10), 12941-12957. https://doi.org/10.3390/ijerph121012941





