Importance of All Movement Behaviors in a 24 Hour Period for Overall Health
Abstract
:1. Introduction
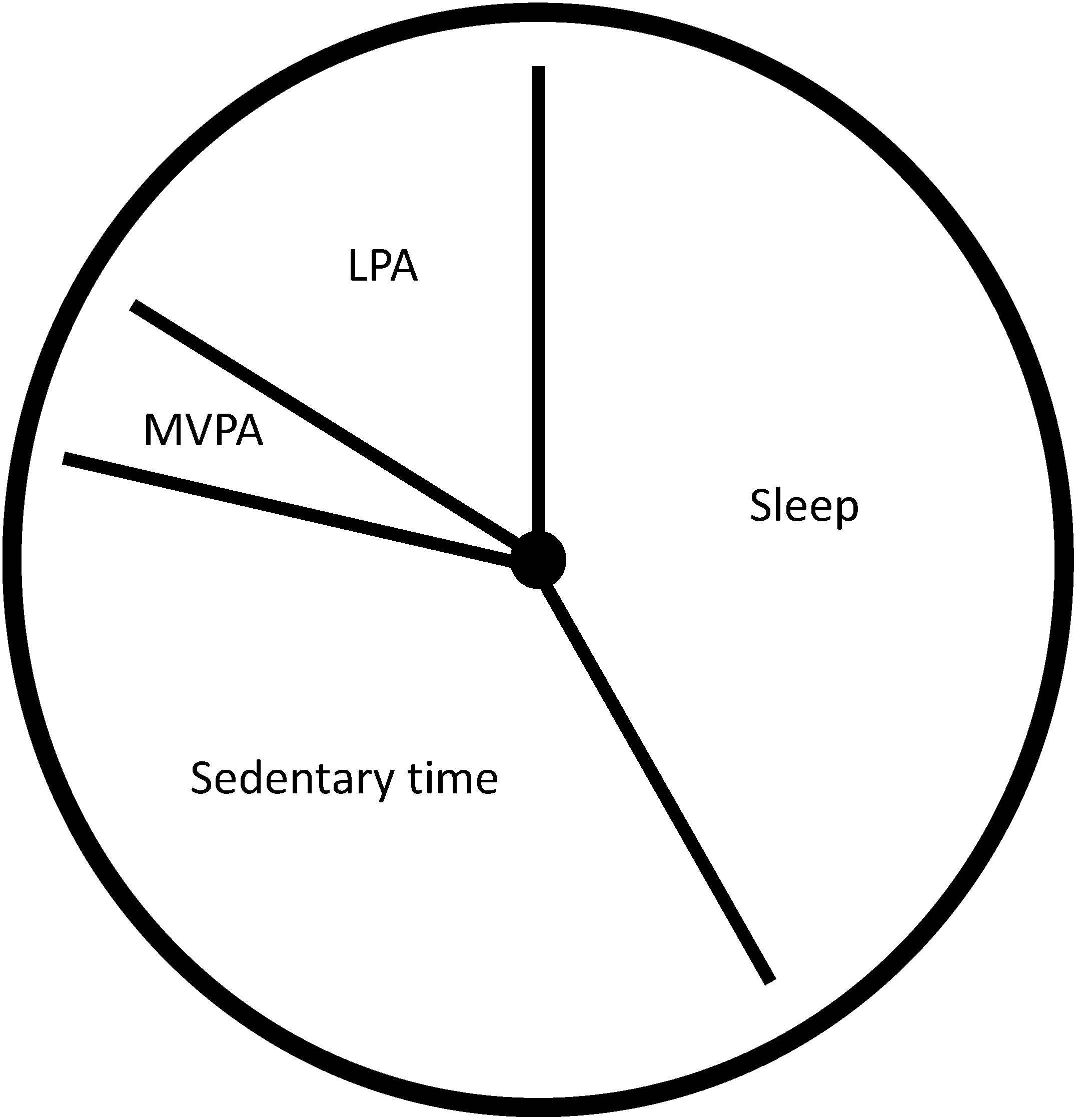
2. Is There a Need for 24 Hour Movement Behavior Guidelines?
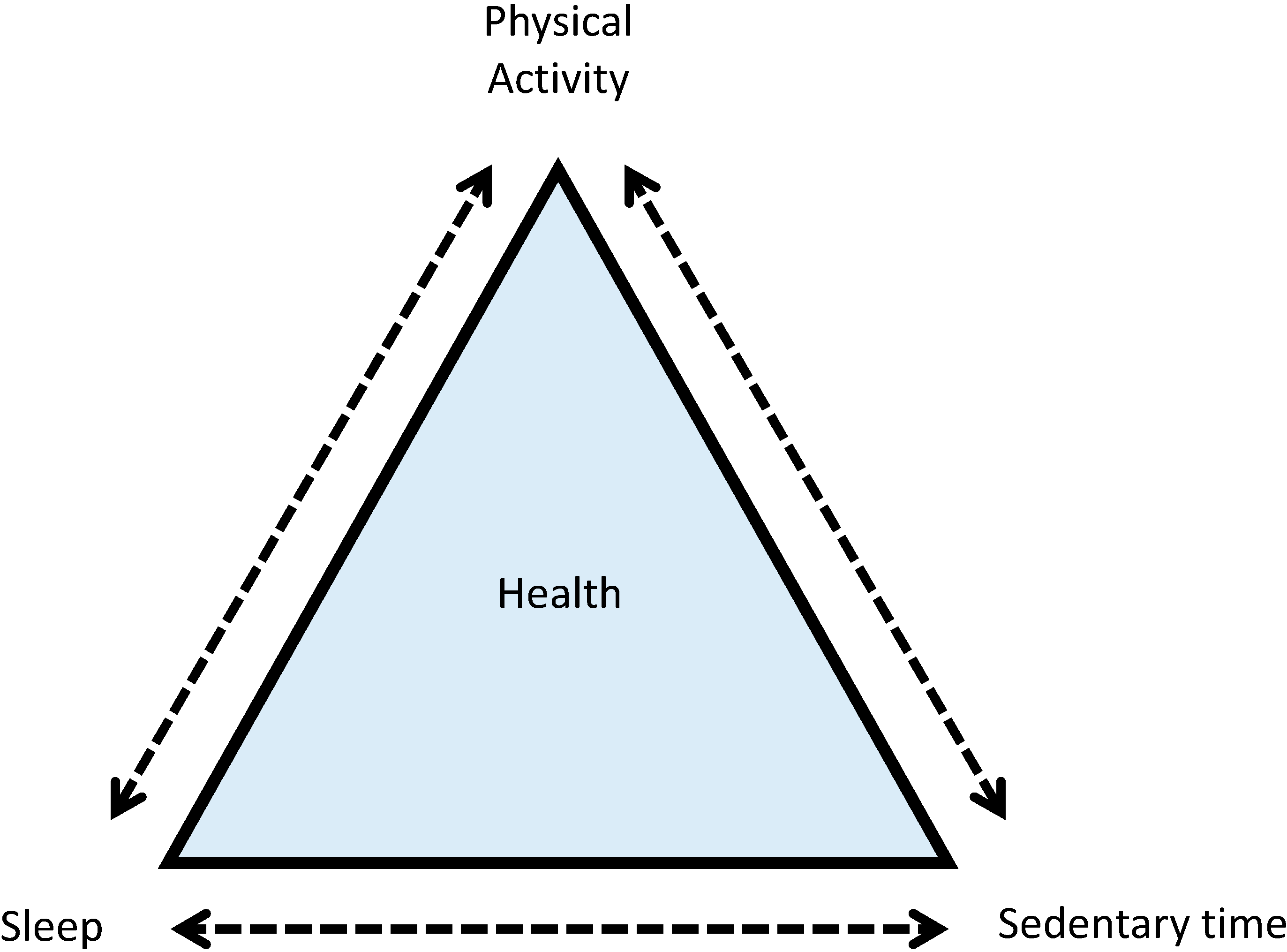
3. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Dunstan, D.W.; Howard, B.; Healy, G.N.; Owen, N. Too much sitting—A health hazard. Diabetes Res. Clin. Pract. 2012, 97, 368–376. [Google Scholar] [CrossRef]
- Hawley, J.A.; Holloszy, J.O. Exercise: It’s the real thing! Nut. Rev. 2009, 67, 172–178. [Google Scholar] [CrossRef]
- Booth, F.W.; Lees, S.J. Physically active subjects should be the control group. Med. Sci. Sport. Exercise 2006, 38, 405–406. [Google Scholar] [CrossRef]
- Chaput, J.P.; Klingenberg, L.; Rosenkilde, M.; Gilbert, J.A.; Tremblay, A.; Sjödin, A. Physical activity plays an important role in body weight regulation. J. Obes. 2011, 2011, 1–11. [Google Scholar]
- Tremblay, A.; Therrien, F. Physical activity and body functionality: Implications for obesity prevention and treatment. Can. J. Physiol. Pharmacol. 2006, 84, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Hallal, P.C.; Anderssen, L.B.; Bull, F.C.; Guthold, R.; Haskell, W.; Ekelund, U.; Lancet Physical Activity Series Working Group. Global physical activity levels: Surveillance progress, pitfalls, and prospects. Lancet 2012, 380, 247–257. [Google Scholar] [CrossRef]
- Swinburn, B.A.; Sacks, G.; Hall, K.D.; McPherson, K.; Finegood, D.T.; Moodie, M.L.; Gortmaker, S.L. The global obesity pandemic: Shaped by global drivers and local environments. Lancet 2011, 378, 804–814. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.S.; Colley, R.C.; Saunders, T.J.; Healy, G.N.; Owen, N. Physiological and health implications of a sedentary lifestyle. Appl. Physiol. Nutr. Metab. 2010, 35, 725–740. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.S.; LeBlanc, A.G.; Kho, M.E.; Saunders, T.J.; Larouche, R.; Colley, R.C.; Goldfield, G.; Gorber, S.C. Systematic review of sedentary behaviour and health indicators in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2011, 8. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.S.; LeBlanc, A.G.; Janssen, I.; Kho, M.E.; Hicks, A.; Murumets, K.; Colley, R.C.; Duggan, M. Canadian sedentary behaviour guidelines for children and youth. Appl. Physiol. Nutr. Metab. 2011, 36, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Owens, J.; Adolescent Sleep Working Group and Committee on Adolescence. Insufficient sleep in adolescents and young adults: An update on causes and consequences. Pediatrics 2014, 134, 921–932. [Google Scholar] [CrossRef]
- Schmid, S.M.; Hallschmid, M.; Schultes, B. The metabolic burden of sleep loss. Lancet Diabetes Endocrinol. 2014, in press. [Google Scholar]
- Chaput, J.P.; Tremblay, A. Insufficient sleep as a contributor to weight gain: An update. Curr. Obes. Rep. 2012, 1, 245–256. [Google Scholar] [CrossRef]
- Gruber, R.; Wiebe, S.T.; Wells, S.A.; Cassoff, J.; Monson, E. Sleep and academic success: Mechanisms, empirical evidence, and interventional strategies. Adolesc. Med. State Art Rev. 2010, 21, 522–541. [Google Scholar] [PubMed]
- Matricciani, L.; Olds, T.; Petkov, J. In search of lost sleep: Secular trends in the sleep time of school-aged children and adolescents. Sleep Med. Rev. 2012, 16, 203–211. [Google Scholar] [CrossRef] [PubMed]
- Leger, D.; Beck, F.; Richard, J.B.; Godeau, E. Total sleep time severely drops during adolescence. PLoS One 2012, 7. [Google Scholar] [CrossRef]
- Buman, M.P.; Winkler, E.A.; Kurka, J.M.; Hekler, E.B.; Baldwin, C.M.; Owen, N.; Ainsworth, B.E.; Healy, G.N.; Gardiner, P.A. Reallocating time to sleep, sedentary behaviors, or active behaviors: Associations with cardiovascular disease risk biomarkers, NHANES 2005–2006. Amer. J. Epidemiol. 2014, 179, 323–334. [Google Scholar] [CrossRef]
- Stone, M.R.; Faulkner, G.E. Outdoor play in children: Associations with objectively-measured physical activity, sedentary behavior and weight status. Prev. Med. 2014, 65, 122–127. [Google Scholar] [CrossRef] [PubMed]
- Carson, V.; Ridgers, N.D.; Howard, B.J.; Winkler, E.A.; Healy, G.N.; Owen, N.; Dunstan, D.W.; Salmon, J. Light-intensity physical activity and cardiometabolic biomarkers in U.S. adolescents. PLoS One 2013, 8. [Google Scholar] [CrossRef]
- Chaput, J.P.; Leduc, G.; Boyer, C.; Bélanger, P.; LeBlanc, A.G.; Borghese, M.M.; Tremblay, M.S. Objectively measured physical activity, sedentary time and sleep duration: independent and combined associations with adiposity in Canadian children. Nutr. Diabetes 2014, 4. [Google Scholar] [CrossRef]
- Zagaar, M.; Dao, A.; Alhaider, I.; Alkadhi, K. Regular treadmill exercise prevents sleep deprivation-induced disruption of synaptic plasticity and associated signaling cascade in the dentate gyrus. Mol. Cell. Neurosci. 2013, 56, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Mônico-Neto, M.; Antunes, H.K.; Dattilo, M.; Medeiros, A.; Souza, H.S.; Lee, K.S.; de Melo, C.M.; Tufik, S.; de Mello, M.T. Resistance exercise: A non-pharmacological strategy to minimize or reverse sleep deprivation-induced muscle atrophy. Med. Hypotheses 2013, 80, 701–705. [Google Scholar] [CrossRef] [PubMed]
- Ferrar, K.; Chang, C.; Li, M.; Olds, T.S. Adolescent time use clusters: A systematic review. J. Adolesc. Health 2013, 52, 259–270. [Google Scholar] [CrossRef]
- Schuit, A.J.; van Loon, A.J.; Tijhuis, M.; Ocke, M. Clustering of lifestyle risk factors in a general adult population. Prev. Med. 2002, 35, 219–224. [Google Scholar] [CrossRef] [PubMed]
- Prochaska, J.O. Multiple health behavior research represents the future of preventive medicine. Prev. Med. 2008, 46, 281–285. [Google Scholar] [CrossRef] [PubMed]
- Rogers, E.M. Diffusion of Innovations, 5th ed.; Free Press: New York, NY, USA, 2003. [Google Scholar]
- Carson, V.; Leblanc, C.M.; Moreau, E.; Tremblay, M.S. Paediatricians’ awareness of, agreement with and use of the new Canadian Physical Activity and Sedentary Behaviour Guidelines for children and youth zero to 17 years of age. Paediatr. Child. Health 2013, 18, 538–542. [Google Scholar] [PubMed]
- Tremblay, M.S.; Haskell, W.L. From science to physical activity guidelines. In Physical Activity and Health, 2nd ed.; Bouchard, C., Blair, S.N., Haskell, W.L., Eds.; Human Kinetics: Champaign, IL, USA, 2012; pp. 359–378. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chaput, J.-P.; Carson, V.; Gray, C.E.; Tremblay, M.S. Importance of All Movement Behaviors in a 24 Hour Period for Overall Health. Int. J. Environ. Res. Public Health 2014, 11, 12575-12581. https://doi.org/10.3390/ijerph111212575
Chaput J-P, Carson V, Gray CE, Tremblay MS. Importance of All Movement Behaviors in a 24 Hour Period for Overall Health. International Journal of Environmental Research and Public Health. 2014; 11(12):12575-12581. https://doi.org/10.3390/ijerph111212575
Chicago/Turabian StyleChaput, Jean-Philippe, Valerie Carson, Casey E. Gray, and Mark S. Tremblay. 2014. "Importance of All Movement Behaviors in a 24 Hour Period for Overall Health" International Journal of Environmental Research and Public Health 11, no. 12: 12575-12581. https://doi.org/10.3390/ijerph111212575
APA StyleChaput, J.-P., Carson, V., Gray, C. E., & Tremblay, M. S. (2014). Importance of All Movement Behaviors in a 24 Hour Period for Overall Health. International Journal of Environmental Research and Public Health, 11(12), 12575-12581. https://doi.org/10.3390/ijerph111212575




