Chitosan: An Update on Potential Biomedical and Pharmaceutical Applications
Abstract
:1. Introduction
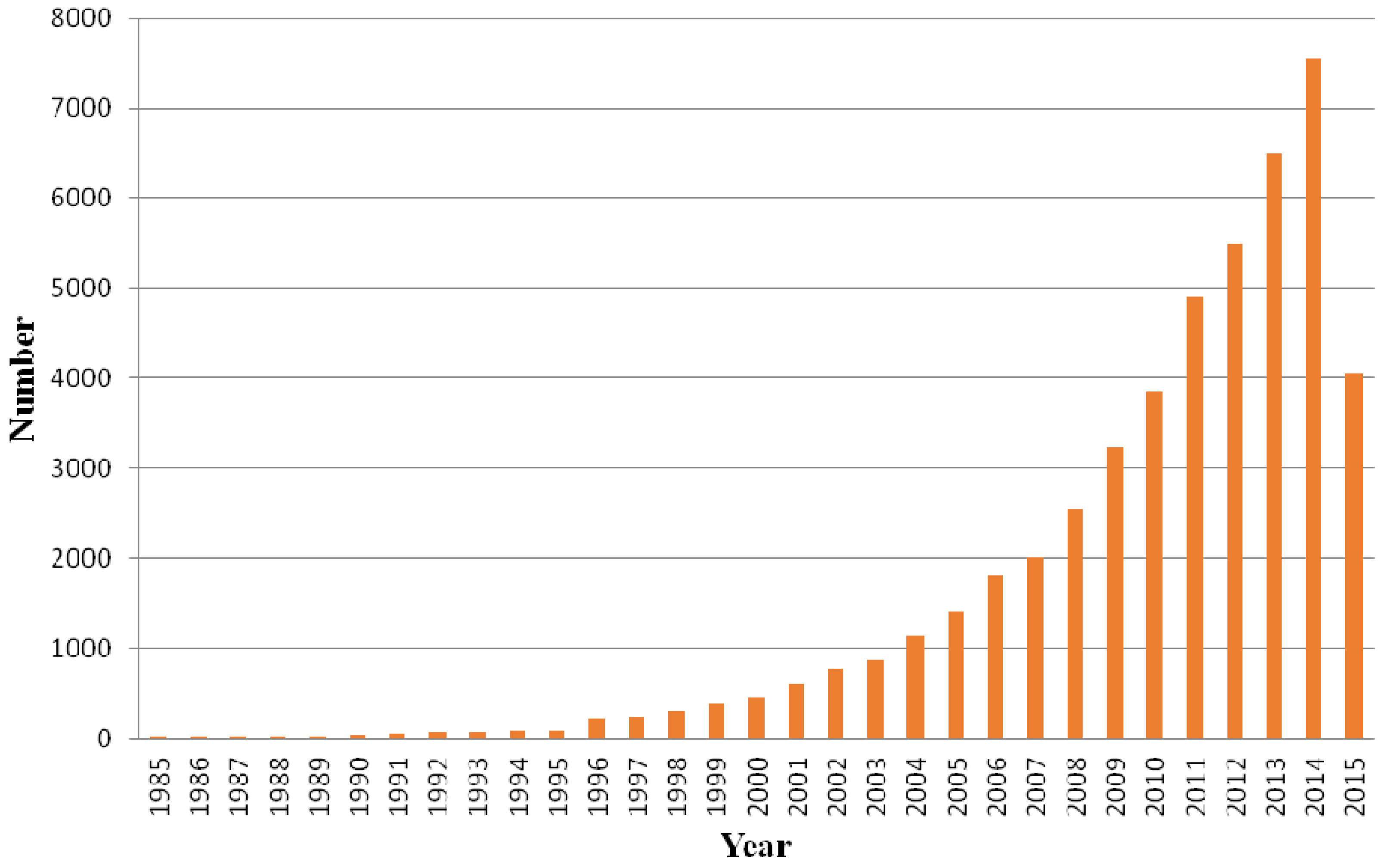
2. Production and Characterization of Chitosan
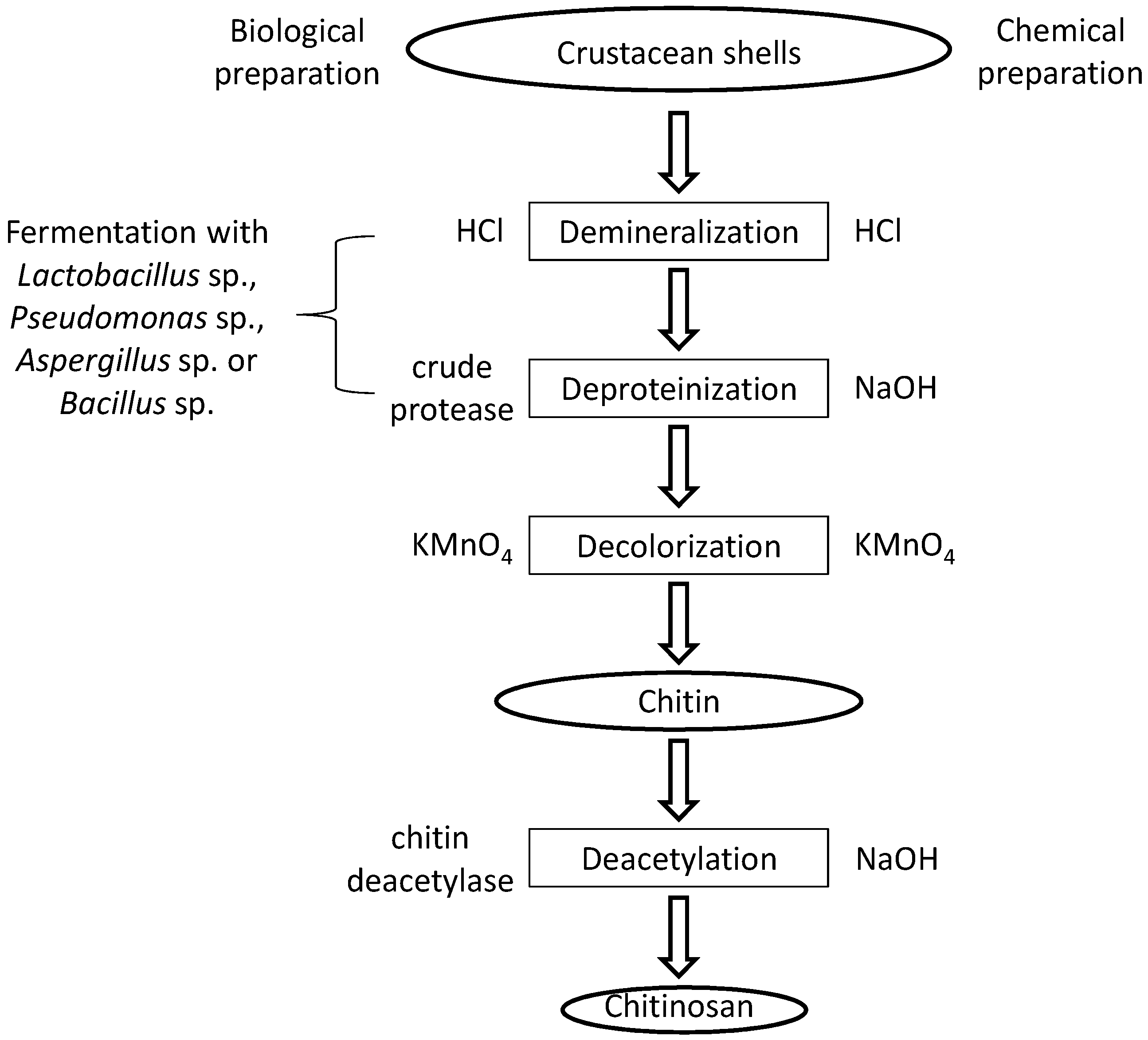
| Physiochemical Characteristics | Method of Determination |
|---|---|
| molecular weight | viscometry; gel permeation chromatography; light scattering; high performance liquid chromatography; matrix-assisted laser desorption/ionization-mass spectrometer |
| degree of deacetylation | infrared spectroscopy; ultra violet spectrophotometry; nuclear magnetic resonance spectroscopy (1H-NMR and 13C-NMR); conductometric titration; potentiometric tiltration; differential scanning calorimetry |
| crystallinity | X-ray diffraction |
3. Bioactivities of Chitosan
3.1. Antibacterial Activity
3.2. Antifungal Activity
3.3. Anti-HIV-1 Activity and for Construction of Nanoparticles Loaded with Anti-HIV Drugs
| Targets | Chitosan or Its Derivatives/MIC in μg/mL Reference | |
|---|---|---|
| Gram-negative bacteria | Escherichia coli | chitosan 0.025% [38]; chitosan-Zn complex 0.00313% [38]; á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41]; N,N-diethyl-N-methylchitosan 16 μg/mL [44]; N,N-dihexyl-N-methylchitosan 16 μg/mL [44] |
| E. coli K88 | chitosan 8 μg/mL [38]; chitosan nanoparticles 0.0625 μg/mL [38]; Cu loaded chitosan nanoparticles 0.0313 μg/mL [38] | |
| E. coli ATCC 25922 | chitosan 8 μg/mL [38]; chitosan nanoparticles 0.0313 μg/mL [38]; Cu loaded chitosan nanoparticles 0.0313 μg/mL [38] | |
| E. coli O157 | á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41] | |
| Pseudomonas aeruginosa | chitosan 0.0125% [38]; chitosan-Zn complex 0.00625% [38]; á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41]; N,N-diethyl-N-methylchitosan 32 μg/mL [44] | |
| Proteus mirabilis | chitosan 0.025% [38]; chitosan-Zn complex 0.00625% [38] | |
| Salmonella enteritidis | chitosan 0.05% [38]; chitosan-Zn complex 0.00625% [38] | |
| S. choleraesuis ATCC 50020 | chitosan 16 μg/mL [38]; chitosan nanoparticles 0.0625 μg/mL [38]; Cu loaded chitosan nanoparticles 0.0313 μg/mL [38] | |
| S. typhimurium | á-chitosan 5 μg/mL [41]; â-chitosan 9 μg/mL [41] | |
| S. typhimurium ATCC 50013 | chitosan 16 μg/mL [38]; chitosan nanoparticles 0.125 μg/mL [38]; Cu loaded chitosan nanoparticles 0.0625 μg/mL [38] | |
| Gram-negative bacteria | Enterobacter aerogenes | chitosan 0.05% [38]; chitosan-Zn complex 0.00625% [38] |
| Listeria monocytogenes | á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41] | |
| Gram-positive bacteria | Staphylococcus aureus | chitosan 0.05% [38]; chitosan-Zn complex 0.00625% [38]; á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41]; N-ethyl-N,N-dimethylchitosan 4 μg/mL [44] |
| S. aureus ATCC 25923 | chitosan 8 μg/mL [38]; chitosan nanoparticles 0.125 μg/mL [38]; Cu loaded chitosan nanoparticles 0.0625 μg/mL [38] | |
| Corynebacterium | chitosan 0.025% [38]; chitosan-Zn complex 0.0313% [38] | |
| Staphylococcus epidermidis | chitosan 0.025% [38]; chitosan-Zn complex 0.0125% [38]; á-chitosan 5 μg/mL [41]; â-chitosan 5 μg/mL [41] | |
| Enterococcus faecalis | chitosan 0.05% [38]; chitosan-Zn complex 0.0125% [38]; N,N-diethyl-N-methylchitosan 16 μg/mL [44] | |
| Bacillus cereus | á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41] | |
| Bacillus megaterium | á-chitosan 9 μg/mL [41]; â-chitosan 9 μg/mL [41] | |
| Fungi | Candida albicans | chitosan 0.1% [38]; chitosan-Zn complex 0.1% [38]; chitosan 5 μg/mL [52] |
| Candida parapsilosis | chitosan 0.1% [38]; chitosan-Zn complex 0.05% [38]; chitosan 40 μg/mL [52] | |
| Candida krusei | chitosan 5 μg/mL [52] | |
| Candida glabrata | chitosan 20 μg/mL [52] | |
| Penicillium digitatum | chitosan 65 μg/mL [46] | |
| Penicillium italicum | chitosan 57.5 μg/mL [46] | |
| Fusarium proliferatum | chitosan 2.5 μg/mL [52] | |
| Hamigera avellanea | chitosan 2.5 μg/mL [52] | |
| Aspergillus fumigatus | chitosan 1 μg/mL [52] | |
| Rhizopus stolonifer | chitosan 100 μg/mL [52] | |
| Cryptococcus neoformans | chitosan 5 μg/mL [52] | |
| Cryptococcus gatti | chitosan 2.5 μg/mL [52] | |
| Macrophomina phaseolina | chitosan 12.5 mg/mL [53] | |
| Virus | IC50 of cytopathic effect by HIV-1RF | QMW-chitosan oligomers 48.14 μg/mL [56] |
| IC50 of cytopathic effect by HIV-1IIIB | WMQ-chitosan oligomers 48.01 μg/mL [56] | |
| IC50 of p24 production by HIV-1IIIB | QMW-chitosan oligomers 67.35 μg/mL [56] | |
| IC50 of p24 production by HIV-1Ba-L | WMQ-chitosan oligomers 98.73 μg/mL [56] | |
| IC50 of p24 production by HIV-1RTMDR1 | QMW-chitosan oligomers 81.03 μg/mL [56]; WMQ-chitosan oligomers 144.02 μg/mL [56] | |
| IC50 of luciferase expression by HIV-1RF | QMW-chitosan oligomers 68.13 μg/mL [56]; WMQ-chitosan oligomers 163.94 μg/mL [56] | |
| IC50 of interaction between gp41 and CD4 by HIV-1 | QMW-chitosan oligomers 39.13 μg/mL [56]; WMQ-chitosan oligomers 51.48 μg/mL [56] | |
| IC50 of syncytia formation by HIV-1RF | sulfated chitooligosaccharides 2.19 μg/mL [57] | |
| EC50 of protection of lytic effect by HIV-1 | sulfated chitooligosaccharides 1.43 μg/mL [57] | |
| IC50 of p24 production by HIV-1RF | sulfated chitooligosaccharides 4.33 μg/mL [57] | |
| IC50 of p24 production by HIV-1Ba-L | sulfated chitooligosaccharides 7.76 μg/mL [57] | |
3.4. Antitumor Activity
| Compound | Target Cell Lines or in vivo Model | Results | Ref. |
|---|---|---|---|
| chitosan | meth-A solid tumor transplanted into BALB/c mice | increased production of interleukins 1 and 2, sequentially, leading to the manifestation of antitumor effect through proliferation of cytolytic T-lymphocytes with the optimum inhibition ratio at the dose of 10 mg/kg | [66] |
| chitosan | aberrant crypt tumor lesions in the colon of mice | elevated lymphokine production and proliferation of cytolytic T-lymphocytes at the dose of 5 mg/kg | [67] |
| chitosan | A375, SKMEL28, and RPMI7951 cell lines | chitosan was coated in culture wells in which cultures with A375, SKMEL28, and RPMI7951 cells were carried out. | [68] |
| decreased adhesion of A375 cells | |||
| decreased proliferation of SKMEL28 cells | |||
| inhibited specific caspases, upregulated Bax and downregulated Bcl-2 and Bcl-XL in RPMI7951 cells | |||
| induced CD95 receptor expression in RPMI7951 cell surface which renders them more susceptible to FasL-induced apoptosis | |||
| carboxymethyl chitosan | hydrogen peroxide induced apoptosis models of Schwann cells | The cell viability was improved in a dose-dependent manner with maximum effect of 2.02 ± 0.16 fold at the dose of 200 μg/mL carboxymethyl chitosan | [69] |
| decreased caspase-3, -9 and Bax activities and increased Bcl-2 activity | |||
| carboxymethyl chitosan | BEL-7402 cell line | reduced the expression of MMP-9 in a dose-dependent manner | [70] |
| hepatoma-22 cells in Kunming mice | inhibited the lung metastasis mouse model with the highest inhibition of 66.56% at the dose of 300 mg/kg | ||
| chitosan | PC3 A549 and HepG2 cell line | suppressed cancer cell growth of PC3 A549 and HepG2 cells for 50% cell death at 25 μg/mL, 25 μg/mL and 50 μg/mL, respectively | [71] |
| chitosan | HepG2 and LCC cell line | inhibited MMP-9 expression, reduced cells in S-phase and decreased the rate of DNA synthesis, upregulated p21 and downregulated PCNA, cyclin A and CDK-2 with the highest inhibition at the dose of 1 mg/kg | [72] |
| HepG2 and LCC xenografts in mouse model | inhibited tumor growth and decreased the number of metastatic colonies at the dose of 500 mg/kg |
3.5. Antioxidant Activity
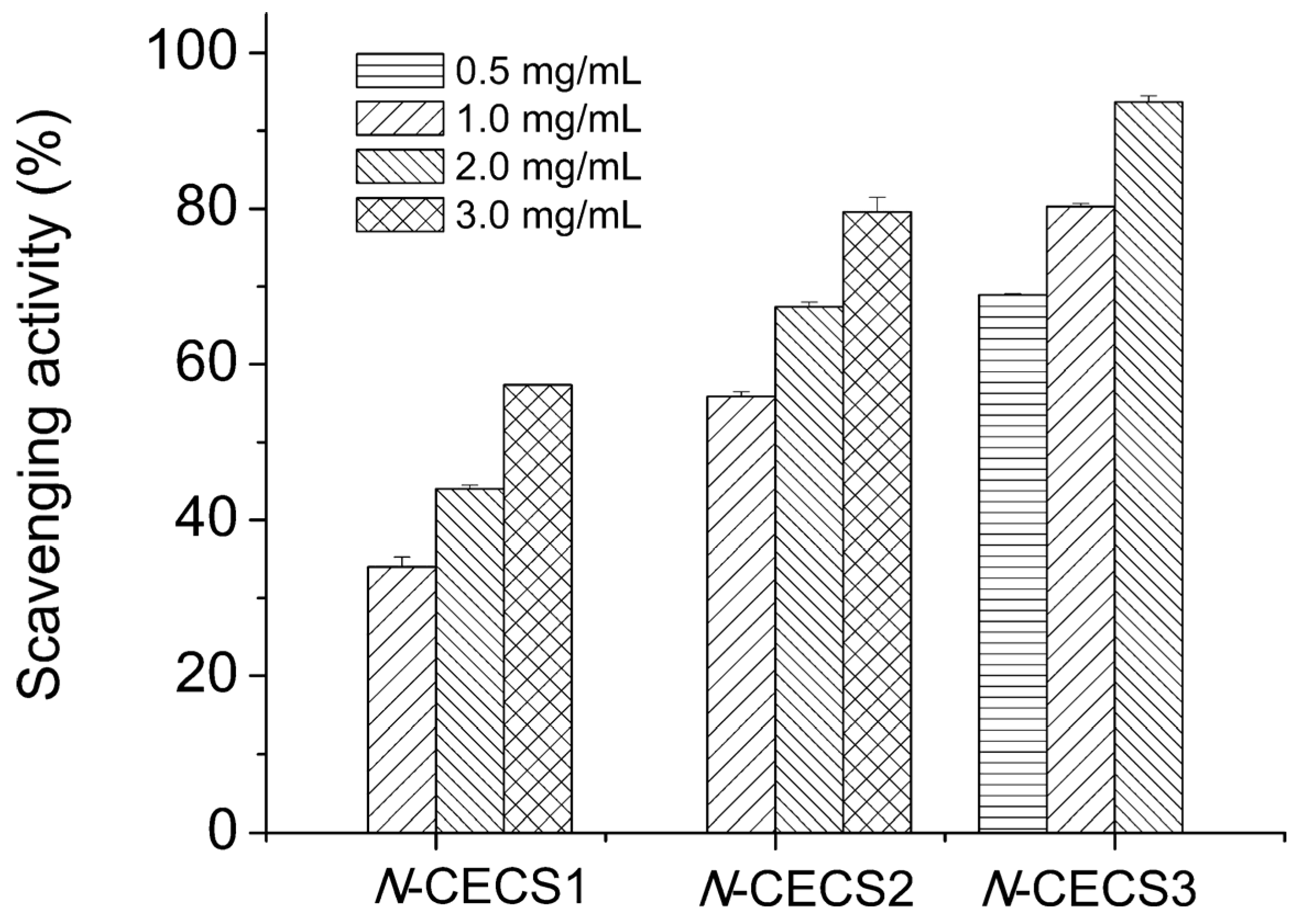
4. Applications
4.1. Tissue Engineering
4.2. Drug Delivery System
4.3. Wound Healing
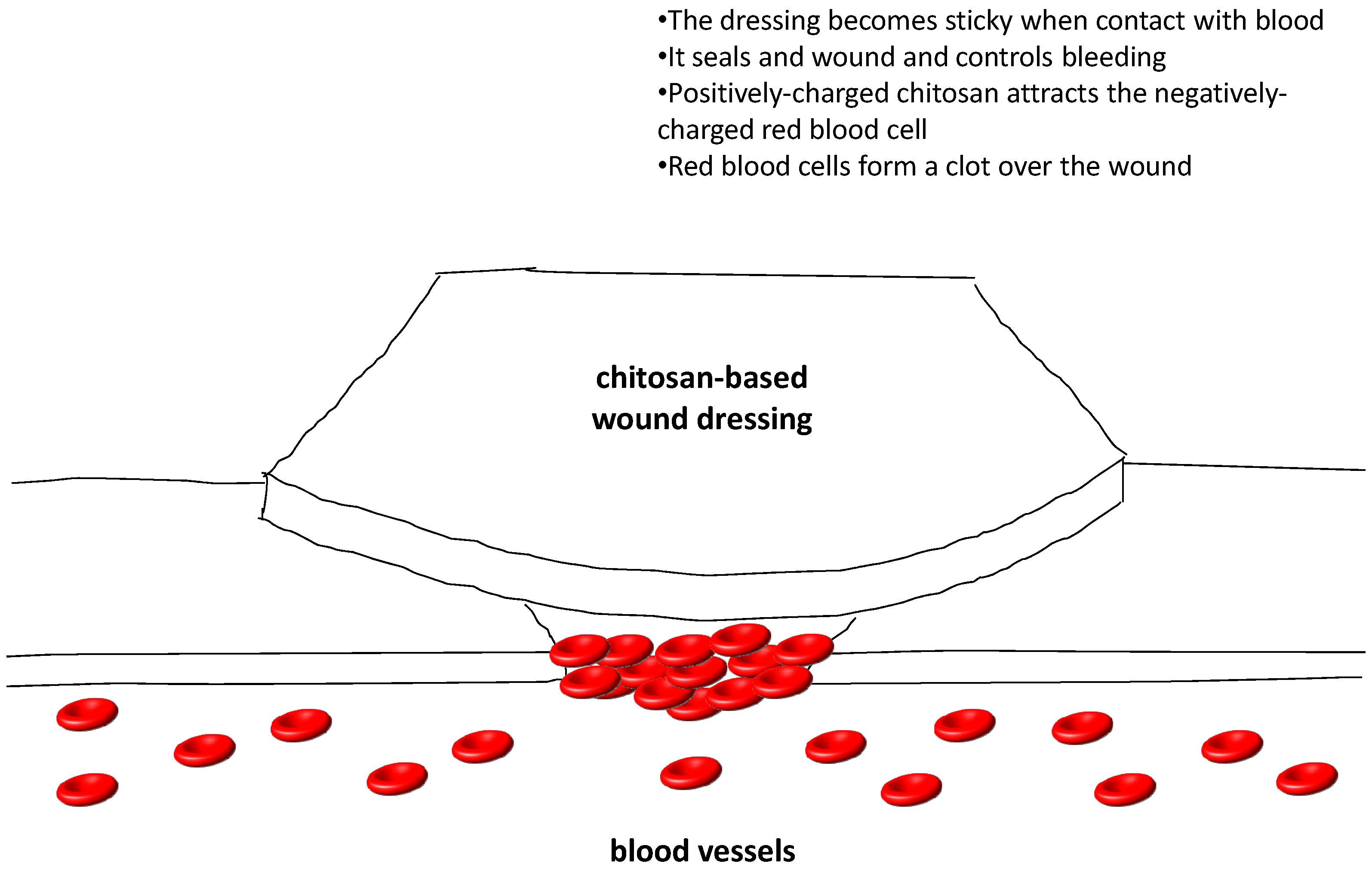
4.4. Water Treatment
4.5. Obesity Treatment
4.6. Other Applications
4.6.1. Cardiovascular Diseases Treatment
4.6.2. Treatment of Age-Related Diseases
4.6.3. Mucosal Immunity Enhancer
4.6.4. Dry Mouth Syndrome Treatment
4.6.5. Food Industry
4.6.6. Gene Silencing in Disease Vector Mosquito Larvae
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Chandy, T.; Sharma, C.P. Chitosan-as a biomaterial. Biomater. Artif. Cells Artif. Organs 1990, 18, 1–24. [Google Scholar] [CrossRef] [PubMed]
- Venkatesan, J.; Kim, S.K. Chitosan composites for bone tissue engineering—An overview. Mar. Drugs 2010, 8, 2252–2266. [Google Scholar] [CrossRef] [PubMed]
- Kumar, M.N.; Muzzarelli, R.A.; Muzzarelli, C.; Sashiwa, H.; Domb, A.J. Chitosan chemistry and pharmaceutical perspectives. Chem. Rev. 2004, 104, 6017–6084. [Google Scholar] [CrossRef] [PubMed]
- Karagozlu, M.Z.; Kim, S.-K. Chapter Twelve—Anticancer effects of chitin and chitosan derivatives. In Advances in Food and Nutrition Research; Kim, S.K., Ed.; Academic Press: Waltham, MA, USA, 2014; Volume 72, pp. 215–225. [Google Scholar]
- Martins, A.F.; Facchi, S.P.; Follmann, H.D.; Pereira, A.G.; Rubira, A.F.; Muniz, E.C. Antimicrobial activity of chitosan derivatives containing N-quaternized moieties in its backbone: a review. Int. J. Mol. Sci. 2014, 15, 20800–20832. [Google Scholar] [CrossRef] [PubMed]
- Ngo, D.H.; Kim, S.K. Chapter Two—Antioxidant effects of chitin, chitosan, and their derivatives. In Advances in Food and Nutrition Research; Kim, S.K., Ed.; Academic Press: Waltham, MA, USA, 2014; Volume 73, pp. 15–31. [Google Scholar]
- Aranaz, I.; Mengíbar, M.; Harris, R.; Paños, I.; Miralles, B.; Acosta, N.; Galed, G.; Heras, Á. Functional characterization of chitin and chitosan. Curr. Chem. Biol. 2009, 3, 203–230. [Google Scholar]
- Onsosyen, E.; Skaugrud, O. Metal recovery using chitosan. J. Chem. Technol. Biotechnol. 1990, 49, 395–404. [Google Scholar] [CrossRef]
- Felt, O.; Buri, P.; Gurny, R. Chitosan: A unique polysaccharide for drug delivery. Drug Dev. Ind. Pharm. 1998, 24, 979–993. [Google Scholar] [CrossRef] [PubMed]
- Han, L.K.; Kimura, Y.; Okuda, H. Reduction in fat storage during chitin-chitosan treatment in mice fed a high-fat diet. Int. J. Obes. Relat. Metab. Disord. 1999, 23, 174–179. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Zhang, M. Three-dimensional macroporous calcium phosphate bioceramics with nested chitosan sponges for load-bearing bone implants. J. Biomed. Mater. Res. 2002, 61, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Younes, I.; Rinaudo, M. Chitin and chitosan preparation from marine sources. Structure, properties and applications. Mar. Drugs 2015, 13, 1133–1174. [Google Scholar] [CrossRef] [PubMed]
- Percot, A.; Viton, C.; Domard, A. Optimization of chitin extraction from shrimp shells. Biomacromolecules 2003, 4, 12–18. [Google Scholar] [CrossRef] [PubMed]
- Jung, W.J.; Jo, G.H.; Kuk, J.H.; Kim, K.Y.; Park, R.D. Extraction of chitin from red crab shell waste by cofermentation with Lactobacillus paracasei subsp. tolerans KCTC-3074 and Serratia marcescens FS-3. Appl. Microbiol. Biotechnol. 2006, 71, 234–237. [Google Scholar] [CrossRef] [PubMed]
- Kafetzopoulos, D.; Martinou, A.; Bouriotis, V. Bioconversion of chitin to chitosan: Purification and characterization of chitin deacetylase from Mucor rouxii. Proc. Natl. Acad. Sci. USA 1993, 90, 2564–2568. [Google Scholar] [CrossRef] [PubMed]
- No, H.K.; Meyers, S.P. Preparation and characterization of chitin and chitosan—A review. J. Aquat. Food Prod. Technol. 1995, 4, 27–52. [Google Scholar] [CrossRef]
- Rege, P.R.; Block, L.H. Chitosan processing: Influence of process parameters during acidic and alkaline hydrolysis and effect of the processing sequence on the resultant chitosan’s properties. Carbohyd. Res. 1999, 321, 235–245. [Google Scholar] [CrossRef]
- Galed, G.; Miralles, B.; Inés Paños, I.; Santiago, A.; Heras, Á. N-Deacetylation and depolymerization reactions of chitin/chitosan: Influence of the source of chitin. Carbohyd. Polym. 2005, 62, 316–320. [Google Scholar] [CrossRef]
- Nwe, N.; Furuike, T.; Tamura, H. Chapter One—Isolation and characterization of chitin and chitosan from marine origin. In Advances in Food and Nutrition Research; Se-Kwon, K., Ed.; Academic Press: Waltham, MA, USA, 2014; Volume 72, pp. 1–15. [Google Scholar]
- Philippova, O.E.; Korchagina, E.V.; Volkov, E.V.; Smirnov, V.A.; Khokhlov, A.R.; Rinaudo, M. Aggregation of some water-soluble derivatives of chitin in aqueous solutions: Role of the degree of acetylation and effect of hydrogen bond breaker. Carbohyd. Polym. 2012, 87, 687–694. [Google Scholar] [CrossRef]
- Bhattarai, N.; Gunn, J.; Zhang, M. Chitosan-based hydrogels for controlled, localized drug delivery. Adv. Drug Deliv. Rev. 2010, 62, 83–99. [Google Scholar] [CrossRef] [PubMed]
- Tsao, C.T.; Leung, M.; Chang, J.Y.; Zhang, M. A simple material model to generate epidermal and dermal layers in vitro for skin regeneration. J. Mater. Chem. B Mater. Biol. Med. 2014, 2, 5256–5264. [Google Scholar] [CrossRef] [PubMed]
- Lindborg, B.A.; Brekke, J.H.; Scott, C.M.; Chai, Y.W.; Ulrich, C.; Sandquist, L.; Kokkoli, E.; O’Brien, T.D. A chitosan-hyaluronan-based hydrogel-hydrocolloid supports in vitro culture and differentiation of human mesenchymal stem/stromal cells. Tissue Eng. Part A 2015, 21, 1952–1962. [Google Scholar] [CrossRef] [PubMed]
- Salis, A.; Rassu, G.; Budai-Szucs, M.; Benzoni, I.; Csanyi, E.; Berko, S.; Maestri, M.; Dionigi, P.; Porcu, E.P.; Gavini, E.; et al. Development of thermosensitive chitosan/glicerophospate injectable in situ gelling solutions for potential application in intraoperative fluorescence imaging and local therapy of hepatocellular carcinoma: A preliminary study. Expert Opin. Drug Deliv. 2015, 2, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Rahaiee, S.; Shojaosadati, S.A.; Hashemi, M.; Moini, S.; Razavi, S.H. Improvement of crocin stability by biodegradeble nanoparticles of chitosan-alginate. Int. J. Biol. Macromol. 2015, 79, 423–432. [Google Scholar] [CrossRef] [PubMed]
- Zeng, W.; Rong, M.; Hu, X.; Xiao, W.; Qi, F.; Huang, J.; Luo, Z. Incorporation of chitosan microspheres into collagen-chitosan scaffolds for the controlled release of nerve growth factor. PLoS ONE 2014, 9, e101300. [Google Scholar] [CrossRef] [PubMed]
- Kiechel, M.A.; Beringer, L.T.; Donius, A.E.; Komiya, Y.; Habas, R.; Wegst, U.G.; Schauer, C.L. Osteoblast biocompatibility of premineralized, hexamethylene-1,6-diaminocarboxysulfonate cross-linked chitosan fibers. J. Biomed. Mater. Res. A 2015. [Google Scholar] [CrossRef] [PubMed]
- Kucharska, M.; Walenko, K.; Lewandowska-Szumiel, M.; Brynk, T.; Jaroszewicz, J.; Ciach, T. Chitosan and composite microsphere-based scaffold for bone tissue engineering: Evaluation of tricalcium phosphate content influence on physical and biological properties. J. Mater. Sci. Mater. Med. 2015, 26. [Google Scholar] [CrossRef] [PubMed]
- Venkatesan, J.; Vinodhini, P.A.; Sudha, P.N.; Kim, S.K. Chitin and chitosan composites for bone tissue regeneration. Adv. Food Nutr. Res. 2014, 73, 59–81. [Google Scholar] [PubMed]
- D’Ayala, G.G.; Malinconico, M.; Laurienzo, P. Marine derived polysaccharides for biomedical applications: Chemical modification approaches. Molecules 2008, 13, 2069–106. [Google Scholar] [CrossRef] [PubMed]
- Tan, L.; Hu, J.; Huang, H.; Han, J.; Hu, H. Study of multi-functional electrospun composite nanofibrous mats for smart wound healing. Int. J. Biol. Macromol. 2015, 79, 469–476. [Google Scholar] [CrossRef] [PubMed]
- Reddy, D.H.; Lee, S.M. Application of magnetic chitosan composites for the removal of toxic metal and dyes from aqueous solutions. Adv. Colloid Interface Sci. 2013, 201–202, 68–93. [Google Scholar] [CrossRef] [PubMed]
- Sudarshan, N.R.; Hoover, D.G.; Knorr, D. Antibacterial action of chitosan. Food Biotechnol. 1992, 6, 257–272. [Google Scholar] [CrossRef]
- Zheng, L.Y.; Zhu, J.F. Study on antimicrobial activity of chitosan with different molecular weights. Carbohyd. Polym. 2003, 54, 527–530. [Google Scholar] [CrossRef]
- Muzzarelli, R.; Tarsi, R.; Filippini, O.; Giovanetti, E.; Biagini, G.; Varaldo, P.E. Antimicrobial properties of N-carboxybutyl chitosan. Antimicrob. Agents Chemother. 1990, 34, 2019–2023. [Google Scholar] [CrossRef] [PubMed]
- Rhoades, J.; Roller, S. Antimicrobial actions of degraded and native chitosan against spoilage organisms in laboratory media and foods. Appl. Environ. Microbiol. 2000, 66, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Younes, I.; Sellimi, S.; Rinaudo, M.; Jellouli, K.; Nasri, M. Influence of acetylation degree and molecular weight of homogeneous chitosans on antibacterial and antifungal activities. Int. J. Food Microbiol. 2014, 185, 57–63. [Google Scholar] [CrossRef] [PubMed]
- Kong, M.; Chen, X.G.; Xing, K.; Park, H.J. Antimicrobial properties of chitosan and mode of action: A state of the art review. Int. J. Food Microbiol. 2010, 144, 51–63. [Google Scholar] [CrossRef] [PubMed]
- Mujeeb Rahman, P.; Muraleedaran, K.; Abdul Mujeeb, V.M. Applications of chitosan powder with in situ synthesized nano ZnO particles as an antimicrobial agent. Int. J. Biol. Macromol. 2015, 77, 266–272. [Google Scholar]
- Machul, A.; Mikolajczyk, D.; Regiel-Futyra, A.; Heczko, P.B.; Strus, M.; Arruebo, M.; Stochel, G.; Kyziol, A. Study on inhibitory activity of chitosan-based materials against biofilm producing Pseudomonas aeruginosa strains. J. Biomater. Appl. 2015. [Google Scholar] [CrossRef] [PubMed]
- Park, S.C.; Nam, J.P.; Kim, J.H.; Kim, Y.M.; Nah, J.W.; Jang, M.K. Antimicrobial action of water-soluble beta-chitosan against clinical multi-drug resistant bacteria. Int. J. Mol. Sci. 2015, 16, 7995–8007. [Google Scholar] [CrossRef] [PubMed]
- Fan, L.; Yang, J.; Wu, H.; Hu, Z.; Yi, J.; Tong, J.; Zhu, X. Preparation and characterization of quaternary ammonium chitosan hydrogels with significant antibacterial activity. Int. J. Biol. Macromol. 2015, 79, 830–836. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Peng, L. Antimicrobial and antioxidant surface modification of cellulose fibers using layer-by-layer deposition of chitosan and lignosulfonates. Carbohyd. Polym. 2015, 124, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Sahariah, P.; Benediktssdottir, B.E.; Hjalmarsdottir, M.A.; Sigurjonsson, O.E.; Sorensen, K.K.; Thygesen, M.B.; Jensen, K.J.; Masson, M. Impact of chain length on antibacterial activity and hemocompatibility of quaternary N-alkyl and n,n-dialkyl chitosan derivatives. Biomacromolecules 2015, 16, 1449–1460. [Google Scholar] [CrossRef] [PubMed]
- Sarhan, W.A.; Azzazy, H.M. High concentration honey chitosan electrospun nanofibers: Biocompatibility and antibacterial effects. Carbohydr. Polym. 2015, 122, 135–143. [Google Scholar] [CrossRef] [PubMed]
- Tayel, A.A.; Moussa, S.H.; Salem, M.F.; Mazrou, K.E.; El-Tras, W.F. Control of citrus molds using bioactive coatings incorporated with fungal chitosan/plant extracts composite. J. Sci. Food Agric. 2015. [Google Scholar] [CrossRef] [PubMed]
- Ben-Shalom, N.; Ardi, R.; Pinto, R.; Aki, C.; Fallik, E. Controlling gray mould caused by Botrytis cinerea in cucumber plants by means of chitosan. Crop. Prot. 2003, 22, 285–290. [Google Scholar] [CrossRef]
- Atia, M.M.M.; Buchenauer, H.; Aly, A.Z.; Abou-Zaid, M.I. Antifungal activity of chitosan against Phytophthora infestans and activation of defence mechanisms in tomato to late blight. Biol. Agric. Hortic. 2005, 23, 175–197. [Google Scholar] [CrossRef]
- Saharan, V.; Sharma, G.; Yadav, M.; Choudhary, M.K.; Sharma, S.S.; Pal, A.; Raliya, R.; Biswas, P. Synthesis and in vitro antifungal efficacy of Cu-chitosan nanoparticles against pathogenic fungi of tomato. Int. J. Biol. Macromol. 2015, 75, 346–353. [Google Scholar] [CrossRef] [PubMed]
- Bai, R.K.; Huang, M.Y.; Jiang, Y.Y. Selective permeabilities of chitosan-acetic acid complex membrane and chitosan-polymer complex membranes for oxygen and carbon dioxide. Polym. Bull. 1988, 20, 83–88. [Google Scholar] [CrossRef]
- Wang, L.S.; Wang, C.Y.; Yang, C.H.; Hsieh, C.L.; Chen, S.Y.; Shen, C.Y.; Wang, J.J.; Huang, K.S. Synthesis and anti-fungal effect of silver nanoparticles-chitosan composite particles. Int. J. Nanomedicine 2015, 10, 2685–2696. [Google Scholar] [PubMed]
- Lopez-Moya, F.; Colom-Valiente, M.F.; Martinez-Peinado, P.; Martinez-Lopez, J.E.; Puelles, E.; Sempere-Ortells, J.M.; Lopez-Llorca, L.V. Carbon and nitrogen limitation increase chitosan antifungal activity in Neurospora crassa and fungal human pathogens. Fungal Biol. 2015, 119, 154–169. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, S.; Chatterjee, B.P.; Guha, A.K. A study on antifungal activity of water-soluble chitosan against Macrophomina phaseolina. Int. J. Biol. Macromol. 2014, 67, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Simonaitiene, D.; Brink, I.; Sipailiene, A.; Leskauskaite, D. The effect of chitosan and whey proteins-chitosan films on the growth of Penicillium expansum in apples. J. Sci. Food Agric. 2015, 95, 1475–1481. [Google Scholar] [CrossRef] [PubMed]
- Gabriel Jdos, S.; Tiera, M.J.; Tiera, V.A. Synthesis, characterization, and antifungal activities of amphiphilic derivatives of diethylaminoethyl chitosan against Aspergillus flavus. J. Agric. Food Chem. 2015, 63, 5725–5731. [Google Scholar] [CrossRef] [PubMed]
- Karagozlu, M.Z.; Karadeniz, F.; Kim, S.K. Anti-HIV activities of novel synthetic peptide conjugated chitosan oligomers. Int. J. Biol. Macromol. 2014, 66, 260–266. [Google Scholar] [CrossRef] [PubMed]
- Artan, M.; Karadeniz, F.; Karagozlu, M.Z.; Kim, M.M.; Kim, S.K. Anti-HIV-1 activity of low molecular weight sulfated chitooligosaccharides. Carbohydr. Res. 2010, 345, 656–662. [Google Scholar] [CrossRef] [PubMed]
- Meng, J.; Zhang, T.; Agrahari, V.; Ezoulin, M.J.; Youan, B.B. Comparative biophysical properties of tenofovir-loaded, thiolated and nonthiolated chitosan nanoparticles intended for HIV prevention. Nanomedicine. (Lond.) 2014, 9, 1595–1612. [Google Scholar] [CrossRef] [PubMed]
- Aghasadeghi, M.R.; Heidari, H.; Sadat, S.M.; Irani, S.; Amini, S.; Siadat, S.D.; Fazlhashemy, M.E.; Zabihollahi, R.; Atyabi, S.M.; Momen, S.B.; et al. Lamivudine-PEGylated chitosan: A novel effective nanosized antiretroviral agent. Curr. HIV Res. 2013, 11, 309–320. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.B.; Thakur, R.S. Formulation and evaluation of mucoadhesive microspheres of tenofovir disoproxil fumarate for intravaginal use. Curr. Drug Deliv. 2014, 11, 112–122. [Google Scholar] [CrossRef] [PubMed]
- Ramana, L.N.; Sharma, S.; Sethuraman, S.; Ranga, U.; Krishnan, U.M. Evaluation of chitosan nanoformulations as potent anti-HIV therapeutic systems. Biochim. Biophys. Acta. 2014, 1840, 476–484. [Google Scholar] [CrossRef] [PubMed]
- Belletti, D.; Tosi, G.; Forni, F.; Gamberini, M.C.; Baraldi, C.; Vandelli, M.A.; Ruozi, B. Chemico-physical investigation of tenofovir loaded polymeric nanoparticles. Int. J. Pharm. 2012, 436, 753–763. [Google Scholar] [CrossRef] [PubMed]
- Meng, J.; Sturgis, T.F.; Youan, B.B. Engineering tenofovir loaded chitosan nanoparticles to maximize microbicide mucoadhesion. Eur. J. Pharm. Sci. 2011, 44, 57–67. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Chen, L.; Zeng, R.; Li, C.; Qiao, R.; Hu, L.; Li, Z. Synthesis, nanosizing and in vitro drug release of a novel anti-HIV polymeric prodrug: Chitosan-O-isopropyl-5′-O-d4T monophosphate conjugate. Bioorg. Med. Chem. 2010, 18, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Nayak, U.Y.; Gopal, S.; Mutalik, S.; Ranjith, A.K.; Reddy, M.S.; Gupta, P.; Udupa, N. Glutaraldehyde cross-linked chitosan microspheres for controlled delivery of zidovudine. J. Microencapsul. 2009, 26, 214–222. [Google Scholar] [CrossRef] [PubMed]
- Tokoro, A.; Tatewaki, N.; Suzuki, K.; Mikami, T.; Suzuki, S.; Suzuki, M. Growth-inhibitory effect of hexa-N-acetylchitohexaose and chitohexaose against Meth-A solid tumor. Chem. Pharm. Bull. (Tokyo) 1988, 36, 784–790. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.Y.; Chan, H.Y.; Shen, F.H.; Chen, M.H.; Wang, Y.J.; Yu, C.K. Chitosan prevents the development of AOM-induced aberrant crypt foci in mice and suppressed the proliferation of AGS cells by inhibiting DNA synthesis. J. Cell Biochem. 2007, 100, 1573–1580. [Google Scholar] [CrossRef] [PubMed]
- Gibot, L.; Chabaud, S.; Bouhout, S.; Bolduc, S.; Auger, F.A.; Moulin, V.J. Anticancer properties of chitosan on human melanoma are cell line dependent. Int. J. Biol. Macromol. 2015, 72, 370–379. [Google Scholar] [CrossRef] [PubMed]
- He, B.; Tao, H.Y.; Liu, S.Q. Neuroprotective effects of carboxymethylated chitosan on hydrogen peroxide induced apoptosis in Schwann cells. Eur. J. Pharmacol. 2014, 740, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Z.; Han, B.; Li, H.; Li, X.; Yang, Y.; Liu, W. Preparation and anti-tumor metastasis of carboxymethyl chitosan. Carbohydr. Polym. 2015, 125, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Park, J.K.; Chung, M.J.; Choi, H.N.; Park, Y.I. Effects of the molecular weight and the degree of deacetylation of chitosan oligosaccharides on antitumor activity. Int. J. Mol. Sci. 2011, 12, 266–277. [Google Scholar] [CrossRef] [PubMed]
- Shen, K.T.; Chen, M.H.; Chan, H.Y.; Jeng, J.H.; Wang, Y.J. Inhibitory effects of chitooligosaccharides on tumor growth and metastasis. Food Chem. Toxicol. 2009, 47, 1864–1871. [Google Scholar] [CrossRef] [PubMed]
- Park, P.J.; Je, J.Y.; Kim, S.K. Free radical scavenging activity of chitooligosaccharides by electron spin resonance spectrometry. J. Agric. Food Chem. 2003, 51, 4624–4627. [Google Scholar] [CrossRef] [PubMed]
- Je, J.Y.; Park, P.J.; Kim, S.K. Free radical scavenging properties of hetero-chitooligosaccharides using an ESR spectroscopy. Food Chem. Toxicol. 2004, 42, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.; Xie, H.; Hu, S.; Xie, T.; Gong, J.; Jiang, C.; Ge, Q.; Wu, Y.; Liu, S.; Cui, Y.; et al. Preparation, characterization, and biochemical activities of N-(2-Carboxyethyl)chitosan from squid pens. J. Agric. Food Chem. 2015, 63, 2464–2471. [Google Scholar] [CrossRef] [PubMed]
- Sun, T.; Xie, W.; Xu, P. Antioxidant activity of graft chitosan derivatives. Macromol. Biosci. 2003, 3, 320–323. [Google Scholar] [CrossRef]
- Shukla, S.K.; Mishra, A.K.; Arotiba, O.A.; Mamba, B.B. Chitosan-based nanomaterials: A state-of-the-art review. Int. J. Biol. Macromol. 2013, 59, 46–58. [Google Scholar] [CrossRef] [PubMed]
- Kim, I.Y.; Seo, S.J.; Moon, H.S.; Yoo, M.K.; Park, I.Y.; Kim, B.C.; Cho, C.S. Chitosan and its derivatives for tissue engineering applications. Biotechnol. Adv. 2008, 26, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Li, B.; Wang, L.; Xu, F.; Gang, X.; Demirci, U.; Wei, D.; Li, Y.; Feng, Y.; Jia, D.; Zhou, Y. Hydrosoluble, UV-crosslinkable and injectable chitosan for patterned cell-laden microgel and rapid transdermal curing hydrogel in vivo. Acta. Biomater. 2015, 22, 59–69. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Wang, Q.; Peng, L.; Yue, H.; Zhang, Z. Vascularization of repaired limb bone defects using chitosan-β-tricalcium phosphate composite as a tissue engineering bone scaffold. Mol. Med. Rep. 2015, 12, 2343–2347. [Google Scholar] [CrossRef] [PubMed]
- Chameettachal, S.; Murab, S.; Vaid, R.; Midha, S.; Ghosh, S. Effect of visco-elastic silk-chitosan microcomposite scaffolds on matrix deposition and biomechanical functionality for cartilage tissue engineering. J. Tissue Eng. Regen. Med. 2015. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Zhou, G.; Yu, X.; Wang, T.; Xi, Y.; Tang, Z. Porous deproteinized bovine bone scaffold with three-dimensional localized drug delivery system using chitosan microspheres. Biomed. Eng. OnLine 2015, 14. [Google Scholar] [CrossRef] [PubMed]
- Shapira, Y.; Tolmasov, M.; Nissan, M.; Reider, E.; Koren, A.; Biron, T.; Bitan, Y.; Livnat, M.; Ronchi, G.; Geuna, S.; et al. Comparison of results between chitosan hollow tube and autologous nerve graft in reconstruction of peripheral nerve defect: An experimental study. Microsurgery 2015. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, N.; Matsumoto, I.; Suzuki, M.; Kaneko, M.; Nitta, K.; Seguchi, R.; Ooi, A.; Takemura, H. Chitosan tubes can restore the function of resected phrenic nerves. Interact. Cardiovasc. Thorac. Surg. 2015, 21, 8–13. [Google Scholar] [CrossRef] [PubMed]
- Jian, R.; Yixu, Y.; Sheyu, L.; Jianhong, S.; Yaohua, Y.; Xing, S.; Qingfeng, H.; Xiaojian, L.; Lei, Z.; Yan, Z.; et al. Repair of spinal cord injury by chitosan scaffold with glioma ECM and SB216763 implantation in adult rats. J. Biomed. Mater. Res. A 2015. [Google Scholar] [CrossRef] [PubMed]
- Correia, C.O.; Leite, A.J.; Mano, J.F. Chitosan/bioactive glass nanoparticles scaffolds with shape memory properties. Carbohydr. Polym. 2015, 123, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Jabbal-Gill, I.; Watts, P.; Smith, A. Chitosan-based delivery systems for mucosal vaccines. Expert Opin. Drug Deliv. 2012, 9, 1051–1067. [Google Scholar] [CrossRef] [PubMed]
- Kofuji, K.; Qian, C.J.; Nishimura, M.; Sugiyama, I.; Murata, Y.; Kawashima, S. Relationship between physicochemical characteristics and functional properties of chitosan. Eur. Polym. J. 2005, 41, 2784–2791. [Google Scholar] [CrossRef]
- Jiang, H.L.; Park, I.K.; Shin, N.R.; Kang, S.G.; Yoo, H.S.; Kim, S.I.; Suh, S.B.; Akaike, T.; Cho, C.S. In vitro study of the immune stimulating activity of an atrophic rhinitis vaccine associated to chitosan microspheres. Eur. J. Pharm. Biopharm. 2004, 58, 471–476. [Google Scholar] [CrossRef] [PubMed]
- Borchard, G.; Lueβen, H.L.; de Boer, A.G.; Verhoef, J.C.; Lehr, C.M.; Junginger, H.E. The potential of mucoadhesive polymers in enhancing intestinal peptide drug absorption. III: Effects of chitosan-glutamate and carbomer on epithelial tight junctions in vitro. J. Control. Release 1996, 39, 131–138. [Google Scholar] [CrossRef]
- Thanou, M.; Verhoef, J.C.; Junginger, H.E. Oral drug absorption enhancement by chitosan and its derivatives. Adv. Drug Deliv. Rev. 2001, 52, 117–126. [Google Scholar] [CrossRef]
- Elsabee, M.Z.; Morsi, R.E.; Al-Sabagh, A.M. Surface active properties of chitosan and its derivatives. Colloids Surf. B Biointerfaces 2009, 74, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Harada, A.; Kataoka, K. Formation of polyion complex micelles in an aqueous milieu from a pair of oppositely-charged block copolymers with poly(ethylene glycol) segments. Macromolecules 1995, 28, 5294–5299. [Google Scholar] [CrossRef]
- Supper, S.; Anton, N.; Boisclair, J.; Seidel, N.; Riemenschnitter, M.; Curdy, C.; Vandamme, T. Chitosan/glucose 1-phosphate as new stable in situ forming depot system for controlled drug delivery. Eur. J. Pharm. Biopharm. 2014, 88, 361–373. [Google Scholar] [CrossRef] [PubMed]
- Supper, S.; Anton, N.; Seidel, N.; Riemenschnitter, M.; Curdy, C.; Vandamme, T. Thermosensitive chitosan/glycerophosphate-based hydrogel and its derivatives in pharmaceutical and biomedical applications. Expert Opin. Drug Deliv. 2014, 11, 249–267. [Google Scholar] [CrossRef] [PubMed]
- Lai, P.; Daear, W.; Lobenberg, R.; Prenner, E.J. Overview of the preparation of organic polymeric nanoparticles for drug delivery based on gelatine, chitosan, poly(d,l-lactide-co-glycolic acid) and polyalkylcyanoacrylate. Colloids Surf. B Biointerfaces 2014, 118, 154–163. [Google Scholar] [CrossRef] [PubMed]
- Hudson, D.; Margaritis, A. Biopolymer nanoparticle production for controlled release of biopharmaceuticals. Crit. Rev. Biotechnol. 2014, 34, 161–179. [Google Scholar] [CrossRef] [PubMed]
- Calvo, P.; Remuñán-López, C.; Vila-Jato, J.L.; Alonso, M.J. Novel hydrophilic chitosan-polyethylene oxide nanoparticles as protein carriers. J. Appl. Polym. Sci. 1997, 63, 125–132. [Google Scholar] [CrossRef]
- Kato, Y.; Onishi, H.; Machida, Y. Contribution of chitosan and its derivatives to cancer chemotherapy. In Vivo 2005, 19, 301–310. [Google Scholar] [PubMed]
- Anraku, M.; Hiraga, A.; Iohara, D.; Pipkin, J.D.; Uekama, K.; Hirayama, F. Slow-release of famotidine from tablets consisting of chitosan/sulfobutyl ether beta-cyclodextrin composites. Int. J. Pharm 2015, 487, 142–147. [Google Scholar] [CrossRef] [PubMed]
- Pereira, P.; Pedrosa, S.S.; Wymant, J.M.; Sayers, E.; Correia, A.; Vilanova, M.; Jones, A.T.; Gama, F.M. siRNA inhibition of endocytic pathways to characterize the cellular uptake mechanisms of folate-functionalized glycol chitosan nanogels. Mol. Pharm. 2015, 12, 1970–1979. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, N.; Wakte, P.; Naik, J. Development of floating chitosan-xanthan beads for oral controlled release of glipizide. Int. J. Pharm. Investig. 2015, 5, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Al-Kurdi, Z.I.; Chowdhry, B.Z.; Leharne, S.A.; Al Omari, M.M.; Badwan, A.A. Low molecular weight chitosan-insulin polyelectrolyte complex: Characterization and stability studies. Mar. Drugs 2015, 13, 1765–1784. [Google Scholar] [CrossRef] [PubMed]
- Gadalla, H.H.; Soliman, G.M.; Mohammed, F.A.; El-Sayed, A.M. Development and in vitro/in vivo evaluation of Zn-pectinate microparticles reinforced with chitosan for the colonic delivery of progesterone. Drug Deliv. 2015, 8, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Jana, S.; Laha, B.; Maiti, S. Boswellia gum resin/chitosan polymer composites: Controlled delivery vehicles for aceclofenac. Int. J. Biol. Macromol. 2015, 77, 303–306. [Google Scholar] [CrossRef] [PubMed]
- Qinna, N.A.; Karwi, Q.G.; Al-Jbour, N.; Al-Remawi, M.A.; Alhussainy, T.M.; Al-So’ud, K.A.; Al Omari, M.M.; Badwan, A.A. Influence of molecular weight and degree of deacetylation of low molecular weight chitosan on the bioactivity of oral insulin preparations. Mar. Drugs 2015, 13, 1710–1725. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Ryu, J.H.; Lee, H. Chitosan-catechol: A polymer with long-lasting mucoadhesive properties. Biomaterials 2015, 52, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, S.; Judeh, Z.M. A. Encapsulation of fish oil with N-stearoyl O-butylglyceryl chitosan using membrane and ultrasonic emulsification processes. Carbohyd. Polym. 2015, 123, 432–442. [Google Scholar] [CrossRef] [PubMed]
- Jayasree, R.S.; Rathinam, K.; Sharma, C.P. Development of artificial skin (Template) and influence of different types of sterilization procedures on wound healing pattern in rabbits and guinea pigs. J. Biomater. Appl. 1995, 10, 144–162. [Google Scholar] [PubMed]
- Ueno, H.; Mori, T.; Fujinaga, T. Topical formulations and wound healing applications of chitosan. Adv. Drug Deliv. Rev. 2001, 52, 105–115. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.; Mattioli-Belmonte, M.; Pugnaloni, A.; Biagini, G. Biochemistry, histology and clinical uses of chitins and chitosans in wound healing. EXS 1999, 87, 251–264. [Google Scholar] [PubMed]
- Azuma, K.; Izumi, R.; Osaki, T.; Ifuku, S.; Morimoto, M.; Saimoto, H.; Minami, S.; Okamoto, Y. Chitin, chitosan, and its derivatives for wound healing: Old and new materials. J. Funct. Biomater. 2015, 6, 104–142. [Google Scholar] [CrossRef] [PubMed]
- Naseri, N.; Algan, C.; Jacobs, V.; John, M.; Oksman, K.; Mathew, A.P. Electrospun chitosan-based nanocomposite mats reinforced with chitin nanocrystals for wound dressing. Carbohydr. Polym. 2014, 109, 7–15. [Google Scholar] [CrossRef] [PubMed]
- Ishihara, M.; Obara, K.; Nakamura, S.; Fujita, M.; Masuoka, K.; Kanatani, Y.; Takase, B.; Hattori, H.; Morimoto, Y.; Ishihara, M.; et al. Chitosan hydrogel as a drug delivery carrier to control angiogenesis. J. Artif. Organs 2006, 9, 8–16. [Google Scholar] [CrossRef] [PubMed]
- Biagini, G.; Bertani, A.; Muzzarelli, R.; Damadei, A.; DiBenedetto, G.; Belligolli, A.; Riccotti, G.; Zucchini, C.; Rizzoli, C. Wound management with N-carboxybutyl chitosan. Biomaterials 1991, 12, 281–286. [Google Scholar] [CrossRef]
- Stone, C.A.; Wright, H.; Devaraj, V.S.; Clarke, T.; Powell, R. Healing at skin graft donor sites dressed with chitosan. Br. J. Plast. Surg. 2000, 53, 601–606. [Google Scholar] [CrossRef] [PubMed]
- Azad, A.K.; Sermsintham, N.; Chandrkrachang, S.; Stevens, W.F. Chitosan membrane as a wound-healing dressing: Characterization and clinical application. J. Biomed. Mater. Res. B Appl. Biomater. 2004, 69, 216–222. [Google Scholar] [CrossRef] [PubMed]
- Valentine, R.; Athanasiadis, T.; Moratti, S.; Hanton, L.; Robinson, S.; Wormald, P.J. The efficacy of a novel chitosan gel on hemostasis and wound healing after endoscopic sinus surgery. Am. J. Rhinol. Allergy 2010, 24, 70–75. [Google Scholar] [CrossRef] [PubMed]
- Bennett, B.L.; Littlejohn, L.F.; Kheirabadi, B.S.; Butler, F.K.; Kotwal, R.S.; Dubick, M.A.; Bailey, J.A. Management of external hemorrhage in tactical combat casualty care: Chitosan-based hemostatic gauze dressings—TCCC guidelines-change 13-05. J. Spec. Oper. Med. 2014, 14, 40–57. [Google Scholar] [PubMed]
- Hatamabadi, H.R.; Asayesh Zarchi, F.; Kariman, H.; Arhami Dolatabadi, A.; Tabatabaey, A.; Amini, A. Celox-coated gauze for the treatment of civilian penetrating trauma: A randomized clinical trial. Trauma Mon. 2015, 20, e23862. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, N.; Hasan, S.; Caufield, L.; Ling, F.S.; Narins, C.R. Randomized controlled trial of topical hemostasis pad use for achieving vascular hemostasis following percutaneous coronary intervention. Catheter. Cardiovasc. Interv. 2007, 69, 801–807. [Google Scholar] [CrossRef] [PubMed]
- Weng, M.H. The effect of protective treatment in reducing pressure ulcers for non-invasive ventilation patients. Intensive Crit. Care Nurs. 2008, 24, 295–259. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.; Zhou, W.; Wei, B.; Wang, X.; Tang, R.; Nie, J.; Wang, J. Carboxyl-modified poly(vinyl alcohol)-cross-linked chitosan hydrogel films for potential wound dressing. Carbohydr. Polym. 2015, 125, 189–199. [Google Scholar] [CrossRef] [PubMed]
- Jebahi, S.; Saoudi, M.; Farhat, L.; Oudadesse, H.; Rebai, T.; Kabir, A.; El Feki, A.; Keskes, H. Effect of novel curcumin-encapsulated chitosan-bioglass drug on bone and skin repair after gamma radiation: Experimental study on a Wistar rat model. Cell Biochem. Funct. 2015, 33, 150–159. [Google Scholar] [CrossRef] [PubMed]
- Vakili, M.; Rafatullah, M.; Salamatinia, B.; Abdullah, A.Z.; Ibrahim, M.H.; Tan, K.B.; Gholami, Z.; Amouzgar, P. Application of chitosan and its derivatives as adsorbents for dye removal from water and wastewater: A review. Carbohyd. Polym. 2014, 113, 115–130. [Google Scholar] [CrossRef] [PubMed]
- Boamah, P.O.; Huang, Y.; Hua, M.; Zhang, Q.; Wu, J.; Onumah, J.; Sam-Amoah, L.K. Sorption of heavy metal ions onto carboxylate chitosan derivatives-A mini-review. Ecotoxicol. Environ. Saf. 2015, 116, 113–120. [Google Scholar] [CrossRef] [PubMed]
- Tran, V.S.; Ngo, H.H.; Guo, W.; Zhang, J.; Liang, S.; Ton-That, C.; Zhang, X. Typical low cost biosorbents for adsorptive removal of specific organic pollutants from water. Bioresour. Technol. 2015, 182, 353–363. [Google Scholar] [CrossRef] [PubMed]
- Kyzas, G.Z.; Bikiaris, D.N. Recent modifications of chitosan for adsorption applications: A critical and systematic review. Mar. Drugs 2015, 13, 312–337. [Google Scholar] [CrossRef] [PubMed]
- Yong, S.K.; Shrivastava, M.; Srivastava, P.; Kunhikrishnan, A.; Bolan, N. Environmental applications of chitosan and its derivatives. Rev. Environ. Contam. Toxicol. 2015, 233, 1–43. [Google Scholar] [PubMed]
- Sayed, S.; Jardine, A. Chitosan derivatives as important biorefinery intermediates. Quaternary tetraalkylammonium chitosan derivatives utilized in anion exchange chromatography for perchlorate removal. Int. J. Mol. Sci. 2015, 16, 9064–9077. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Chen, N.; Tang, Z.; Yu, Y.; Hu, Q.; Feng, C. A study of the mechanism of fluoride adsorption from aqueous solutions onto Fe-impregnated chitosan. Phys. Chem. Chem. Phys. 2015, 17, 12041–12050. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Shi, L.; Gao, L.; Wei, Q.; Cui, L.; Hu, L.; Yan, L.; Du, B. The removal of lead ions from aqueous solution by using magnetic hydroxypropyl chitosan/oxidized multiwalled carbon nanotubes composites. J. Colloid Interface Sci. 2015, 451, 7–14. [Google Scholar] [CrossRef] [PubMed]
- Prabhu, S.M.; Meenakshi, S. A dendrimer-like hyper branched chitosan beads toward fluoride adsorption from water. Int. J. Biol. Macromol. 2015, 78, 280–286. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Li, Y.; Cao, L.; Yang, C. Enhanced chromium (VI) adsorption using nanosized chitosan fibers tailored by electrospinning. Carbohyd. Polym. 2015, 125, 206–213. [Google Scholar] [CrossRef] [PubMed]
- Kimura, Y.; Takahashi, A.; Kashiwada, A.; Yamada, K. Removal of bisphenol derivatives through quinone oxidation by polyphenol oxidase and subsequent quinone adsorption on chitosan in the heterogeneous system. Environ. Technol. 2015, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Boamah, P.O.; Huang, Y.; Hua, M.; Zhang, Q.; Liu, Y.; Onumah, J.; Wang, W.; Song, Y. Removal of cadmium from aqueous solution using low molecular weight chitosan derivative. Carbohyd. Polym. 2015, 122, 255–264. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Pan, G. Simultaneous removal of harmful algal blooms and microcystins using microorganism- and chitosan-modified local Soil. Environ. Sci. Technol. 2015, 49, 6249–6256. [Google Scholar] [CrossRef] [PubMed]
- Sivakami, M.S.; Gomathi, T.; Venkatesan, J.; Jeong, H.S.; Kim, S.K.; Sudha, P.N. Preparation and characterization of nano chitosan for treatment wastewaters. Int. J. Biol. Macromol. 2013, 57, 204–212. [Google Scholar] [CrossRef] [PubMed]
- Heber, D. Herbal preparations for obesity: Are they useful? Prim. Care 2003, 30, 441–463. [Google Scholar] [CrossRef]
- Ylitalo, R.; Lehtinen, S.; Wuolijoki, E.; Ylitalo, P.; Lehtimaki, T. Cholesterol-lowering properties and safety of chitosan. Arzneimittelforschung 2002, 52, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Gallaher, D.D.; Gallaher, C.M.; Mahrt, G.J.; Carr, T.P.; Hollingshead, C.H.; Hesslink, R., Jr.; Wise, J. A glucomannan and chitosan fiber supplement decreases plasma cholesterol and increases cholesterol excretion in overweight normocholesterolemic humans. J. Am. Coll. Nutr. 2002, 21, 428–433. [Google Scholar] [CrossRef] [PubMed]
- Maezaki, Y.; Tsuji, K.; Nakagawa, Y.; Kawai, Y.; Akimoto, M.; Tsugita, T.; Takekawa, W.; Terada, A.; Hara, H.; Mitsuoka, T. Hypocholesterolemic effect of chitosan in adult males. Biosci. Biotechnol. Biochem. 1993, 57, 1439–1444. [Google Scholar] [CrossRef]
- Wuolijoki, E.; Hirvela, T.; Ylitalo, P. Decrease in serum LDL cholesterol with microcrystalline chitosan. Methods Find. Exp. Clin. Pharmacol. 1999, 21, 357–361. [Google Scholar] [CrossRef] [PubMed]
- Hernández-González, S.O.; Manuel González-Ortiz, M.; Martínez-Abundis, E.; Robles-Cervantes, J.A. Chitosan improves insulin sensitivity as determined by the euglycemic-hyperinsulinemic clamp technique in obese subjects. Nutr. Res. 2010, 30, 392–395. [Google Scholar] [CrossRef] [PubMed]
- Pittler, M.H.; Abbot, N.C.; Harkness, E.F.; Ernst, E. Randomized, double-blind trial of chitosan for body weight reduction. Eur. J. Clin. Nutr. 1999, 53, 379–381. [Google Scholar] [CrossRef] [PubMed]
- Mhurchu, C.N.; Poppitt, S.D.; McGill, A.T.; Leahy, F.E.; Bennett, D.A.; Lin, R.B.; Ormrod, D.; Ward, L.; Strik, C.; Rodgers, A. The effect of the dietary supplement, chitosan, on body weight: A randomised controlled trial in 250 overweight and obese adults. Int. J. Obes. Relat. Metab. Disord. 2004, 28, 1149–1156. [Google Scholar] [CrossRef] [PubMed]
- Egras, A.M.; Hamilton, W.R.; Lenz, T.L.; Monaghan, M.S. An evidence-based review of fat modifying supplemental weight loss products. J. Obes. 2011. [Google Scholar] [CrossRef] [PubMed]
- Yu, Y.; Luo, T.; Liu, S.; Song, G.; Han, J.; Wang, Y.; Yao, S.; Feng, L.; Qin, S. Chitosan oligosaccharides attenuate atherosclerosis and decrease non-HDL in apoE-/- mice. J. Atheroscler. Thromb. 2015. [Google Scholar] [CrossRef] [PubMed]
- Kerch, G. The potential of chitosan and its derivatives in prevention and treatment of age-related diseases. Mar. Drugs 2015, 13, 2158–2182. [Google Scholar] [CrossRef] [PubMed]
- Bento, D.; Staats, H.F.; Gonçalves, T.; Borges, O. Development of a novel adjuvanted nasal vaccine: C48/80 associated with chitosan nanoparticles as a path to enhance mucosal immunity. Eur. J. Pharm. Biopharm. 2015, 93, 149–164. [Google Scholar] [CrossRef] [PubMed]
- Laffleur, F.; Fischer, A.; Schmutzler, M.; Hintzen, F.; Bernkop-Schnürch, A. Evaluation of functional characteristics of preactivated thiolated chitosan as potential therapeutic agent for dry mouth syndrome. Acta Biomater. 2015, 21, 123–131. [Google Scholar] [CrossRef] [PubMed]
- Gudjónsdóttir, M.; Gacutan, M.D., Jr.; Mendes, A.C.; Chronakis, I.S.; Jespersen, L.; Karlsson, A.H. Effects of electrospun chitosan wrapping for dry-ageing of beef, as studied by microbiological, physicochemical and low-field nuclear magnetic resonance analysis. Food Chem. 2015, 184, 167–175. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Mysore, K.; Flannery, E.; Michel, K.; Severson, D.W.; Zhu, K.Y.; Duman-Scheel, M. Chitosan/Interfering RNA nanoparticle mediated gene silencing in disease vector mosquito larvae. J. Vis. Exp. 2015. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cheung, R.C.F.; Ng, T.B.; Wong, J.H.; Chan, W.Y. Chitosan: An Update on Potential Biomedical and Pharmaceutical Applications. Mar. Drugs 2015, 13, 5156-5186. https://doi.org/10.3390/md13085156
Cheung RCF, Ng TB, Wong JH, Chan WY. Chitosan: An Update on Potential Biomedical and Pharmaceutical Applications. Marine Drugs. 2015; 13(8):5156-5186. https://doi.org/10.3390/md13085156
Chicago/Turabian StyleCheung, Randy Chi Fai, Tzi Bun Ng, Jack Ho Wong, and Wai Yee Chan. 2015. "Chitosan: An Update on Potential Biomedical and Pharmaceutical Applications" Marine Drugs 13, no. 8: 5156-5186. https://doi.org/10.3390/md13085156
APA StyleCheung, R. C. F., Ng, T. B., Wong, J. H., & Chan, W. Y. (2015). Chitosan: An Update on Potential Biomedical and Pharmaceutical Applications. Marine Drugs, 13(8), 5156-5186. https://doi.org/10.3390/md13085156





